Cervical Incompetence & Placenta Previa
1/67
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
68 Terms
Transabdominal cervical length measurement requires what condition
Full bladder
When should you switch from transabdominal to transvaginal cervical measurement
When cervical length is < 2.5 cm
If a provider specifically orders cervical length, which method must be used
Transvaginal ultrasound
Gold standard method for evaluating cervical length
Transvaginal ultrasound
What landmarks are used to measure cervical length
Internal os to external os
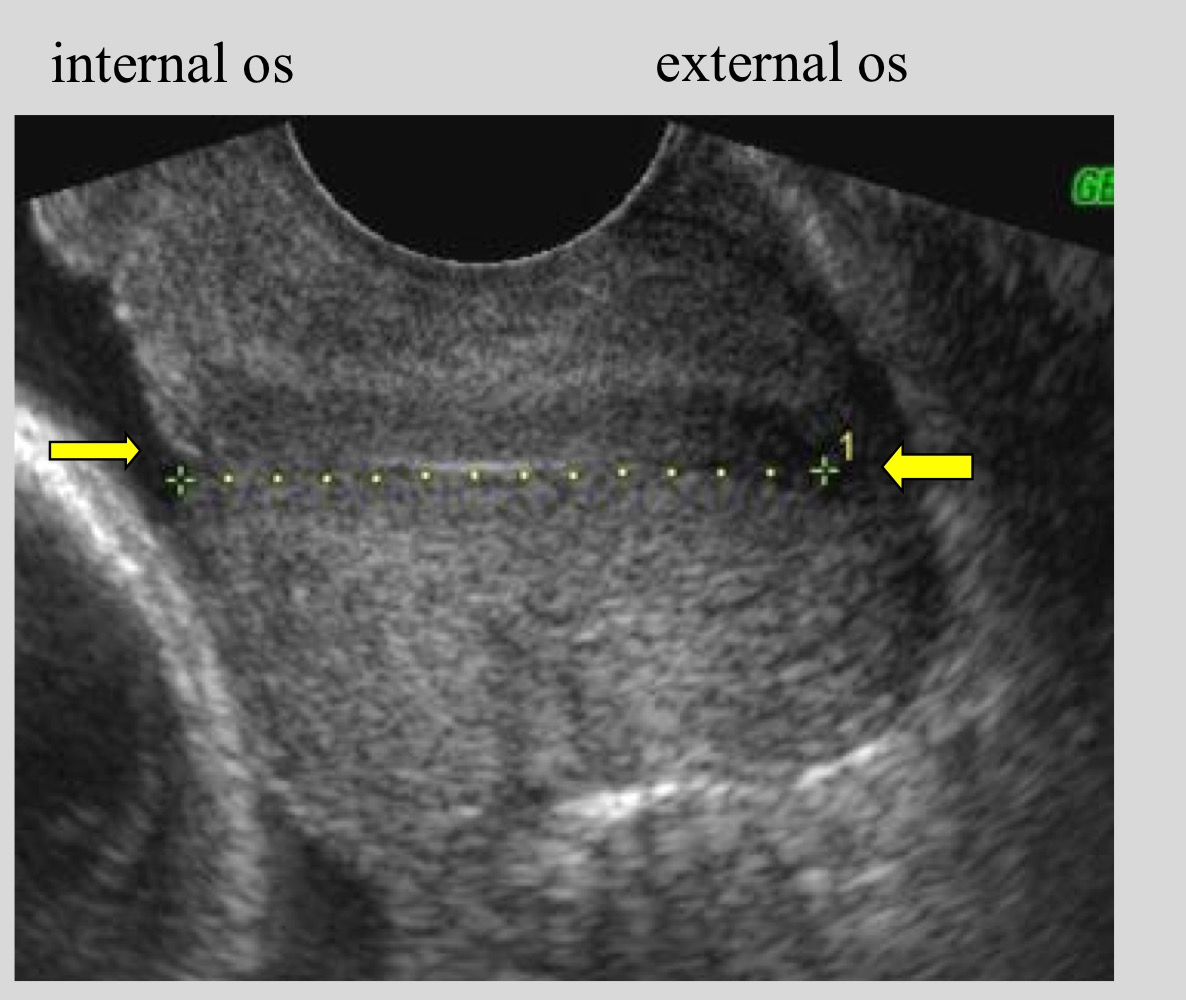
What structure is used as a guide when measuring cervical length
Cervical canal
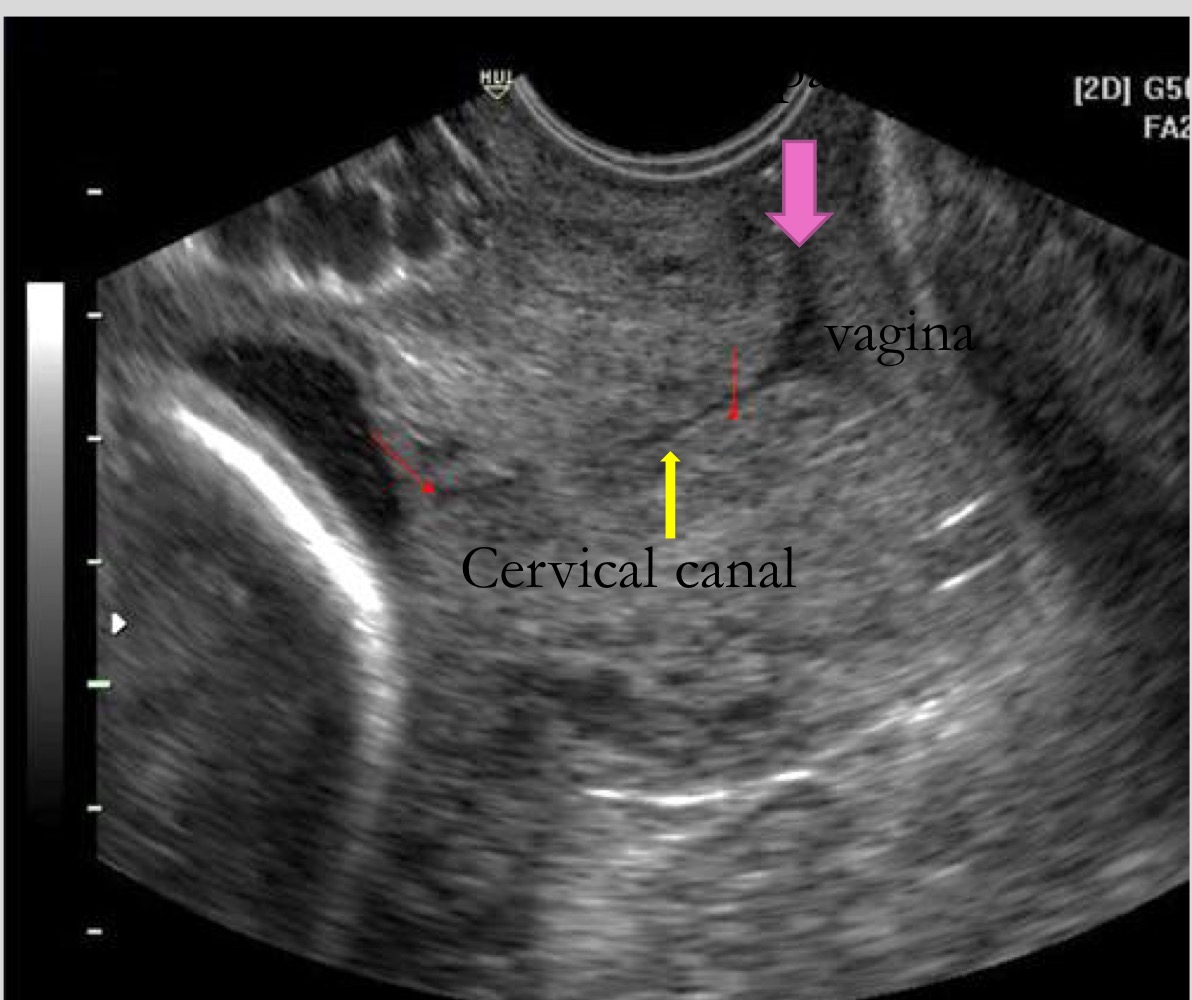
Where is the internal os located
Opposite the uterine body curve
