(3.2b) L5+6(Antibodies+The Elisa Test
1/11
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
12 Terms
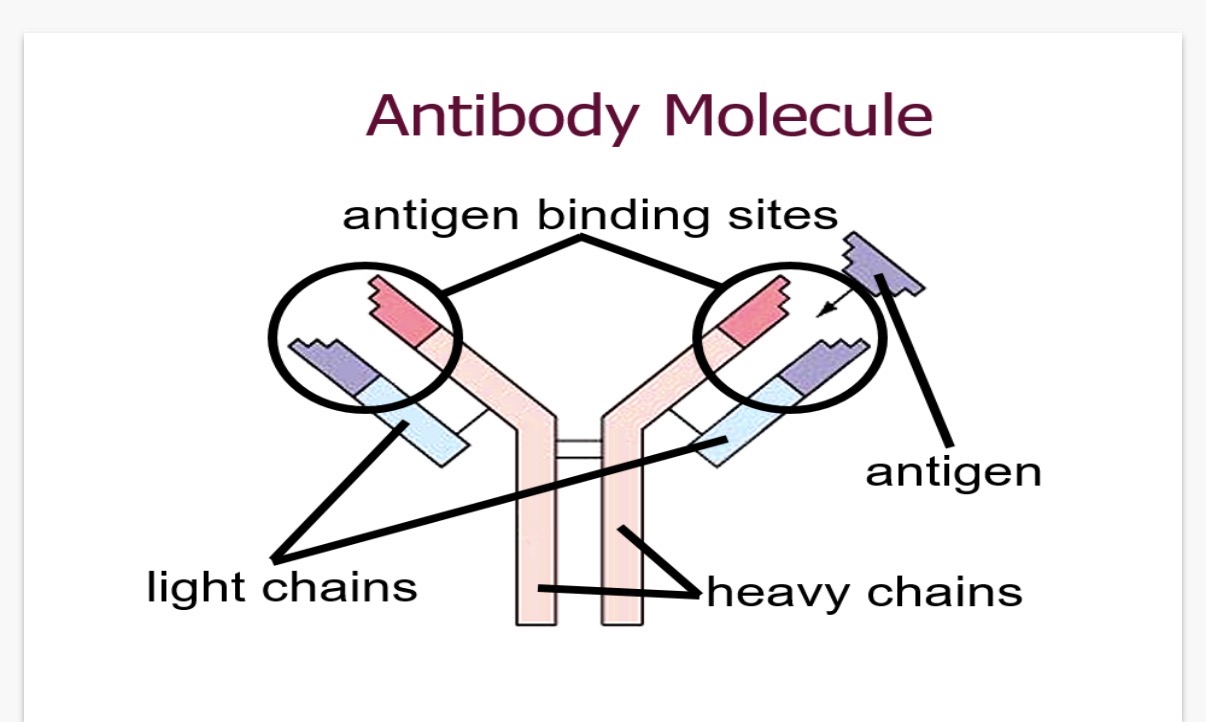
L5:Antibodies
How many polypeptide chains is an antibody made out of?
2. What are the chains called?
3. How is an antibody able to bind to a specific antigen?
4. What is the difference between the constant and variable region of an antibody?
Here's a breakdown of the antibody structure and the answers to your questions:
Drawing and labeling an antibody involves showing its key parts:
* Heavy chains: Two long polypeptide chains.
* Light chains: Two shorter polypeptide chains.
* Variable regions: Located at the tips, these regions bind to the antigen.
* Constant regions: These regions are the same for all antibodies of a given class.
* Antigen-binding sites: The specific areas where the antibody attaches to the antigen.
* Disulfide bonds: These bonds hold the polypeptide chains together.
Now, let's answer your questions:
1. An antibody is made out of four polypeptide chains.
2. The chains are called heavy chains and light chains.
3. An antibody is able to bind to a specific antigen because of the unique shape of its variable regions, which fit the antigen like a lock and key.
4. The constant region is the same for all antibodies of a given class, while the variable region is unique and responsible for antigen binding.
