BIO 300 Lecture10.IntroToCardio Review
1/69
Earn XP
Description and Tags
BIO 300 Pathophysiology
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
70 Terms
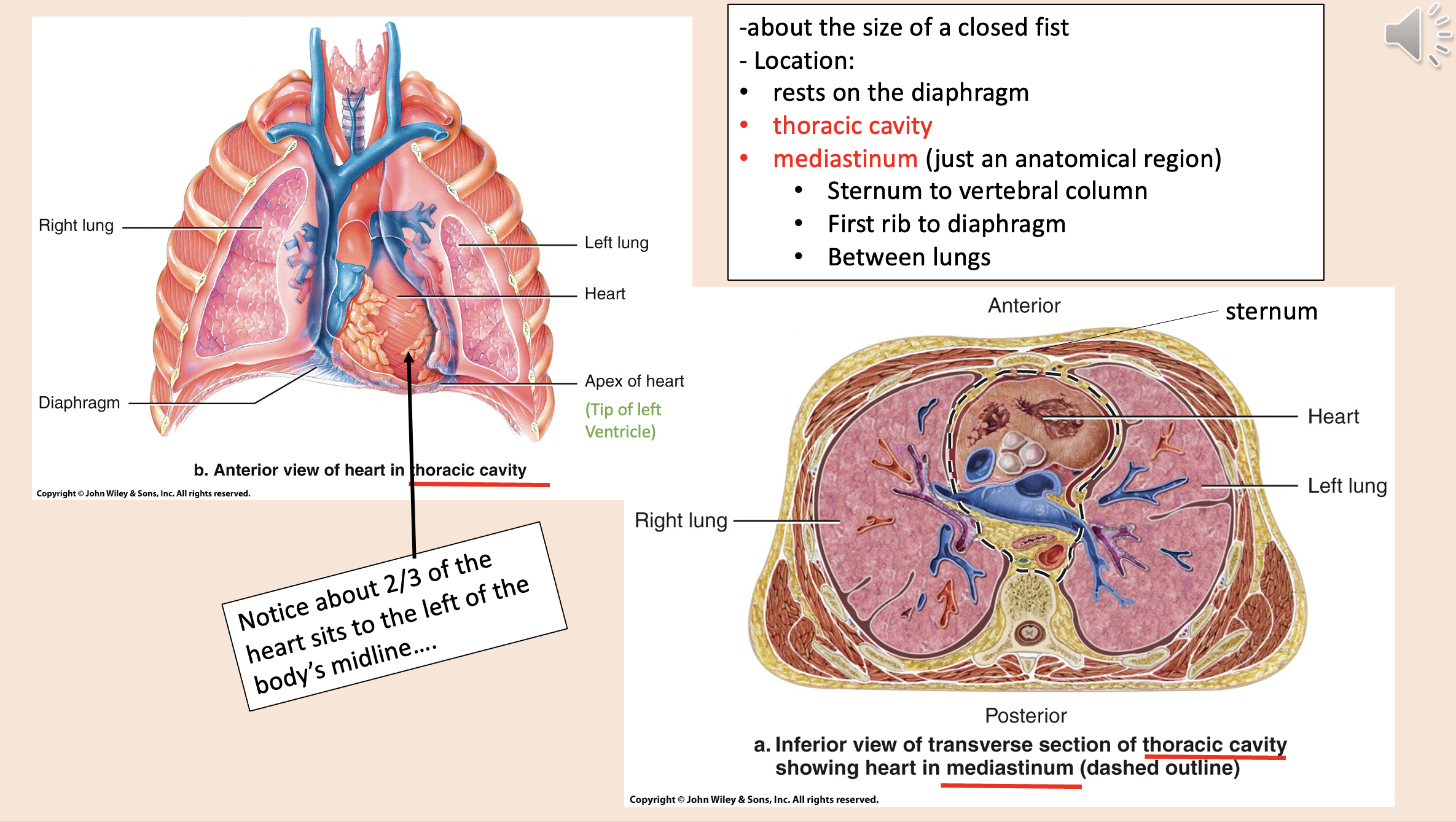
Heart Location:
rests on the diaphragm
thoracic cavity
mediastinum
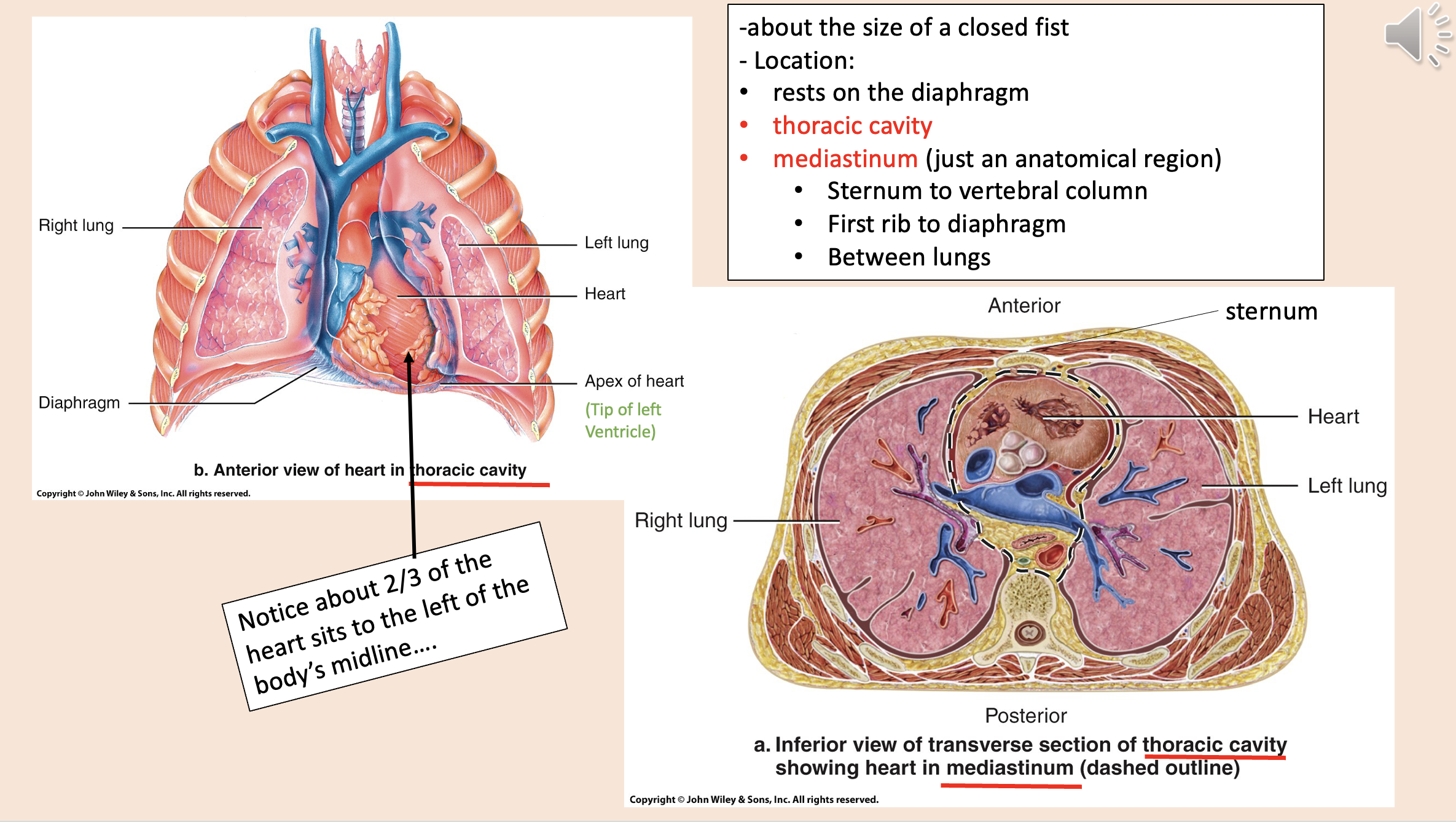
Sternum to vertebral column.
First rib to diaphragm.
Between lungs.
mediastinum
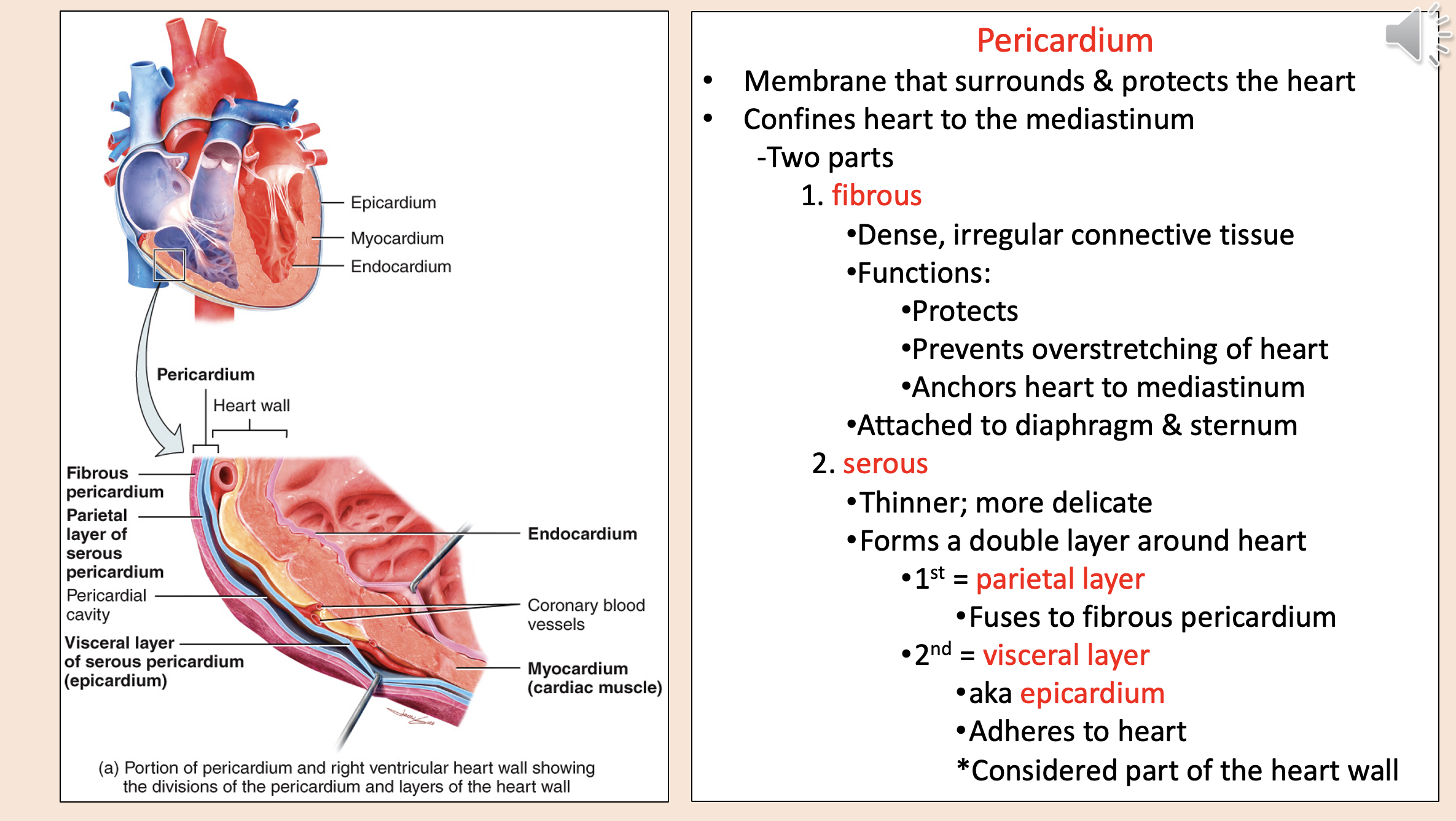
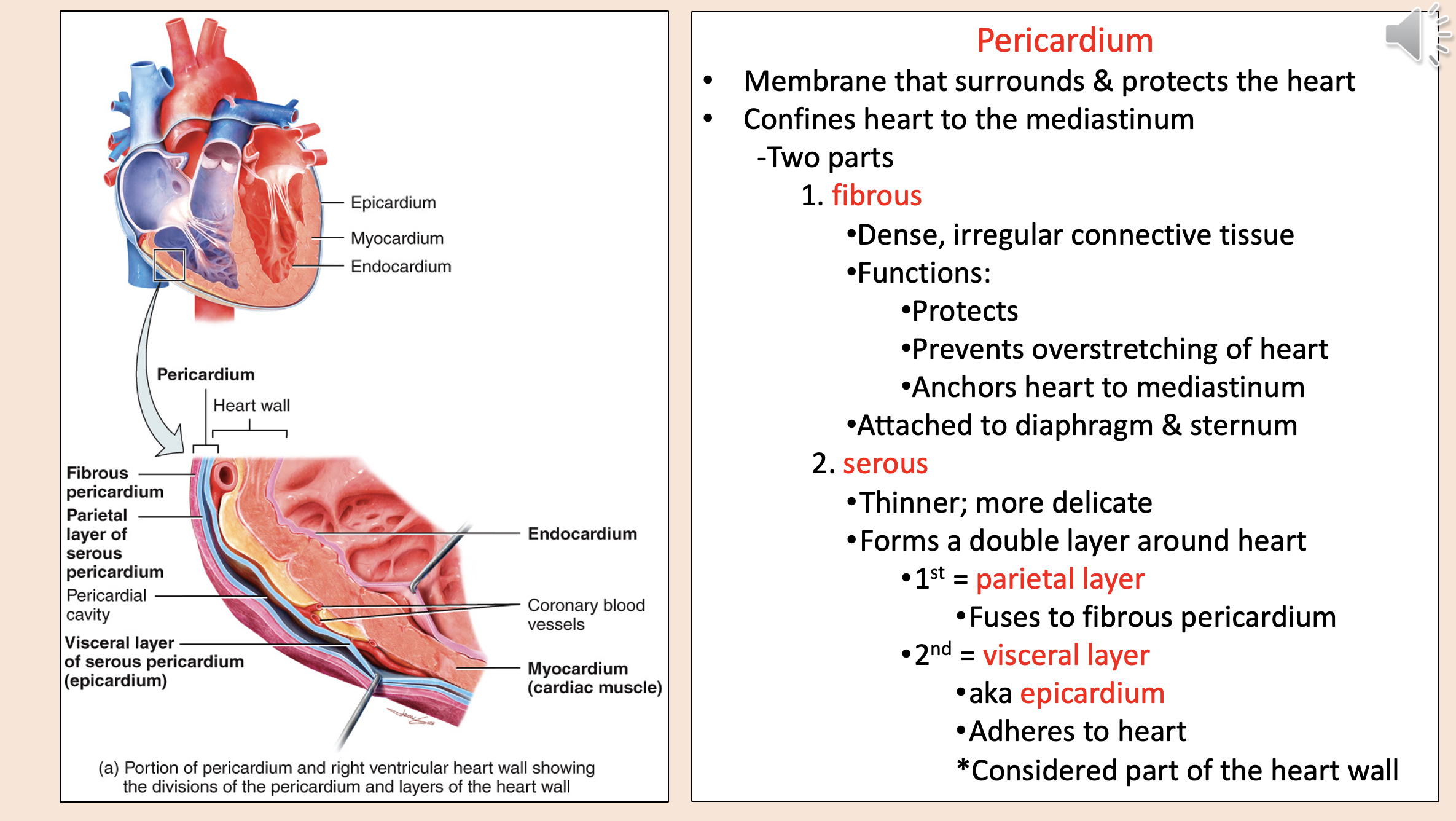
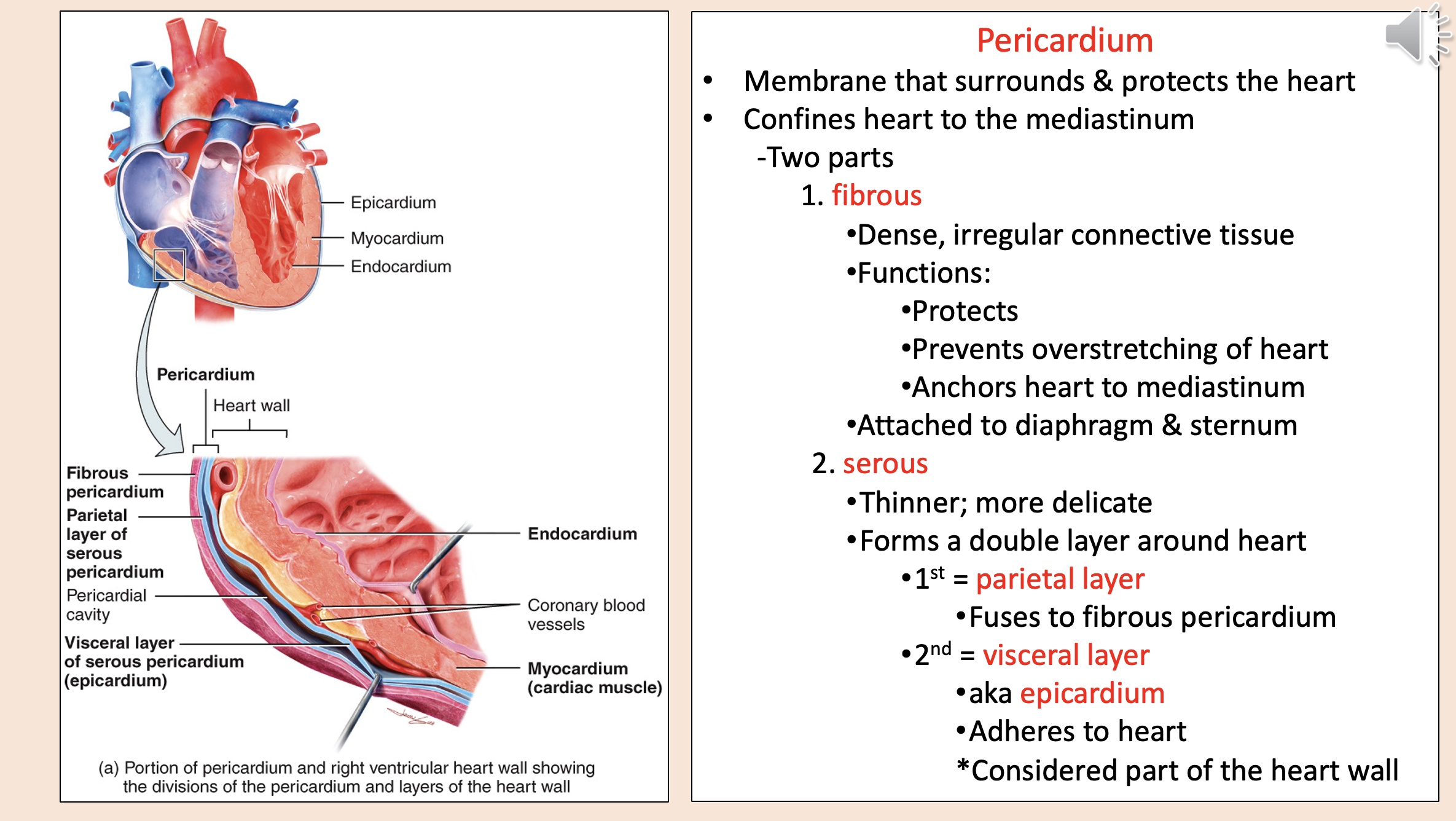
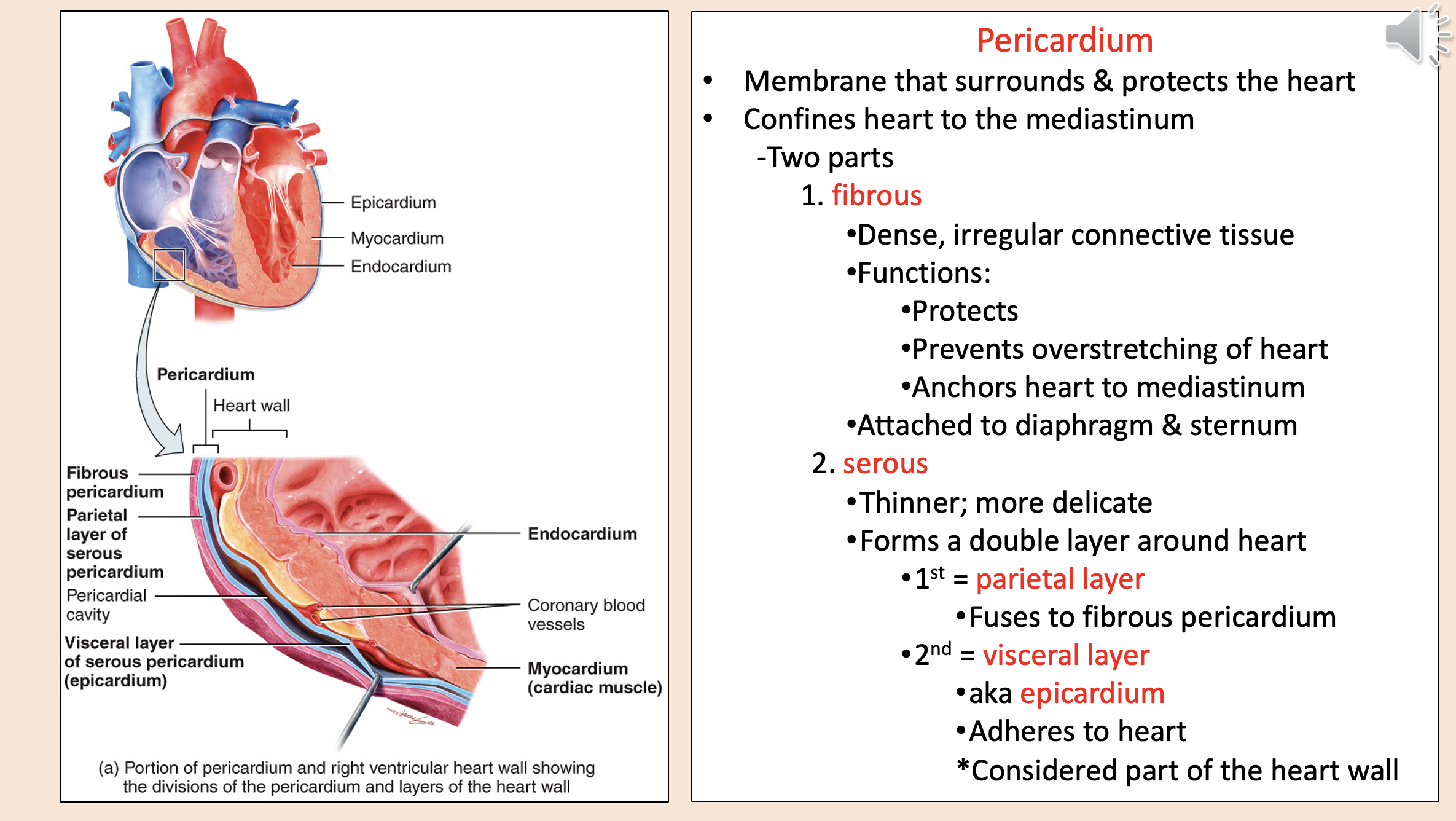
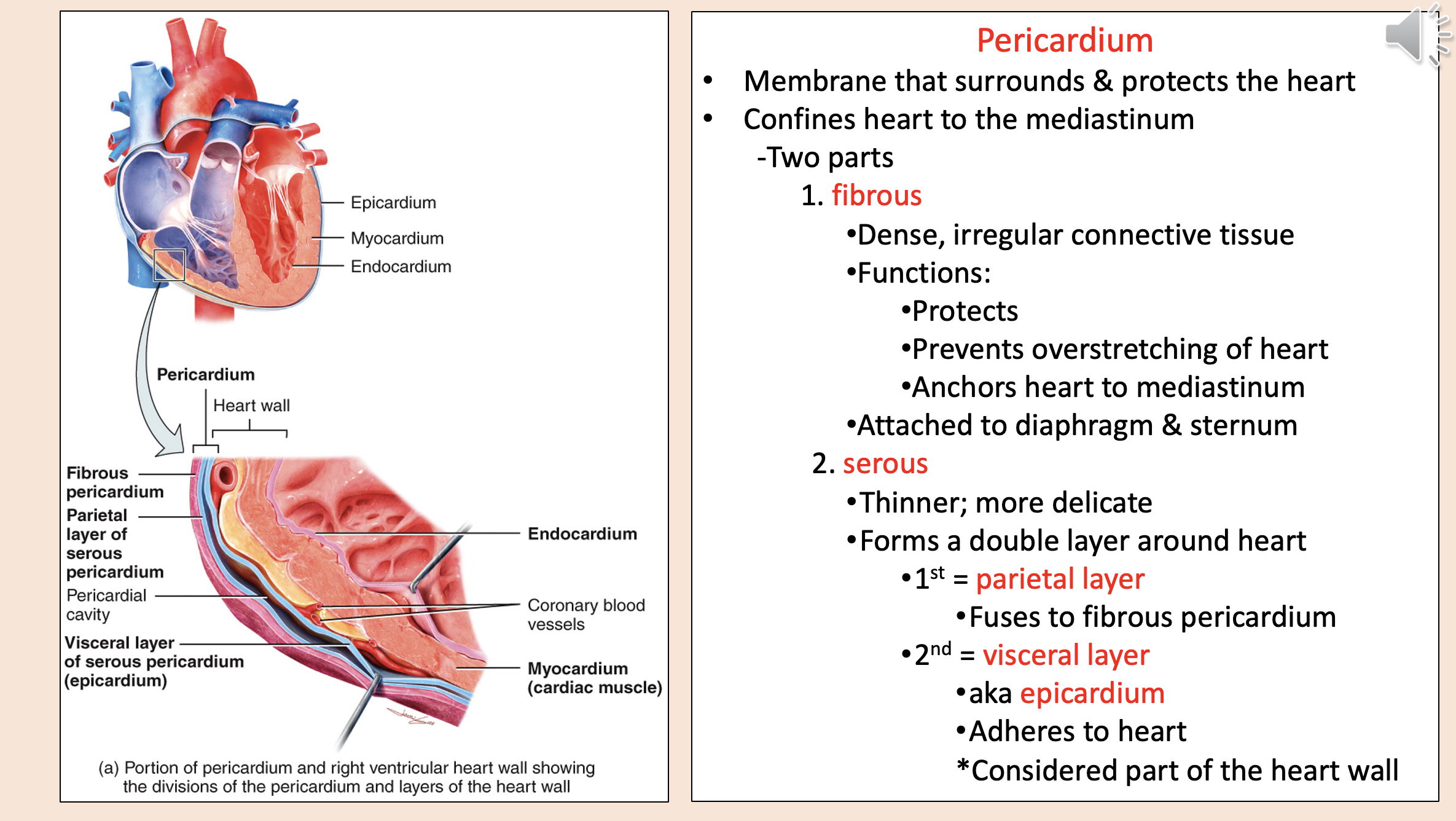
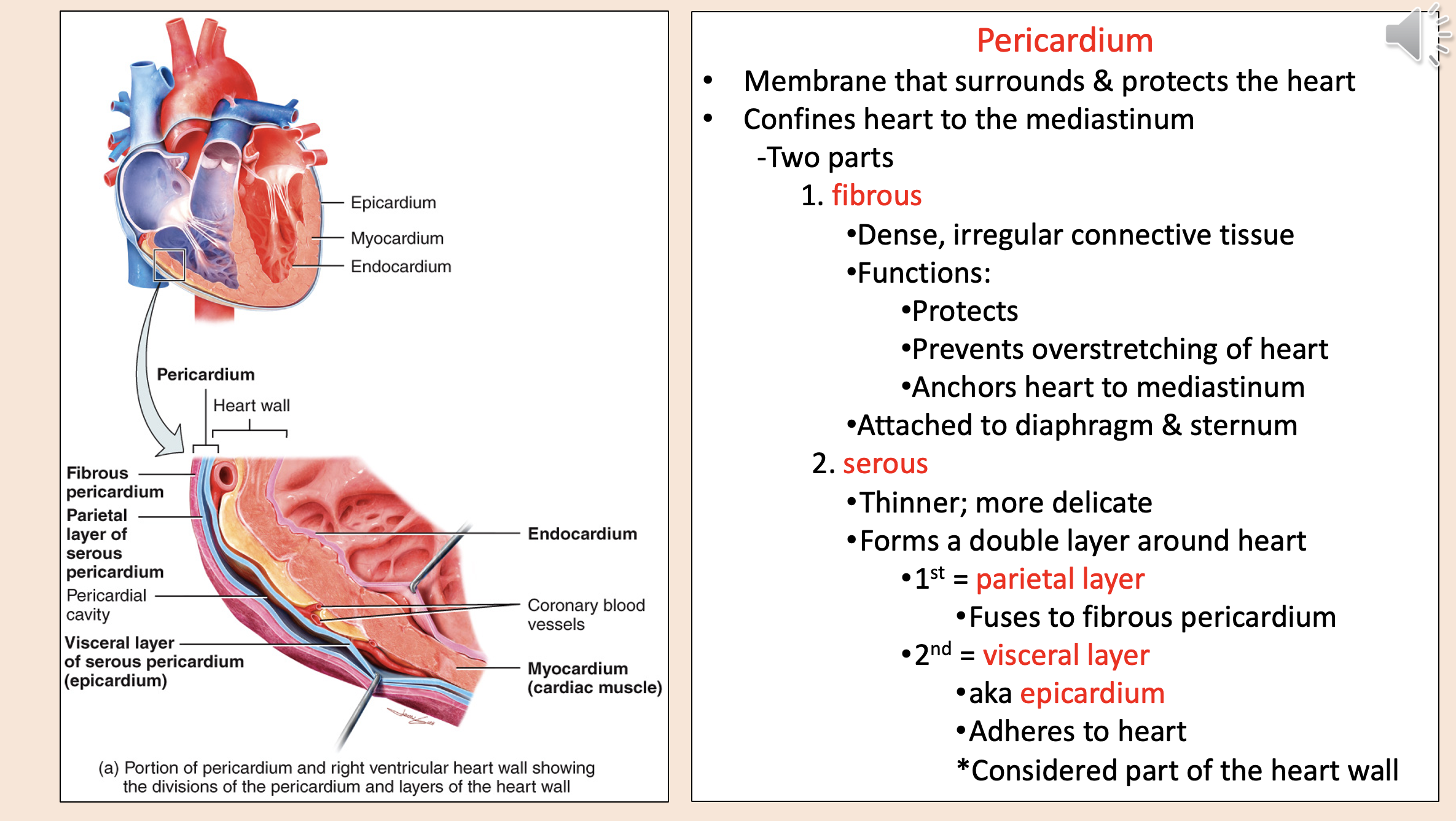
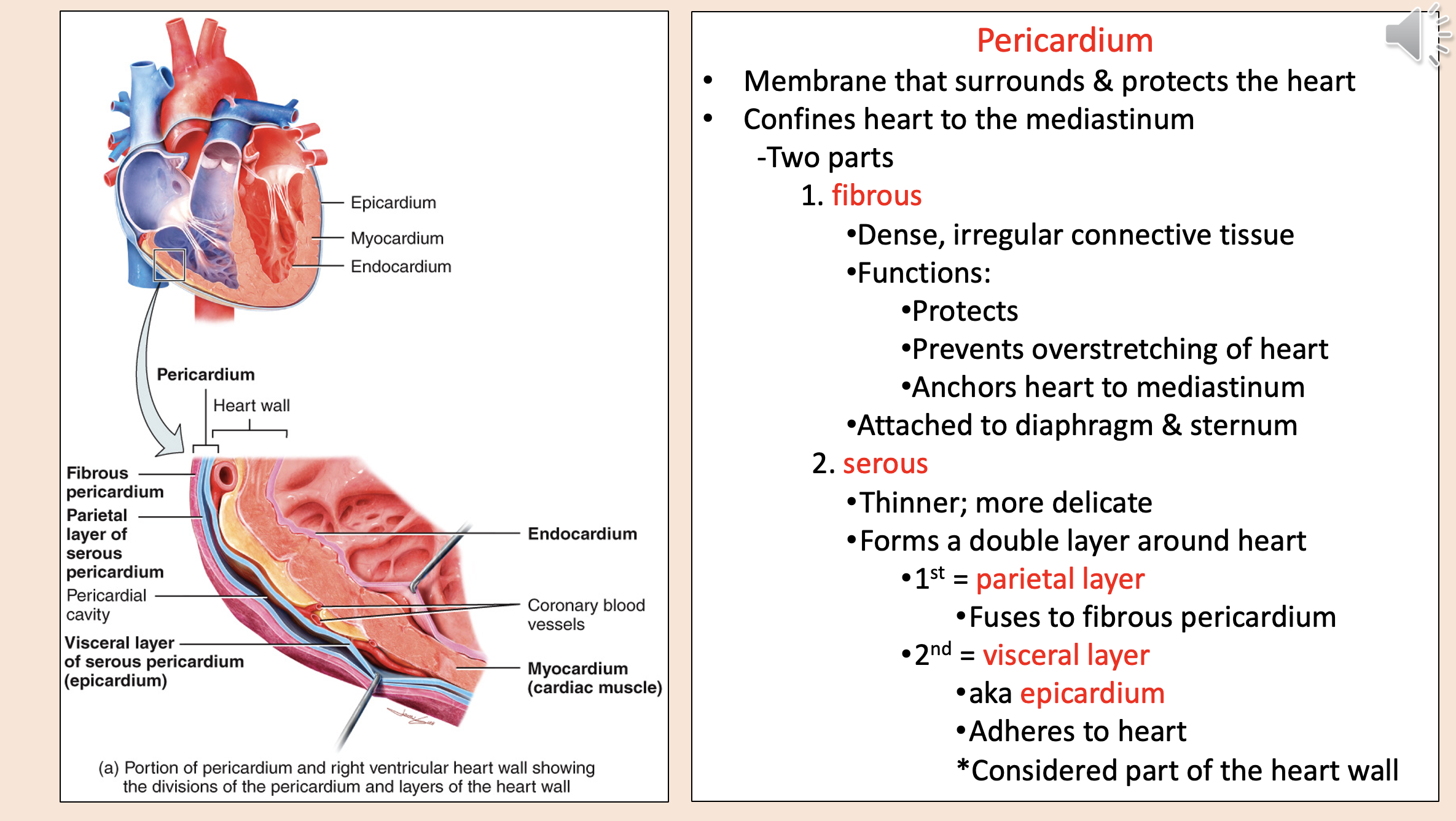
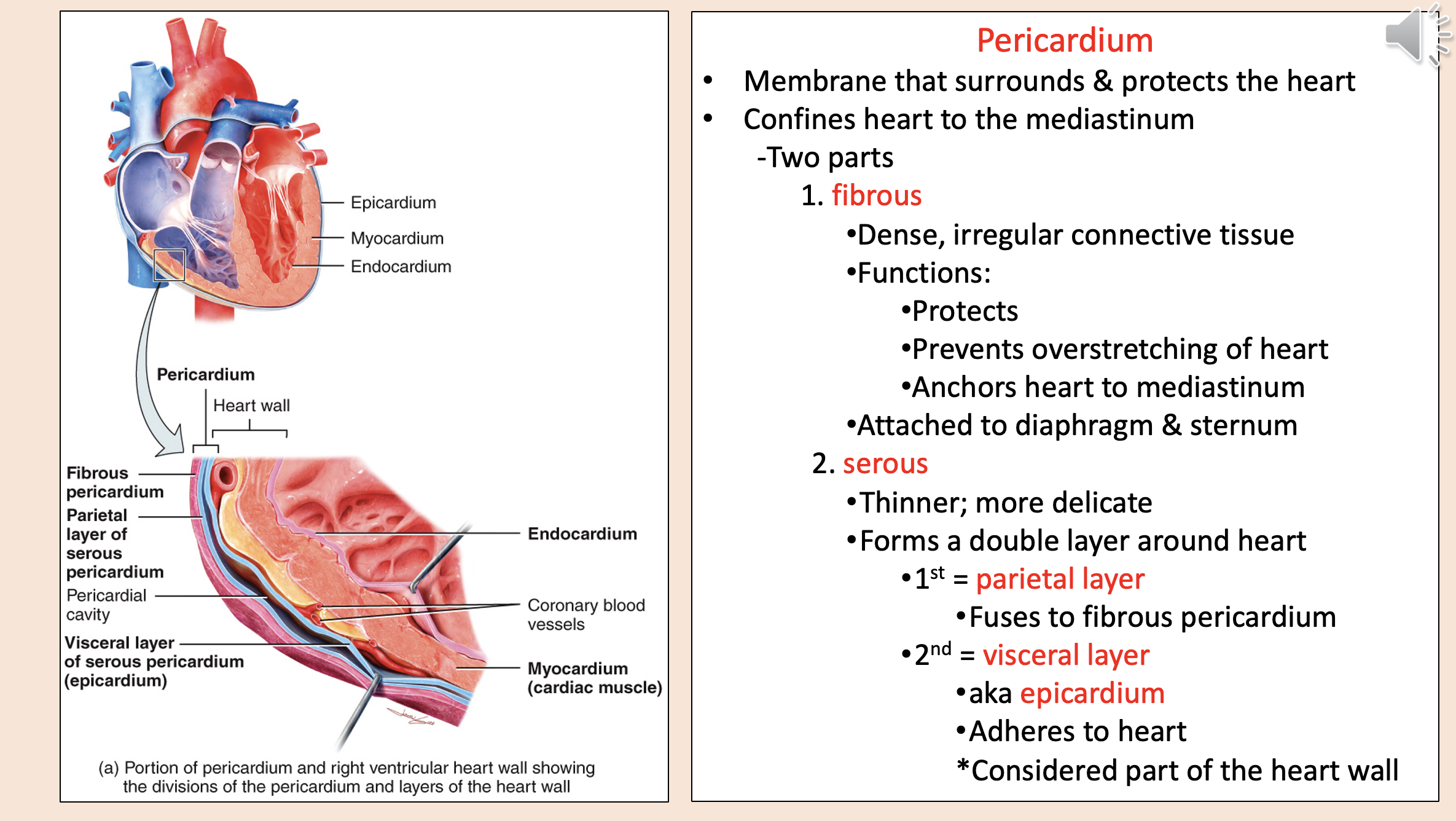
Structural layers of the heart and its protective covering from outermost to innermost
