General Anesthesia
1/30
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
31 Terms
Definition of anesthesia
Insensitivity to pain or painful stimuli(no response), achieved via general or regional techniques.



Three components of anesthesia
Amnesia(volatine anesthetic>sleep and dont remember) , Akinesia(muscle relaxants-dont move), Analgesia(opiods- limited pain)


MAC definition
Minimum alveolar concentration at which 50% of patients are akinetic. MAC 1.3=99% akinetic


Factors increasing MAC
Acute amphetamine use, cocaine, chronic alcohol use, young age, hyperthermia, red hair.


Factors decreasing MAC
Propofol, etomidate, barbiturates, benzos, ketamine, opioids, α2 agonists, acute alcohol, local anesthetics, hypothermia, hypercarbia, pregnancy, advanced age.


Inhaled anesthetics examples
Isoflurane, Sevoflurane, Desflurane, Nitrous oxide.


Blood solubility effect
Lower solubility → faster induction/recovery.


Lipid solubility effect
Higher solubility → higher potency (1/MAC).


IV anesthetics used for induction
Propofol, Etomidate, Ketamine, Benzodiazepines, Barbiturates.


Propofol mechanism
Potentiates GABA-A chloride currents.


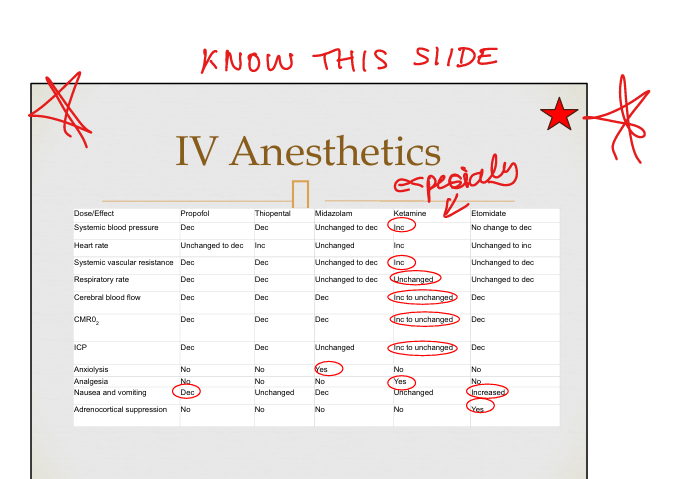
Propofol key effects
Hypnosis, ↓Cerebral metabolic rate of O2, ↓CBF, ↓ICP, profound vasodilation, respiratory depression, antiemetic.


Etomidate key effects
Minimal hemodynamic change; adrenal suppression; no analgesia.


Ketamine mechanism
NMDA receptor antagonist.


Ketamine key effects
Cerebral vasodilator(inc CBF and Cerebral Metabolic Rate of O2) , Profound Analgesia, dissociation, ↑BP/HR/CO, bronchodilation, emergence reactions.



Benzodiazepine key effects
Sedation, anxiolysis, anterograde amnesia, anticonvulsant.


Barbiturate key effects
CNS depression, ↓CMRO2, ↓CBF, apnea, modest hypotension.


Methohexital
Barbituate, activates epileptic foci(stimulatory) and is used in ECT


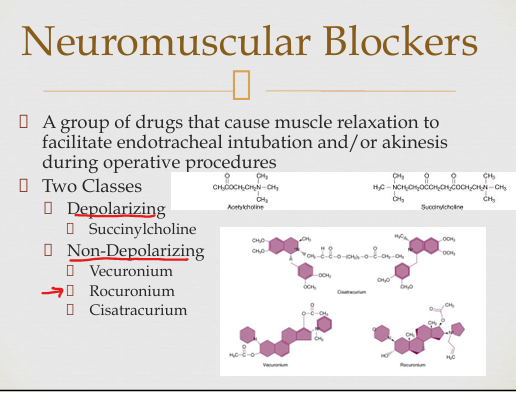
Neuromuscular blocker classes and examples
Depolarizing (succinylcholine) and non-depolarizing (rocuronium, vecuronium, cisatracurium).

Succinylcholine contraindications
Burns, trauma, immobility, denervation injuries(ex: Stroke, spinal cord injury), muscular dystrophy, hyperkalemia risk.


Succinylcholine side effects
Bradycardia, arrhythmias, hyperkalemia, myalgia, ↑ICP, ↑IOP, malignant hyperthermia.


Malignant hyperthermia triggers
Volatile anesthetics + succinylcholine.

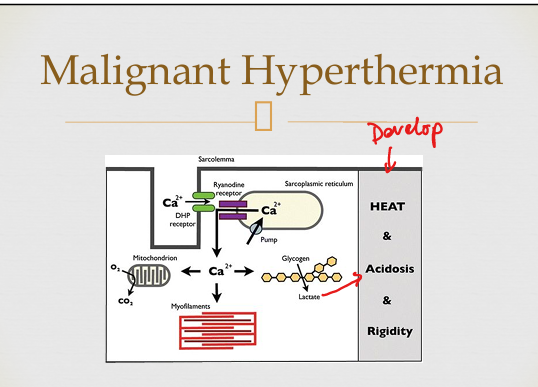

Malignant hyperthermia treatment
Stop triggers, give IV dantrolene, correct acidosis/hyperkalemia.


