4: eyelids and lacrimal (copy)
1/120
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
121 Terms
eyelids and the lacrimal system
eyelids
the eyelids, or palpebrae are fold of skin and tissue that when closed cover the globe.
what are the 4 main functions of the eyelids
cover the globe for protection
move tears toward drainage at the medial canthus on closure
spread the tear film over the anterior surface of the eye on opening
contain structures that produce the tear film
on closure the upper eyelid moves down to cover the cornea
whats lagophthalmos
refers to incomplete closure of the eyelids
cause may be physiolgic , mechanical or paralytic
tarsal section
first crease is top of cornea
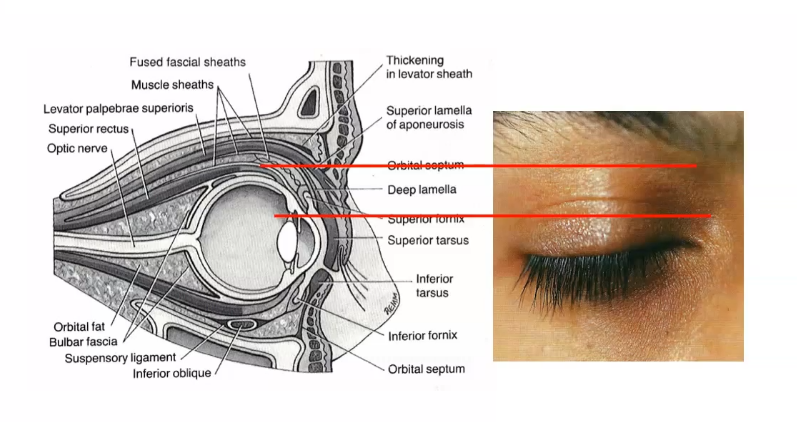
palpebral fissure
area betwee the open eyelids.
upper lid just covers the superior limbus when one eyes are open
upper and lower eyelids meet at the corners of the palpebral fissure in the lateral and medial canthi
what is the floor of the lacrimal lake
the plica semilunaris
this narrow screscent shaped fold of conjunctiva , located in medial canthus, allows lateral movement of the eye without stretching the bulbar conjunctiva
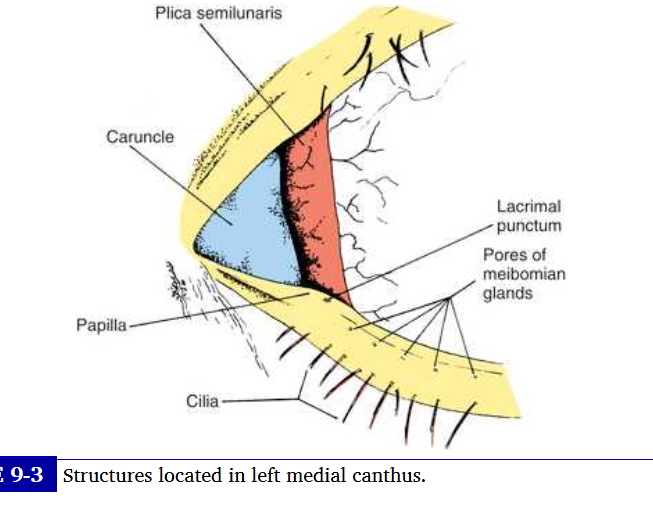
carnucle
small pink mass of modified skin located just medial to the plica. covered with epithelium that contains goblet cells and fine hairs and their associated sweat and sebaceous gland
upper eyelid
extends to the eyebrow and is divided into the tarsal and the orbital parts
the tarsal portion
lies clostest to the lid margin, rests on the globe and contains tarsal plates
the skin i sthin and the underlying loose connective tissue is devoid of adipose tissue.
orbital portion
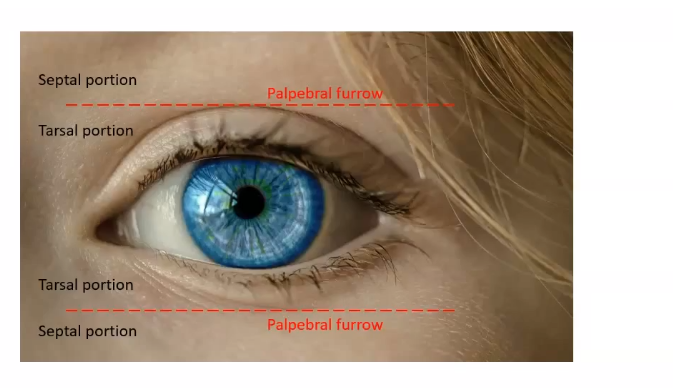
extends from the tarsus to the eyebrow , and a furrow- superior palpebral sulcus- separates the tarsal portion from the orbital portion
This sulcus separates the pretarsal skin, which is tightly adherent to the underlying tissue, from the preseptal skin which is only loosely adherent to ts underlying tissue which contains a cushion of fat
surafce anatomy of the right eyelid
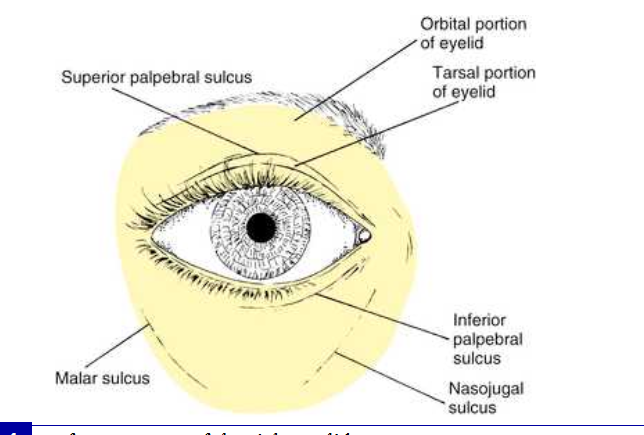
inferior palpebral sulcus
in the lower eyelid, this seperates the lower lid into tarsal and orbital parts.