endocardium
myocardium
coronary blood vessels
visceral layer of serous pericardium epicardium
pericardial cavity
parietal layer of serous pericardium
fibrous pericardium
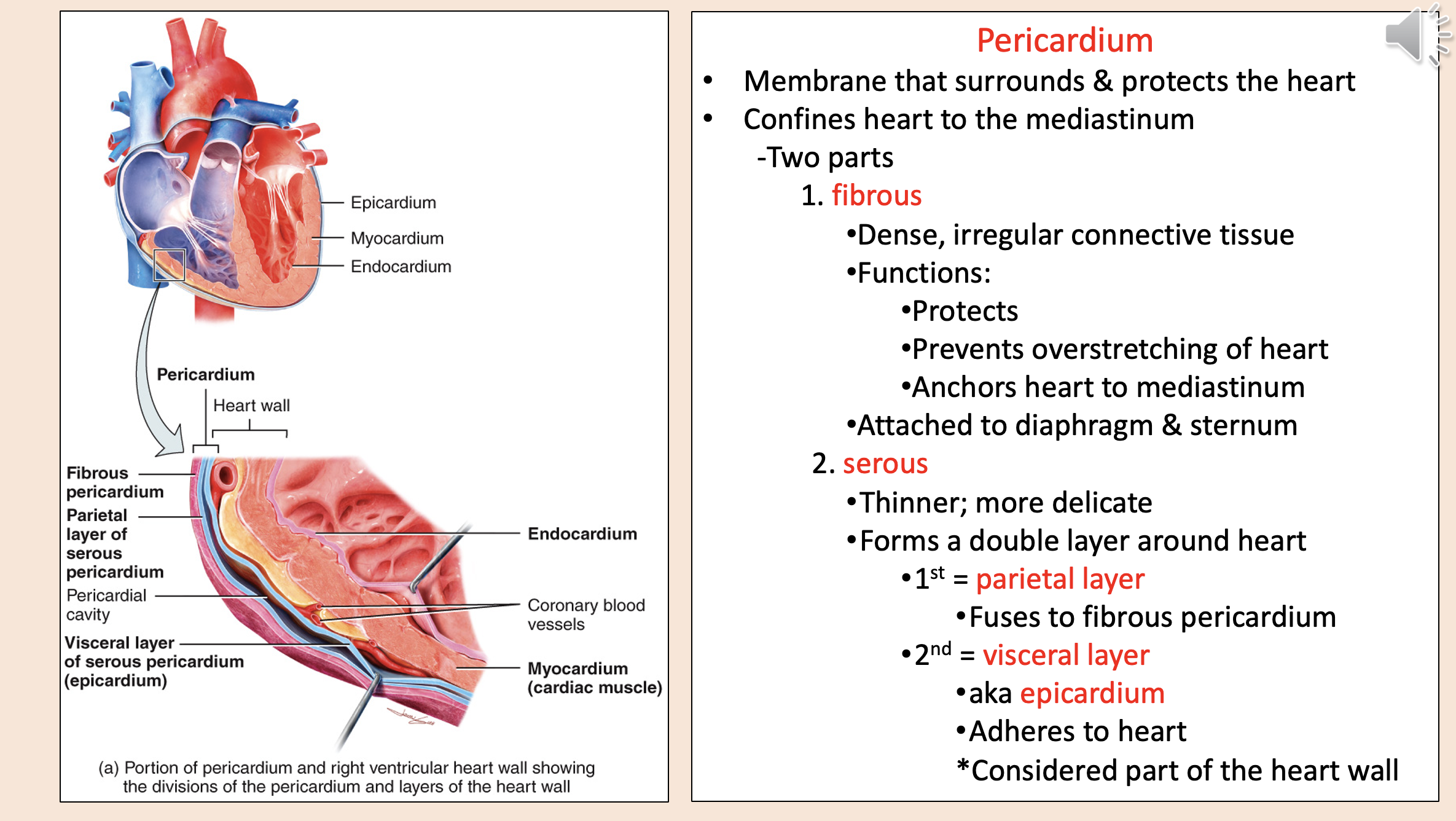
Membrane that surrounds & protects the heart.
Confines heart to the mediastinum.
pericardium
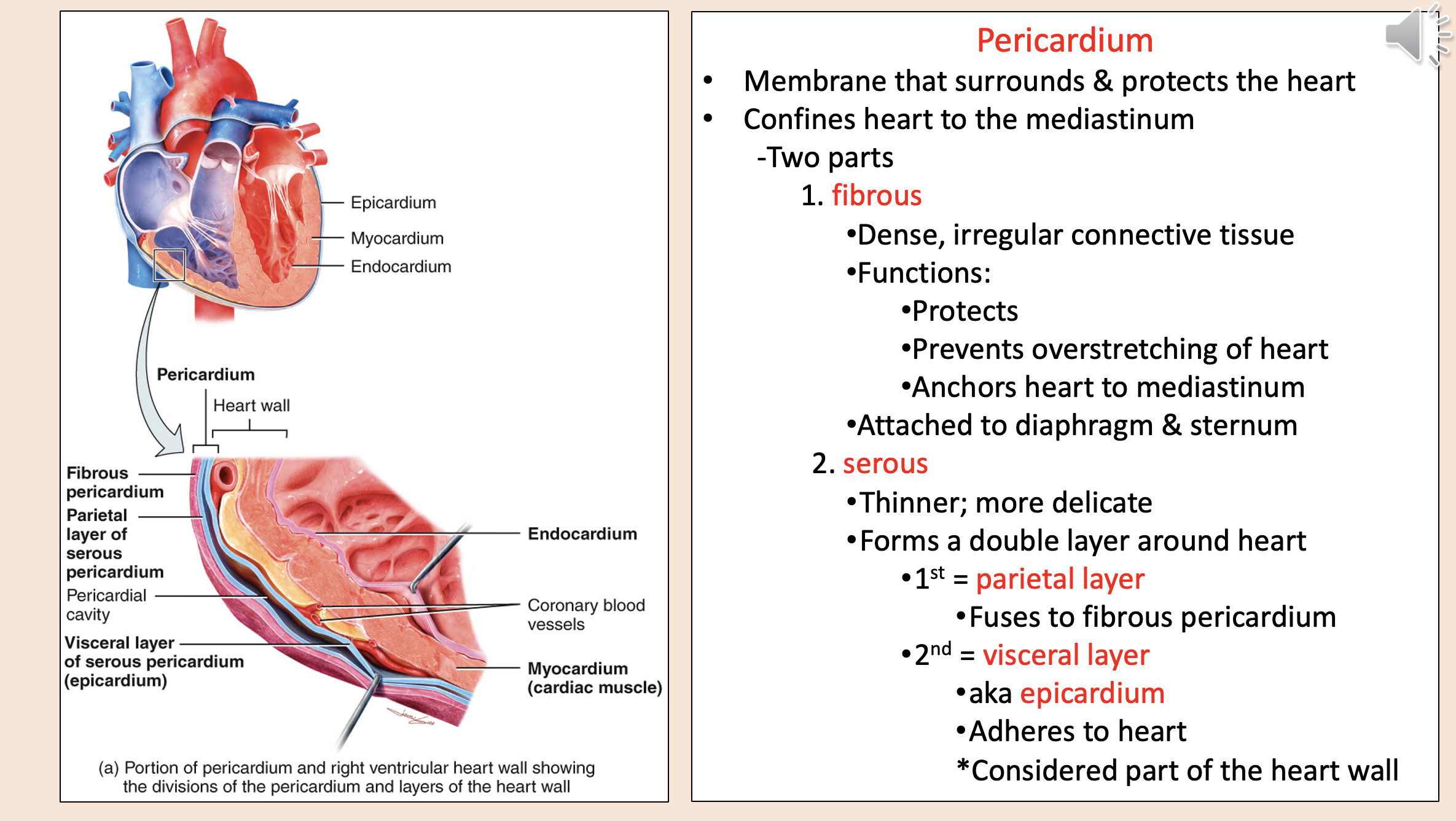
Two parts of pericardium
fibrous
serous
Dense, irregular connective tissue.
Partially fused to tendon of diaphragm.
fibrous
Fibrous Functions:
protects
prevents overstretching of heart
anchors heart to mediastinum
Thinner; more delicate.
Forms a double layer around heart.
serous
Serous Forms a double layer around heart:
parietal layer
visceral layer
Fuses to fibrous pericardium
parietal layer
aka epicardium
visceral layer
Adheres to heart.
