Topic 20 - Capillaries and Lymp vessels
1/27
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
28 Terms
structure of capillaries
- Branch from arterioles, then connect into venules
- Single layer of endothelial cells = thin diffusion distance
- lumen is only wide enough for 1 RBC
- Each capillary is tiny but there are millions, so total surface area is immense (adding up all capillaries in a tissue)
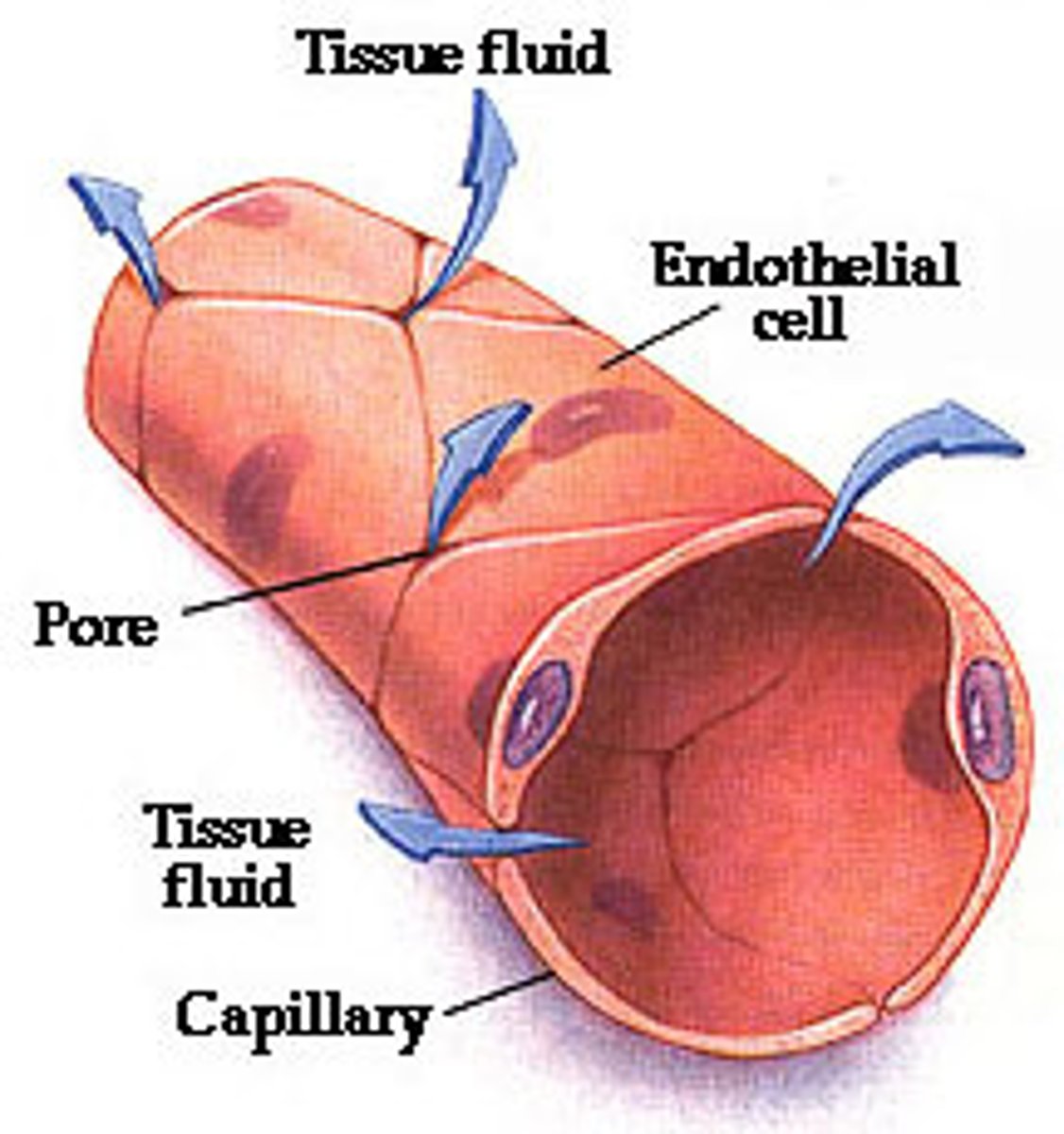
fnction of capillaries
Site of gas, nutrient, waste and water exchange
pressure in capillaries
40-20mmHg
As blood travels through capillaries towards venules the pressure drops
This low pressure is important bc of how flimsy and small the vessel is
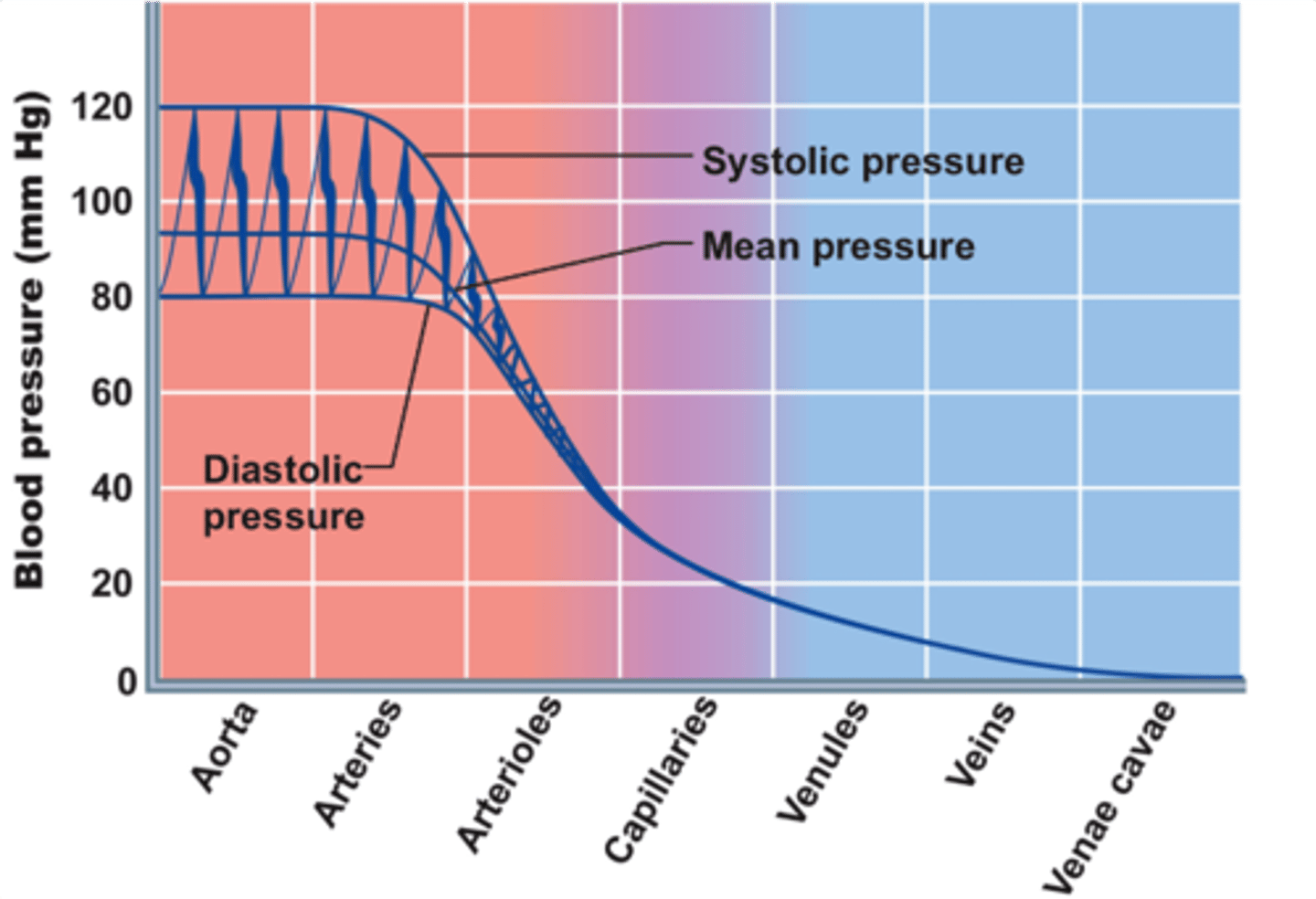
Gas & Nutrient exchange across capillary wall
Substances must pass through ... to exit the circulatory system
1. Pass through the capillary wall,
2. Pass through interstitial fluid,
3. Enter the tissue cells
(and metabolic waste products go the reverse direction)
