L48 - Cardiac Output: Mechanical events and Stroke volume
1/27
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
28 Terms
What does systole mean?
Ventricular contraction, so blood is ejected
What does diastole mean?
Ventricular relaxation and blood filling
What does isovolumetric mean?
It means the volume stays the same.
During isovolumetric ventricular contraction, what is happening?
The phase of systole where the ventricles contract but all valves are closed, so the volume of blood in the ventricles remains constant.
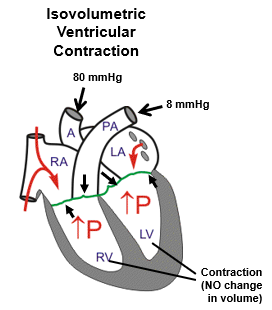
During ventricular ejection, what is happening?
The AV valves are closed
The aortic and pulmonary semilunar valves are open
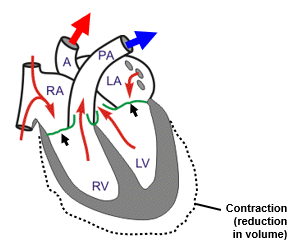
During isovolumetric ventricular relaxation, what is happening?
AV valves closed
Aortic and pulmonary valves closed
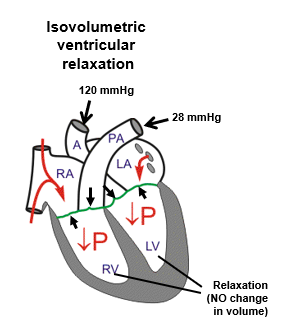
During ventricular blood filling, what is happening?
AV valves are open
Aortic and pulmonary valves are closed
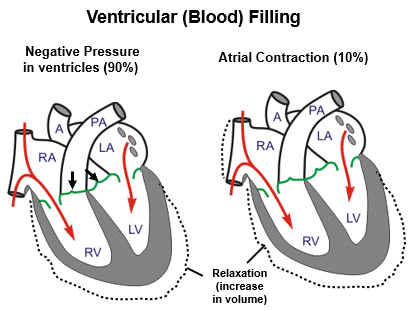
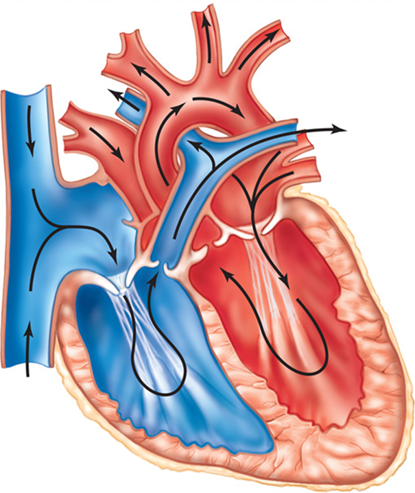
What causes heart sounds?
The closure of heart valves
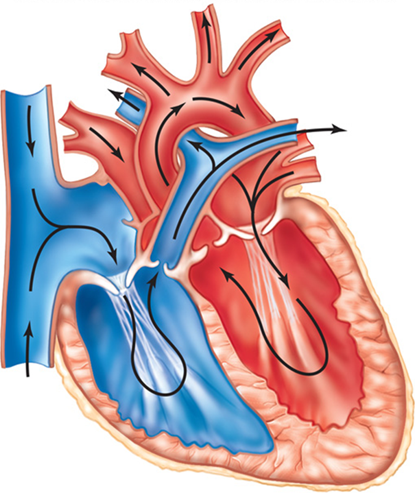
What causes the heart sounds “lub dub” when you listen through a stethoscope?
“lub” = Closure of the AV valves, onset of systole
“dub” = Closure of the pulmonary and aortic SL valves, onset of diastole
What regulates stroke volume?
Stroke volume is regulated by preload, afterload, and contractility.
