Overview of the Urinary System and Kidney Functions
1/175
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
176 Terms
Functions of the urinary system
Maintains homeostasis by managing the volume and composition of fluid reservoirs, primarily blood.
Major organs of the urinary system
Consists of kidneys, ureters, bladder, and urethra.
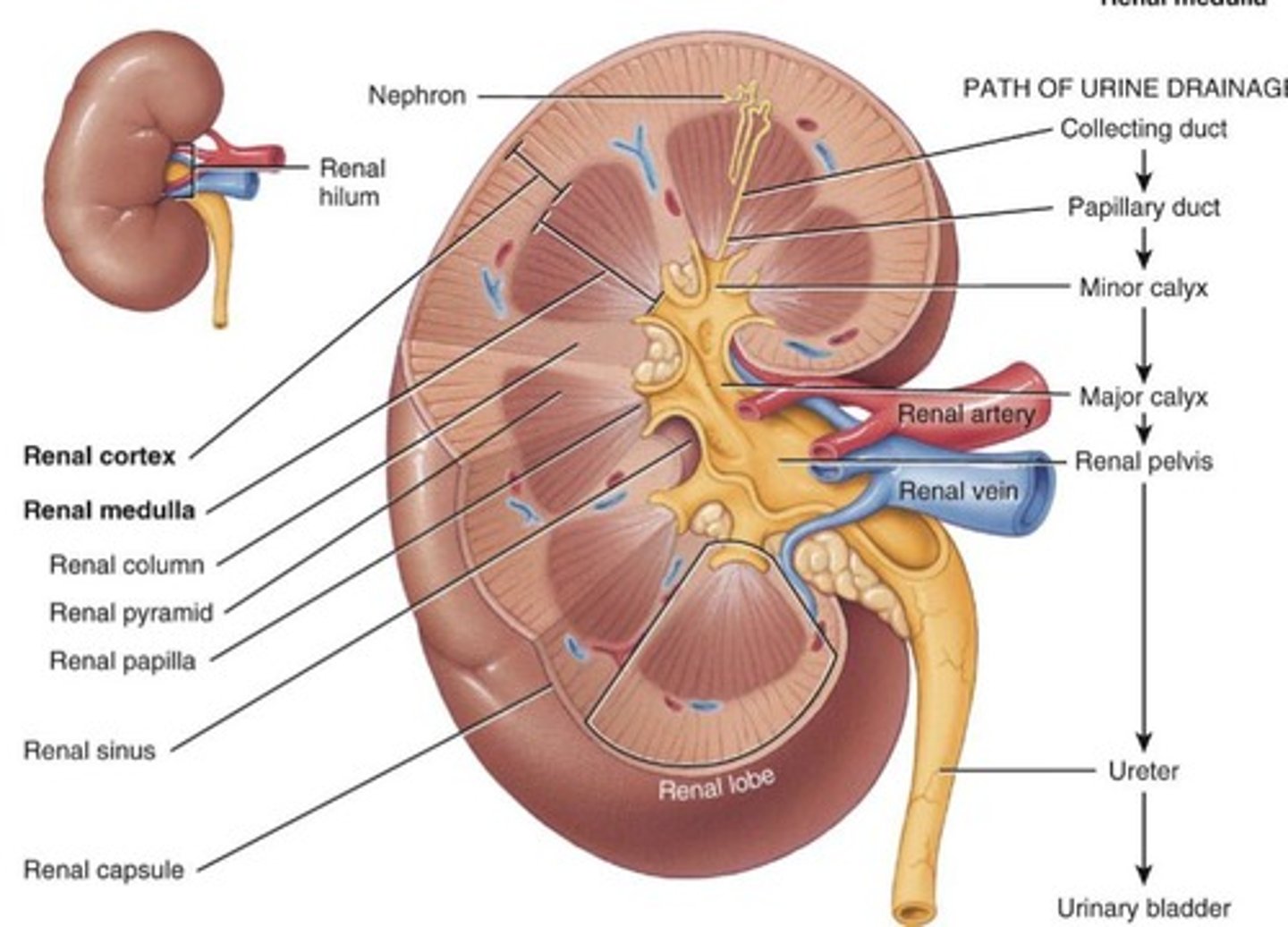
Renal pelvis
Collects urea inside kidney and funnels it into the ureter.
Ureter
Takes urine to the bladder.
Kidney
Filters blood to form urine.
Urinary bladder
Helps with micturition (peeing) and stores urine.
Homeostatic Kidney Function
Regulation of blood ionic composition - Na+, K+, Cl-.

Blood pH regulation
Regulation of blood pH, H+, HCO3-.
Blood volume regulation
Regulation of blood volume H2O.
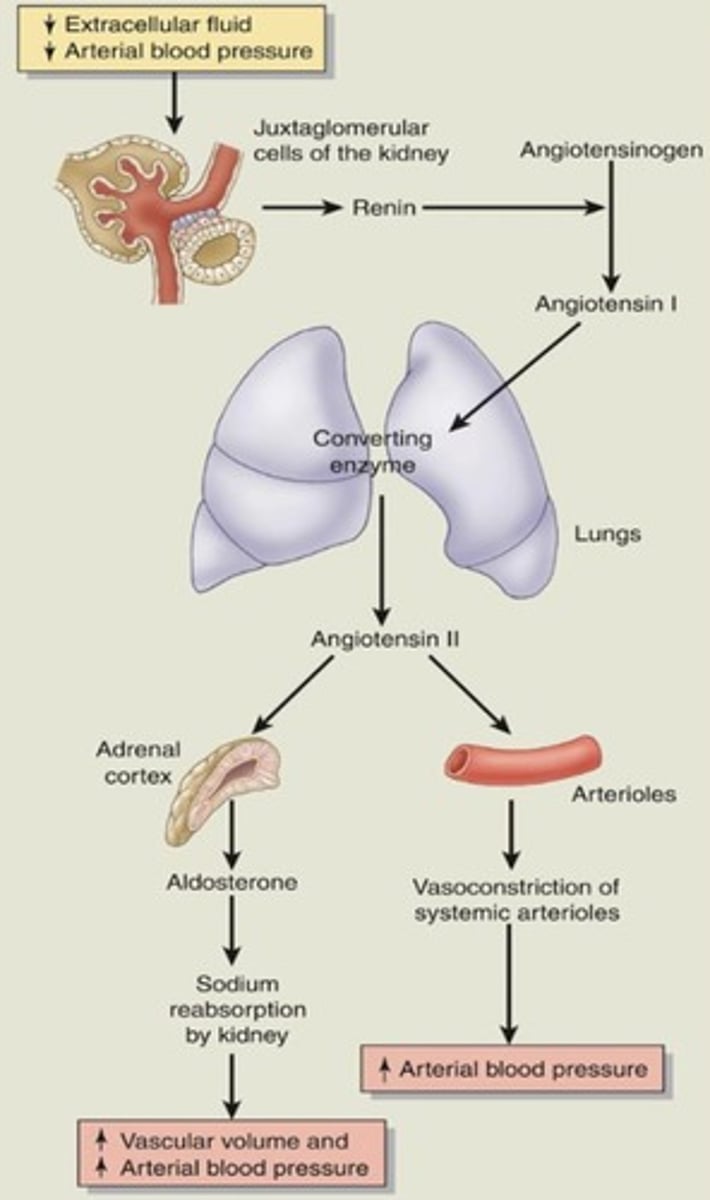
Blood pressure regulation
Regulation of blood pressure.
Blood osmolarity maintenance
Maintenance of blood osmolarity.
Hormones produced by kidneys
Production of hormones: calcitriol and erythropoietin.
Excretion by kidneys
Excretion of metabolic wastes and foreign substances (drugs or toxins).
Blood glucose level regulation
Regulation of blood glucose level.
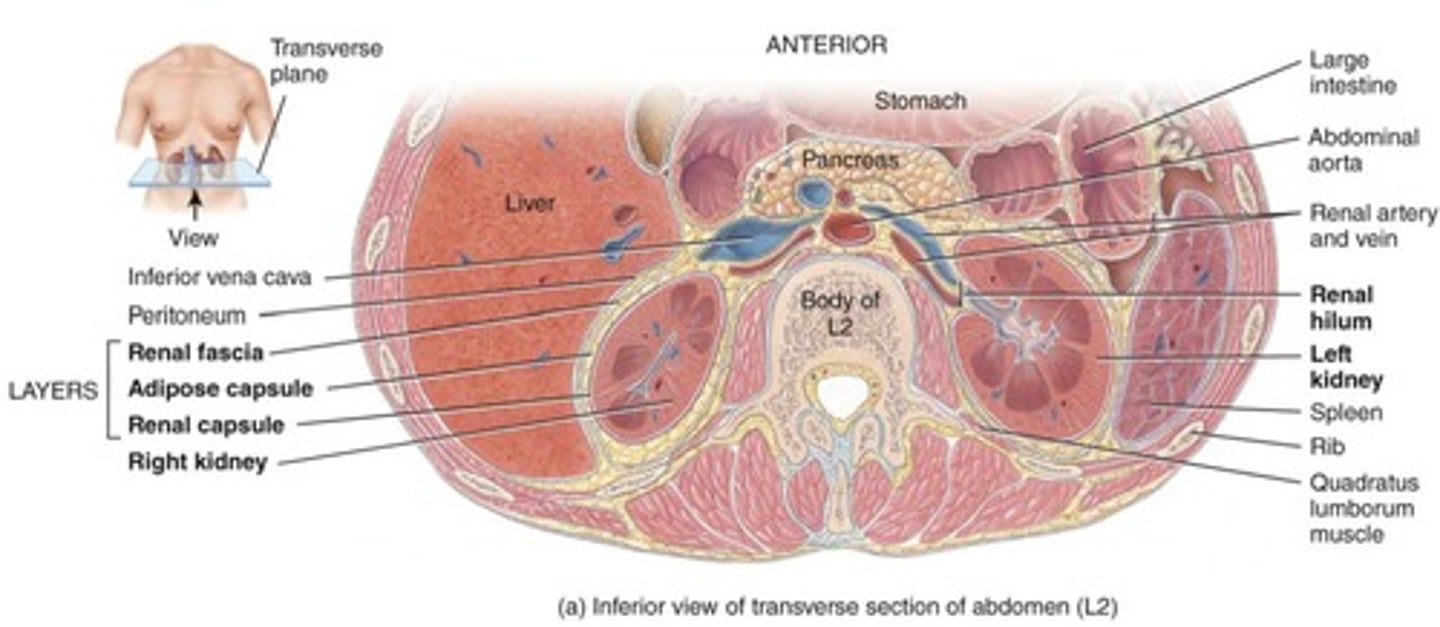
Kidney location and protection
Kidneys are retroperitoneal, partly protected by the lower ribs.