Considered part of the heart wall.
visceral layer
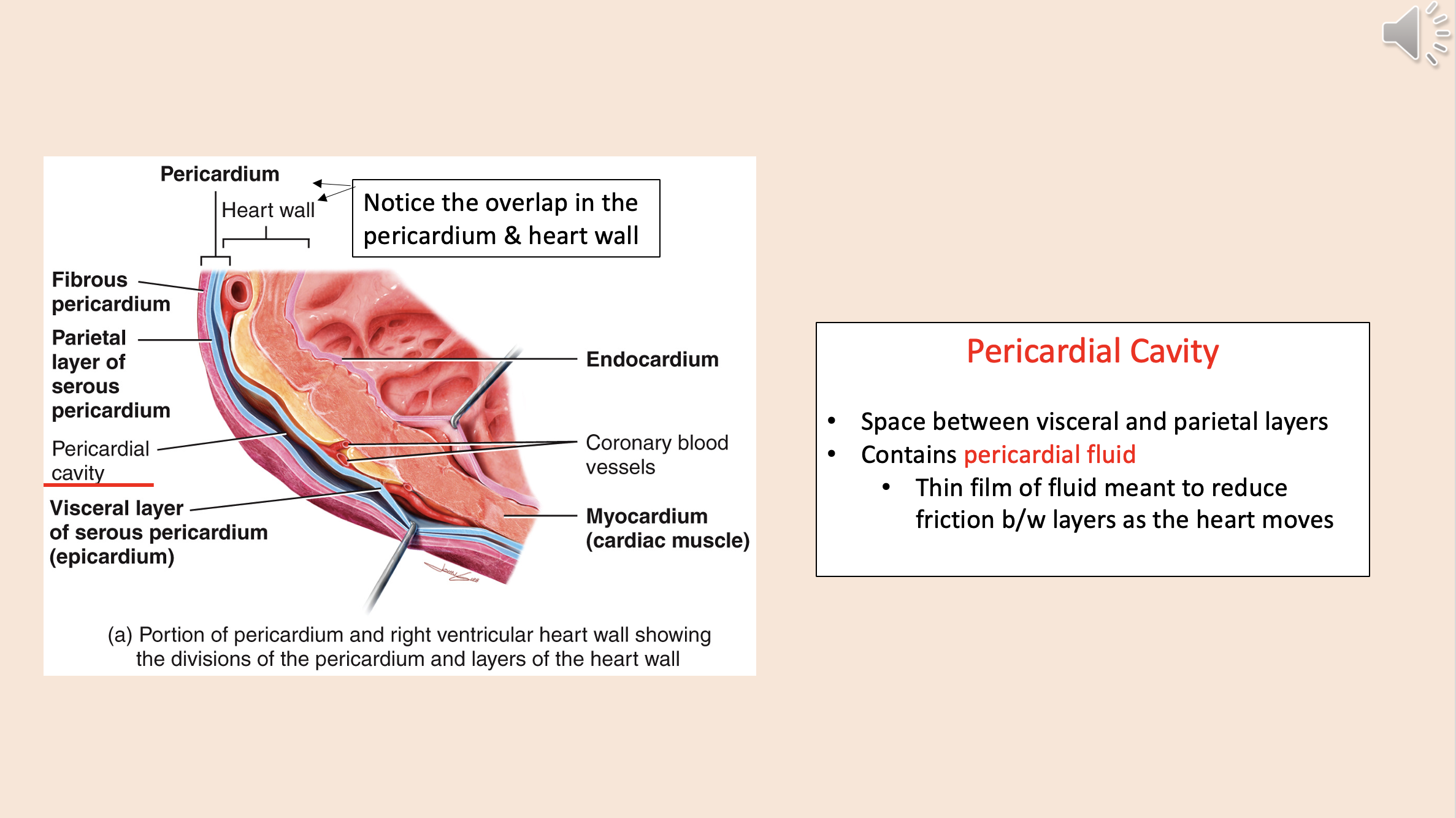
Space between visceral and parietal layers.
Contains pericardial fluid.
pericardial cavity
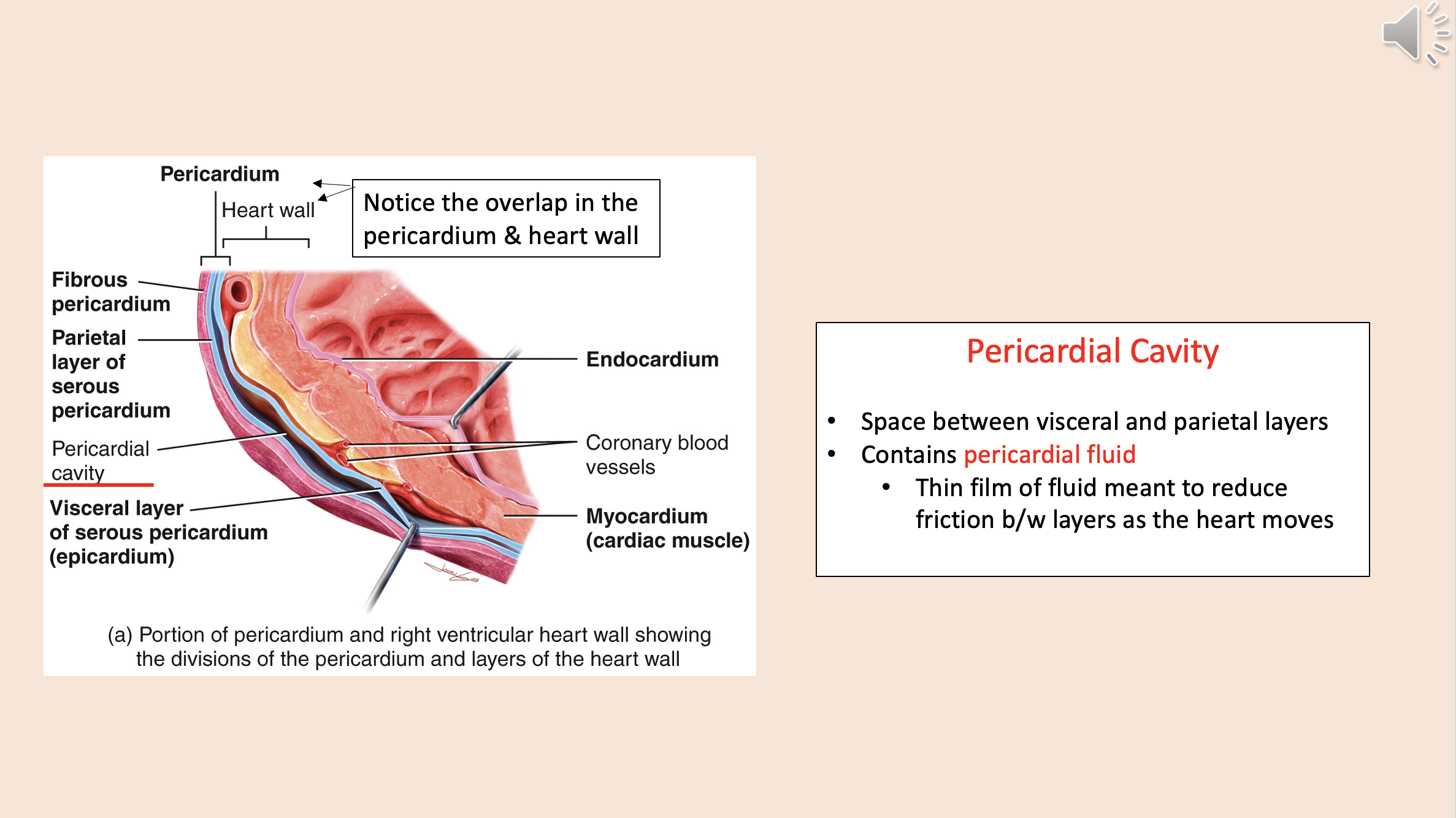
Thin film of fluid meant to reduce friction between layers as the heart moves
pericardial fluid
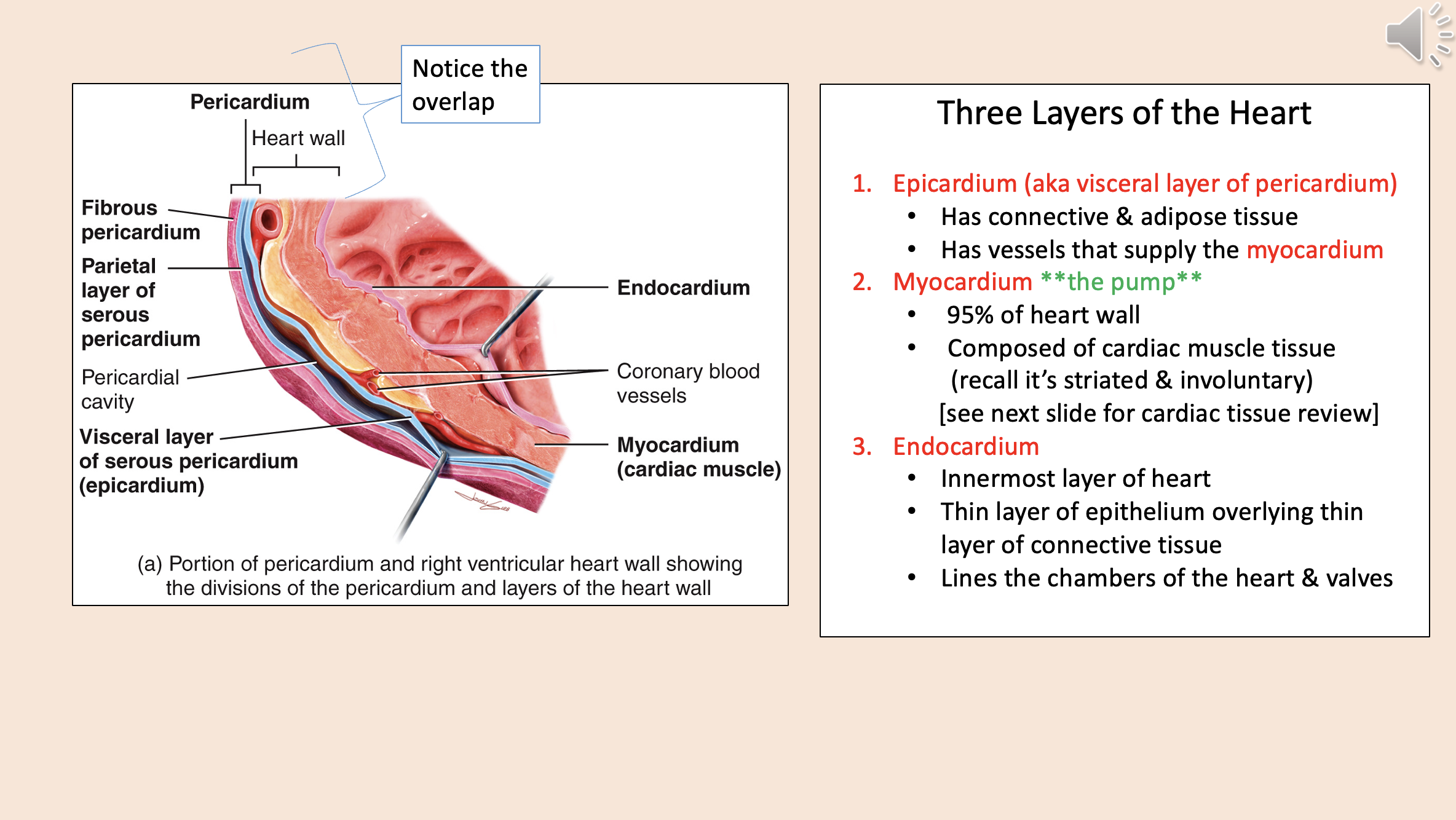
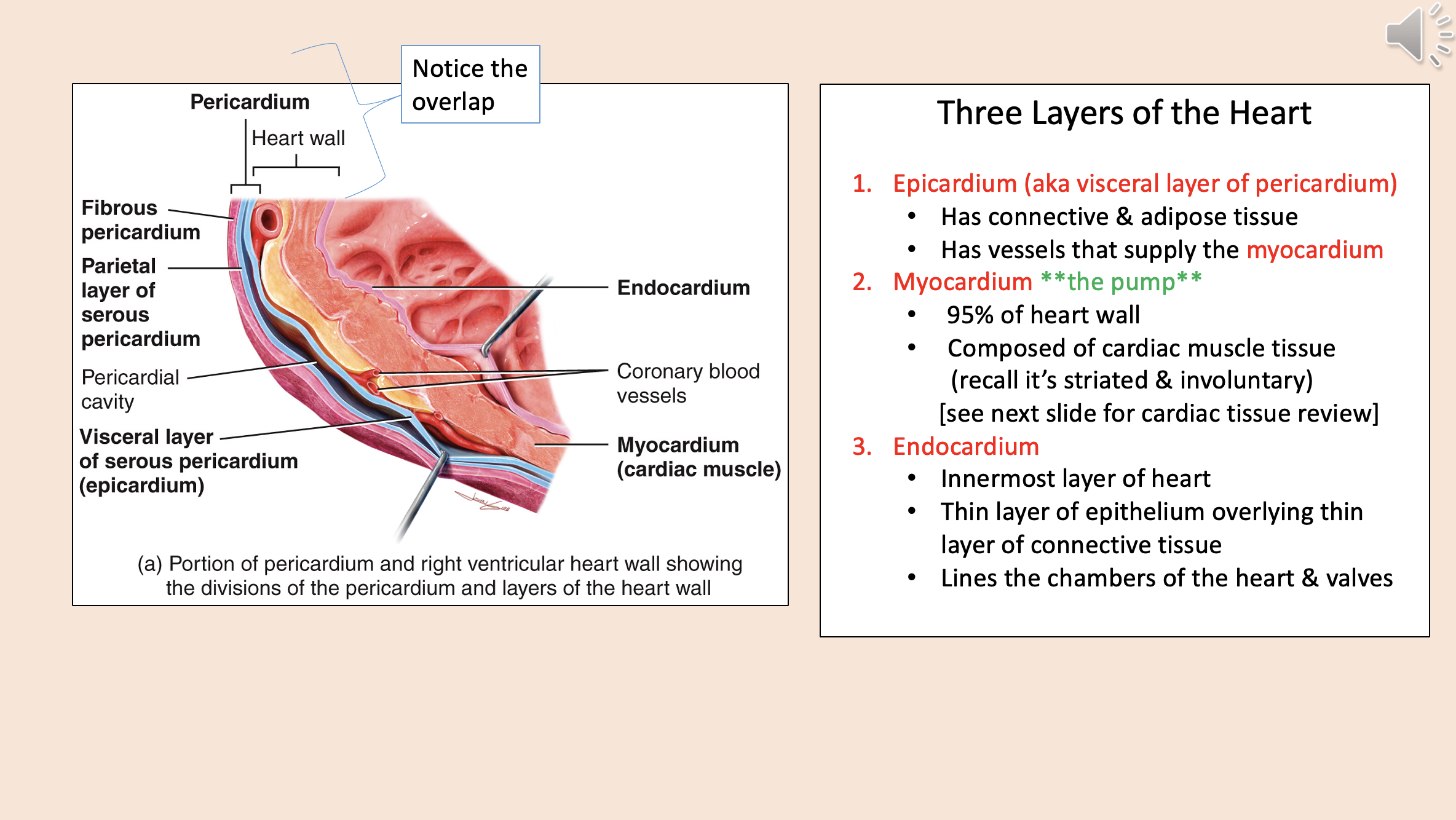
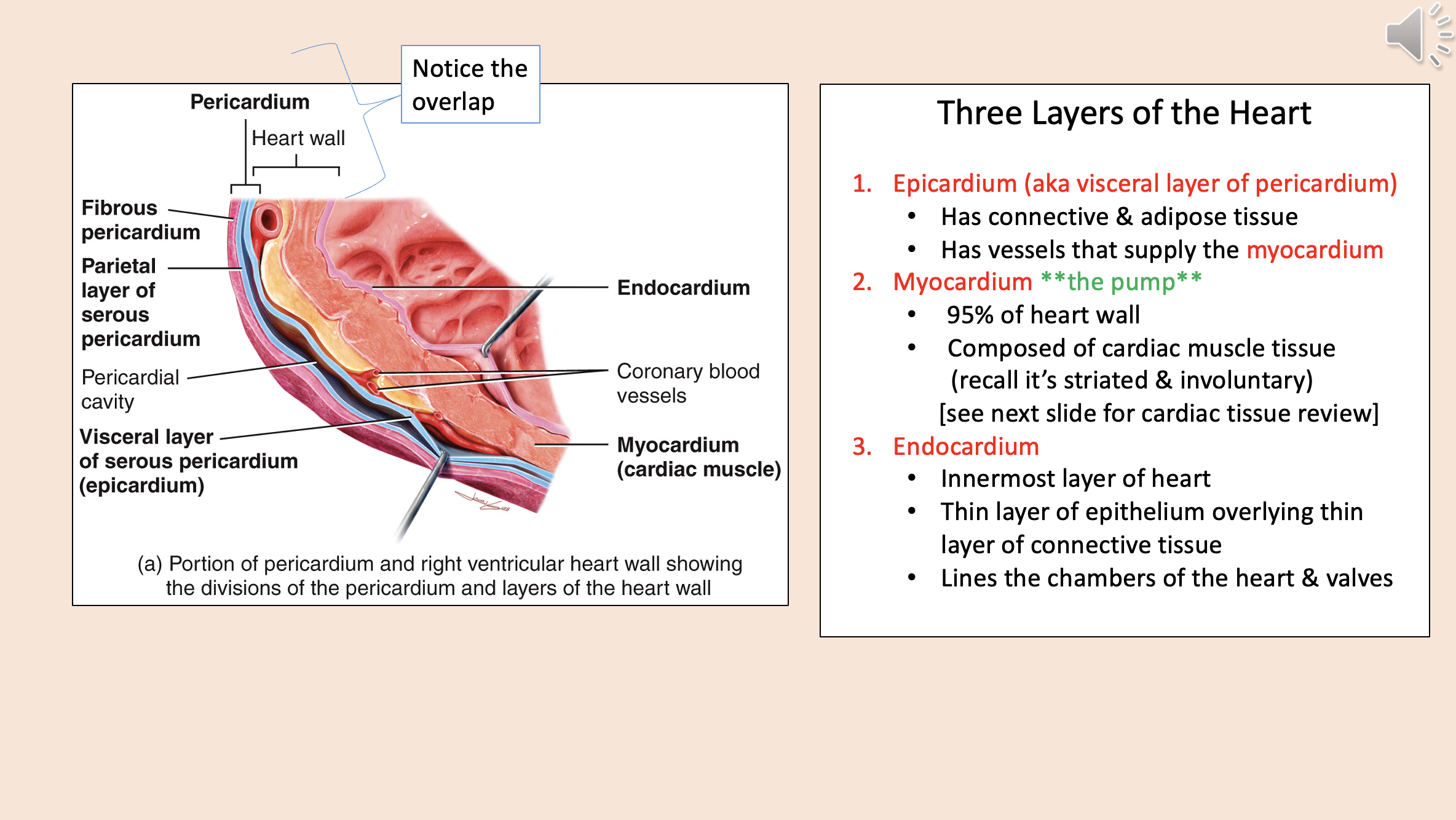
Three Layers of the Heart
epicardium
myocardium
endocardium
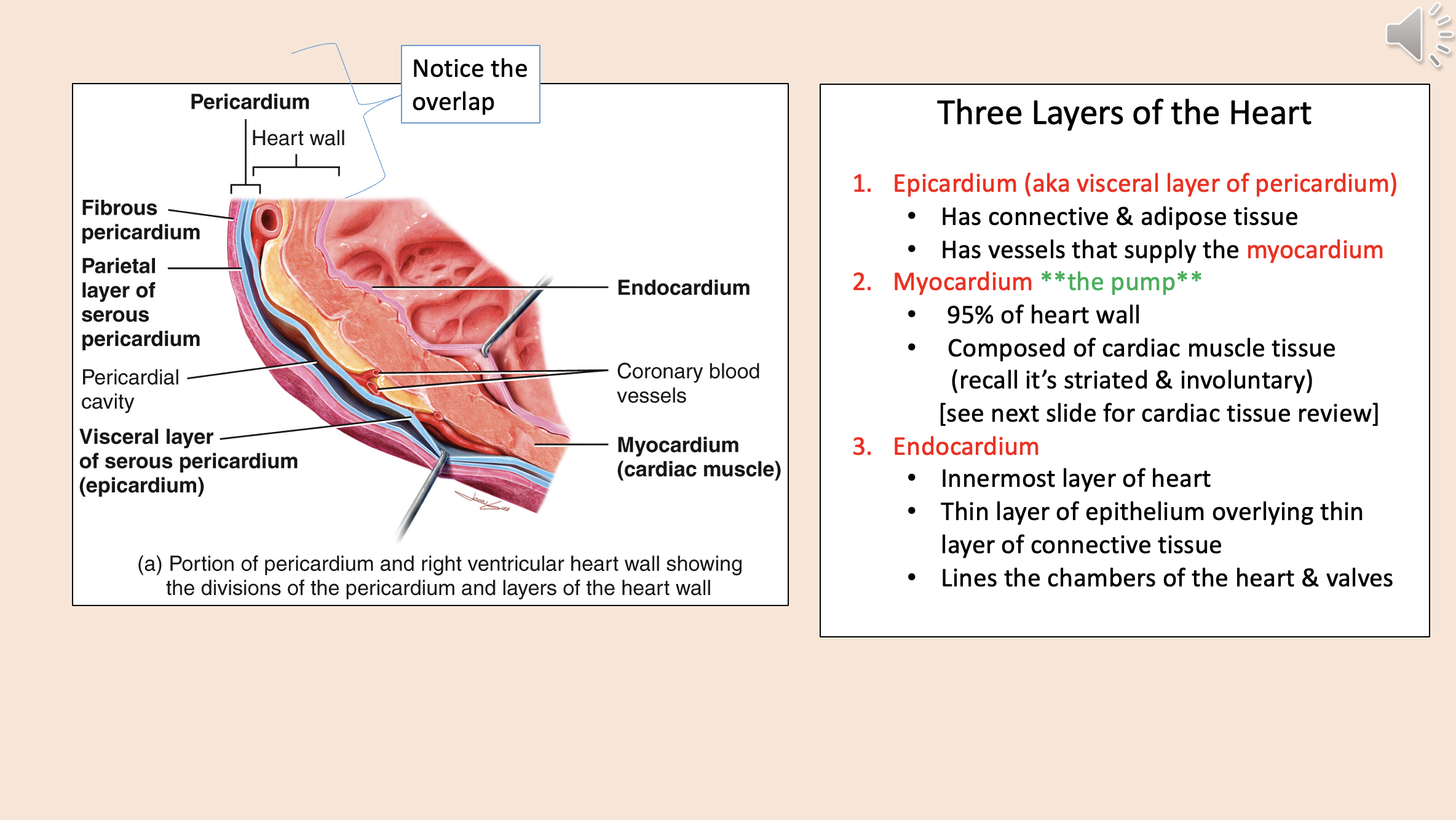
aka visceral layer of pericardium
epicardium
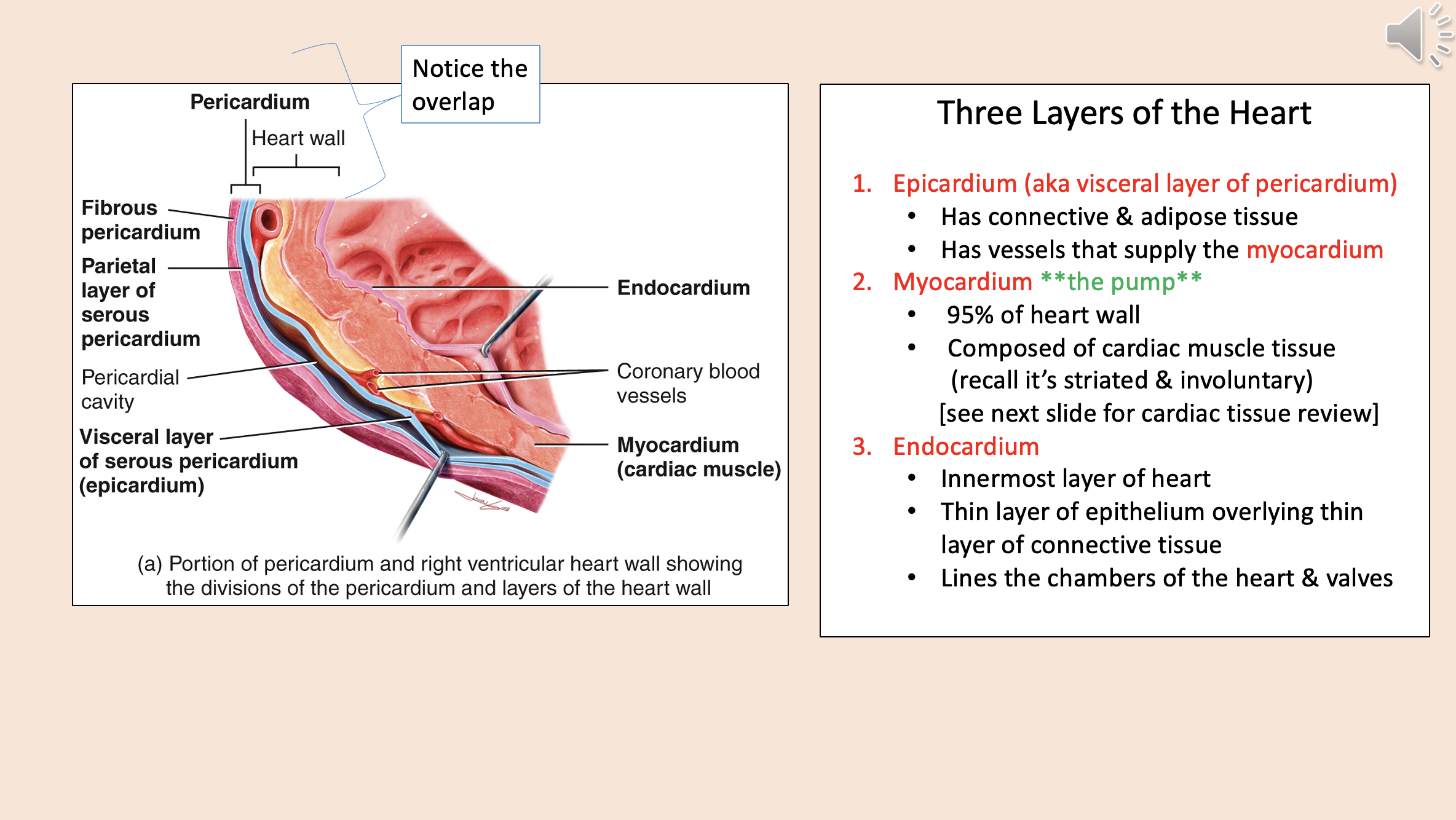
Has connective & adipose tissue.