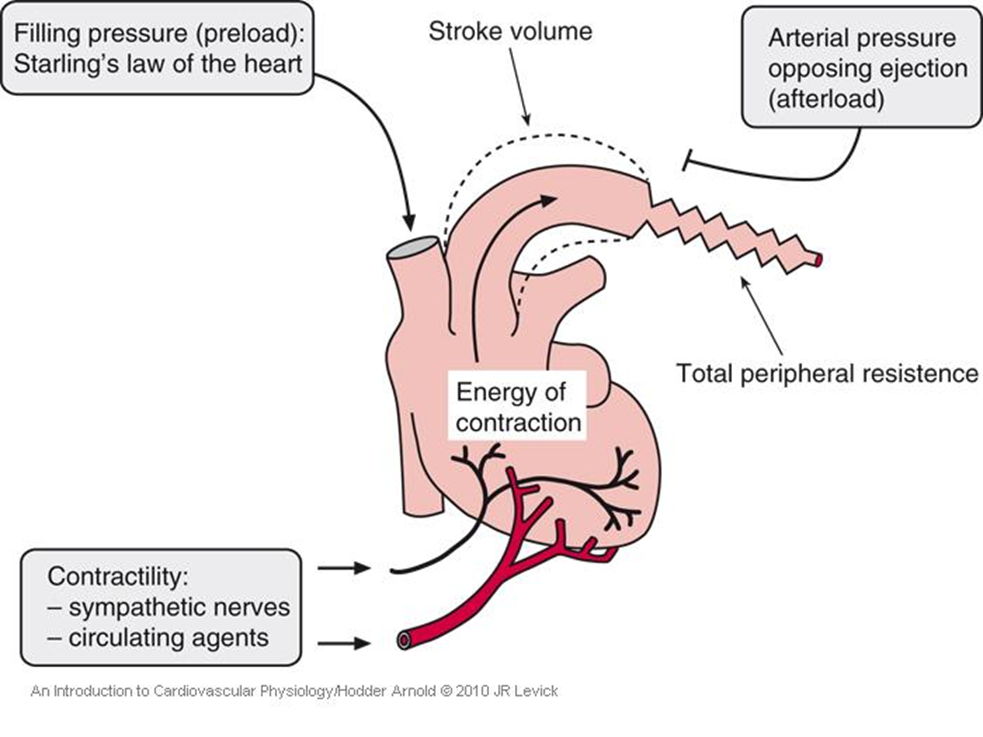
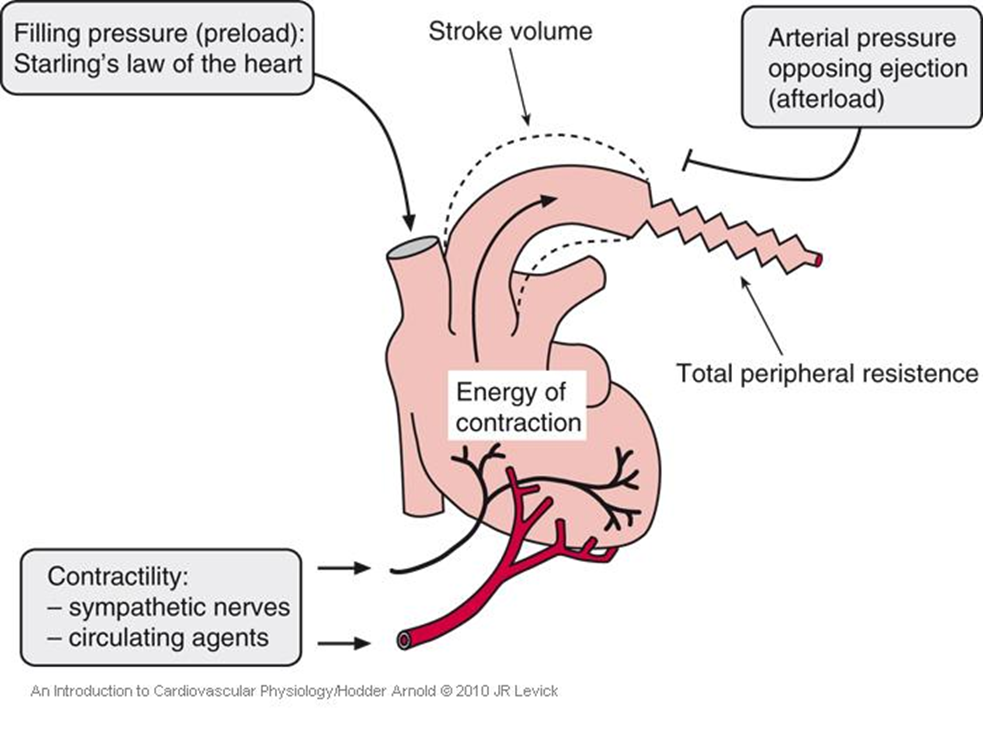
What is preload?
