HCMC Chemistry Critical Competencies
1/65
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
66 Terms
List the types of pipettes and pipetting devices used
Volumetric (transfer)
Mohr (measuring)
Serological (measuring)
Micropipettes/mechanical
Bulb
Pipette pump
Propipette
Describe the volumetric pipette
Designed to deliver a single volume with high accuracy.
Consists of a cylindrical bulb joined at both ends to narrow glass tubing.
Colored bands on the top of the pipette denote the volume that is dispensed. These
are used when reconstituting QC and calibrators
Above the bulb is a calibration mark (ring). Fluid must be drawn up the pipette to above the ring and then released slowly until the bottom of the meniscus is exactly at the ring. To transfer the volume, touch the pipette tip to the inside of the container and allow liquid to drain out (do not blow the remaining drop out).
Several sizes (1,2 and 5 mL).

Describe Mohr (measuring) pipettes
these pipettes are graduated but stop at a baseline before the pipette begins to narrow (tip).
To accurately transfer fluid, the meniscus must be
precisely on a mark both at the beginning and end of transfer.

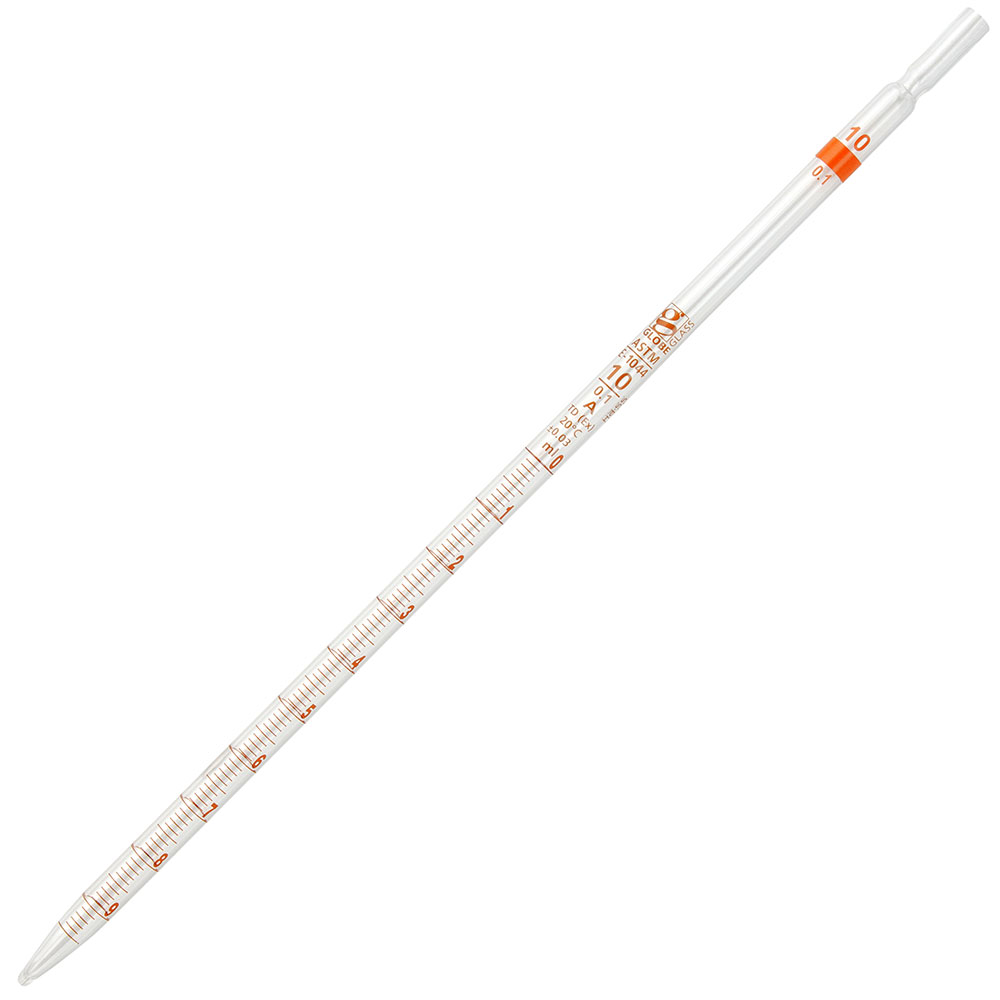
Describe serological (measuring) pipettes
Graduated so that multiple volumes can be delivered.
