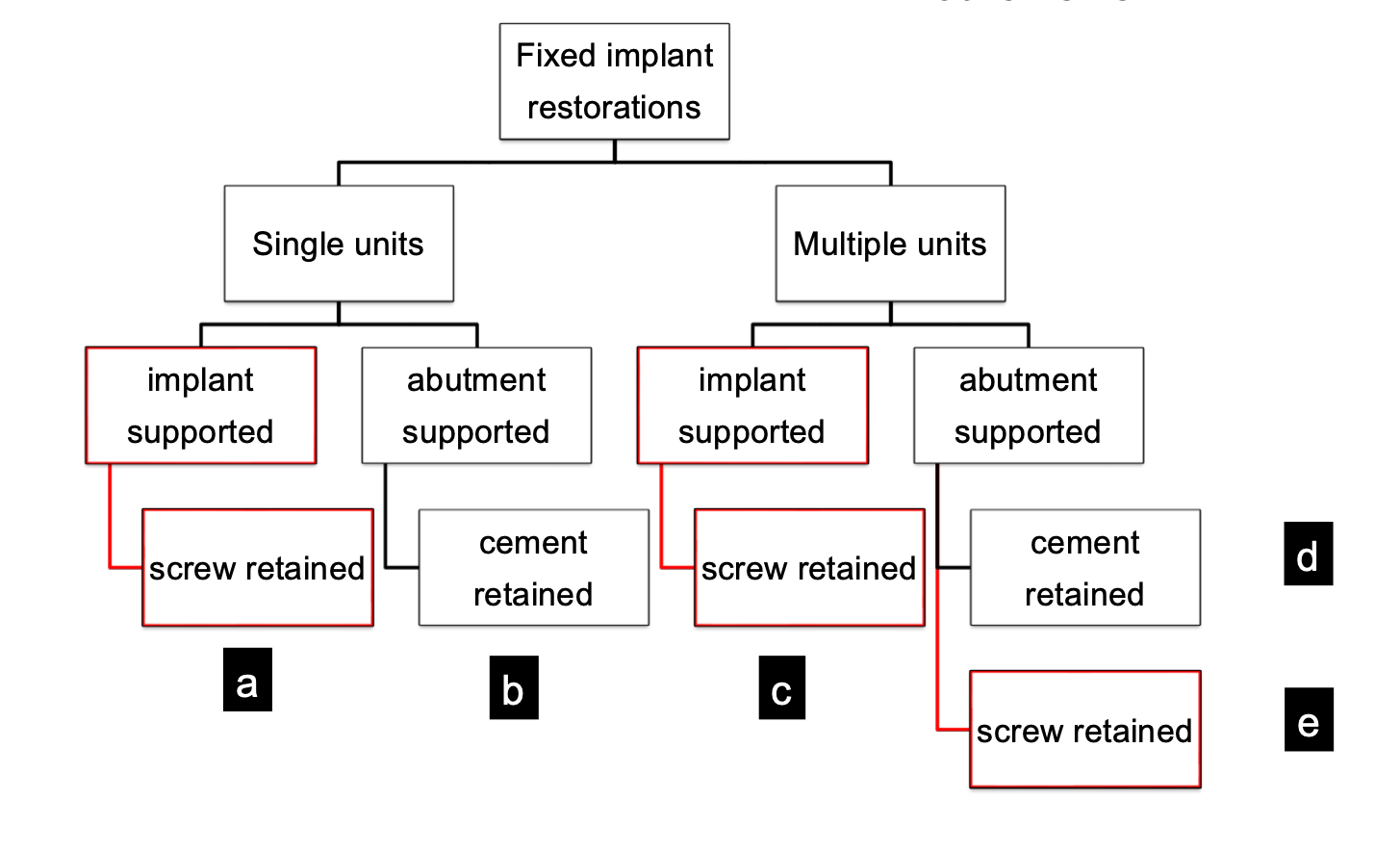
3-4. adapted from quizlet ryanef123: 5 - Implant-Supported Fixed Restorations Part 1 & 2 (Dr. Muftu)
1/178
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
179 Terms
What are four treatment options for single tooth replacement?
No treatment
Removable partial denture
Fixed partial denture (on natural teeth)
Implant crown
What is NOT a treatment option for single tooth replacement?
Tooth-implant supported prostheses (connecting teeth and implants for FPDs)
What are some reasons for selecting a single implant crown over a 3-unit FPD? (!)
Preservation of tooth structure on the teeth adjacent to the edentulous area
Avoiding tooth hypersensitivity that can accompany tooth preparation
Avoiding the potential need for root canal treatment when teeth are prepared for fixed partial denture (11% may require RCT)
Improved access for oral hygiene
Enhanced gingival response
Fewer complications
What is the most common biological complication of a fixed partial denture?
Caries on abutment teeth
What is the most common biological complication of a single implant crown?
Peri-implantitis and soft tissue complications
The survival of three-unit TFDPs and ISCs over 15 years (was/not) statistically different when replacing posterior teeth, but ISCs survived significantly better when replacing (anterior/posterior) teeth.
was NOT, anterior
The complication rates between tooth-supported fixed dental prostheses (TFDPs) and Implant Supported Single Crowns (ISCs) were similar but the economic burden for the TFDPs was (greater/less) (!)
greater
Which is more cost effective, retaining teeth through periodontal care and both initial root canal treatment and root canal retreatment OR tooth extraction and rehabilitation with a single implant?
Retaining teeth through periodontal care
patients consider implant treatment to be (expensive/affordable)?
expensive
T/F: Literature suggest single implants appear to be more cost-effective than fixed partial dentures
True
Success rates increase by 22%
25% total cost savings over 20 years vs 3-unit fixed prosthesis
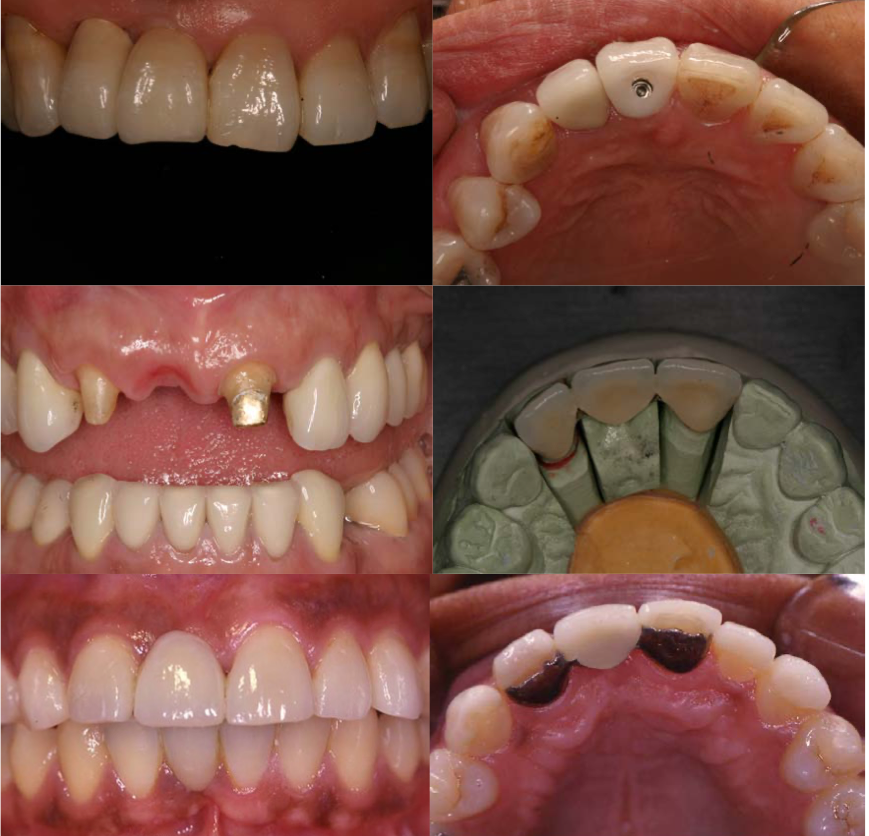
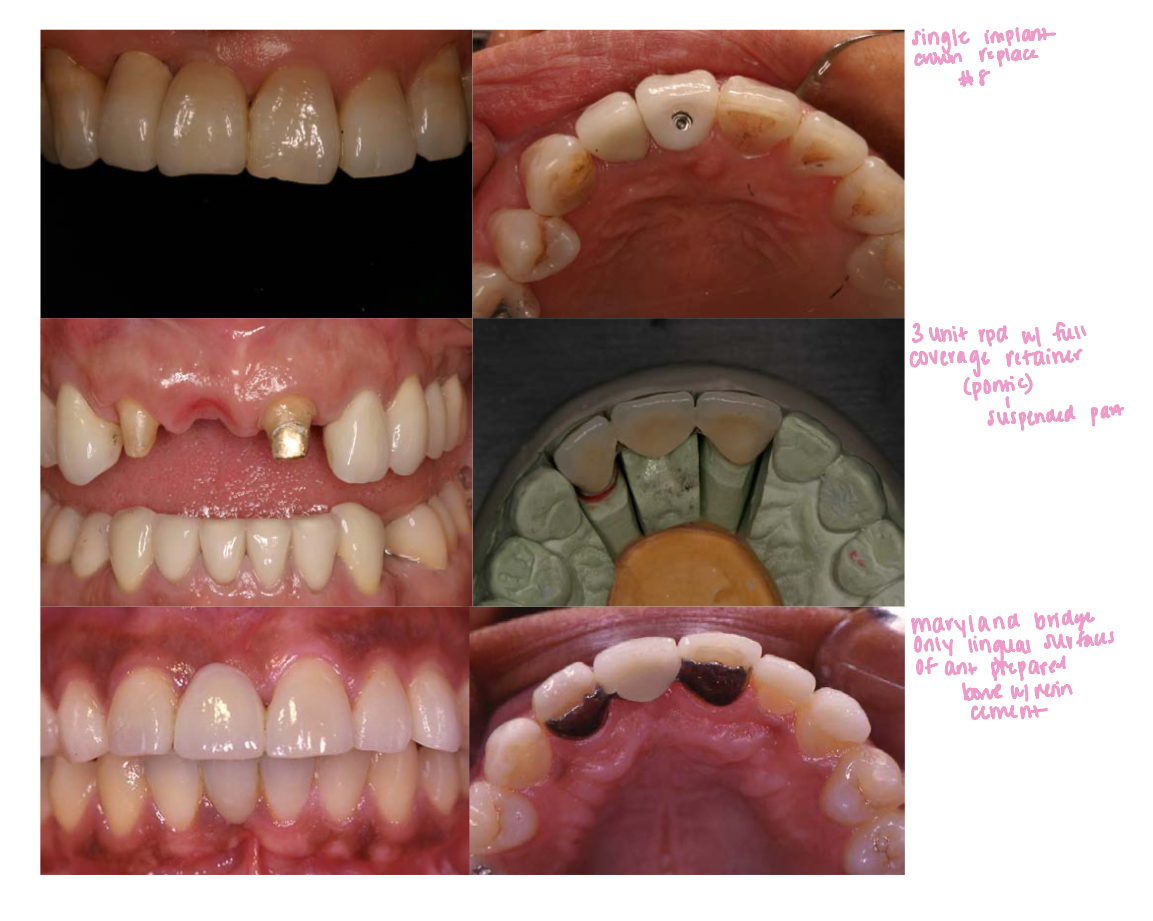
describe the differences in outcomes of restored endodontically treated teeth compared to implant-supported restorations?
survival rate, time to complete (!), proprioception, failure mode, cost, esthetics
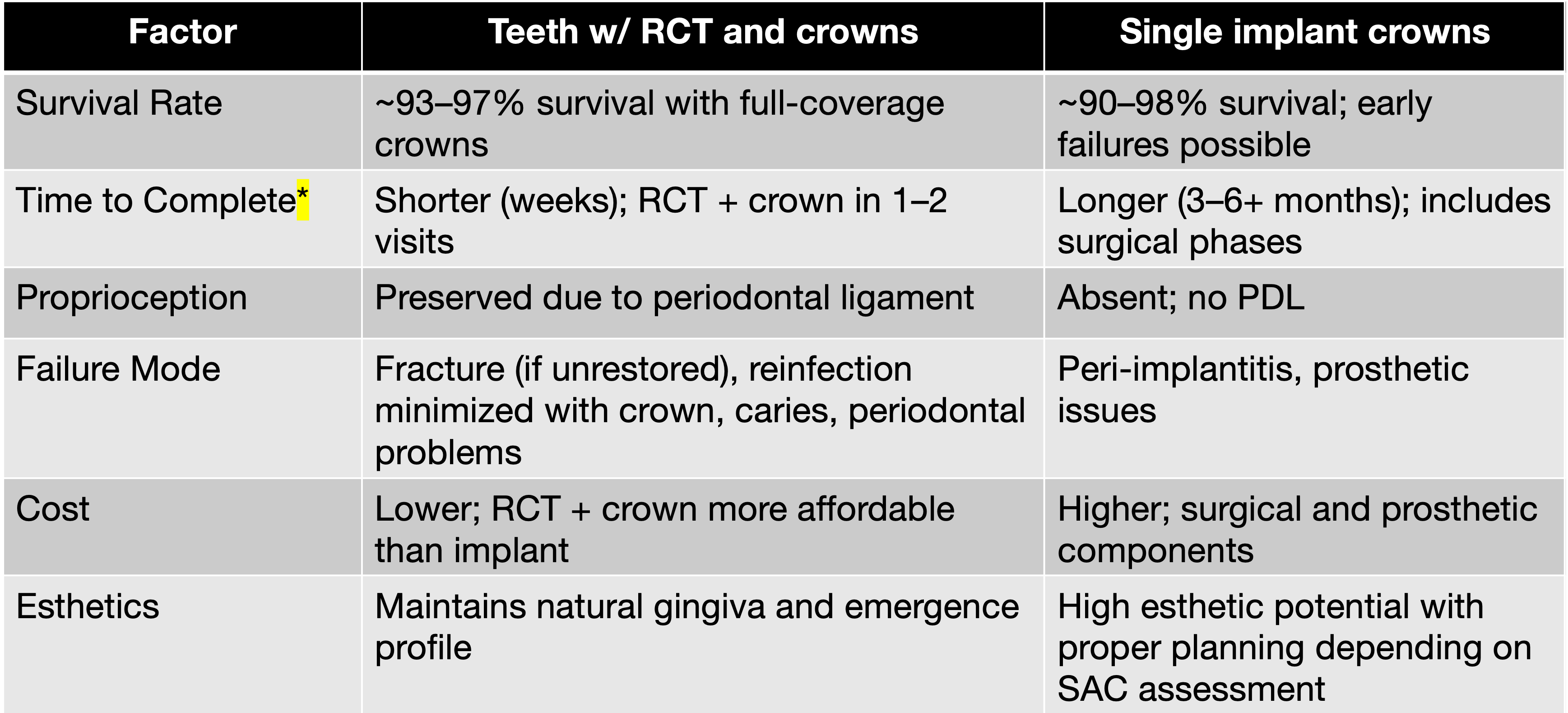
The decision to treat a tooth endodontically or replace it with an implant must be based on factors other than the treatment outcomes of the procedures themselves, such as what?
Periodontal condition
Available bone
Esthetics
Failing RCT and re-tx
Patient preference
T/F: Both nonsurgical root canal therapy followed by an appropriate restoration and single-tooth implants are excellent treatment modalities for treatment of compromised teeth (!)
True
Define the following:
Part of a structure that directly receives thrust or pressure; an anchorage
A tooth, a portion of a tooth, or that portion of a dental implant that serves to support and/or retain a prosthesis
Abutment
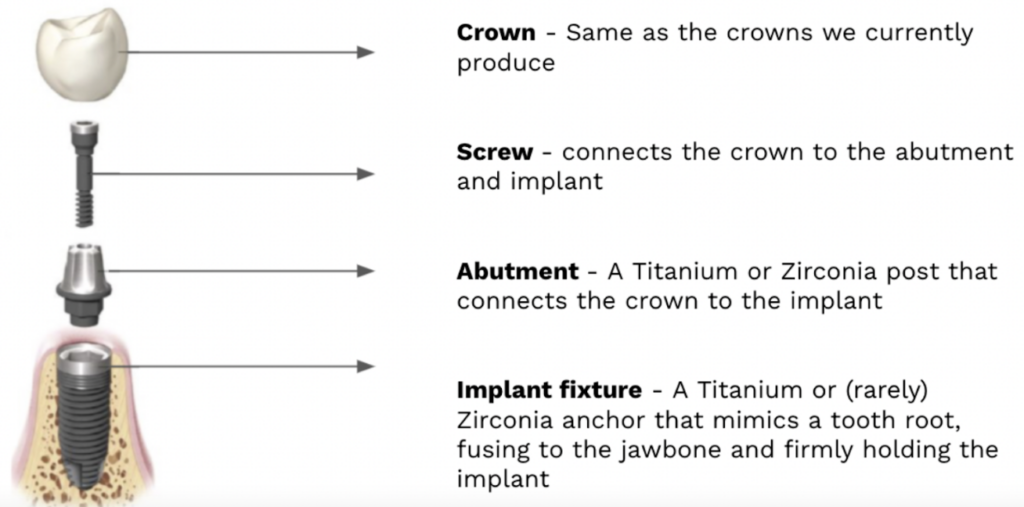
Define the following:
Refers to the coronal aspect of a dental implant to which abutments, components, and the prosthesis may be connected.
