immunology pt 2 electric boogaloo
1/72
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
73 Terms
what do we study in immunology
how does out body fight and defeat pathogens
examples of pathogenic viruses
influenza
measles
Hepatitis B and C
HIV (Human immunodeficiency virus)
examples of pathogenic bacteria
staphylococcus aureus
neisseria gonorrhoeae
bordatella pertussis
examples of pathogenic protozoa
giardia
leishmania
plasmodium
examples of pathogenic fungi
candida albicans
cryptococcus neoformans
aspergillus
examples of pathogenic worms
schistosomes
helminths
immunology
the study of mechanisms of defence
immune response
the responses that we make against pathogens
immunity
the state of protection from infectious disease
how is immunity to pathogens achieved- what is involved?
innate and adaptive immunity working together to first eliminate pathogen and remember pathogen
they need each other to work, they cannot work separately
innate immunity is the immediate response
adaptive immunity is activated approx 4 days later
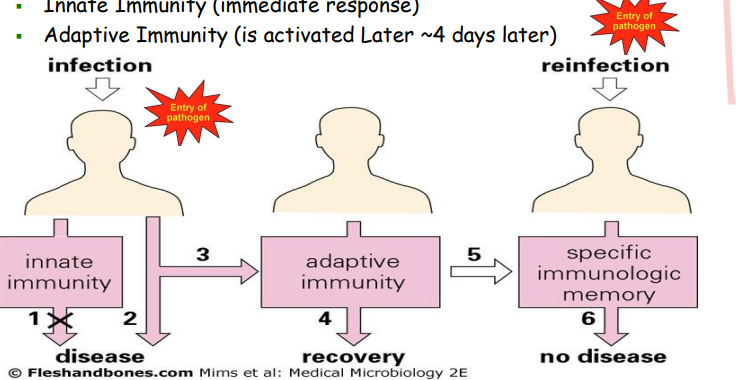
innate immunity
immediate response
antigen non specific
no memory
components: barriers eg skin, cells eg phagocytes, non cellular eg cytokines (small proteins secreted)
adaptive (acquired) immunity
approx 96 hours after entry of pathogen
antigen specific
has memory response
components: cells eg B and T cells, humoral→ antibodies ( produced by B cells that bind pathogen to eliminate it from body and cytokines also produced by B and T cells
cells of innate immune response vs adaptive
monocytes B and T lymphocytes
eosinophil
neutrophil
macrophage
dentritic cell
natural killer (NK) cell
- Antibody based (humoral) immunity
- T cell based (cell mediated) immunity
- Both are closely linked and based on lymphocyte
- Any molecule that can be recognised by the adaptive immune response
- Usual antigens are proteins, glycoproteins and polysaccharides of pathogens, antigens include protien coats of viruses, bacterial surface proteins, pollens, nickel and other allergens, vaccines….
- Phagocytosis
