ECMO / Bypass / Dialysis
1/54
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
55 Terms
Hyper, metabolic acidosis, blood volume, uremia, albumin
Patient with hx ESRD vitals and key findings
__kalemia
__ __ (acid base state)
__ __ overload
__ (blood finding)
Low __ in blood
SOB, sharp central, confusion, leg
ESRD Sx
__ (resp)
__, __ chest pain
__ - AMS
__ swelling
Peripheral, friction rub, T waves, breath sounds, metabolic acidosis
ESRD sx PE
__ edema
Cardiac “__ __”
EKG - peaked/tented _ __
Diminished __ __ bil
Increased work of breathing from __ __ (acid-base)
Extracorporeal Membrane Oxygenation (ECMO)
Artificial gas exchange and circulation
Venous blood, external, gas exchange
ECMO Goals
Withdraw __ __ and pump through an __ (internal/external) oxygenator
Adds O2 and removes CO2 - Facilitating __ __
Vein, vein, right atrium, gas exchange
V-V ECMO
Drain blood from __ → oxygenate → Return blood via __ to the __ __ (heart)
Support __ __ of failing lungs
Vein, artery, right to left shunt
V-A ECMO
Drain blood from __ → oxygenate → Return blood via __
Creating a __ __ __ __ = stable O2 supply to heart
Heart failure, PE, cardiac arrest
Why might a patient require a V-A ECMO rather than a V-V ECMO?
For (3)
Right atrium, vena cava, vein, anesthetic, aorta, artery
ECMO
Venous blood is typically withdrawn from the__ __, __ __, femoral __ (2-heart, 1-vasc)
With some machines, volatile __ gases can be added to oxygenator
In V-A ECMO, blood is often returned via a cannula into __ or femoral __ (1-heart, 1-vasc)
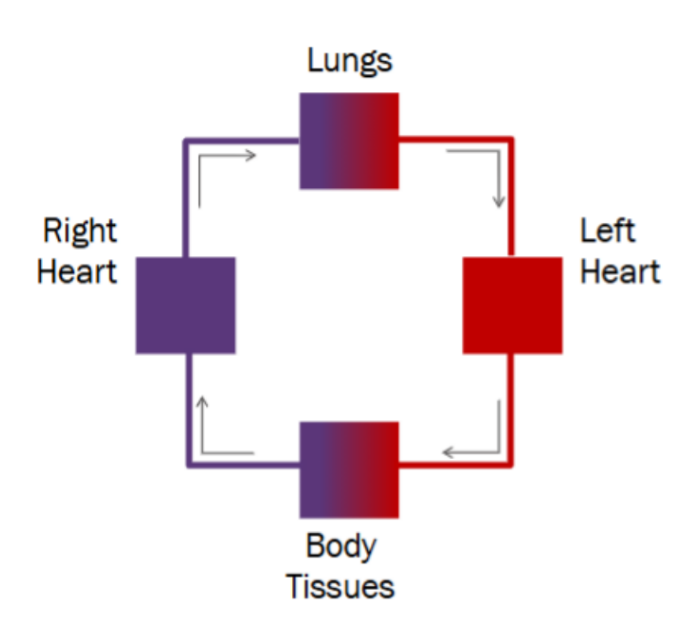
Healthy Heart (Normal circulation)
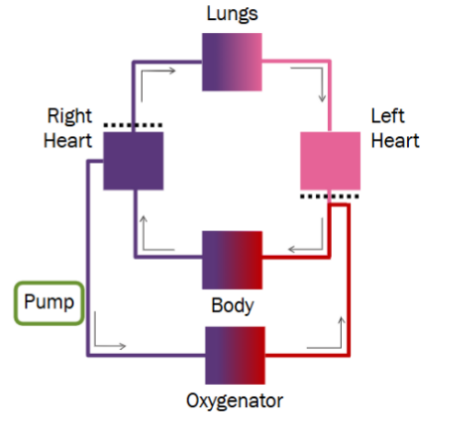
Poor Gas Exchange, requiring V-V ECMO
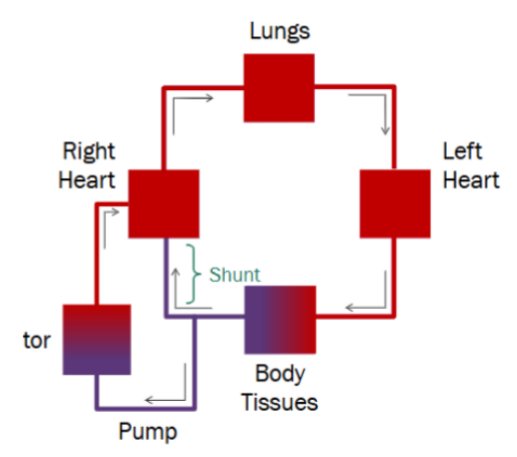
Poor Circulation, requiring V-A ECMO
Severe respiratory failure from ARDS
V-V ECMO is most appropriate in which scenario?