Preload is the amount of blood returning to the heart (venous return).
Increased preload stretches ventricular muscle fibres.
Greater stretch leads to stronger contraction, which results in a larger stroke volume.
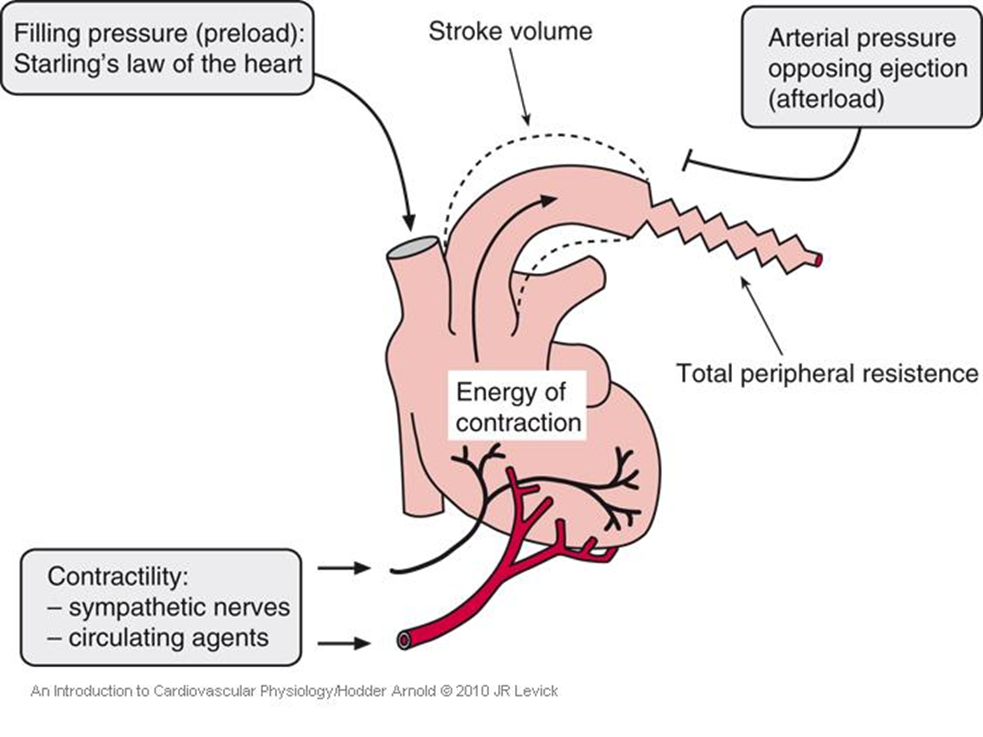
