bio 230 unit 3
1/121
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
122 Terms
mutualism
depend on each other
humans and e. coli

symbiotic
one dependent, other may or may not

commensalism
one benefits, other is unaffected

parasitism
one benefits, other harmed

normal microbiota behavior
do not cause disease under normal conditions.
cause disease during suppression of immune system, change in residing environment, location change in body
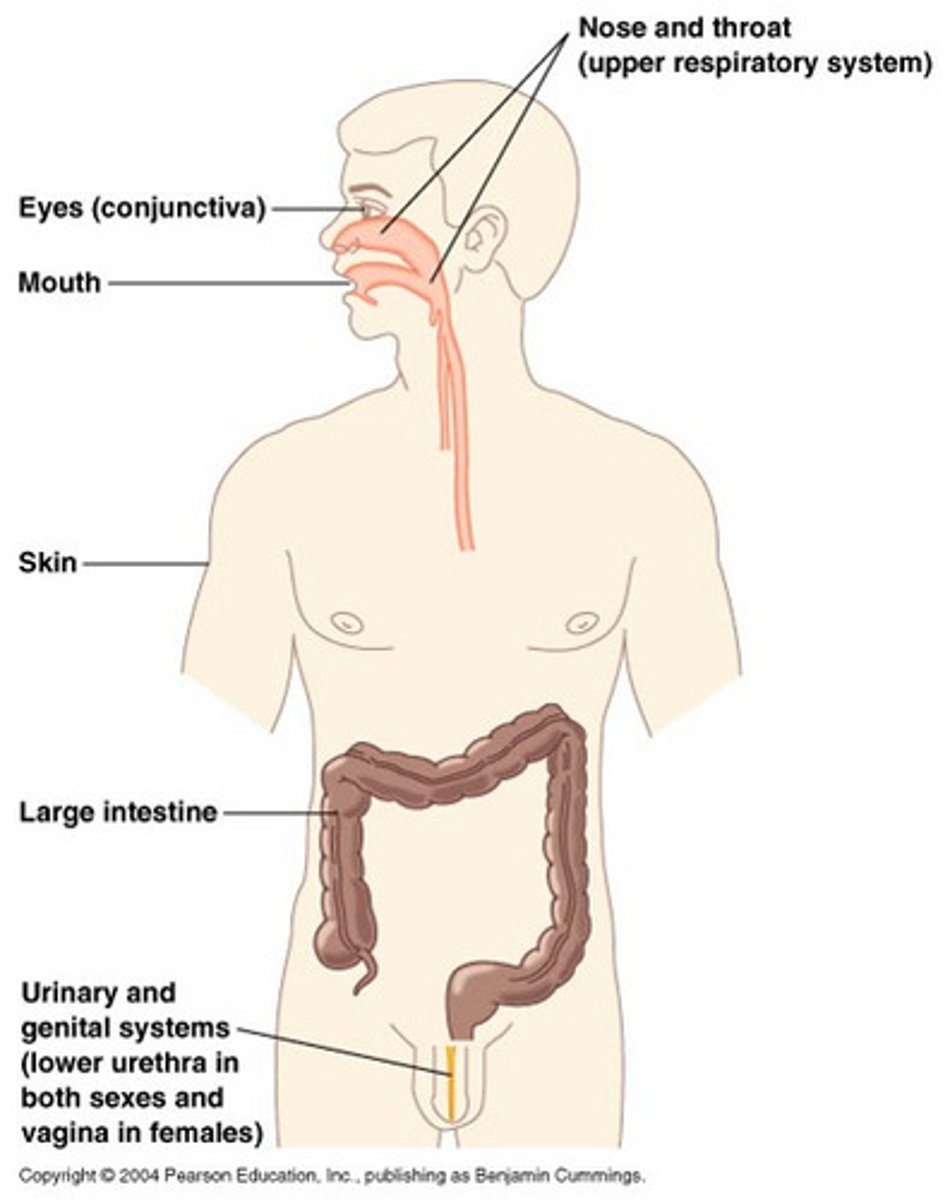
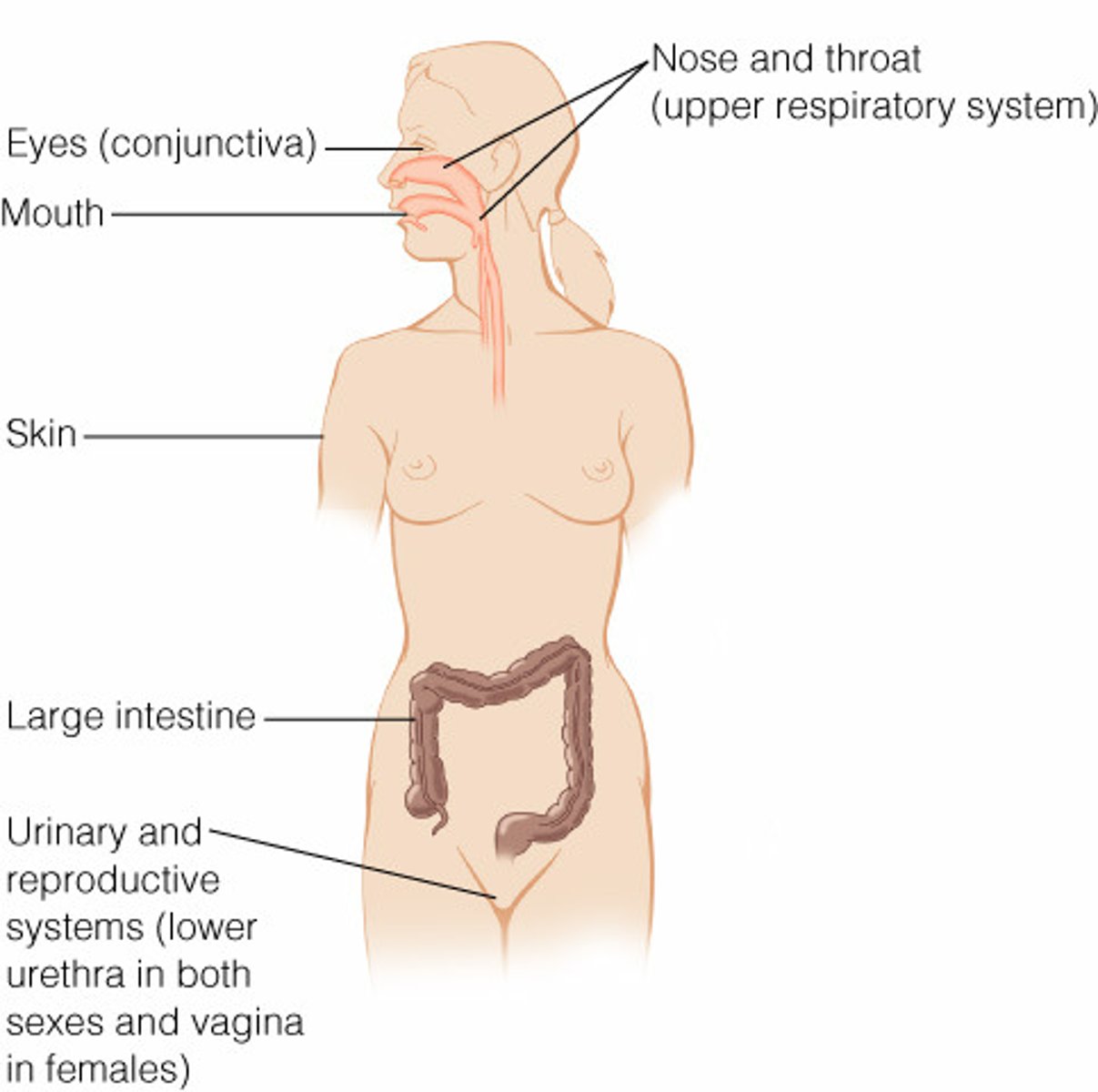
normal microbiota locations
upper respiratory tract, upper & lower digestive tract, urinary & reproductive system, eyes & skin
endemic
local in population
epidemic
greater than normal frequency for given population
pandemic
greater than normal frequency throughout world
sporadic disease
occurs only occasionally
epidemiology
study of occurrences, distribution, spread of disease in humans
acute disease
symptoms and disease run quickly
chronic disease
slow symptoms develop over long period of time
asymptomatic disease
disease without symptoms
latent disease
appears after being dormant in the body for a long time
communicable disease
transmitted from one host to another
contagious disease
spreads quickly and easily
noncommunicable disease
cannot transfer host to host
systemic infection
widespread throughout the body.
travel by blood or lymph
local infection
limited to a small region of the body
primary infection
initial infection
secondary infection
follow primary.
opportunistic or normal microbiota taking advantage of weakened immune system
