VLP ultra flashcard set
1/282
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
283 Terms
canine puberty duration
6 months
what type of estrus cycle do canines have
monoestrus - one estrus per year
stages of the canine estrous cycle
proestrus
estrus - heat
metestrus
anestrus
when should a vaginal cytology begin
at the first sign of proestrus and repeat every few days until 70% cornified cells noted
ideal serial progesterone levels for breeding potential
>2ng/ml
5ng/ml preferred
how often should breedings take place
every other day for 2 - 3 breedings or until the female goes out of heat
how long does canine sperm live in uterus/oviducts of a female in estrus
4 - 6 days
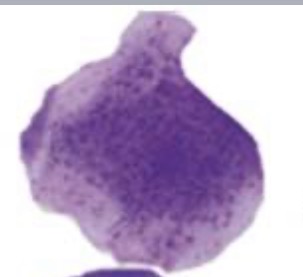
anuclear

superficial
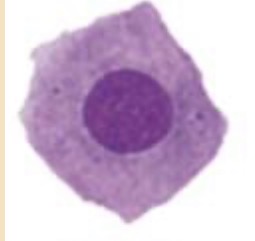
intermdiate
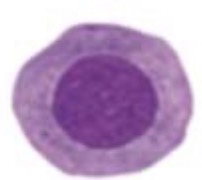
parabasal
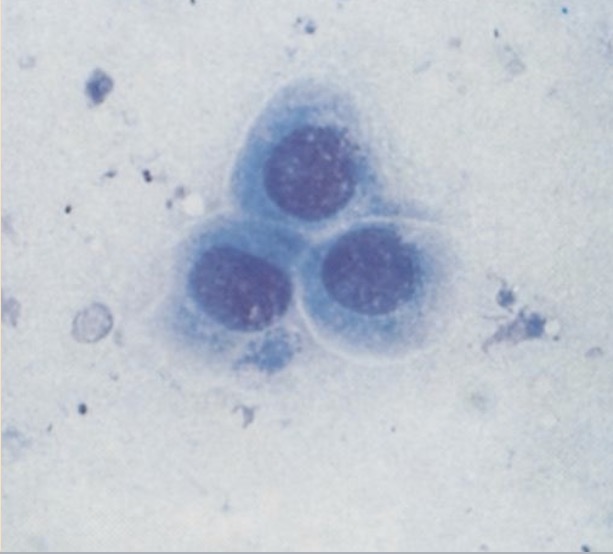
anestrus
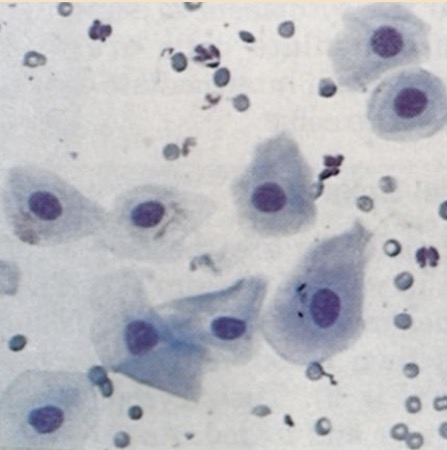
proestrus
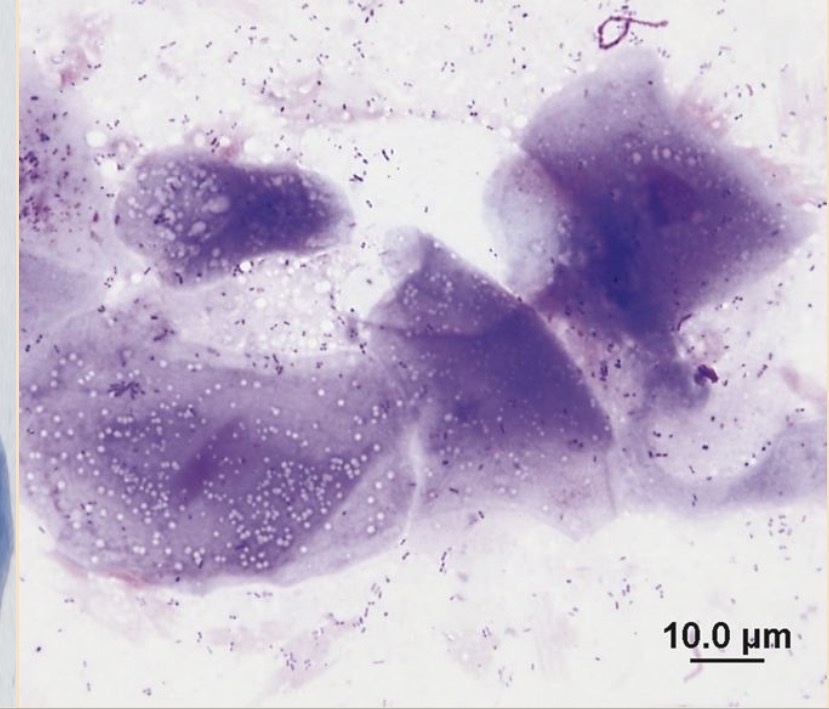
estrus
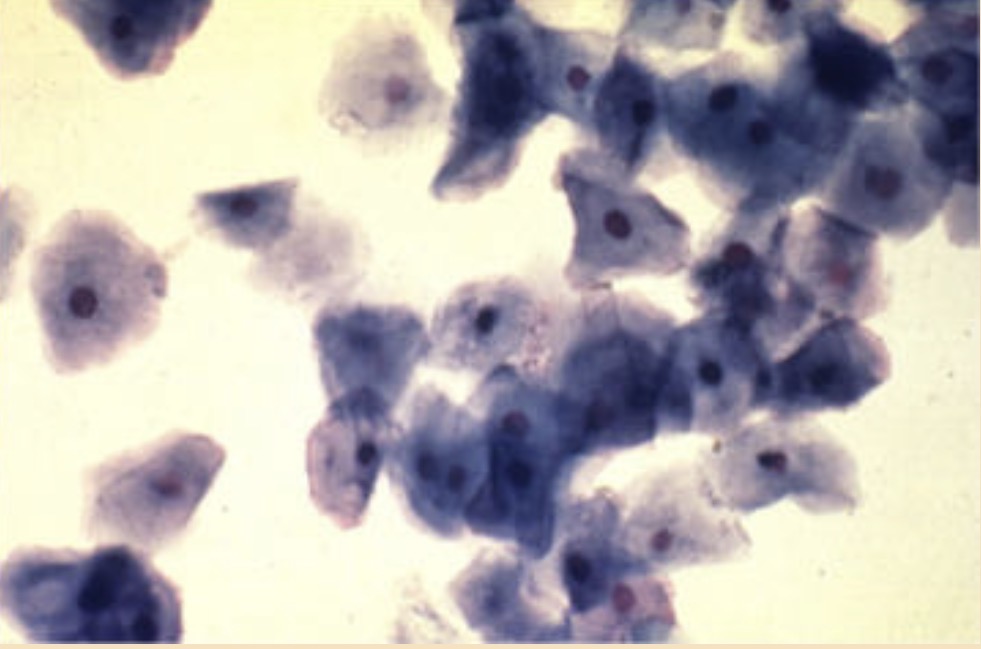
cornified cells
how long does estrus last
4 - 8 days after LH surge
when is peak canine fertility
5 - 6 days after LH surge - 2 - 3 days before diestrus
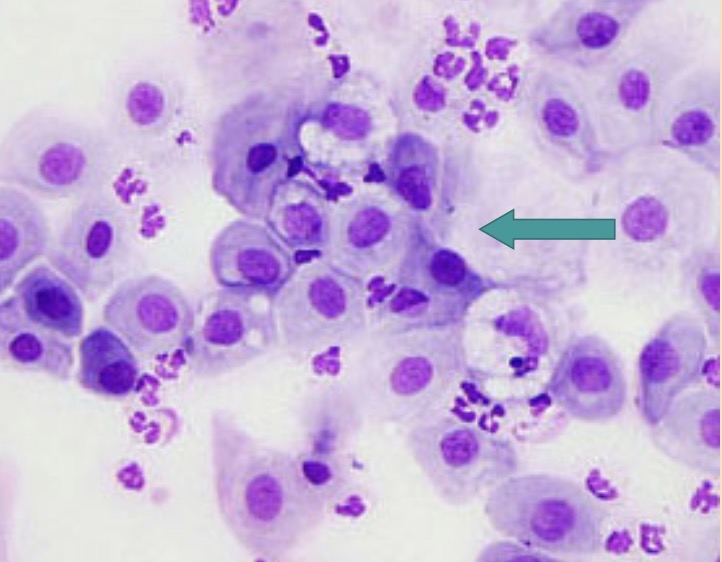
diestrus
materials/equipment needed to perform vaginal cytology
microscope, slides, clean cotton swabs, saline solution, cell stain - modified wright’s or giemsa
clinical signs that warrant performing an ear cytology
pruritus, erythema, discharge, shaking head, head tilt, malodorous ears,
what type of things should be checked during an otoscopic exam
ensure tympanic membrane is intact, check for erythema, exudate deepeer in the canal, check for ectoparasites/foreign debris