Has vessels that supply the myocardium.
epicardium
The pump.
95% of heart wall.
Composed of cardiac muscle tissue (recall it’s striated & involuntary).
myocardium
Innermost layer of heart.
Thin layer of epithelium overlying thin layer of connective tissue.
Lines the chambers of the heart & valves.
endocardium
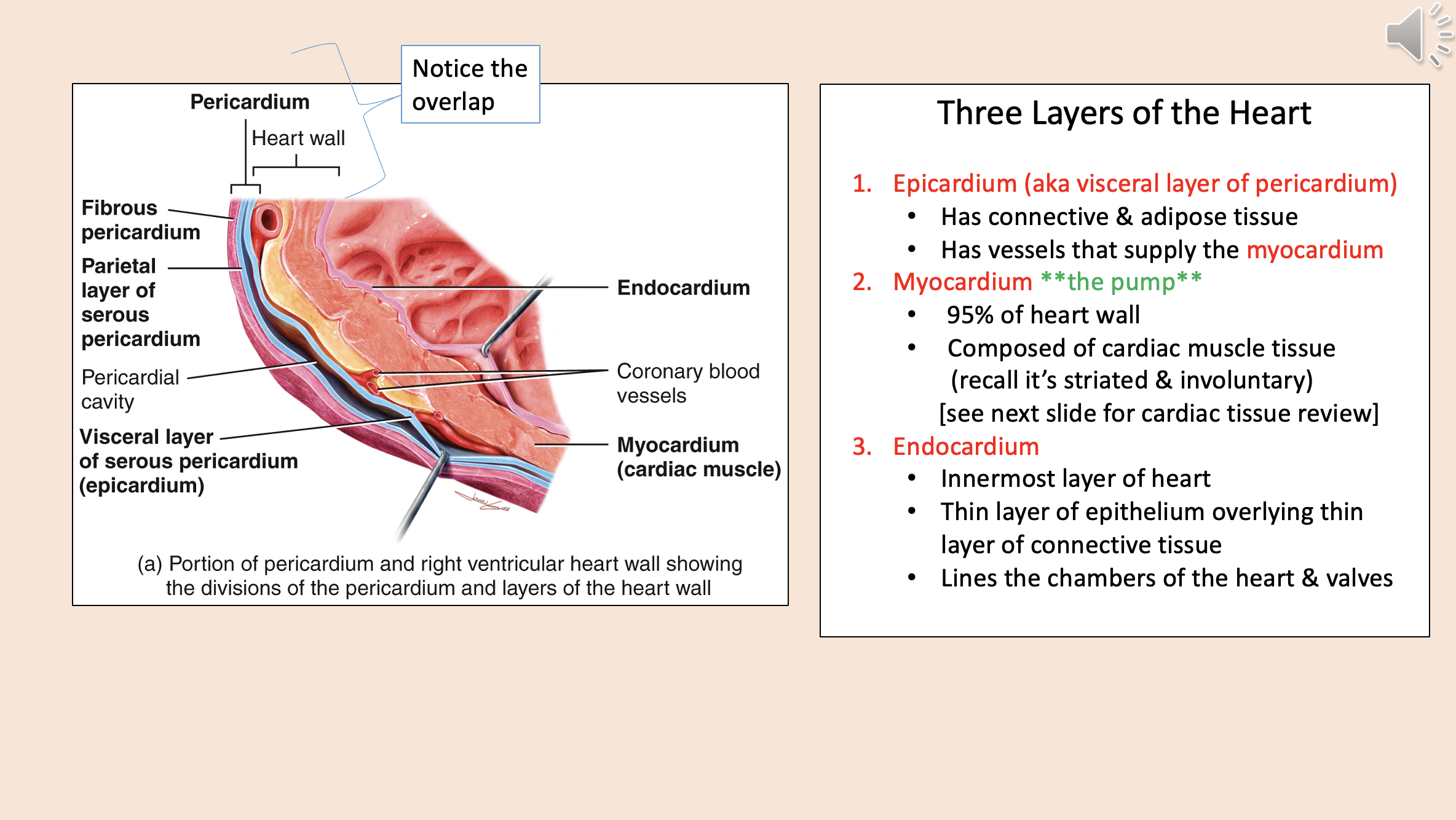
Divisions of the pericardium and layers of the heart wall
endocardium
myocardium
coronary blood vessels
visceral layer of serous pericardium epicardium
pericardial cavity
parietal layer of serous pericardium
fibrous pericardium
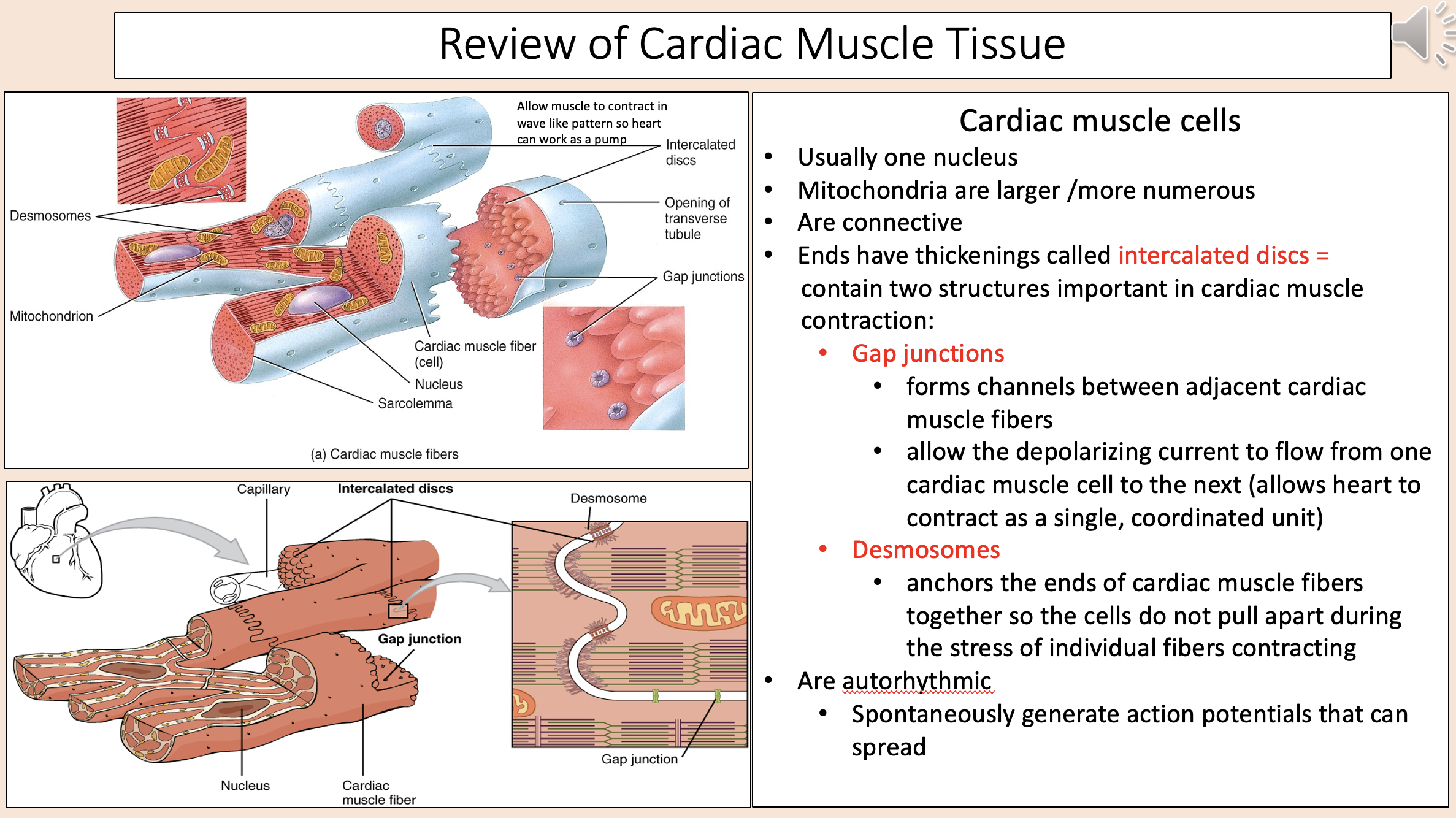
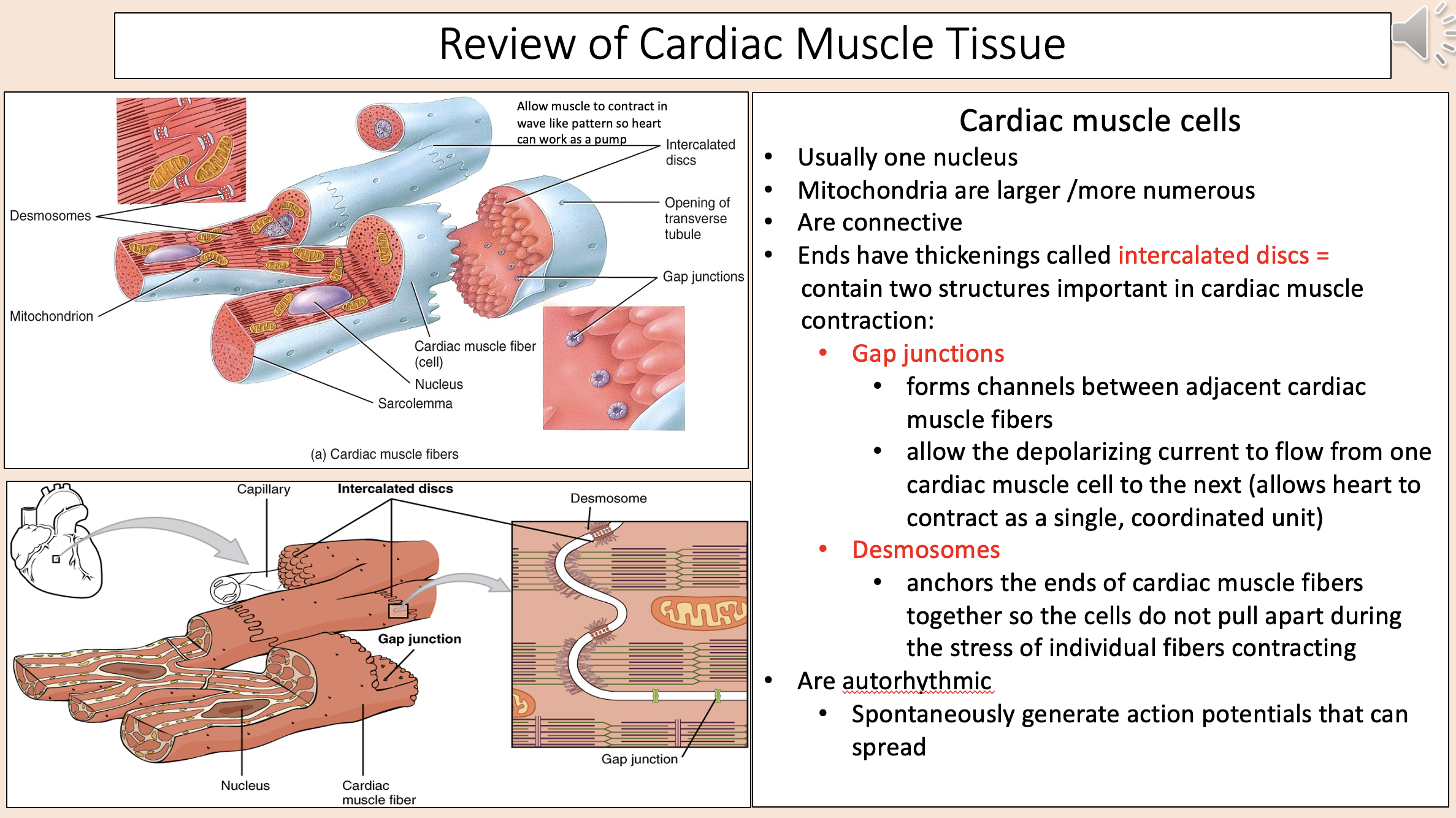
Usually one nucleus.
Mitochondria are larger /more numerous.
Are connective.
cardiac muscle cells
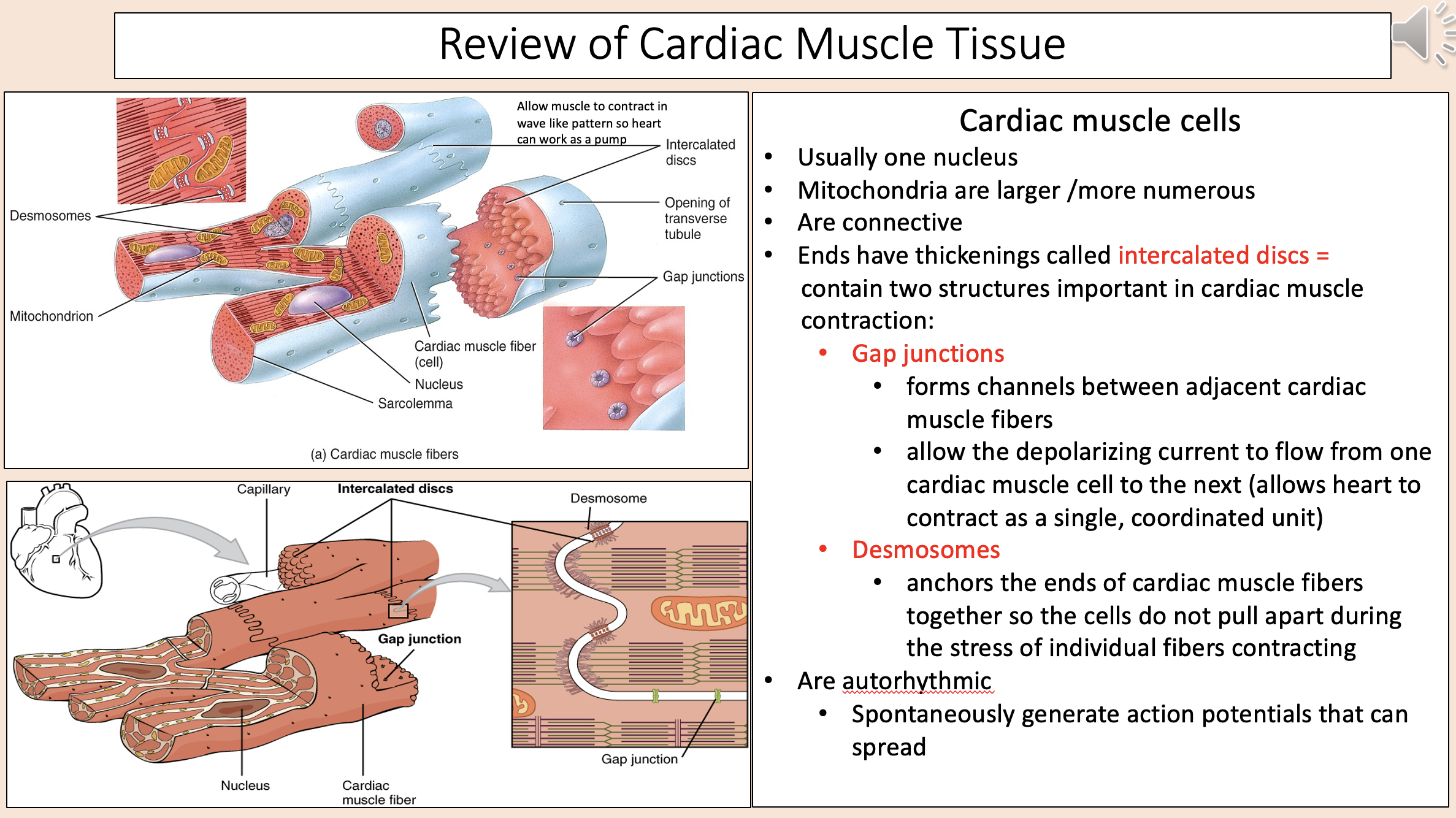
Ends have thickenings.
Contain two structures important in cardiac muscle contraction.
intercalated discs
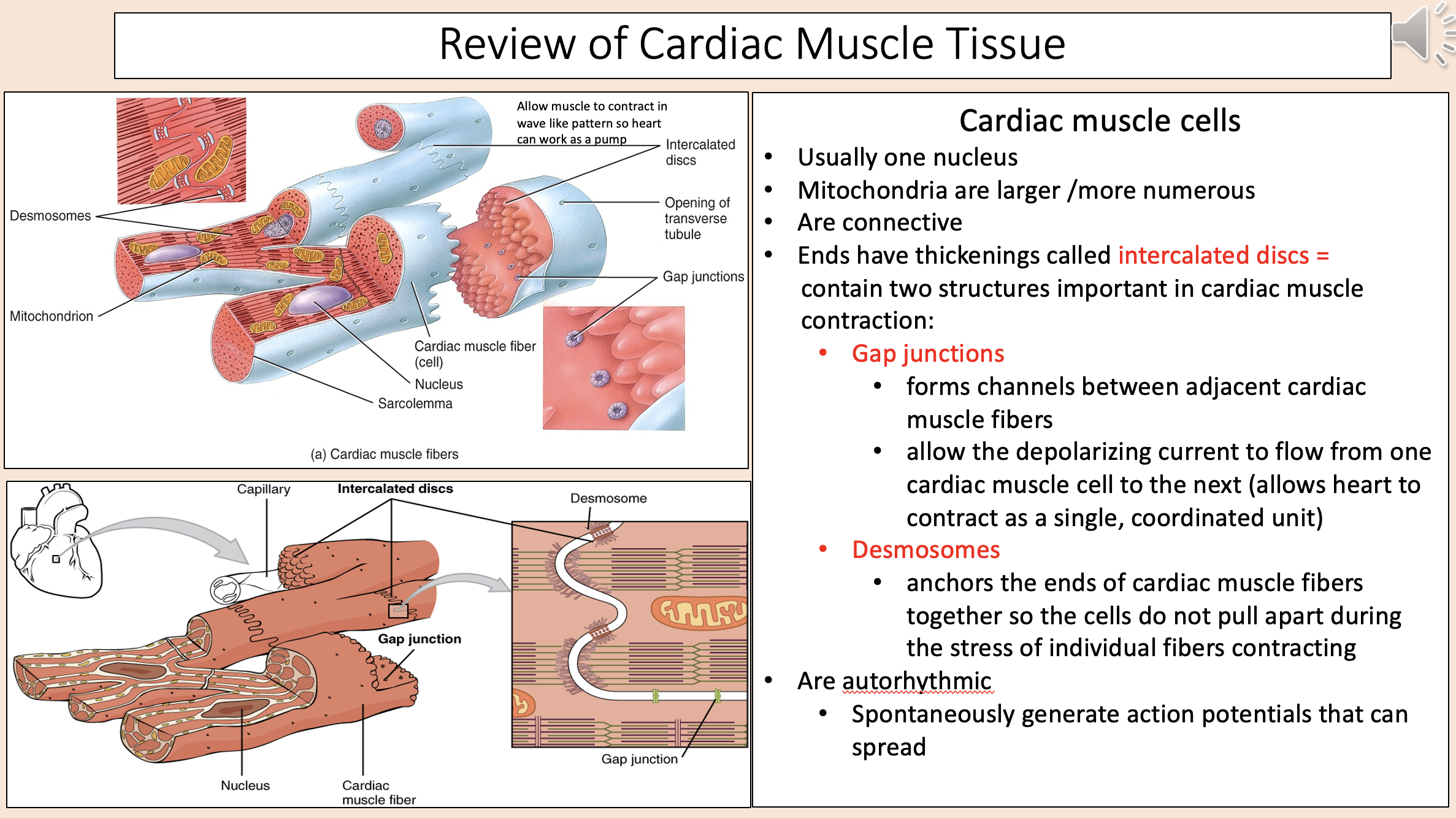
Intercalated discs two structures:
gap junctions
desmosomes
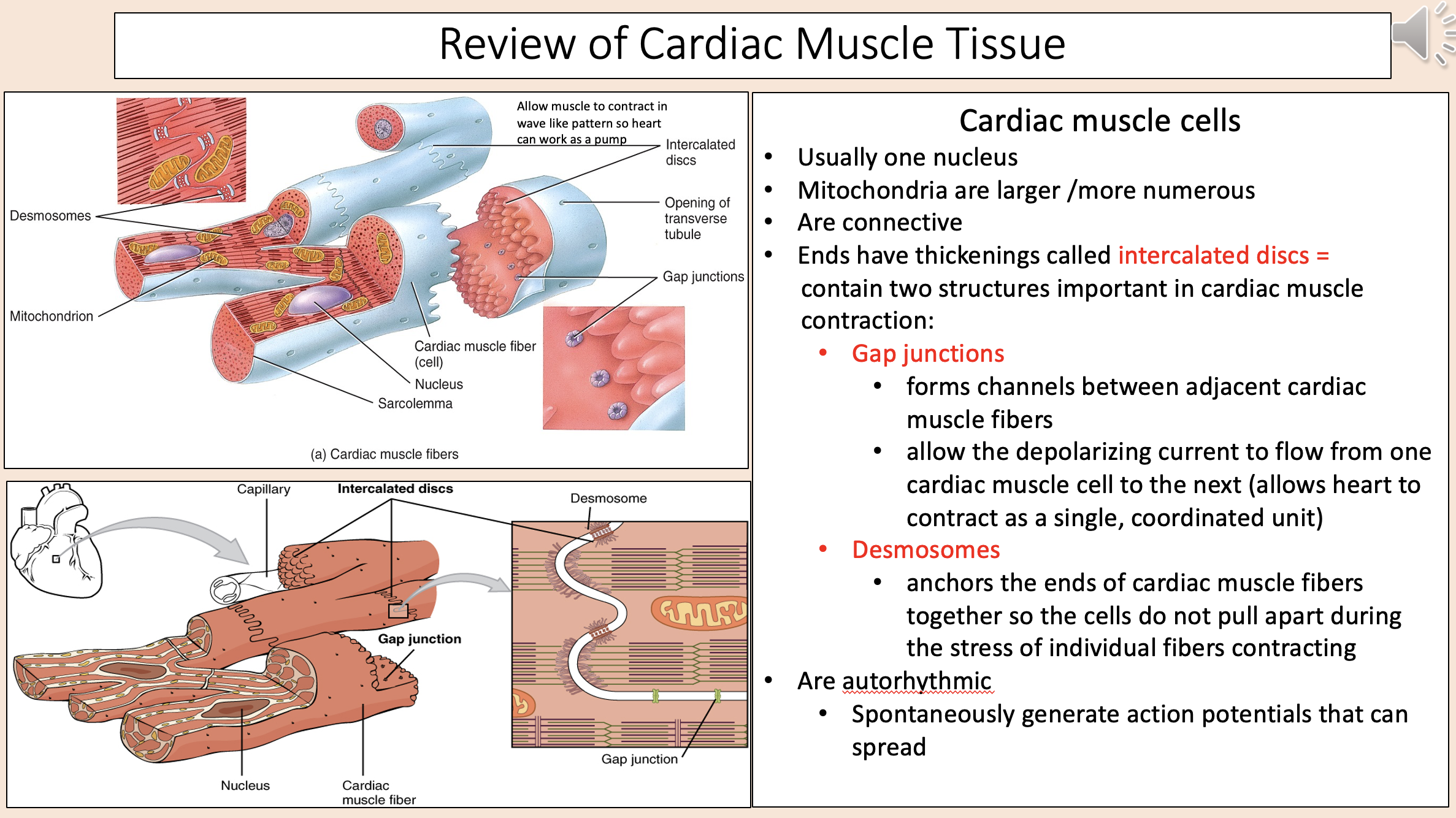
Forms channels between adjacent cardiac muscle fibers.