Platform
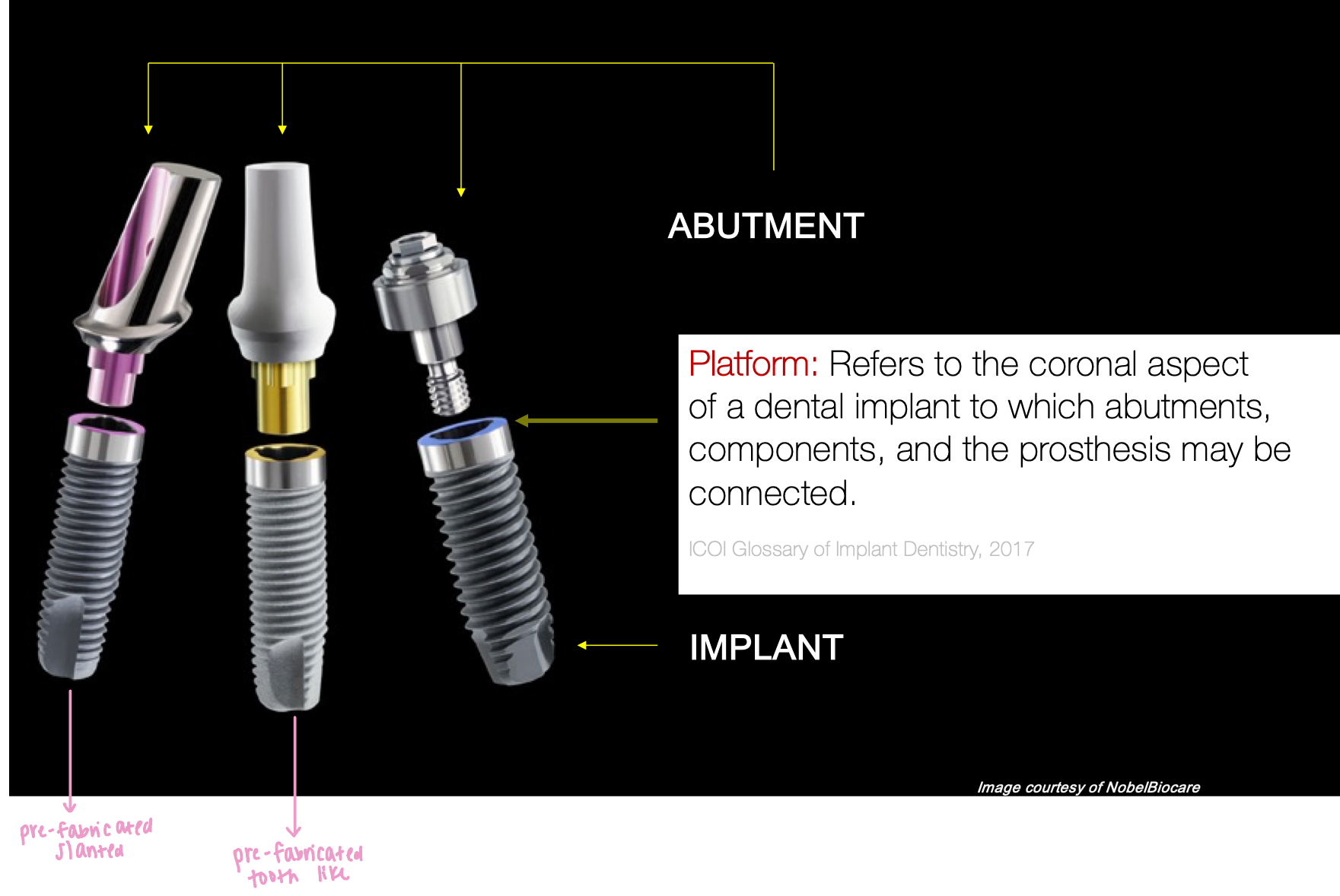
Define the following:
Act of connecting an abutment to an endosseous implant
Abutment connection - external, internal, morse taper, conical connections
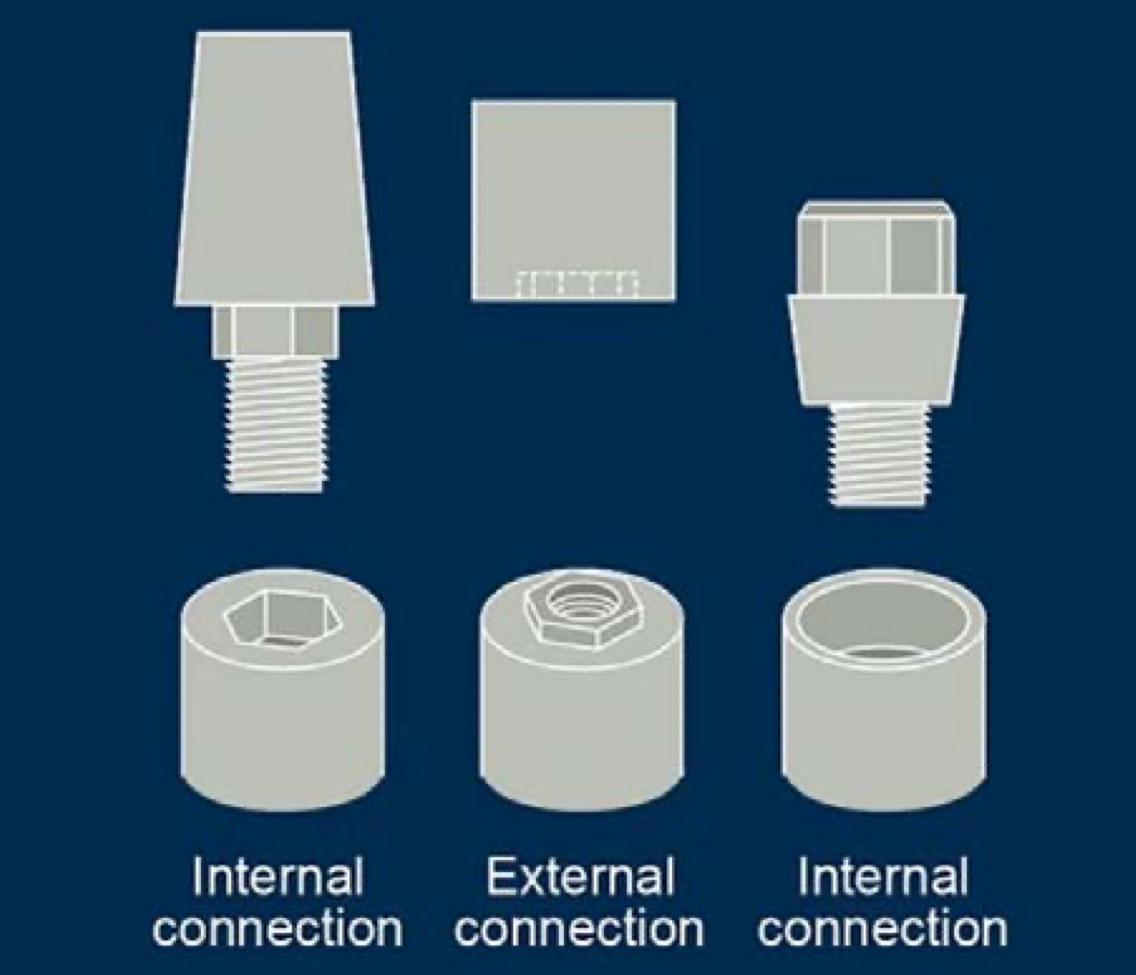
Define the following:
Common contact surface area between an implant abutment and the supporting implant
Abutment-implant interface
What connection mechanisms do we use at TUSDM? what was historically used?
Nobel Biocare Conical Connection or Straumann
hexagonal “branemark”
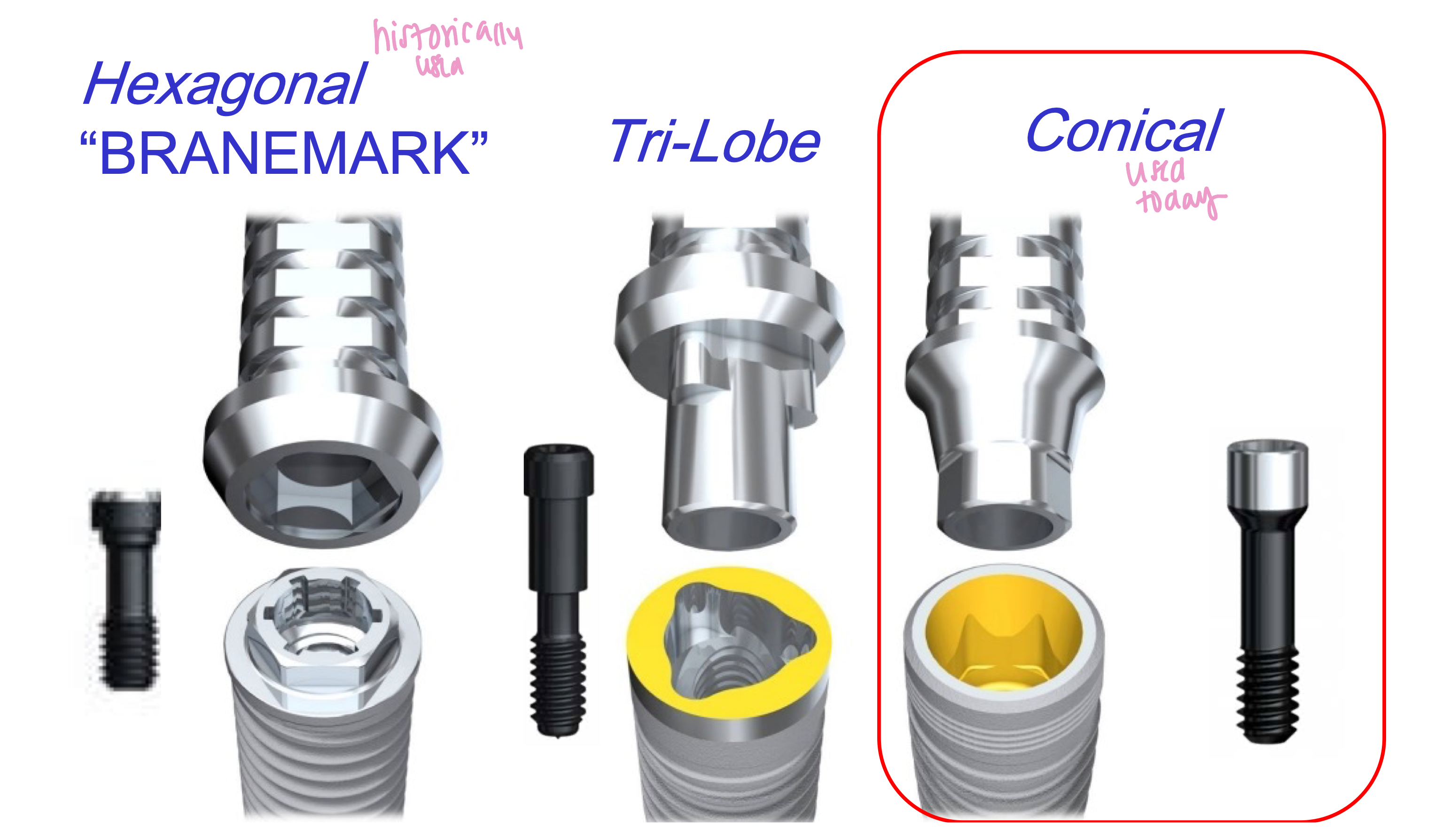
Define the following:
Interface between a transmucosal component (abutment) and the coronal surface of an implant.
Abutment connection interface - external
Define the following: The implant's coronal surface may have an external hexagon, which is engaged when the transmucosal component is seated. (internal or external abutment connection interface)
External abutment connection interface

Define the following: Connection between an abutment and implant in which the a coronal surface of the implant has a core that is threaded or tapered or has a polygonal design (internal or external abutment connection interface)
internal abutment connection interface
what is more common/do most clinicians prefer external or internal abutment connection?
internal connection
Define the following: Refers to presence of anti-rotational features of the implant abutment connection mechanism
Engaging abutments
"Loosening" of the implant crowns was a frequent observation
"engaging" the hex was thought as a way to prevent rotation of the restorations over the implants, this is known as
antirotational feature of engaging abutments
What is more at risk of loosening: multiple unit (splinted) restorations or single unit restorations?
Single unit more at risk
explain the difference in engaging vs non engaging abutments?
engaging: hexagonal, more rotation w single so used this shae to counteract
non engaging: used w multiple implants (bridge) bc rotation is less likely to occur on a larger scale - no lobes
Today anti-rotational features can be either...
internal or external just depends on the implant abutment connection mechanism
What type of restorations always require ENGAGING (antirotational) connections?
Single tooth restorations
Using NON-ENGAGING connections makes fabrication and fit easier for what type of restoration?
Multiple Unit Restorations
What is most important: platform, length, or width of implant?
Platform of implant
T/F: Implant abutment connection designs vary between manufacturers. Components are typically not interchangeable across systems. Additionally, specific connection geometries (e.g., trilobe, conical, SynOcta, CrossFit, Torcfit) are often brand-specific.
