Anatomy- Chp 5
1/124
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
125 Terms
functions of the skeletal system
support, mineral storage, blood cell production, protection, leverage
support
framework for body and soft tissues
mineral storage of skeletal system
stores Ca2+ and phosphate (98& of body calcium in bones0
blood cell production of skeletal system
hematopoiesis; occurs in red bone marrow
protection
_____ of skull (brain), ribs (heart/lungs), vertebrae (spinal cord)
leverage of skeletal system
bones act as levers for muscle movement
bone (osseous) tissue
specialized connective tissue
components of osseous tissue
cells, protein fibers, extracellular matrix hardened by calcium salts
covered by periosteum (outer surface)
lined internally by endosteum
bone matrix
2/3 inorganic, 1/3 organic- combo= strong but not brittle
inorganic bone matrix
calcium phosphate, hydroxyapatite crystals- provides compression resistance
organic bone matrix
collagen fibers, proteins- provides tensile strength and flexibility
lamellae
layers of calcified matrix
lacunae
spaces holding osteocytes
canaliculi
tiny channels connecting lacunae
bone cells
osteocytes, osteoblasts, osteoproginator cells, osteoclasts
osteocytes
mature bone cells
maintain matrix
regulate calcium exchange
osteoblasts
bone- forming cells
secrete osteoid
responsible for osteogenesis
osteoproginator cells
stem cells
differentiate into osteoblasts
important for growth and repair
osteoclasts
bone-resorbing cells
break down bone via osteolysis
release calcium into blood
strength
bone ____ depends on balance between osteoblasts and osteclasts
compact bone
dense, strong
made of osteons (Haversian systems) → central canal (blood vessels), perforating (volkmann’s) canal (connect canals)
best at resisting force in one direction
spongy bone
cancellous/trabecular
lattice of trabeculae
lighter, more flexible
resists stress from many directions
contains red marrow
ossification
bone formationt
types of ossification
intramembranous ossification, endochondral ossification
intramembranous ossification
bone develops from mesenchyme; forms- flat bones of skull, face, clavicle
endochondral ossification
bone replaces hyaline cartilage model; forms- long bones, vertebrae
length bone growth
occurs at epiphyseal cartilage (growth plate)
stops at epiphyseal closure
leaves epiphyseal line
diameter bone growth
appositional growth
osteoblasts add bone to outer surface
osteoclasts remove bone from inner surface
medullary cavity enlarges as bone thickens
blood and nerve supply
nutrient artery and vein- diaphysis
metaphyseal vessels- near growth plate
epiphyseal vessels- epiphyses
periosteal vessels- outer bone surface
bones are highly innervated → fractures are painful
factors regulating bone growth
minerals
vitamins
PTH
calcitonin
GH, thyroxine, sex hormones
bone minerals
calcium, phosphate, magnesium
vitamin A
in bone growth; osteoblast activity
vitamin C
in bone growth; collagen synthesis
vitamin D3
in bone growth; calcium absorption
PTH
hormone; in bone growth; increases osteoclast activity
Calcitonin
hormone; in bone growth; inhibits osteoclasts
GH, thyroxine, sex hormones
hormone; in bone growth; stimulates growth
bone maintenance
bone is constantly remodeled; 20% of adult skeleton replaced each year
bone remodling
responds to stress (exercise increases bone mass); lack of stress → bone loss
bone fracture repair
requires intact blood supply, periosteum, endosteum; healed bone is usually stronger at repair site
osteopenia
reduced bone mass (normal aging0
osteoporosis
severe bone loss → fracture risk
faster
women lose bone ___ than men after 30-40 years
bone shape categories
long
short
flat
irregular
sesamoid
sutural (wormian)
pneumatized
bone markings
used for identification and anatomical landmarks
projections
muscle/ligament attatchment
depressions/openings
nerves and vessels
integration with other systems
muscular- movement
cardiovascular- blood supply
endocrine- hormone regulation
digestive & urinary- mineral balance
skeleton acts as mineral reservoir
bone marrow transplant
Transferring healthy bone marrow stem cells from one person into another to replace bone marrow that either is dysfunctional or has been destroyed by chemotherapy or radiation.