Allow the depolarizing current to flow from one cardiac muscle cell to the next (allows heart to contract as a single, coordinated unit).
gap junctions
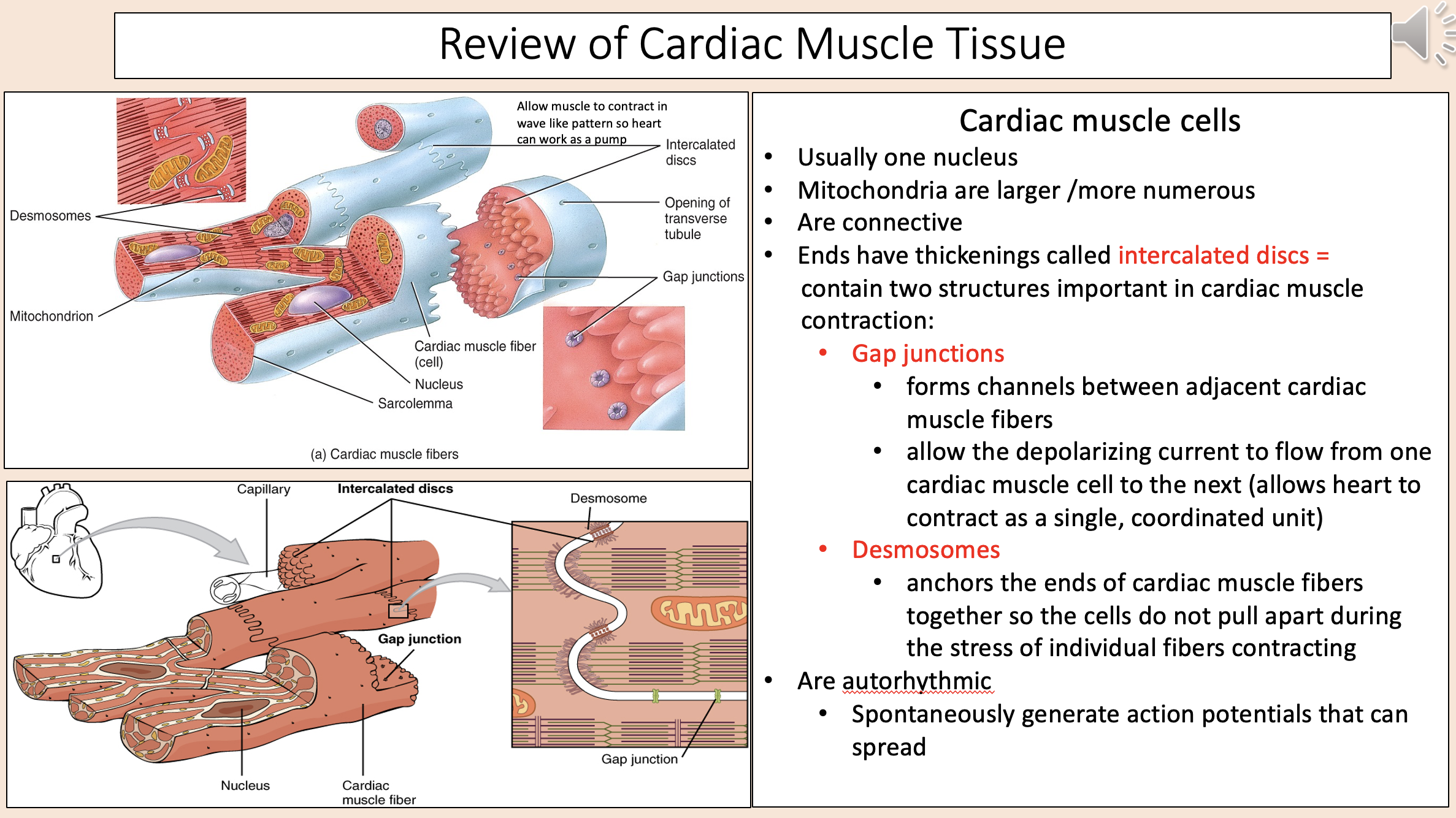
Anchors the ends of cardiac muscle fibers together so the cells do not pull apart during the stress of individual fibers contracting
desmosomes
Spontaneously generate action potentials that can spread
autorhythmic
2 upper atria & 2 lower ventricles
right atrium
right ventricle
left atrium
left ventricle
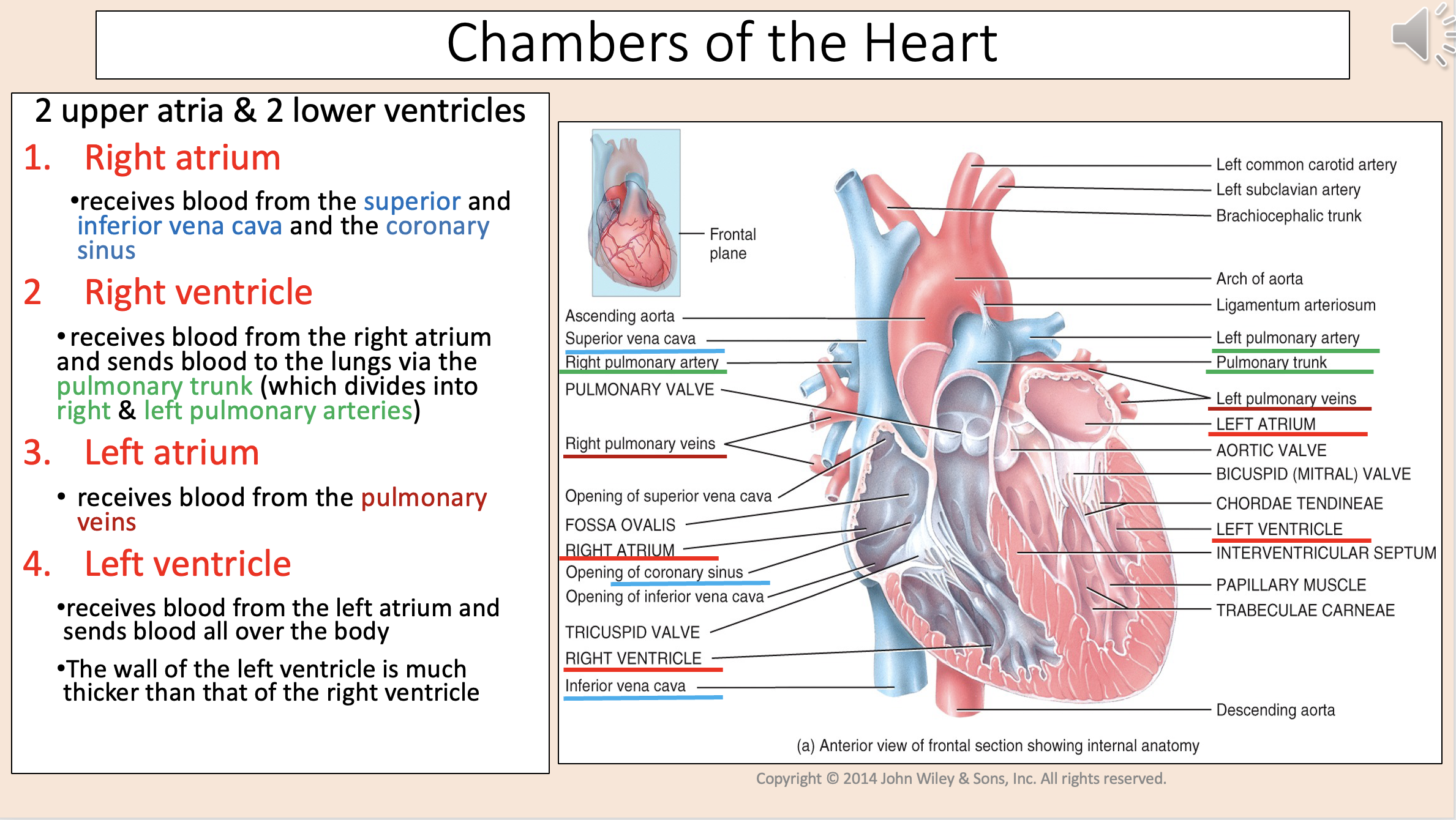
Receives blood from the superior and inferior vena cava and the coronary sinus
right atrium
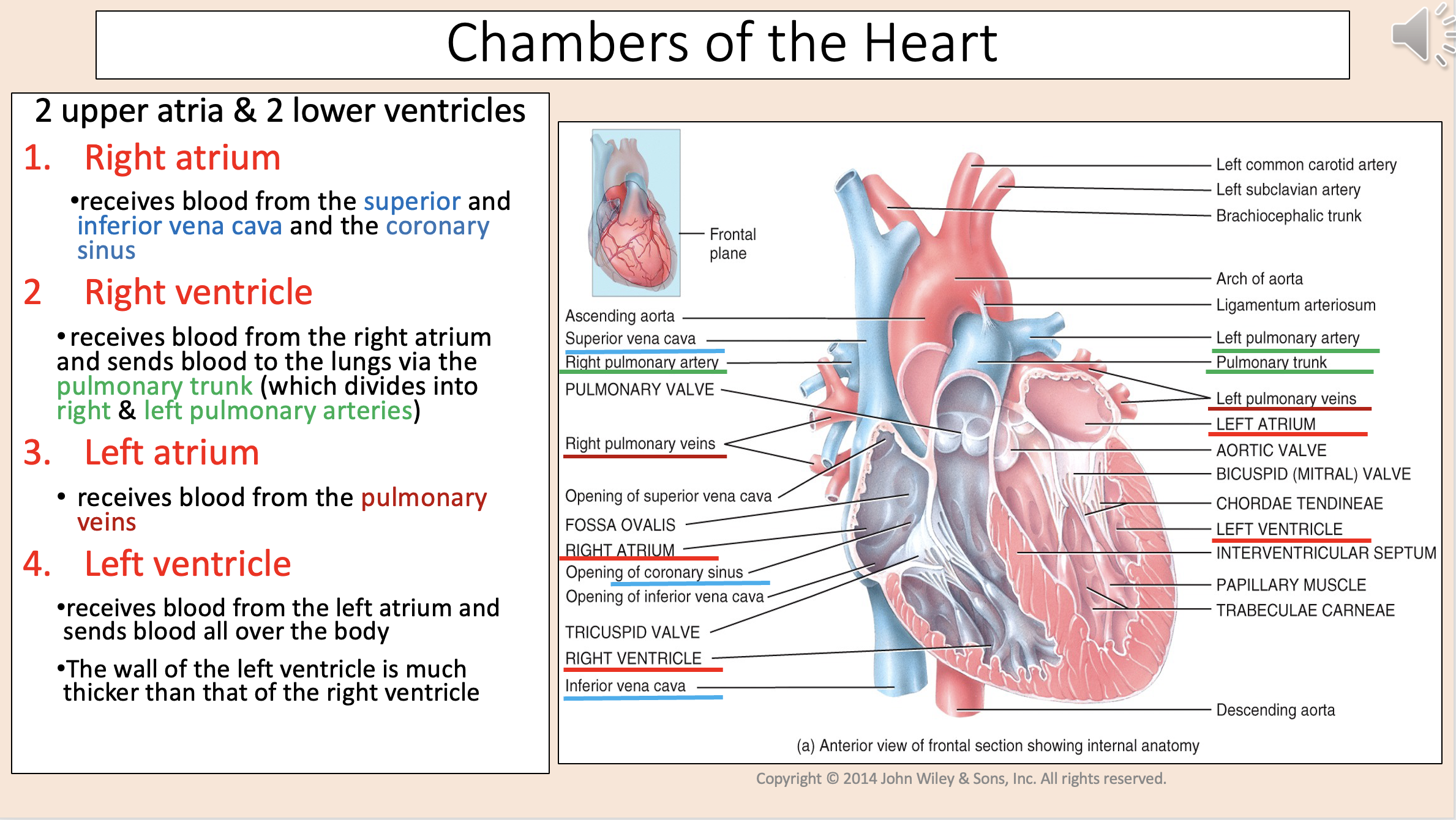
Receives blood from the right atrium and sends blood to the lungs via the pulmonary trunk (which divides into right & left pulmonary arteries)
right ventricle
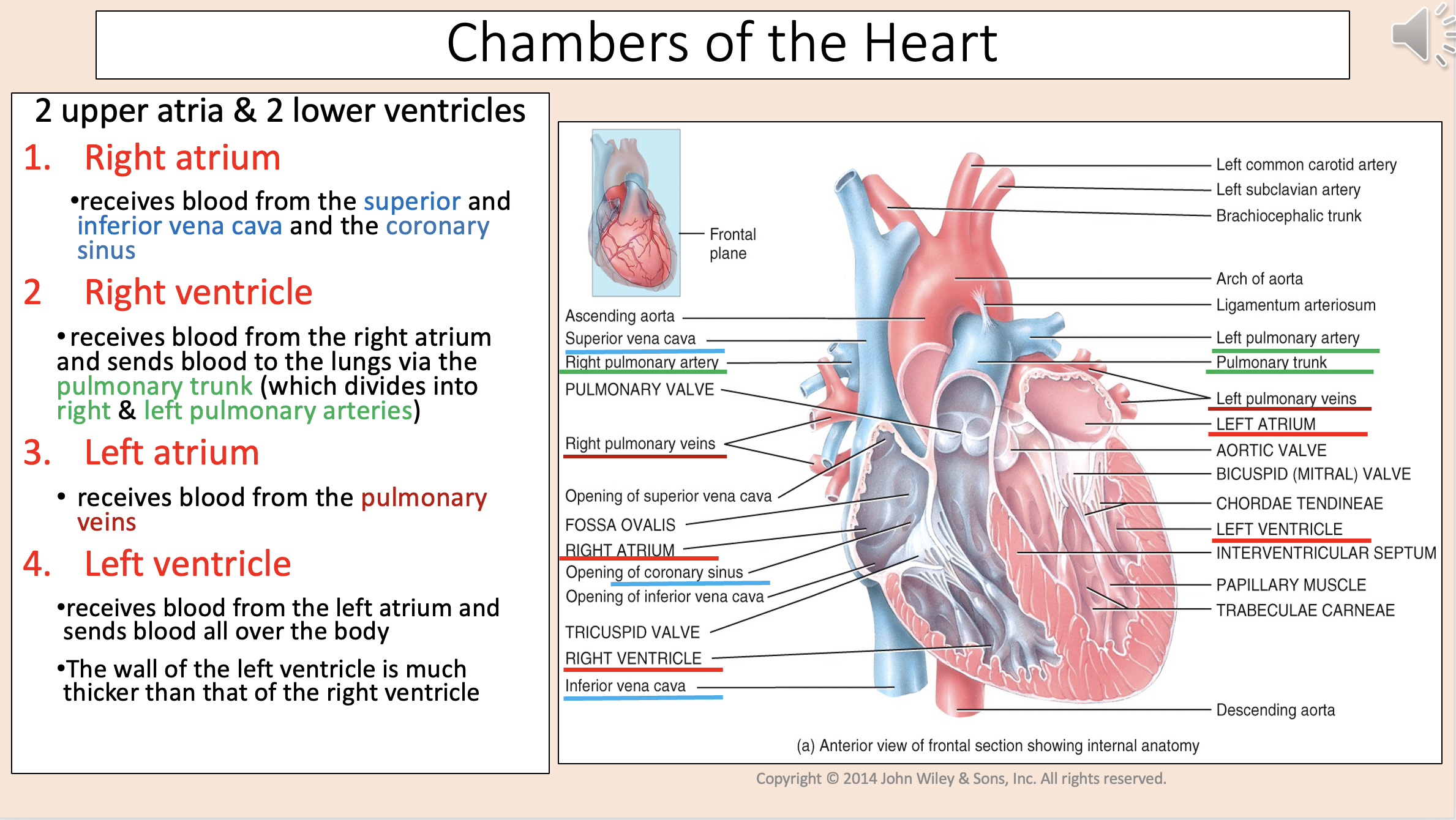
Receives blood from the pulmonary veins
left atrium
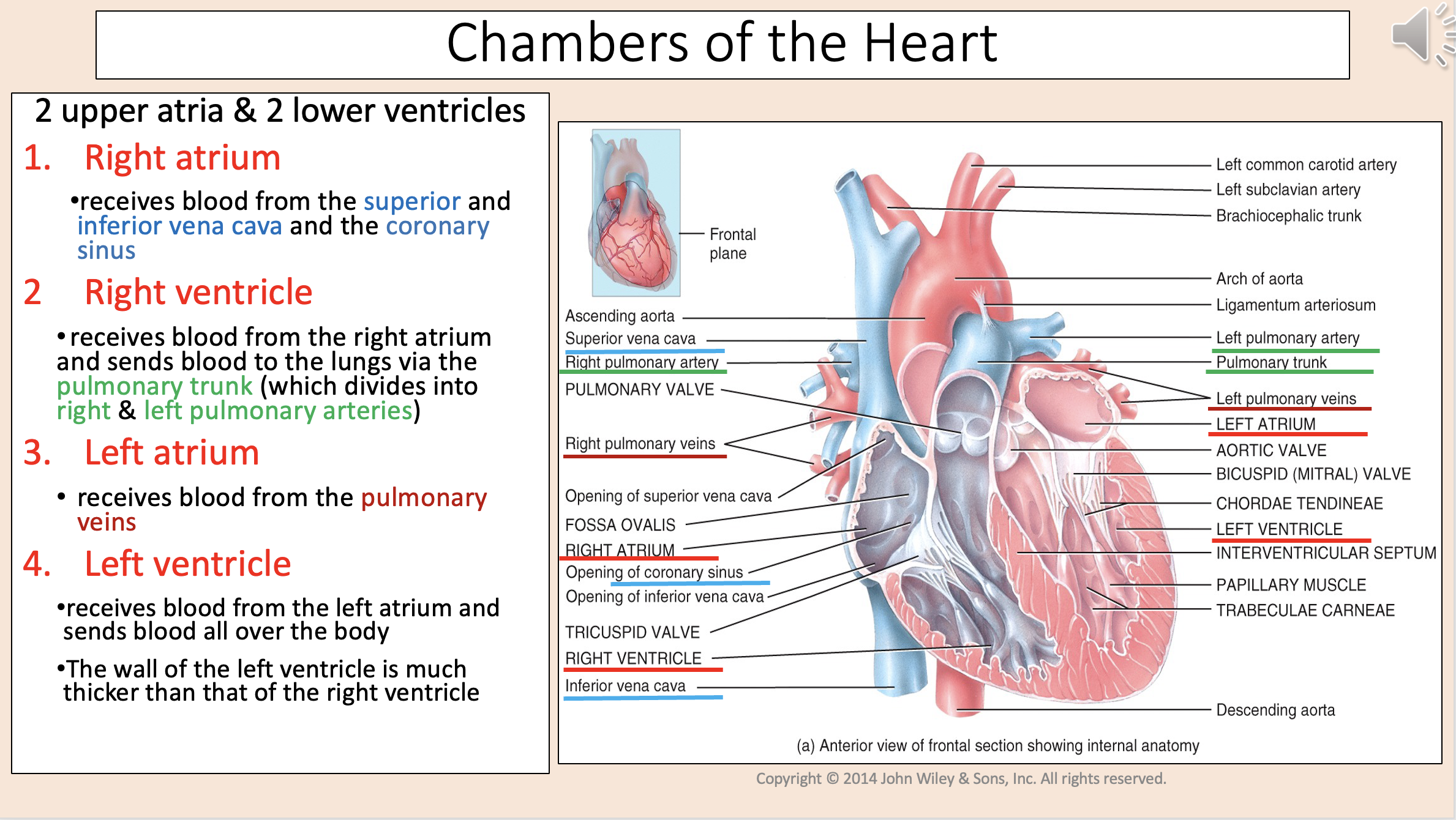
Receives blood from the left atrium and sends blood all over the body.
