ECG Signals and Pacing
1/159
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
160 Terms
During depolarization, changes in voltage can be measured using what?
intracardiac electrograms (EGMs)
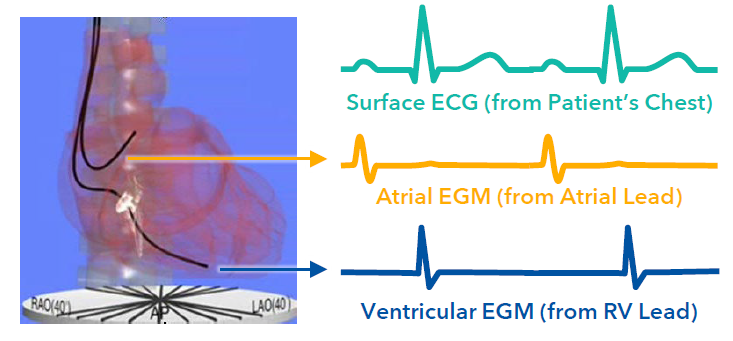
What are the 3 characteristics of an Electrical Signal?
1) Slew rate: a change in voltage over time, measured in volts per second
2) Duration: the length of the waveform, measured in milliseconds
3) Amplitude: the size of the signal (measured peak to peak) in millivolts
What is the slew rate also defined as?
It determines the time taken for a cardiac signal to move from peak to peak.
The longer it takes for the signal to go from peak to peak, the lower the slew rate, and the flatter the signal.
A higher slew rate results in a sharper signal.
Generally, higher slew rates result in better sensing (T/F)
T
Lead impedances should remain stable over the device’s lifetime. Generally, what percentage change (or abrupt change) is cause for concern?
30%
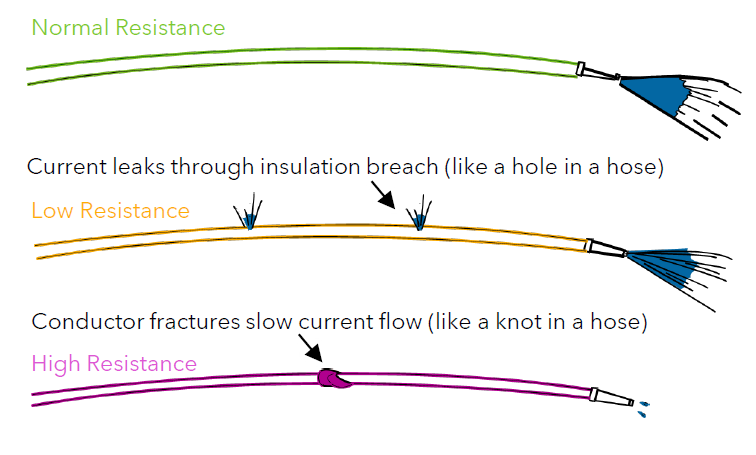
What is capture threshold?
the minimum electrical stimulus required to consistently depolarize the heart outside of the heart’s own refractory period (i.e., outside of the effective refractory period).
How is myocardial capture obtained?
A pacing output must be large enough (amplitude) and long enough (pulse width) to depolarize cardiac tissue.
What is Failure to Capture?
when a pacing stimulus is delivered but does not depolarize the myocardium
A pacing spike without subsequent myocardial depolarization (failure to capture) can be identified on the surface ECG
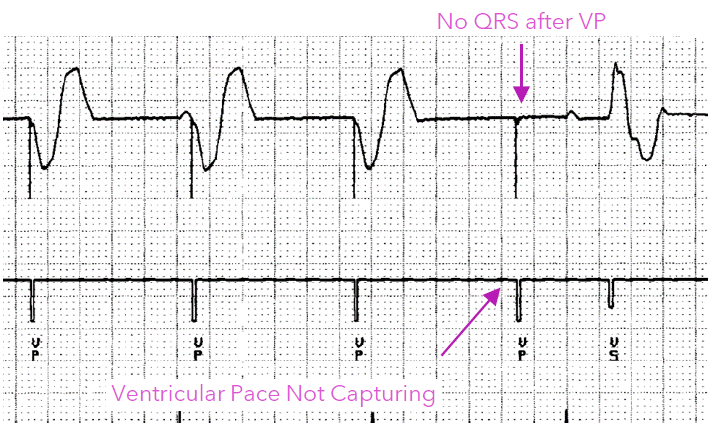
What are the 2 types of capture threshold testing?
1) Amplitude Threshold
2) Pulse Width Threshold
How does one run a amplitude threshold?
With this approach, the pulse width remains constant, but the amplitude (voltage) is decreased until loss of capture occurs. The threshold is the lowest amplitude value that consistently captured the myocardium.
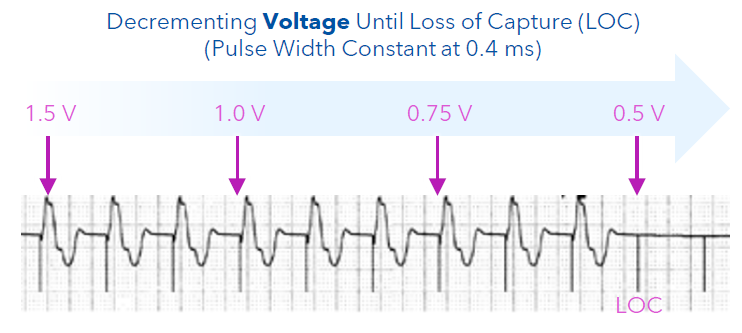
How does one run a pulse width threshold?
With this approach, the amplitude (voltage) remains constant, but the pulse width is shortened until loss of capture occurs. The threshold is the shortest pulse width duration that consistently captured the myocardium.
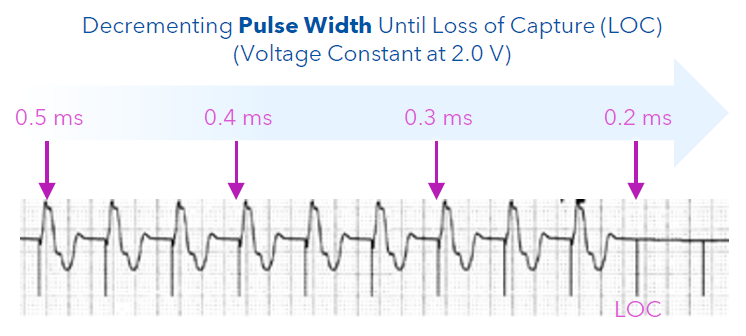
What are the acceptable threshold values?

What is the Strength-duration curve?
plots the lowest combinations of voltage and pulse width necessary for myocardial capture.
Any combination of pulse width and voltage on or above the strength duration curve will result in capture
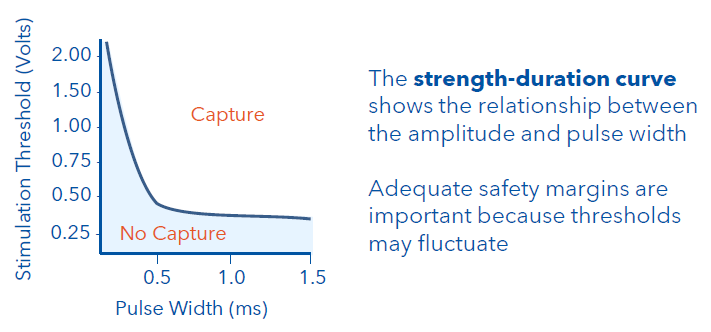
Why would a lead need more energy to capture the heart?
At implant, trauma to cardiac cells surrounding the electrode cause edema (swelling), and subsequent development of a fibrotic capsule.
The capsule requires more energy to capture the heart (there is usually no measurable effect on impedance).
Steroid-eluting leads help mitigate this inflammatory response.
What are the 3 phases of post-implant lead maturation?
1) Acute Phase - where thresholds are low immediately after implant.
2) Peaking Phase - which thresholds rise and reach their highest point. This phase usually occurs about a week after implant. This is followed by a decline in the threshold over the next 6 to 8 weeks as the tissue reaction subsides
3) Chronic Phase - which thresholds stabilize. During this phase, thresholds are typically higher than they were at implant, but lower than the peak threshold
What is the Wedensky effect?
However, if sub-threshold outputs are delivered first and then slowly raised until capture is achieved, that method of acquiring a capture threshold would produce a higher threshold value than would be obtained by lowering outputs until loss of capture.
