DEN 150 - Dental Specialties Proc & Exp Funct- FINAL EXAM
1/173
Earn XP
Description and Tags
Includes 54, 55, 56, 57, 58, 59, 60
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
174 Terms
What is the main focus of oral and maxillofacial surgery?
It involves the diagnosis and surgical treatment of diseases, injuries, and defects in the oral and maxillofacial region.
What are the indications for maxillofacial surgery?
Indications include extractions of decayed or impacted teeth, treatment of jaw fractures, reconstructive surgery, and more.
What advanced training does an oral and maxillofacial surgeon (OMFS) receive?
An OMFS completes 4 to 6 years of postgraduate training in a hospital residency after dental school.
Why is the chain of asepsis important during surgery?
It helps prevent infection by ensuring that sterile techniques are followed during the surgical procedure.
What is the role of a surgical assistant in oral surgery?
The surgical assistant must have knowledge in patient assessment, surgical asepsis, and handling specialized instruments.
What are some specialized instruments used in oral surgery?
Instruments include surgical curettes, scalpels, hemostats, and various types of forceps.
What should be included in patient preparation before surgery?
Update medical history, confirm premedication intake, check vital signs, and position the patient appropriately.
What postoperative care instructions are important for patients?
Patients should be instructed on bleeding control, swelling management, diet, and when to return for suture removal.
What is alveolitis and how can it be prevented?
Alveolitis, or dry socket, can occur due to improper care of the extraction site and can be prevented by following postoperative instructions.
What types of sutures are commonly used in oral surgery?
Absorbable sutures such as plain catgut, chromic catgut, and synthetic materials like Vicryl; nonabsorbable sutures include silk and nylon.
Orthodontic Treatment
Provides the following types of treatment:
Straightens teeth that are rotated, tilted, or otherwise improperly aligned
Corrects crowded or unevenly spaced teeth
Corrects bite problems
Aligns the upper and lower jaws
Benefits of Orthodontic Treatment
Psychosocial problems
Severe malocclusion and dental facial deformities can be a social handicap
Oral malfunction
Malocclusion can compromise all aspects of oral function
Dental disease
Malocclusion can contribute to dental decay and periodontal disease
The Orthodontic Assistant
Depending on the expanded functions that are legally permitted in the state in which you practice, the clinical assistant can participate in various procedures that involve
diagnostic records
preliminary appointments
adjustment visits
The Orthodontic Office
The orthodontic office is designed to accommodate many patients at a time
The patient care area of the office can be sectioned off to serve three functions
Obtain records and create a more private setting
Take radiographic images
Provide clinical care at all stages of treatment
Open Bay concept
In larger practices, it is common to see up to 30 patients a day
Environmental Causes of Malocclusion
Injuries can occur at birth in two major categories
Fetal molding, when an arm or leg of the fetus is pressed against another part of the body
Trauma during birth, such as an injury to the jaw
Injury throughout life
Dental trauma can lead to the development of malocclusion in three ways
Damage to permanent tooth buds when an injury to primary teeth has occurred
Movement of a tooth or teeth as a result of premature loss of a primary tooth
Direct injury to permanent teeth
Habits
Tongue thrusting
Tongue-thrust swallowing
Thumb and finger sucking (beyond the age of 5 will affect facial structure development and growth.
Bruxism (excessive grinding of the teeth or clenching of the jaw)
Mouth breathing
Malocclusion
Angle’s classification
Class I malocclusion
Class II malocclusion
Class III malocclusion
Class I Malocclusion
For class I malocclusion, there is a normal relationship with the molars, but the anterior teeth will be out of alignment with malpositioned or rotated teeth
The mesiobuccal cusp of the maxillary first molar occludes with the mesiobuccal groove of the mandibular first molar.
