Neuropathology I: Stroke and Epilepsy
1/147
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
148 Terms
high and continuous
What is the oxygen requirement like for the brain?
-2% body weight
-15% cardiac output
-20% total body oxygen
-> an organ that comprises such a small fraction of total body mass requires significant blood flow and oxygen...shows its importance
What percent of body weight, cardiac output, and total body oxygen is used by the brain, and explain?
few minutes of ischemia -> irreversible injury
What happens if the body fails to meet the continuous oxygen requirement for the brain?
neurons are predominantly aerobic, requiring oxygen for energy
What is the oxygen requirement like for neurons?
age
What do the areas of the brain that are sensitive to hypoxia/ischemia depend on?
-hippocampus
-3, 5th, and 6th layer of cortex
-Purkinje cells
-Border zone (watershed areas)
What are the 4 main sensitive areas of the brain in adults?
brain stem nuclei
What is the main sensitive area of the brain in infants?
the circle of Willis
What is the major blood supply to the brain via?
anterior flow and posterior flow, which anastomose via the anterior and posterior communicating arteries at the base of the brain
What is the circle of Willis formed by, and explain?
through the internal carotid arteries
What does the anterior blood flow go through?
70% of CBF
What fraction of cerebral blood flow is anterior flow responsible for?
through the vertebral arteries, which fuse to form the basilar artery
What does the posterior blood flow go through?
30% of CBF (less than anterior)
What fraction of cerebral blood flow is posterior flow responsible for?
anastomotic pathway between the external and internal carotid arteries via the ophthalmic arteries
What is the anastomotic pathway like in the Circle of Willis?
if the pathway is normal, then even the occlusion of one of the four main arteries will not necessarily lead to insufficient regional cerebral blood flow -> very important for blood supply to the brain
What is the significance of the anastomotic pathway in the Circle of Willis?
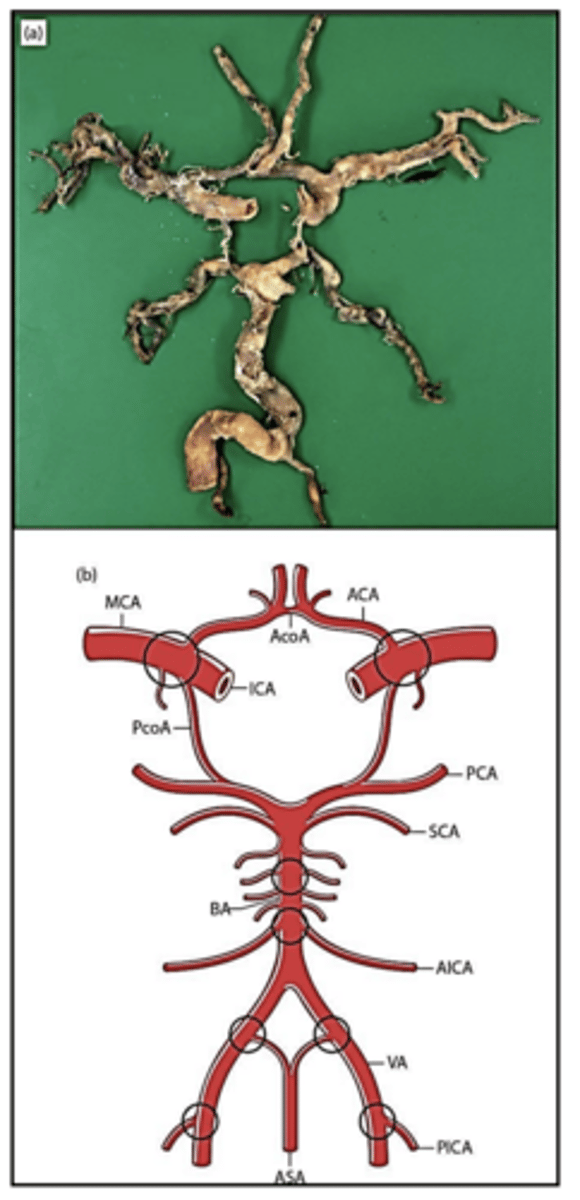
Circle of Willis with the most common sites for atheroma circled:
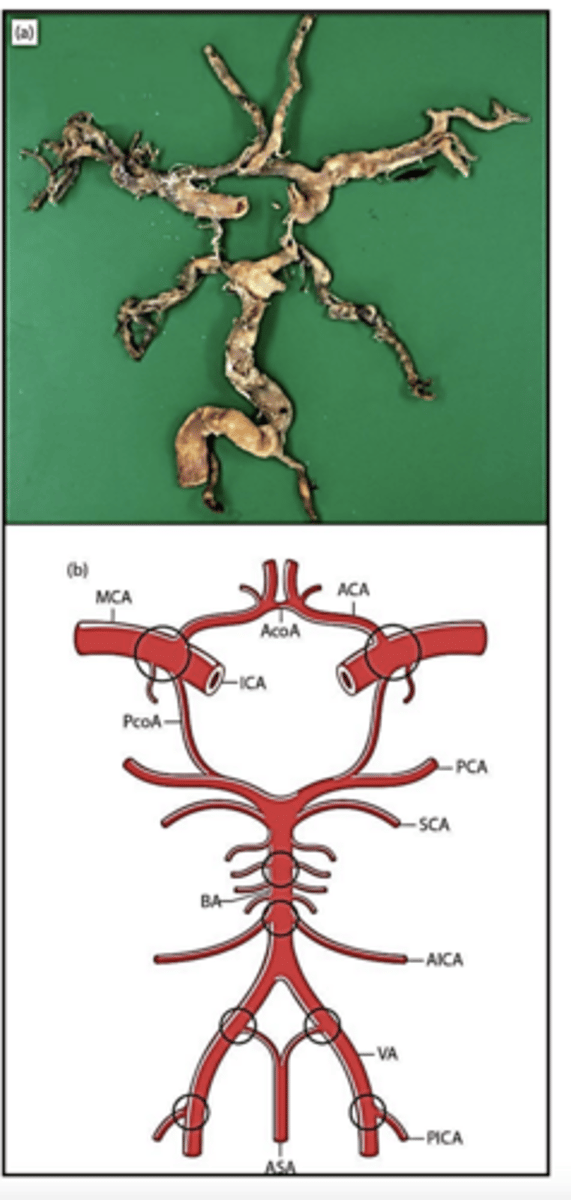
-heart disease
-cancer
-cerebrovascular disease (CVD)
What are the 3 leading causes of death in the USA?
very common, the leading neurological disorder in terms of morbidity and mortality
What is the prevalence of cerebrovascular disease (CVD) like?
-stroke
-transient ischemic attack (TIA)
What 2 conditions can cerebrovascular disease (CVD) cause?
sudden focal neurological symptoms due to a vascular cause
What is a stroke?
-ischemic stroke
-hemorrhagic stroke
What are the 2 main types of strokes?
ischemic strokes (>80%)
Are ischemic strokes or hemorrhagic strokes more common?
a region of the brain with impaired blood flow due to vascular blockage
What is an ischemic stroke?
a region of the brain with a ruptured blood vessel (blood leaks out)
What is a hemorrhagic stroke?
