PA Prof: Labs and Radiology
1/89
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
90 Terms
What does a "Left Shift" in a WBC differential typically imply?
Increase in Segmented and Bands (immature) neutrophils
An increase in Red Blood Cell (RBC) count suggests anemia.
False
The normal reference range for Platelet count is ________ to ________ x 103/uL.
150 – 400
Which RBC index indicates the "average size" of an RBC?
Mean Corpuscular Volume (MCV)
An increase in _________ indicates folate deficiency
Mean Cell Hemoglobin (MCH)
The normal reference range for Red Cell Distribution Width (RDW) is ________ to ________ %.
11.7 – 15.4%
What is the normal reference range for Prothrombin Time (PT)?
11.0-13.5 sec
The International Normalized Ratio (INR) normal range for a patient not on anticoagulation is 0.8 to 1.2.
True
To calculate the Upper Limit of Normal (ULN) for ESR in men, the formula is ________.
Age / 2
To calculate the Upper Limit of Normal (ULN) for ESR in women, the formula is _______.
(Age + 10) / 2
A ___________ measures, counts, evaluates and studies the aspects of blood; without differential counts the total number of WBCs and with differential differentiates how many of each kind of WBC.
Complete Blood Count (CBC)
A normal ________ measures the amount of hemoglobin (Hgb), hematocrit (HCT), white blood cells (WBC), and platelets (PLT).
Hemogram
The normal WBC count for a CBC is ___________. An increase indicates infection or physiologic stress and a decrease indicates marrow suppression or chemotherapy.
3.4 -10 × 103 cells/mm3
What is the normal white cell count differential value for neutrophils? What does an increase represent?
45%-73% ; Increase → bacterial infection
What is the normal white cell count differential value for eosinophils? What does an increase represent?
0-4% ; Increase → parasitic infection or hypersensitivity reaction(drug/allergies)
What is the normal white cell count differential value for basophils? What does an increase represent?
0-1% ; Increase → chronic inflammation or leukemia
What is the normal white cell count differential value for lymphocytes? What does an increase or decrease represent?
20-40% ; Increase → Mono, TB, syphilis, viral infections ; Decrease → HIV, radiation, steroids
What is the normal white cell count differential value for monocytes? What does an increase represent?
2-8% ; Increase → in recovery from bacterial infection, leukemia, TB-disseminated infection
What is the normal RBC count for males and females respectively?
4.6-6.2 × 106 cells/mm3 ; 4.2-5.2 × 106 cells/mm3
What do changes in RBC values indicate?
Increase → dehydration, erythrocytosis, polycythemia ; Decrease → anemia
What is the CBC value for hemoglobin in males and females respectively? What do changes indicate?
Male: 14-18 g/dL, Female: 12-16 g/dL ; Increase → hemoconcentration, polycethemia; Decrease → anemia
What is the CBC value for hematocrit in males and females respectively? What do low and high values indicate?
Males - 39-49%, Female - 35-45% ; Low → anemic or acute heavy bleeding; High → thick, sludgy blood
What indices describe the appearance of red blood cells (RBCs)?
MCV, MCH, MCHC, RDW
What does the Mean Corpuscular Volume (MCV) test indicate?
Expresses the volume of an “average” single RBC; normocytic (80-100fL), microcytic (<80 fL), macrocytic (>100fL)
Why would RBC be macrocytic or microcytic?
Macrocytic → B12 or folate deficiency; Microcytic → iron deficiency
What is a reticulocyte count test used to measure?
An indirect measure of RBC production; increase during RBC production
What is a normal CBC platelet count value? what do high and low values indicate?
140,000 - 440,000 per microL ; Low → Thrombocytopenia; High → Thrombocytosis (potential CVA, MI, thrombophlebitis)
What blood chemistry lab includes electrolytes (CO2, Cl-, K+, Na+), 2 kidney function tests (Creatinine and BUN), and glucose?