Class II Malocclusion
This condition is also referred to as distoclusion
The body of the mandible is in an abnormal distal relationship to the maxilla
The mesiobuccal cusp of the maxillary first molar occludes in the interdental space between the mandibular second premolar and the mesial cusp of the mandibular first molar
Class III Malocclusion
This condition is also referred to as mesioclusion
The body of the mandible is in an abnormal mesial (outward appearance) relationship to the maxilla
Class III malocclusion causes the mandibular anterior teeth to protrude in front of the maxillary anterior teeth
Malaligned Teeth
Crowding
In this, the most common contributor to malocclusion, one or many teeth are involved in misplacement
Overjet
An excessive protrusion of the maxillary incisors results in space or distance between the facial surfaces of the mandibular incisors and the lingual surface of the maxillary incisors
Overbite
This is an increased vertical overlap of the maxillary incisors
Open bite
A lack of vertical overlap of the maxillary incisors results in an opening of the anterior teeth when occluded
Cross-bite
A tooth is not properly aligned with its opposing tooth
Photographs
Two standard extraoral photographs are taken as follows:
. The frontal view
. A profile view
Three standard intraoral photographs are also routinely taken
. Full direct view
. Maxillary occlusal view
. Right buccal view
Craniofacial Images
Panoramic projection
Used to view the eruption process of the primary and permanent teeth as well as to evaluate the amount of space available for the eruption process
Cephalometric projection (Most Commonly Used)
Extraoral radiographs make it possible to evaluate the anatomic basis for malocclusion, as well as the skull, bones, and soft tissue
Computed Tomography (CT)
Orthodontist can gain specific information like:
Accurate measurements
Localization of impacted teeth
Asymmetry
Periodontal structures
Placement sites for anchorage devices
Views of condylar joint and TMJ
Specialized Instruments and Accessories
Intraoral instruments
Orthodontic scaler
Used in bracket placement, removal of elastomeric rings, and removal of excess cement or bonding material
Ligature director
Used to guide the elastic or wire ligature tie around the bracket and to tuck the twisted and cut ligature tie under the arch wire
Band plugger
Used to help seat a molar band for a fixed appliance
Bite stick
Used to help seat a molar band for a fixed appliance
Bracket placement tweezers
Used to carry and place the bonded bracket on the tooth
Bird‑beak pliers
Used to form and bend wires
Weingart utility pliers
Used in placing arch wires
Contouring pliers
Used in fitting bands
Three‑prong pliers
Used to close and adjust clasps
Posterior band remover pliers
Used to remove bands
Wire-bending pliers
Used to hold, bend, and adjust arch wires to create movement
Pin and ligature cutter
Cuts the ligature wire for removal
Ligature‑tying pliers
Used for ease in ligature tying
Howe (110) pliers
Allow for placement and removal of, and the making of adjustment bends in, the arch wire
Sequence of Appointments for Fixed Appliances
1.Placement of separators
2.Cementation of molar bands
3.Bonding of brackets
4.Insertion of arch wire and tying in with ligature ties or elastomeric ties
5.Adjustment checks
6.Removal of appliance
7.Retention of teeth
Auxiliary Attachments
Headgear tubes
These round tubes, routinely placed on maxillary first molar bands, are used for the insertion of the inner bow of a facebow appliance
Edgewise tubes
Rectangular tubes are placed on the buccal surfaces of the upper and lower first molar bands to receive the arch wire
Labial hooks
Located on the facial surfaces of the first and second molar bands for both arches, these hooks hold the interarch elastics
Lingual arch attachment
This button or bracket, located on the lingual portion of the bands, stabilizes the arch and reinforces anchorage and tooth movement
Types of Arch Wires
Nickel titanium (NiTi)
For movement (initial stage) because of its flexibility
Stainless steel wire
Stiffer and stronger (gives more force and better stability to control the teeth)
Beta titanium (TMA)
Provides a combination of strength, flexibility, and memory
Optiflex
Used for light force and its esthetics
Shapes of Arch Wires
Round wires
Used in the initial and intermediate stages of treatment to correct crowding, level the arch, open a bite, and close spaces
Square or rectangular wires
Used during the final stages of treatment to position the crown and root in the correct maxillary and mandibular relationship
Ligating the Arch Wire
Ligature ties
Elastic ligature tie or stainless steel wire ligature is used to “tie” in arch wires
Kobayashi hooks
Ligature ties that have been spot-welded at the tip form hooks for the attachment of elastics
Power Products
Elastic chain ties
These ties, continuous “Os” that form a chain, are used to close space between teeth or to correct rotated teeth
Elastics
Commonly referred to as rubber bands, elastics are placed from one tooth to another in the same arch or from one tooth to another tooth in the opposing arch
Elastics help close spaces between teeth and correct occlusal relationships
Elastic thread
A type of tubing used to close space or aid in the eruption of impacted teeth
Comfort tubing
Aids in patient comfort by covering an arch wire that may be causing discomfort
Retention
Retention is necessary to:
Allow gingival and periodontal tissues the required time for reorganization
Support the teeth that are in an unstable position
Control changes caused by growth
Different types of appliances for retention include:
Orthodontic positioner
Hawley retainer
Lingual retainer
Lingual Retainer
A fixed lingual wire bonded canine-to-canine on the lingual surfaces
This provides lower incisor position during late growth
The fabrication consists of light steel wiring that is bent so that it rests against the flat portion of the lingual surface of the incisors with a long loop over the cingulum of the canines
What is pediatric dentistry?