Average normal cervical length
3.5 cm
Why must the cervix be observed for more than 3 minutes during transvaginal scan
Because the cervix is dynamic and can change quickly
What changes can occur in the cervix over a short time
Shortening, funneling, dilation
Images taken 20 sec apart!!!!
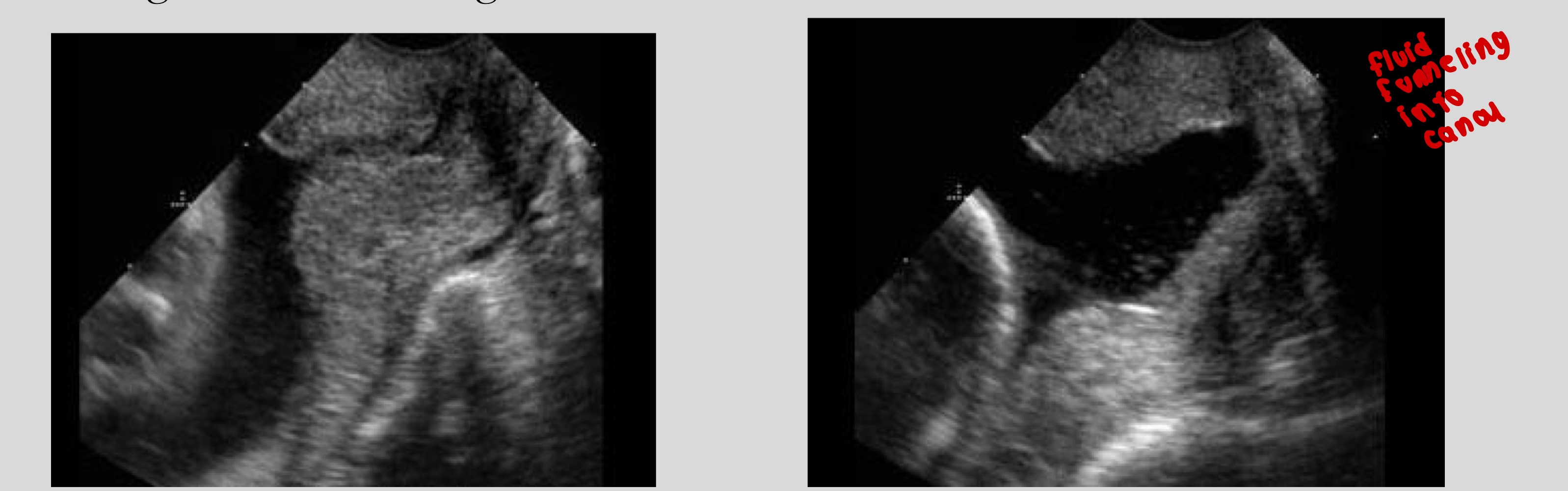
Definition of cervical incompetence
Inability of the cervix to retain a pregnancy in the second trimester without uterine contractions
How common is cervical incompetence
About 1 in 100 pregnancies
What percentage of second trimester losses is due to cervical incompetence
About 25%
What is another term for incompetent cervix
Cervical insufficiency
What can cervical incompetence lead to
Miscarriage or premature delivery
How often are cervical lengths typically monitored in at-risk patients