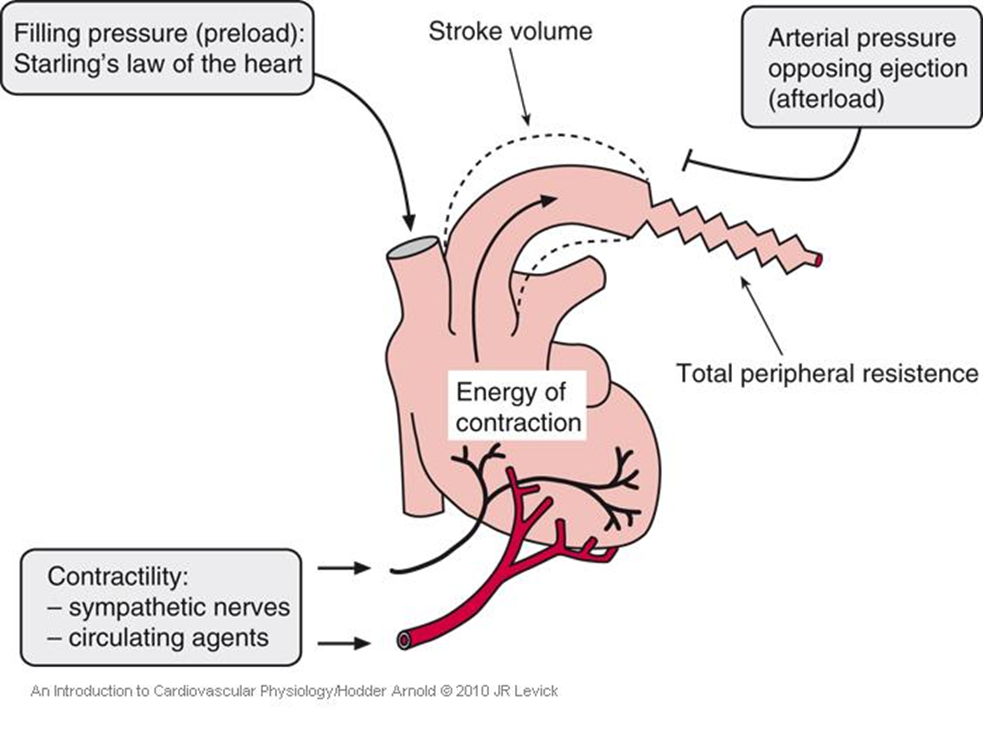
What is afterload?
Afterload is the resistance the ventricle must overcome to pump blood, mainly determined by arterial pressure
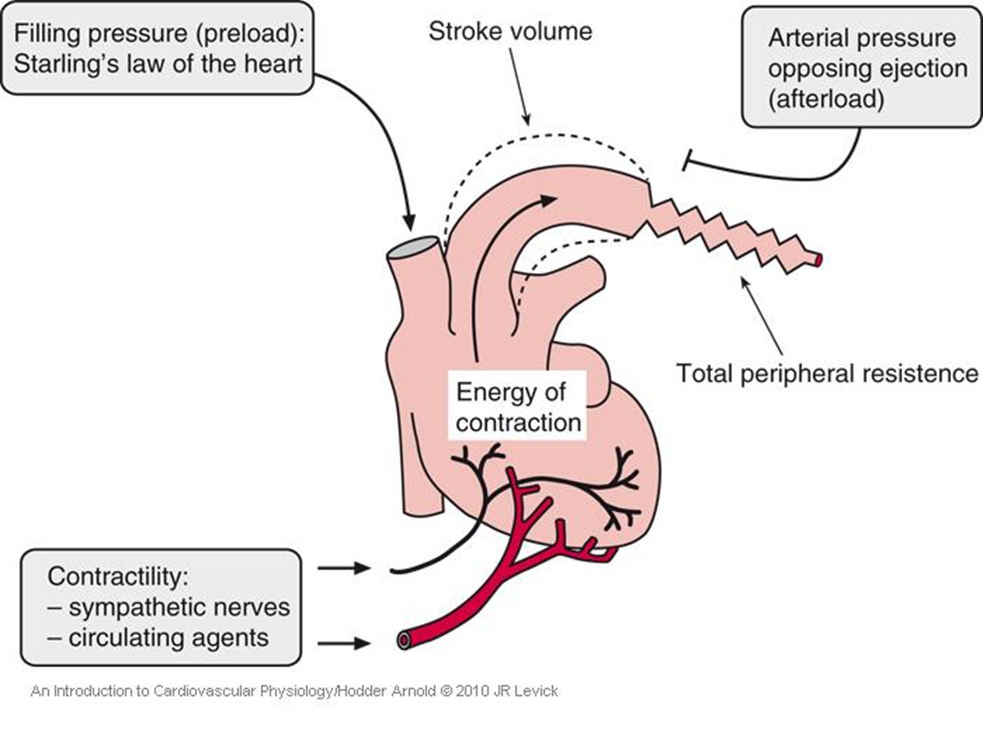
What is the effect of higher afterload?