- Antiviral responses (interferons)
- Antigen presentation leads to the activation of T cells
- Defence against parasitic infections
- Tears/ saliva
- Stomach acid
- Mucus linings
- Skin and mucosal epithelial
- Neutrophil-- released into blood and die within hours
- Macrophage-- found in tissues
- Dendritic cell
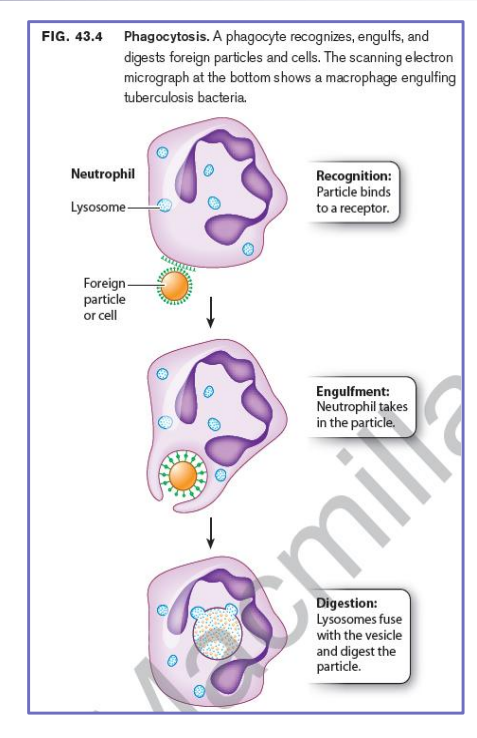
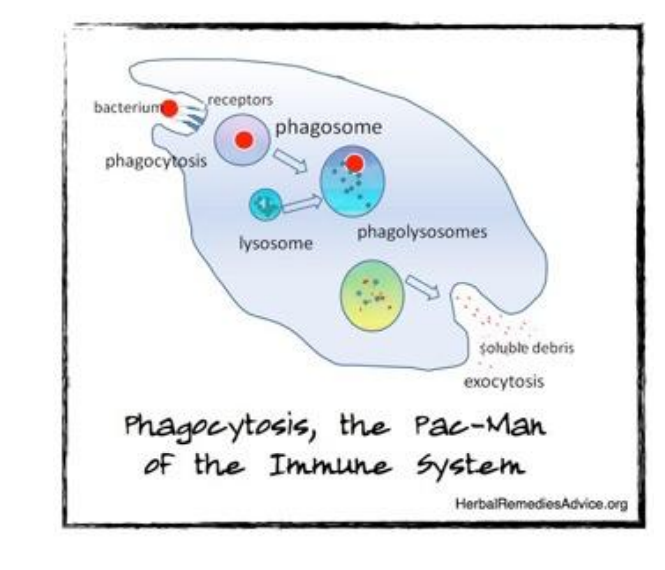
- Bacterium binds to cell surface receptors on the phagocyte, inducing engulfment of the bacterium into a vesicle called a phagosome.
- This then fuses with lysosomes, now called a phagolysosome, which contains toxic small molecules and hydrolytic enzymes that kill and degrade the bacterium
- Tissue resident immune cell ( derived form blood monocytes)
- Cytoplasmic granules
- Primary function-- patrol tissues to kill bacteria and clear dead cells
- Attracted by chemokines
- Recognise bacteria
- Eat bacteria to clear ( phagocytosis)
- Eat dead/ dying cells
- Attract other leukocytes
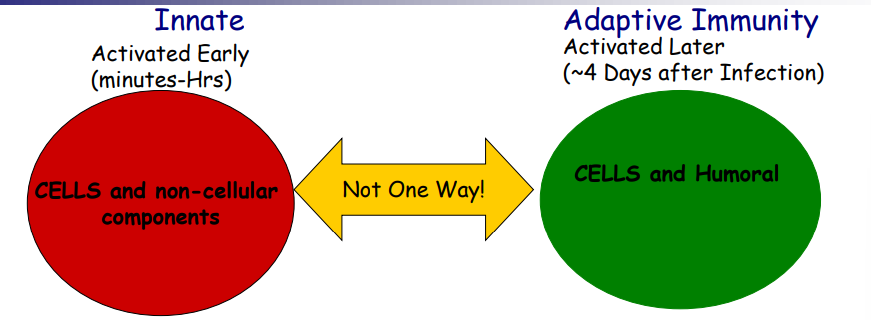
- Innate activated first following pathogen entry
- Innate-- non cellular components includes cytokines
- Adaptive the response learns and improves with time
- Part of innate activation response leads to activation of cells from adaptive immunity-- which can heighten the activities from innate cells
- Humoral (fluid component) normally reserved for the antibody response generated by B cells
Where do B and T lymphocytes mature?
Bone marrow and Thymus
- Each B cell expresses a specific B cell receptor on the surface membrane
- This receptor can be secreted as antibody or immunoglobin
- Any particular B cell clone will only express antibody of one specificity
- The overall B cell population within an individual will be very diverse
- Antigen only binds to specific B cell
- This cline proliferates (expands)-- expanded clones differentiate into Memory B cells and antibody secreting Plasma cells hence lag time
- Result-- large amount of antibody secreted specific for selecting antigen
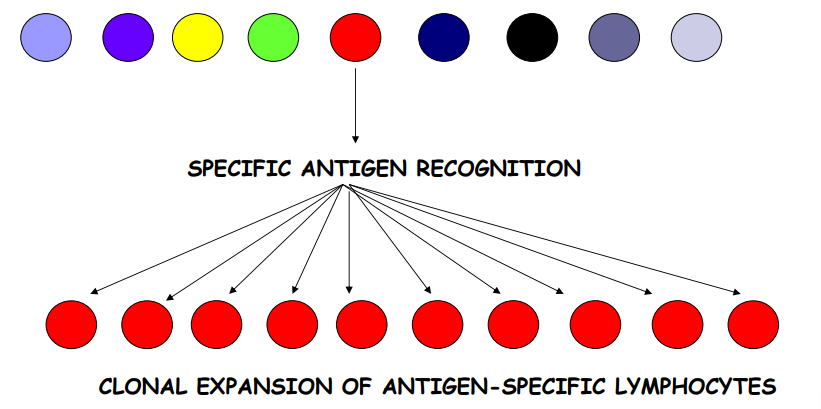
Antibody is most effective against?
