HMI201 Theory Test Revision
1/51
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
52 Terms
Radio frequency (RF) interference in MRI is prevented with:
A. A Faraday cage.
B. Superconducting coils.
C. Gradient coils.
D. An RF transmitter/receiver.
A: A Faraday cage
--> enclosure made of conductive materials which block signals
A high magnetic field strength is obtained with:
A. A Faraday cage.
B. Superconducting coils.
C. Gradient coils.
D. An RF transmitter/receiver.
B: Superconducting coils
--> generate the magnetic field
Position encoding in MRI is obtained with:
A. A Faraday cage.
B. Superconducting coils.
C. Gradient coils.
D. An RF transmitter/receiver.
C: Gradient Coils
--> creates spatial variation used to identify location
MRI excitation is obtained with:
A. A Faraday cage.
B. Superconducting coils.
C. Gradient coils.
D. A radio frequency (RF) transmitter/receiver.
D: A radio frequency (RF) transmitter/reciever
--> RF pulse applied to body to manipulate protons. Pulses are emitted by transmitter coils. The signal emitted by the protons realigning themself to the magnetic field is detected by receiver coils.
An MRI T1 weighted image is obtained with:
A. A short Repetition Time (TR) and short Echo Time (TE).
B. A long TR and short TE.
C. A long TR and long TE.
D. A short TR and long TE.
A: A short TR and short TE
REMEMBER: 1<2, therefore short for both.
Features of T1 Contrast:
(Repetition Time, Echo Time, Signal Quality, Tissue Contrast quality)
Short RT
Short ET
High Signal
Good Tissue Contrast --> Dark lesions
An MRI T2 weighted image is obtained with:
A. A short Repetition Time (TR) and short Echo Time (TE).
B. A long TR and short TE.
C. A long TR and long TE.
D. A short TR and long TE.
C: Long TR and long TE
REMEMBER: 2>1, therefore 2=long for both
Features of T2 Contrast:
(Repetition Time, Echo Time, Signal Quality, Tissue Contrast quality)
Long RT
Long ET
Low Signal
High Tissue Contrast --> Bright lesions
What does the pixel brightness in an MR image represent in the corresponding voxel in the patient?
The Radiointensity emitted by a corresponding Voxel.
OR
Pixel brightness corresponds to the radiofrequency intensity in the corresponding voxel.
What generates the MRI radio frequency (RF) signal in the patient?
The longitudinal magnetisation of tissues (Mz) being flipped to the transverse axis to become transverse magnetisation (Mxy). The transverse magnetisation produces a measurable radiofrequency signal in the patient which is received by the receiver coils
Which Tissue characteristic corresponds to the Longitudinal Magnetisation Regrowth rate:
A. Proton Spin Density (rho)
B. T1
C. T2
D. TI
B. T1
REMEMBER: 1 looks like l = L therefore longitudinal
Which Tissue characteristic corresponds to the Transverse Magnetisation Decay rate:
A. Proton Spin Density (rho)
B. T1
C. T2
D. TI
C: T2
REMEMBER: 2 gives the same vibes as T, therefore transverse
What Tissue characteristic determines the Saturation Magnetisation:
A: Proton Spin Density (rho)
B: T1
C: T2
D: TI
A. Proton Spin Density (rho)
PSD - S = Saturation
A FLAIR sequence is designed to suppress the MR signal from:
A: Water
B: CSF
C: Fat
D: Bone
A: Water
Water shows up as bright --> suppresses this
F = Fluid = Water (mostly)
A STIR sequence is designed to suppress the MR signal from:
A: Water
B: CSF
C: Fat
D: Bone
C. Fat
Think: STIR to bake --> Fat
Gadolinium contrast agent is used in:
A: Rho imaging
B: T1 imaging
C: T2 imaging
D: TI imaging
B. T1 Imaging
Think -> Has L+I in it, therefore T1
Explain the technique used for MR Angiography imaging
Excite the entire volume.