the tarsal portion rests against the globe and the orbital portion extends from the lower borde of the tarsus onto the cheek extending just past the inferior orbital margin to the nasojugal and malar sulci
eyelid margin
rests against the globe and contains the eyelashes and the pores of the meibomian glands, the clia (eyelashes) are arranged at the lid margin in a double or triple row
lashes curl upwards and down on the lower lid
eyelashes are richly supplied with nerves, causing them to be sensitive to the slightest touch , which we elicit a reflex - blink
abnormalities affecting cilia
various epithelial diseases can cause madarosis ( loss of lashes) or trichiasis (misdirected growth) in which the eyelashes grow toward rather than away from palpebral fissure. contact with the cornea can cause irritation anf painfl abrasions can lead to ulceration
epilation can remove the problem lashes
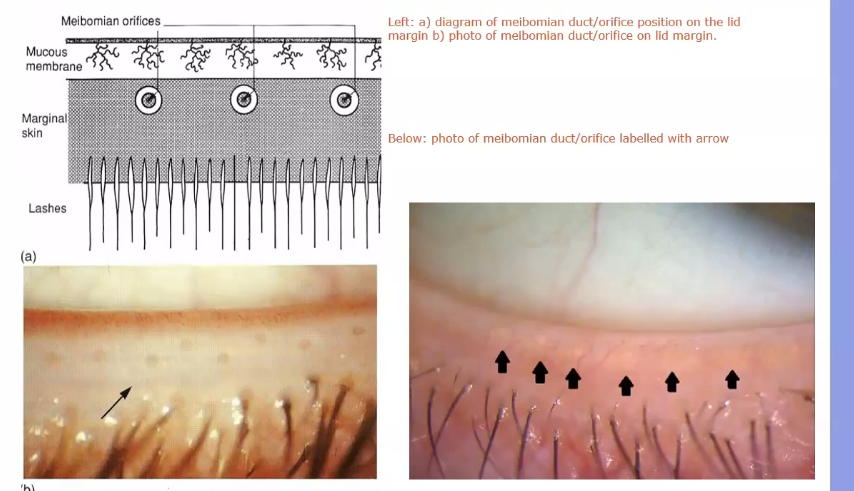
pores of meibomian glands
located posterior to the cilia, and the transition from skin to conjunctiva, the mucotaneous junction, occurs posterior to these openings
a groove called the gray line runs along the eyelid margin between the cilia insertions and the powers of the meibomian glands
this groove is the location of a surgical plane that divides the lid into anterior and posterior portions
eyelid margin divisions
2 parts:
the medial one sixth is the lacrimal portion and the lateral 5/6 is the ciliary portion,
division occurs at the lacrimal papilla
a small elevation containing the lacrimal punctum, the opening that carries the tears into the nasolacrimal drainage system
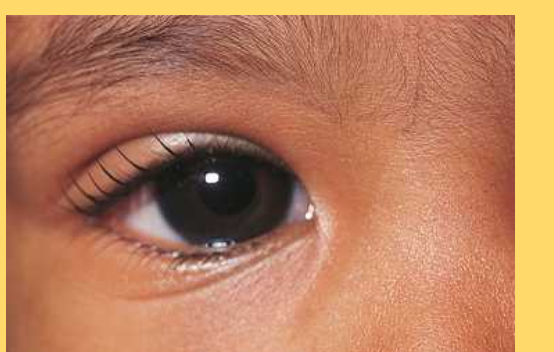
epicanthus
vertical fold at the nasal canthus in the medial area of the upper eyelid and terminating in the nasal cathus area
common in babies
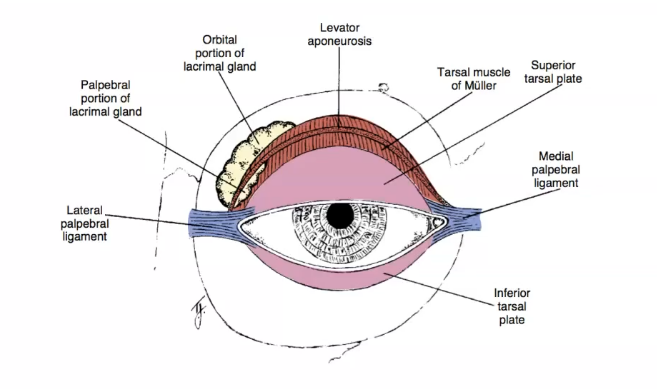
tarsal plate
toughest part - protective area of eyelid
made of connective tissue
protects from foreign bodies
covers the globe
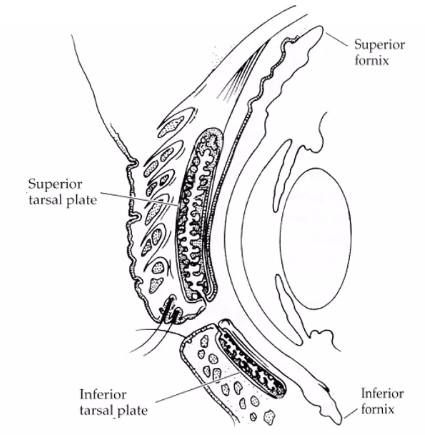
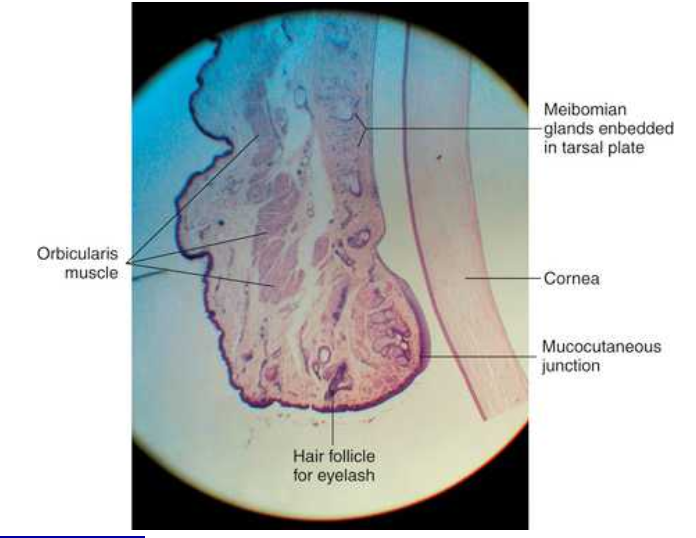
cross section of middle of the eye
the tarsal meibomian glands are embedded in the tarsal plates. Their ducts empty onto the lid margins. they secrete lipid which forms part of the pre ocular rear film
superior lid the tarsal plate is bigger
meibomian gland
meibomian gland will several alveoli emptying into a single duct
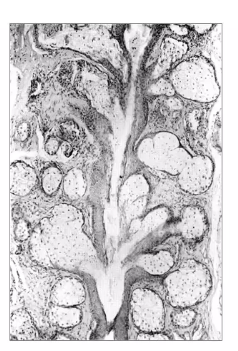
tarsal plate scan
runs all the way up
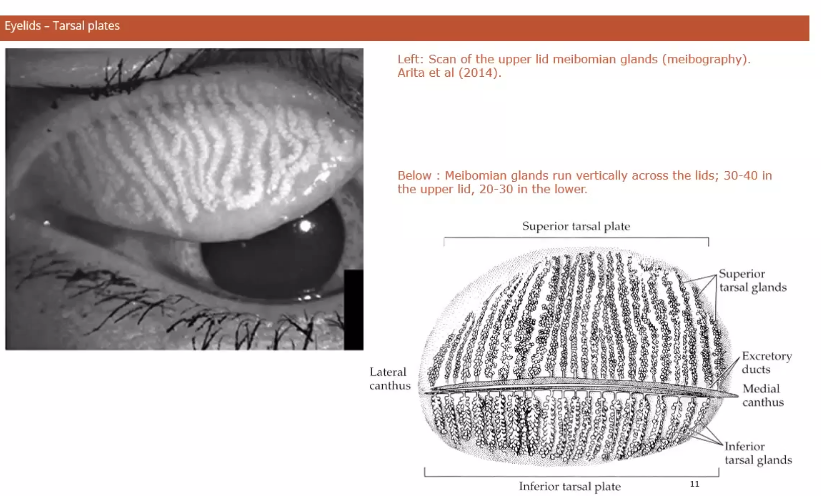
tarsal glands on the edge of the lid
glands exiting at the edge of the lids
in between the lashes and ocular surface and conjunctiva
when squeezed, the glands secrete oil
orbicularis muscle
the striated fibres of the orbicularis oculi muscle are located below the subcutaneous connective tissue layer and encircle the palpebral fissure from the eyelid magin to overlap onto the orbital margin, muscle divided into 2 regions- palpebral and orbital
palpebral portion
the palpebral portion of the orbicularis oculi muscle occupies the area of the eyelid that rests on the glod and is closest to the eylid margin
sometimes divided further into pretarsal and preseptal parts
composed of semi circles of muscle fibres that run from the medial orbital margin and the medial palpebral ligament to the lateral palpebral raphe
contraction of orbicularis assists in moving the tears through the canaliculi into nasolacrimal drainage system
also another muscle in this portion - riolan, lies near the lid margin on both sides of meibomian gland openings , it maintains lid margins close to the globe
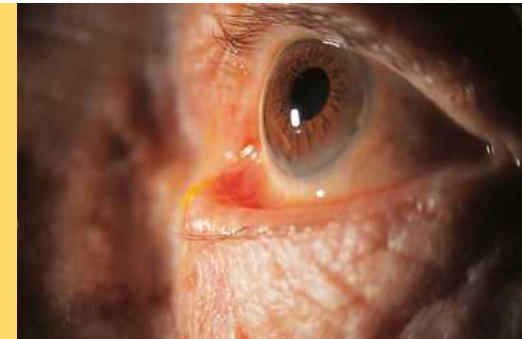
ectropion
eversion of the eyelid margin. common cause of which is loss of muscle tone, a normal occurence in aging
lacrimal punctum no longer in position to drain tears from lacrimal lake
epiphora- an overflow of tears onto the cheek may occur
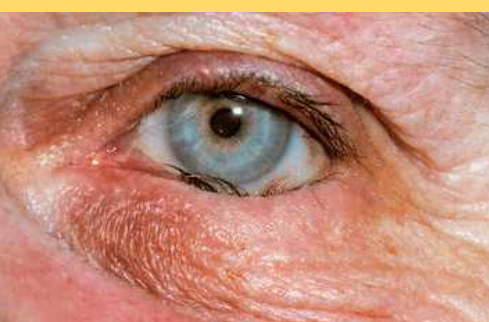
entropion
inversion of the lid margin may result from spasm of the orbicularis oculi muscle causing lid margin to turn inwards,
this puts th eyelashes in contact with the glob =e and can cause corneal abrasion
orbital portion of orbicularis oculi muscle
attached superiorly to the orbital margin medial to the supraorbital notch
fibres encircle the area outer to the palpebral portion and attach inferiorly to the orbital margin , medial to the infraorbital foramen
these centric fibres extend throughout the rest of the lid and over the orbital rim
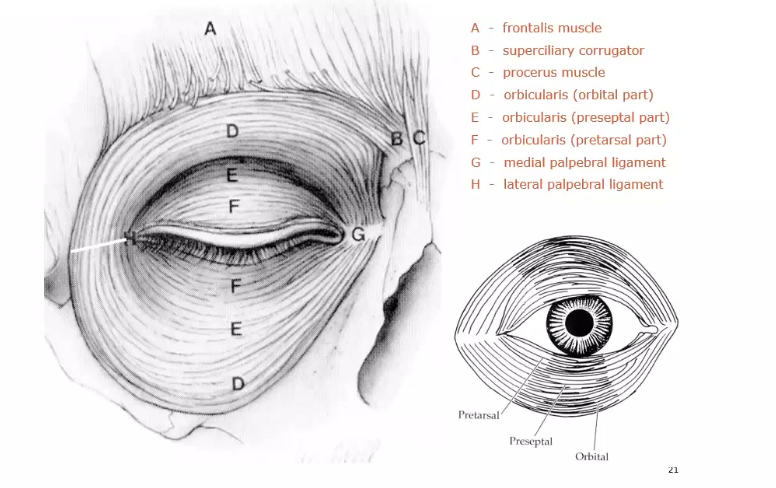
orbicularis action
ring shaped muscle
orbic oculi is innervated byy cranial nerve VII
contraction of palpebral portion closes eyelid gently and the palepbra; orbicularis is the muscle of action in an involunatry blink and voluntary wink; relaxation of the levator muscle follows
the antagonist to the palpebral portion of the obicularis is the levator muscle
the antagonist to the orbital portion is the frnotalis muscle
when sphincters contract , palpebral aperture gets smaller
spontaneous involuntary blinking
renews the precorneal tear film
reflex blink
protective and may be elicited by a number of stimuli- loud noise, cilial touch , conjunctival.
