Infection- associated carcinogenesis and prevention
1/16
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
17 Terms
What are the three major mechanisms of viral carcinogenesis?
Signalling mimicry
DNA damage response (DDR) disruption
chronic inflammation.
What is signalling mimicry in viral carcinogenesis?
Viral proteins hijack host signalling pathways controlling growth and survival, mimicking oncogenic signalling.
How does viral activation of the DNA damage response promote cancer?
DDR activation increases genomic instability, accelerating accumulation of oncogenic mutations.
How does chronic viral infection promote carcinogenesis?
Persistent inflammation → Reactive oxidative species (ROS) → DNA damage → fibrosis → malignant transformation.
What is the role of HPV E6 in cervical cancer?
E6 degrades p53 and activates telomerase, promoting immortality.
What is the role of HPV E7 in cervical cancer?
E7 degrades Rb, releasing E2F activating p53
What HBV protein contributes to hepatocellular carcinoma?
HBx antigen, which interferes with p53 and promotes proliferation.
What are oncolytic viruses?
Viruses engineered to selectively infect and lyse tumour cells while stimulating anti‑tumour immunity.
Name three mechanisms by which bacteria induce carcinogenesis.
Chronic inflammation
genotoxin production
immune dysregulation
carcinogenic metabolites.
What is colibactin and why is it important?
A genotoxin produced by E. coli that causes DNA double‑strand breaks.
How can bacteria be used therapeutically in cancer?
By stimulating innate/adaptive immunity, inhibiting angiogenesis, or delivering therapeutic molecules.
Which parasite is linked to Burkitt lymphoma?
Plasmodium falciparum (via malaria‑induced immune dysregulation)
How does Toxoplasma gondii exert anti‑cancer effects?
By increasing cytotoxic T‑cell activity and enhancing MHC I/II expression
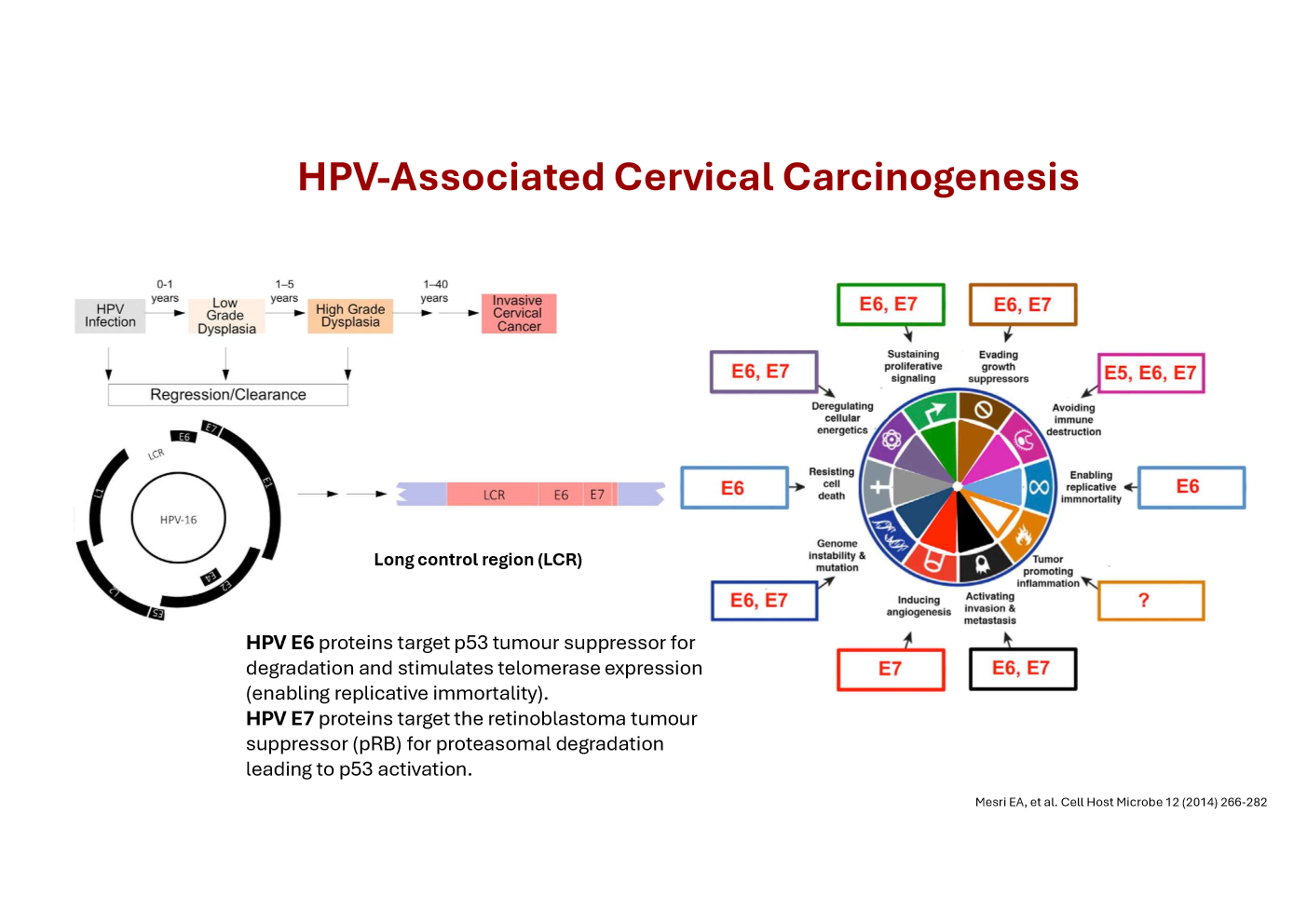
Describe the mechanism of HPV associated carcinogenesis
E7 degrades pRb → releases E2F → uncontrolled S‑phase entry.
