Anatomy 2 Lab Practical #2 Stuff
1/125
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
126 Terms
Table for normal values for different substances found in urine

How do kidneys achieve homestasis?
by regulating the pH and concentration of ions and water in the various body fluids; elimination of waste products of metabolism
How many nephrons in the kidneys contain two main structures?
1 million nephrons
What are the 2 structures the one million nephrons in the kidneys contain?
renal corpuscle & renal tubule
Where is blood first filtered through?
a tuft of capillaries called glomerulus
What is the rate that blood passes through the tuft of capillaries (glomerulus)?
120 mL/min
What are the 3 major parts of the renal tubule?
proximal convoluted tubule (PCT), nephron loop (Loop of Henle), and the distal convoluted tubule (DCT)
The tubular filtrate similar to blood plasma in composition, except large molecules over what are excluded?
70,000 MW (e.g., plasma proteins)
What by-products are retained in the filtrated and are finally exerted in the urine?
toxic by-product of metabolism and excess substances (salt)
How much urine is formed per minute?
1 mL of urine formed per minute
What does the final composition of urine reflect?
reflects the integrity of kidney function and changes in blood composition
Urinalysis
an analysis of urine that can yield valuable information about the health of the kidney and of the body in general
Phenylketonuria (PKU)
when an individual is genetically unable to metabolize the amino acid phenylalanine
What is phenylalanine converted into when accumulated in the body?
phenylpyruvic acid
What can an accumulation of phenylalanine in individuals with PKU result in?
developmental delays, seizures, and intellectual impairments
Diabetes Mellitus (diabetes)
when an individual has either an imbalance or a deficit in the amount of insulin produced by the pancreas
Ketones
when the sugars in the blood cannot be used as cellular fuel, the body will utliize fat as an energy source, leading to an increase in fatty acid metabolites called this
What will an increase in ketones do to blood pH?
cause it to decrease
What is indicative of diabetes mellitus?
presence of both glucose and ketones in the urine
Labstix Test
a combined test of urinary pH, protein, glucose, ketones, and occult blood
What is the Urinary pH?
pH of 6
What can a more acidic urine mean?
diet rich in proteins or respiratory disorders, dehydration, or starvation
What can a more alkaline urine mean?
diet rich in citrus fruits and dairy, vomiting, urinary tract infections, or cystitis
Cystitis
urine decomposes in the bladder with the production of ammonia
Proteinuria or Albuminuria
the presence of protein in the urine
Glycosuria
high glucose levels in urine, which indicate the body’s inability to process glucose, leading to an accumulation of glucose in the blood that is then secreted in the urine
Ketonuria
abnormally large amounts of ketone excretion, suggest that the body is using fat as an energy source as opposed to glucose
What can ketonuria indicate?
diabetes mellitus or starvation
What can glycosuria indicate?
diabetes mellitus
Occult Blood
blood not visible to the naked eye
What can blood present in the urine indicate?
an individual has a urinary tract infection, kidney stones, or cancerous cells
Nephritis
a disease in which the glomeruli are damaged and plasma proteins and erythrocytes leak into the nephrons (blood present in urine and high levels of protein)
When should you examine the strip?
examine BEFORE conducting the test so you know which portions to read first.
How many seconds should you wait to read the glucose test portion?
10 seconds
How many seconds should you wait to read the ketone portion?
5 more seconds
How many seconds should you wait to read the occult portion?
15 more seconds
What is one of the kidney’s main functions?
to regulate the osmolarity of the body fluids
At what rate do the kidneys regulate the osmolarity of the body fluids?
300 milliosmoles per L
What happens to the concentration of urine for someone who is dehydrated?
will produce a SMALL amount of highly concentrated urine
What happens to the concentration of urine for someone who is overhydrated?
will produce a LARGE amount of minimally concentrated (dilute) urine
What are Group 1’s consumed fluid solute concentrations?
800 mL water
What are Group 2’s consumed fluid solute concentrations?
800 mL water with 7 g NaCl
What are Group 3’s consumed fluid solute concentrations?
80 mL water with 7 g NaCl
Specific Gravity
the rate of the density of a substance compared to the density of distilled water
Should you drop the urinometer float directly into the cylinder?
do NOT drop the urinometer float directly into the cylinder
What calibration temperature for the urinometer?
15oC
How will you correct the specific gravity value?
by adding 0.001 for every 3oC above, or by subtracting 0.001 for every 3oC below the calibration temperature (15oC)
What is the normal range of urine specific gravity?
1.0015 to 1.035
What is the specific gravity of distilled water?
1.000
Chronic Nephritis
a low specific gravity reading in individuals (slow, onset kidney disease)
Acute Nephritis
a high specific gravity in individuals (sudden, onset kidney disease)
Mohr Method (NaCl Concentration)
the process of titrating silver nitrate to analyze the presence of chloride ions in a substance using potassium chromate as an indicator
How many drops of 20% potassium chromate do you add to the test tube?
ONE drop
How do you add 2.9% silver nitrate solution?
DROP by DROP
How much NaCl does each drop of 2.9% silver nitrate represent?
1 g/L of NaCl
How many separate plots for your data should you make?