Renal hilum
The indented area is the entrance for renal artery, renal vein, ureter, nerves, lymphatics.
Renal fascia
Anchors kidneys to other structures.
Adipose capsule
Protects and anchors the kidneys.
Renal capsule
Continuous with the ureter.
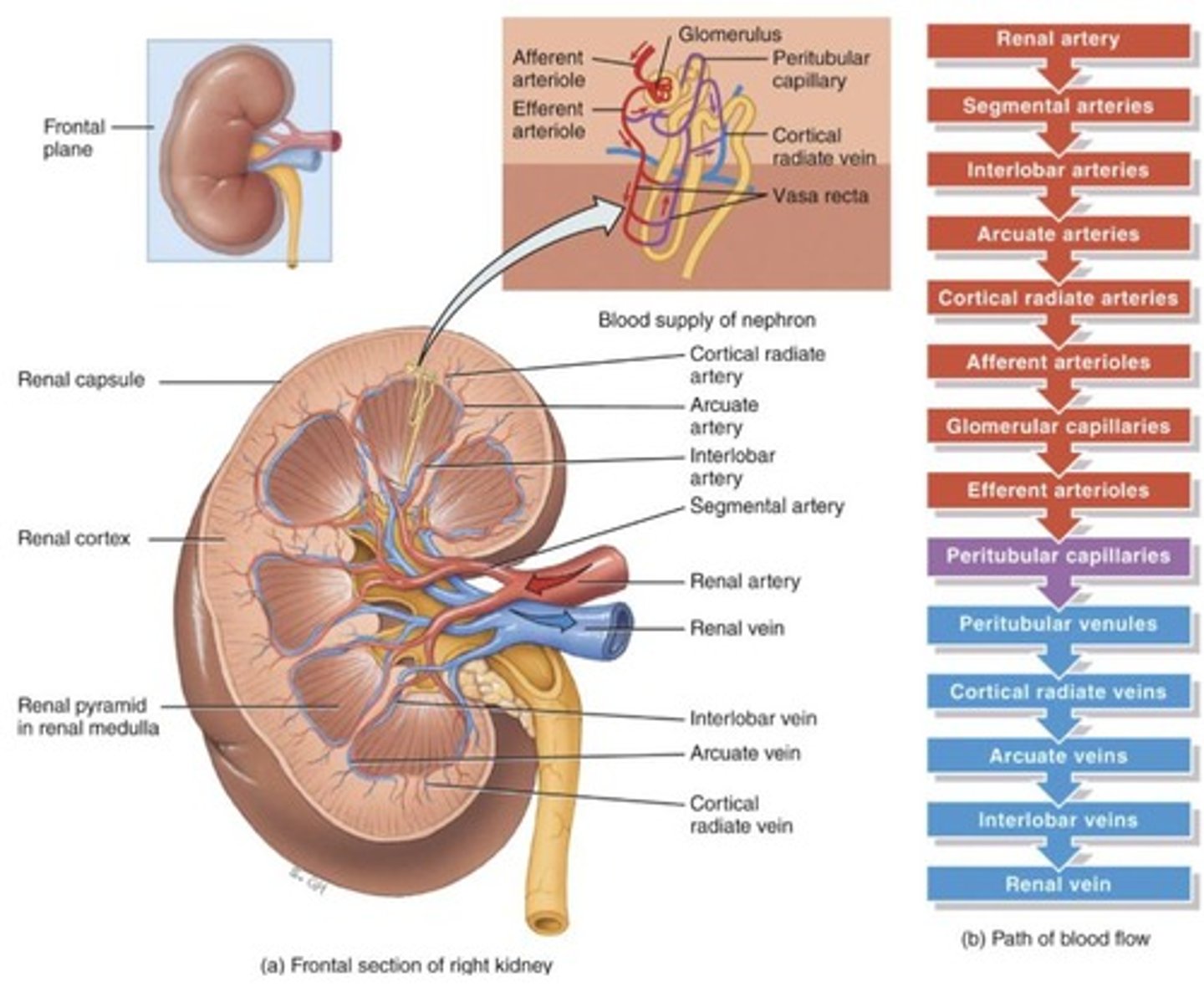
Renal cortex
Outer layer of the kidney.
Renal medulla
Inner region of the kidney.
Renal pyramids
Secreting apparatus and tubules.
Renal columns
Anchor the cortex.
Blood supply of the kidney
Although kidneys constitute less than 0.5% of the total body mass, they receive 20-25% of resting cardiac output.
Renal nerves
Primarily carry sympathetic outflow and regulate blood flow through the kidneys.
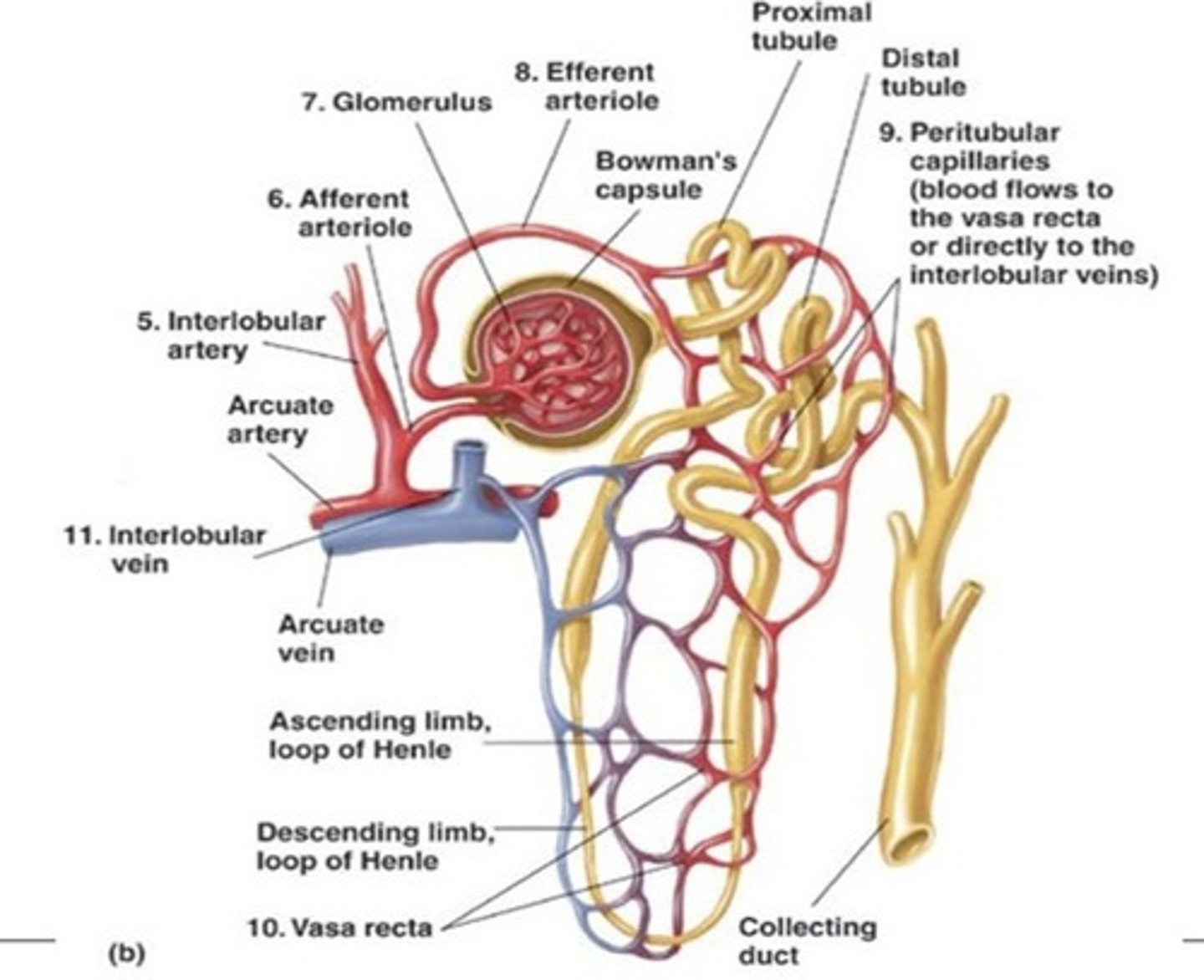
Nephron
The functional unit of the kidney - 'a tiny funnel with a long winding stem'.
Number of nephrons
Over a million in each kidney - filter 45 gallons of blood a day.
Parts of a nephron
Made of renal corpuscle and renal tubule.
