Anatomy Exam 3
1/224
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
225 Terms
What surrounds the heart?
The Heart is surrounded by a lining called the Pericardium
Where is the heart located?
Located in thorax (in middle mediastinum – between lungs)
Which vessels travel out of and into the heart?
Arteries travel out of heart (ascending aorta, pulmonary trunk)
Veins travel into heart (Superior & Inferior vena cava)
What is the purpose of the circulatory system?
To pump blood throughout the body including oxygen, carbon dioxide, nutrients, water, hormone, nitrogenous wastes, etc.
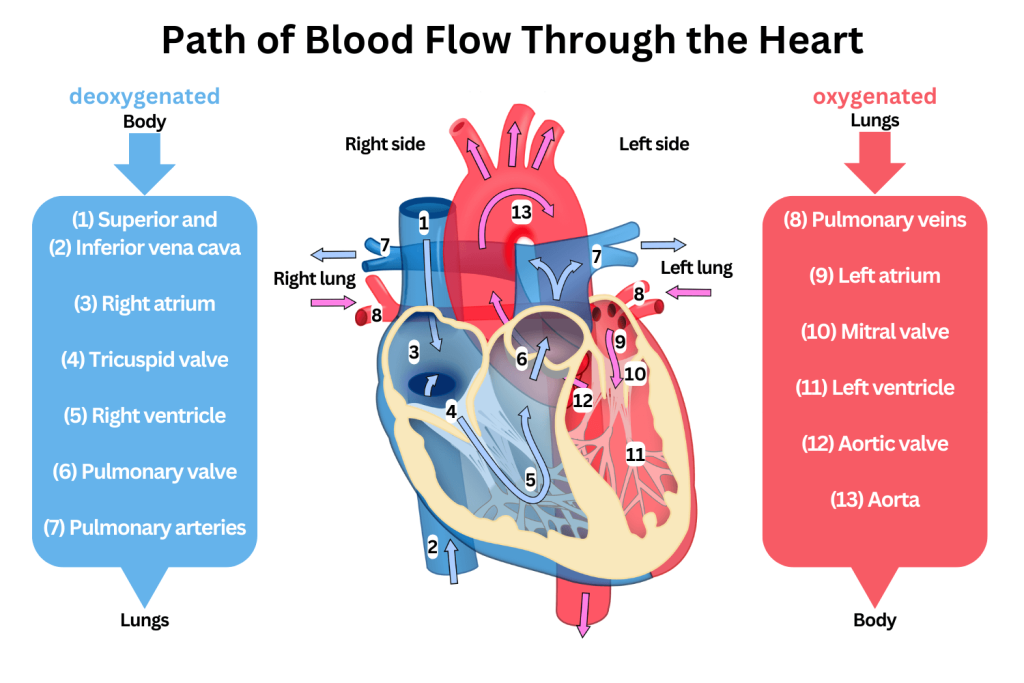
Pathway of blood flow (complete sequence)
Superior/Inferior Vena Cava → Right Atrium → Tricuspid Valve → Right Ventricle → Pulmonary Valve → Pulmonary Artery → Lungs → Pulmonary Vein → Left Atrium → Mitral (bicuspid) Valve → Left Ventricle → Aortic Valve → Aorta
What are the two functional units of the heart?
Pulmonary circuit: right side receives deoxygenated blood and pumps it to lungs
Systemic circuit: left side receives oxygenated blood and pumps it throughout the body
Define artery vs vein
An artery carries blood away from the heart
A vein carries blood towards the heart
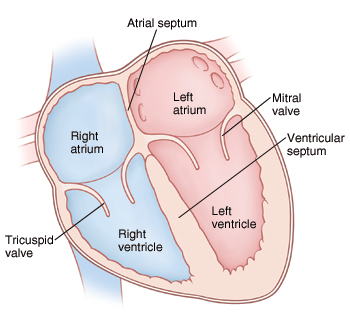
What are the four chambers of the heart?
Right Atrium
Left Atrium
Right Ventricle
Left Ventricle
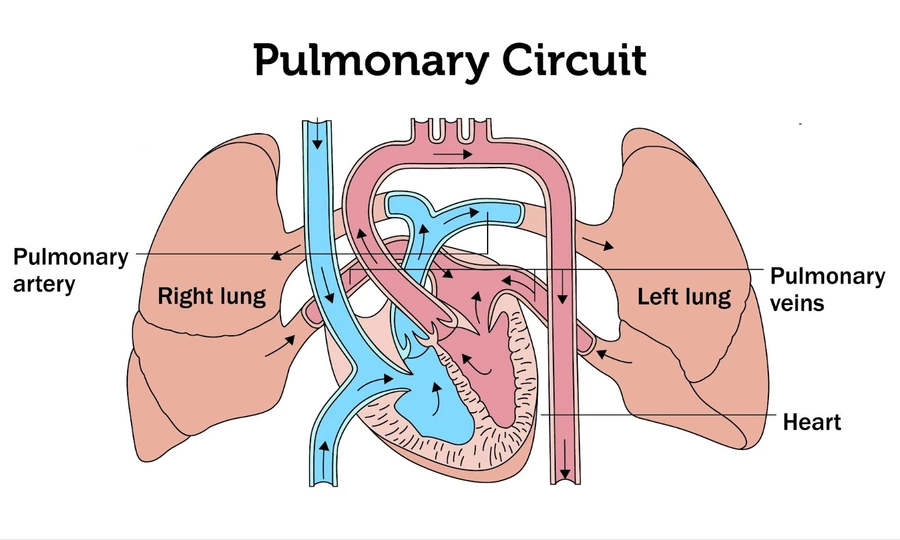
What do pulmonary arteries and veins carry?
Pulmonary arteries – carry deoxygenated blood to lungs
Pulmonary veins – return oxygenated blood to heart
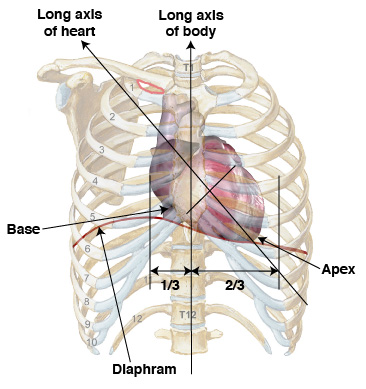
Position of the heart in the thorax
Not a midline structure Situated obliquely: 2/3 left, 1/3 right
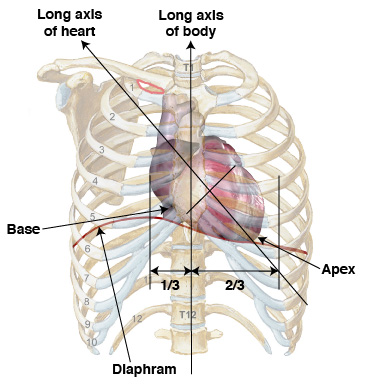
Where are the base and apex of the heart located?
Base: at the sternal angle Apex: 5th intercostal space (left), directed anteriorly and left
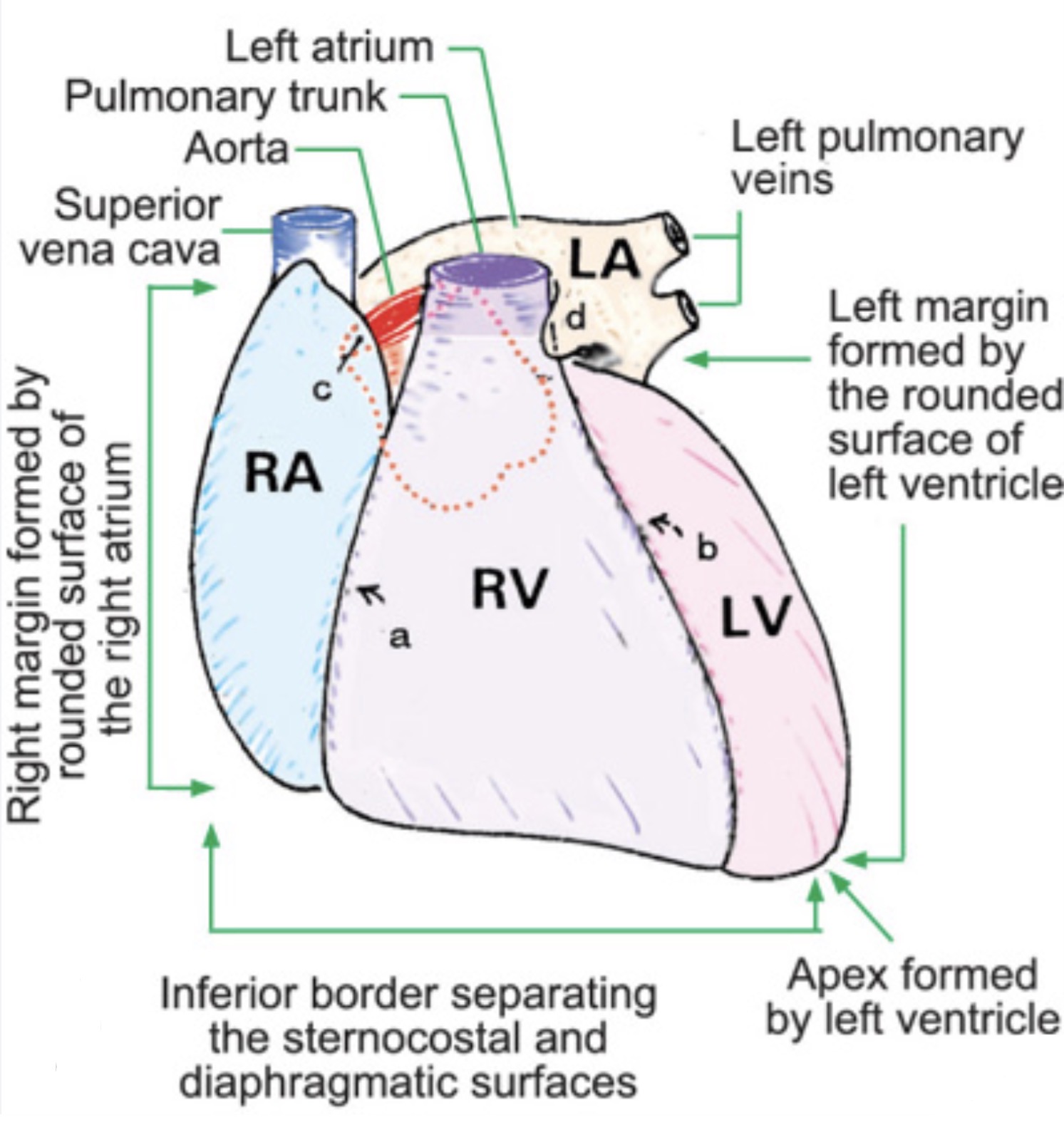
Borders of the heart
Anterior/inferior border: right and left ventricle
Left/lateral border: left ventricle and left atrium
Right border: right ventricle and right atrium
Superior border: aorta, superior vena cava, pulmonary trunk
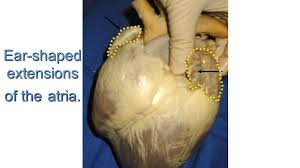
What is an auricle?
Each atrium has an Auricle (L: “ear”)
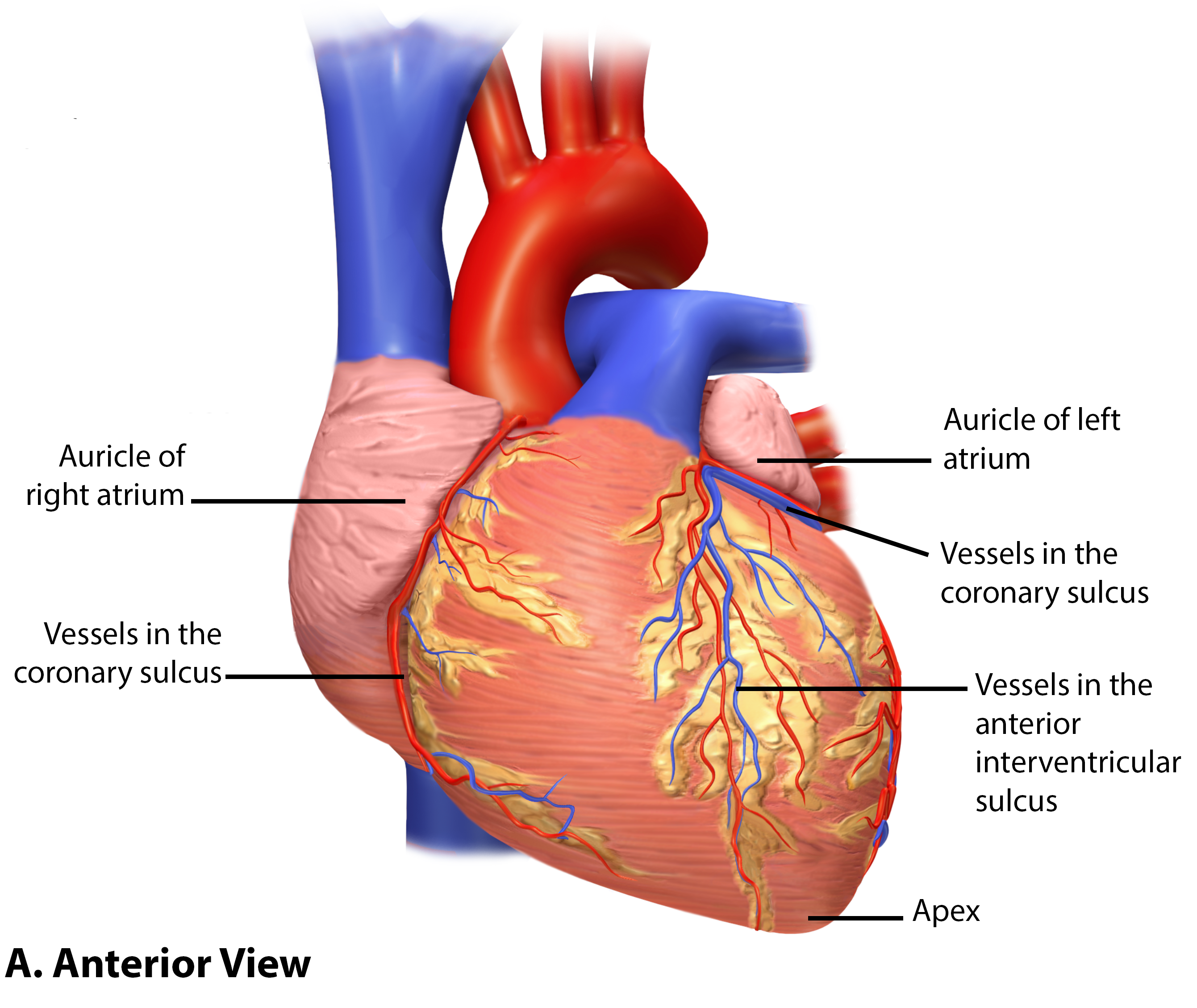
What structures exit the heart from the base?