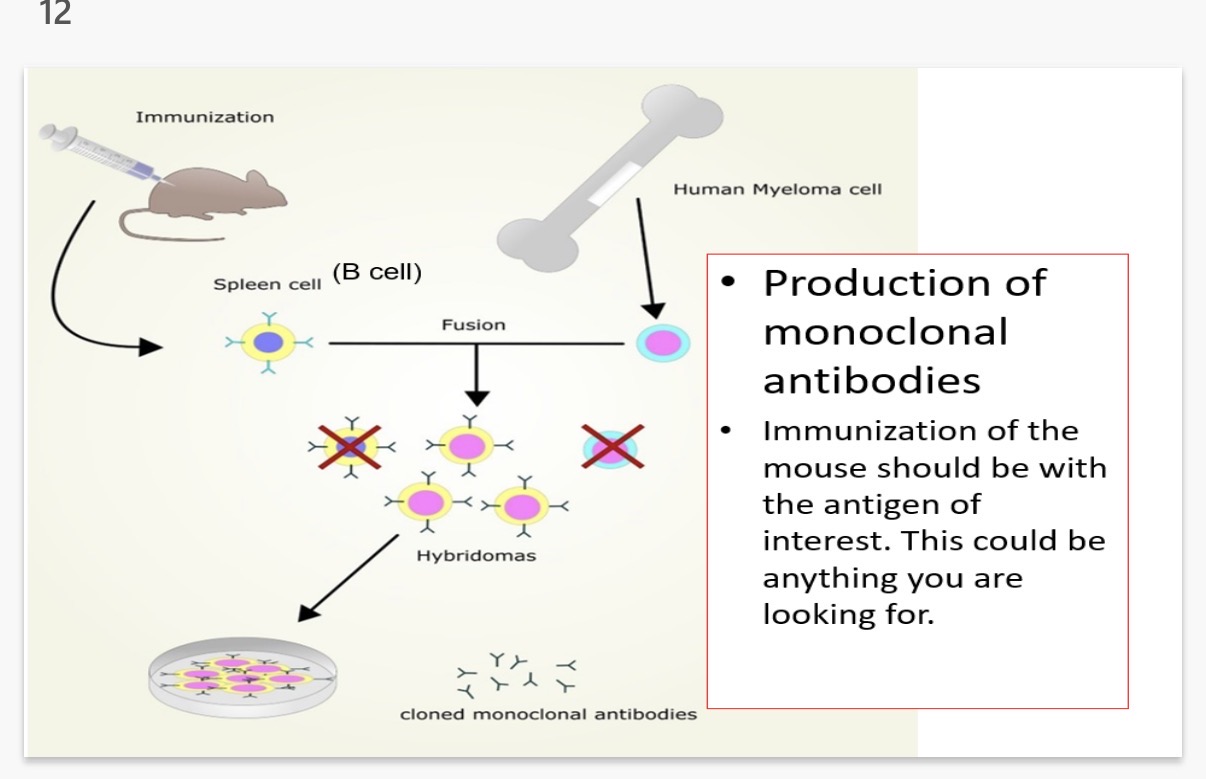
Monoclonal antibodies - how science works.
• A bacterium or other organisms entering the body has hundreds of different …1? on its surface and each will induce a …2? B-cell to clone itself.
• A single type of antibody can be isolated outside of the body and …3?. These are called …4? antibodies.
• Antibodies can be used in science laboratories, for detection of specific proteins.
What is the process of monoclonal antibody cloning?
State 4 uses of monoclonal antibodies?
After a disease is diagnosed, monoclonal antibodies are used in some medical treatments. Give 2 examples of using monoclonal antibodies in a medical treatments?
1.antigens. 2.different. 3.cloned. 4.mono-clonal
(1. Immunization: An animal (typically a mouse) is injected with an antigen to stimulate an immune response, causing it to produce antibodies.
(2. Spleen cell isolation: The animal's spleen, which is rich in antibody-producing B cells, is removed. The spleen cells are then isolated.
(3. Myeloma cell culture: Myeloma cells are cancerous plasma cells, which can grow indefinitely in culture, are selected.
(4. Cell fusion (Hybridoma formation): The spleen cells are mixed with the myeloma cells and are fused using a fusion agent (like polyethylene glycol) to form hybridoma cells. These hybridomas have the antibody-producing capabilities of the spleen cells and the immortality of the myeloma cells.
(5. Selection of hybridomas: The hybridomas are grown in a selective medium (like HAT medium) that allows only the hybridomas to survive.
(6. Screening and Cloning: The hybridomas are screened to identify those producing the desired antibody. The positive hybridomas are then cloned to ensure a pure population of cells, each producing the same antibody (monoclonal).