What is the Rheobase?
the lowest voltage amplitude that captures the heart muscle at an infinitely long pulse duration
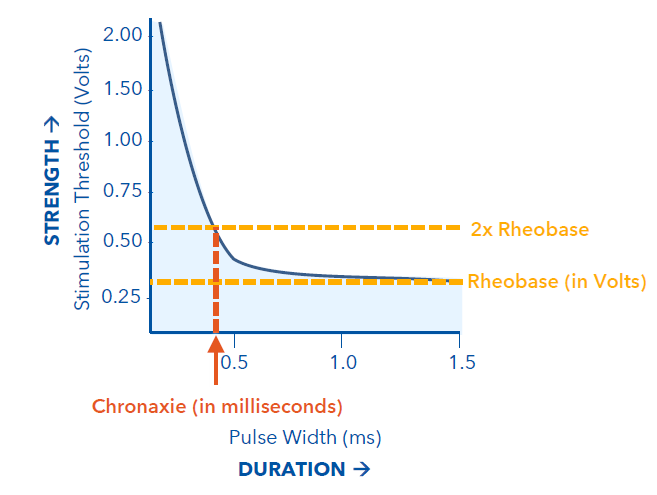
What is the Chronaxie?
double the rheobase and find the minimum pulse duration required to capture the heart
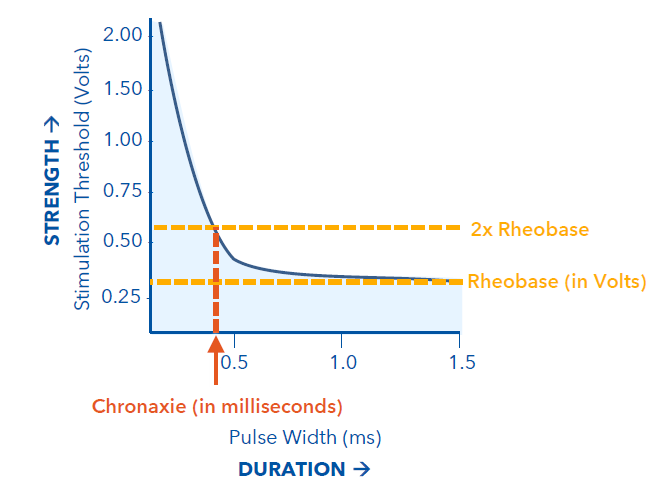
What is pacing output?
should be programmed high enough to reliably capture the heart, but not so high that the battery is prematurely depleted.
What are the primary and secondary goals of programming pacing output?
1) The primary goal of pacing output programming is patient safety through consistent myocardial capture.
2) A secondary goal is extending the service life of the battery when possible. Programming amplitudes to < 2.5 V is preferred as long as adequate safety margins are maintained.
What is the safety margin for amplitude threshold?
2x amplitude (voltage) safety margin on a chronic system is adequate
may be higher to accommodate for lead maturation process
What is the safety margin for pulse width threshold?
3x the pulse width threshold value.
A pulse width duration > 1.0 ms increases energy expenditure without significantly improving capture reliability.
Therefore, it is beneficial to program the pulse width to < 1.0 ms
What is the purpose of a sensing test?
pacing parameters are temporarily adjusted to uncover intrinsic P- and R-waves
If a patient does not have intrinsic P-waves or R-waves, there may be no sensed value after running a sensing test (T/F)
True
What are acceptable sensing values for leads?

Programming a device to be less sensitive means increasing the sensitivity value (T/F)
True - For example, a sensitivity value of 2.8 mV is less sensitive than a sensitivity value of 0.3 mV.

What is Fixed sensitivity?
The sensitivity setting remains constant.
What is a disadvantage with fixed sensitivity?
Fixed sensitivity could lead to the undersensing of smaller signals during arrhythmias such as atrial fibrillation or ventricular fibrillation
What does Auto-Adjusting sensitivity do?
automatically changes the sensing threshold after paced and sensed events to help reduce oversensing T-waves, far-field R-waves or pacing afterpotentials.
The device becomes less sensitive after a sensed or paced event, then gradually becomes more sensitive until reaching the programmed max sensitivity.
What is undersensing?
a device does not “see” an intrinsic depolarization and therefore does not respond appropriately
With undersensing, the device does not accurately see intrinsic depolarizations and may fail to inhibit pacing.
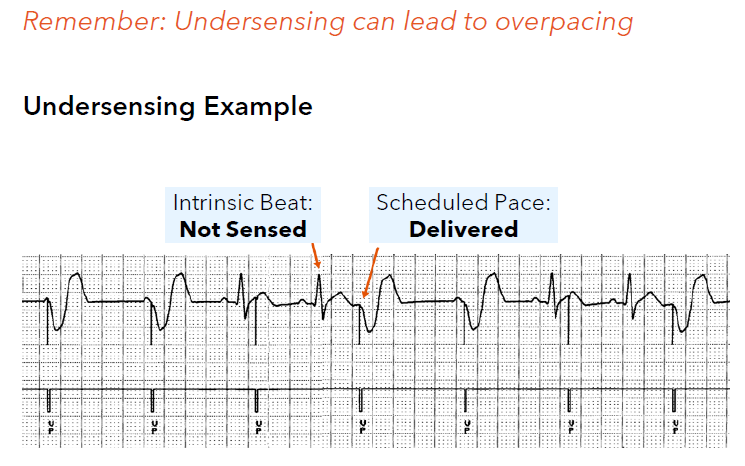
What phenomenon can under sensing lead to?
competitive pacing, where the device delivers pacing impulses at about the same time as (undersensed) intrinsic depolarizations occur.
In some cases, competitive pacing can trigger atrial or ventricular arrhythmias.
What is oversensing?
an electrical signal other than an intrinsic cardiac depolarization is detected
Oversensing may inappropriately withhold pacing due to oversensing-induced inhibition
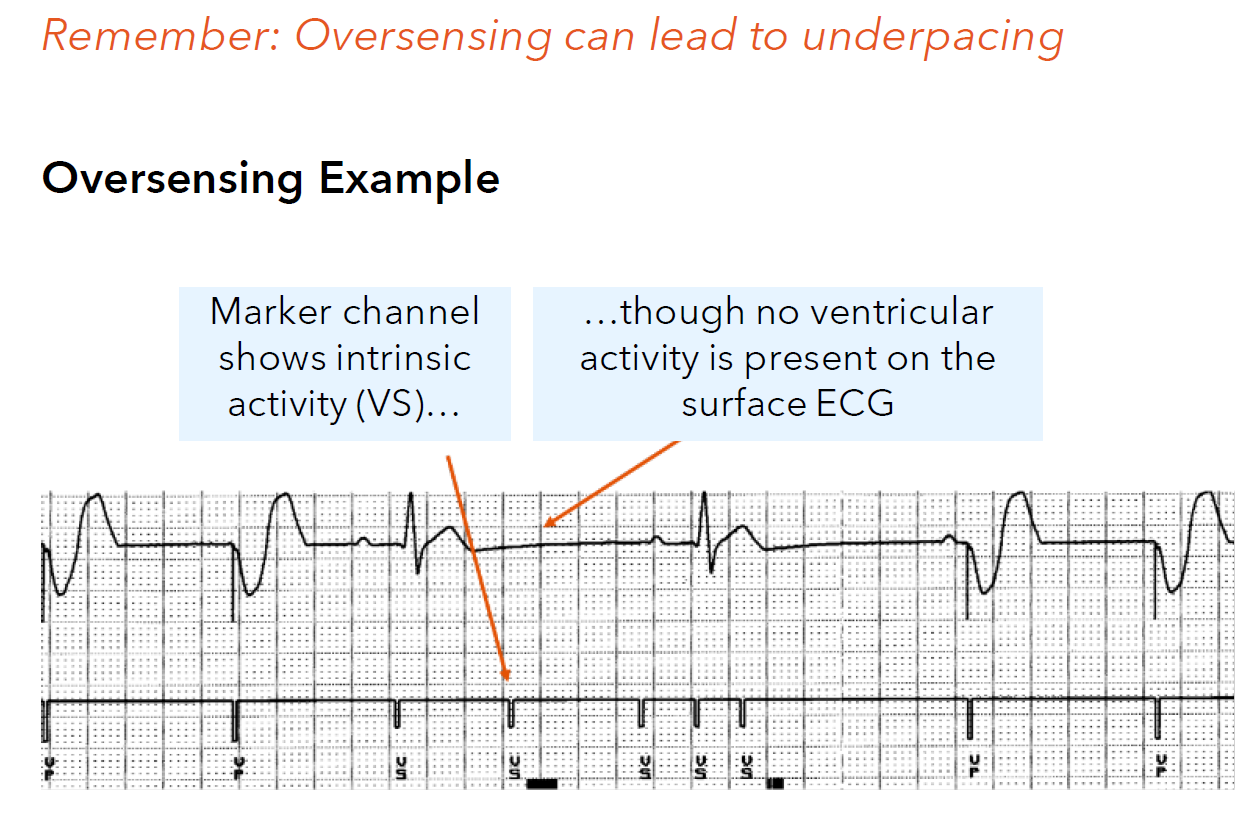
What are some unwanted signals that may be oversensed?