Pulmonary trunk and Aorta
Coronary sulcus and interventricular sulcus
Coronary sulcus: depression between atria and ventricles
Interventricular sulcus: depression between right and left ventricles
Define pericardium
Peri = around + kardium = heart
A serous membrane that surrounds the heart
Layers of the pericardium
Inner: Visceral pericardium (Epicardium)
Outer: Parietal pericardium
Outside: Fibrous pericardium
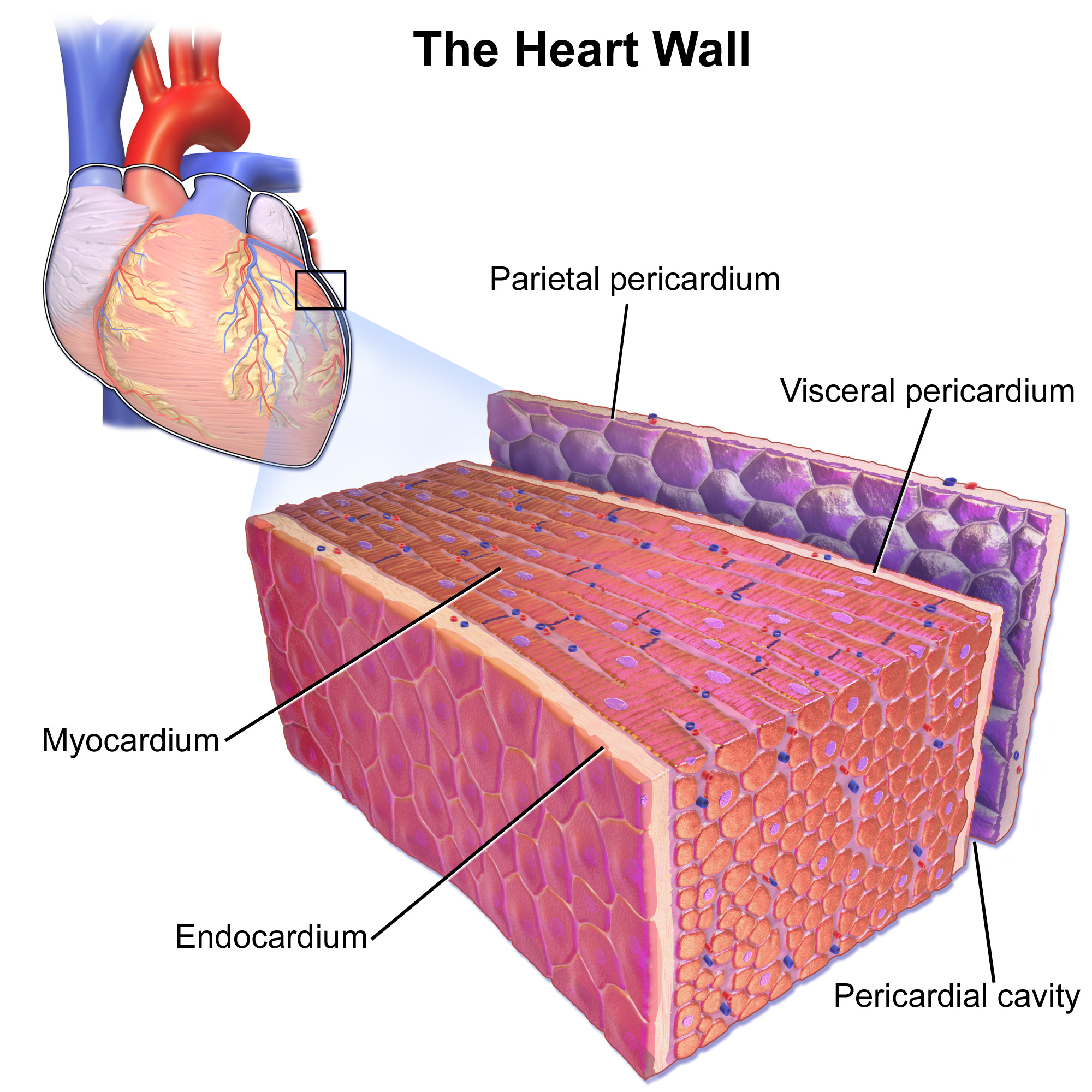
What is the pericardial cavity?
A serous fluid-filled space between visceral and parietal pericardium
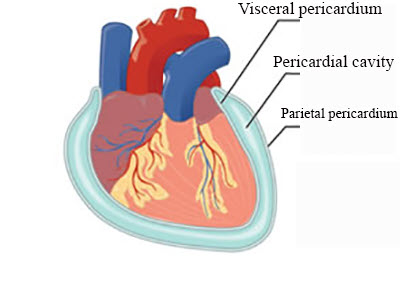
What is cardiac tamponade?
Accumulation of fluid in pericardial space prevents heart chambers from expanding and filling
Layers of the heart wall
Endocardium: endothelial lining
Myocardium: cardiac muscle
Epicardium: visceral pericardium
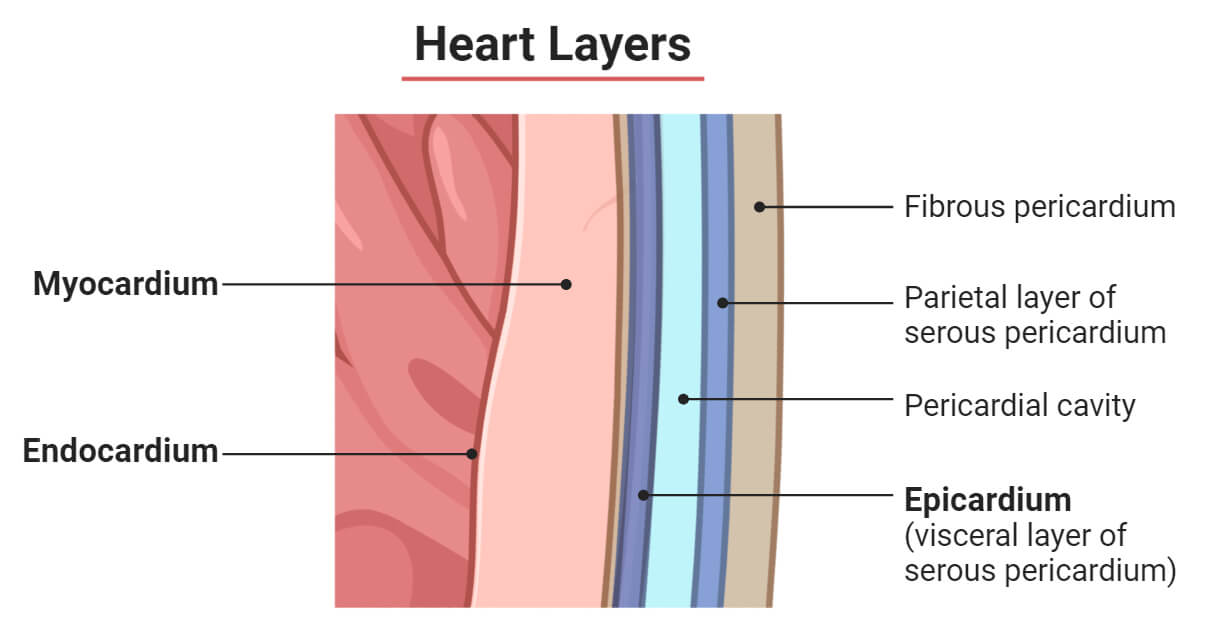
Characteristics of cardiac muscle
Striated, branching, single central nuclei
Cells communicate via gap junctions (intercalated discs)
Function of atria vs ventricles
Atria = filling chambers
Ventricles = pumping chambers
Blood flow into atria
Right atrium: receives deoxygenated blood (SVC & IVC)
Left atrium: receives oxygenated blood (pulmonary veins)
Septa of the heart
Interatrial septum: separates atria
Interventricular septum: separates ventricles
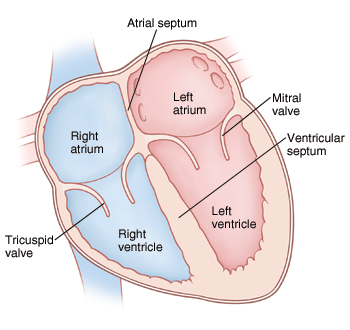
Why is left ventricular myocardium thicker?
Because it pumps blood through the aorta to the entire body
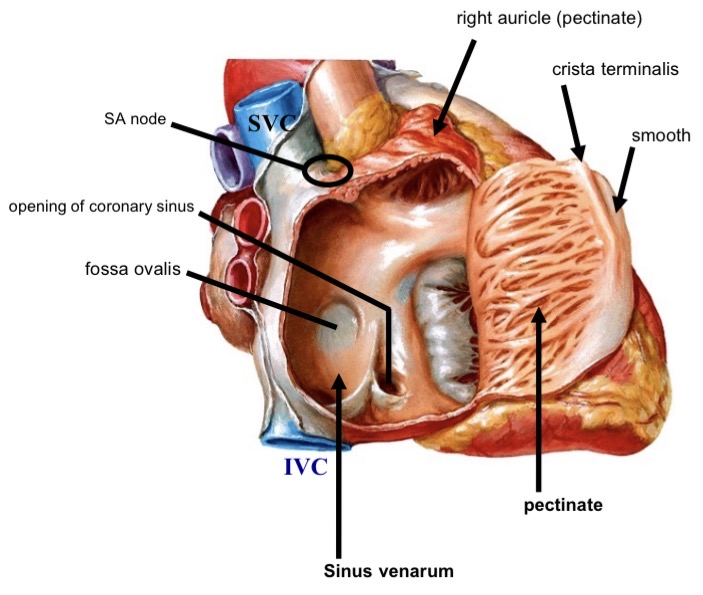
Structures of the right atrium
Sinus venarum (smooth posterior)
Pectinate muscle (anterior)
Crista terminalis
SVC
IVC
Coronary sinus
Fossa ovalis
SA node
AV node
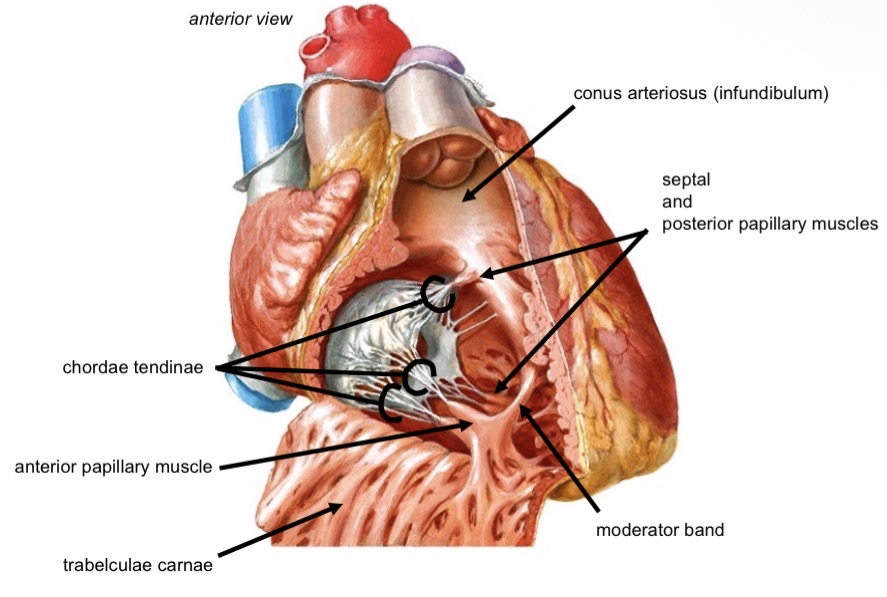
Structures of the right ventricle
Trabeculae carnae
Conus arteriosus (infundibulum)
Papillary muscles (anterior, posterior, septal)
Chordae tendinae
Moderator band (Purkinje fibers)
Function of papillary muscles and chordae tendinae
Papillary muscles contract to tighten valve cusps
Chordae tendinae connect papillary muscles to valves
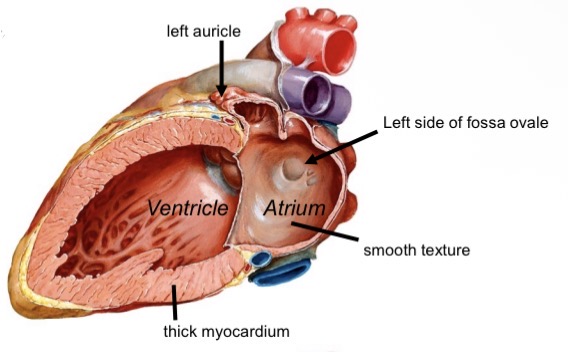
Left atrium structure
Smooth-walled chamber
Receives four pulmonary veins
Contains left auricle with pectinate muscle
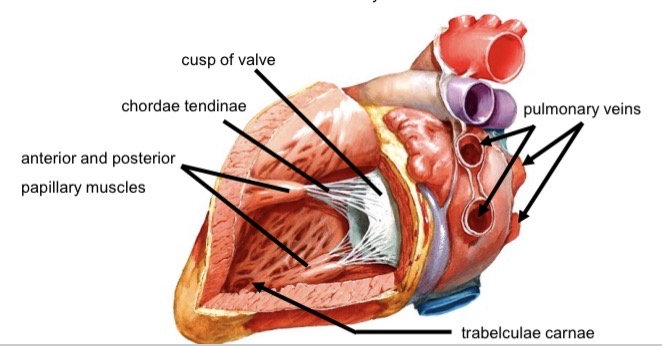
Left ventricle structure
Trabeculae carnae
Thickest myocardium
Papillary muscles (anterior, posterior)
Chordae tendinae
Atrioventricular valves
Tricuspid valve (right)
Mitral/Bicuspid valve (left)
Semilunar valves
Aortic semilunar valve
Pulmonary semilunar valve
Fetal circulation – umbilical vessels
Umbilical vein: oxygenated blood to heart
Umbilical artery: deoxygenated blood to placenta
Foramen ovale
