Radiation Safety Final Exam
1/87
Earn XP
Description and Tags
you got this!
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
88 Terms
Radiation
Energy that travels through space or matter as waves or particles.
Ionizing Radiation
Any type of radiation that is capable of removing an orbital electron from the atom
ALARA
“As Low As Reasonably Achievable” keeping radiation exposure as low as possible.
Inverse Square Law
As distance increases, radiation intensity decreases.
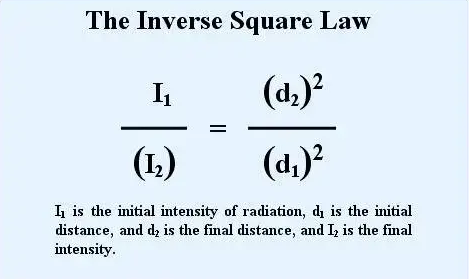
Principles of radiation protection
Time: Direct Relationship
Distance: Indirect Relationship
Shielding: Indirect Relationship
0.25 mm Pb minimum
Time and radiation protection are _______ly related
Direct
Distance and radiation protection are _______ly related
Indirect
Shielding and radiation protection are _______ly related
Indirect
4 special quantities to measure radiation
Air KERMA (Kinetic Energy per unit Mass: Gya
Absorbed Dose: Gyt
Effective Dose: Sv
Radioactivity: Becquerel (Bq)
What does KERMA stand for?
Kinetic Energy per unit Mass
4 radiation measurement quantities - What does the absorbed dose express?
Tells us how much radiation doses is absorbed in the patient and tells us short-term effects such as skin erythema and hair loss but not long-term effects
Gyt
4 radiation measurement quantities - What does the effective dose express?
Express long-term effects-used to express the quantity of radiation received by radiation workers and populations
Sv
4 radiation measurement quantities - What does radioactivity express?
Spontaneous release of energy from an unstable atom to get to a more stable state
Bq (Becquerel)
4 radiation measurement quantities - What does Air KERMA express?
Exposure: kinetic energy released per unit mass-measure total energy of ions in air
Gya
Exposure relationship
More time = more exposure
More distance = less exposure.
When were X-rays discovered?
November 8th, 1895: Wilhelm Conrad Rontgen in Germany
HVL
Half-value layer; thickness of material needed to reduce beam intensity by half.
Largest natural radiation source
Radon Gas
Others:
Cosmic Rays
Terrestrial Radiation
Internally Deposited Radionucleotides
Human-made:
X-ray/CT
Nuclear medicine
Interventional fluoroscopy
Conventional radiography/fluoroscopy
Radiation can be…
Absorbed
Reflected
Scattered
Refracted
Transmitted
Radiation Actions - Absorbed
Energy is retained by a substance (create x-rays)
Radiation Actions - Reflected
The surface returns a portion of the energy (sun)
Radiation Actions - Scattered
The electromagnetic waves are changed from propagating in one direction to all directions (goes where it shouldn’t, which can negatively impact images)
Radiation Actions - Refracted
The electromagnetic waves are changed from propagating in one direction to another direction
Radiation Actions - Transmitted
Energy passes through space or the media
X-ray tube parts
Cathode, anode, filament, focusing cup, target, rotor, stator, glass envelope, tube housing.
Positive/negative sides
Cathode = negative side.
Filament - coil of wire approximately 2mm in diameter and 1 or 2 cm long
Dental imaging systems, portable imaging systems
Focusing cup - metal shroud that surrounds the filament
Anode = positive side. 2 types
Stationary - high tube current and power are not required
Rotating - capable of producing high-intensity x-ray beams in a short time
Positive/negative sides - What are the 2 types of anodes?
Stationary - high tube current and power are not required
Rotating - capable of producing high-intensity x-ray beams in a short time
Why does x-ray tube failure occur?
Anode being at high temperatures for a long period of time
Filament breaks and becomes thin because of excessive heat
The enormous amount of heat that is not dissipated
Radiation - transfer of heat by the emission of infrared radiation
Conduction - transfer of heat from one area to another
Convection - transfer of heat by the movement of a heated substance from one place to another
Tube interactions
Heat 99%
X-rays 1%
Tube Failure - Conduction
Transfer of heat from one area to another
Tube Failure - Convection
Transfer of heat by the movement of a heated substance from one place to another
Two types of x-rays generated
Characteristic radiation
Bremsstrahlung radiation
Characteristic radiation
X-rays are produced when outer-shell electrons fill an inner-shell
Projectile electrons interact with inner shell electron
Projectile electron has energy high enough to totally remove an inner-shell electron of the target atom
Bremsstrahlung radiation
X-rays produced when fast electrons slow down near the nucleus.
