MSK - Osteology (Complete)
1/51
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
52 Terms
The axial skeleton includes the
Skull, spine, and thorax
The appendicular skeleton includes the
Limbs, hands, feet, shoulder girdle, pelvis
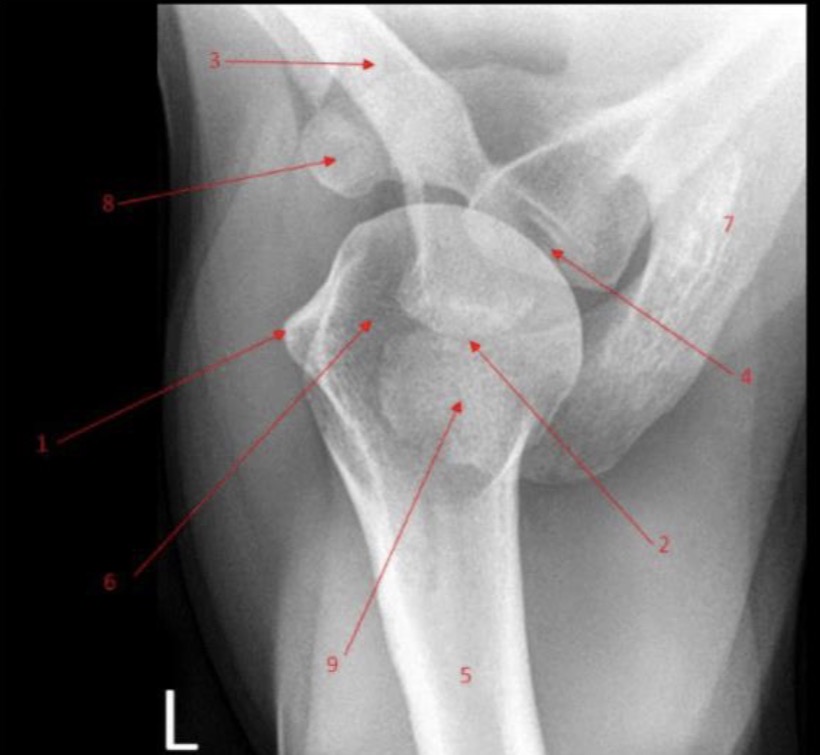
Label the shoulder
bonus: which side is anterior?
1 - lesser tubercule
2 - acromion-clavicular joint
3 - clavicle
4 - glenoid cavity
5 - shaft of humerus
6 - head of humerus
7 - scapula
8 - coracoid process
9 - acromion process
bonus: the left side
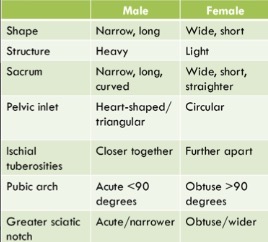
Difference between male and female pelvis
What are accessory ossicles?
How do they form?
What can they be mistaken for?
Small extra bones near joints
Arise from unfused ossification centres
Can be mistaken for fractures and may become painful after trauma
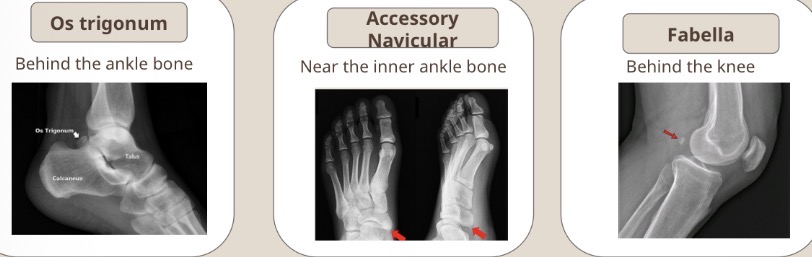
3 types of accessory ossicles
Os trigonum
Accessory navicular
Fabella
Radiopaque and radiolucent meaning and examples
Radiopaque means anything which appears WHITE on X-ray
Radiolucent means anything which appears black or transparent
Bone, metal = radiopaque
tissue, fat and air = more radiolucent
What is each modality (CT, MRI, X-ray and ultrasound) best for:
Assessing whether a tumor is benign or malignant
