Week 5- Part 2- Anatomy of the Respiratory System
1/65
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
66 Terms
what do the bones of the thorax consist of
The bones of the thorax consist of the sternum, 12 pairs of ribs and their costal cartilages, and the 12 thoracic vertebra (T1 - T12).
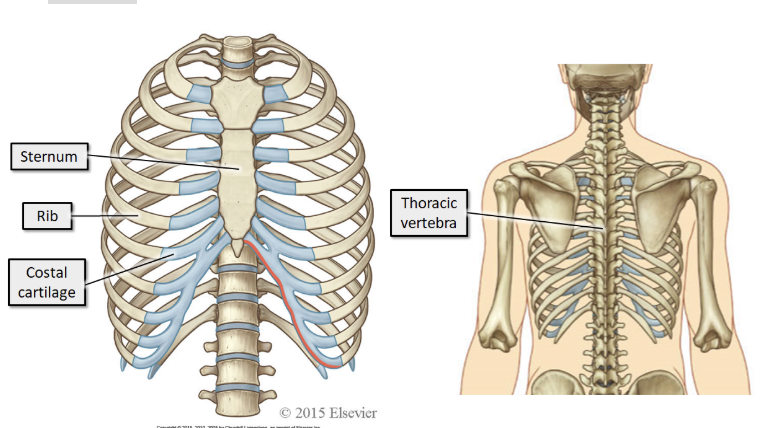
what is the function of the bones of the sternum
Provide attachment points for the muscles of respiration
Move to facilitate breathing
Provide protection for the vulnerable organs within the thorax
where does the sternum sit, what does it consist of
The sternum sits anteriorly. It consists of the manubrium, sternal body and xiphoid process.
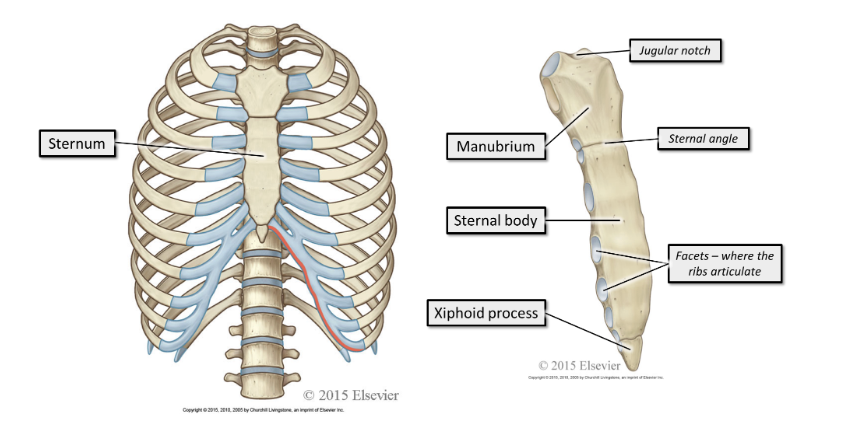
where do the ribs articulate
All the ribs articulate posteriorly with the thoracic vertebra. The end of the rib that articulates with the vertebra is the head of the rib.
Anteriorly, the ribs end in costal cartilage
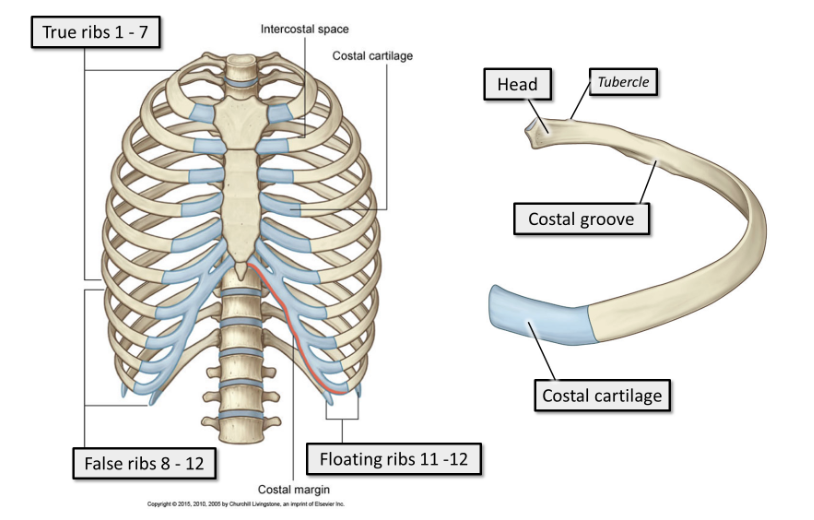
what are ribs 1-7
true ribs.
True ribs articulate directly with the sternum anteriorly, via short costal cartilages. Every true rib has its own costal cartilage
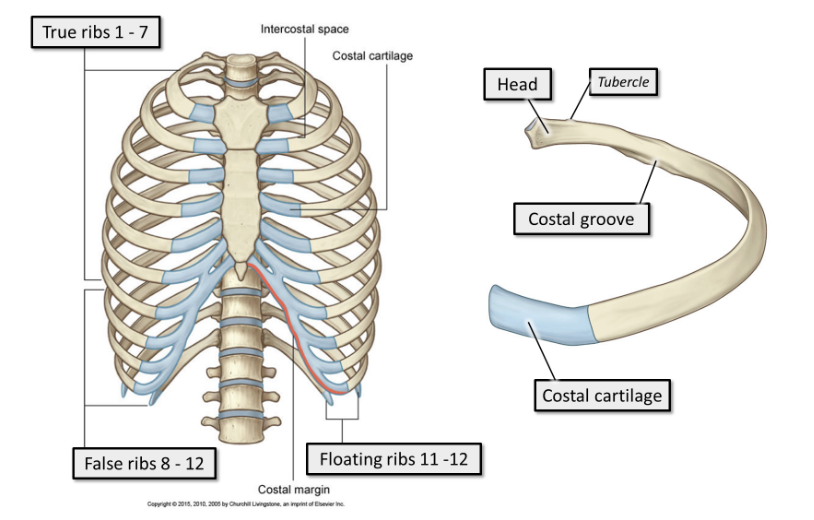
what are ribs 8-12
false ribs.
False ribs articulate indirectly with the sternum anteriorly, via long, shared costal cartilages, or do not articulate with the sternum at all.
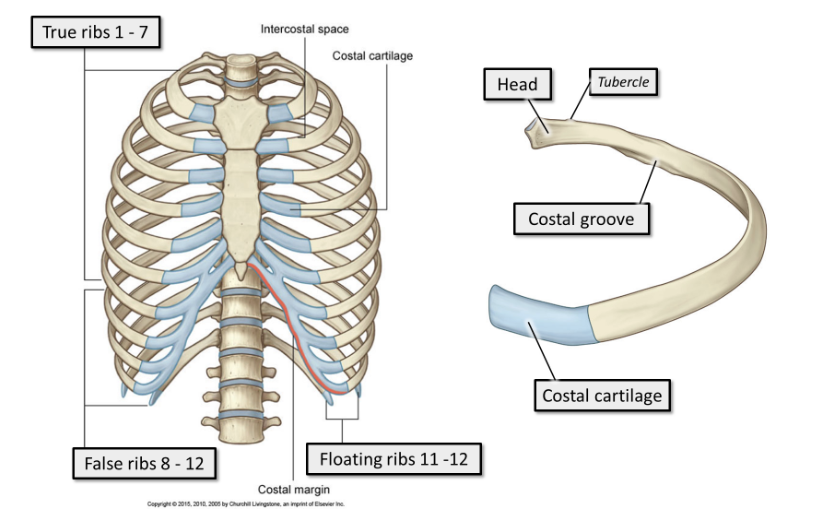
what are ribs 11-12
floating ribs.
They do not articulate with the sternum anteriorly, and are shorter and pointier than the other ribs.