Nutrient /Metabolite exchange depends on:
1. Diffusion gradients
2. Accessible route
- direct passage
- between endothelial cell junctions: essentially a water filled channel
- Via vesicle transport
how do lipid soluable substances pass thorugh the capillary + ex
Directly Pass through endothelial cells membrane anywhere
Eg. O2 into the cap , CO2 out of the cap
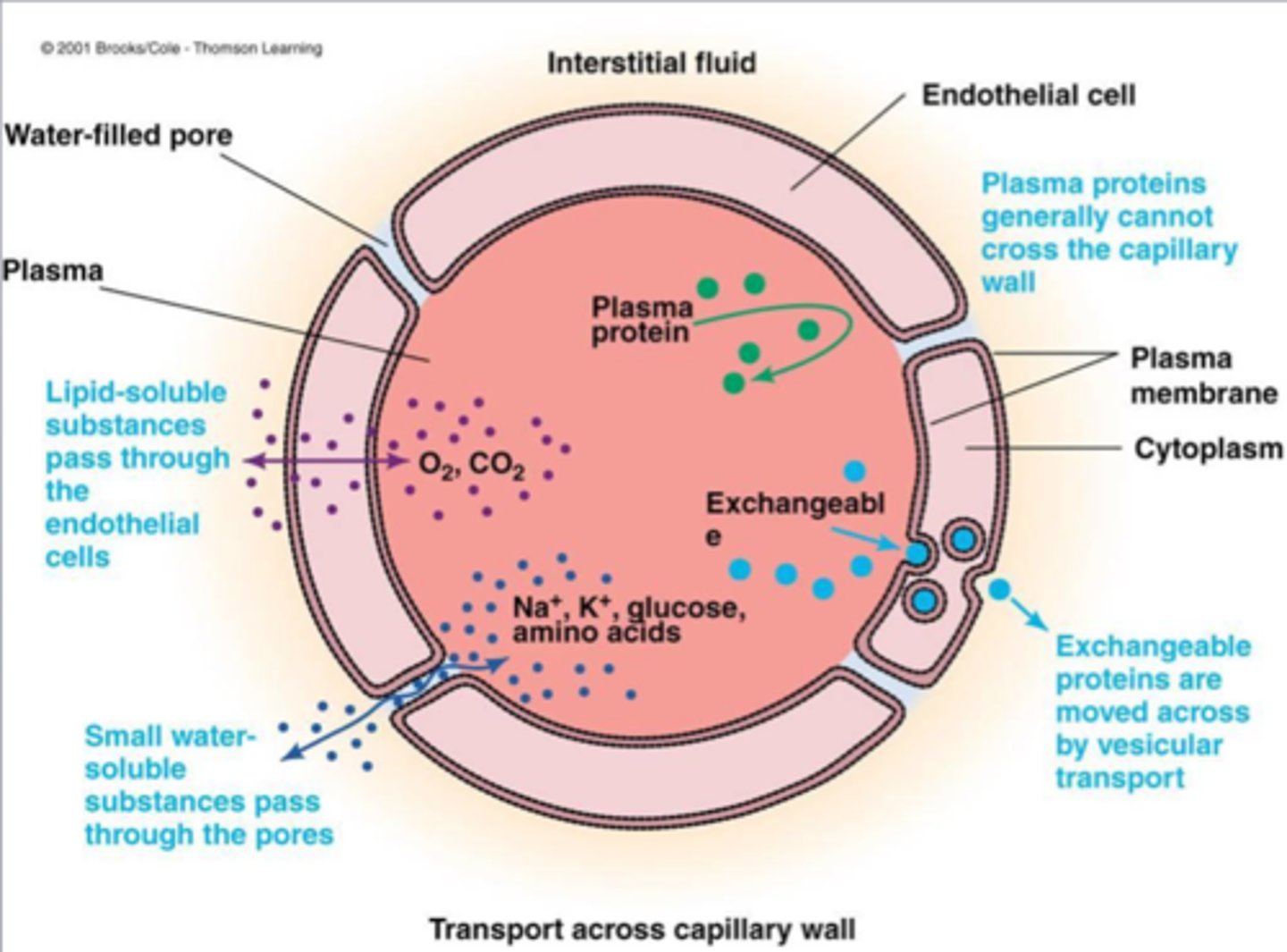
how do small water soluable molecules pass through the capillary + ex
Pass through capillaries only at cell-cell junctions/ pores
Eg. water, glucose, K+, Na+, Some amino acids
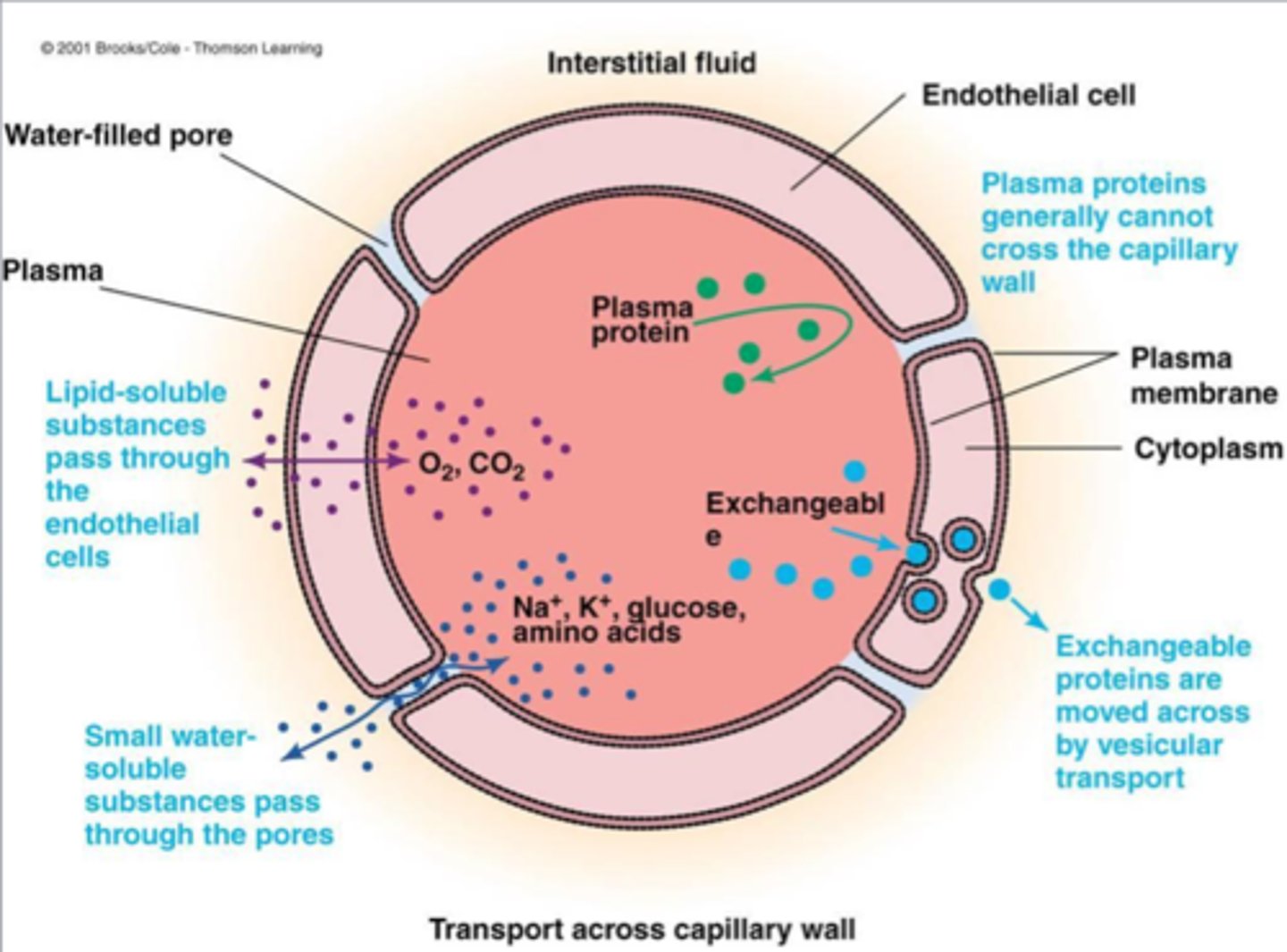
how do LARGE water soluable proteins pass through the capillary + ex
Pass through endothelial cells via vesicular transport out of the capillary
- Require receptors
Eg. most amino acids
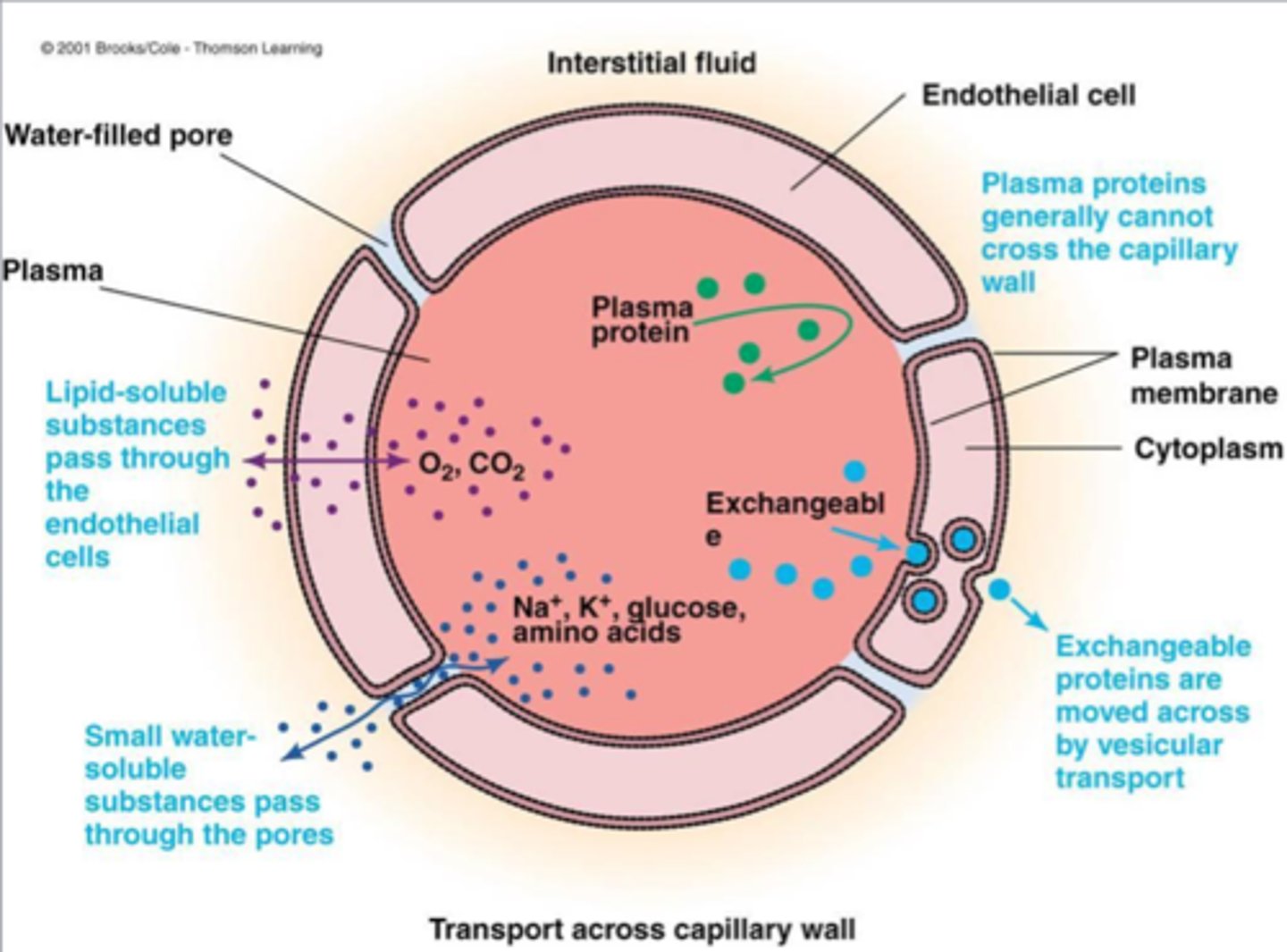
how do large plasma proteins pass through capillaries + ex
they don't - Rarely leave the capillary plasma
Eg. albumin