Hole allowing blood flow from right atrium to left atrium
Closes after birth → fossa ovalis
Ductus arteriosus
Carries blood from pulmonary artery to aorta
Diverts oxygenated blood away from lungs
Atrial septal defect (ASD)
Patent foramen ovale remains open
Right atrium pressure increases over time
Deoxygenated blood enters left atrium → hypoxia
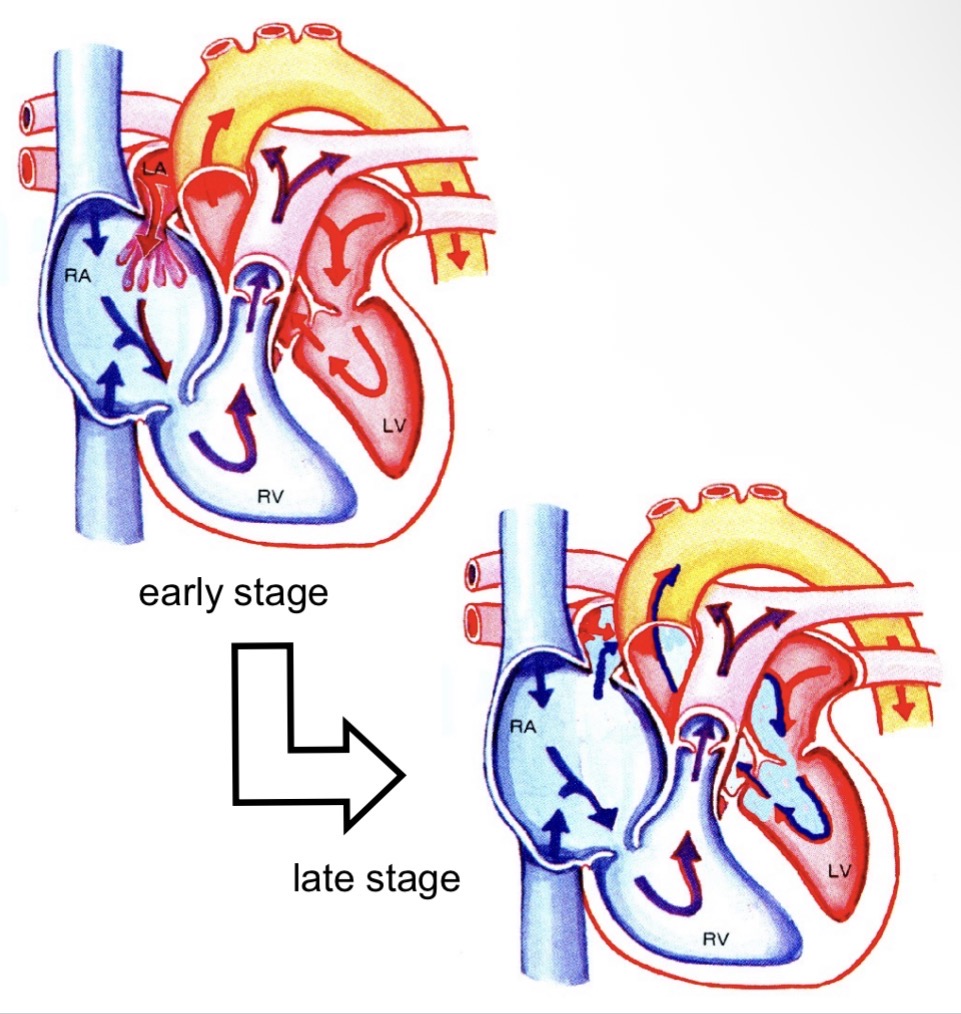
Ventricular septal defect (VSD)
Incomplete interventricular septum
“Hole in the heart”
Coronary arteries origin and function
Supply myocardium
Arise from aorta distal to aortic semilunar valve
Fill during diastole
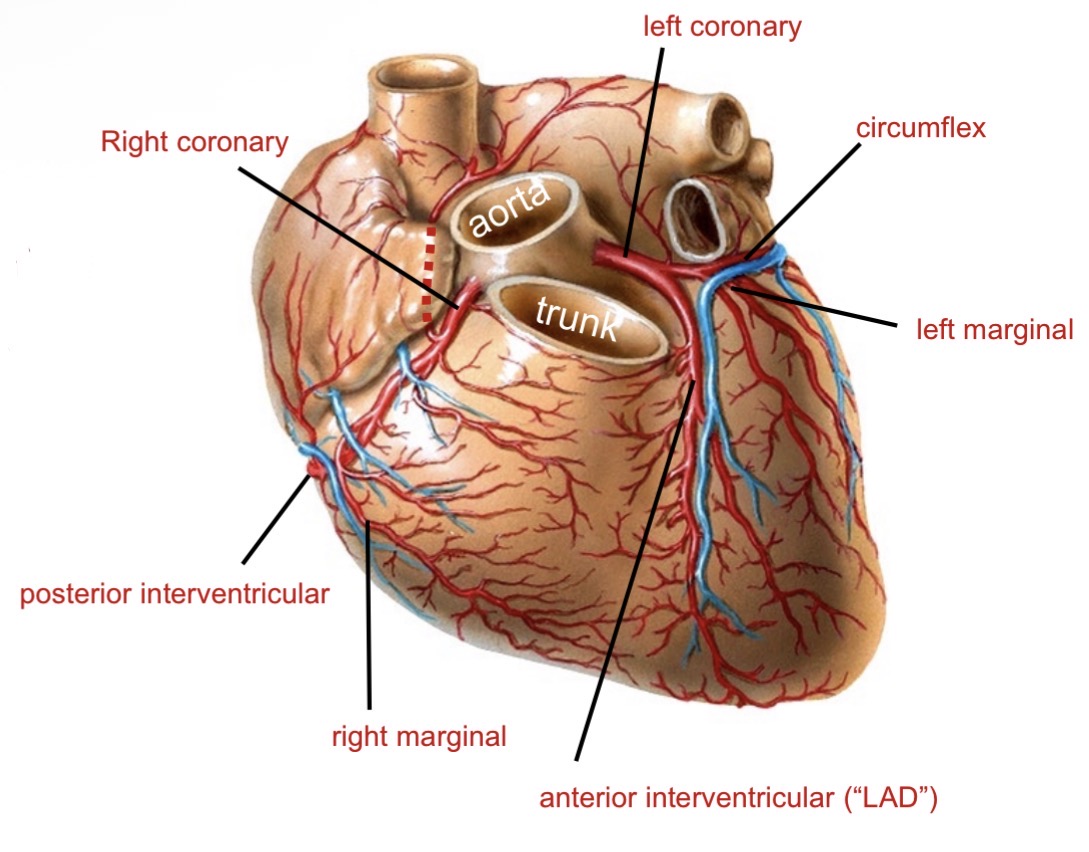
Branches of coronary arteries
Left coronary → LAD + circumflex
Right coronary → right marginal + posterior interventricular
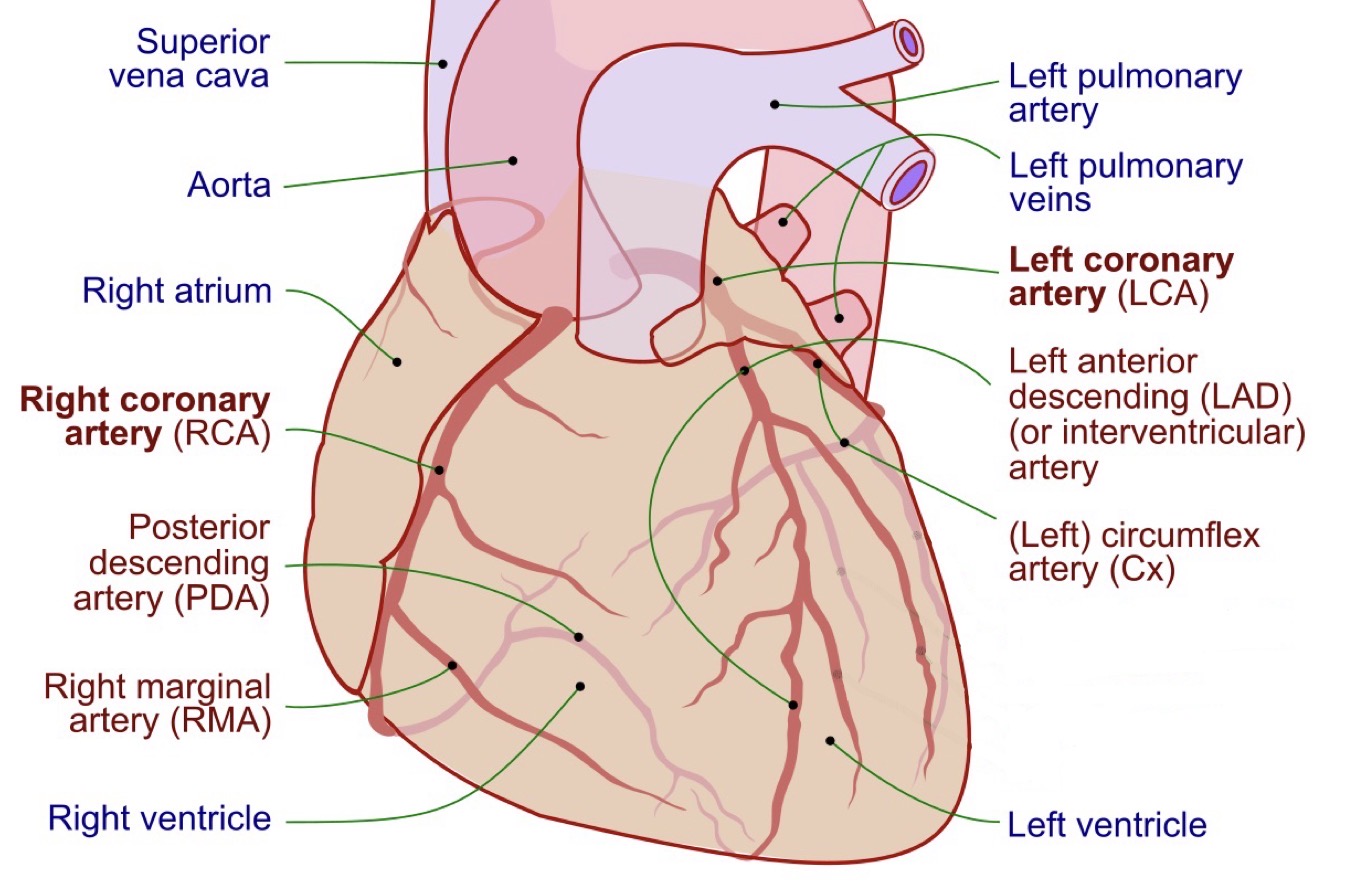
What causes myocardial infarction?
Arteriosclerosis → plaque → rupture → thrombus → occlusion → heart attack (cell death)
Cardiac veins and drainage
Great, middle, small cardiac veins
Drain into coronary sinus → right atrium
Smallest cardiac veins
Drain directly into chambers (right atrium and ventricle)
“Running mates” in cardiac circulation
Arteries and veins run together
Great cardiac vein with Anterior Interventricular Artery and Circumflux
Middle cardiac vein with Posterior interventricular artery
Small cardiac artery with Right marginal branch
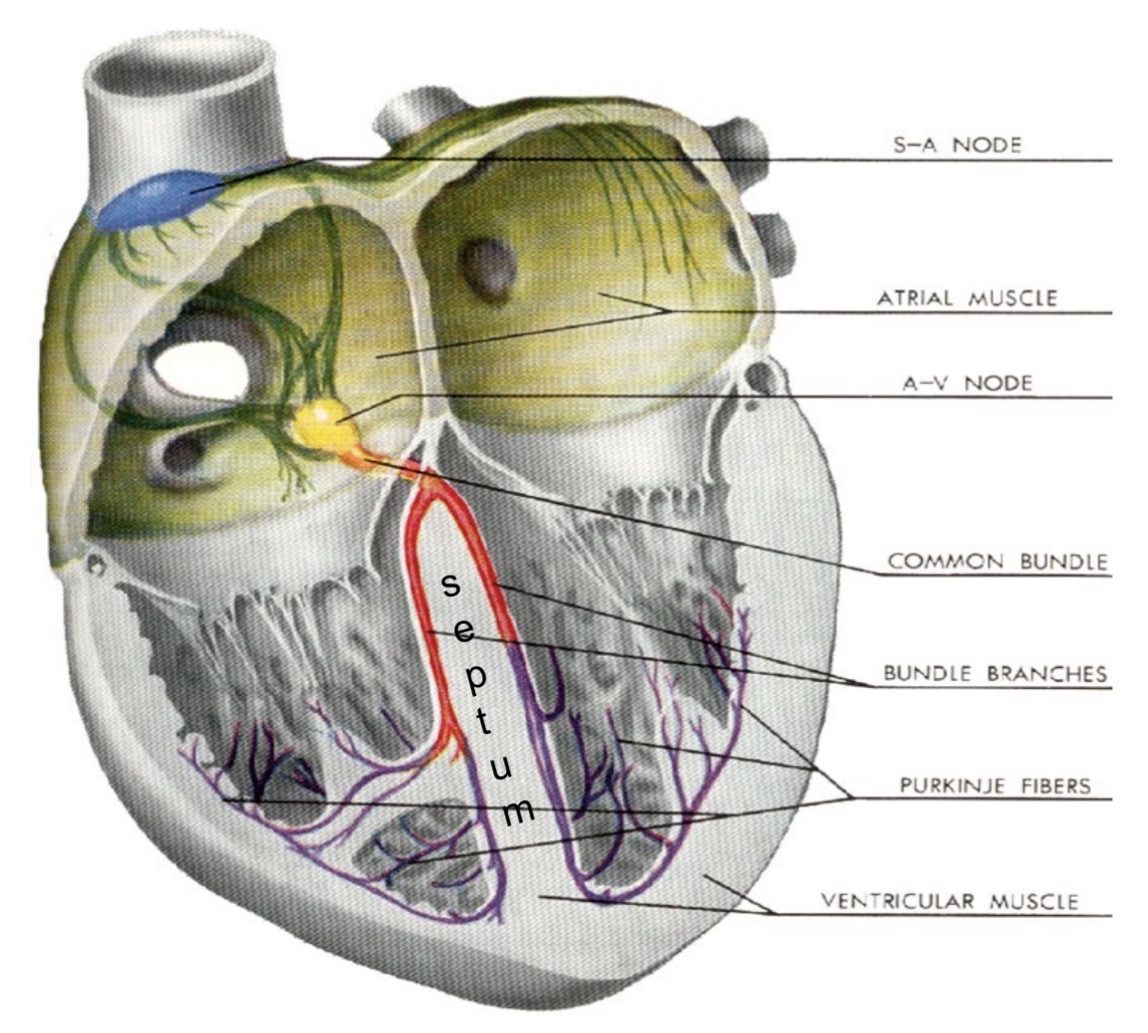
Cardiac skeleton functions
Dense connective tissue
Encircles valves
Anchors myocardium
Supports valves
Blocks electrical impulse between atria and ventricles
Electrical conduction pathway of the heart
SA node → atrial myocardium → AV node → bundle branches → apex → Purkinje fibers → ventricular myocardium
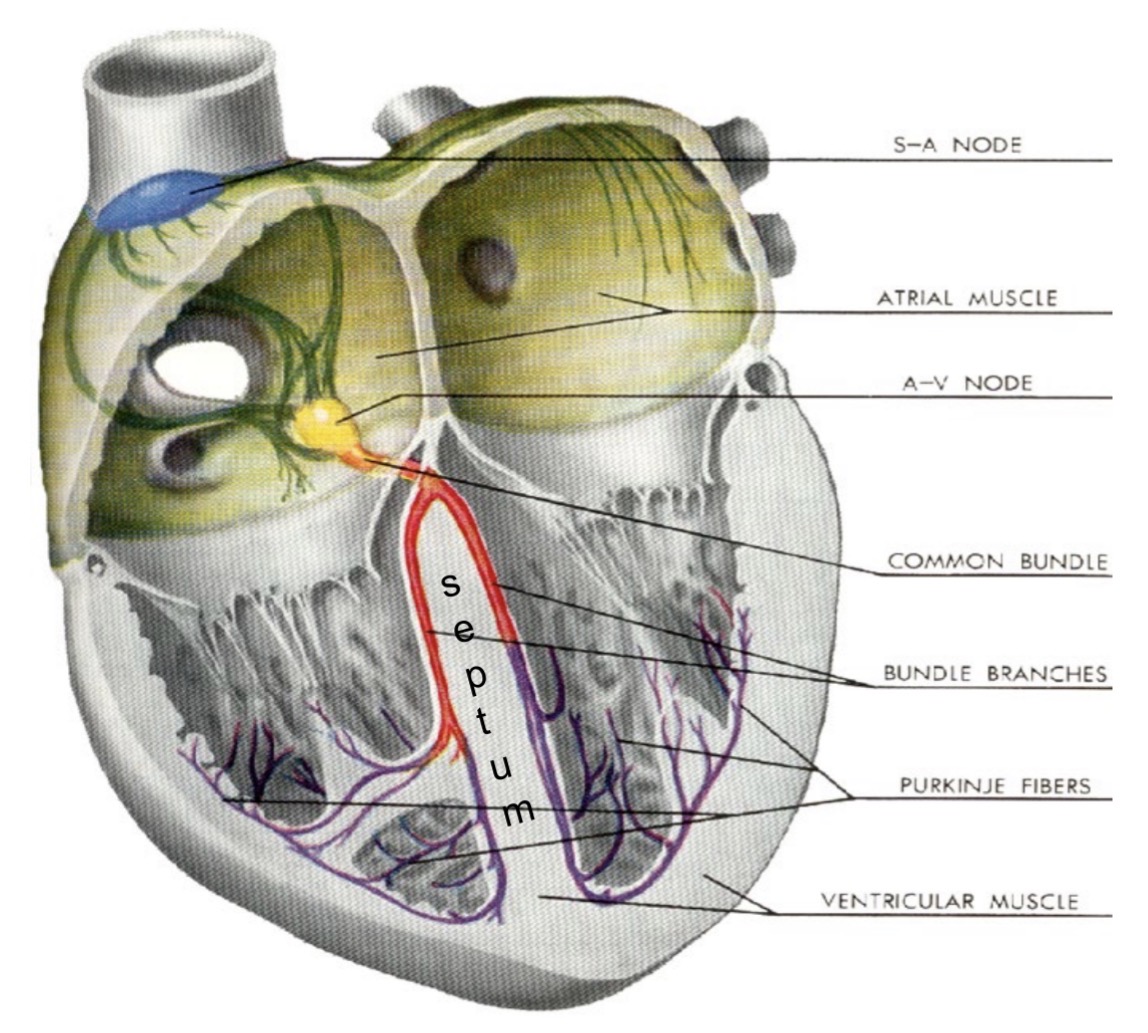
Role of Purkinje fibers
Carry impulses from bundle branches to papillary muscles and ventricular myocardium
Define systole and diastole
Systole = contraction
Diastole = relaxation
Heart sounds (LUB and DUB)
LUB: AV valves close during systole
DUB: semilunar valves close during diastole
Sympathetic and Parasympathetic innervation of the heart
Vagus nerve (CN X) = parasympathetic innervation
Sympathetic nerves innervate cardiac plexus to increase heart rate
Typical pattern of blood flow through vessels
heart → artery → arteriole → capillary → venule → vein → heart
Define systole in terms of vessels and circulation
Systole = ventricular contraction (atrial relaxation), pump blood to lungs, exchange CO2 for O2
Define diastole in terms of vessels and circulation
Diastole = ventricular relaxation (atrial contraction), return O2 to heart
How does the heart move blood through vessels in terms of pressure?
