Anatomy and Physiology 2- Digestive System
1/73
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
74 Terms
Digestive Tract
• Also called gastrointestinal (GI) tract or alimentary canal
• Is a muscular tube that extends from oral cavity to anus
• Passes through pharynx, esophagus, stomach, and small and large intestines
Digestive System accessory organs
Teeth, tongue, various glands, liver, pancreas
Peristalsis
Smooth muscle contraction to move the food bolus forward
Oral cavity, teeth, and tongue function
Mechanical breakdown, lubricating, and mixing of food with saliva
Pharynx function
Muscular pushing of food down into the esophagus
Esophagus function
Movement of food to the stomach
Stomach function
Chemical breakdown of food by acid and enzymes; mechanical breakdown through muscular contractions
Small intestine function
Chemical digestion (enzymes) and absorption of water, organic substrates, vitamins, ions
Large intestine function
Bacterial digestion and absorption of water, organic substrates, vitamins, and ions
Salivary glands function
Secretion of fluid that lubricates and contains enzymes that break down carbohydrates
Liver function
Secretion of bile (for lipid digestion), storage of nutrients, and various vital functions
Gall bladder function
Storage, concentration, and secretion of bile
Pancreas function
Exocrine cells secrete buffers and enzymes; endocrine cells secrete hormones
Ingestion
Occurs when materials enter digestive tract via the mouth
Propulsion
Smooth muscle contraction - peristalsis
Mechanical processing
• Crushing and shearing
• Makes materials easier to propel along digestive tract
• Increases surface area
Digestion
• The chemical breakdown of food into small organic molecules that can be absorbed by digestive epithelium
• Hydrolysis reactions are aided by digestive enzymes
Secretion
Is the release of water, acids, enzymes, buffers, and salts by the epithelium of digestive tract and by glandular organs
Absorption
• Movement of organic substrates, electrolytes, vitamins, and water
• Across digestive epithelium
• Into interstitial fluid of digestive tract
Excretion
• Removal of waste products from body fluids
• Process called defecation removes feces
Protection
Mucosal enzymes, IgA, MALT, Peyer’s Patch, defensive rejections
Functions of the Tongue
• Speech
• Manipulation of food to assist in chewing and to prepare material for swallowing
• Sensory analysis of texture, temperature, and taste of food
Functions of the Oral Cavity
Sensory analysis
Of material before swallowing
Mastication (mechanical processing)
Through actions of teeth, tongue, and palatal surfaces
Lubrication
Mixing with mucus and salivary gland secretions
Limited digestion
Of carbohydrates and lipids
Three pairs of salivary glands
• Parotid salivary glands
• Sublingual salivary glands
• Submandibular salivary glands
Each pair has distinctive cellular organization
Each pair produces saliva with different properties
Saliva production locations and contents
• Glands produce 1.0–1.5 liters of saliva each day
• 70% by submandibular glands
• 25% by parotids
