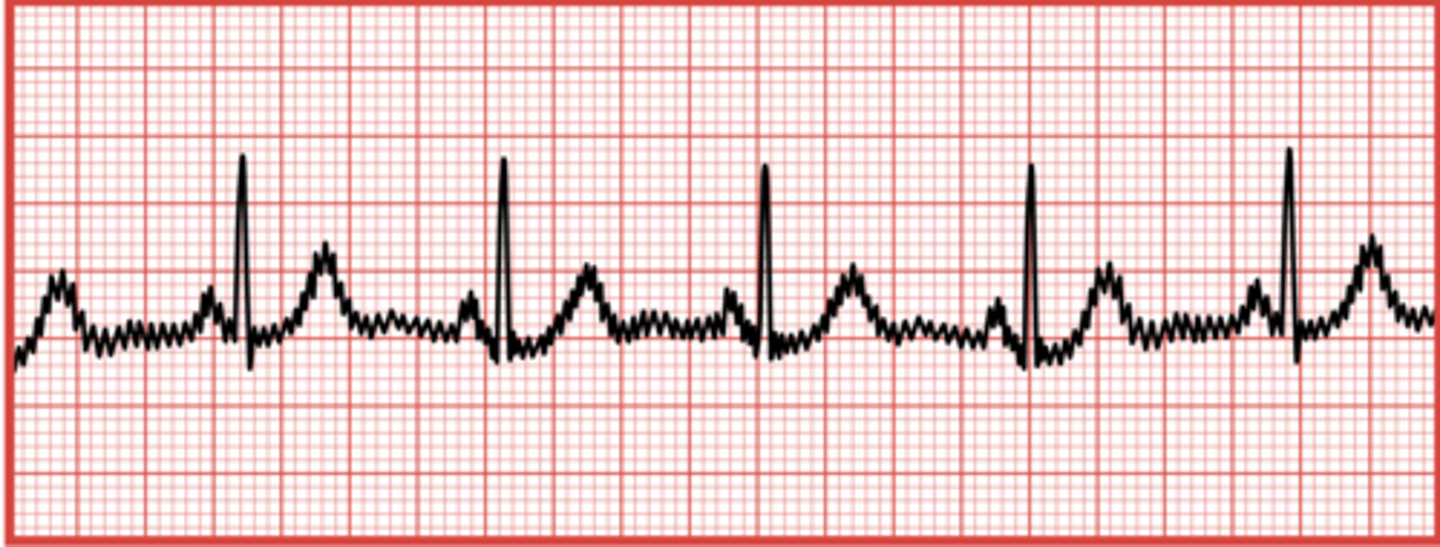
PCT - ECG
1/90
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
91 Terms
What is the role of the sinoatrial (SA) node?
It acts as the pacemaker of the heart, initiating electrical impulses.
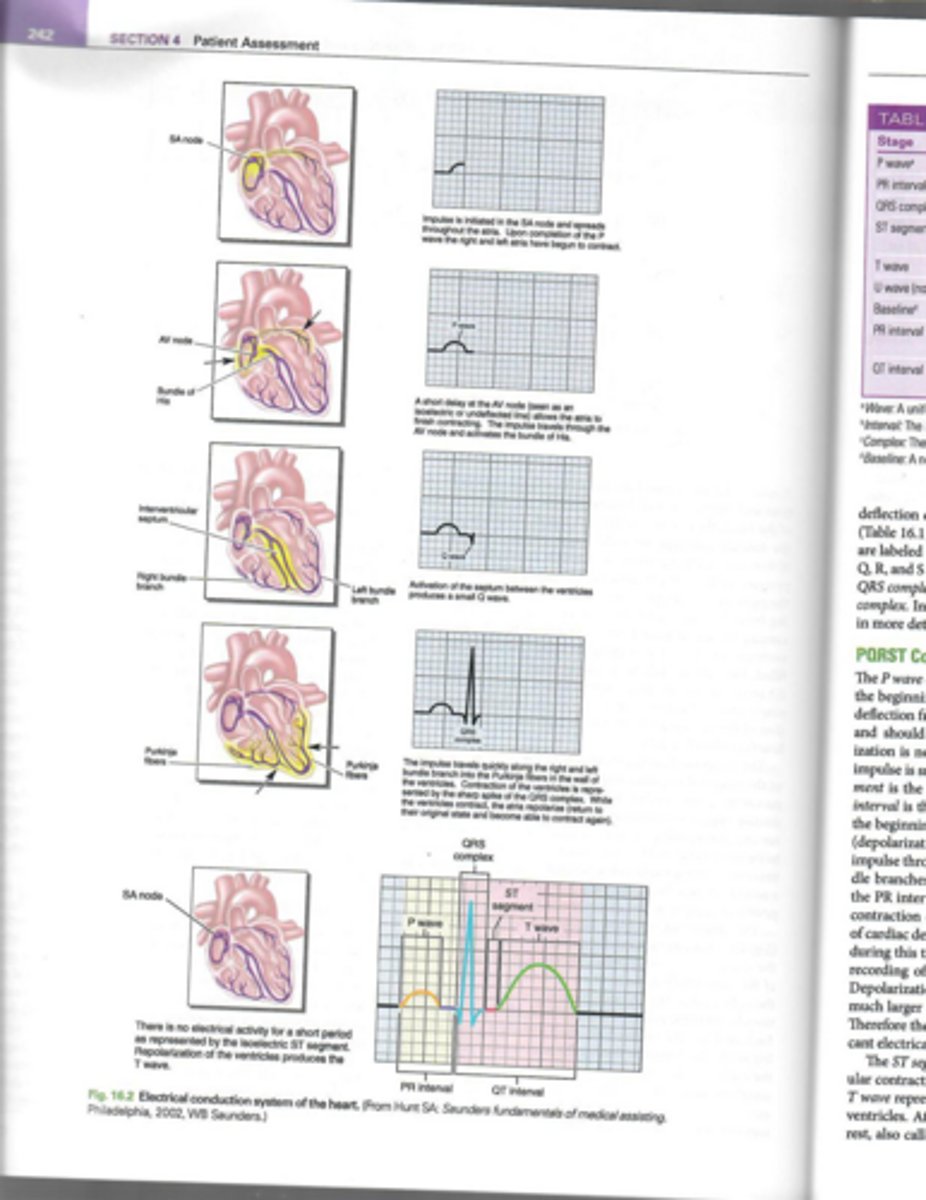
What is the function of the atrioventricular (AV) node?
To relay electrical impulses from the atria to the ventricles.
Define diastole.
The relaxation phase of the heart when the chambers refill with blood.
Define systole.
The contraction phase of the heart when blood is pumped out of the chambers.
What is the bundle of His?
A group of specialized muscle fibers that conduct electrical impulses from the AV node to the ventricles.
What is ischemia?
Decreased blood flow to a body part or organ due to constriction or blockage of the supplying artery.
What does myocardial refer to?
Pertaining to the heart muscle.
What is the typical heart rate range for normal sinus rhythm (NSR)?
60 to 100 beats per minute.
What is an arrhythmia?
An irregular cardiac rhythm caused by disruptions in the heart's conduction pathway.
What occurs during depolarization?
The heart muscle contracts in response to electrical stimulation.
What is repolarization?
The process of the heart muscle returning to a resting state after contraction.
What does the term ectopic mean in a cardiac context?
Originating outside the normal tissue.
What is the duration of a typical cardiac cycle in a healthy adult?
Approximately 0.8 seconds.
What is the difference between sinus bradycardia and sinus tachycardia?
Bradycardia is a heart rate below 60 beats/min; tachycardia is above 100 beats/min.
What is the purpose of the Purkinje fibers?
To spread electrical impulses across the ventricles, stimulating contraction.
What is the role of the right and left bundle branches?
To carry electrical impulses to the respective ventricles.
What does the P wave represent in an ECG?
Atrial depolarization and contraction.
What occurs during the PR interval?
The time from the beginning of atrial contraction to the beginning of ventricular contraction.
What does the QRS complex represent?
Ventricular depolarization and contraction.
What does the ST segment indicate?
The time between the end of ventricular contraction and the beginning of ventricular recovery.