(7. Antibody production: The selected hybridomas are cultured in vitro (in a lab) or injected into animals to produce large quantities of the monoclonal antibody.
(8. Antibody purification: The monoclonal antibodies are purified from the cell culture medium or animal serum.
1. Immunoassay (pregnancy testing, drug testing in athletics, AIDS test).
2. ADEPT (fighting cancer)
3. Transplant surgery
4. Radioimmunotherapy
• they can be attached to drugs or medicines
•They can be used to target specific cells.
L6-The use of antibodies in the Elisa Test:
1) What is antigenic variation?
2) Explain why you can become infected with Flu even if you have had it before
•As soon as 28 days after recovery, those people who have tested positive for coronavirus or even those who just had symptoms can help the national effort by donating …3?
What is convalescent plasma?
In plasma therapy, convalescent plasma derivatives are infused into newly infected individuals.
Identify the component of the convalescent plasma which will be so useful to the newly infected individual? (1 mark)
A possible limitation to the success of plasma therapy is the mutation of the virus.
Define a genetic mutation?
(2 marks)
The ability of pathogens to change their surface antigens which occurs through mutations or genetic recombination.(leads to the emergence of new strains)
You can become infected with the Flu even if you have had it before because of antigenic variation. The influenza virus undergoes frequent mutations, which cause changes in its surface antigens. If the new flu strain has antigens that are different from the ones your immune system has encountered before, your existing antibodies may not be able to effectively neutralize the virus, making you susceptible to infection again.
Plasma
Convalescent plasma is plasma or plasma derivatives that are obtained from donors who have recovered from severe infection
Antibodies
A random change to the genetic material of an organism
The variable region of these antibodies will be complementary in shape to the …1? on the surface of the virus
The injection of antibodies is an example of what type of immunity?
Passive immunity does not result in the retention of …3? cells. Therefore, if an individual is infected a second time, they will not be …4?
How do mutations affect how antibodies work on viruses(pathogens)?
Note-The rest of the lesson focuses on the use of antibodies* in the 4 steps of the (ELISA) test. 6. What does ELISA stand for?———————————————————> These antibodies are known as detection antibodies.7.Explain why?
They may also be referred to as primary antibodies. 8. Explain why?
Antigens. 2. Artificial,passive immunity(since it involves medical intervention(artificial) and is supplied from another source(passive)
Memory. 4.immune
The mutation could result in a change to the shape of the surface antigens. This means that antibodies that were specific to the antigens and were able to prevent the virus from infecting a host cell may no longer be effective against this new variant
enzyme- linked immunosorbent
assay Test
as they are specific to the antigen on the surface of a particular pathogen, which if detected will allow a particular disease to be diagnosed.
Because they bind directly to the antigen
The ELISA Test:
Step 1: known Antigens from the sample are …1? On a surface.
Note-The antigens can be bound to the supporting surface (usually a …2?) by a combination of hydrophobic interactions and …3? links. This is known as …4? and is an example of …5?-specific immobilisation
Note-The antigens would be immobilised in the wells of the microtiter plate.
1.immobilised(fixed in place)
Polystyrene microtiter plate
Ionic. 4.adsorption. 5.non
ELISA Test:
What happens in step 2 and 3 of the ELISA Test?
Step 2: The detection antibodies are added over the solid surface and the complementary shape of their …2? region for the antigens allows them to form a …3? with …4? of these antigens that may be found in the sample. Note that Each detection antibody is …5? linked to an enzyme(The enzyme will catalyze a reaction that produces a measurable signal I.e. colour change)
Why do we wash the plate with mild detergent solution?
Step 2:Detection antibodies are applied over the surface.
Step 3:The plate is washed with a mild detergent solution.(stage microtiter plate)
2.Variable. 3.complex. 4.any. 5.covalently
The washing between each step removes any antigens or antibodies that are not specifically bound
ELISA Test:
What happens in step 4?
Step 4 key point: If any antigens are present in the sample, meaning that …2? have formed between these antigens and their specific antibodies, then the reaction which is catalysed by the binding of the substrate and the enzyme produces a detectable signal such as a …3?(A colour change indicates the presence of the target molecule [e.g. antibodies against a specific pathogen],while no colour change means it’s absent)
The Link between the tertiary structure and the success of the ELISA TEST:
The shape of the variable region on the antibody is controlled by the …4? structure and this allows this protein to bind to the …5? in the sample
• The shape of the enzyme's active site is controlled by the …6? structure and this allows this enzyme to bind with the …7? resulting in the detectable change.
