Microbio final exam-projects
1/147
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
148 Terms
What is the structure and function of the epidermis?
The epidermis is the outermost layer of skin composed of tightly packed cells filled with keratin proteins.
Keratin provides mechanical strength and creates a barrier that protects against physical damage, abrasion, and water loss/penetration.
What is the role of the stratum corneum in immune defense?
outermost epidermal layer made of dead keratinized cells.
It contains antimicrobial peptides (positively charged chemicals) that disrupt negatively charged bacterial membranes, leading to bacterial death.
What components are found in the dermis and their function?
The dermis contains connective tissue, collagen (for strength and elasticity), macrophages (phagocytosis), and mast cells (inflammatory response). It supports immune defense and structural integrity.
How do sebaceous glands contribute to antimicrobial defense?
secrete sebum, an oily substance with a low pH that creates an acidic environment, making the skin inhospitable to many microorganisms.
How does sweat act as a defense mechanism?
low pH and high salt concentration, both of which inhibit microbial growth and survival on the skin surface.
What are the characteristics of microorganisms that live on the skin?
Skin microbes must tolerate dry, salty, and acidic environments, making them uniquely adapted to survive harsh surface conditions.
Where are microbes typically found on the body and why?
Flat, dry areas (e.g., back) → fewer microbes
Moist areas (e.g., underarms, groin) → more microbial growth
Protected areas (hair follicles, glands) → stable environments for microbes
What is meant by microbial specificity on the skin?
Different microbial species prefer specific areas of the body, and each individual has a unique microbiota composition.
How stable is the skin microbiome over time?
it remains relatively constant unless disrupted by illness, antibiotics, or environmental changes.
How does the microbiome affect skin aging?
Certain bacteria are associated with collagen degradation, which contributes to wrinkles and skin sagging.
How does keratinized skin prevent infection?
it forms a tough, impermeable barrier that physically blocks microbial entry.
What is sloughing and why is it important?
Sloughing is the shedding of dead skin cells, which removes attached microorganisms and prevents colonization.
Why is acidic pH important for skin defense?
Low pH inhibits growth of many pathogenic microorganisms.
What is the function of lysozyme in the skin?
Lysozyme breaks down bacterial cell walls, especially in Gram-positive bacteria.
What are antimicrobial peptides?
Small proteins that directly kill microbes by disrupting their cell membranes.
How does Streptococcus benefit the skin?
Competes with pathogenic microbes for nutrients and space.
What is the role of Staphylococcus in normal flora?
Produces antimicrobial substances that inhibit harmful bacteria.
What does Corynebacterium do?
Competes with harmful microorganisms, helping maintain balance.
How does Propionibacterium contribute to skin defense?
Breaks down sebum into fatty acids, lowering pH and inhibiting pathogens.
What is the role of Lactobacillus?
Produces lactic acid, maintaining an acidic environment.
What is the significance of Candida on the skin?
A yeast that is normally harmless but can become opportunistic if balance is disrupted.
What is Methicillin-resistant Staphylococcus aureus?
A strain of Staphylococcus aureus resistant to many antibiotics, causing skin and soft tissue infections.
How is MRSA transmitted?
Direct skin contact or indirect contact via contaminated objects (fomites like gym equipment, razors)
How is MRSA diagnosed?
PCR testing, culture, Gram stain, coagulase and catalase tests.
How is MRSA prevented?
Hygiene, wound coverage, no sharing personal items.
What are key prevention strategies for MRSA?
Hand hygiene, covering wounds, avoiding sharing personal items.
How is MRSA treated?
Combination antimicrobial therapy due to resistance.
What defines a maculopapular rash?
Flat (macules) and slightly raised (papules) discolored skin lesions.
What causes Measles and how is it transmitted?
Caused by measles virus; transmitted via respiratory droplets.*airborne
What are hallmark signs of measles?
Rash begins on head and spreads downward; lasts >1 week.
How is measles prevented and treated?
Prevented with MMR/MMRV vaccine; treatment is supportive care
What causes Rubella?
Rubella virus transmitted via droplets.
What are key features of rubella?
Mild rash lasting ~3 days; dangerous in pregnancy (congenital rubella).
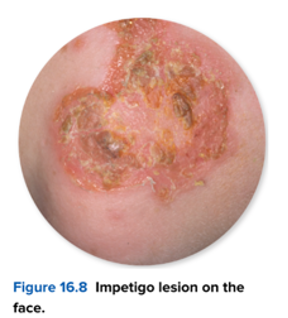
What is Impetigo and its cause?
Superficial skin infection caused by Streptococcus pyogenes and/or Staphylococcus aureus.
What are classic signs of impetigo?
