homeostasis full topic
1/71
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
72 Terms
homeostasis
the maintenance of a dynamic equilibrium in the body, with small fluctuations over a narrow range of conditions
why is homeostasis important
the enzyme controlled reactions can only take place if the temperature is right
the concentration of chemicals such as glucose and sodium ions must be kept at a narrow range
negative feedback systems
a small change in one direction is detected by sensory receptors
effectors work to reverse the change and restore conditions to their base level
negative feedback systems work to reverse the initial stimulus
positive feedback systems
a change in the internal environment of the body is detected by sensory receptors, and effectors are stimulated to reinforce that change and increase the response
eg, blood clotting cascade - when a vessel is damaged, platelets stick to the damaged region and they release factors that initiate clotting and attract more platelets
if the kidneys are infected or affected by high blood pressure this may cause:
protein in the urine - if the basement membrane or podocytes of the bowman’s capsule are damaged, they no longer act as filters and large plasma proteins can pass into the filtrate and are passed out in the urine
blood in the urine - another symptom that the filtering process is no longer working
effects of the concentrations of urea and minteral ions in the body if the kidneys fail
loss of electrolyte balance - if the kidneys fail, the body cannot excrete excess sodium, potassium and chloride ions. This causes osmosis imbalances in the tissue and eventually death
build up of toxic urea in the blood - if the kidney’s fail, the body cannot get rid of urea and it can poison the cells
high blood pressure - the kidneys play an important role in controlling the blood pressure by maintaining the water balance of the blood.
weakened bones as the calcium/ phosphorus balance in the blood is lost
pain and stiffness in joins as abnormal proteins build up in the blood
Aneamia - the kidney’s are involved in the production of a hormone called erythropoietin that stimulates the formation of red blood cells.
How does glomerular filtration rate measure that there is an issue in the kidneys
GFR is estimated by a blood test to show the levels of creatine in the blood
if the levels of creatine in the blood goes up, it is a sign that the kidneys are not working properly
haemodialysis
involves the use of a dialysis machine in the hospital
blood leaves the patients body into the dialysis machine where it flows between partially permeable dialysis membranes
theres membranes mimic the basement membranes of the bowman’s capsule
on the other side of the membranes is the dialysis fluid. During dialysis, patients must lose urea and excess mineral ions but no glucose or useful mineral ions. This fluid contains normal plasma levels of glucose to ensure there is no net movement of glucose out of the blood + normal mineral ions levels so excess mineral ions diffuse out of the blood
dialysis fluid contains no urea meaning there is a steep concen gradient and much of the urea leaves the blood
the blood and dialysis fluid flow in opposite directions to maintain a counter current system
problems with treating kidney failure using a transplant
risk of rejections
antigens on the donor organ differ from the antigens of the recipient and the immune system is likely to recognise this. This can result in the rejection and destruction of the new kidney.
ways of reducing the risk of rejection of a kidney transplant
match the antigens of the donor and the kidney as closely as possible
recipient is given immunosuppresant drugs
immunosuppresent drugs prevent the patient from being able to properly response to infectious diseases
dialysis or transplant
dialysis is far more readily available
on dialysis patients have the manage their diet and need regular sessions on the machine
long term dialysis is expensive and may cause damage to the body
kidney transplants remove the restrictions of regular dialysis sessions
the main source of kidneys is from people who die suddenly from road accidents/ strokes/ heart attacks
there is a shortage of donor kidneys
the renal cortex
the dark outer layer of the kidney