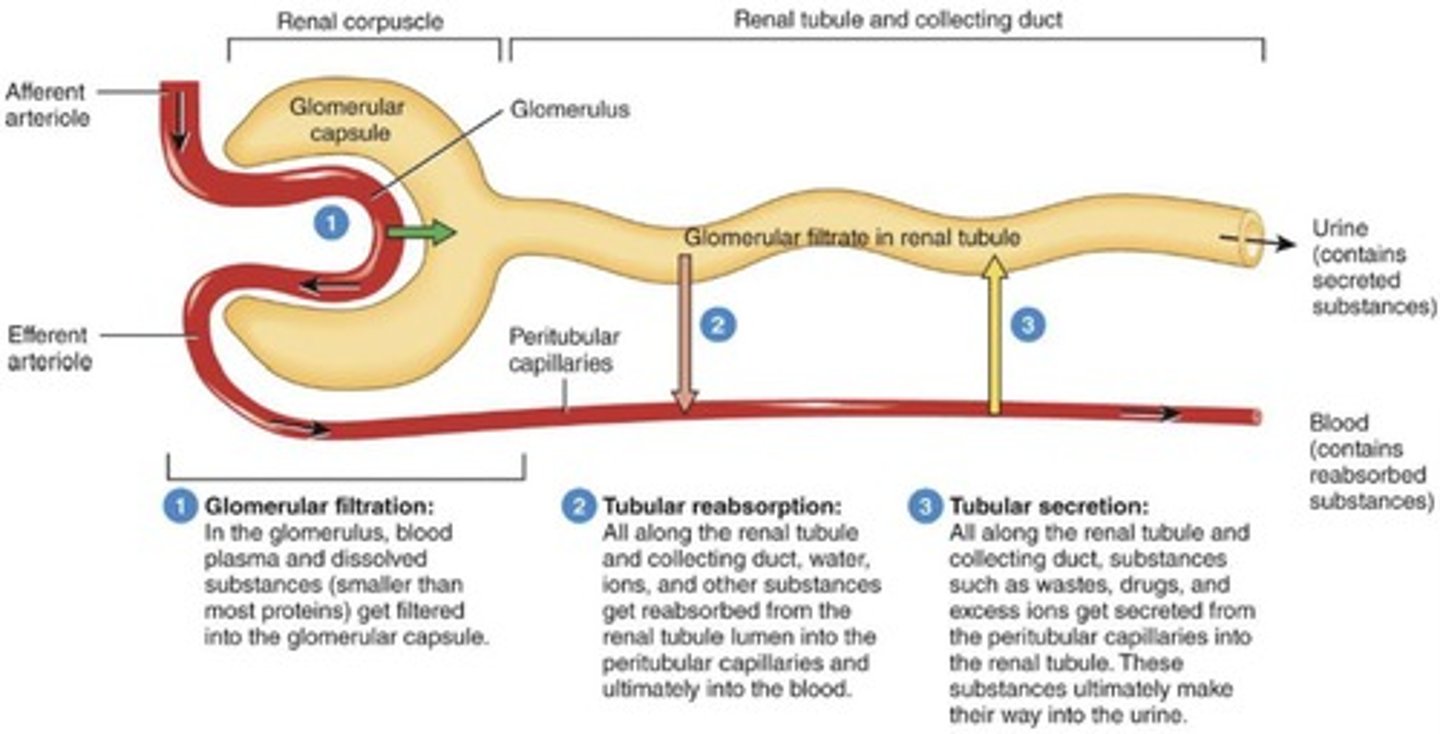
Glomerular filtration
Two parts: outer - glomerular (Bowman's) capsular, inside - glomerular capillaries.
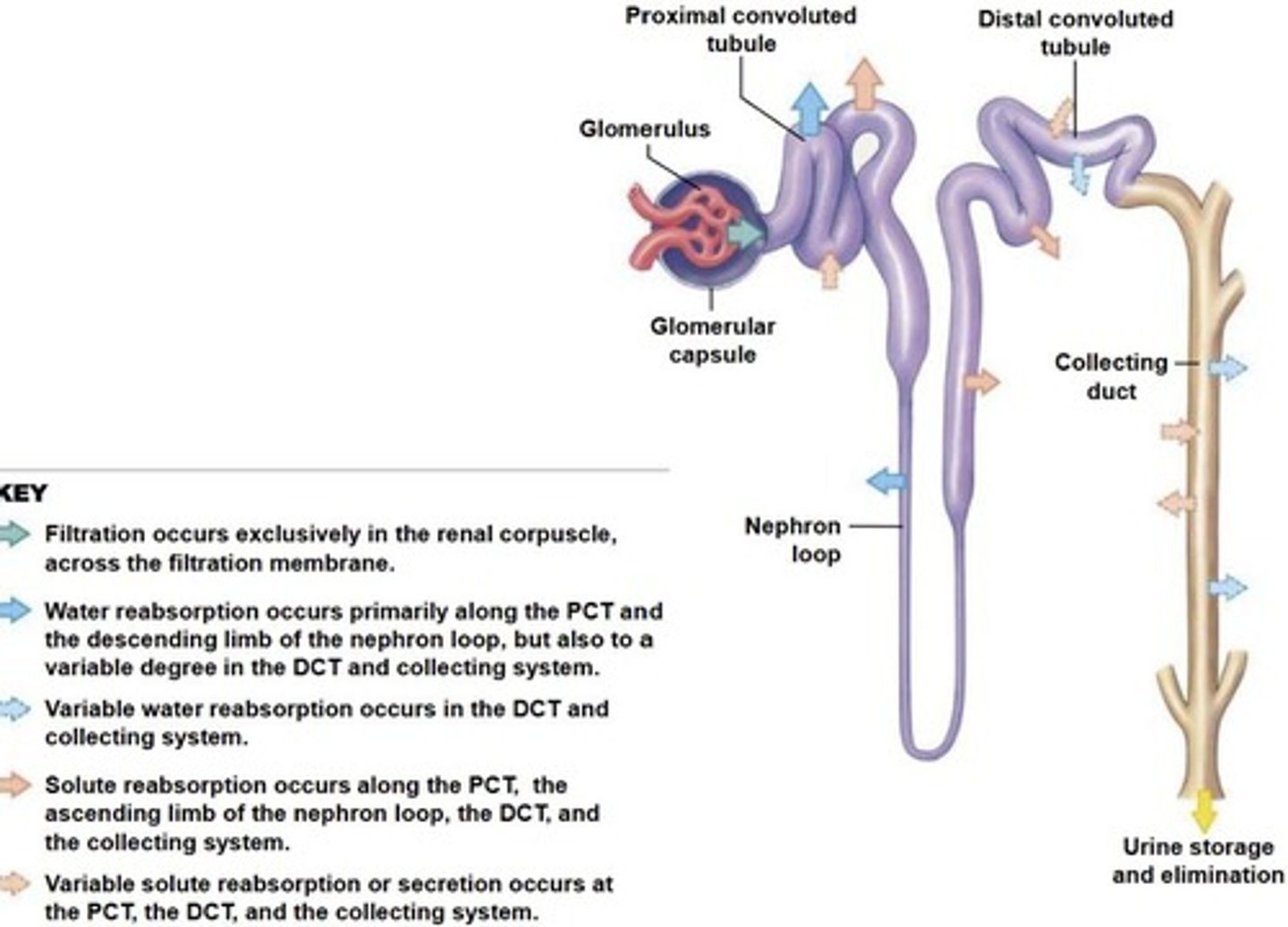
Proximal convoluted tubule (PCT)
Next after renal corpuscle.
Nephron loop
Also known as loop of Henle, consists of descending limb and ascending limb.
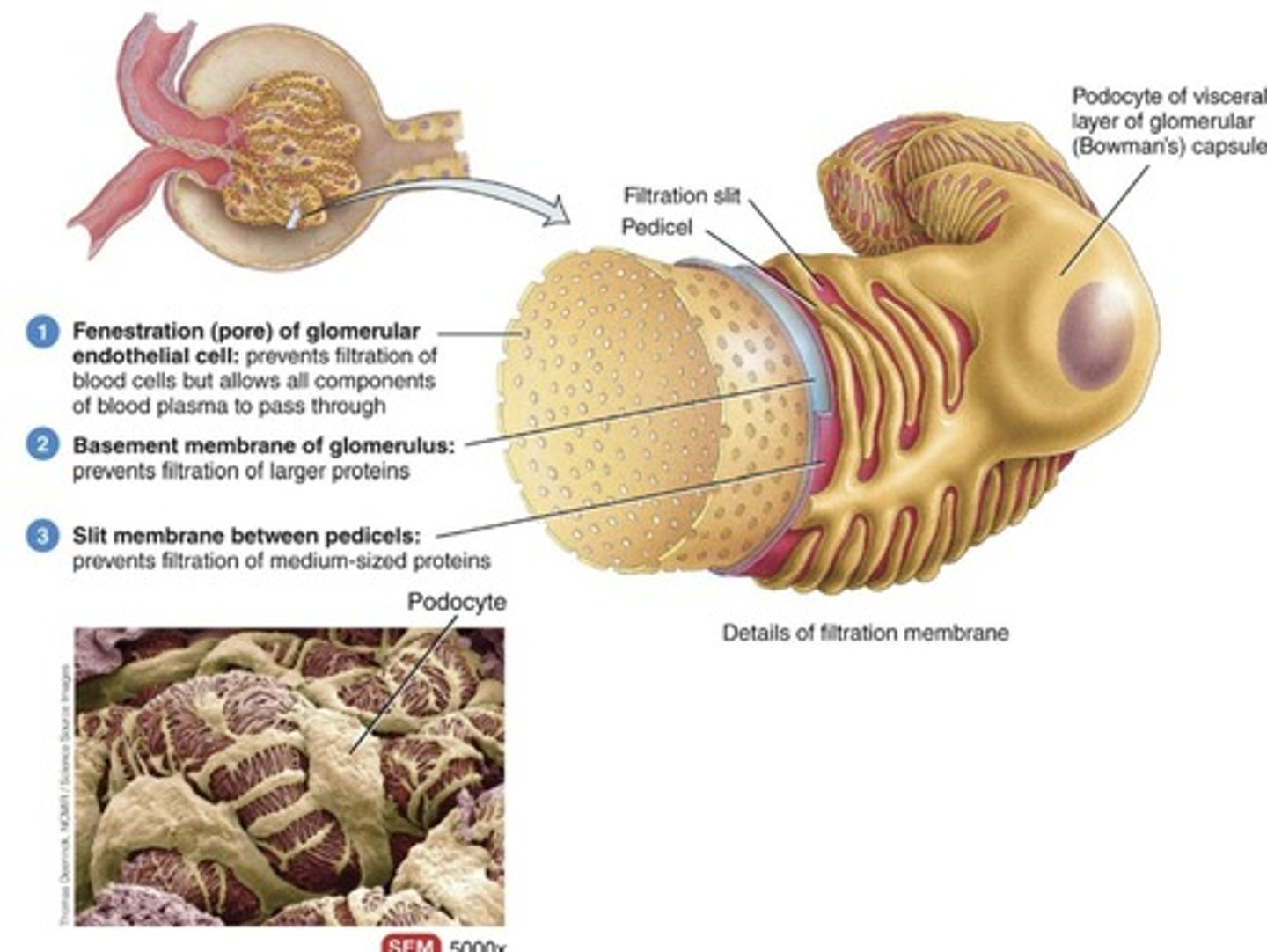
Filtration membrane
Inside of glomerulus tubes is endothelial cells with fenestrations/pores, then basement membrane to prevent filtering of big proteins.