1) T-waves (would be misinterpreted as R-waves)
2) far-field events (R-waves sensed on the atrial channel, would be misinterpreted as P-waves)
3) skeletal muscle myopotentials (such as those from the pectoral muscle, which the device may misinterpret as P-waves or R-waves)
4) signals from the pacemaker (such as an atrial pacing spike sensed on the ventricular channel, known as “crosstalk”)
5) Electromagnetic Interference (EMI)
What are the 5 columns of NBG code?
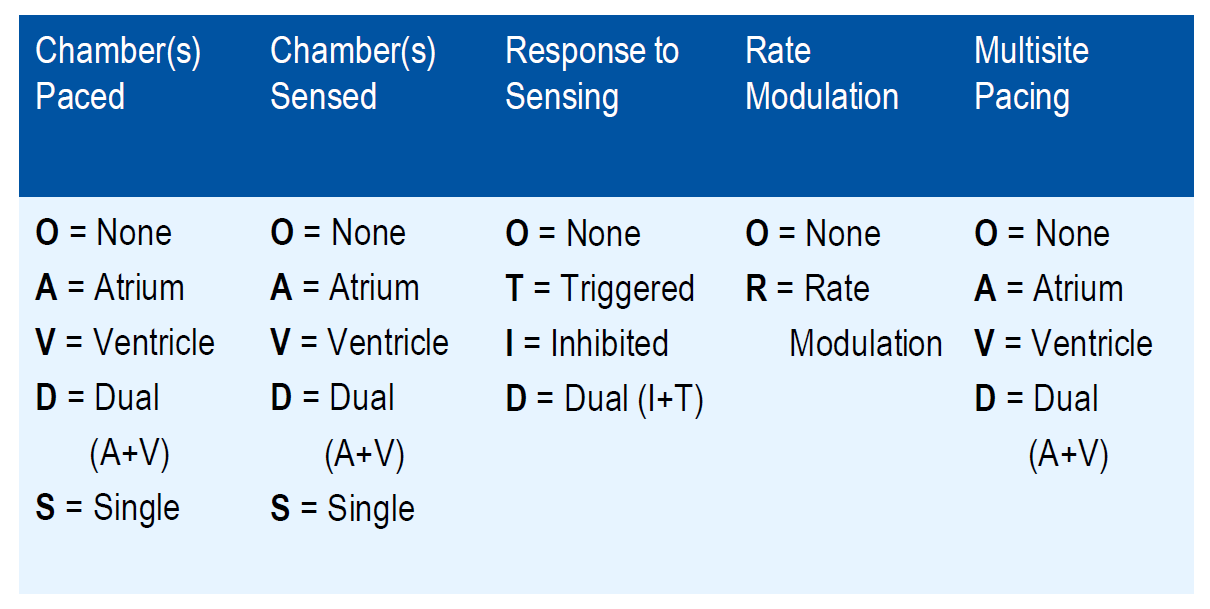
What are some Dual-Chamber Pacing Mode Examples?
1) DDD(R)
2) DDI(R)
What are some Single-Chamber Pacing Mode Examples?
1) VVI(R)
2) AAI(R)
What are some Single/Dual Chamber Asynchronous Mode Examples (often programmed during surgery or MRI)?
1) VOO
2) AOO
3) DOO
What is Rate Modulation (Rate Response)?
Rate-responsive pacing uses a sensor to detect patient motion and adapt the pacing rate to changes in physical activity.
Goals of rate-responsive pacing:
Recognize the need for a higher or lower heart rate to meet a patient’s metabolic demands
Real-time rate modulation based on a patient’s activity level
Adapt to changes in patient activity levels over time (achieved through automatic optimization).
How is Rate Response defined in the NBG Code?
When Rate Response is programmed ON, the fourth letter of the NBG code will be “R” (such as DDDR)
What is Chronotropic Incompetence?
the inability of the sinus node to increase the heart rate in response to physical activity
What is the Lower Rate?
which determines the device’s minimum pacing rate.
If this interval expires before an intrinsic depolarization is sensed, the device will deliver a paced event in that chamber
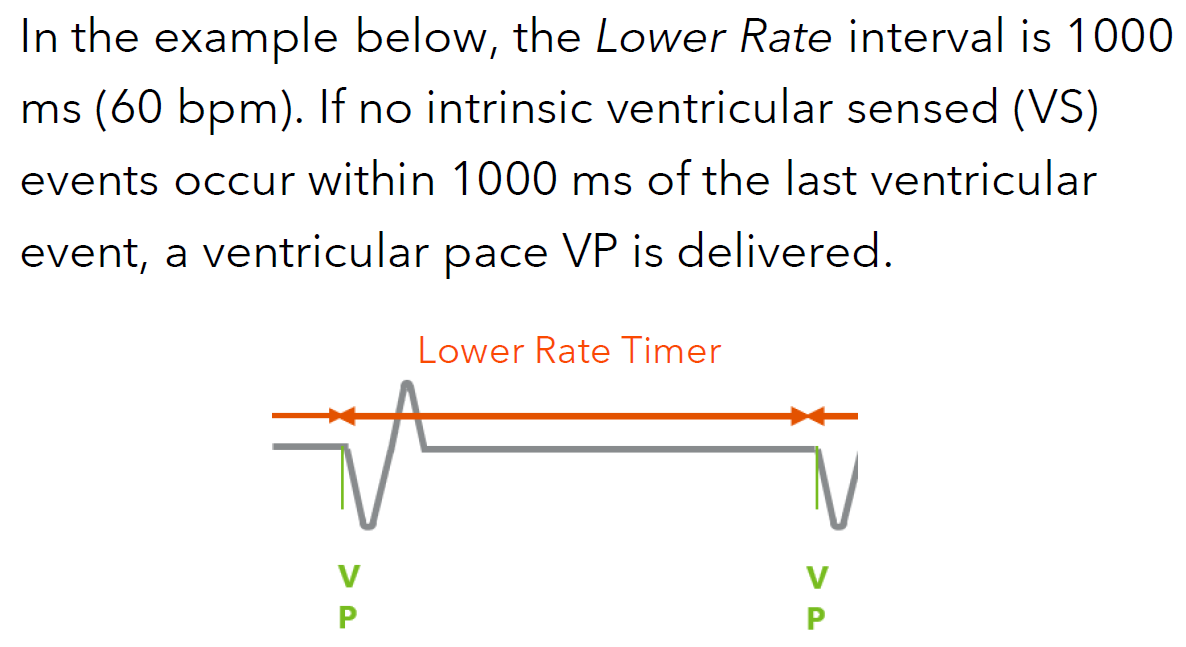
What is the Upper Sensor Rate?
limits how fast the sensor-driven pacing rate will pace the heart in the presence of vigorous physical activity.
The paced rate will not exceed the Upper Sensor Rate.
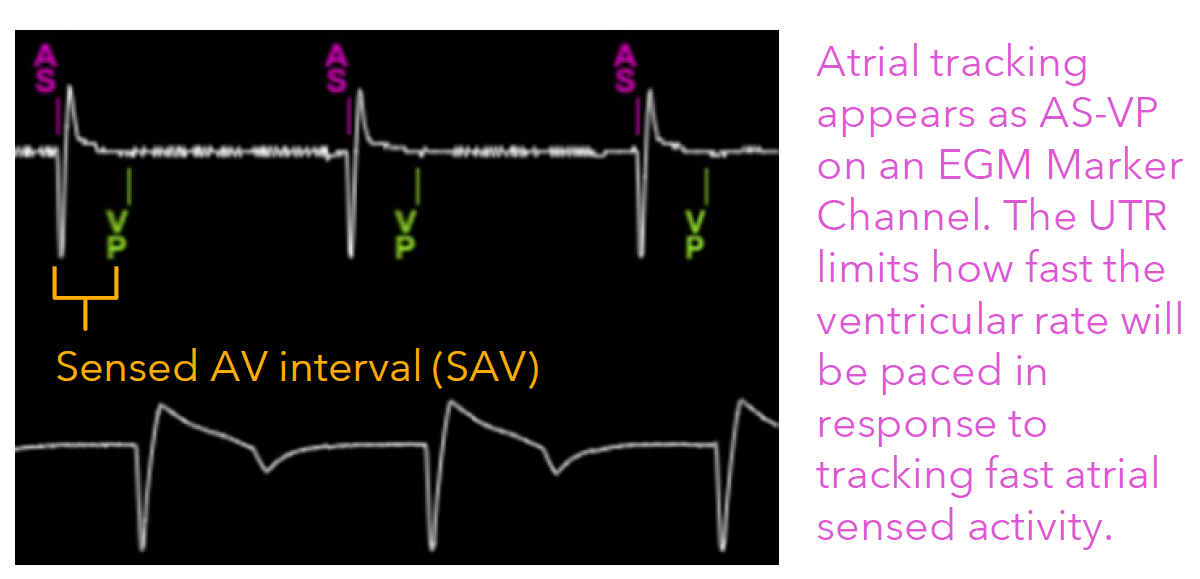
What is the Upper Tracking Rate?
limits how fast the device will pace the ventricle when tracking fast atrial sensed events (AS events)
What does Upper Tracking Rate safeguard against?