when orbital portion of orbicularis oculi contract the eye is closed tightly and the areas surrounding the lids- foreheadm teple cheek, are involved in contaction
this is a protective mechanism
forcing the eyelids are closed too tightly forces compressing the orbital contents can significantly increase intraocular pressure
superior palpebral levator muscle
is the retracctor of the upper eyelid
located within the orbit above the globe and extends into the upper eyelid.
originates on the lesser wing of the sphenoid bone aboove and infront of the optic foramen
superior transverse ligament- act as a fulcrum, changing the anteriposterior direction of the levator to superinferior.
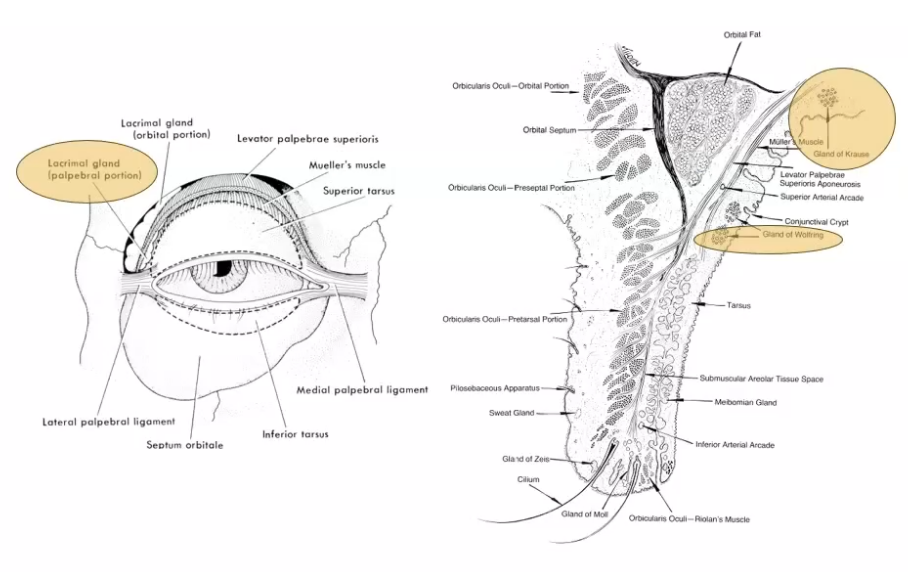
picture shows saggital section of upper lid
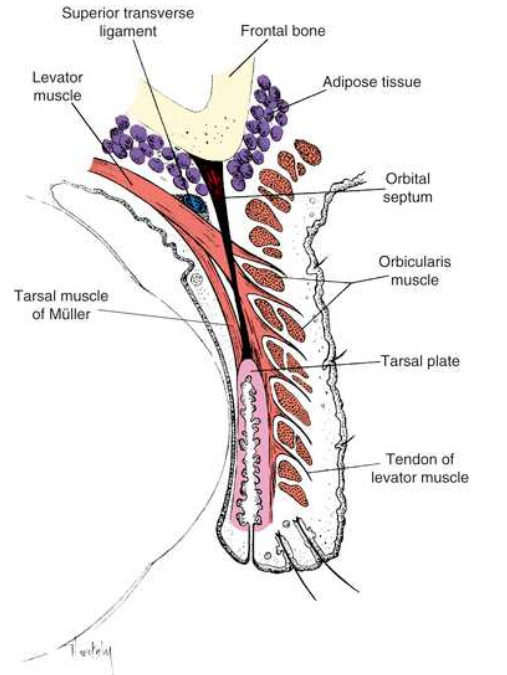
superior transverse ligament
a fibrous band that spans the anterior superior orbit from the rochlea to the lacrimal gland fascia
provides support for the upper lid and orbital structures as well as acting a a fulcrum.
ligament is located at the point where the levator muscle fibres end and the aponeurosis begins
levator aponeurosis
as it enters the eyelid, the levator becomes a fan shaped tendinous expansioin, the levator aponeurosis
spreads out into an extensive sheet posterior to the orbital septum.
fibres of aponeurosis penetrate the orbital septum and extend into upper lid
these fibres pass through submuscular connective tissue ; posterior fibres insert into lower anterior surface of tarsal plate, anterior run between the muscle bundles of orbicularis to nsert into the skin of eyelid
this attachment of fibres from levator aponeurosis anchors the skin to underling tissues in pretarsal area of eyelid and creates the palpebral sulcus
what are the 2 side extensions of the aponeurosis
referred to as horns.
