Evaluation of Prosthetic Valves
1/83
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
84 Terms
For patients with what? it will be inevitable they receive intervention. (should need a prosthetic valves)
For patients with significant valvular stenosis/regurgitation, it will be in inevitable they receive intervention.
Types of Interventions: name 3 types of repair and for one of them tell me especially for what valves with what conditions?
• Valvular Repair
• Especially for mitral and tricuspid regurgitation
• Surgical Valve Replacement
• Percutaneous Valve Replacement
Percutaneous valves are what type of valves?
Percutaneous valves are bioprosthetic
Surgically implanted prosthetic valves can be either what?
Surgically implanted prosthetic valves can be either bioprosthetic or mechanical
Surgically implanted prosthetic valves can be either bioprosthetic or
mechanical;
Both are associated with what durability
Both need chronic what meds
Mechanical valve implantation has what over the past 10 years
• Both are associated with greater durability
• Both need chronic anticoagulation.
• Mechanical valve implantation has declined over the past 10 years
which valve repair and replacement have changed the demographics
and clinical characteristics of patients undergoing surgical valve
replacements.
Transcatheter valve repair and replacement have changed the demographics
and clinical characteristics of patients undergoing surgical valve
replacements.
Idk how to ask this?
Need for concurrent procedures such as aortic root and ascending aorta
modification, as well as left ventricular outflow tract (LVOT) or right
ventricular outflow tract (RVOT) alteration may also affect PHV choice
what is the first-line method for noninvasive evaluation of prosthetic alve function.
Echocardiography is the first-line method for noninvasive evaluation of prosthetic valve function.
This is complemented with two-dimensional and three- dimensional transesophageal echocardiography for further refinement of valve morphology and function
what is the best method to evalute MV and TV prosthetic valve
TEE
What other two have also enhanced their roles in evaluating valvular heart disease (gets rid of the artifact)
Computed tomography and cardiac magnetic resonance have also enhanced their roles in evaluating valvular heart disease
Types of Prosthetic valves
A wide variety of PHV types and sizes are available,
Selection is dependent upon what name 4 things
• Implantation location
• Underlying valvular pathology
• Implantation technique
• Patient-specific factors
Types of Prosthetic valves
• Selection for Patient-specific factors*** name 6
• Patient anatomy
• Procedural risk
• Expected patient longevity
• PHV durability
• Patient preferences
• Patient lifestyle
Mechanical vs. Bioprosthesis vs. Homograft:
• Mechanical describe two things
• Durability
• Hemodynamics

Mechanical vs. Bioprosthesis vs. Homograft:
• Bioprosthetic
• No anticoagulation
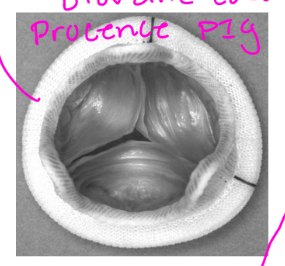
Mechanical vs. Bioprosthesis vs. Homograft:
Homograft
• No anticoagulation
• SBE prevention
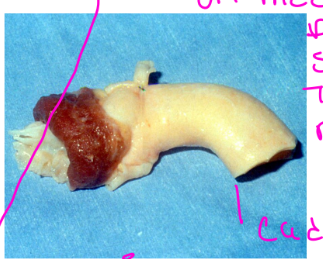
Prosthetic Valve Regurgitation:
Mechanical Prosthesis
what should you see physiologic MR
and what is abnormal regurigitant flow
Physiologic mitral regurgitation is a low velocity
jet and seen in small amounts between and
around the valve assembly.
Abnormal regurgitant flows have high velocities.
Prosthetic Valve Regurgitation
Bioprosthesis, what well you see in normal functioning valves?
• In normal functioning valves, backflow is less Bioprosthesis common.
Prosthetic Mechanical Valves, name 3
Bileaflet tilting disk valve
• Single tilting disk valves with low thrombogenicity
• The Starr-Edwards ball-in-cage valve is no longer implanted
what is the most common type Prosthetic Mechanical Valves?