True
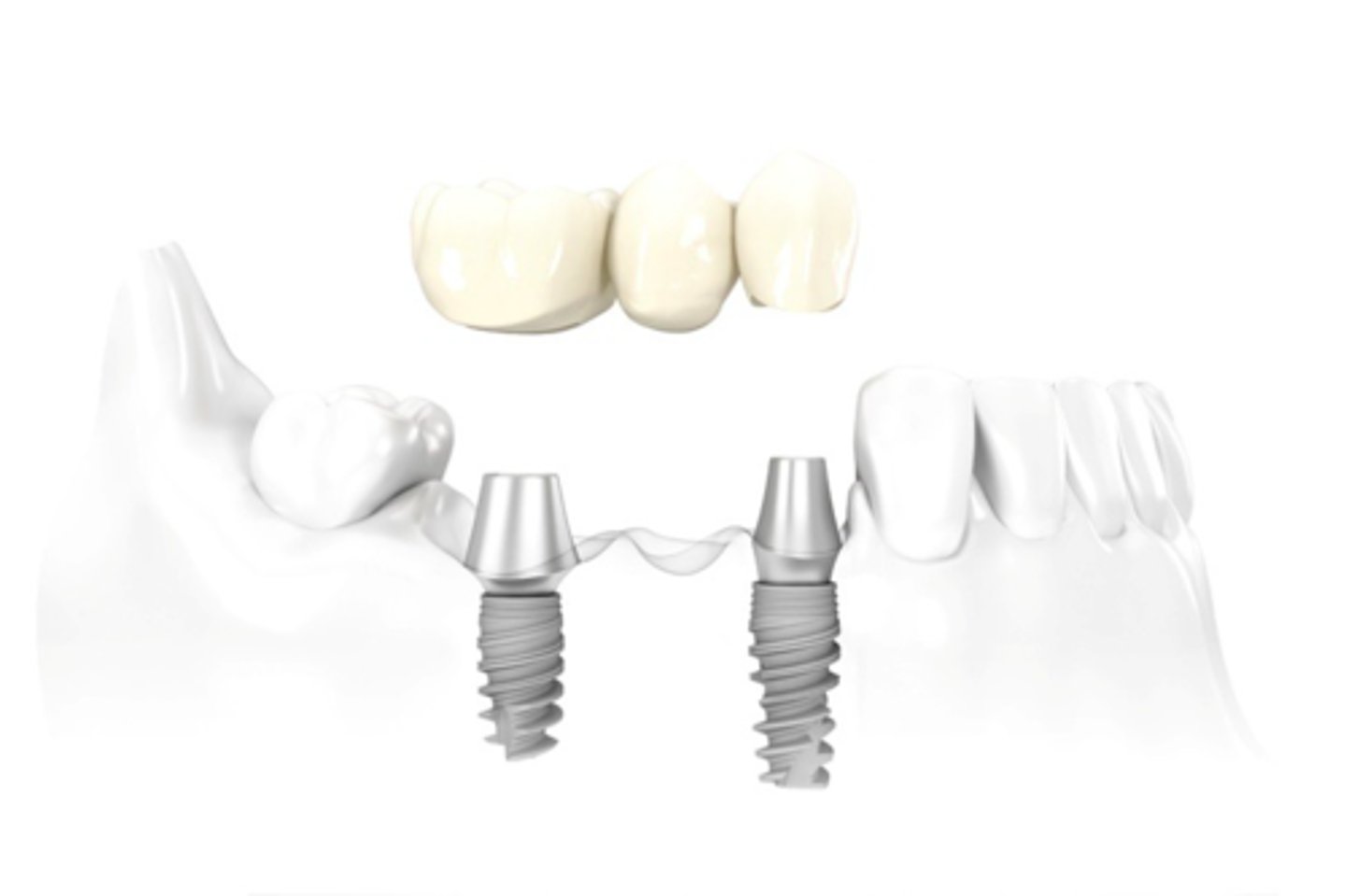
ID the type of implant fixed partial denture:
abutment supported, cement retained FPD
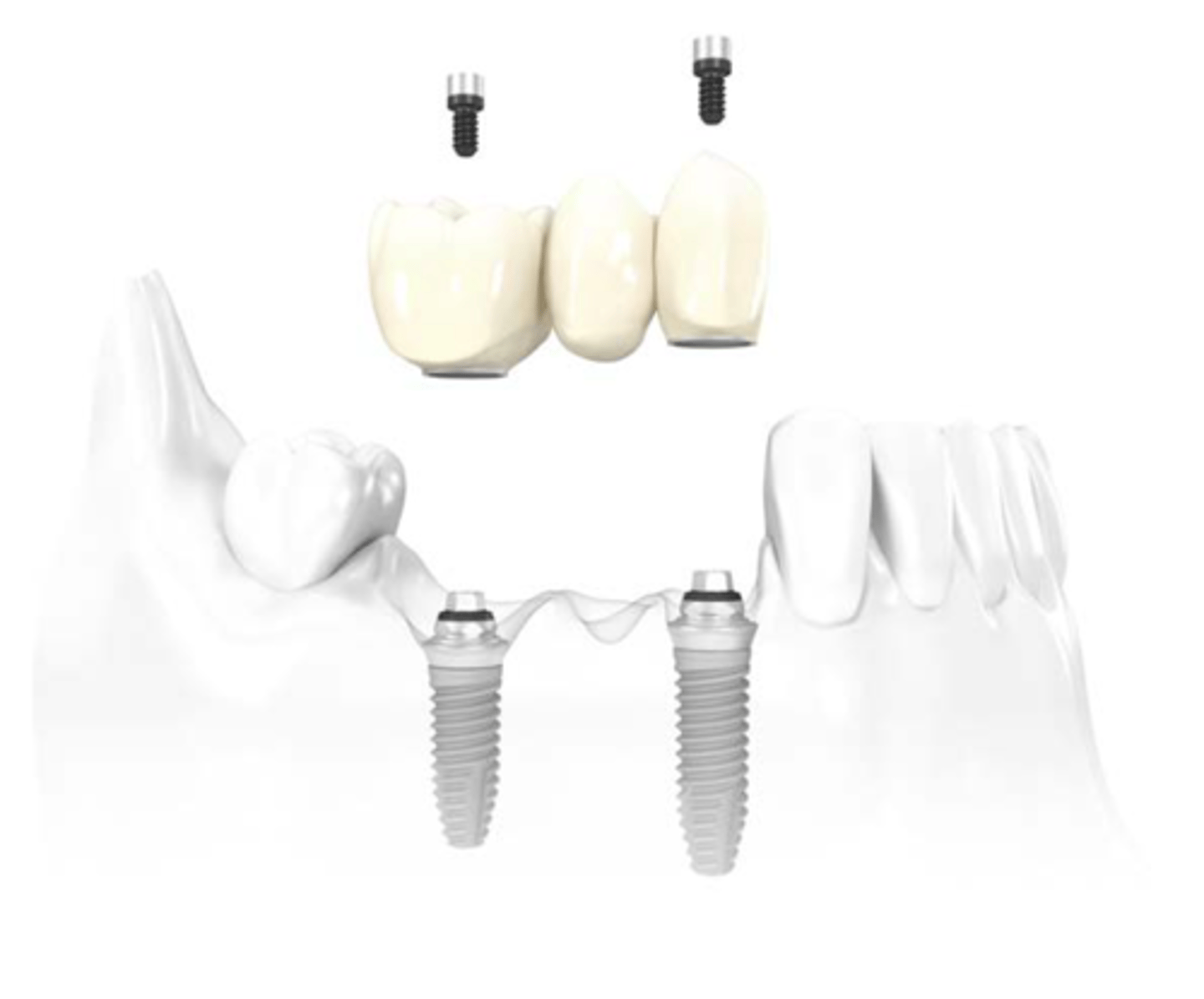
ID the type of implant fixed partial denture:
abutment supported, screw retained FPD - multi unit, internal
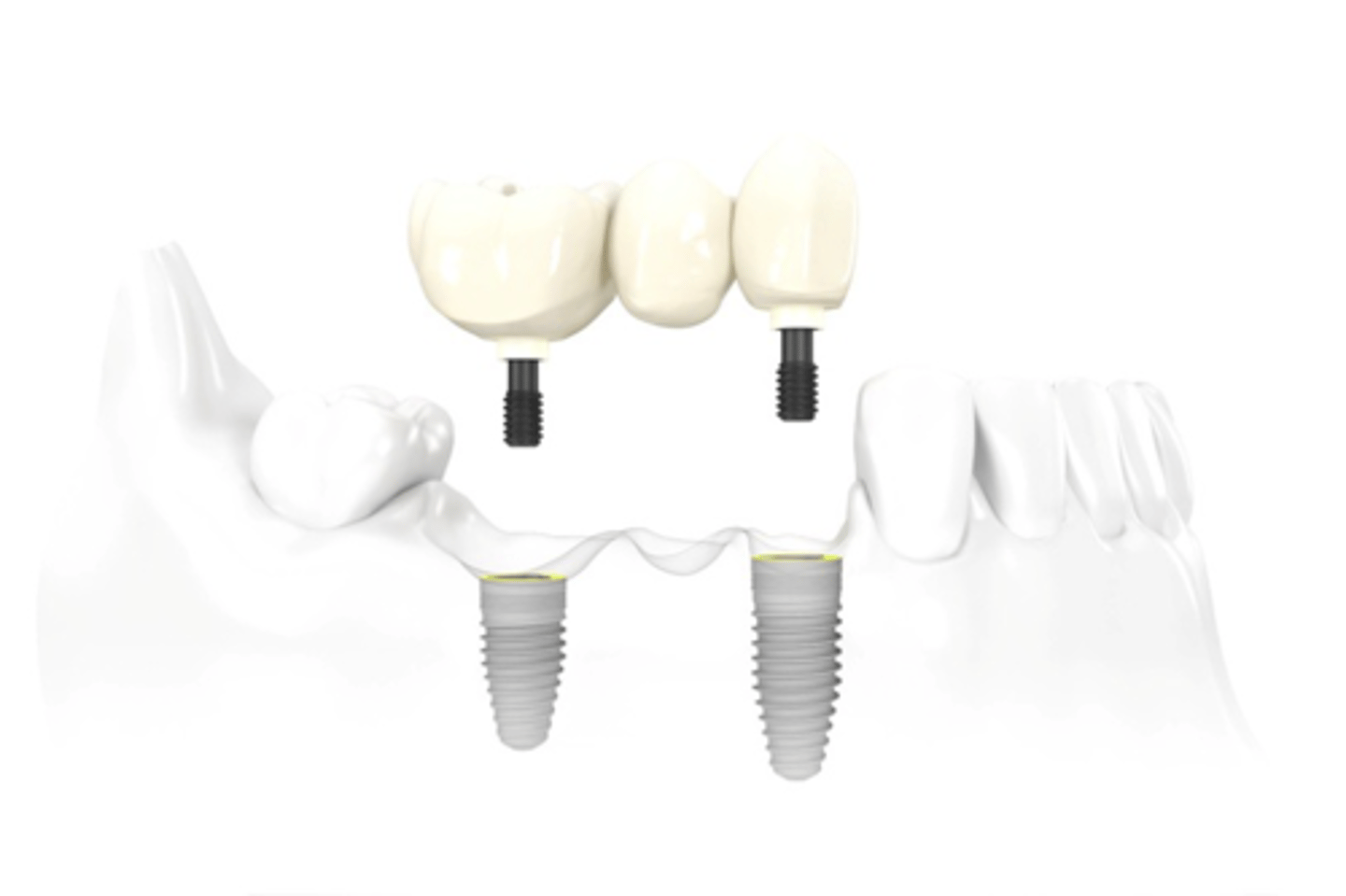
ID the type of implant fixed partial denture:
implant supported, screw retained FPD
holes in crown and finish w composite, no abutments but still implant supported
what are the two main branches for implant abutment classification
healing vs restorative
healing → anatomical vs non-anatomical
restorative → fixed → definitive vs temporary
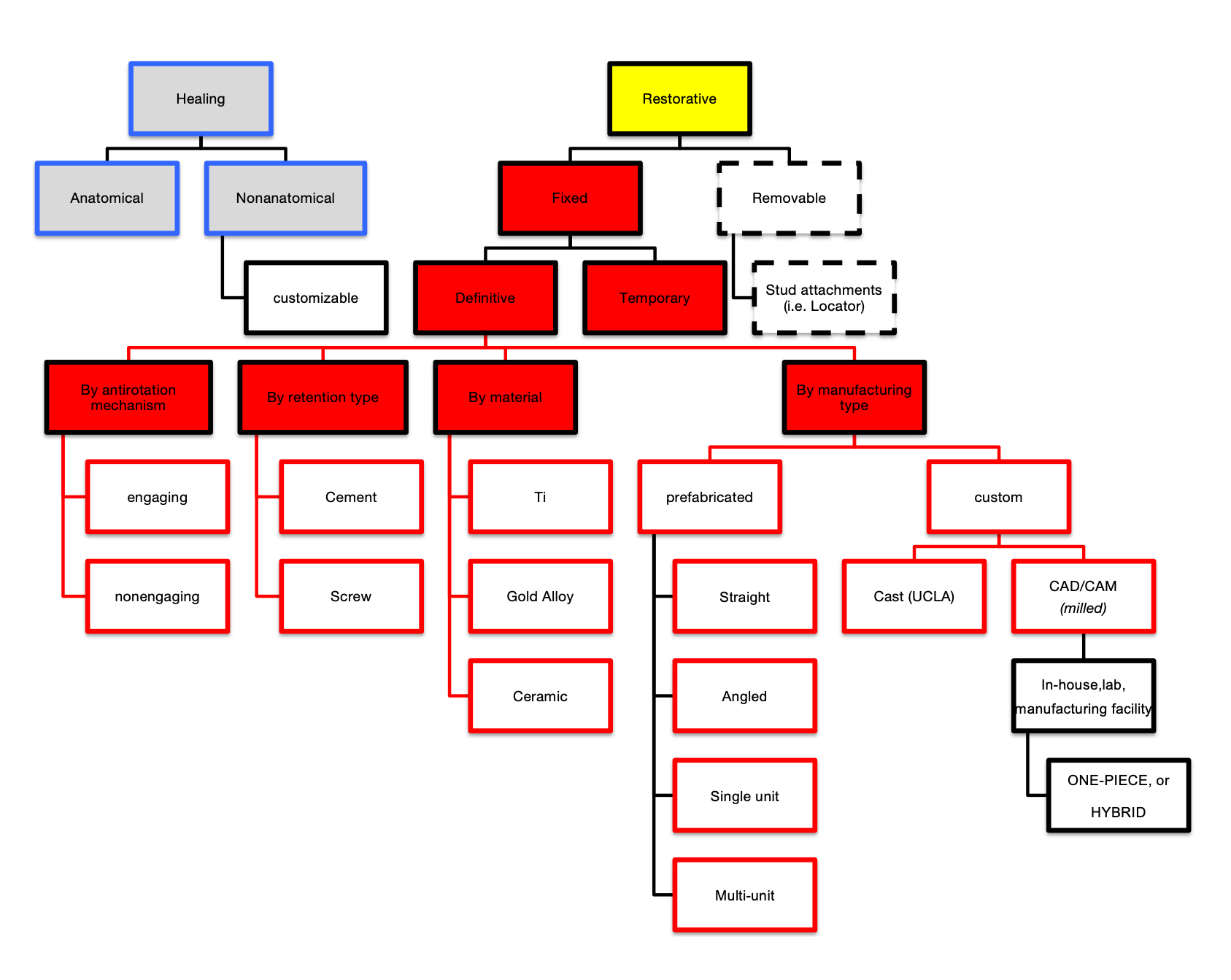
Define the following: Implant component placed at stage-two surgery to guide periodontal soft tissue healing prior to definitive prosthetic restoration
Healing abutment
Typical cross-sectional design for a healing abutment is ?
Cylindrical
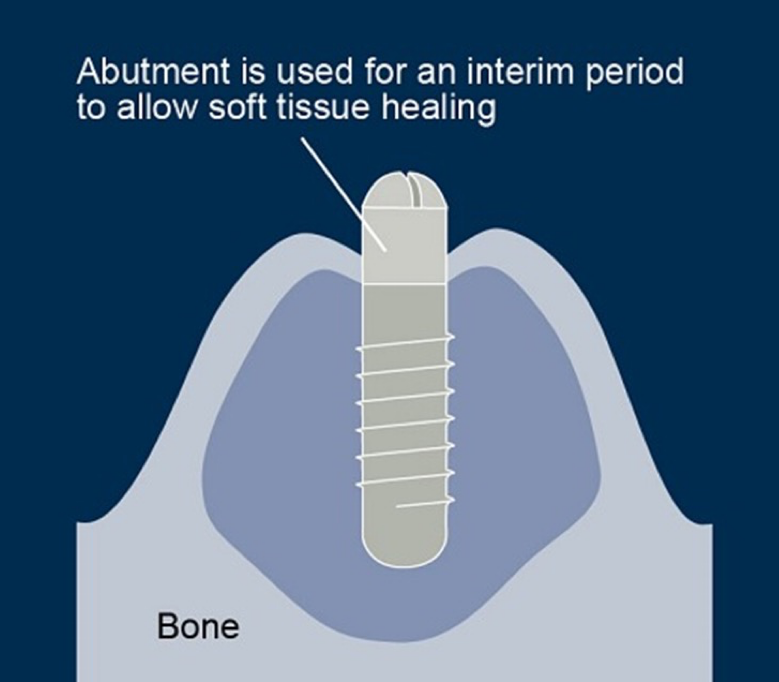

ID the type of healing abutment:
Non-anatomical
Anatomical healing abutments are mimic the natural tooth's emergence profile
Non-anatomical (standard) healing abutments are cylindrical, often resulting in circular gingival cuffs that require more tissue conditioning and create less natural aesthetics, particularly for non-circular teeth
Why are prefabricated healing abutments supplied in different diameters?
Different options to try to match emergence profile.
