Ch 17 LO: Mech of Breathing
1/19
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
20 Terms
What are the four major functions of the respiratory system.
Exchange of gases between the atmosphere and blood
• Obtain O2 and eliminate CO2
Homeostatic regulation of blood pH
• Retain or excrete CO2
Protection from inhaled pathogens and irritating substances
• Epithelium traps and destroys substances
Vocalization
• Air movement across vocal cords provides communication
what is the anatomy of the respiratory system and explain the function of each structure?
Conducting System – passages that lead from external
environment to surface of lungs
• Upper respiratory tract – Nose, sinuses, pharynx, larynx
• Lower respiratory tract – Trachea, bronchi, bronchioles
• No gas exchange occurs in the above structures
• Exchange Surfaces– tissues associated pulmonary capillaries
that are specialized for gas exchange between atmosphere and
blood
• Respiratory bronchioles – the terminal segments of airways
that branch into alveoli
• Alveoli – small sacs lined with simple squamous epithelium
• Bones and muscles of the thorax and abdominal cavity
• Inspiratory muscles - sternocleidomastoid, scalenes, external
intercostals, and diaphragm
• Expiratory muscles - internal intercostals and abdominal
muscles
What are the functions of the conducting system?
Warms air
• Humidifies air by adding saline and water vapor to
the airway lumen
• Reduces friction between air and epithelium
• Keeps epithelial cells hydrated
• Traps and clears foreign particles
• Goblet cells – secrete mucins/mucous
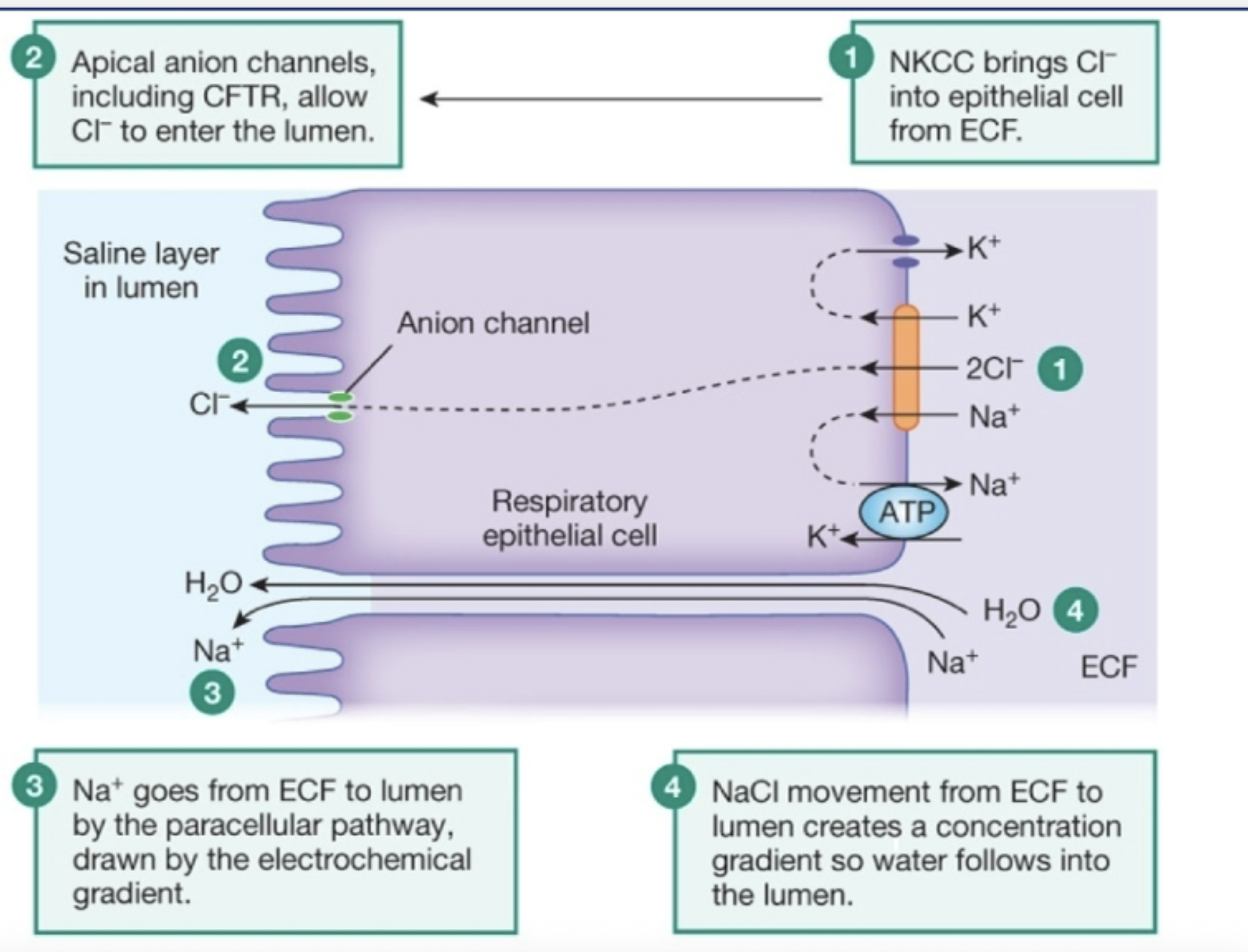
what is the epithelial mechanism for saline secretion
What 2 cell types make up alveoli
Type 1 alveolar cells (95% of alveolar cells) – thin, large
cells and promote diffusion
• Simple squamous epithelial cells
Type 2 alveolar cells (5% of alveolar cells) – secrete
pulmonary surfactant and increase ‘compliance’ of alveoli
• Compliance – an alveoli’s ability to stretch and expand
what is the mathematical the relationship between atmospheric pressure, water vapor pressure, and the partial pressures of individual gases?