Typical volume range from 0.2 mL to 10mL and have graduation marks that continue
to the tip. These are blown out.
Calibrated TD (to deliver) with etched rings at the top.
Several sizes: 5, 10, 25.
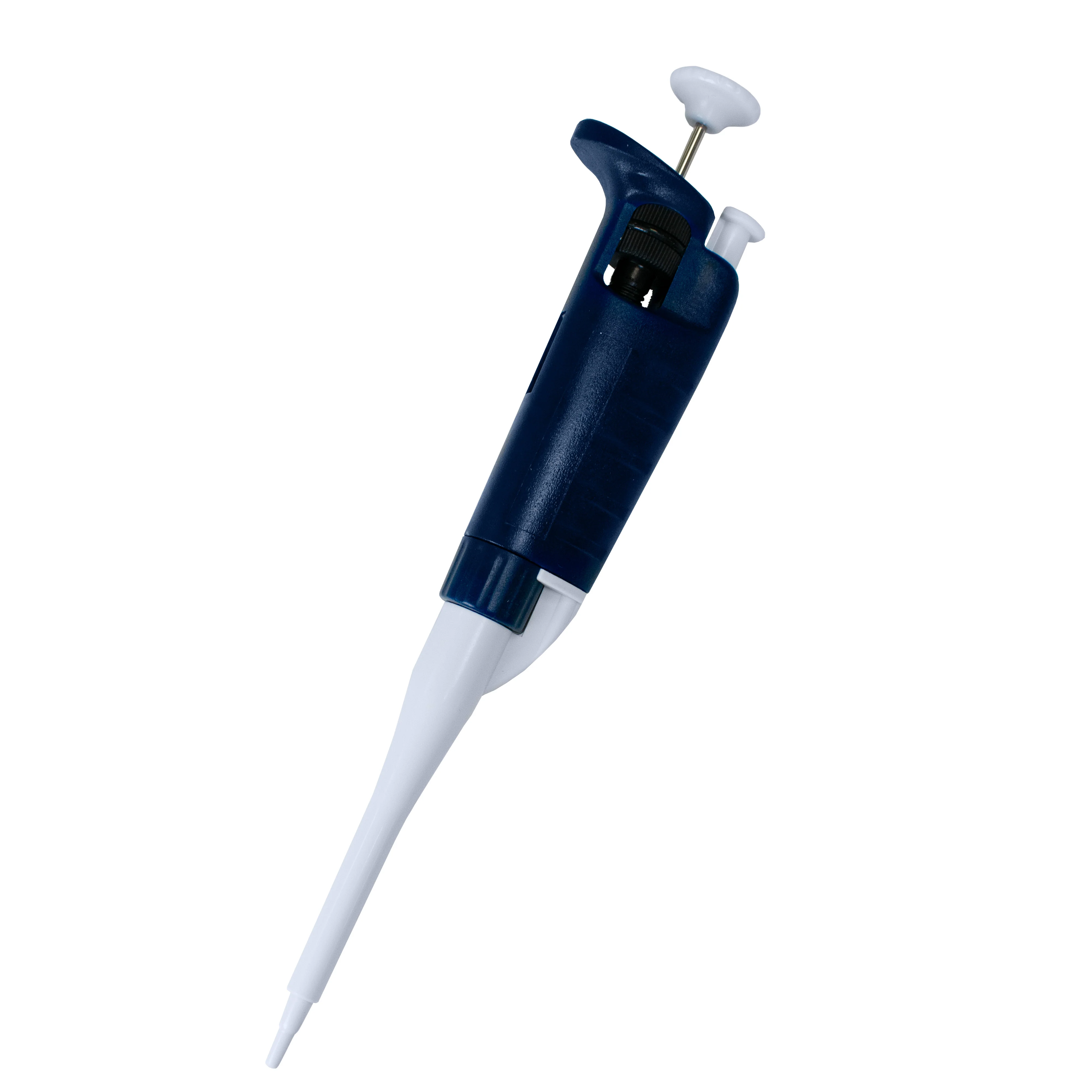
Describe micropipettes/mechanical
can be set to drawn and dispense different volumes.