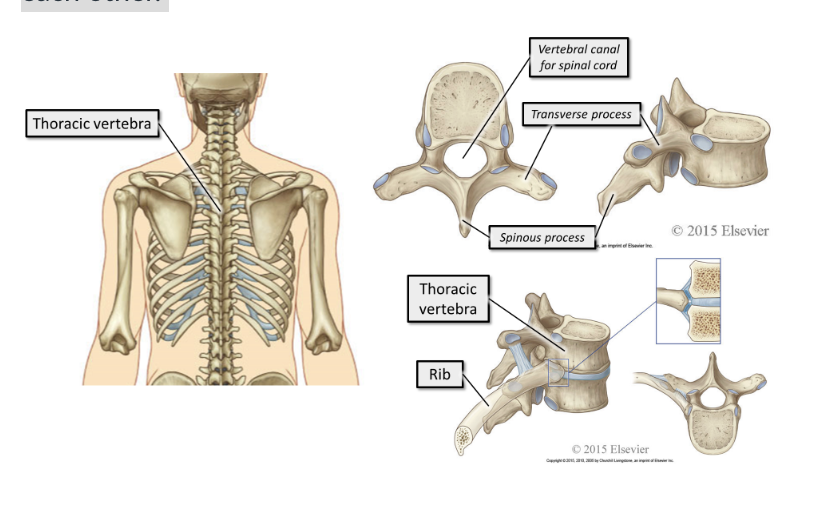
what do thoracic vertebra make up
The 12 thoracic vertebrae make up the posterior element of the thoracic cage. They articulate with the ribs and with each other.
what muscles are involved in respiration
The muscles involved in ventilation are skeletal muscles. Their structure and function is identical to those of other skeletal muscles.
what is the diaphragm
The diaphragm is a thin, musculotendinous, dome-shaped sheet of muscle that separates the thorax from the abdomen.
It has a large, flat central tendon
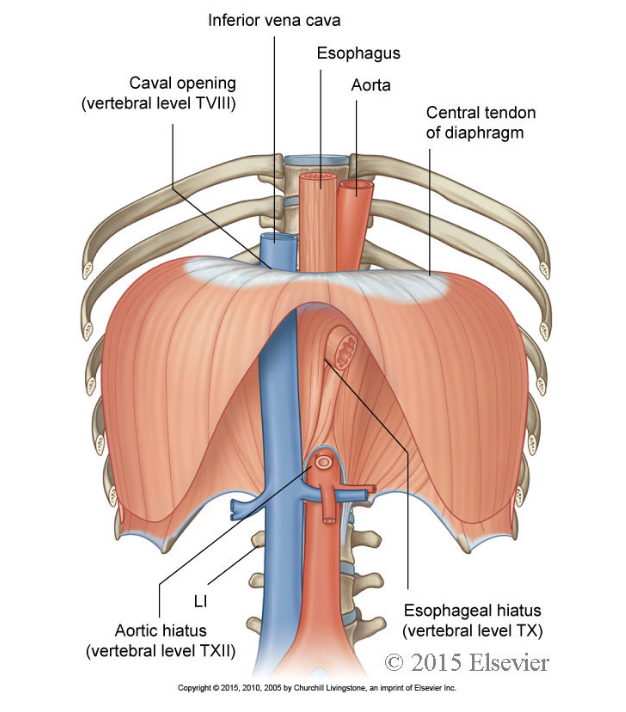
what is the diaphragm attached to
The diaphragm is attached to the lower ribs and vertebral column.
what is the diaphragm innervated by
It is innervated by the right and left phrenic nerves, which have their origins at the third to fifth cervical spinal nerves (C3-C5).
You can remember this with the rhyme: "C3, C4, C5 keeps the diaphragm alive"!
what is the highest point of the diaphragm at rest
While at rest, its highest point it is level with T9, inferiorly it is attached to the body wall level with T12.
where is blood supplied and drained from the diaphragm
Blood supply of the diaphragm originates from the intercostal arteries
Venous drainage is to the inferior vena cava.
what 3 major structures travel through the diaphragm
The aorta
The inferior vena cava
The oesophagus
what happens whrn the diaphragm contracts
Contraction of the diaphragm flattens it. This increases the volume of the thorax and aids inspiration.
In addition, the rib margins are lifted and moved out, which increases the transverse diameter of the thorax.
how far does the diaphragm move during quiet and deep breathing
During quiet breathing, the diaphragm contracts and flattens, the apex moves inferiorly by 1-2cm.
During deep breathing the diaphragm can move inferiorly up to 10 cm.
where are the intercostal muscles located
As the name indicates, the intercostal muscles are located between the ribs.
what are the features of the intercostal muscles
The external intercostals are superficial to the internal intercostals. The innermost intercostals are the deepest of the three.
There are 11 sets of each.
Their blood supply comes from the intercostal arteries
Venous drainage is via the intercostal veins. They are innervated by the intercostal nerves.
what is the intercostal neurovascular bundle
The intercostal artery, vein and nerve travel together in the intercostal space. They lie at the lower border of each rib.
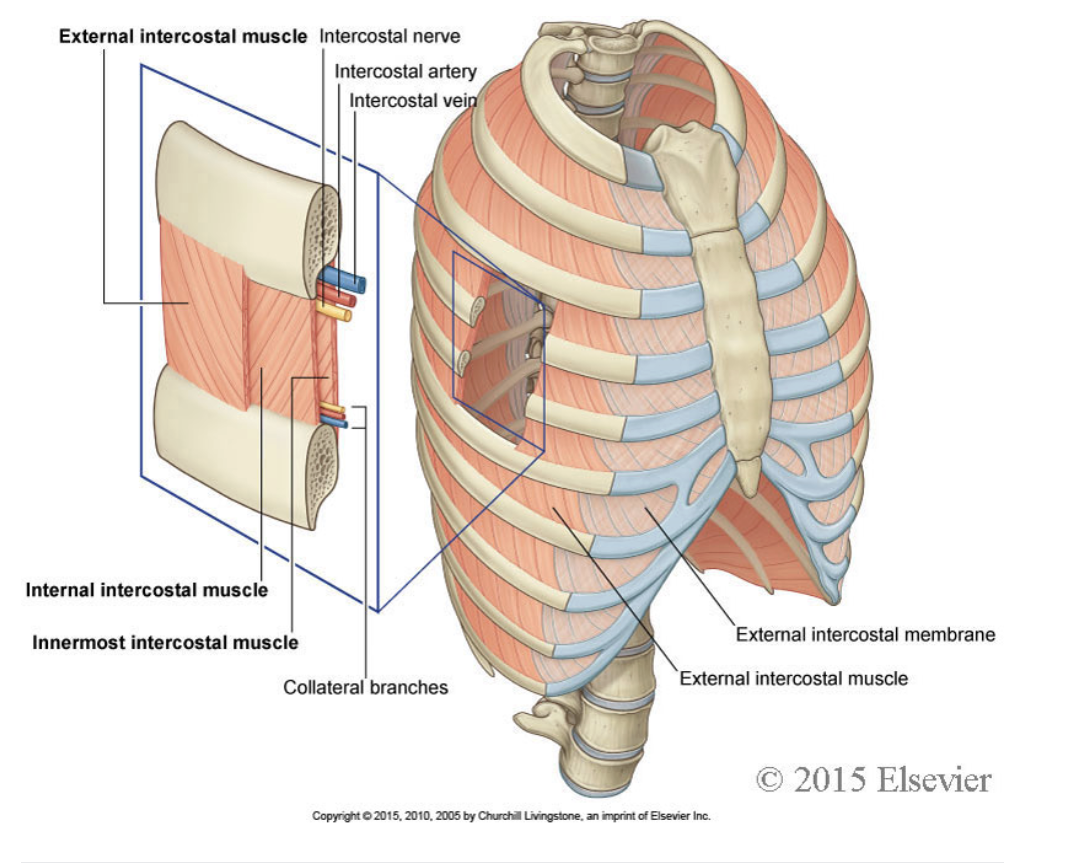
where do external intercostals extend from
extend from the lower border of the rib above, to the upper border of the rib below.
They run around the wall of the thorax, from the tubercles each rib posteriorly, to the cartilages of the ribs anteriorly.
They end anteriorly in thin membranes, the anterior (external) intercostal membranes, which continue forward to the sternum.