bone mineral density test (BMD)
A test to predict the risk of bone fractures by measuring how much calcium and other types of minerals are present in the patient's bones.
closed reduction
The correction of a bone fracture by manipulation without incision into the skin
open reduction
The correction of a bone fracture by making an incision into the skin and rejoining the fractured bone parts, often by mechanical means such as a rod, plate, or screw.
orthopedics
The branch of medicine dealing with the correction of deformities of bones or muscles.
osteogenesis imperfecta (OI)
An inherited (genetic) disorder characterized by extreme fragility of the bones; also called brittle bone disease.
osteomyelitis
An acute or chronic bone infection.
osteopertrosis
A rare hereditary bone disorder in which the bones become overly dense; it presents in one of three forms: osteopetrosis tarda, osteopetrosis congenita, or “marble bone” disease.
osteosarcoma
A type of cancer that starts in the bones; also called osteogenic sarcoma.
paget’s disease
A chronic disorder that can result in enlarged and misshapen bones due to abnormal bone destruction and regrowth.
traction
The application of a sustained pull on a limb or muscle in order to maintain the position of a fractured bone until healing occurs or to correct a deformity.
skeletal system
skeleton
cartilage
ligaments
axial skeleton
skull, thoracic cage, spine
appendicular skeleton
limbs, pectoral girdle, pelvic girdle
functions of skeleton
support: framework for attachment of other organs
movement/locomotion: muscles use bones as levers
storage of minerals (calcium ions, phosphate ions)
blood cell production (hematopoiesis)
protection
skull protects brain
ribs protect heart and lungs
vertebrae protect spinal cord
pelvic bones protect reproductive organs
hematopoiesis
blood cell production; bone marrow produces erythrocytes, leukocytes, and platelets
osseous tissue
matrix of bone consists of
hydroxyapatite
collagen fibers
bone cells
hydroxyapatite crystals
mainly calcium phosphate (and calcium hydroxide) will resist compression, but inflexible; 2/3 of bone mass
collagen fibers
contribute to tensile strength of bones; imparts limited flexibility to matrix; 1/3 of bone mass
bone cells
2% of bone mass
intramembranous ossification
produces the roofing bones of the skull
endochondral ossification
replaces cartilages of embryonic skull
primary ossification
centers of the diaphyses (bones of lower limb)
steps of intramembranous ossification
differentiation of osteoblasts within mesenchyme
formation of bony spicules
entrapment of blood vessels
formation of spongy bone
differentiation of osteoblasts within mesenchyme
Mesenchymal tissue becomes highly vascularized (many blood vessels form).
Mesenchymal cells cluster, enlarge, and differentiate into osteoblasts.
Osteoblasts group together and begin secreting the organic bone matrix (osteoid).
Osteoid mineralizes as calcium salts crystallize within it.
The site where bone formation begins is called an ossification center.
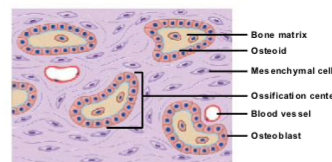
formation of bony spicules
As ossification continues, osteoblasts surrounded by osteoid become osteocytes.
Osteocytes remain trapped in small spaces called lacunae.
Bone grows outward from the ossification center in small structures called spicules.
More mesenchymal cells divide and differentiate into osteoblasts, allowing bone formation to continue.
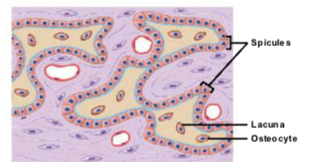
entrapment of blood vessels
Bone growth is an active process, so osteoblasts need oxygen and nutrients.
Blood vessels branch and grow between the spicules, increasing the rate of bone growth.
As spicules connect, they trap blood vessels within the developing bone.
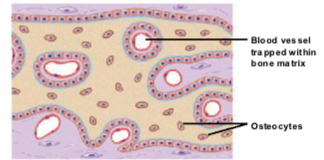
formation of bony spicules
Osteoblasts continue depositing bone, forming a bony plate.
The plate is perforated by blood vessels.
As adjacent plates fuse together, the bone structure becomes more complex.