stages of acute infectious disease
1. incubation
2. prodromal
3. illness
4. decline
5. convalescent
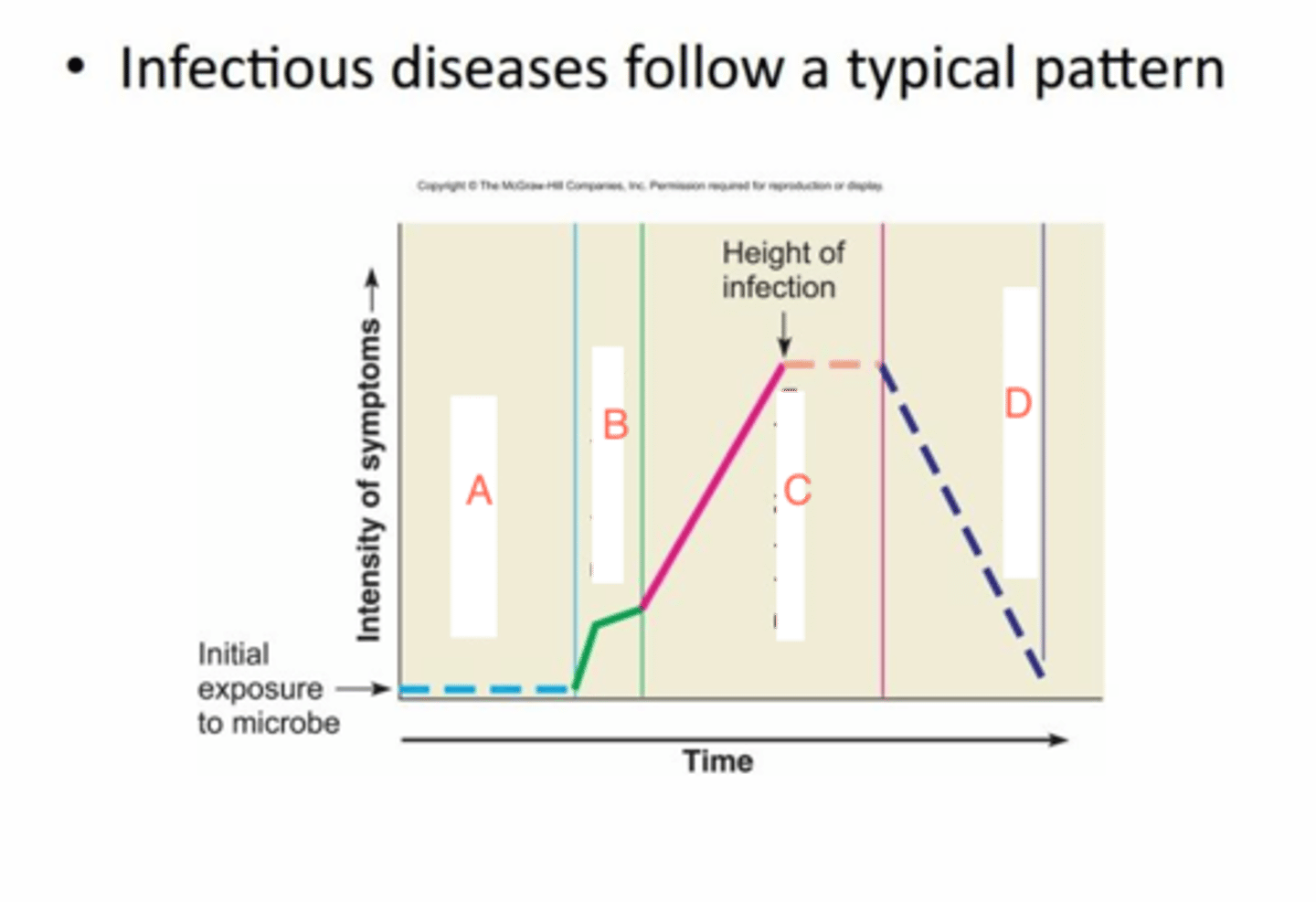
incubation
exposure/day zero, no signs or symptoms
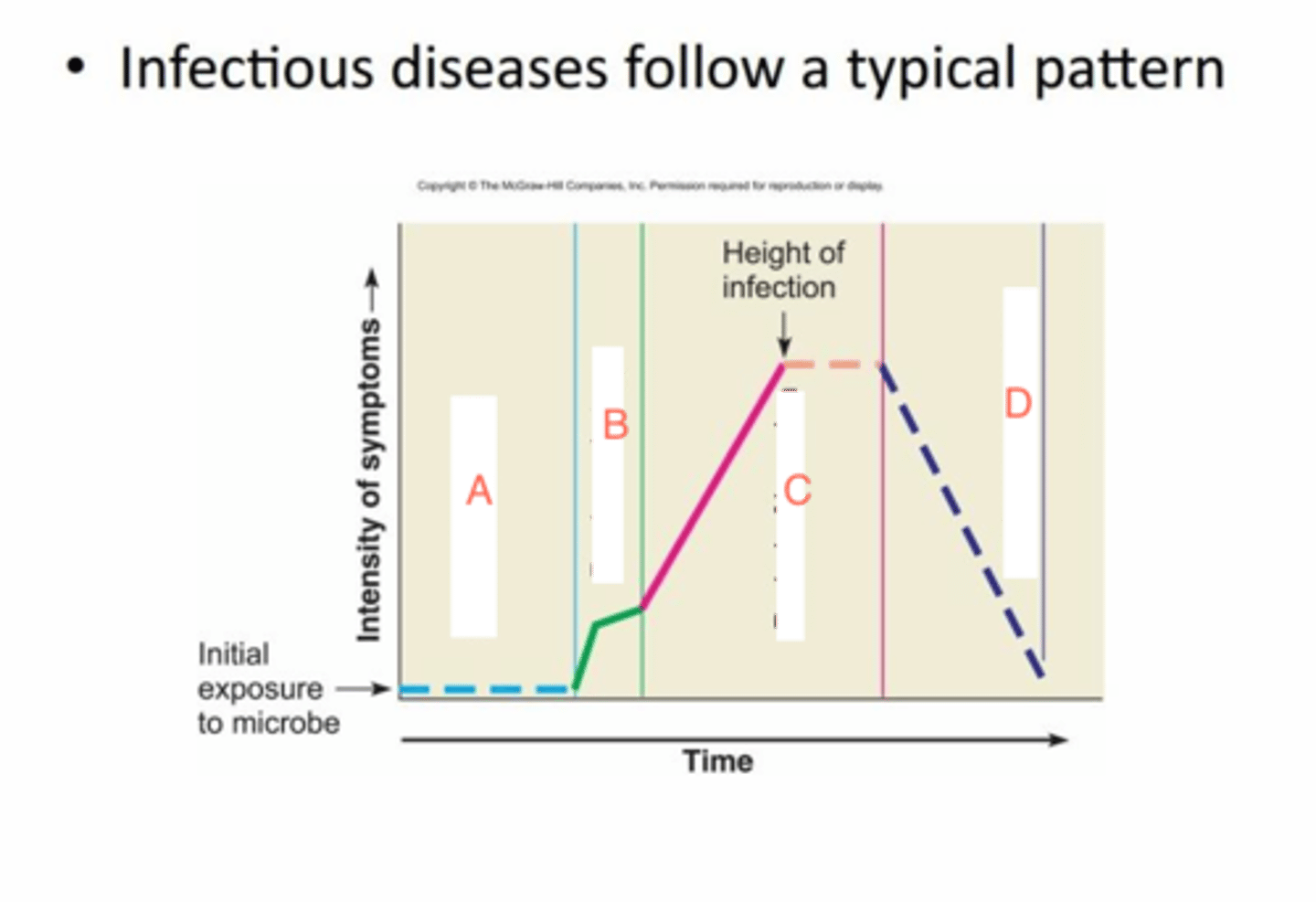
prodromal
vague, general symptoms or feeling of discomfort
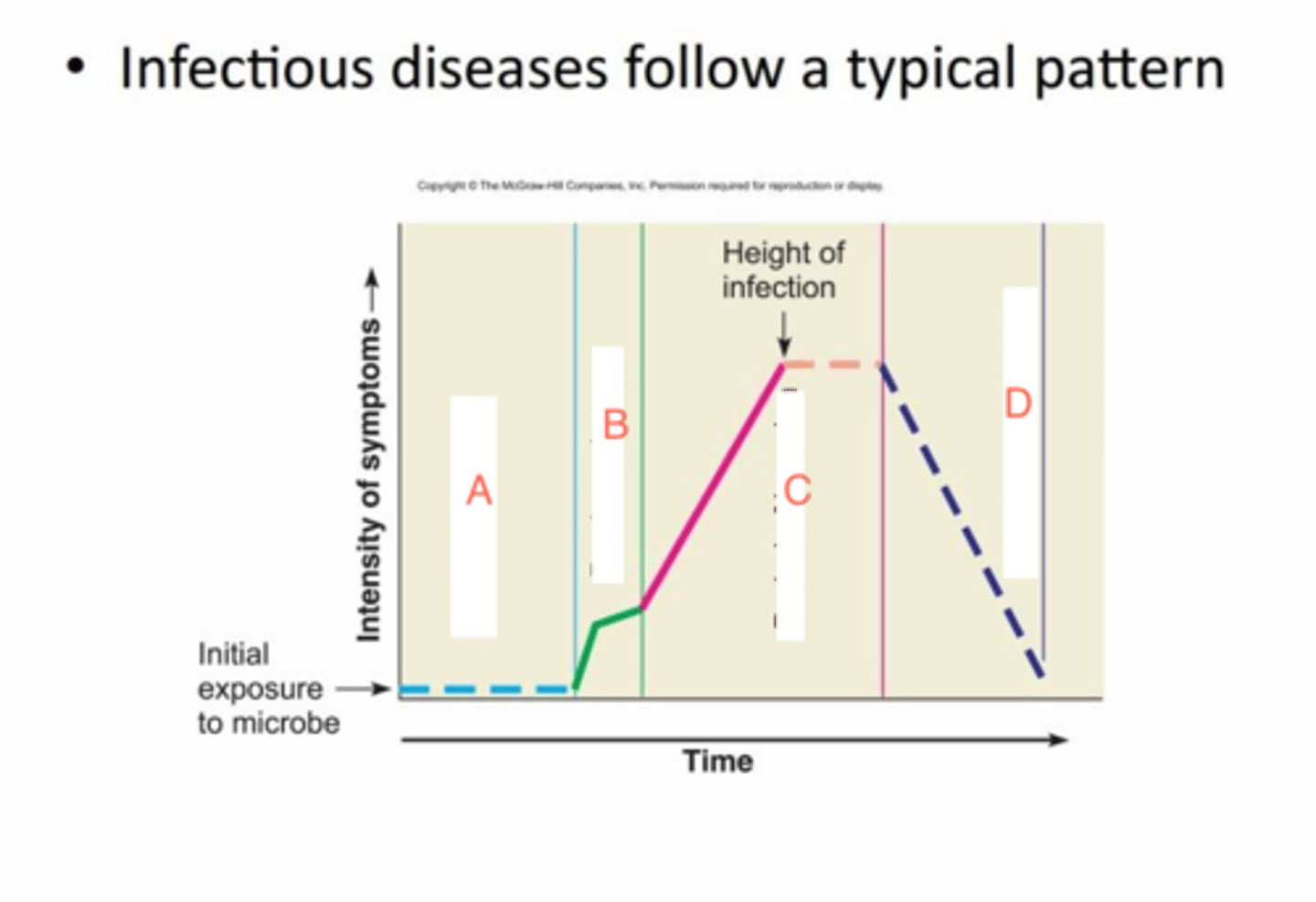
illness
microorganisms multiplying rapidly, specific symptoms are most severe
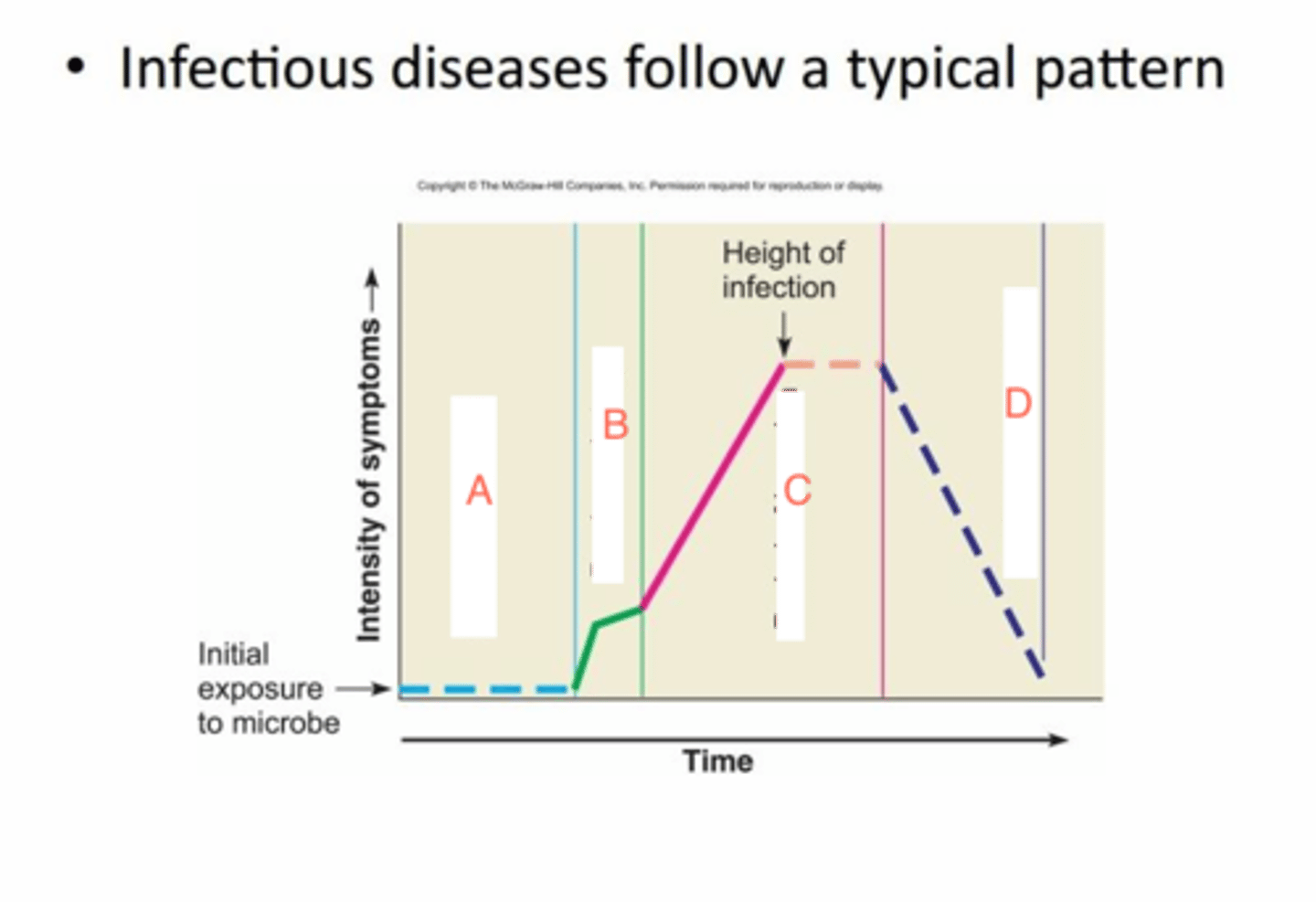
decline
microorganisms decline in numbers, where secondary infection may occur, decline in symptoms
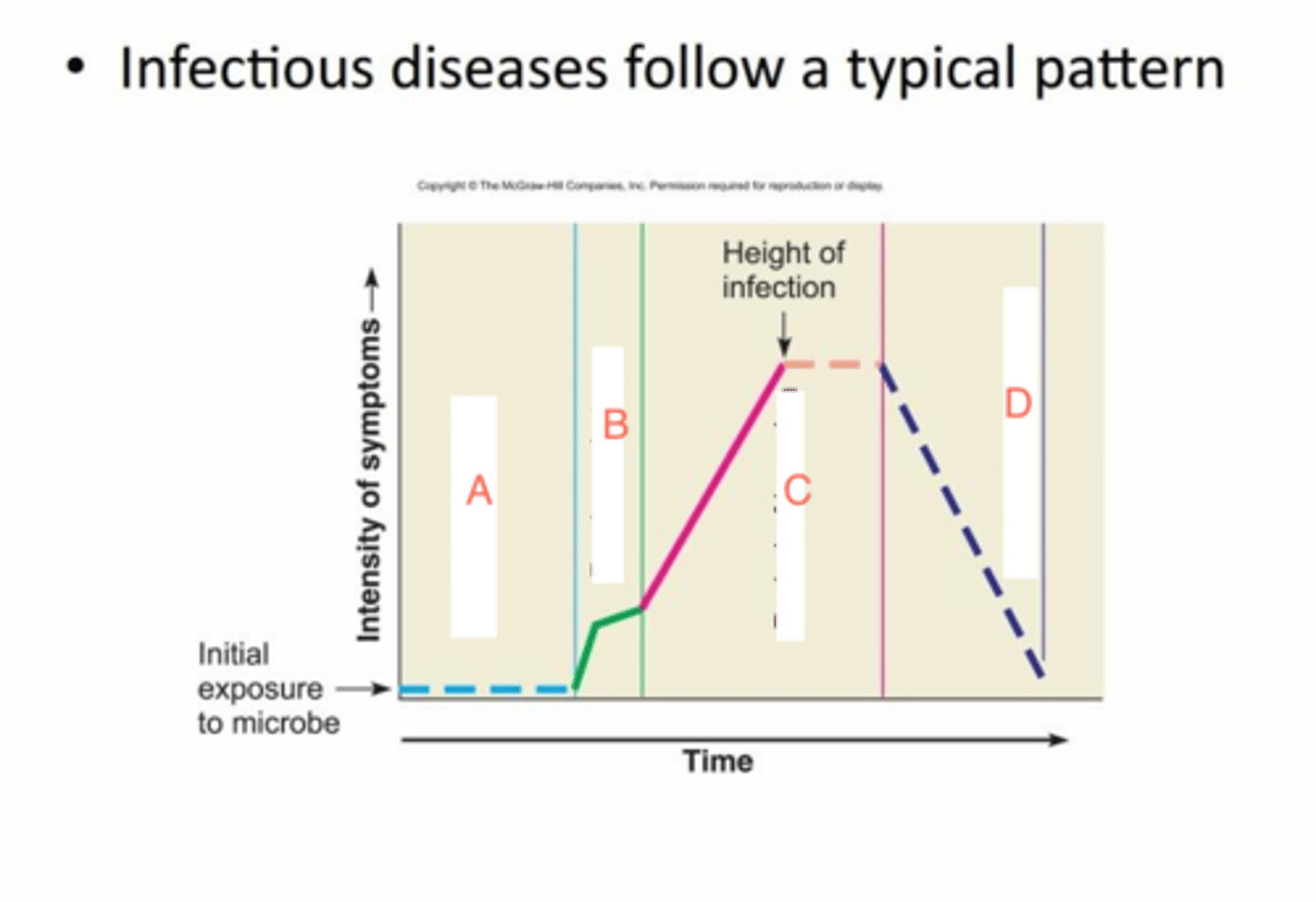
convalescence
feeling better but microorganisms still present
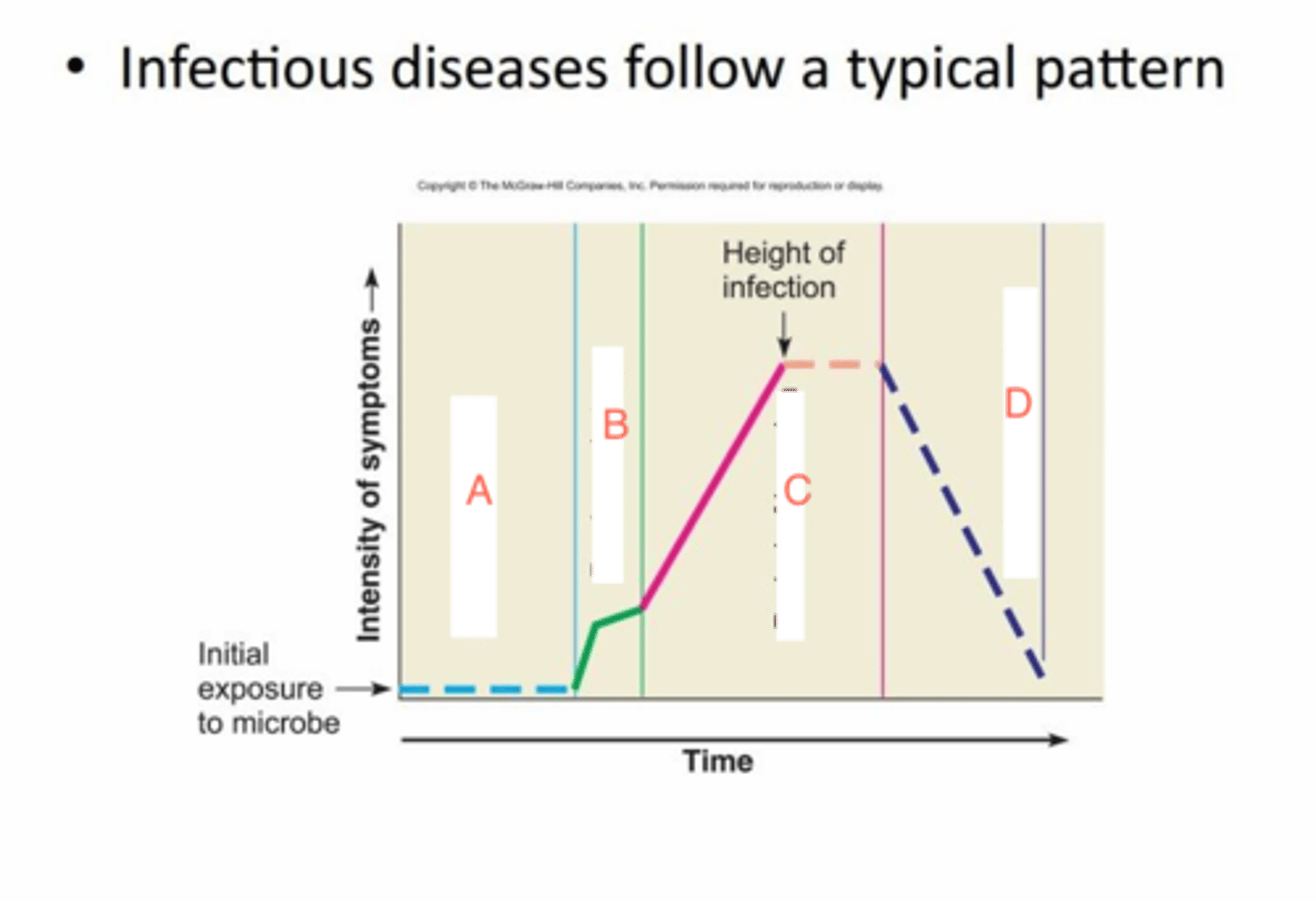
koch's postulates
1. agent present in every case
2. agent isolated in pure culture
3. agent causes disease in healthy host
4. same agent reisolated from experimental host
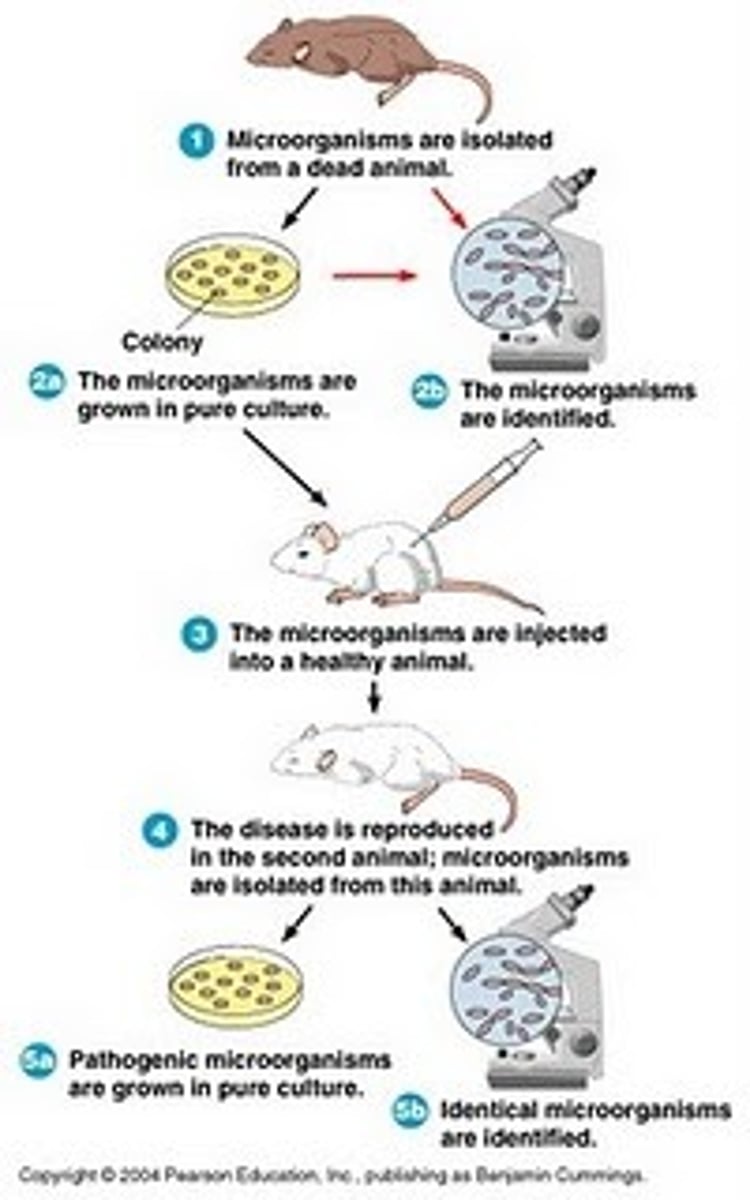
exceptions to koch's postulates
1. multiple agents cause disease (pneumonia)
2. agent may not be culturable (hep B, syphilis)
3. may not have experimental healthy host (HIV)

reservoir
where a pathogen can survive and be transmitted.
living: animals, humans (healthy & sick)
nonliving: water, soil
host
organisms supports growth of the pathogen
vector
arthropod capable of transmission

zoonotic
disease transmitted between animals and humans
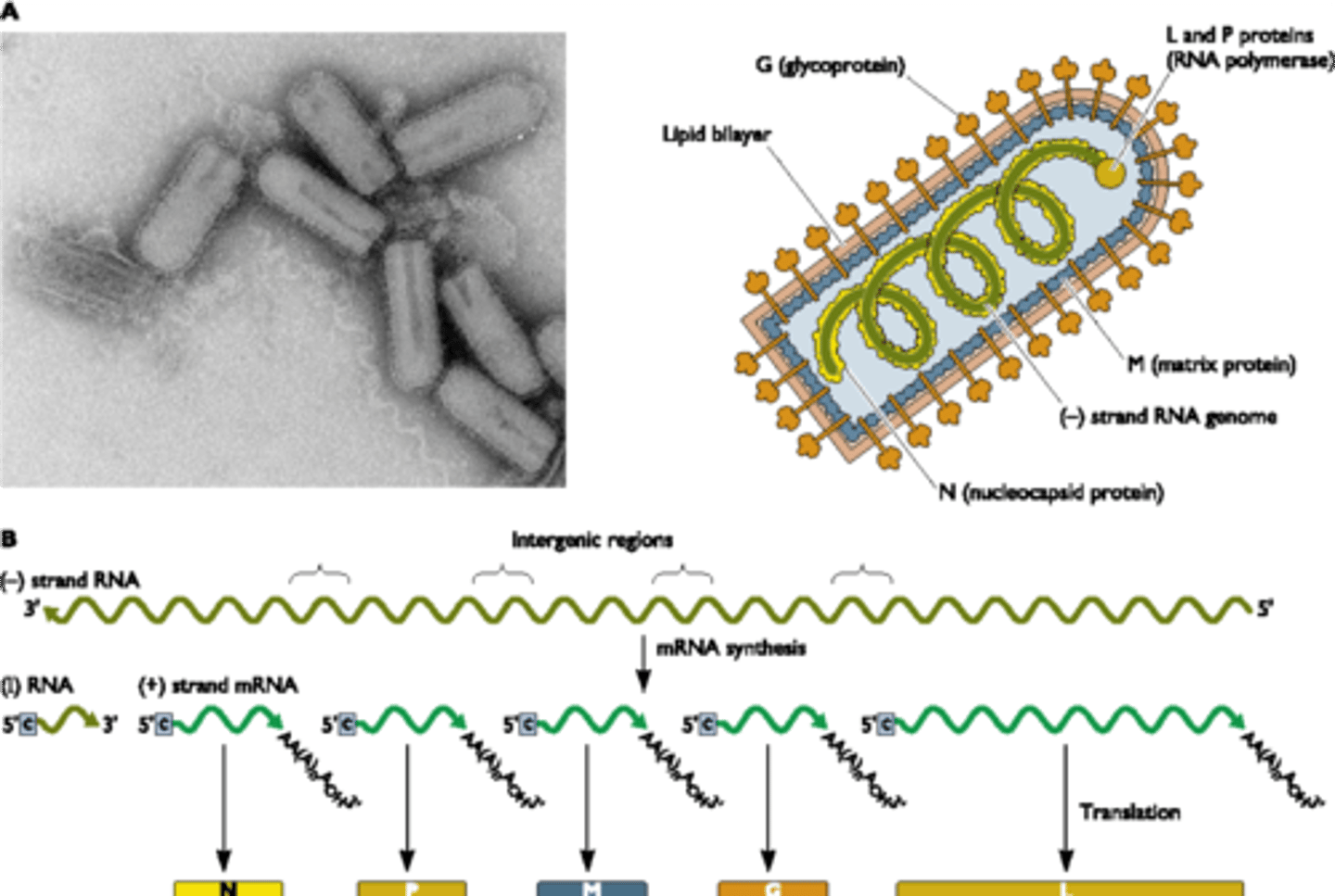
rabiesvirus
transmitted by animal bite, fatal once symptoms occur.
travels from bite up nervous system to brain.
reservoir typically racoons, bats, dogs.