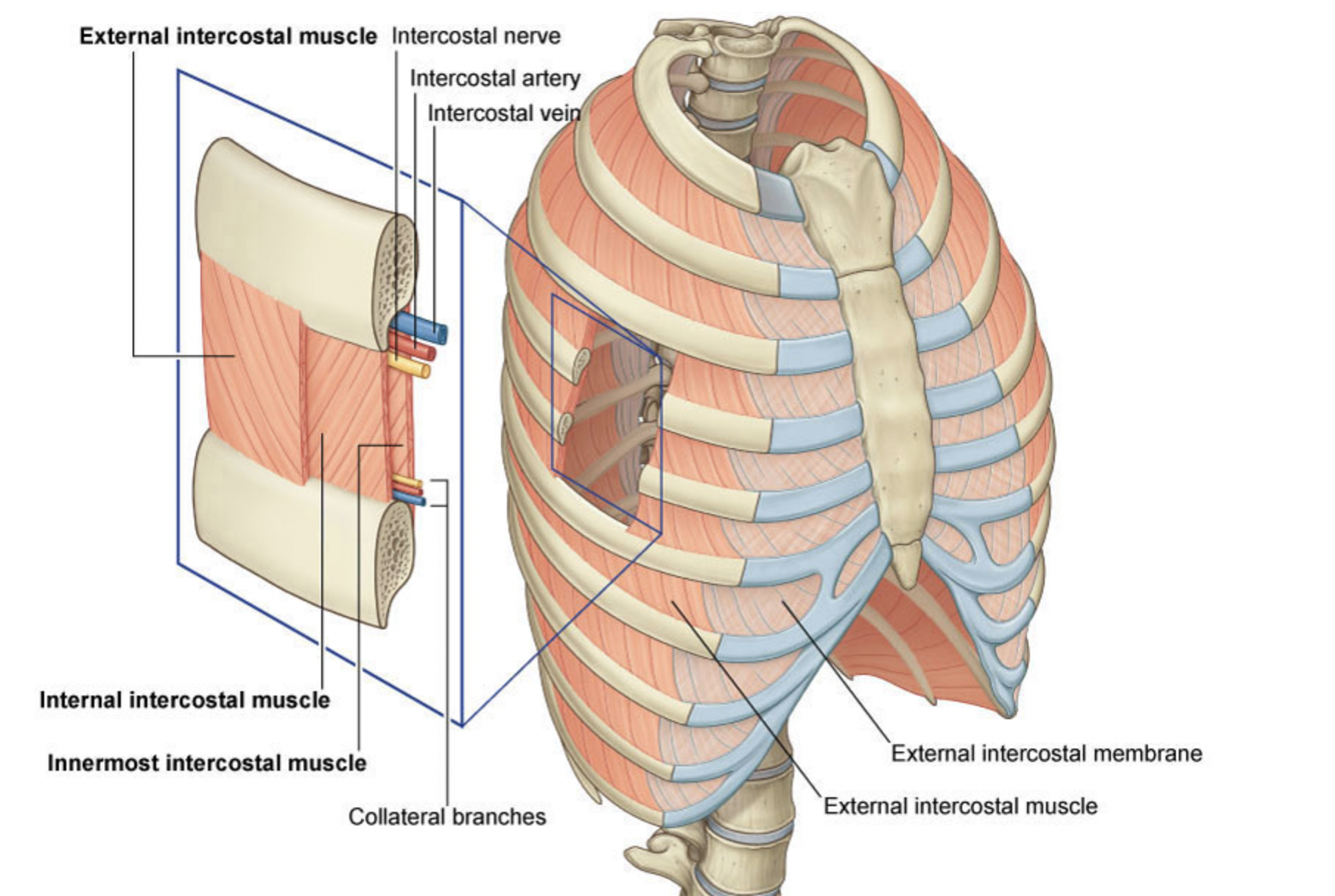
what do the external intercostal muscles do
They pull the ribs upwards and forwards during inspiration causing an increase in both the lateral and anteroposterior diameters of the thorax.
They are most active in inspiration.
where do internal intercostals extend from
run between the most inferior lateral edge of the costal grooves of the ribs above, to the superior margins of the ribs below.
They begin anteriorly, at the sternum in the spaces between the cartilages of the true ribs (ribs 1-7) and at the most anterior edge of the cartilages of the false ribs (8-12).
They extend downward as far as the angles of the ribs, where they continue to the vertebral column as thin membranes called the posterior (internal) intercostal membranes.
what do the internal intercostal muscles do
They pull the ribs down and inward during active respiration.
what are the innermost intercostals
are incomplete and variable.
They pass from rib to rib deep to the internal intercostals.
Their fibres run in the same direction as the internal intercostals.
The innermost intercostal muscles are separated from the internal intercostal muscles by the bundle of intercostal blood vessel and nerves.
what are the accessory muscles of respiration
Muscles such as sternocleidomastoid, pectoralis minor and the scalene muscles have main functions that are not related to breathing.
However, due to their attachments to the ribs, in forced respiration they assist in expansion of the thoracic cavity to maximise respiratory efficiency.
what is the difference between the external and internal intercostals
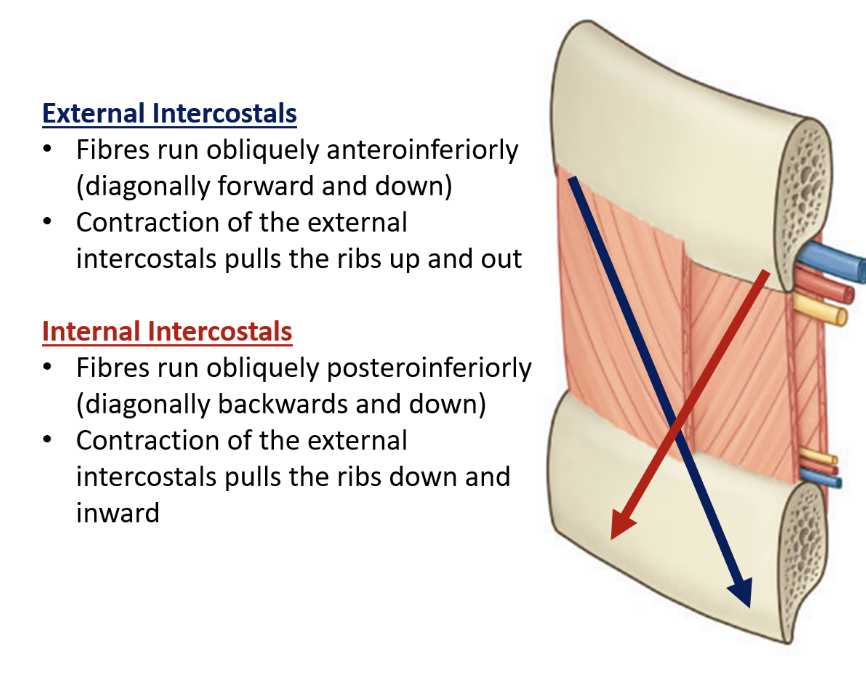
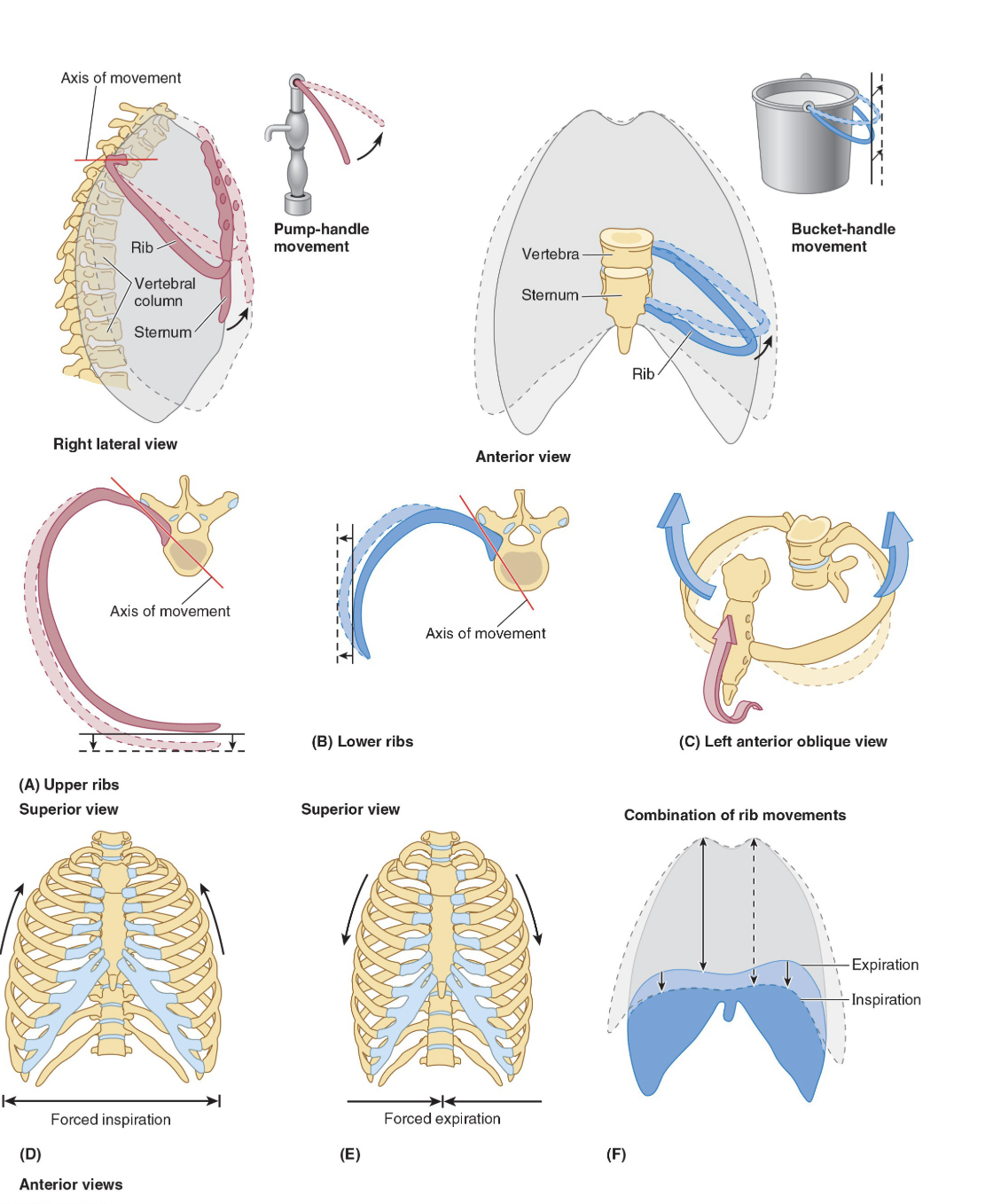
where do the ribs move during breathing
During breathing the ribs move in two planes, forwards and backwards (anteroposterior) and laterally.