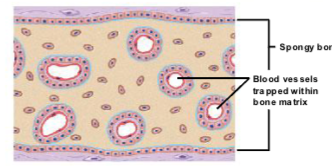
steps of endochondral ossification
cartilage calcification and cartilage death
formation of bone collar
formation of primary ossification center
formation of medullary cavity
formation of secondary ossification centers
formation of epiphyseal plate and bone lengthening
epiphyseal closure
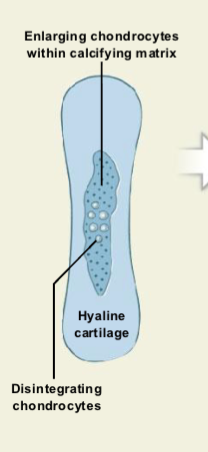
Cartilage Calcification and Chondrocyte Death
Cartilage model enlarges as chondrocytes grow bigger.
The surrounding cartilage matrix begins to calcify.
Calcification cuts off nutrient supply.
Chondrocytes die and break down, leaving empty cavities in the cartilage.
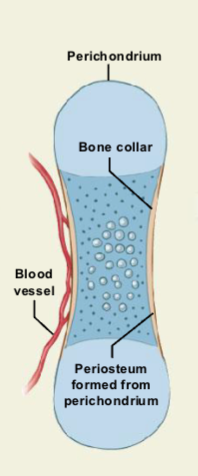
Formation of the Bone Collar
Blood vessels grow around the outer cartilage.
Perichondrium cells differentiate into osteoblasts.
The perichondrium becomes the periosteum.
Osteoblasts form a bone collar (thin compact bone layer) around the shaft.
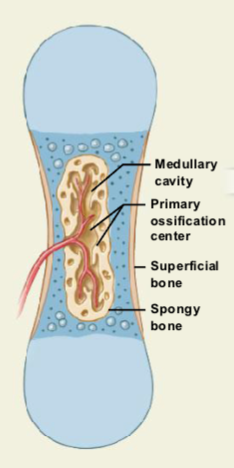
Formation of the Primary Ossification Center
Blood vessels and osteoblasts invade the center of the cartilage.
They enter the spaces left by dead chondrocytes.
Calcified cartilage breaks down.
Osteoblasts replace cartilage with spongy bone.
Bone formation spreads from the primary ossification center in the shaft toward both ends.
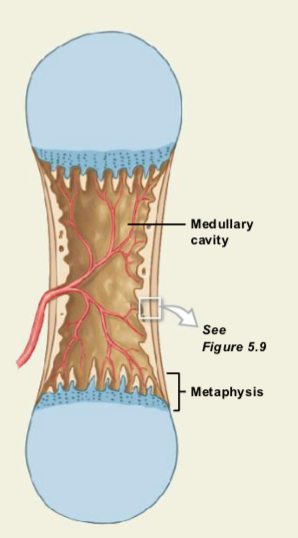
Formation of the Medullary Cavity
The shaft initially fills with spongy bone.
Osteoclasts break down bone in the center.
This creates the medullary (marrow) cavity.
The shaft becomes thicker while bone continues forming near the metaphysis.
Formation of Secondary Ossification Centers
Capillaries and osteoblasts enter the epiphyses (ends of the bone).
Secondary ossification centers form in these regions.
The timing varies by bone and individual.
Some bones have these centers present at birth, while others remain cartilage during childhood.