This safeguards against excessively fast ventricular pacing during fast atrial arrhythmias.
Tracking modes help ensure atrioventricular (AV) synchrony
What is the Lower Rate Interval for Dual Chamber Timing?
LR = A-V interval + V-A interval
What is the A-V Interval?
mimics the PR interval of the heart’s natural conduction system (i.e. AV Delay)
This delay allows for atrial kick and ventricular filling prior to ventricular systole and ensures A-V synchrony for patients with heart block
How does the A-V interval begin?
begins with an atrial event (atrial pace or atrial sense) and lasts for a programmed duration (typically 150 ms – 180 ms).
The device will deliver a ventricular pace when the A-V Interval expires unless an intrinsic ventricular event occurs within the A-V interval
What are the 2 types of programmable AV Delays in DDD mode?
1) Paced AV Delay (PAV): This interval begins with a paced atrial event (AP)
2) Sensed AV Delay (SAV): This interval begins with a sensed atrial event (AS)
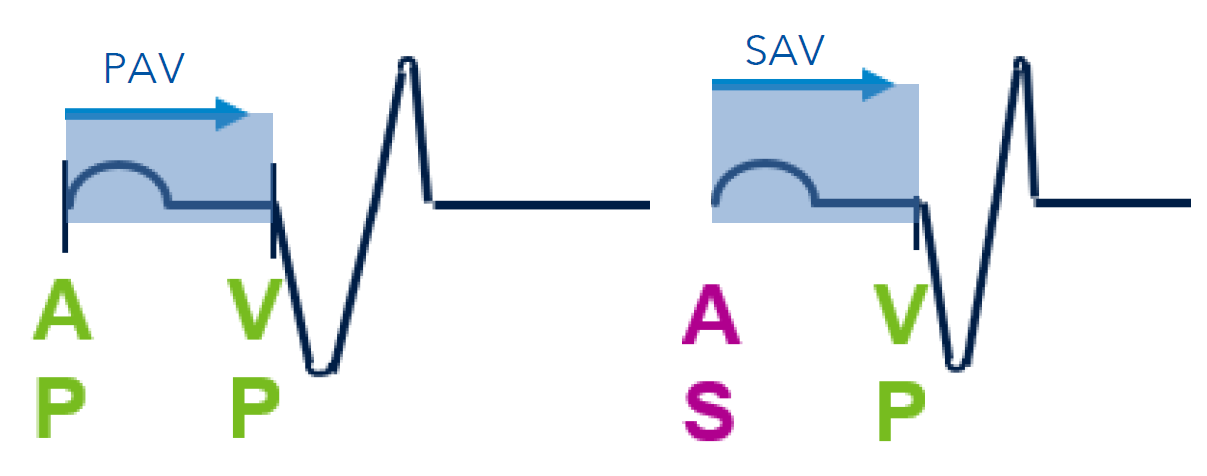
Which AV delay tends to be shorter?
Typically, the SAV is programmed 30 ms shorter than the PAV.
For example, if the PAV is 180 ms, the SAV will be 150 ms.
Intrinsic atrial events (AS) originate in the sinus node and travel down the heart’s fast conduction pathways. In contrast, an atrial pace (AP) depolarizes the atria more slowly, via cell-to-cell conduction.
What is the V-A Interval?
begins after a paced or sensed ventricular event.
The device delivers an atrial pace (AP) when the V-A Interval expires, unless an intrinsic atrial (AS) or ventricular (VS) event occurs within that interval.
V-A Interval defines when the device should pace the atrium (AP) after a ventricular event
What is Atrial-based Timing (A-A Timing)?
the A-A interval remains constant - Focuses on the interval between two atrial events (paced or sensed).
The V-A interval shortens or lengthens to maintain a constant A-A interval.
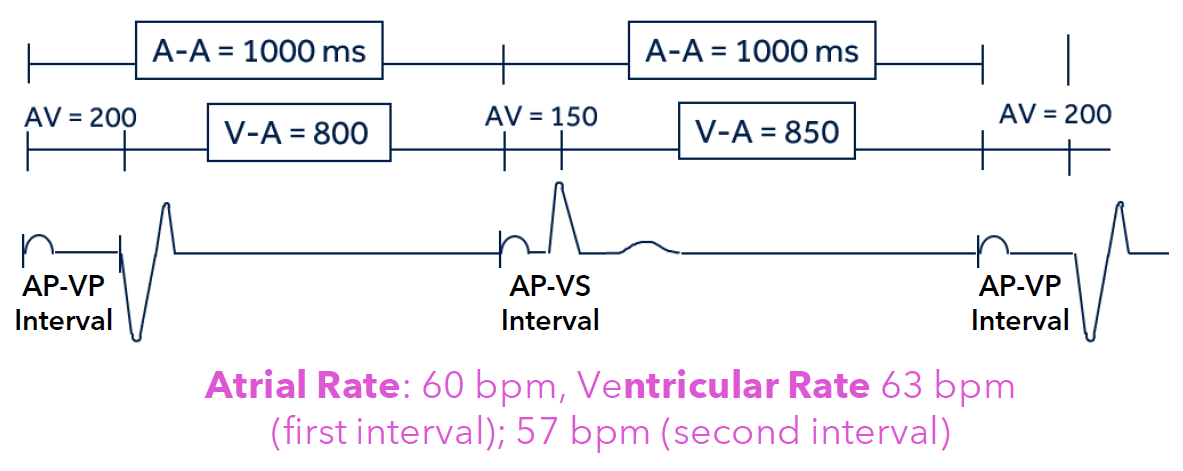
What is Ventricular-based Timing (V-V Timing)?
the V-V interval remains constant - Focuses on the interval between two ventricular events (V-A interval).
This leads to an A-A interval less than 1,000 ms
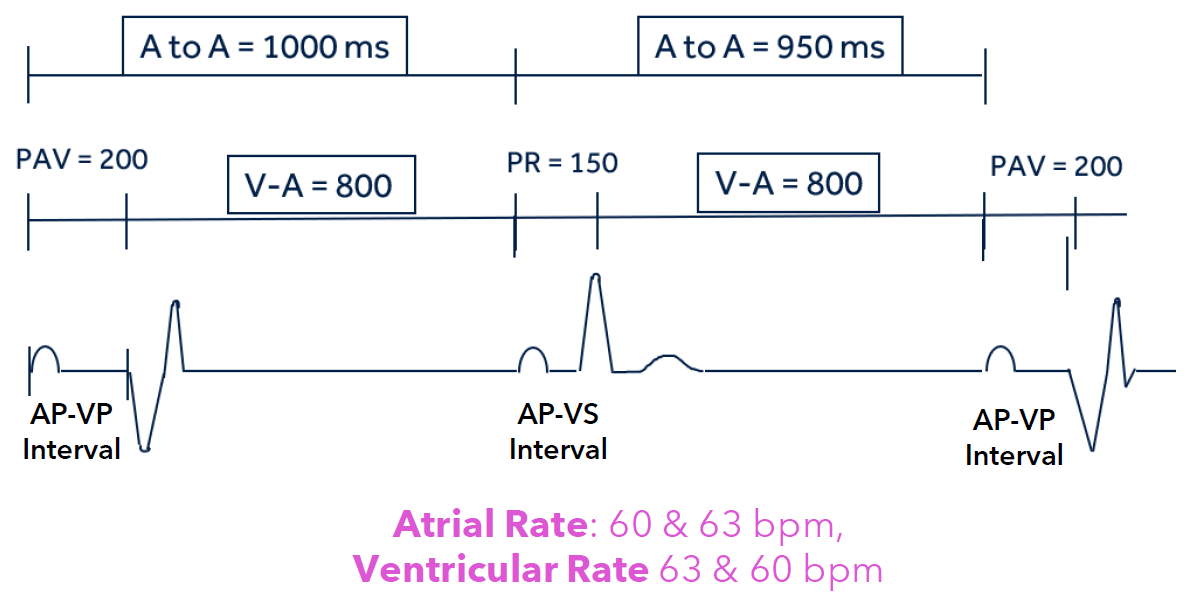
What is Hybrid or Modified A-A Timing?
In modified A-A timing, devices use atrial based timing unless PVCs occur
After a PVC, the interval from the VS to the next scheduled atrial pace is calculated by subtracting the Paced-AV interval (PAV) from the current A-A interval (either the Lower Rate or Sensor-Indicated Rate)
In other words, Uses atrial timing but modifies the reset rules based on ventricular events to provide a "smooth transition".
