Mammography part of exam
1/44
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
45 Terms
What is the 2nd most common cancer among women?
Breast cancer
What are the 3 most common methods to detecting breast cancer early on?
Mammography, clinical breast exams, and MRI (in extreme cases)
Mammo can detect lesions as small as ____ mm or ____ cm.
2 mm or 0.2 cm
How long does it typically take for a small lesion to grow large enough to be detected on a clinical breast exam?
2-4 years to grow to 2 cm or an 1 inch
If a lesion reaches 2 cm it has often ...
metastasized
What is the life span for a patient with metastasis?
2 years
What is the MQSA and when was it enacted?
The Mammography Quality Standards Act was enacted in 1994. Prompted by the wide range of poor quality mammo at the time.
What are the 3 major tenets of the MQSA?
-Facilities performing mammo must be approved by an accredited body like the Joint Commission
-Facilities must be certified by Department of Health and Human Services
-Facilities must receive on-site inspections by state agency on behalf of the DHHS
What is mediolateral diameter?
Width of the breast from side to side
What is craniocaudad diameter?
vertical measurement (top to bottom)
What is the inframmatory fold?
The junction of inferior part of breast with anterior chest wall
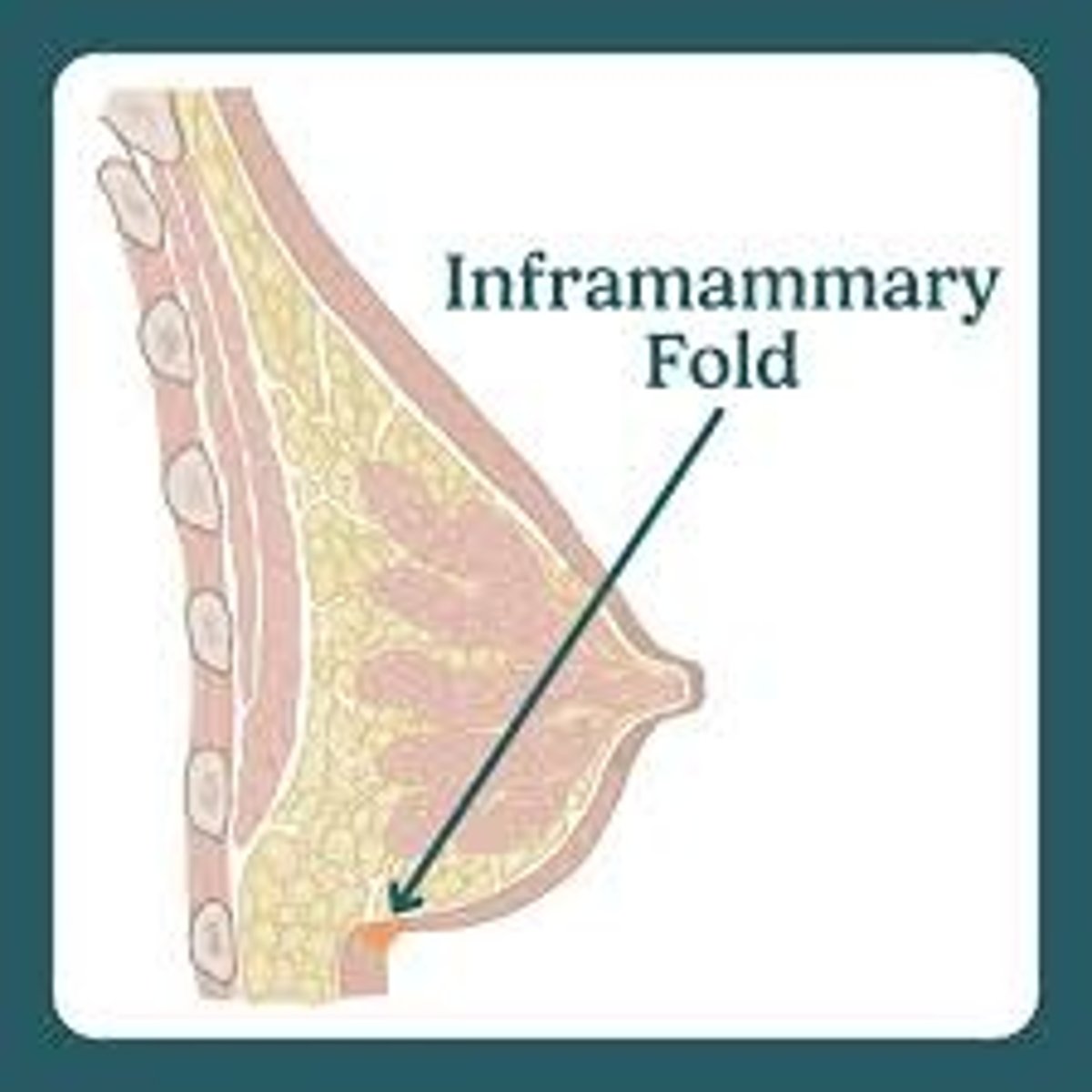
What is the axillary tail?