Imaging muscle, tendon or ligaments
Imaging soft tissue
Imaging fractures
CT - to assess whether a tumor is benign or malignant
MRI - Muscle, tendon or ligaments
Ultrasound - Soft tissue
X-ray - Fracture
What are the 5 types of bone
Long
Short
Flat
Irregular
Sesamoid
Bone properties - explain what is meant by anisotropic
Bone strength varies with direction of force
strongest = the longitudinal axis
Intermediate strength = oblique angles
weakest = on the transverse axis
Bone properties - explain what is meant by viscoelasticity
Bones can deform under load and return to its original shape if force remains below the yield point
Forces beyond the yield point cause permanent damage/fracture
Bone properties - explain what is meant by Wolff’s Law
Bone adapts to the stresses placed upon it by altering its structure and mass
Increased loading = greater bone density
Decreased loading = lower bone density
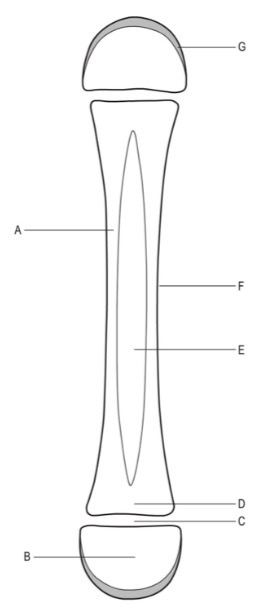
Anatomy of the long bone
A - diaphysis
B - epiphysis
C - epiphyseal plate
D - metaphysis
E - medullary cavity
F - periosteum
G - articulated hyaline cartilage
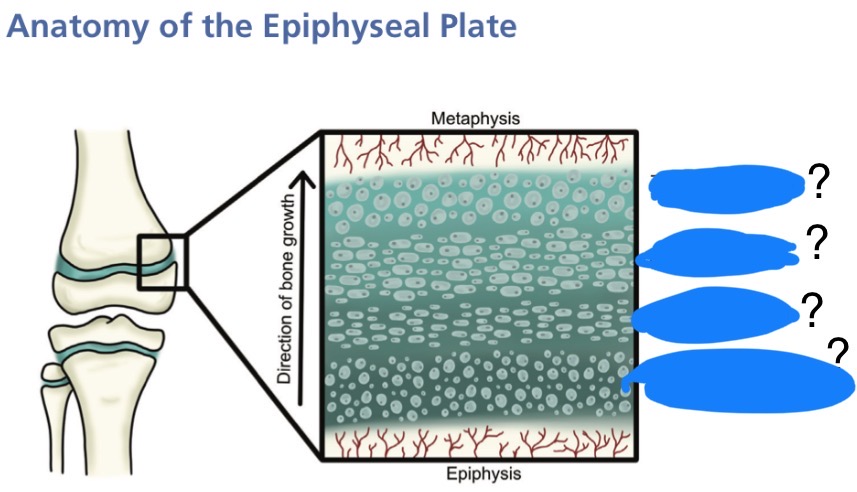
Label the areas of the epiphyseal plate
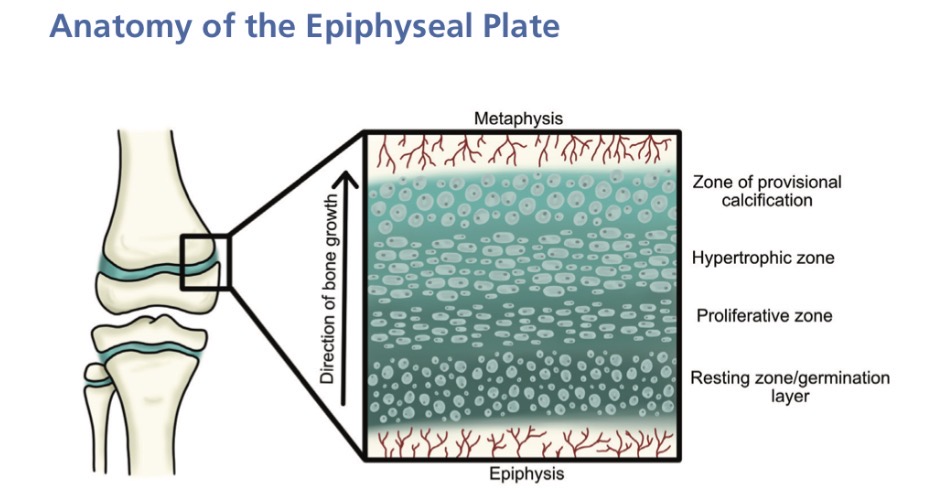
What is the role of the epiphyseal plate?