Re-excite only the volume of interest with 90-degree excitation pulse to nullify transverse magnetisation (measurable signal) of surrounding tissues (sends it to 180-degree flip).
Nullifies the background tissues.
Rephrase as excited fluid flows into volume of interest.
Explain the technique used for Spinal Fat Suppression
Fat’s signal is similar to water, poses problems for obtaining good contrast.
Can be solved through exploiting spinal fat’s precessional frequency, which is slightly different to water.
Pre-saturation of the fat (excite volume containing the spine by sending an RF pulse tuned to fat’s precessional frequency, then re-excite it at the same frequency to nullify its measurable transverse signal while leaving the signal from the rest of the spine intact).
Which of these tissues appears brightest in a CT image?
A. Air
B. Bone
C. Fat
D. Water
B. Bone
Which tissue has a Hounsfield Unit (HU) equal to 0?
A. Air
B. Bone
C. Fat
D. Water
D. Water
What type of CT artefact is commonly seen in 3rd Generation CT scanners?
A. Aliasing artefact
B. Susceptibility artefact
C. Uniformity ring artefact
D. Zipper artefact
C. Uniformity Ring Artefact
Which of the following algorithms is NOT used in CT image reconstruction?
A. Back-projection
B. Convolution
C. Fourier transformation
D. Gaussian smoothing
D. Gaussian Smoothing
What does CT detector High Capture Efficiency mean?
The efficiency refers to how able the detector is to capture the X-ray photons transmitted after they’ve gone through the patient
High efficiency therefore means majority of the transmitted photons are captured by the detector rather than lost.
Both the geometry and material of dectector optimises interaction with X-rays.
What is a CT Scanogram?
A 2D low-dose scan acquired before a CT scan, usually with both sagittal and coronal views.
It’s used to plan the positioning of the patient and define start and end limits of the scanning region.
Helps avoid unnecessary radiation dose.
In CT imaging, what is the DLP and what is it used for?
Stands for Dose-Length Product.
A measure of total radiation output during a CT scan (mGy x cm).
When multiplied by a conversion factor (k), can be used to estimate the effective dose for patients.
Also useful for comparing radiation output between protocols or different machines.
For Digital Mammography, What is the National Reference Level dose for the Mean Glandular Dose (MGD) measured on the 2cm PMMA phantom?
A: 1mGy
B: 2mGy
C: 3mGy
D: 4.5mGy
A: 1mGy
In Mammography, the minimum Aluminium Equivalent Tube Filtration is:
A: 0.1mm
B: 0.5mm
C: 1.0mm
D: 2.5mm
B: 0.5mm
Removes low-energy x-rays, increasing image contrast and decreasing patient dose.
In Mammography, the Heel Effect can be used to:
A: Give a higher intensity at the chest wall
B: Ensure a uniform entrance intensity
C: Give a smaller intensity at the chest wall
D: Reduce scatter radiation
A: Give a higher intensity at the chest wall
In Mammography, the Line Focus Effect can be used to:
A: Give higher spatial resolution at the chest wall
B: Give higher spatial resolution in the breast tissue
C: Ensure uniform spatial resolution
D. Reduce scatter radiation
B: Give higher spatial resolution in the breast tissue
--> giving finer detail @ breast
In soft tissue the wavelength of a 1 MHz Ultrasound transducer is:
A. 1.54 mm
B. 1.54 um
C. 1.54 sec
D. 1.54 cycles/sec
A: 1.54mm
1MHz = 1x10^6Hz
Wavelength = speed of sound (constant)/frequency (Hz)
= 1 540 000m/s / 1x10^6Hz
= 1.54mm
Which of the following Ultrasound transducers has the greatest penetration depth?
A: 2MHz
B: 8MHz planar
C: 10MHz focused
D: 15MHz
A: 2MHz
REMEMBER: Increased depth with decreased frequency.