Honey-colored crusts, flaky lesions, often around mouth and face.
How is impetigo treated?
Often self-limiting; topical antibiotics (mupirocin) or oral antibiotics if needed.
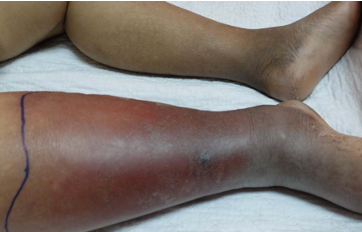
What is cellulitis and its cause?
A deep skin infection affecting dermis and subcutaneous tissue, usually caused by Streptococcus or Staphylococcus.
What are symptoms of cellulitis?
Pain, warmth, redness, swelling, fever, and lymph node enlargement.
How is cellulitis treated?
Oral antibiotics (mild) or IV antibiotics (severe/immunocompromised).
What is Staphylococcal Scalded Skin Syndrome?
A toxin-mediated condition caused by Staphylococcus aureus leading to skin peeling.
Who is most at risk for SSSS and why?
Newborns/infants due to immature immune systems.
What causes Chickenpox?
Human herpesvirus 3 (varicella-zoster virus).
What are hallmark symptoms of chickenpox?
Itchy vesicles filled with clear fluid.
What causes Smallpox?
Variola virus.
What is the progression of smallpox rash?
starts in pharynx → spreads to face → then extremities.
What causes Cutaneous anthrax?
Entry of bacterial endospores through skin cuts.
How is leishmaniasis transmitted?
Through sand fly bites.
What organisms cause cutaneous mycoses?
Dermatophytes (Trichophyton, Microsporum, Epidermophyton).
Example of cutaneous fungal infection?
Ringworm (tinea).
What causes superficial mycoses?
Malassezia species (part of normal flora).
Example of cutaneous fungal infection?
Dandruff (seborrheic dermatitis), folliculitis.
CASE STUDY #1
What is the most likely diagnosis for a 6-year-old unvaccinated child with fever, fatigue, and a red rash starting on the head and spreading downward?
Measles
What key symptoms point toward measles in this case?
High fever (102.6°F)
Fatigue
Red, patchy rash starting on head → spreading to trunk
Respiratory changes (“breathing differently”)
Why is vaccination history critical in this case?
Lack of MMR vaccination significantly increases risk for measles infection, especially in children.
How is measles transmitted?
Airborne via respiratory droplets and aerosols → highly contagious.
How is measles confirmed diagnostically?
IgM antibody testing (serology) or PCR.
What are common complications of measles?
Laryngitis
Bronchopneumonia
Secondary bacterial infections
What are severe complications of measles?
Pneumonia (most common cause of death)
Encephalitis (can cause permanent brain damage)
What is the primary treatment for measles?
Supportive care:
Antipyretics (e.g., acetaminophen/Tylenol)
Rest
Fluids
When is Vitamin A used in measles?
In malnourished children → reduces severity and complications.
When are antibiotics used in measles?
Only if secondary bacterial infections (e.g., pneumonia) develop.
When is the MMR vaccine given?
First dose: 12–15 months
Booster: before school entry
Why does measles require high herd immunity?
Extremely contagious → requires ~92–94% immunity to prevent outbreaks.
What conditions should be considered in the differential diagnosis of measles?
Fifth disease
Dengue fever
Hand, foot, and mouth disease
Toxic shock syndrome
Kawasaki disease
What are the two exposed surfaces of the eye?
Conjunctiva
Cornea
What is the function of tears in eye defense?
Contain lysozyme, lactoferrin, and sugars → antimicrobial action.
What is “immune privilege” in the eye?
Reduced immune response to prevent inflammation that could impair vision.
What is conjunctivitis?
Infection/inflammation of the conjunctiva; highly contagious.
How can you differentiate bacterial vs viral conjunctivitis?
Bacterial → thick, milky discharge
Viral → clear, watery discharge
What is a classic sign of conjunctivitis?
Eyes “glued shut” in the morning from dried secretions.
What organisms commonly cause conjunctivitis?
Bacterial: Staph, Strep, H. influenzae
Viral: Adenovirus
Neonatal: N. gonorrhoeae, C. trachomatis
How is bacterial conjunctivitis treated?
Topical antibiotics (e.g., ciprofloxacin, erythromycin).
What is keratitis?
Infection of the cornea → can lead to vision loss or blindness.
What symptoms suggest keratitis over conjunctivitis?
Eye pain
Blurred vision
Photophobia
Difficulty opening eye
Progressive worsening
What is the most likely cause of viral keratitis?
Herpes simplex virus
What is the treatment for viral keratitis?
Antivirals (e.g., acyclovir, trifluridine).