Chem 7/BMP (Fishbone)
What blood chemistry lab includes glucose, calcium, electrolytes, albumin, total protein, alkaline phosphatase, alanine transaminase, aspartate transaminase, bilirubin, blood urea nitrogen, and creatinine?
Comprehensive Metabolic Panel (CMP) /Chem 12/14
What normal values are found on the serum electrolyte panel?
Na+ - 136 - 145 mEq/L
K+ - 3.5 - 5.0 mEq/L
HCO3- - 24 - 30 mEq/L
Cl- - 96-106 mEq/L
What do extreme values of sodium indicate?
Greater than 145 mEq/L → Hypernatremia - occurs in renal or GI loss, impaired thirst
Less than 136 mEq/L → Hyponatremia - occurs in CHF, diarrhea, sweating, thiazides
What do extreme values of potassium indicate?
less than 3.5 mEq/L → Hypokalemia - indicates true or apparent depletion
greater than 5.0 mEq/L → Hyperkalemia - Indicates true or apparent excess
(Panic >6 → Cardiac arrest)
What do extreme values of Carbon dioxide or Bicarbonate indicate?
Decreased → Acidosis
Increased → Alkalosis
What do extreme values of chloride indicate?
Reduced → metabolic alkalosis
Increased → metabolic or respiratory acidosis
________ is an indicator of kidney function, with normal values being 0.7-1.5 mg/dL for adults and 0.2-0.7 mg/dL for children.
Serum Creatinine (SCr)
What does an increase in SCr indicate?
Worsening renal function that can lead to hyperprexia, hyperthyroidism, renal dysfunction, dehydration.
_____________ is an indicator of kidney function that may be a reflection of GFR, important in renal function, may be used to assess or monitor hydrational status, protein tolerance and catabolism.
Blood Urea Nitrogen (BUN)
What is a normal Blood Urea Nitrogen (BUN) value and what do changes indicate?
8-20 mg/dL ; Increased → leads to decreased renal perfusion, acute renal failure, obstruction; Decreased → leads to malnutrition, profound liver disease
(Panic > 100 mg/dL)
The _________ relationship has a normal ratio of 10:1, as BUN by itself is not as clinically significant. Greater than 20:1 pre-renal causes of dysfunction, 10:1 - 20:1 intrinsic renal damage, but 20:1 may be normal if both are in normal ranges.
BUN/SCr
What are the normal blood chemistry glucose values and what do changes indicate?
70-110 mg/dL ; Hyperglycemia → 3Ps, may progress to coma ; Hypoglycemia → caused by fasting, insulin administration
What are the normal blood chemistry calcium values and what do changes indicate?
8.5 - 10.8 mg/dL; Less than 8.5 mg/dL → Hypocalcemia and more than 10.8 mg/dL → Hypercalcemia
What are the normal blood chemistry total protein and albumin values and what do changes indicate?
5.5-9.0 g/dL, 3.0-5.0 g/dL ; Low could be caused by liver dysfunction
What are the normal blood chemistry alkaline phosphatase values and what do changes indicate?
Ranges vary widely; Increase → occurs in liver dysfunction
What are the normal blood chemistry aminotransferases (ALT, AST) values and what do changes indicate?
3-30 IU/L, 8-42 IU/L ; Increase AST occurs after MI, muscle diseases, hemolysis.
(Ratio of AST:ALT of 2:1 → suggests Alcoholic Liver Disease (ALD))
___________ are measure indicators of liver disease, sensitive to hepatic inflammation and necrosis.
Aminotransferases
What are the normal blood chemistry bilirubin (direct, conjugated) values and what do changes indicate?
0.1 -0.3 mg/d ; Increase associated with increases in other liver enzymes, reflect liver disease
What are the normal blood chemistry lactate dehydrogenase values and what do changes indicate?
100 - 225 IU/L ; Increase caused by hemolysis, Gilberts syndrome, Crigler-Najar syndrome, or neonatal jaundice
What are the normal blood chemistry magnesium values and what do changes indicate?