What is the maximum temperature increase allowed in the foetus during Ultrasound scanning in excess of 5 minutes?
A: 0˚C
B: 1˚C
C: 4˚C
D: 10˚C
B: 1˚C
If soft tissue has an Ultrasound attenuation co-efficient of 0.3db/cm at 1MHz, what is the Half Value Thickness:
A: 1cm
B: 3cm
C: 5cm
D: 10cm
Half Value Thickness = 3db/attenuation coefficient
= 3dB / 0.3dB/cm
= 10cm
Which of the following Ultrasound QA tests does not need to be done routinely:
A: Uniformity
B: Distance accuracy
C: Axial Resolution
D: Maximum depth of visualisation
C: Axial Resolution
Ultrasound is a:
A: Orthogonal wave
B: Transverse wave
C: Longitudinal wave
D: Piezoelectric wave
C: Longitudinal wave
REMEMBER: longitUUUUdinal wave = UUUltrasound
Which of the following statements on the Ultrasound Near Field is not true:
A: It is near the deep bone interface
B: Also called the Fresnel Zone
C: Has a converging beam profile
D: Depends upon the transducer effective diameter.
A: It is near the deep bone interface
REMEMBER:
NEAR --> DEEP
Which of the following statements on the Ultrasound Far Field is not true:
A: Also called the Fraunhofer Zone
B: Has a diverging beam profile
C: Less divergence with lower frequency
D: Less divergence with larger transducer effective diameter.
C: Less divergence with lower frequency
REMEMBER:
FAR (high) FIELD = LOW F
Name 3 effects of concern in Ultrasound Imaging safety:
Thermal, cavitation, radiation force
Scatter dose rate drops off from the patient approximately as:
A. Inverse square with distance
B. Inverse linear with distance
C. Stays constant with distance
D. Increases slightly with distance
A. Inverse square with distance
To reduce occupational exposure from scatter radiation during interventional radiography: (select all that apply)
A. Stand as far away from the patient as possible.
B. Expose the patient for as little time as possible.
C. Wear a protective Pb apron.
D. Wear a radiation badge.
A, B, C
X D --> doesn't reduce occupational dose
The Pb apron will attenuate scatter radiation:
A. More strongly than primary radiation
B. Less strongly than primary radiation
C. To the same extent as primary radiation
D. Has no effect on scatter radiation
A. More strongly than primary radiation
If a Digital Fluoroscopy system is acquiring 1024^2 dynamic images in a 12 cm mode, what is the pixel size:
A. 1.17 mm/pixel
B. 0.117 mm/pixel
C. 1.17 um/pixel
D. 0.117 um/pixel
B. 0.117 mm/pixel
120mm / 1024px = 0.117
In a Pulse Progressive Fluoroscopy system which energises the x-ray tube with 2x 50msec pulses in every second, the duty cycle is:
A. 50%
B. 10%
C. 5%
D. Continuous
B. 10%
2x50ms in 1 second (1000ms)
50ms + 50ms = 100ms
100/1000=10%
For an undertable Fluoroscopy system what is the minimum Focus to Tabletop distance allowed?
A. 25 cm
B. 50 cm
C. 100 cm
D. 125 cm
C: 100cm
In Pulsed Fluoroscopy, for the same kVp and mA, which of the following pulse sequences gives the lowest dose:
A. 20 msec pulses at 10 frames/s
B. 15 msec pulses at 10 frames/s
C. 12 msec pulses at 12 frames/s
D. 10 msec pulses at 12.5 frames/s
D. 10 msec pulses at 12.5 frames/s
Just maths it out
A: 20*10 = 200
B: 15*10 = 150
D: 10*!2.5 = 125
How do you decrease the noise by 50% in Pulsed Fluoroscopy?