3 separate plots
Chronic Obstructive Pulmonary Disorder (COPD)
obstruction of the lungs causes air to be “trapped” in the lungs when it cannot be exhaled
over time → causes stretching of the lung tissue
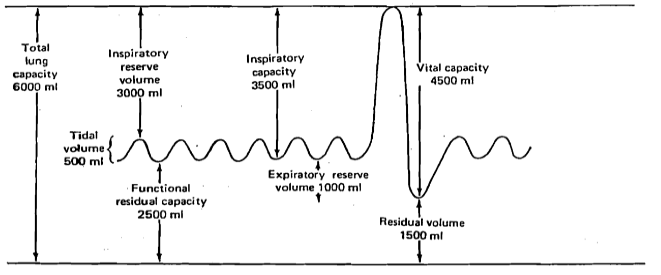
Tidal Volume (TV)
the amount of air inhaled or exhaled on a normal breath
Inspiratory Reserve Volume (IRV)
the additional air that can be forcefully inhaled past a normal tidal volume inspiration
Expiratory Reserve Volume (ERV)
the additional air that can be forcefully exhaled past a normal tidal volume expiration
Residue/Residual Volume (RV)
the volume of air remaining in the lungs following a maximal exhalation
Vital Capacity (VC)
the total amount of air that can be forcefully expired after a maximum inhalation
Vital Capacity (VC) Equation
VC = TV + IRV + ERV
vital capacity = tidal volume + inspiratory reserve volume + expiratory reserve volume
Inspiratory Capacity (IC)
the maximum amount of air that can be inspired after a normal inhalation
Inspiratory Capacity (IC) Equation
IC = TV + IRV
inspiratory capacity = tidal volume + inspiratory reserve volume
Functional Residual Capacity (FRC)
the total amount of air remaining in the lungs after a normal exhalation
Functional Residual Capacity (FRC) Equation
FRC = RV + ERV
functional residual capacity = reserve/residual volume + expiratory reserve volume
Total Lung Capacity (TLC)
the total amount of air the lungs can contain
Total Lung Capacity (TLC) Equation
TLC = TV + IRV + ERV + RV
total lung capacity = tidal volume + inspiratory reserve volume + expiratory reserve volume + reserve/residual volume
Spirometry
a medical test used to measure the four lung volumes with the use of a simple, non-invasive instrument (spirometer)
Spirometer
non-invasive instrument used during spirometry
Respiratory Minute Volume (mL air/min)
total amount of air that flows into and out of the respiratory tract in 1 minute
Respiratory Minute Volume (mL/min) Equation
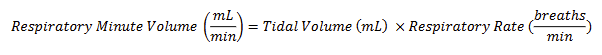
Vital Capacity
the largest volume found during vital capacity
Predicted Vital Capacity
the vital capacity predicted with the use of a nomogram
What does a longer breath-holding indicate?
indicated better pulmonary function, functional reserve, and larger lung capacity because the lungs are better able to help maintain the body pH
What are the functions of the respiratory system and cardiovascular system?
function to take oxygen into the body from the atmospheric air and deliver it to the tissue cells
Respiratory Acidosis
condition indicated by carbon dioxide build up in the blood, the pH of the blood becomes more acidic
Dry Gas Meter
measures tidal volume by breathing into a mouthpiece and Douglas bag connected to the dry gas meter, and measuring the volume of air stored in the bag
Minute Volume (Vm)
calculated by multiplying the total volume of air exhaled (mL) by the number of breaths taken over the collection period (minutes)
the flow of air into and out of the lungs
Metabolic Rate
dry gas meter measures this; is the body’s rate of energy expenditure
What is the percentage of oxygen in inhaled air?
20.95%
How is metabolic rate calculated?
the difference between the percentage of oxygen in inhaled air (20.95%) and the percentage of oxygen in the exhaled air stored in the bag → and multiplying this difference by the minute volume (Vm)
Is the metabolic rate of skeletal muscle tissue cells higher or lower during physical activity?
metabolic rate of skeletal muscle tissue cells is significantly higher, requiring more oxygen uptake and delivery to the cells
Respiratory Capacities Graph
Rate of Oxygen Consumption (VO2)
equal to both the rate at which you obtain oxygen from the environment across the surface of the lungs (i.e., ventilation) and the rate at which oxygen is delivered to body tissue cells through the capillary walls (i.e., perfusion) of the cardiovascular system
Ventilation-Perfusion Coupling
the balance in exchange between the oxygen you obtain from the environment across the surface of the surface of the lungs and the oxygen delivered to body tissue cells through capillary walls (rate of oxygen consumption [VO2])
How is Ventilation increased?
ventilation is increased by increasing the respiratory rate and respiratory depth (tidal volume)
How is Perfusion increased?
perfusion is increased by increasing heart rate
What is the flow of blood related to in the cardiovascular system?
related to Cardiac Output (CO)
What leads to a difference in the concentration of oxygen in inhaled air (CO2i) and the concentration of oxygen in exhaled air (CO2e)?
lungs extracting oxygen from the air we breathe
What leads to a difference in the concentration of oxygen in arterial blood (CO2a) and the concentration of oxygen in venous blood (CO2v)?
oxygen is lost from the blood supply through the capillary beds in systemic circulation
VO2 Equation
VO2 = (minute volume) (concentration of oxygen in inhaled air - concentration of oxygen in exhaled air)
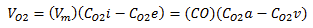
How saturated is arterial blood and venous blood in most resting people?
Arterial Blood Saturation = 100%
Venous Blood Saturation = 60%
How much oxygen can 1 gram of hemoglobin bind to?
1.34 mL of O2
Maximum Oxygen Content Equation
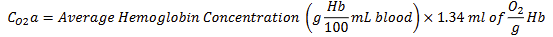
Oxygen Content of Venous Blood Equation
CO2v = 0.6 (maximum oxygen content)
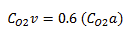
Resting Cardiac Output Equation
CO = rate of oxygen consumption / (maximum oxygen content - oxygen content of venous blood)
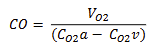
Resting Stroke Volume (SV) Equation
SV = resting cardiac output / heart rate
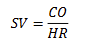
What happens to oxygen content of the venous blood during exercise?
oxygen content of venous blood falls due to increased oxygen demands by the body cells