The wall of the left ventricle is much thicker than that of the right ventricle.
left ventricle
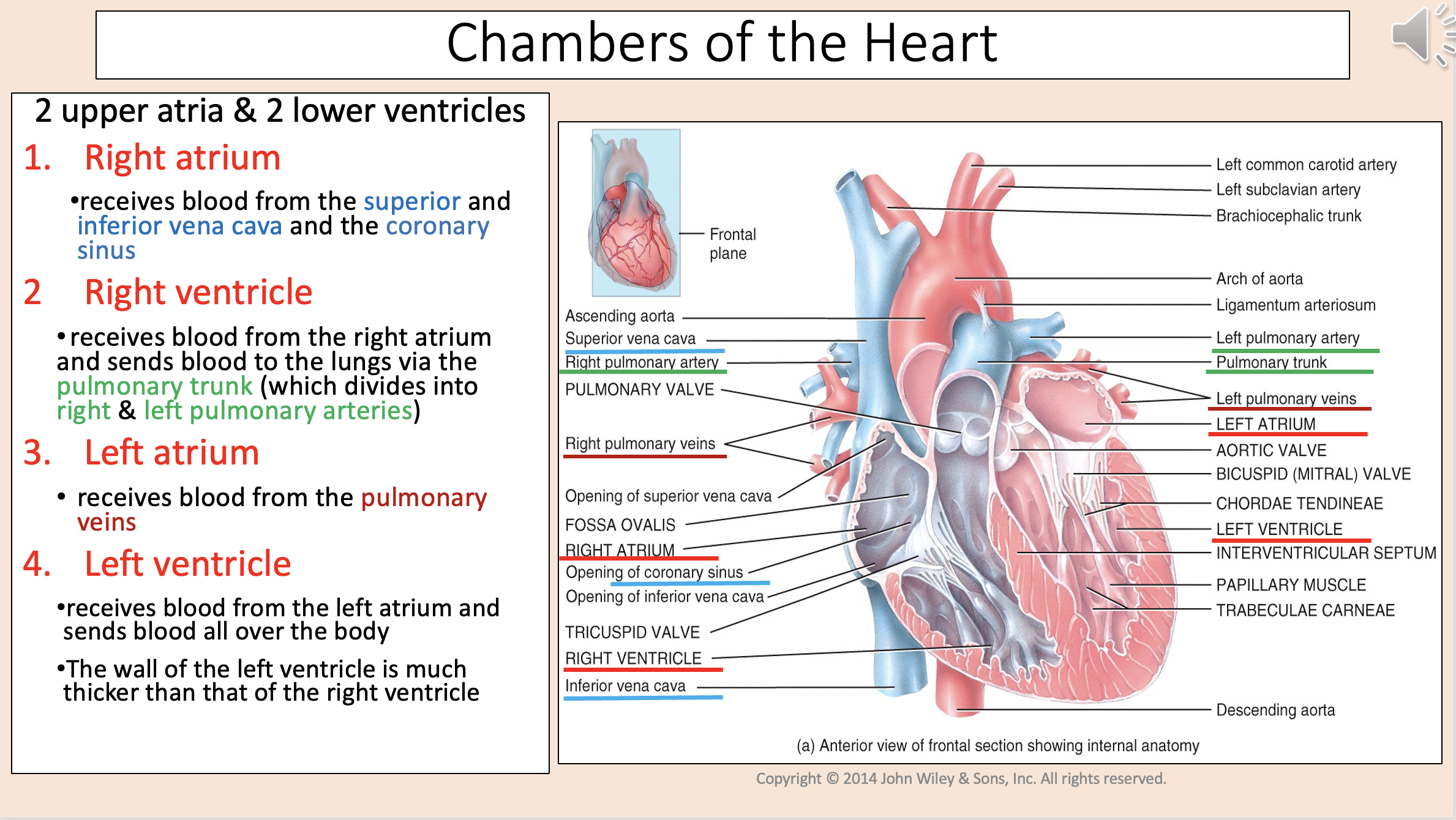
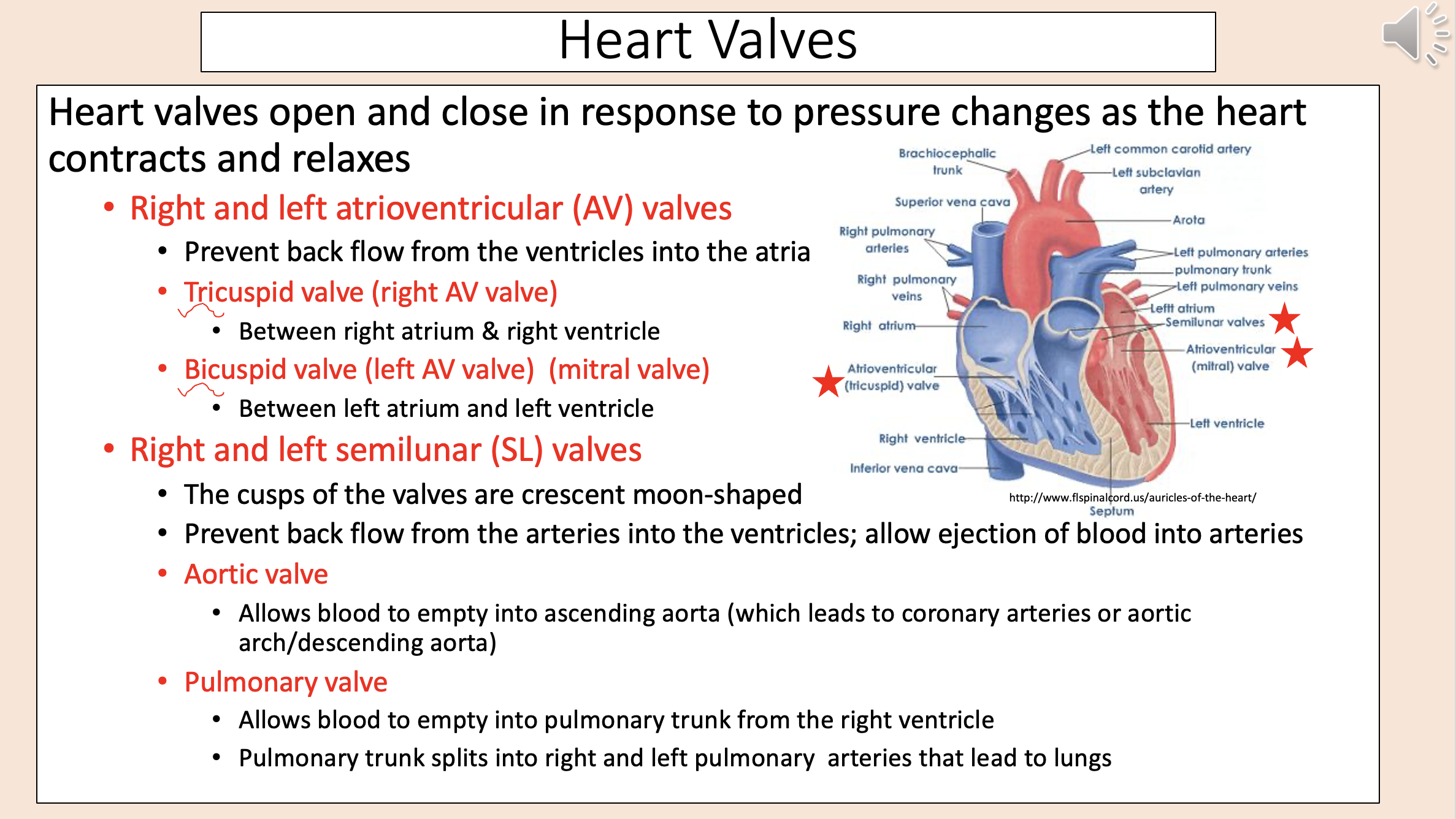
Heart Valves
right and left atrioventricular valves
right and left semilunar valves
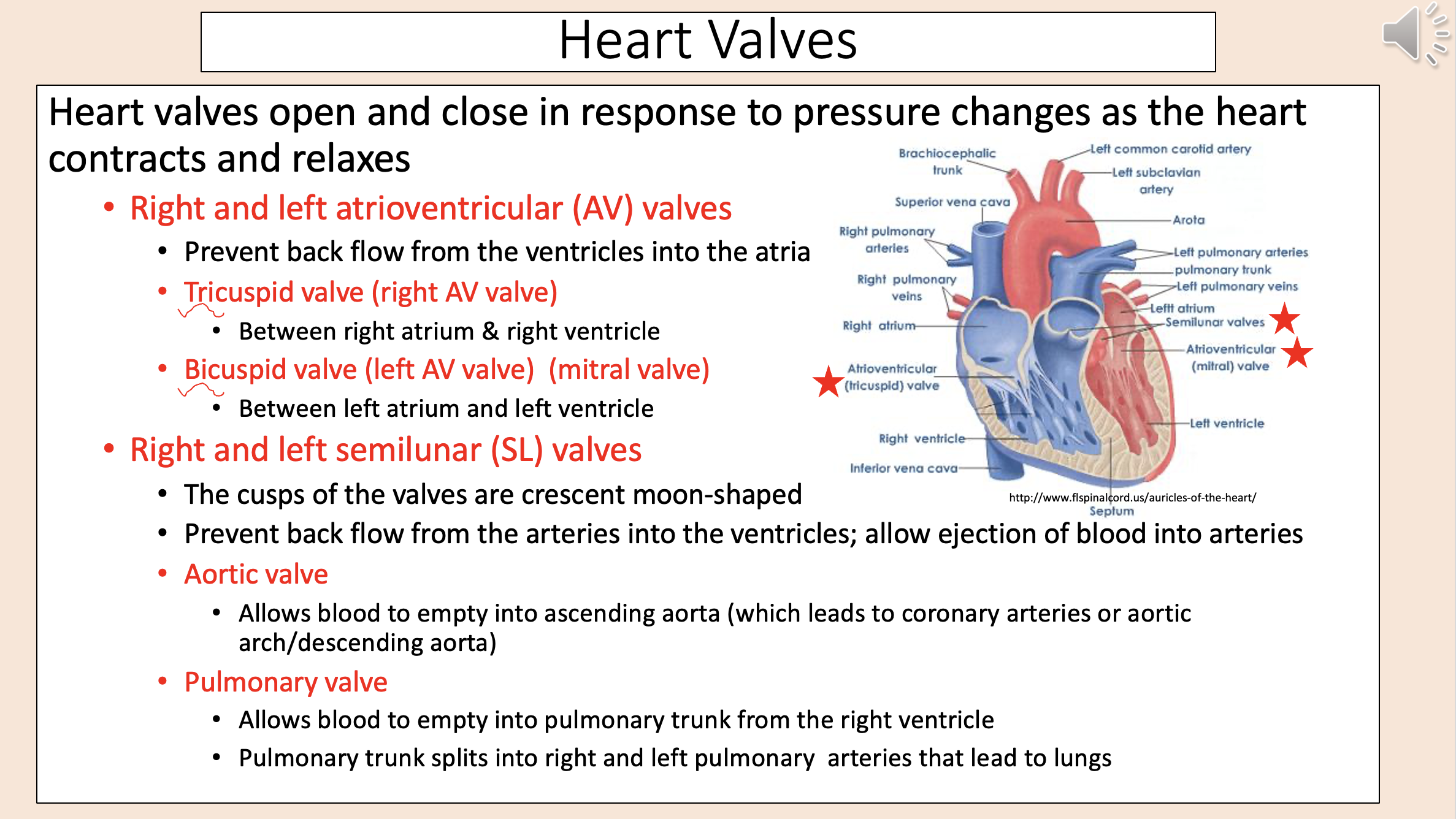
Prevent back flow from the ventricles into the atria
right and left atrioventricular (AV) valves
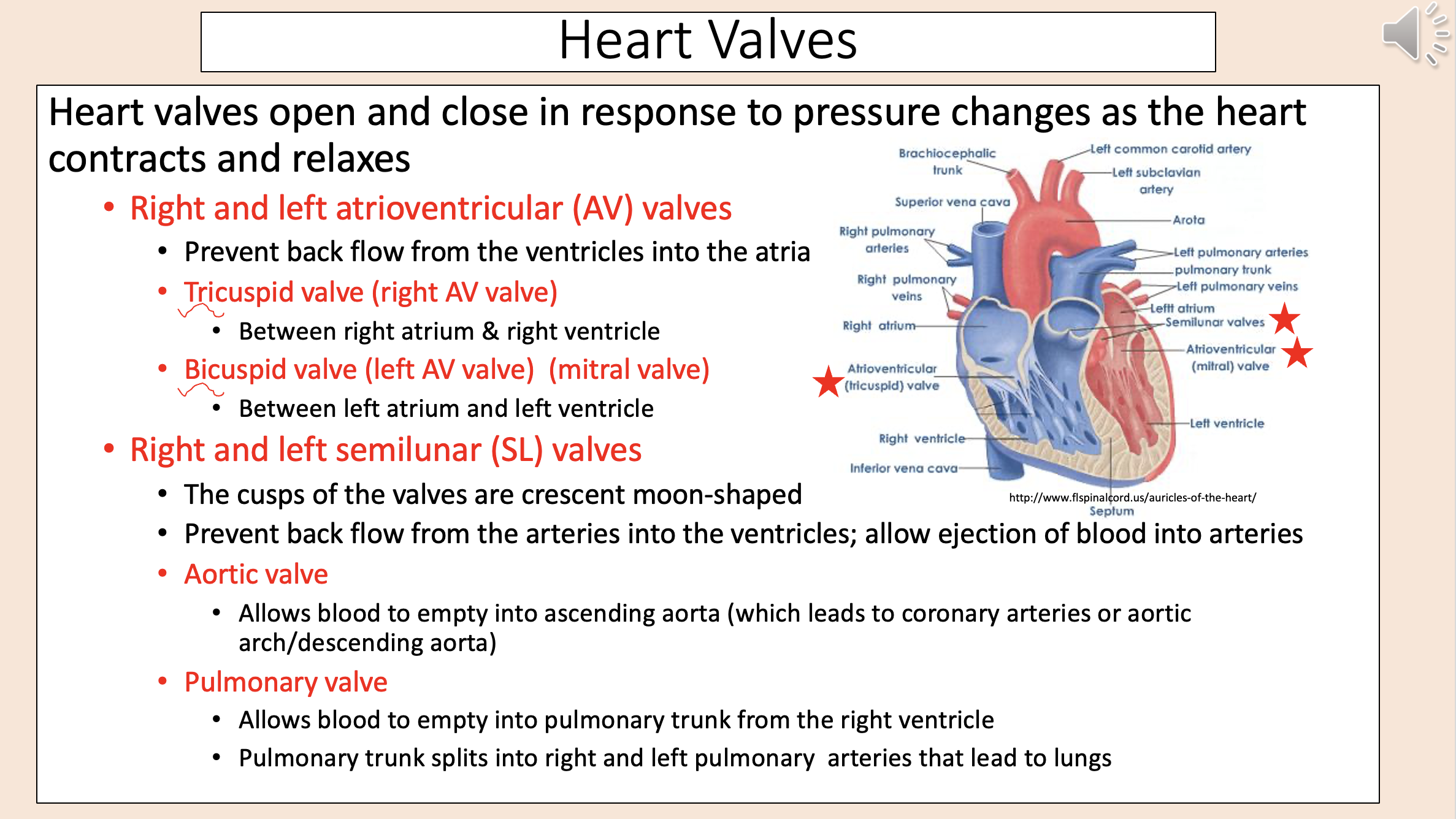
Right AV valve.
Between right atrium & right ventricle.
tricuspid valve
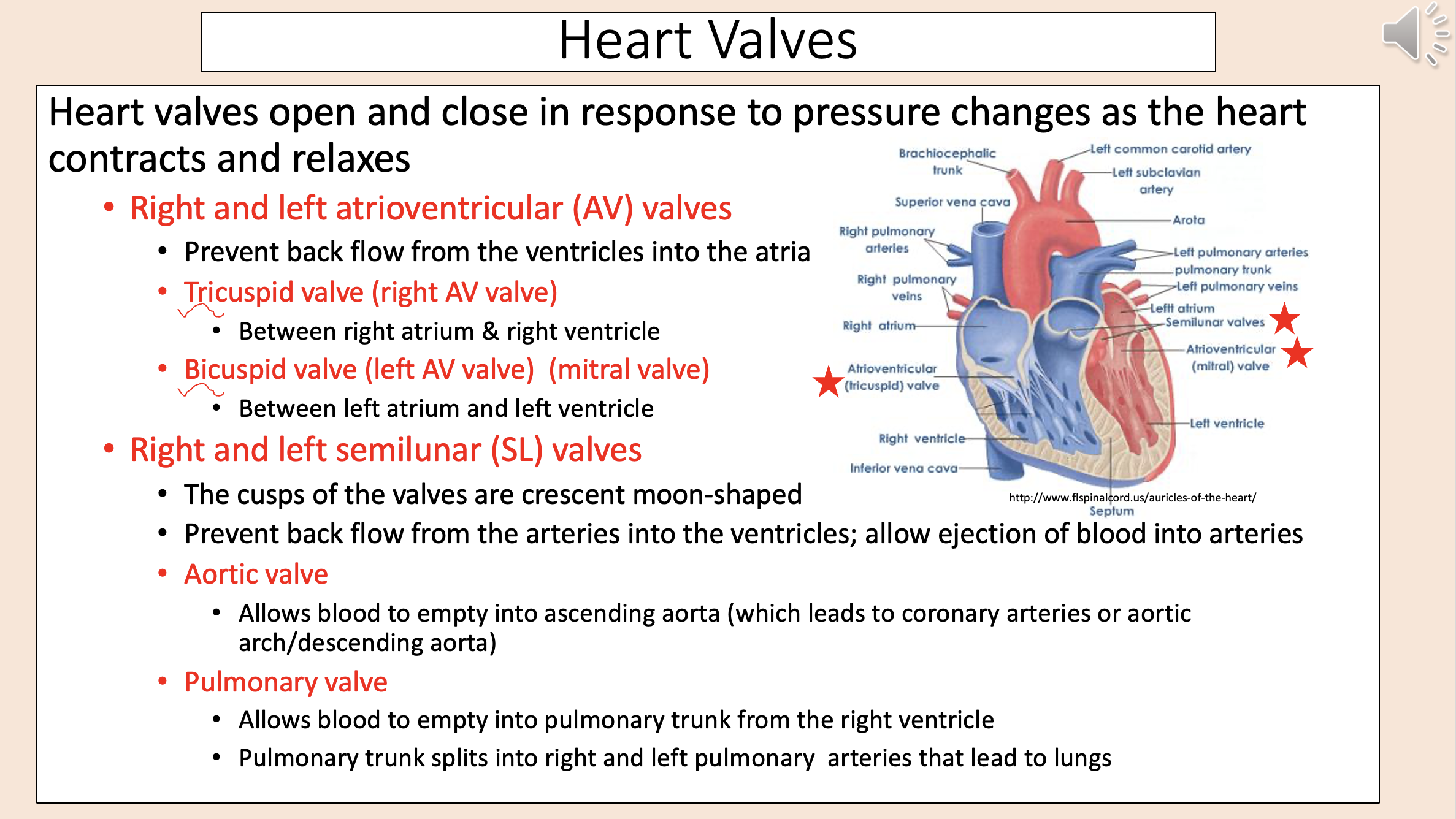
Left AV valve.
Between left atrium and left ventricle.
bicuspid valve
mitral valve
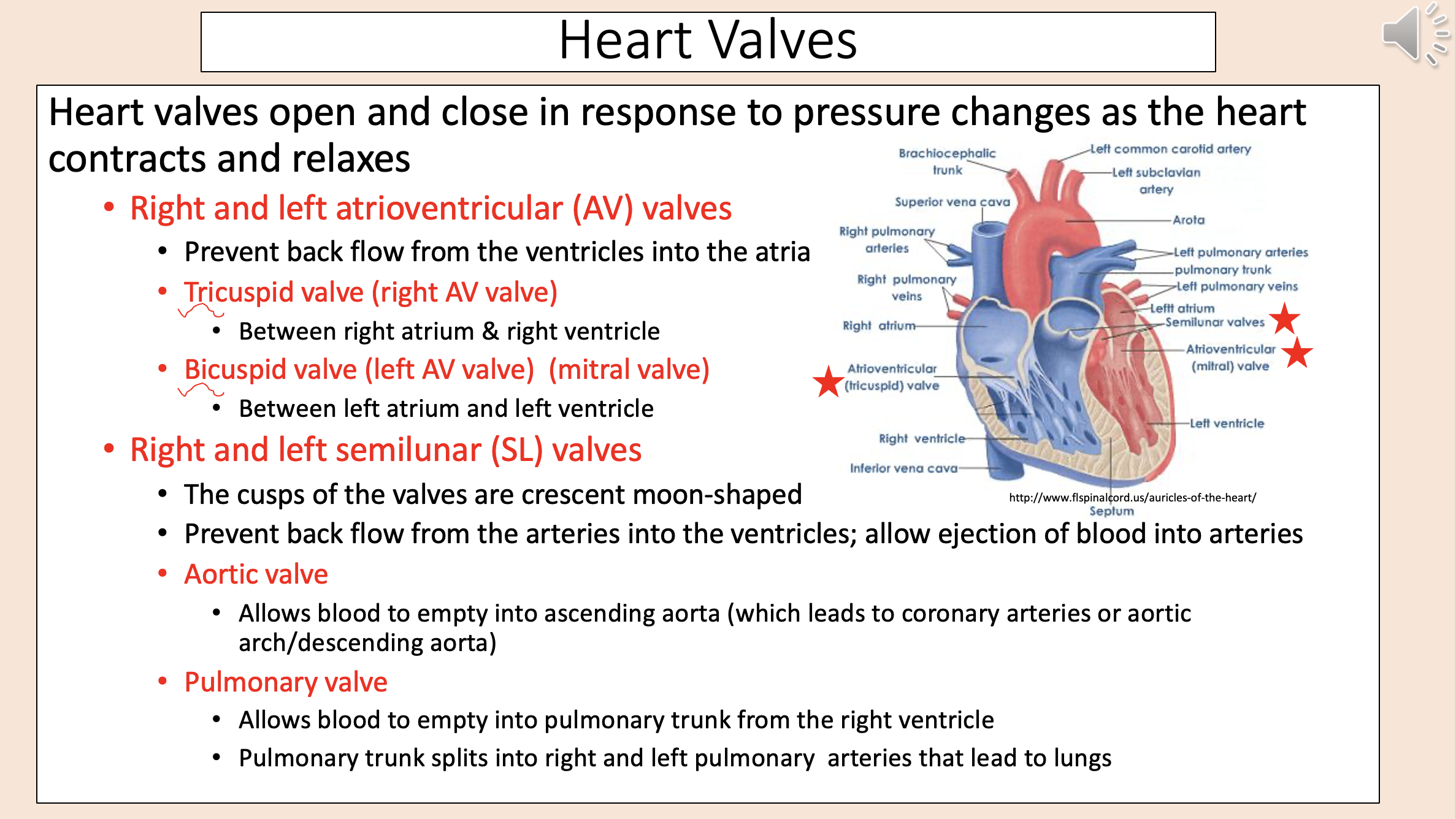
The cusps of the valves are crescent moon-shaped.
