Physiology lecture 27
1/28
Earn XP
Description and Tags
Gut function, saliva and the stomach
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
29 Terms
processing of food
Motility - mechanical breakdown and controlled movement along gut
Secretion - addition of enzymes, electrolytes etc.
Digestion - chemical breakdown
Absorption - transport proteins
Excretion - secretion of metabolic waste products and xenobiotics, and elimination of faeces
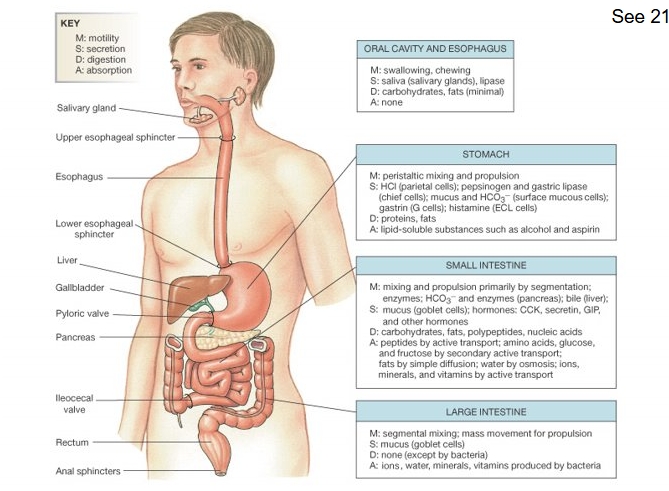
Compartments of GI tract
Hollow tube
Oral cavity and easophagus (only non mucosal part)
Lower esophageal sphincter not as effective as other spincters
Stomach - around 25% of fat digestion (gastric lipase)
Small intestine
Large intestine
All have roles in MDSA (motility, digestion, secretion and adsorption)
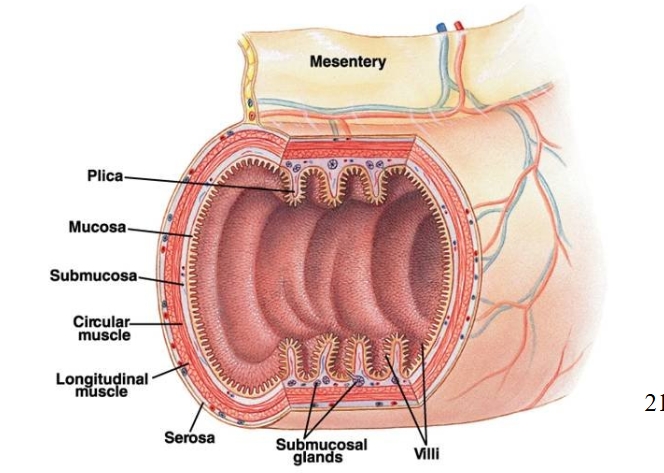
structure of gut tube
has mucosa and submucosa secreted from glands
layers of muscle to aid movement and motility
Large surface area due to plica, villi and microvilli
Regulation of gut function
Neural (neuralcrine) - autonomic NS, vagus nerves, enteric NS
Hormonal (endocrine) - dispersed entero-endocrine cells
Local (paracrine)
E.g. histamine
Three key stages of regulation
Cephalic
Gastric
Intestinal
saliva
