BCMB 230 UTK Exam 3
1/244
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
245 Terms
What Body Systems Affect the Cardiovascular System?
- Endocrine, nervous, and urinary systems
3 Main Components of Cardiovascular System
1: The Heart
2: Blood Vessels
3: Blood
Heart Component of Cardiovascular System
- The Pump Itself
Blood Vessels Component of Cardiovascular System
- Tubes carrying blood around the body
Blood Component of Cardiovascular System
- Liquid connective tissue containing many different nutrients and other products
The 3 Layers of the Heart
1. Epicardium
2. Myocardium
3. Endocardium
Epicardium
- Outer layer of the heart
- Made up of fibrous tissue
Myocardium
- Middle layer of the heart
- Muscular
Endocardium
- Inner layer of the heart
- Made of endothelial cells (continuous with the lining of blood vessels)
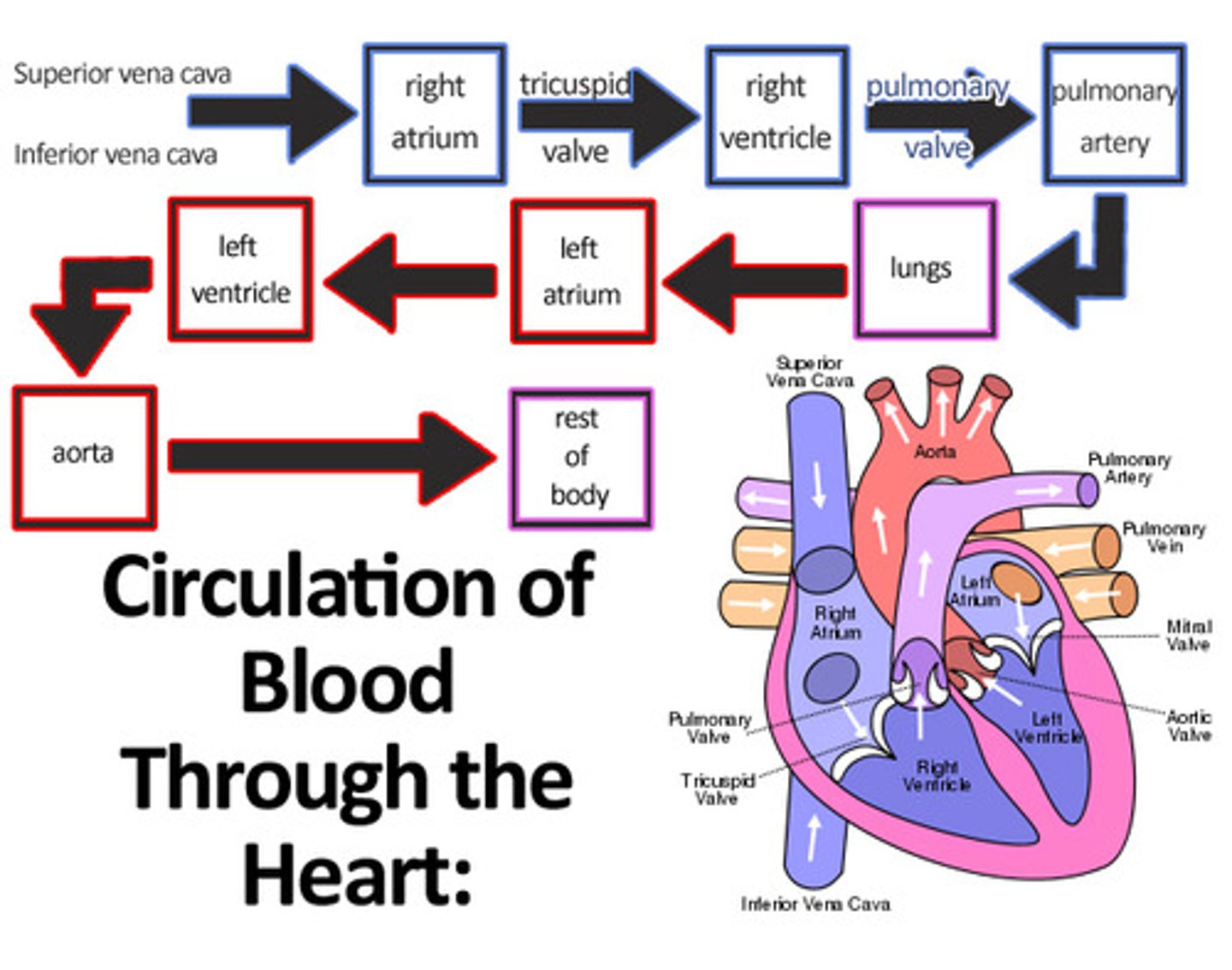
Blood Flow Through The Heart
Deoxygenated Blood
1-Superior & Inferior Vena Cava
2- Right Atrium
3-Tricuspid Valve
4- Rt Ventricle
5-Pulmonary Valve
6-Pulmonary Artery
7- Lungs pick up oxygen
Oxygenated Blood
8-Pulmonary Veins
9- Lt Atrium
10- Mitral Valve (Bicuspid)
11-Lt Ventricle
12- Aortic Valve
13- Aorta
14- Body tissues
Semilunar Valves
- Pulmonary valve and aortic valve
- Separate the ventricles from the great arteries
- Prevent back-flow of blood in heart
AV Valves
- Bicuspid (mitral) and Tricuspid valve
- Separate atria from ventricle
- Prevent back-flow of blood in heart