what type of fixative should be used for an ear cytology
a methanol based fixative
what type of stain is appropriate for an ear cytology
diff quik or other romanowsky stain
three most common bacilli found in ear infections
pseudomonas aeruginosa ,proteus, e. coli
examples of surface level pyoderma
moist dermatitis, fold pyoderma, generalized bacteria overgrowth
examples of superficial pyoderma
bacterial folliculitis, epidermal collarettes, miliary dermatits
examples of deep pyoderma
pyogranulomatous, ulceration, draining tracts
What categories of inflammation can be identified in cytological samples?
suppurative, granulomatous, pyogranulomatous, and eosinophilic.
what evaluation is done on 40x
differentiate cell types present and in what proportion to one another
what evaluation is done on 100x
looking for nuclear and cytoplasmic abnormalities
how is suppurative inflammation classified
large number of neutrophils, >85% of total nucleated cells
how is pyogranulomatous inflammation classified
significant number of macrophages present 15 - 50% macrophagees
how is granulomatous inflammation classified
>50% macrophages
how is eosinophilic inflammation classified
presence of >10% eosinophils in the sample
karyolysis inflammation
rapid cell death - swollen, ragged nucleus without intact nuclear membrane
pyknosis inflammations
slow cell death (aging) small condensed nucleus
karyorrhexis inflammation
nuclear fragmentation - often follows pyknosis
what are the abnormal nuclear configurations
anisokaryosis, pleomorphism, high or variable nucleus/cytoplasm ratio, increased mitotic activity, coarse chromatin pattern, nuclear molding, multinucleation, nucleoli that vary in size
what does discolorations and increased turbidity mean in fluid evaluation