Ex: Push tissue vs safe tissue. The push tissue allows tissue healing for restorations that require wider emergence as it is slightly wider than implant platform
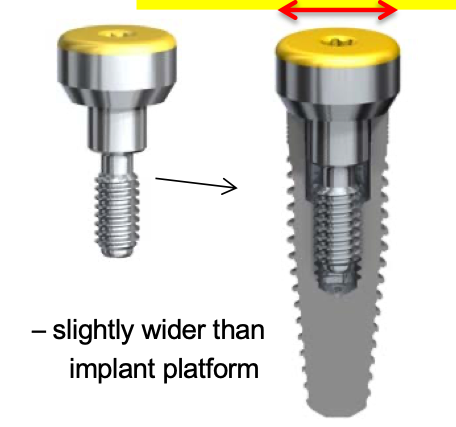
push tissue prefabricated healing abutment

sage tissue prefabricated healing abutment

ID the type of healing abutment:
Anatomical - peek healing abutment
ID the type of healing abutment:
Radio-opaque material
Anterior and posterior designs
Anatomically shaped emergence profile and scalloping
Indexing feature for clear positioning
anatomical healing abutment
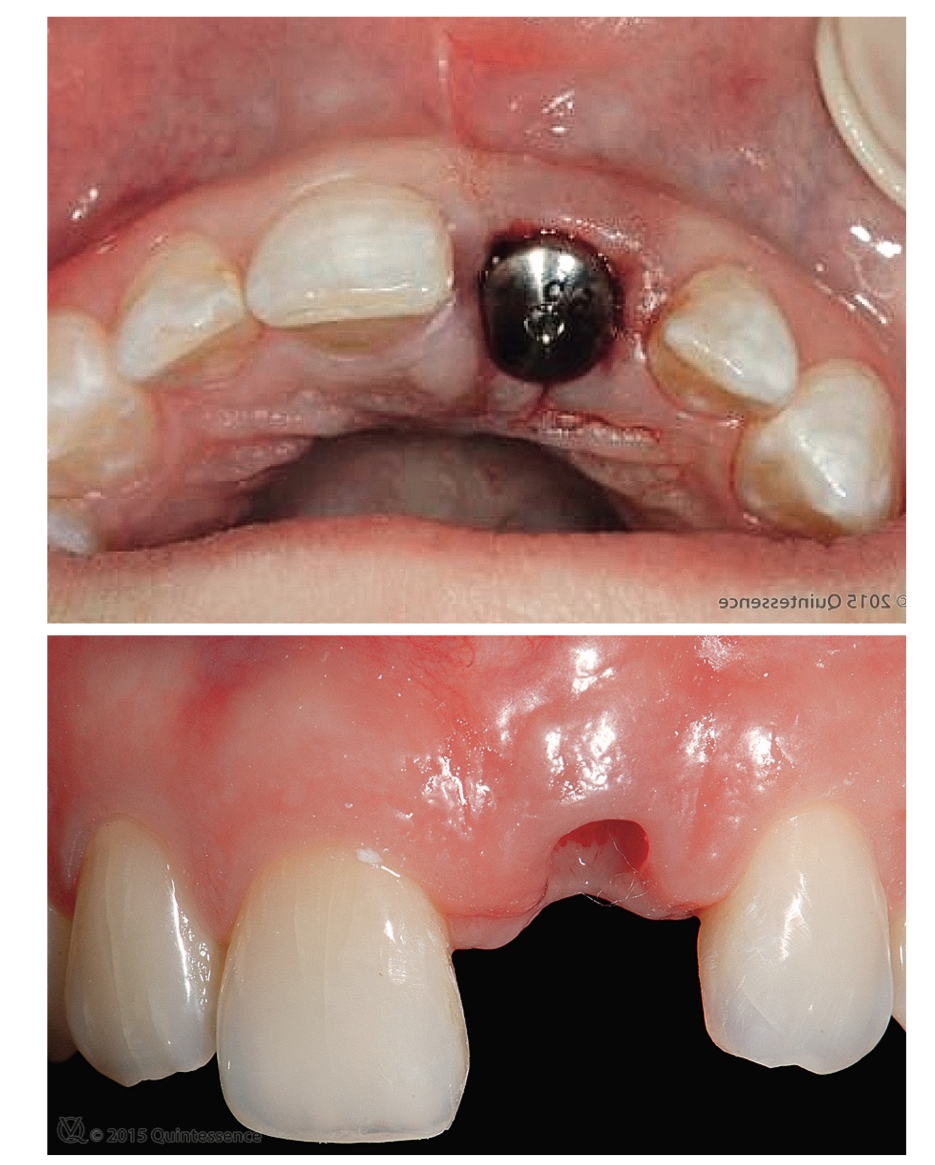
anatomical or non-anatomical healing abutment
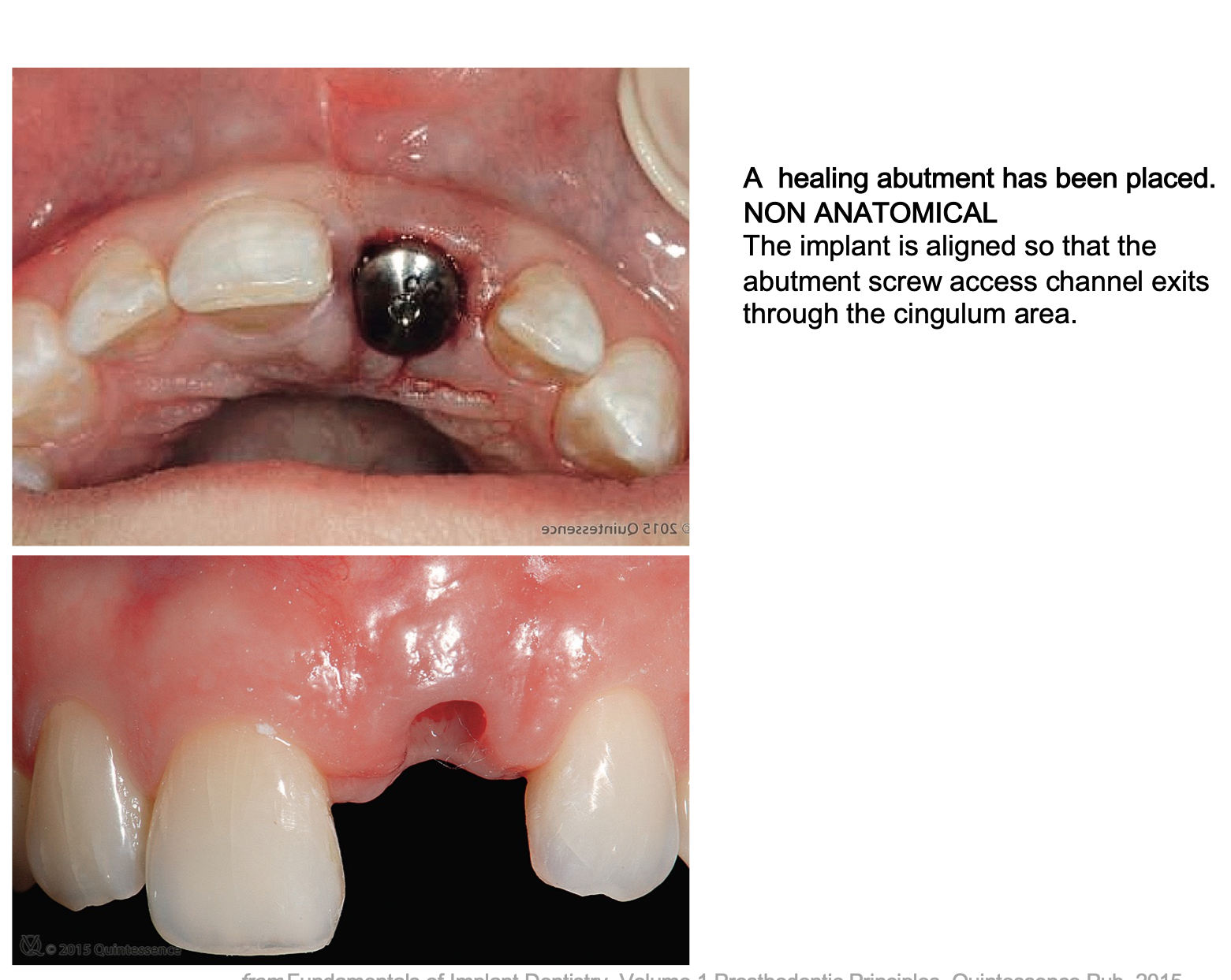
what are the two ways to take implant impressions?
traditional and digital
traditional → implant (UG level) and abutment level and both have open and closed tray techniques
digital → scanbody and scanpost
pick up impression
open tray
transfer impression
pick up
in traditional implant impressions, the implant location is picked up via _______
impression coping
in digital implant impressions, the implant location is picked up via _______
scanbody scanpost
How can you get ready to take an impression of an implant?
Identify implant brand, type, platform- Case Notes
Decide what kind of impression to make-
Open tray, closed tray, scan body
Know indications for each type
Find the implant catalog, look up the part number, and order the parts
Ensure impression copings are ordered at least one week prior to the patient's appointment
Define the following:
Any device that registers the position of the dental implant or dental implant abutment relative to adjacent structures;
Most such devices are indexed to assure reproducible three dimensional location
impression coping
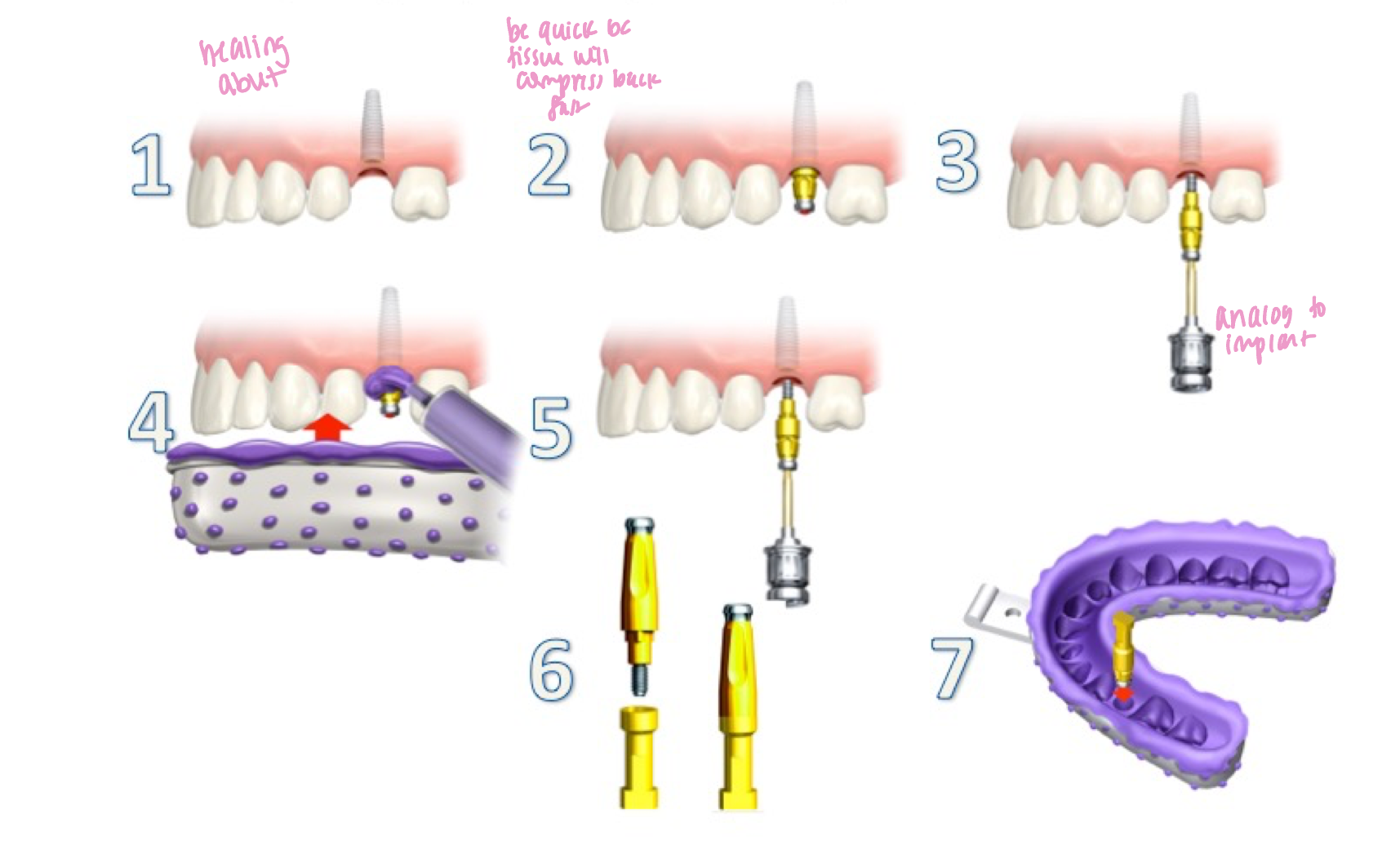
ID the technique:
closed tray / transfer technique
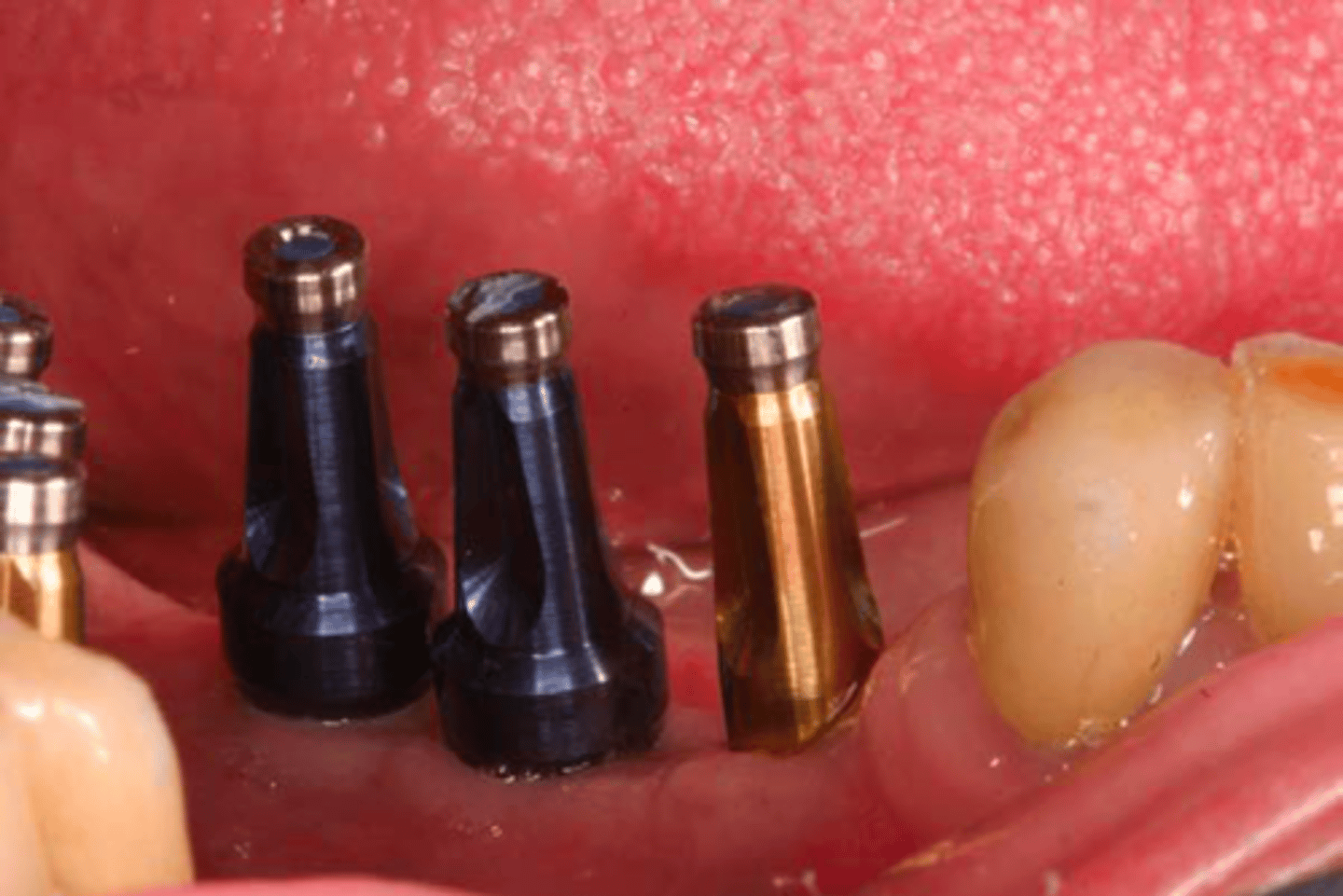
ID the technique: remove healing abutment and place appropriate impression copings