What are Blanking Periods?
help to prevent the device from sensing pacing pulses, post-pacing depolarization, T-waves, and double-sensing of the same event
What is Absolute blanking?
will not see or mark an event that falls into a blanking period
What is Partial blanking?
Some devices will “see” a signal during the blanking period and mark it as a blanked event
These blanked events may be used for detection of atrial arrhythmias but will not impact pacemaker timing
What is a Refractory period?
prevent inappropriately sensed signals (such as far-field R-waves, electrical noise, or retrograde conduction) from triggering certain pacemaker timing intervals
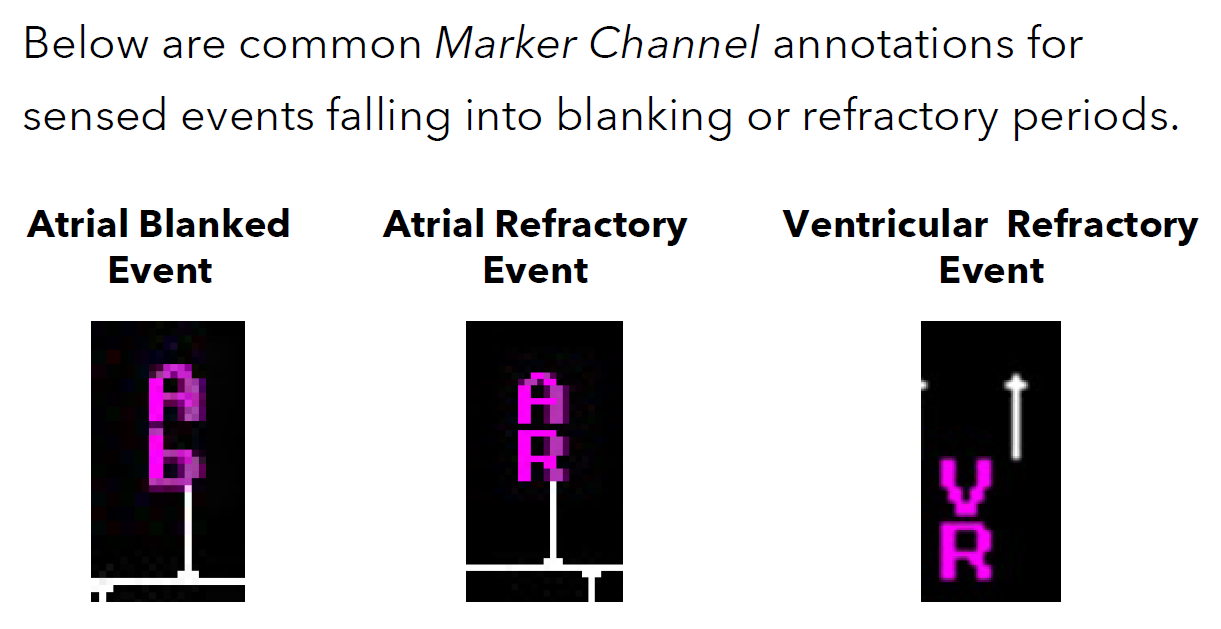
What is Atrial Blanking (AB)?
This interval is triggered by an atrial sensed (AS) or atrial paced (AP) event.
Atrial sensing is disabled during the atrial blanking period
What is Paced AV Delay (PAV)?
This interval is triggered by an atrial paced (AP) event.
A ventricular pace (VP) will be delivered at the end of the PAV interval unless a sensed ventricular event (VS) occurs first
What is Sensed AV Delay (SAV)?
This interval is triggered by an atrial sensed (AS) event.
A ventricular pace (VP) will be delivered at the end of the SAV interval unless a sensed ventricular event (VS) occurs first
What is Post-Ventricular Atrial Blanking (PVAB)?
This interval is triggered by a ventricular sensed (VS) or ventricular paced (VP) event
At times, small ventricular signals may appear on the atrial channel. These are called far-field R-waves (FFRW). The PVAB interval is designed to avoid sensing FFRWs on the atrial channel
What is Post-Ventricular Atrial Refractory Period (PVARP)?
This interval is triggered by a ventricular sensed (VS) or ventricular paced (VP) event
At times, premature atrial contractions (PACs) or retrograde P-waves occur on the atrial channel. The PVARP interval is designed to avoid tracking PACs or retrograde P-waves
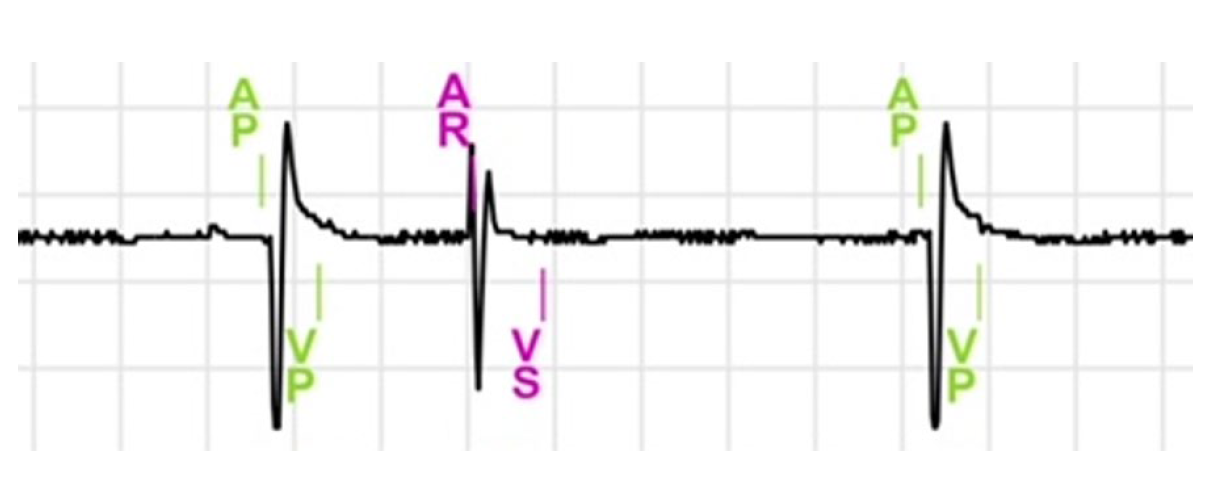
What are the main Intervals on the Atrial Channel?
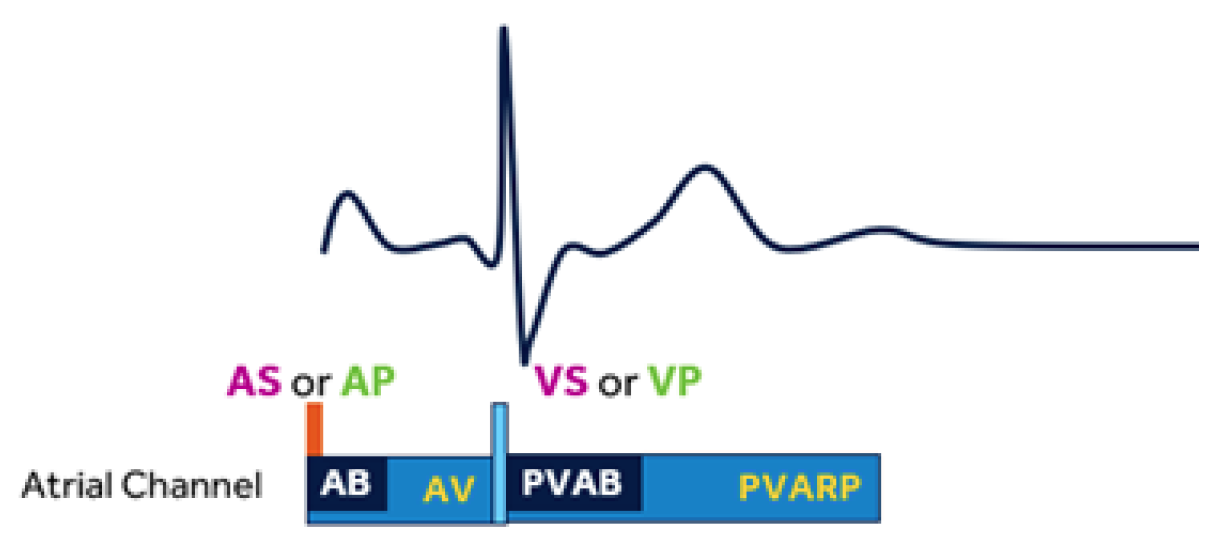
What is Post-Atrial Ventricular Blanking (PAVB)?
This interval is triggered by an atrial paced (AP) event.
The PAVB helps prevent ventricular sensing of far-field atrial signals or atrial pacing stimuli (crosstalk)
What is Ventricular Blanking?
This interval is triggered by a ventricular sensed (VS) or ventricular paced (VP) event.