- Cytotoxic T cells (CTL) expresses the CD8 molecule on surface-- once activated can kill virally infected cells and CTLs also target cancer cells
- T helper (Th) cells express the CD4 molecule on the surface-- once activated can help other cells eg B cells, CTL and macrophage
- They are co-receptors (required for T cell activation)
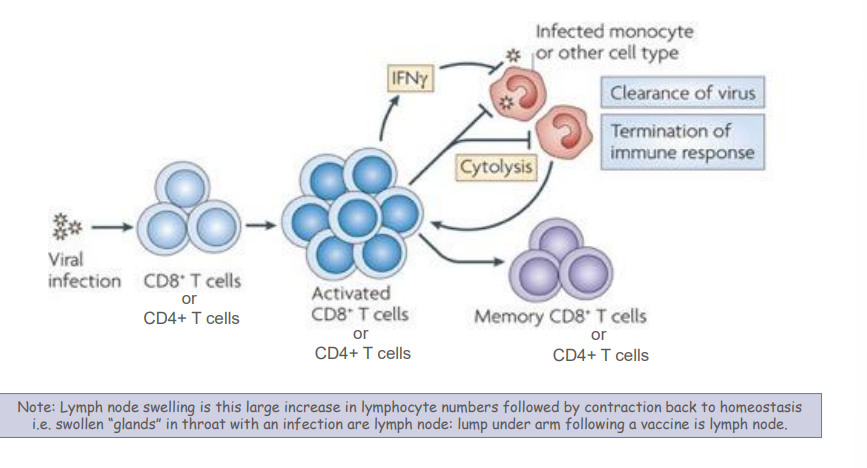
What does the T helper cell do?
- Helps B cell
- Produce antibodies against extracellular bacteria
- Helps CTL
- CTLs kill virally infected cells
- Activates macrophage (Mo)
- Killing activity is increased in Mo eg against intracellular pathogens eg Mycobacteria
- Professional antigen presenting cells (APCs)-- dendritic cell, macrophage (innate immunity) and B cell (adaptive immunity)
- Role of APCs-- enables the T cell to 'see pathogen' leading to its activation
- Key APC for Naïve T cell activation is the dendritic cell
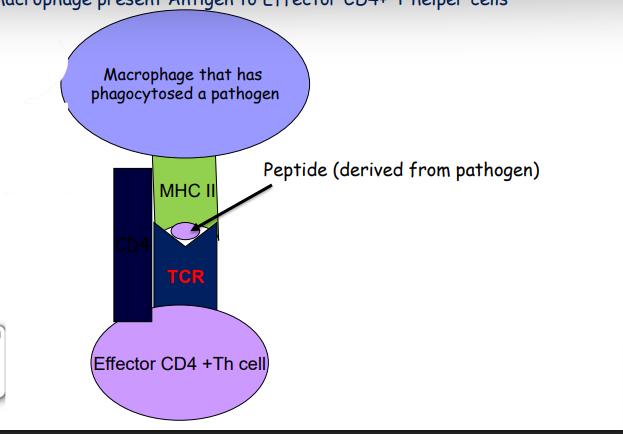
- The macrophage and B cell act as APCs to effector T cells
- Pathogens and their proudcts must be transported to lymphoid tissue
- Pathogens that gain entry at a skin wound for example are transported in lymph and trapped in lymph nodes nearest to the sit of infection
- Pathogens infecting mucosal sites are transported across the mucosa into lymphoid tissue such as the tonsils and Peyer's patches
- Antigens introduced directly into the bloodstream are picked up by APCs in the spleen
- Microbes enter the body most often through the skin and the gastrointestinal and respiratory tracts
- These tissues are lined by epithelia that contain dendritic cells and all are drained by lymphatic vessels