(yellow = regular, blue = wide)
closed tray / transfer technique
ID the technique:
after obtaining pa or bitewing radiograph to verify fit of impression copings
prepare tray for impression (apply adhesive) - there is no need to “open” the tray
closed tray / transfer technique
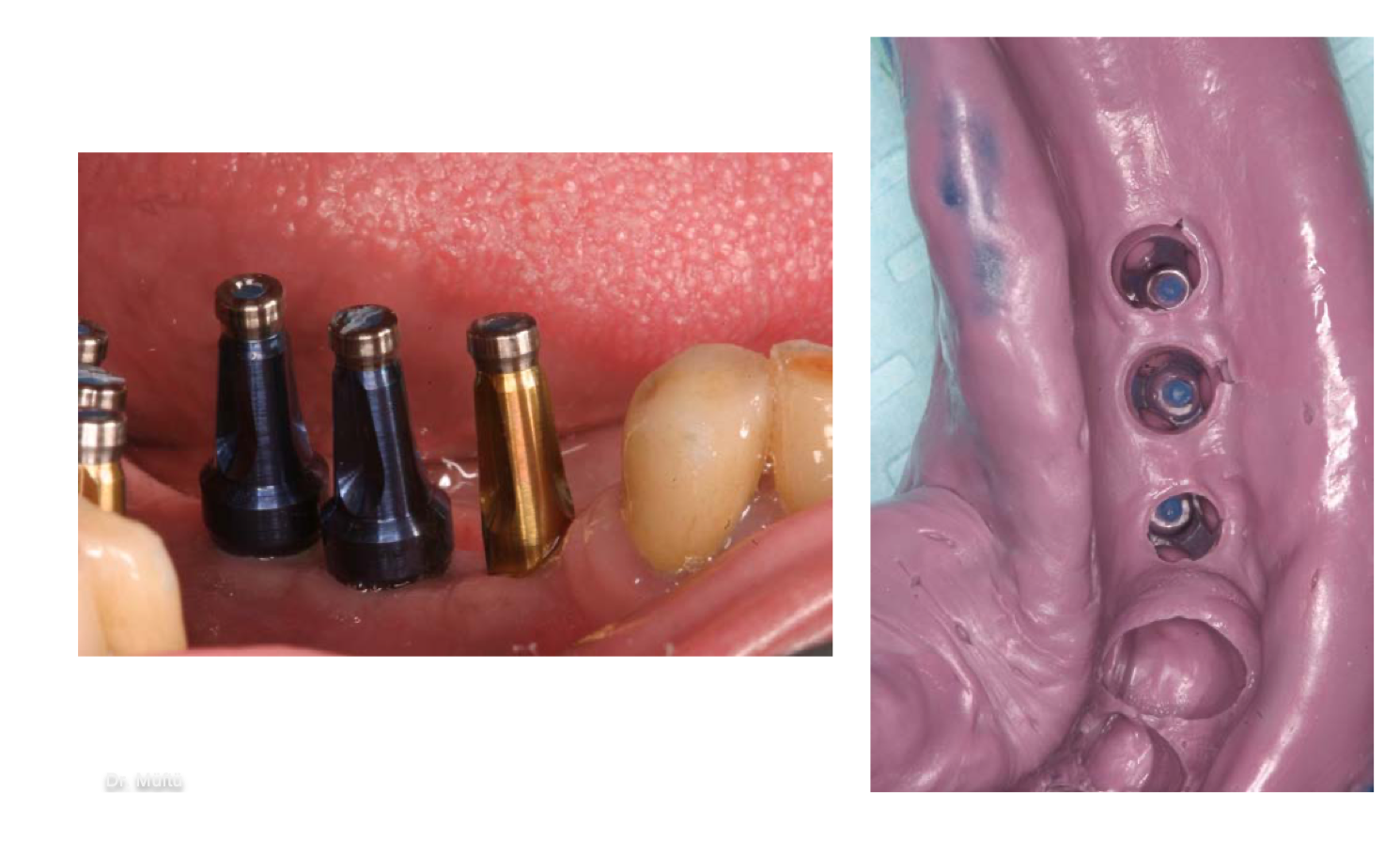
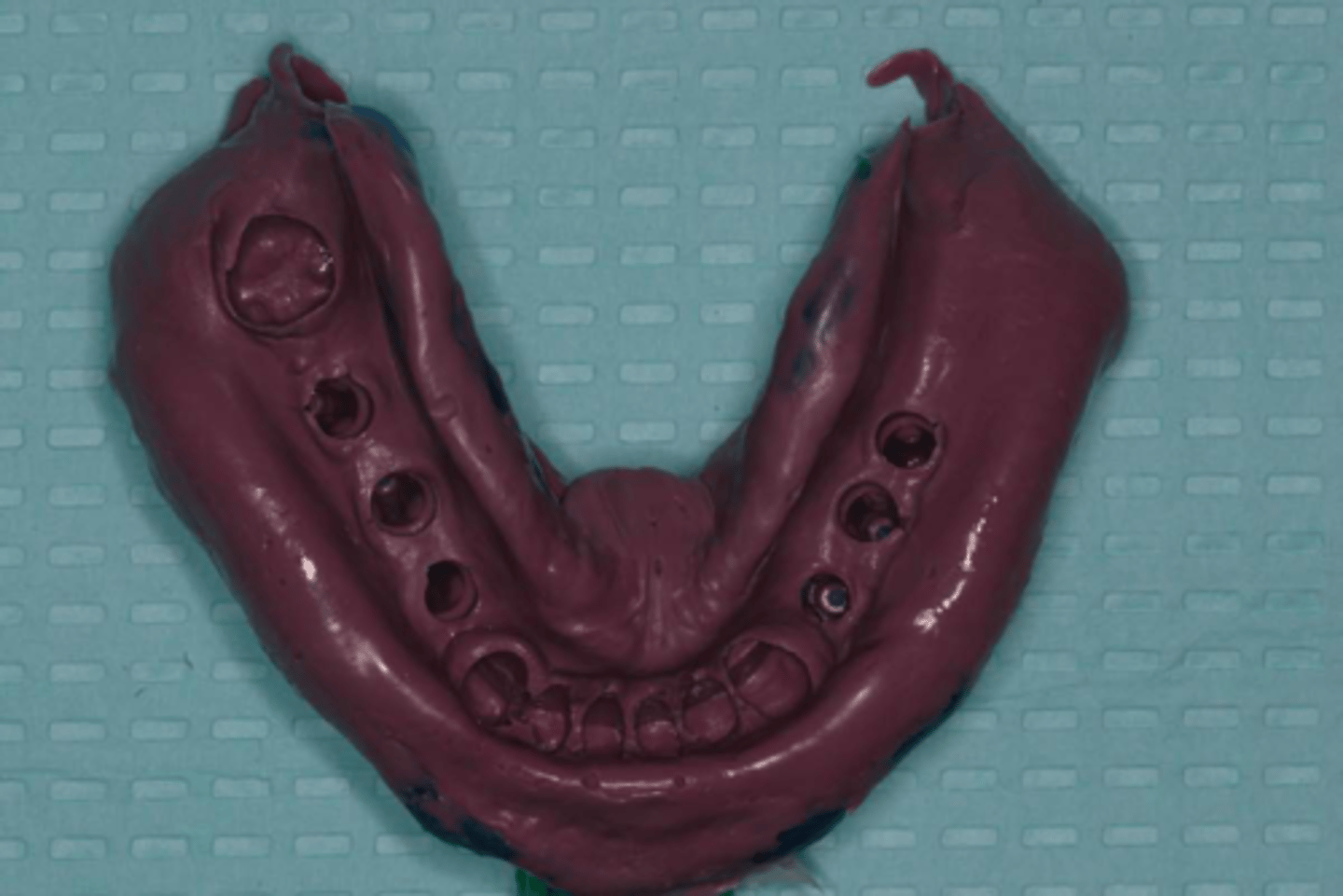
how do we know this is the closed-tray technique?
close-up view of the impression note that impression copings are not ‘picked up’ in the impression, they stay in the mouth
ID the technique:
Remove healing abutment
Place appropriate impression copings
After obtaining pa or bitewing radiograph to verify fit of impression copings, prepare tray for impression (apply adhesive)
There is no need to "open" the tray
Close-up view of the impression note that impression copings are not 'picked up' in the impression, they stay in the mouth
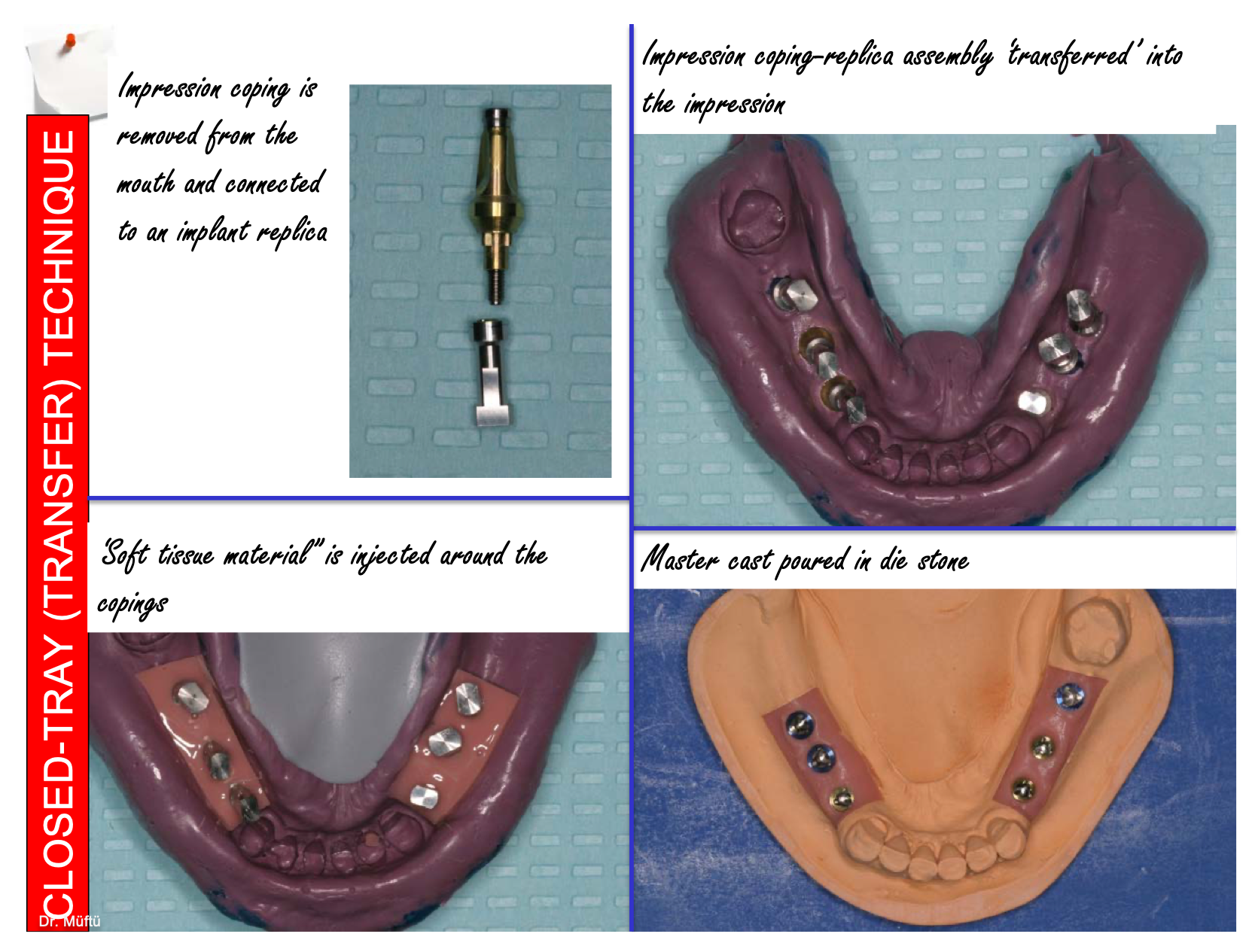
Impression coping is removed from the mouth and connected to an implant replica
Impression coping-replica assembly 'transferred' into the impression
'Soft tissue material" is injected around the copings
Master cast poured in die stone
closed tray / transfer technique
ID the technique:
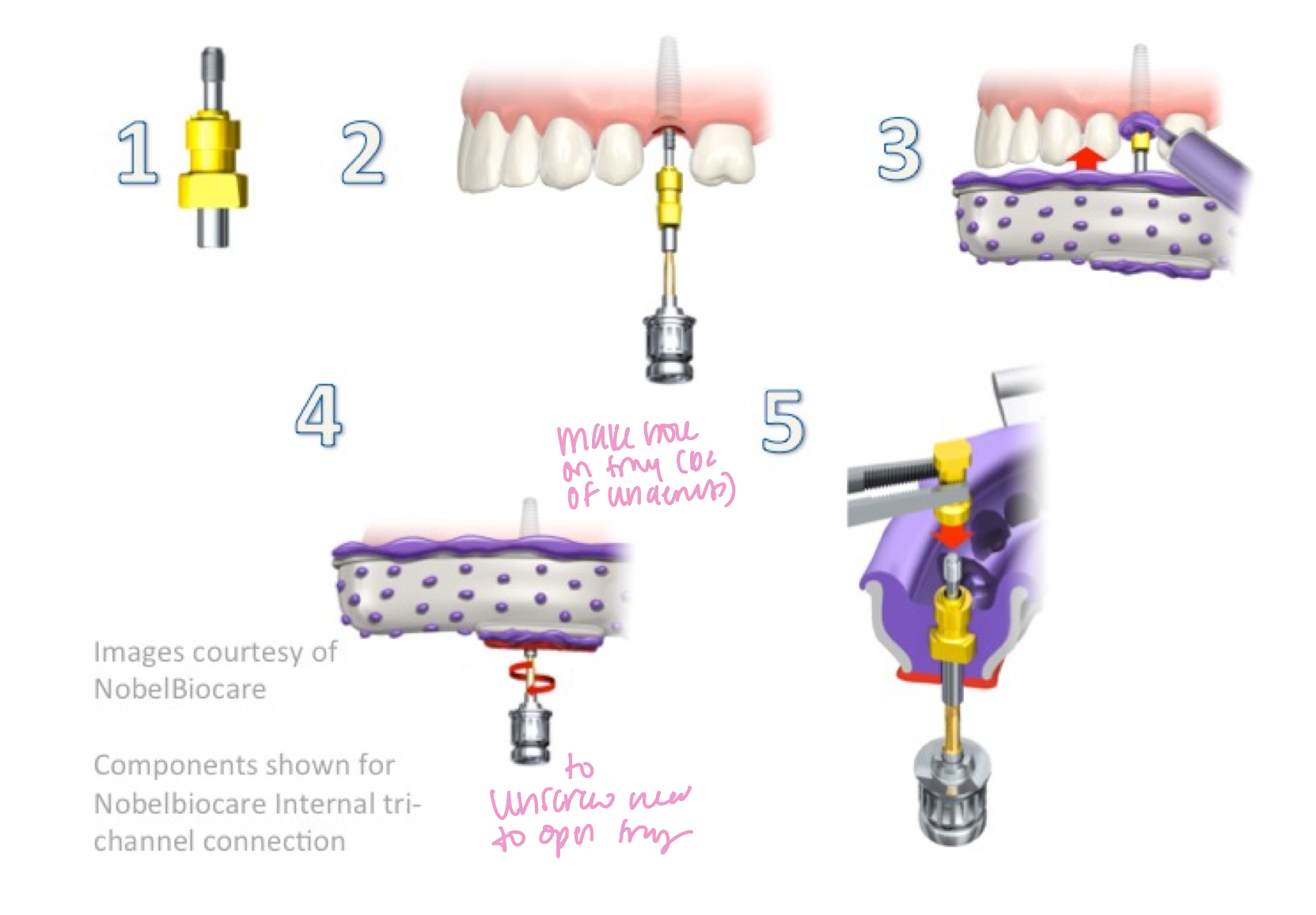
open tray/ pick-up technique
ID the technique:
Remove healing abutment
Place appropriate impression coping
Obtain PA or bitewing radiograph to verify fit of the impression coping
Prepare tray for impression (open a hole if necessary, apply adhesive, etc)
Seat the tray
Make sure that the screw is exposed through impression material
Loosen impression coping screw
Remove impression from the mouth
Impression coping stays in the impression
open tray/ pick-up technique
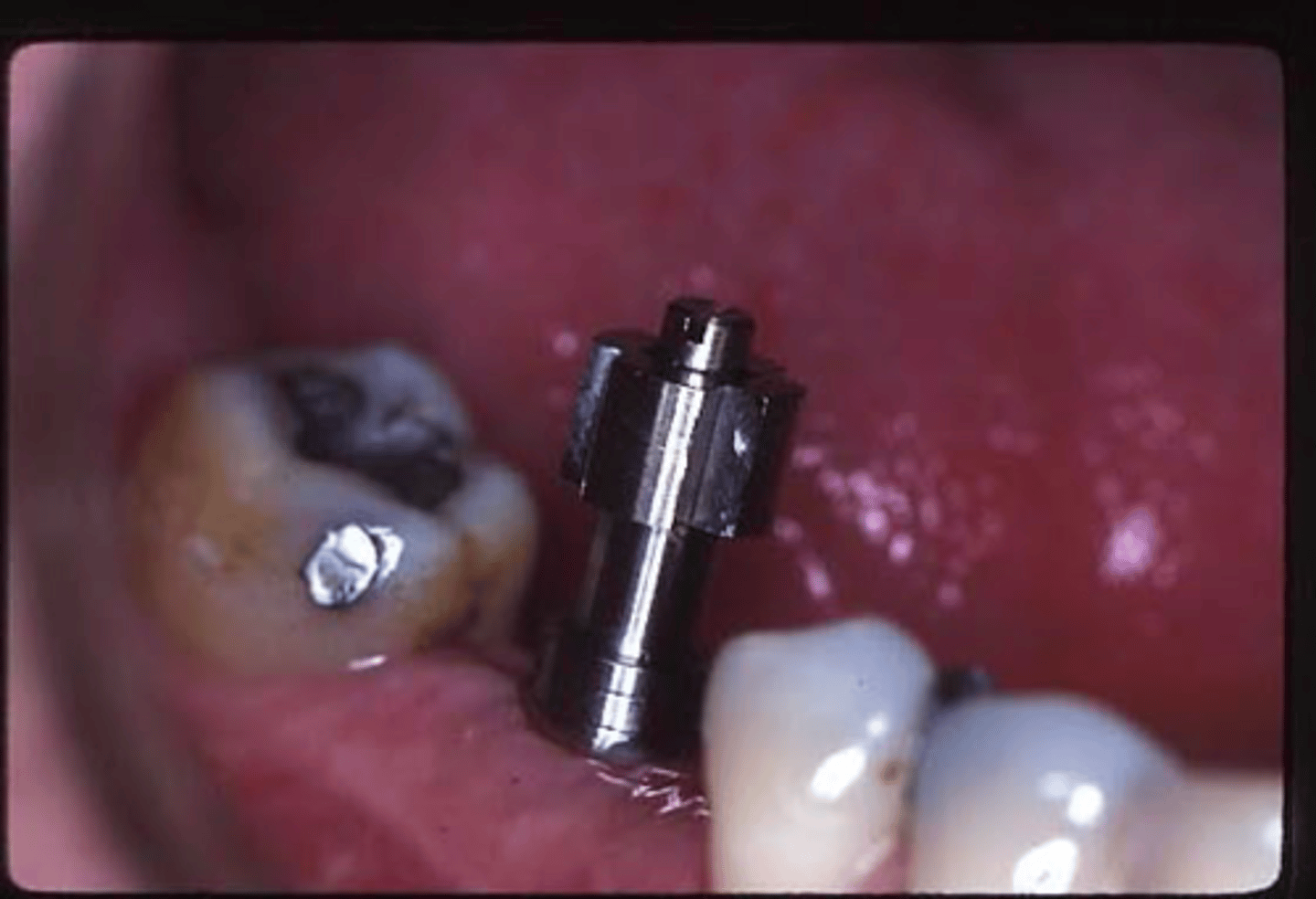
ID the technique and describe what is going on/next steps?
open tray/ pick-up technique
remove healing abutment, place appropriate impression coping
what radiographic technique is used to verify fit of impression coping?