The pressure in arteries is high
The pressure in capillaries and veins is low
Arterioles serve to reduce pressure
The pressure is high during systole
The pressure is lower during diastole
What are blood vessels structurally?
Blood vessels are tubules
What are the three tunics of blood vessels?
Tunica intima
Tunica media
Tunica externa
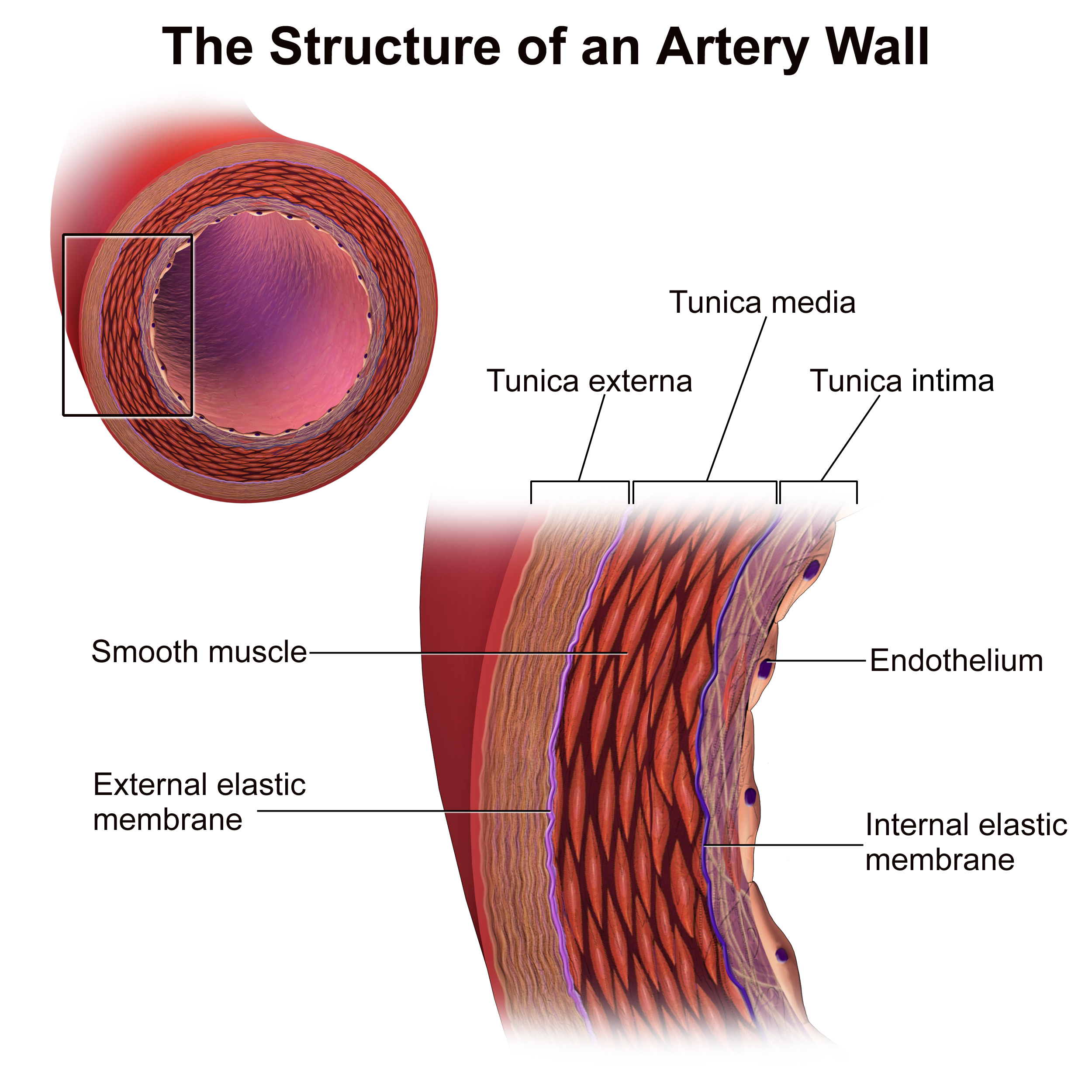
Describe the tunica intima
Innermost, thinnest layer of an artery or vein
Smooth endothelial lining
Supportive basement membrane
What is the internal elastic lamina?
Provides ability to expand and recoil
Separates intima from media
Describe the tunica media
Smooth muscle under autonomic innervation
Regulates blood flow and pressure
Thickest layer in arteries, but thinner in veins
Describe the tunica externa (adventitia)
Outermost layer
Made of collagen and elastic fibers
Supports and protects vessel
Anchors to surrounding tissues
What is the external elastic lamina?
Provides ability to expand and recoil
Separates media from external
Febestrated
What is the size of a capillary?
A capillary has a diameter of a single Red Blood Cell
How is an artery structured compared to a capillary?
An artery = a capillary (endothelium + sub-endothelial) with 2 more layers
Thus 3 tunics around a lumen
Types of capillaries
Continuous
Fenestrated
Sinusoidal
Continuous capillaries
Permeable to gases (O2 & CO2) and water
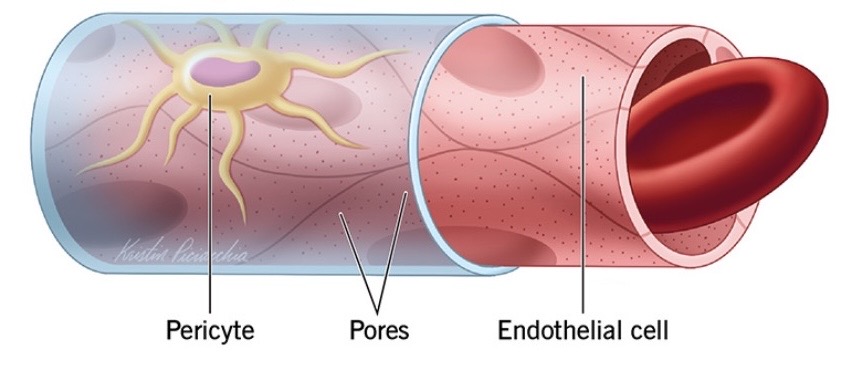
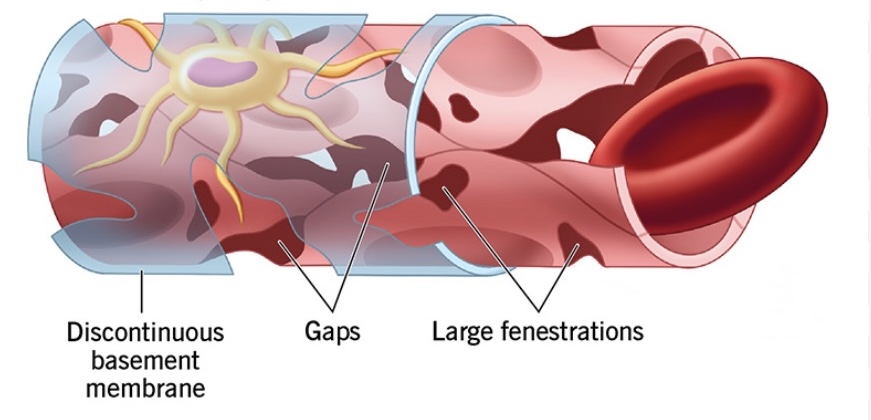
Fenestrated capillaries
(L. “window”) permeable to molecules and peptides (i.e. hormones)
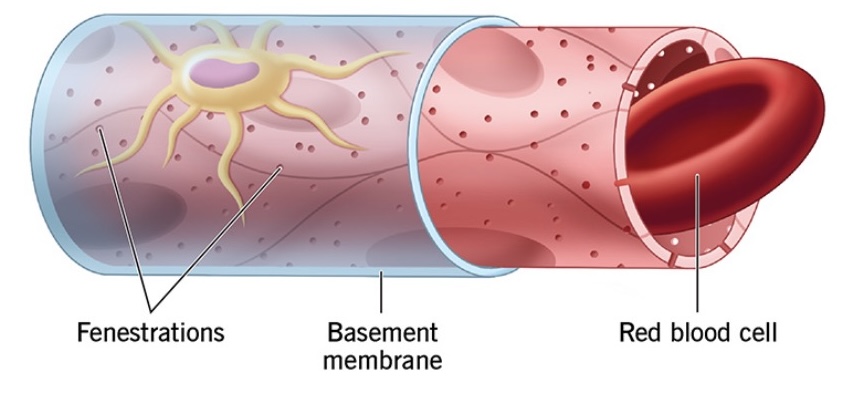
Sinusoidal capillaries
(“open space”) permeable to proteins and cells Found in liver and spleen
Segments of the aorta
Ascending aorta
Arch
Descending aorta
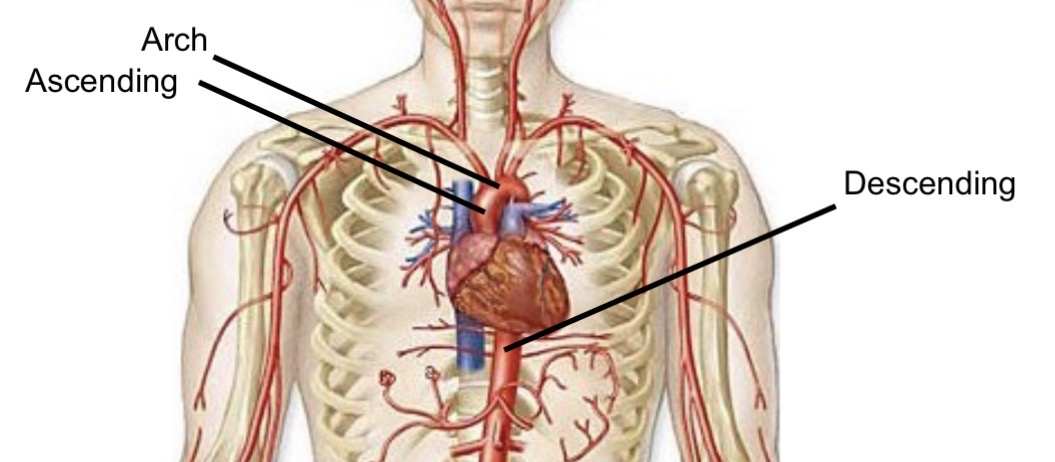
What happens to the descending aorta after the thorax?