Note:The ELISA test has been used as a …8? tool for HIV, malaria, coeliac disease, hepatitis B and C and numerous other animal diseases but, it can also be used in plant …9? and in the food industry to detect potential …10? like peanuts
The enzymes substrate is added.
Complexes. 3.colour change
Tertiary. 5. Antigen. 6.tertiary 7.substrate. 8.diagnostic. 9.pathology(scientific study of diseases in plants)
Allergens
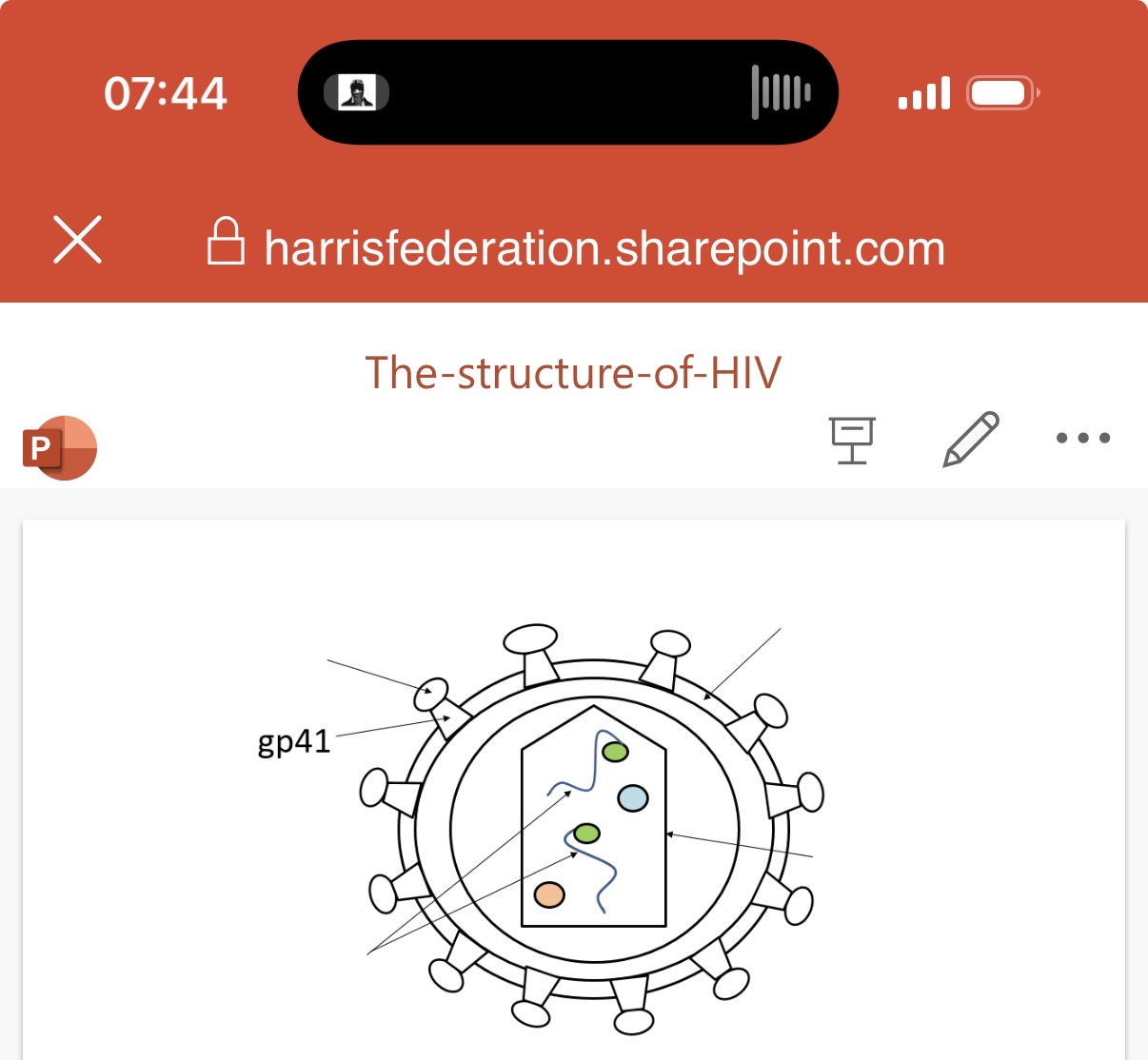
Label the image of the structure of hiv ?