Reversal of Ach non-depolarizers
Neostigmine + glycopyrrolate OR Sugammadex (for roc/vec).


Sugammadex mechanism
Encapsulates rocuronium/vecuronium, removing them from NMJ.


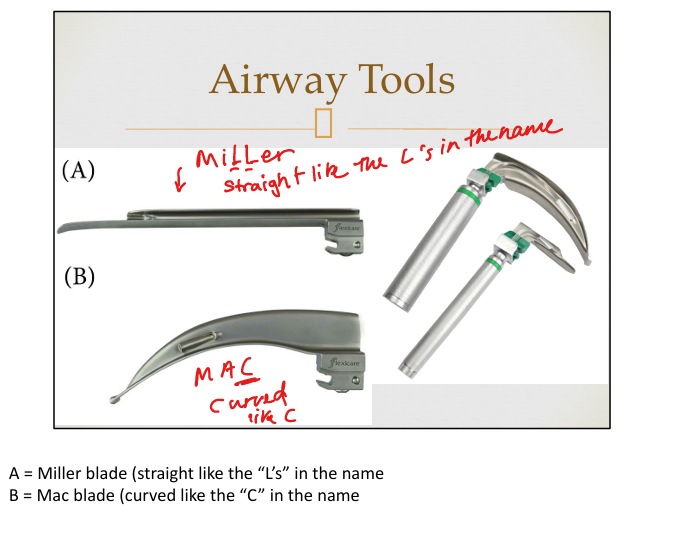
Miller vs MAC Airway blade
MiLLer=straight L’s and MAC is curved like C

Rapid Sequence Intubation definition
Rapid induction + succinylcholine; no mask ventilation; used for full stomach or aspiration risk.
Reasons NOT to use RSI
Contraindication to succinylcholine (hyperkalemia, MH, ↑ICP).
Airway assessment predictors
Oral Aperture/Interincisor gap(less than 3cm inc risk to inability to open mouth) Mallampati classification, thyromental distance(shortened=decreased space to dispalce tongue), cervical ROM, BMI(>30 is difficult airway)


Mallampati I,II,III, IV
I: Full visibility of soft palate, fauces, tonsillar pillars and uvula.
II: Visible soft palate, fauces and uvula
BAD:
III: Only soft palate and base of uvula visible
IV: Soft palate is not visible; only Hard palate
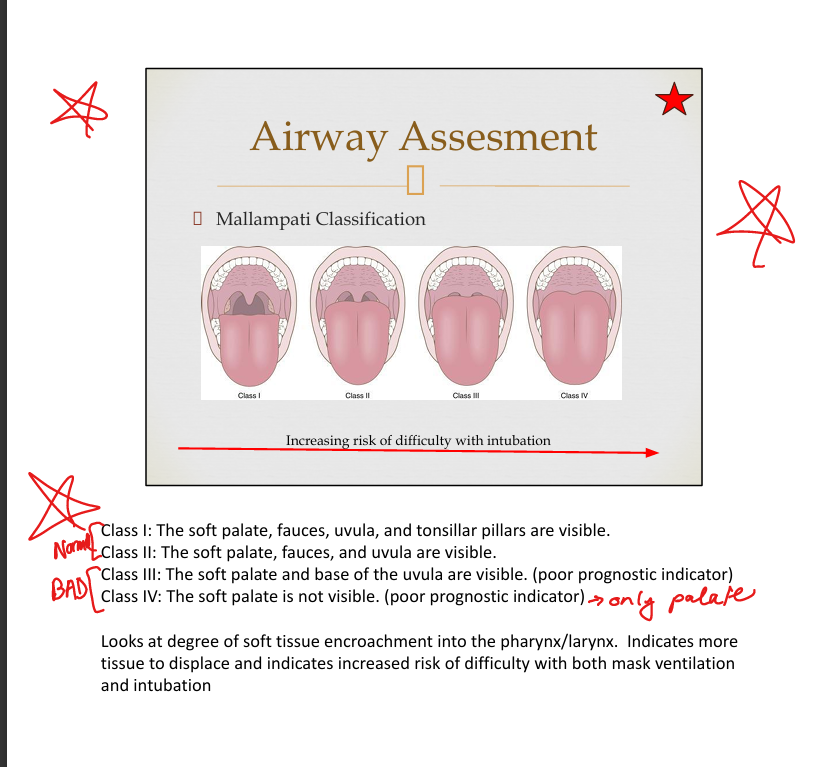

Mallampati IV
Only hard palate visible; highest difficulty risk.
IV Anesthetics Summary