Function
composition
control of saliva
Saliva functions
Lubrication - fluid and mucus
Digestion - amylase and R proteins
Solution
Moistness
Protection - fluid and bicarbonate, lysozyme, immunoglobulins
salivary glands
3 pairs account for 90% of saliva
Parotid glands - serous (watery), amylase
Sublingual and submandibular glands - mixed secretion (serous and mucus)
10% from minor glands - mucus, mucins
Total secretion around 1.5 litres a day
salivary gland structure
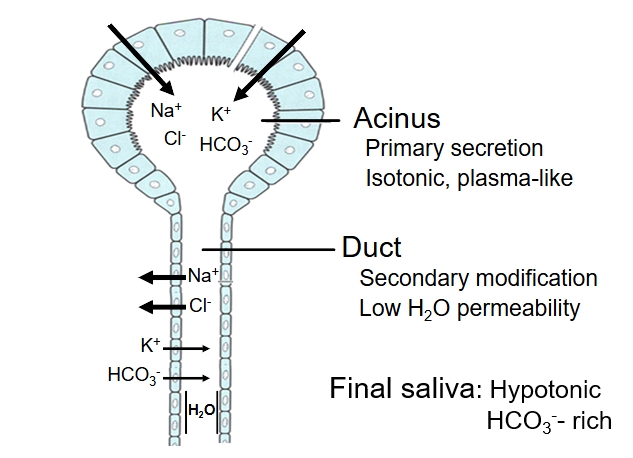
salivary fluid secretion
primary fluid from acinar epithelial cells - isotonic, plasma like
Secondary ductal modification - Na+Cl- reabsorption, K+ HCO3 secretion, ducts impermeable to water therefore final saliva is hypotonic and bicarb rich
control of salivation
cephalic phase (unconditioned and conditioned) - sight, smell, taste and thought of food
Parasympathetic (cholinergic) - cranial nerves VII and IX (NOT VAGUS), large volume
Sympathetic (noradrenergic) - smaller volume rich in enzymes and mucus
stomach to know
gastric functions, structure, gastric juice comp, control
gastric functions
Reservoir
Mixing food with gastric secretions
Digestion - mechanical, chemical
Controlled gastric emptying - moves food (chyme) to duodenum