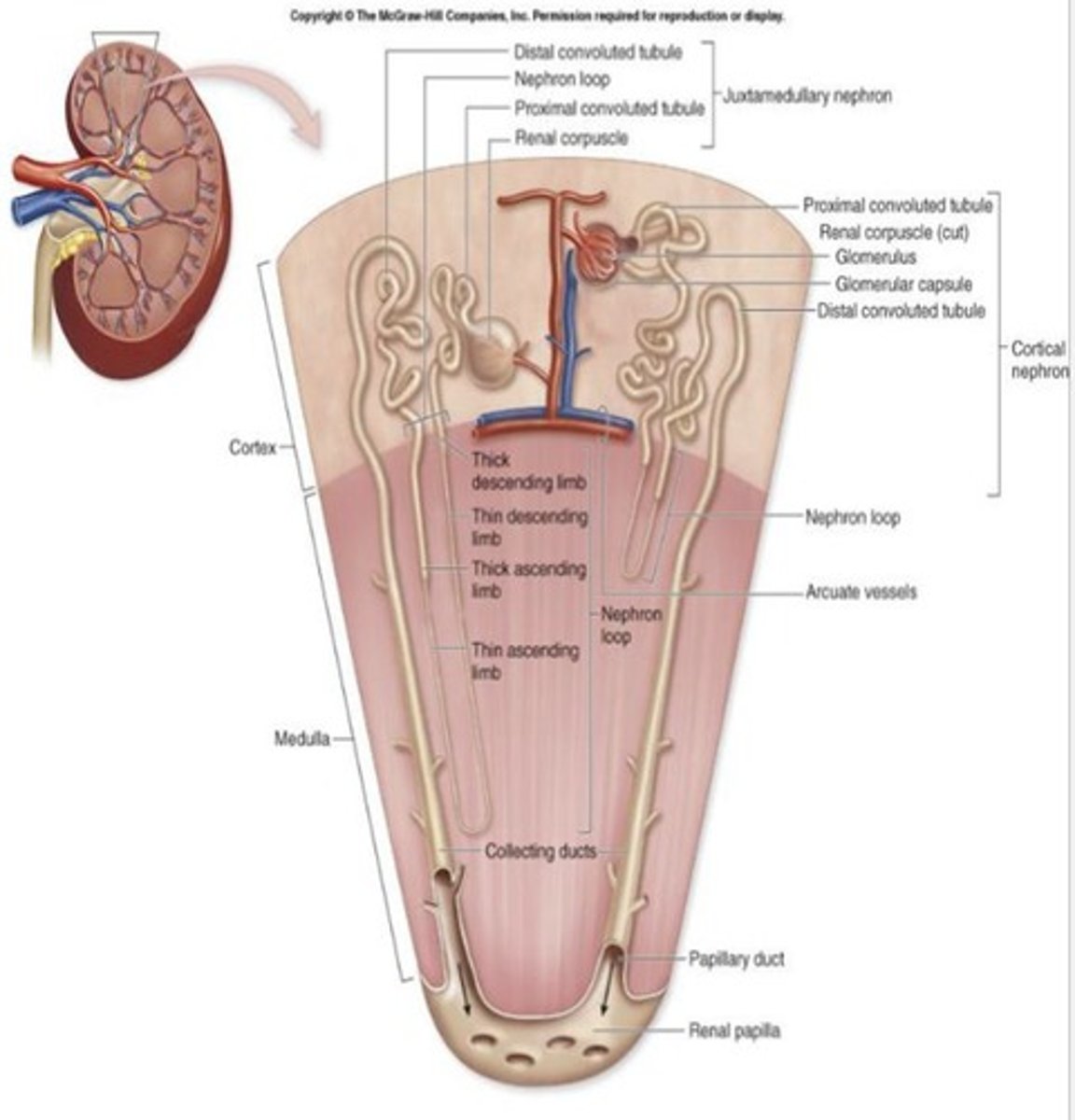
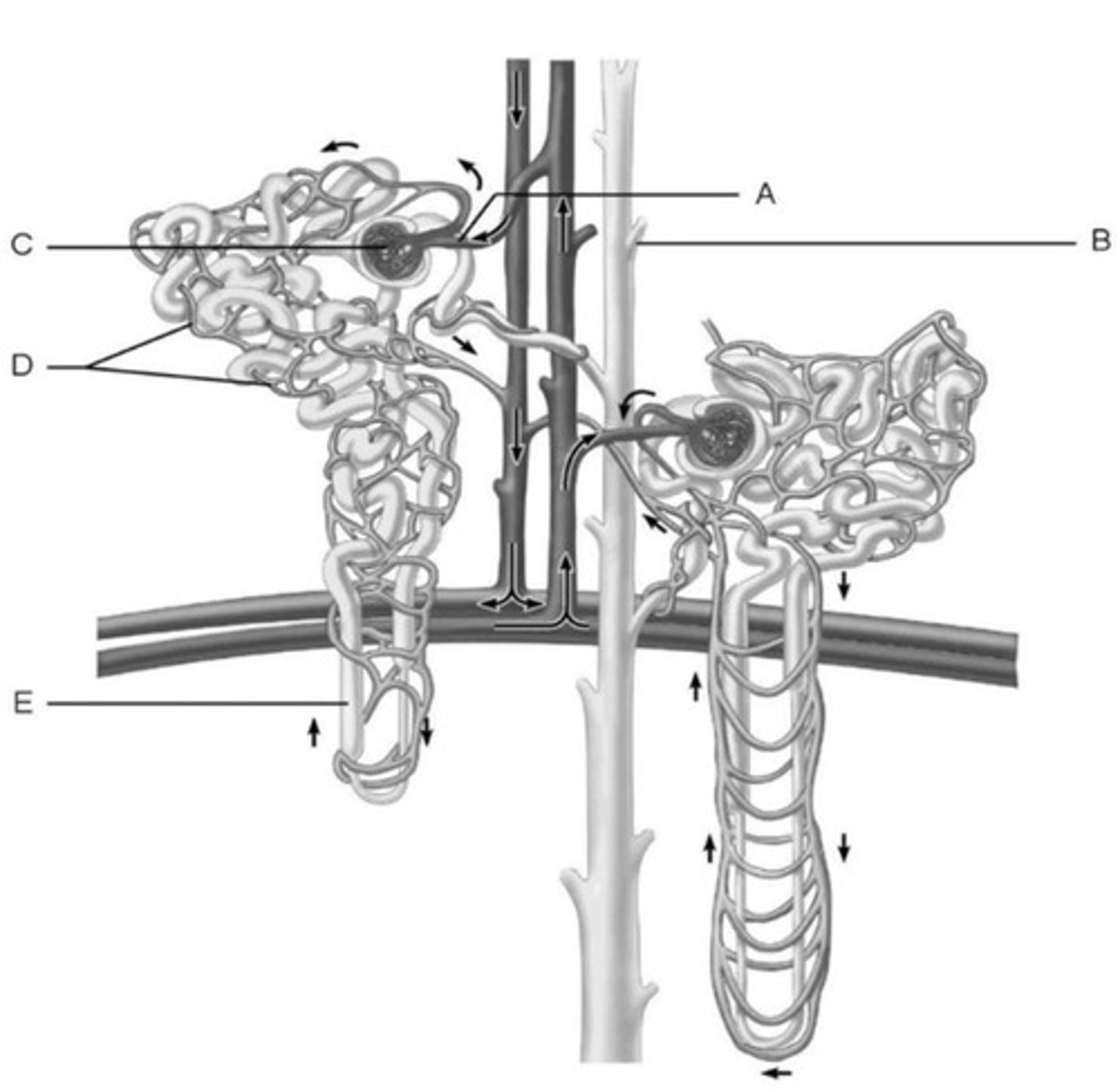
Cortical nephrons
80-85% of nephrons.
Cortical nephron structure
Renal corpuscle in outer portion of cortex.
Cortical nephron loop
Short loops of Henle extend only into outer region of medulla.
Cortical nephron urine osmolarity
Create urine with osmolarity similar to blood.
Flow of fluid through a cortical nephron
Glomerular (Bowman's capsule) → proximal convoluted tubule → descending limb of the nephron loop → ascending limb of the nephron loop → distal convoluted tubule (drains into collecting duct).
Juxtamedullary nephrons
15% of nephrons.
Juxtamedullary nephron structure
Renal corpuscle deep in cortex with long nephron loops.
Juxtamedullary nephron blood supply
Receive blood from peritubular capillaries and vasa recta.
Juxtamedullary nephron ascending limb
Ascending limb has thick and thin regions.
Juxtamedullary nephron function
Enable kidney to secrete very concentrated urine during times of dehydration.
Juxtamedullary nephron loop depth
Much longer nephron loop - deeper in medulla.
Flow of fluid through a juxtamedullary nephron
Glomerular (Bowman's) capsule → proximal convoluted tubule → descending limb of the nephron loop → thin ascending limb of the nephron loop → thick ascending limb of the nephron loop → distal convoluted tubule (drains into collecting duct).
Juxtaglomerular apparatus
Purpose is to regulate blood pressure in kidney with ANS; ascending loop contacts afferent arteriole at the macula densa.
Importance of filtration
Nephron's purpose is to increase surface area for urine processing, allowing time for stages and urine making steps.
Glomerular filtration
Driven by blood pressure.
Opposition to glomerular filtration
Opposed by capsular hydrostatic pressure and blood colloid osmotic pressure.
Glomerular filtration output
In one day, 150-180 liters of water pass out into the glomerular capsule.
Glomerular filtration rate (GFR)
Amount of filtrate formed by both kidneys each minute.
Homeostasis and GFR
Homeostasis requires kidneys to maintain a relatively constant GFR.