This is done by turning the knob at the top. The tips are disposable.To draw liquid up, depress the plunger to the first stop and immerse the tip into the liquid. Release
the plunger back to the rest position. Depress the plunger to the first stop and then press the plunger to the second stop to expel all the liquid
Describe the pipette bulb
Hand squeeze the bulb and touch the opening to the mouth of the pipette. Insert into the liquid and slowly release pressure.
Liquid will be drawn up into the pipette, and pull the bottom of the meniscus up past
the desired level.
Quickly remove the bulb as you slip your free index finger over the
top of the pipette.
Lift out of the solution and twist until desired level.
Remove finger and allow the pipette to drain.
Touch tip to the inside of the container after all liquid has been drained.

Describe the pipette pump
insert pump to end of the pipette.
Put the tip into the solution and turn the wheel with your thumb to draw up liquid.
Press on the wheel gently to hold the liquid in the pipette until you are ready to expel it.
To expel the fluid, turn the wheel in the opposite direction.
Touch the tip of the pipette to the flask to drain the last bit of liquid

Describe propipette
Use your thumb and forefinger to press on valve "A" and squeeze the bulb with other fingers to produce a vacuum for aspiration.
Release valve "A" once the bulb is completely deflated.
Hold the pipette close to its upper end and insert into the bottom of the
propipette.
Insert the pipette into the liquid to be transferred. Press on valve "S". Suction will draw liquid up into the pipette.
Continue pressing valve "S" until the liquid reaches the desired level.
Carefully adjust the fluid level so that the bottom of the meniscus coincides
with the calibration line on the pipette.
Press on valve "E" to expel liquid

Reading micropipettes and volumes
never rotate the volume adjustment knob past the upper or lower range of the pipetman
look at the front of the pipette and you will see a window with digits inside.
Examples:
P1000 reads 040 = 400 uL
P20 reads 125 = 12.5 uL
P100 or 200 reads 100 or 200 = 100 uL or 200 uL
P20 ranges from 2-20 uL
P200 ranges from 20-200 uL
P1000 ranges from 200-1000 uL (1 mL)
Pre-analytical variable and sample requirements
Dilutions
Define glycogen
polysaccharide that is major storage form of glucose in liver and muscles
What is the function of glycogen
main function is to store chemical energy in the liver and muscles for later use.
Glycogen is converted from glucose for storage and broken down into glucose when energy is needed.
How does the body regulate glycogen
Regulated through the formation of glycogen from glucose (glycogenesis) stimulated by insulin and the breakdown of glycogen into glucose (glycogenolysis) stimulated by glucagon.
Glycogenesis = Glucose + insulin = glycogen
Glycogenolysis = Glycogen + glucagon = Glucose
Define glucagon
A hormone produced by alpha-cells of islets of Langerhans of pancreas
What is the function of glucagon
Increases blood glucose (hyperglycemic agent) and stimulates the liver to release stored glycogen as glucose.
Helps maintain plasma glucose levels by increasing them when they are low and prevents insulin from decreasing levels too low.
Increases blood glucose levels by stimulating the release of glycogen
How does the body regulate glucagon
Regulated through levels of blood glucose.
