BIOL 1412 Urinary system
1/173
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
174 Terms
What organs form urine + regulate the composition of blood plasma?
Kidneys
What is the functional unit of the kidney?
Nephron
What 4 structures transport urine?
Renal pelvis, ureters, urinary bladder, urethra
As one of its many functions, what do the kidneys maintain?
Plasma volume (∴ maintain bp [MAP])
What 3 things do the kidneys regulate?
[Ions] + [H2O], acid-base balance
What 3 things do the kidneys eliminate?
Wastes, drugs, hormones
The kidneys produce + secrete what 2 hormones as per its endocrine function?
Renin + erythropoietin
What is renin secreted to maintain?
Blood pressure
What is erythropoietin secreted for?
RBC production
What are the 2 broad parts of a nephron unit?
Renal corpuscle + tubules
What 2 things is the renal corpuscle made up of?
Glomerulus + renal capsule
What are the 5 tubules of a nephron?
Proximal convoluted tubule (PCT), descending loop (DL), ascending loop (AL), distal convoluted tubule (DCT), collecting duct (CD)
What 3 processes in the nephron lead to urine filtration?
Glomerular filtration → tubular reabsorption → tubular secretion
What is the premise of glomerular filtration?
H2O + small solutes forced out of blood → glomerulus → Bowman’s capsule
Why does glomerular filtration happen?
Due to pressure differences across the filtration membrane
What is the premise of tubular reabsorption?
Valuable substances are transported from filtrate in nephron → back to bloodstream
What is the premise of tubular secretion?
Additional waste/excess products are actively transported from peritubular capillaries → lumen of nephron (to be excreted as urine)
What are peritubular capillaries?
Tiny blood vessels that wrap around the renal tubules in the kidney
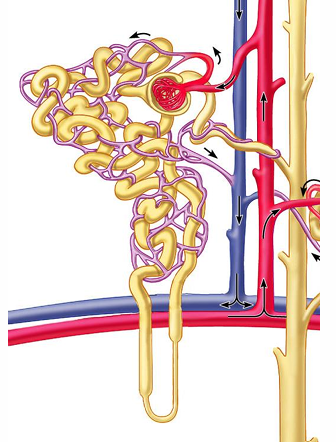
During the process of glomerular filtration, how much plasma in the glomerulus is filtered into Bowman’s capsule?
20%
By what transportation method is plasma filtered into Bowman’s capsule from the glomerulus?
Bulk flow (pressure difference/ΔP across filtration membrane)
What 3 parts make up the filtration membrane?
Glomerulus (fenestrated endothelium), fused basement membranes, podocytes w/ filtration slits between (layer of Bowman’s capsule)
Filtrate is almost identical to plasma, but differs in that it does not contain what?
Large proteins
What 5 things are contained in filtrate, besides ions + vitamins?
H2O, glucose, aa, urea, some small proteins
What is the approximate pH of filtrate?
~7.45
What are the 4 pressures relating the urinary physiology?
HP = Hydrostatic Pressure ~~~ OP = Osmotic Pressure
Glomerular HP, blood HP, capsular HP, capsular OP
Which pressure represents blood pressure inside glomerular capillaries?
Glomerular HP
What is the pressure of glomerular HP, + does it favour/oppose filtration?
55 mmHg, favours filtration
What is the pressure of blood OP, + does it favour/oppose filtration?
30 mmHg, opposes filtration
What is the pressure of capsular HP, + does it favour/oppose filtration?
15 mmHg, opposes filtration
What is the pressure of capsular OP, + does it favour/oppose filtration?
0 mmHg, favours filtration
Adding up pressures that favour + oppose filtration separately, then calculating the difference leaves us with what Net Filtration Pressure (NFP)?
NFP = (55 + 0) - (30 + 15) = 10mmHg
What is glomerular filtration rate (GFR)?
Amount of filtrate the kidneys filter from the blood into Bowman’s capsules per a chosen unit of time
At an NFP of 10mmHg, there is about ~___L/day of filtrate (both kidneys)
“180”
With both kidneys collectively making ~180L of filtrate a day, how many mL are made per minute?
125mL/min
Normally, one’s entire plasma volume is filtered how many times per day?
~65 times per day
Though one’s plasma volume is continuously being filtered, how much of filtered volume remain at the end of the collecting duct?
< 1%
Why does GFR need to be regulated?
So it doesn’t change when systemic blood pressure changes
If GFR wasn’t kept from changing along with systemic blood pressure, what would happen?
⬆MAP = ⬆GFR
(vise versa)
What can happen if GFR is too high?
Valuable nutrients and H2O may be lost in the urine (filtrate passes through too quickly for proper reabsorption)
What can happen if GFR is too low?
Blood is not being filtered fast enough, wastes may accumulate in the blood
What 2 regulatory processes are there for GFR?
Intrinsic + extrinsic
Which type of regulation is autoregulation?
Intrinsic regulation
Intrinsic regulation of GFR monitors blood pressure within what range?
Resting to moderate exercise
What are the 2 types of intrinsic regulation for GFR?
Myogenic + juxtaglomerular complex (apparatus)
If ⬆MAP, how does myogenic regulation work (works vise versa)?
Causes a stretch → afferent arteriole sm. musc. contracts → prevents ⬆BP in glomerular capillaries
What monitors [NaCl] in filtrate flowing past it?
Macula densa (specialized cells in the DCT)
As for juxtaglomerular complex (apparatus), what does it mean for [NaCl] if filtrate flow/GFR is high (works vise versa)?