Every 2 weeks until 24 weeks
Best imaging method to evaluate cervical incompetence
Transvaginal ultrasound
What measurement is always used when assessing cervical length
External os to internal os
What should you do if you see funneling during scanning
Apply fundal pressure and wait to rule out contraction
Why should you wait if funneling is seen
It may be due to a temporary uterine contraction
What is funneling
Dilatation of the internal os with shortening of cervical length
What shapes can funneling appear as
U-shaped or V-shaped
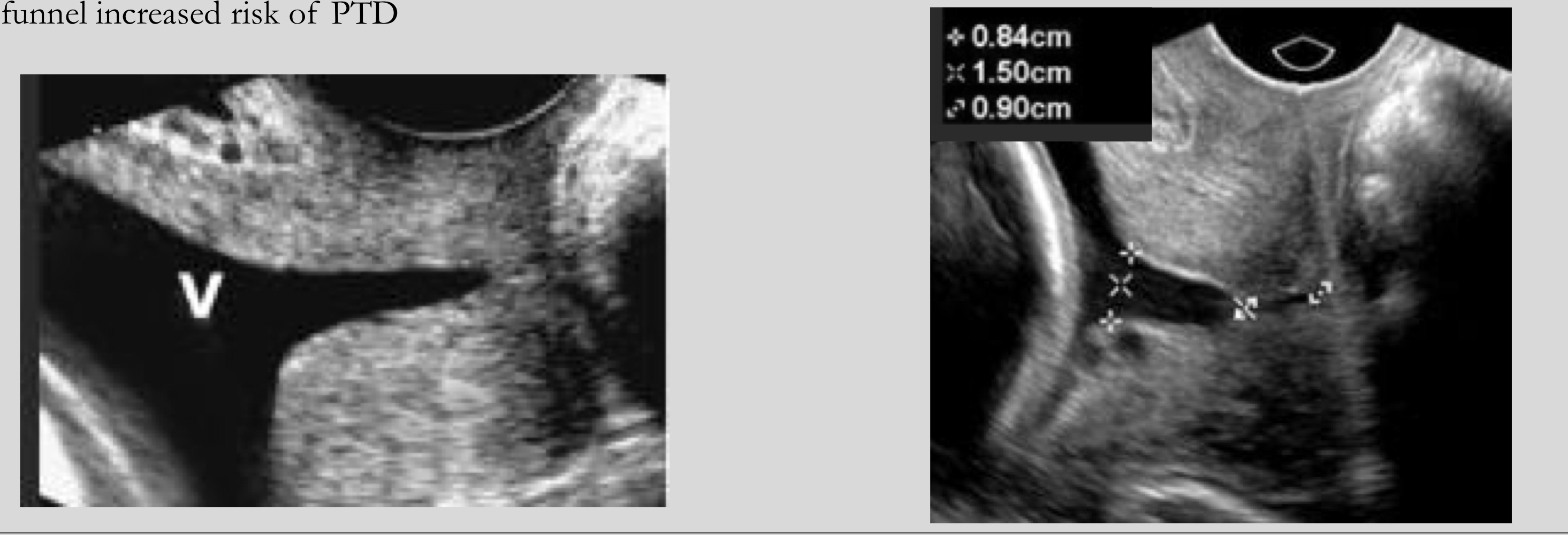
Which funnel shape is associated with higher risk of preterm delivery
U-shaped funnel
What is a short cervix defined as
Cervical length less than 2.5 cm
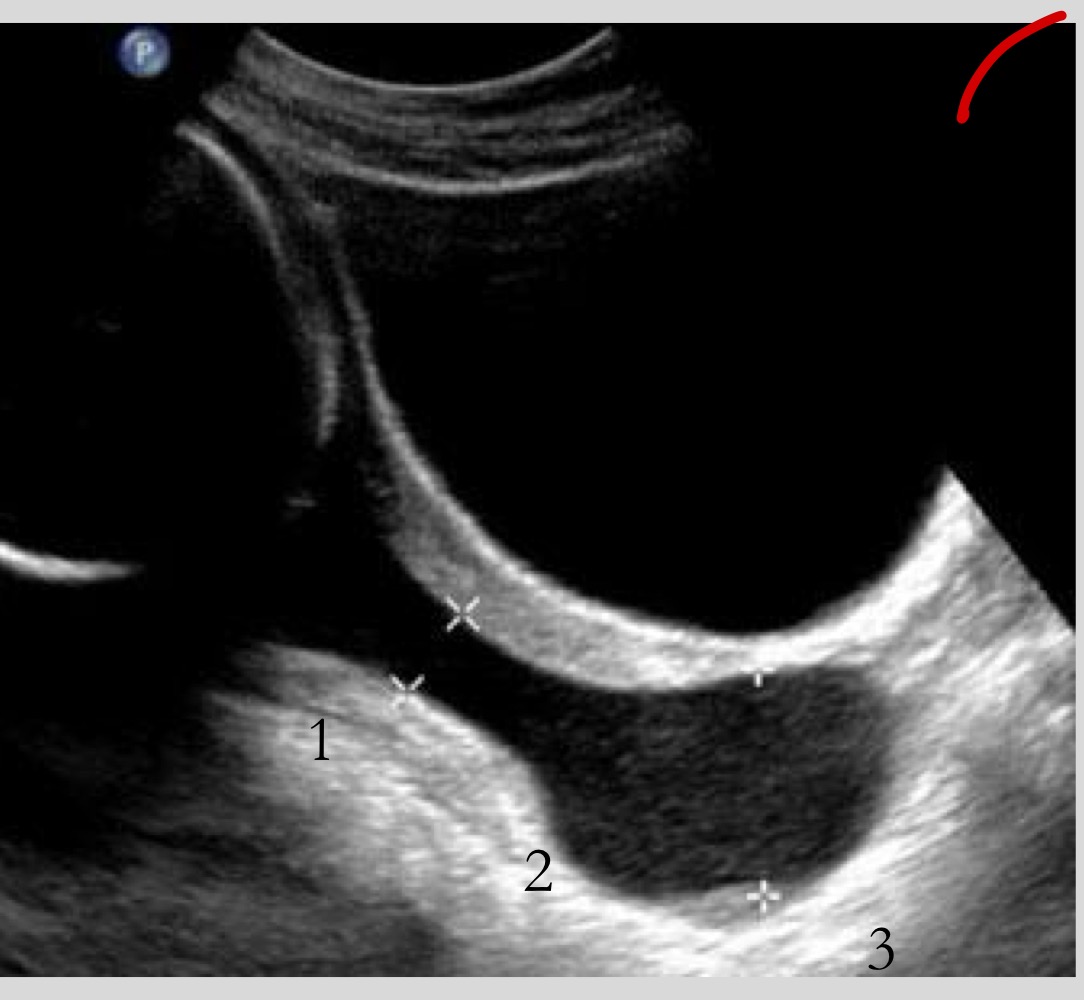