Longitudinal bone growth in the immature skeleton
What is the role of each zone in the epiphyseal plate?
Germination layer/resting zone - where chondrocytes (cartilage cells) are produced
Proliferation zone - chondrocytes divide and form columns, driving bone length
Hypertrophic zone - the weakest part of the plate, where chondrocytes lengthen, then enlarge and die
Zone of provisional calcification — cartilage matrix calcifies, then osteoblasts move in and deposit bone
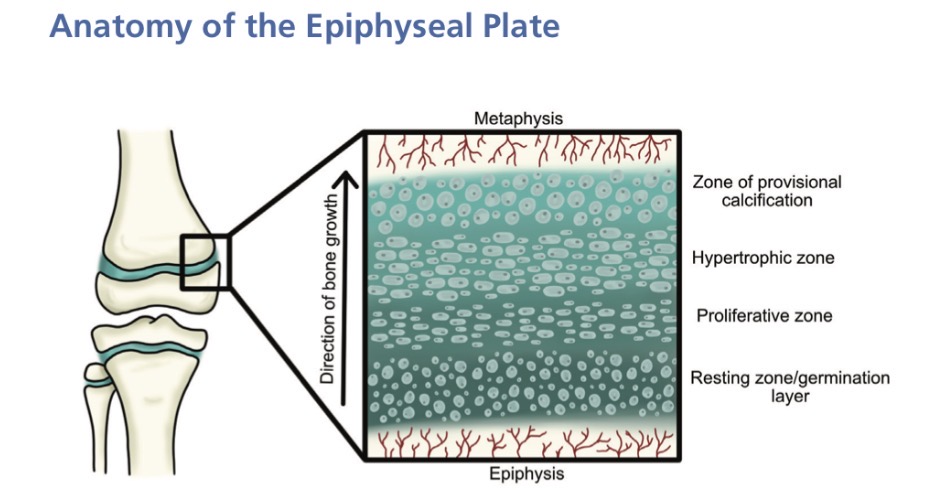
What are ossification centres and what can they be used for?
Meaning —> where bone ossification begins and spreads outward
Uses —> Identify bone growth deficiencies, identify the age of a child
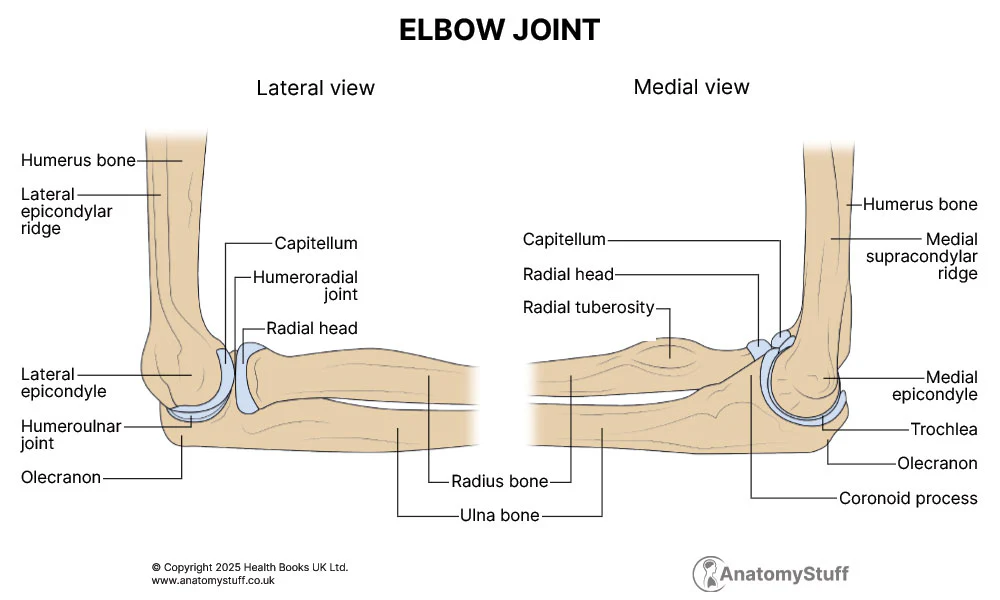
State where each part of CRITOE is located (on which bone)
Capitulum
Radial head
Internal epicondyle
Trochlea
Olecranon
External epicondyle
Capitulum - distal humerus (lateral)
Radial head - proximal radius
Internal (medial) epicondyle - sticky out bit on the internal humerus
Trochlea - distal humerus (medial, right beside the capitulum)
Olecranon - proximal ulna (forms the point of the elbow)
External (lateral) epicondyle - sticky out bit on the lateral humerus
What is the Salter-Harris classification