When blood glucose is low, increased levels are seen
When blood glucose is high, decreased levels are seen
Define glucose
Monosaccharide (simple sugar) utilized as the body’s main source of energy
What is the function of glucose
Functions to provide energy for metabolic processes
How does the body regulate glucose
Regulated through hormones such as insulin (decreases levels) and glucagon (increases levels).
Define insulin
Pancreatic enzyme secreted by beta cells of the islets of Langerhans
What is the function of insulin
Controls metabolism of sugars and is principal hormone responsible for decreasing blood glucose
Lowers glucose levels when they are elevated
How does the body regulate insulin
Regulated through blood glucose levels
When blood glucose is increased, increased levels are seen
When blood glucose is decreased, decreased levels are seen
Lipid structure
A class of extremely hydrophobic organic compounds.
Made primarily out of carbon, hydrogen, and oxygen.
Classified into five classes
sterol derivatives
fatty acids
glycerol esters
sphingosine derivatives
terpenes.
Define HDL
the smallest and most dense lipoprotein that make up 15-20% of total cholesterol.
“good cholesterol”
What is the function of HDL
Functions to return cholesterol to the liver for extraction
Define LDL
Class of lipoproteins that are principal carriers of cholesterol, accounting for approximately 70% of total cholesterol in plasma
“Bad cholesterol”
What is the function of LDL
Function to transport cholesterol in the plasma to peripheral tissues
Define VLDL
Class of lipoproteins that are primarily transporters of endogenous triglycerides from liver to muscles and adipose cells
contain greater lipid-to-protein ratio and are least dense of lipoproteins.
What is the function of VLDL
Functions to transport endogenous triglycerides from the liver to muscle and adipose tissue
Define cholesterol
Sterol that contains 27 carbon atoms and four fused rings (A, B, C, and D) called a perhydrocyclopentanophenathrene nucleus
The primary sterol derivative from lipids
What is the function of cholesterol
serves as a structural component of cell membranes and a precursor for bile acids, vitamin D, and steroid hormones (cortisol, aldosterone, progesterone, estrogen, and testosterone).
Define chylomicrons
largest and least dense (<0.94) of lipoprotein classes; formed from lipids absorbed in intestines
What is the function of chylomicrons
Transports exogenous triglycerides from the intestines to the liver and peripheral cells
Define triglycerides
the most common glycerol esters in plasma, comprising glycerol and three fatty acids
What is the function of triglycerides
Functions as the main storage of energy in the body
main storage of energy in the bod
Lipid digestion and absorption
Lipid- fatty acid catabolism and anabolism
lipid- cholesterol and metabolism
lipids- lipoproteins
Define acid-base balance
the maintenance of homeostasis of the hydrogen-ion concentration of body fluids
Describe buffer systems of the blood
First line of defense to a deviation in homeostasis due to the resistance of pH changes.
The blood buffers included in the body are
bicarbonate
hemoglobin
phosphate
protein.
Bicarbonate is the most important buffer system due to the large amount of CO2 and the acid potential of the body
Describe the roles of the respiratory system and kidney’s in acid-base balance
Respiratory system:
Eliminates CO2
moves air in and out (external convection)
Consists of the lungs, airway, and respiratory muscle that maximize gas exchange
maintains high external PO2 and low external PCO2
Circulatory system
internal convection system
Delivers blood with a low PO2 and high PCO2
Kidneys
Maintains pH through excretion
Exchanges Na+ and H+
Produces and excretes ammonia
reclamation of HCO3-
Describe factors contributing to acidosis and alkalosis
Development is due to an imbalance of acid-base concentrations.
Acidosis:
Factors that influence acidosis include…
the accumulation of acids or a loss of extracellular buffers.
This can be caused by conditions, such as severe diarrhea, abdominal fistulas, renal failure, or diabetes mellitus.
Alkalosis
results from an accumulation of alkalis or a reduction of acids.
This can be caused by many factors, such as vomiting, hypocalcemia, bicarbonate retention, or diuretics.