What is the nurse’s priority for a patient with keratitis?
Monitor vision changes
Ensure medication adherence
Early recognition of worsening symptoms
How can viral keratitis be prevented?
Hand hygiene
Avoid touching eyes
Avoid contact with HSV lesions
Do not share personal items
Adhere to antiviral medications
Key difference between conjunctivitis and keratitis?
Conjunctivitis → superficial, usually not vision-threatening
Keratitis → deeper, vision-threatening emergency
You are a school nurse that is working at an elementary school. A student walks in crying due to tripping on the playground. The student has a small amount of blood running down their leg. What level of skin did the student break to bleed?
❏Dermis
❏Epidermis
❏Subcutaneous
❏All of the above
❏Epidermis
You are a a school nurse at a elementary school, which statement made by the children indicates correct understanding?
A.High pH is a natural defensive mechanism of the skin
B.Moist enviroment is natrual defence of the skin
C.Macrophages protect the epidermis from bacteria
D.Low pH is a natural defensive mechanism of the skin
D.Low pH is a natural defensive mechanism of the skin
Which of the following skin conditions can be prevented through good hygiene practices? Select all that apply
❏A. MRSA Skin and Soft-Tissue Infection
❏B. Maculopapular Rash Diseases
❏C. Impetigo
❏D. Cellulitis
❏A. MRSA Skin and Soft-Tissue Infection
❏C. Impetigo
❏D. Cellulitis
You are assigned with a client that has been confirmed to have Smallpox, what will you expect to do for this patient? Select all that apply
❏A. Wear a surgical mask when entering the room
❏B. Use a gown and gloves for all interactions
❏C. Put on a N95 respirator before entering the room
❏D. Place a surgical mask on patient when transporting
❏E. Ensure patient is in a negative pressure room
B. Use a gown and gloves for all interactions
❏C. Put on a N95 respirator before entering the room
❏D. Place a surgical mask on patient when transporting
❏E. Ensure patient is in a negative pressure room
When giving a vaccine to an infant, the nurse will tell the mother to expect which adverse effect?
A. Fever over 101F
B. Rash
C. Soreness at the injection site
D. Chills
C. Soreness at the injection site
A nurse is assessing a child with suspected conjunctivitis. Which finding is most consistent with bacterial conjunctivitis?
A. Clear, watery discharge
B. Itching that worsens outdoors
C. Milky, thick drainage from the eye
D. Sensitivity to light without discharge
C. Milky, thick drainage from the eye
Which situations can increase risk for eye infection by disrupting normal defenses? (Select all that apply)
❏A. Improper contact lens hygiene
❏B. Decreased tear production
❏C. Frequent blinking
❏D. Use of topical antibiotics
❏E. Damage to the corneal surface
Improper contact lens hygiene
❏B. Decreased tear production
❏D. Use of topical antibiotics
❏E. Damage to the corneal surface
What are the main components of the central nervous system (CNS)?
Brain and spinal cord, supported by neurons, meninges, and cerebrospinal fluid (CSF), which provide both structural and protective functions.
What are the three layers of the meninges?
Dura mater (outer), arachnoid mater (middle), and pia mater (inner).
What is the function of cerebrospinal fluid (CSF)?
Cushions the brain and spinal cord, reduces impact, and helps maintain a stable environment for neural function.
What is the blood-brain barrier (BBB) and its significance?
A highly selective barrier formed by tightly joined endothelial cells that restricts entry of toxins, pathogens, and many drugs into the CNS.
How does the vascular system contribute to CNS protection?
Blood vessels provide structural support and, through the BBB, regulate what substances can enter the brain.
What are microglia and their role in the CNS?
Specialized macrophage-like cells that perform phagocytosis and respond to infection or injury within the brain.
Does the CNS contain normal microbiota?
o—the CNS is normally sterile; presence of microbes indicates infection or pathology.
What does it mean that the CNS is immunologically privileged
It has restricted immune responses and strong protective barriers to prevent inflammation that could damage neural tissue.
Which viruses can remain dormant in nerve cells?
Herpes simplex virus, HIV, and varicella-zoster virus.
What is the role of the gut microbiome in the nervous system?
Influences brain development, formation of the blood-brain barrier, and development of peripheral nerves.
What is the psychobiome?
The interaction between gut microbiota and brain function, affecting mood, behavior, and neurological health.
what is meningitis?
Inflammation of the meninges, often caused by bacterial or viral infection.
What is the most common bacterial cause of meningitis?
Neisseria meningitidis infection
What are key virulence factors of Neisseria meningitidis?
Capsule (immune evasion), pili (attachment), and endotoxin (inflammatory response).