Atria
- At the top of the heart
Ventricles
- At the bottom of the heart
- Have thicker muscle walls so that they are stronger and can p
Chordae Tendineae
- "Strings" within the heart that hold the valves in place to prevent blood from flowing backward
- aka "heart strings"
Cardiac Output (CO)
- Volume of blood pumped out of the left ventricle in one minute.
Heart Rate (HR)
- Number of cardiac cycles (heartbeats) per minute
- Denoted in beats per minute (bpm)
Stroke Volume (SV)
- Amount of blood pumped out of the ventricles per heartbeat
- Denoted as (mL/beat)
Cardiac Output
- Heart Rate x Stroke Volume
- Overall performance of heart
Factors Affecting Heart Rate
- Autonomic innervation
- Hormones
- Fitness levels
- Age
Factors Affecting Stroke Volume
- Heart size
- Fitness levels
- Gender
- Contractility
- Duration of Contraction
- Preload (EDV)
- Afterload (resistance)
Blood Pressure
- Force that exerts on the blood vessel wall
- Difference in pressure in vessels allows for the flow of blood
2 Readings:
- Systolic (Top #): Systole represents ventricular contraction
- Diastolic (Bottom #): Represents ventricular filling
Blood Resistance
- Force that hinders blood flow
- Vessel diameter, length, and blood viscosity
Blood Flow
- Rate that blood moves through the vessel
- Blood Flow = Blood Pressure/Resistance
Cardiac Communication
- Contains excitable cells that make up the conducting system of the heart