1.5 - 2.2 mEq/L; Less Than 1.5 mEq/L → Hypomagnesemia; Greater Than 2.2 mEq/L → Hypermagnesemia
(primarily eliminated by the kidney)
What are the normal blood chemistry phosphate values and what do changes indicate?
2.6 - 4.5 mg/dl; Less than 2.6 → Hypophosphatemia; Greater than 4.5 → Hyperphosphatemia
What do various urine test results indicate?
Clear yellow - normal
Cloudy - caused by urates (acid), phosphates (alkaline), RBC/WBC
Foam - caused by protein/bile acids
______ refers to a test’s ability to designate an individual with a disease as positive. High percentage means few false negatives.
Sensitivity (SnNOut)
_________ of a test is its ability to designate an individual who does not have a disease as negative. Higher percentage will show patients without a finding having no disease.
Specificity (SpPIn)
__________ interpret imaging, perform image-guided procedures, effectively communicate the interpretation, and ensure patient safety.
Radiologist
_________ involves synthesizing image findings with clinical history to formulate the best conclusion.
Image interpretation
What are some examples of image guided procedures?
Biopsies
Thoracentesis, Paracentesis, Lumbar puncture
Drain placement
Vascular intervention
Oncology
What are the safety precautions for MRI?
No metal
What are the safety precautions for Interventional radiology?
Time-out
Limit risks by blood thinners, NPO, allergies, sterile equipment
Follow for complication
What is the active ingredient in CT contrast?
Iodinated
What is the active ingredient in MRI contrast?
Gadolinium
What is the active ingredient in Enteric contrast?
Barium, Gastrograffin, etc.
How can contrast be administered?
By mouth (PO) or by rctm (PR)
Intravenously (IV), arteially (IA)
Retrograde urethrally
Instilled by catheter
Percutaneously into cavities
_________ allergy is not a contraindication to CT contrast.
Shellfish
What are some mild adverse reactions to contrast?
Urticaria
Nausea/vomiting
What are some moderate to severe adverse reactions to contrast?
Vasovagal
Bronchospasm
Anaphylactoid
____________ can occur with iodinated IV (CT) contrast and is defined as a serum creatinine increase of 25%.
Contrast nephrotoxicity
_______________ is a risk of MRI contrast that is an extremely debilitating fibrotic condition of the skin and solid organs, rare.
Nephrogenic Systemic Fibrosis (NSF)
_________ contrast has been shown to cross the human placenta and ________ is thought to cross the placenta.
Iodinated, Gadolinium
List imaging tests in terms of lowest to highest radiation exposure.
Ultrasound → MRI → X-Rays → CT → Nuclear medicine
What are the special patient populations to consider in radiology?
Pregnant, Children, Renal Insufficiency
When is the use of contrast in CT most helpful?
Abdomen - evaluating for most primaries, especially renal, pancreas, liver
Brain - metastatic tumors
Angiogram of the head and neck
Characterizing an aortic aneurysm
_______________ is the best resource for determining best imaging to order for various situations.
American College of Radiology (ACR) Appropriateness Criteria
What can be visualized in the PA view of a plain field X-Ray?
Scapula is seen in the periphery of the thorax
Clavicles project over lung fields
Posterior ribs are distinct
Position of markers
What can be visualized in the AP view of a plain field X-Ray?
Scapula over lung fields
Clavicles are above the apex of lung fields
Anterior ribs are distinct
Position of markers
___________ refer to bone because they absorb the greatest amount of x-ray; bone is white on radiographs.
Radiodense / Radiopaque
_________ refers to air because it absorbs little to no x-ray; air is black on x-ray.
Radiolucent
What are the 5 basic densities of X-Ray?
air
fat
fluid or soft tissue
calcium
metal
__________ refers to white structure on an MRI image.
Bright signal
__________ refers to dark gray to black on an MRI image.
Dark signal
Signal intensity of MRI is dependent on …
Tissue content of H20
Sequence (T1 or T2)
_______________ involves the injection of radiopharmeceutical that is scanned with radiation sensitive detectors, that reconstruct images from levels of radiation received.