The anteroposterior motion is often compared to a pump handle action where the ribs are the handle of the pump.
The lateral movement is often compared to a bucket handle where the ribs are a handle pivoting at the spine and sternum.
what trees are each lung composed of
Each lung is composed of two treelike structures, the vascular tree and the airway tree, embedded in lung tissue.
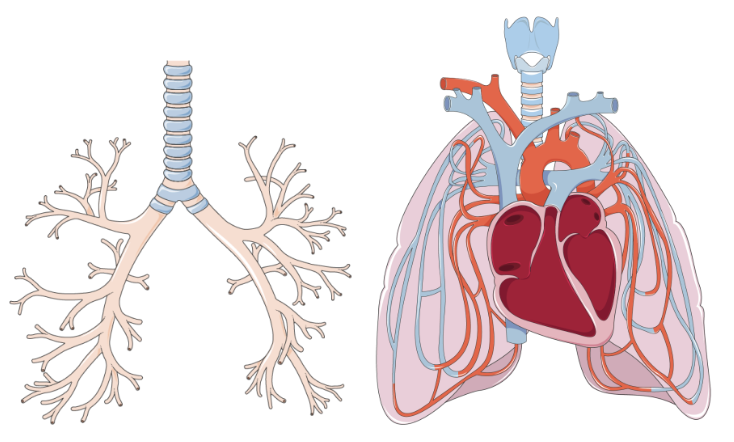
what is the vascular tree made up of
The vascular tree is composed of the arteries, veins and capillaries which conduct poorly oxygenated blood to the lungs and returns highly oxygenated blood to the heart.
what is the airway tree made up of
The airway tree consists of air-filled branching tubes, originating from the trachea, which conduct ‘new’ atmospheric air to the gas exchange surfaces and return ‘used’ air to the environment.
what is the trachea
the single widest of the conducting airways, however it has the smallest total cross-sectional area and therefore is responsible for most of the airway resistance.
To prevent collapse on inspiration, it is surrounded and supported by rings of hyaline cartilage which can be easily felt at the base of the neck.
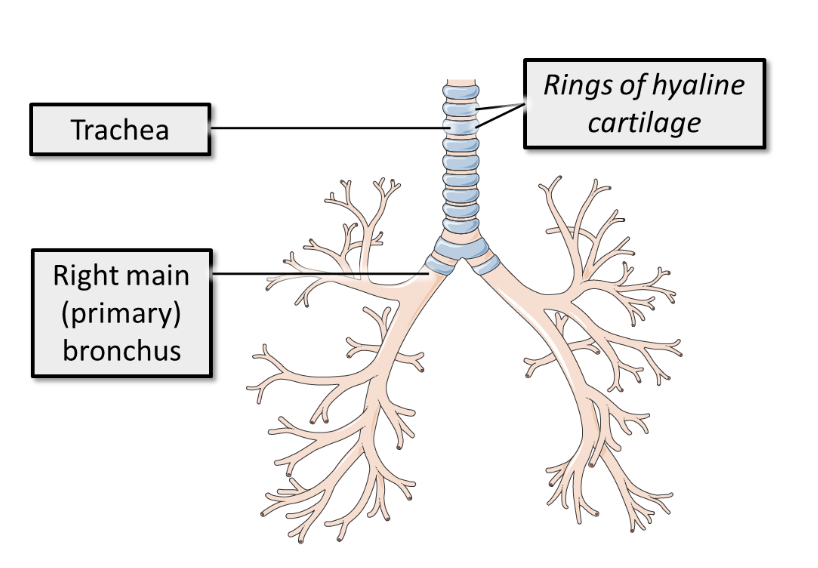
what does the trachea bifurcate into
into two primary or main bronchi which enter the lung. The bifurcation of the trachea occurs at vertebral level T4.
what is vertebral level T4
an important vertebral level to be aware of, as it is the level of several important landmarks:
It is the level of the sternal angle (angle between the manubrium and body of the sternum)
It is the level where the trachea bifurcate into the two main bronchi
It is the level of the arch of the aorta
It is where the second rib articulates with the sternum
how is the structure of the left and right primary/main bronchus slightly different
The right main bronchus is wider and shorter and runs more vertically than the left main bronchus to enter the hilum of the lung
The left main bronchus is oriented more horizontally, and runs inferior to the arch of the aorta and anterior to the esophagus and thoracic aorta, to reach the hilum of the lung.
what does the primary bronchi form
form the trunks of each of the lungs and go on to further divide (up to 11 times) into smaller and smaller bronchi.
These conducting tubes are also supported by rings of cartilage.
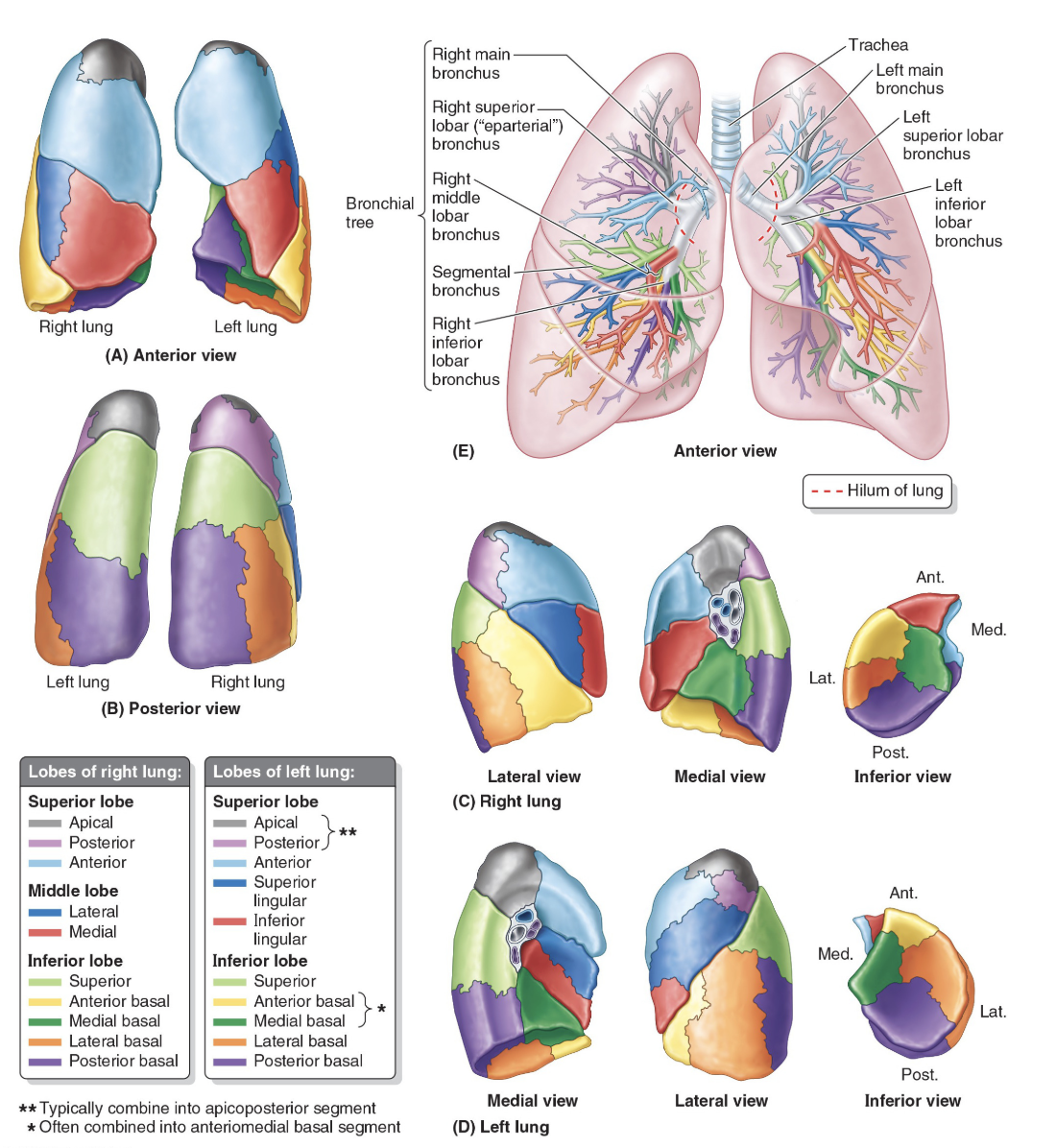
The main bronchi first divide into secondary/lobar bronchi, one per lobe of each lung, and then these divide into tertiary/segmental bronchi.