Protection - bactericidal, mucus and bicarbonate
Structure of stomach
Fundus, body, then antrum
Movement controlled by pyloric sphincter (more effective than esophageal sphincter)
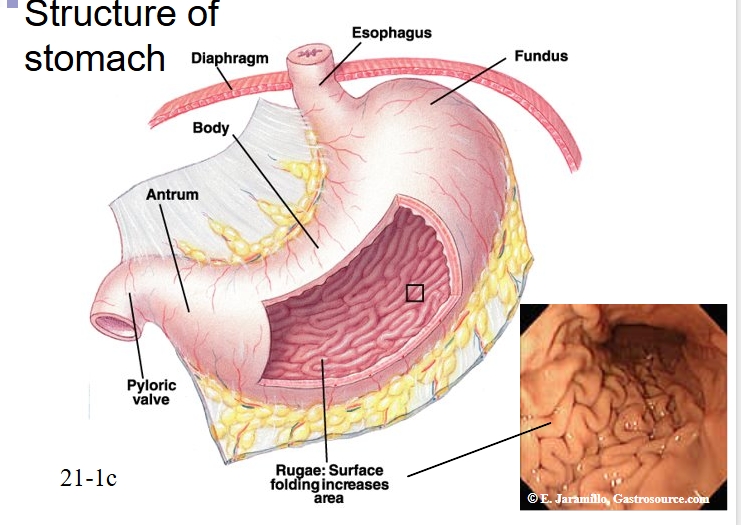
Microanatomy of stomach
Muscles, lymphs, arteries and veins
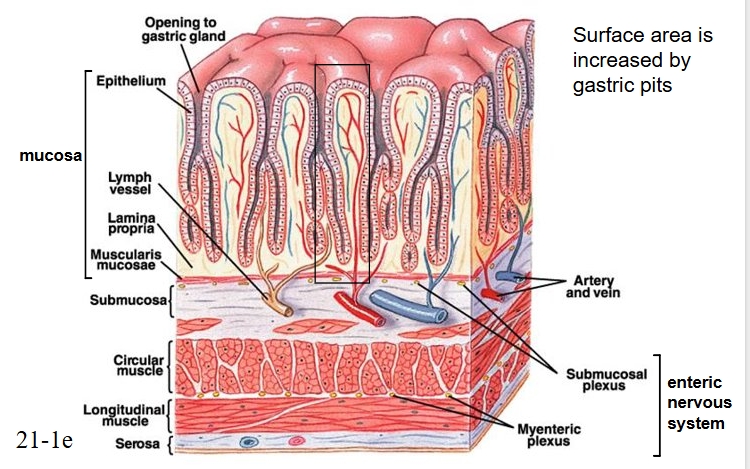
cells in gastric mucosa
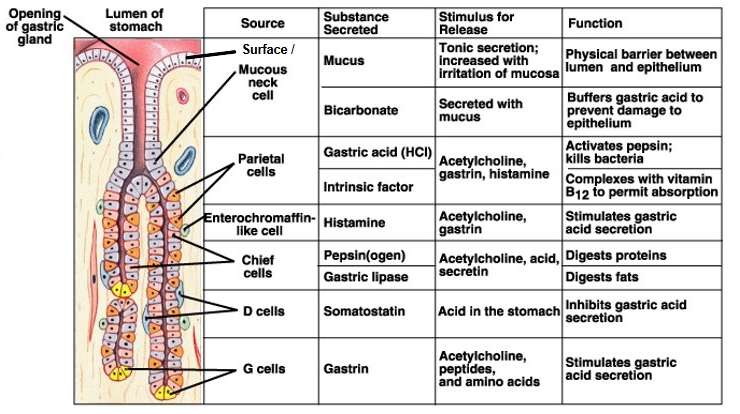
Composition of gastric juice
HCl - parietal cells
Pepsinogen to pepsin - chief cells
Mucus and bicarbonate - mucus neck and surface epithelial cells
intrinsic factor - parietal cells
Around 2 litres produced a day
parietal cells
also known as oxyntic
present in antrum and body
Secrete gastric acid and intrinsic factor
Stimulated
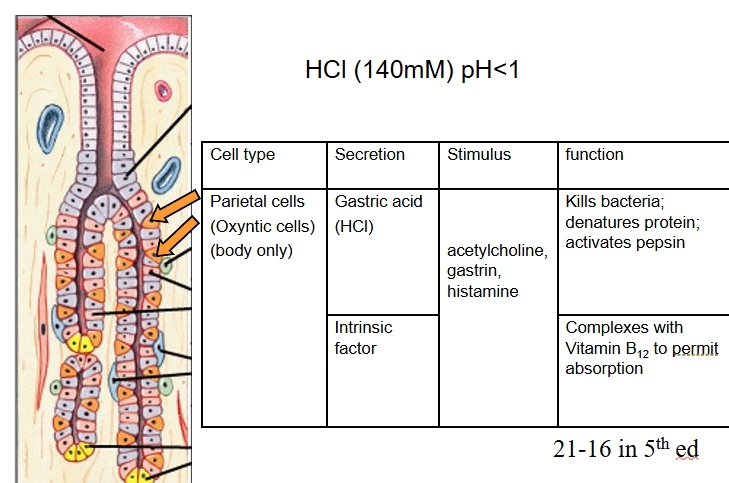
parietal cells in action
carbonic anhydrase converts water and carbon dioxide into H+ and bicarbonate ions
Proton pumps allow H+ to enter stomach lumen - also contain transporters for potassium to facilitate efflux from parietal cell
Bicarbonate secreted out through a chloride transporter into interstitial fluid
Proton pump inhibitors like omeprazole work to attempt to prevent acid reflux from causing issue
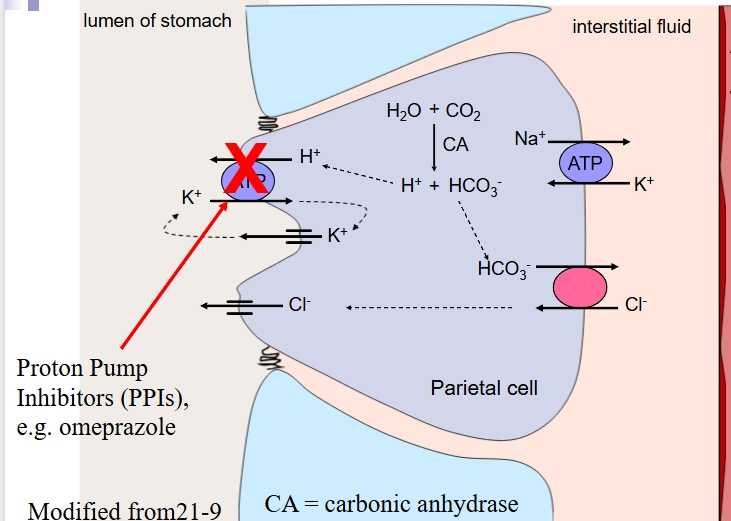
what do parietal cells secrete?