Becomes the abdominal aorta
Branches of the aortic arch
Brachiocephalic trunk
Right Subclavian and Right Common carotid branch off of brachiocephalic trunk
Left common carotid artery
Left subclavian artery
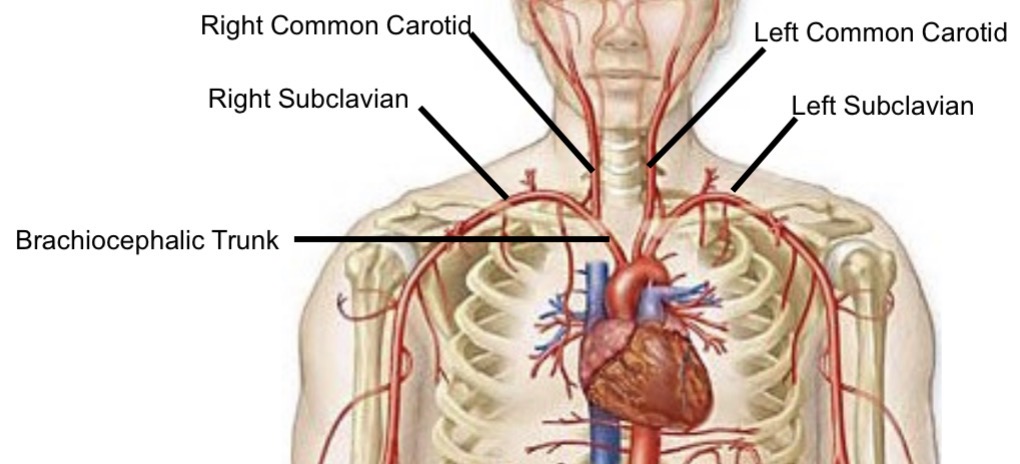
Brachiocephalic trunk branches
Right subclavian artery
Right common carotid artery
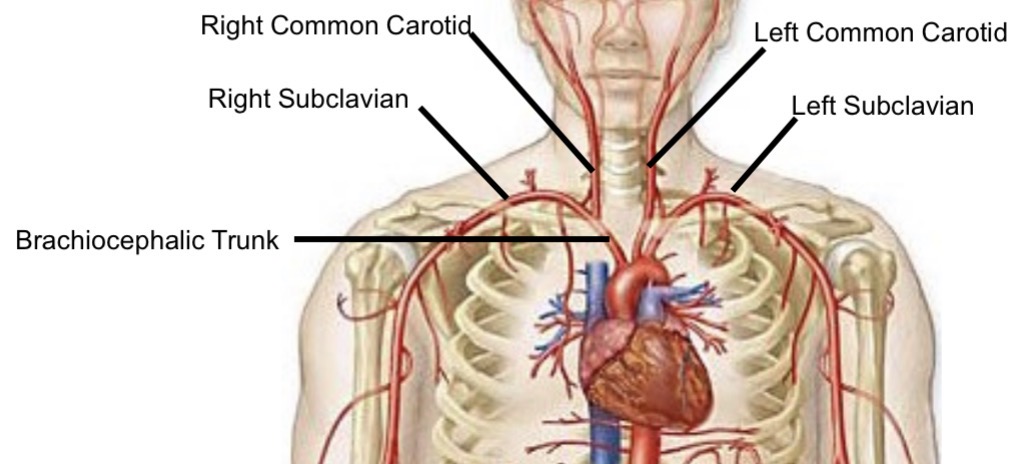
Meaning of “common” in arteries
Indicates an artery that will bifurcate
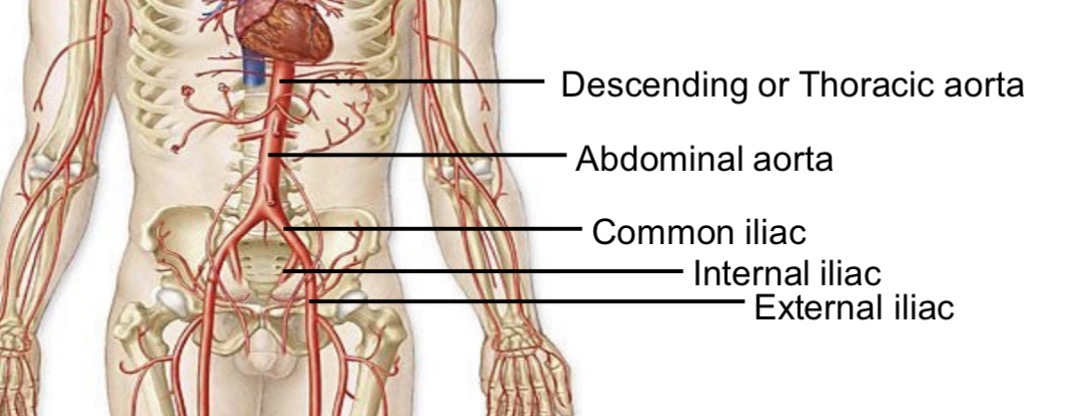
Abdominal aorta branching
Bifurcates to left and right common iliac arteries
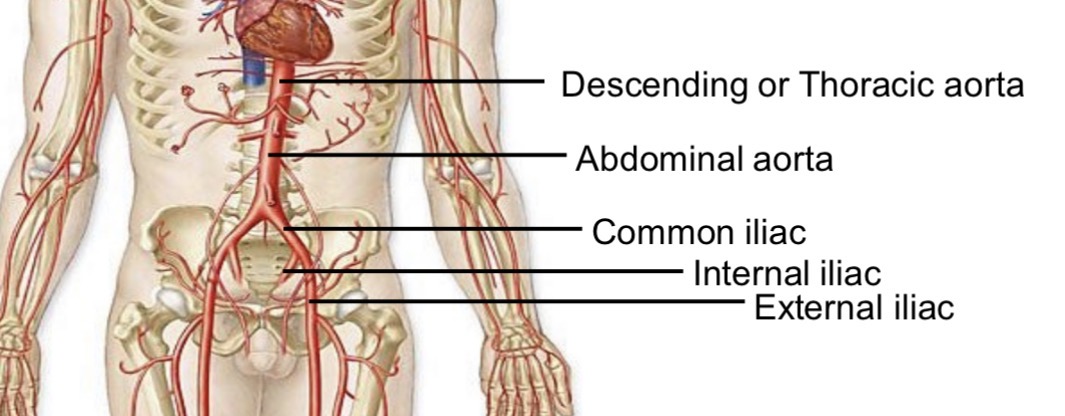
Common iliac artery branches
Internal iliac
External iliac
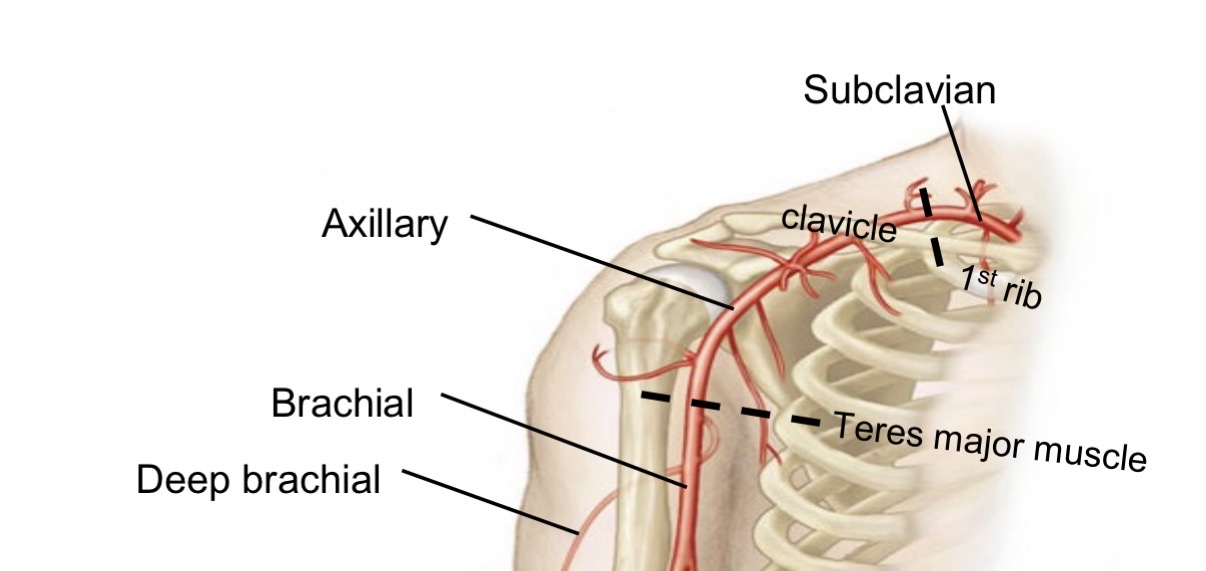
Subclavian artery pathway in upper limb
Becomes axillary artery (passes first rib)
Becomes brachial artery (passes teres major)
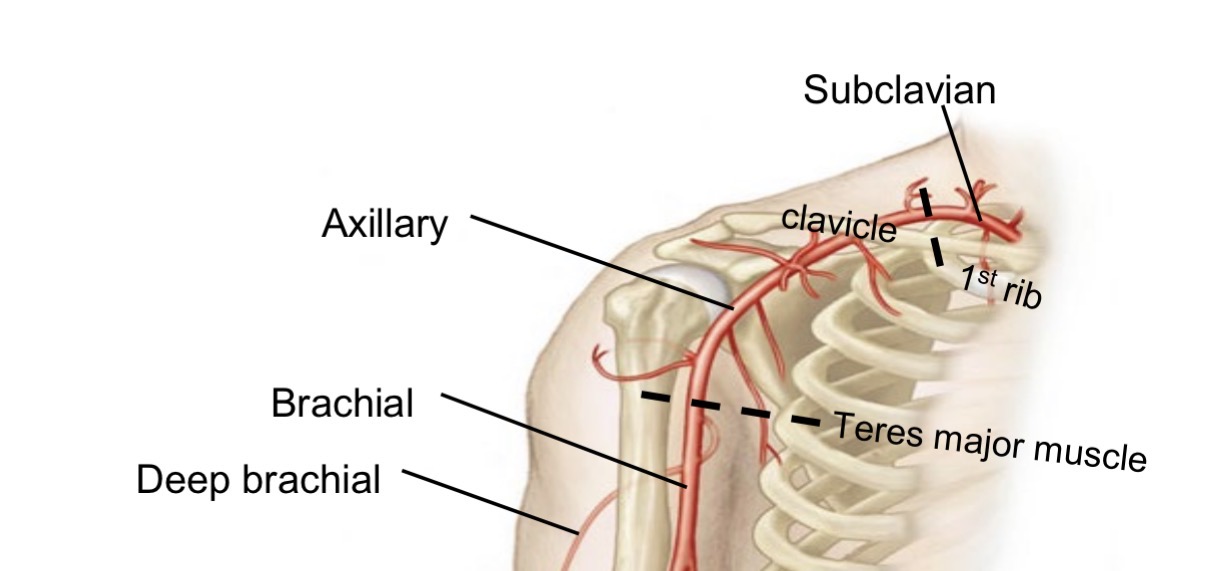
Deep brachial artery
Branch of brachial artery
Runs posterior to humerus