Each tertiary bronchus supplies a different segment of the lung
what forms the conducting zones of the lower respiratory system
The first 17 generations of airway (i.e. the trachea and 16 successive airway branches) form the conducting zone of the lower respiratory system.
where are bronchioles formed
At about the 12th division of the bronchi, bronchioles can be found. These are small, collapsible passageways with smooth muscle walls.
The bronchioles then continue to further branch (up to 11 times) until the respiratory bronchioles begin to appear.
what do bronchioles act as the transition between
Respiratory bronchioles are the transition between the conducting airways and the gas exchanging tissues of the lung. These terminate at the alveolar ducts which lead to the alveoli.
The structures from the respiratory bronchioles to the alveoli form the respiratory zone of the lower respiratory system.
respiratory system table
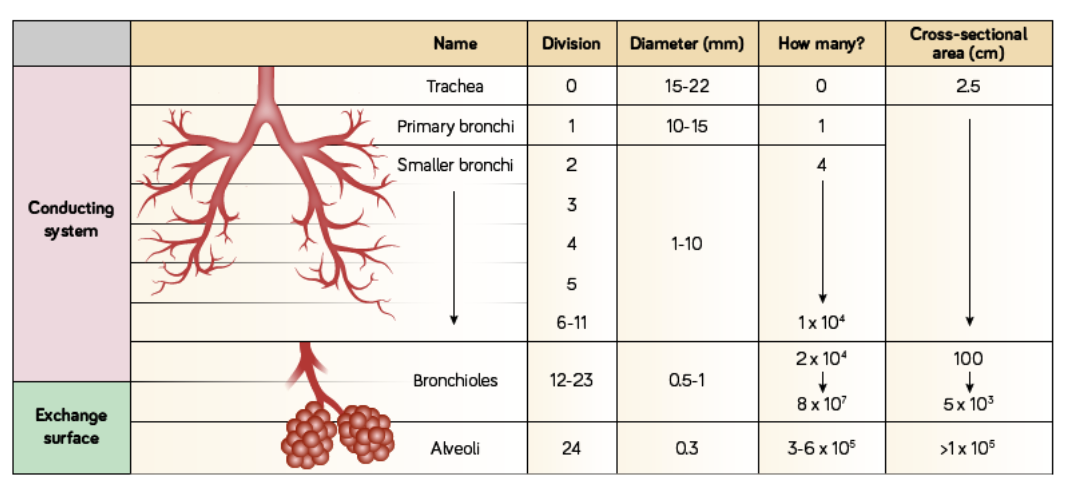
what is the tracheobronchial tree
Each tertiary bronchus supplies a different bronchopulmonary segment of the lung. You don't need to remember all of these, but it is interesting to see!
what are the alveoli
the primary site of gas exchange.
They are small outpockets which greatly increase the surface area for gas exchange.
what are alveoli on the tree model
On the tree model, alveoli are the leaves of the airway tree,
however they are also the point of contact between the two trees where the ‘air sacs’ become wrapped in capilliaries.
wha are lung lobules
Alveoli are arranged in lung lobules which are a cluster of alveoli surrounded by elastic fibres and a network of capillaries.
A lung lobule is a cluster of alveoli supplied by a single respiratory bronchiole, surrounded by the connective tissue of the lung:
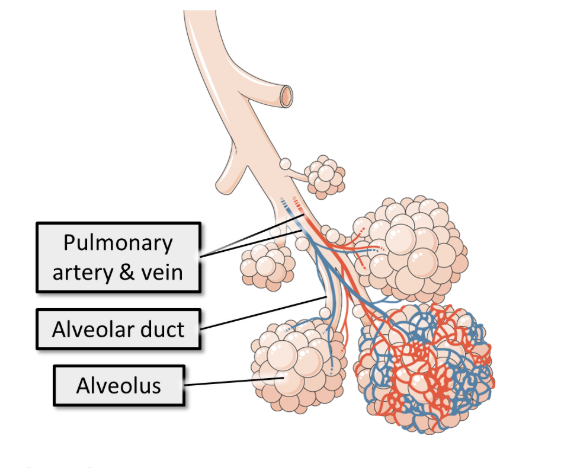
describe the features of the alveoli
Alveoli have extremely thin walls (only one cell thick) with basement membranes fused to the endothelium of the capillaries surround them.
The apical surface is covered in a surfactant into which gases dissolve to aid their diffusion.
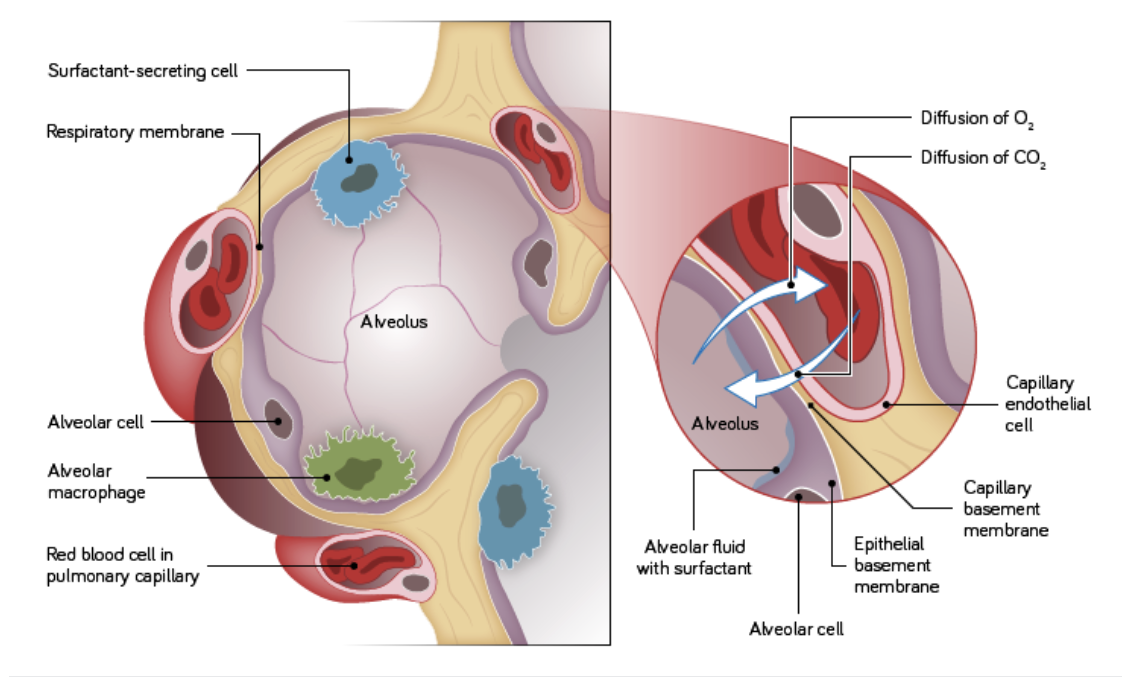
What are the structural features and function of the upper respiratory tract?
Large surface area in nasal cavity and sinuses helps:
Warm inhaled air
Moisten inhaled air
Lined with pseudostratified columnar epithelium
Columnar cells have cilia on their surface
Contains mucus-secreting goblet cells
This combination is called respiratory epithelium
What supports the trachea and bronchi, and how does this change down the airway?
Trachea and large bronchi:
Supported by rings of hyaline cartilage
Have incomplete smooth muscle support
Intrapulmonary bronchi:
Cartilage rings become cartilage plates
Smaller airways:
Cartilage decreases
Smooth muscle becomes the main support
How does the epithelium change through the bronchial tree into bronchioles?
Larger bronchi:
Lined with respiratory epithelium
Peripheral bronchi:
Epithelium becomes thinner
Still ciliated columnar cells + goblet cells
Bronchioles:
Lined with simple ciliated columnar epithelium
Goblet cells are sparse
Located between bronchi and where cilia stop
What are the epithelial types in the distal respiratory tract and where does gas exchange occur?