Eg. immunoglobulins, antibodies
**important bc we need these plasma proteins in the steam bc...
If there is albumin in the interstitial fluid that is a sign of damage in the capillary structure
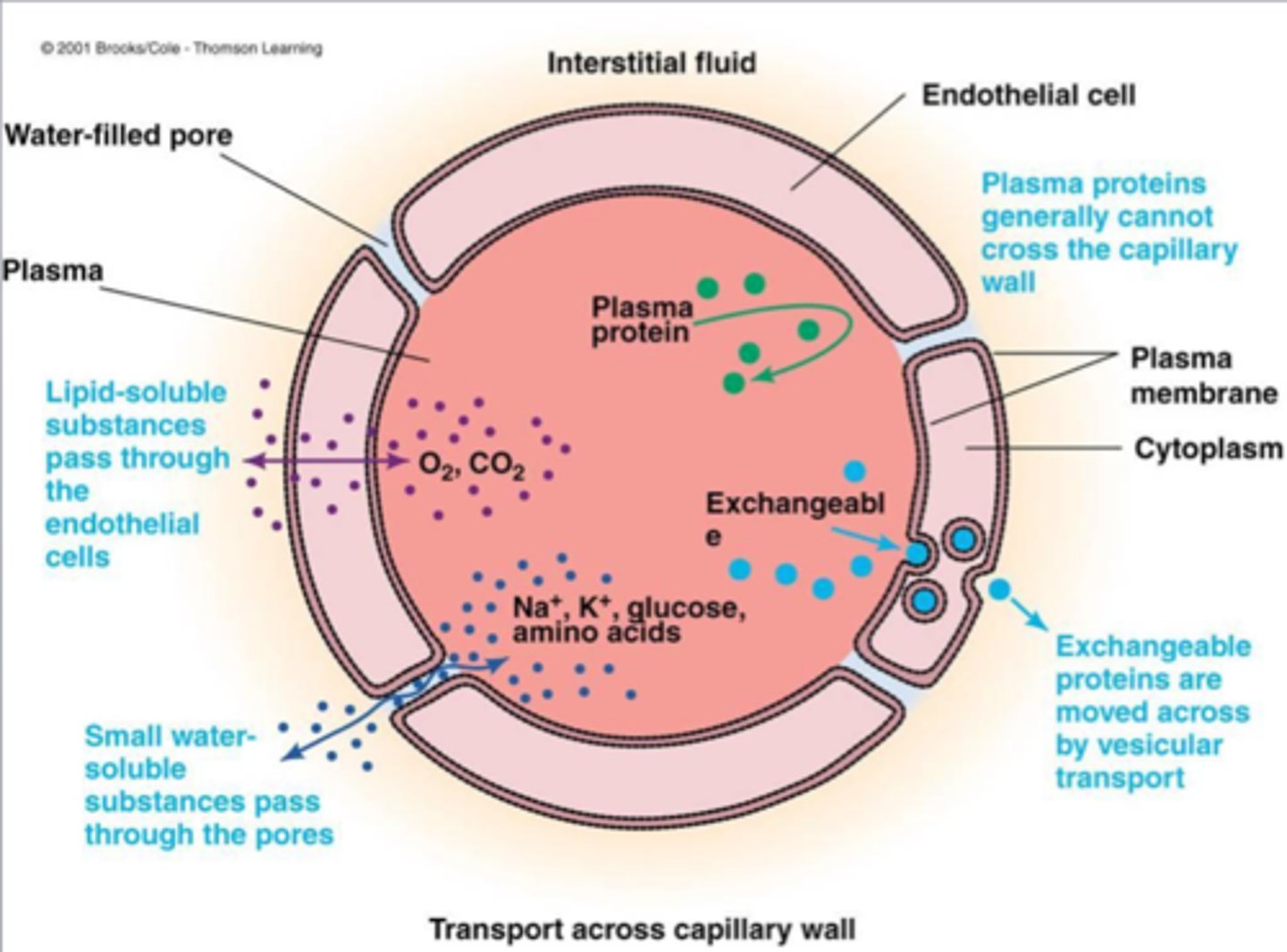
Capillary filtration and reabsorption
Continuous exchange of fluid across the capillary wall.
= the control of fluid (specifically water) between the plasma (in the capital) and interstitial compartment
In addition, to water through cell-cell junctions
Filtration = moving from blood/capillary → tissue
Reabsorption = fluid moving from interstitial fluid back into the capillary
hydrostatic pressure
pressure exerted by a fluid within a confined space (mmHg)
Osmotic pressure (mmHg)
force exerted by a dissolved substance to draw water towards it to try and equilibrate the [ ] of molecules across of membrane
Ions tend to balance each other on either side of the capillary that usually contribute to osmotic pressure → dissolved plasma proteins