Effects of high GFR
Too high: substances pass too quickly and are not reabsorbed.
Effects of low GFR
nearly all reabsorbed and some waste products not adequately excreted.
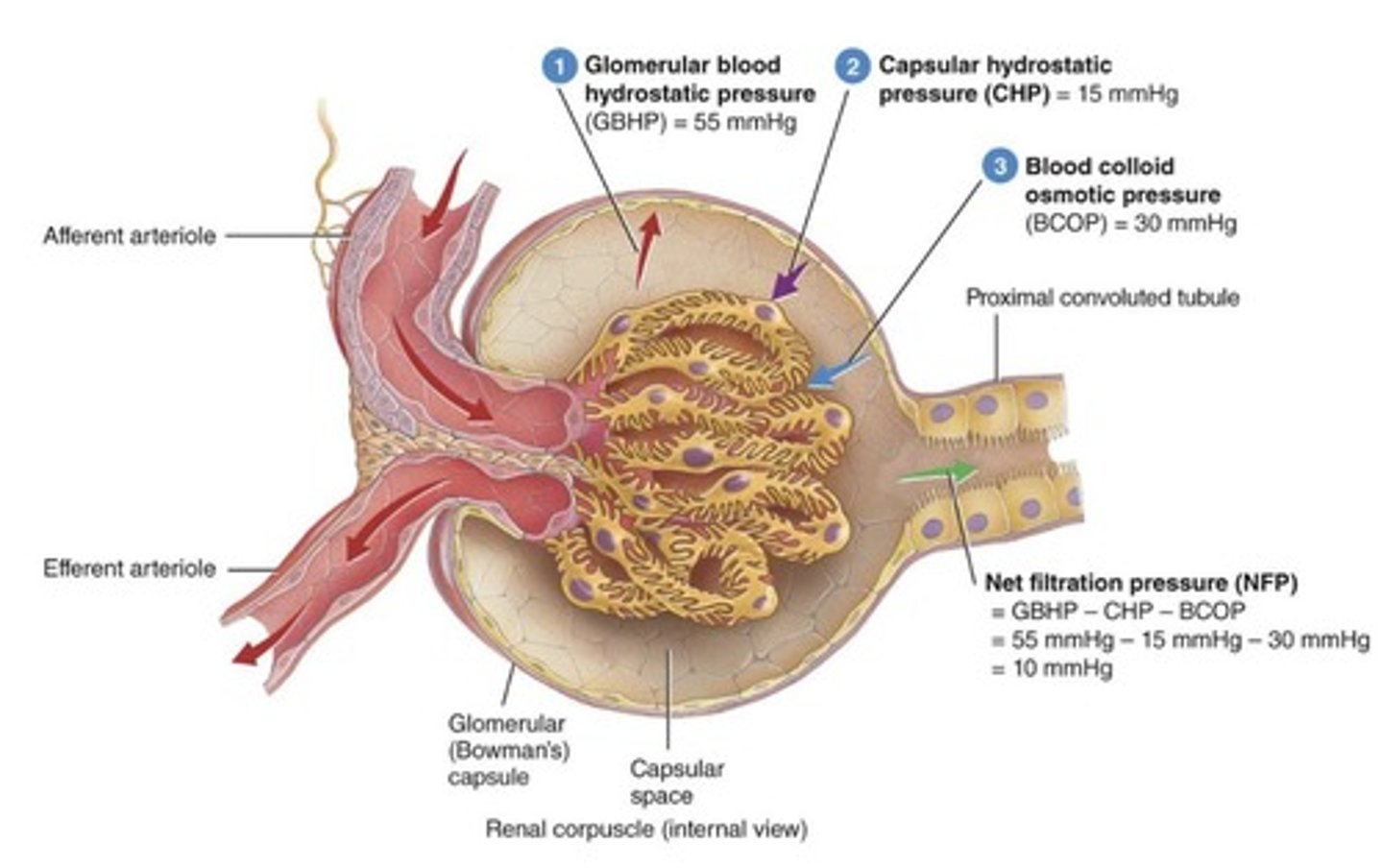
Glomerular blood hydrostatic pressure (GBHP)
GBHP = 55 mmHg.
Capsular hydrostatic pressure (CHP)
CHP = 15 mmHg.
Blood colloid osmotic pressure (BCOP)
BCOP = 30 mmHg.
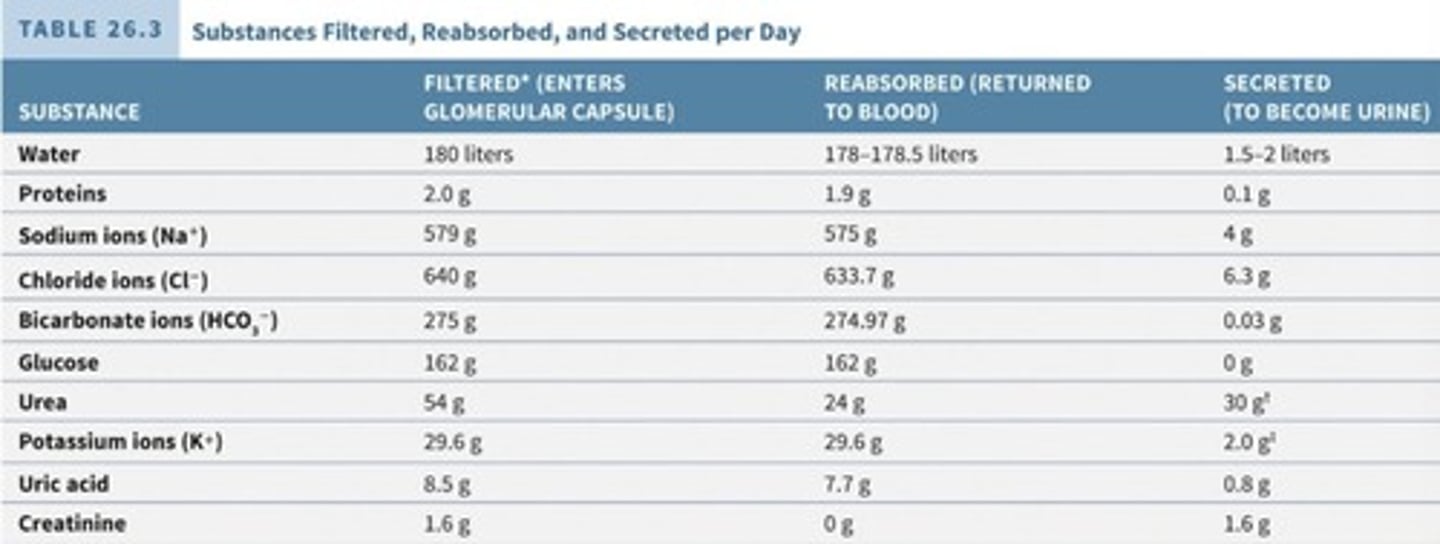
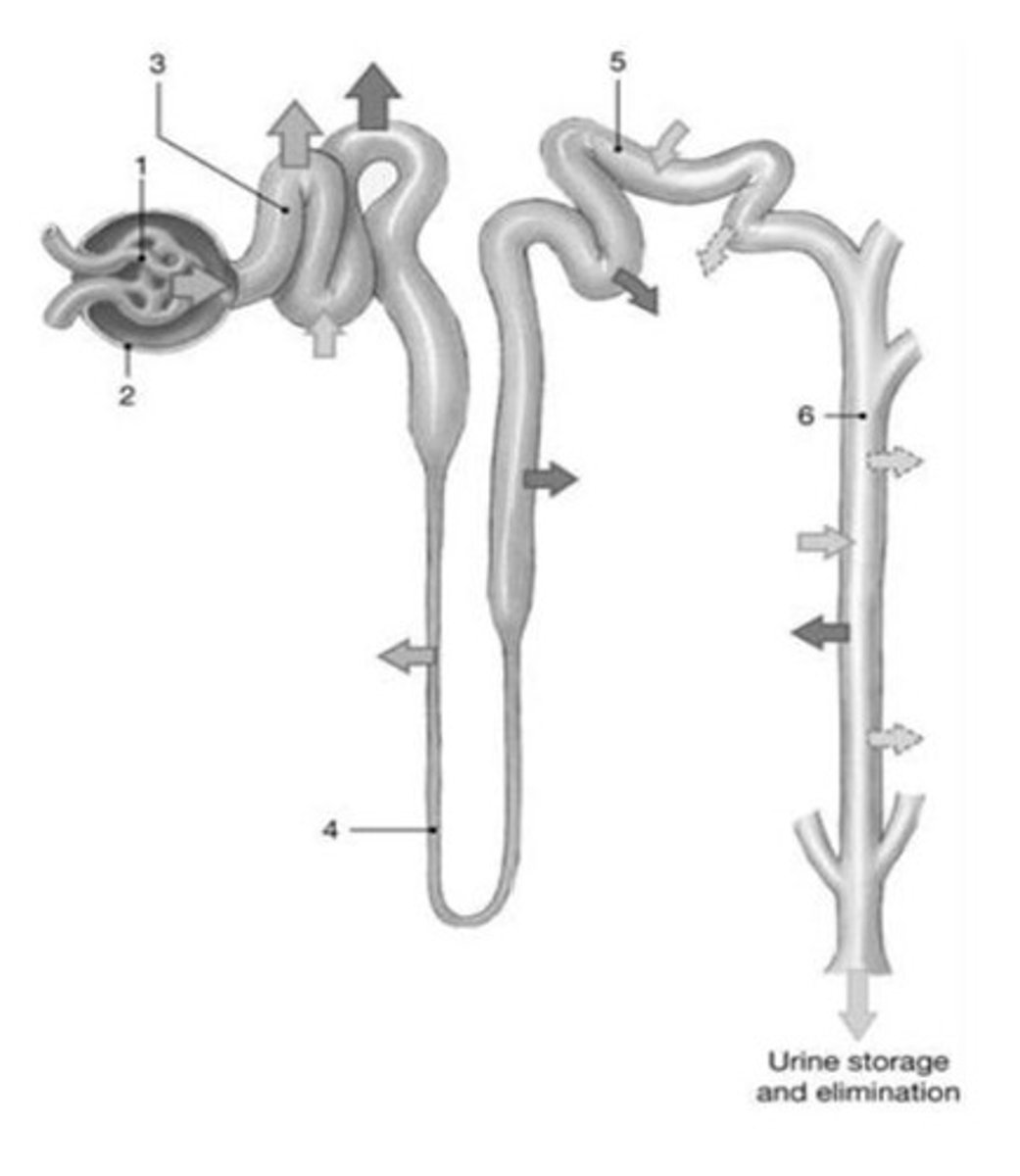
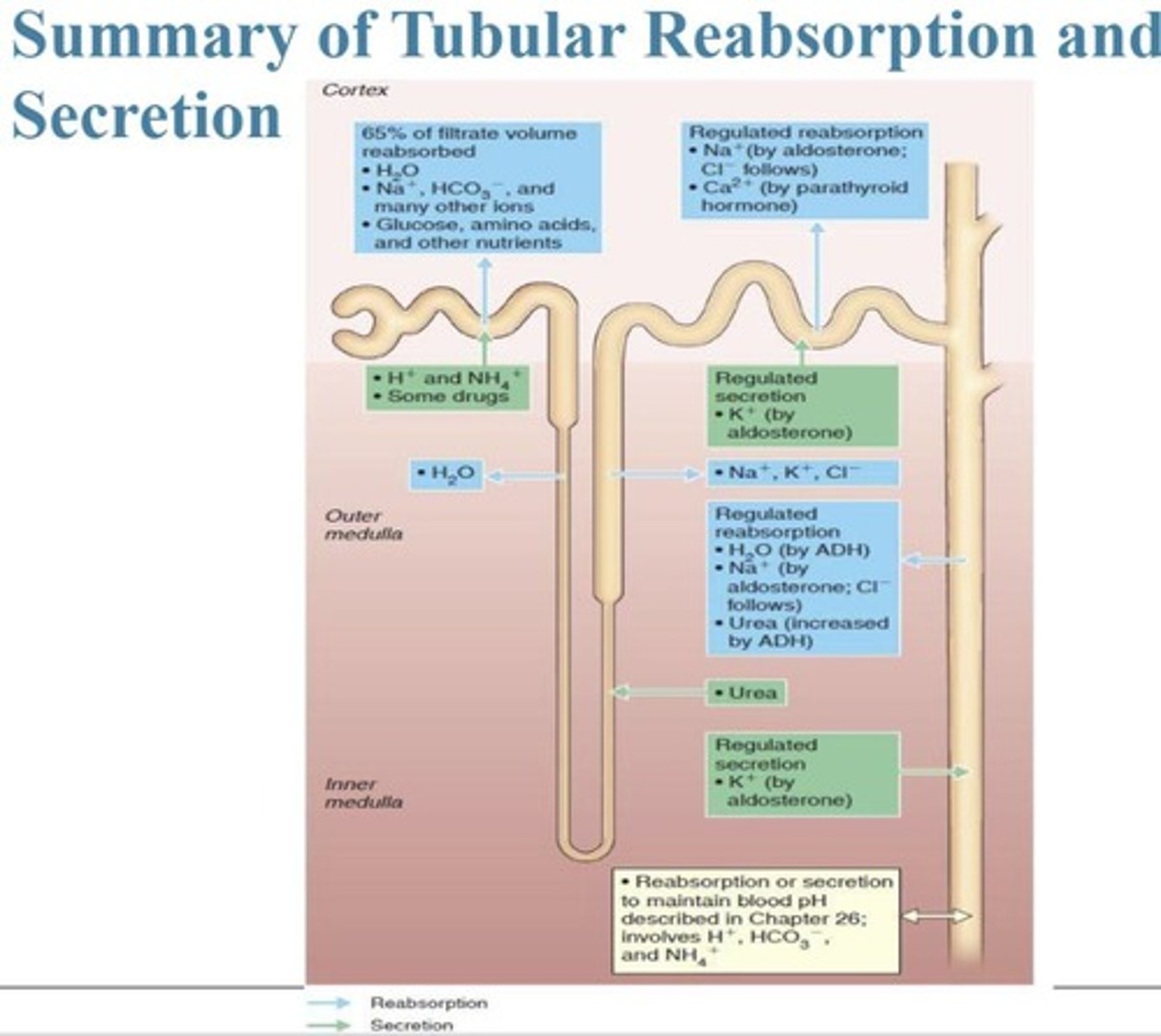
Tubular reabsorption
Along renal tubule/collecting duct, water and ions get reabsorbed from renal tubule into peritubular capillaries and go into bloodstream.
Tubular secretion
Waste/drugs/extra ions get secreted from peritubular capillaries into renal tubule, ending up in urine.
Urine excretion formula
Excretion of urine = glomerular filtration + secretion - reabsorption.
Renal Corpuscle
Consists of two parts: the glomerulus and the glomerular (Bowman's) capsule.
Glomerulus
A mass of capillaries that is fed by the afferent arteriole and drains into the efferent arteriole.
Glomerular (Bowman's) Capsule
Has a visceral layer of podocytes, which wrap around the capillaries and a parietal layer with a capsular cavity.
Filtrate
Collected between the visceral and parietal layers of the glomerular capsule.
Fenestrations
Large pores in glomerular endothelial cells that are leaky and prevent filtration of blood cells but allow all components of blood plasma to pass through.
Basal Lamina
Lies between endothelium and podocytes.
Podocytes
Form pedicels, between which are filtration slits.
Filtration Membrane