A specialized area of dentistry focused on the care of children from birth through adolescence.
How long does a pediatric dentist continue their education after dental school?
An additional 2 to 3 years.
What is the role of a pediatric dental assistant?
To provide preventive procedures and assist in the clinical practice environment in pediatric dentistry.
What is an important characteristic of a pediatric dental office's environment?
Cheerfulness with a nonthreatening décor.
What are Erikson’s stages of development related to trust?
Learning basic trust occurs during infancy when a child is nurtured and develops security.
What is an important factor to consider when managing child behavior in a dental office?
Always consider the child’s point of view and practice honesty.
What are the common IQ ranges for mild intellectual disability?
IQs ranging from 50 to 70.
Describe Down Syndrome.
A chromosomal aberration resulting in abnormal physical characteristics and potentially mild to moderate mental impairment.
What is the main challenge of treating patients with autism?
They may exhibit behavioral problems and management difficulties.
What should be reviewed in preventive dentistry for children?
Oral hygiene, fluoride intake, and dietary nutrients.
What type of procedures might a pediatric dentist perform?
Restorative, endodontic, and prosthodontic procedures.
What happens in a traumatic intrusion injury?
The tooth is driven into the alveolus with only a portion of the crown visible.
What should be done if a tooth is avulsed?
Recover the tooth immediately, wrap it in moistened gauze, and go to the dentist.
What signs might indicate child abuse in a dental setting?
Injuries in various stages of healing, chipped teeth, and inconsistent injuries relative to explanations.
What information is required when reporting suspected child abuse?
Details about the child and adult custodian, descriptions of abuse or neglect, and any evidence of previous injuries.
What is the purpose of dental sealants?
To prevent dental caries in the pits and fissures of teeth.
How do dental sealants work?
Sealants act as a physical barrier that prevents bacteria and food particles from entering pits and fissures.
What age group is indicated for sealant placement?
Patients between the ages of 6 to 15 years.
What are contraindications for sealant placement?
Lack of pits and fissures, apparent occlusal or interproximal decay, insufficient eruption, soon-to-be-lost primary teeth, and poor patient cooperation.
What are the two types of polymerization methods for sealants?
Self-cured materials and light-cured materials.
What is an advantage of light-cured sealants?
No mixing required and allows the operator to place and cure the material at their discretion.
Why is etching important before sealant application?
Etching with phosphoric acid helps achieve retention of the sealant.
What can lead to the failure of sealants?
Moisture contamination and inadequate etching.
What is a potential benefit of sealants that release fluoride?
They create a fluoride-rich layer at the base of the sealed groove.
What precautions should be taken when using etching agents?
Wear protective eyewear and avoid contact with skin, eyes, and oral soft tissue.
How long do most sealant products last at room temperature?
Shelf lives range from 18 to 36 months.
What should be checked during recall visits regarding sealants?
To ensure that the sealant material has not been partially or totally lost.
Coronal Polishing
A procedure that removes plaque and stains from the coronal surfaces of the teeth.
Selective Polishing
A procedure in which only stained teeth or surfaces are polished to avoid removing surface enamel.
Extrinsic Stains
Stains on the exterior of the tooth caused by environmental sources, which may be removed.
Intrinsic Stains
Stains that cannot be removed as they have become incorporated into the structure of the tooth.
Dental Abrasives
Polishing materials used to remove stains and polish teeth, available in extra-coarse, coarse, medium, fine, and extra-fine.
Fulcrum
A point of support on which the handpiece is stabilized to allow movement during polishing.
Prophy Angle
A reusable or disposable attachment that holds the polishing cup or brush for coronal polishing.
Fluoride Application
A treatment performed after polishing, historically thought to be enhanced by prior polishing.
Rheostat
A foot pedal used to control the speed of the handpiece during dental procedures.
Patient Preparation
The process of checking medical history, seating the patient, and explaining the polishing procedure.