Supplies triceps brachii
Brachial artery branches
Radial artery (lateral)
Ulnar artery (medial)
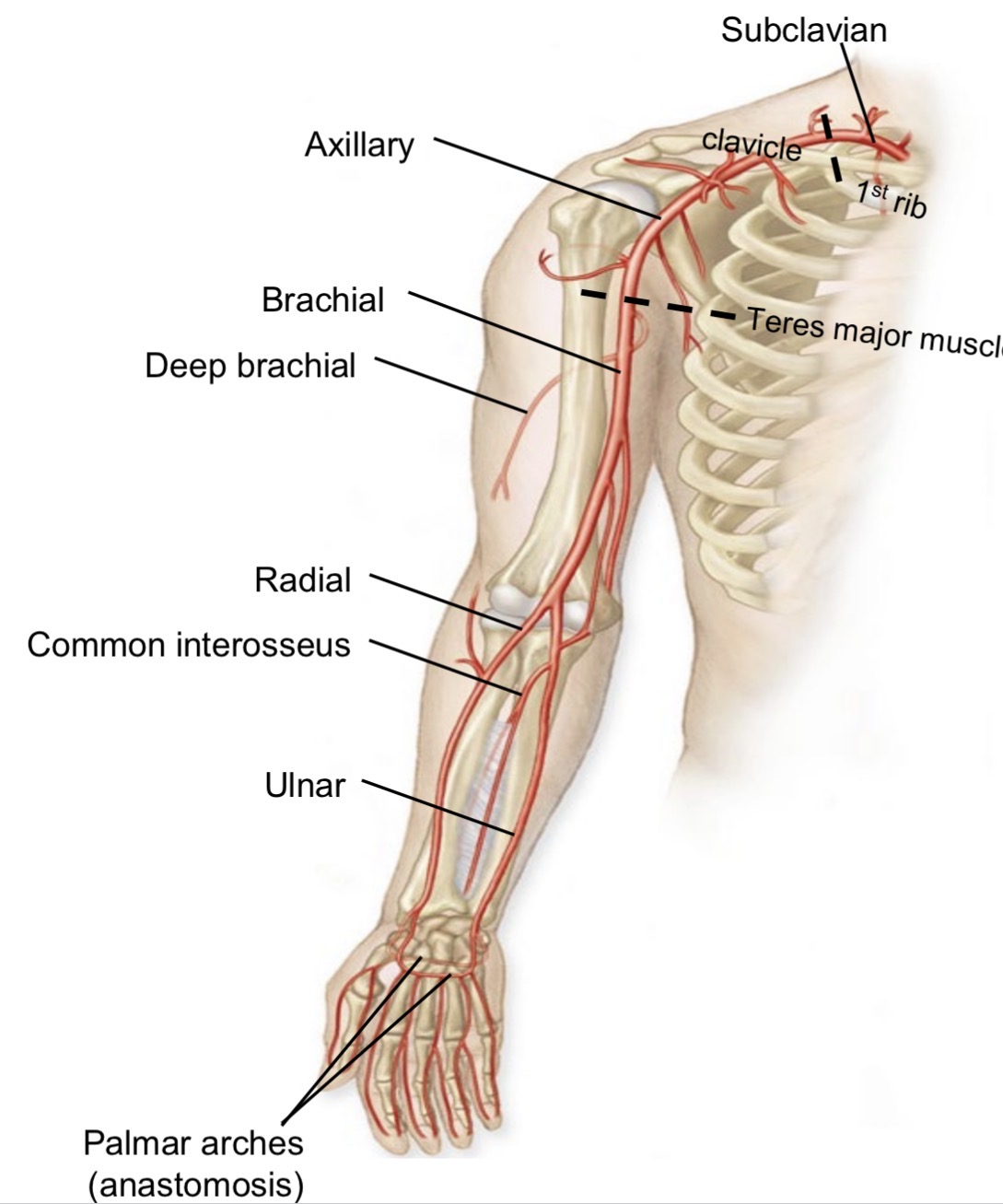
Common interosseous artery
Branch of ulnar artery
Runs between bones
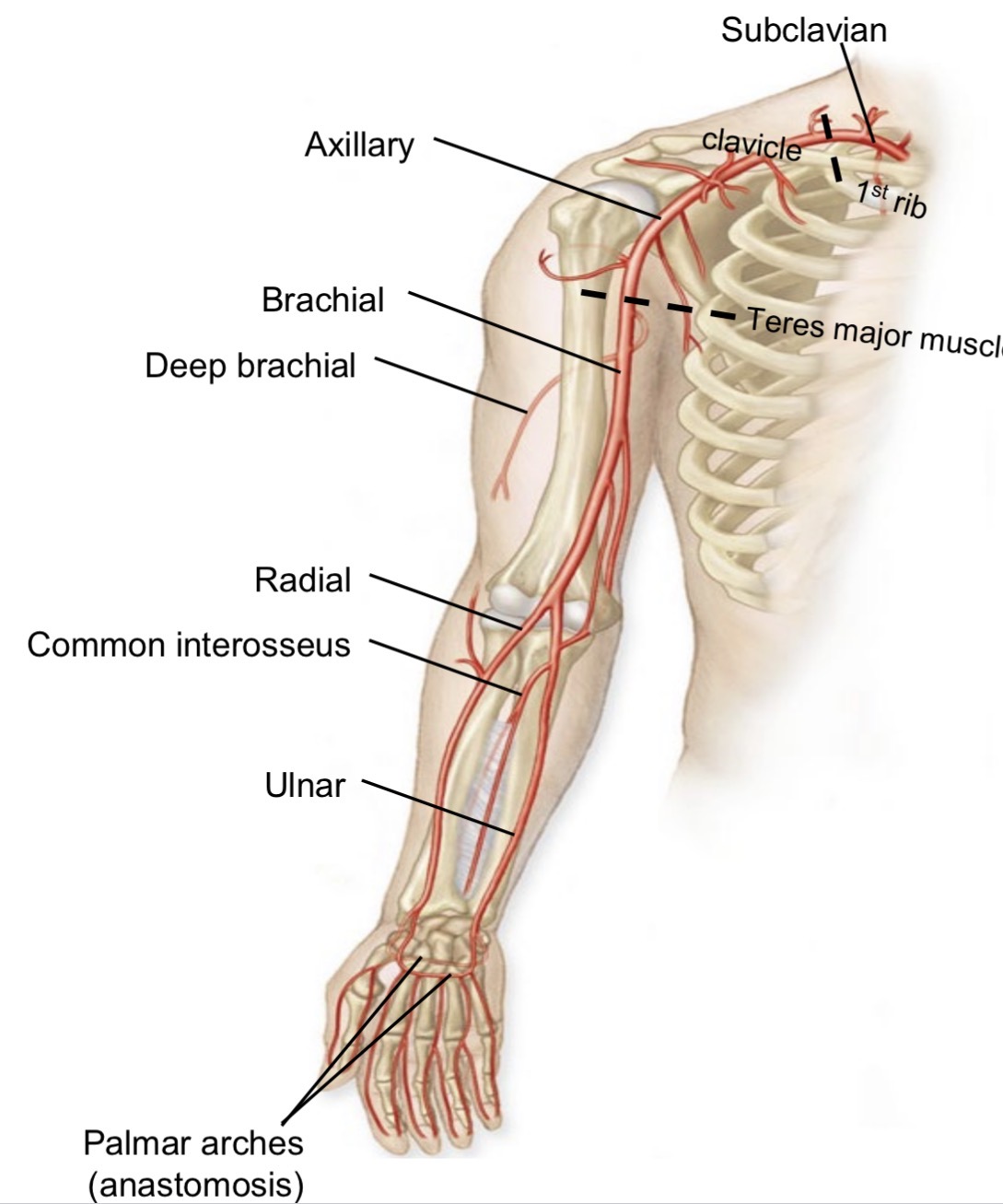
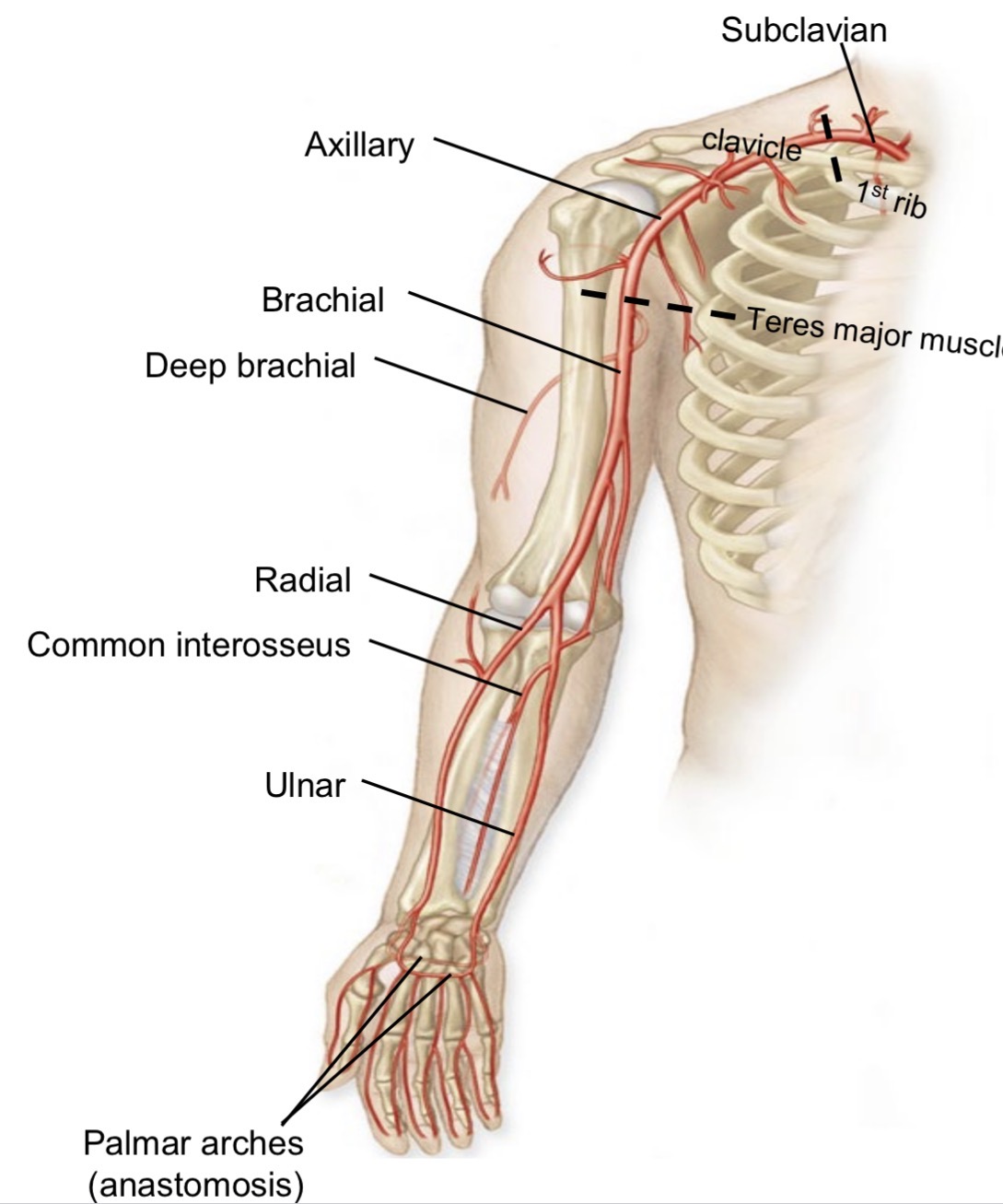
Palmar arches
Formed by radial and ulnar arteries
Anastomose to form collateral circulation of forearm and hand
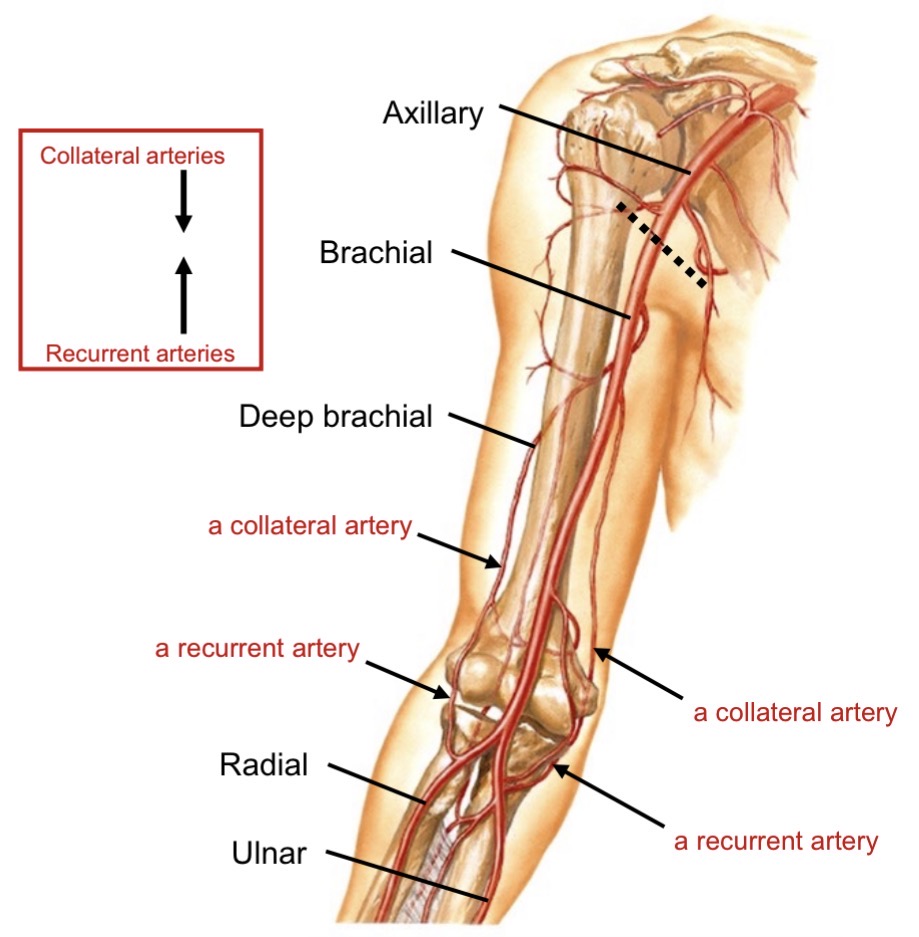
Collateral circulation around elbow
Occurs if brachial artery occluded
Collateral arteries and recurrent arteries anastomose
Define collateral vs recurrent arteries
Collateral: branches from brachial artery
Recurrent: branches from radial or ulnar arteries
Common carotid artery branching
Bifurcates to internal and external carotid arteries
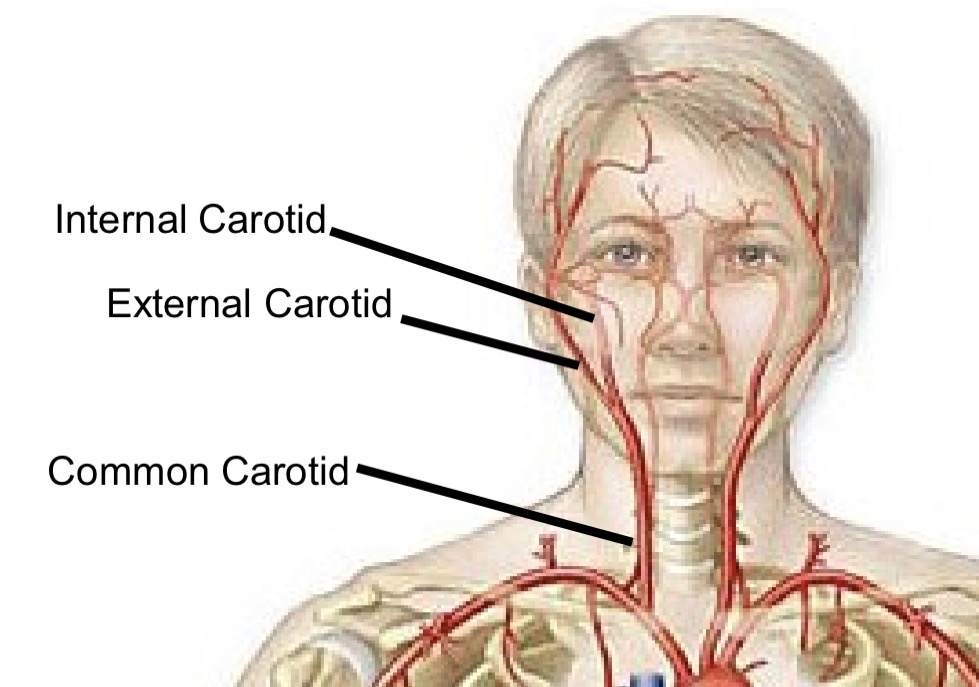
External carotid artery function
Supplies external head (lots of branching)
Internal carotid artery function
Supplies anterior and middle cerebral hemispheres