Ventricular blanking helps prevent oversensing of the same ventricular event
What is Ventricular Refractory?
This interval is triggered by a ventricular sensed (VS) or ventricular paced (VP) event.
The ventricular refractory period helps prevent oversensing of the same ventricular event
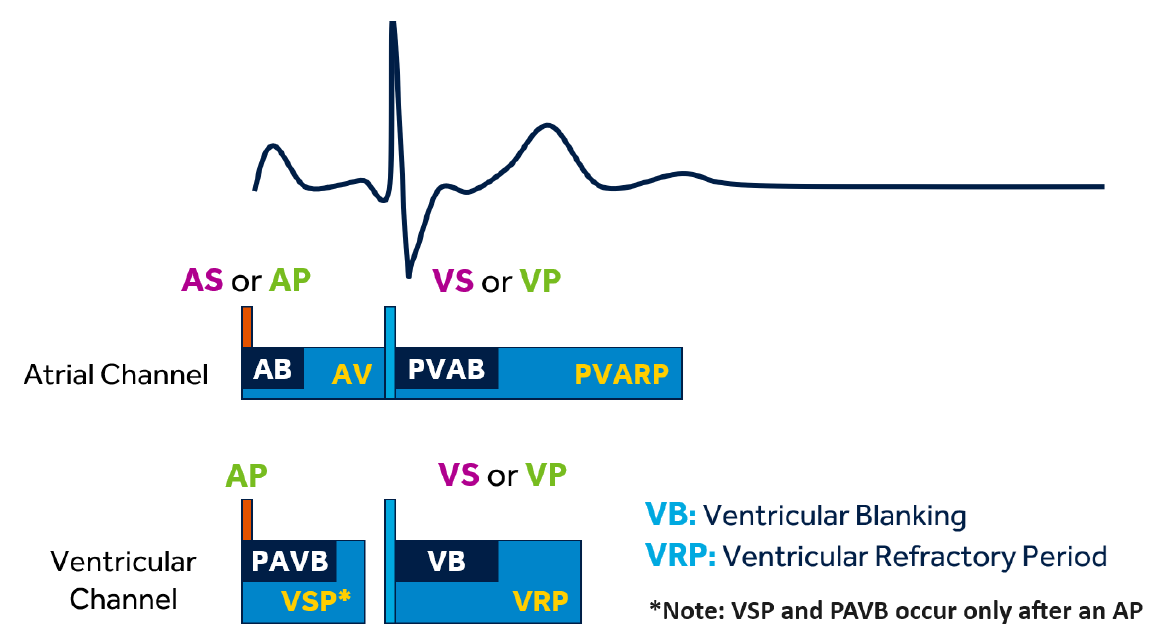
What is Ventricular Safety Pacing (VSP)?
This interval (typically 110 ms) is triggered by an atrial paced (AP) event
If a sensed ventricular event (VS) occurs during this period, a ventricular pace (VP) will be delivered at the end of the VSP window to prevent inappropriate inhibition of ventricular pacing
This feature is designed to detect non-physiologic (very short) AP-VS intervals, such as those caused by an atrial pacing impulse being oversensed on the ventricular channel (crosstalk)
What is the goal of Tracking?
Tracking is a common phenomenon for patients in complete heart block.
The goal is for every AS to be followed by a VP
If the sensed atrial rate increases above the Upper Tracking Rate (UTR), upper rate behaviors (pacemaker Wenckebach and 2:1 block) will occur (T/F)
True
What is Pacemaker Wenckebach Behavior?
The UTR is the maximum rate at which the device will pace the ventricles in response to atrial tracking.
Therefore, atrial rates above the UTR will exhibit a phenomenon of lengthening AS-VP intervals, until eventually atrial events fall into PVARP
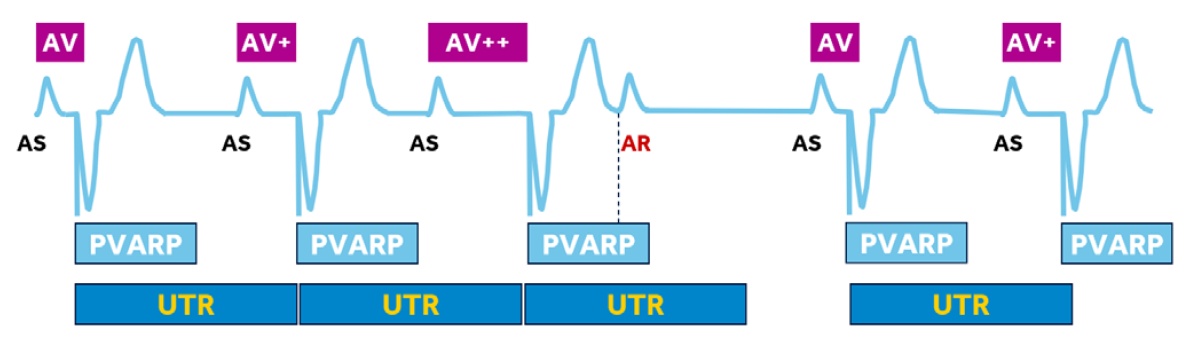
Pacemaker Wenckebach may progress to what if the atrial rate continues to rise?
2:1 block - In 2:1 block, every other atrial sensed (AS) event is tracked. The other half of atrial events fall into PVARP (AR) and do not start an SAV interval
Therefore, tracking is lost, and the ventricular rate becomes one-half of the atrial rate.
2:1 block during exercise is undesirable as the sudden reduction in ventricular pacing can reduce cardiac output
What causes 2:1 block to occur?
when the atrial rate reaches the Total Atrial Refractory Period (TARP) value
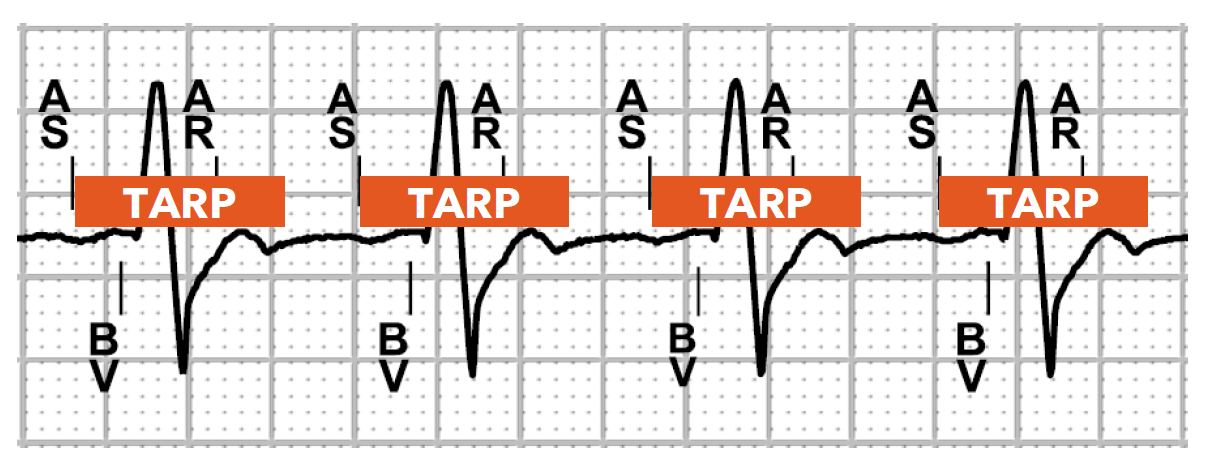
The TARP consists of what 2 intervals added together?
TARP = SAV+PVARP
What are 3 key features when programming Upper Rate Behavior?
1) The Upper Tracking Rate is appropriate for the patient’s age and activity level
2) The TARP (SAV+PVARP) value is at least 30 bpm faster than the Upper Tracking Rate (this is called the Wenckebach window)
3) Features like Rate Adaptive AV and Auto PVARP are optimized to promote tracking at faster atrial rates
What are the magnetic modes for Pacemakers and CRT-P?
includes temporary asynchronous pacing (such as DOO or VOO) and changes to the pacing rate (to 85 or 65 bpm)
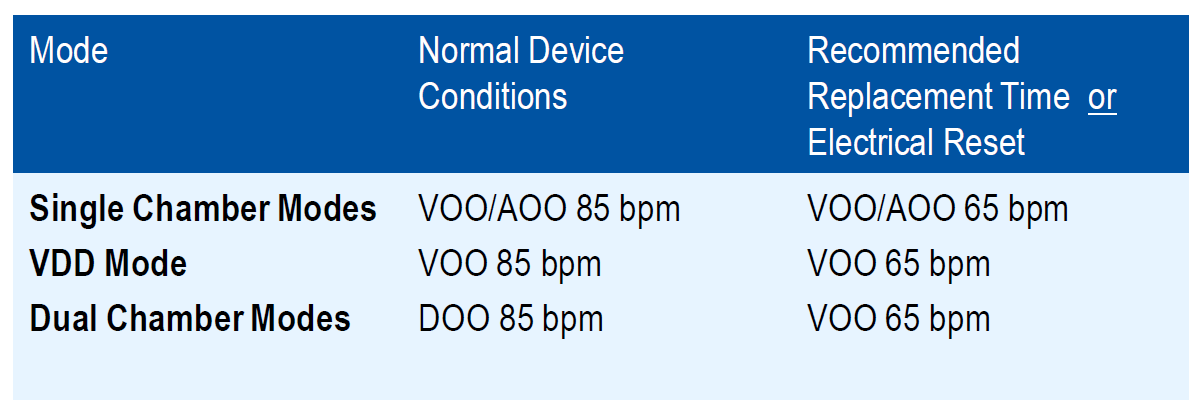

What is the typical magnet pacing rate?