Define ALT
An intracellular enzyme involved in amino acid metabolism
catalyzes the transfer of an amino group from alanine to α-oxoglutarate
present in high concentrations in the liver and one of the analytes measured in a liver function profile
What disease states is ALT elevated?
Elevated levels are seen in…
hepatitis C
alcoholic hepatitis
choledocholithiasis
cirrhosis
Define ALP
Enzyme with an optimal pH of 9.0–10.0
frees inorganic phosphate from an organic phosphate monoester
present in highest concentration in the cells of the biliary tract and osteoblasts, so elevated levels are present in obstructive liver disease and various bone disorders
What disease states is ALP elevated?
Elevated levels are seen in…
primary sclerosing cholangitis
primary biliary cirrhosis
hepatitis
Define AST
One of a group of enzymes that catalyze interconversion of amino acids and α-oxoacids by transfer of amino groups
catalyzes deamination of aspartate to oxalacetate
highest levels found in…
liver
muscle
brain
Its measurement is included in liver function profile
What disease states is AST elevated?
Elevated levels are seen in…
Alcoholic hepatitis
choledocholithiasis
primary sclerosing cholangitis
NAFLD.
Define amylase
Class of enzymes that catalyze the hydrolysis of starch
two main sources of amylase are the pancreas and salivary glands, so serum levels are elevated in pancreatic and salivary gland disorders
What disease states is amylase elevated?
Elevated levels are seen in…
acute pancreatitis
chronic pancreatitis
Define GGT
Membrane-associated enzyme that transfers γ-glutamyl group from glutathione and other γ-glutamyl peptides to amino acids or small peptides to form γ-glutamyl amino acids and cysteinyl-glycine
What disease states is GGT elevated?
elevated in various conditions involving hepatic damage, especially hepatobiliary, and may also indicate alcohol or drug toxicity.
Elevated levels are seen in…
primary biliary cirrhosis
hepatitis
NAFLD.
Define direct bilirubin
bilirubin conjugated by UDP-glucoronyl transferase that adds two glucuronic acid molecules
water soluble and excreted in urine
What disease states is direct bilirubin elevated elevated?
Elevated levels are seen in…
hepatitis
cirrhosis.
Define BUN and its functions
nitrogen found in urea as distinguished from nitrogen in other blood proteins.
Functions as a measurement for renal function
What disorders are increased or decreased levels of BUN seen?
Elevated levels of BUN are seen in…
dehydration
congestive heart failure
acute glomerulonephritis
acute renal failure
nephrotic syndrome
acute kidney injury
Decreased levels are seen with…
severe liver disease
overhydration
pregnancy
SIADH
Define and describe the function of creatinine
product formed by breakdown of creatine phosphate
functions as a measurement to assess renal function
What disorders are increased or decreased levels of creatinine seen?
Elevated creatinine levels are because of prerenal, renal, and postrenal causes.
Elevation is seen in…
acute glomerulonephritis
acute renal failure
Decreased levels are seen with…
low muscle mass
Define and describe the function of microalbumin
excretion of minute amounts of albumin in urine, too small to be detected by reagent dipsticks
Functions as a measurement used to detect early onset renal disease
What disorders are increased or decreased levels of microalbumin seen?
Increased microalbumin levels are seen in…
diabetic nephropathy.
Define and describe ammonia
product of amino acid and protein catabolism that is converted to urea in liver by Krebs–Henselheit urea cycle
functions to assess renal function
What disorders are increased or decreased levels of ammonia seen?
Ammonia is elevated in cases of…
impending hepatic coma
advanced liver disease
acute viral hepatitis
severe gastrointestinal bleeding
chronic hepatitis
Reye’s syndrome.
Define and describe the function of potassium
A primary cation electrolyte found in the body
functions as a measurement for tubular reabsorption status
What disorders are increased or decreased levels of potassium seen?
Elevated potassium levels are seen in…
pseudohyperkalemia
leukocytosis
vigorous arm exercise
metabolic acidosis.