E6 degrades p53 → no apoptosis, no DNA‑damage checkpoint.
E6 activates telomerase (hTERT) → replicative immortality.
E5 enhances growth‑factor signalling + reduces immune detection.
Viral genome integration disrupts E2 → ↑↑ E6/E7 expression.
Loss of p53 + pRb → genomic instability + mutation accumulation.
Persistent infection → CIN1 → CIN2 → CIN3 → invasive carcinoma.
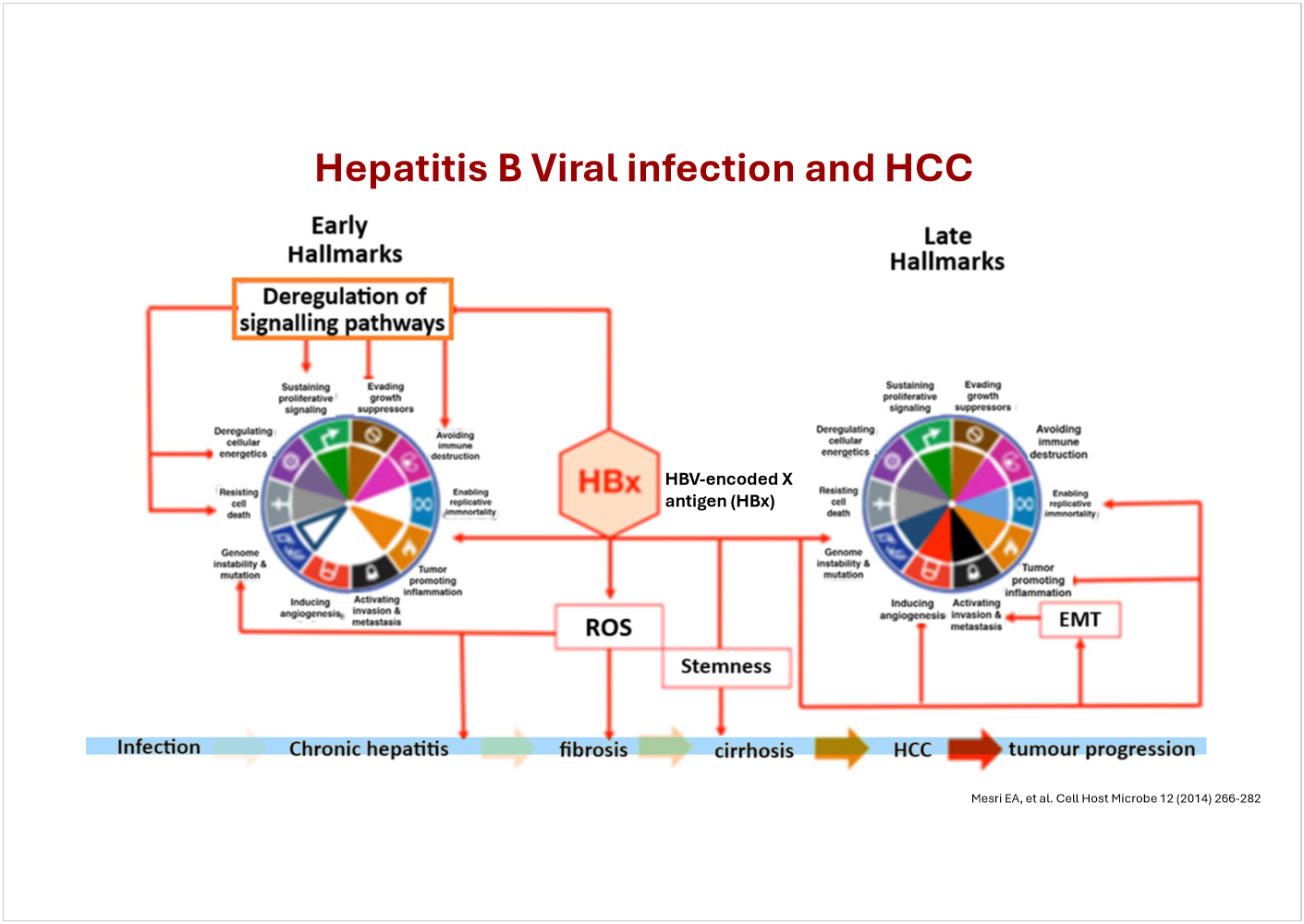
Describe how Hepatitis B viral infection can lead to hepatocellular carcinoma
HBx protein drives oncogenic signalling.