4 pressures that depict filtration adn reabsoribtion and their common values in mmHg
- capillary hydrostatic pressure (P_c)
= 37 - 17mmHg
- Interstitial fluid hydrostatic pressure (P_IF)
= 1mmHg
- Capillary Plasma protein osmotic pressure (π_C)
= 25mmHg
- Interstitial plasma protein osmotic pressure (π_IF)
= 0mmHg
Net filtration pressure
the difference between net hydrostatic pressure and net osmotic pressure
= Pc + πIF - PIF - πC
(outward pressures) - (inward pressures)
*if tjis. results in a (+) there is a net outward movement (filtration)
define the 4 presures
Capillary hydrostatic pressure (Pc) = pressure exerted from the blood in the capillary
Interstitial fluid hydrostatic
pressure (PIF) = the pressure exerted by the fluid in the interstitial space (the fluid between cells) on the capillary wall
Capillary Plasma protein osmotic pressure (πC) = the pulling force created by proteins (mainly albumin) inside the capillary that draws water INTO the capillary
Interstitial plasma protein osmotic pressure (πIF) = the pulling force created by proteins in the interstitial fluid that draws water OUT of the capillary (into the tissues)
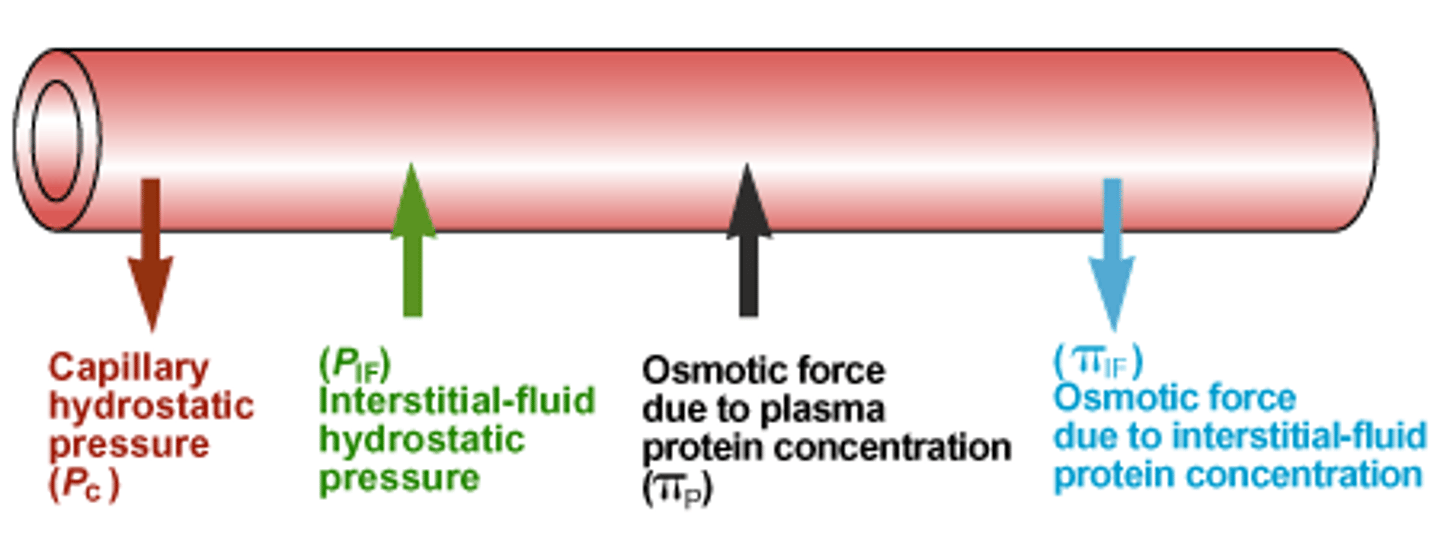
Think of capillary with 2 distinct ends!!
Net filtration pressure at arterial vc venous end
arterial end:
NFP = (+) --> net movement outward=filtration
(20L/day)
venous end:
NFP = (-) --> net movement inward=reabsorbtion
(17L/day)
what variables change Net fiiltreation pressure at arterial vs venous end
Capillary hydrostatic pressure (PC) is the only changing value bc as fluid is leaving the capillary to tissues (filtration) its lowering the blood pressure. Once at venous side Pc is much lower causes inward forces (like πC) to dominate → reabsorption
the other variables remain fairly contsant
- P_IF remains low at both ends bc the interstitial fluid is spread over a large surface area
- both osmotic pressure stay constant bc plsma proteins do not often pass endothelial cells (πC ab 25 and πIF ab 0)