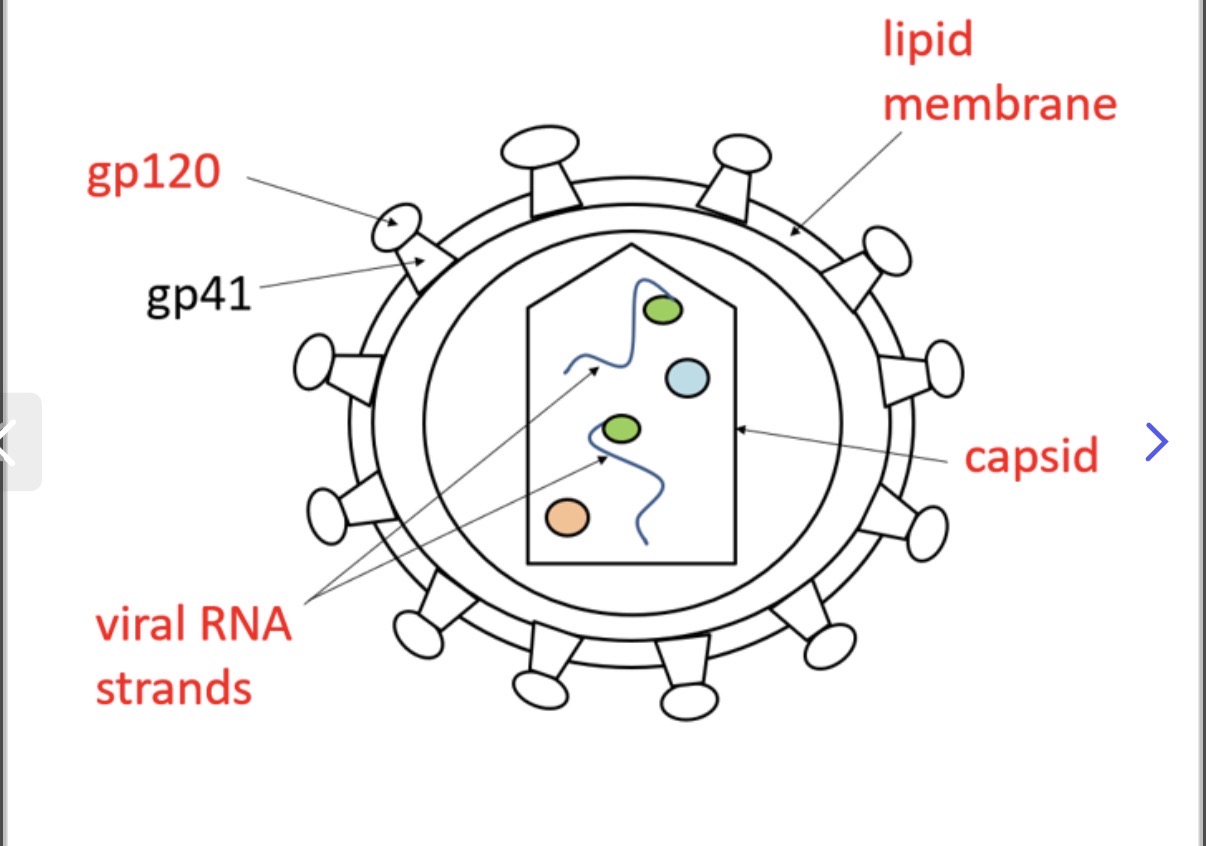
(May not needs this so confirm with teacher first)
Okay, for AQA A-level Biology, you need to understand the general principles and key steps of an ELISA test, particularly the indirect ELISA, which is commonly used to detect antibodies.
Here are the essential steps you should know:
1. Antigen Immobilization:
* First, known antigens are adsorbed (stuck) onto the wells of a polystyrene microtiter plate. These antigens are specific to the antibodies you are trying to detect.
2. Blocking:
* A blocking solution (like bovine serum albumin or milk protein) is added to coat any remaining empty sites on the well surface. This prevents non-specific binding of other proteins later in the test, which would lead to false positive results.