Higher afterload makes it harder to eject blood, which decreases stroke volume.
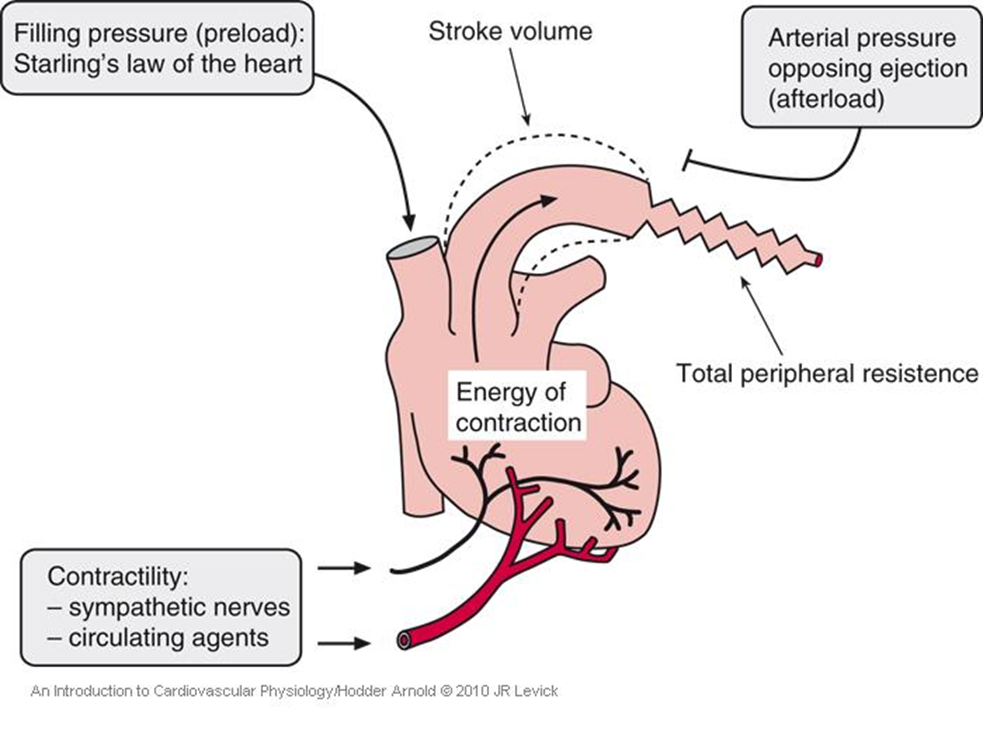
What is contractility?
Contractility is the intrinsic strength of the myocardium independent of preload, i.e. even if the amount of blood entering the heart (preload) stayed the same, the heart can still contract more strongly or weakly.
Higher contractility results in greater stroke volume.