PA and BW
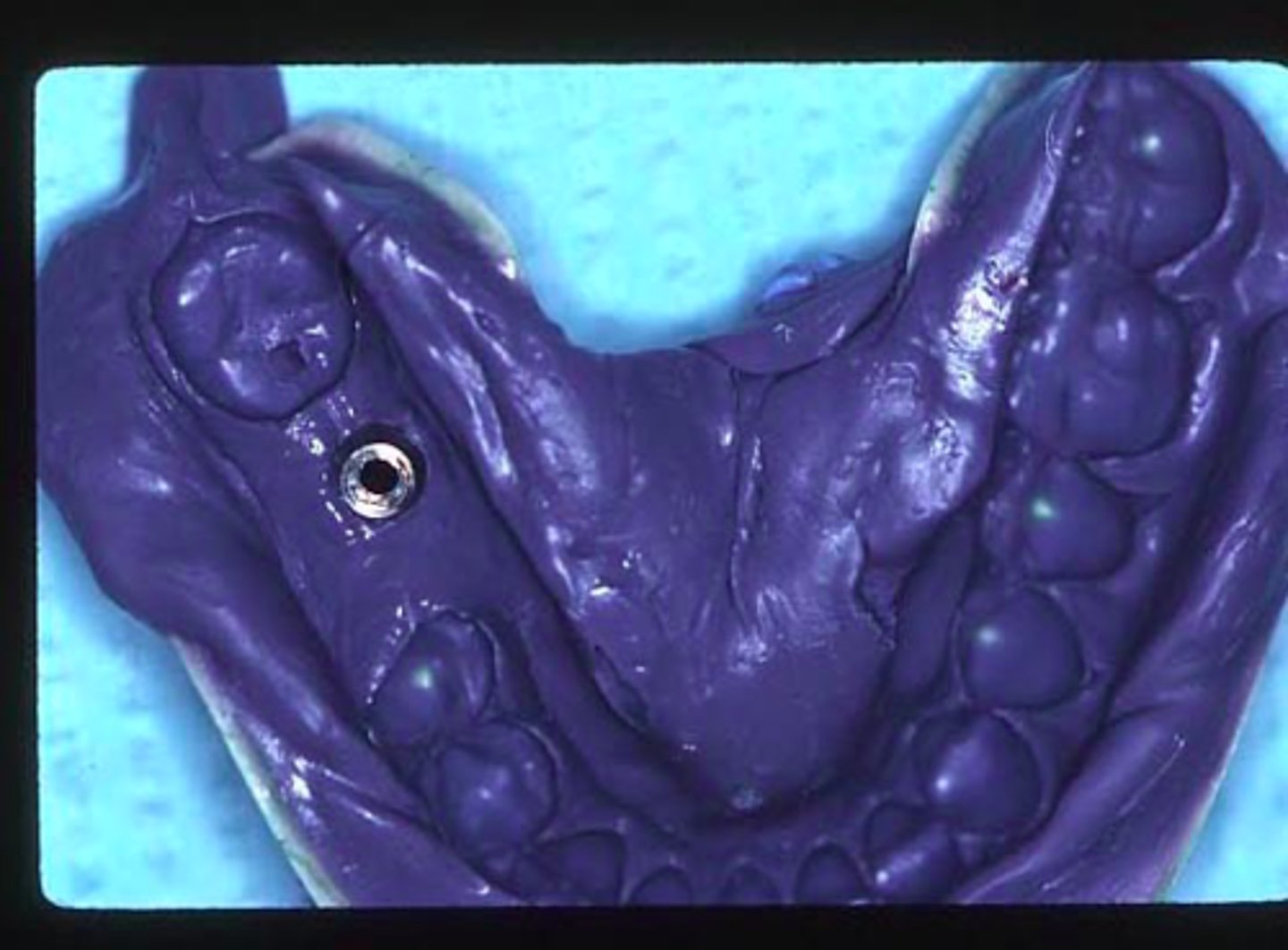
ID the technique:
open tray/ pick-up technique - pick-up bc coping stays on the impression
loosen impression coping screw
remove impression from the mouth
impression coping stays in the impression for the open tray technique
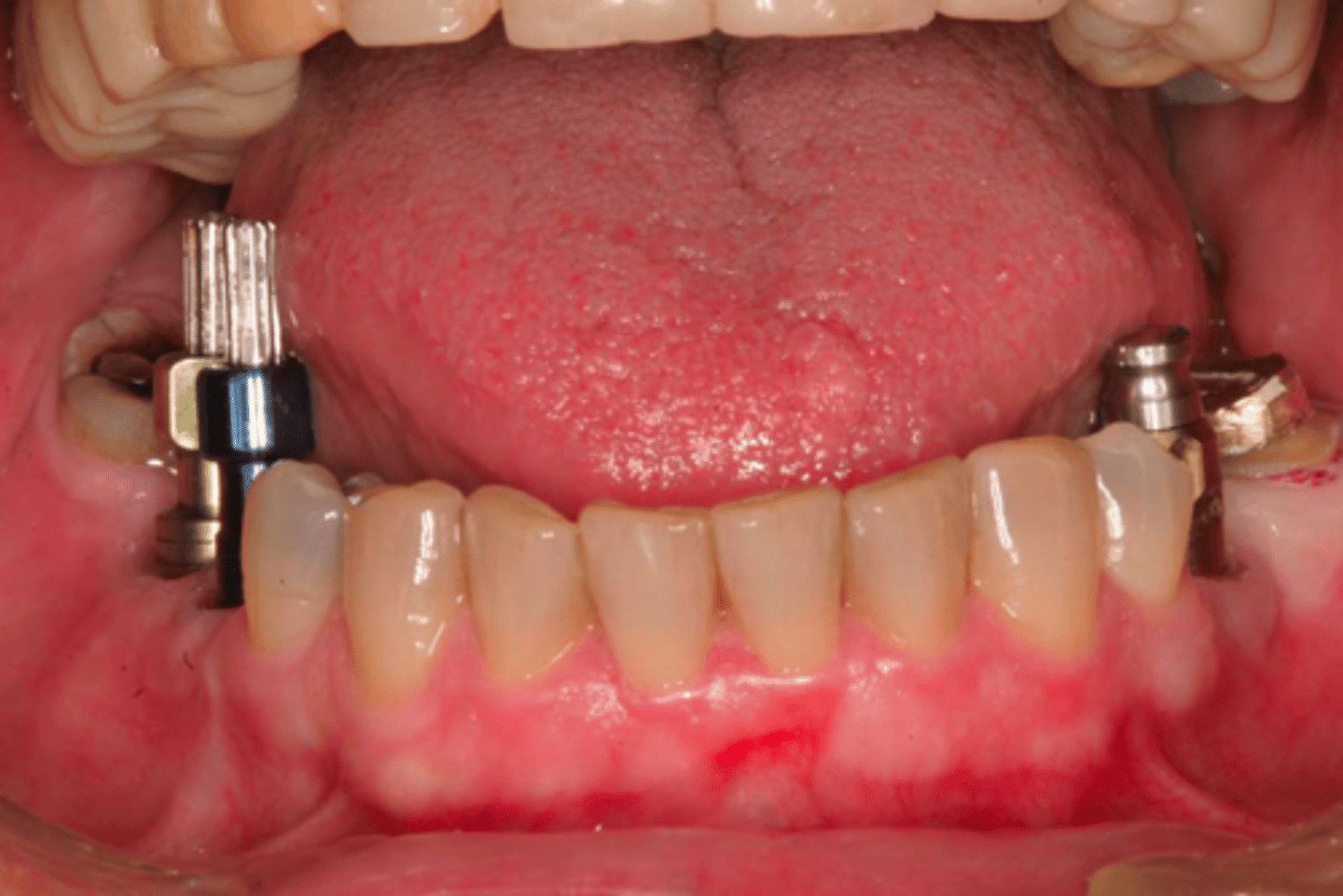
ID the technique on the patient's left:
closed tray / transfer technique
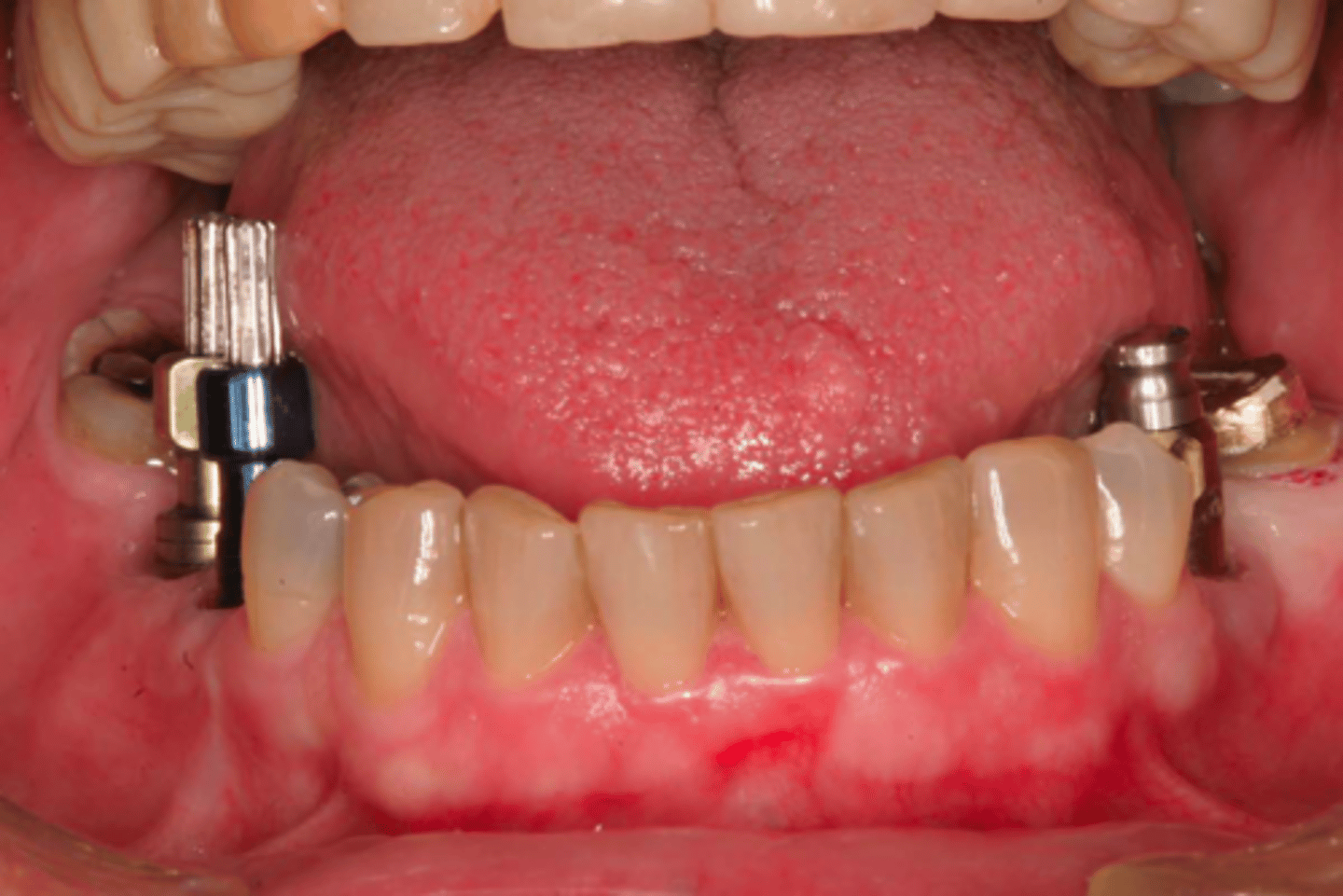
ID the technique on the patient's right:
open tray/ pick-up technique

ID the part:
implant replica
Define the following:
Replica of the implant that is embedded in the working cast
Has same platform and connection mechanism as the implant
Used during fabrication of the implant prosthesis
implant replica/analog
_______ in which the implant analog is enveloped in an elastic material simulating mucosal tissues to facilitate laboratory procedures
This material is removable
By shaping the soft tissue simulating material, an optimum crown emergence can be fabricated
Makes fabrication of the implant crown and assessment of marginal fit easier
Soft tissue cast
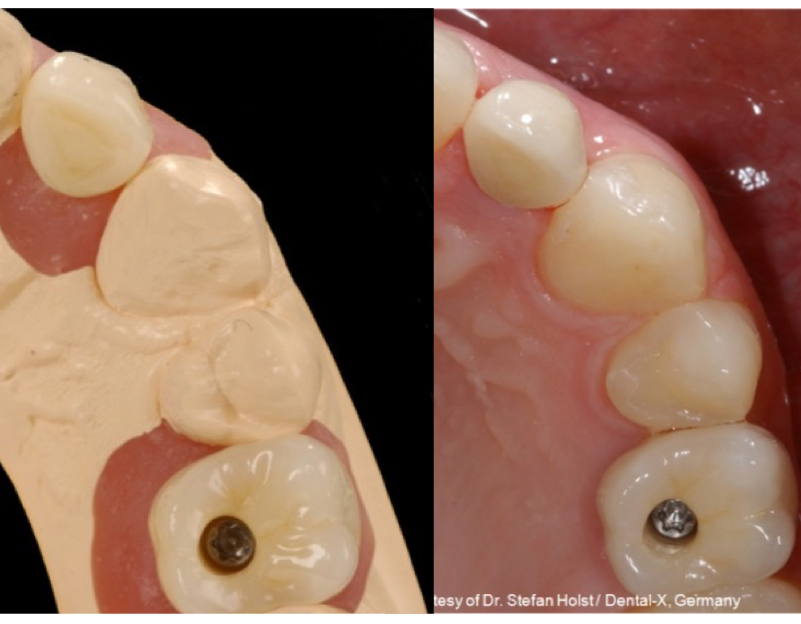
what type of stone is used for soft tissue cast?