direct trasmission
direct contact: skin to skin
close contact: within 1 meter
indirect transmission
fomite: touching objects, anything nonliving
vehicle: air, water, food
airborne transmission
droplets travel greater than 1 meter

foodborne transmission
eating contaminated food
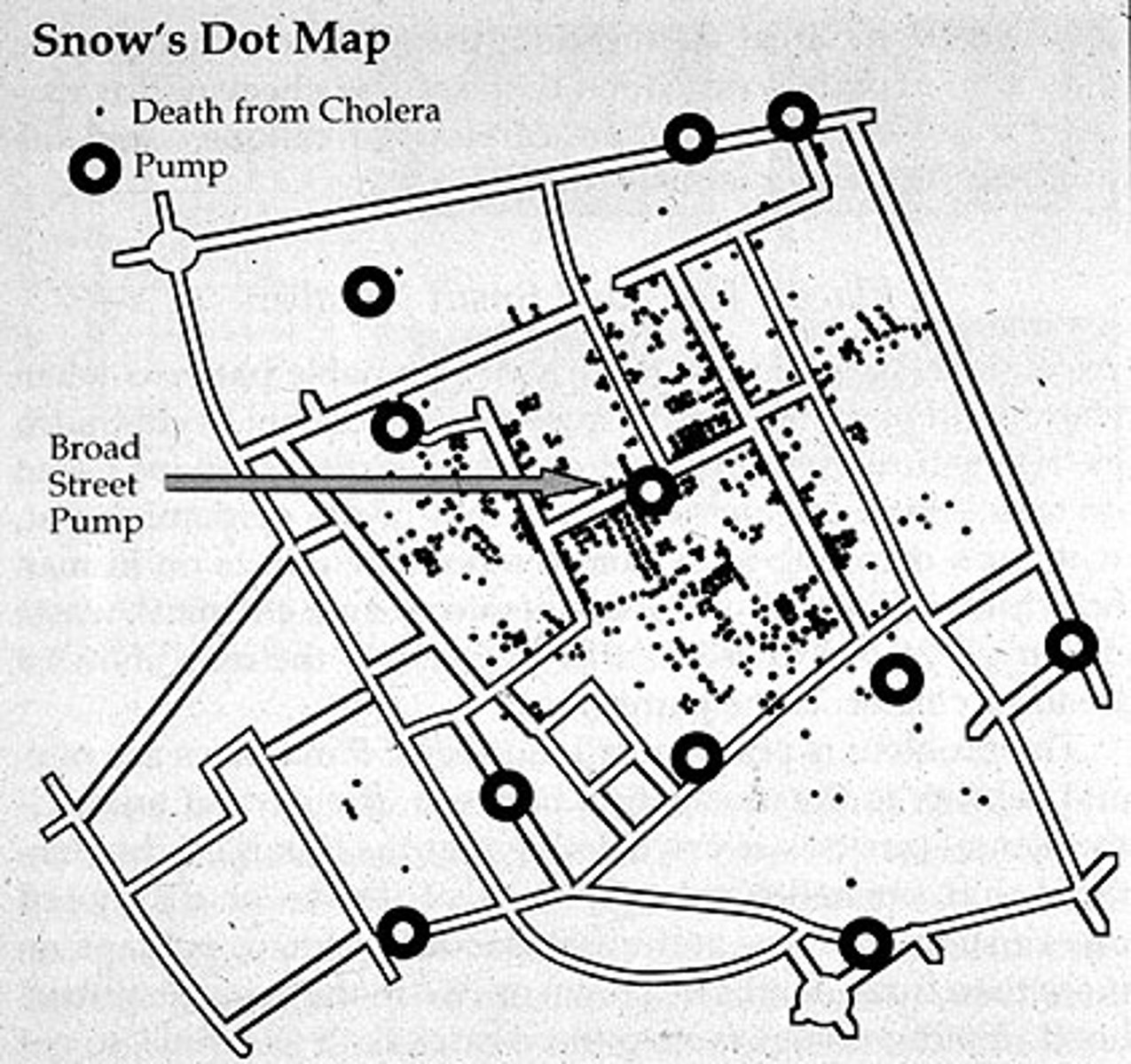
waterborne transmission
drinking contaminated water
nosocomial infection
acquired in hospital
1. presence of microorganisms
2. immunosuppressed patients
3. transmission between patients and staff (only preventable)
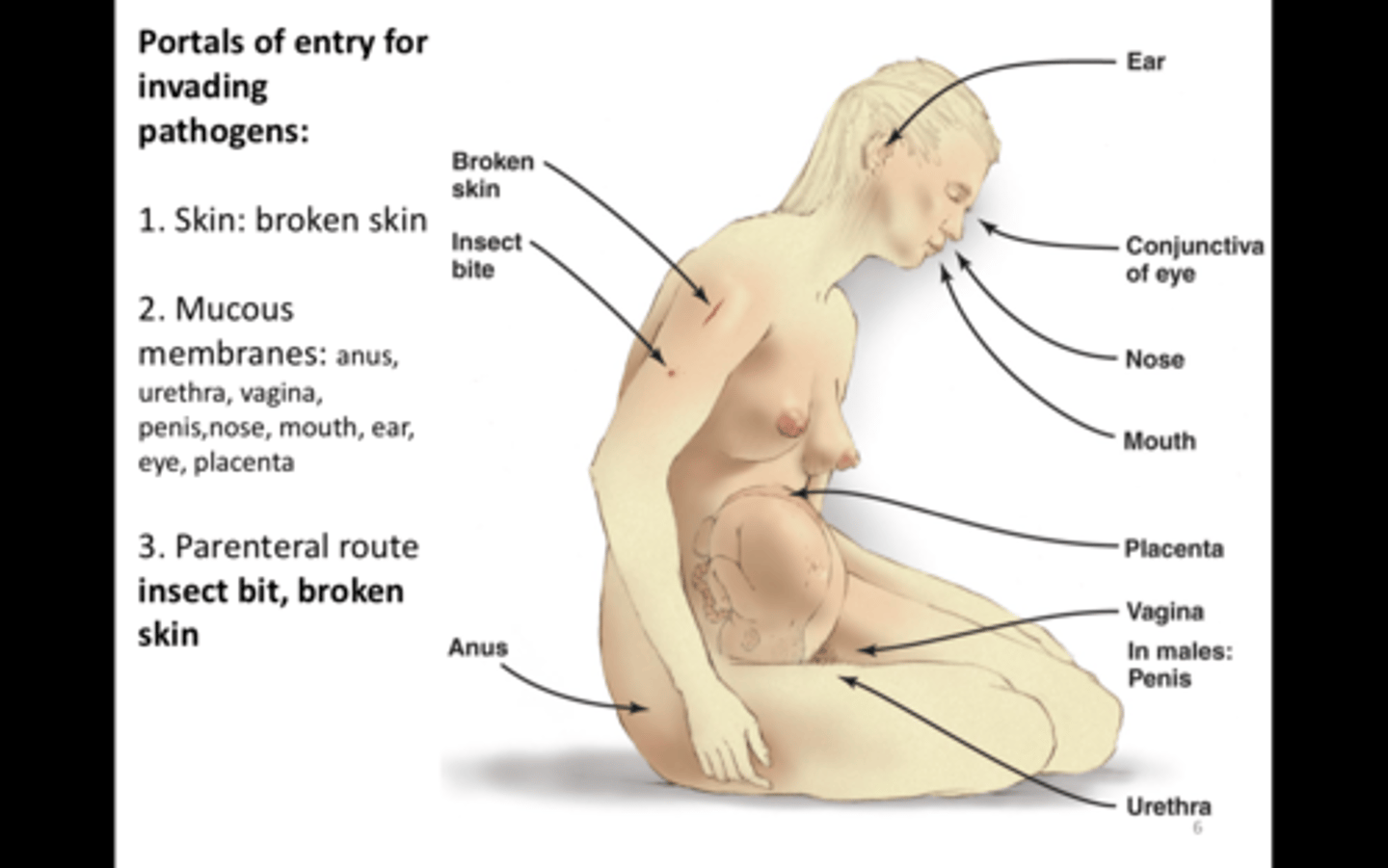
portals of entry/exit
skin (wounds)
mucus membrane (respiratory, eyes, genital, gastrointestinal)
parenteral (penetration)
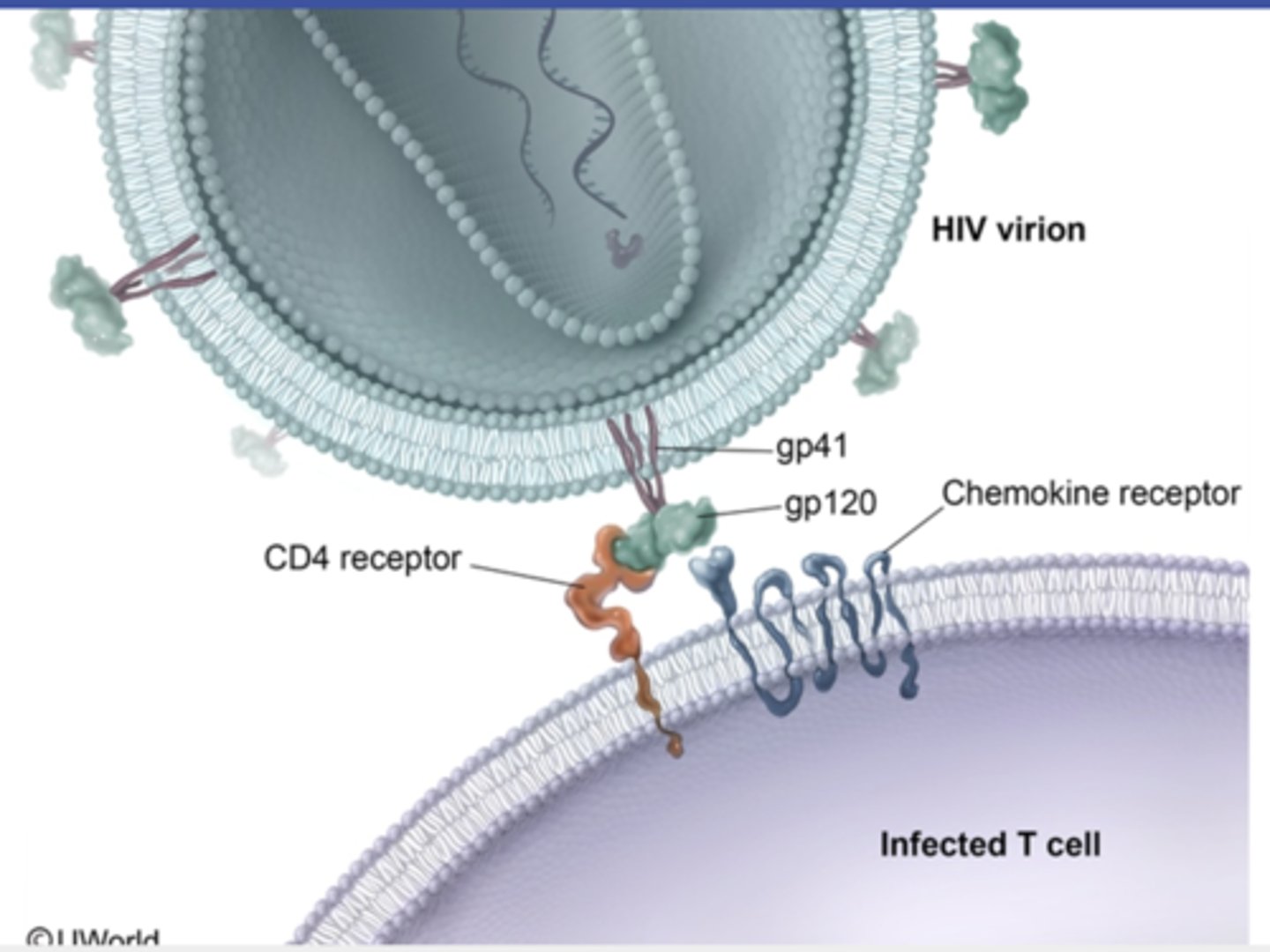
adhesion factor
need adhesion to tissue for infection
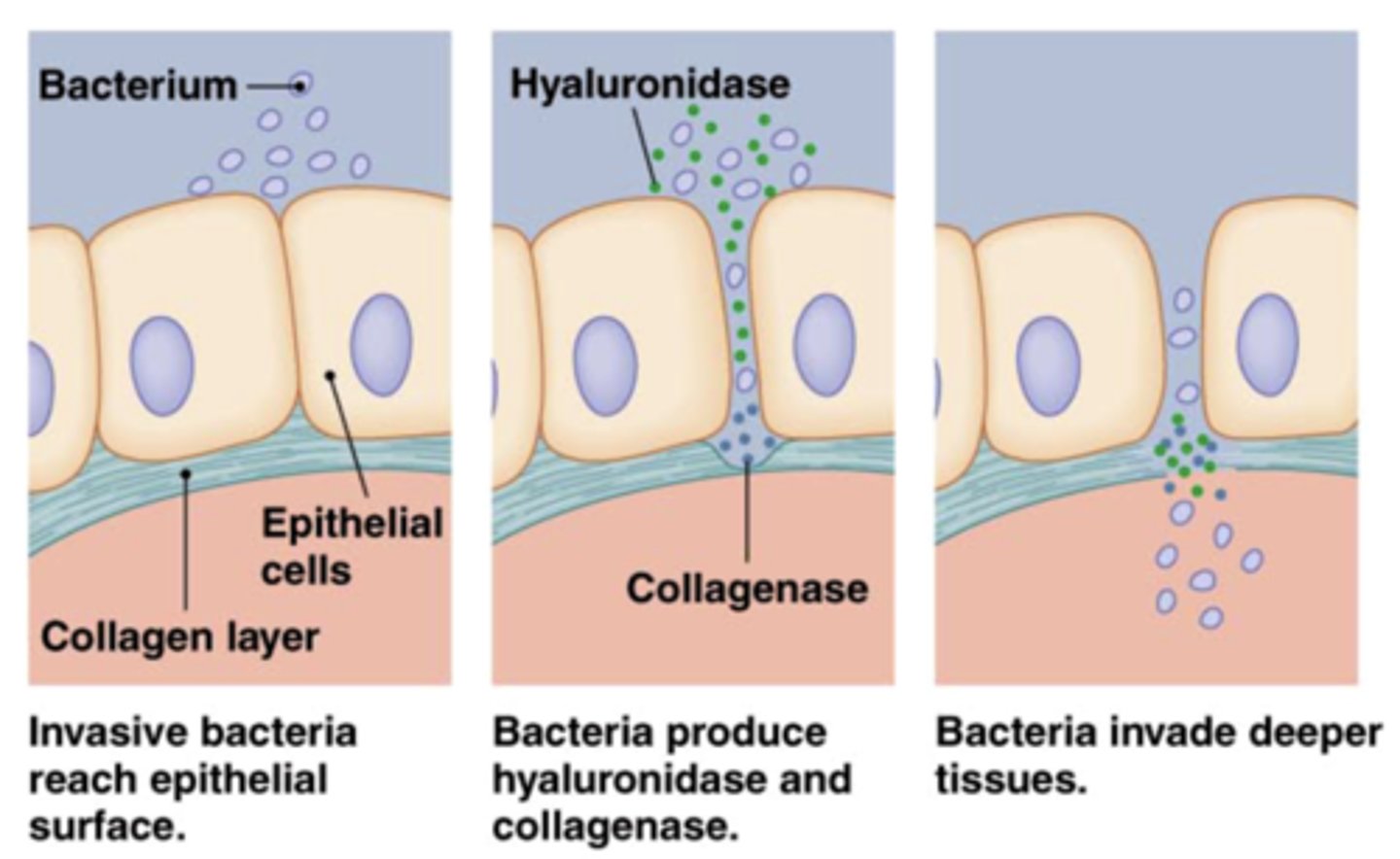
virulence factors
increases ability to cause an infection
hyaluronidase & coagulase
virulence factor by allowing penetration into deep tissues. coagulase escapes immune response
capsules
virulence factor by resisting phagocytosis
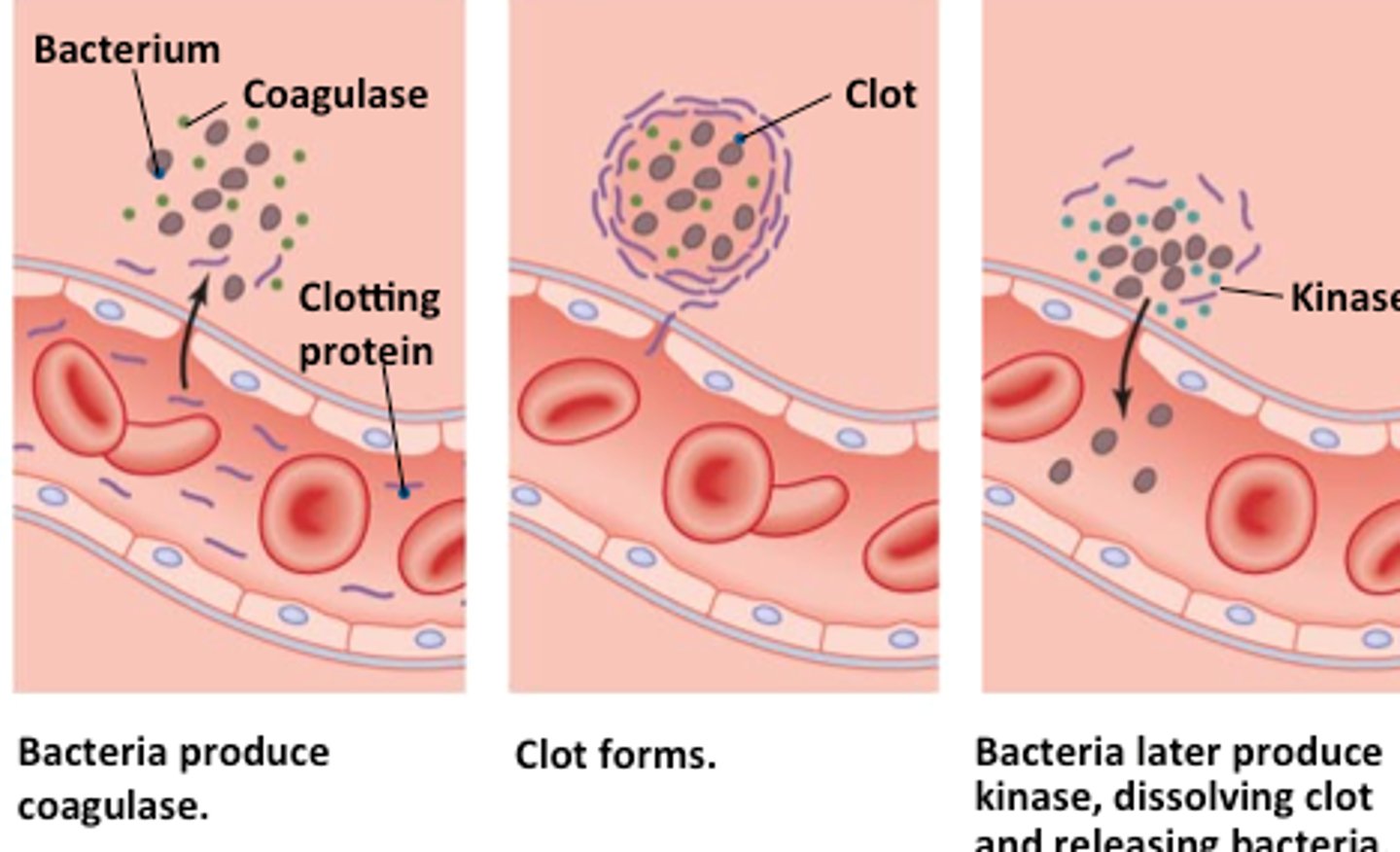
coagulase and kinase
coagulase allows clots to form around bacteria. fibrin allows bacteria to remain undetected until released by kinase production
endotoxins
outer membrane of G- bacteria.
when cell dies, lipopolysaccharides are released as lipid A.