85 bpm
A magnet produces pacing at 65 BPM means what?
the Recommended Replacement Time (RRT) interval has been reached or a full electrical reset has occurred
Removing the magnet allows the pacemaker to resume permanently programmed operation within how many seconds?
2 seconds
What is Rate Adaptive AV?
shortens AV intervals at elevated heart rates to maintain 1:1 tracking and AV synchrony for patients in heart block
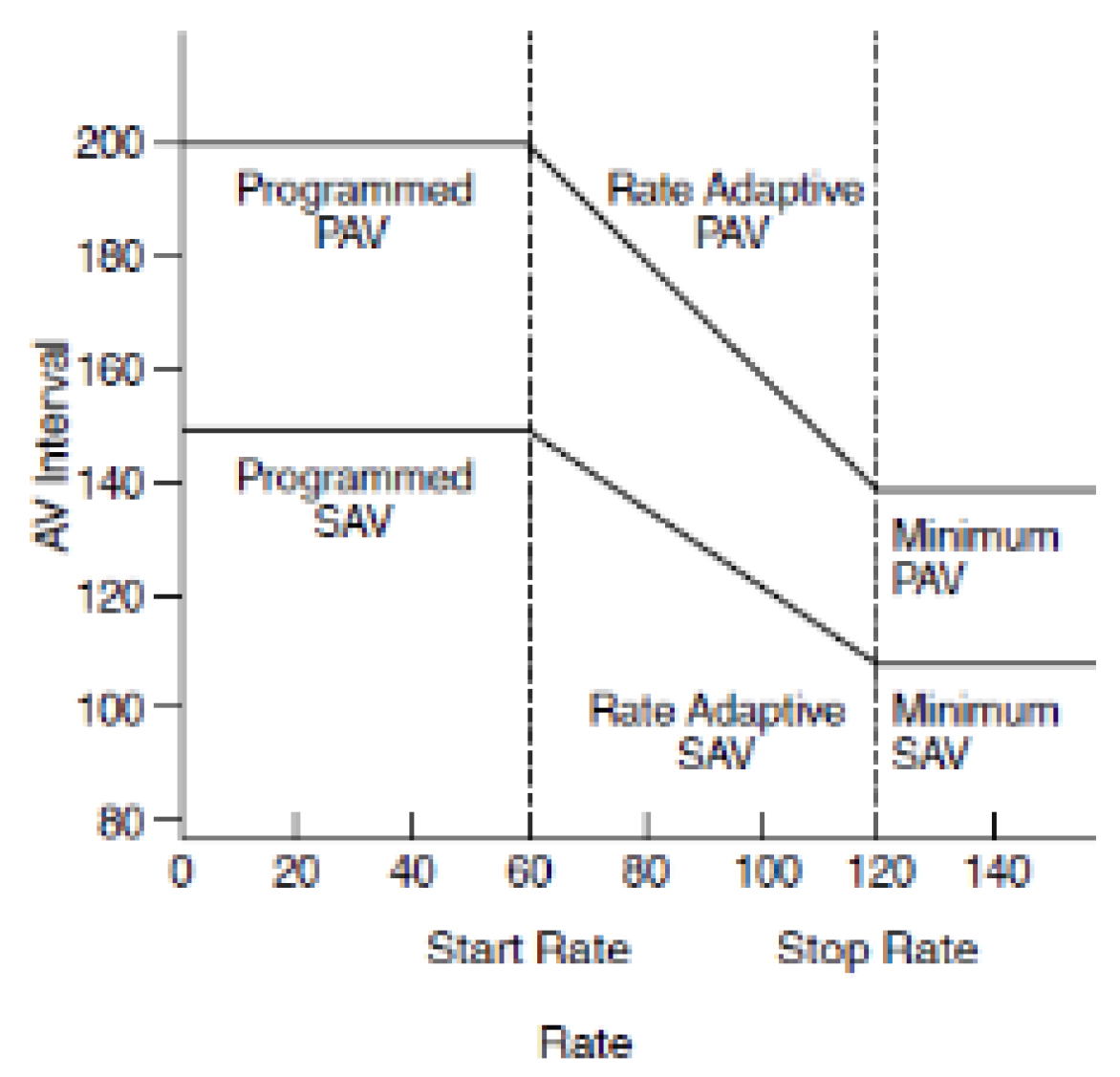
What is Auto PVARP?
lengthens or shortens PVARP based on a patient’s heart rate (allows 1:1 tracking of atrial events up to 30 bpm above the heart rate, or up to 100 bpm, whichever is greater)
When the heart rate is low, PVARP is longer to prevent PMT (pacemaker-mediated tachycardia). As the heart rate increases, PVARP shortens to maintain 1:1 tracking
What is Rate Response?
uses an activity sensor to measure patient movement, then converts that information into a target pacing rate (assesses Rate Response daily and adjusts as needed)
What is an Activity Sensor?
(accelerometer) in the device detects patient movement.
1) In the absence of motion, the patient will pace at their programmed Lower Rate (for example, 60 bpm).
2) For moderate levels of activity, the patient will pace at their Activities of Daily Living (ADL) rate (for example, 95 bpm).
3) With heavy activity, the patient will pace at rates closer to their Upper Sensor Rate (USR), (for example, 130 bpm).
What is Rate Profile Optimization?
automatically adjusts the patient’s rate response to ensure they spend appropriate amounts of time pacing in the ADL and exertional rate ranges
What helps provide information on Rate Response?
Rate Histograms
For example, if Rate Response was programmed to be more aggressive, the histograms will likely show that more time has been spent at faster pacing rates than before the programming change
What is Mode Switch?
occurs when the device detects the onset of an atrial tachyarrhythmia
Upon detection, the device switches to DDIR. It gradually adjusts the ventricular pacing rate from what it was during tracking, towards the device-determined Sensor Rate
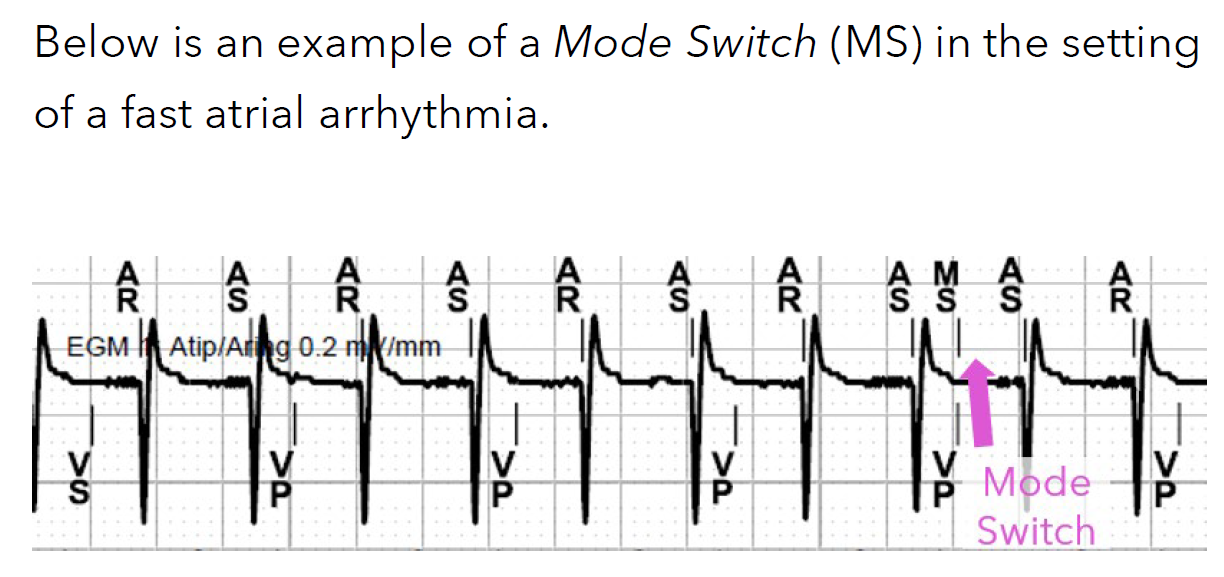
What does the Conducted AF Response do?
responds to irregularly conducted beats by sending pacing impulses at intervals that help regularize the ventricular rate
What is Capture Management?
measures pacing thresholds daily and can adjust pacing outputs to ensure appropriate safety margins
What is Managed Ventricular Pacing (MVP)?
promotes AV conduction by reducing unnecessary RV pacing.
