PCT need to know questions
1/88
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
89 Terms
What is the first choice for the vein for blood draw?
median cupital
What is the second vein choice for blood draw?
cephalic vein
What 3 patient identifiers do you need?
Name, DOB, MRN #
What is the purpose of the tourniquet?
So the vein can puff up making an easier draw, INCREASE VENUS PRESSURE.
What could cause a hematoma during blood draw?
Skin cells breaking and trying to rebuild. No pressure, probed.
What is hemolysis?
Destruction of red blood cells in the sample.
What could cause a fainting during blood draw?
Syncope; un-comfortability, anxious, over probing, too much blood.
What is the last vein to choose for blood draw?
Basilic
What are three reasons why you would preform capillary puncture and not venous puncture?
Children, deformities, veins are too small, only small amount of blood needed, patient age development.
When should you label the specimen?
After draw, facing patient, before they leave.
What do you do if you forget to label the specimen?
Redraw.
If a specimen requires to be maintained at body temp. what do you use?
A warmer, or foil.
GTT testing (glucose) Should the pt be fasting?
yes.
What is does the yellow stand for in venous order of draw?
Sterile → blood cultures.
What is the additive for the yellow color of venous order of draw?
SPS
What do you use for a capillary order of draw?
Use a lancet.
What is the first tube for order of draw for capillary puncture?
Lavender
What is the only test that you would draw before the tube listed in #1 for capillary order of draw?
Green tip, tests oxygen
How many ml of urine does a urinalysis need?
30ml
What method do you use to obtain urine for a urinalysis/culture?
Clean catch.
What are the directions for a urinalysis?
move labia/ foreskin
clean with wipe
urinate a small amount into the toilet
catch the rest in the cup
After obtaining urine for a urinalysis, before what amount of time do you have to refrigerate the specimen?
1 hr.
What does cloudy urine mean?
It is not refrigerated ro bacteria is in the patients urinary system.
What doe chain of custody examples include?
BAC and drug testing.
What time should you collect sputum samples?
In the morning.
What instructions should be given to a pt that is doing the sputum samples?
Move into fowlers position, instruct them to deep breath 3 times then cough until thick mucus comes up. They should release it into the container.
What are stool samples used for?
They are used to detect bacteria, cancer (blood in specimen), and parasites.
What should you do if a patient comes back positive for C-DIFF?
they will be put into contact precautions so everyone will wear gown, gloves before entering room.
What is the first order of electrical conductions?
SA or Sinoatrial node.
R to R greater than 5lg. boxes means what?
Bradycardia.
R to R gless than 3 lg boxes is…
tachycardia.
Where is the V6 located?
Mid axillary
Where is V4 located?
5th intercostal, mid clavicular (APICAL PULSE)
What is the Left Leg or LL called?
Ground Green.
How many seconds is the small box?
0.04 seconds.
Which wave is considered ventricular?
QRS.
Which wave is considered atria?
P wave.
What is the paper speed for a regular EKG?
25mm/sec.
What is the paper speed for Tachycardia?
50mm/sec.
What does artifact mean?
Patient movement or EKG problem.
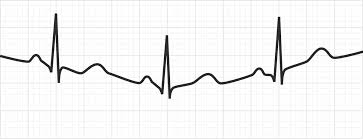
.
Wandering Baseline (patient movement)
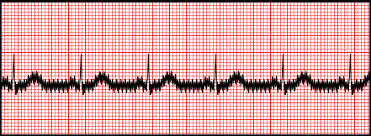
.
AC 60-cycle interference (electrical current nearby)
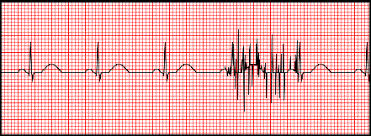
Somatic tremor (cough, sneezing, etc.)
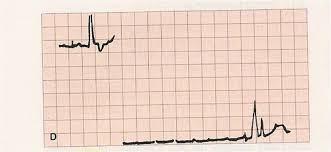
Interrupted Baseline. (wire or lead dislodged)
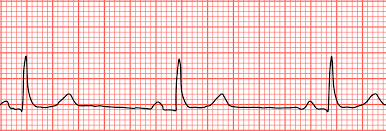
Sinus Bradycardia (5 big box)
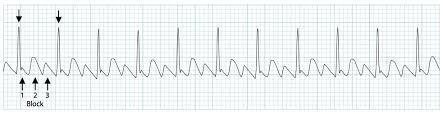
atrial flutter (classic sawtooth waves)
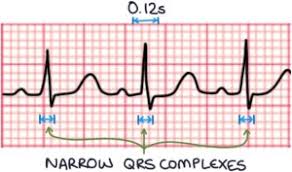
Sinus Tachycardia (less than 3 large boxes)
what does sinus mean?