-intraparenchymal
-subarachnoid
What are the 2 main types of hemorrhagic strokes?
transient focal neurological deficit due to ischemia
What is a transient ischemic attack (TIA)?
"ministroke" (milder)
What is a transient ischemic attack (TIA) also known as?
<24 hours or even <1 hour (short!)
What is the duration of symptoms like in a transient ischemic attack (TIA)?
no evidence of infarction
What does imaging (CT/MRI) reveal in the case of a transient ischemic attack (TIA)?
up to 10% risk for subsequent stroke in the next 48 hours; need immediate medical attention
What is the risk associated with a transient ischemic attack (TIA), and explain?
-cardioembolism
-large vessel atherosclerosis (intracranial and extracranial vessels)
-small vessel disease (lacunar strokes)
-uncommon cases of stroke
-idiopathic (etiology unknown)
What are the 5 main causes of ischemic stroke?
cardioembolism; up to 20% of ischemic stroke
Which of the main causes of ischemic stroke is most common, and explain?
can involve multiple vascular territories
What vasculature can cardioembolism involve?
-CNS emboli
-systemic emboli
Based on location in the body, what are the 2 types of emboli that can result from cardioembolism?
has highest in-hospital mortality
What is a characteristic of cardioembolism, considering mortality?
increased functional limitations at discharge (compared to other ischemic stroke subtypes)
What is the discharge of patients like who have experienced a cardioembolism?
-arrhythmia (ex: atrial fibrillation)
-left heart structural abnormalities
-valvular disease
What are 3 main sources of cardioembolism?
-LV mitral thrombus
-congenital heart failure
-cardiac tumors (rare)
What are 3 examples of left heart structural abnormalities that function as sources of cardioembolism?
-prosthetic valves
-endocarditis (ex: infection)
What are 2 examples of valvular diseases that function as sources of cardioembolism?
-extracranial large arteries
-intracranial large arteries
What are the 2 main types of large arteries that can experience atherosclerosis and contribute to ischemic stroke?
-internal carotid artery (ICA)
-common carotid artery (CCA)
-vertebral artery
What are the 3 extracranial large arteries that are susceptible to atherosclerosis?
-middle cerebral artery (MCA)
-anterior cerebral artery (ACA)
-posterior cerebral artery (PCA)
-basilar artery
What are the 4 intracranial large arteries that are susceptible to atherosclerosis?
vessels in Circle of Willis = at risk of large artery atherosclerosis
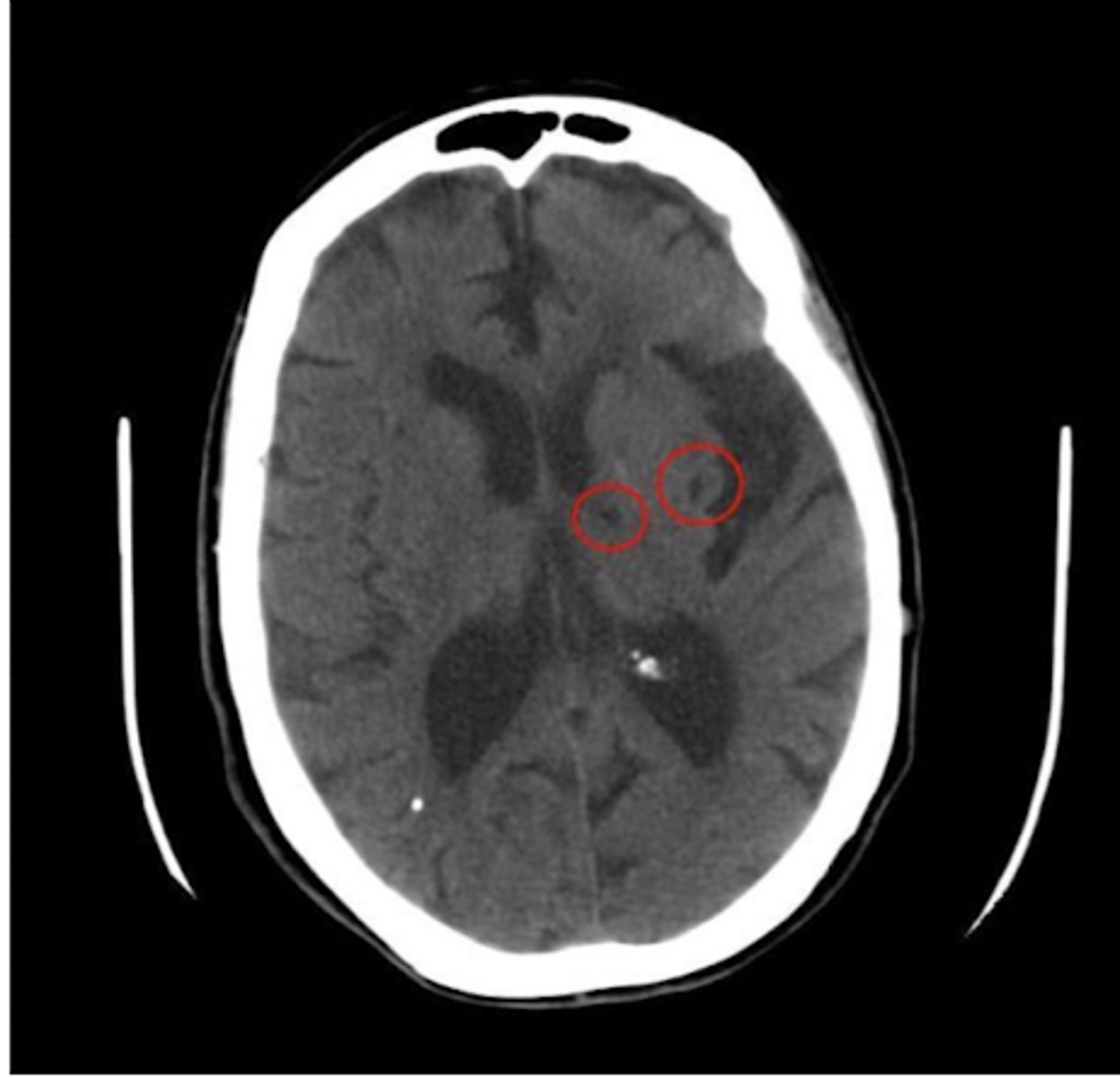
Lacunar infarcts (strokes)
What does small vessel disease lead to?
up to 25%
What fraction of all ischemic strokes do small vessel/Lacunar infarcts account for?
in subcortical locations; basal ganglia and thalamus
Where do small vessel/Lacunar infarcts occur, and explain?
small, <1.5 cm in size
What is the size of small vessel/Lacunar infarcts like?
-small vessel hyalinosis (hyaline arteriosclerosis secondary to HTN)
-microatheroma
What are 2 pathologies that often co-exist with small vessel disease?
clinically may be silent (may not present with symptoms)
What is the clinical presentation of small vessel/Lacunar infarcts like?
pure motor stroke
What type of stroke occurs if there is internal capsule involvement in the small vessel disease/Lacunar infarct?
pure sensory stroke
What type of stroke occurs if there is thalamus involvement in the small vessel disease/Lacunar infarct?
small artery and arterioles
What vessels does hypertensive small vessel disease involve?
atherosclerosis
Based on the pathophysiology of hypertensive small vessel disease, what is the 1st stage in the progressive sequence?
fibrinoid necrosis
What follows atherosclerosis in the sequence of hypertensive small vessel disease progression?
arteriosclerosis
What follows fibrinoid necrosis in the sequence of hypertensive small vessel disease progression?
thickened eosinophilic walls (hyalinosis)
What is arteriosclerosis, a stage of hypertensive small vessel disease?
microaneurysms
What follows arteriosclerosis in the sequence of hypertensive small vessel disease progression?