result of increased cell numbers and/protein
what does malodorous fluid mean
necrosis or infection
now is the normal total nucleated cell count
less that 10,000 nucleated cell/ul
tranudate
non inflammatory, vascular, stasis, neoplasia
modified transudate
FIP, chylous fluid, lymphatic fluid
exudate
iinflammatory, infection, necrosis
what are mesothelial cells
line the body cavity
what does increased mesothelial cells mean
increased fluid present - cells become reactive
what are mesothelial cells difficult to differentiate from
neoplastic cells
How are absolute WBC counts calculated from percentages?
Multiply the percentage of WBC type by total WBC count.
What are toxic changes in neutrophils?
Toxic granulation, cytoplasmic vacuolation, cytoplasmic basophilia.
What is the appearance of reactive lymphocytes?
They are larger with coarse chromatin and deep blue cytoplasm.
What visual characteristic distinguishes reactive monocytes?
Subtle granular or foamy appearance.
What hormone stimulates erythropoiesis?
Erythropoietin.
What does an increased number of nucleated RBCs in peripheral blood indicate?
It can indicate normoblastosis or a disease process.
Which components are involved in the hematopoietic system?
Bone marrow, spleen, liver, lymph tissues.
How many types of reticulocytes are there?
Two types: punctate and aggregate.
What do you call the immature stages of granulocytes?
Myelocyte, metamyelocyte, and band.
What organ produces thrombopoietin?
The liver.
What is normoblastosis?
Increased nucleated red blood cells in peripheral blood.
What are the two types of proerythroblast?
Rubriblasts and prorubricytes.
How can reticulocytes be identified?
Using a vital stain or specific types of Romanowsky stains.