Only used for paediatric
Grading scale to describe disruption of the epiphyseal growth plate from I-V (1-5). I is the least damaged with the best prognosis, V is the most damaged with the worst prognosis
Explain the Salter-Harris classification
S - Slipped - type I
A - Above (the growth plate) - type II
L - Lower (than the growth plate) = type III
TE - through everything = type IV
R - rammed = Type V
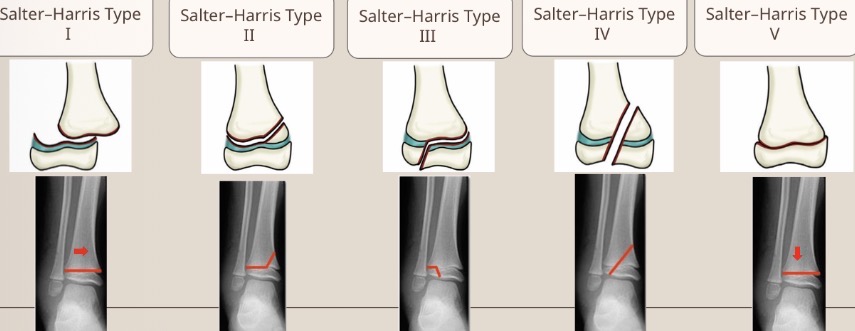
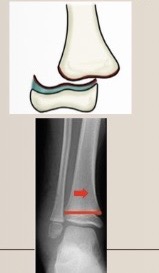
Use the Salter-Harris classification system to describe the fracture pattern
Type I - slipped
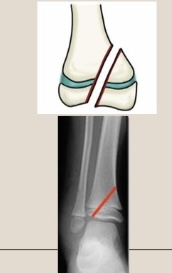
Use the Salter-Harris classification system to describe the fracture pattern
Type IV - though everything
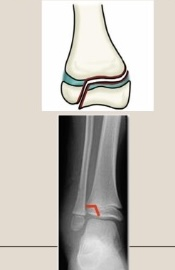
Use the Salter-Harris classification system to describe the fracture pattern
Type III - lower than the growth plate
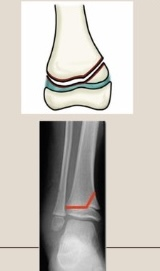
Use the Salter-Harris classification system to describe the fracture pattern
Type II - above the growth plate
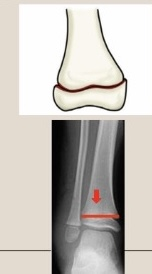
Use the Salter-Harris classification system to describe the fracture pattern
Type V - growth plate rammed into the metaphysis
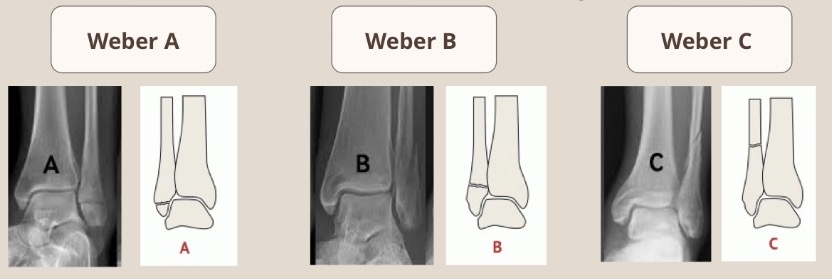
What is the Weber Classifaction?