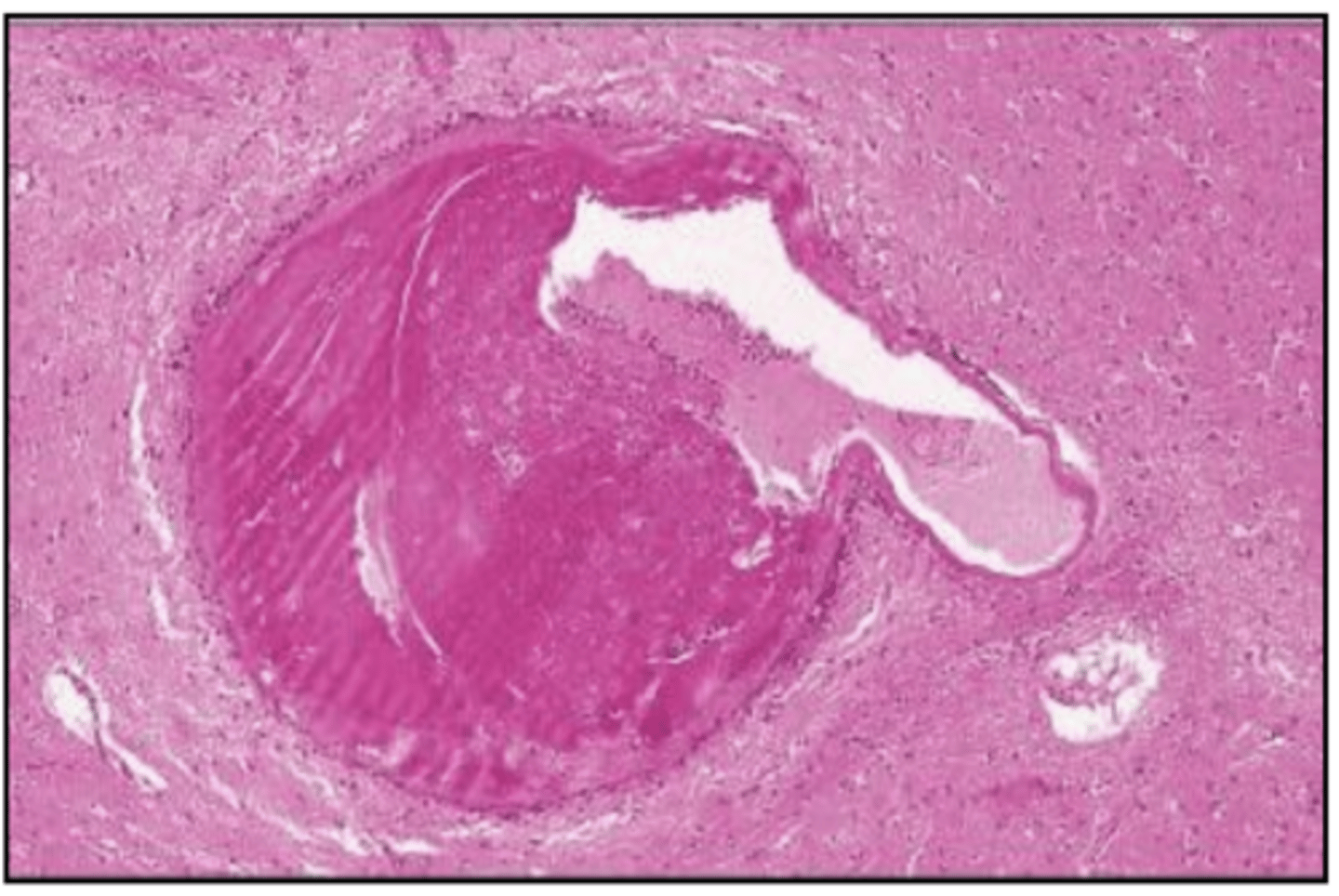
hypertensive small vessel disease:
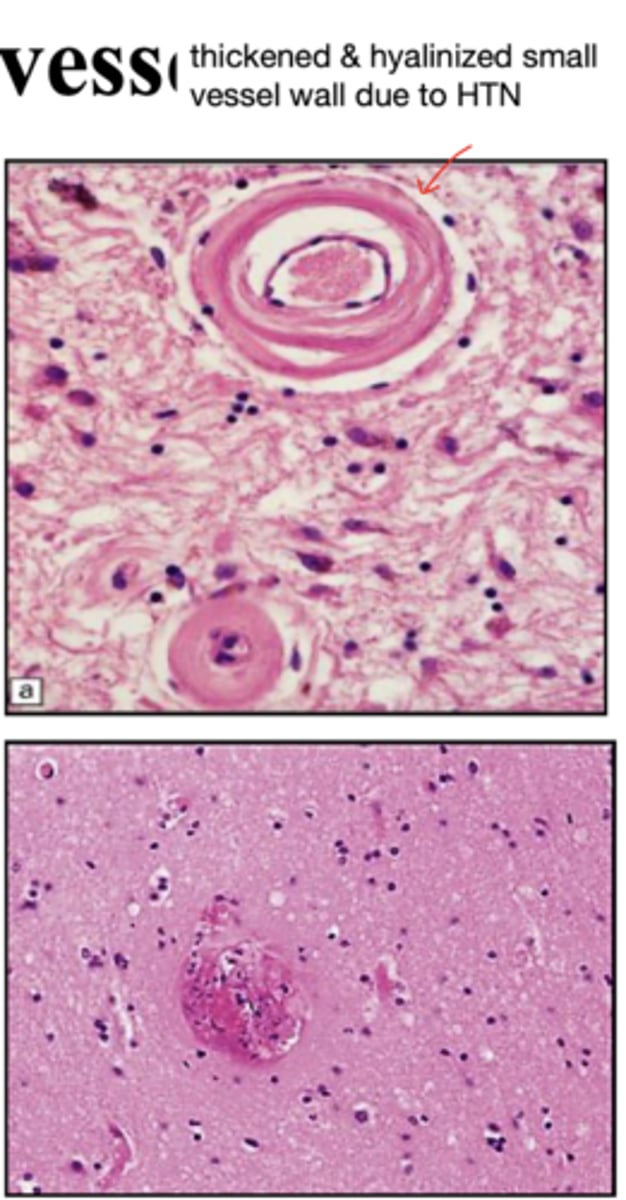
dilation and thickening of the arteriole wall -> "Charcot-Bouchard aneurysms"
What happens to the arteriole wall in hypertensive small vessel disease?
rupture and hemorrhage
What may dilation and thickening of the arteriole wall in hypertensive small vessel disease predispose a person to?