What is seen in severe cervical incompetence
Bulging (hourglassing) membranes into the vagina

What does hourglassing refer to
Membranes protruding through the cervix into the vagina
What are common causes of cervical incompetence
Müllerian anomalies,
cervical surgeries,
naturally short cervix,
prior traumatic birth
What is a cerclage
A stitch placed to close the cervix and prevent premature dilation
When is elective (known incompetence) cerclage typically placed
12-14 weeks
What is the success rate of cerclage
80-90%
When are vaginal cerclage stitches typically removed
Around 37 weeks
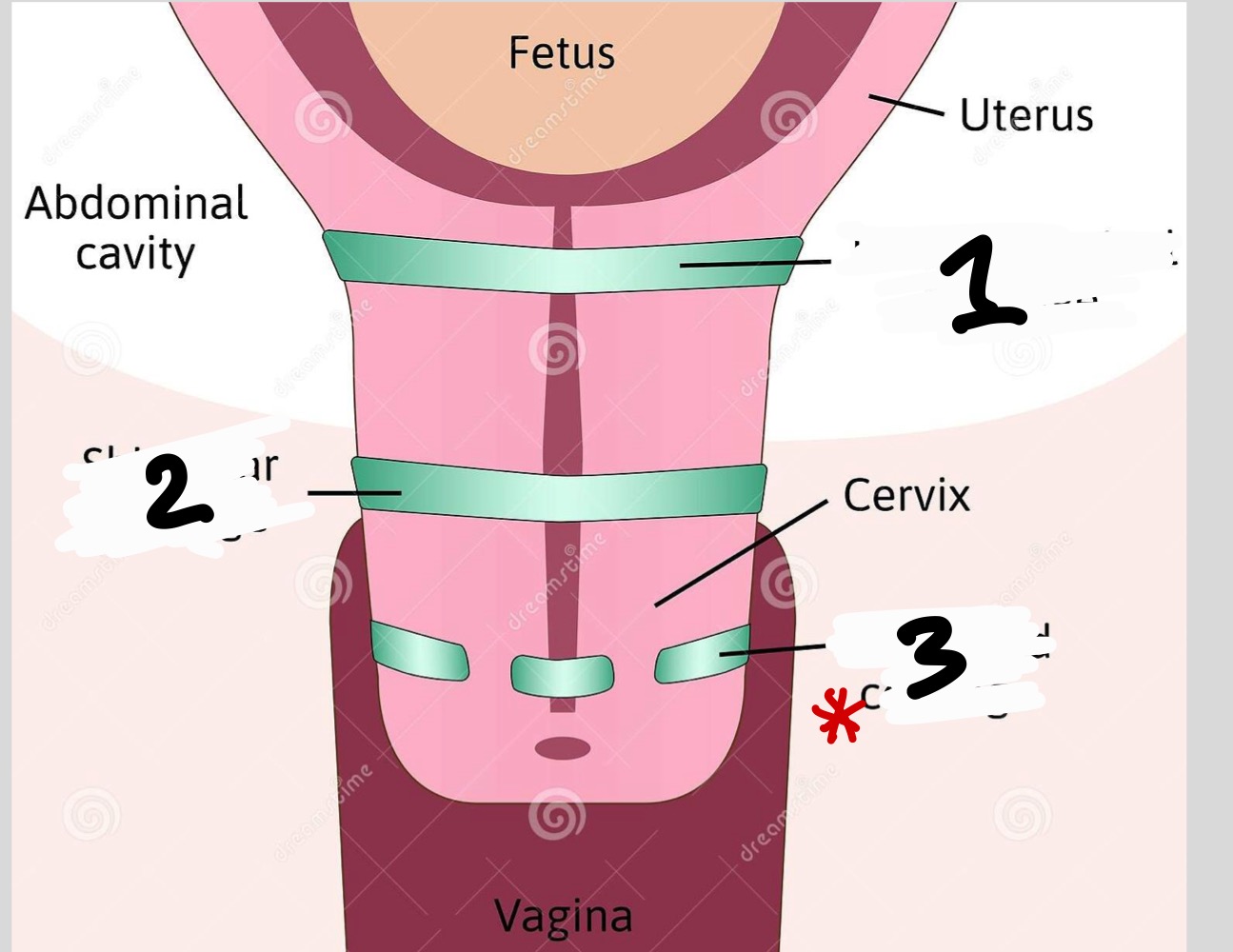
What are the three types of cerclage
McDonald, Shirodkar, Abdominal
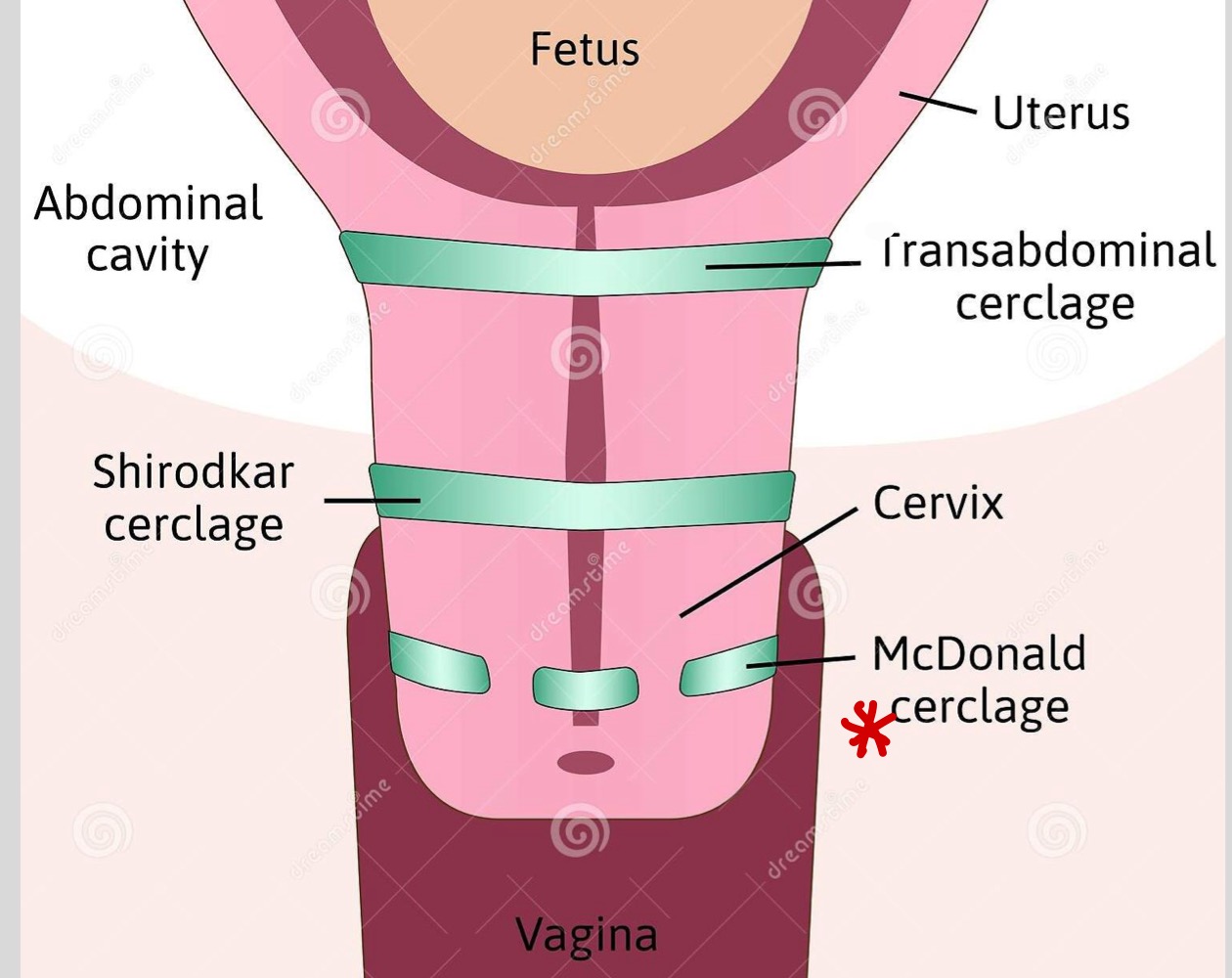
Most common type of cerclage
McDonald