Gas exchange occurs in the distal respiratory tract
Respiratory bronchioles:
Lined with cuboidal ciliated epithelium
Alveolar ducts:
Lined with flattened epithelium
Form passageways leading into alveoli
What additional details are important about respiratory epithelium, bronchioles, and alveolar ducts?
Goblet cell hyperplasia:
Pathological increase in number/size of goblet cells
Leads to excess mucus production in respiratory epithelium
Bronchioles definition (more precise):
Distal airways between cartilage-walled bronchi and the point where ciliated epithelium ceases
Alveolar ducts structure:
Passageways formed mostly from openings of alveoli
Lined with flattened epithelium
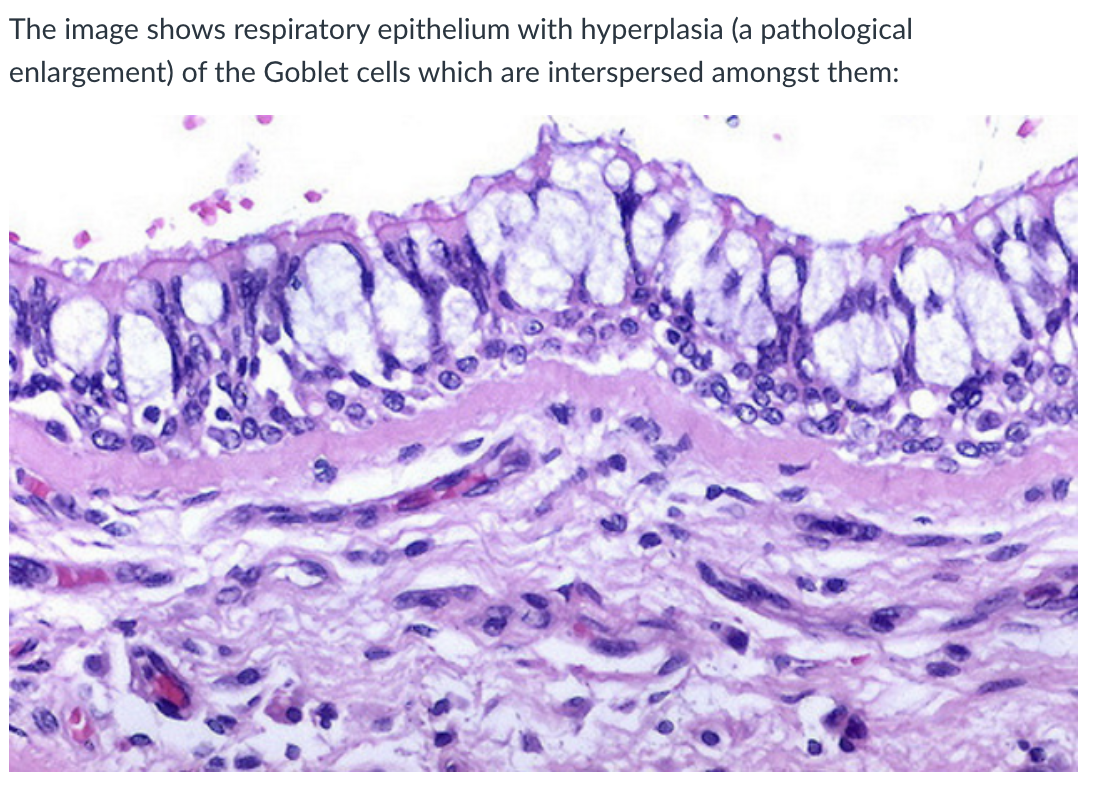
what type of cells do the avleoli consist of
The alveoli consist of Type I and II pneumocytes that lie on the basement membrane and also of alveolar macrophages.
The alveolar wall contains considerable amounts of elastin.
what does elastin in the alveolar wall allow for
Elastin allows the lungs to stretch to accommodate inspired air, it recoils to its original shape, allowing air to be expelled and it acts as a support, attaching airways with no cartilage firmly to the connective tissue of the lung.
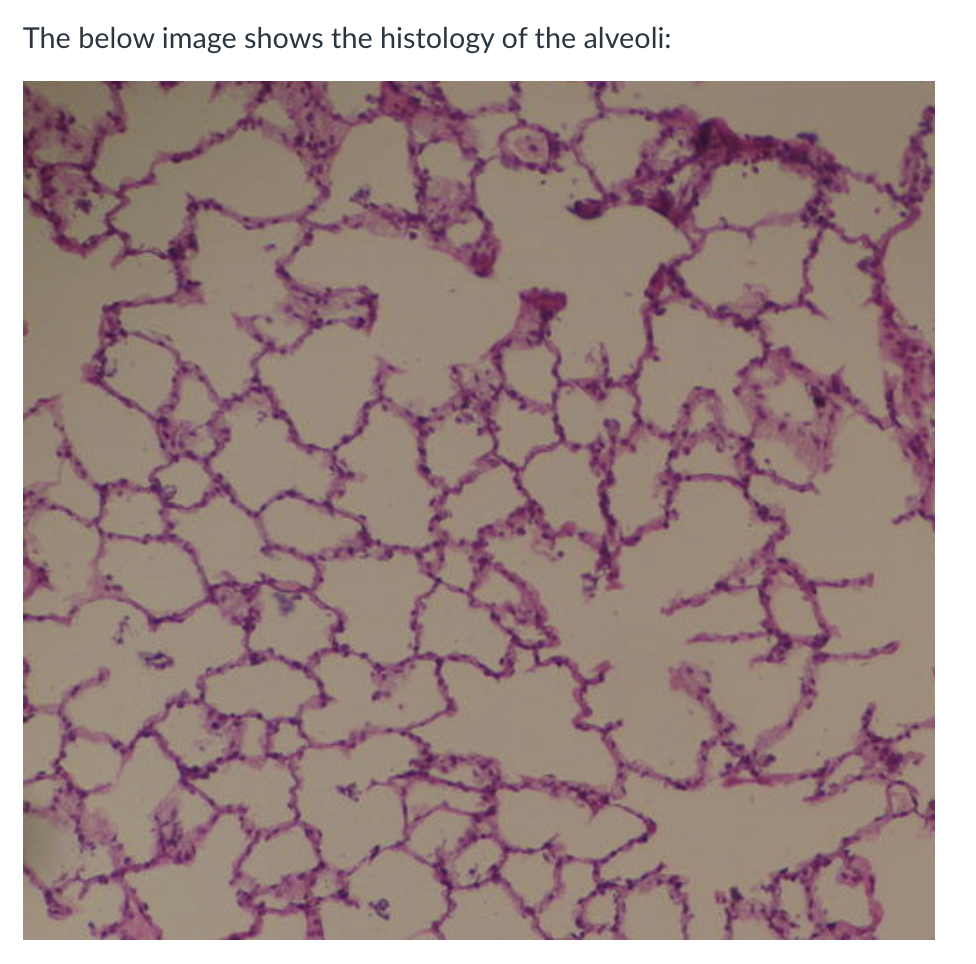
what are Type I Pneumocytes
very thin cells which allow gaseous diffusion. They represent about 40% of the number of alveolar cells but 90% of the surface area lining the alveoli.
They are flattened cells with flattened nuclei and are joined together by tight junctions.
They have few organelles and provide a very thin covering over the basement membrane; the thinness of which contributes to the efficiency of gaseous exchange.
