SLO5 (Ch11,12,13)
1/75
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
76 Terms
What are abcteria, fungi, protozo, and viruses classified as (not all are pathogenic)
microbes
gram-positive bacteria

gram-negative bacteria

_______ are “social creatures” Interact with one another,Live together in complex microbial communities,Contain different species of microbes that are spatially organized within community
bacteira
whats the typical timeline for biofilm formation
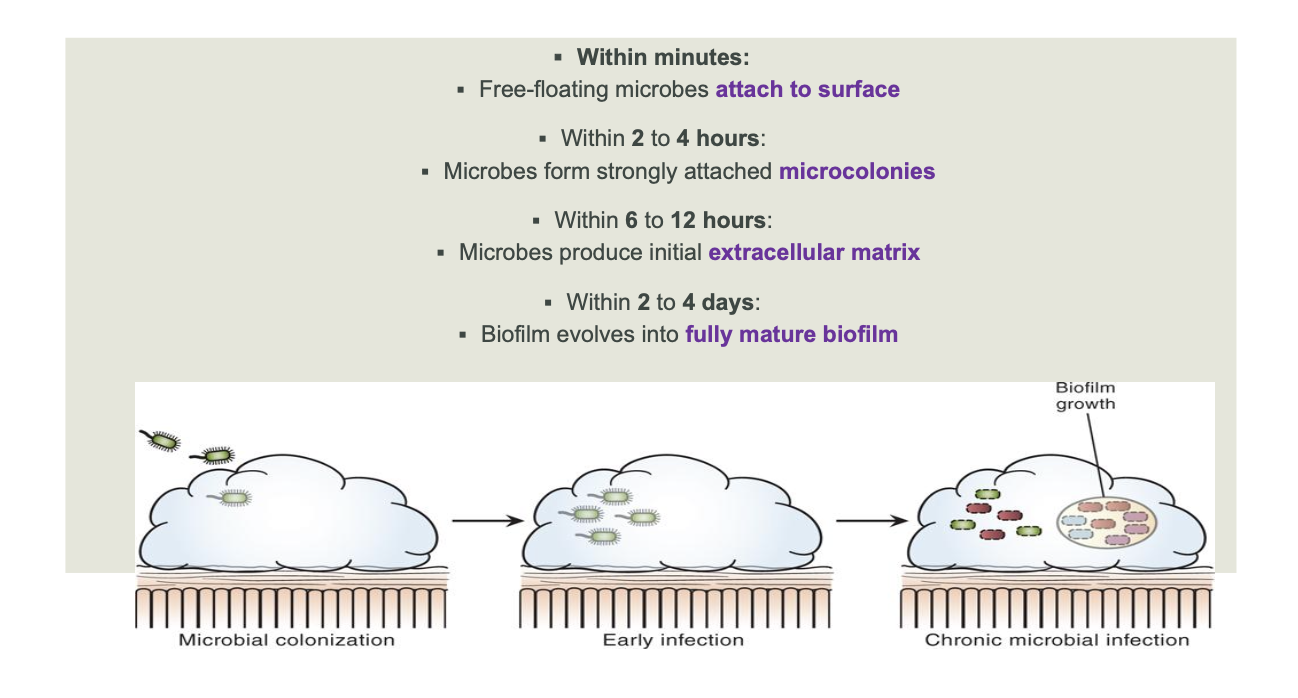
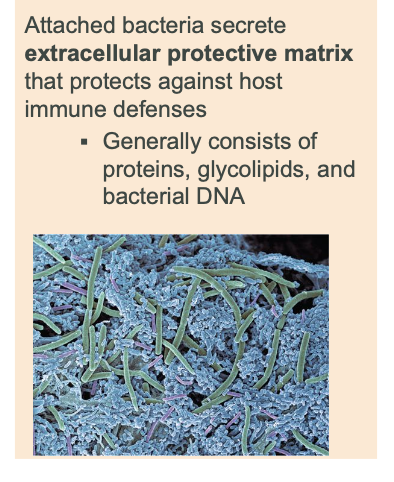
how to mature biofilms protect bacteria?