- Dendritic cells can uptake pathogen by several mechanisms
- Phagocytosis, pinocytosis, receptor mediated endocytosis and process antigen for presentation to naïve CD4+ and naïve CD8+ T cells
- Sites of microbe entry-- skin, GI tract, lungs (organs with epithelial layers, populated by DC)
- Sites of lymphocyte activation-- peripheral lymphoid organs (lymph nodes, spleen), mucosal and cutaneous lymphoid tissues
- DC's migrate antigens and present them to naïve T cells in lymph nodes
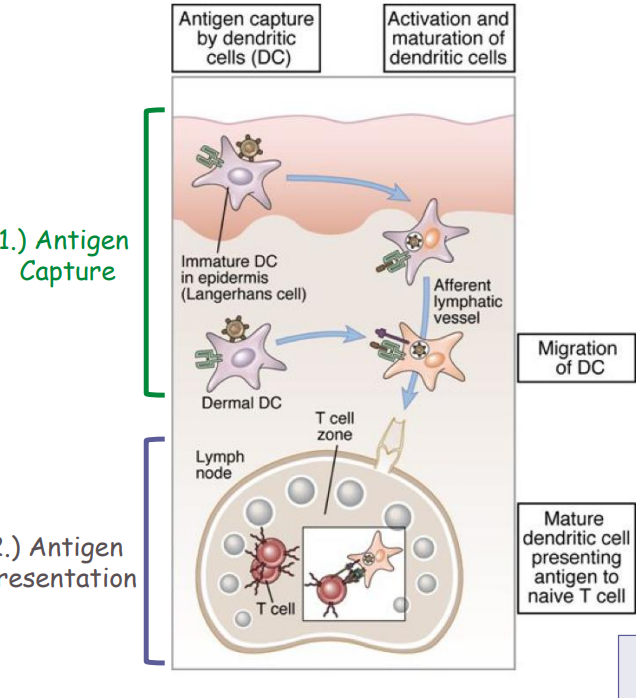
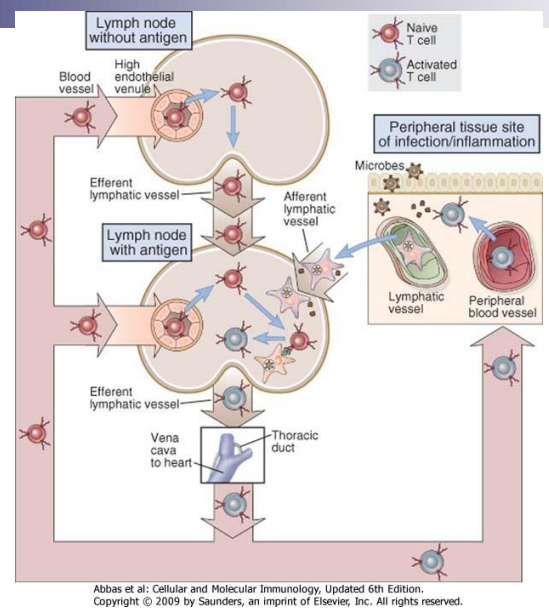
- Name derives from finding that this gene loci is involved in tissue compatibility in transplants
- Transplanted organ recognised as 'non self' by the immune system
- What does it recognise?-- MHC molecules
- MHC genotype matching between donor and recipient is needed for allografts
- MHC class I and II act as antigen presenting structures-- function is to bind peptide and present to T cells
- MHC II molecules are expressed on professional APCs
- MHC I molecules are expressed on all nucleated cells
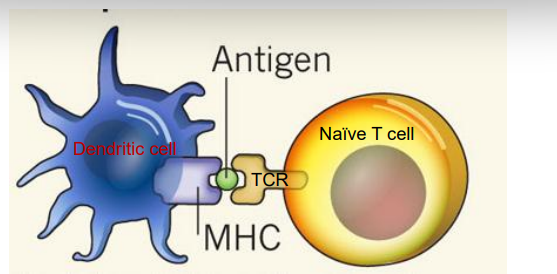
- Dendritic cell presents antigen peptide bound to MHC molecules to naïve T cells
- In this case the naïve T cell recognises the MHC/ peptide complex through its TCR
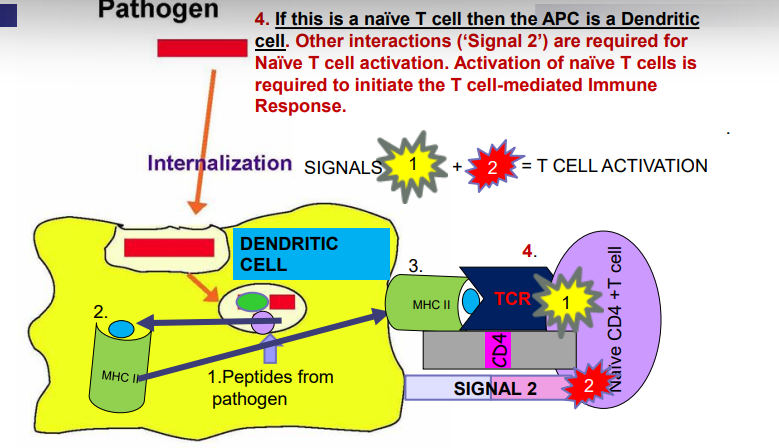
- This provides 'signal 1' for naïve T cell activation
- Naïve CD4+ T cell activation-- dendritic cells present peptide from processed pathogen on MHC II molecules to CD4+ T cells
- Naïve CD8+ T cell activation-- dendritic cells present peptide (eg viral peptide) on MHC class I molecules to CD8+ T cells
What can phagocytes act as?