Band of tissue that wraps around the pectoral muscle laterally
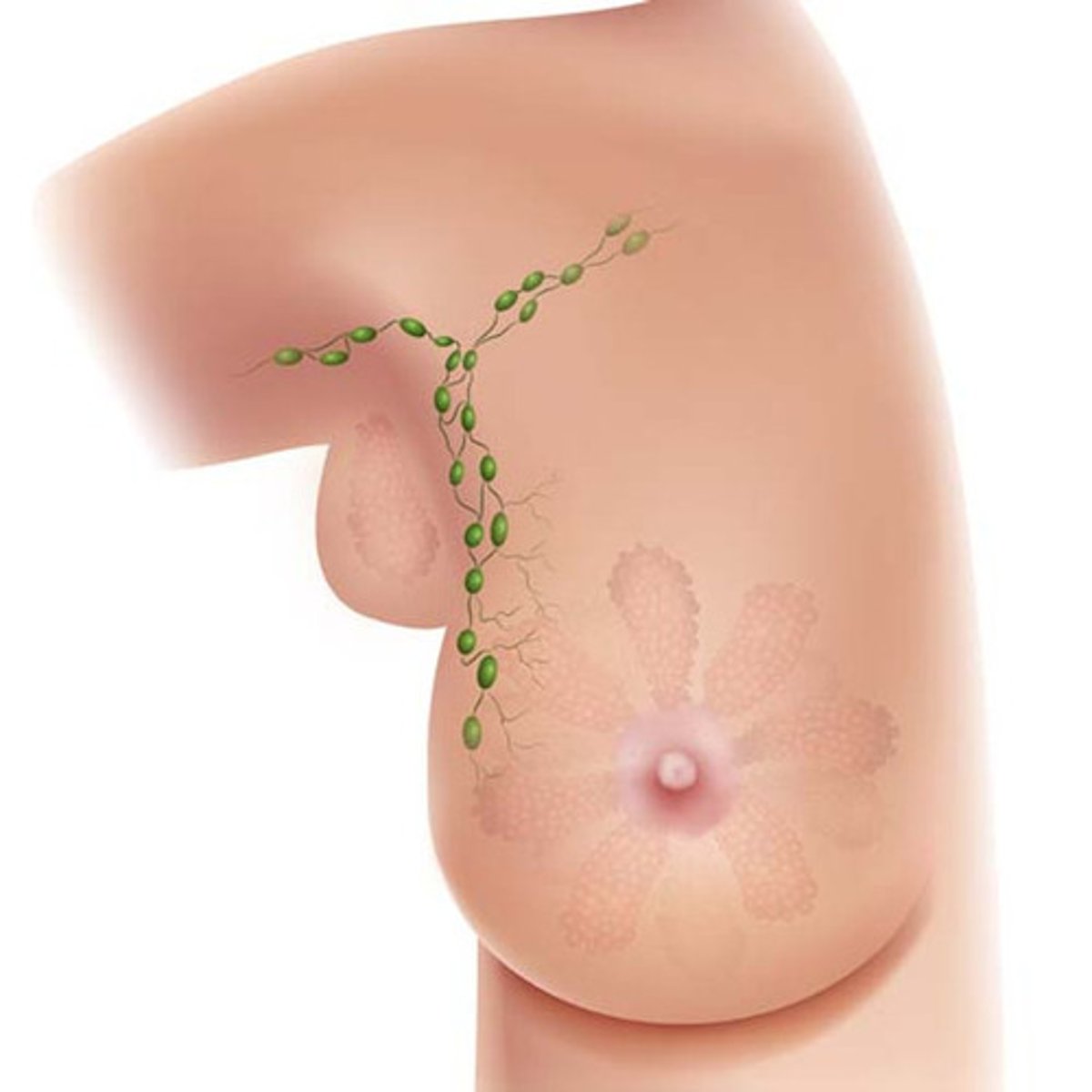
What is the most common site for breast cancer?