Prevent back flow from the arteries into the ventricles; allow ejection of blood into arteries.
right and left semilunar (SL) valve
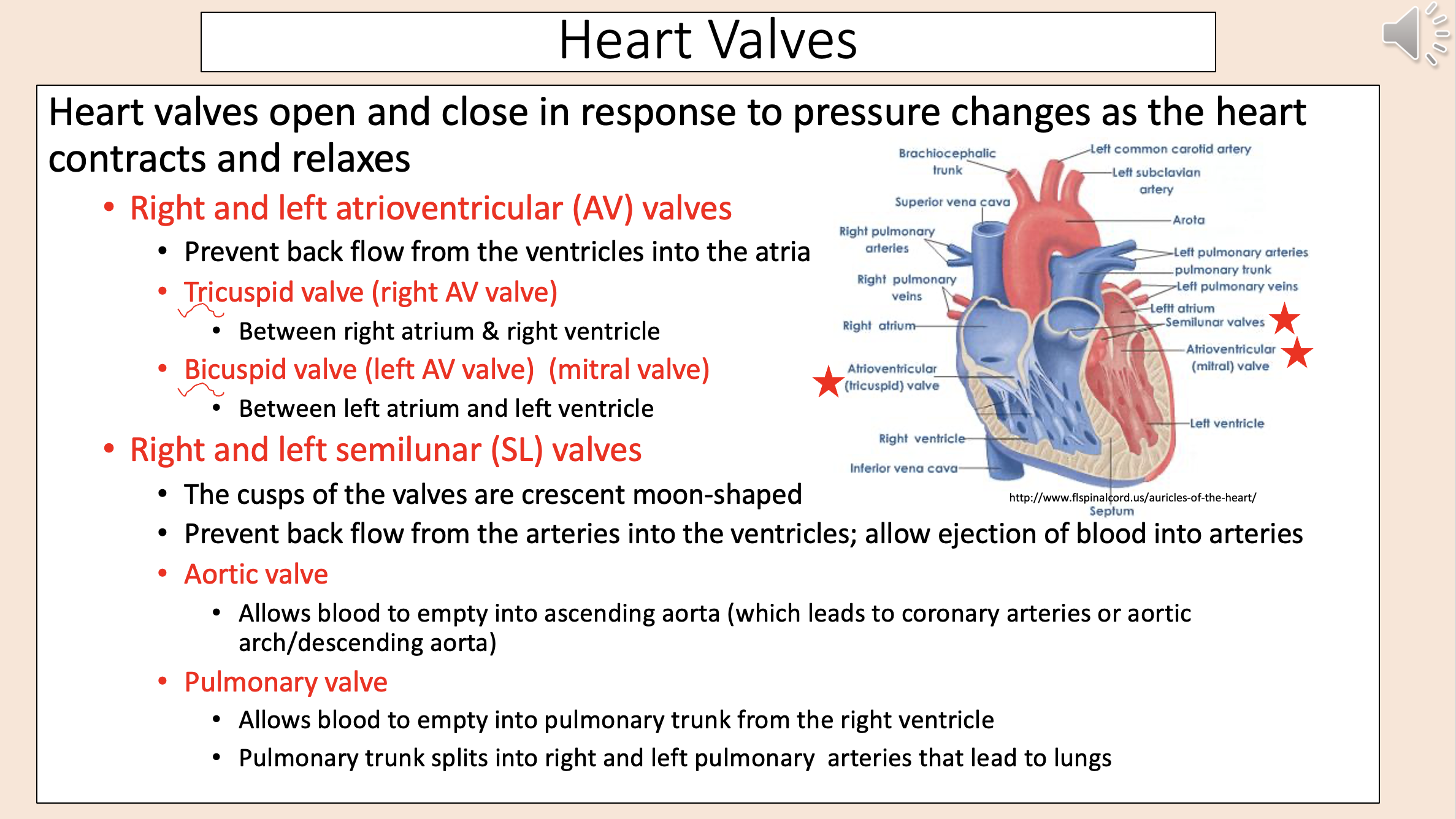
Left semilunar (SL) valve.
Allows blood to empty into ascending aorta (which leads to coronary arteries or aortic arch/descending aorta)
aortic valve
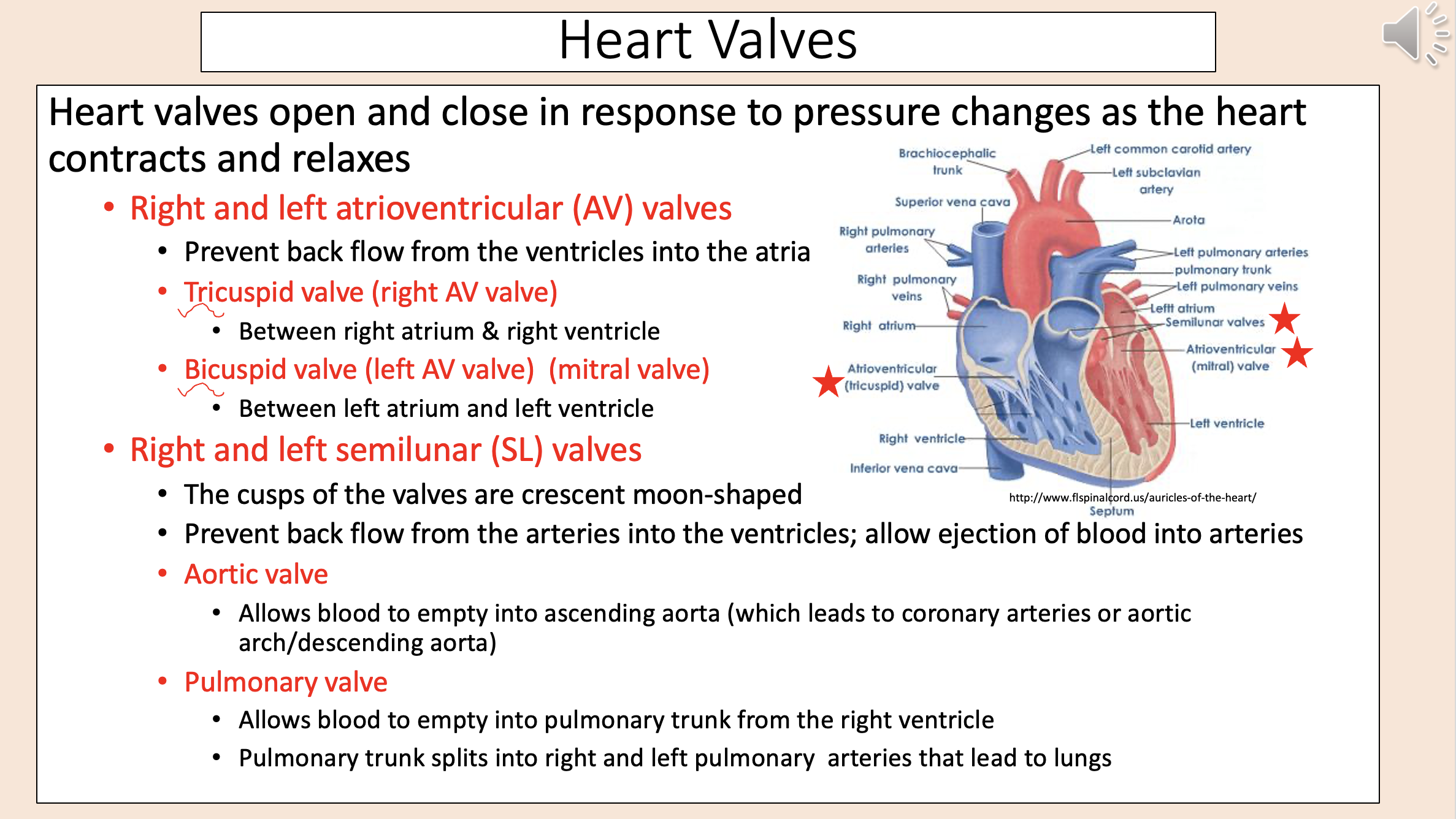
Right semilunar (SL) valve.
Allows blood to empty into pulmonary trunk from the right ventricle.
Pulmonary trunk splits into right and left pulmonary arteries that lead to lungs.
pulmonary valve
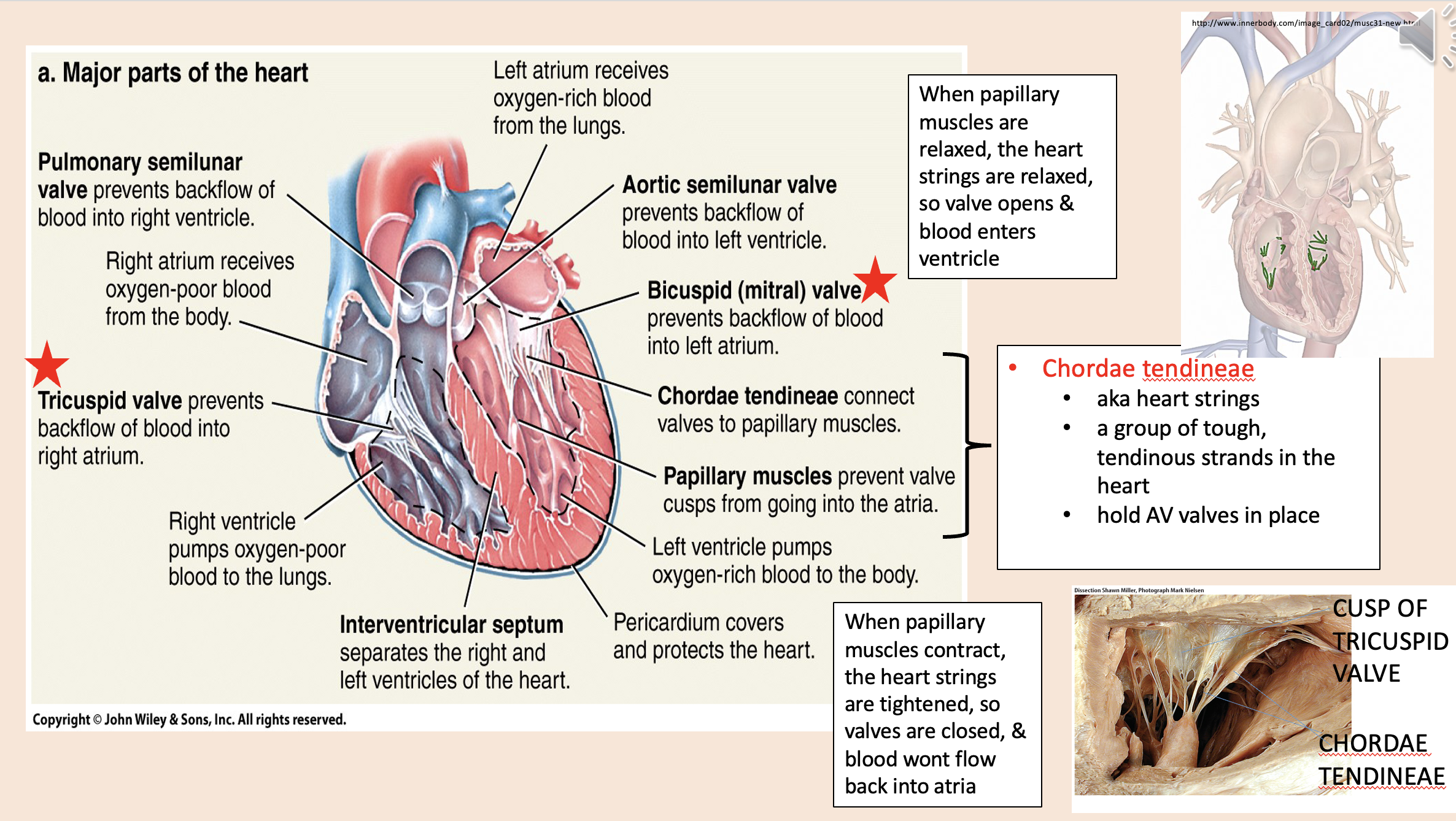
aka heart strings
chordae tendineae
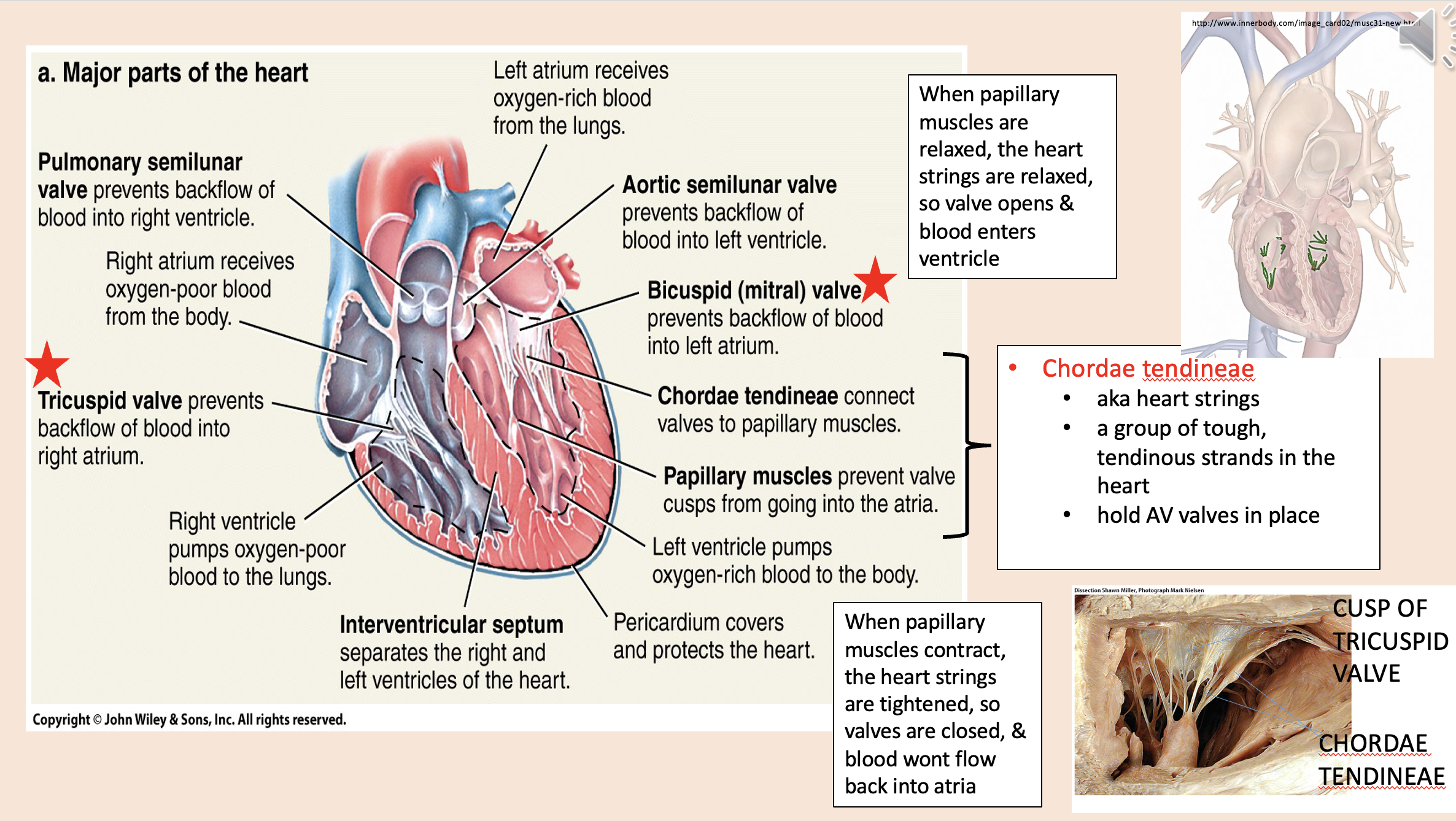
A group of tough, tendinous strands in the heart.
Hold AV valves in place.
chordae tendineae
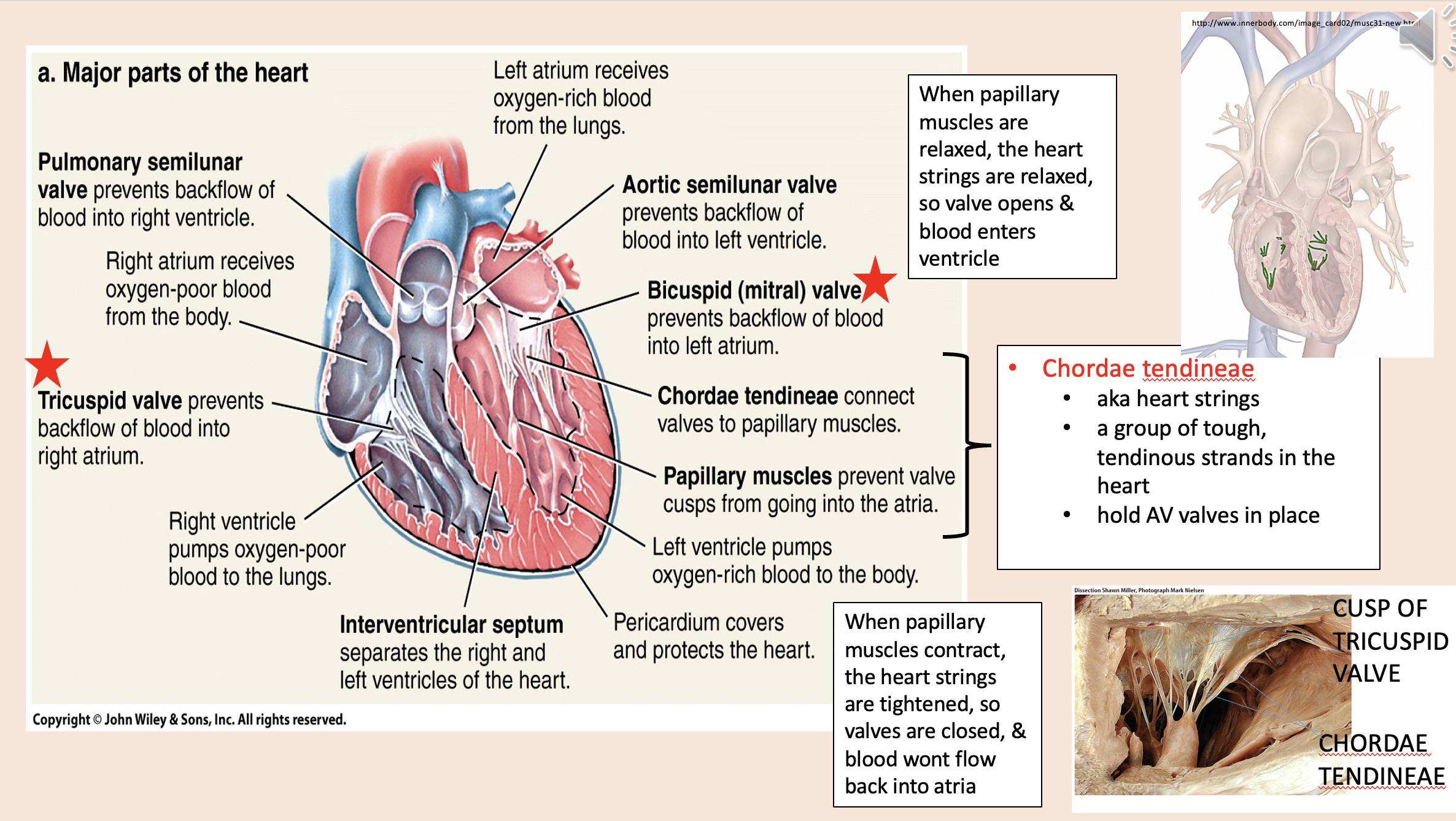
When papillary muscles are relaxed, the heart strings are relaxed, so
valve opens
blood enters ventricle
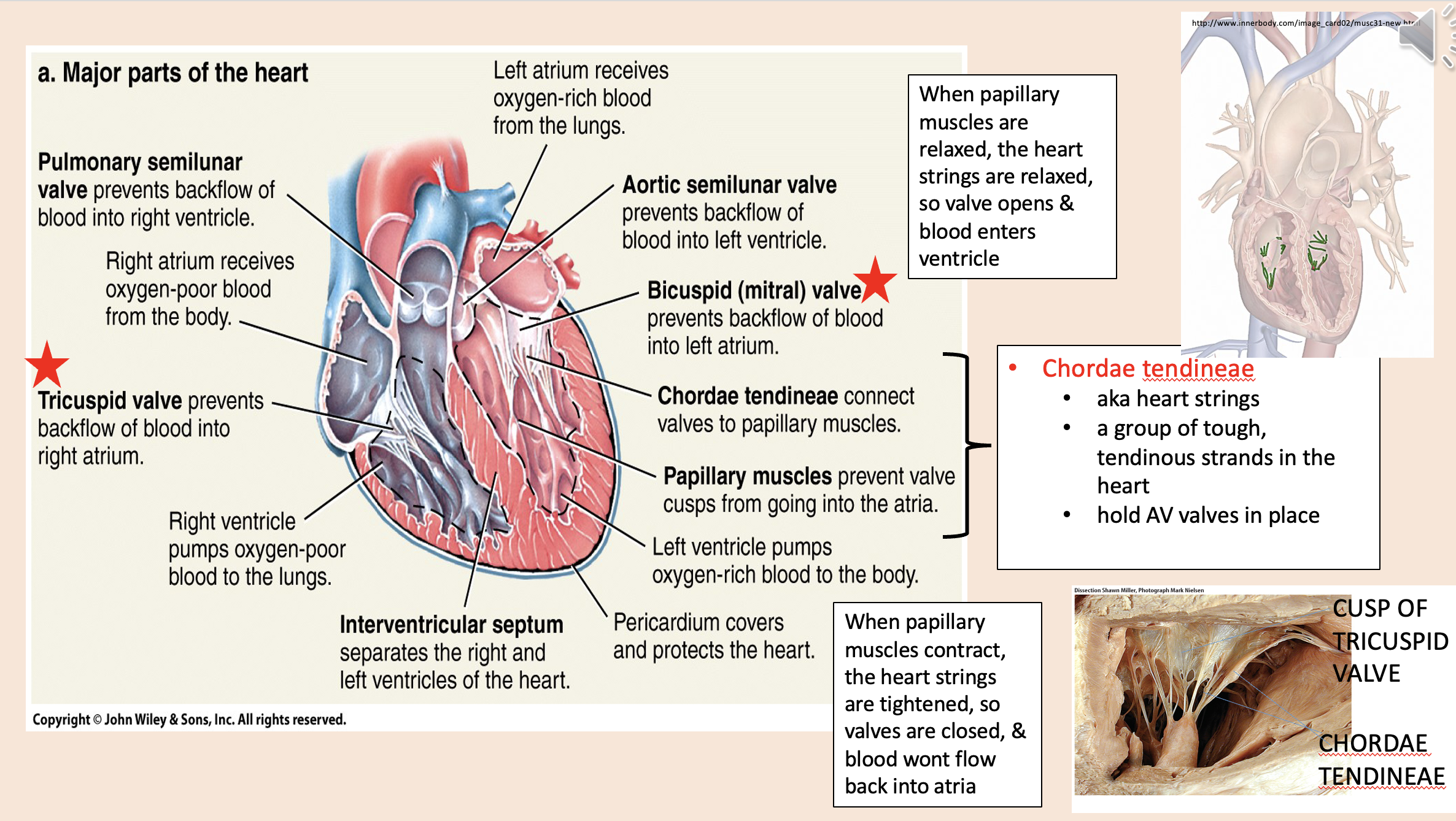
When papillary muscles contract, the heart strings are tightened, so
valves are closed
blood wont flow back into atria
Specialized cardiac muscle fibers.
~1% of the cardiac fibers.
Are self-excitable.
Generate action potentials that trigger heart contraction.