the lateral horn helps to support the lacrimal gland by holding it against the orbital roof , dividing the gland into orbital and palpebral lobes
lateral horn then attaches to the lateral palpebral ligament and lateral orbital tubercle
medial horn is attached to the medial palpebral ligament and medial orbital rim
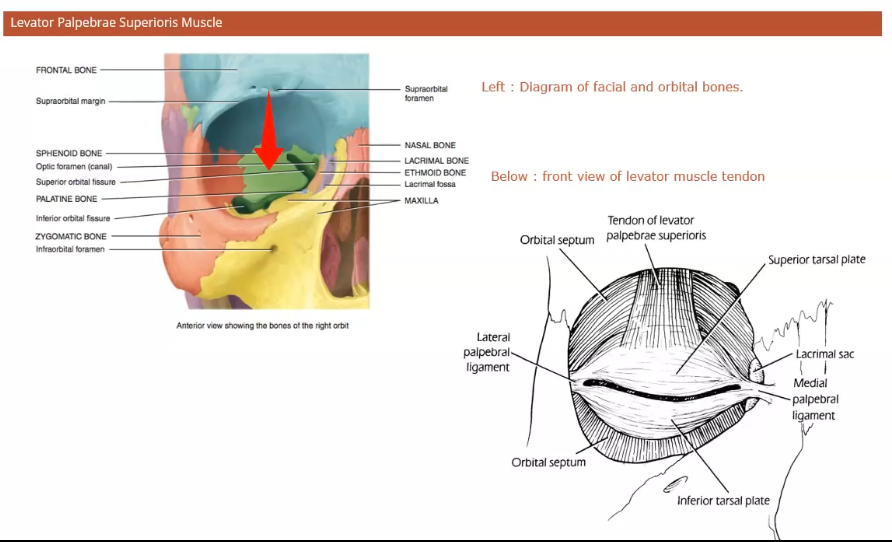
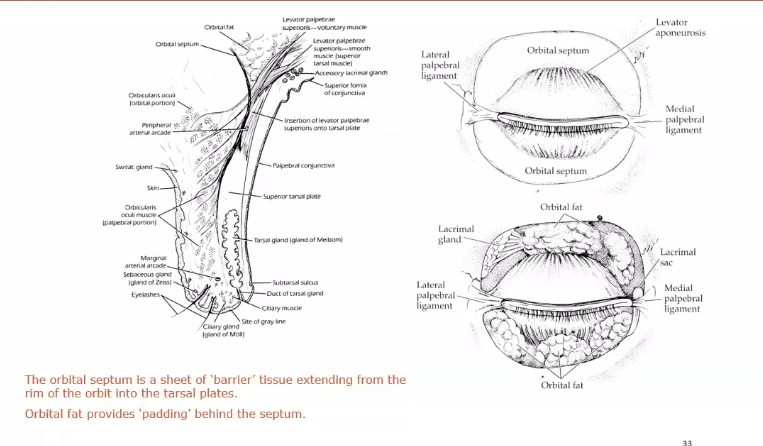
orbital area viewed in front with skin, subcutaneous tissie and orbital septum removed
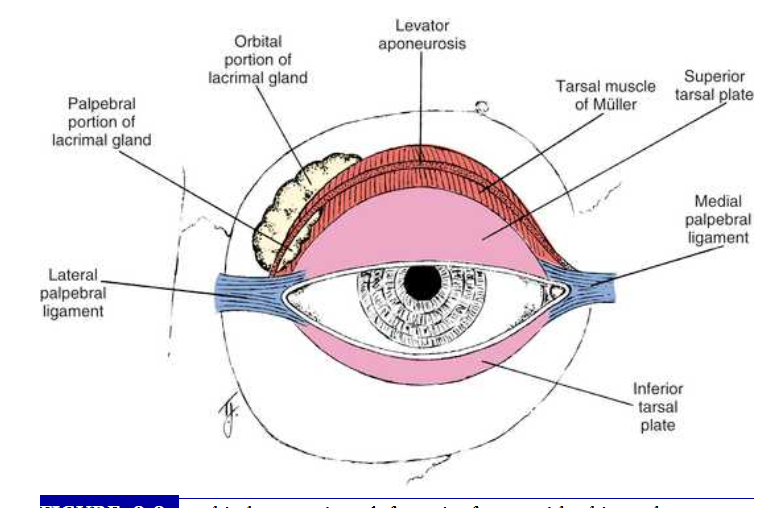
levator action (levator muscle ) superior
attached to the tarsal plate by aponerosis
contraction of the levator muscle causes elevation of the eyelid
connection between the sheath of the levator and sheath of superior rectus coordinates eyelid position wih eye position so the eye is elevatedm lid is raised
levator muscle has to flatten out to be attached
when the muscle contracts the tarsal plate is pulled back
what is the levator muscle innervated by
innervated by the superior division of the oculomotor nerve, cranial nerve III
what 2 muscles open the superior lid
levator palpebrae superiosis
superior tarsal muscle
what muscle pulls down inferior lid
inferior tarsal plate
how are the eyelids closed
closed by the relaxation of the levator and contraction of theorbicularis oculi muscles.
the tonic activity of the levator and relaxation of orbicularis oculi holds eyelid open.
in a blink the tonic activity of the levator muscle is suspended , and bursts of activity the orbiculatis rapidly lowers the lid
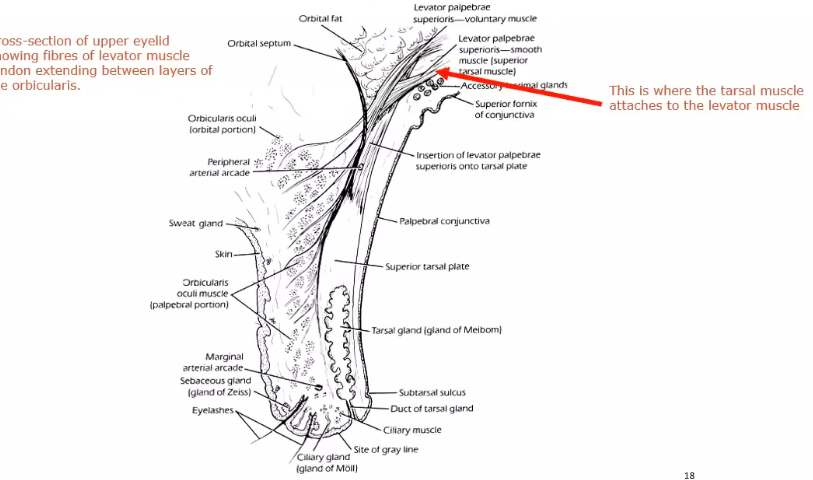
levator palpebrae superiosis muscle (levator muscke)
the muscle goes up and over the eyeball and attaches to the skull
sphenoid bone is where it attaches ot
tarsal muscle attaches to levator muscle
evator attaches to tarsal plate
retractor of the lower eyelid
capsulopalpebral fascia (lower eyelid aponeurosis )
an anteror extension from the sheath of inferior rectus muscle and suspensory ligament
inserts into the inferior edge of the tarsal plate
this insertion coordinates the lid position with globe movement
lower eyelid is depressed on globe depression and the lower eyelid elevates slightly on upwards movement of the globe
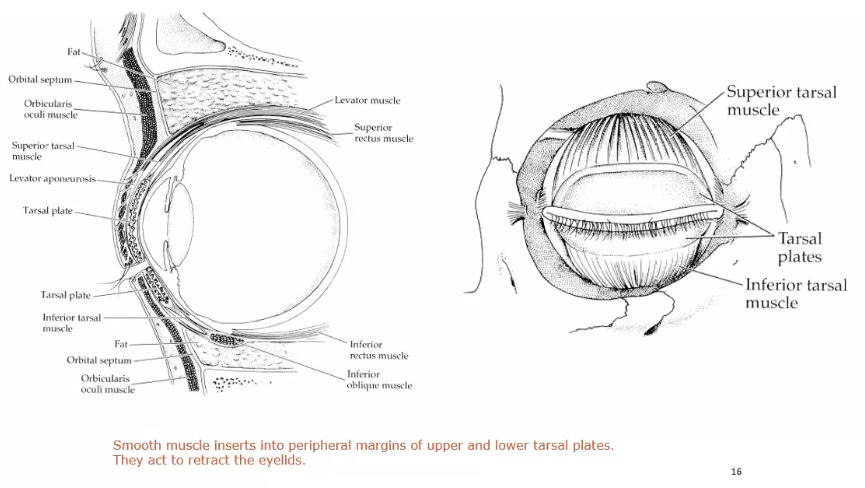
tarsal muscle (muller )
the superior tarsal muscle is composed of smooth muscle and originates from the postoinferior apect of the inferior muscle
the smooth muscle fibres appear within the striated muscle at the point whch the muscle becomes aponeurootic
supeiror tarsal inserts on the superior edge of tarsal plate
contraction of the tarsal muscle can provide 2mm of additional lid elevation
inferior tarsal muscle
found on lower eyelid
arises from inferior rectus sheath muscle and inserts into the lower conjunctiva and lower border of tarsal plate
both tarsal muscles are innervated by sympathetic fibres that widen the papebral fissue when activated
superior and inferor tarsal muscles
these are just underneath the levator muscle
smaller and smoother
attaches to levator muscle
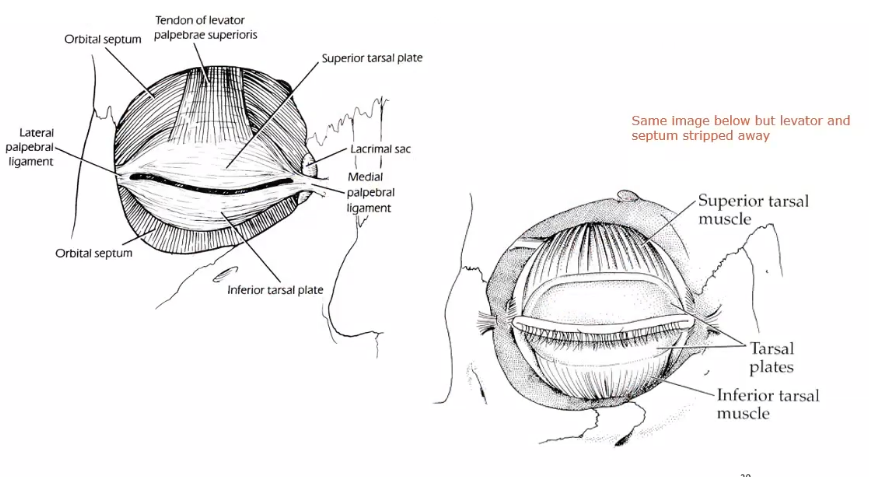
tarsal plate
each eyelid contains tarsal plate that gives the lid rigidity and structure and shapes it to the curvature of the globe
palpebral ligaments
also known as tarsal ligaments