• Bileaflet tilting disk valve
Give me examples of Bileaflet tilting disk valve
Examples inlude St. Jude Medical, Carbomedics, On-X
what does Bileaflet tilting disk valve offer of the currently available mechanical valves
Offer the best hemodynamics of currently available mechanical valves
• Single tilting disk valves with low thrombogenicity
tell me an example of one?
infrequenctly used in what practice ?
• Example is Medtronic-Hall
• Infrequently used in contemporary practice
The Starr-Edwards ball-in-cage valve is no longer implanted
• Given its durability, some of these valves continue to function
satisfactorily and may be encountered in clinical practice.
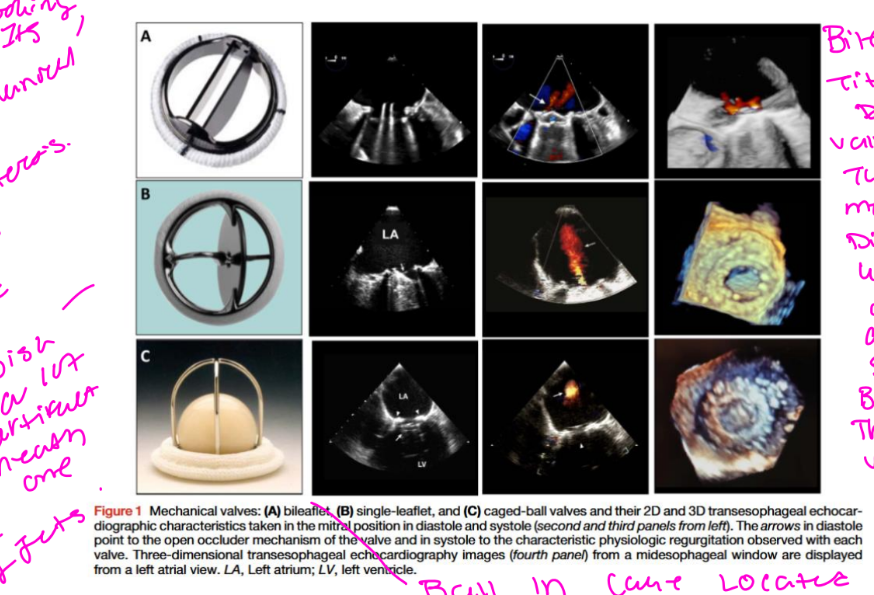
• Mechanical valves typically have how much regurgitant jets.
• Mechanical valves typically have minor regurgitant jets.
Mechanical valves typically have minor regurgitant jets. Two types of
‘‘physiologic’’ regurgitation may be seen:
a closing volume (retrograde displacement of blood caused by the motion of the occluder) and true trivial or mild regurgitation at the hinges of the occluder
Mechanical Valve;
Bileaflet, tilting disc – St. Jude’s
2 pyrolytic carbon semicircular discs
attached to rigid valve ring by small hinges
• Opening angle 75-90 degrees
• 3 orifices - small central and 2 larger
lateral orifices
• Normal regurgitant volume 5-10 mL
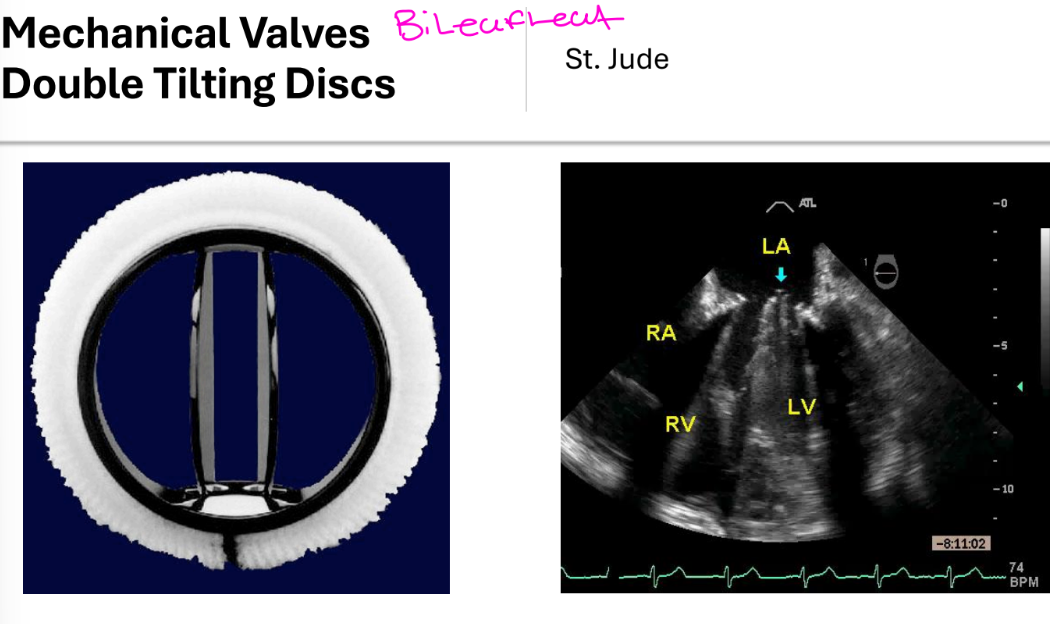
Mechanical Valve;
Bileaflet, tilting disc – St. Jude’s. Auscilatation
• Softer opening and louder closing click