Grading A-C used to describe ankle fractures based in the fibula’s level relative to the ankle joint
C is worse than A
What is the syndesmosis?
a fibrous joint where two bones, such as the tibia and fibula, are connected by strong ligaments and an interosseous membrane, allowing minimal movement
Explain Weber classification
A = Below the level of the syndesmosis (good prognosis)
B = at the level of the syndesmosis
C = above the level of the syndesmosis (makes the joint unstable, requires surgery)
Fractures of the proximal femur are either intracapsular or extracapsular. Describe what is meant by intracapsular fracture and the risk it poses
Intracapsular = involving femoral head and neck
Risk = can damage blood supply to femoral head, increasing the chance of
avascular necrosis (cutting off the bones blood supply which can lead to death of the bone tissue)
nonunion (bone fails to heal)
malunion (bone heals in the wrong position)
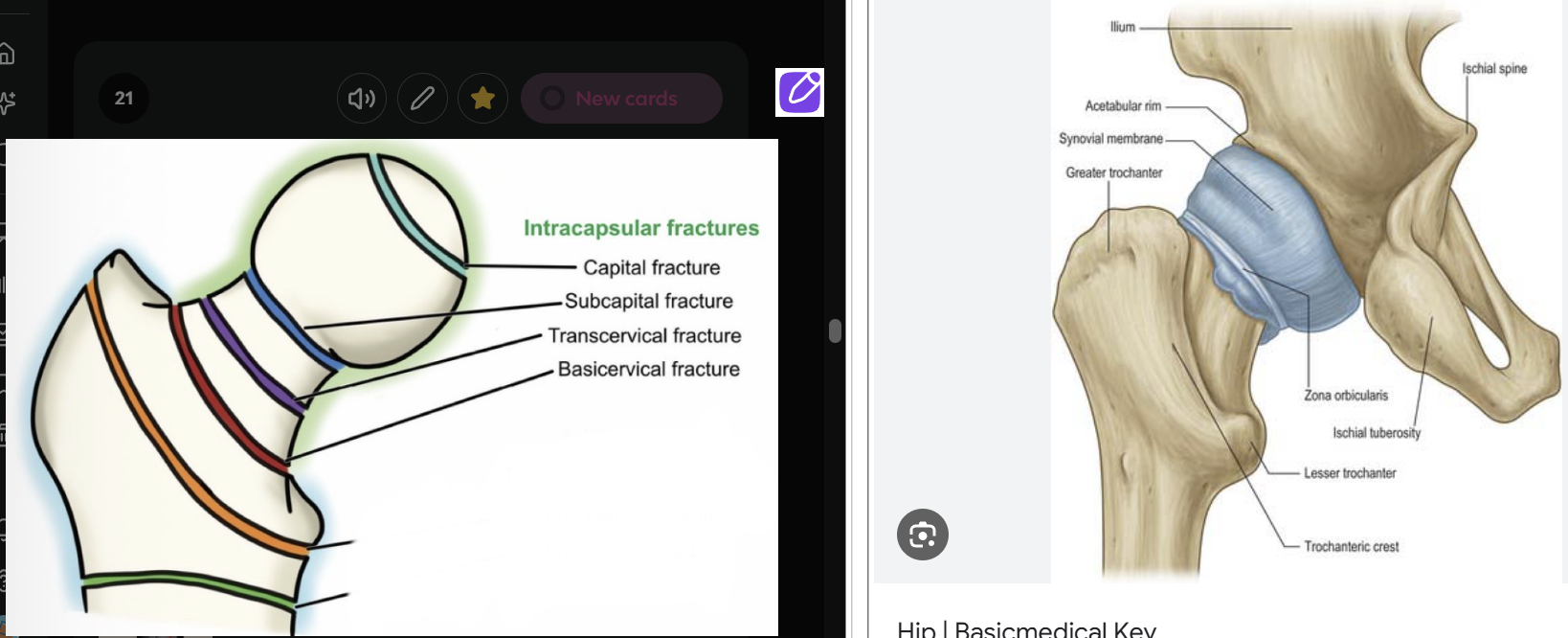
Describe what is meant by extracapsular fracture and the risk it poses
Extracapsular - fractures below the femoral neck, or involving the trochanteric region
Risks
high 1-year mortality (up to 50%)
substantial bleeding
risks related to immobility - deep vein thrombosis, chest infections, and pressure ulcers
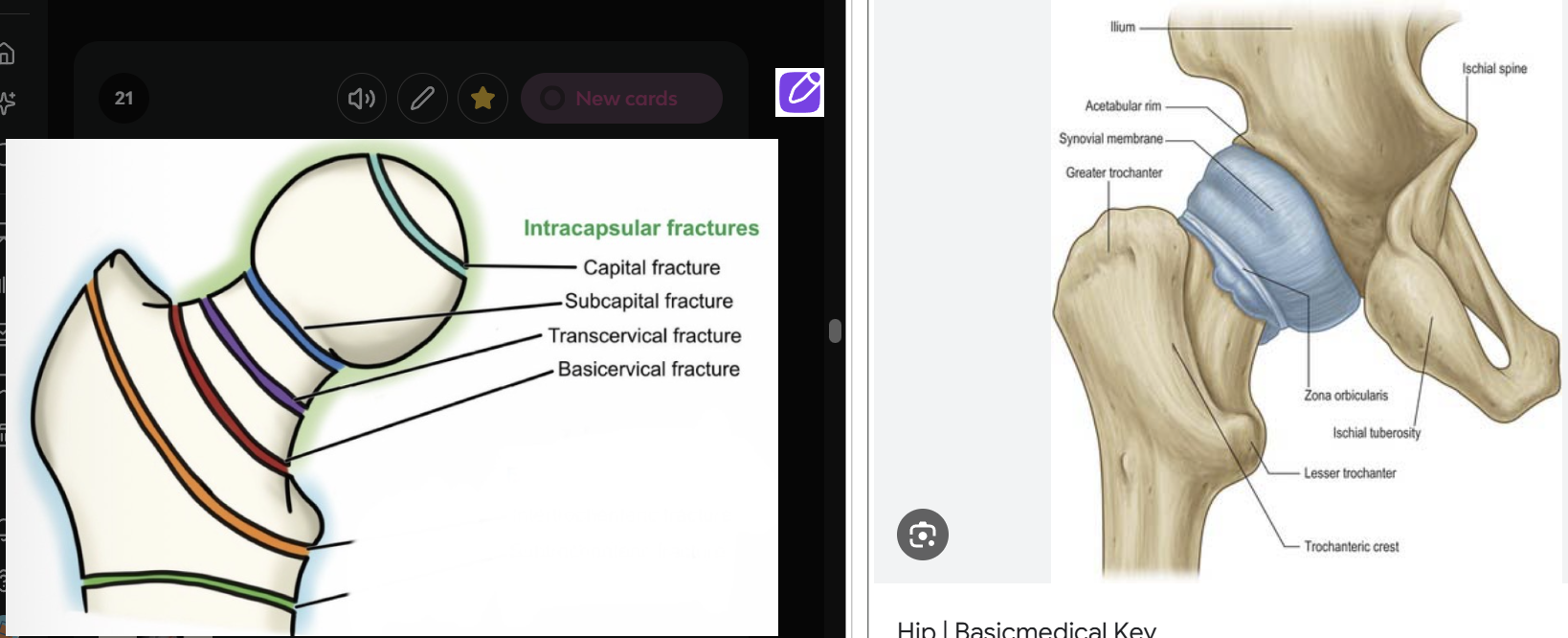

Typical exam question: Using your knowledge of anatomy, pathology and pattern recognition can you explain the differences between the two X-ray images?
Image on the left shows intracapsualar hip fracture whereas the image on the right is normal.
Image on the left shows adequate exposure whereas image on the left is slightly underexposed.