- System initiates heartbeat and helps spread action potential throughout the heart
!! Communicate via gap junctions
2 nodes present:
1: SA node
2: AV node
SA node (sinoatrial node)
- The pacemaker of the heart
AV node (atrioventricular node)
- Receives signal from SA node to help ventricles contract
Conducting System of the Heart
- SA node -> AV node -> Bundle of His -> Left/Right Bundle Branches -> Purkinje fibers
First Step of Cardiac Excitation
1) The SA node sends signals to the AV node
Second Step of Cardiac Excitation
2) Atria becomes depolarized by the SA node and contracts
- AV node holds onto the signal for a moment to prevent atria and ventricles from contracting at the same time
Third Step of Cardiac Excitation
- AV node allows the signal to progress, and it is spread by the Purkinje fibers
Fourth Step of Cardiac Excitation
- Ventricles can now contract
Fifth Step of Cardiac Excitation
- Cyclical Process
Sequence of Cardiac Excitation and Reading an EKC
- P Wave
- QRS complex
- T wave
P Wave in an EKG
- Represents atrial depolarization
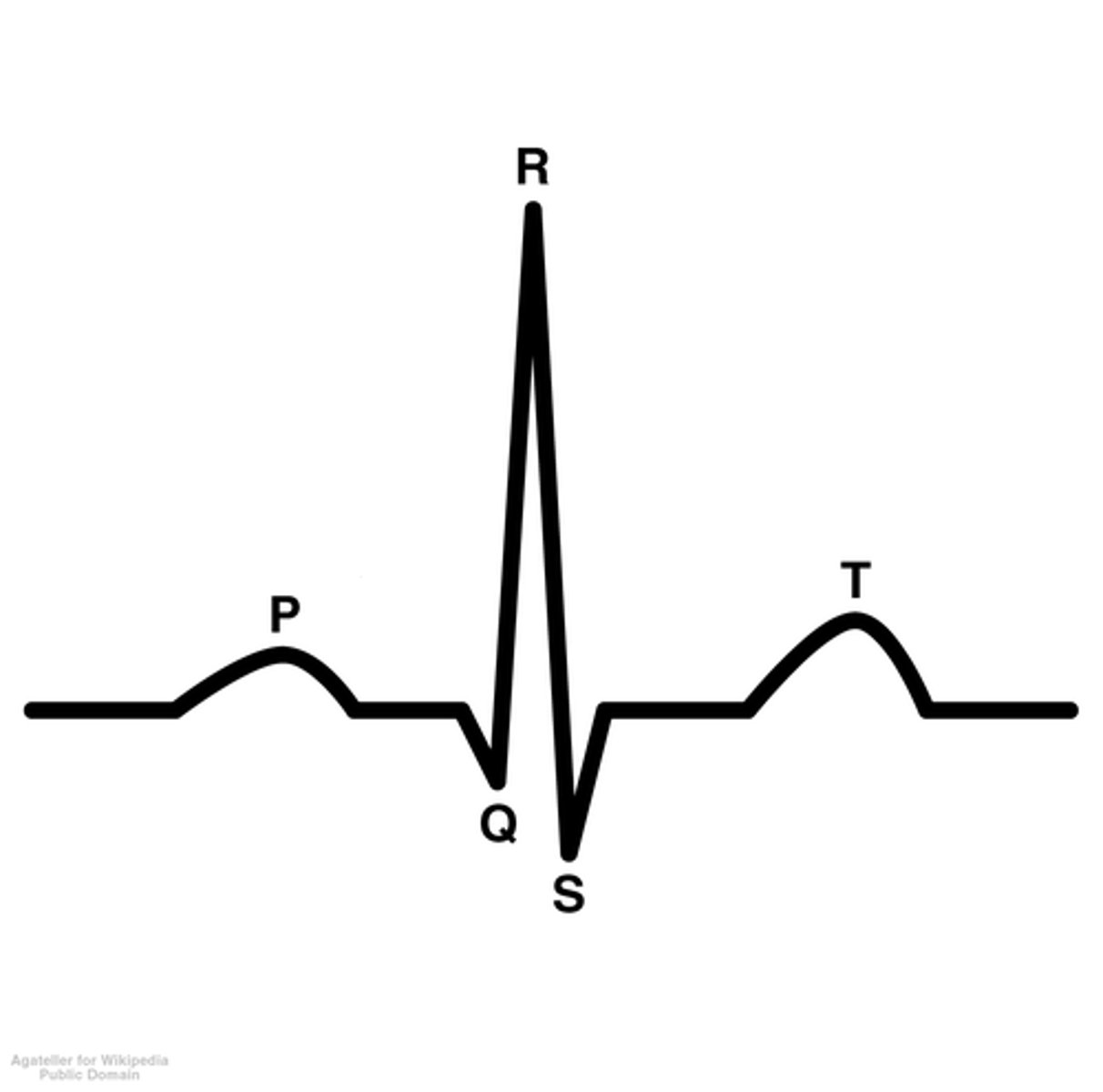
QRS Complex in an EKG
- Represents ventricle depolarization
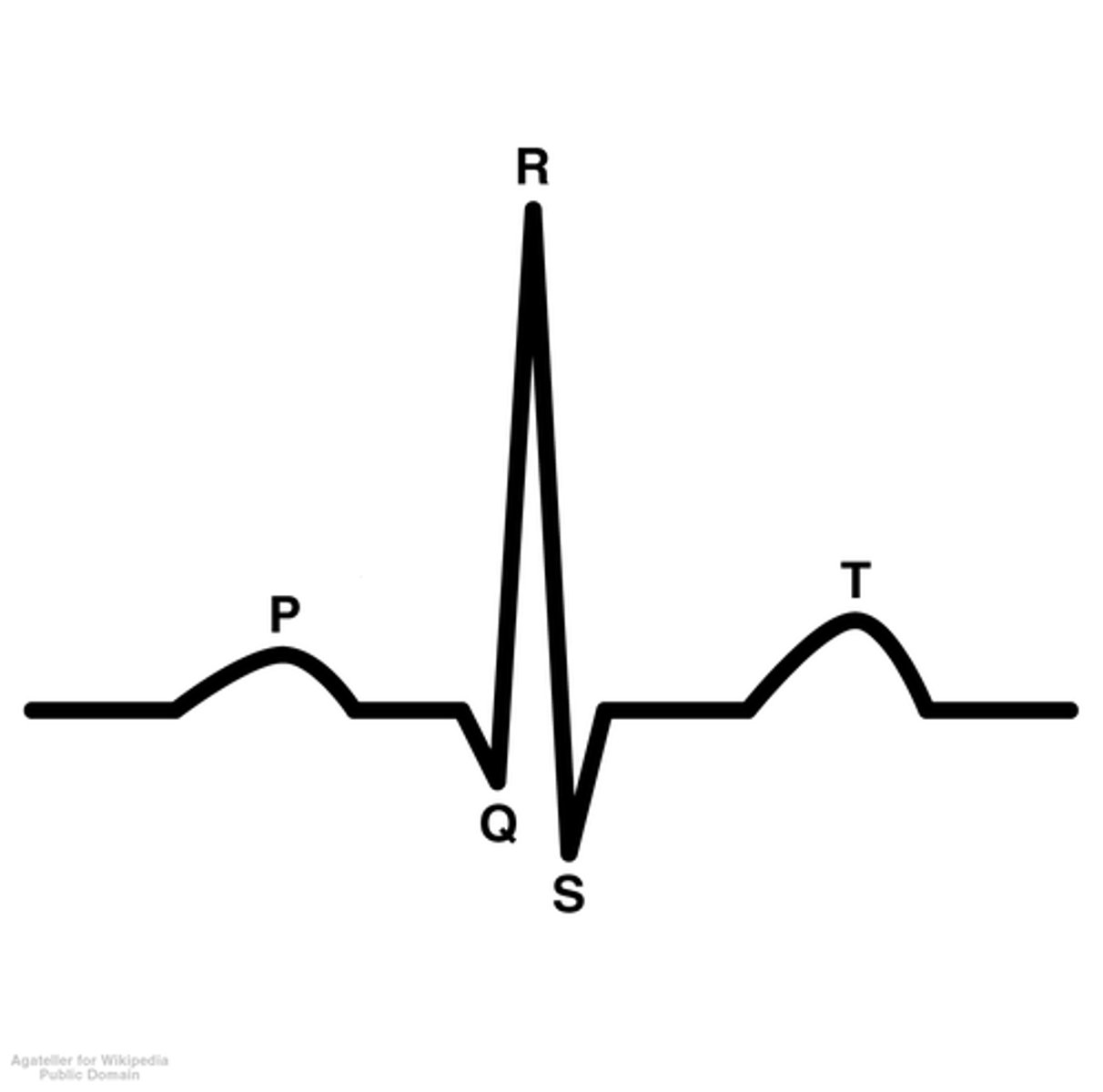
T Wave in an EKG
- Represents ventricle repolarization
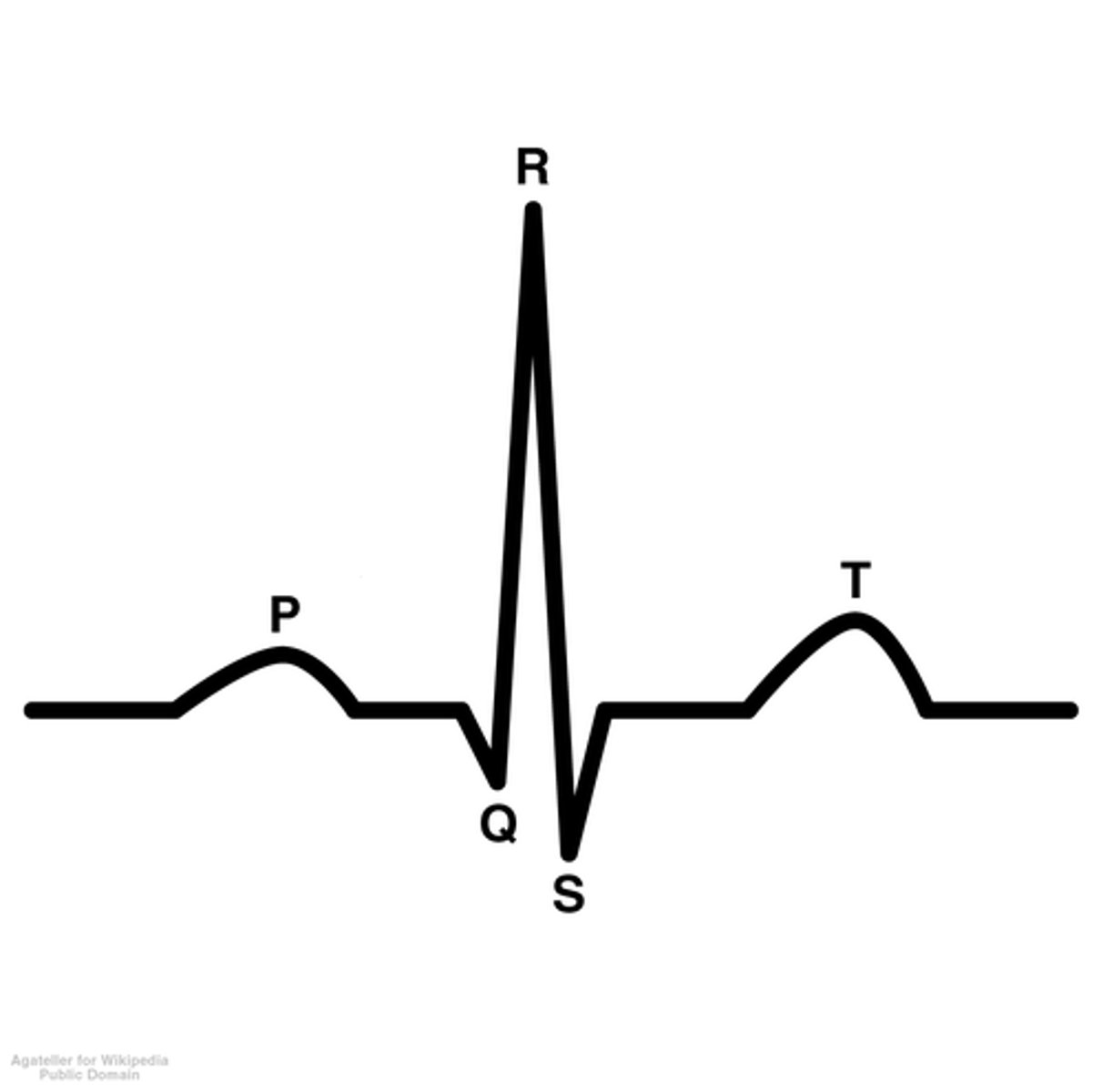
Arteries
- Carry O2- rich blood away from the heart
Veins
- Carry O2-poor blood toward the heart
Arterioles
- Small arteries
Venules
- Small veins
Capillaries