What can the dental assistant assist with during periodontal procedures?
periodontal charting
periodontal surgeries
provide home care instructions to the patient
The Periodontal Practice
Patients are referred by the general dentist or dental hygienist for treatment of a periodontal condition
*After the periodontal treatment, the patient will return to the general dentist for routine dental care
*Frequently, periodontal patients will alternate periodontal maintenance (cleaning) appointments between the periodontist’s office and the general dentist’s office
The Periodontal Examination
A periodontal examination includes:
Medical and dental history
Radiographic evaluations
Examination of the teeth
Examination of the oral tissues
Supporting structures
Periodontal charting
Periodontal charting includes pocket readings, furcation's,*tooth mobility, exudate (pus), and gingival recession
Medical and Dental History
Systemic diseases such as acquired immunodeficiency syndrome, human immunodeficiency virus infection, and diabetes can decrease resistance of the tissue to infection
Dental history used to gather information about conditions that could indicate periodontal disease
For example, patients with periodontal disease often complain
* of bleeding gums
* loose teeth
* bad taste in the mouth
Dental Examination
Mobility
It is normal for teeth to have a slight amount of mobility (tooth movement) because of the cushioning effect of the periodontal membranes
Excessive mobility important sign of periodontal disease
Oral Tissues and Supporting Structures
The periodontal examination includes:
Assessment of the amounts of plaque and calculus
Changes in gingival health and bleeding
Assessment of the level of bone
Detection of periodontal pockets
Supporting Structures
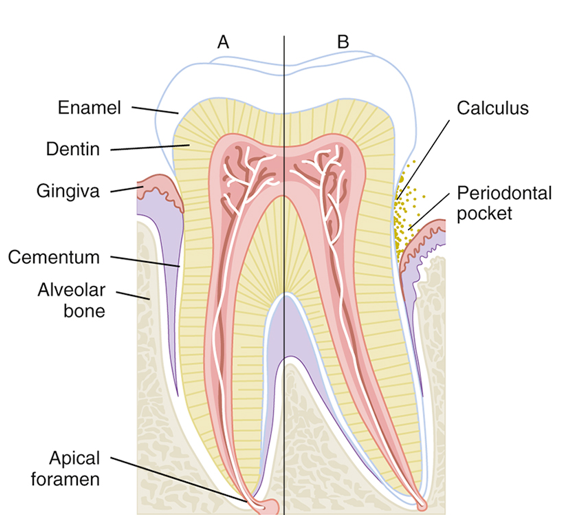
Periodontal Probing
A periodontal pocket results when the gingival sulcus becomes deeper than normal (<3 mm)
Periodontal probing measures how much epithelial attachment has been lost to disease
The greater the depth of the periodontal pocket results in
* the greater the loss of epithelial attachment
*the greater loss of bone
*more serious the periodontal disease
Periodontal pockets are very difficult, and sometimes impossible, for the patient to clean
Early Signs of Periodontal Disease
Changes in the gingiva (color, size, shape, texture)
Gingival inflammation
Gingival bleeding
Evidence of exudates
Development of periodontal pockets
Bleeding Index
The severity of gingival inflammation can be measured by the bleeding index
Several different systems of recording bleeding scores are used
Occlusal Adjustment
Patient’s bite is evaluated for areas of unequal pressure
Occlusal trauma can result if excessive biting pressure is noted in a specific area
Occlusal adjustment: Procedure that adjusts patient’s bite so that occlusal forces are equally distributed over all the teeth
Radiographic Analysis
Radiographs are a valuable aid for evaluating periodontal disease
Bitewing radiograph: Can accurately depict bone height along the root surface
Vertical bitewing radiographs are excellent for determining the extent of crestal bone loss
Periodontal Instruments
Periodontal therapy requires the use of specialized instruments
*to remove calculus,
*smooth root surfaces
* measure periodontal pockets,
*perform periodontal surgery
In general, the dentist or registered dental hygienist who uses these instruments takes responsibility for maintaining their sharpness
Periodontal Probes
Used to locate and measure the depth of periodontal pockets
On some types of probes, the tip is color-coded to make the measurements easier to read
Periodontal probe
* tapered to fit into the gingival sulcus
* shape is blunt or rounded tip
Six measurements are taken and recorded for each tooth
Scalers and Files
Sickle scalers are used primarily to remove large deposits of supragingival calculus
Chisel scalers are used to remove supragingival calculus in the contact area of anterior teeth
The blade on the chisel scaler is curved slightly to adapt to the tooth surfaces
Hoe Scalers are used to remove heavy supragingival calculus
Hoe Scalers are most effective when used on buccal and lingual surfaces of the posterior teeth
Curettes
Curettes are used to remove
*subgingival calculus,
*smooth rough root surfaces (root planning),
*remove the diseased soft tissue lining of the periodontal pocket (soft tissue curettage)
A curette has a rounded end, unlike a scaler, which has a pointed end
Two basic designs of curettes