_________ are Polymicrobial, three-dimensional community embedded in protective matrix that consists of microbial metabolic products and/or host components
Oral biofilms
Resident microbes of the oral cavity;__________ are part of normal flora in mouth
▪ Prevent colonization by opportunistic pathogenic bacteria
▪ Comprise biofilm found on all epithelial-lined surfaces
commensal bacteria
Residnent microbes of the oral cavity have _________ with host
▪ Contribute to host nutrition, maintain robust immune
system, and provide cover over mucous membranes
▪ Host provides nutrients, stable environment for survival
symbiotic relationship
explain early dysbiosis

explain established dysbiosis

Biofilm bacteria can be transmissible via direct or indirect. Most common route is ______ transmission (Via sharing saliva between caregiver and child). Less common route is _______ transmission( Via individuals of same generation kissing)
vertical, horizontal
Periodontal pathogens transmissible, but periodontal disease not an ____________.
infectious disease
examples of gram + bacteria capable of clonizing the mouth

examples of gram - bacteria capable of clonizing the mouth

Stages of Biofilm Formation: Stage 1
attachment of microbes

Stages of Biofilm Formation: Stage 2
permanent attachment

Stages of Biofilm Formation: Stage 3 (Maturation Phase I)
self protective matrix formation
Stages of Biofilm Formation: Stage 4 (Maturation Phase II)
mushroom-shaped colonies

Stages of Biofilm Formation: Stage 5
escape from the matrix

whats the sequence of bacterial colonization

nonspecific plaque biofilm hypothesis (historial perspective)