Reabsorption may be inadequate, leaving more NaCl in the filtrate to be excreted as urine
As for juxtaglomerular complex (apparatus), how does GFR return to resting after increasing due to ⬆BP in glomerular capillaries (works vise versa)?
⬆[NaCl] in filtrate at macula dense → afferent arteriole constricts → GFR ⬇ to resting
What is extrinsic regulation primarily controlled by?
SNS
How does the SNS affect both arterioles (afferent + efferent) in a nephron?
Vasoconstricts them
What is the effect of the afferent arteriole constricting?
⬇Flow into glomerulus
What is the effect of the efferent arteriole constricting?
Blood backs up in glomerulus
How would GFR be affected with a moderate SNS activation?
Both arterioles balance → GFR doesn’t change much
How would GFR be decreased by extrinsic regulation under extreme stress?
Constricting afferent arteriole
For what 2 reasons would the afferent arteriole constrict under extreme stress?
Conserve fluid + redirect blood to critical organs
NFP can change from what 2 pressures?
Blood OP + capsular HP
In the case of dehydration, how would blood OP + GFR change (⬆/⬇)?
⬆BOP, ⬇GFR
Why would a higher blood OP = lower GFR?
Because it opposes filtration at the glomerulus
What is nephrotic syndrome?
When proteins leak into the urine (abnormal)
In the case of burns or nephrotic syndrome, how would blood OP + GFR change (⬆/⬇)?
⬇BOP, ⬆GFR
What are 3 given examples of a urinary tract obstruction?
Kidney stones, inflammation, prostate enlargement
How does a urinary tract obstruction affect capsular HP + GFR?
⬆CHP, ⬇GFR
Approximately, how may litres of urine are produced per day?
1-1.5 L/day
Approximately, how many litres of fluid are filtered per day?
180L/day
99% of filtrate is reabsorbed from the tubules into what 2 capillaries?
Peritubular + vasa recta
Tubular reabsorption may be what 2 types?
Active or passive
What 4 things are actively reabsorbed?
Na+, some other ions, glucose, amino acids
What 3 things are passively reabsorbed?
Cl-, H2O, urea
Proximal Convoluted Tubule (PCT) is un/regulated?
Unregulated
What 2 things are 100% reabsorbed in the PCT via active transport?
Glucose + amino acids
What ion is 65% reabsorbed in the PCT via active transport?
Na+
How are small proteins reabsorbed in the PCT?
Endocytosis into tubule cell → amino acids → blood
What 2 additional things are reabsorbed in the PCT?
Vitamins + H2O (via osmosis - follows solutes)
After the PCT, a large amount of solute has been removed, meaning what for the volume of the filtrate?
It is now reduced
After the PCT, what is the tonicity of filtrate to plasma?
Isotonic
What is the unit of measurement for osmotic pressure?
mOsmoles/L
What is the osmolarity of filtrate after the PCT?
300 mOsm/L
Loop of Henle reabsorbs into what capillary bed?
Vasa recta
What is the only thing that the descending limb (DL) is permeable to?
H2O (via osmosis)
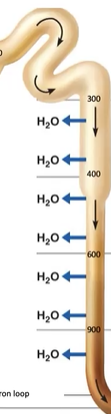
What is the only thing that the ascending limb (DL) is permeable to?
NaCl (via active transport)
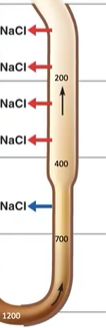
The initial part of the Distal Convoluted Tubule (DCT) reabsorbs what 3 ions?
Na+, Cl-, Ca+2
The initial part of the Distal Convoluted Tubule (DCT) is impermeable to what?
H2O
The later part of the Distal Convoluted Tubule (DCT) + Collecting Duct (CD) reabsorb what 2 things?
Na+ + H2O
What hormone increases Na+ reabsorption?
Aldosterone
What hormone decrease Na+ reabsorption by inhibiting aldosterone?
ANP (Atrial Natriuretic Peptide)
What hormone increases H2O reabsorption in the late DCT → CD, which further concentrates the urine?
ADH (antidiuretic hormone)
Nephrons normally reabsorb what percentage of filtered H2O, NaCl, glucose, + urea, respectively?
H2O (99%), NaCl (99.5%), glucose (100%), urea (50%)
Filtrate may contain trace amino acids + small proteins, but abnormal underlying causes may cause someone to contain what 2 things in their urine?
Glucose + blood
Tubular secretion involves movement of substances from __________ blood into filtrate of nephron lumen
“peritubular”
What are the 4 main substances that are secreted into filtrate to be eliminated from the body as urine?
Wastes (urea, uric acid, some hormones), K+, H+ or NH4+
⬆K+ by what hormone?
Aldosterone
Why would the body want to eliminate H+ or NH4+?
To maintain blood plasma pH
What does the countercurrent multiplier mechanism permit excretion of?
Urine on a spectrum from dilute to concentrated (100-1200mOsm/L)
What does the countercurrent multiplier mechanism produce + maintain?
A vertical osmotic gradient
Does vertical osmotic gradient mean there is more or less [solute] in the ISF as you move deeper into the medulla (i.e. lower down the descending limb)
⬆[solute]
What is the vertical osmotic gradient specifically produced by?
Juxtamedullary nephrons
Within the Loop of Henle, considering the countercurrent multiplier mechanism, fluid flows in parallel tubes (DL, AL) in _________ directions
“opposite”
The ascending limb actively filters the salt/NaCl from filtrate → ISF via what mechanism?
NaCl pump
As filtrate moves down the DL, ___ enters the ISF
“H2O”
Does concentrated or dilute filtrate enter the AL?
Concentrated with solute (because H2O was just reabsorbed)