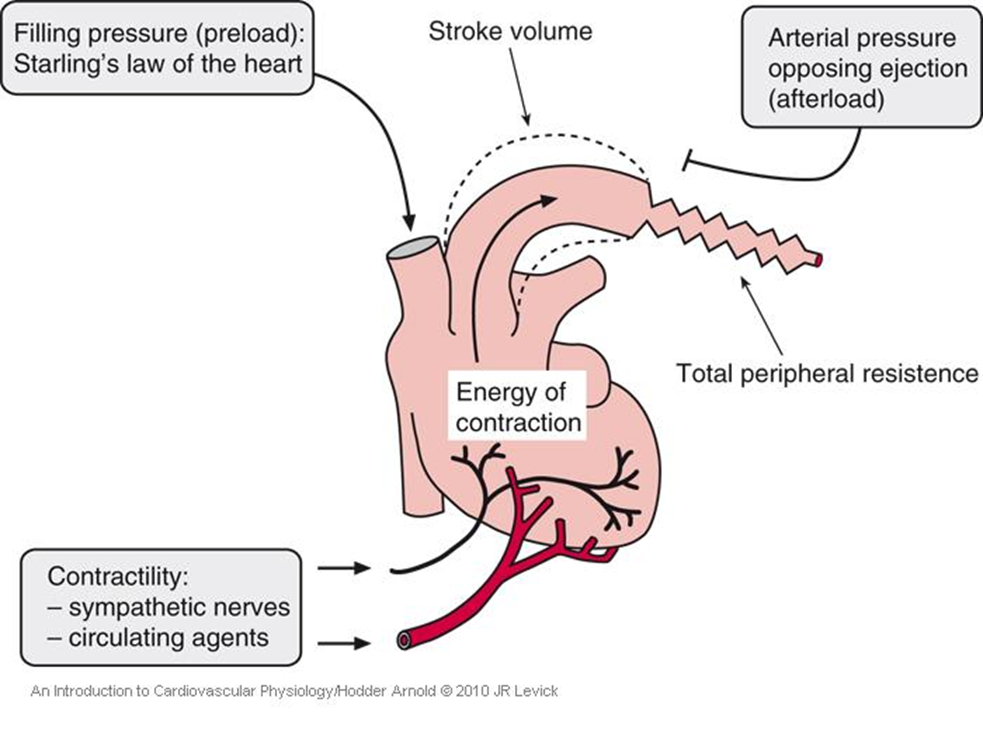
What increases contractility?
Contractility is increased by sympathetic stimulation, adrenaline, and increased intracellular Ca²⁺.
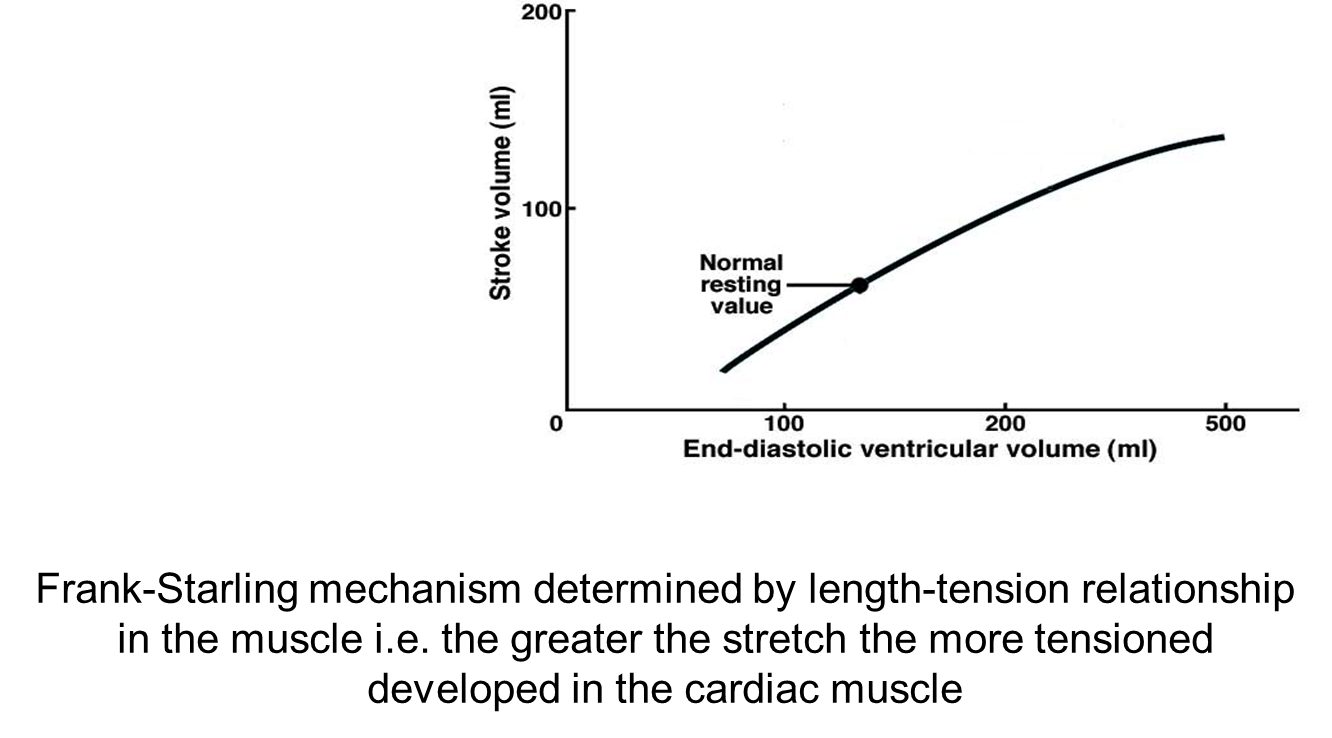
What is the Frank-Starling mechanism?
The Frank–Starling mechanism states that when more blood returns to the heart (higher venous return), the ventricles fill more, and so the muscle fibres are stretched more. This extra stretch makes the heart contract more strongly, so it pumps out more blood (higher stroke volume).
Ventricles contract with more force (higher stroke volume) if it contains more blood
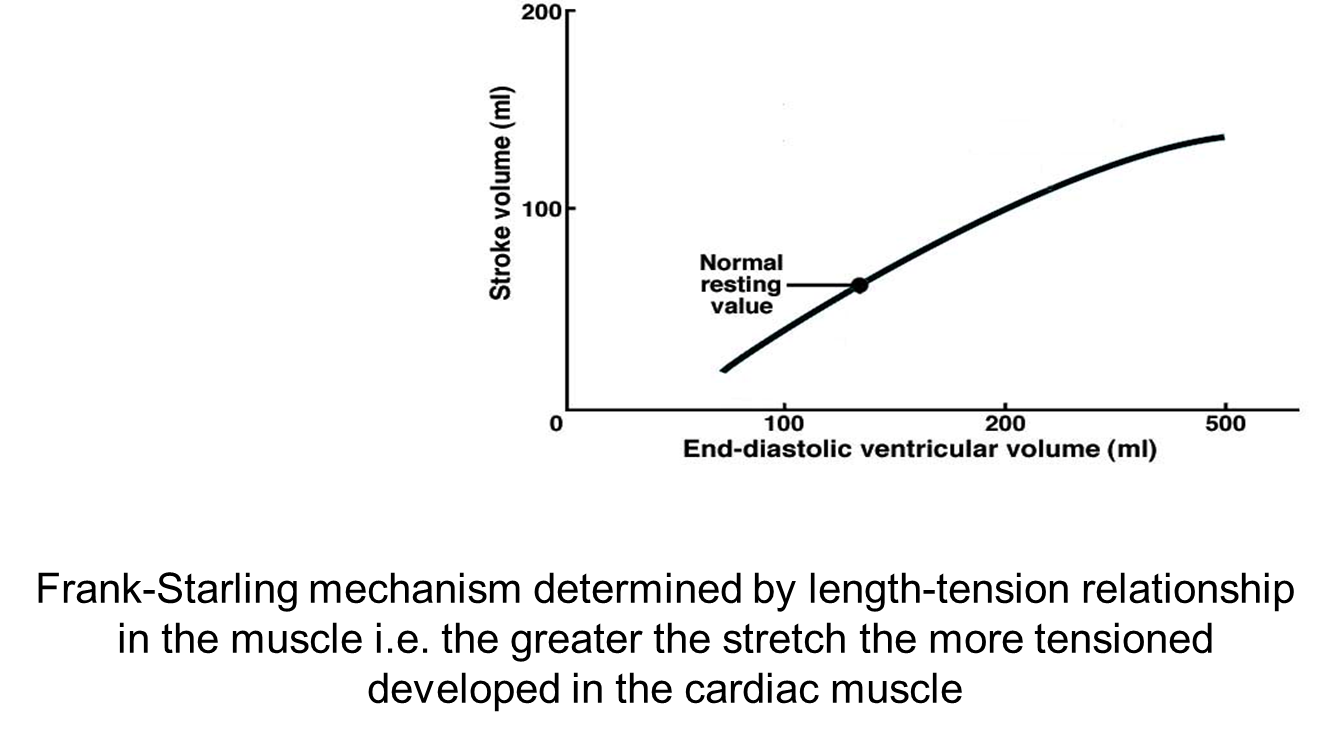
What determines the Frank-Starling mechanism?
The length-tension relationship in the muscle i.e. the greater the stretch, the more tension is developed in the cardiac muscle
What is the role of the Frank–Starling mechanism in balancing the output of the right and left sides of the heart?
The Frank–Starling mechanism ensures that increased venous return to either ventricle stretches the cardiac muscle and produces a stronger contraction, so each side of the heart pumps out the extra blood it receives and prevents blood from accumulating in the lungs.