specific plaque/microbial shift hypothesis (historical perspective)
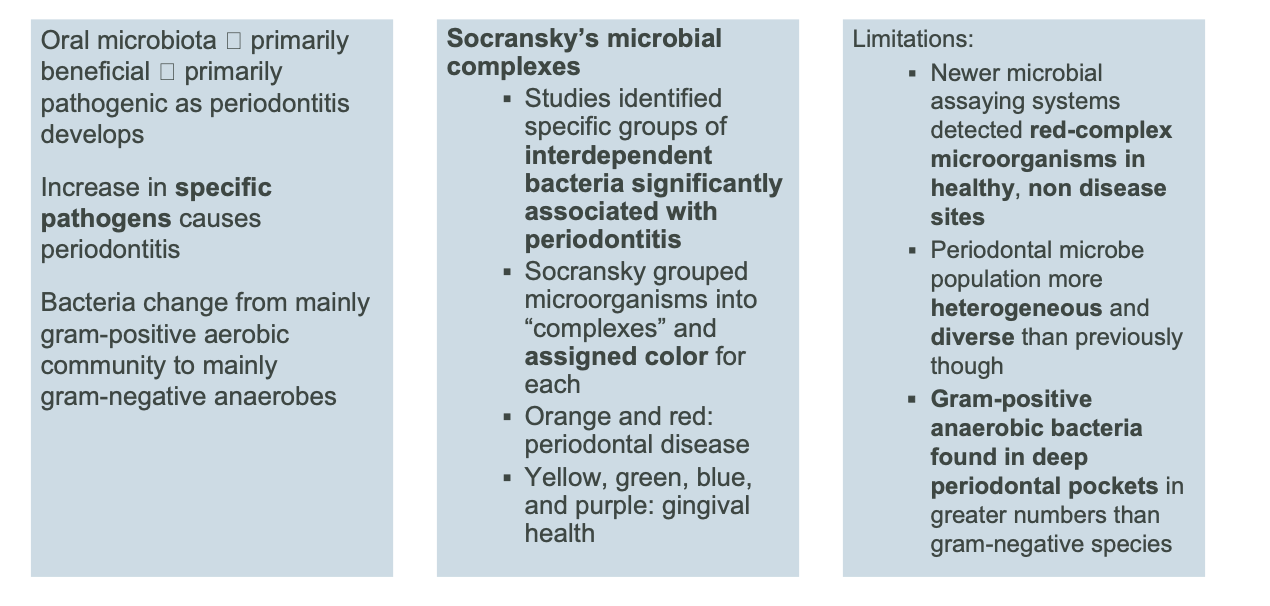
ecological plaque hypothesis (current perspective)
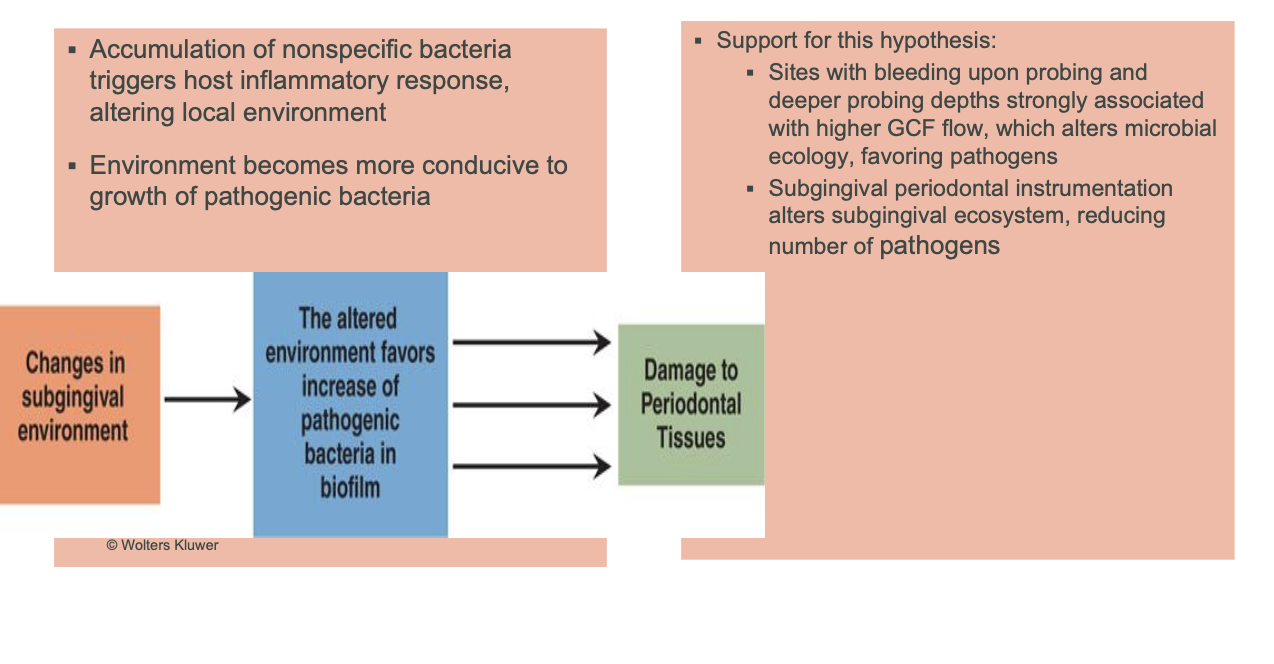
microbial homeostasis-host repsonse hypothesis (current perspective)