What does the T wave represent?
Ventricular repolarization or recovery.
What is the QT interval?
The time between the beginning of the QRS complex and the end of the T wave.
What is the U wave in an ECG?
A small waveform that may appear after the T wave, often associated with low serum potassium levels.
What is the significance of the isoelectric line on an ECG?
It represents periods of no electrical activity.
What is the role of the AV node in the heart's electrical conduction?
It provides a short delay to allow the atria to finish contracting before the impulse travels to the ventricles.
What does the horizontal axis on ECG paper represent?
Time.
What does the vertical axis on ECG paper represent?
Amplitude.
What is the normal speed of an ECG machine?
One small 1-mm square passes the stylus every 0.04 seconds.
What happens to the PR interval as the heart rate increases?
The PR interval typically shortens.
What does the term 'polarization' refer to in the cardiac cycle?
The period of complete heart rest indicated by a straight line on the ECG.
What is the role of Purkinje fibers in the heart?
They conduct the electrical impulse throughout the ventricles, leading to contraction.
What is the significance of the cardiac cycle being called the PQRST complex?
It encompasses the entire sequence of electrical events in one complete heartbeat.
How often does one small 1-mm square pass the stylus on an ECG?
Every 0.04 seconds.
How long does it take for one large 5-mm square to pass the stylus?
Every 0.2 seconds.
What is the speed at which the ECG paper travels past the stylus?
25 mm per second.
How much deflection does 1 millivolt (mV) of electrical activity produce on the ECG?
More than 10 mm (two large squares).
What must be done to calibrate the ECG machine?
It must be calibrated so that 1 mV of electrical activity produces a deflection of 10 mm above or below the baseline.
What does lead I record?
The electrical activity between the right arm and left arm.
What does lead II record?
The electrical activity between the right arm and left leg.
What does lead III record?
The electrical activity between the left arm and left leg.
What are augmented leads in an ECG?
Leads that amplify the electrical potential recorded from a single positive electrode. (Unipolar)
What does lead aVR record?
The electrical activity of the atria from the right shoulder.
What does lead aVL record?
The electrical activity of the lateral wall of the left ventricle from the left shoulder.
What does lead aVF record?
The electrical activity of the inferior surface of the left ventricle from the left leg.
What are precordial leads?
Unipolar leads that provide a transverse plane view of the heart.
Where is electrode V1 placed?
In the fourth intercostal space just to the right of the sternum.
Where is electrode V2 placed?
In the fourth intercostal space just to the left of the sternum.
Where is electrode V4 placed?
In the fifth intercostal space at the left midclavicular line.
What alternative position can be used if a patient has difficulty breathing?
The semi-Fowler's position or seated on a wooden chair.
Where should the RA lead be attached?
To the electrode on the patient's right arm.
Where should the LA lead be attached?
To the electrode on the patient's left arm.
Where should the RL lead be attached?
To the electrode on the patient's right leg.
Where should the LL lead be attached?
To the electrode on the patient's left leg.
What should be avoided before the ECG test?
Heavy meals, cold drinks, ice cream, smoking, and excessive exercise.
What causes a wandering baseline in an ECG?
Slight movement of the patient during the tracing or poor electrode attachment.