• 5% by sublingual glands
• Contents:
• 99.4% water
• 0.6% solutes: Electrolytes, Buffers, mucins, Antibodies, Enzymes
Functions of Saliva
Flushing oral surfaces to protect from bacteria buildup
IgA, lysozyme control bacteria populations
Moistening and lubricating materials in the mouth
Mucins: glycoproteins that give saliva lubricating property
Liberates taste chemicals that stimulate taste buds
Initiationg digestion of carbohydrates (salivary amylase)
Polysaccharides to di and tri saccharides
Deactivated in acid pH of stomach
Secretion of lingual lipase
Begins lipid digestion
pH 3-6
The Pharynx (Throat) purpose and muscle functions
-Passageway for food, liquids, and air
-Food passes through the oropharynx and laryngopharynx to the esophagus
-Pharynx has muscles that:
Push bolus of food towards the esophagus
Elevate larynx to force epiglottis over glottis
Elevate soft palate and pharyngeal wall to protect nasal cavity
At rest: bottom portion remains constricted to prevents air from entering the esophagus and stomach (upper esophageal sphincter)
Esophagus
Muscular tube that brings food and liquid to the stomach
Histology of the esophagus
Mucosa consists of stratified squamous epithelium
Esophageal glands
Located in the submucosa
Secretes mucous onto the mucosa
Reduces friction between bolus and esophageal lining
Muscularis externa
Peristalsis - smooth rhythmic contraction of the esophagus and rest of GI tract
Lower esophageal sphincter (LES)
Stomach functions
• Storage of ingested food
• Mechanical breakdown of ingested food to produce semi- liquid Chyme
• Chemical breakdown of food
• Disruption of chemical bonds by acid
• Chemical digestion of proteins
• Production of intrinsic factor
Intrinsic factor
A glycoprotein required for absorption of vitamin B12 in ilium of the small intestine
Histology of the stomach
Simple columnar epithelium forms mucosa of stomach
Gastric pits of stomach
• Gastric pits are shallow depressions that open onto the gastric surface
• Each gastric pit communicates with several gastric glands
• Contain cells that make gastric secretions
• Mucous cells produce mucous that covers interior surface
• Mucous neck cells (in gastric pits)
• Protects epithelium from acidic chyme and digestive enzymes
Gastric glands of stomach
• Secrete 1500 mL of gastric juice / day
• Dominated by 4 types of cells
Parietal cells
Chief cells
Goblet cells
G-Cells
All stimulated by: Ach (PNS), histamine, and gastrin
Parietal cells
Secrete intrinsic factor and hydrochloric acid (HCl)
Chief cells
Secrete pepsinogen (inactive proenzyme) and gastric lipase
Goblet cells
Mucous producing
G-Cells
Secrete Gastrin (stimulates gastric secretion, intestinal motility, relaxation of ileocecal valve)
Acidic environment of stomach
• Kills microbes that are ingested
• Breaks down plant cell walls and animal connective tissues
• Activates pepsinogen to pepsin
• Stomach performs preliminary digestion of proteins by pepsin (proteins into smaller peptides)
• Lingual lipase remains active and gastric lipase digests lipids
• Salivary amylase is deactivated