-carotid/vertebral dissection
-vasculopathy (ex: vasculitis)
-genetic (ex: sickle cell disease)
-hypercoagulable states (ex: cancer, infection, Factor V Leiden, etc)
-pregnancy, oral contraceptives
What are 5 uncommon causes of ischemic stroke (cause up to 5% of ischemic stroke)?
*non-modifiable
*modifiable
What are the 2 main categories of stroke risk factors?
-age
-gender
-hereditary
What are 3 non-modifiable stroke risk factors?
-HTN
-cardiac disease
-diabetes
-hypercholesterolemia
-cigarette smoking
-alcohol
What are 6 modifiable stroke risk factors?
-reperfusion
-supportive care
-prevent recurrent stroke
What are the 3 main treatment methods for acute ischemic stroke?
restore cerebral blood flow to specific region affected by the lack of O2
What is the goal of reperfusion in acute ischemic stroke?
-minimize damage
-prevent complications
What are the 2 main goals of supportive care in acute ischemic stroke?
-antithrombotic therapy
-determine the cause(s) of stroke
What are the 2 methods of preventing recurrent stroke in the case of an acute ischemic stroke?
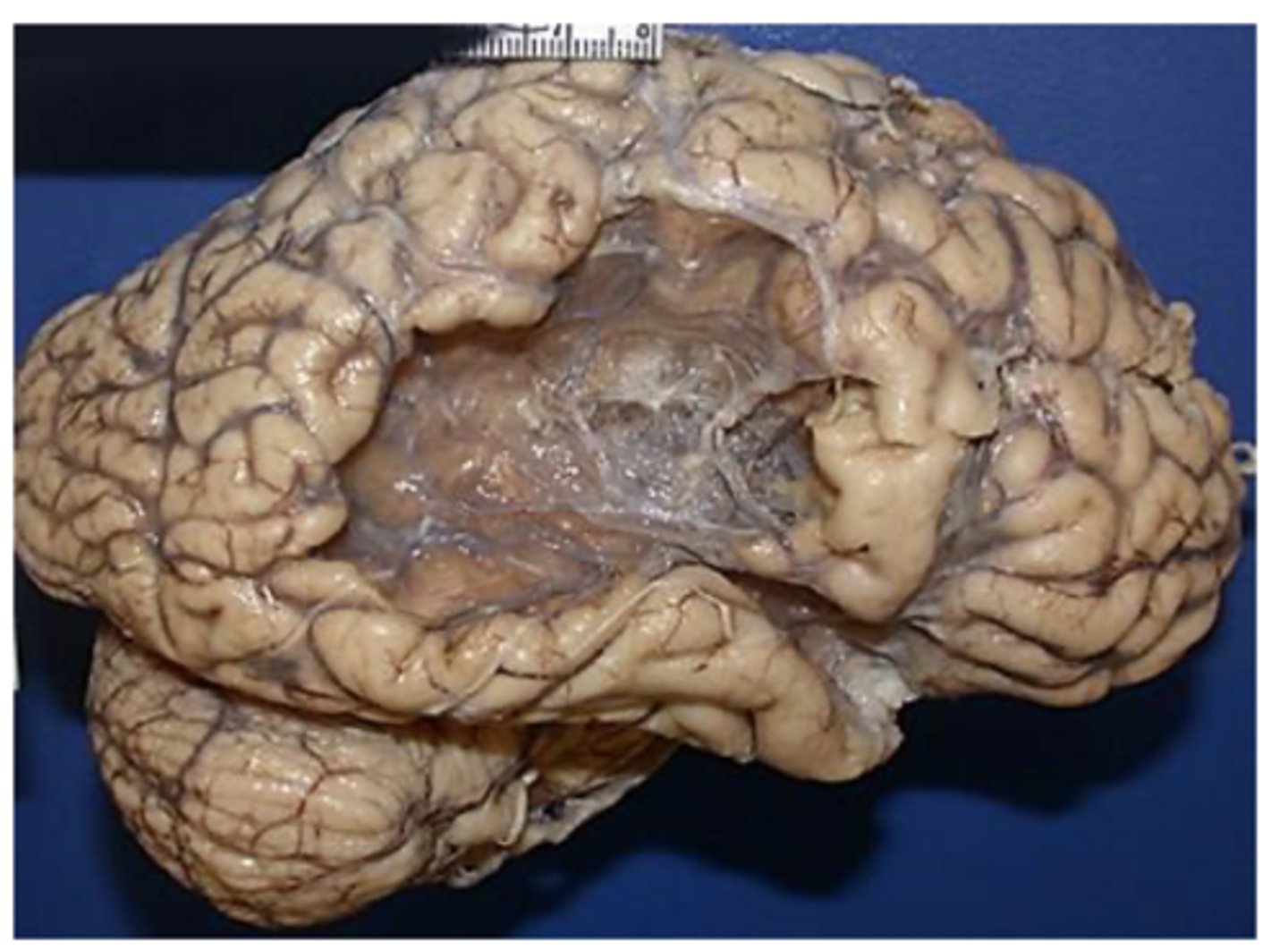
smaller lacunar infarct
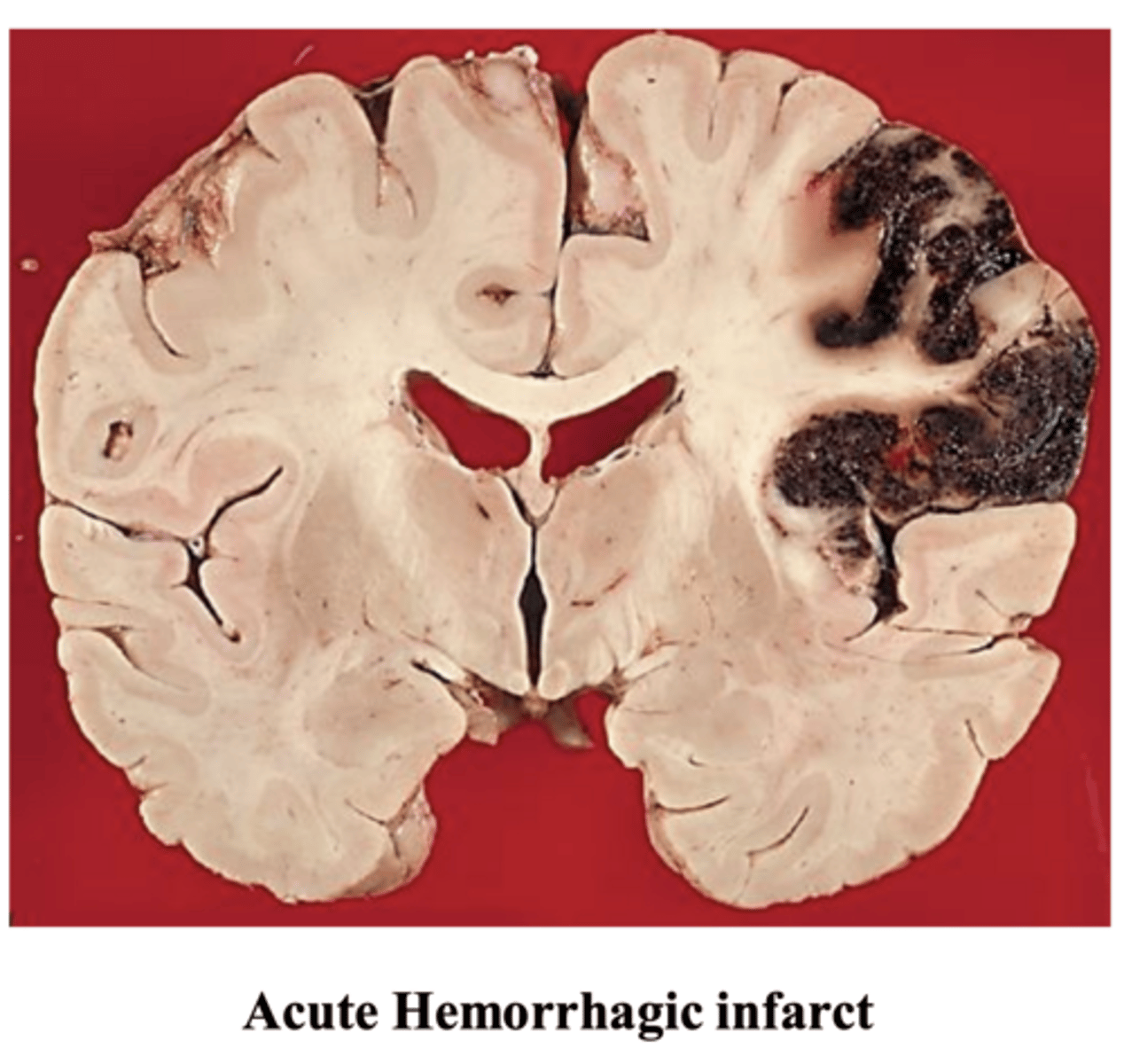
old MCA infarct -> not the cause of death, but can see the changes/damage post-mortem from a previously experienced MCA infarct
the timing at which the stroke occurred; acute, subacute, chronic
What can the histopathology of ischemic stroke (infarcts) be used to determine, and explain?