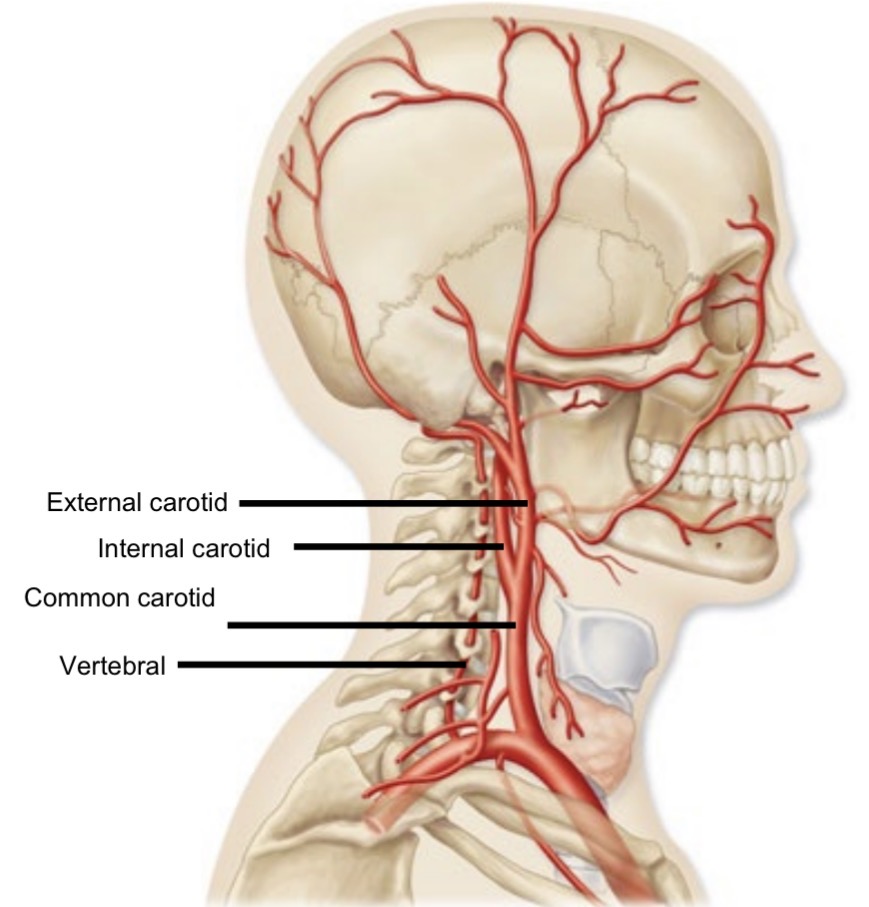
Vertebral artery
Branch of subclavian artery
Supplies posterior cerebral hemisphere
Travels through transverse foramina
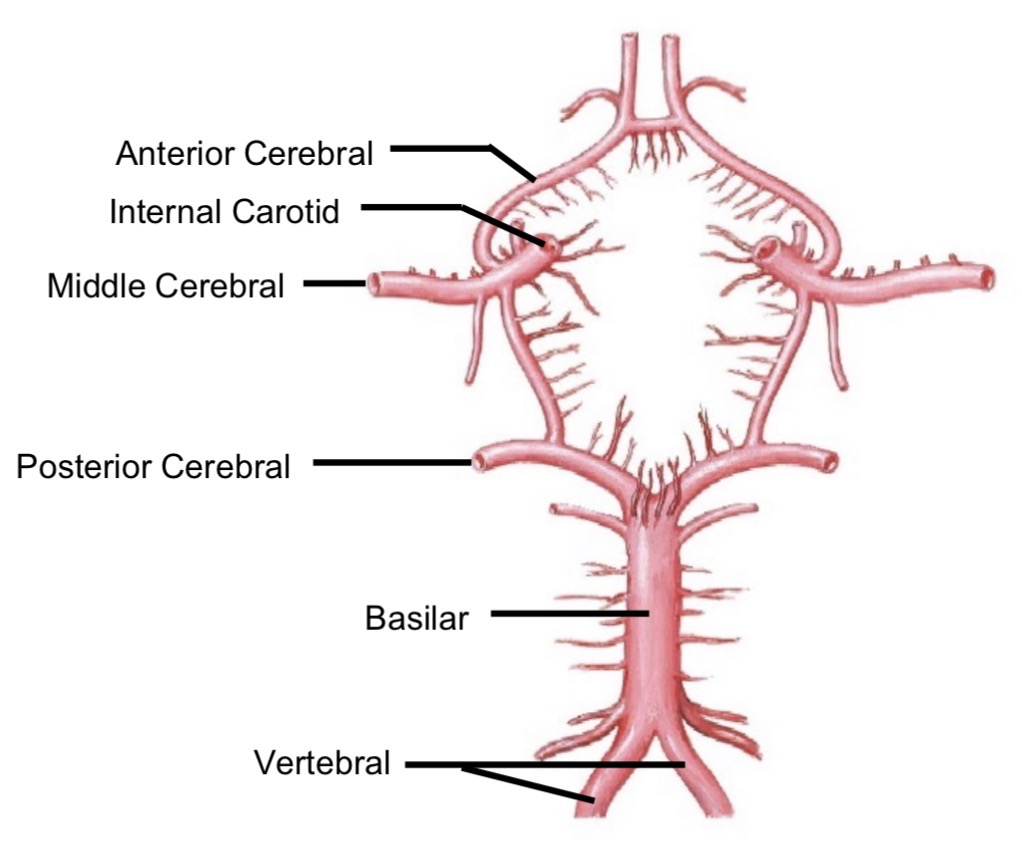
Circle of Willis
Cerebral arterial circle providing collateral circulation
Internal carotid artery pathway
Carotid canal → foramen lacerum → middle cranial fossa
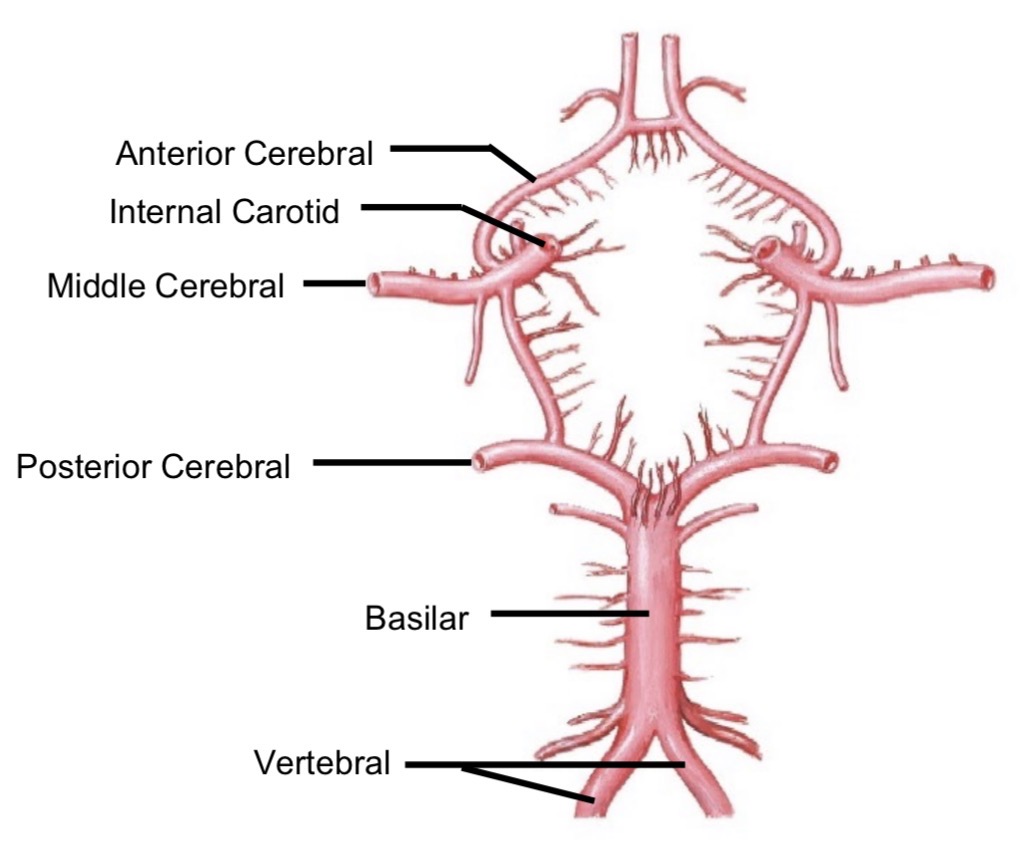
Anterior cerebral artery
Supplies frontal lobes
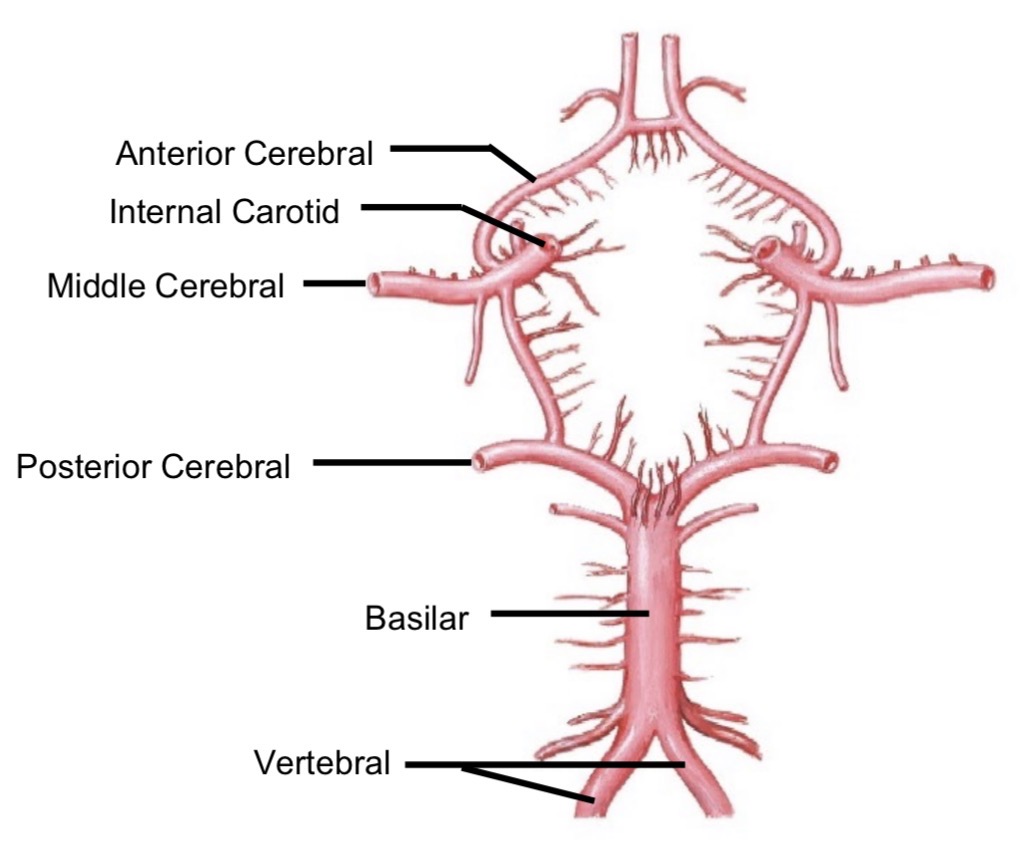
Middle cerebral artery
Supplies anterior portions of parietal and temporal lobes
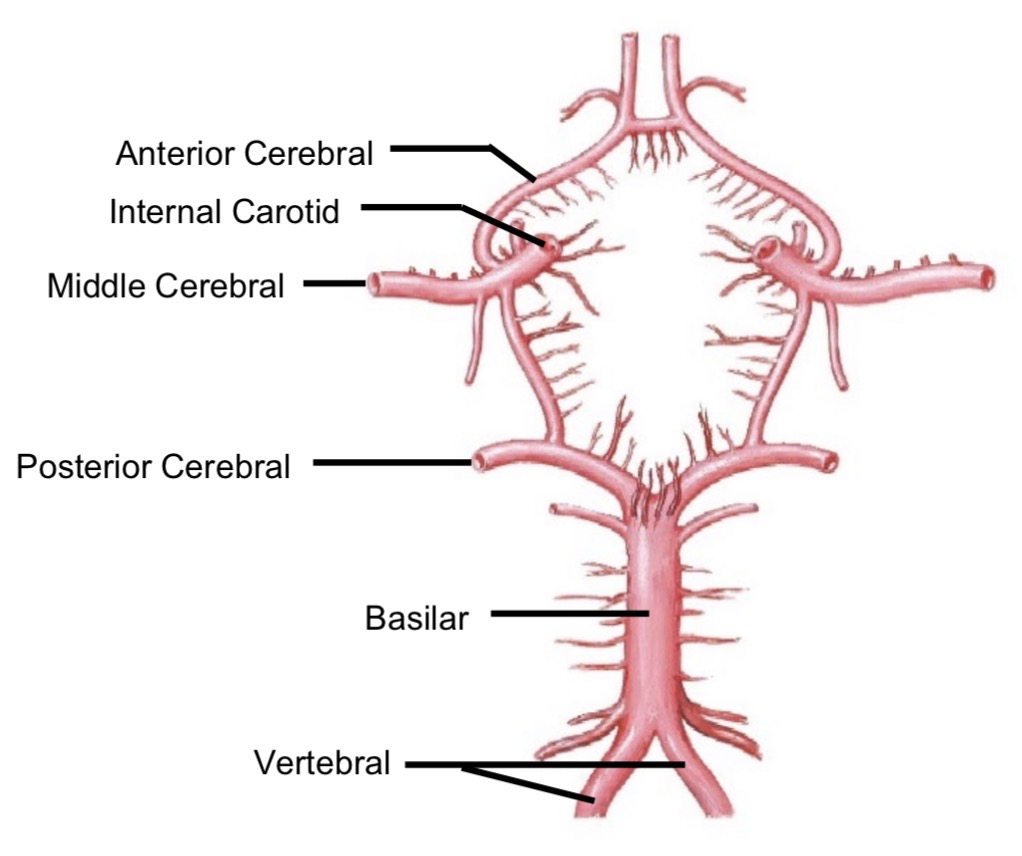
Vertebral artery pathway
Vertebral artery → Transverse foramina → foramen magnum → posterior cranial fossa → right and left posterior cerebral arteries
Posterior cerebral artery
Supplies posterior parietal, temporal, occipital lobe, cerebellum
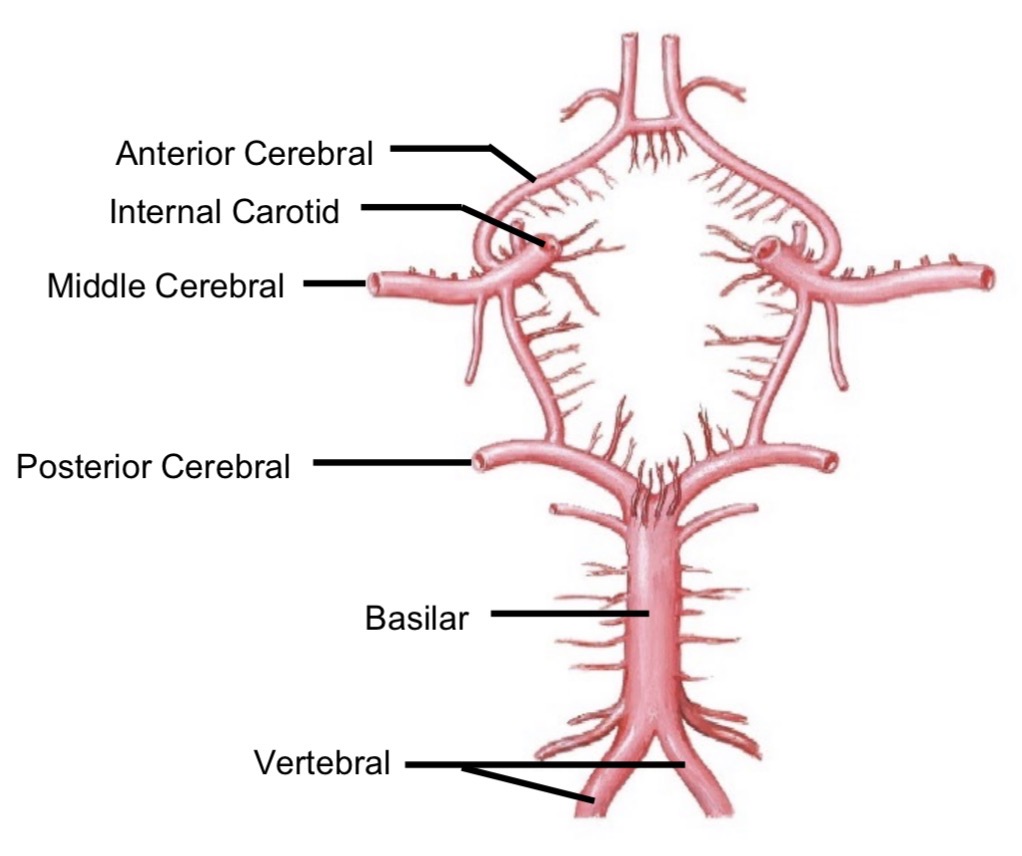
Why is the Circle of Willis important?