HCl
Carbonic anhydrase - catalyses formation of H+
Apical membrane
H+,K+-ATPase - Primary proton pump
K+ channels - Supplies K+ for recycling through the proton pump
Cl- channels - Supplies anion for HCl
Basal membrane
Na+/K+-ATPase
Cl-/HCO3- exchange
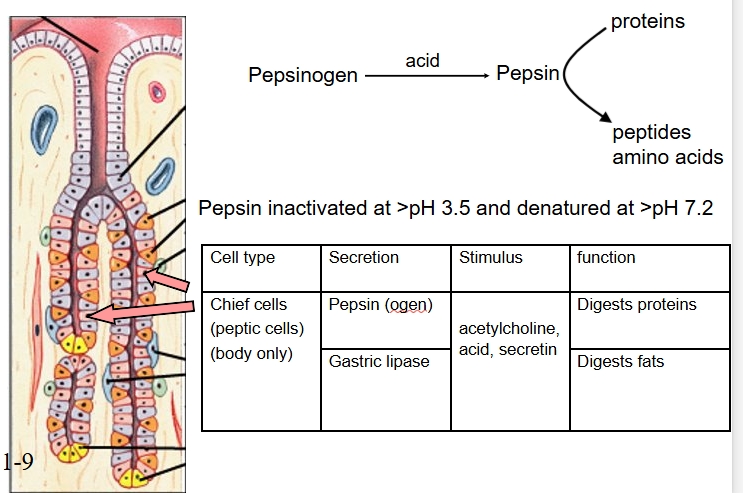
Chief cells
Or peptic cells, in body and antrum
Secretes pepsin and gastric lipase for digestion of proteins and fats
Ach, acid, secretin cause stimulation of chief cells
pepsinogen converted to pepsin by acid which then digests proteins to peptides and AAs
pepsin mostly inactivated at pH above 3.5 and denatured at 7.2 (irreversibly)
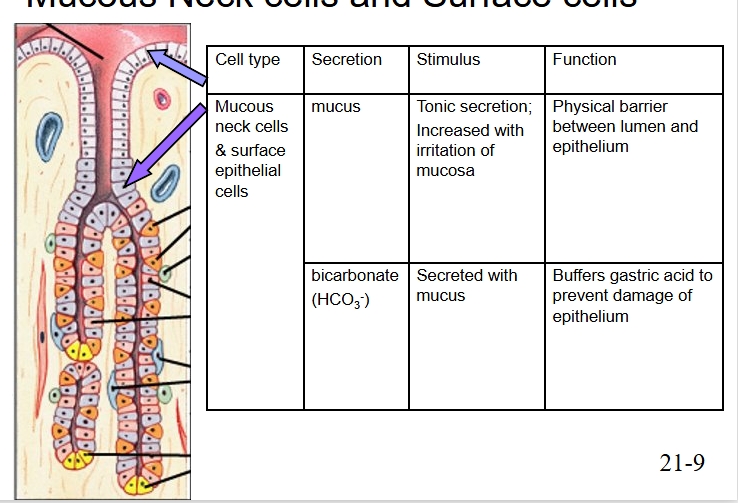
Mucus neck cells and surface cells
Secrete mucus and bicarbonate
Stimulated for mucus secretion by tonic secretion or irritation of mucosal layer
Bicarb secreted with mucus
Mucus provides physical barrier between lumen and epithelium
Bicarb buffers gastric acid to prevent epithelial damage
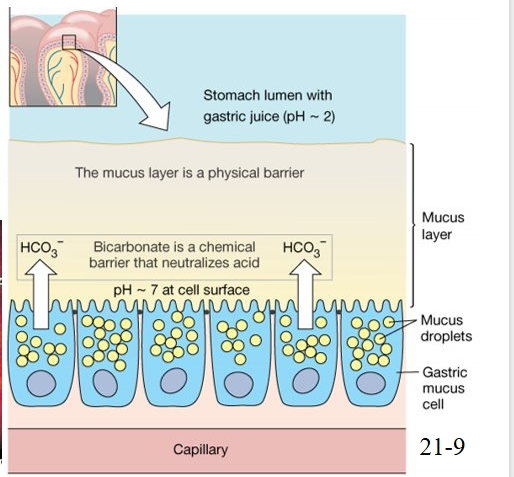
how stomach prevents autodigestion
