mammography
1/9
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
10 Terms
what is the x-ray spectrum
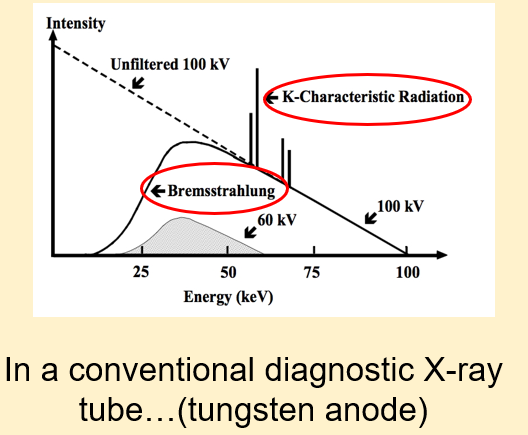
what is the aim of mammography units
•AIM of mammography units is to image soft tissue only!
•Very small differences in physical density that are the source of contrast for imaging;
•Significant sign of some breast Ca are very small ‘micro-calcifications’, beyond capability of most methods
•Design of equipment must allow for this functionality
•µ value of soft tissue is very low: need photons of very low energy to image
what are the challenges of mammography units
•Mammography units operate in the low kV range of 20-45
•Thermionic electrons do not have enough energy to cross to anode
•This produces a beam of low quality: low intensity
•Problem: longer exposure times = movement unsharpness
•Breast tissue has very little subject contrast
what are the solutions
•Shorter distance between cathode and anode
•Short SID- 45-60cm
•Focal spot (smaller): 0.3mm for general mammos and 0.1mm for magnification views = reduces geometric unsharpness
•Need AEC control due to varying breast composition/size
•High-voltage generator must supply near DC high voltage with a ripple less than 5%
•High tube current reduces exposure time required and risk of movement unsharpness
•High tube current: increased heat, therefore use rotating anode
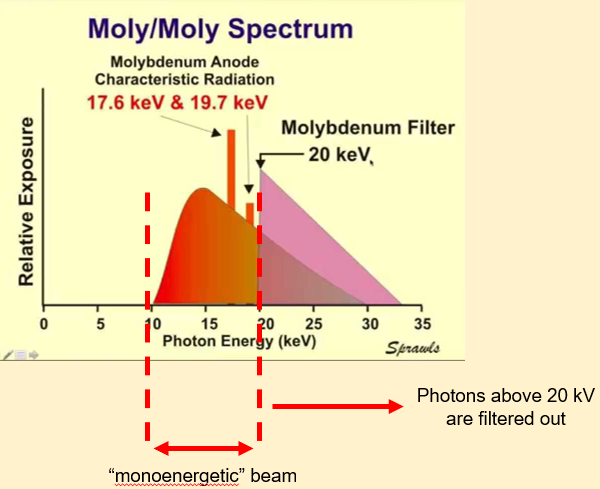
what’s the anode and filtration of mammography units
Molybdenum:
•High melting point and low atomic number (Z = 42)
•Used as X-ray tube anode and filter
•Anode: produces characteristic X-ray peaks at 17.6 kV and 19.7 kV
•Filter: attenuation k-edge at 20 kV
•X-ray spectrum:
•relatively narrow range of energies near 20 kV
•Optimum with respect to image contrast and radiation dose…especially for smaller breasts
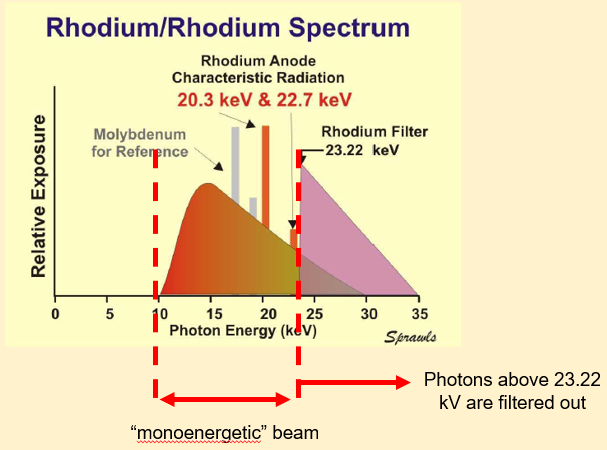
what is rhodium
Rhodium:
•Moly-moly spectrum not optimum for all
•High melting point and higher atomic number (Z=45) than molybdenum
•Shifts both the characteristic radiation and k-edge energies up to higher values
•Optimum for larger/denser breasts
why is compression needed
•Variation in thickness from the chest wall to the nipple creates a wide range of exposures to the receptor;
•Adequate visualisation of micro-calcifications requires total blurring to be limited to approximately 0.15mm;
•Exposure times can be several seconds (very long compared to most other radiographic procedures);
•Almost any patient motion during the exposure can be detrimental to image quality;
•Physical compression and stabilisation of the breast was developed to improve image quality both with respect to contrast and reduced blurring.
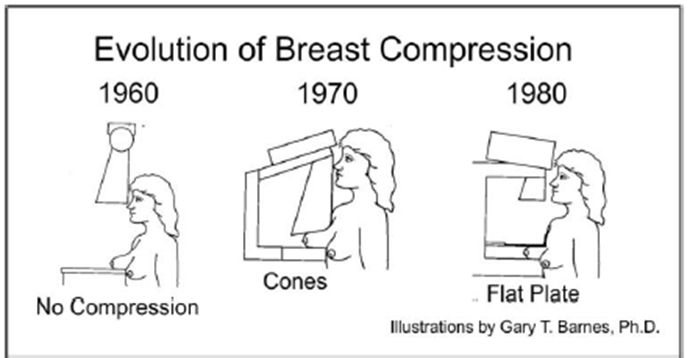
whats the evolution of breast compression
•1960s: conventional X-ray tubes with tungsten anodes
•1970s: specific mammography X-ray systems were developed, some type of compression and breast stabilisation was included by the X-ray beam cone and sometimes with soft components in contact with the breast
•1980: the introduction of continuing flat plate development was a major contribution to image quality
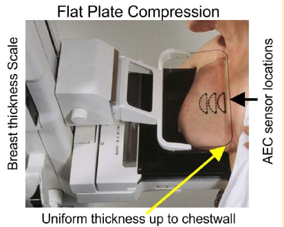
what is flat-plate compression
•Major contribution is reshaping of the breast into a more uniform thickness spread over a slightly larger area;
•Uniform thickness reduced range of X-ray exposure to the receptor and loss of contrast due to latitude limitations;
•Spreading of breast tissue, especially thicker regions, reduced overlapping of objects & structures that could interfere with visualisation;
•Especially significant for imaging tissues up to the chest wall.
•Display and measurement of thickness: exposure factor selection
•AEC sensor location: selection desired density
summary
•Mammography units have modifications of the tube to meet the goal of X-ray imaging of soft tissue.
•This is primarily through changes to the anode material and the use of filtration to create a ‘mono-energetic beam’.
•Compression plays an important role in obtaining high-quality images