Dalton’s law

What is the relationship between volume and pressure?
P1V1 = P2V2
Pressure and volume are inversely related
In lungs:
↑ Volume → ↓ Pressure → air flows in
↓ Volume → ↑ Pressure → air flows out
What are the lung volumes?
Tidal Volume (VT) – volume ventilated during quiet
breathing
• Expiratory Reserve Volume (ERV) – max volume
possible to expire after a normal tidal expiration
• Inspiratory Reserve Volume (IRV) – max volume
possible to inspire after a normal tidal inspiration
• Residual Volume (RV) – The volume of air that remains in
lungs after maximal expiration
What are the lung capacities?
sum of 2 or more lung volumes
Total Lung Capacity = IRV + VT + ERV + RV
Vital Capacity = IRV + VT + ERV
Inspiratory Capacity = VT + IRV
Functional Residual Capacity = ERV + RV
How do pressures and lung volumes change during normal breathing, and how that affects air flow in the respiratory system?
Inspiration
Thoracic volume ↑
Alveolar pressure ↓ (below atmospheric)
Air flows into lungs
Expiration
Thoracic volume ↓
Alveolar pressure ↑
Air flows out
What is the relationship between the atmospheric and intrapleural pressures during a pneumothorax?
Normally:
Intrapleural pressure is negative
Keeps lungs inflated
In pneumothorax:
Air enters pleural space
Pressure = atmospheric
Lung collapses
how does pressure change during breathing cycle
Alveolar pressure
Slightly negative during inspiration
Slightly positive during expiration
Intrapleural pressure
Always negative
Becomes more negative during inspiration
what is the difference between compliance an elastance in respiratory physiology?
Compliance (stretchability)
High compliance → easy to expand
Example: Emphysema
Lungs stretch easily but don’t recoil
Elastance (recoil ability)
Opposite of compliance
High elastance → strong recoil
what is the he role of surface tension and surfactants in respiratory physiology?
Alveoli contain fluid → creates surface tension
This tends to collapse alveoli
Surfactant
Produced by Type II cells
Reduces surface tension
Prevents collapse and improves compliance
law of laplace: P=2T/r
What factors affect airway resistance?
Depends mainly on:
Airway diameter
Control mechanisms:
Parasympathetic (ACh) → bronchoconstriction
Epinephrine (β₂ receptors) → bronchodilation
Local factors:
High CO₂ → dilation
Histamine → constriction
What is the difference between total pulmonary ventilation and alveolar ventilation.
Total pulmonary ventilation = Ventilation rate x VT
• “Normal” rates for each:
• Ventilation rate: 12-20 breaths per minute
• Tidal volume: 500 mL
• 12 br/min x 500 mL/br = 6000 mL/min or 6 L/min
Total alveolar ventilation = Ventilation rate x (VT – Vdead space)
• Not all 6L actually reaches the alveoli
• Anatomical dead space: 150 mL
why does gas composition in the alveoli remain relatively constant during normal breathing and how does it change with hyper- and hypoventilation?
Even though we breathe intermittently:
Large residual volume prevents big swings
Continuous gas exchange with blood stabilizes levels
Changes:
Hyperventilation
↓ CO₂
↑ pH (alkalosis)
Hypoventilation
↑ CO₂
↓ pH (acidosis)
what is the local control mechanisms by which ventilation and alveolar blood flow are matched?