mucus-bicarbonate barrier
if this doesn’t happen peptic ulcers can form
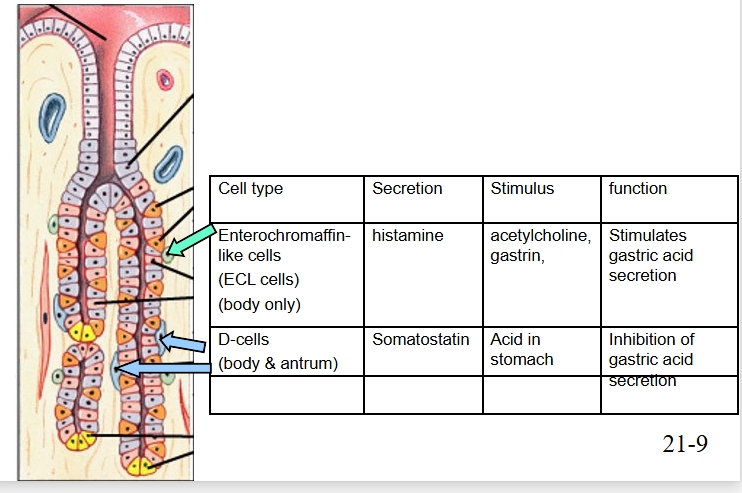
control of perietal cell function
Direct and indirect chemical regulators:
Histamine from ECL cells
Somatostatin from D cells
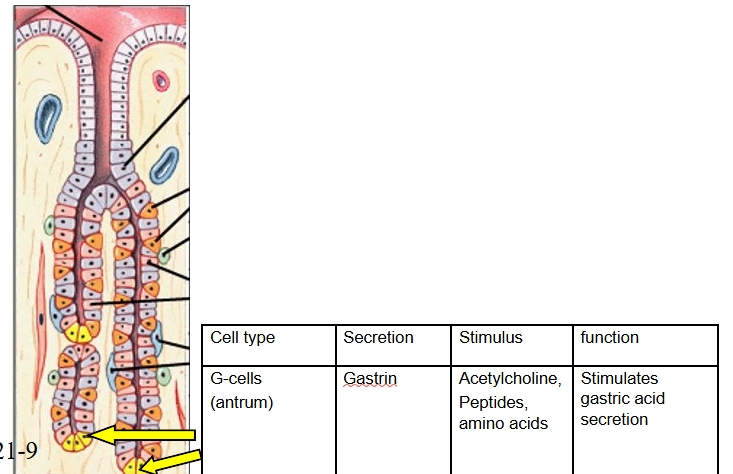
Gastrin from G cells
Acetylcholine from vagus and enteric neurons
ECL and D cells
G cells
H2 receptor inhibitor
Cimetidine
control of parietal cells
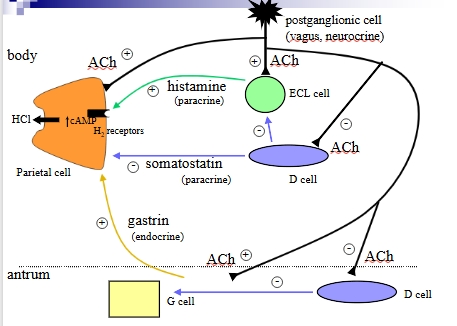
Overview of control mechanisms
Cephalic phase
Sight, smell, taste & thought of food
Vagal efferent nerves
direct effect
histamine release
gastrin release
Gastric phase
Food in the stomach (stretch & chemical nature)
Gastrin release
Negative feedback inhibition by acid
somatostatin release
Intestinal phase
Inhibitory
LOs
List the functions of saliva
Describe the mechanisms of saliva secretion
Explain the control of saliva secretion
List the functions of the stomach
Explain the mechanism of gastric acid secretion
Give an account of the control of gastric acid secretion