bands of dense connective tissue connecting the tarsal plates to the orbital rim and holding the tarsal plates in position against the globe during eye and lid movement
meibomian glands (tarsal glands )
sebaceous glands embedded in the tarsal plates
long multilobed glands resemble a large bunch of grapes and are arranged vertically such that their openings are located in a row o=along the lid margin posterior to cilia
in the upper and lower lid
secrete the outer lipid layer of the tear film
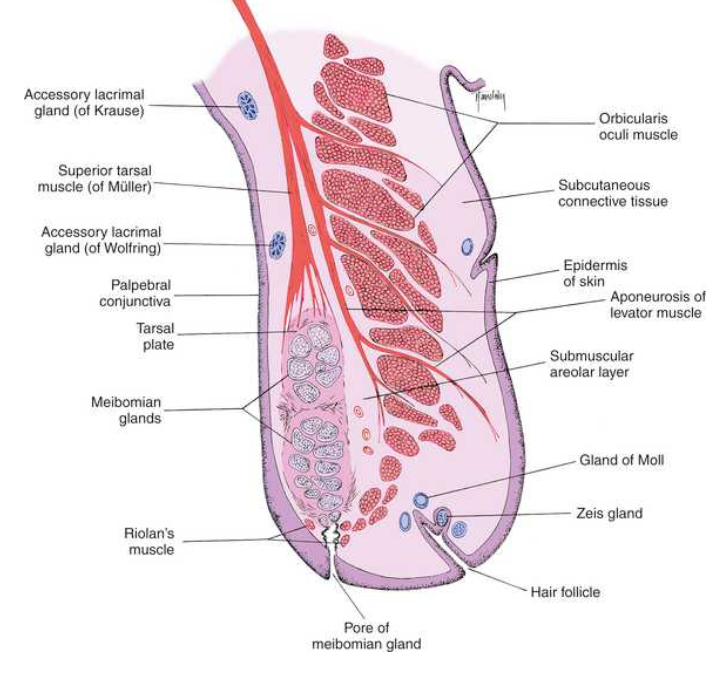
saggital section of the eyelid
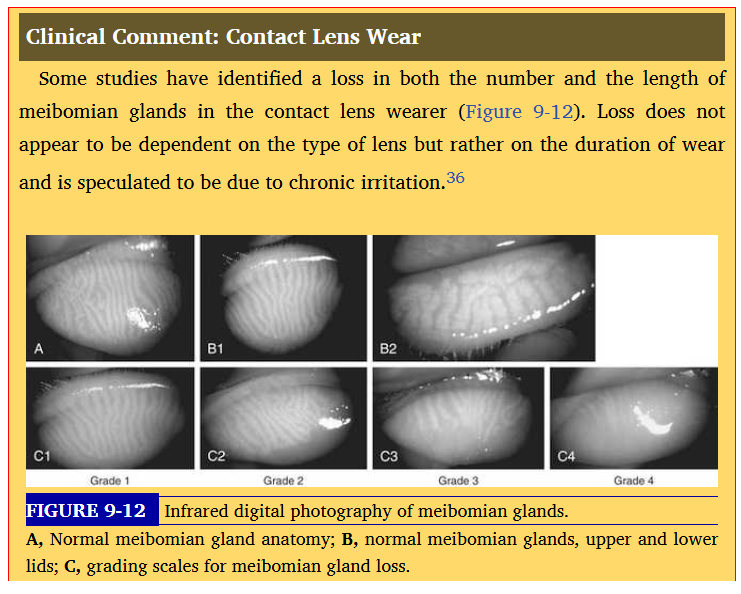
contact lens wear
loss of number of meibomian glands in cls
glands of zeis
secrete sebum into the hair folicle of the cilia coating the eyelash shaft to keep it from becoming brittle
glands of moll
modified sweat glands
located near the lid margin anf their ducts empty into the hair folicle, into the zeis gland
accessory lacrimal glands of krause
located in stroma of conjunctival fornix, and the accessory lacrimal glands of wolfring are located along orbital border of tarsal plate
glands are oval .
secretion contributes to the aqueous layer of the
more on orbicularis muscle
striated muscle along the lid margin small muscle bundles located on both sides of meibomian glands represent a specific part of orbiculairs, the ciliary part - riolans muscle,which holds the lid margin against the globe
attachments are nasal and temporal by tendons
medial- attached to maxillary process
temporally- zygomatic bone
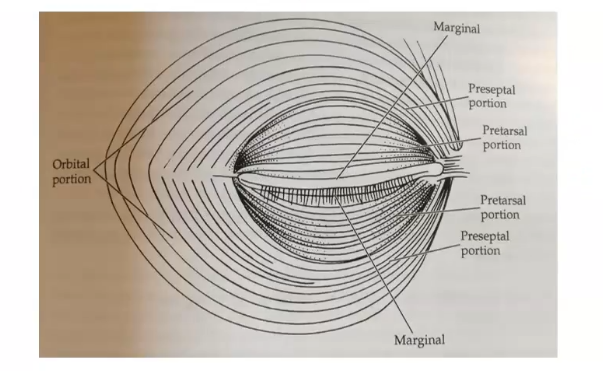
orbital portion of orbicularis
lies in front of the bones forming the orbit
preseptal portion of orbicularis
lies in front of the orbital septum
pretarsal portion of orbicularis
lies in front of the tarsal plate
marginal / ciliary portion of orbicularis
closest to the lid margin
submuscular areolar layer
posterior to orbicularis
loose connective tissue
separates the muscle from the tarsal plate
between this layer and tarsal plate lies the pretarsal space
pretarsal space is between the orbicularis and orbital septum
where are the superor tarsal muscles located
above the superior tarsal plate and insert into its upper edge
what are the tarsal plates composed of
dense connective tissue
collagen fibrils of this tissue are uniform size and run vertically and horizontally to surround meibomian glands
what 2 layers are the palpebral conjuctiva composed of
stratfied epithelial layer and connective tissue stromal layer - submucosa
as conjunctiva lines the lid squamous l=cells are replaced by cuboidal and columnar cells forming a stratfied columnar mucoepithelial layer
this layer continues into the bulbar conjunctiva vecoming continous with corneal epithelium
whats the surface of superficial conjunctival cells and thei microvilli covered with
glycocalyx
malanin granules found in cytoplasm of conjunctival epithelial cells near the limbus
goblet cells
produce mucous component of the tear film located in epithelium of conjunctival
most dnense at the fornix
subsurface vesicles fuse with epithelial cells increase adg=herence to tear film to the globe
goblet cells are scattered thoughout the stratofied columnar conjunctival epithelium
decrease with age and increases in inflammatory conditions as they produce mucin droplets that accumulate causing swelling in cells. surface cell thn ruptures releasing mucus