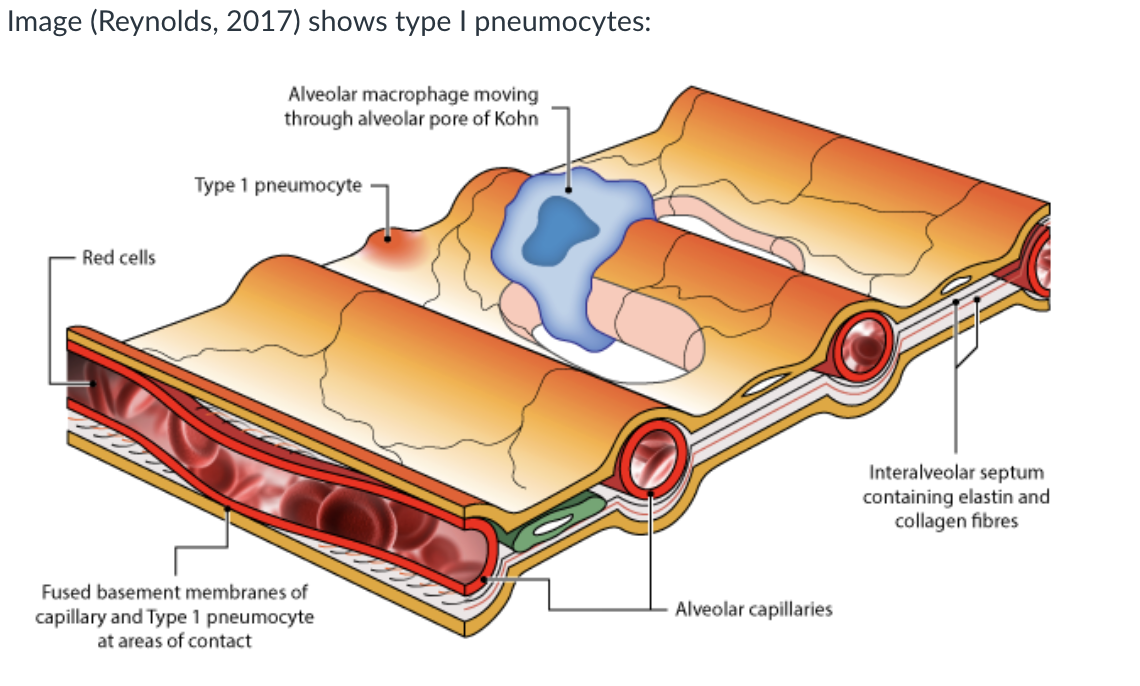
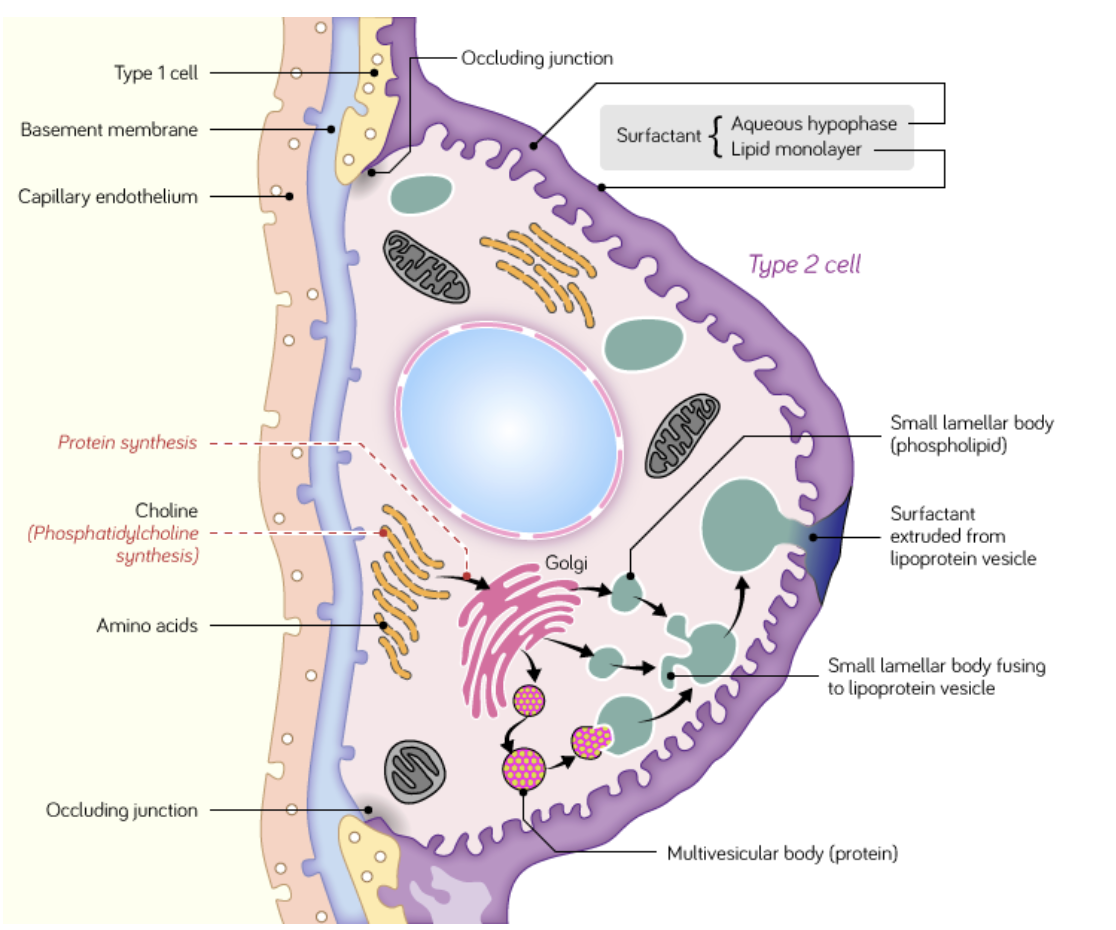
what are Type II Pneumocytes
secrete surfactant. They represent 60% of the number of alveolar cells but only 5-10% of the surface area lining the alveoli.
These cells are rounded in shape and contain numerous mitochondria.
Surfactant acts as a detergent, reducing alveolar surface tension, preventing collapse of the alveoli during expiration and facilitating inspirational expansion.
Some type II pneumocytes act as precursor stem cells for type I pneumocytes.
what are alveolar macrophages
‘patrol’ the alveolar air spaces and the interalveolar septa (the walls of the alveoli) and can pass freely between the two.
phagocytose inhaled debris and pathogens.
Following phagocytosis- may pass into the lymphatic system or adhere to mucous-coated ciliated epithelium and continue up the mucociliary escalator to the trachea where they are cleared by coughing.
how can Infections of the respiratory tract be separated
nto upper respiratory tract infections (URTI) and lower respiratory tract infections (LRTI).
However, some infections like influenza can affect both the upper and lower tracts.
what are URTI commonly like
generally milder, include things like tonsillitis and the common cold.
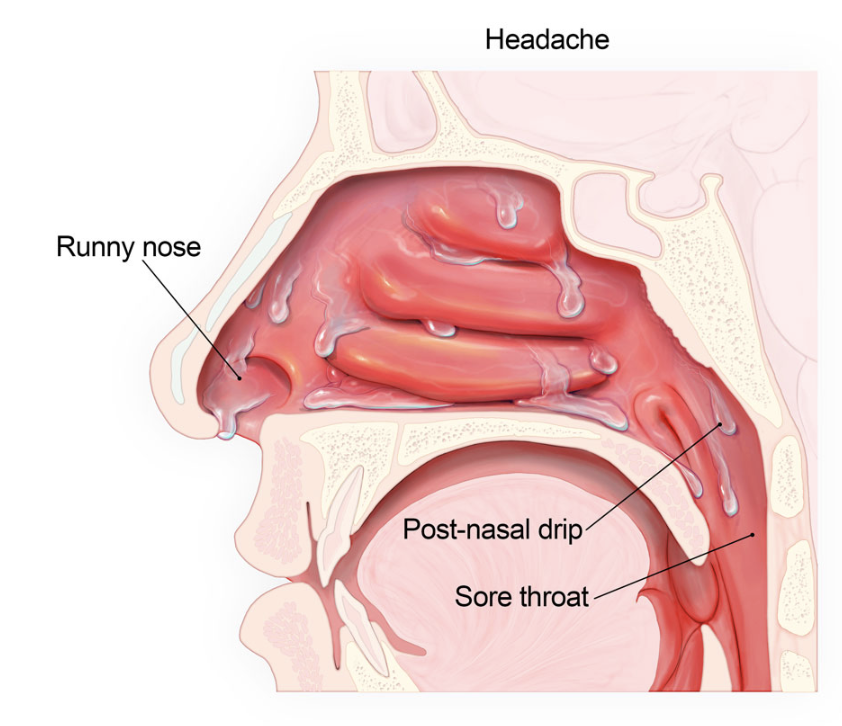
Inflammation of the sinuses (sinusitis) and increased mucus production causes symptoms like a runny nose (coryza), headache, low-grade fever, and sneezing.
Some mucus can drip down the posterior side of the pharynx (post-nasal drip) into the larynx, contributing to symptoms like a cough and sore throat. In most cases,
URTIs are viral and will self-resolve without treatment.
what are LRTI commonly like
generally more severe and include things like bronchitis and pneumonia.
Inflammation and the presence of pathogens in the lungs can cause the airways to narrow and the alveoli to fill with pus and fluid instead of air.