Chronic inflammation → repeated liver injury + regeneration.
↑ ROS → DNA damage + genomic instability.
Deregulated pathways → ↑ proliferation, ↓ apoptosis, immune evasion.
Stemness promoted → cells become more mutation‑prone.
Fibrosis → cirrhosis creates a pro‑cancer microenvironment.
EMT + late hallmarks accelerate tumour progression.
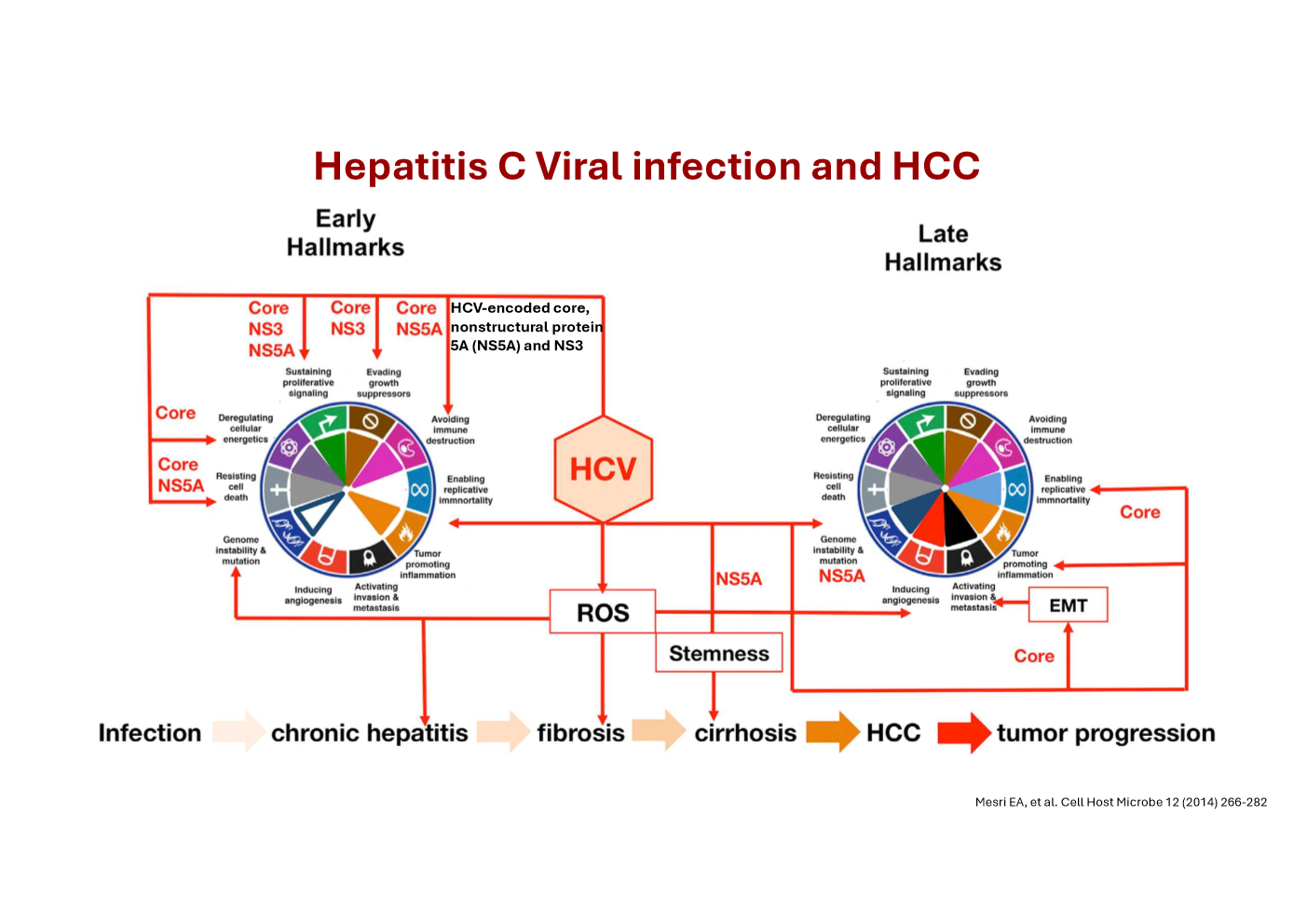
Describe how Hepatitis C viral infection can lead to hepatocellular carcinoma
Core/NS3/NS5A proteins drive oncogenic signalling.
Chronic inflammation → repeated injury + regeneration.
↑ ROS → DNA damage + genomic instability.
Deregulated pathways → ↑ proliferation, ↓ apoptosis, immune evasion.
Stemness promoted → mutation‑prone cells.
Fibrosis → cirrhosis → pro‑cancer microenvironment.
EMT + late hallmarks → tumour progression.
Why doesn’t HPV E7 activation of p53 prevent cancer?
E7 destroys pRb, causing uncontrolled proliferation; this would activate p53 as a safety response, but HPV E6 simultaneously degrades p53, removing both tumour‑suppressor pathways and enabling carcinogenesis.