Composed of fenestration of glomerular endothelial cells, basement membrane of glomerulus, and slit membrane between pedicels.
Glomerular Filtration
Driven by blood pressure, opposed by hydrostatic pressure and blood colloid osmotic pressure, with about 150 L moving out of renal tubule into blood daily.
Capsular Hydrostatic Pressure (CHP)
Pressure that causes stuff to go into kidney (15 mmHg).
Blood Colloid Osmotic Pressure (BCOP)
Pressure that causes stuff to go into kidney (30 mmHg).
Net Filtration Pressure (NFP)
Calculated as GDHP - CHP - BCOP = 10 mmHg.
Glomerular Filtrate
Has more urea than plasma and lacks big proteins like blood cells/plasma proteins that plasma filtrate has.
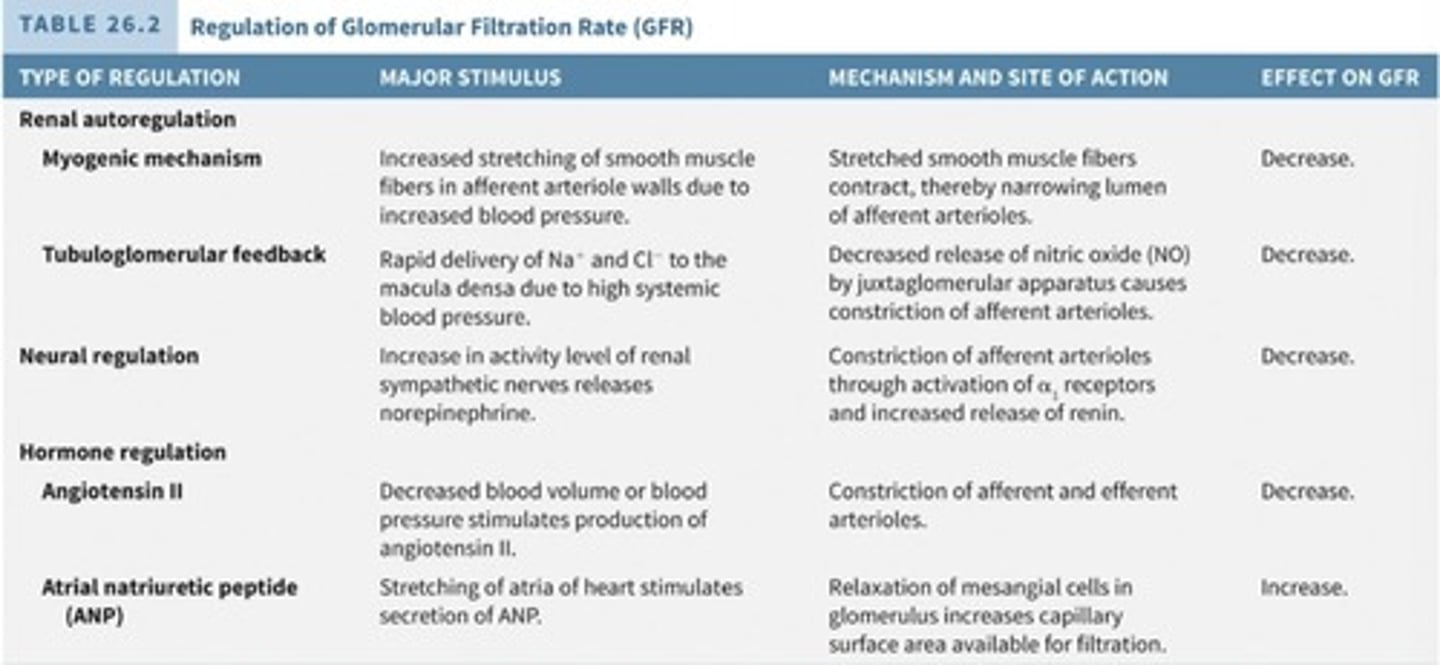
Renal Autoregulation
Includes myogenic mechanism and tubuloglomerular feedback to control GFR.
Myogenic Mechanism
Contracts afferent arteriole walls to reduce blood into kidney, lowering GFR, triggered by stretched arterioles.
Tubuloglomerular Feedback
Constriction of afferent arterioles (lowers GFR) by releasing less nitric oxide from juxtaglomerular apparatus, triggered by too much Na/Cl going into kidneys.
Neural Regulation
In cases of strong sympathetic stimulation, afferent arterioles are constricted, reducing urine output and increasing blood availability for other organs.
Hormonal Regulation
Includes angiotensin II, which constricts afferents and efferent arterioles, decreasing GFR, and atrial natriuretic peptide (ANP), which relaxes mesangial cells, increasing capillary surface area and GFR.
Glomerular Blood Hydrostatic Pressure (GDHP)
Pressure that causes stuff to leave kidney (55 mmHg).