- Smallest of blood vessels
- Site of gas exchange
Veins vs. Arteries
Arteries:
- Contain thick muscular layers that contract to help move blood forward
- No valves
Veins:
- Do not have thick muscular layers
- Rely on surrounding muscles to contract and push blood
- Contain valves
!!! Both contain 3 layers
3 Layers of Veins and Arteries
1) Endothelium
2) Smooth Muscle
3) External Lamia
3 Types of Capillaries
1) Continuous
2) Fenestrated
3) Sinusoidal
Continuous capillaries
- Complete basement membrane
- Complete endothelial layer
- Found in the blood-brain barrier and skin
Fenestrated Capillaries
- Complete basement membrane
- Endothelial layer has holes in it to aid in diffusion
- Found in kidney, small intestine, spleen, and bone marrow
Sinusoidal Capillaries
- Incomplete basement membrane
- Large gap between cells
- In liver, spleen, bone marrow, and endocrine glands
Vasoconstriction
- Blood vessels shrink in diameter
- Raises blood pressure
Vasodilation
- Blood vessels increase in diameter
- Lowers blood pressure
Components of Blood
1) Formed Elements: 45% of blood
1a) Red Blood Cells (erythrocytes)
2b) White Blood Cells (Leukocytes)
3c) Platelets (Thrombocytes)
2) Plasma: 55% of blood
Blood Plasma
- Liquid portion of blood
- Carries blood cells, nutrients, proteins, metabolic wastes, and other molecules
Red blood Cells
- Small and flexible with no nucleus or organelles when mature