red neurons:
-eosinophilic cytoplasm
-hyperchromatic nucleus
-loss of Nissl granules
What does the histopathology of an ischemic stroke (infarct) reveal at 6-12 hours after the stroke (acute)?
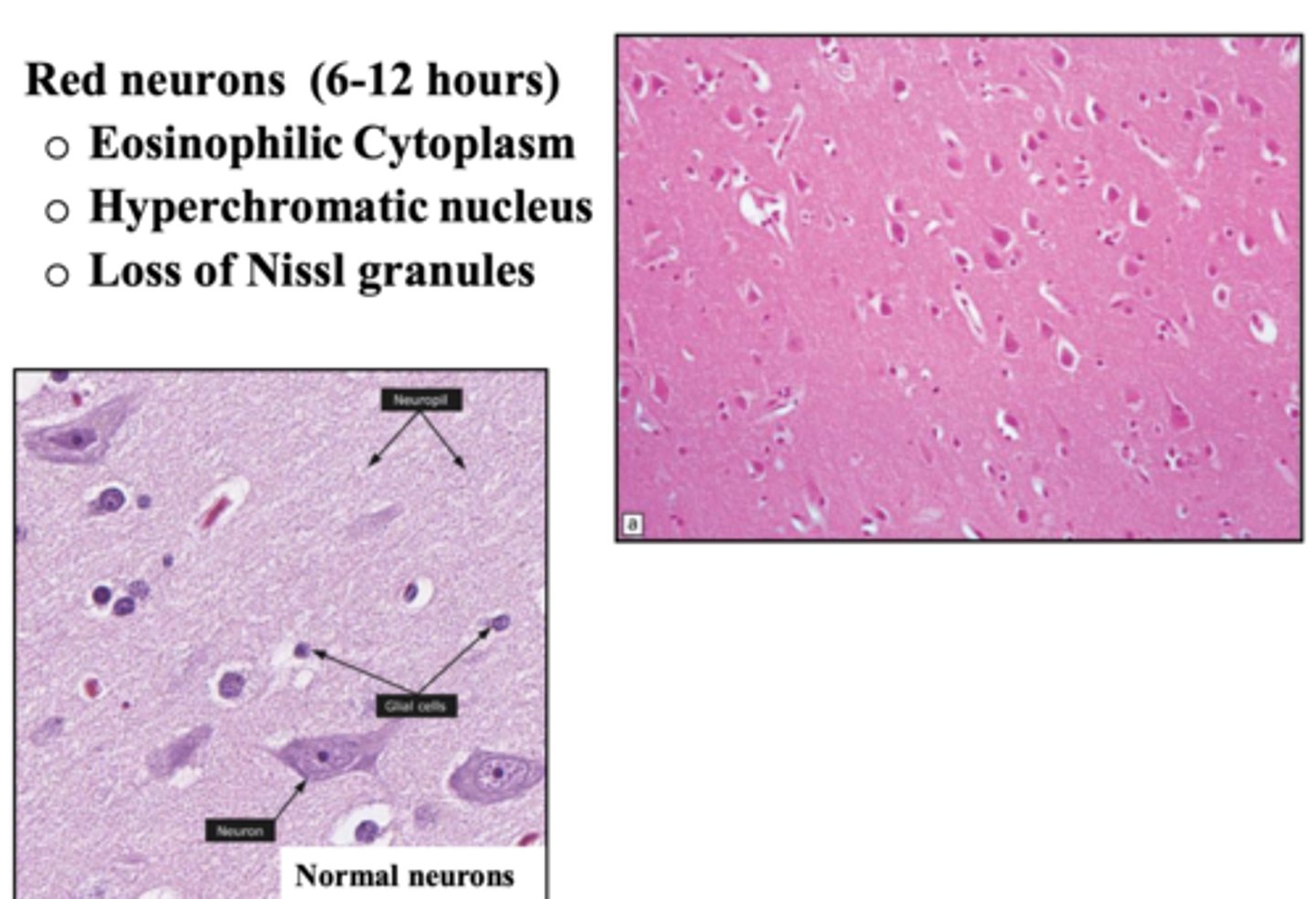
-red neurons and rarefaction of neuropil (loss/thinning of dense network of axons, dendrites, and glial cell processes in brain's gray matter)
-necrosis
-neutrophils infiltration (12 hours after infarction)
What does the histopathology of an ischemic stroke (infarct) reveal at 1-3 days after the stroke?
-neuronal dropout
-influx of macrophages (microglial cells -> clean up necrotic debris), fewer lymphocytes and polys
-vascular proliferation
What does the histopathology of an ischemic stroke (infarct) reveal at 4-7 days after the stroke?