submucosa of the palpebral conjunctiva
thin in the tarsal portion of eyelid but gets thicker in orbital portion
loose vascularised connective tissue subdivided into an oter lymphoid layer and deep fibrous layer
immunoglobin A is in lymphoid layer making the conjucntiva an immunoglobically active tissue
types of blink- reflex
quickest - fully open to fully closed tales 20-30 ms
subconcious
tightest
could damage the eye
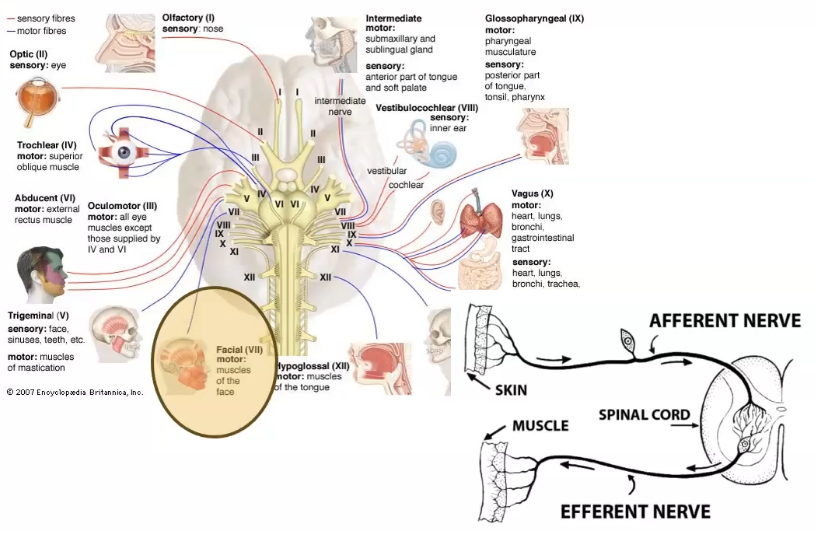
reflex arc
signals dont go to the brain, it goes straight to the spinal cord
using facial motor nerve which innervates orbicularis muscle
types of blink - spontaneous bilnk
using tarsal portion of the orbicularis
more slowly - 250 - 300 ms
less tight
in response to any reflex or stimuli
keeps the eye moist
vary depending on age and environment
if eye is super dry blink more, i
there to re new tear film
purpose for spontaneous blink
tear film spreads on the blink
types of blink - voluntary blink
accompanied by an upward and outward movement of the actual eyeball beneath the lid ( bells phenomenon)
lower lid moves the most during this type of voluntary blink
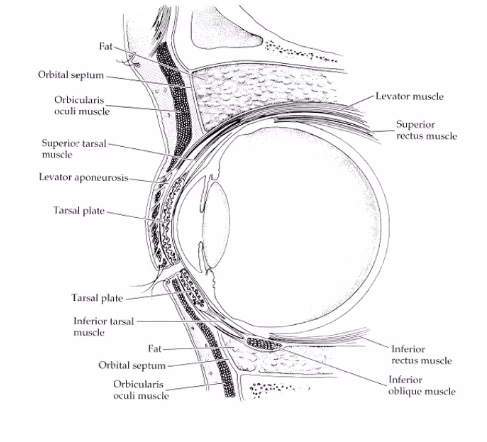
orbtal septum
barrier from the top of the tarsal plate up to the top of the orbit connextive tissue sheet
barrier between orbital rim and fat and the lids
keep stuff outsid the orbit
orbital fat provides padding behind the septum
orbital septum bigger than eyeball
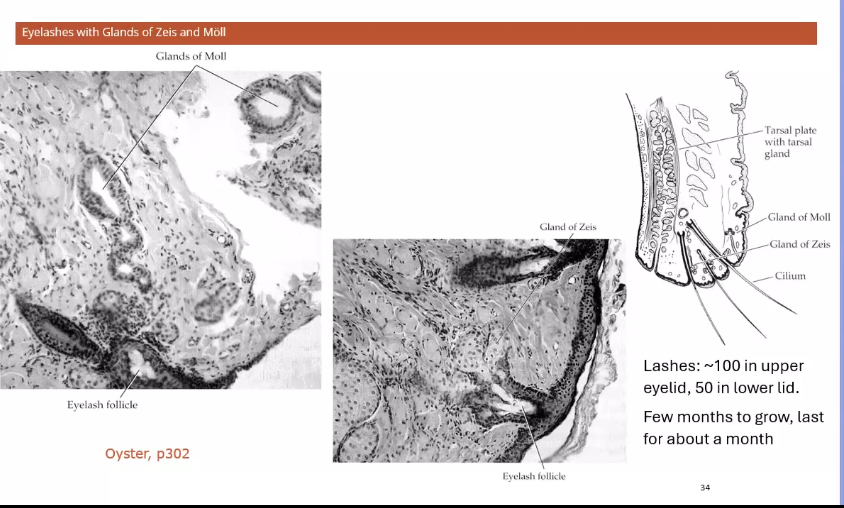
edge of eyelids
eyelashes
have glands of zeis and moll
secretes oily substances
these glands are associated with lashes- keeps them oily
lashes are for protection from debris
when the lashes are dry they struggle to portect from debris
so these glands secrete the oil
palpebral conjunctiva
dense vacular
regions of conjunctiva
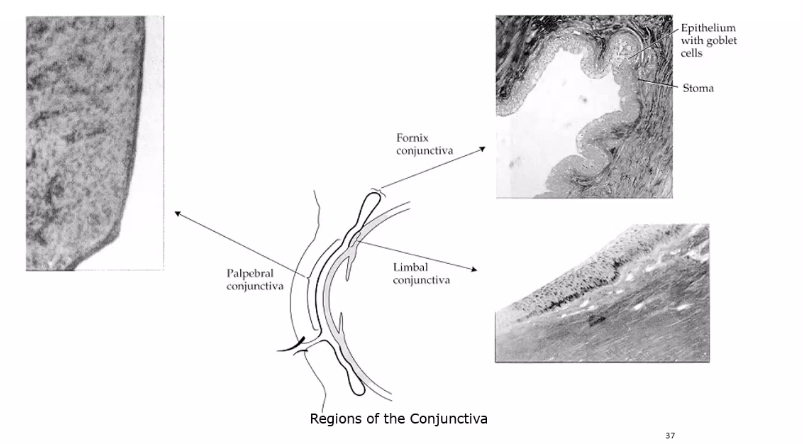
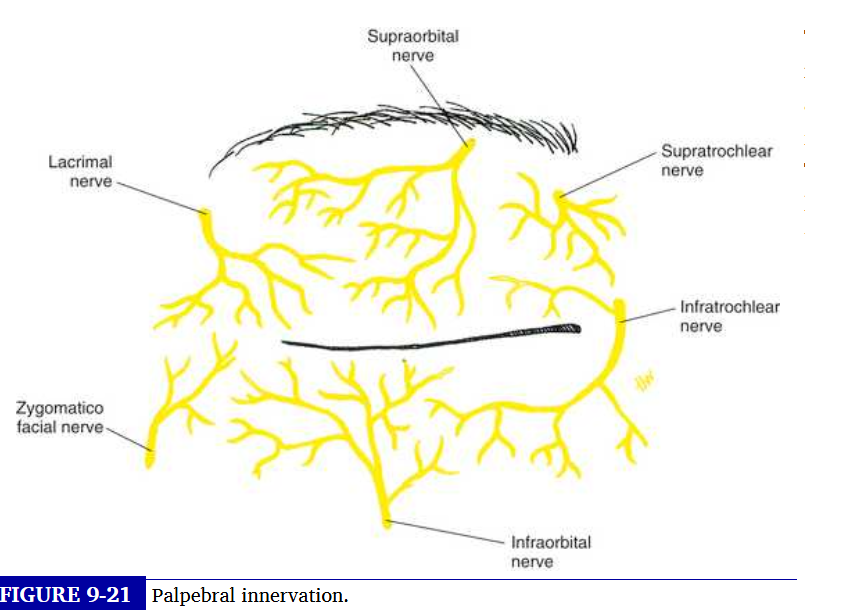
innervation of the eyelids
the opthalmic and maxillary divisions of the trigeminal nerve provide sensory innervation of the eyelids
upper is supplied by supraorbital , supra trochlear, infratrochlear and lacrimal nerves which are branches of opthalmic division
supply to the lower lid
infratrochlear branch of opthalmic nerve and infraorbital nerve, a branch of the maxillary division
motor control of the orbicularis muscle
done through the temopral and zygomatic branches of facial nerve
motor control of levator muscle
done through the superior division of the ocularmotor nerve
the tarsal smooth muscles are innervated by the sympathetic fibres from superior cervical ganglion
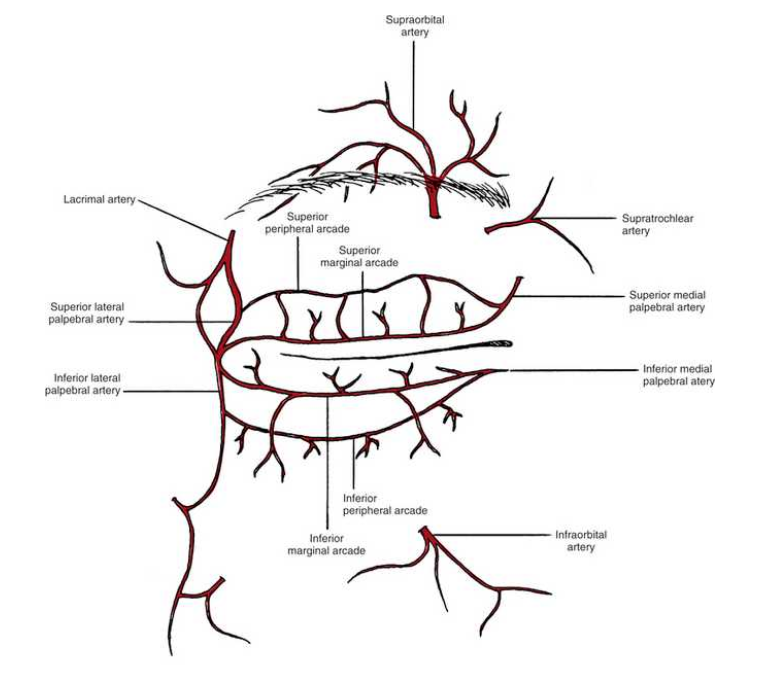
blood supply to the eyelid
blood vessels located in a series of arcades or arches in each eyelid
marginal palpebral arcade lies near lid margin and peripheral near orbital edge of tarsal plate
these vessels are branches from the medial and lateral palpebral arteries
and the arteries are branches from the opthalmic and lacrimal arteries
normal variations occur in the blood supply and most common variation is a lack of peripheral arcade in lower eyelid
opthalmic and carotid - superior blood supply
lacrimal system
lacrial fluid ( tears) production - lacrimal gland and ducts
location is superior temporal region of the orbit