keystone pathogen-host response hypothesis (current perspective)
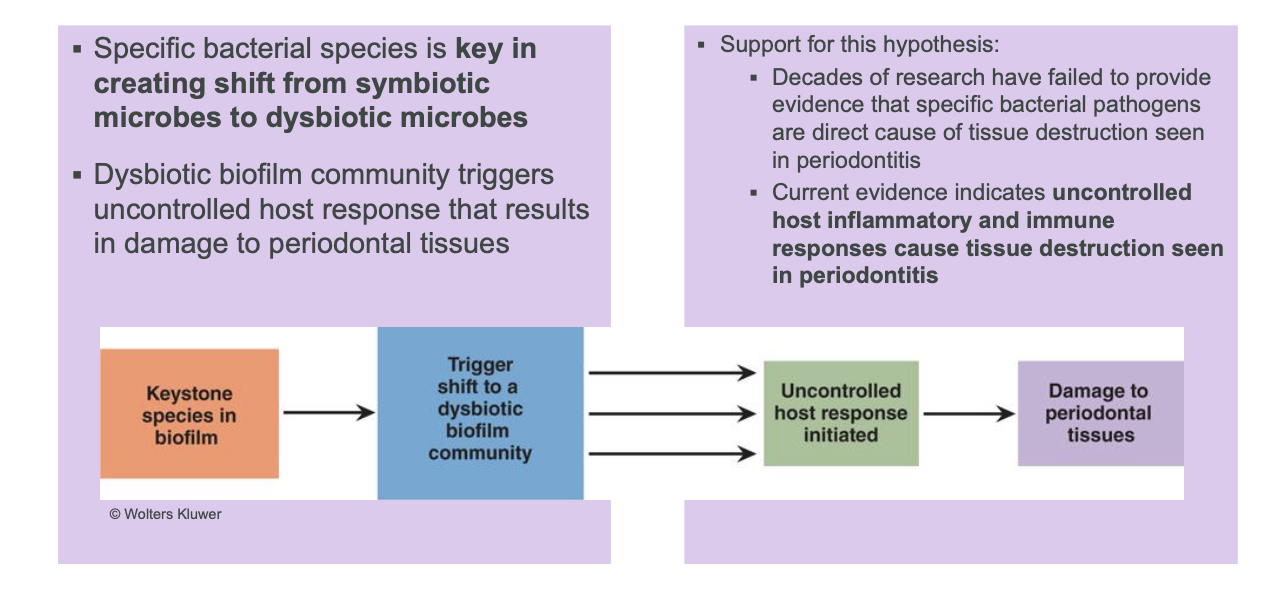
The ________ is Network of different types of leukocytes & proteins that work together to defend the host, Necessary for survival
immune system
adaptive vs innate immunity
innate (immediate response), adaptive has a lag time (delay)