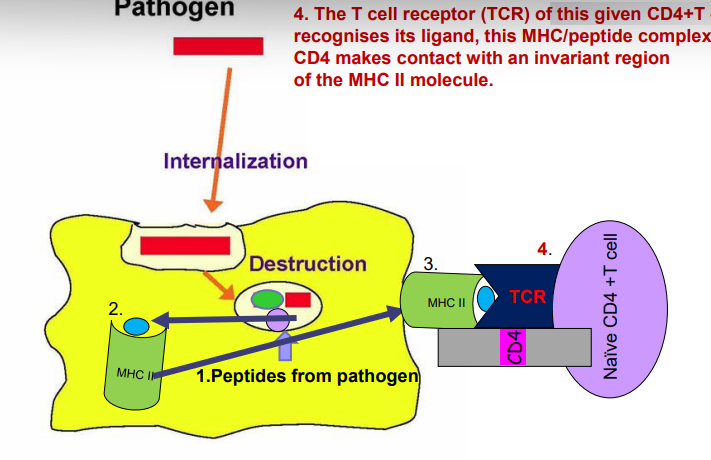
1. Catabolism of protein antigen to peptides inside host cell-- some peptides bind to an MHC molecule
2. MHC II molecule binds to a peptide derived from the pathogen
3. Loaded MHC II/ peptide complex travels to the cell surface to display antigen to T cells
4. The T cell receptor (TCR) of this given CD4+ T cell recognises its ligand, this MHC/ peptide complex. CD4 makes contact with an invariant region of the MHC II molecule
- Neutrophil, macrophage-- Killing activity is increased in Macrophage
- Killer T cell-- Cytotoxic T lymphocyte (CTLs kill virally infected cells
- B cells-- Produce antibodies against extracellular bacteria
What does CD8+ T cell do
Effector cell ( cytotoxic T lymphocyte) and following recognition of MHC I/ viral peptide complex it can kill this virally infected tissue
Cytokines, secreted chemical messengers to instruct differetn function
Perforings pierce holes in target cell and granzymes initiate programmed cell death (apoptosis)
CTLs also key cellular players in killing tumour cells-- in this case tumour antigen is displayed on MHC class I molecules by cancer cells
1. Phagocytosis
2. Antigen presentation leads to activation of T cells
3. Antiviral responses (interferons)
4. Defence against parasitic infections
- Cytokines (proteins) produced by host cells in response to viral and microbial infections
- Induces an antiviral state in cells
- Natural killer (NK) cells and plasmacytoid dendritic cells are important cellular sources of interferons
- Severe acute respiratory syndrome coronavirus 2 is a new β coronavirus responsible for the viral pandemic known as COVID-19
- SARS-CoV-2 can lead to an excessive inflammatory innate immune response and impaired adaptive immune response, leading to tissue damage at the systemic level.