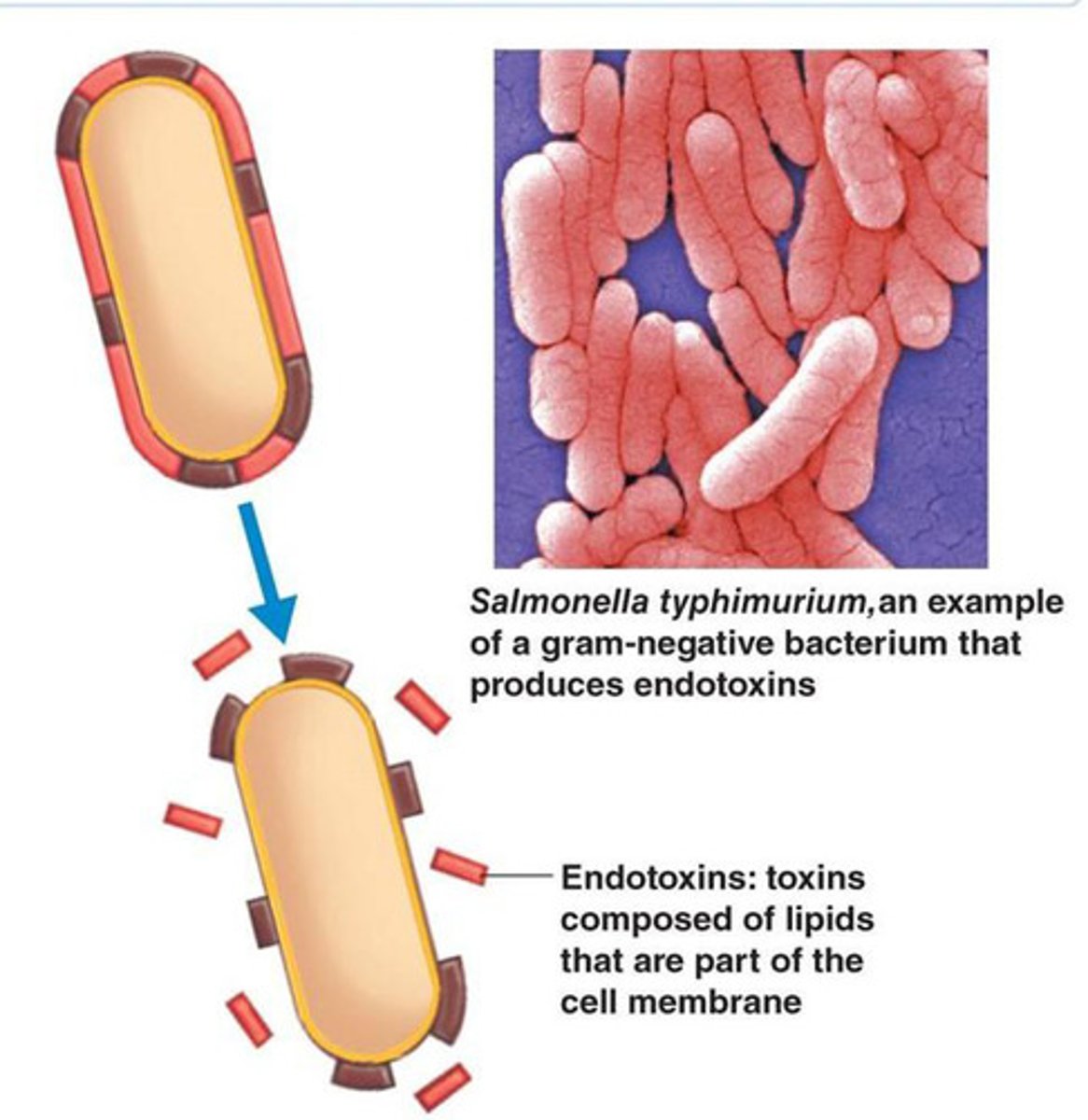
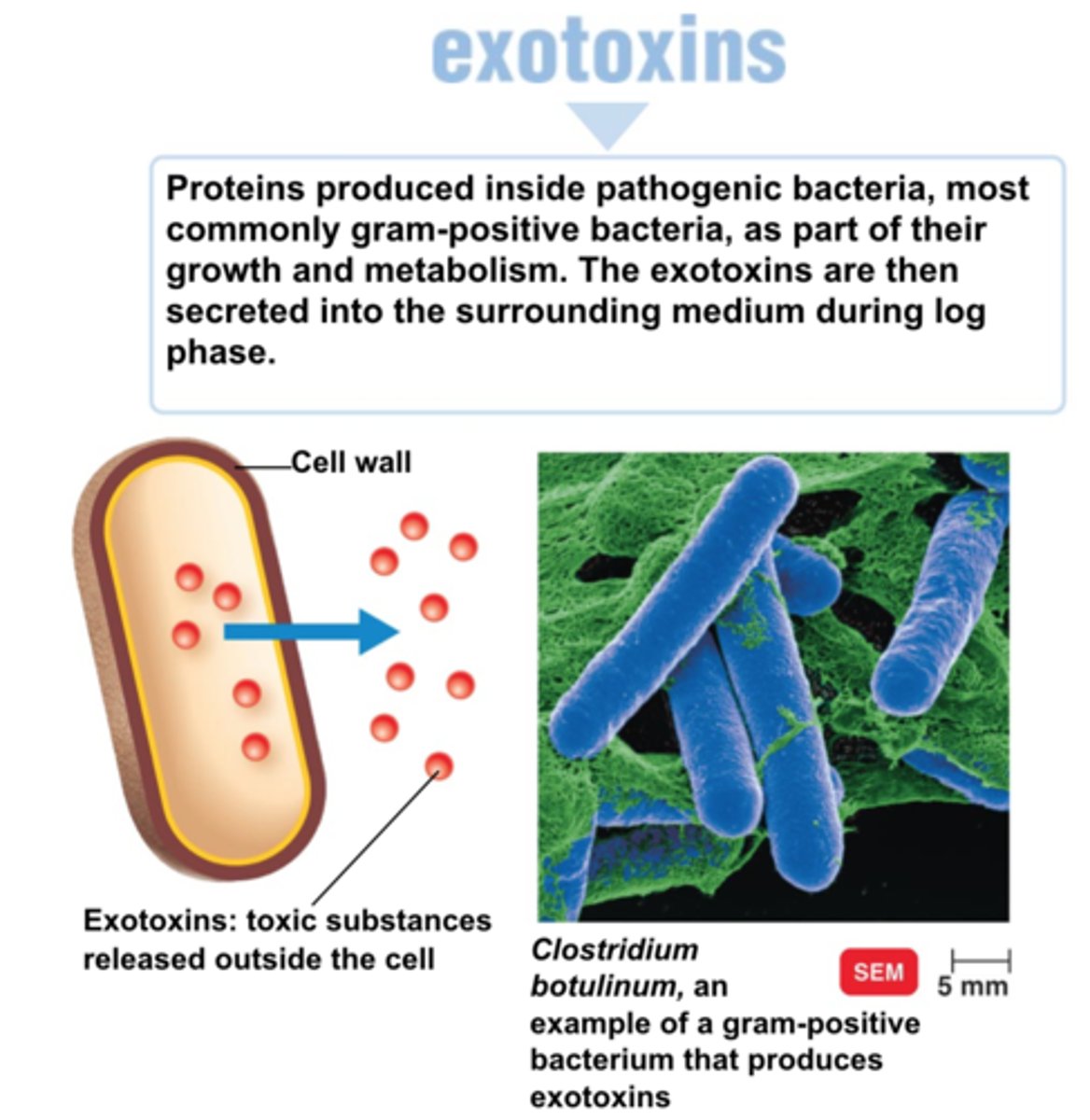
exotoxins
mostly G+, some G-.
metabolic production from a living cell releases protein.
categorized based on body part infected. gene on plasmids.
neurotoxin
exotoxin in brain.
clostridium tetani (tetanus) produce neurotoxins that travel up spinal cord to block signals that allow muscle relaxation leading to spastic paralysis.
clostridium botulinum (botulism) causes flaccid paralysis in nervous system
enterotoxin
exotoxin in gastrointestinal tract.
intoxication of foodborne illness, food inoculated with staphylococcus at room temperature allows for multiplication and production of enterotoxin. after vomiting toxin leaves.
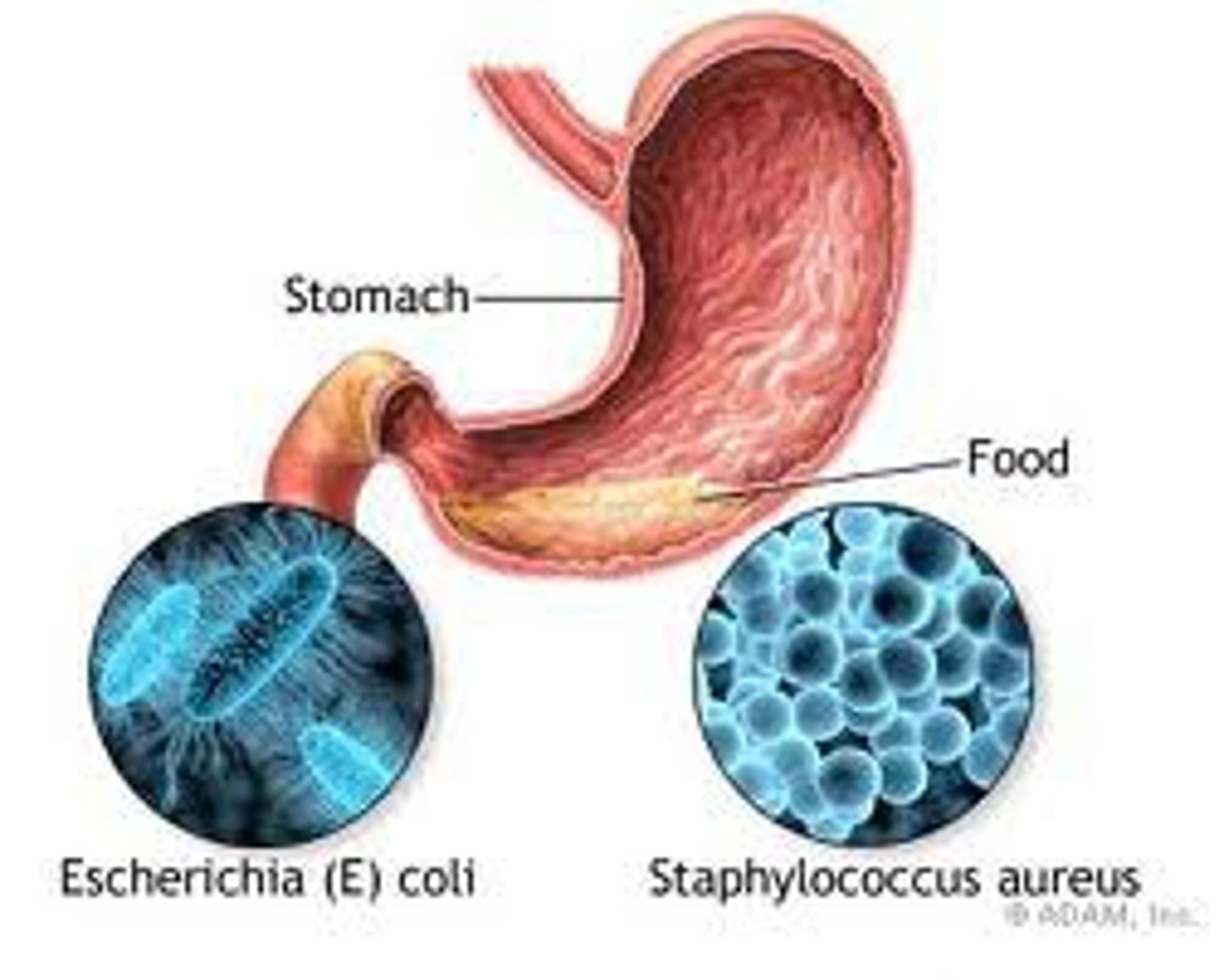
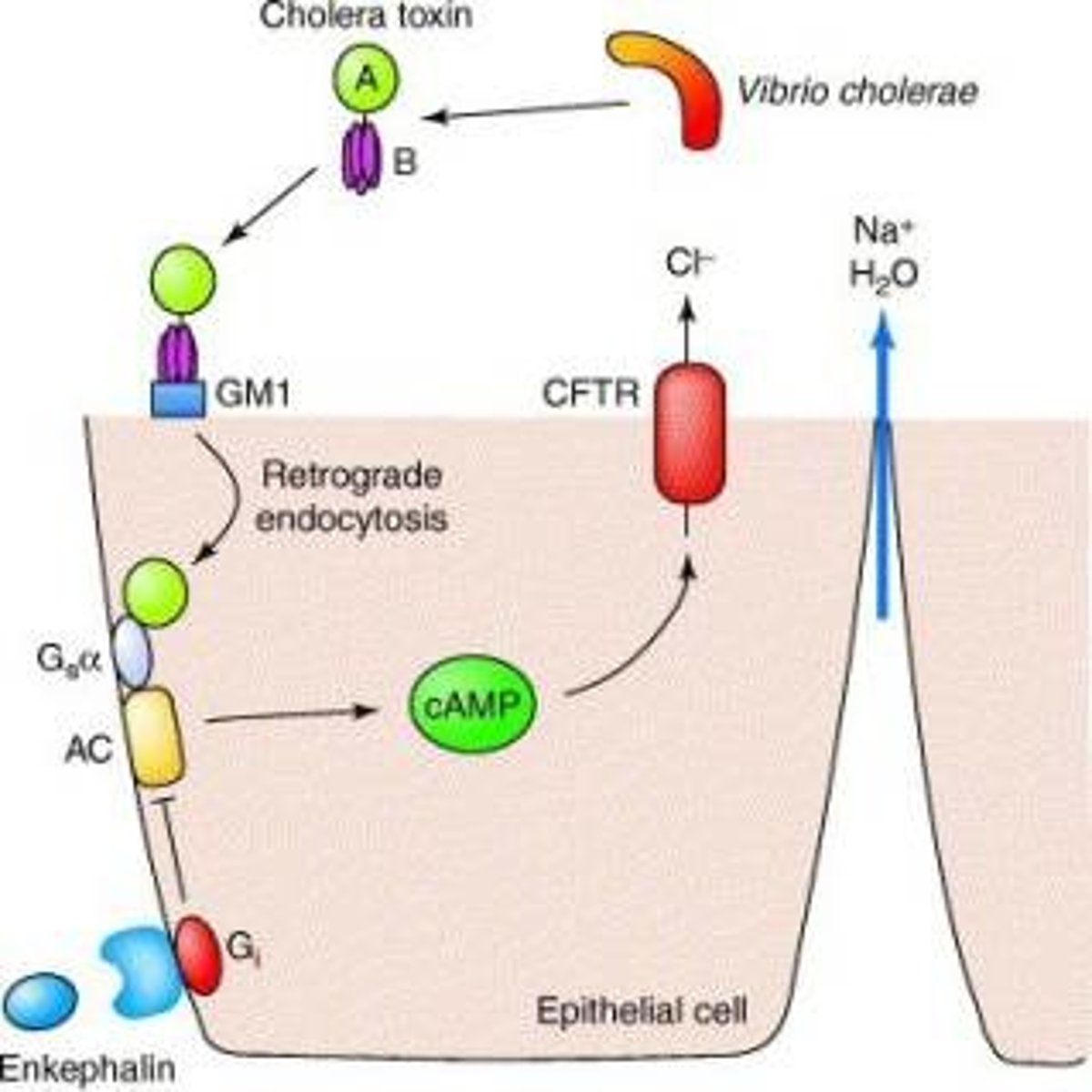
cytotoxin
exotoxin that disrupts the structure of individual cells.
vibrio cholerae (cholera) triggers electrolytes to leave cell & water follows causing diarrhea and dehydration.
poly peptide A enters cell, B interacts with surface.
infection
successful invasion of body by microorganisms
intoxcation
ingest toxin.