• Although digestion occurs in the stomach, nutrients are not absorbed there
The Duodenum
• The segment of small intestine closest to stomach
• 25 cm (10 in.) long
• “Mixing bowl” that receives chyme from stomach and digestive secretions from pancreas and bile from liver
The Duodenum functions
• To receive chyme from stomach
• To neutralize acids before they can damage the absorptive surfaces of the small intestine
• NaHCO3 is released by the pancreas into the duodenum
The Jejunum
• Is the middle segment of small intestine
• 2.5 meters (8.2 ft) long
• Is the location of most chemical digestion and nutrient absorption
The Ileum
• The final segment of small intestine
• 3.5 meters (11.48 ft) long
• Ends at the ileocecal valve
Ileocecal valve
• Controls flow of material from the ileum into the cecum
• Prevents feces from backing up into ileum
Muscosa
• Consists of simple columnar epithelium (absorptive cells)
• Folded into Villi to increase surface area
• Lacteal extends up the center of each villus
• Mucous (Goblet) cells between columnar epithelial cells
• Brunner glands in duodenum: submucosal glands
• Enteroendocrine cells release hormones (Gastrin, Secretin, CCK)
Intestinal glands
• Depressions at bases of villi
• Secrete 1-2 L intestinal juices
• Dividing cells contain brush border enzymes
Brush border enzymes function
• Integral membrane proteins
• Located on microvilli on the surface of absorptive cells (the brush border)
• Break down materials in contact with brush border
• Break down materials in central lumen after cells are shed from villus

Small Intestine Movements
• Segmentation contractions mix chyme with digestive secretions
• Weak peristaltic contractions move it slowly toward jejunum
Gastroenteric (enterogastric) Reflex
• Stimulates motility along small intestine
• Initially, Enteroendocrine cells release gastrin, secretin, CCK
• Inhibits gastrin secretion, causes pyloric sphincter contraction
The Gastroileal Reflex
Gastrin: Relaxation of ileocecal valve allowing materials to pass from small intestine into large intestine
Pancreas location
• Lies posterior to stomach
• Starts at curve of duodenum, goes toward spleen
Pancreas functions
• Endocrine: Cells of the pancreatic islets secrete hormones into bloodstream
• Exocrine: Acinar cells and epithelial cells of duct system secrete pancreatic juice into lumen of duodenum
Exocrine function of the Pancreas
• Secretes 1000 mL (1 L) pancreatic juice per day
• Contains pancreatic enzymes
• Pancreatic alpha-amylase: Starches to di/trisaccharides
• Pancreatic lipase: Triglycerides to fatty acids and monoglycerides that are easily absorbed
• Nucleases: RNA or DNA to nucleotides
• Proteolytic enzymes: Proteins to peptides and amino acids
• Secreted as inactive proenzymes
• Activated after reaching small intestine
Liver functions
• Is the largest glandular organ (1.5 kg; 3.3 lb)
• Performs essential metabolic and hematologic functions
• Carb, lipid, and amino acid metabolism
• Waste product removal
• Drug inactivation and disposal
• Phagocytosis and antigen presentation
• Synthesis of plasma proteins
• Removal of circulating hormones, antibodies, toxins