what are the cells of adaptive immunity
t-lymphocytes, b-lymphocytes
_______ are Colorless, nucleated cells that originate from hemopoietic stem cells in bone marrow. Categorized according to presence or absence of cytoplasmic granules. Granulocytes and Agranulocytes.
Leukocytes
________ carry granules and include neutrophils, eosinophils, basophils, and mast cells. _________ are leukocytes lacking granules; includes lymphocytes and monocytes/macrophages.
Granulocytes, Agranulocytes
________ aka polymorphonuclear leukocytes (PMNs) phagocytose invading pathogens. They can pass through capillary walls through chemotaxis. Their cytoplasm contains bactericial digestuve enzymes. They are short lived because they die during phagocytosis.
Neutrophils
_________ are large phagocytes with a single irregular shaped nucleus. They are 2 to 3 times larger than red blood cells. They lack cytoplasmic granules, so they are classified as agranulocytes.
Monocytes
__________ are the largest leukocytes and are highly phagocytic. They are classified as agranulocytes. They are slower to arrive at infection site than neutrophils. They primarily function as antigen-presenting cells.
macrophages
Lymphocytes are small monoclear agranulocytes that play important role in recognizing and neutralizing foreign invaders. There are 3 types: ________, ________, _________.
B-lymphocytes (B-cells), T-lymphocytes (T-cells), NK (natural killer) lymphocytes
________ are smaller than neutrophils and monocytes/macrophages. They originiate from hematopoietic cells in bone marrow. They consist of two subclasses; plasma B-cells that produce antibodies (immunoglobulins) and memory B-cells that “remember” previous exposures and evoke more rapid and more enhanced response.
B-lymphocytes
_____ is the most abundant antibody, responds to invading pathogens, potent activator of the complement system, and the only immunoglobulin that can pass thru the placental barrier.
IgG
_____ is the largest antibody, first to respond to initial exposure to antigen in blood and lymph fluid, has pentamer structure, and a potent activator of the complement system.
IgM
____ is the principal defense at mucosal barriers, most prevalent from is secretory dimeric ___ (sigA), passes to neonate throguh breast milk, and is a poor activator of the complement system.
IgA
____ is a type of antibody and is the most powerful mediator of host allergic response. _____ is a type of antibody that is the least abundant and least understood.
IgE, IgD
_______ eliminate offending agents by coatinf the target to make it more readily phagocytosed and activate the complement system. IN certain individuals it can trigger the hypersensitivity immune reaction to substance that is typically ahrless or would not trigger immune response (allergic response).
Antibodies
T-lymphocytes are a type of agranulocyte that plays role in adaptive
immune response to pathogens. It consists of 4 subsets:
▪ T-helper (TH)-lymphocytes
▪ T-cytotoxic (TC)-lymphocytes