shorter incubation period, no immune response, no microorganism
cytopathic effect
structural changes in host seen with light microscope
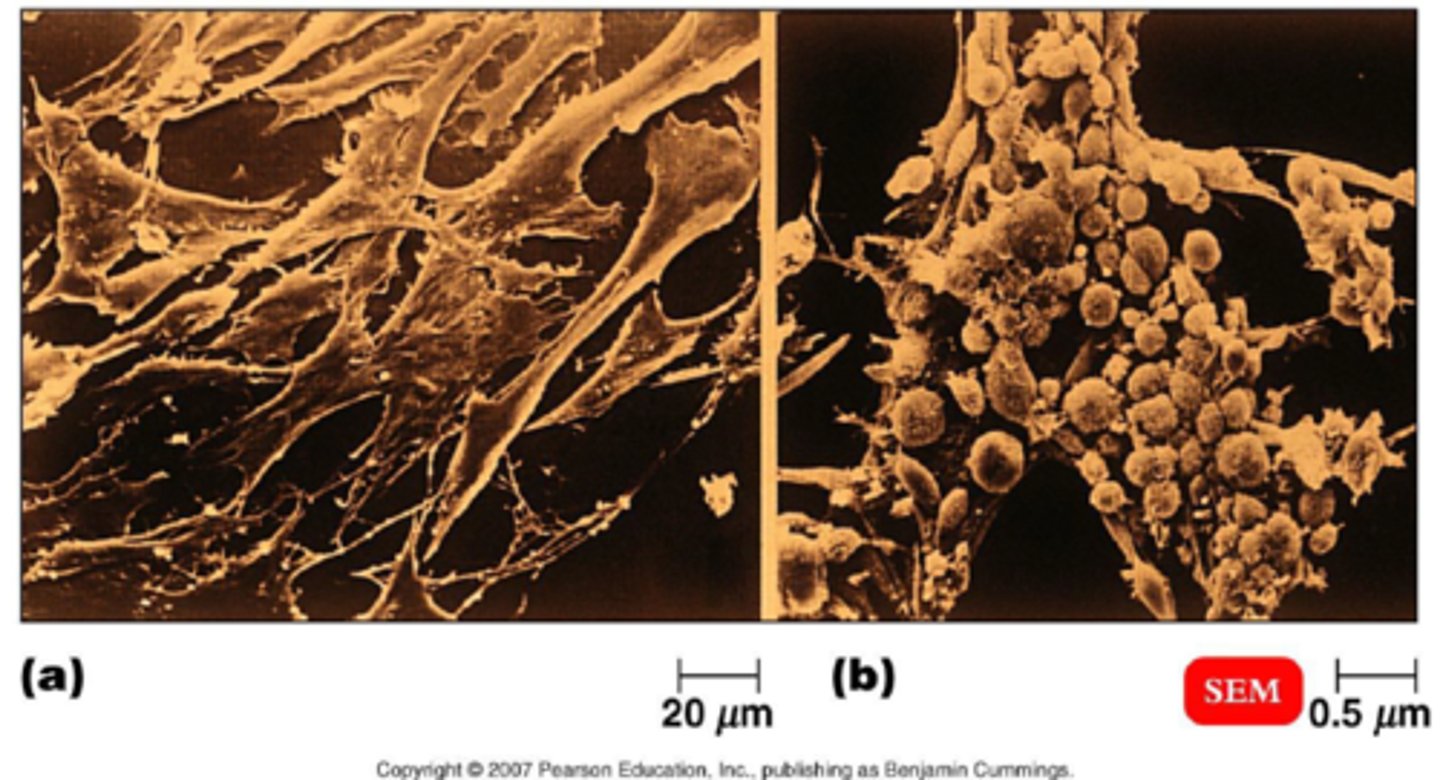
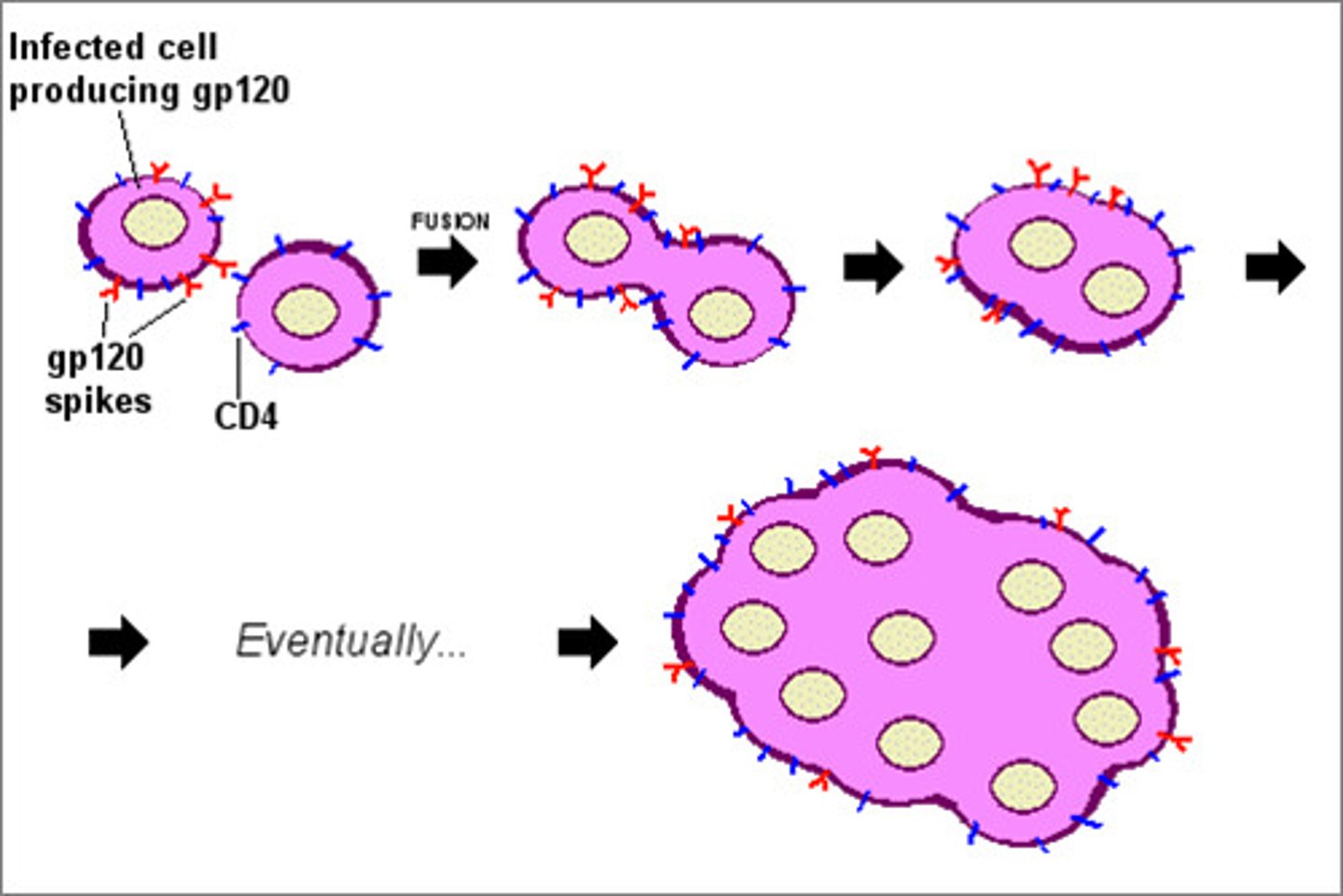
syncytia formation CPE
fusing of cells
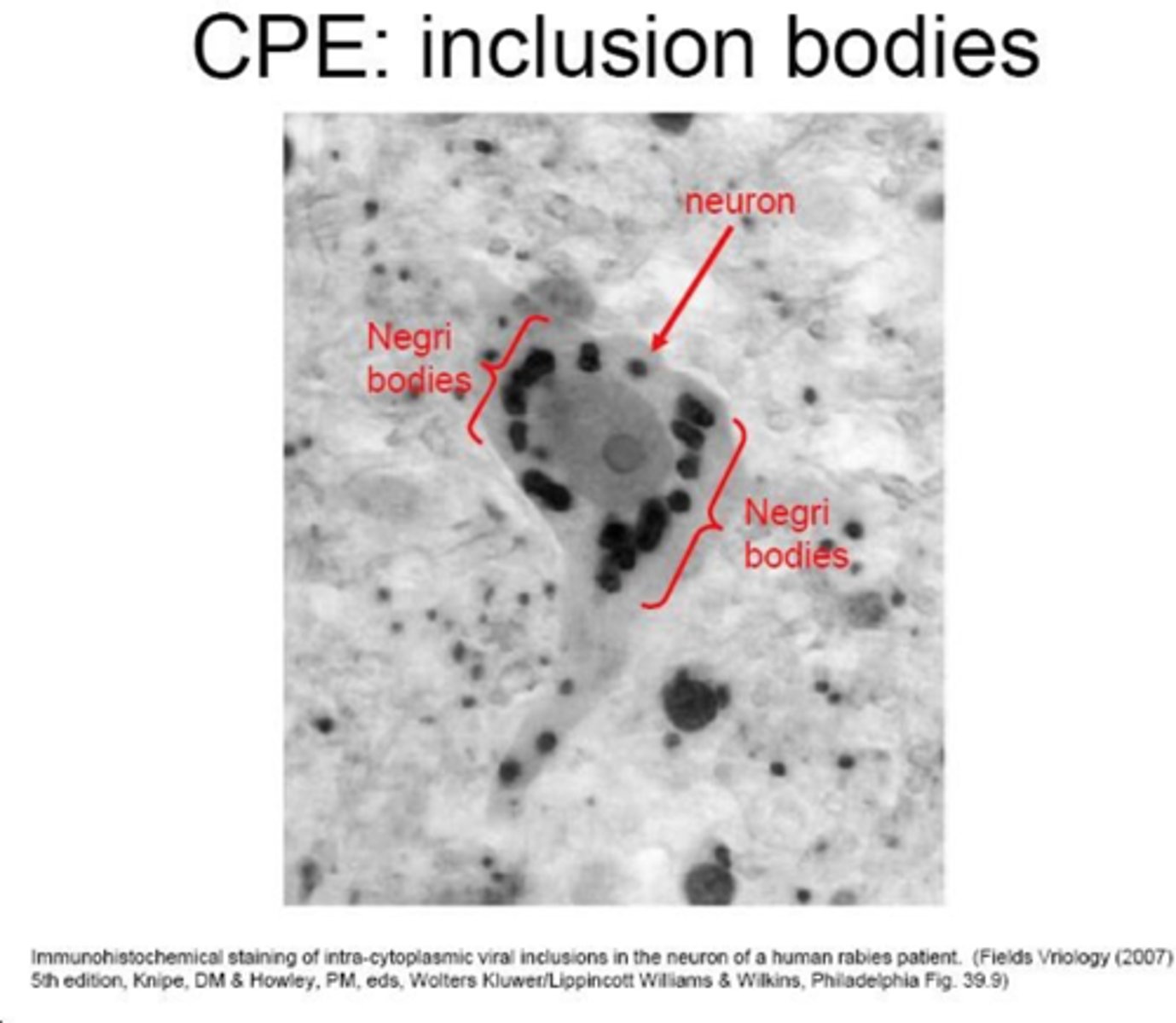
inclusion bodies CPE
structure in infected cells, sites of viral assembly
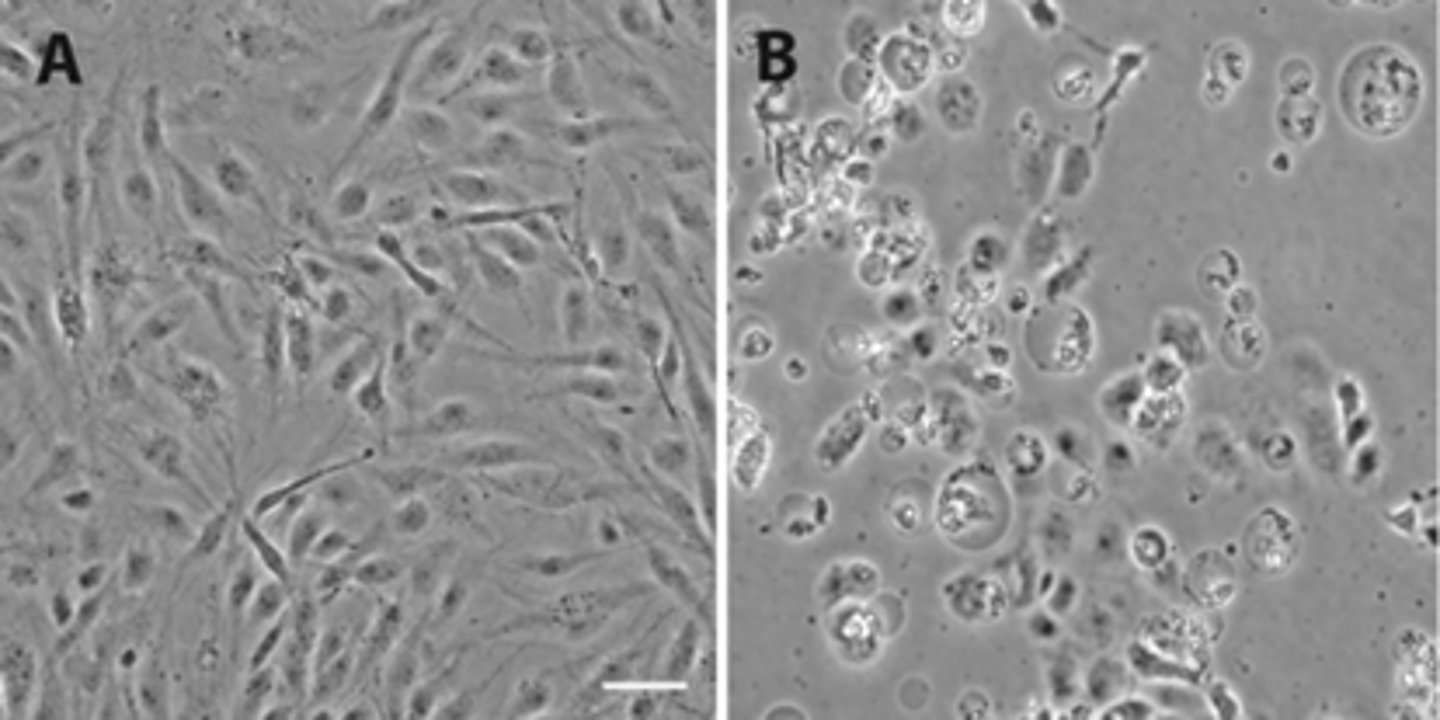
rounding up and lysis CPE
infected cells bunch up and lyse when virus leaves the cell
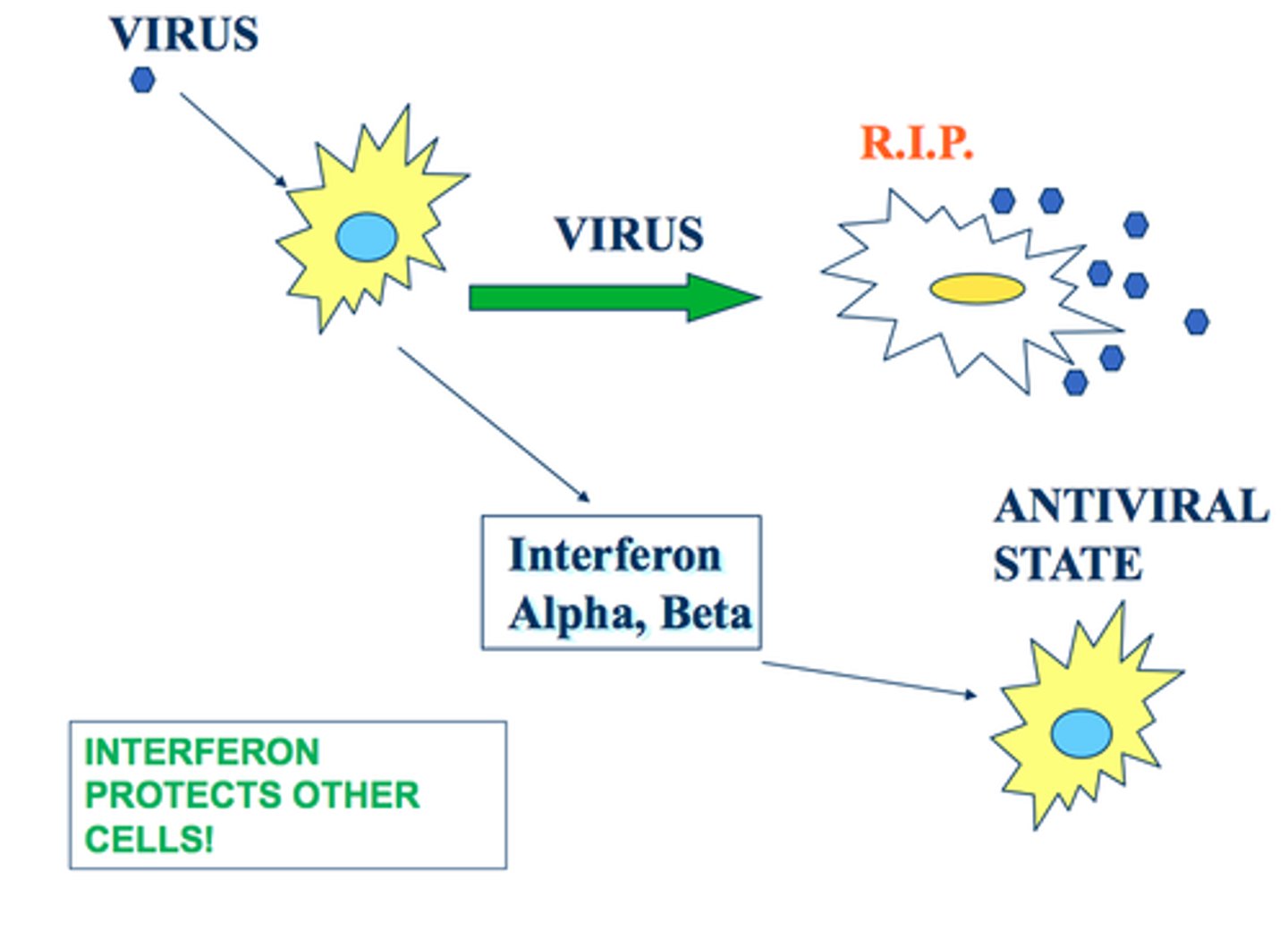
interferon
protein produced by infected cells to limit spread of infection by blocking biosynthesis
antigenic change
MHC-I receptor peptide is replaced with viral peptide triggering immune response
co-evolution
viruses overtime evolves to infect host, as host evolves to resist virus infection

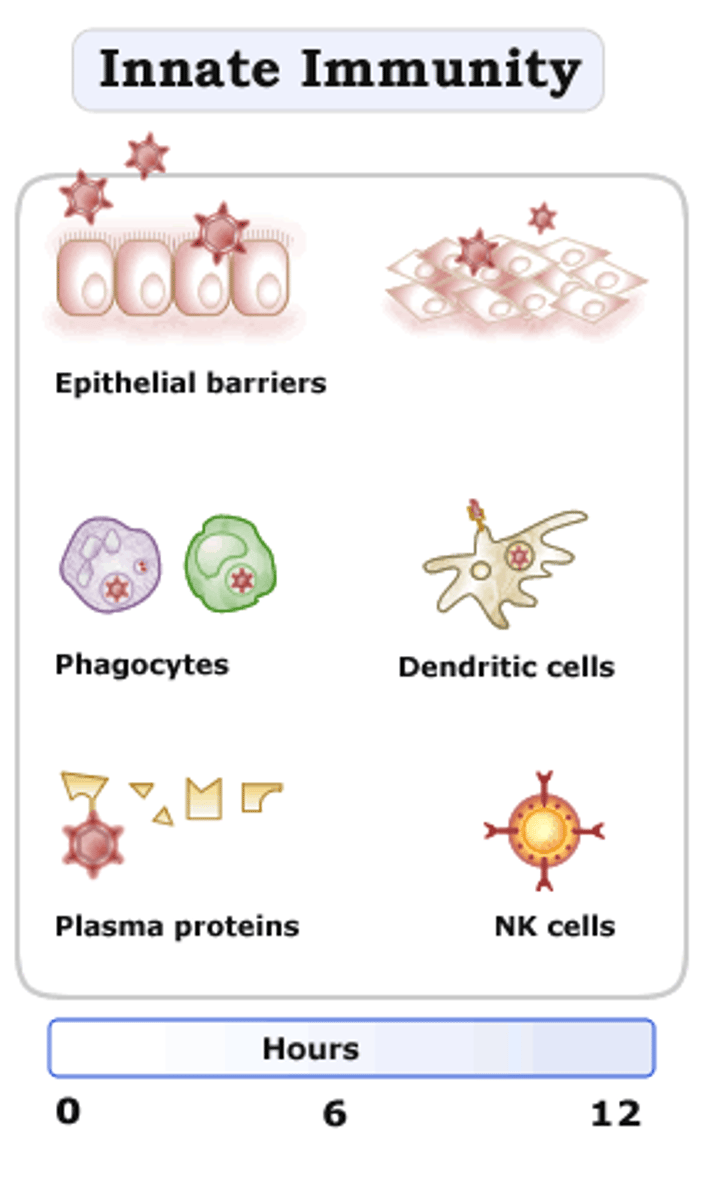
innate immunity
present since birth, response is always the same.
no memory.
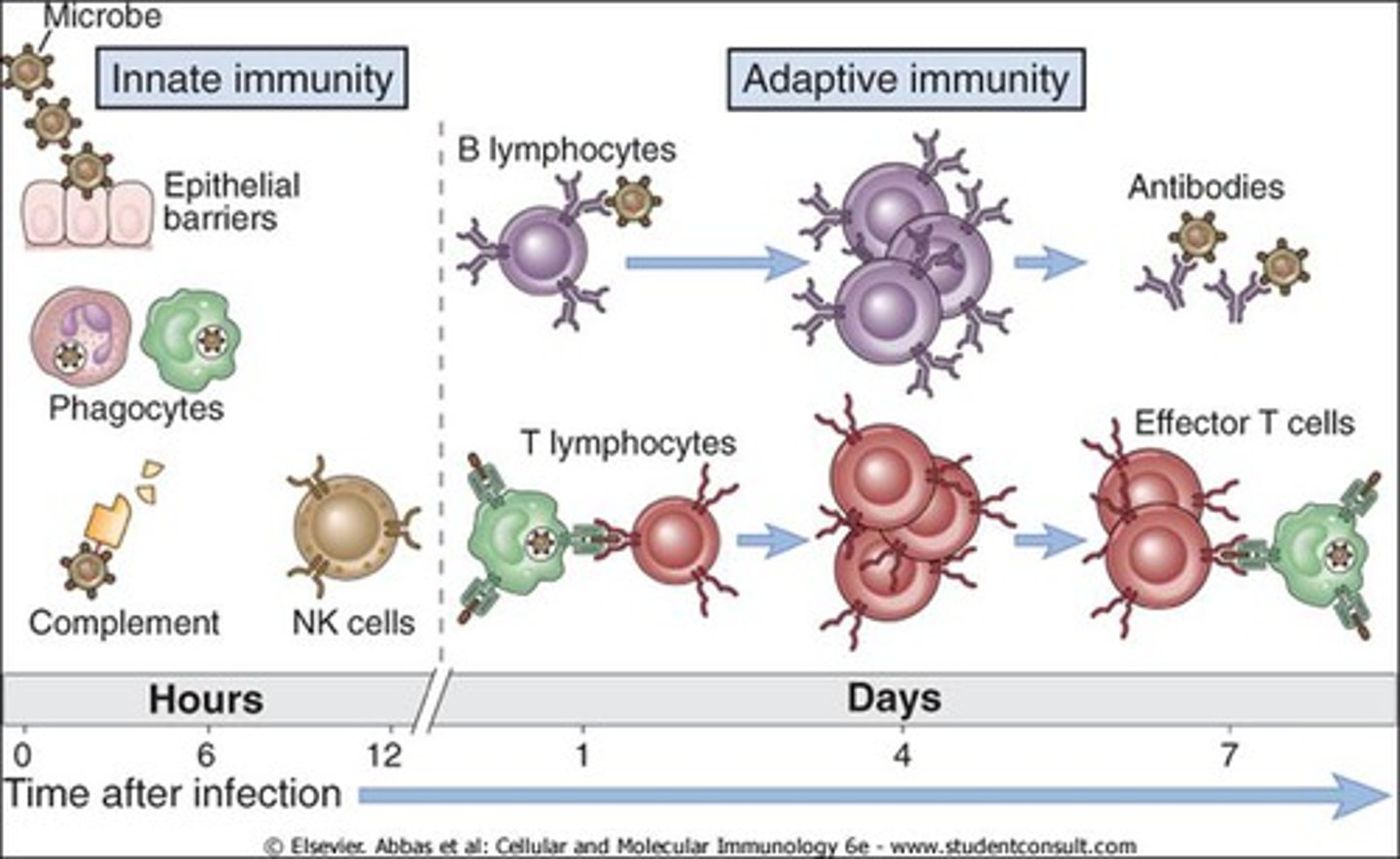
adaptive immunity
acquired over time, built.
stronger response after exposure, memory of pathogen.