die keen
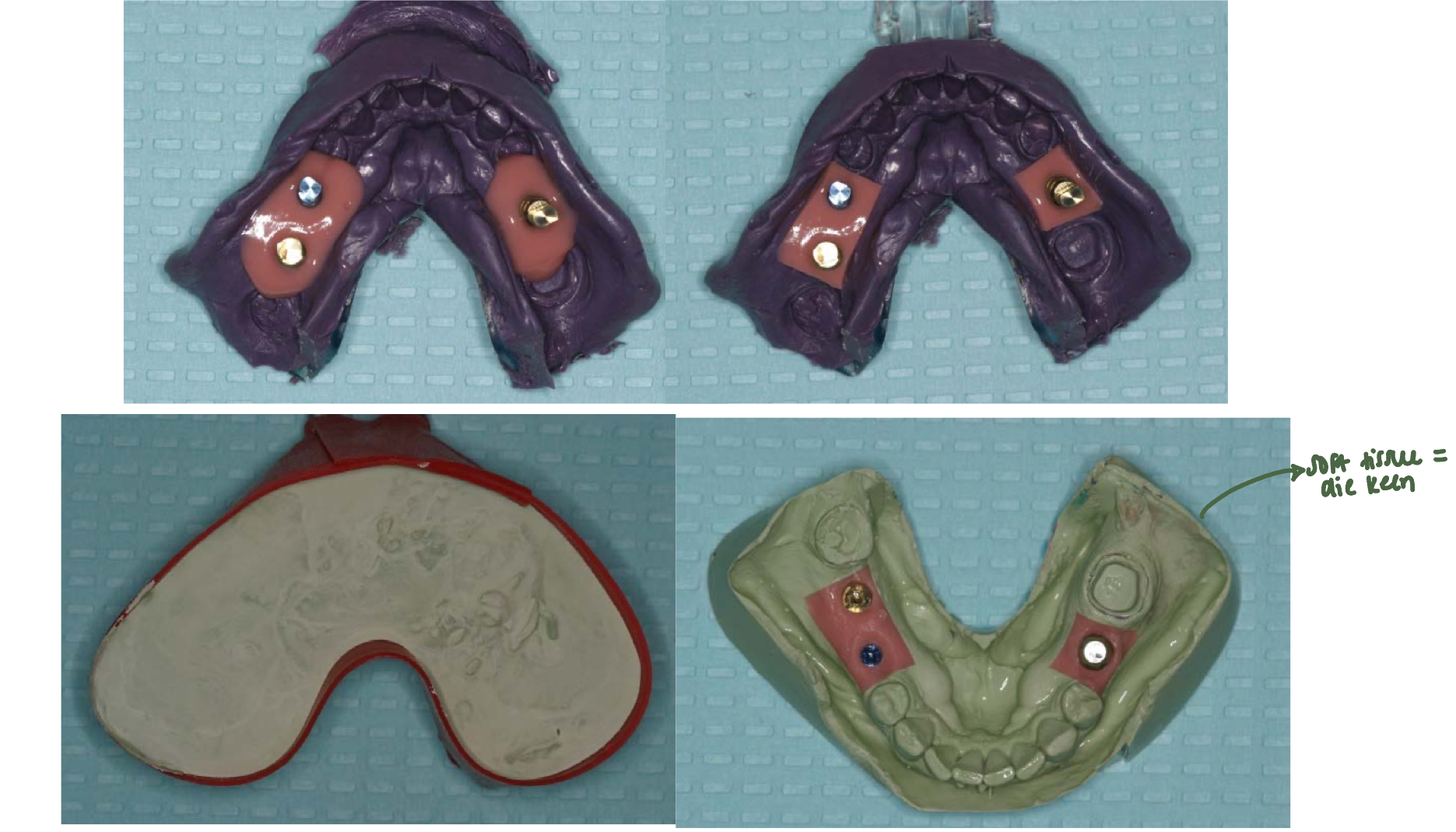
ID which technique the following quality belongs to:
reduces the effect of the implant angulation (the deformation of the impression material upon recovery from the mouth)
removes the concern for replacing the coping back into its respective space in the impression
increased difficulty but more forgiving
open tray/ pick-up technique
ID which technique the following quality belongs to:
there are more parts to control when fastening
there may be some rotational movement of the impression coping when securing the implant analog
blind attachment of the implant analog to the impression coping may result in a misfit of components
open tray/ pick-up technique
ID which technique the following quality belongs to:
Better for pts with gag reflexes
Better for pts with limited mouth opening
If impression of natural teeth are to be made at the same time with the implant(s)
Less number of implants
closed tray / transfer technique
T/F: An open tray impression coping will reduce the effect of the implant angulation (the deformation of the impression material upon recovery from the mouth)
True
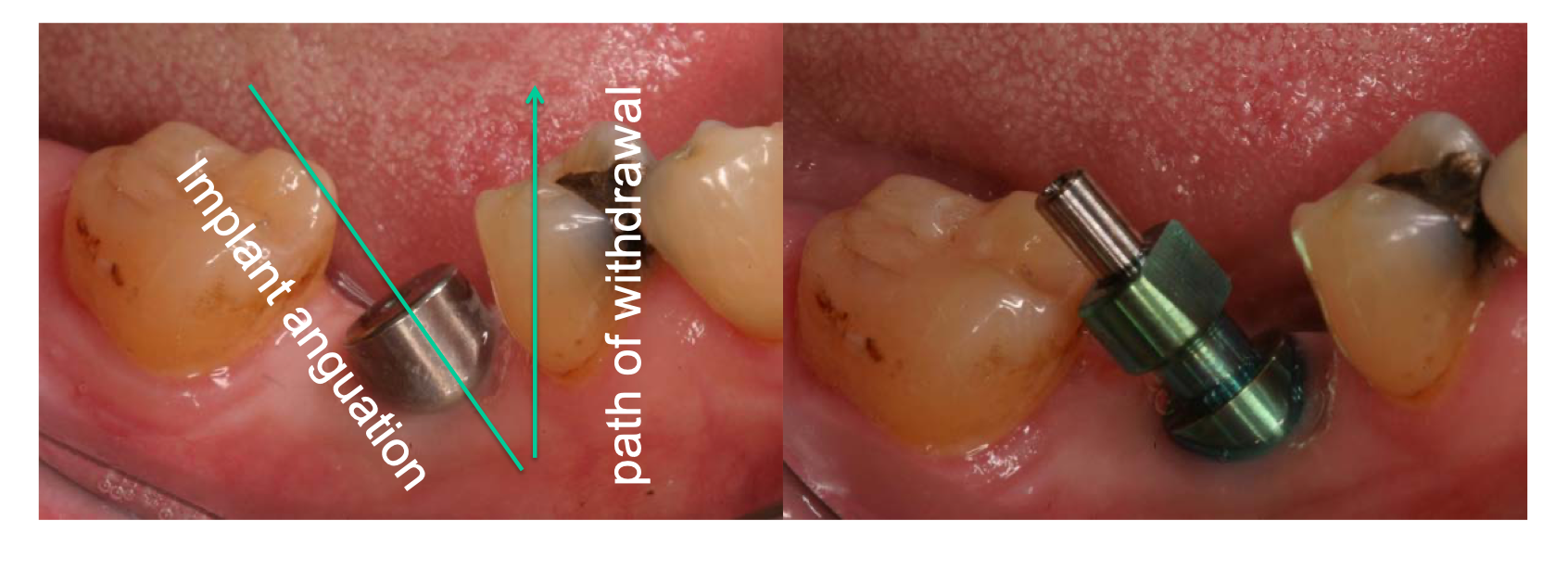
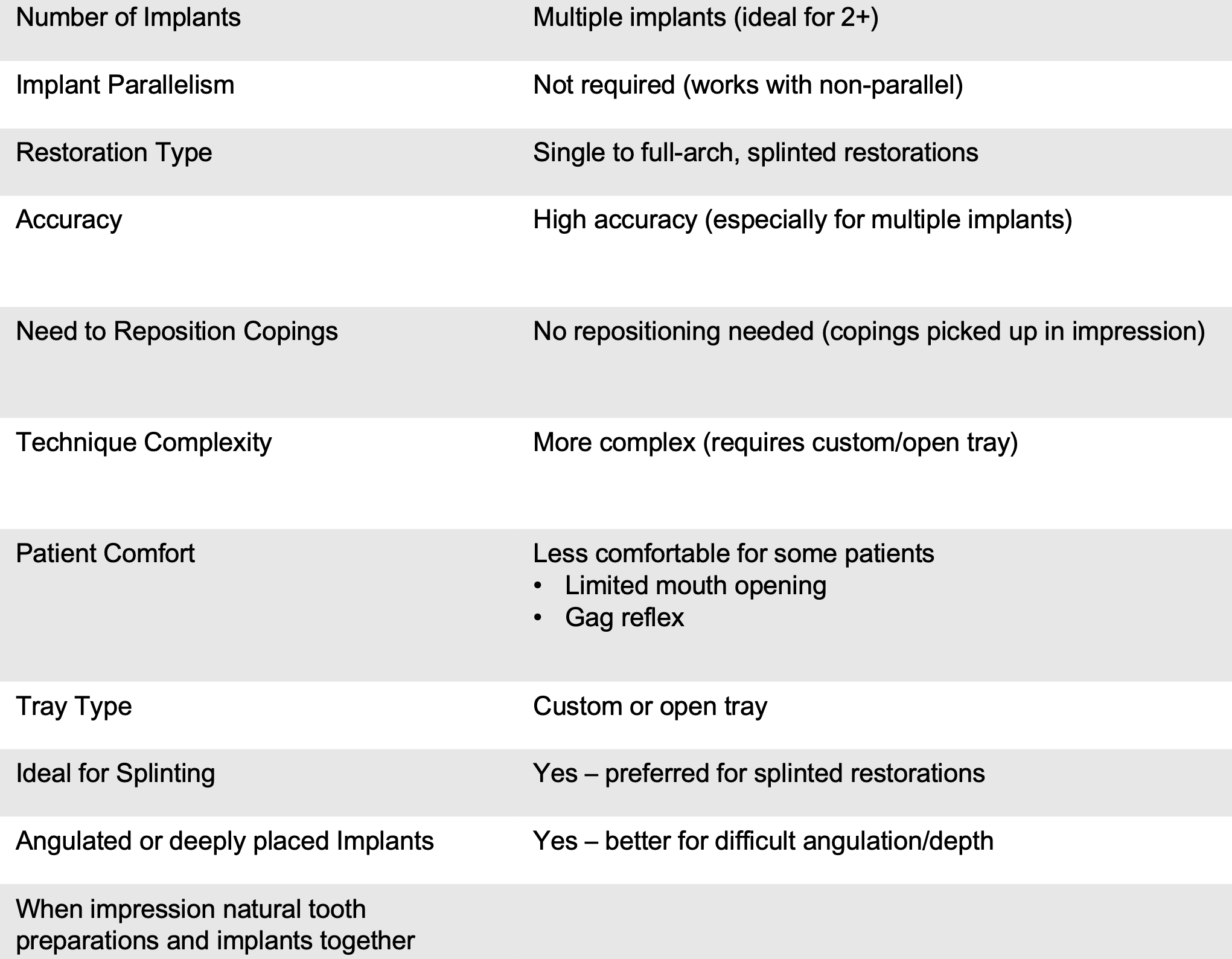
open tray
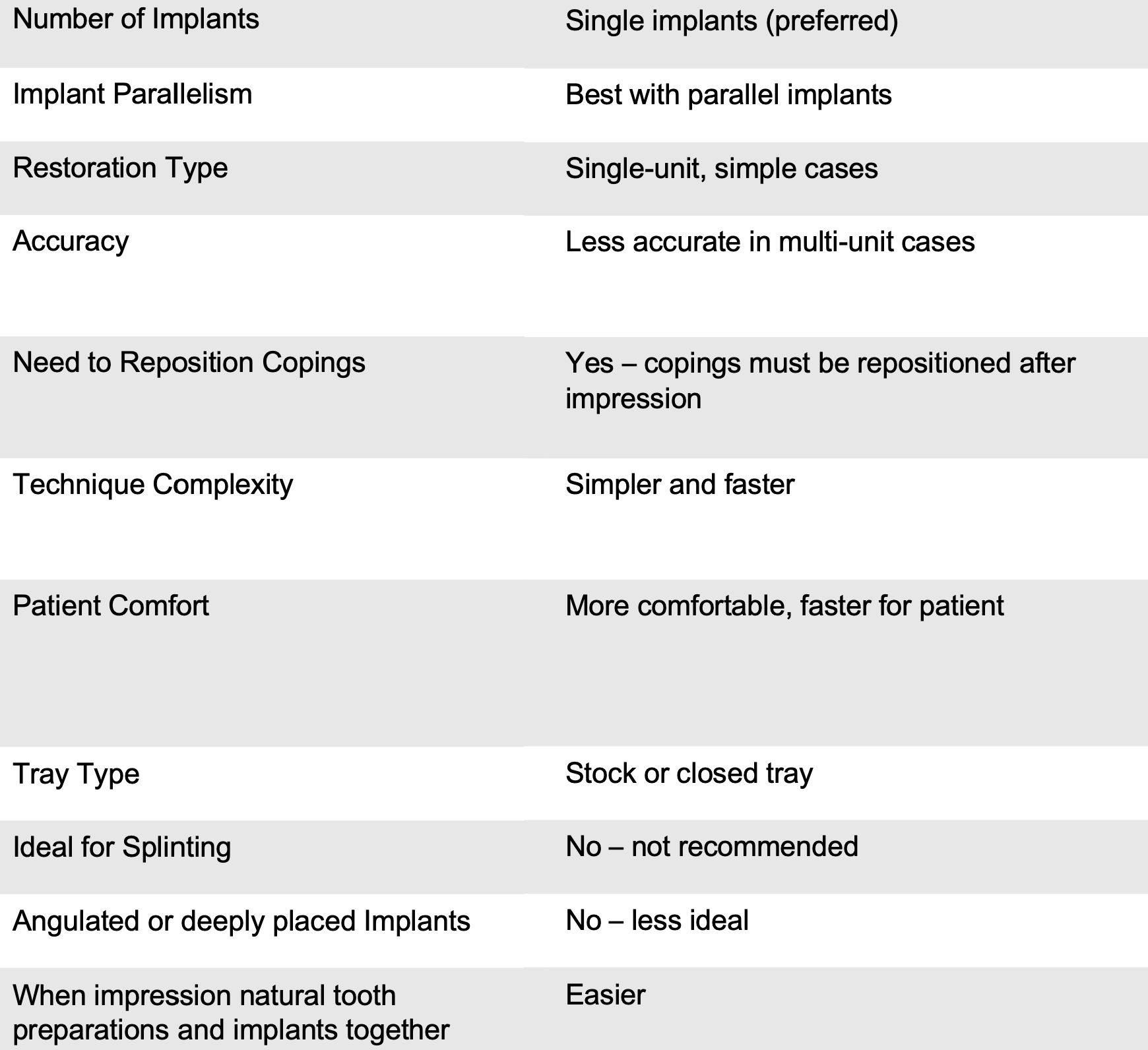
closed tray
Accurate casts can be made with either the open or closed tray impression technique for 3 implants angled up to ____ degrees
15 degrees
Situations in which there were 4 or more implants, more accurate impressions with which technique: the pick-up technique (open tray) or the transfer technique (closed tray)?
open tray/ pick-up technique
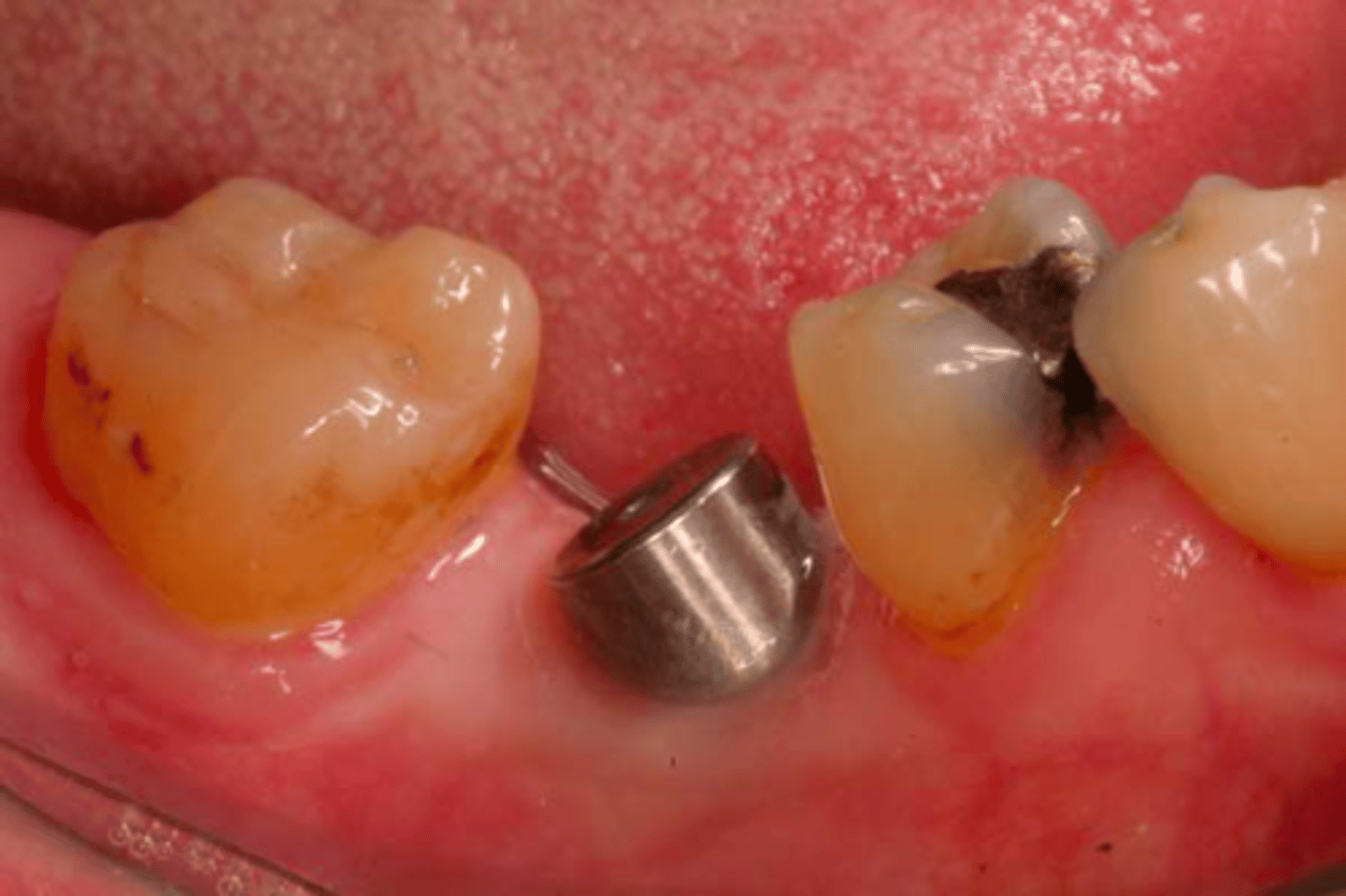
Which impression technique should be used here?
open tray/ pick-up technique
Which technique will reduce the effect of the implant angulation?
open tray/ pick-up technique
for multiple unit splinted restorations or FPDs accuracy of the cast must be checked (after/before) fabrication of the restoration(s) (!)
before
what can you use to verify the accuracy of a multiunit implant bridge?