• Softer closing click could represent
malfunction
• Suspect regurgitation when diastolic
murmur with AVR
• Suspect mitral regurgitation when
holosystolic murmur with MVR
Mechanical
Prosthesis;
Single tilting disc
• Circular sewing ring
• Opening angle 60-80 degrees
• Flow occurs through major and minor
orifices
• Normal regurgitant volume 5-9 mL
Mechanical
Prosthesis;
Single tilting disc, Auscultation
Sounds similar to bileaflet disc, 2-3 washing jets
Mechanical Valve
• Ball-in-Cage (Starr-Edwards)
• No longer implanted
• Due to durability may still be
encountered
• Sewing ring with metal struts
forming a cage
• Hollow ball in cage
• Appearance of echoes in the left
atrium due to speed of sound in
the ball
• Flow occurs around the ball
• Normal regurgitant volume 2-5mL
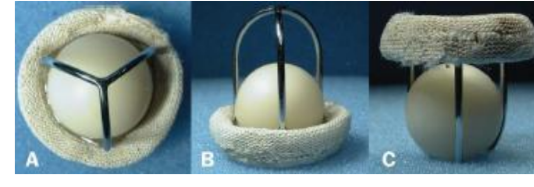
• Ball-in-Cage (Starr-Edwards)
Mechanical Valve • Auscultation
• Loud opening click, followed by several
clicks of different intensity due to ball-in-
cage
• If closing click is louder, could suggest
dysfunction
• If a diastolic murmur is heard with AVR
suggests aortic regurgitation
• Suspect mitral regurgitation when holo-
systolic murmur with MVR
• Prolonged diastolic rumble suggests
prosthetic stenosis, high flow state, small
prosthesis
Bioprosthetic Valves
Xenografts
Most frequently used
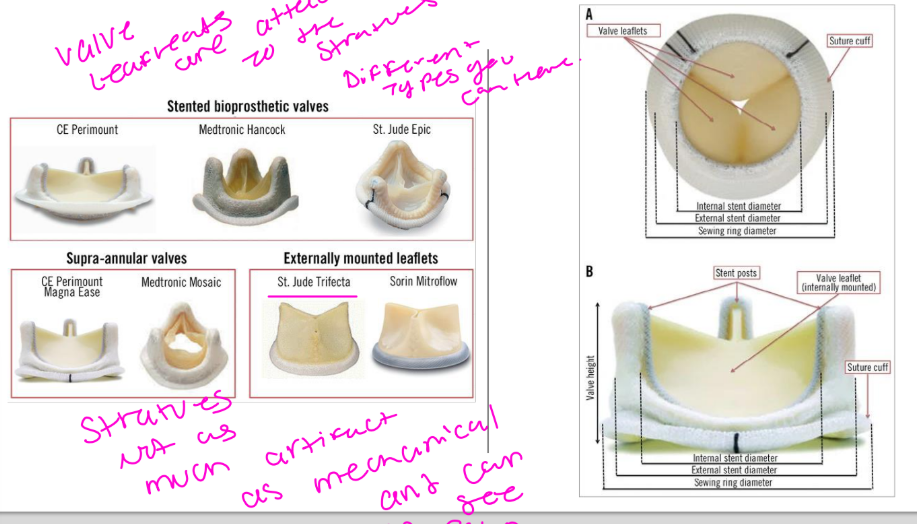
• Made of porcine or bovine pericardial tissue
• Stented xenografts are most frequently used
• Pericardial leaflets are mounted onto either the inside or outside of a