Universal
Gracey
Types of Curettes
Universal curettes are designed so that one instrument can be used on all tooth surfaces
Gracey curettes have only one cutting edge and are area-specific
They are designed for use on specific tooth surfaces (mesial or distal)
Treatment of the entire dentition requires the use of several curettes
Pocket Markers
These perforations, which are referred to as bleeding points, are used to outline the area for an incision on the gingivae
Ultrasonic Scaler
Allows for rapid calculus removal and reduces hand fatigue for the operator
Works by converting very-high-frequency sound waves into mechanical energy in the form of very rapid vibrations
A spray of water at the tip prevents the buildup of heat and provides a continuous flushing of debris and bacteria from the base of the pocket
Because of the spray of water at the tip, there is a large amount of potentially contaminated aerosol spray
Highly desirable for the operator of an ultrasonic scaler to have the dental assistant help with using the high-volume evacuator to minimize aerosol contamination.
Indications for Use of the Ultrasonic Scaler
Removal of supragingival calculus and difficult stains
Removal of subgingival calculus, attached plaque, and endotoxins from the root surface
Cleaning of furcation areas
Removal of deposits before periodontal surgery
Removal of orthodontic cements; debonding
Removal of overhanging margins of restorations
Contraindications to Use of the Ultrasonic Scaler
Communicable disease: transmitted by aerosols, such as tuberculosis, poses a risk to the operator
Immunocompromised: A compromised patient is open to infection
Respiratory problems: Materials can be aspirated into the lungs of a patient with respiratory problems
Swallowing difficulty: Problems with swallowing or a severe gag reflex
Cardiac pacemaker: Consultation with the patient’s cardiologist is necessary
Precautions for Children
Young tissues are very sensitive to ultrasonic vibrations
These vibrations and heat may damage the pulp tissue of primary and newly erupted permanent teeth
Nonsurgical Periodontal Treatment
Dental prophylaxis
Prophylaxis is the complete removal of
*calculus
* soft deposits
* plaque
*stains from all supragingival
* unattached subgingival tooth surfaces
Dentist and dental hygienist are licensed to perform this procedure
Scaling, Root Planing, and Gingival Curettage
Scaling and root planing are done as part of a periodontal debridement
In some cases, gingival curettage, a nonsurgical technique, may also be indicated
A local anesthetic is usually administered before these procedures
Scaling
Scalers
*supragingival calculus from the tooth surface
Curettes
*remove supragingival and subgingival calculus
Root Planing
Root planing is performed after scaling procedures to remove any remaining particles of calculus and necrotic cementum embedded in the root surface
After root planing, the surfaces of the root are smooth and glasslike
Anesthetic is usually required for this procedure
Gingival Curettage
Curettage means scraping or cleaning with a curette
Some patients also require gingival curettage in addition to scaling and root planing
Gingival curettage, also known as subgingival curettage, is the scraping of the gingival lining of a periodontal pocket
This is performed to remove necrotic (dead) tissue from the pocket wall
Antimicrobial and Antibiotic Agents
Tetracycline is an antibiotic that is particularly useful for the treatment of periodontitis
Penicillin
Fluoride mouth rinses
A twice-daily chlorhexidine rinse (Peridex) is the most effective means available for reducing plaque and gingivitis
Locally Delivered Antibiotics
New methods can be used to apply antibiotics directly into the periodontal pockets
In one technique, a fiber that contains tetracycline is packed into periodontal pockets
Other methods include using a syringe to insert dissolvable materials such as a gel into the pocket
A dissolvable chip that releases chlorhexidine is inserted into deep pockets
Surgical Periodontal Treatment
When nonsurgical treatment is ineffective in stopping the disease process, periodontal surgery is indicated to control the progress of periodontal destruction and loss of attachment.
Advantages of Periodontal Surgery
*Allows access to the root surface for scaling and root planing
*Makes it easier for the patient to clean difficult areas
*Results in better access to furcations and other areas that are very difficult to reach during traditional scaling and root planing