Ventilation-Perfusion Matching
• The body tries to match air flow to blood flow in the alveoli
Local control:
Low O₂ in alveoli
→ vasoconstriction of nearby vessels
→ redirects blood to better-ventilated areasOpposite of systemic circulation!
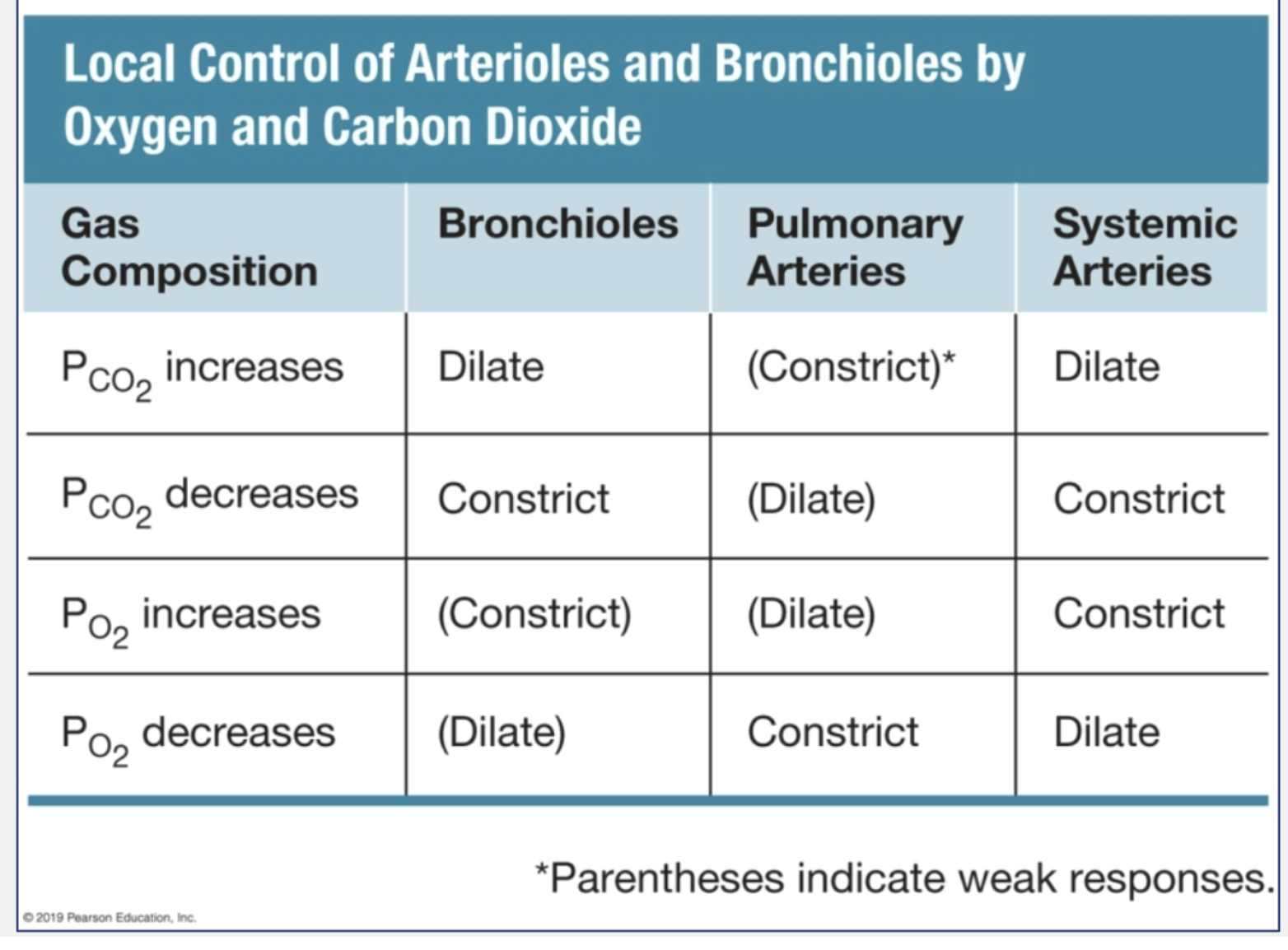
local control of arterioles and bronchioles
What happens when CFTR is blocked?
Cystic Fibrosis Pathology:
no Cl transport → no Na+ attracted to by electrochemical gradient → no water/saline secretion → thick undiluted mucous unable to be cleared by mucociliary escalator