stent frame
• Externally mounted leaflets and stentless bioprostheses have the
advantage of larger valve areas and lower transvalvular gradients
• high rates of early structural valve dysfunction (SVD), particularly in younger patients
Allografts vs, autografts
Allografts from cadaveric donors
Autografts (such as in the Ross procedure)
Bioprosthetic Regurgitation
Regurgitation is increasingly reported in normal biologic valves
• Stentless valves, including homografts and autografts, are more
likely than stented valves to have minor regurgitant jet
Stented heterograft valves
• Sewing ring with 3 semi-rigid stents or struts
• Normal regurgitant volume 1 mL
• 10% demonstrate a small degree of regurgitation
by color flow imaging
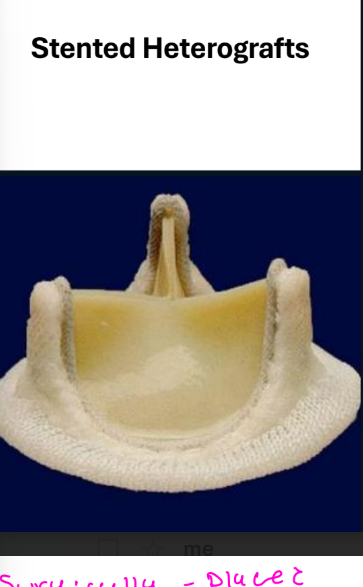
Stented Heterografts
• Auscultation
• Made of tissue and do not click
• Normal and abnormal opening and closing sounds
similar to native valves
• Aortic position - have a systolic ejection murmur
• Mitral position - have a early-mid systolic ejection
murmur attributable to turbulent flow in the LVOT
• Ejection murmur is followed by second heart
sound and then valve opening
• Low flow diastolic rumble maybe heard at the
apex
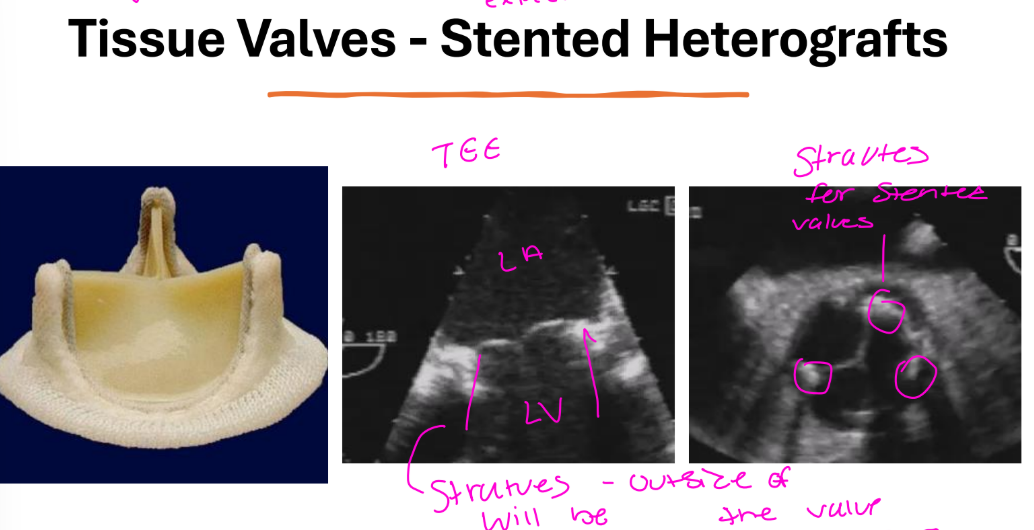
Bioprosthetic Valves
Stentless heterograft valves
• No rigid stents – larger
effective orifice area
• Better hemodynamic
performance as compared to
stented or biological valves
Bioprosthetic Valves, Homograft valves
• Antibiotic-sterilized,