4-7 days after the stroke:
-neuronal dropout
-influx of macrophages (microglial cells -> clean up necrotic debris), fewer lymphocytes and polys
-vascular proliferation
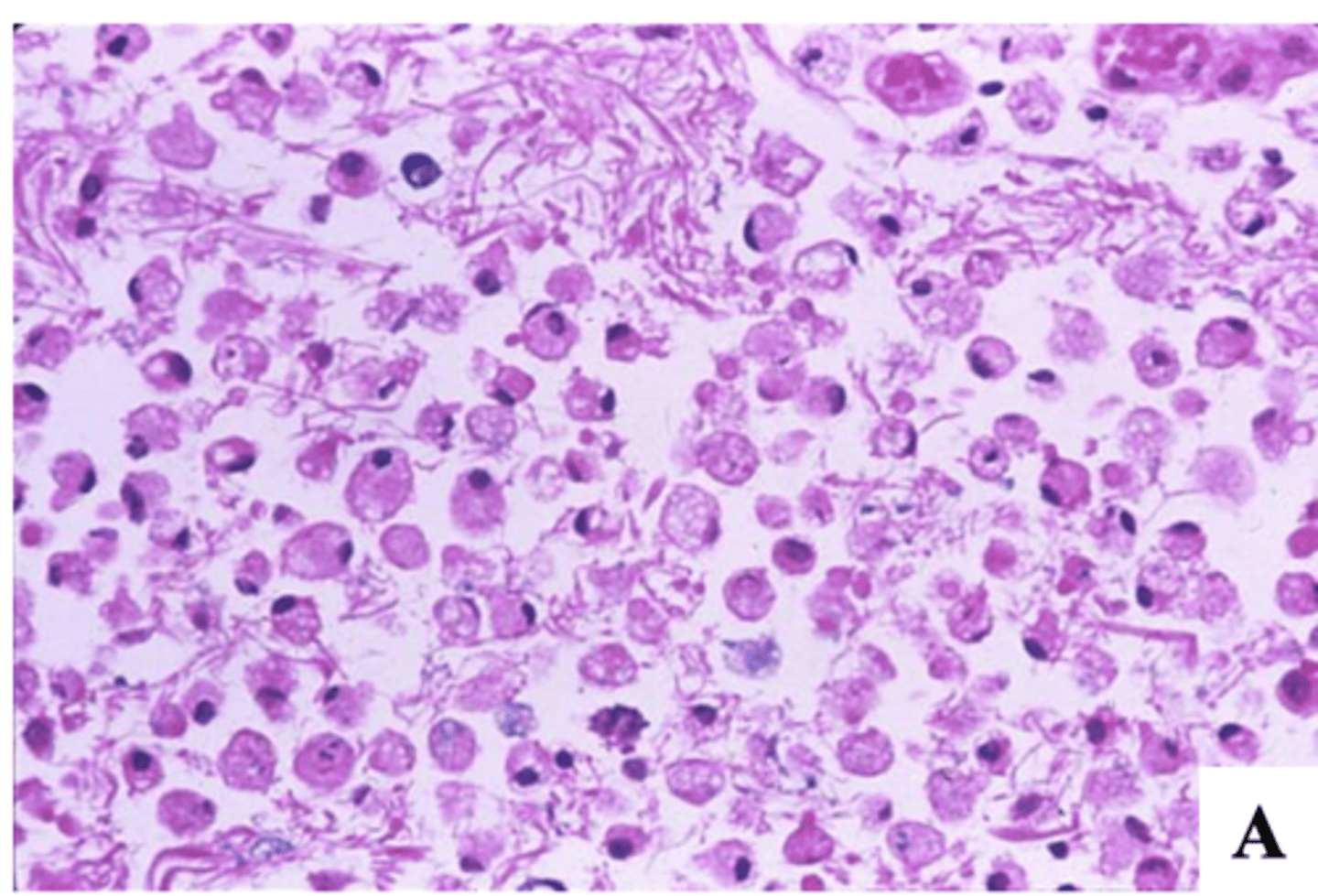
-gliosis
-cystic cavity
What does the histopathology of an ischemic stroke (infarct) reveal at 2-3 weeks or months after the stroke?
2-3 weeks or months after the stroke:
-gliosis
-cystic cavity
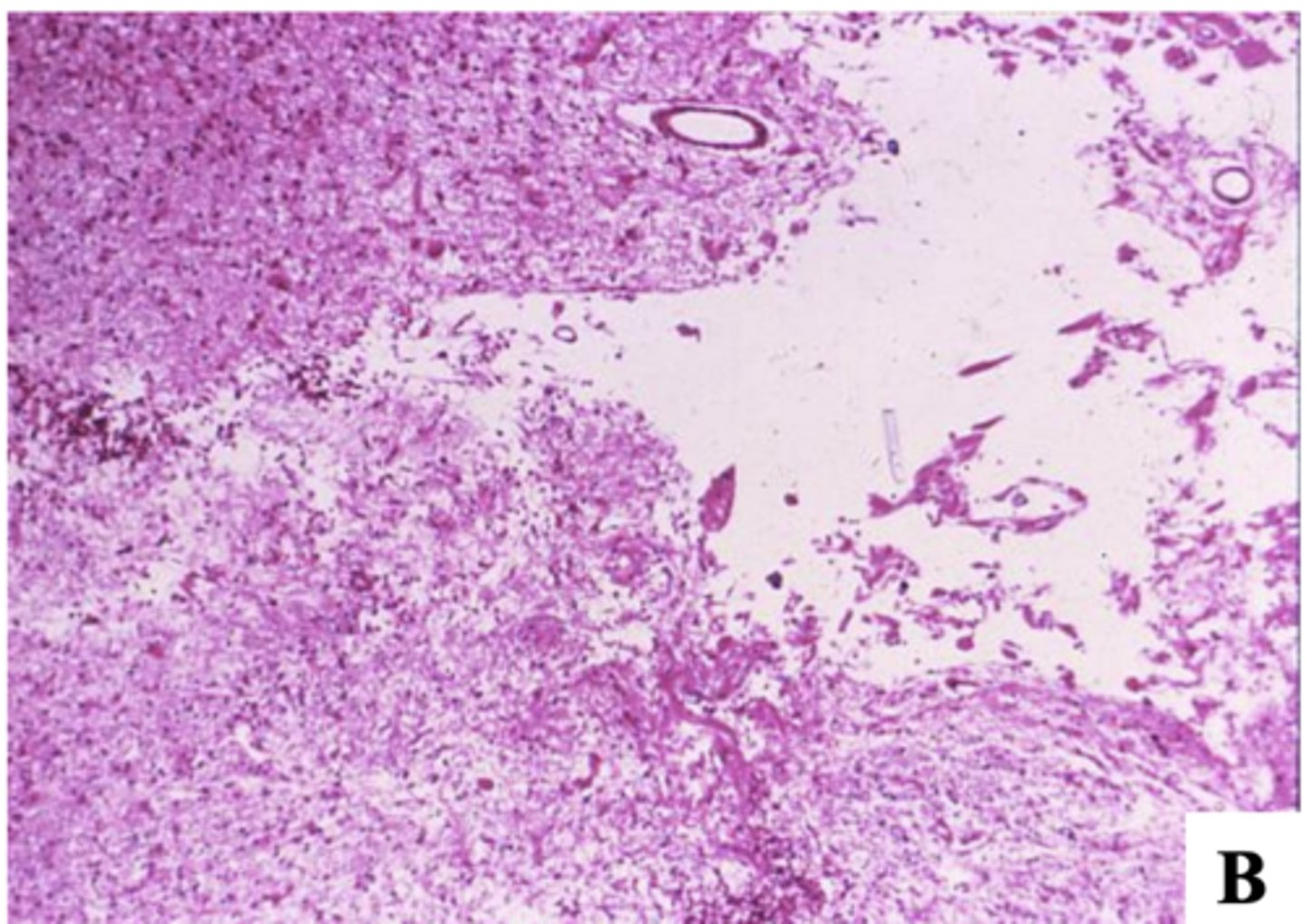
intracerebral hypertensive hemorrhage (70-80%)
What is the most common type of intracerebral hemorrhage stroke?