What indicates a strong regenerative response in anemia?
High numbers of reticulocytes.
What is a typical leukocyte response in dogs during leukocytosis?
30,000 to 50,000/μL, sometimes exceeding 100,000/μL.
What ranges are typical for equine leukocytosis?
15,000 to 40,000/μL.
What is a significant threshold for bovine leukocytes?
15,000/μL represents a dramatic response.
What indicates a degenerative left shift in leukocyte classifications?
An increase in band neutrophil numbers only, with segmented neutrophils normal or decreased.
What changes are commonly seen in a stress leukogram?
Neutrophilia, lymphopenia, eosinopenia, and monocytosis.
What is the upper limit of leukocyte count in cats under stress?
About 75,000/μL.
What is the purpose of the urine sediment examination in veterinary medicine?
To evaluate the cellular and non-cellular components present in urine to detect abnormalities.
What is the standard volume ratio of urine supernatant to sediment in a microscopic urine sediment exam?
9:1 ratio.
What type of crystals are commonly found in the urine of horses and rabbits?
Calcium carbonate crystals.
What is the recommended centrifugation speed for urine sediment examination?
450G (1,000 – 2,000 rpm depending on the centrifuge).
When performing a urine sediment exam, how should the urine be mixed with the sediment after centrifugation?
Gently mix the urine sediment with the remaining supernatant.
What stains can be used for examining urine sediment?
Sedi-stain® or New Methylene Blue.
How do you report the quantity of constituents observed in urine sediment?
Report as Rare; 1+; 2+; 3+, 4+ (or few, moderate, many).
What cellular constituents can be found in urine sediment?
WBCs, RBCs, and epithelial cells.
What does the presence of more than 2-3 WBCs per high power field indicate?
Potential inflammatory or infectious process.
What condition can cause RBCs to be crenated in urine?
Concentrated urine or highly alkaline urine.
Where do squamous epithelial cells originate?
From the distal urethra, vagina, vulva, or prepuce.
Why are transitional epithelial cells considered significant?
Their presence in increased numbers may indicate cystitis or pyelonephritis.
What distinguishes renal (tubular) epithelial cells?
They are round to cuboidal with a large, eccentrically placed nucleus.
How are casts formed in urine sediment?
In the lumen of the loop of Henle, distal tubules, and collecting ducts, where urine concentration and acidity are greatest.
What type of casts indicate renal bleeding?
RBC casts.
What is a characteristic of granular casts?
Indicates more severe kidney damage and contains cellular material from renal tubules.
What are fatty casts associated with?
Degeneration of renal tubules or lipid accumulation in the kidneys.
What factors affect crystal formation in urine?
Urine pH, concentration, temperature, and solubility of elements.
What is the appearance of struvite crystals in urine?
Six to eight sided prisms with tapering ends, found in alkaline to slightly acidic urine.
What defines calcium oxalate dihydrate crystals?
Small squares with an 'X' across the crystal resembling an envelope.
What clinical significance do ammonium biurates have?
They indicate portal vascular abnormalities and are most noted in Dalmatians.
Which crystals can indicate renal tubular dysfunction?
Cystine crystals.
What are typical features of molds in urine sediment?
Filamentous and usually branching; uncommon but serious if noted.
What clinical action should be taken if bacteria are found in urine?
Collect urine aseptically for culture.
What signifies the presence of yeast in urine specimens?
Characteristic budding and rare infections of the external genitalia.
What is the significance of lipid droplets in urine sediment?
Indicates possible conditions like obesity or diabetes mellitus, especially in cats.
What conditions can yield starch granules in urine sediment?
Contamination from powdered gloves used by technicians.
What are the key types of crystals identified in urine sediment?
Struvite, calcium oxalate, amorphous phosphates, and ammonium biurates.
What does the presence of tyrosine crystals suggest about an animal's health?
Possible liver disease.
How do transitional epithelial cells appear microscopically?
Larger than WBCs, may appear granular, and typically have small nuclei.
What common urinary issue can struvite crystals indicate in animals?
Urolithiasis.
What can be inferred from the presence of excessive renal epithelial cells in urine?
Potential kidney parenchyma disease.
When might mucus be found in urine sediment?
As a result of irritation in the urinary tract.