Which one controls stroke volume, sympathetic or parasympathetic?
Sympathetic
The sympathetic ganglia increases heartbeat, and also regulates force/stroke volume
The Vagus nerve (parasympathetic) reduces heartbeat
What effect does sympathetic stimulation (noradrenaline acting on β₁‑adrenergic receptors) have on the heart?
It increases the force and speed of cardiac muscle contraction by raising contractility, meaning the ventricle contracts more strongly even at the same ventricular volume.
How does hypertension contribute to heart failure?
Hypertension increases the resistance the heart must pump against, making it harder to open the aortic valve and eject blood, which over time weakens the heart and can lead to heart failure.
Cardiac output is controlled by 2 main things:
Heart rate
Set by SAN
Increased by sympathetic nerves and adrenaline
Decreased by parasympathetic activity
Stroke volume
Preload
Afterload
Contractility
What is Congestive Heart Failure (CHF) characterized by?
Reduced cardiac output
Tiredness and shortness of breath
How does change in cardiac output regulation result in heart failure due to coronary artery disease?
Cardiac output is regulated by heart rate and stroke volume, which depend on preload, afterload, and contractility. In heart failure caused by coronary artery disease, reduced blood supply weakens the myocardium and lowers contractility, leading to reduced stroke volume and reduced cardiac output.
What are the main causes of chronic left ventricular failure?
The most common causes are coronary artery disease leading to ischaemic heart disease and myocardial infarction (causing systolic dysfunction), hypertension which increases afterload (causing diastolic dysfunction), cardiomyopathies such as those from viral infection or heavy alcohol use, and age‑related weakening of the myocardium.
What causes systolic dysfunction in heart failure?
A myocardial infarction damages the ventricular muscle, reducing its contractility and lowering stroke volume because the ventricle cannot eject blood effectively
What does infarction mean?
Tissue death caused by a loss of blood supply
What causes diastolic dysfunction in heart failure?
Chronic hypertension increases afterload
This leads to ventricular hypertrophy and stiffening of the ventricular wall
The stiff ventricle cannot relax or fill properly, reducing end-diastolic volume, and lowering stroke volume