• Digestive function:
• Secretes bile
• Bile is stored and concentrated by the gallbladder
Bile
• Bile has bile salts that aid in lipid digestion
• Dietary lipids are not water soluble
• Mechanical processing in stomach creates large drops containing lipids
• Pancreatic lipase is not lipid soluble
• Interacts only at surface of lipid drop
• Bile salts break drops apart (emulsification)
• Increases surface area exposed to enzymatic attack
• Creates tiny droplets coated with bile salts
• Keeps droplets in solution
• Aids in absorption by intestinal epithelia
Intestinal absorption: monosaccharides and amino acids
Enter absorptive cells by facilitated diffusion and cotransport
Intestinal absorption: lipids
• Fatty acids diffuse into absorptive cells
• Re-formed into triglycerides and packaged into chylomicrons inside intestinal cells
• Chylomicrons undergo exocytosis then enter lacteal
Intestinal absorption: vitamins
• Most enter cells by diffusion, fat soluble enter with fatty acids
• Vitamin B12 must bind to intrinsic factor before active transport can occur
Intestinal absorption: water
Flows along osmotic gradient (Not active)
Functions of the large intestine
• Reabsorption of water
• Compaction of intestinal contents into feces
• Absorption of important vitamins produced by intestinal bacteria
• Storage of fecal material prior to defecation
Histology of the large intestine
• Lacks villi
• Presence of distinctive intestinal glands
• Deeper than glands of small intestine
• Do NOT produce digestive enzymes
• Dominated by mucous cells
• Mucous provides lubrication as fecal material becomes drier
• The longitudinal layer of the muscularis externa is reduced to the muscular bands of taeniae coli
Reabsorption: Large Intestine
• Large Intestine: Less than 10% of nutrient absorption
• Reabsorption of water
• Reabsorption of bile salts
In the cecum
Transported in blood to liver for recycling
• Absorption of vitamins produced by bacteria
Vitamin K
Vitamin B5
Biotin
• Absorption of organic wastes (urobilinogens to be excreted by kidneys)
Gastroileal and gastroenteric reflexes
Move materials into the cecum while you eat
Movement from cecum to transverse colon
Is very slow, allowing hours for water absorption
Peristaltic waves
Move material forward along length of colon
Segmentation movements (Haustral Churning)
Mix contents of adjacent haustra
Movements of large intestine
• Movement from transverse colon through rest of large intestine results from powerful peristaltic contractions (mass movements)
• Stimulus is distension of stomach and duodenum; relayed over intestinal nerve plexuses
• When contents get to rectum, distension of the rectal wall triggers defecation reflex
Elimination of feces
• Requires relaxation of internal and external anal sphincters
• Reflexes open internal sphincter, close external sphincter
• Opening external sphincter requires conscious effort
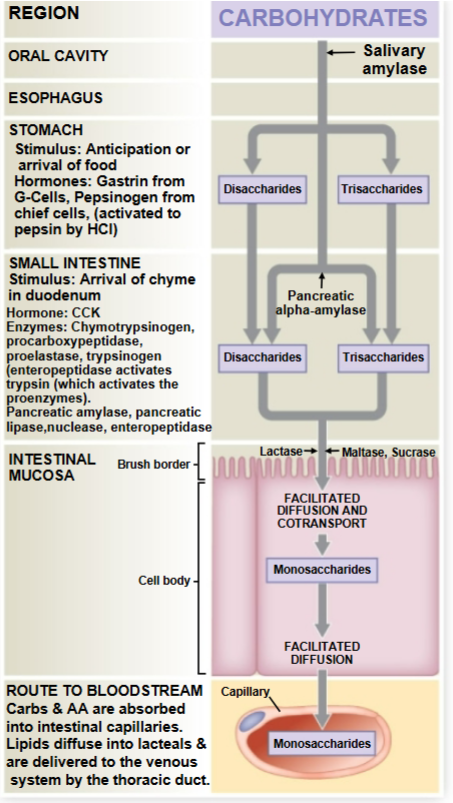
Carbohydrate absorption
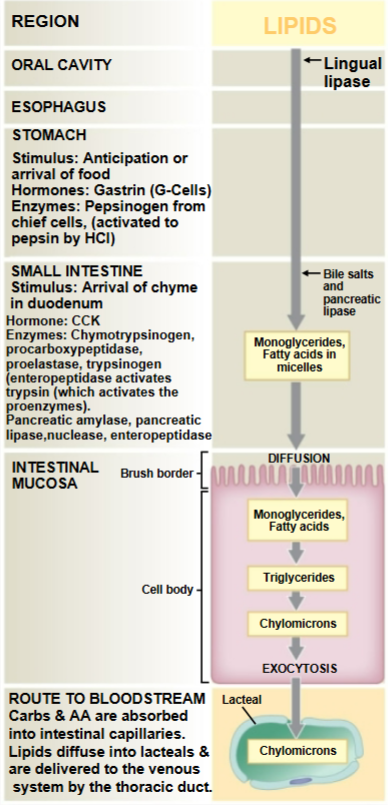
Lipid absorption
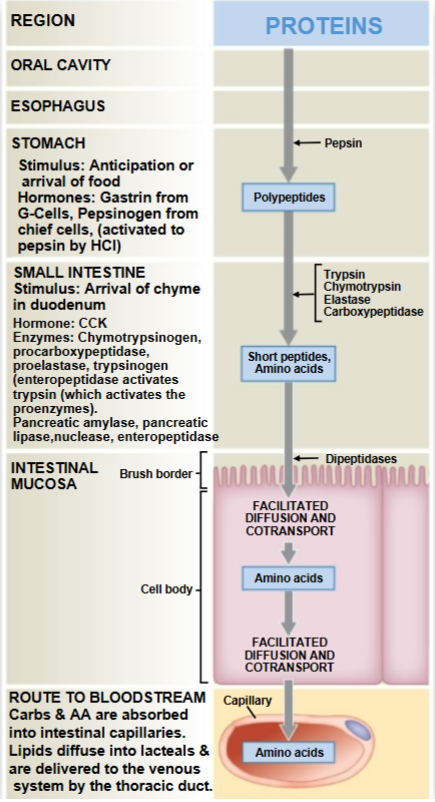
Protein absorption