where the filtering of the blood takes place
has a very dense capillary network carrying the blood from the renal artery to the nephrons
the medulla
lighter in colour
contains the tubules of the nephrons that form the pyramids of the kidney and then the collecting duct
the pelvis
the central chamber where the urine collects before passing down the ureter
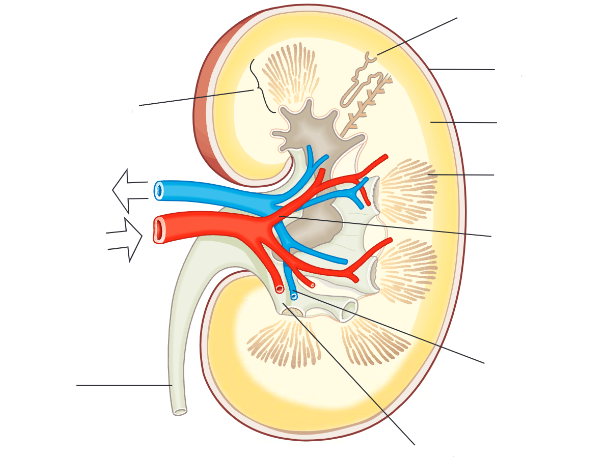
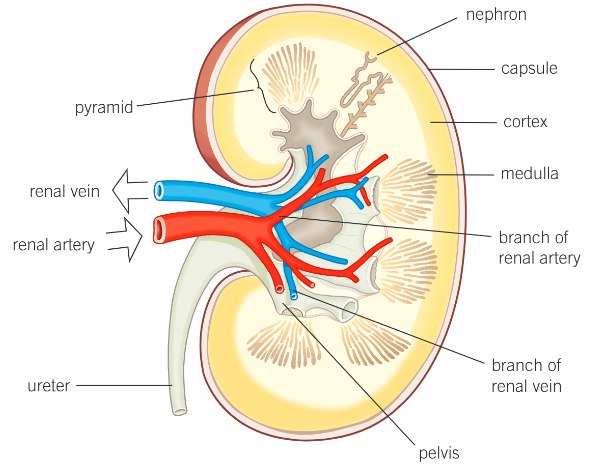
structure of the nephron
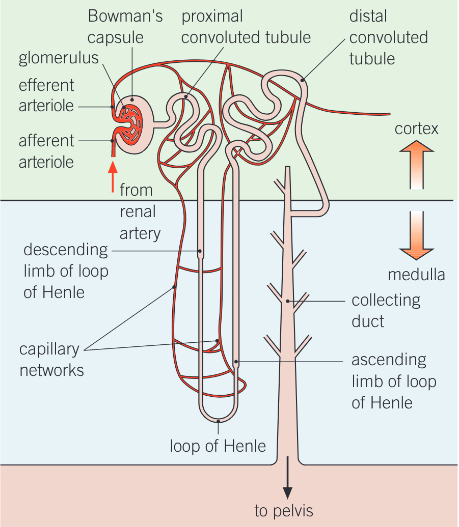
what is the bowmans capsule
cup-shaped structure that contains the glomerulus, a tangle of capillaries. Where ultra filtration takes place
what is the proximal convoluted tubule
the first, coiled region of the tubule after the bowman’s capsule, found in the cortex of the kidney. This is where many of the substances needed by the body are reabsorbed into the blood
what is the loop of henle
a long loop of tubule that creates a region with a very high solute concentration in the tissue fluid deep in the kidney medulla. The descending loop runs down from the cortex through the medulla to a hairpin bend at the bottom of the loop. The ascending limb travels back up through the medulla to the cortex
what is the distil convoluted tubule
the second twisted tubule where the fine tuning of the water balance of the body takes place. The permeability of the walls to wall varies with ADH
collecting duct
the urine passes down the collecting duct through the medulla to the pelvis. More fine-tuning of water balance takes place
the process of ultrafiltration
glomerulus is supplied with blood from a wide afferent arteriole and blood leaves through a narrower efferent arteriole
the forces blood out from the capillary wall which functions like a sieve
the fluid passes through the basement membrane which contains a network of collagen fibres and other proteins which act as a second sieve
most of the plasma contents pass through the basement membrane but the blood cells and many proteins are retained in the capillaries because of their size
the wall of the bowman’s capsule also involves special cells called podocytes that act as an additional filter
they have extensions called pedicels that wrap around the capillaries, forming slits to make sure that any cells, platelets or large plasma proteins that have managed to get through the epithelial cells do not get into the tubule itself
glomerular filtration rate
the volume of blood that is filtered through the kidneys in a given time
what happens in the proximal convoluted tubule
the glucose, amino acids, vitamins, and hormones are moved from the filtrate back into the blood by active transport
85% of sodium chloride and water are reabsorbed (sodium ions by active transport and water and chloride ions move passively down the concentration gradient)
once the substances have been removed from the nephron, they diffuse into the extensive capillary network which surrounds the tubules down steep concentration gradients
the concen gradients are maintained by the constant flow of blood through the capillaries
the filtrate reaching the loop of henle at the end of the proximal convoluted tubule is isotonic with the tissue fluid and blood
80% os glomerular filtrate has been selectively reabsorbed back into the body
adaptations of the cells lining the proximal convoluted tubule
they are covered with microvilli, greatly increasing the surface area over which substances can be absorbed
they have many mitochondria to provide the ATP needed in active transport systems
purpose of the loop of henle
allows mammals to produce urine more concentrated than their own blood
descending limb of the loop of henle
where water moves out of the filtrate down a concentration gradient
the upper part is impermeable to water but the lower point is permeable to water and runs down into the medulla
the concentration of sodium and chloride ions in the tissue fluid of the medulla gets higher and higher moving through the cortex to the pyramids, as a result of the activity in the ascending limb
the filtrate entering the descending limb of the loop of henle is isotonic with the blood. As it travels down the limb, water passes out of the loop by osmosis down a concentration gradient → the blood of the surrounding capillaries