- Shaped like a biconcave disk (gives a high surface to volume ratio to aid in gas exchange)
- Function: Gas transport (both O2 and CO2)
- Contains hemoglobin- Protein that reversibly binds to O2 and CO2
Hemoglobin
- Spleen filters the blood and removes old RBCs, which are then sent to the liver to be broken down
- Iron is conserved and brought to the bone marrow by a protein called transferrin so it can be reused to make new RBCs
- Excess iron is stored in the spleen and liver by binding to a protein called ferritin
- Heme is converted into bilirubin
- Globulin proteins are broken down, and their AAs are reused
Jaundice
- Yellowing of skin caused by build-up of Bilirubin
Erythropoiesis
- Production of red blood cells in bone marrow
- Triggers differentiation of stem cells in bone marrow, signaling them to mature into RBCs
Erythropoetin
- Hormone made by the kidney which stimulates erythropoiesis
- Secreted in response to low O2 concentration in tissues (hypoxia)
White Blood Cells
- Made in bone marrow
- Function: All are immune cells that fight infection
2 Main Categories:
1) Granulocytes
2) Agranulocytes
Granulocytes
Neutrophils, eosinophils, basophils
- Contain granules in their cytoplasm
Agranulocytes
- Monocytes and lymphocytes
- Do NOT contain granules in their cytoplasm
Neutrophils
- Phagocytes whose release is stimulated during infection
- First to arrive at infection
- Found in blood and tissues
Eosinophils
- Fight infection by injecting their toxic granules into parasites