- There is an excessive release of cytokines and chemokines, referred to as a 'cytokine storm' seen in patients with severe lung disease with the development of acute respiratory distress syndrome (ARDS) during SARS-CoV-2 infection
- Severe COVID-19 patients show an impaired type I interferon response characterised by undetectable IFN-b and low IFN-a production/activity together with heightened production of pro-inflammatory cytokines - Age and sex influence disease severity
- Each b cell expresses a specific B cell receptor on the surface membrane
- This receptor can be secreted as antibody or immunoglobin
- Any particular B cell clone will only express antibody of one specificity
- But the overall B cell population (within an individual) will be very diverse
- B cell acts as an antigen presenting Cell (APC) to T cell
- Immunoglobin (Ig) molecule has 2 identical light chains and 2 identical heavy chains
- The Ig molecule has a variable region and a constant region
- Variable region is the site where antigen binding site is located
- Constant region is region which determines the effector function if the Ig molecule
- IgM
- IgD
- IgG
- IgE
- IgA
- IgG has 4 subclasses (IgG1, IgG2, IgG3, IgG4)
- IgA has 2 subclasses (IgA1 and IgA2)
- Lower case Greek letters-- μ (mu), δ (delta), γ (gamma), ε (epsilon), and α (alpha)
- Different classes determine effector functions
- (κ) kappa and (λ) lambda
- No functional differences have been found between antibodies carrying kappa or lambda light chains
- Each antibody has kappa or lambda, not both
1. Neutralisation--eg neutralises toxins by binding to them before they bind to cells and do harm to host cells, binds to viral particles and prevents virus from entering cell)
2. Opsonisation-- process of coating microbes with antibodies so that they are more easily phagocytosed, this is because phagocytes (eg macrophage) express recptors (FcRs) for antibodies so can bind antibody microbe complex
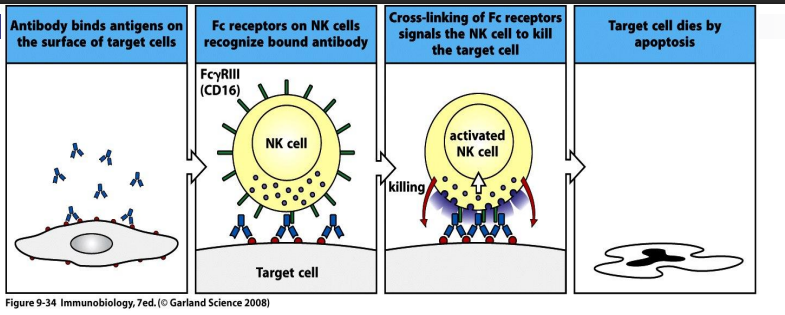
3. Antibody dependent cell mediated cytotoxicity-- antibody binds to antigen (eg viral antigen) receptors for Fc region of antibodies are located on Natural Killer (NK) cells, binds and leads to release of toxic granule contents, cell destruction
FcRs which bind to Fc region of different classes of an antibody eg IgG, IgE etc
a. Ab recognises antigen on infected cell eg virally infected cell
b. NK cell has receptor for Fc region of IgG
c. NK cell releases toxic granule contents-- leads to death of target cell
- Important in defense against extracellular parasites like helminths worms
- Cells involved include NK cells, eosinophils, neutrophil, macrophage
- Antibodies bind to antigens on the parasite, cells have receptors for Fc portion of Ig molecule present on eosinophils, NK cells, macrophages, neutrophils
- Release of lytic enzymes eg neutrophil (lytic enzymes) macrophage (lytic enzymes), tumor necrosis factor (TNF), NK cell (lytic enzymes, perforin, granzymes)
Immunoglobin mediated effector function-- 2. opsonisation
antibodies can coat microbes (ie antibodies bind to antigens through the Fab region. Macrophages have receptors which recognise the Fc region of antibodies (FcRs)-- uptake of microbe by macrophage. Antibody acts as an opsonin
a. Ab recognises antigen on infected cell eg virally infected cell
b. NK cell has receptor for Fc region of IgG
c. NK cell releases toxic granule contents-- leads to death of target cell
- Important in defense against extracellular parasites like helminths worms
- Cells involved include NK cells, eosinophils, neutrophil, macrophage
- Antibodies bind to antigens on the parasite, cells have receptors for Fc portion of Ig molecule present on eosinophils, NK cells, macrophages, neutrophils
- Release of lytic enzymes eg neutrophil (lytic enzymes) macrophage (lytic enzymes), tumor necrosis factor (TNF), NK cell (lytic enzymes, perforin, granzymes)