capillary filtration graph
the capillary pressure vs the capillary length from arterial to venous end
- inward pressure (πC + PIF) = the blue line, constant
- outward pressure (πIF + Pc) = red line, decreasing as capillary hydrostatic pressure drops
transition point = point where outward pressure drops below inward pressure changing movment from untrafiltration to reabsorbtion
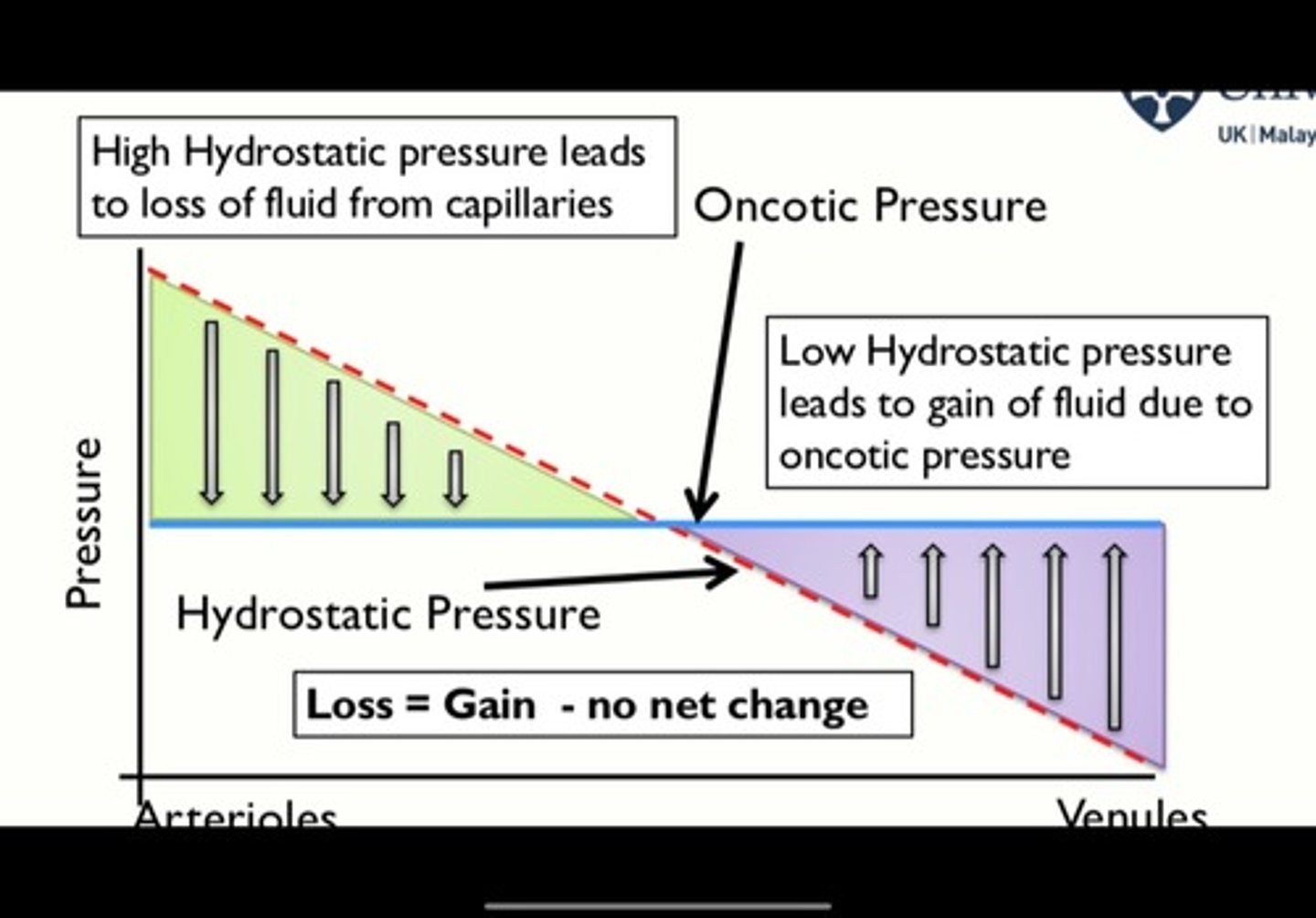
capillary filtration graph when upstream arterioles vasodilate
more blood travels into capillaries --> Pc ↑ --> outward pressure shifts right (above normal parallel)
causes transition point to be latter along the cap. length
OUTCOME = FILTRATION>REABSORBTION
(look at graph)
capillary filtration graph when upstream arterioles vasoconstrict
LESS blood travels into capillaries --> Pc ↓ --> outward pressure shifts left (below orginal)
causes transition point to be earlier along the cap. length
OUTCOME = REABSORBTION>FILTRATION
(look at graph)