1) AAI(R) mode during intact AV conduction
2) DDD(R) mode during AV block
3) Periodic conduction checks while operating in DDD(R) mode, with the ability to switch back to AAI(R) mode when AV conduction resumes
4) Backup ventricular pacing support for transient loss of AV conduction
What is Pacemaker-mediated tachycardia (PMT)?
a rapid, inappropriately paced rhythm that can occur in devices operating in atrial tracking modes (DDD or DDDR)]
PMT occurs when a device senses and tracks retrograde P-waves, resulting in an elevated ventricular pacing rate
These signals do not originate from the sinus node but may be sensed by the device (AS) and initiate a Sensed AV (SAV) interval
What is Pacemaker-mediated tachycardia (PMT) also known as?
Endless Loop Tachycardia
For Pacemaker-mediated tachycardia (PMT) to occur, a retrograde conduction pathway must be present (T/F)
True
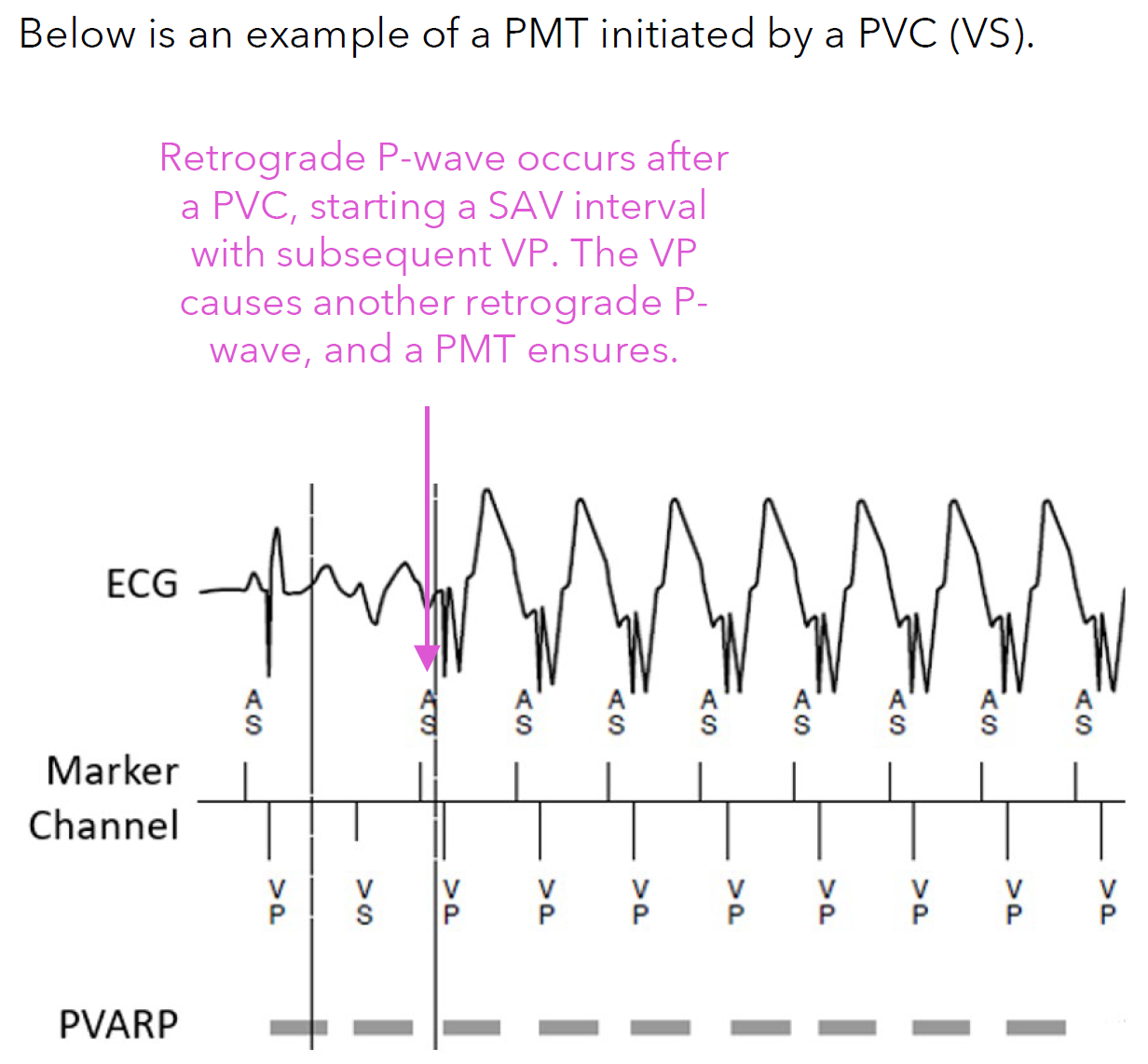
What is PMT Intervention?
extends the PVARP after detecting a PMT.
This interrupts the PMT by causing the subsequent atrial-sensed event to fall within the refractory period (PVARP) for one cycle
What is PVC Response?
extends the PVARP following a PVC to avoid tracking a retrograde P-wave and to prevent retrograde conduction from inhibiting an atrial pace
What is Ventricular Safety Pacing (VSP)?
detects crosstalk by monitoring for nonphysiologic ventricular sensed events after an atrial pace.
If detected, the device will respond by sending a ventricular pace (VP) shortly after the suspected ventricular oversensing
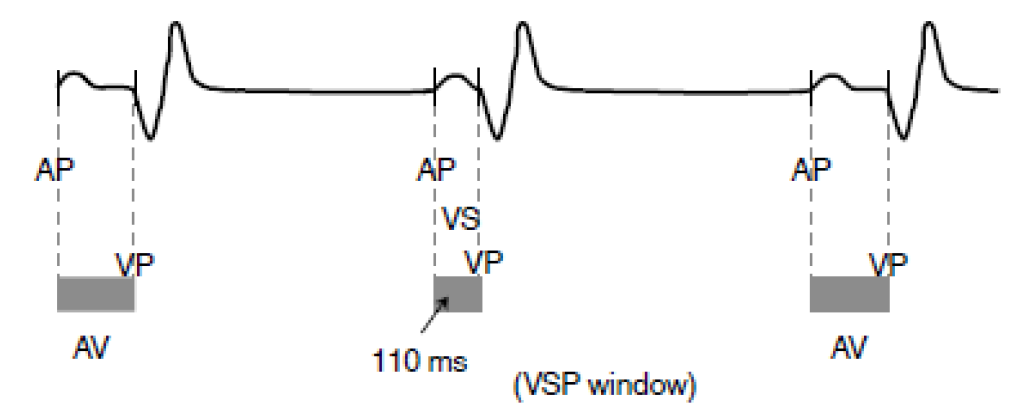
What is Non-Competitive Atrial Pacing (NCAP) do?
delays atrial pacing after a PAC that occurs during PVARP (AR)
An atrial tachycardia may be initiated if an atrial paced (AP) event occurs within the atrial vulnerable period after a PAC
What is Atrial Preference Pacing (APP)?
helps ensure atrial overdrive pacing when the patient is not experiencing an atrial tachyarrhythmia
The device responds to changes in the atrial rate by accelerating the pacing rate until reaching an atrial paced rhythm that is slightly faster than the intrinsic rate
What is Atrial Rate Stabilization (ARS)?
adapts the atrial pacing rate in response to a PAC to avoid long sinus pauses following short atrial intervals (short-long-short sequences that may cause the onset of some atrial tachycardias)
What is Post Mode Switch Overdrive Pacing (PMOP)?
This is designed to maintain an elevated atrial pacing rate after sinus rhythm has been restored
feature works with the Mode Switch feature to deliver overdrive atrial pacing for a period following the termination of an atrial tachyarrhythmia
What is Ventricular Rate Stabilization (VRS)?
designed to eliminate the long pause that commonly follows a PVC by increasing the pacing rate, then gradually adjusting it down to the current paced or intrinsic ventricular rate
What is AT/AF Detection?
When the device is in an atrial tracking mode (such as DDD), atrial tachyarrhythmias can cause inappropriately fast ventricular pacing.
Mode Switch allows the device to switch from a tracking mode to a non-tracking mode (DDIR) to avoid high-rate ventricular pacing
It does this by monitoring for the presence of fast atrial rates along with evidence that there are more atrial events than ventricular events