What is special about an abdominal cerclage regarding delivery
Requires cesarean section
What medication may be given in cases of cervical incompetence to help the fetus
Betamethasone
What is the purpose of betamethasone
To help mature fetal lungs in case of preterm birth
What is dilation of the cervix in incompetence
Opening of the internal os with shortening or complete dilation
What is the relationship between short cervix and preterm birth
Increased risk of preterm birth
What is placenta previa
Placenta located near or covering the cervical os
When is placenta previa commonly seen but often resolves
Before 20 weeks of pregnancy
What percentage of early placenta previas remain at term
About 15%
Why does placenta previa often resolve
The uterus grows and the placenta moves upward away from the cervix
What is a false placenta previa
Apparent previa caused by lower uterine segment contraction
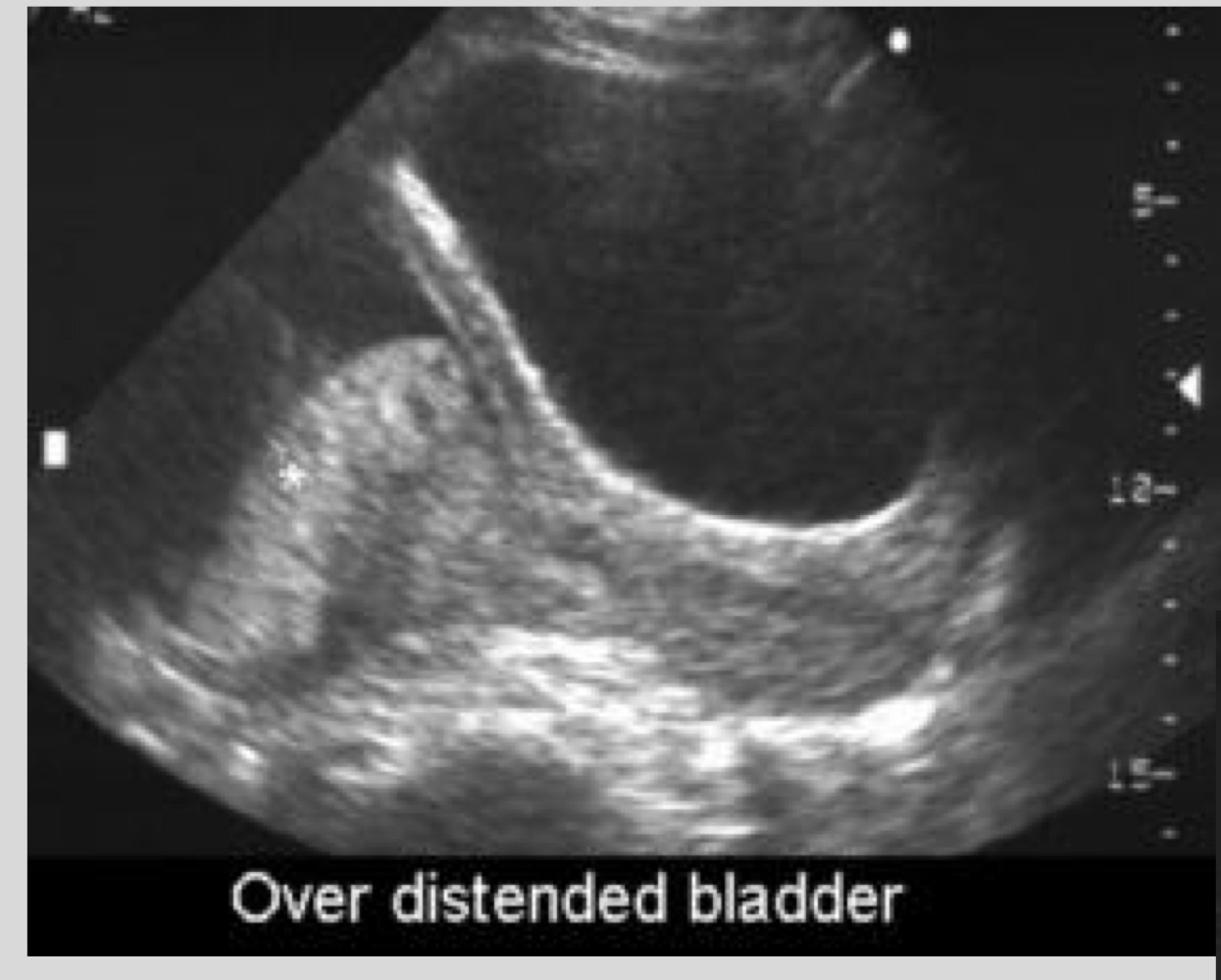
What should you do if a contraction mimics previa
Rescan in 10-20 minutes
What must be done before diagnosing placenta previa
Post-void scan or transvaginal ultrasound
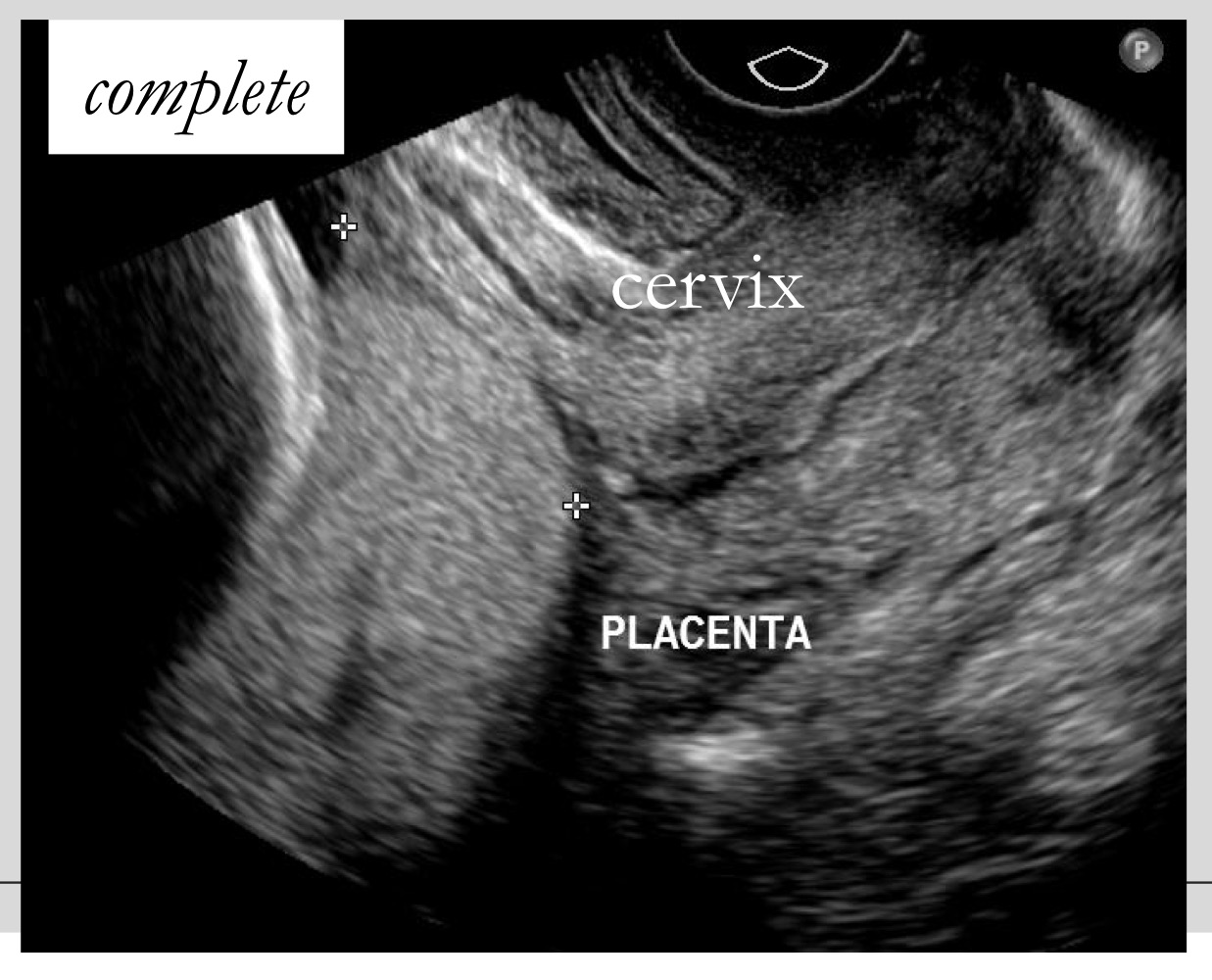
Definition of complete placenta previa
Placenta completely covers the internal os
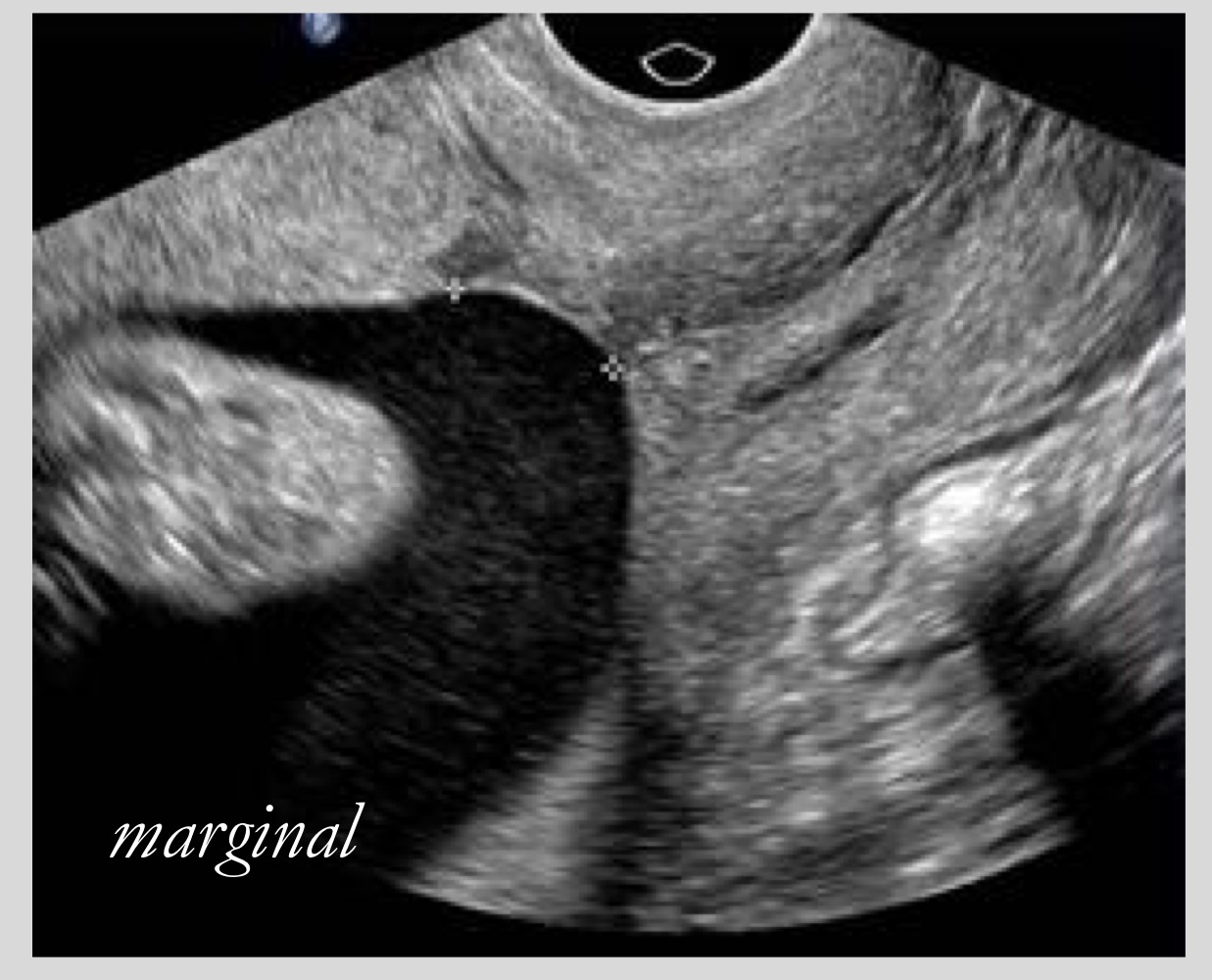
Definition of marginal or low-lying placenta
Placenta is within 2 cm of the internal os but not covering it
What distance defines a low-lying placenta
Within 2 cm of the internal os
What is the main symptom of complete placenta previa
Bright red painless vaginal bleeding in second half of pregnancy
Is bleeding in placenta previa painful or painless