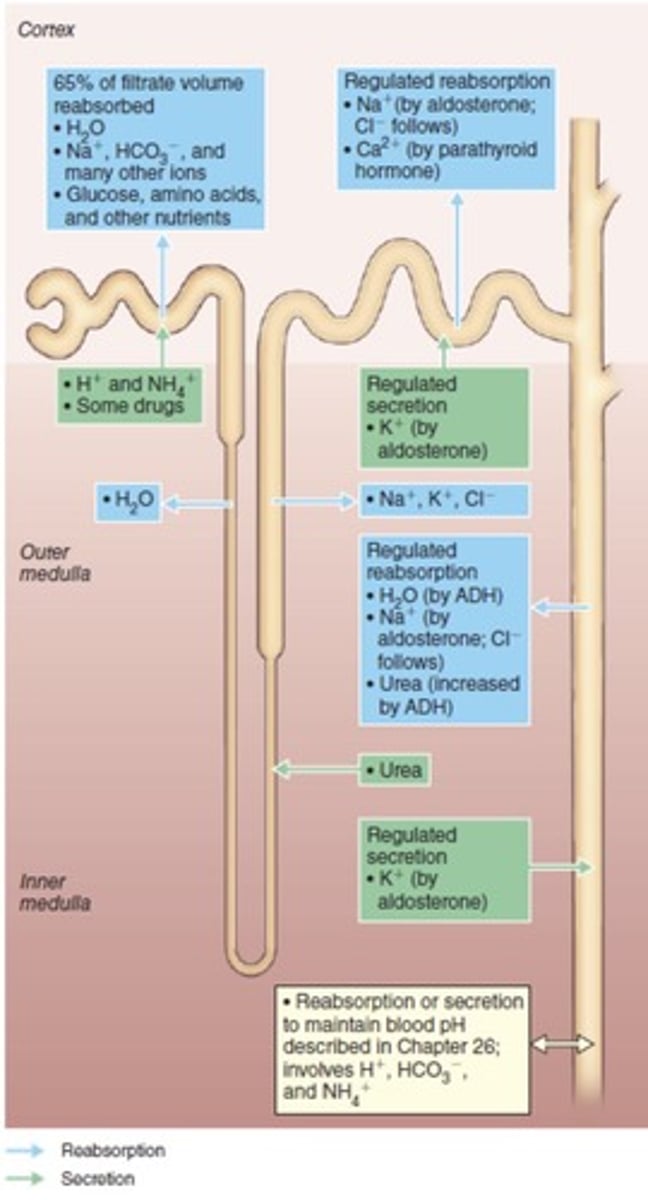
Tubular reabsorption
The process by which most of the filtrate is reabsorbed, especially water, glucose, amino acids, and ions.
Secretion
Helps to manage pH and rid the body of toxic and foreign substances.
Urine production
Healthy individuals form about 2 liters of urine.
Primary active transport
Uses ATP, like Na+/K+ pumps, and at rest accounts for 6% of total body ATP use.
Secondary active transport
Driven by ion's electrochemical gradient.
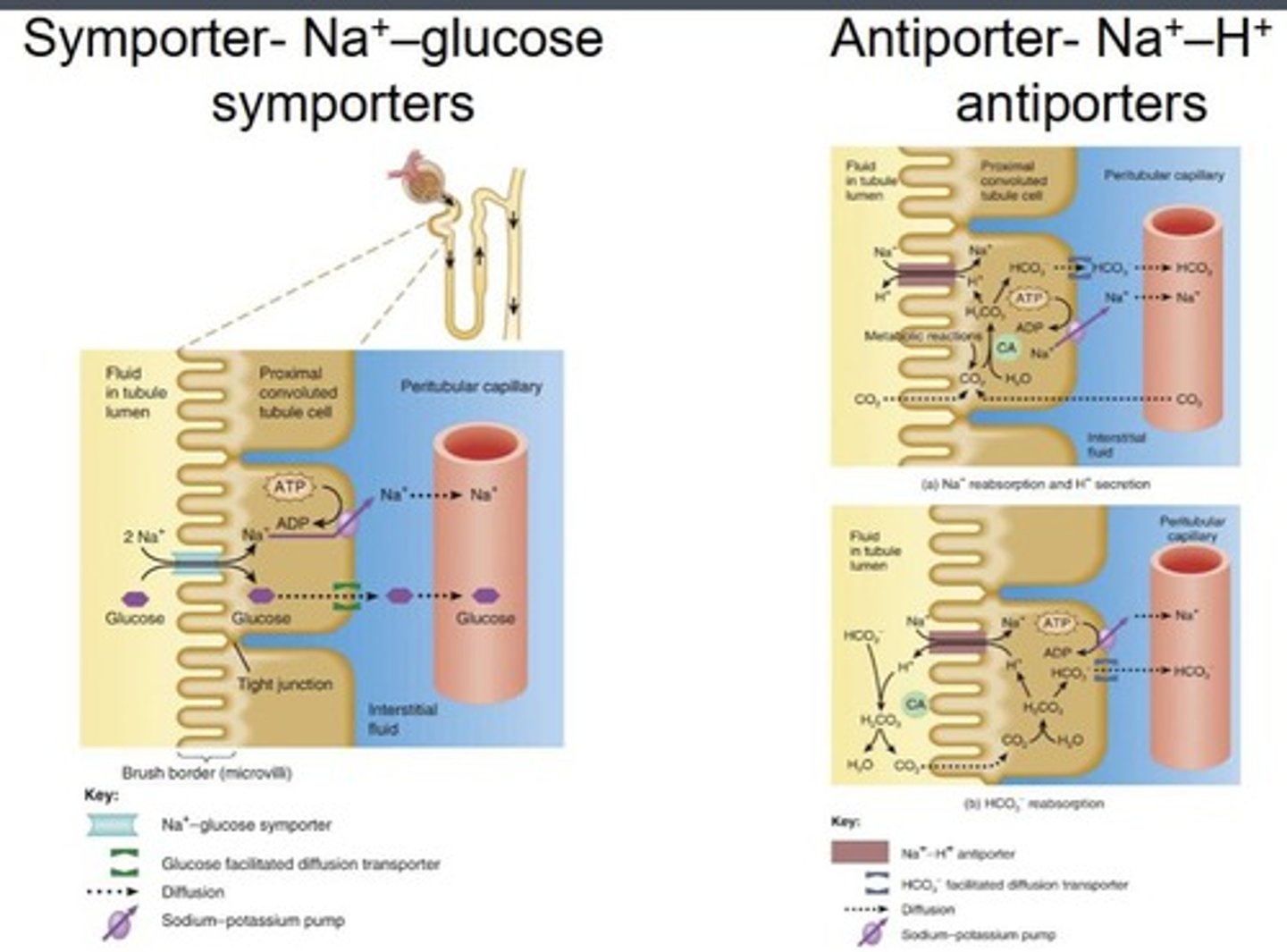
Symporters
Transport proteins that move substances in the same direction, such as Na+ - glucose.
Antiporters
Transport proteins that move substances in opposite directions, such as Na+ - H+.
Obligatory water reabsorption
90% of water reabsorption that occurs as water follows the solutes that are reabsorbed.
Facultative water reabsorption
10% of water reabsorption that is regulated by ADH (antidiuretic hormone).
Metabolic acidosis
Condition where sodium hydrogen antiport is not working, causing hydrogen ions to remain in the body and increase acidity.
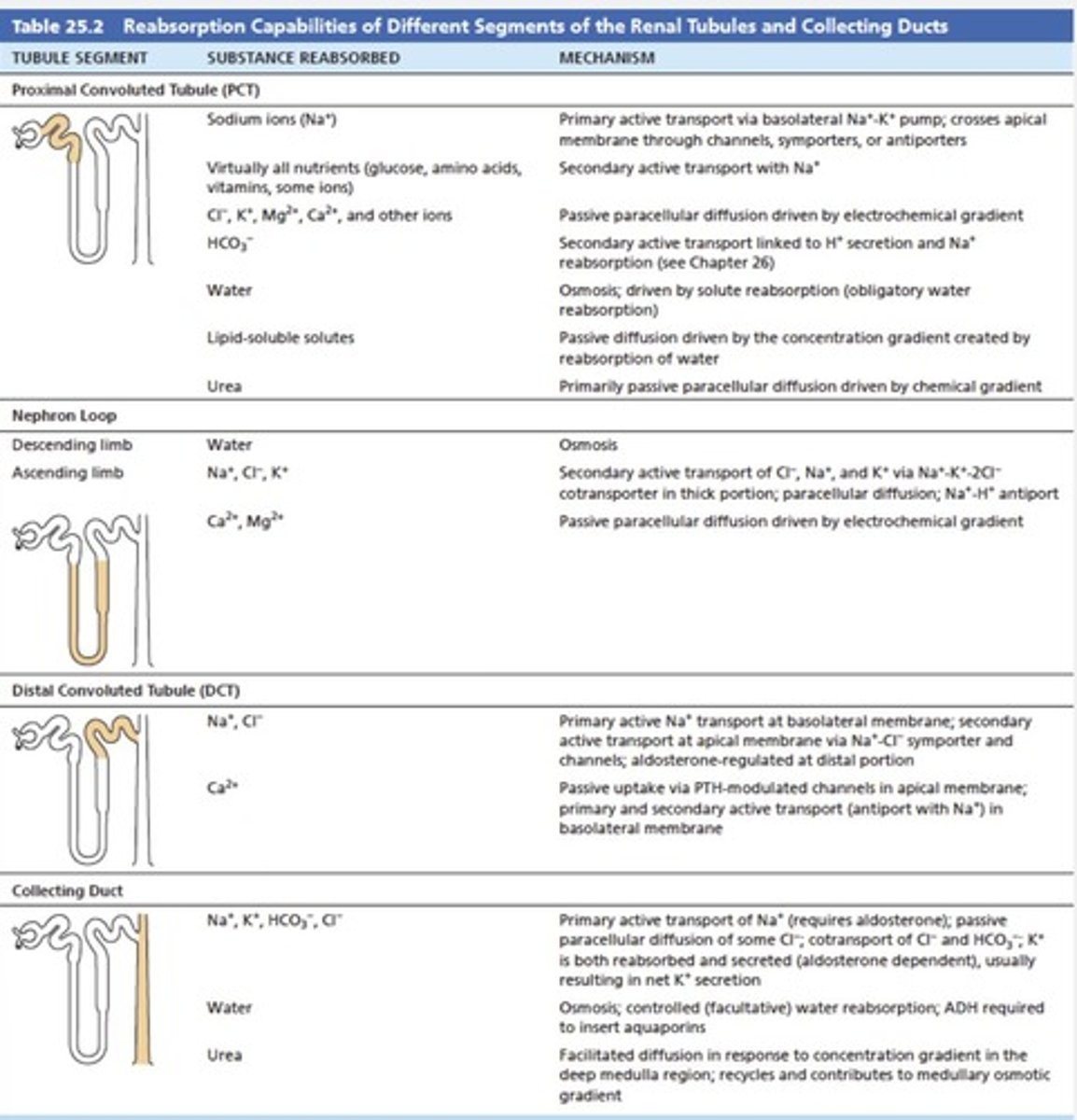
Passive transport
The movement of substances such as Cl, K, Ca, Mg, and Urea into capillaries by diffusion and water into capillaries by osmosis.