the descending limb is not permeable to sodium and chloride ions and no active transport takes place
fluid that reaches hairpin bend is very concentrated (hypertonic to blood in capillaries)
acending limb of the loop of henle
the first section is very permeable to sodium and chloride ions and they move out of the concentrated solution by diffusion down a concentration gradient
in the second section, sodium and chloride ions are actively pumped out out into the medulla tissue fluid against a concentration gradient → produces high Na+ and Cl- ions concentration in medulla tissue
the ascending limb is impermeable to water so water cannot follow the chloride and sodium ions down a concentration gradient
the fluid left in the ascending limb become increasingly dilute, while the tissue fluid of the medulla develops the very high concentration on ions that is essential to produce concentrated urine
when fluid reaches the top of the ascending limb, it is hypotonic to the blood again
what happens in the distal convoluted tubule
the permeability of the walls of the tubule varies with ADH
the cells lining the distal convoluted tubule also have many mitochondria so they are adapted to carry out active transport
if the body lacks salt, sodium ions will be actively pumped out of the distsal convoluted tubule with chloride ions following down an electrochemical gradient
water can also leave the distal tubule, concentrating the urine, if the walls of the tubule are permeable in response to ADH
what happens in the collecting duct
the main site where concentration/ volume of urine is determined
water moves out of the collecting duct by diffusion down a concentration gradient as it passes through the renal medulla → urine becomes more concentrated
levels of sodium ions in surrounding fluid increases through the medulla to the cortex to the pelvis
this means water can be removed from the collecting duct all the way along its length, producing very hypertonic urine
what does ADH do
increases the permeability of the distal convoluted tubule and collecting duct to water
where is ADH released from
the pituitary gland
How does ADH cause an affect
Low water potential triggers more ADH, which binds to receptors on the collecting duct, triggering cAMP to insert aquaporins into membranes, increasing water reabsorption and producing concentrated urine
the events caused by cAMP which is relased from the actions of ADH
vesicles in the cell lining the collecting duct fuse with the cell surface membrane on the side of the cell in contact with the tissue fluid of the medulla
the membranes of these vesicles contain protein-based water channels and when they are inserted into the cell surface membrane, they make it permeable to water
this provides a route for water to move out of the tubule cells into the tissue fluid of the medulla and the blood capillaries by osmosis
what happens when ADH levels fall
levels of cAMP fall
the water channels are removed from the tubule cell membranes are enclosed in vesicles again
the collecting duct becomes impermeable to water once more, so no water can leave
this results in the production of large amounts of very dilute urine, and maintains the water potential of the blood and the tissue fluid
where are osmosreceptors
in the hypothalamus
what happens when water is in short supply
concentration of inorganic ions in blood increases
water potential of the blood becomes more negative
this is detected by the osmoreceptors in the hypothalamus
they send nerve impulses to the posterior pituitary which in turn releases stored ADH into the blood
the ADH is detected by receptors in the cells of the collecting duct and increases the permeability of the tubules to water
water leaves the filtrate in the tubules and passes into the blood in the surrounding capillary network
a small volume of concentrated urine is produced
what happens when there is an excess of water
blood becomes more dilute and its water potential becomes less negative
the change is detected by the osmoreceptors in the hypothalamus
nerve impulses to the posterior pituitary are reduced or stopped and so the release of ADH by the pituitary is inhibited
very little reabsorption of water can take place because the walls of the collecting duct remain impermeable to water