V-V ECMO
Support when lungs are NOT oxygenating adequately, but systemic and pulmonary blood flow are preserved → Respiratory failure
V-A ECMO
Support when heart is not pumping adequately (+ or lung dysfunction) → shunt
Cardiopulmonary Bypass
Artificial ventilation and circulation device during open-heart surgery
Movement, bleeding, oxygen delivery, heart tissue
Heart surgery requirements for CP Bypass
Minimize heart __
Minimize __
Maintain __ __ to systemic tissues
Preserve __ __
Venous Cannula
Sends deoxygenated blood to external oxygenator (CP B cannula)
Aortic Cannula
Returns oxygenated blood (CP B cannula)
Cardioplegia, left ventricle
Additional cannulae in CP B for:
Administering __ solutions (antegrade, retrograde, or both)
Draining blood from the __ __ (heart)
Bronchial circulation, thebesian veins, aortic valve regurgitation
Blood accumulates in the left ventricle over time
leads to (3)
O2 demand, stress, oxygenator, air, embolism
Left ventricular vent
LV distension increases myocardial __ __
Must drain to avoid __ to the heart
Filter drained blood and send to the __ (component)
Also removes __ introduced during surgery → To prevent an __ (condition)
20-35, 10-15
Myocardial tissue preservation in CP B
Systemic and local hypothermia
Core temperature actively or passively lowered to __-__ degrees C
Cardiac temperature reduced to __-__ degrees C
Crystalloid fluid, potassium, bicarbonate, glucose, cold
Cardioplegia solution for CP B
Blood or __ __
__ and __ (electrolytes)
__ (macromolecule)
__ (temp)
Cold cardioplegia, topical cooling, Ca2+, contraction
Myocardial tissue preservation in CP B
Myocardial temperature can be reduced via __ __ solution and __ __ with an ice slush
Cardioplegia solutions must have carefully controlled __ (ion) levels, excessive leads to __ of heart
Cardioplegia pump, coronary, aortic clamp
Cardioplegia administration in CP B
A separate __ __ allows for better control
Admin into __ vasculature (coronary arteries excluded by an __ __)
Aortic clamp, aorta, coronary sinus
Cardioplegia admin into coronary vasculature in CP B
Coronary arteries excluded by an __ __
Antegrade via catheter in __ (goes L to R)
Retrograde via catheter in __ __ (goes R to L)
Dialysis
Artificial renal function in case of renal failure
Hyperfiltration, progressive, GFR
__ = High whole kidney GFR, high single nephron GFR
__ destruction of more nephrons
Failure of compensatory mechanisms will lower __ over time
CKD Stage III
Low whole kidney GFR, high single nephron GFR
ESRD
Very low whole kidney GFR, very high single nephron GFR
60, 3
Chronic Kidney Disease (CKD) Criteria
GFR < __ mL/min for _ months or longer
I, 90
Stage _ CKD: Kidney damage with normal or elevated GFR
GFR is __ or higher
II, 60-89
Stage _ CKD: Kidney damage with mild decrease in GFR
GFR is __-__
III, 30-59
Stage _ CKD: Moderate decrease in GFR
GFR is __-__
IV, 15-29
Stage _ CKD: Severe decrease in GFR
GFR is __-__
V, 15
Stage _ CKD: Kidney failure or ESRD
GFR is less than __
30, 15
CKD
Stages I-III are in GFR increments of __ ml/min/1.73
Stage IV-V are in GFR increments of __ ml/min/1.73
Metabolic wastes, body water, buffers
Functions of Dialysis - (3)
Remove __ __
Remove excess __ __
Replenish __
Acid/base, electrolyte, hyperkalemia, intoxication, overload, uremia
Emergent Indications for Dialysis = AEIOU
__/__ disturbances
__ disturbances (i.e. __**)
__ (i.e. salicylates)
__ (of volume)
__ - GU
Semi-permeable, concentration gradient, solute, permeability, surface area, flow rate
Dialysis is diffusion across a __ __ membrane
Affected by…
__ __ between blood and dialysate
__ size
Membrane __
__ __ (dimension)
__ __ of blood to dialysate
Equilibrium, plateaus, concentration gradient
In Dialysis
Since smaller solutes diffuse faster, they reach __ and clearance __
Larger solutes diffuse slower, maintaining their __ __ between blood and dialysate
Ultrafiltration
Setting pressures to remove appropriate volume of fluid over time
Hydrostatic, blood compartment, dialysate component
Ultrafiltration in Dialysis
Dialysis machine generates a __ pressure gradient
Positive pressure applied to the __ __
Negative pressure (suction) applied to the __ __
High, fistula, graft, central line
Vascular access for hemodialysis
Need stable access to bloodstream with __ blood flow
Options - Arteriovenous __, arteriovenous __, and __ __
AV Fistula
Vein connected to artery, with increased pressure and flow in vein downstream to anastomosis (for dialysis)
Months, weeks
AV Fistula is created surgically several __ prior to dialysis
AV Graft is created surgically several __ prior to dialysis
Pressure, bleeding
Why should you avoid venipuncture and blood pressure measurements on a limb with a fistula?
Higher __ to fistula than typical vein will lead to higher risk of __ or infection
AV Graft
Connects artery to vein, with synthetic tube; used sooner (for dialysis)
Central Line
Large double or triple lumen catheters for immediate use (in dialysis)
Subclavian, IJV, lower flow
Central Line
Think tube to the __ or __, used immediately
Con - __ __ than AV fistula or graft
Flow, resistance
Why are large-gauge catheters used for central hemodialysis lines?
Maximize highest __ via Ohm’s Law and decrease __
Peritoneal Dialysis
Dialysis solution localized, equilibrates with ECF and drains
Home, longer
Peritoneal Dialysis
Patients can perform at __, but takes __ than hemodialysis
Anaerobic, lactic acid, bicarbonate
Why does myocardium produce acidic metabolites during bypass?
Myocardium reacts on __ metabolism in bypass, producing __ __
__ in cardioplegia solutions neutralize this