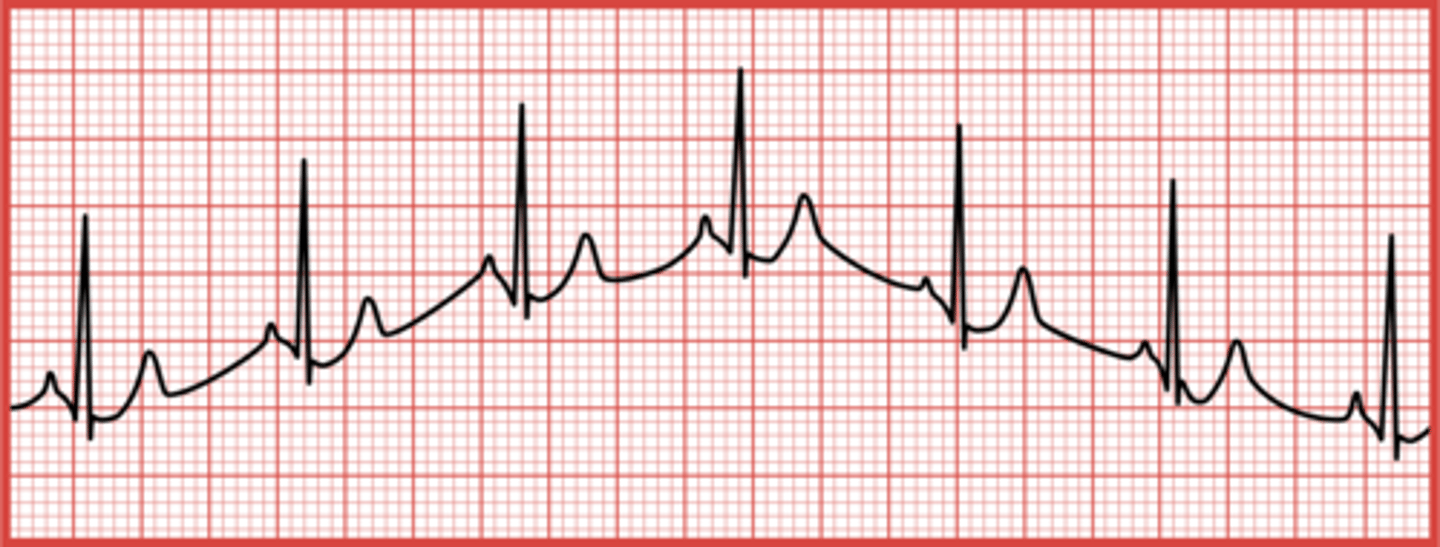
What is somatic tremor?
Muscle movement that produces measurable electrical impulses, causing jagged peaks on the ECG.
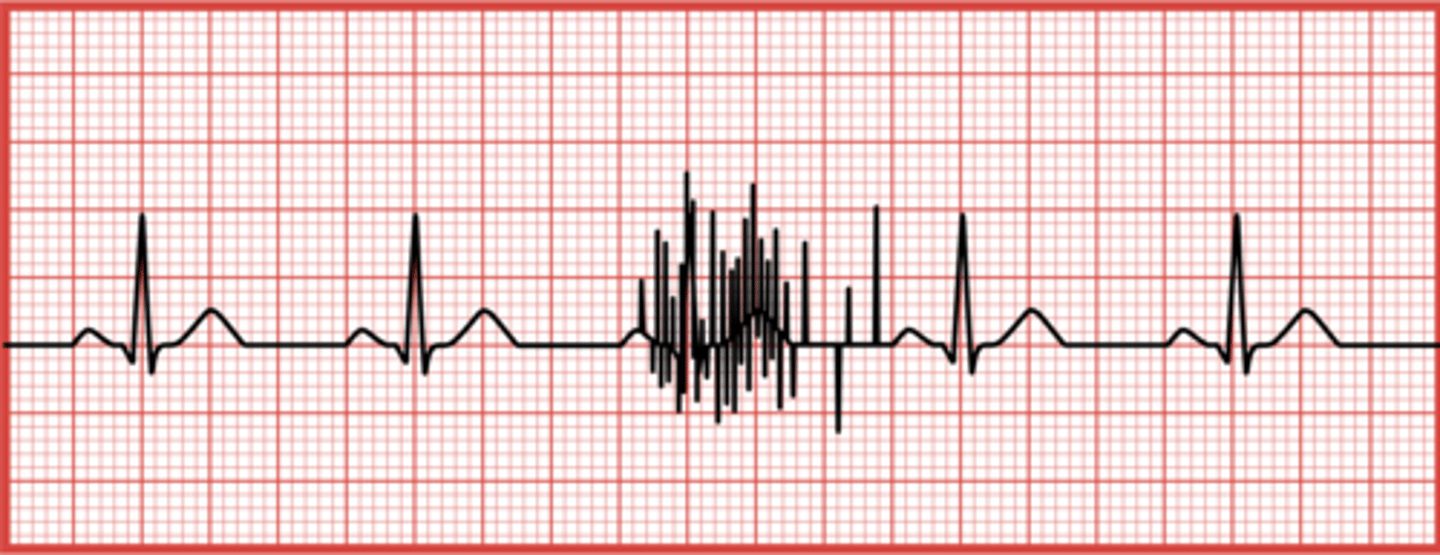
What indicates an interrupted baseline on an ECG?