Verification jig/index
*verification accuracy is especially important for multiple units only, must be checked before fabrication of restoration!
Define the following: Assembled recording of the positional relationship of implants made on a cast or in the mouth for interchangeable validation of fit
verification jig/index
What has the following characteristics?
Ensures Passive Fit: Multiple-unit splinted fixed implant-supported restorations, require a passive fit to avoid mechanical complications (e.g., screw loosening, framework fractures, bone loss from stress)
Checks Impression Accuracy: A jig helps verify that the impression and subsequent master cast accurately capture the spatial relationship and angulation of implants
Reduces Remakes and Adjustments: Catching inaccuracies early saves lab time, material cost, and chair time later
Fabrication: On the master cast, connect the implant analogs using GC pattern resin and temporary abutments
Sectioning (Optional): Section it before try- in
verification jig/index
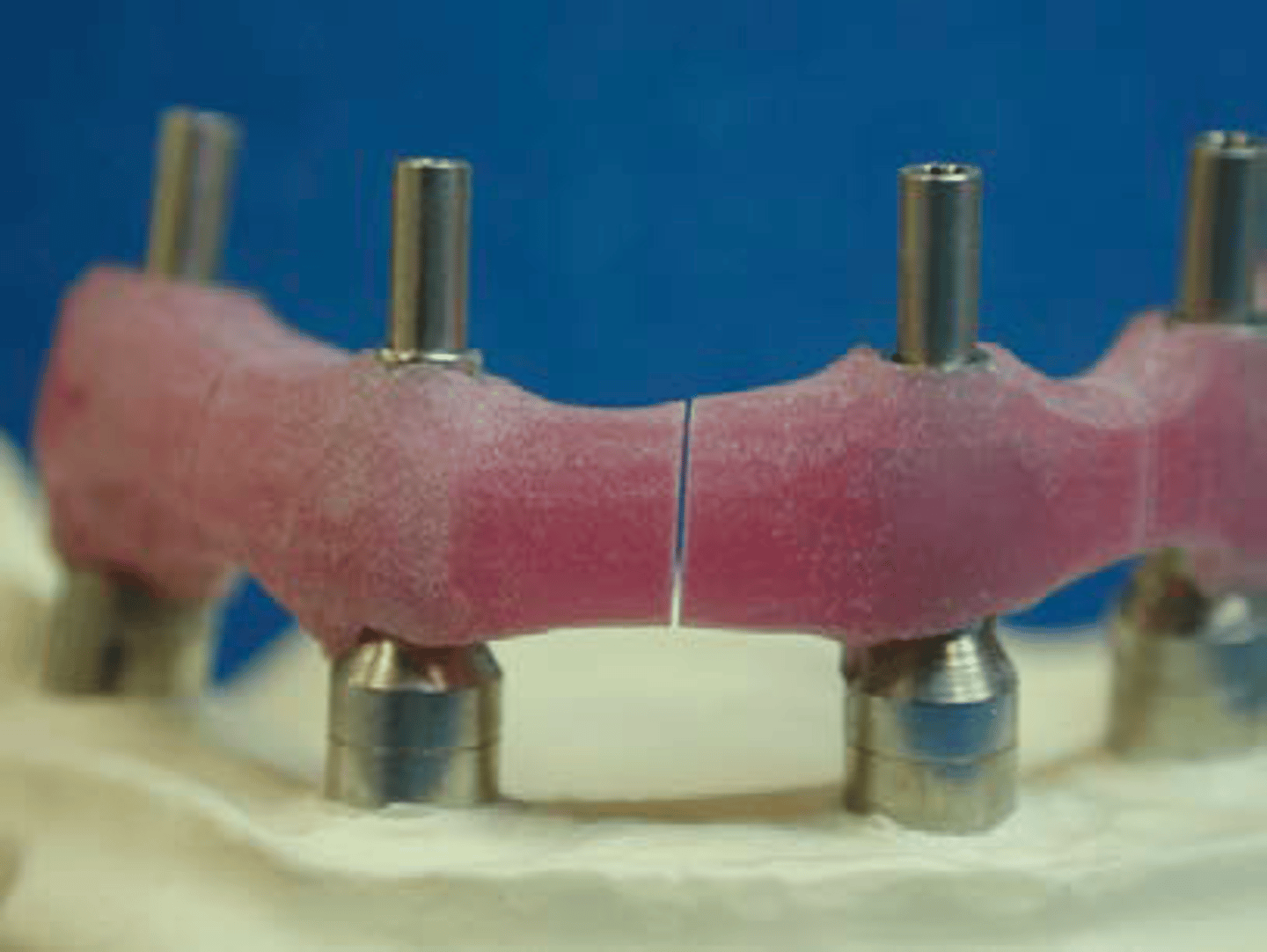
ID the method:
verification jig/index
ID the method:
Place the separate units onto the implants and tighten the screws
Connect the individual parts with GC pattern resin or a light cure material
Obtain radiographs if needed
Remove the jig from the mouth and reseat it on the master cast to check passive fit
verification jig/index
What do you do if the verification jig/index is a good fit? (!)
Proceed towards final restoration
What do you do if the verification jig/index is not a good fit? (!)
Correct the cast or remake the impression
(when you’ve put it on the cast and there is a gap)
What two things are connected on the model with pattern resin to make a verification jig?
Impression copings
Temporary abutments
what three elements are the development of CAD?CAM based around?
data acquisition ~ impression
data processing ~ prep of virtual cast and restoration design
manufacturing ~ fabrication of restoration
all in-office or lab
Define the following: Part of the scanner that has the camera, guided intraorally by the operator
Wand

Define the following: Scannable object used to accurately translate the position of an implant into a digital file for use in the digital design of an implant abutment
Scan body/scan post

Digital scans are read and stored in ______ format
Standard Tessellation Language

CBCTs are read and stored in ______ format
Digital Imaging and Communication In Medicine (DICOM)
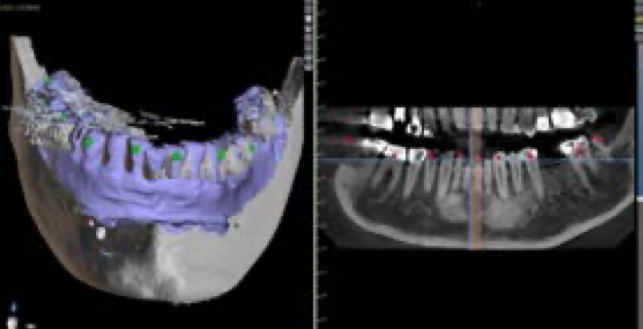
What mode of capture: requires stabilization of the wand?
stable image capture
What mode of capture: requires continuous movement of wand?
continuous image capture
What has the following characteristics?
Implant, implant abutment connection mechanism and implant platform specific
Made by implant manufacturers or CAD/CAM manufacturers
Scan body "impression copings" for scanners
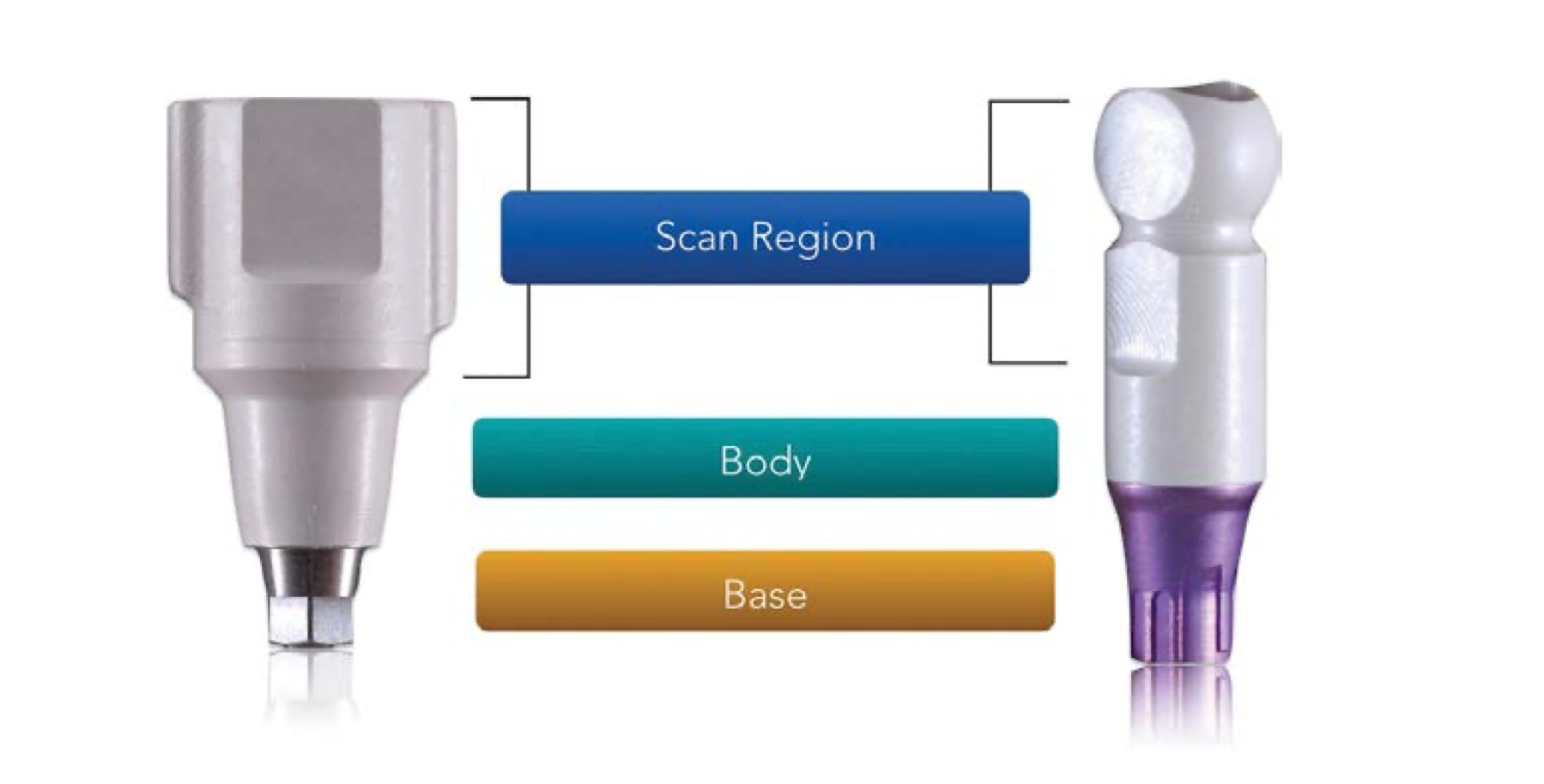
What has the following characteristics?
Serves the same purpose in digital design that the impression coping serves in the traditional impression and model technique
All are secured on the implant with screws
Can be 1 or 2 pieces (more operator error with 2 piece, communication with lab is critical)
Scan body
what are some disadvantages of digital implant scans:
Complete arch scans (particularly for mandible) may not be possible or accurate
Scans for removable prosthesis may not be possible or accurate
High initial/ acquisition cost
Learning curve
All of the following are advantages of what?
Real-time imaging
Easy repeatability
Step-by-step imaging of relevant segments
No need to disinfect and clean impressions or impression trays
Chairside analysis
Rapid communication and availability
Archivability
Material savings
Chairside CAD/CAM option
Color selection
Shorter overall treatment time
More comfortable for the patient
Easy bite registration
Digital implant scans
In the study by Lee & Gallucci, what did most people prefer: conventional or digital impressions?
Digital impressions
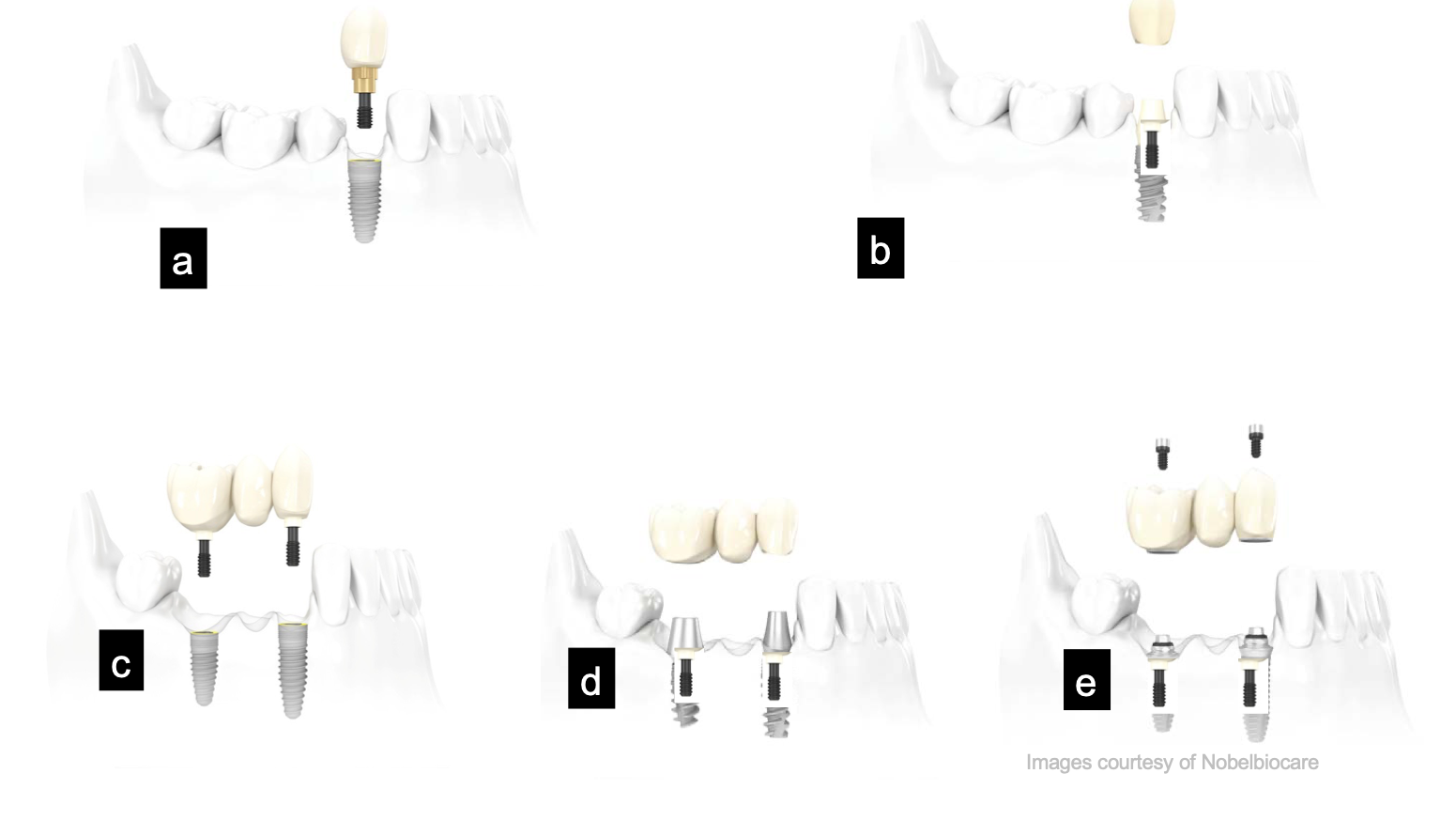
single vs multiple unit, implant or abutment supported, cement vs screw retained