function is secretion of aqueous tears and their transport to the conjunctival fornix
lacrimal tear drainage- lacrimal sac and nasolacrimal duct
location is nasal inferior region of the orbit
function is drainage of tears from conjunctival sac into the nasal cavity
tear film functions
optically smooth surface covers the anterior surface of the globe
keeps surface moist and serves as lubricant between globe and eyelids
traps debris and helps remove sloughed epithelial cells and debris
primary soruce of atmospheric oxygen for the cornea
antibacterial function protects against infection
flushing action revomes the cell debris and freign bodies
helps with corneal wound healing - provides a pathway for WBC
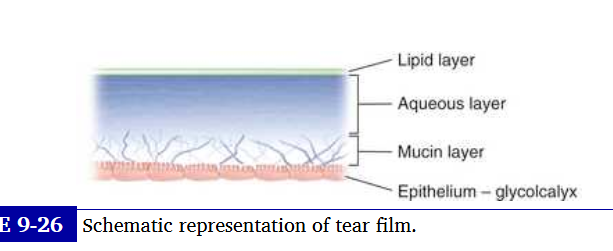
tear film layers
composed of 3 layers
lipid layer
aquous layer
mucous layer
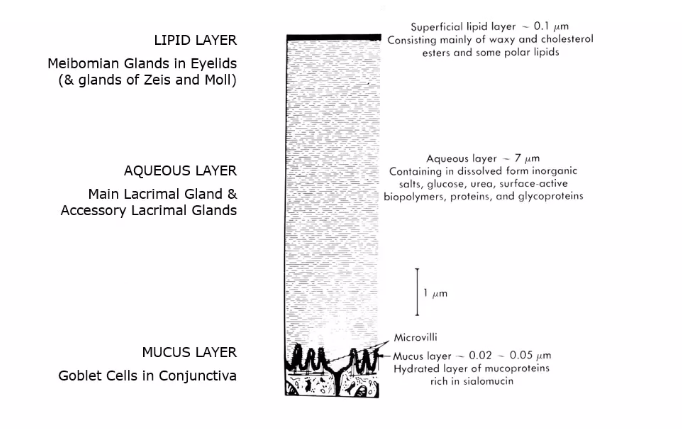
lipid layer
outermost layer containing waxy esters, cholesterol and free fatty acids, primarily produced by the meibomian glands
the layer retards evaporation snd porvides lubrication for smooth eyelid movement
aqueous layer
middle layer
contains inorganic salts, glucose , urea enzymes portients glycoprotiens anf antibacterial substances.
it is secreted by the main and accessory lacrimal glands
mucous layer
innermost layer
acts as an interface that facilitates adhesion of the aqueous layer of tears to the ocular surface
composed of the glycocalyx secretion from the surface epithelia and mucin produced and secreted by conjunctival goblet cells
mucins also bind and entrap bacteria and viruses blocking binding sites on microbes and preventing them from penetrating the ocular surface
base layer - mucus
primary mucus secretion is by goblet cells of the conjunctiva, secondary secretion is by the lacrimal gland and non goblet cells in conjunctival epithelium
function is to change tear dynamics:
helps viscosity when between blinks
helps maintain a stable tear film
low vsicosity in motion during blinks - aids tear film spreading
function also is that mucin adheres to cell debris and foreign bodies, and hydrophobic cell membranes to allow aqueous to stick
loss of mucus secretion increases tear film breal up and corneal dry spots
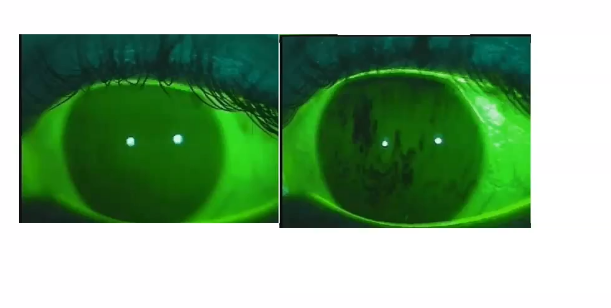
poor mucin layer is shown on the right ,
dark areas are dry spots
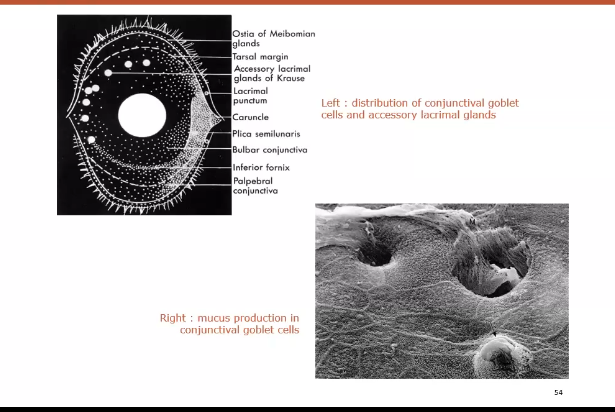
middle layer - aqueous
produced by lacrimal gland
most of the tear film is porduced here
acessory lacrimal gland ( keause and wolfring) are in conjunctiva and have the same structure as the main lacrimal gland
aq layer protiens- defence mechanism:
immunoglobin A ,
lactoferin- combats infection and inflammation
lysozyme: antimicrobial agent
tear specific prealbumin (TSP)
lacrimal secretory system
includes main lacrimal glabd, the accessory lacimal glands, meiobiam gland and conjunctival goblet cells
where is main lacrimal gland located
located in a fossa on the temporal side of the orbital pplate of the frontal bone, posterior to the superior orbital margin
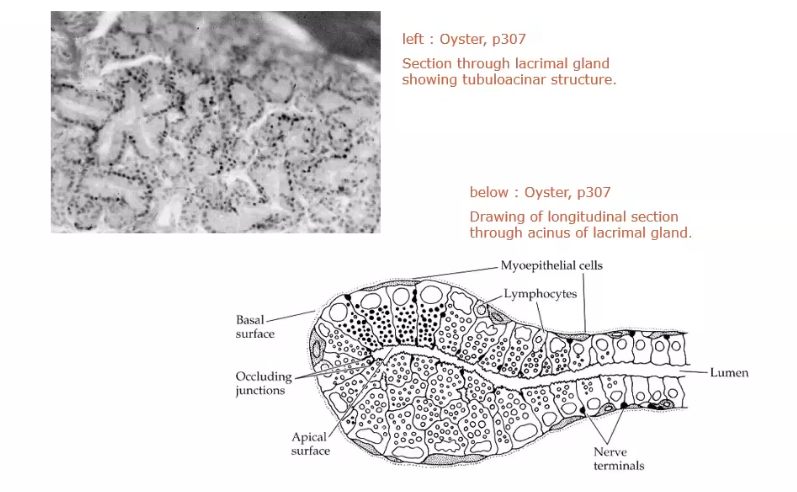
what does lacrimal gland consist of
lobules made up of numerous acini. each acinus is an irregular arrangment of secretory cells around a central lumen surroundedby an incomplete layer of myopithelial cells.