Image on the left has lower bone density than image in the right
2 main processes by which bones form
state the role of osteoclasts and the epiphyseal plate
Intramembranous ossifcation - forms flat bones from fibrous membranes (eg forms the skull)
Endochondral ossification - forms most bones
Osteoclasts form the medullary cavity while the epiphyseal plate enables growth until maturity
Bone cells and their roles
Osteogenic cells
Osteoblasts
Osteocytes
Osteoclasts
Osteogenic cells - stem cells which divide and differentiate into osteoblasts
Osteoblast - build bone
Osteocytes - primary cell of the bone
Osteoclasts - break bone down
How bones heal
Stage 1 - a blood clots at the site, inciting inflammation (temporary scaffolding)
Stage 2 - soft callus hardens into a hard callus which closes the fracture gap
Stage 3 - the hard callus is remodelled into mature bone
Factors affecting bone healing (will be in exam)
Most to least important
Vascular integrity
Location
Type of fracture
Age
Metabolic factors
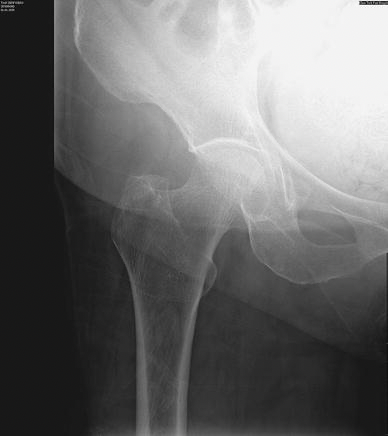
Osteoporosis - what is it and what causes it?
Radiographic appearance
A metabolic diseases which reduces bone mineral density, reducing it’s strength - mostly in older people
Radiographic appearance - The bone has a thinner cortex and larger trabecula.
Patient presentation for osteoporosis - physical signs and symptoms
Physical Signs
Kyphosis/Hunchback
Back pain
Loss of height
Symptoms
sudden fractures
Back pain
Weak grip strength
How can osteoporosis be imaged and which areas are looked at to assess bone density?
T-score diagnoses
DEXA scan - spine, forearm, left hip
T-scores
Normal between +1 and -1
Osteopenia between -1 and -2.5
Osteoporosis -2.5 or less
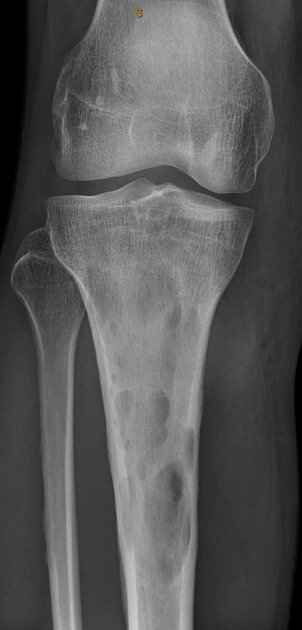
Osteomyelitis - what is it and what is it caused by?
Radiographic appearance
Inflammation of the bone caused by bacterial infection - often seen in diabetic patients
Radiographic appearance
Lower bone density
Lytic lesions - dark areas of bone with ‘moth-bitten appearance’
Patient presentation for osteomyelitis - physical signs and symptoms
Physical signs
swollen, warm and tender limbs
Symptoms
pain
Limping
Refusal to weight-bear
Which imaging methods can be used diagnose osteomyelitis?
CT, MRI, X-ray, Ultrasound
What is osteogenesis imperfecta and what causes it?
Radiographic appearance
A genetic mutation causing underproduction of collagen, resulting in brittle bones
Radiographic appearance
decreased bone density
Bowing of the bones
Frequent and unexplained deformities leading to deformations
Patient presentation for osteogenesis imperfecta - physical signs and symptoms
Physical signs
Bowed legs
Short stature
Symptoms
fragile bones which fracture easily
Loose joints (hypermobility)
Muscle weakness
Which imaging method can be used to diagnose osteogenesis imperfecta?
X-ray
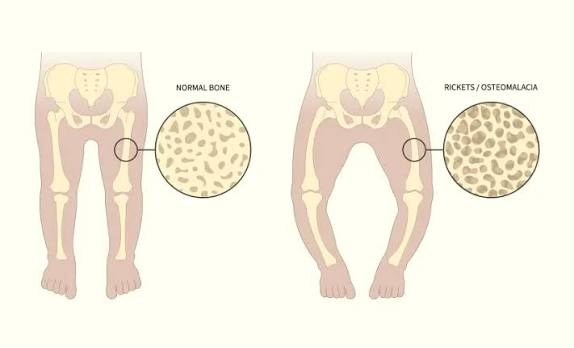
Osteomalacia - what is it and what causes it?