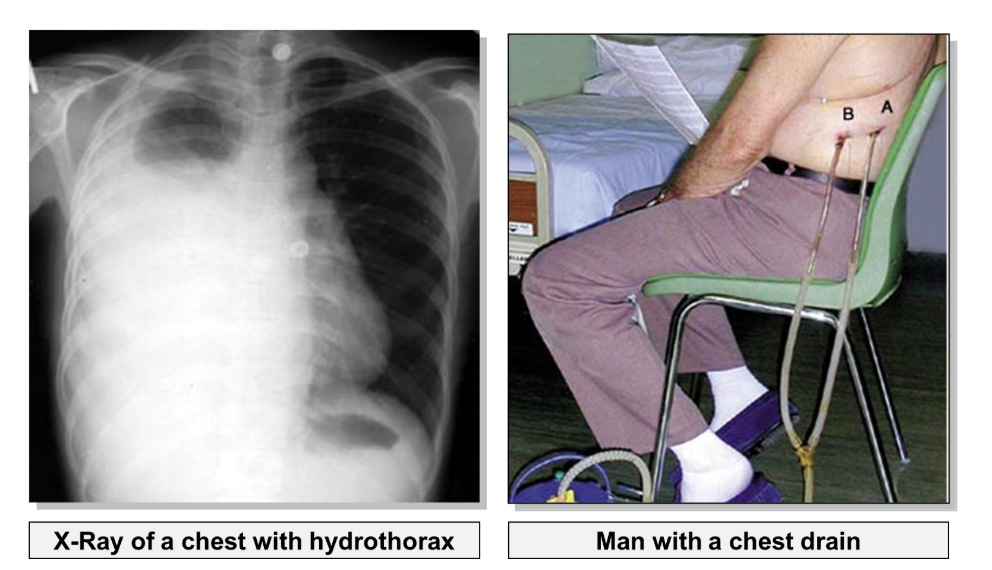
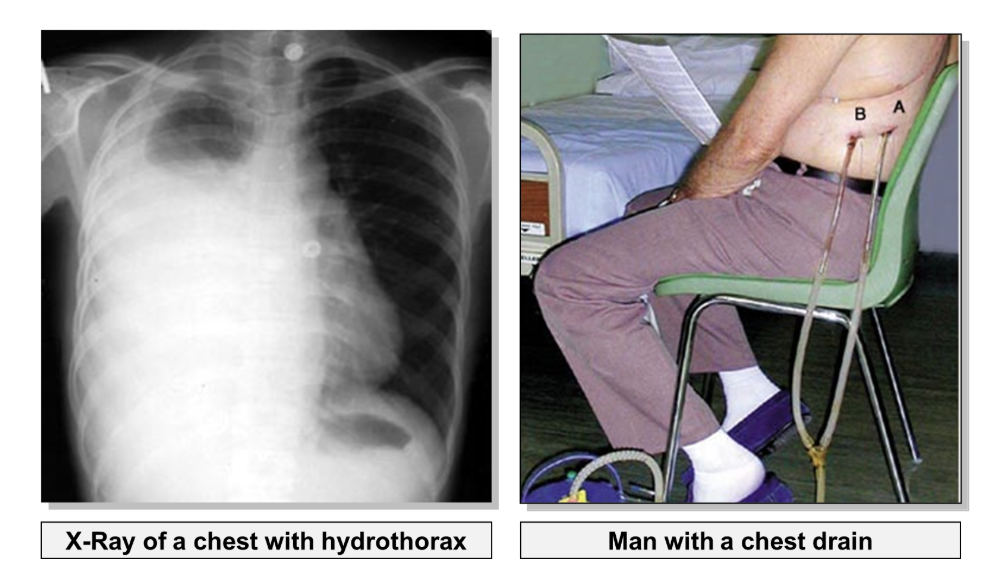
On an x-ray, air is completely black whereas the pus and fluid can appear as a hazy white:
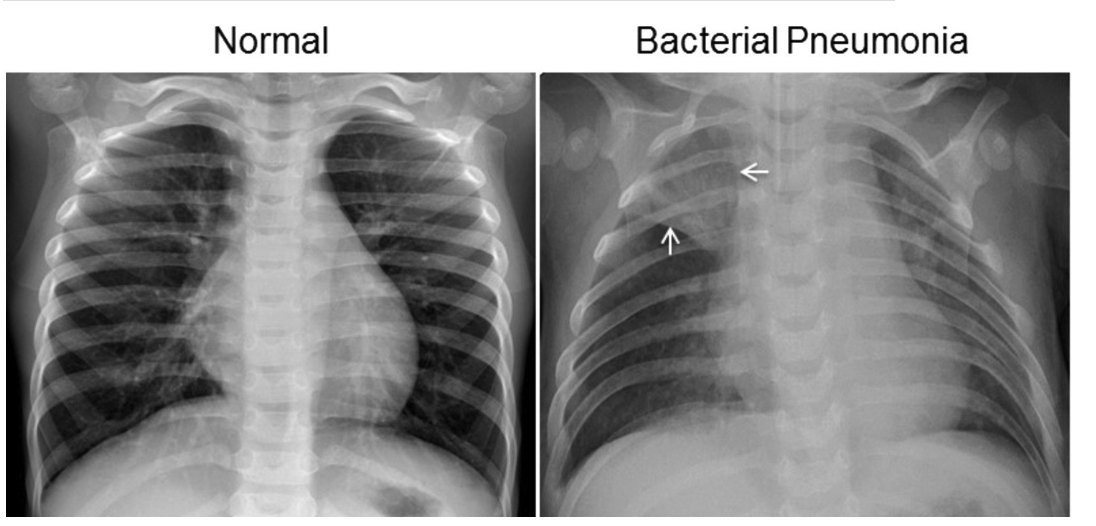
what are LTRIs characterised by
symptoms like a high-grade fever, cough, shortness of breath, and chest pain.
In some cases this will require treatment like antibiotics to help fight the infection and supplemental oxygen to help maintain sufficient gas exchange in the lungs.
what is the relation between LRTI and secondary infection
Even if the original cause of a LRTI is viral (e.g. COVID-19) accumulation and stasis of mucus in the lungs inhibits the clearance of bacteria. This can allow the bacteria to grow and cause a secondary infection, which requires antibiotic treatment.
what is a collapsed lung often the result of
pressure on an airway/ lungs from outside - a swollen lymph nodes or fluid/ air between the lining of the lungs (visceral pleura) and the chest wall (parietal pleura) i.e, in the pleural cavity.
what causes a collapsed lung
If a significant amount of air or fluid enters the pleural cavity, the surface tension adhering the visceral and parietal pleura is broken and pleural cavity becomes a real space (no longer a potential space).
As a result, the lung collapses, due to the elastic nature of the lung tissue.
what is a common cause of a collapsed lung
A common cause of this is a puncture wound to the thorax (e.g. a gunshot wound, stabbing injury). As a result air rushes into the pleural cavity. This is called a pneumothorax
what may accumulation of fluid in the pleural cavity be a result of
Accumulation of fluid in the pleural cavity may result from pleural effusion (escape of fluid into the pleural cavity), this is called hydrothorax.
what is a haemothorax
In a chest injury, blood may also enter the pleural cavity. This is called haemothorax. Haemothorax is usually a result of injury to a major intercostal vessel (usually by a fractured rib), rather than laceration to the lung.
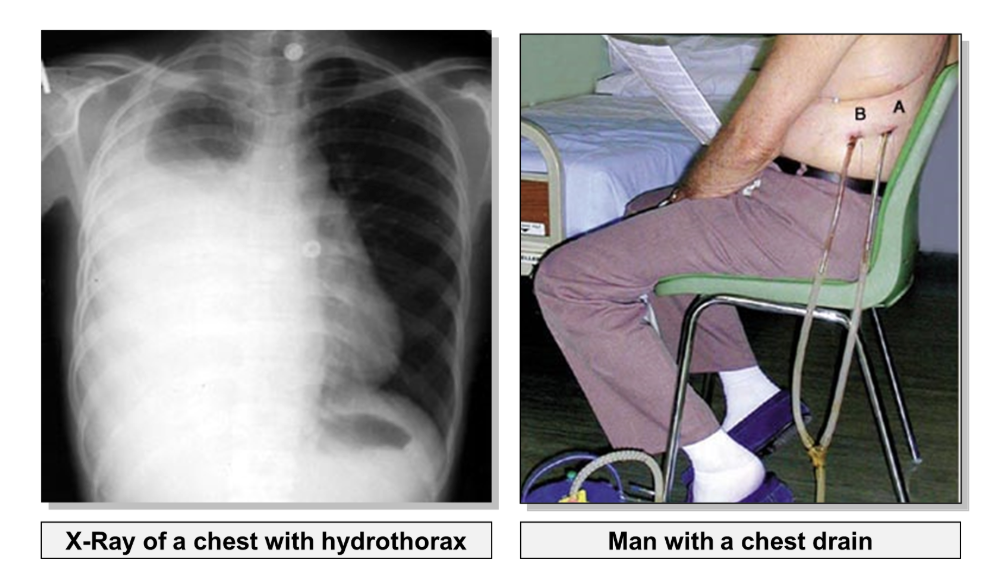
how is a collapsed lung treated
In order to re-inflate the lung, fluid must be drained from the pleural cavity using a chest drain.