- Capable of phagocytosis
Basophils
- Secrete anti-clotting factor called heparin
- Also secrete histamine which attracts WBCs
Heparin
- Anticoagulant which makes you bleed longer to flush bacteria from wound
Monocytes
- Phagocytes that only circulate within the blood temporarily. - - Migrate into tissues and organs to later develop into macrophages to fight at the site of infection
Macrophages
- Large phagocytes capable of engulfing viruses and bacteria
Lymphocytes
- Two main types (T and B Lymphocytes that protect against specific viruses, bacteria, toxins, and cancer cells
Platelets
- Non-nucleated cell fragments containing numerous granules
- Causes blood clotting
Makeup of Blood Plasma
~ 91% water
- 7% proteins: Albumins, Globulins, Fibrinogen, other specialized enzymes and proteins
2% other solutes:
- Electrolytes: Na+ and K+
- Nutrients: AAs and lipids
- Gases: O2 and CO2
- Wastes: Bilirubin and Urea
- Vitamins
- Regulatory Substances
Albumins
- Aid in transport of other proteins
Globulins
- Antibodies
Fibrinogen
- Clotting factor
Hemostasis: Blood Coagulation
1) Vascular Spasm
2) Formation of Platelet Plug
3) Platelet Plug/Clot Formation
Vascular Spasm
- Cells contract and release chemicals to make muscles within the walls of the blood vessel contract in response to damage to endothelial cells
- Results in cell division and release of other proteins that attract other blood cells to the area.