What happens to the fluid that is filtered but not reabsorbed?
If 20L filtered, but only 17L reabsorb, 3L/day are missing
We get them back with the lymph system!!!
EDEMA
excess fluid accumulates in the interstitial space around our bv and cell --> causing swelling
eg.
- Edema due to trauma eg. sprained ankle
- Elephantiasis
Due to lamage to lymphatic system caused by parasite
3 functions of the lymphatic system
- fluid balance,
- immune surveilance
- movement of immune cells
how does lymp. system balance fluid
Removes excess fluid from interstitium and returns it to blood
system Made up of lymphatic vessels parallel to venous circulation until it reach the vena cava where it will dump the lymph after having it checked (ensure venous return stays the same)
ussually 3L/day
how does lymph. sys do immune surveilance and movemnet of immune cells
- Lymph vessels pass by lymph nodes filled with specialized immune cells, acting as a checkpoint
movement of immune cells
- Certain immune cells in the lymph node will get activated and move into the circulatory system through the lymph vessels
(e.g. thought vena cava or diffuse through lymph capillaries)
lymphatic vessel structure
- open circulation = Unlike blood vessels (which are a closed loop), lymph vessels start as open-ended tubes in tissues (allows them to pick up fluid that leaks out of capillaries from the surrounding tissue)
- single layer of OVERLAPPING endothelial cells
- smooth mucle in large vessels
- one-way valves to prevent back flow
since lymph system doesn't have the heart to help pump the fluid to vena cava how does it move it forward
- mooth muscle
in larger vessels to create rhythmical contractions to propel them
- surrounding tissues also help by compressing the vessels
How do lymph vessels collect interstitial fluid?
Lymph vessels' overlapping endothelial cells allow for the interstitial fluid to enter the vessel when the interstitial pressure is greater than the pressure i n the lumen