Erratic movement of the stylus, often due to noticeable patient movement or a broken cable wire.
How can you calculate the heart rate from an ECG strip?
Count the number of P waves in a 6-second strip and multiply by 10.
What does a heart rate calculation involving small squares between R waves entail?
Count the number of small squares between two R waves and divide that number into 1500.
What is the normal duration of a P wave in an ECG?
0.06 to 0.11 seconds
What does a normal PR interval range from?
0.12 to 0.20 seconds
What is the duration of a normal QRS complex?
0.08 to 0.12 seconds
What defines a normal sinus rhythm (NSR) in terms of heart rate?
A heart rate between 60 and 100 beats per minute.
What is sinus bradycardia?
A heart rate below 60 beats per minute.
What is sinus tachycardia?
A heart rate above 100 beats per minute.
What is a premature atrial contraction (PAC)?
When the atria contract before they should for the next cardiac cycle.
What can cause premature atrial contractions (PACs)?
Smoking and consumption of large amounts of caffeine.
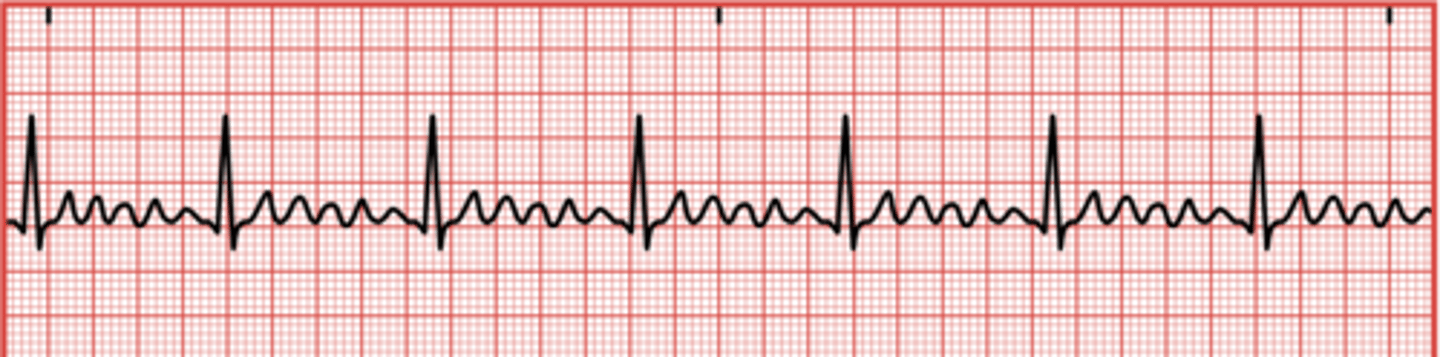
What is atrial flutter?
A condition where the atria beat at an extremely rapid rate, up to 300 beats per minute.
What are the characteristics of ventricular tachycardia (V-tach)?
Rapid ventricular beats, often seen with multiple PVCs.