Radiographic appearance?
‘Soft bone’ - caused by vitamin D, calcium or phosphate deficiency
Radiographic appearance
incomplete fractures
smudgy/erased looking trabeculae due to decreased bone density
Looser zones (pseudofractures) appearing as lucent bands in the femoral neck
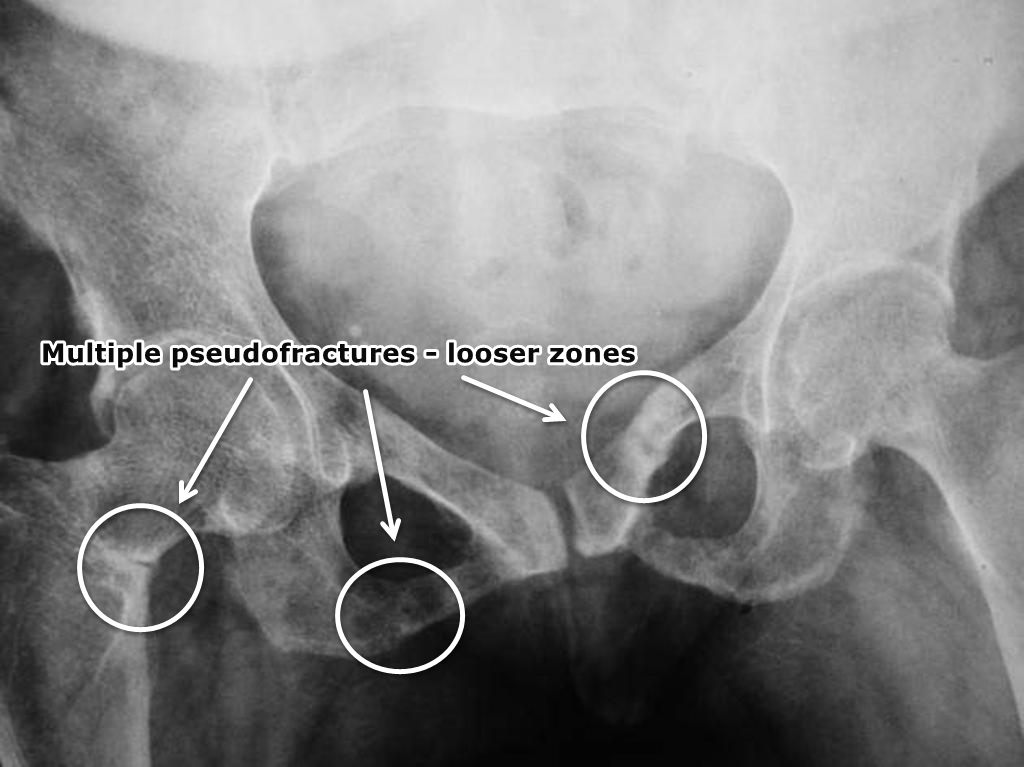
Patient presentation for osteomalacia - physical signs and symptoms
Physical signs
bowed legs
Waddling walk
Dull persistent bone pain
Symptoms
muscle weakness
Cramps
Fatigue
Which imaging methods can be use to diagnose osteomalacia?
CT, MRI, PET and X-ray
Osteosarcoma - what is it and what causes it?
Radiographic appearance?
Malignant bone cancer caused by genetic mutation. It is aggressive and can metastasize.
Radiographic appearance
can appear totally sclerotic (dense)
Lytic lesions
Patient presentation for osteosarcoma - physical signs and symptoms
Physical signs
lump near joint
Warmth
Easily brushing
Limping
Symptoms
weight loss
Fever
Persistent bone pain
Fatigue
What can be used to diagnose osteosarcoma?
CT, MRI, PET and X-ray
Preventing osteoporosis
Limit alcohol intake
Stop smoking
Take calcium and vitamin d supplements
Walk or jog regularly
Osteoporosis risk factors
Overconsumption of alcohol
Smoking
Lack of exercise
Lack of vitamin d and calcium
Poor diet
Genetics
Hormones