mast & basophil cells
granulated, respond to inflammation
neutrophils, eosinophils, macrophages
phagocytes that fight infection and remove pathogens

dendritic cells
trigger adaptive response by collecting info for T and B cells
B cells
produce antibodies
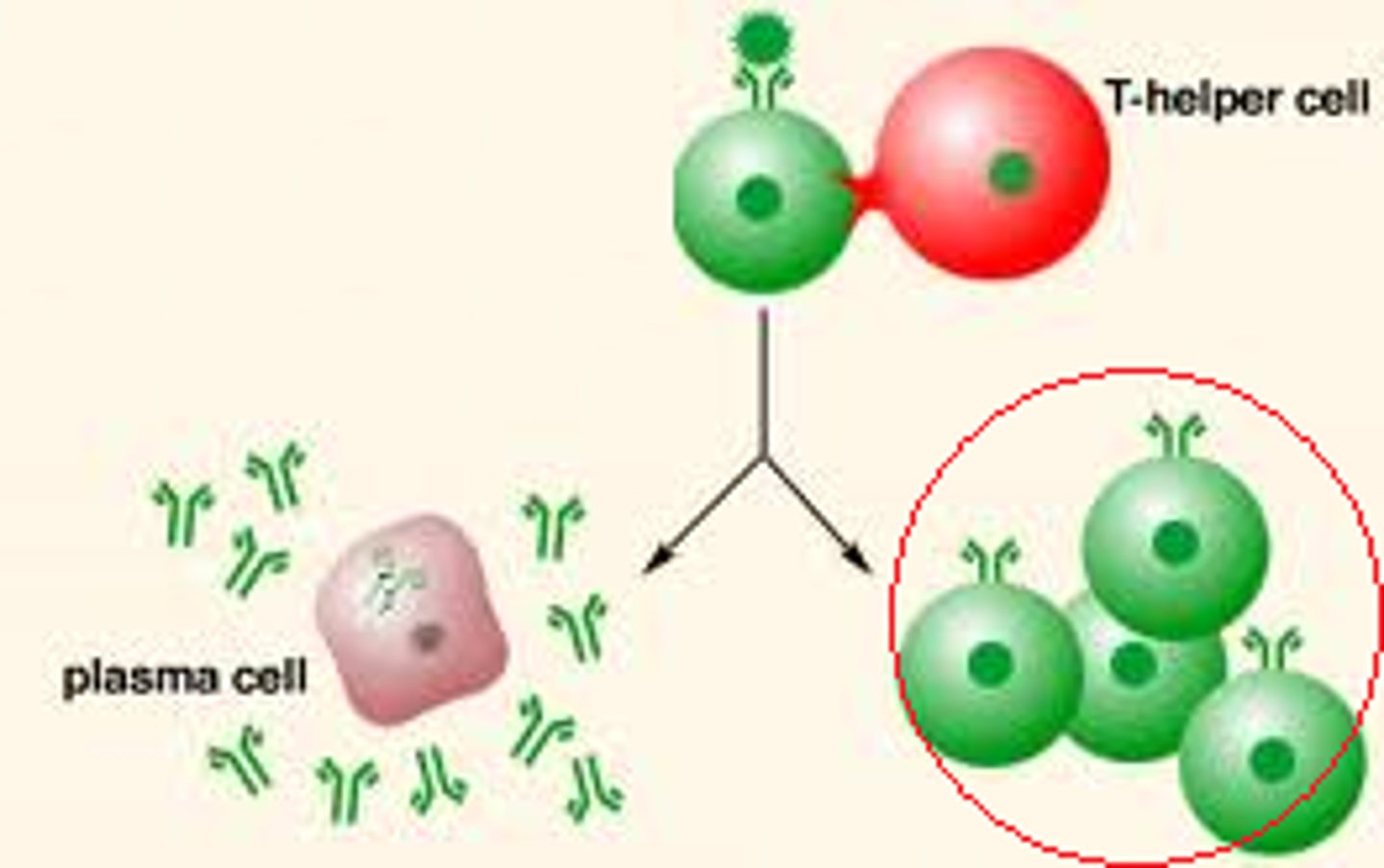
T cells
helper: adaptive response
cytotoxin: kill cells
natural killer cells (NK)
pathogen must be brought to cell,
kill without antigen-antibody interaction
opsonization
coating antigen with antibody to enhance phagocytosis ingestion
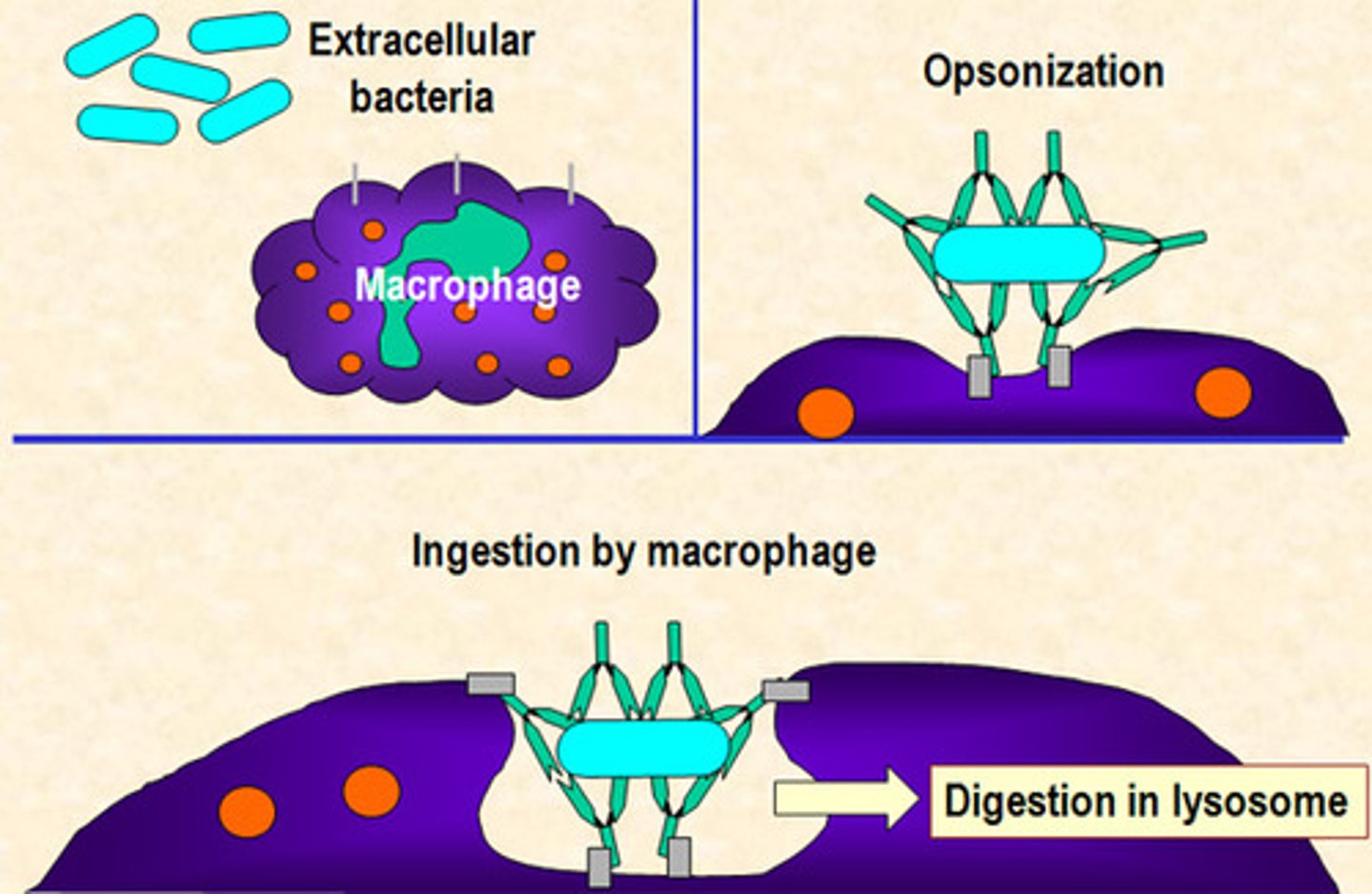
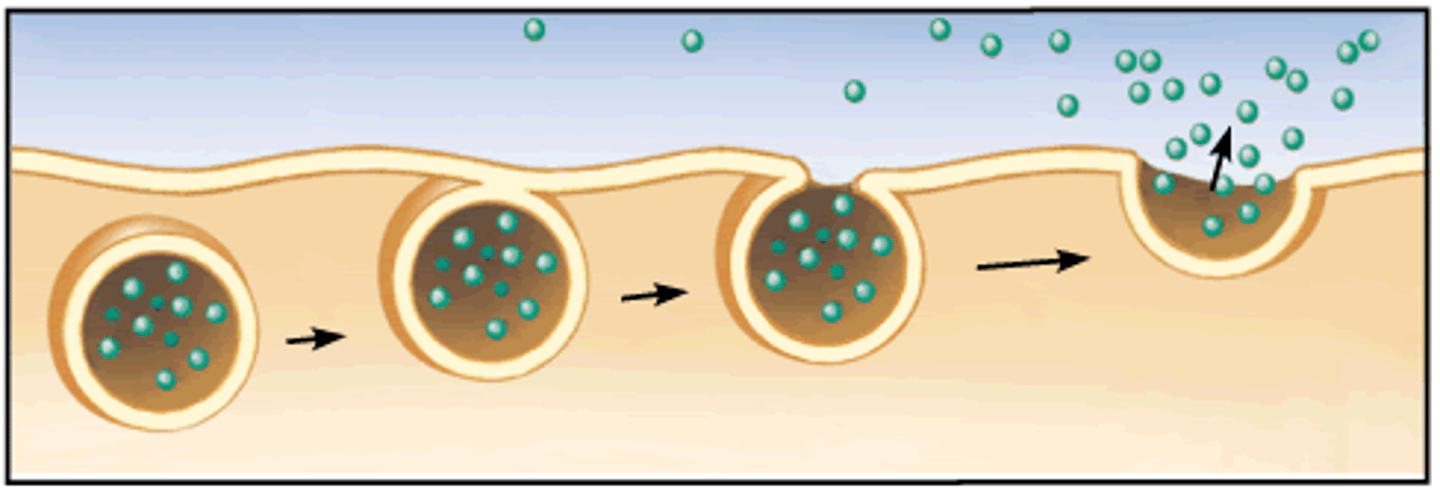
phagocytosis
1. chemotaxis
2. adherence
3. ingestion
4. fusion
5. digestion
6. exocytosis
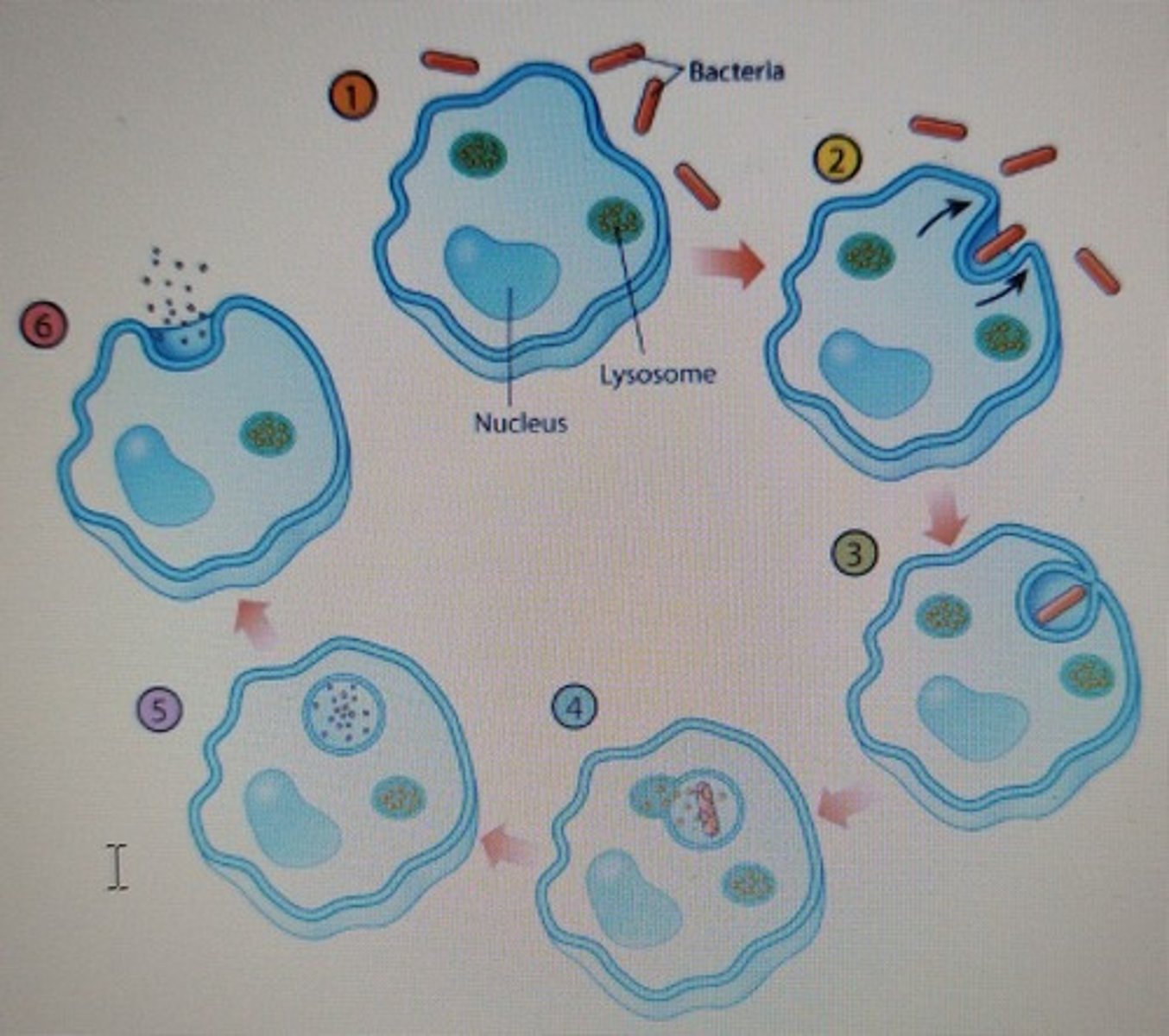
1. chemotaxis
chemical signals attract microorganisms to phagocyte
2. adherence
pattern recognition receptors (PRR) recognize structures on pathogens to trigger ingestion
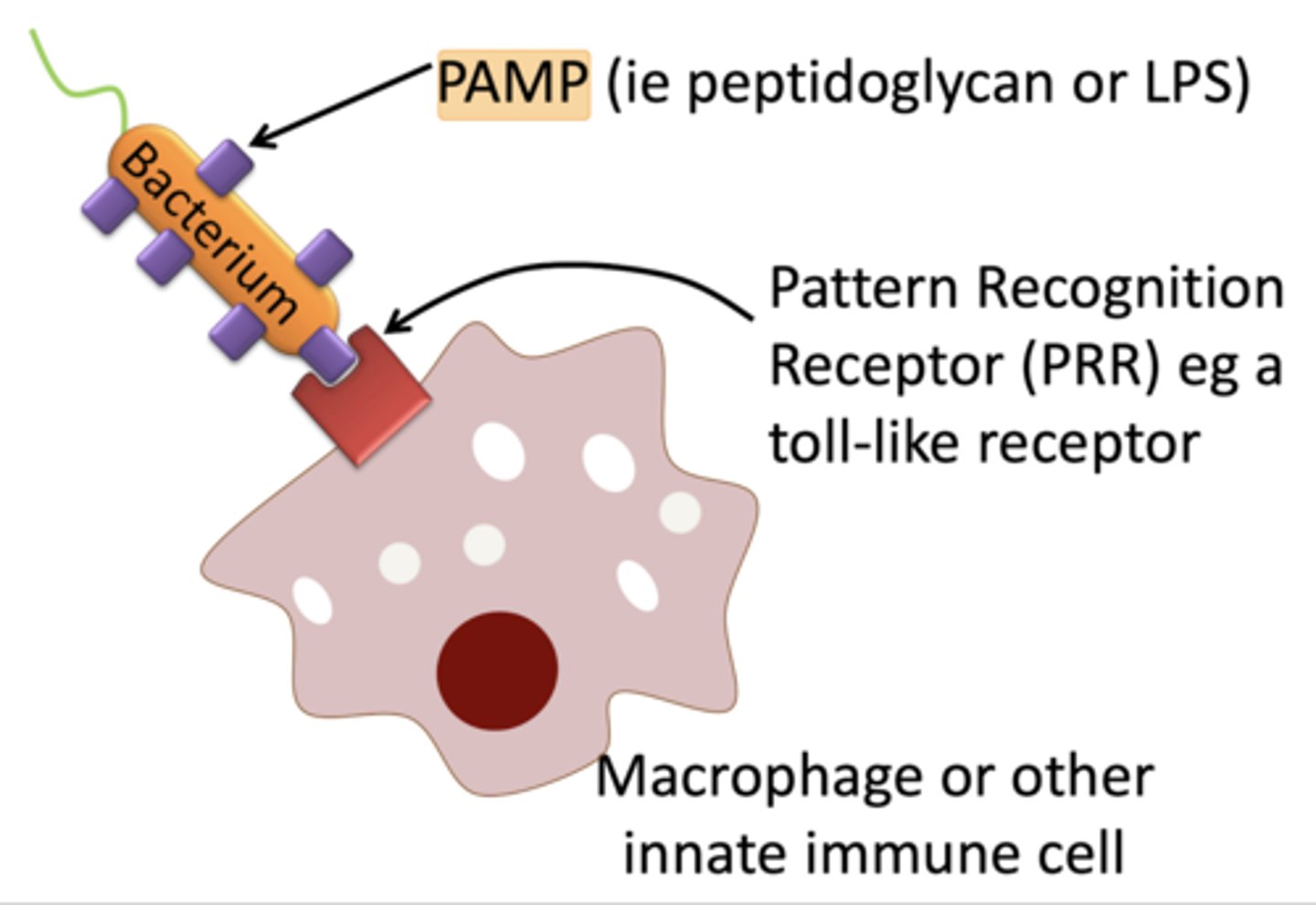
3. ingestion
pseudopods (plasma membrane extensions) engulf microorganism, bringing it inside the cell.
opsonins make ingestion easier!