Provides collateral circulation in case of occlusion
Compensation for internal carotid occlusion
Blood flows via posterior cerebral + posterior communicating and/or anterior cerebral + anterior communicating
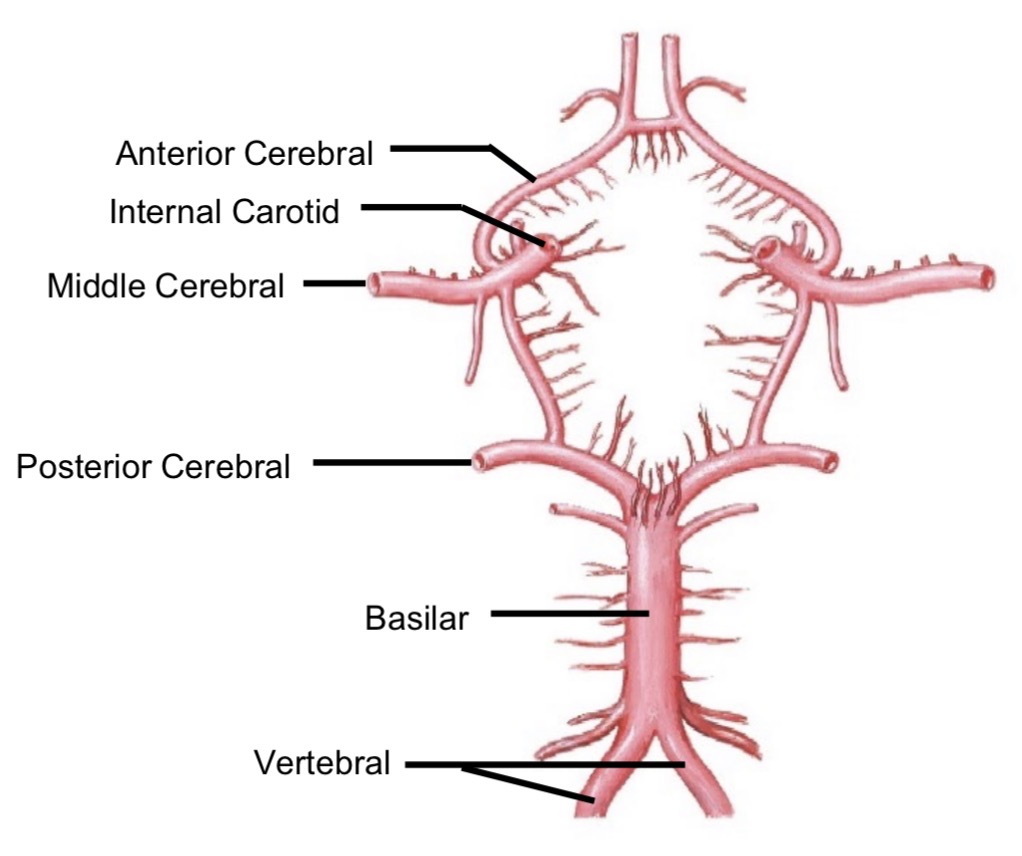
Compensation for basilar artery occlusion
Blood flows via middle cerebral + posterior communicating
Lower limb arterial pathway (overview)
Abdominal aorta → common iliac → external iliac → femoral → popliteal → tibial arteries
External iliac artery transition
Passes under inguinal ligament → becomes femoral artery
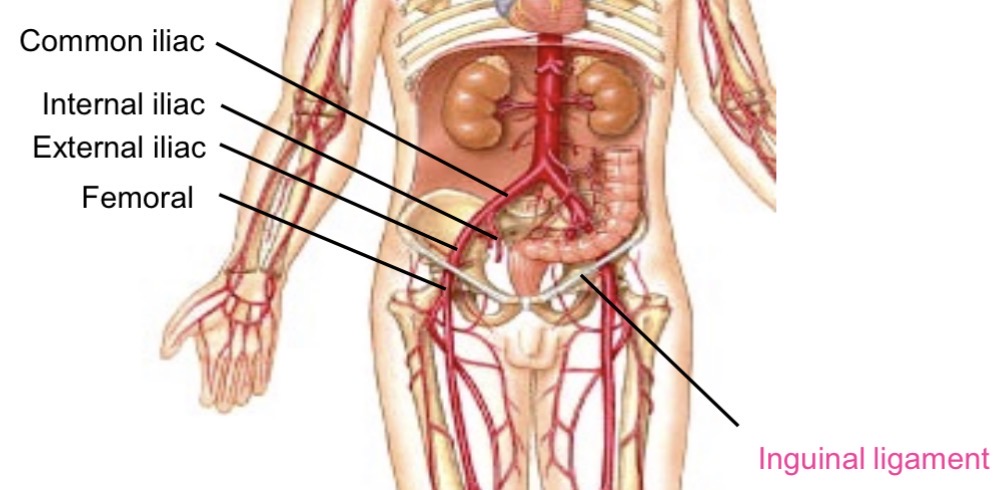
Deep femoral artery
Supplies hamstrings
Runs posterior to femur
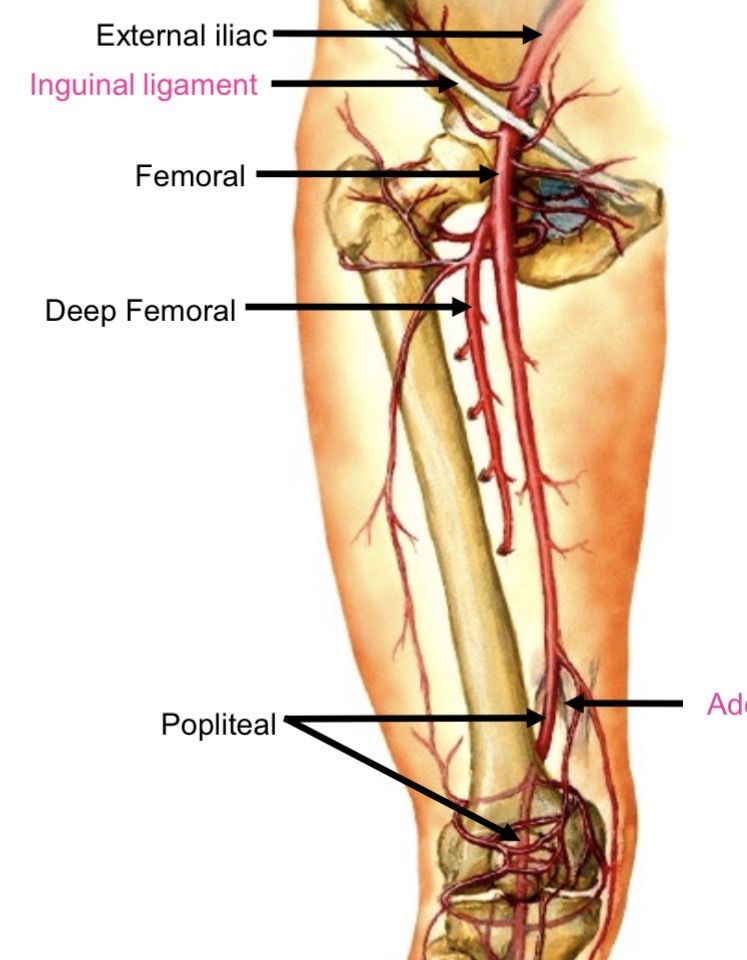
Femoral to popliteal transition
Passes through adductor hiatus to posterior knee
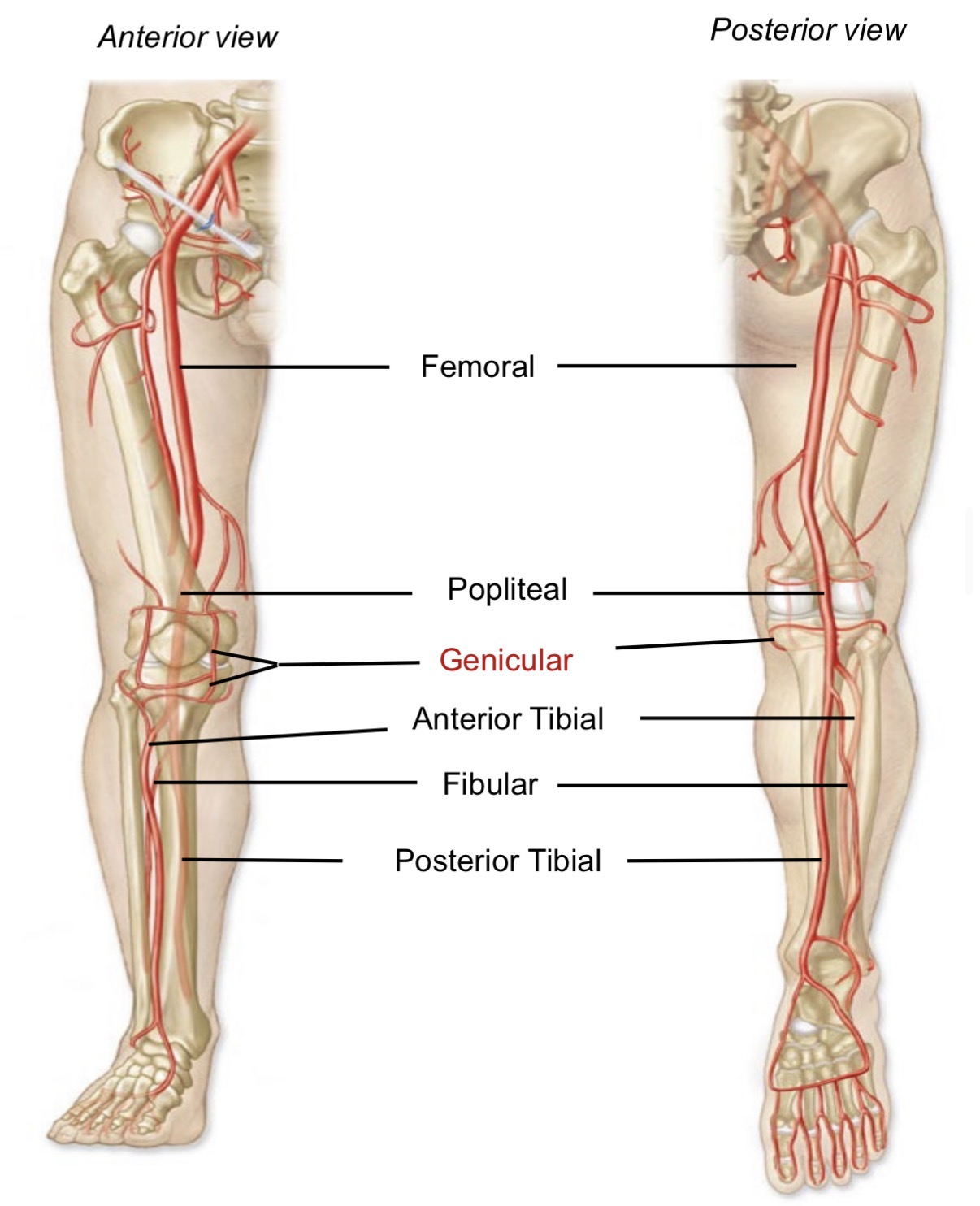
Collateral circulation at knee
Genicular arteries connect femoral and tibial arteries
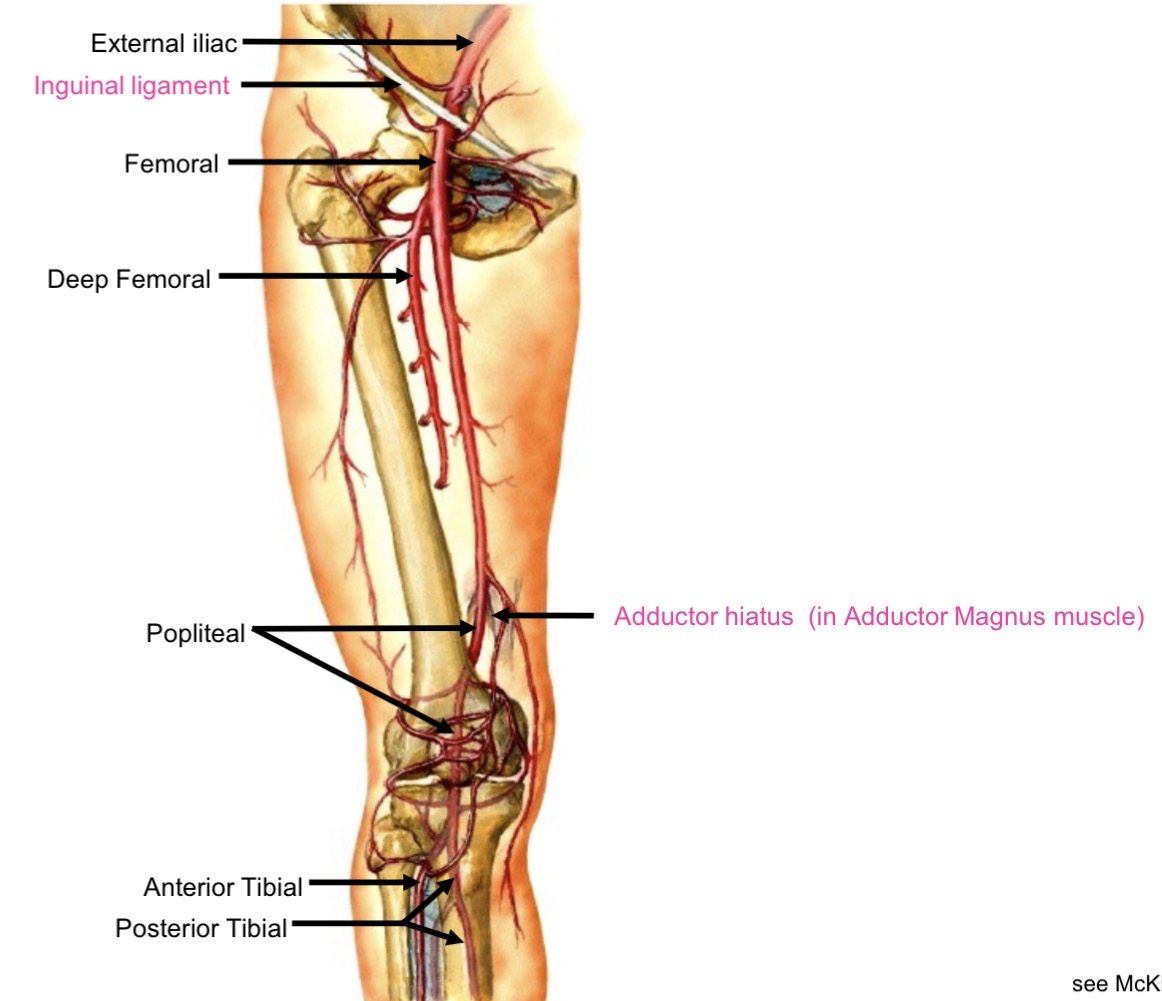
Popliteal artery branches
Anterior tibial
Posterior tibial
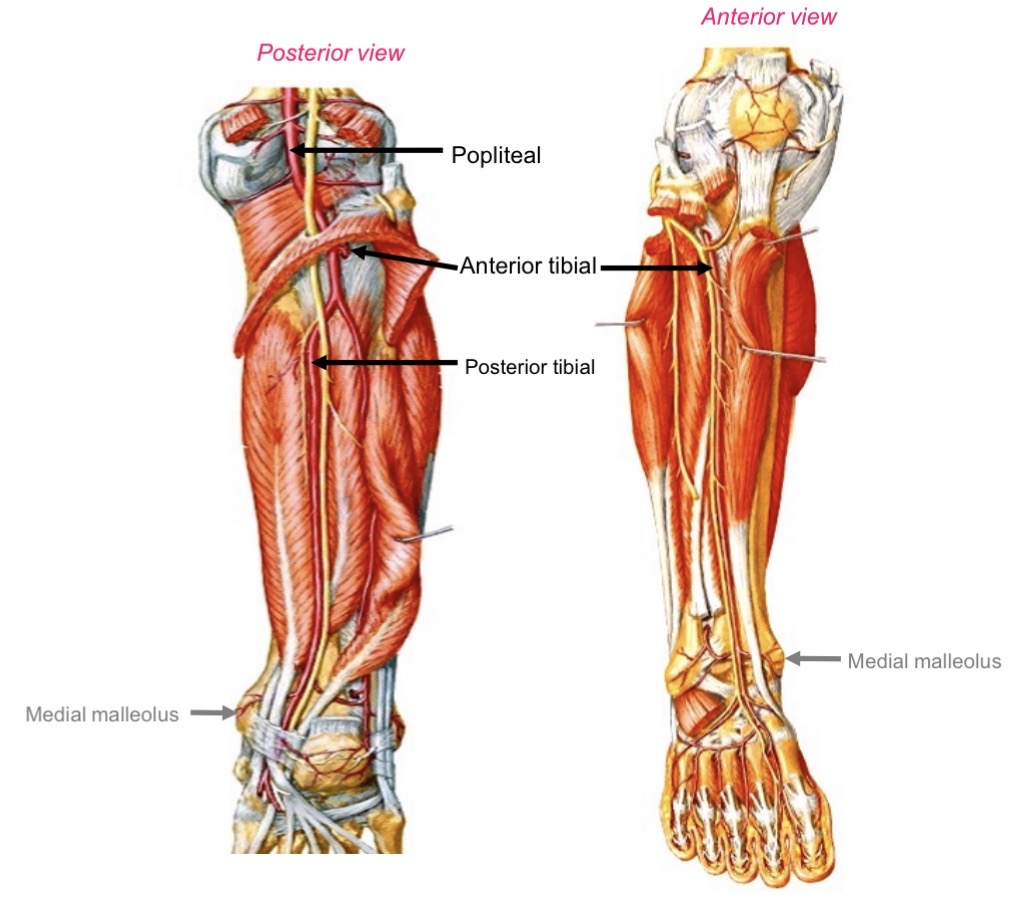
Posterior tibial artery supply
Posterior compartment (flexor muscles of foot)
Gastrocnemius
Soleus
Plantaris
Tibialis posterior
Flexor digitorum longus
Flexor hallucis longus