▪ T-memory (TM)-lymphocytes
▪ NKT (Natural Killer T)-lymphocytes
__________ plays a “helper” role by regulating the differentiation and maturation of B cells and activation of cytotoxic T cells and macrophages, they dont directly neutralize or clear pathogens.
TH lympocytes (T-helper lymphocytes)
_________ upon activation this cell directly attacks viral infected cells or tumor cells by releasing perforin which ounches holes through the plasma membrane of the target cell, thereby having direct cytotoxic effect. Indirectly, it produces antiviral and antitumor cytokines such as TNF-a and IFN-y.
TC-lymphocyte (T-cytotoxic)
__________ are memory t-lymphocytes, they remember past exposure so that upon re-exposure the immune response is faster and stronger than initial response.
TM-lymphocyte
__________ following activation, these T-lymphocytes immediately commence with cytokine secretion, the rapidity of their response makes these lympocytes impiortant players in the very first lines of defense against some types of bacterial and viral infections.
NKT-lymphocytes
_________ are large granular lymphocytes that are larger than B and T lymphocytes. They have attributes of innate and adpative immunity. They are preprogrammed to be “_____” of virus -infected cells and tumor cells. They are a separate, distinct category of lymphocyte and dont require preactivation unlike ________.
NK (nautral killer) lymphocytes, NKT lymphocytes
________ is composed of inactive nonucleated proteins that patrol the body for potential invaders and, upon exposure, either directly or indirectly neutralize them. Works with antiodies and phagocytes to neutralize invading pathogens.
The complement system
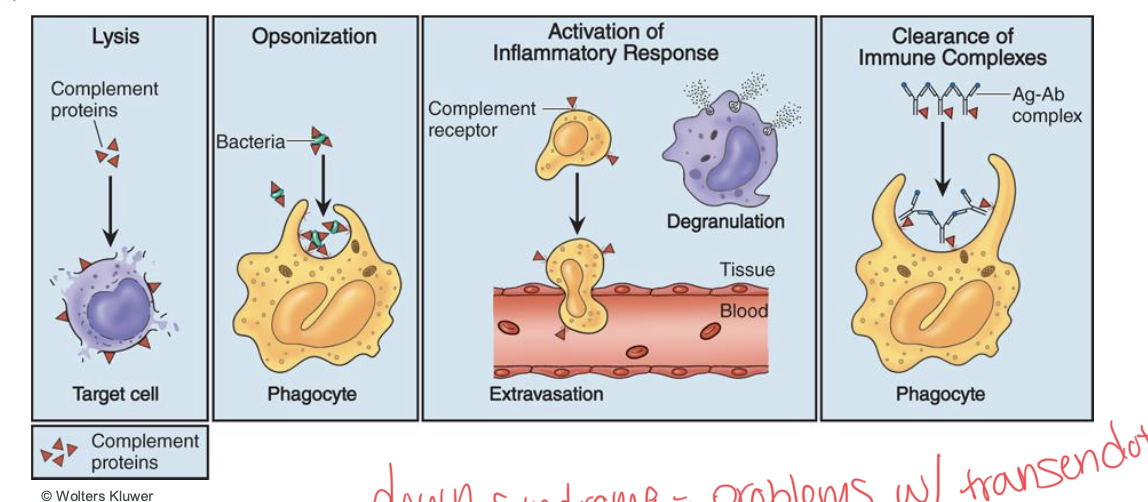
The process of the complement system:
______ forms pores in the target cells membrane with complement proteins that form a unit called the membrane attack complex.
_______, facilitates the engulfment aand destruction of microorganisms by phagocytes (most important of the complement system), the complement proteins bind and coat the surface of the pathogen which “marks” it for eventual engulfment.
_________ the system recruits additional phagocytes to the site of the infection, the proteins act as a potent chemoattractant that draw in more leukocytes to migrate to the infection site.
_________ the systme performs a house keeping function by remove the immune complexes from circulation.
destruction of pathogens, opsonization, recruitment (activation of inflammatory response), and immune clearance
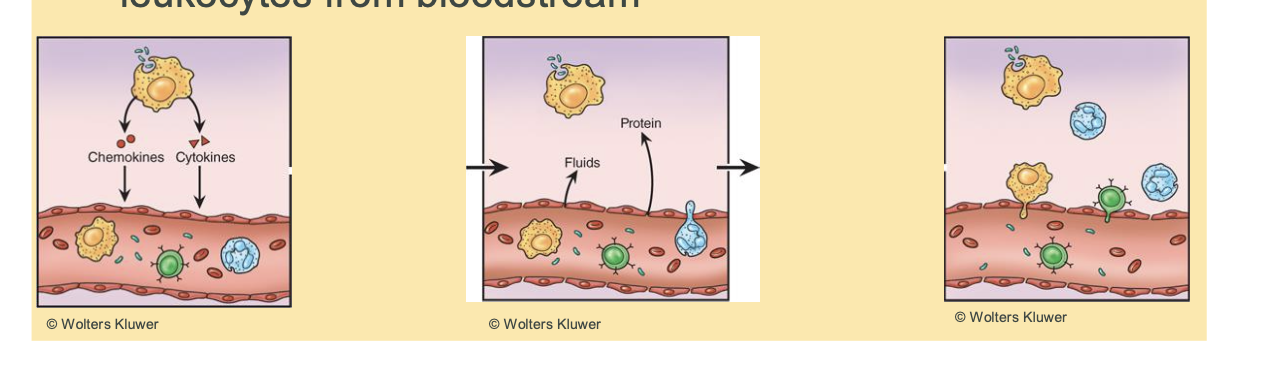
________ is when tissue residnet leukocytes release cytokines and
chemokines into connective tissue to recruit more
leukocytes from bloodstream.
chemotaxis
_________ is the process whereby leukocytes migrate toward infection
site in response to bioactive compounds released by leukocytes (like a following a bread crumb trail). This causes neutrophils to swarm and neutralize invading pathogens.
Chemotaxis