large amounts of dilute urine are produced
what hormones do pregnancy tests test for
hCG
how to make monoclonal antibodies
a mouse is injected with hCG so it makes the appropriate antibody
the B-cells that make the required antibody and then removed from the spleen of the mouse and fused with a myeloma, a type of cancer cell which divides very rapidly
this new fused cell is known as a hybridoma
each hybridoma reproduces rapidly. resulting in a clone of millions of ‘living factories’ which can produce the desired antibody
these monoclonal antibodies are collected, purified and used in a variety of ways
the stages of a pregnancy test
the wick is soaked in urine containing hCG
the test contains mobile monoclonal antibodies that have very small coloured beads attached to them. They will only bond to hCG. If hCG is present in the urine, it will bind to the beads and form a hCG/ anitbody complex
the urine carries on along the test structure until it reaches a window
here there are immobolised monoclonal antibodies arranged in a line which only bind to the hCG/ antibody complex
If the woman is pregnant, a line appears
the urine continues up through the test to a second window
there is a line of immobilised monoclonal antibodies that bind only to mobile antibodies, regardless of whether they are bound to hCG or not. This line shows whether the test is working
how to test for anabolic steroids
vaporise the urine with a known solvent
pass it along a tube
the lining of the tube absorbs the gases and it analysed to give a chromatogram that can be read to show the presence of drugs
how are urine samples tested for drugs
first sample may be tested by an immunoassay, using monoclonal antibodies to bind to the drug or its breakdown product
if this is positive, a second sample may be ran through a gas chromatograph/ mass spectrometer to confirm the presence of the drug
main metabolic waste products in mammals
carbon dioxide - one of the waste products of cellular respiration which is excreted from the lungs
bile pigments - formed from the breakdown on haemoglobin from old red blood cells in the liver. They are excreted in the bile from the liver into the small intestine via the gall bladder and the bile duct
nitrogenous waste products (urea) - formed from the breakdown of excess amino acids by the liver. All mammals produce urea as their nitrogenous waste. Fish produce ammonia while birds and insects produce uric acid
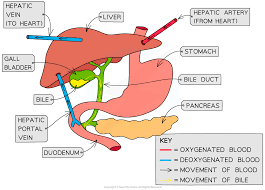
what vessel supplies blood to the liver
hepatic portal vein (blood loaded with products of digestion)
hepatic artery (oxygenated blood)
parts of liver cells (hepatocytes)
large nuclei
prominent golgi apparatus
lots of mitochondria
sinusoids
the spaces where blood from the hepatic artery and hepatic portal vein are mixed
Kupffer cells
act as macrophages in the liver cells - help to protect against disease
secretion of bile
the hepatocytes secrete bile from the breakdown of the blood into spaces called canaliculi
from these, blood drains into the bile bile ductules which take it to the gall bladder
carbohydrate metabolism
when blood glucose levels rise, insulin levels rise and stimulate hepatocytes to convert glucose to the storage carbohydrate glycogen
when blood sugar levels fall, the hepatocytes convert the glycogen back to glucose under the influence of the hormone glucagon
deaminaton of excess amino acids
the removal of an amine group group from a molecule
the body cannot store proteins/ amino acids
the amino group of an amino acid is removed and converted into ammonia
the remainder of the amino acid can then be fed into cellular respiration or converted into lipids for storage
transamination
the conversion of one amino acid into another
the ornithine cycle
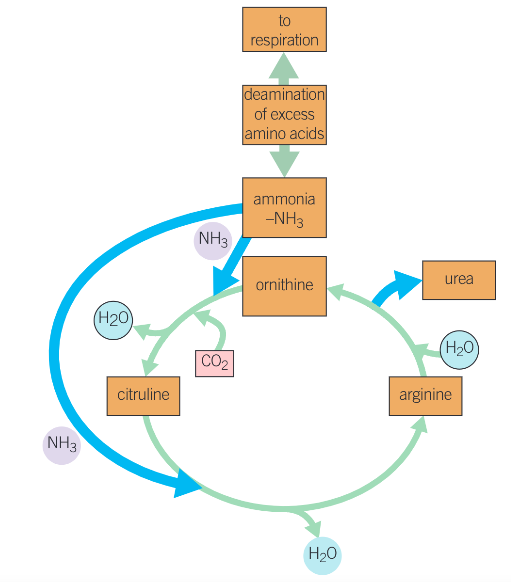
detoxification in the liver
eg, breakdown of hydrogen peroxide using the enzyme catalyse
the liver detoxifies ethanol using the enzyme alcohol dehydrogenase to break the ethanol into ethanal. Ethanal is converted to ethanoate which may be used to build up fatty acids or in cellular respiration
diagram of the structure of the liver
detecting temperature changes
peripheral temperature receptors are in the skin and detect changes in the surface temperature