cryogenically preserved
valves harvested from human
cadavers
• Favorable hemodynamics,
resistant to infection, no
anticoagulation requirement
• Usually implanted as a
complete root replacement
with coronary artery
reimplantation
Bioprosthetic Valves , Auscultation
• Sounds similar to native
valves
• Homografts with small
effective orifices may create
systolic ejection murmurs
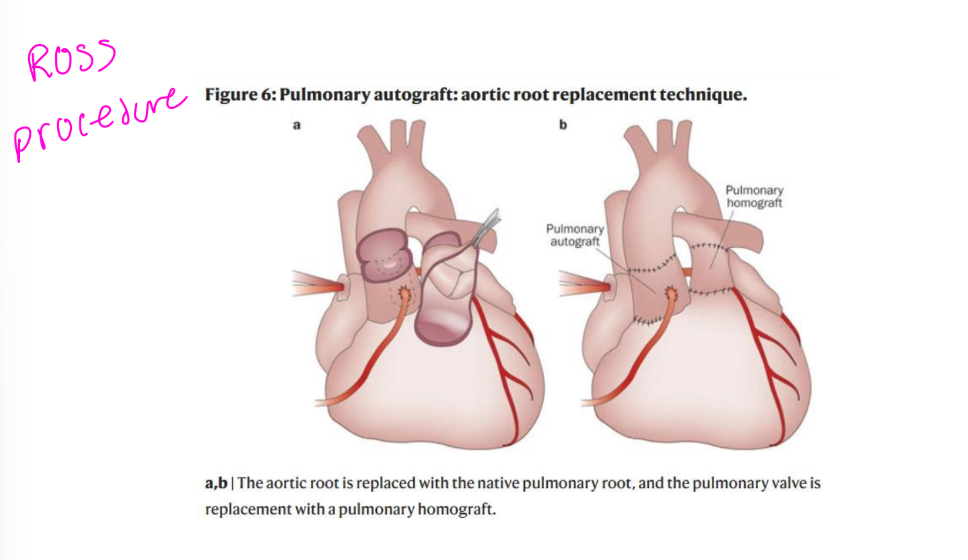
Ross Procedure
Known as switch procedure
Donald Ross, MD pioneered this surgery in 1967 for diseased
aortic valves
Performed on patients younger then 40 to 50 to avoid long-term
anticoagulation
Patient’s own pulmonary valve (autograft) placed in aortic valve
position and coronaries reimplanted
Pulmonary allograft (cadaver valve) placed in pulmonic position
Ross Procedure Assessment
• 2D Echo
• Assess aortic and pulmonic valve leaflets for thickness
• Utilize multiple views
• Color Flow Doppler
• Assess for aortic and pulmonic valve regurgitation
• Doppler
• Assess peak/mean valvular and sub-valvular gradients
• Assess for diastolic flow reversal in aorta
Percutaneous Valve Replacement ( slide 37)
• Transcatheter heart valve technology has
continued to evolve with expanding
indications
• Transcatheter aortic valve implantation
(TAVI) prostheses in commercial use
include balloon-expandable intraannular
devices (e.g., SAPIEN valves; Edwards
Lifesciences)
• Self expanding supra-annular valves (e.g.,
Evolut valves; Medtronic)
• Intra-annular valves (Navitor valves;
Abbott Structural Heart)