PQRST waves present.
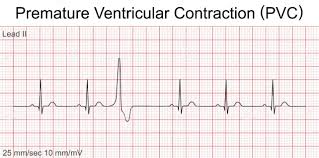
Premature Ventricular Contraction (lg. QRS less than 3 large boxes)
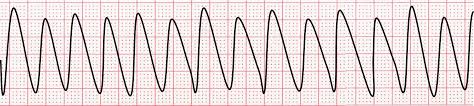
Ventricular Tachycardia (Notify nurse call code, unresponsive)
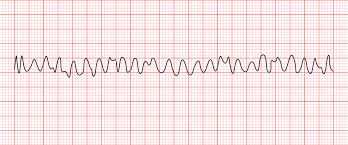
Ventricular Fibrillation (USE defibrillator) (CPR,AED)
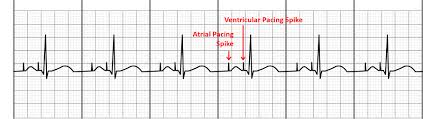
Pacemaker Spike
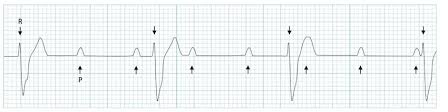
3rd Degree heart Block (No T wavs, emergency; Asystole→ Report call code, start CPR
When do you get an adults vital signs?
Baseline→ at admittance
How many Respirations is normal?
12-20
What happens if respirations are over 20?
tachypnea.
What is the definition of perspiration?
Sweating.
I & O?
Document in a flow/graph sheet.
If a PT needs 400ml every 8 hours, and they consumed 600ml, how many more ml do they need?
600ml more.
How much longer should you cut the wafer larger the stoma?
1/16 of an inch.
When should you change the wafer for the Ostomy bag?
Change 3-7 days.
Ileostomy definition
smell not as bad; liquid consistency; skin irritation
Colostomy definition:
Smells like feces; formed stool; not as irritating to the skin.
What is a nosebleed?
Epistaxis.
What should you use if you get an epistaxis?
pinch bridge of nose, lean forward for 10-15 minutes.
What do you do if you see someone laying on the floor?
Ask them if they are okay and shake them for a response, if there is no response then call 911 and begin CPR.
For CPR, how many chest compressions should you do?
Think of Tachycardia, 100/120 compressions for minute.
What should you do and how should the pt be during CPR?
30 compressions to 2 breaths; 2 inches deep in supine.
Vertebral injury:
pt should remain in supine position.
s/s of Myocardial Infarction (Heart Attack):
agina (CAD too); SOB; chest tightness; diaphoresis; N/V; heartburn; dizzy.
Is a straight Catheter and Foley Catheter placement sterile or nonsterile?
sterile.
Is Foley removal sterile or nonsterile?
nonsterile.
When using a gait belt on a patient, how should you ambulate?
stand on weaker side-slightly behind; with palms facing up.
What should you do for falling patients?
Lower slowly and protect the head.
Reacher’s/grabbers are used for patients who cannot bend:
COPD, Authoritis.
Which denture should you remove first?
remove the upper denture first.
What is a ROM and what is it used for?
Used for patients who are on bed rest; support patient above and below the joint.
Abduction:
movement of the limb away from the body. EX: hip, shoulder.
Flexion:
Decrease the angle. EX: elbow, knee , ankle, wrist.
Incentive spirometer:
relieves mucus buildup to prevent respiratory copmlications.
What position should you be in for incentive spirometer and Nasal Cannula?
Fowlers.
Nasal Cannula:
Can eat/drink.
Restraints:
Reposition every 2hrs. check on pt every 15min.
Fall risk patients:
post-op; children; elders; burns; check on every hr. to offer assistance.
What do SDCs and anti-embolism stockings help prevent?
DBT (deep vein thrombosis) also known as thrombophlebitis.
When should you remove SCDs and anti-embolism stockings?
remove 8hrs or every shift and report skin discoloration.
Contraindication:
Don’t do, could cause harm, EX: bad circulation for SCDs.
Pressure ulcer stage 1:
Sanguineous, fresh red bleeding.