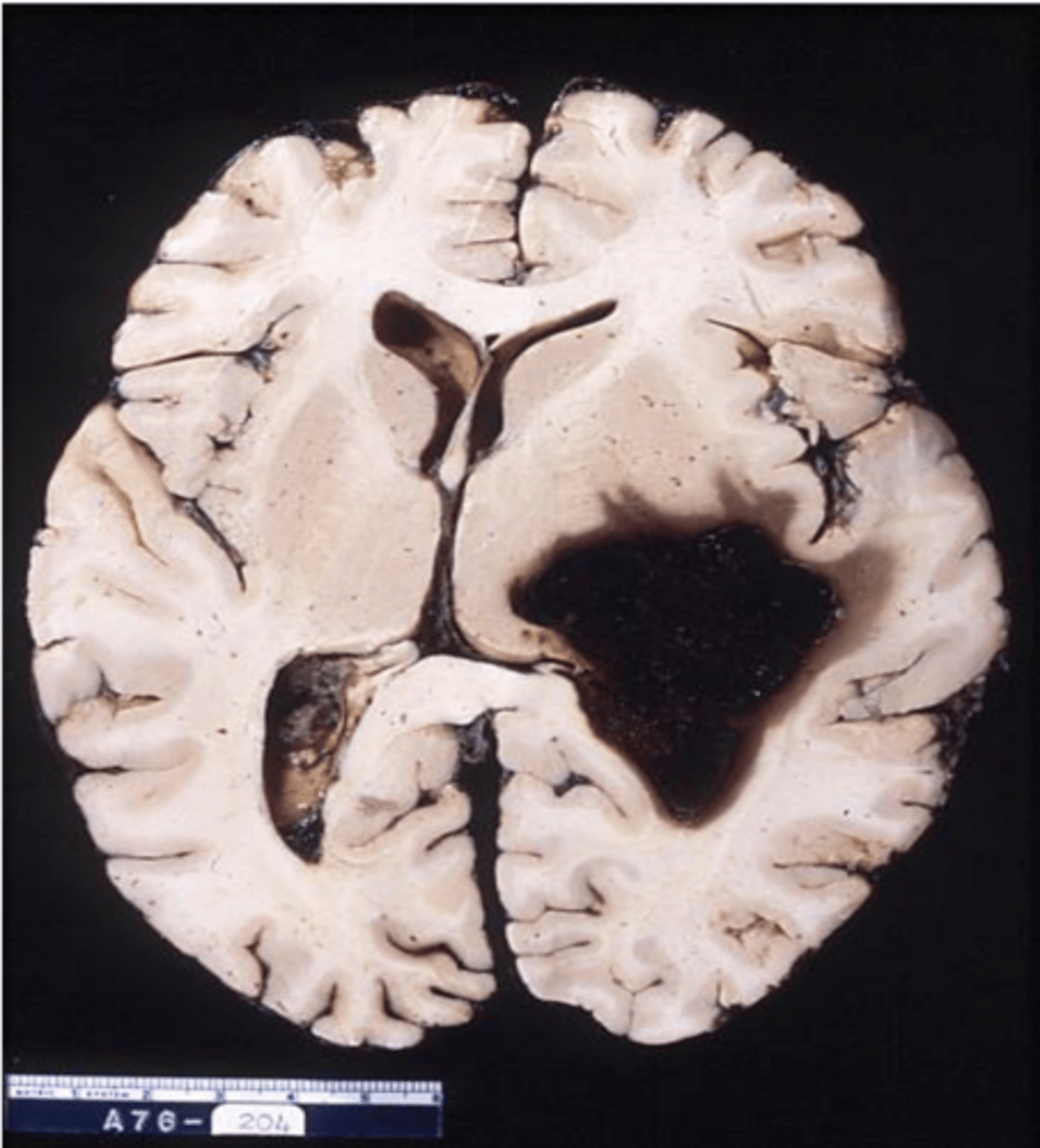
bleeding into brain parenchyma
What happens in intracerebral hypertensive hemorrhage?
-basal ganglia -> most common, up to 50%
-cerebral hemisphere - lobar -> up to 30%
-brainstem/cerebellum -> up to 20%
What are the 3 main locations of intracerebral hypertensive hemorrhage, and the prevalence of each?
rupture of "Charcot-Bouchard" aneurysm
What is the major cause of intracerebral hypertensive hemorrhage?
3rd most common cerebrovascular lesion, after cerebral infarction and HTN hemorrhage
What is the frequency of non-traumatic subarachnoid hemorrhage (SAH), as it pertains to other cerebrovascular lesions?
rupture of a berry aneurysm
What is the most common cause of subarachnoid hemorrhage (SAH)?
is the most frequent intracranial arterial aneurysm (1 per 10,000 people)
What is the prevalence of "berry" aneurysm (aka saccular or congenital aneurysm) like?
in the younger population
In what population are subarachnoid hemorrhage (SAH) seen most often?
20-30% of persons with a berry aneurysm have multiple aneurysms
What is the likelihood of multiple anauerysms with a berry aneurysm?
at vessel branch points in the Circle of Willis; because they contribute to turbulence of blood flow
Where do aneurysms tend to occur, and explain?
most are sporadic
What is the onset of "berries" like?
those with adult-onset polycystic kidney disease
In what patients is there an increased risk of "berries"?
-atherosclerotic
-mycotic (infectious)
-traumatic
-dissecting
-> these typically do not present with SAH
What are 4 other, rarer types of aneurysms, and how does their presentation relate to SAH?