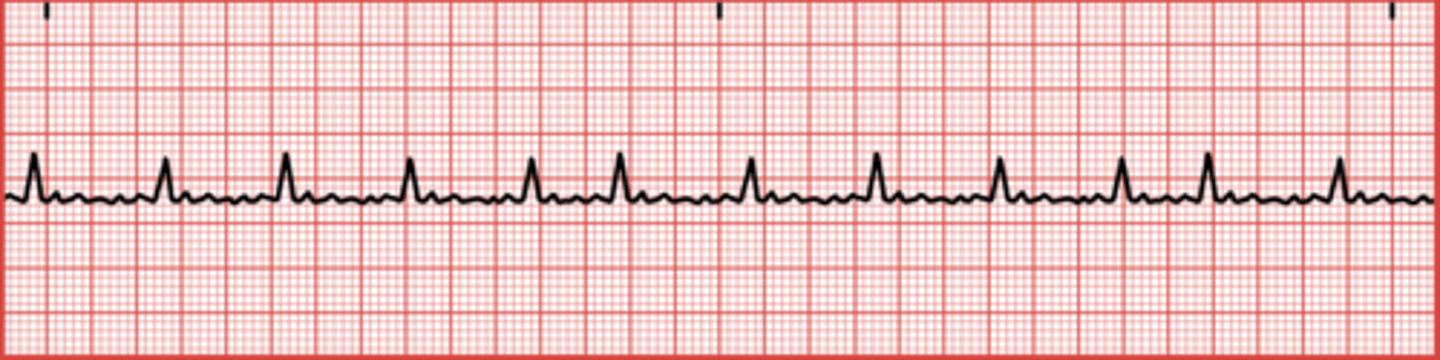
What is the main concern with atrial fibrillation?
It can lead to ineffective pumping of the heart and increase the risk of blood clots.
What is a premature ventricular contraction (PVC)?
When the ventricles contract before they should, resulting in a QRS complex appearing before a P wave.
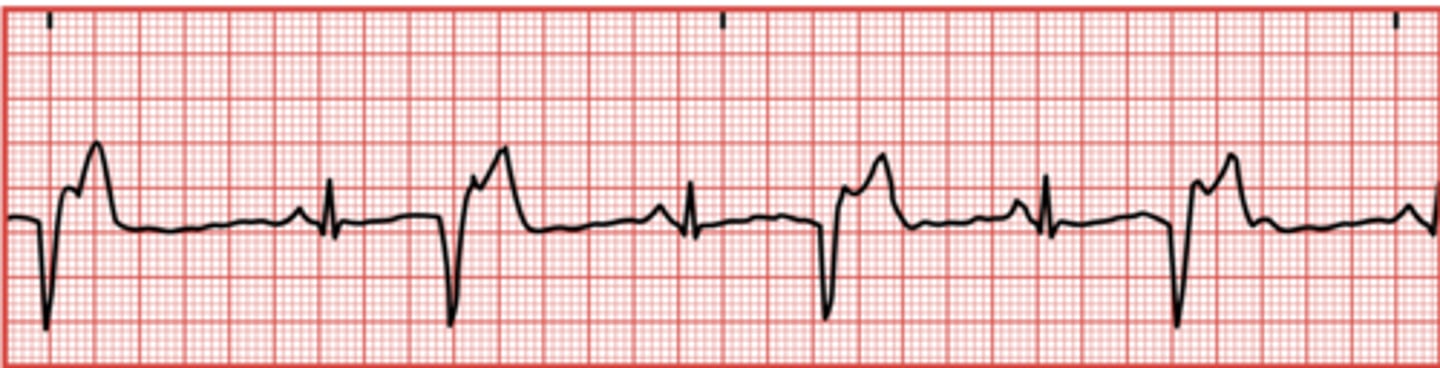
What can cause premature ventricular contractions (PVCs)?
Tobacco use, alcohol, medications containing epinephrine, and anxiety.
What does the term 'arrhythmia' refer to?
Abnormalities in cardiac rhythm.
What is the maximum acceptable QT interval duration in relation to the RR interval?
Should not be more than one-half the RR interval if the patient has a regular rhythm.
What is the risk associated with atrial fibrillation?
Increased risk for blood clots and stroke.
What is the appearance of the QRS complex in PVCs?
Widened QRS complex with absent P wave.
What is the treatment for atrial flutter?
Medication to slow the heart or cardioversion (electrical shock).
What is the expected ECG finding in sinus arrhythmias?
Normal electrical pathway but altered heart rate or rhythm.
What is ventricular tachycardia (V-tach)?
A condition where the ventricles beat at extremely rapid rates, ranging from 101 to 250 beats/min.