a network od ducts connects the acini and drains into one of the main excretory ducts
where are accessory glands located
in the subconjunctival tissue from the fornix area to near tarsal plate. basic secretion maintains the normal volume of aq portion of tears
reflex secretion increases volume in response to a stimulus
what is lacrimal gland supplied by
lacrimal artery, a branch of the opthalmic artery
sensory inervation is through lacrimal nerve , a branch of opthalmic division of trigeminal nerve
glad recieves vasomotor sympathetic innervation ad secretomotor parasympathetic innervation
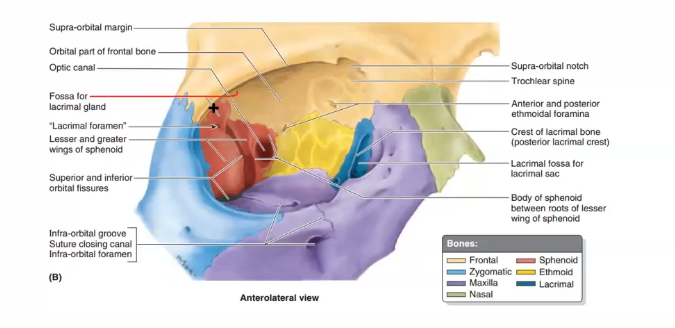
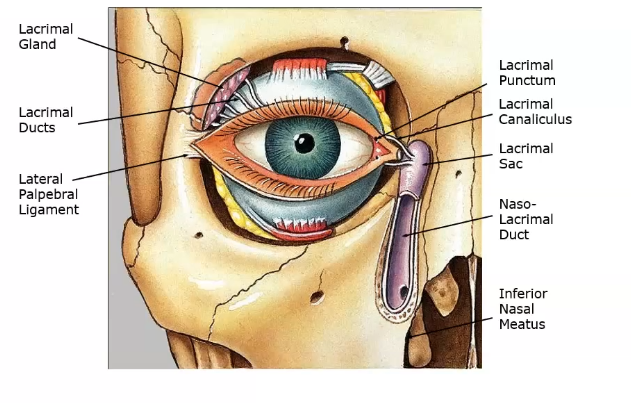
tear production and drainage
tears produced supero tenporally through lacrimal ductsonto ocular surface
the drained via canaliculi
then entes punctum
goes then lacrimal sac and through naso lacrimal duct and into the nose
lacrimal duct- goes from lacrimal gland to eye
nasolacrimal duct- goes from eyeto the nose
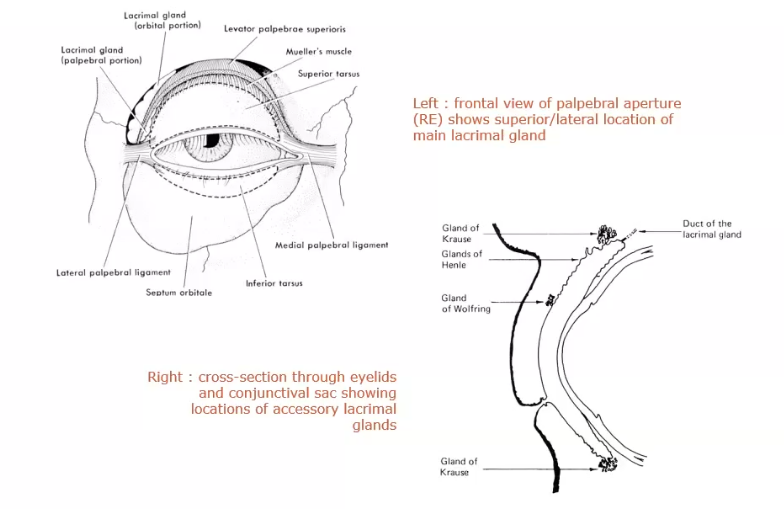
main and accessory lacrimal glands
have superior and inferior accessory and main glands
cross section of lacrimal gland
secretory granules helps create the aq layer
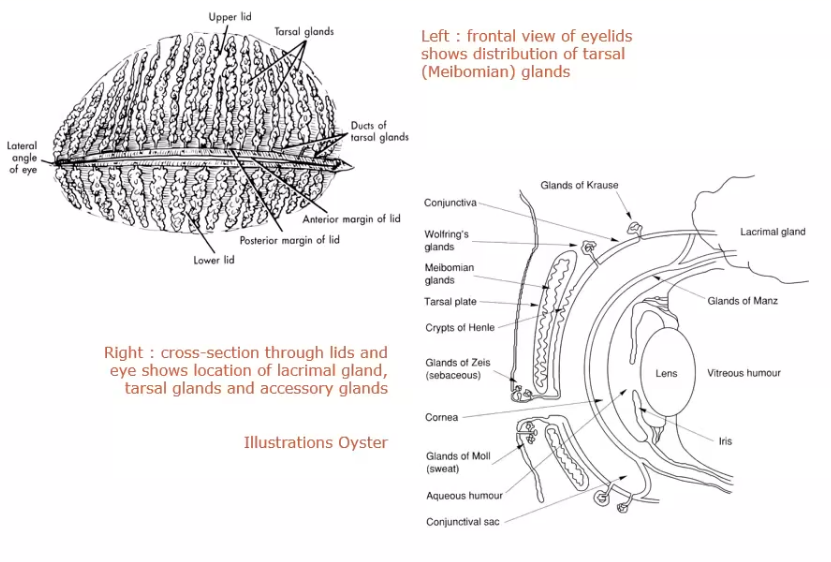
lipid layer
produced mainly from tarsal glands
makes lipid layer of tear film
primary lipid secretion is by tarsal glands and secondary secretion is by glads of zeis at the edge of eyelid
50 tarsal glands in upper 30 in lower
lipid secretion has a low melting point. forms a liquid at the temp of the ocular surface
lipid surface layer reduces evap of the aq tears
glands of the eyelid
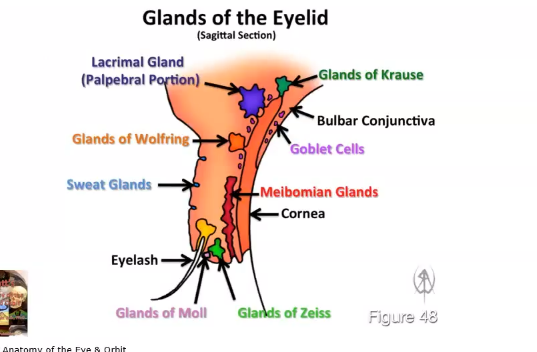
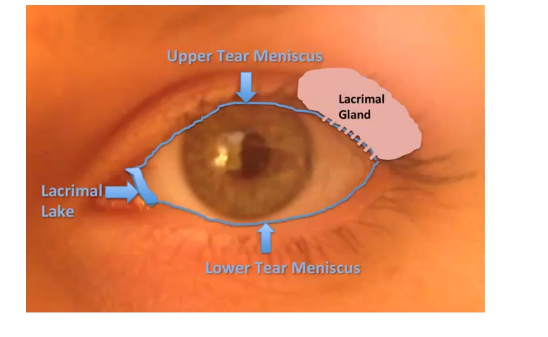
tear film distribution
lacrimal gland fluid is secreted into the lateral part of the upper fornix and descends across the anteriro surface of the globe
contraction of orbiculais forces meium out of the pores and lid motion can spread a thin lipic layer across the surface
each blink reforms the tear film spreading over ocular surface