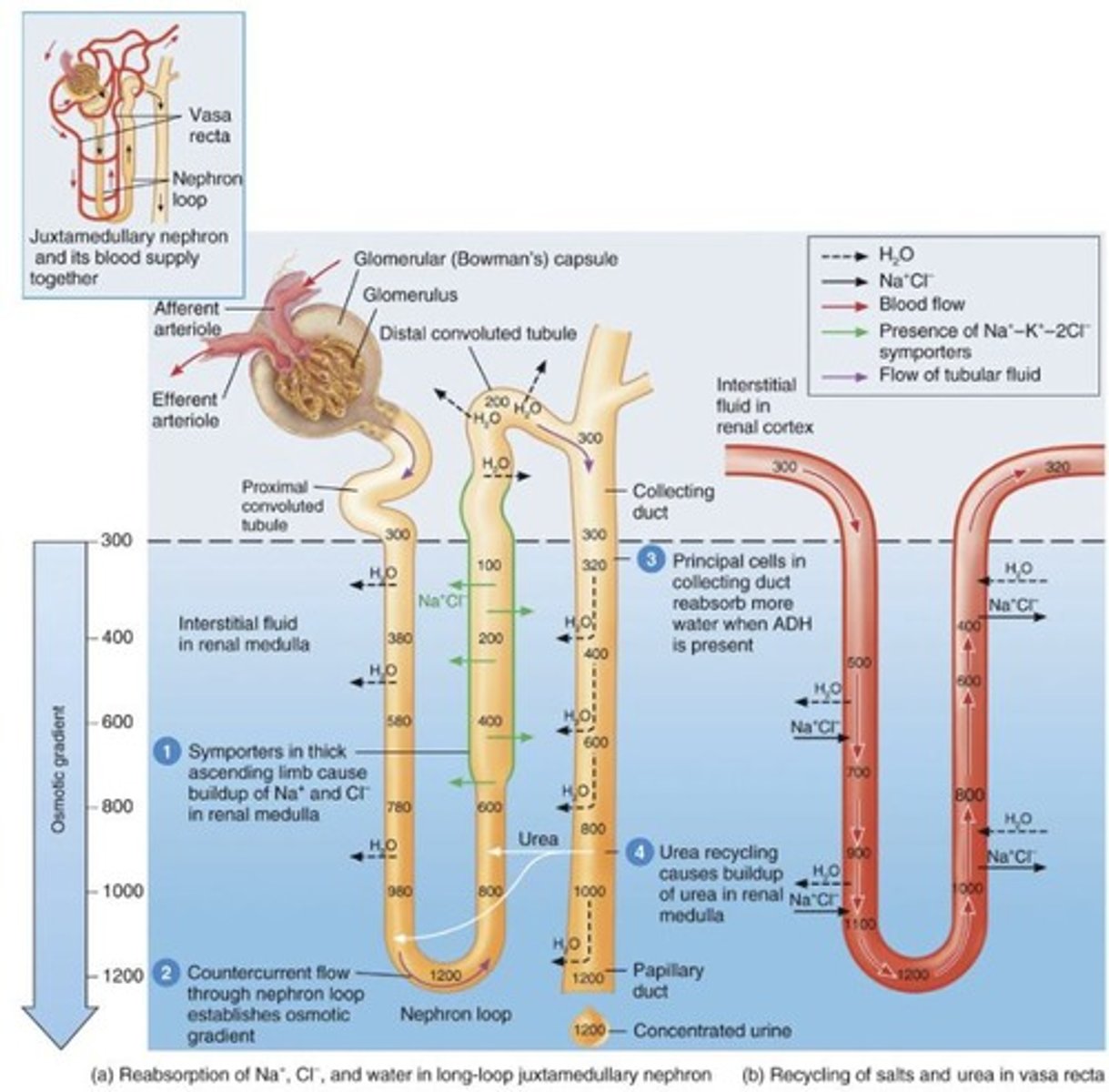
Loop of Henle
Part of the nephron where reabsorption occurs, with the descending limb continuing water reabsorption and the ascending limb only reabsorbing solutes.
Descending limb
Part of the Loop of Henle that continues water reabsorption.
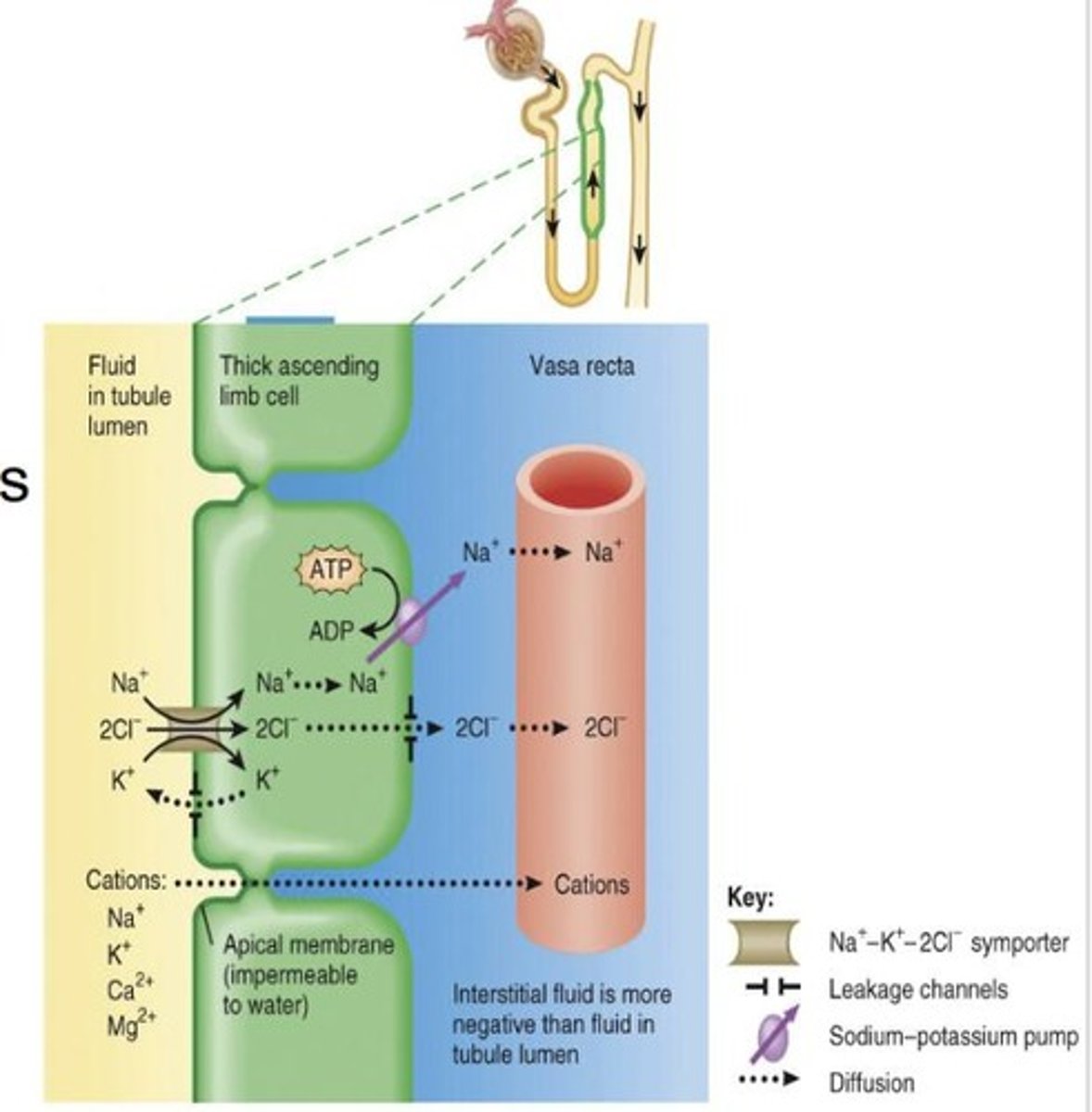
Ascending limb
Part of the Loop of Henle that is relatively impermeable to water and only reabsorbs solutes.
Proximal convoluted tubule (PCT)
Site of constant water and solute reabsorption.
Distal convoluted tubule (DCT)
Site of variable/controlled water reabsorption and final adjustments in tubular fluid composition.
Collecting ducts
Final site for urine composition adjustment, where variable water reabsorption is stimulated by ADH.
Na+ - Cl- symporters
Transport proteins in the DCT that reabsorb ions.
PTH (Parathyroid hormone)
Stimulates reabsorption of Ca2+ and inhibits phosphate reabsorption in the PCT.
Glomerulus
Site where filtrate is made at the renal corpuscle, having the same composition as blood plasma minus plasma proteins.
Renal pelvis
Final destination of filtrate after passing through various parts of the nephron.
Vasa Recta arterioles
Absorb solutes and water reabsorbed by nephron/collecting ducts, maintaining concentration gradient in medulla.