Chapter 26 - Fluid Balance
1/58
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
59 Terms
ICF
where most of the body’s water is found
K, proteins, HPO4
more of these are found in the ICF
Na, Cl, bicarb
more of these are found in the ECF
plasma, IF
two components of ECF
lymph, CSF, humors, serous fluid, synovial fluid
components of IF
electrolytes
anything that dissociates into ions in water, often have a charge and are the most abundant solutes
non-electrolytes
more body fluids are these
young skinny male
this person would have the highest water content
diet
where does most of our water come from?
hypothalamic thirst center
this controls the thirst mechanism
osmoreceptors
this detect changing ECF osmolality
obligatory water loss
the idea the body will always lose water, even if we never drink water
osmoreceptors, baroreceptors
release of ADH is dependent on these two types of receptors
central diabetes insipidus
this condition is marked by a decrease in ADH production by the hypothalamus or lack of PPG release
polyuria, dilute urine, dehydration
s/s of central diabetes insipidus
nephrogenic diabetes insipidus
condition where ADH is produced and released in normal amounts but the kidneys don’t respond to it
280
how many mOsm of the ECF solute come from Na?
out, in
plasma membranes are impermeable to Na, it is almost always kept
___ of cells and ____ the ECF
PCT, nephron loop
where most Na is reabsorbed
aldosterone
this hormone causes increased reabsorption of Na into the DCT and collecting ducts, increasing ECF volume
diuretic, natriuretic, decreased Na reabsorption
effects of ANP
estrogen
this sex hormone has a similar effect to aldosterone
diuretic
progesterone is slightly ________ (relating to urine)
glucocorticoids
in high plasma levels these exert very strong aldosterone-like effects and can cause edema
H+
K moves in the opposite direction of this, acting as a pH buffer
DCT, collecting ducts
principal cells secrete K in these regions
type A
this type of intercalated cells can reabsorb K when levels are very low, but not very well
secretion, excretion
high ECF K concentrations drive this
reabsorption
low ECF K concentrations drive this
stimulates secretion
aldosterone effect on K
7.35-7.45
ideal blood pH
alkalosis
blood pH of 7.45 or higher
physiological acidosis
blood pH of 7.35 or lower
carbonic acid, bicarb salt
two pieces of the bicarbonate buffer system
converting a strong acid to a weak acid using bicarb salt
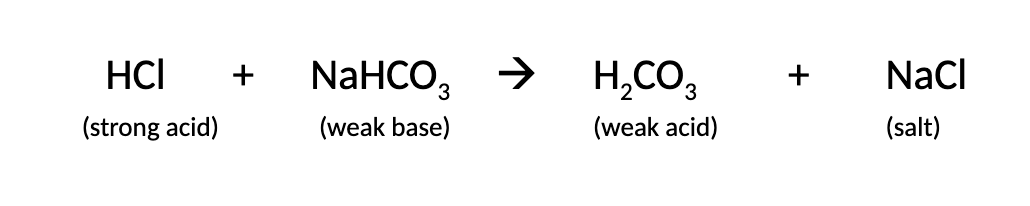
converting a strong base to a weak base using carbonic acid
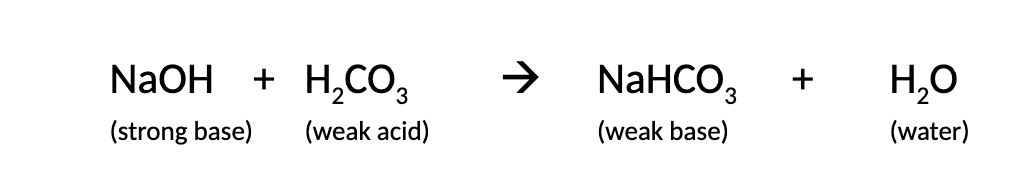
dihydrogen phosphate
weak acid in phosphate buffer system
monohydrogen phosphate
weak base in phosphate buffer system
bicarbonate
main ECF buffer system
phosphate, protein
main ICF buffer systems
urine
phosphate buffer system is used for this pH (aside from ICF)
blood plasma
protein buffer system is used for this pH (aside from ICF)
amphoteric
proteins are this, able to act as an acid or a base
increase
increasing CO2 levels will cause RR/respiratory depth to _________
decrease
decreasing CO2 levels will cause RR/respiratory depth to _________
long-term
renal regulation is important for __________ acid base balance
bicarb content in blood
renal mechanism of regulating pH
PCT, type A intercalated cells
these can generate new bicarb to be released
H+
this must be secreted into filtrate at the same time as bicarb
type B intercalated cells
in collecting ducts these can reabsorb H+ while secreting bicarb ions from filtrate
45 mmHg
a PCO2 over this value indicates respiratory acidosis
35 mmHg
a PCO2 value under this value indicates respiratory alkalosis
metabolic acidosis/alkalosis
any acid-base imbalance that does not involve CO2
metabolic acidosis
this results from low bicarb levels, causes are excessive alc intake or long term diarrhea
metabolic alkalosis
this results from high bicarb levels, causes are excessive vomiting and excessive base intake
CNS depression, death
effect of a blood pH under 6.8
muscle tetany, convulsions, death
effect of a blood pH over 7.8
respiratory compensation
changes in RR/depth when the lungs compensate for metabolic imbalances
renal compensation
when the kidneys compensate for the acid-base imbalances of respiratory organs