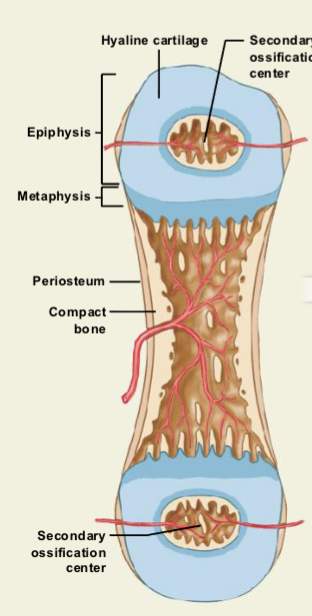
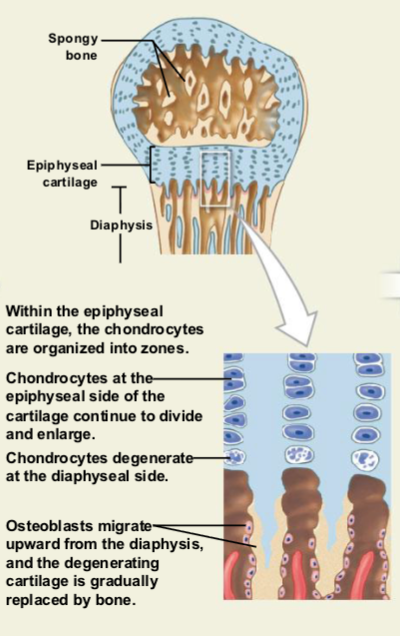
Formation of the Epiphyseal Plate and Bone Lengthening
The epiphyses fill with spongy bone.
A layer of cartilage called the epiphyseal plate remains between the epiphysis and diaphysis.
Cartilage grows on the epiphyseal side, while osteoblasts replace cartilage with bone on the diaphyseal side.
This process pushes the epiphysis away from the shaft, causing the bone to grow in length.
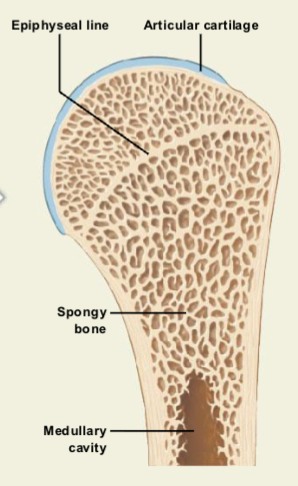
Epiphyseal Closure
At maturity, cartilage growth slows while osteoblast activity increases.
The epiphyseal plate becomes thinner and eventually disappears.
This is called epiphyseal closure, ending bone length growth.
The remaining mark is the epiphyseal line, and articular cartilage remains at the joint surface.
achondroplasia
A genetic disorder that causes short-limbed dwarfism because bones don’t grow normally, especially in the arms and legs. It happens when cartilage doesn’t properly turn into bone during growth.
Key idea: normal torso size but short arms and legs due to abnormal bone development.
osteocyte
mature bone cell that maintains the bone matrix
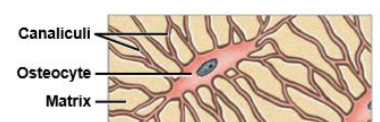
osteoblast
immature bone cell that secretes osteoid, the organic bone matrix
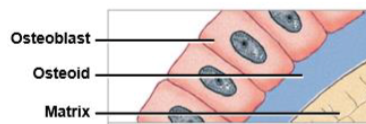
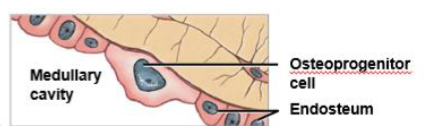
osteoproginator cell
stem cell that divides to produce osteoblasts
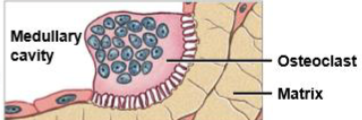
osteoclasts
multinucleate cell that secretes acids and enzymes to dissolve bone matrix
osseous tissue types
compact bone
spongy bone
compact bone
dense bone
dense and solid
forms walls of bone
parallel compression
spongy bone
trabecular bone
open network of plates
multidirectional or light train
surrounds medullary cavity
bone marrow: connective tissue in medullary cavity
epiphysis
ends of long bones
diaphysis
shaft of long bones
metaphysis
transition between epiphysis and diaphysis
medullary cavity
inner cavity of diaphysis; houses bone marrow
epiphyseal line
growth line
periosteum
membrane on outer surface of bone
fibrous layers and osteogenic layer (complete, multi cell layer)
isolates and protects bone from surrounding tissue
attachment for circulatory and nervous supply
actively participates in bone growth and repair
attachment site for tendons and ligaments
perforating fibers
anchors periosteum to bone and other connective tissues
endosteum
membrane on inner surface of bone; single, incomplete layer
line medullary cavity perforating canals and central canals