The __________ is initiated by blood vessels near injured tissue, Neutrophils arrive first, phagocytose, and kill invaders, Short-lived; primarily involved in early inflammation If pathogens eliminated, inflammation ends
Resolution process:
▪ “Stop signals” shut down and clear immune cells
Classic symptoms:
-heat, redness, swelling, pain, and loss of function
acute inflammation
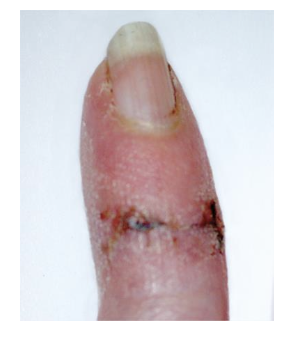
________ can occur if acute inflammatory response is not effetive in eliminating invading microorganisms. It is a prolonged and out of control inflmmaotry response that continues for more than a few weeks and results in varying degrees if tissue damage.
chronic inflammation
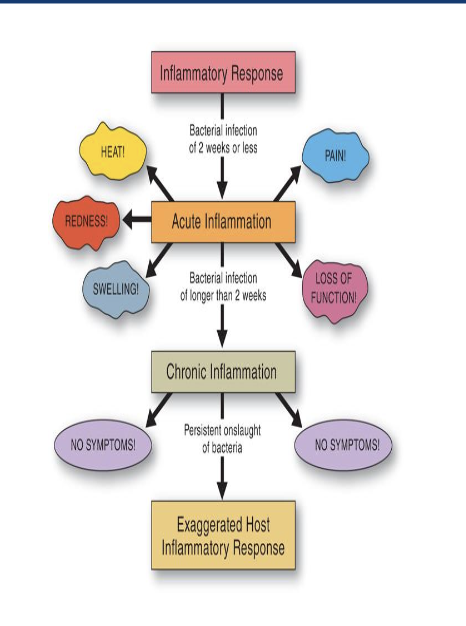
_________ characterized by unresolved, chronic
inflammation that leads to ongoing tissue damage
through continuous, recurring episodes of acute
inflammation
Peridontitis
What are the factors modulating the host immunoinflammatory response?
genetic, environmental, and acquired
The host response for acute inflammation to microbes involves cells includes:
Inflammatory cells
PMNs
Antigen-presenting cells
T- and B- lymphocytes
Fibroblasts
Epithelial cells
Acute inflammation has host-protective effect
▪ ________ against microbial invasion
▪ ______ harmful stimuli
▪ _______ injurious host cells
▪ Creates environment ______ to tissue repair
And it must _______after microbial challenge eliminated
First line of defense, Eliminates, Replaces, favorable, dampen/decrease
_______ is the return to homeostasis after inflammation and is thought to be just as a complex biological process as the onset of inflmattion.
Catabasis
What are the proinflammation mediators present in periodontitis?
Prostaglandins, thromboxanes, prostacyclins, and leukotrienes
Periodontitis lipid mediators are associated with
▪ Recruitment of _____
Destruction of connective tissue matrix
▪ Resorption of alveolar bone
Over-recruitment or overactivity of _____ can amplify inflammatory process
PMNs
__________ worked in programmed systemic process to
▪ Terminate PMN recruitment to site
▪ Stimulate macrophages to remove dead cells
▪ Promote antibacterial activities
▪ Promote tissue repair & regeneration
pro-resolving lipid mediators
Inflammatory __________ in the host response are the “middlemen” sent by host cells to activate the inflammatory response. Important these include _____, ______, and ______.
biochemical mediators, cytokines, prostaglandins, and matrix metalloproteinases (MMPs)
_________ are powerful regulatory proteins released by host immune cells that influence the behavior of other cells. They transmit information/signals between cells, alert and activate immune system for help. Produced by PMNs, macrophages, B-cells, epithelial cells, gingival fibroblasts, and osteoblasts.
Cytokines
What are the key cytokines in periodontitis? (can initiate and perpetuate irreversible tissue destruction in chronic inflammatory diseases)
IL-1, IL-6, IL-8, and TNF-a