non-traumatic subarachnoid hemorrhage (SAH)
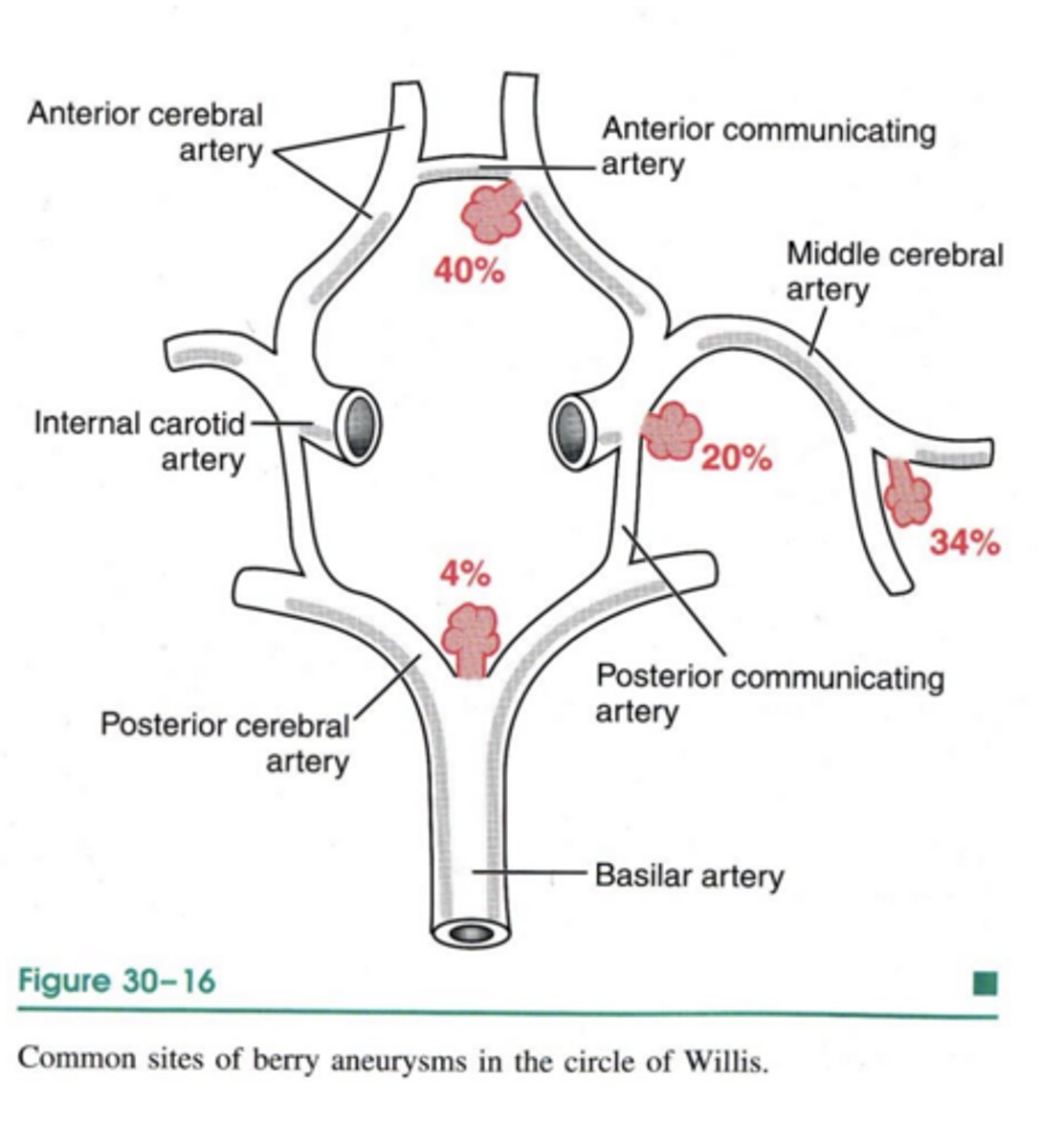
SAH:
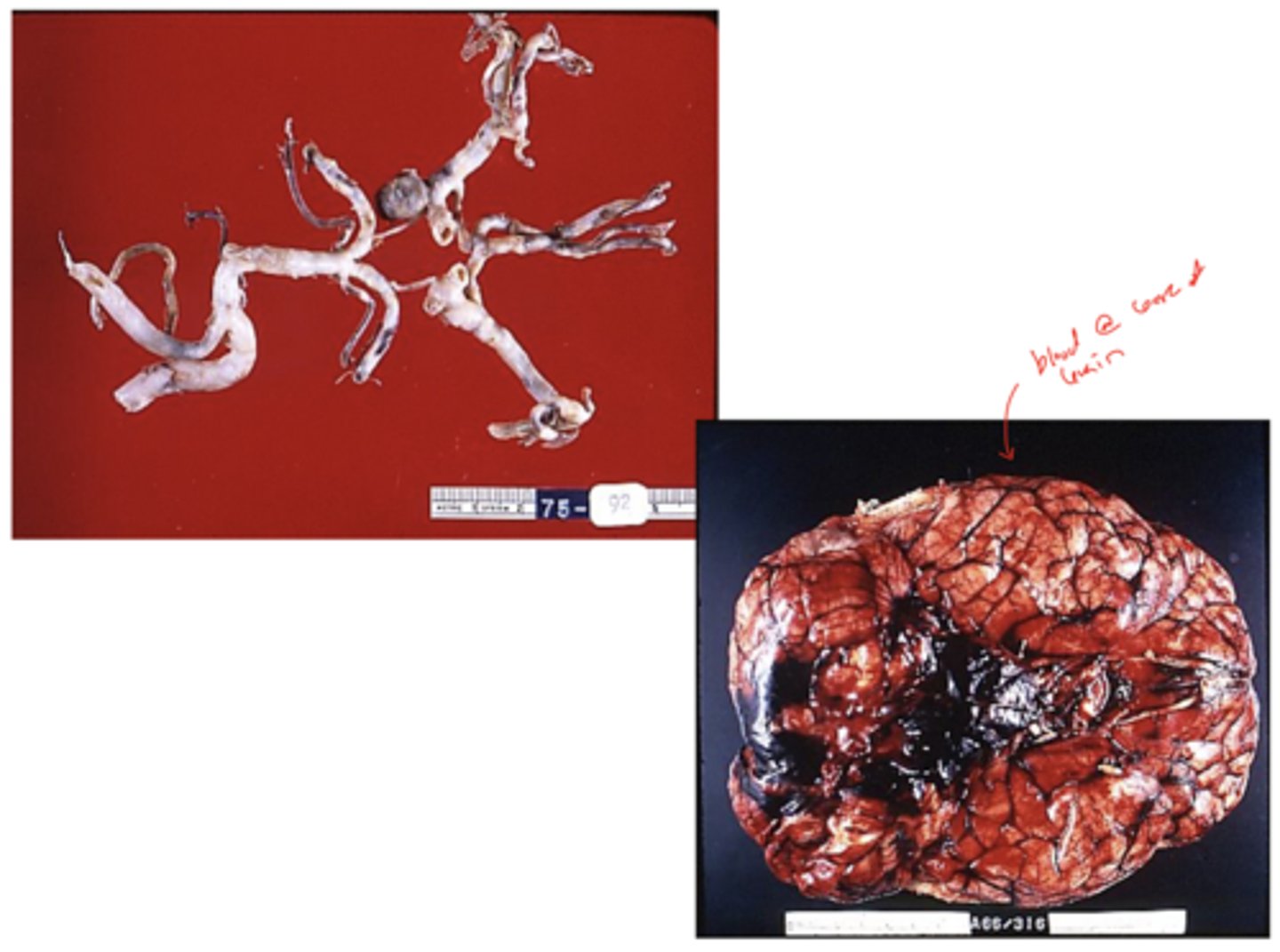
a sudden, excruciating headache...typically "the worst pain I've ever had" -> patient may lose consciousness
What is the typical presentation of subarachnoid hemorrhage (SAH)?
20-50% will die with the 1st rupture -> the rest who survive will recover consciousness within minutes
What happens to patients after the 1st rupture in a subarachnoid hemorrhage (SAH)?
rebleeding; not possible to predict who will rebleed
What is common in subarachnoid hemorrhage (SAH), and explain?
-vasospasms of nearby arteries irritated by the blood
-scarring of the leptomeninges, leading to hydrocephalus
What are 2 other complications associated with subarachnoid hemorrhage (SAH)?

inflammation of the blood vessel walls
What is vasculitis?
-endothelial intima
-smooth muscle media
-connective tissue adventitia
What are the 3 layers that make up the blood vessel wall?