A. Add 4 sequential frames together.
B. Subtract 4 sequential frames together.
C. Multiply 4 sequential frames together.
D. Divide 4 sequential frames together.
A. Add 4 sequential frames together.
Which of the following apply to a FPDF (select all that apply)
A. No warmup is required
B. No Spatial distortion
C. Increased Lag
D. Low Signal to Noise Ratio (SNR)
A. No warmup is required
B. No Spatial distortion
In Direct Flat Panel Fluoroscopy (DFPF), what does the "Direct" mean?
The x-rays interact directly with the amorphous selenium pixels on the detector, which are able to store the x-ray intensity information.
Which of the following is NOT a component of a Picture Archiving and Communications System (PACS)?
A. Diagnostic Workstation
B. Health Level 7 (HL7)
C. Image Storage
D. Network
B. Health Level 7 (HL7)
It is like DICOM, a standard
Draw the Transverse and Longitudinal Magnetisation of T1, T2, Proton Spin Density, and Mixed Contrast
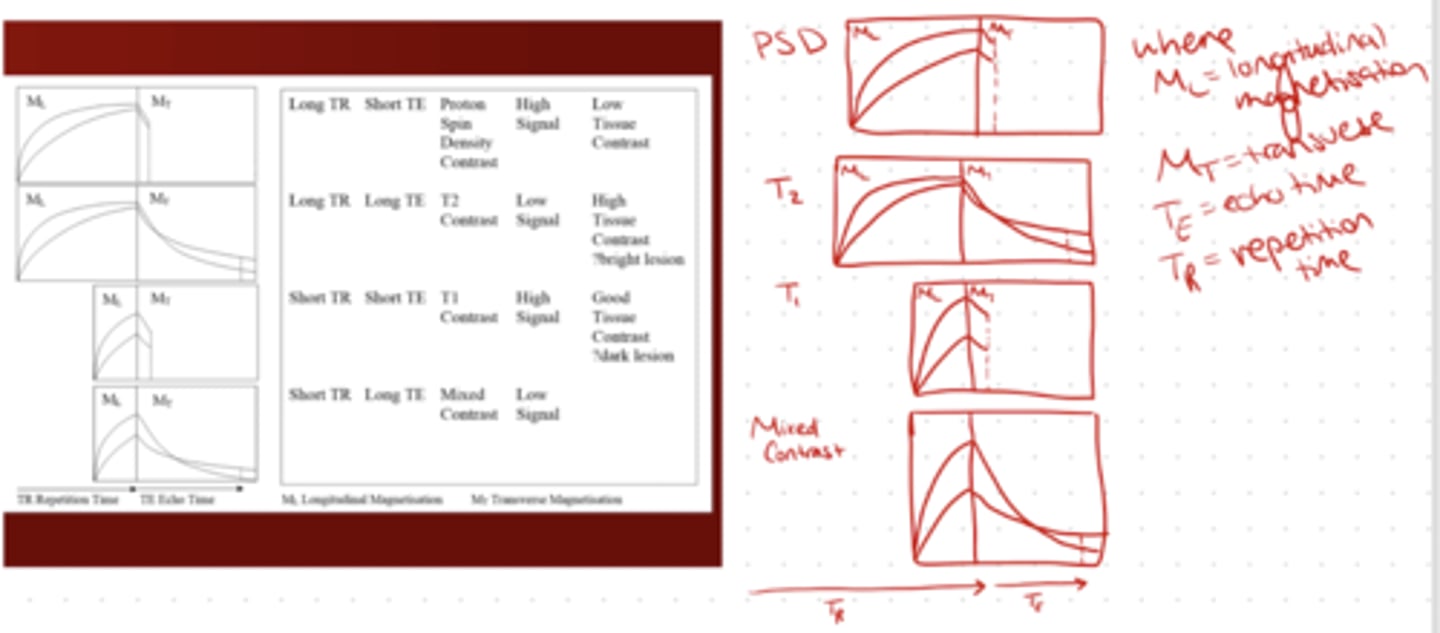
Draw the Transverse and Longitudinal Magnetisation of T1
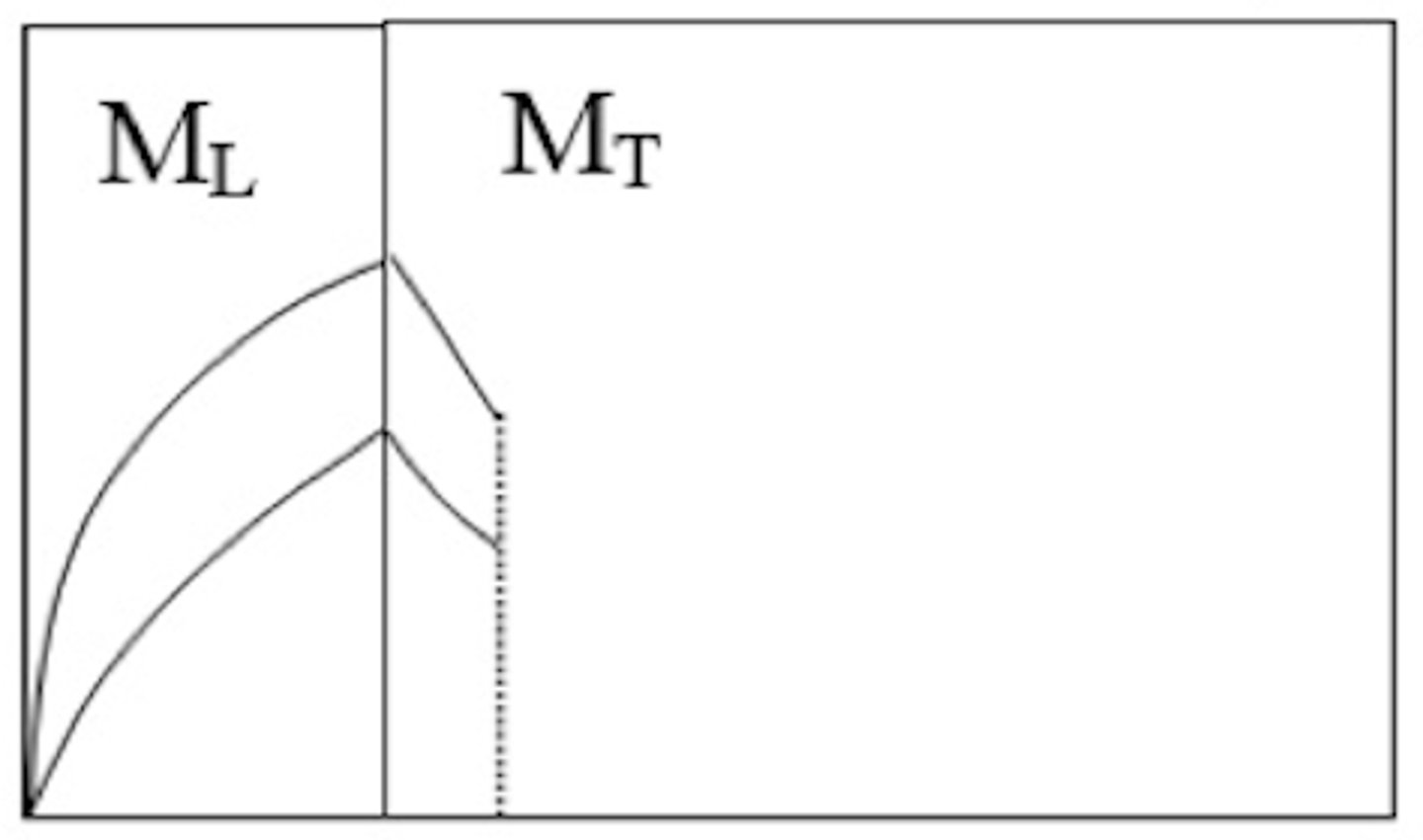
Draw the Transverse and Longitudinal Magnetisation of T2