Painless
What activity restriction is common with placenta previa
Restricted from physical exertion
What type of delivery is usually required for complete placenta previa
Cesarean section
When should follow-up ultrasound be done for placenta previa
After 32 weeks
How common is placenta previa
1 out of 200 pregnancies
What should always be identified about the placenta location
Whether it is anterior or posterior
How is placenta previa measured
From internal os to the placental edge
How should a report describe placenta location
Distance from internal os or if it covers the cervix
What are the two main types of placenta previa
Low-lying (marginal) and complete
What is seen in complete previa on imaging
Placenta covering the cervical canal/internal os
What imaging method is best for evaluating placenta previa
Transvaginal ultrasound
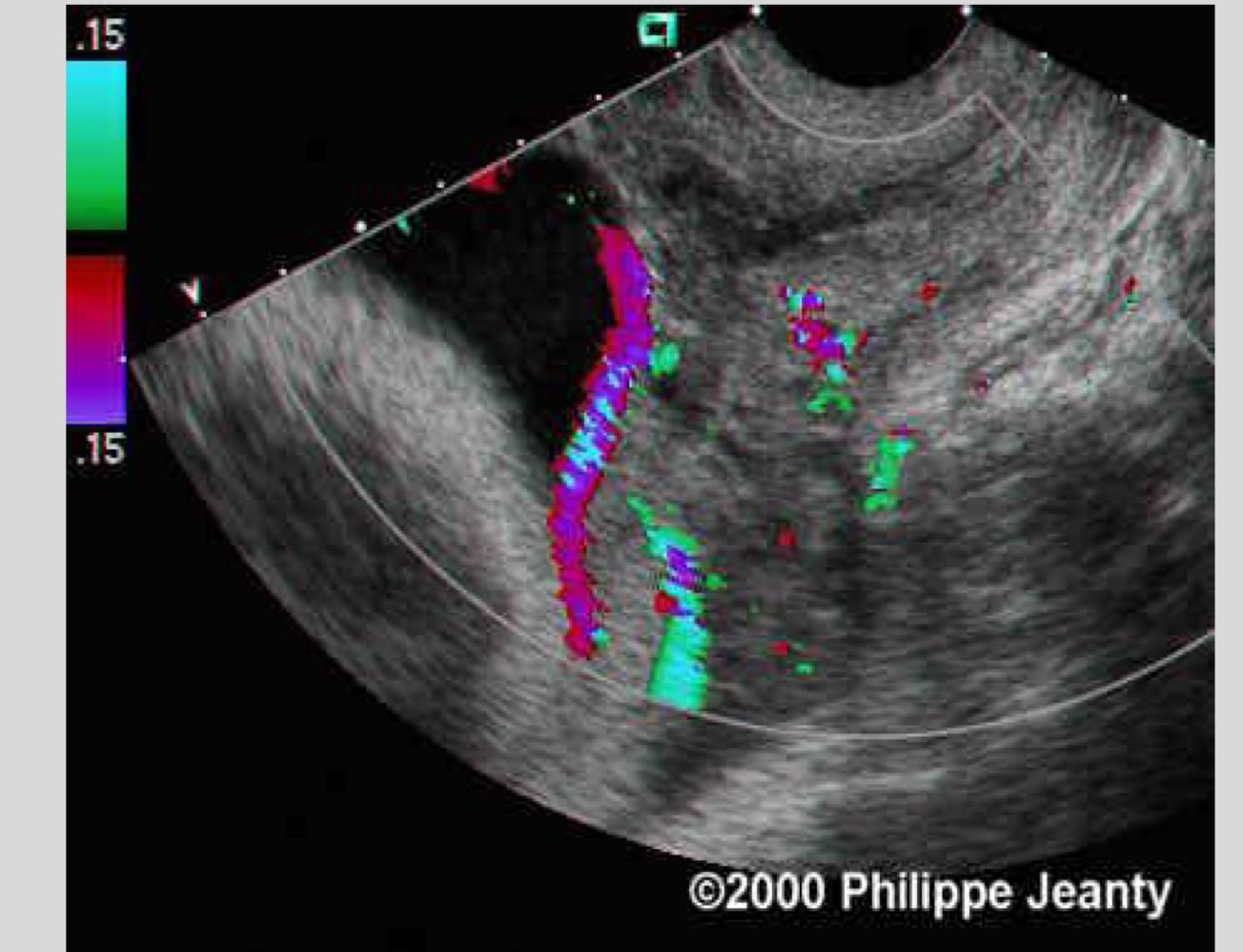
Definition of vasa previa
Fetal vessels pass below the presenting part near the cervix
What is the danger of vasa previa
Vessel rupture during membrane rupture causing fetal hemorrhage
What can cause fetal hemorrhage in vasa previa
Tearing of vessels when membranes rupture
How common is vasa previa
About 2 in 10,000 pregnancies
What placental abnormalities are associated with vasa previa
Bilobed placenta, succenturiate lobe, low-lying placenta
What reproductive method is associated with vasa previa
In-vitro fertilization
How is vasa previa best diagnosed
Transvaginal ultrasound with color Doppler
What is the role of color Doppler in vasa previa
To visualize fetal vessels near the cervix