Nuclear medicine, SPECT, PET
_____ shows anatomy and location of RA in space, ________ show function.
CT; SPECT & PET
__________ refers to light gray to medium gray signal return on an ultrasound.
Isoechoic
_________ refers to very bright, heavy signal return on an ultrasound.
Hyperechoic/Echogenic (sonodense)
_________ refers to dark, without echo return on an ultrasound.
Anechoic (sonolucent)
_________ refers to the visual recognition of figures and whole forms, not a collection of simple lines and curves.
“Gestalt”
________ refers to something that one has seen before and is instantly recognizeable.
“Aunt Minnie”
What is the systematic approach to chest X-rays?
A: airways
B: breathing (lungs and pleural spaces)
C: circulation (cardiomediastinal contour)
D: disability (bones- especially fractures)
E: everything else
What is the systematic approach to abdominal X-rays?
A: air (where should it be)
B: bowel (postion, size, wall thickness)
D: dense structures (calcification and bones)
O: organs and soft tissues
X: external objects and artifacts
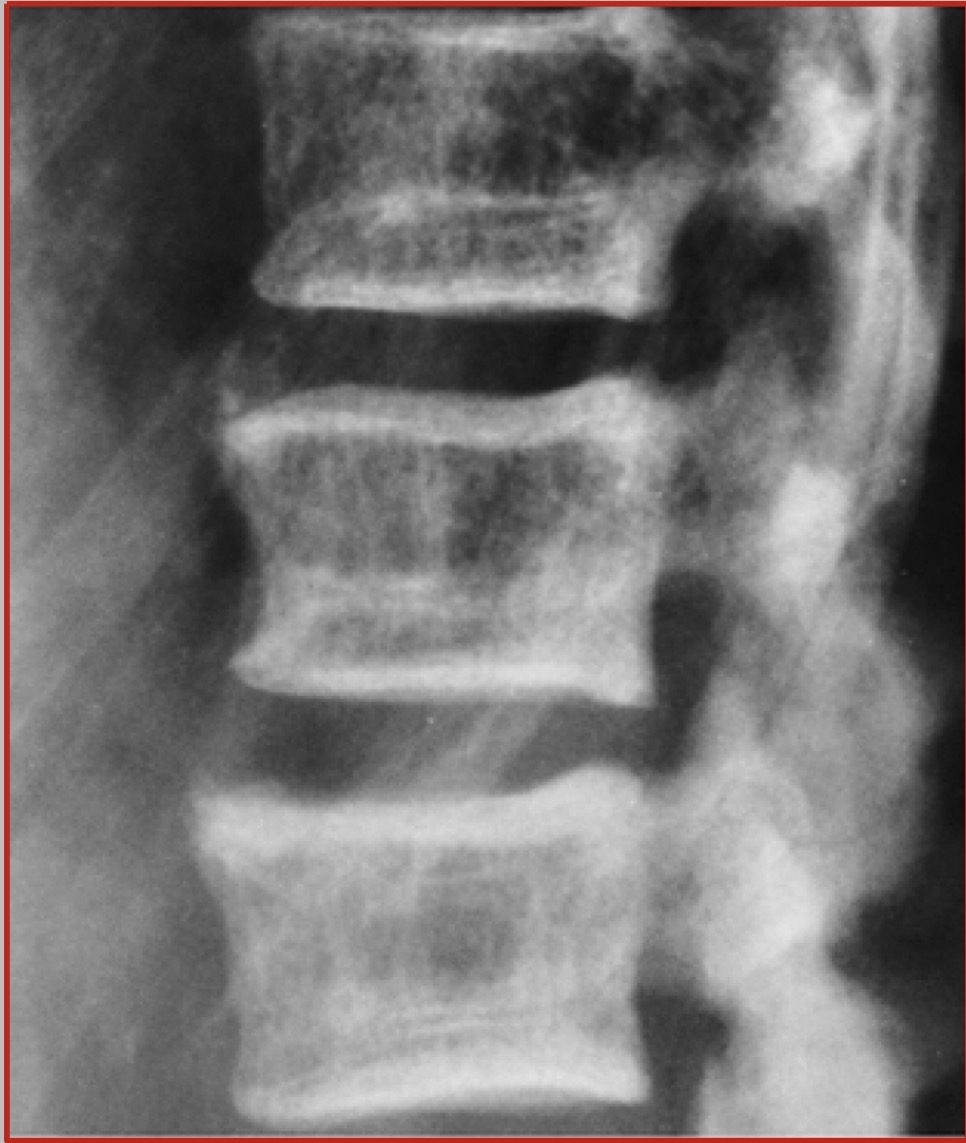
_________ refers to bones that are brittle and fracture.
Osteoporosis
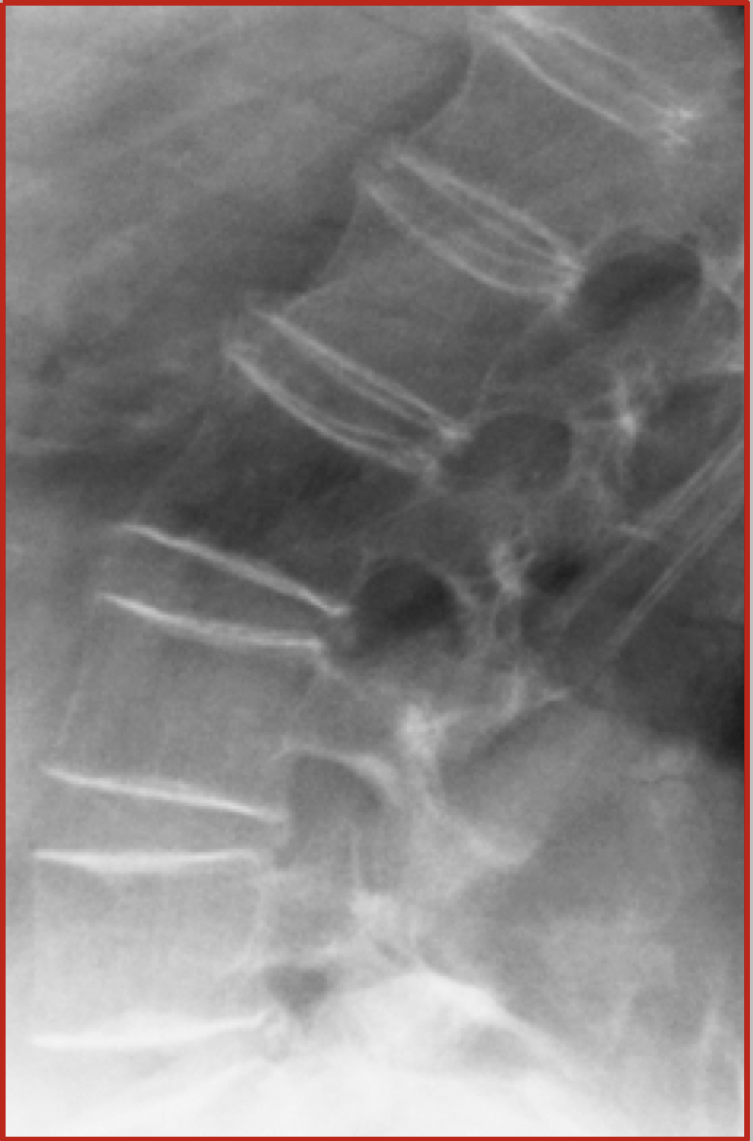
________ refers to bones that are soft and bend.
Osteomalacia