- Release Von Willebrand Factor, which makes endothelial cells "sticky" so that recruited cells can begin to seal up damaged blood vessel
Formation of Platelet Plug
- Platelets begin to adhere to the Von Willebrand Factor.
- Begin to aggregate and form a Platelet plug, further sealing the area.
- Forms thrombus which mostly consists of a protein called fibrin
Protein that Forms Most of the Thrombus
- Fibrin
Platelet Plug/Clot Formation
- Blood coagulates, forming a scab and sealing the injured blood vessel.
- A protein called fibrin stabilizes the clot and keeps it in place
Blood pH
- 7.35-7.45
- Slightly Basic
- CO2 is the body's acid
- Bicarbonate is the body's base
2 Parts of the Circulatory System
1. Pulmonary circulation
2. Systemic circulation
Pulmonary Circulation
- Flow of deoxygenated blood from heart to lungs so it can be reoxygenated
Systemic Circulation
- Flow of oxygenated blood from the heart to the body and the return of deoxygenated blood from the body back to the heart
Arteries vs. Veins
Arteries: Carry blood AWAY from the heart
Veins: Carry blood to the heart
Pulmonary Artery
- Transfers O2-Poor blood away from heart to the lungs
Pulmonary Vein
- Carries O2-rich blood from lungs back to the heart so it can be circulated
Diffusion Gradients
- Drives the movement of gases, nutrients, and waste into and out of the bloodstream
- Osmotic gradients drive diffusion
Regulation of the Cardiovascular System
- Autoregulation
- Neural Mechanisms
- Endocrine Mechanisms
Autoregulation
- Local vasodilators (O2 and CO2) and constrictors (chemicals released by damaged tissues)
Neural Mechanisms
- Medulla can control heart rhythm, blood flow, and gas levels in the blood
Short Term Endocrine Mechanisms
- Epinephrine and norepinephrine
Long Term Endocrine Mechanisms
- Erythropoietin (hormone telling bone marrow to make RBCs)
Congestive Heart Failure
- Heart is unable to pump its required amount of blood
Arrythmia
- Abnormal heart rhythm
Myocardial Infarction (Heart Attack)
- Part of the heart dies because an artery becomes clogged and blocks the blood supply to the myocardium
Atherosclerosis
- The build-up of fats, cholesterol, and other substances in and on the artery walls.
Arteriosclerosis
- Hardening of arteries
- Makes arteries less effective at pumping blood
Arteriostenosis
- Narrowing of the lumen of an artery
Anemia
- Decrease in O2-carrying capacity of blood
- Reduced concentration of hemoglobin
Sickle Cell Anemia
- Genetic mutation resulting in one amino acid change and, therefore, changing the shape of hemoglobin into a sickle
- Painful and can also block blood vessels
Apnea
- Cessation of breathing
Dyspnea
- Labored breathing