4. fusion
lysosome fuses with phagosome containing the pathogen
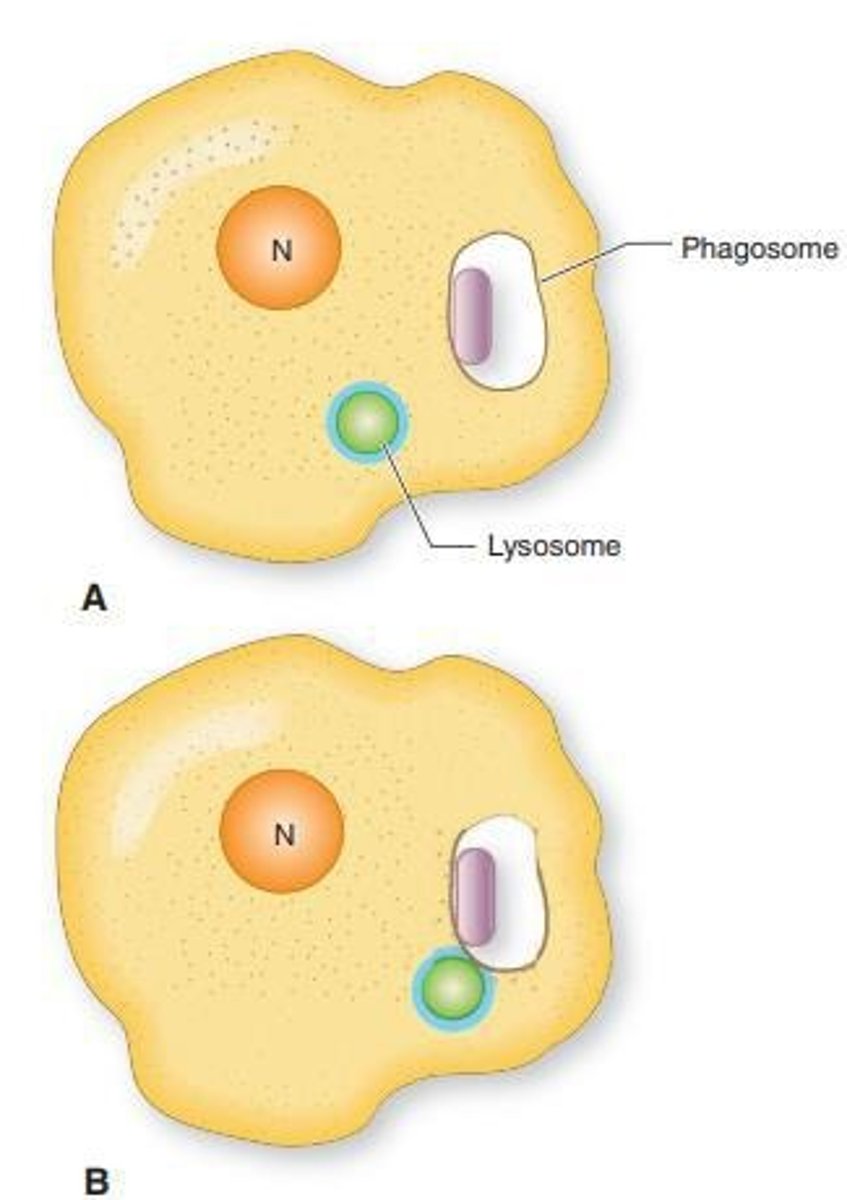
5. digestion
microbes are killed
6. exocytosis
expel remains
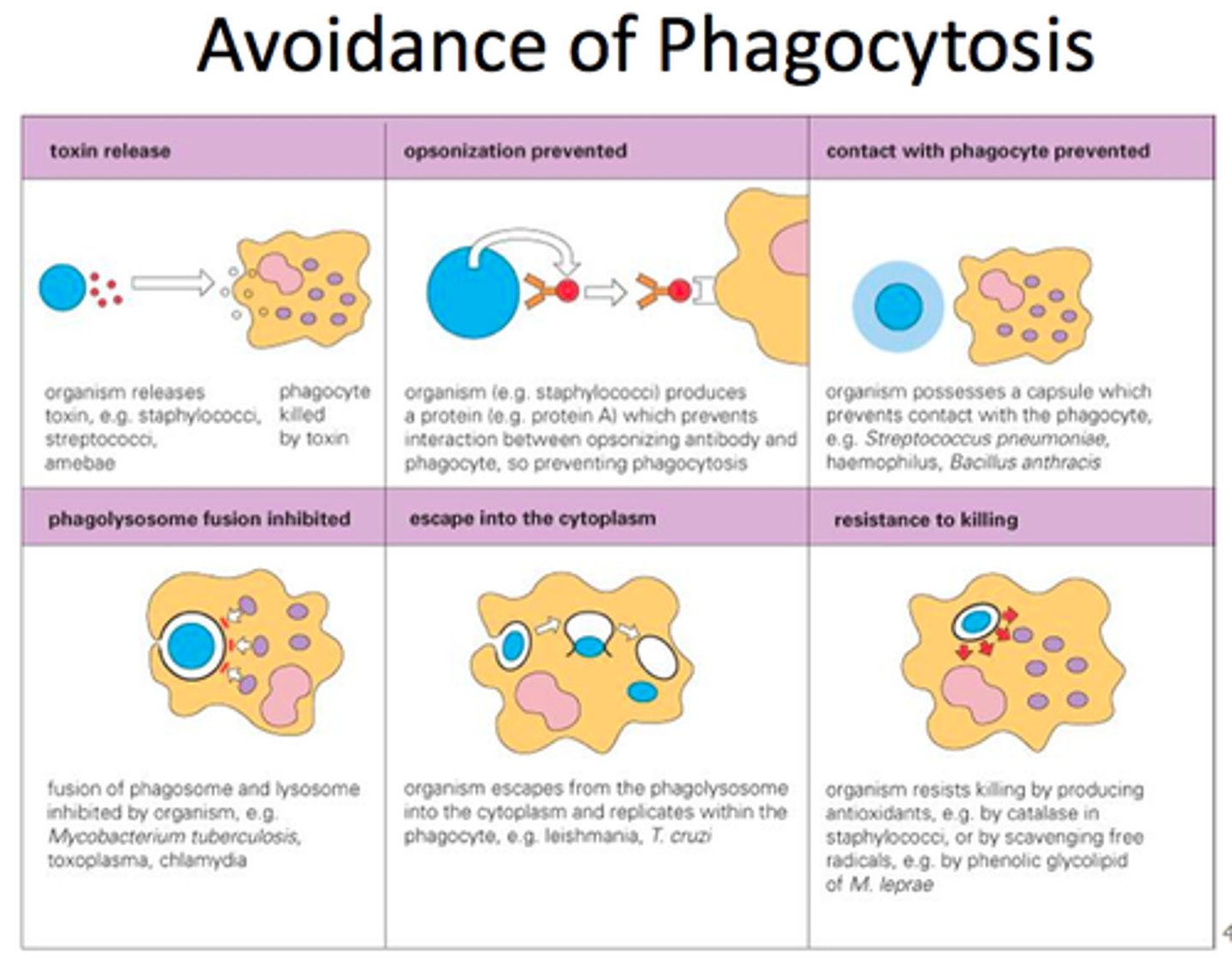
mechanisms of avoiding phagocytosis
coagulase forms fibrin coat around bacteria to avoid adherence.
capsules avoid ingestion.
leishmania avoid digestion by blocking acidification.
TB mycobacteria avoid fusion.
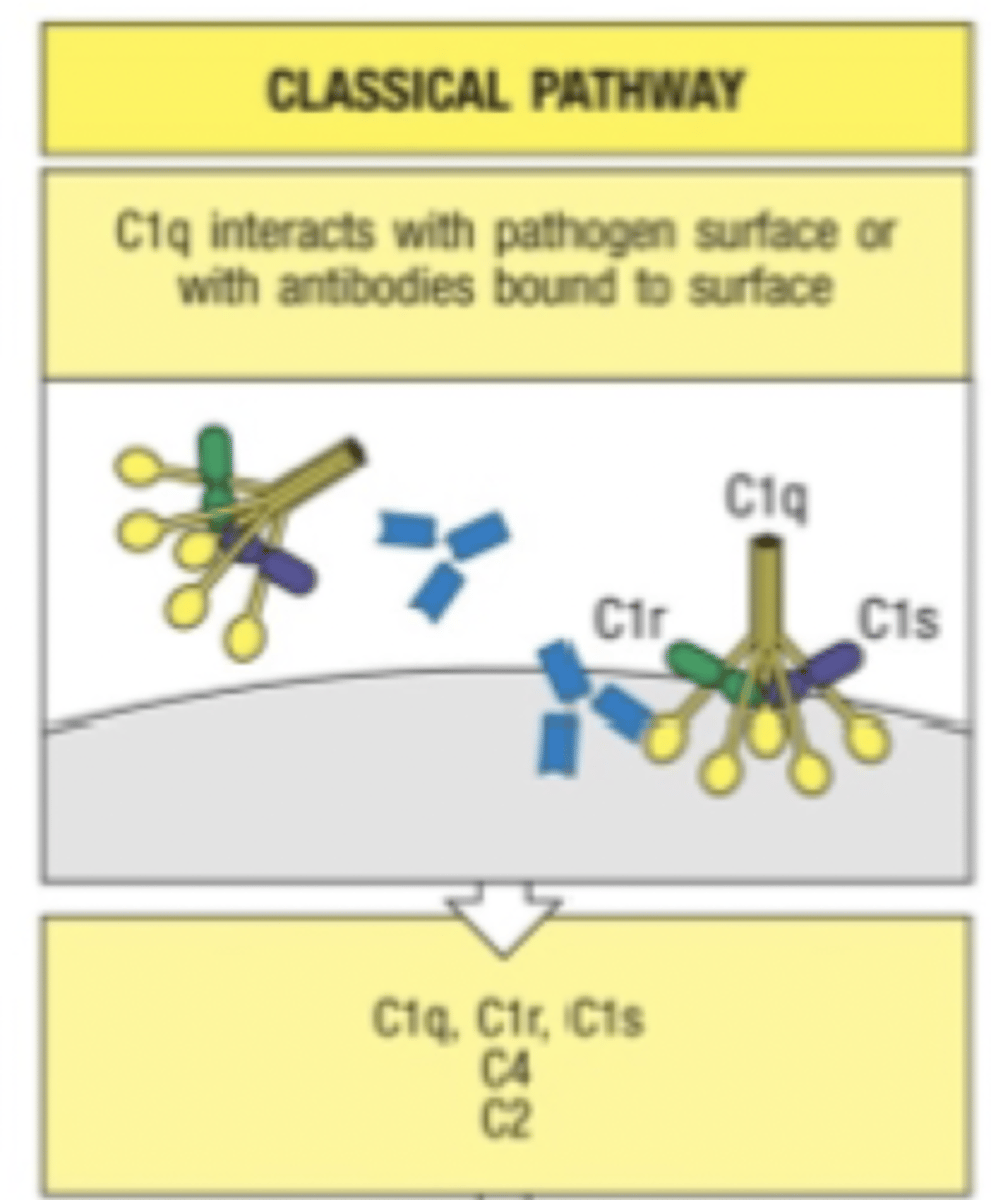
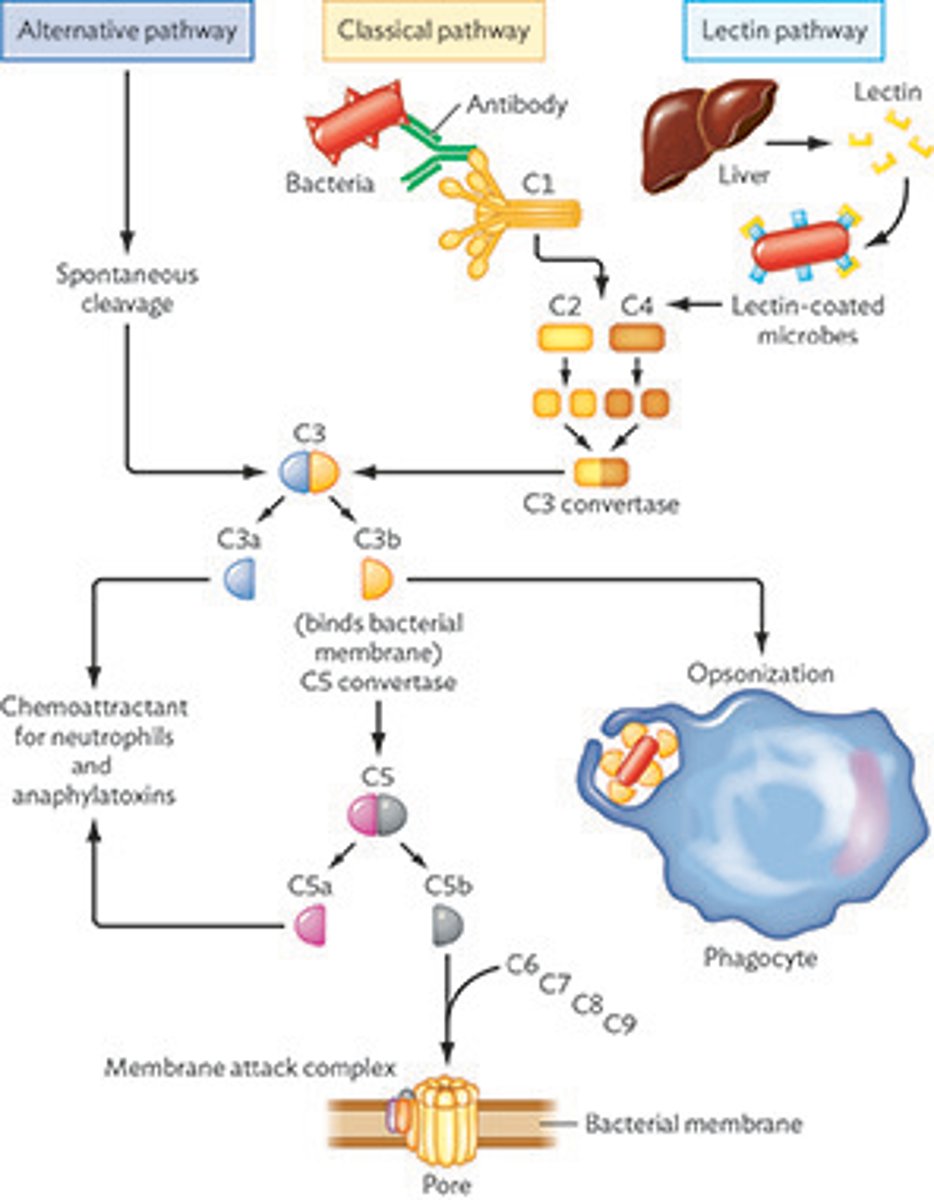
compliment activation pathways
alternative, classical, lectin
classical compliment
antibodies bind to surface of foreign cell for lysis.
C1 binds to antibodies, C3 cleaves to C3A & C3B
C3A
triggers inflammation
C3B
works with other compliment proteins to cleave C5 into C5A & C5B
C5A
triggers inflammation
C5B
joins compliment proteins to "punch holes in the pathogen" to lyse the cell
alternative and lectin pathways
do not use antibodies.
all pathways use C3 and end in either opsonization, inflammation, or cytolysis
inflammation
innate acute response triggered by tissue damage.
damaged cells release inflammatory mediators to trigger increased blood flow and permeability of blood vessels so microorganisms can be taken care of
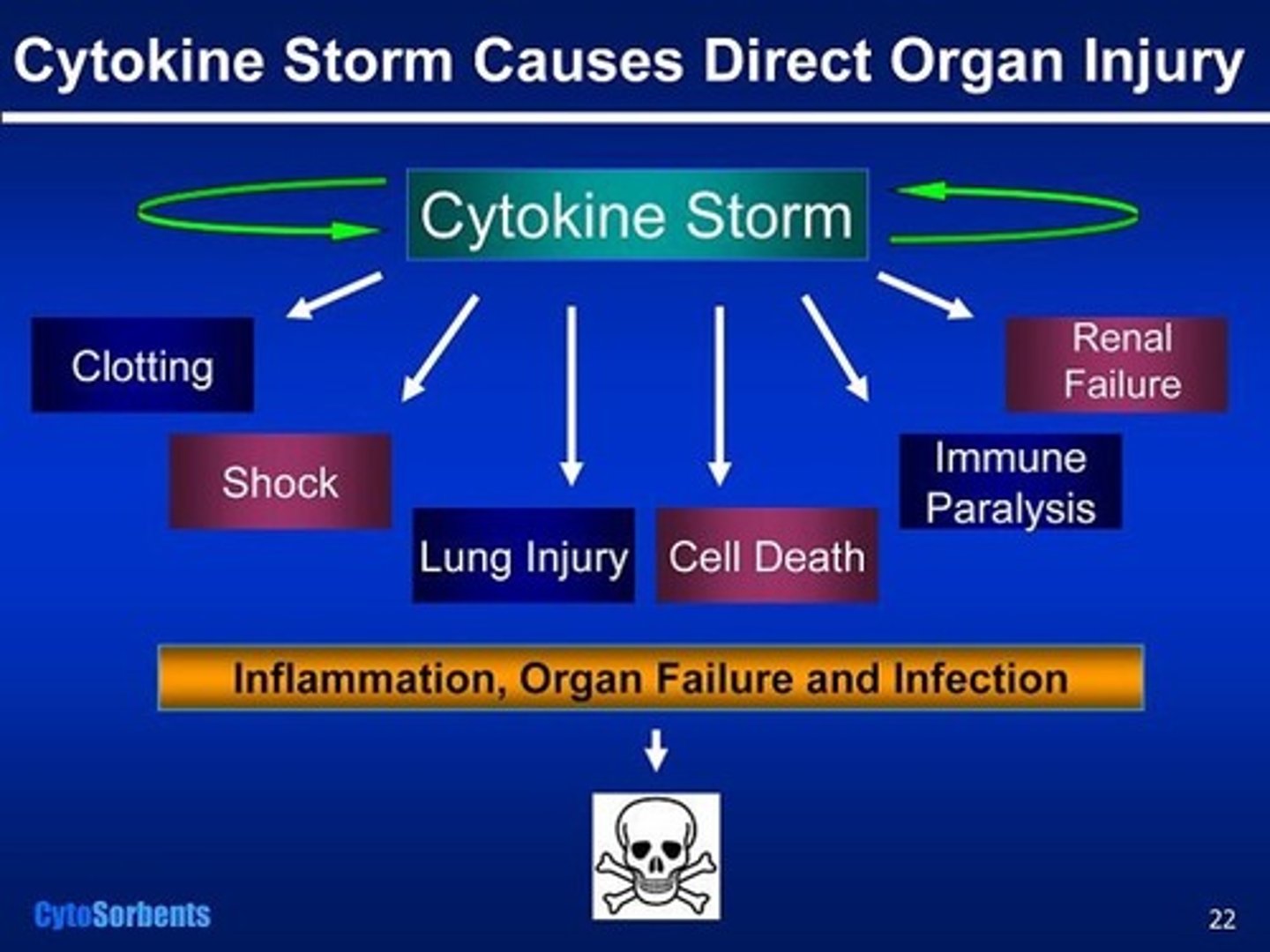
cytokine storm
maladaptive inflammatory response that activates cytotoxic T cells, damaging tissues and leading to bleeding out. unregulated inflammation.
interferon production
limits the spread of viruses.
innate response.
interferon type I
alpha - viral infections
betta - triggers production of IL-10
IL-10
suppresses adaptive response (T cells)
interferon type II
intracellular pathogens trigger gamma
fever
hypothalamus raises body temp to allow enzymes to work better.
innate response.
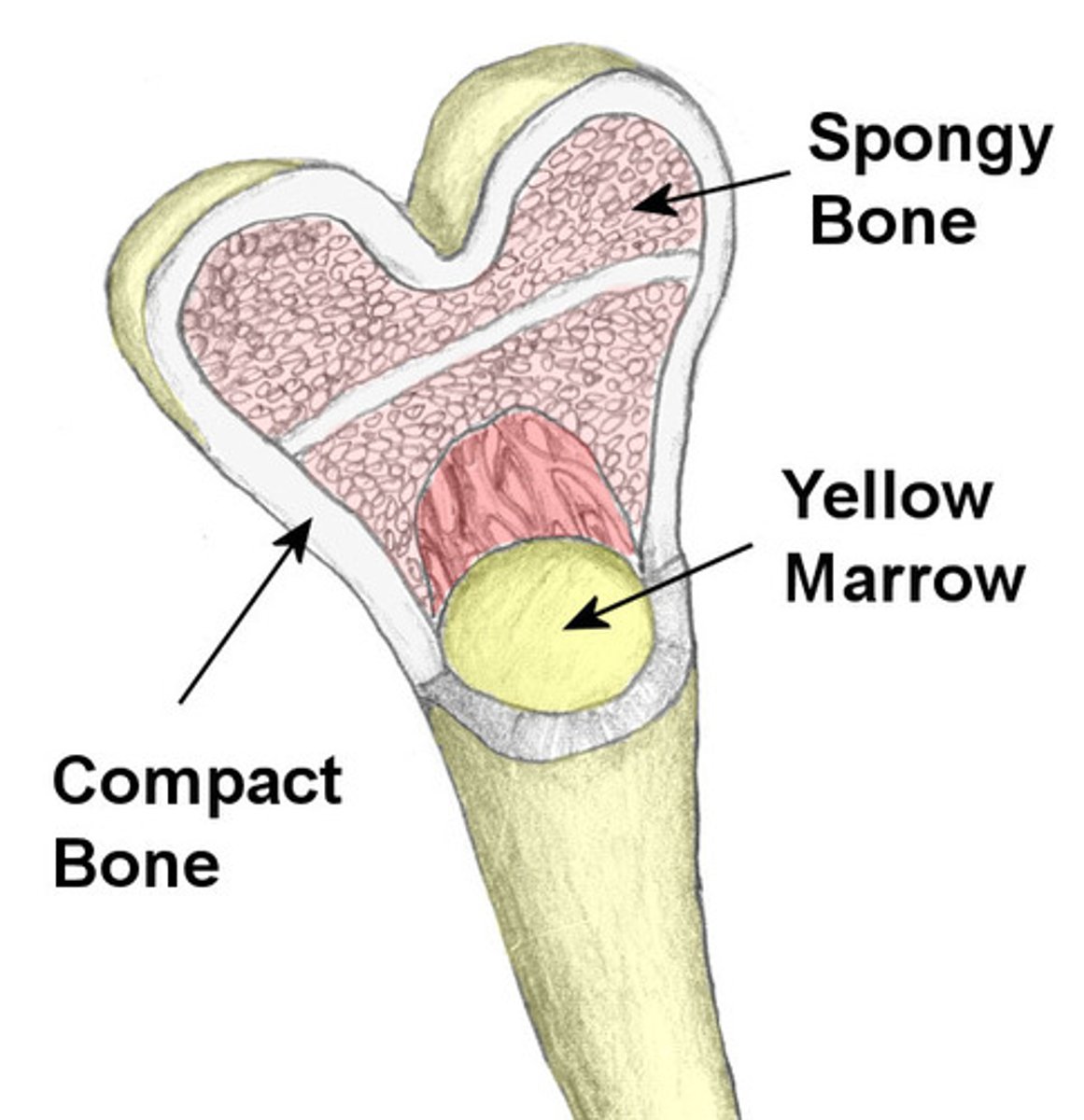
bone marrow
all cells start in bone marrow as T cells and B cells.