3. Sample Addition:
* The patient's blood sample (serum, which contains antibodies if they've been exposed to the pathogen) is added to the wells.
* If specific antibodies are present in the sample, they will bind to the immobilized antigens in the wells.
* If no antibodies are present, they won't bind.
4. First Wash:
* The wells are washed thoroughly with a buffer solution (often containing a mild detergent). This step is crucial to remove any unbound antibodies or other components from the patient's sample, leaving only the specific antibodies that have bound to the antigens.
5. Addition of Secondary Antibody (Conjugate):
* An enzyme-linked secondary antibody is added. This secondary antibody is designed to bind specifically to human antibodies.
* Crucially, this secondary antibody has an enzyme (like horseradish peroxidase or alkaline phosphatase) attached to it.
6. Second Wash:
* Another wash step is performed to remove any unbound enzyme-linked secondary antibodies. This ensures that only the secondary antibodies that have bound to the patient's antibodies (which are themselves bound to the antigen) remain.
7. Substrate Addition:
* A colorless substrate specific to the enzyme attached to the secondary antibody is added to the wells.
8. Color Development and Detection:
* If the enzyme is present (meaning the patient's antibodies and the secondary antibody are bound), the enzyme will act on the substrate, causing a color change.
* The intensity of the color is usually proportional to the amount of antigen or antibody present in the original sample. This color change can be measured using a spectrophotometer.
Key things to remember for AQA:
* Specificity: ELISA relies on the highly specific binding between antigens and antibodies.
* Enzyme Link: The enzyme linked to the secondary antibody is what ultimately produces the detectable signal (color change).
* Washing Steps: These are vital to remove unbound molecules and prevent false positives, ensuring only specific binding is detected.
* Blocking Step: Prevents non-specific binding to the plate itself.
* Interpretation: A color change indicates the presence of the target molecule (e.g., antibodies against a specific pathogen), while no color change means it's absent.
Uses of Monoclonal antibodies include:
•Pregnancy …1?
•Medical diagnosis(…2? Testing)
•Treatment of diseases
•immuno…3? Testing(pregnancy testing,drug testing,AIDS testing)
•…4?immunotherapy
Testing
ELISA
assay
Radio

Using the image, explain the steps on how pregnancy tests allow us to look for the presence of the HcG hormone in females-urine.
(1) When urine is applied to the stick, it moves along the strip via capillary action. This first section contains mobile monoclonal antibodies attached to blue beads (or dye).
• If hCG is present: The hCG hormone binds to these mobile antibodies. The "hormone-antibody-bead" complex then begins to travel up the stick together.
• If hCG is absent: The mobile antibodies and blue beads still travel up the stick, but they aren't carrying any hormone.
(2)The Result Window (The Test Line)
This area contains immobilized antibodies—meaning they are stuck to the paper and cannot move.
• Positive Result: The hCG (which is already stuck to a blue bead) binds to these stationary antibodies. This "sandwiches" the hormone between two antibodies, trapping the blue beads in one place. As the beads accumulate, a blue line appears.
• Negative Result: Since there is no hCG to act as the "glue" between the mobile beads and the stationary antibodies, the blue beads simply sail right past this window without stopping. No line forms.
(3)The Control Window (The Safety Check)
This window shows if the test is working. It contains a third type of antibody that is designed to bind to the mobile antibodies themselves, regardless of whether hCG is present.
• If a blue line appears here, it proves the urine successfully carried the beads all the way up the strip.
• If no line appears in the control window, the test is invalid (perhaps not enough urine was used, or the test is expired).
Radioimmunotherapy(radiation antibody treatment)
• Use of radioactively conjugated …1? Antibodies against antigens
Radioimmunotherapy is a type of …2? treatment that uses both radiation and antibodies. Antibodies are designed to specifically …3? cancer cells. In radioimmunotherapy, these antibodies are linked to a radioactive substance. Once the antibodies attach to the cancer cells, they deliver a dose of radiation directly to the tumor, …4? the cancer cells while minimizing damage to healthy tissues.
Murine refers to antibodies derived from …5?. These antibodies are used in treatments or diagnostic tests, and they have a characteristic of being …6? cleared from the body, which is beneficial for …7? a patient's exposure to radiation.
Murine
Cancer
Target
Killing
Mice
Cleared
Reducing