________ are powerful biochemical mediators derived from fatty acids expressed on the surface of most cells. What are the most important ones of these?
Prostaglandins (D, E, F, G, H, I)
_________ play an important role in the bone destruction in periodontitis. Macrophages are a major source of these, also produced by PMNs and gingival fibroblasts. Their function is to trigger osteoclasts to destroy bone, promote over production of destructive MMPs.
Prostaglandins of E series (PGEs)
________ are a family of at least 12 proteolytic enzymes that break dwon CT matric. They are produced by PMNs, macrophages, gingival fibroblasts, and JE cells. _______ balance helps maintain tissue integrity. Over production of these happens with intense inflammation by stimulation of cytokines and PGs and can cause extensive damage in peridontal tissues.
Matrix Metalloproteinases (MMPs)
Gingival health associated with symbiotic biofilm. In susceptible individuals, dysbiotic biofilm activates _______ to produce excessive cytokinesm ROSm and MMPS leading to collagen breakdown, bone resorption, and PD tissue damage.
dysbiotic biofilm
In the _______ the pt is clinically healthy and there is 2-4 days of biofilm accumulation. In the _______ the pt has inflammatory changes to edmea and erythema with 4-7 days of biofilm accumulation. In the _______ all features of gingivitis are present and its been 21 days after biofilm accumulation. In the ______ JE migration, pocket formation, BOP, PDL and bone destruction, furcation involvement, tooth mobility, is not reversible.
initial, early, established, and advanced
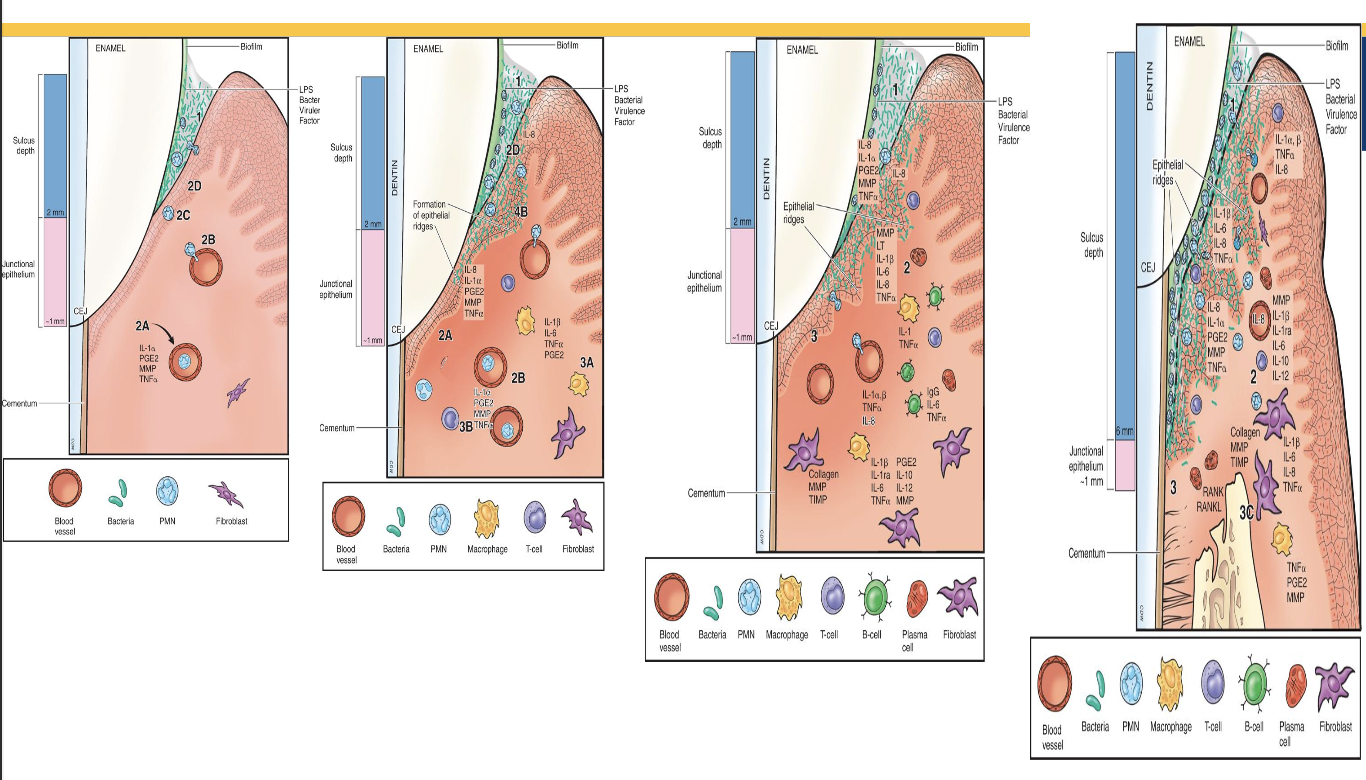
_______ are bone resorbing cells that are multinucleated and are activation mediated by cell-surface activator of nuclear factor kappa-B (RANK). _______ are special bone forming cells that synthesize collegen and other bone proteins, and is involved in mineralization of bone matrix.
Osteoclasts, osteoblasts
_______ is protein catalyst expressed on osteoblast membrane and is an osteoclastic differentiation factor. Resorption occurs when this binds to RANK which stimulates precursor cells to differentiate into osteoclasts.
Receptor activator of nuclear factor kappa-b (kB) ligand (RANKL)
_______ is protein signlaing molecule produced by osteobalsts, it protects bone from excessive resorption by binding to RANKL and blocking binding with RANK.
Osteoprotegerin (OPG)
Homeostatic condition occurs when body maintains stable level of alveolar bone and when _____ and _____ are in balance in peridontal tissues.
Bone resorption occurs when osteoblasts stimulated by RANKL to resorb alveolar bone. _____ decrease with periodontal inflammation, stimulating resorption
RANKL, OPG, OPG levels
Examples of molecules that stimulate resorption:
-RANKL
-Stimulatory cytokines: (IL-1β, TNF-α, IL-6, IL-11, IL-17) ▪ Prostaglandin E2 (PGE2)
-Prostaglandin E2 (PGE2)
Examples of molecules that inhibit resorption:
-OPG
-Inhibitory cytokines (IL-4, IL-10, IL-12, IL-13, IFN-γ)