B cells mature in bone marrow.
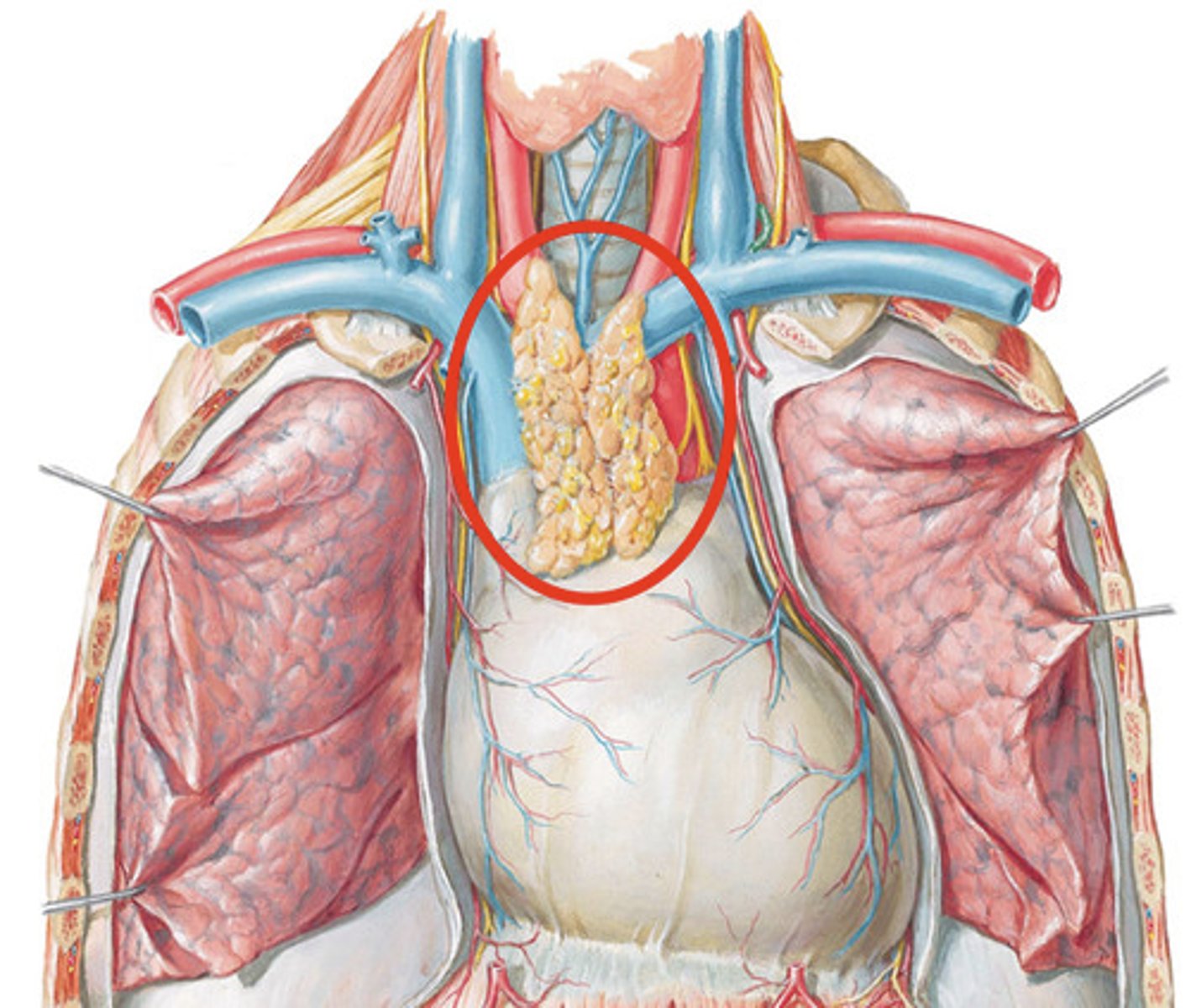
thymus
T cells mature in thymus
lymph nodes & spleen
mature T cells and B cells in lymph nodes that wait to be activated
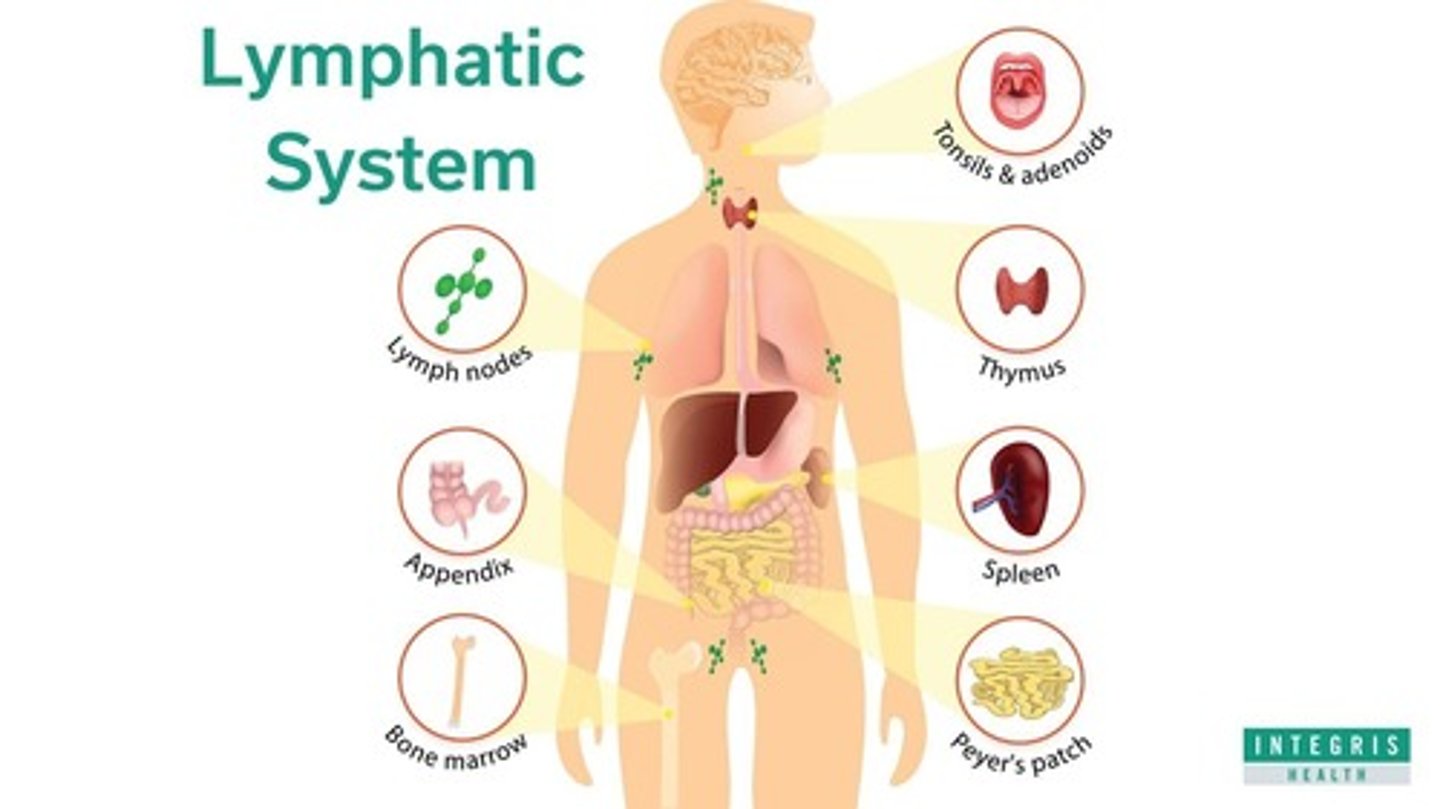
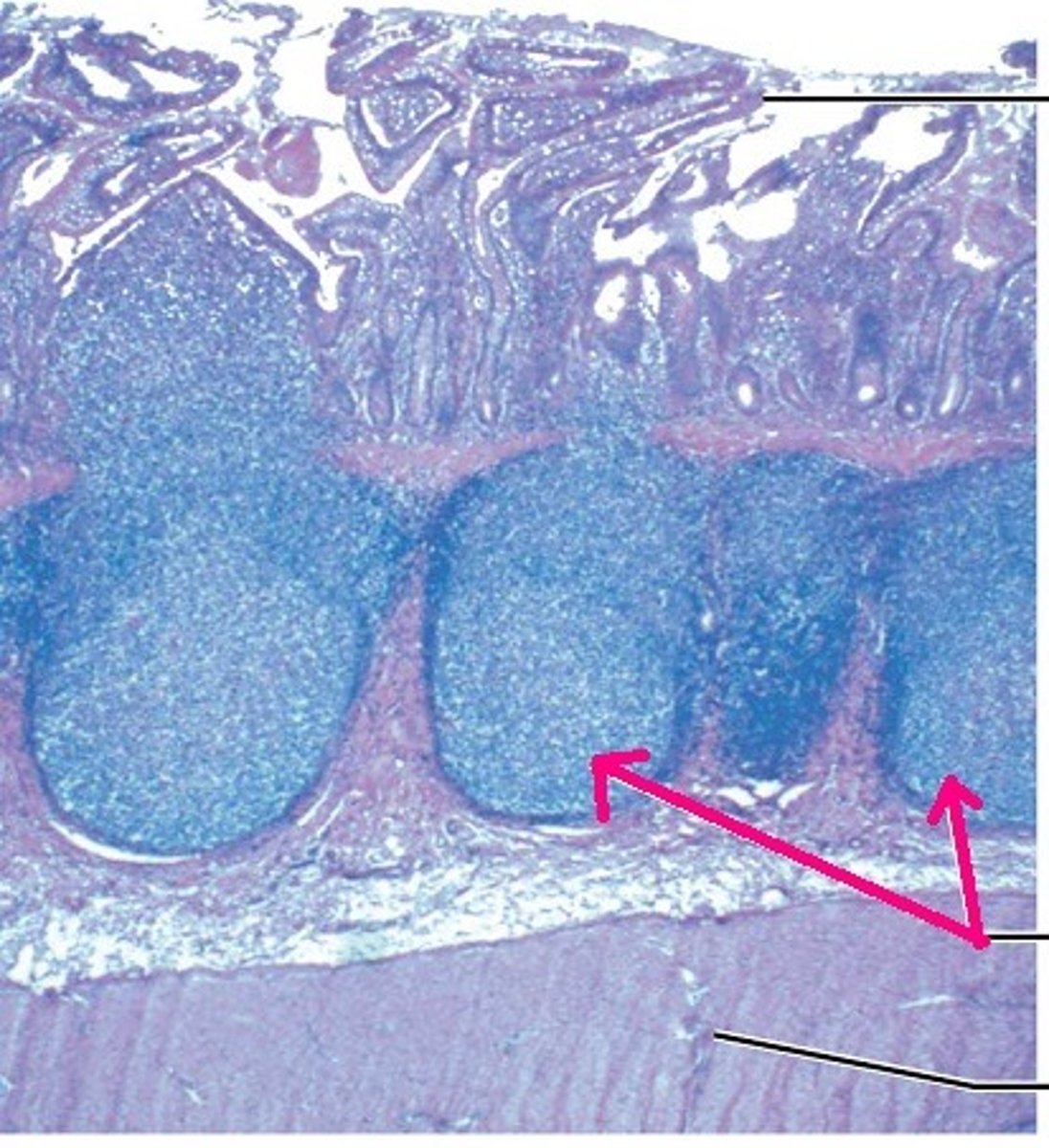
mucosa-associated lymphoid tissue (MALT)
peyer's patches: cells in intestine that produce antibodies
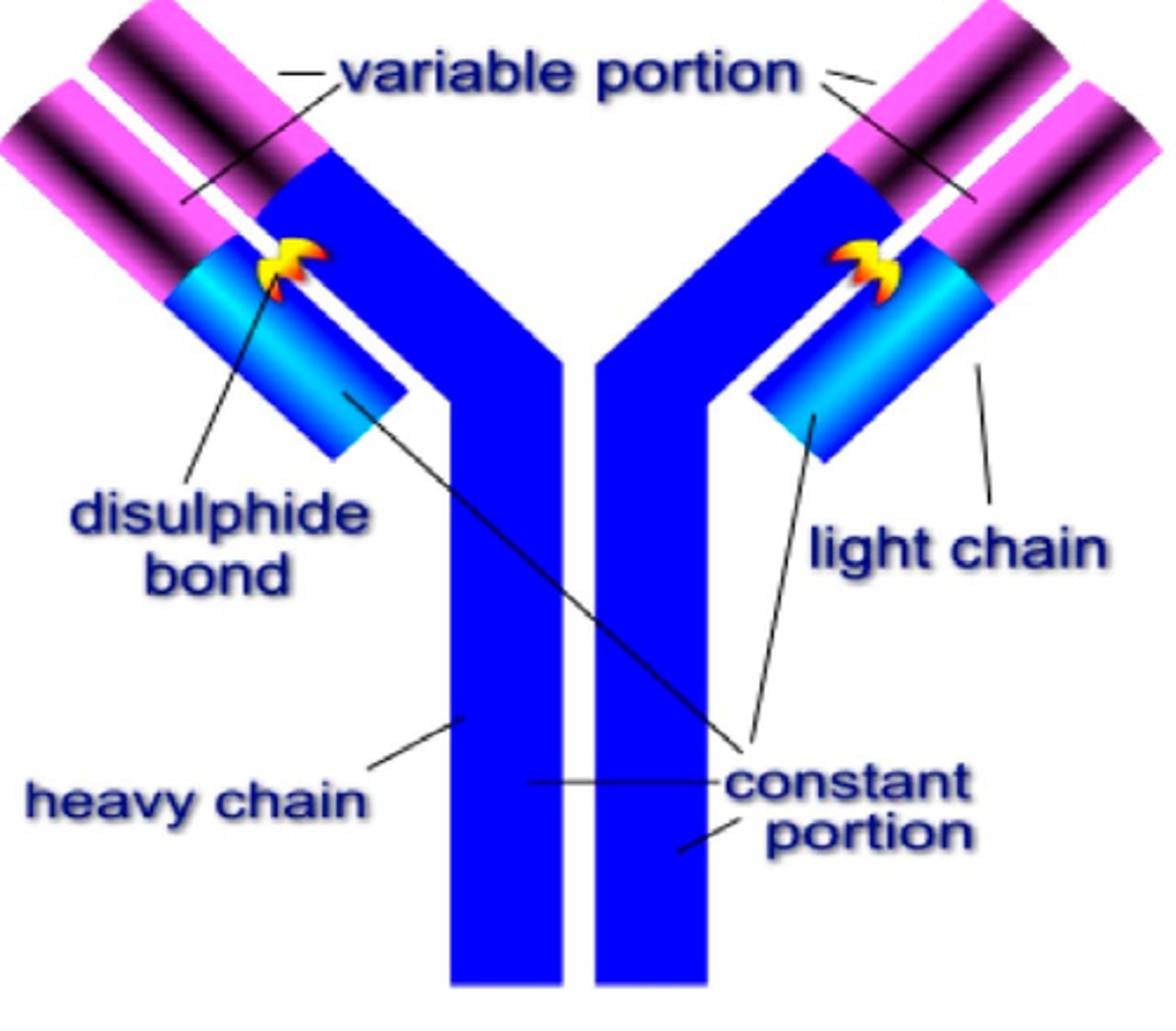
antibody structure
variable region at the end of light chains connected to a constant region heavy chain.
Fc region in constant region of light chains.
Fab region (antigen binding) at end of light chains.
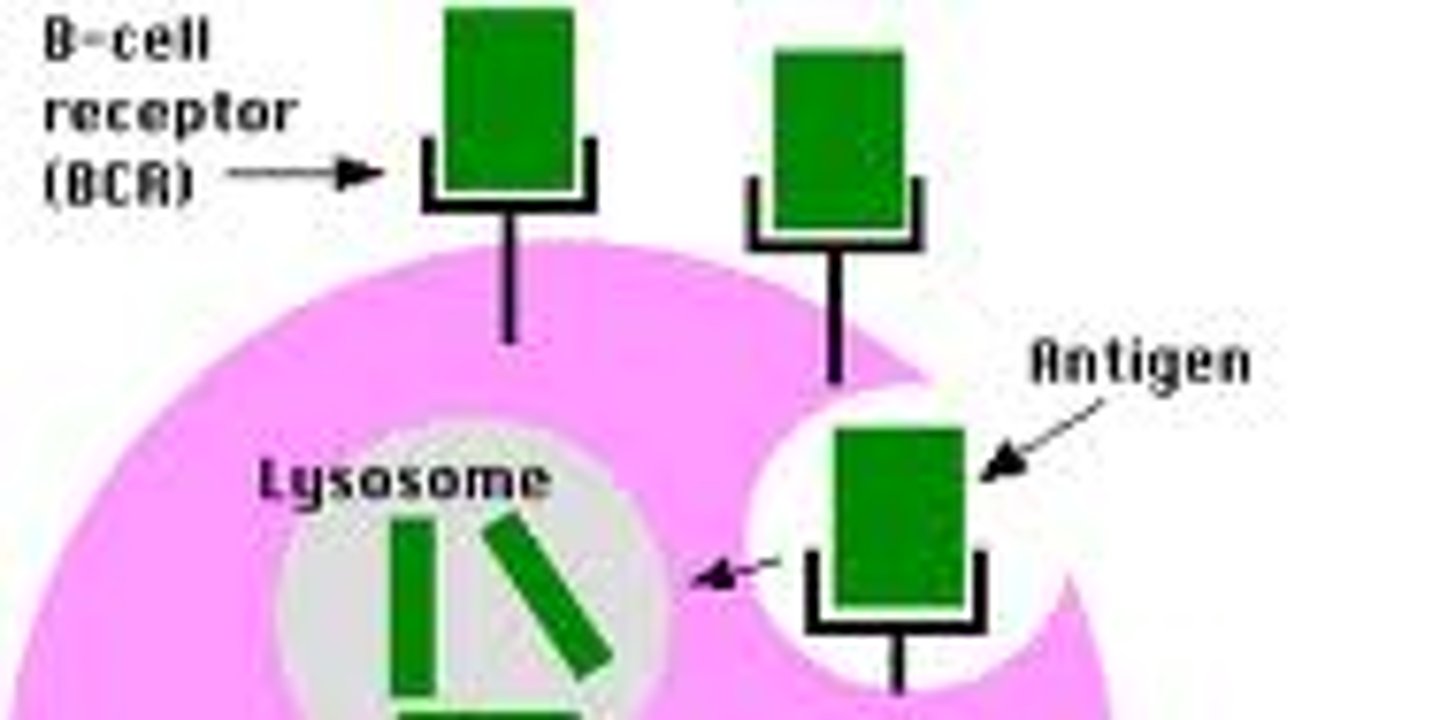
antigen
protein or large polysaccharide that triggers antibody response
epitope
site on antigen where antibody binds. can be multiple per antigen
antibody diversity
DNA segments are rearranged during genetic recombination