Braking radiation
X-ray interaction with matter
The higher the energy of the x-ray, the shorter the wavelength
Low energy x-rays interact with whole atoms
Moderate energy x-rays interact with electrons
High energy x-rays interact with the nuclei
X-ray interaction with matter - Low energy interacts with…
Whole Atoms
X-ray interaction with matter - Moderate energy interacts with…
Electrons
X-ray interaction with matter - High energy interacts with…
Nuclei
Where are X-rays produced? Gamma rays?
X-rays = outside the nucleus/electron cloud.
Gamma rays = inside the nucleus.
Radiopaque vs radiolucent
Radiopaque = white/light on image such as bone
Radiolucent = dark/black on image such as fluid
Pair production
Photon interacts near nucleus and creates a positron and electron
Photodisintegration
High-energy photon hits nucleus and ejects nuclear particles.
Photoelectric effect
Photon is absorbed and ejects an inner-shell electron.
Coherent/classical scattering
Low-energy photon changes direction without ionization
Compton effect
Occurs when x-rays throughout the diagnostic range can undergo an interaction with outer-shell electrons that not only scatters the x-ray but reduces the x-ray and ionizes the atom as well
Most radiation-sensitive cell cycle phase
M phase, also late G2
Low LET radiation
X-rays and gamma rays
Most radiosensitive cells
Blood-forming cells, reproductive cells, and immature rapidly dividing cells
Linear/nonlinear response
Linear = damage increases directly with dose.
Nonlinear = damage does not increase evenly with dose.
Target molecule
DNA.
LD50/60
Dose that kills 50% of exposed people within 60 days
Tissue weighting factor
Measures how sensitive an organ/tissue is to radiation risk
Radiation weighting factor
Compares biological damage from different radiation types
RBE and LET of X-rays
X-rays have low LET and an RBE of 1
Acute radiation syndromes
Hematologic: 1–10 Gy, affects bone marrow, infection, bleeding.
GI: 10–50 Gy, nausea, vomiting, diarrhea, dehydration.
CNS: 50+ Gy, confusion, seizures, coma, death.
Acute radiation syndromes - Hematologic
1–10 Gy, affects bone marrow, infection, bleeding.
Acute radiation syndromes - GI
10–50 Gy, nausea, vomiting, diarrhea, dehydration.
Acute radiation syndromes - CNS
50+ Gy, confusion, seizures, coma, death.
Dose Limits (5)
Occupational whole body: 50 mSv/year or 5 rem/year.
Public: 0.1 rem/year or 1 mSv/year.
Lens: 150 mSv/year or 15 rem/year
Skin/extremities: 500 mSv/year or 50 rem/year.
Fetus: 0.5 mSv per month// 5 mSV per whole preganancy (0.5 rem)
Dose limits - Occupational whole body
5 rem/year
Dose limits - Public
0.1 rem/year or 1 mSv/year
Dose limits - Lens
15 rem/year
Dose limits - Skin/extremities
50 rem/year
Dose limits - Fetus
0.5 rem total pregnancy
RBE Formula
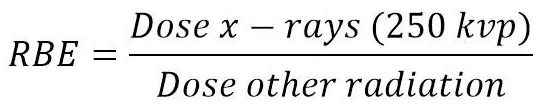
Conversions:
1 Gy = 100 cGy.
1000 mrem = 1 rem.
100 rad = 1 Gy.
1 rad = 0.01 Gy.
Conversions - 1 Gy = __ cGy
100 cGy
Conversions - 1000 mrem = __ rem
1 rem
Conversions - 100 rad = __ Gy
1 Gy
Conversions - 1 rad = __ Gy
0.01 Gy
X-ray production
About 99% heat and 1% X-rays.
Largest man-made radiation source
Medical imaging, especially CT
Public dose limit
1 mSv/year or 0.1 rem/year
Cumulative effective dose
Age × 10 mSv
Radiation therapy
Use of radiation to treat cancer or abnormal tissue
Controlled vs uncontrolled area
Controlled area = radiation workers have safety rules and monitoring.
Uncontrolled area = general public area
Deterministic vs stochastic
Deterministic = has threshold; severity increases with dose.
Stochastic = no threshold; chance increases with dose.
Cell survival
Ability of cells to survive after radiation exposure
Oxygen enhancement ratio
Radiation is more damaging when oxygen is present
Relative biological effectiveness
Compares damage caused by different radiation types
Fractionation/protraction
Gives normal tissue time to repair while still damaging cancer cells
Radiobiology
Study of effects of radiation on living tissue
Radiosensitizer
Substance that makes cells more sensitive to radiation
Radiosensitivity depends on
Cell division rate, cell maturity, oxygen level, and tissue type
Manifest illness
Stage of radiation sickness when symptoms appear
What is Acute radiation syndrome
Illness caused by high whole-body radiation dose over a short time
What is Mean survival time
Average time a person survives after a lethal radiation dose
What is HVL
Amount of shielding needed to reduce radiation intensity by 50%
Target theory
Theory that a cell will die if target molecules are inactivated as a result of radiation exposure