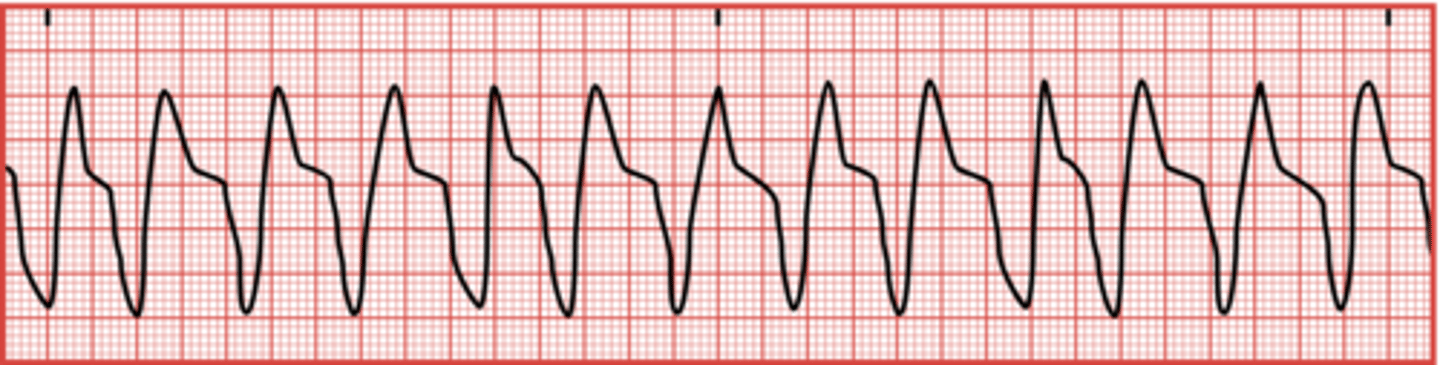
What can V-tach precede if not treated?
Ventricular fibrillation (V-fib).
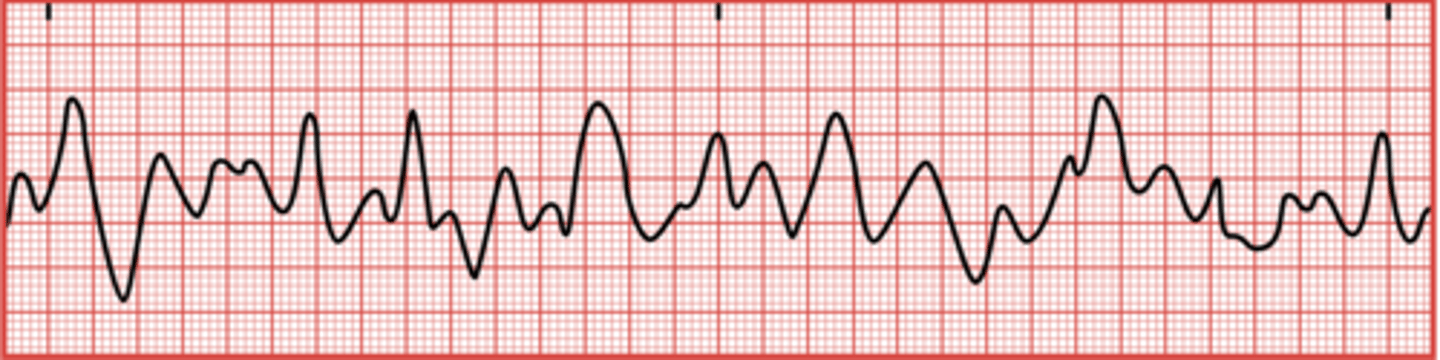
What is ventricular fibrillation (V-fib)?
A life-threatening arrhythmia where the heart muscle quivers uncontrollably, resulting in no effective blood pumping.
What is asystole?
The absence of a heartbeat, shown as a flatline on the ECG.
How should a patient be positioned for an ECG?
Supine.
How many extremities are used for lead placement in a 12-lead ECG?
Four.
V3
Place between V2 and V4
V5
5th IC space, anterior axillary line
V6
5th IC space, midaxillary line
Unipolar Lead
measures in one direction
Biopolar leads
2 Poles (pos and neg): measure potential difference between the two poles
6 sec on ECG
30 large squares
AC Interference
uniform spikes on an EKG caused by electrical interference.