The tail of the breast
What are the two breast localization systems?
Quadrant system and clock system
What is fibroglandular tissue in the breast? What is the age range for this tissue? What TYPE of women? How does it appear radiographically?
Fibrous tissue in the breast. Present in 15-30 year olds. Present in pregnant or lactating women. Radiographically dense. Very little fat.
What is fibrofatty tissue? What is the age range for this tissue? What TYPE of women? How does it appear radiographically?
A combination of fibrous and fatty tissue. 30-50 year olds. Present in young women with 3 or more pregnancies. Average radiographic density. 50% fibrous 50% fatty.
What is fatty tissue? What is the age range for this tissue? What TYPE of women? How does it appear radiographically?
All fatty tissue. Over 50 year olds. Present in postmenopausal women. Minimal radiographic density. Also found in breast tissue of children and men.
What does mammo unit specifically include?
A plastic compression device that evens out the thickness of the breast tissue
How much pressure does the plastic compression device apply?
15-30 pounds
Name the 6 reasons for the use of compression.
-Decrease breast thickness and make it more uniform
-Bring breast structure as close to image receptor as possible
-Decrease radiographic dose needed
-Decrease motion and increase sharpness
-Increase contrast by allowing decrease in exposure factors and dose
-Separate breast structures that may be superimposed
How is mammography magnification achieved?
By increasing OID (object to image distance)
What is patient dose in mammography determined by?
Equipment used, technique factors used, size and density of the patient's breast tissue
During patient preparation, what should surface moles, palpable masses, scars, and warts be marked with?
A radiographic BB
What does patient history usually include?
Number of pregnancies and live births, family history of cancer, medications, previous breast surgery, previous mammogram, reason for mammogram (lumps identified, breast pain, or discharge)
What are the two different types of mammo imaging?
Film/screen and digital
Explain film/screen mammo imaging?
Performed with an imaging cassette that houses an intensifying screen and x-ray film
Explain digital mammo imaging.
Film/screen combo is replaced by an image detector connected to a computer
What are the disadvantages of digital imaging in mammo?
Increased dose and slight loss of spatial resolution
What are the advantages of digital imaging in mammo?
Post-processing functions and the ability to magnify an image on a computer screen
What are some other imaging modalities utilized in mammo?
Ultrasound, MRI, computerized assisted detection, contrast enhanced radiography, PET mammography, Nuclear medicine
What is the cranio-caudal position? Where is the image receptor placed?
Radiographic beam enters the top of the breast and exits the underside of the breast. IR is placed below the breast.
What is the medio-lateral position? Where is the image receptor placed? What angle are they placed at?
Radiographic beam enters the medial side of the breast and exits the lateral side of the breast. IR is placed on the lateral side. Beam and IR are tilted at a 45 degree angle.
What are some mammo special procedures?
Fine needle biopsy, core biopsy (like drilling for oil), and biopsy from surgical resection
What are some challenges in mammography?
-Reassuring the patient about the procedure and outcome
-Silicone and saline implants
Carcinoma of the breast is divided into two categories. What are they?
Noninvasive and invasive
What is noninvasive carcinoma restricted to? What is it referred to as?
Restricted to glandular tissue without access to the lymphatic system or blood vessels.
Referred to as ductal/lobular carcinoma in situ
What is invasive carcinoma referred to as?
Infiltrating ductal carcinoma.
Invasive carcinoma is _____% of breast cancer.
80%
What are fibroadenoma?
Solid lumps of fibrous and glandular tissue; benign
What are fibrocystic changes?
fibrous and cystic dilation of ducts
What is intraductal papilloma?
Small growth in the duct near the nipple; symptoms may include nipple discharge
What is paget disease of nipple?
Crusty or scaly nipple or discharge; may also have a lump in the breast
What is the skin dose for mammography?
800-900 mrads for 4 cm thickness mammo
What repeat rate does the ACR recommend?
A repeat rate of less than 5% to limit patient dose
What is the difference between screening mammograms and diagnostic mammograms?
Screening is for patients who have no identified issues on clinical exams or past mammograms.
Diagnostic is for patients who have an abnormality identified on clinical exam or past mammograms.