temperature receptors in the hypothalamus detect the temperature of the blood deep in the body
the combination of the two allows the brain to pre-empt possible problems and maintain the body temperature from within 1 degree
behavioural ways for endotherms to maintain their body temperature (passive)
basking in the sun
pressing themselves to warm surfaces
wallowing in water or mud
digging burrows
hibernating during cool weather
humans have additional behavioural adaptations of wearing clothes
vasodilation
arterioles near the surface of the skin dilate when the temperature rises
the vessels that directly connect arterioles and venules constrict which forces blood through the capillaries
the skin flushes and cools as a result of increased radiation
increased sweating
as sweat evaporates from the surface of the skin, heat is lost, cooling blood below the surface
reducing the insulating effect of hair and feathers
As the body temperature begin to increase, the erectors pili muscles in the skin relax
as a result, the hair of feathers of the animals lie flat to the skin which avoids trapping an insulating layer of air
animals may have pale fur or feathers to reflect the heat
decreased sweating
the rate of sweating decreases and will stop entirely which reduces cooling by the evaporation of water from the surface of the skin
raising the body hair or feathers
as the body temperature falls, the erector pili muscles in the skin contract, pulling the hair of feathers of the animal
this traps and insulating layer of hair, and so reduces cooling through the skin
shivering
the rapid, involuntary contraction of relaxing of the large voluntary muscles in the body
many animals have adaptations to minimise their SA.V ration to reduce cooling
adaptations of polar bears
small ears and fur on their feet to insulate them from the ice
the hairs are hollow so trap a permanent layer of insulating air
their skin is black
they have a thick layer of fat under the skin
they dig dens in the snow which females give birth to cubs in
controlling thermoregulation
the heat loss centre
activates when the temperature of blood flowing through the hypothalamus increases
sends impulses through motor neurons to effectors in the skin and muscles, triggering responses that act to lower the core temperature
the heat gain centre
activated when the temperature of the blood flowing through the hypothalamus decreases
sends impulses through the nervous system to effectors in the skin and muscles, triggering responses that act to raise the core temperature
what is thermoregulation
the maintenance of a relatively constant core body temperature to maintain optimum enzyme activity
changes the affect the bodily temperature of an organism
exothermic chemical reactions
latent heat of evaporation - objects cool down as water evaporates from a surface
radiation - the transmission of electromagnetic waves to and from the air, water, or ground
convection - the heating and cooling by currents of air or water
conduction - heating as a result of the collision of molecules
what are ectotherms
they use their surroundings to warm their bodies - their core temperature is heavily dependant on their environment
many ectotherms live in water and do not need to thermoregulate due to the high specific heat capacity of water
endotherms
eg. mammals and birds
rely on their metabolic processes to warm up and they usually maintain a very stable core body temperature regardless of the outside temperature
they have a high metabolic rate
they can survive in a wide range of environments
behavioural responses to regulate body temperature
basking in the sun so the maximum surface area is exposed to the sun
insects spread their wings to increase the available surface area exposed to the sun to get warm enough to fly
increase their body temperature through conduction by pressing their bodies against the ground
contracting their muscles and vibrating to increase cellular metabolism to increase their body temperature
to cool down they can seek shade or hide in rocks or dig burrows
physiological responses to regulate body temperature
lizards living in colder climates tend to be a darker colour
ectotherms alter their heart rate to increase or decrease the metabolic rate