Ensure that the chambers contract in a coordinated manner.
autorhythmic fibers
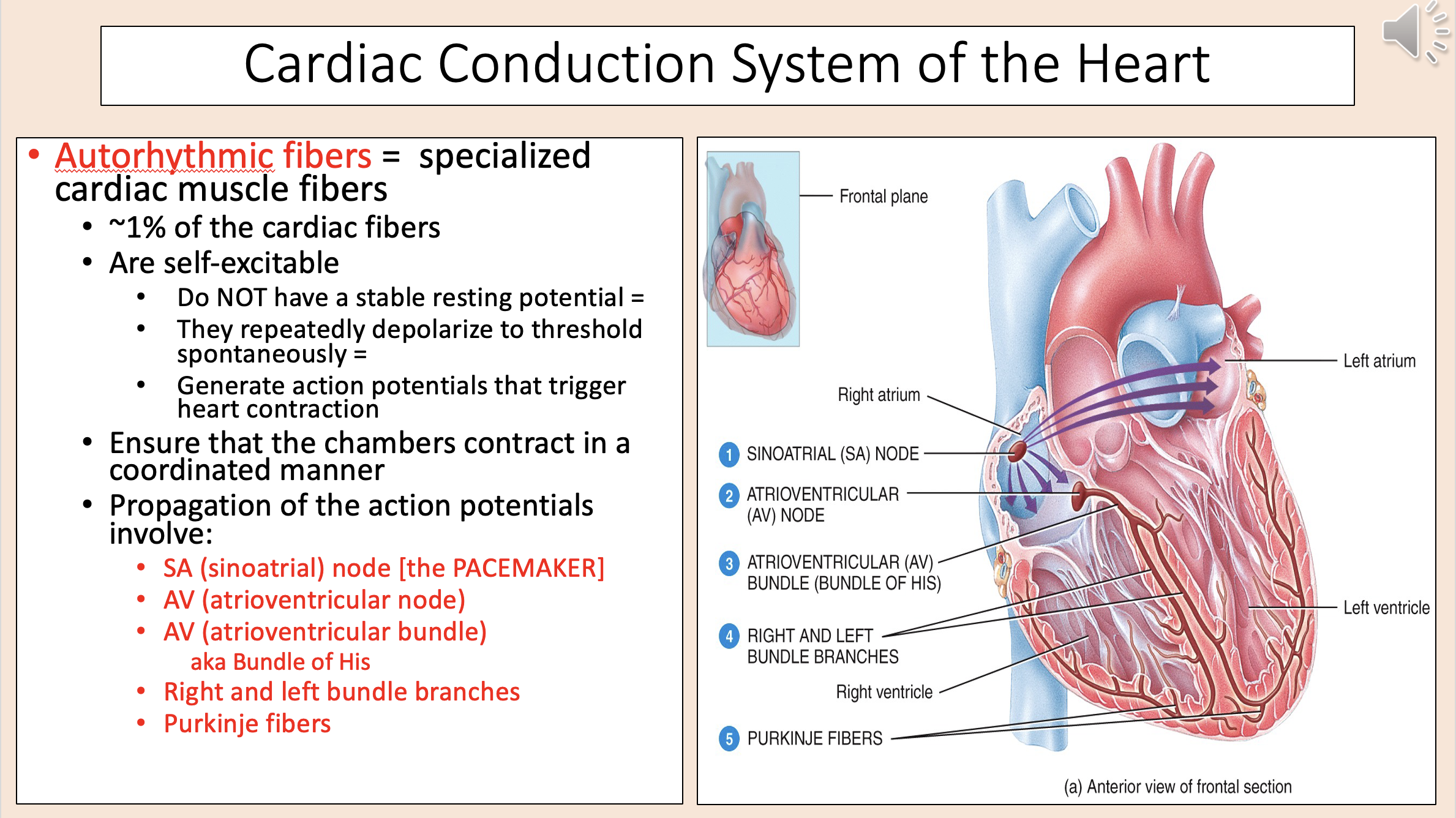
Propagation of action potentials involve:
SA (sinoatrial)
AV (atrioventricular node)
AV (atrioventricular bundle)
right bundle branches
left bundle branches
purkinje fibers
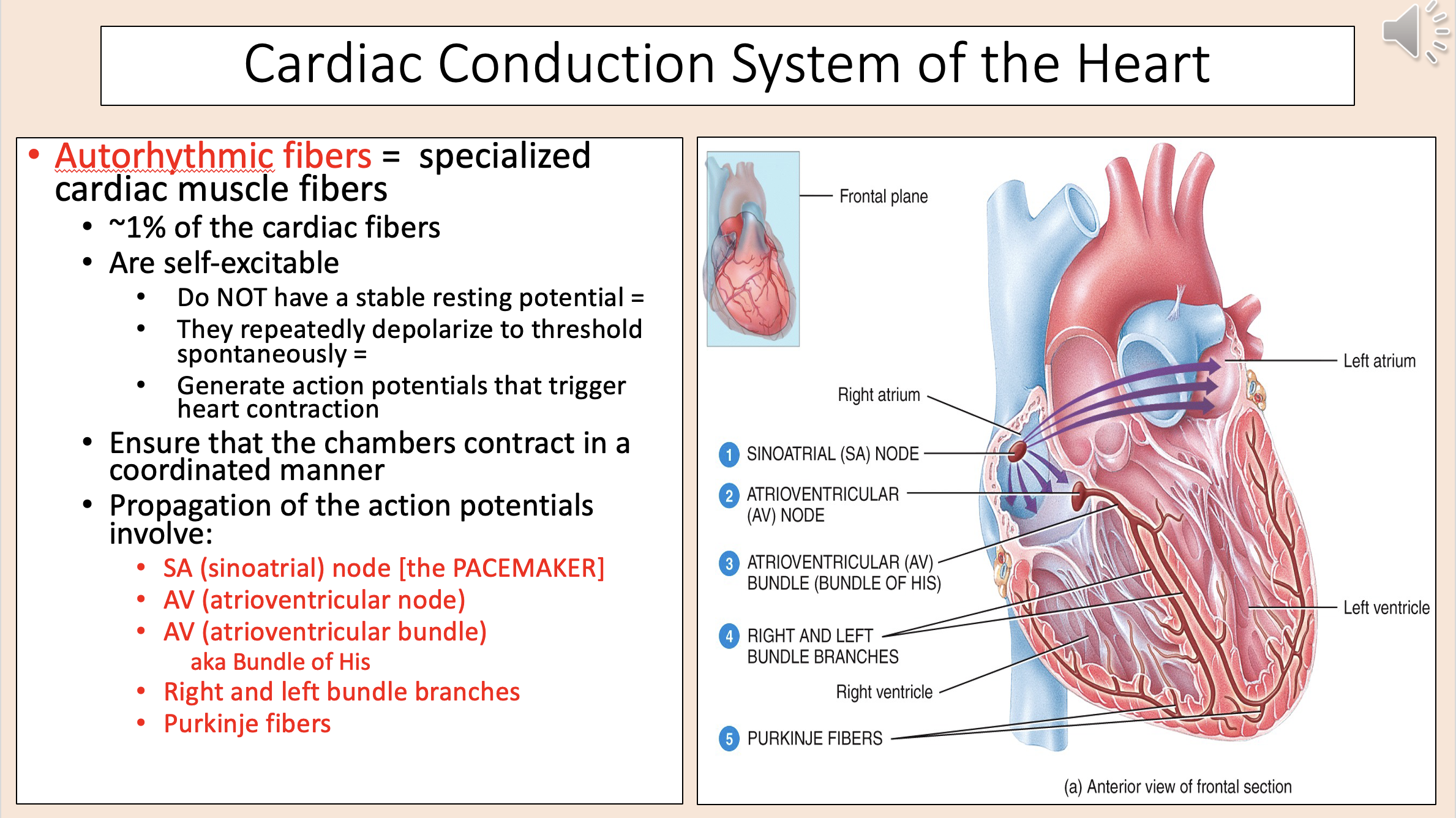
The pacemaker
sinoatrial (SA)
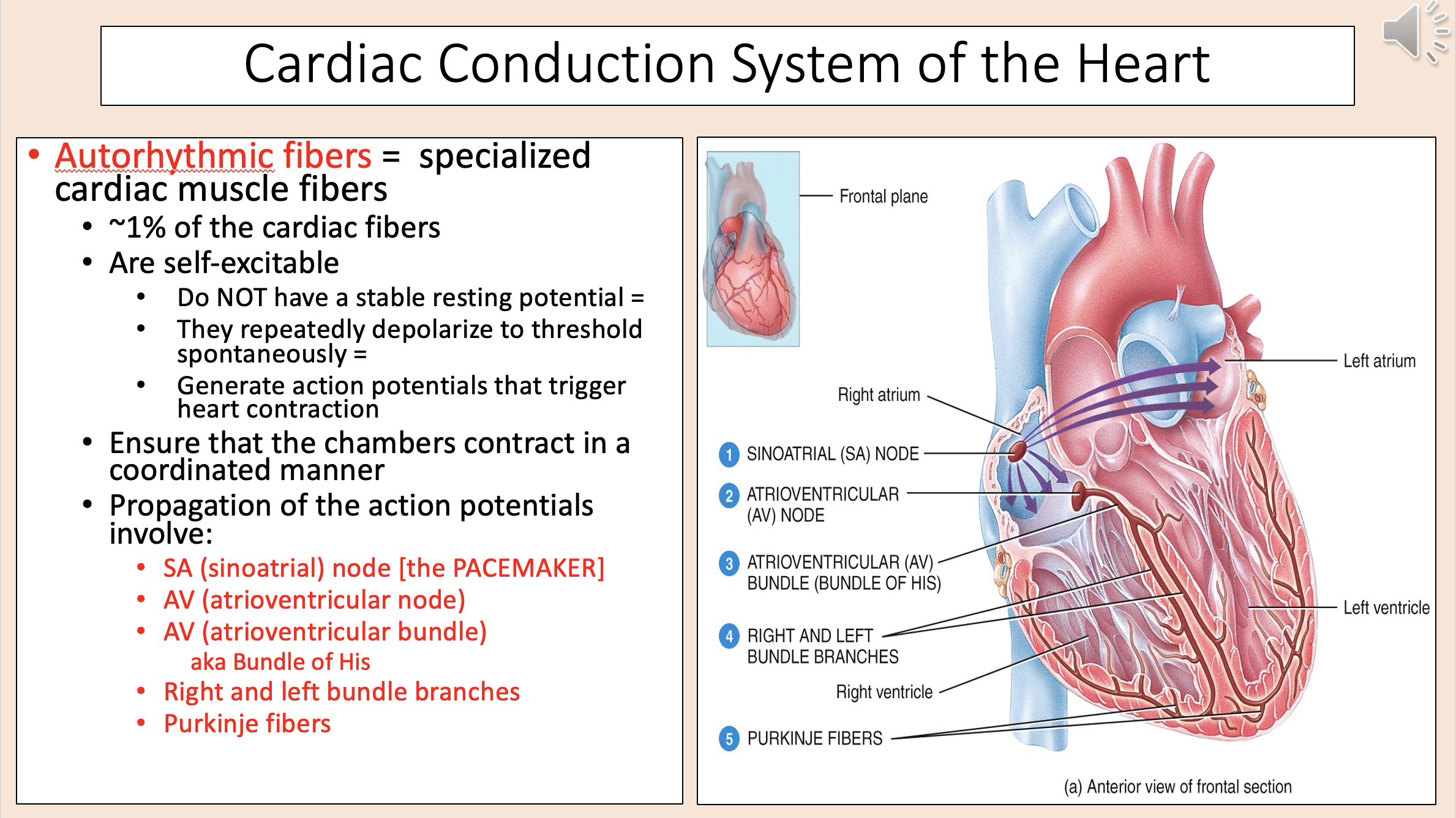
aka Bundle of His
atrioventricular bundle (AV)

The natural pacemaker (sets rhythm for contraction of heart).
In right atrial wall.
SA node

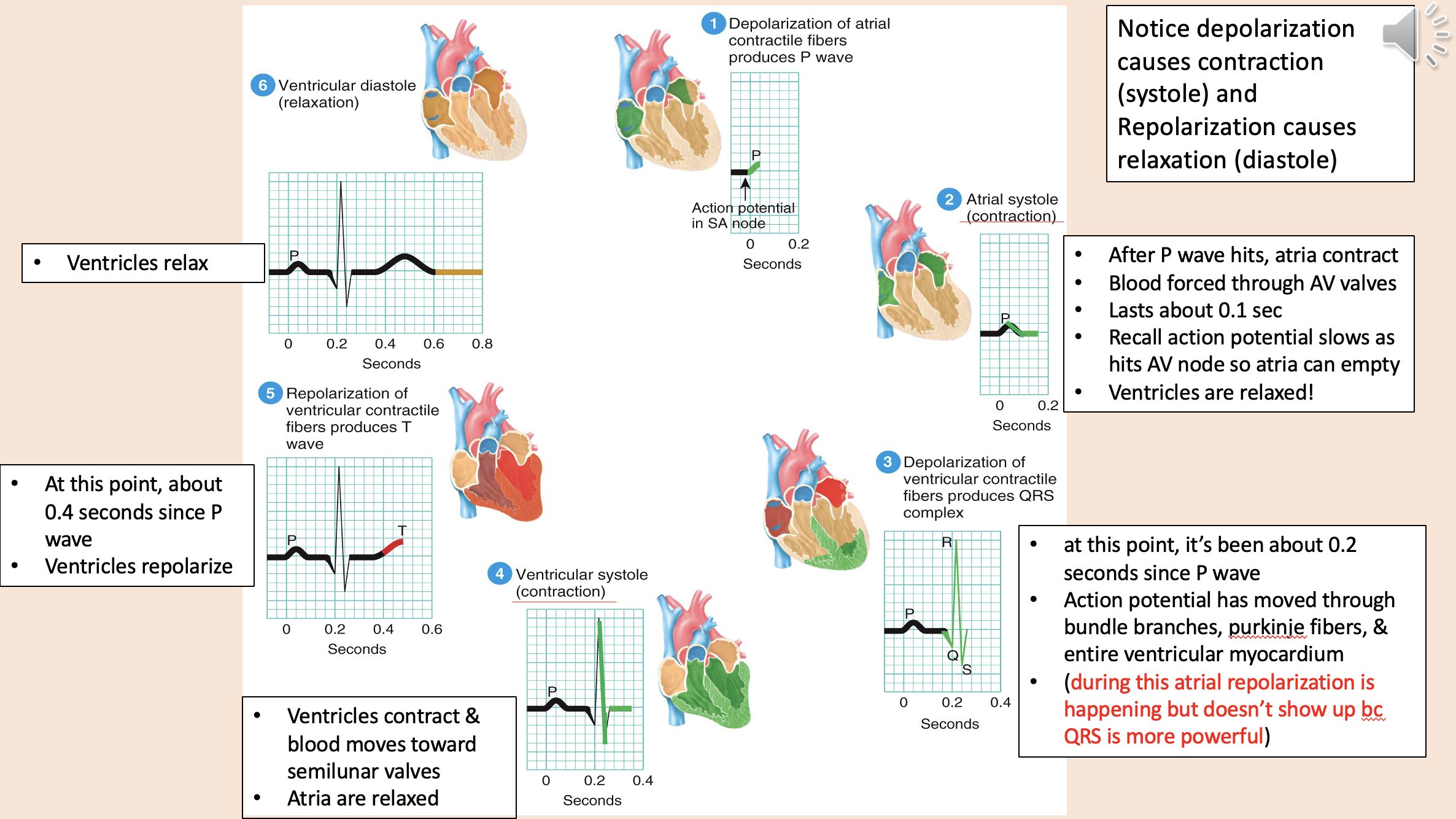
Depolarization causes contraction
systole
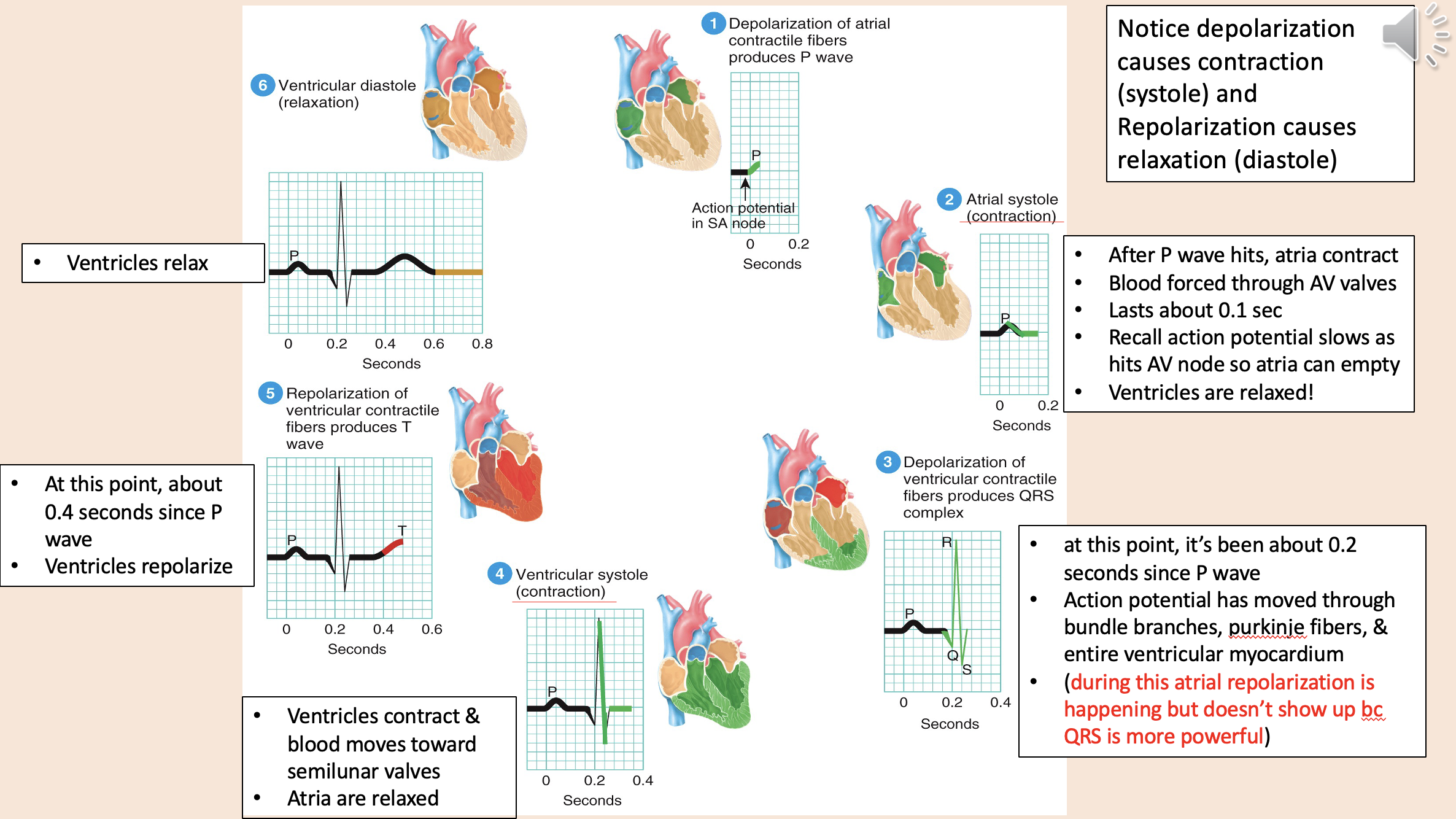
Repolarization causes relaxation
diastole
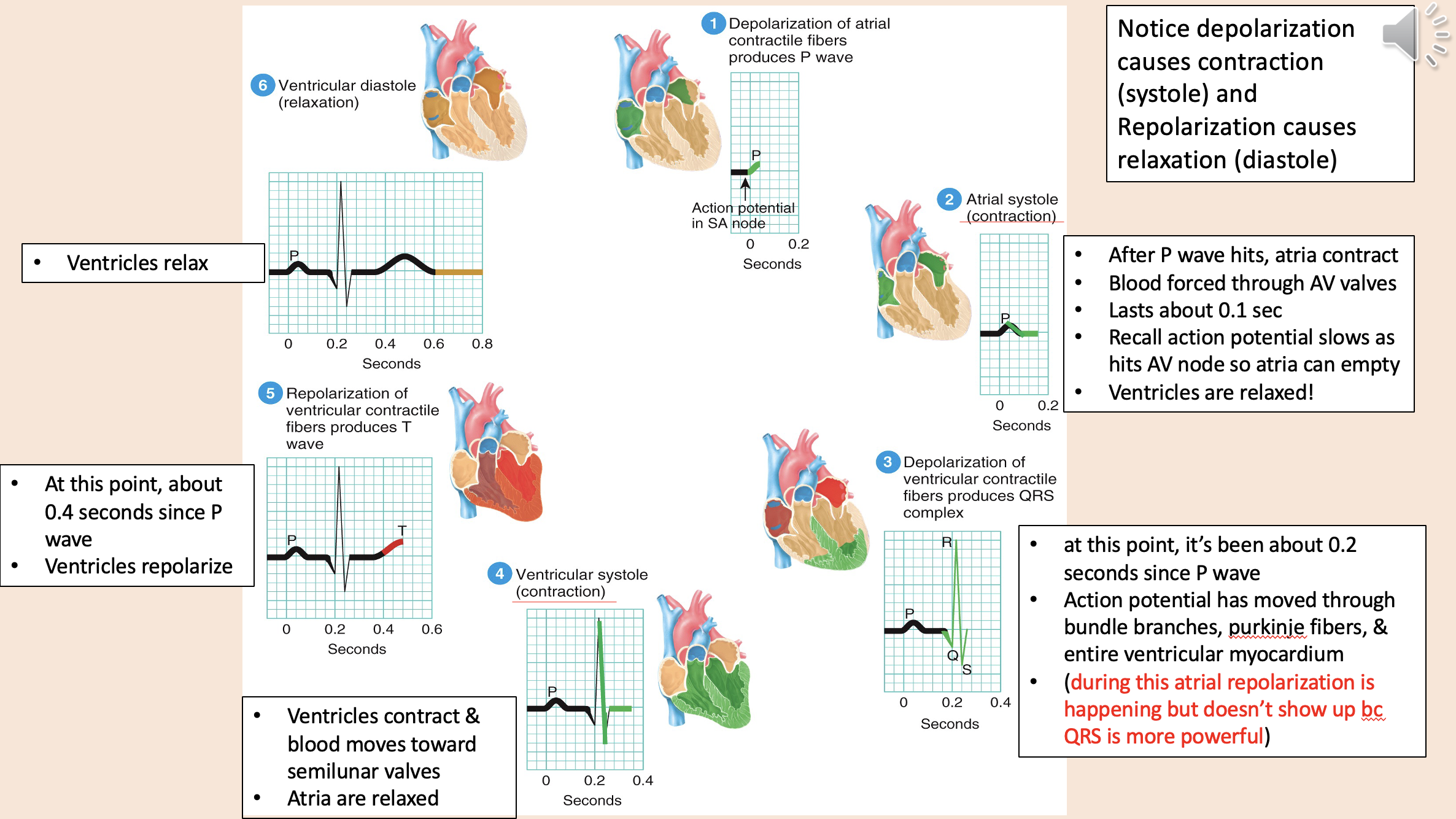
Action potential
depolarization of atria
atrial systole
depolarization of ventricular
ventricular systole
depolarization of ventricular
ventricular diastole
aka electrocardiogram or ECG
EKG
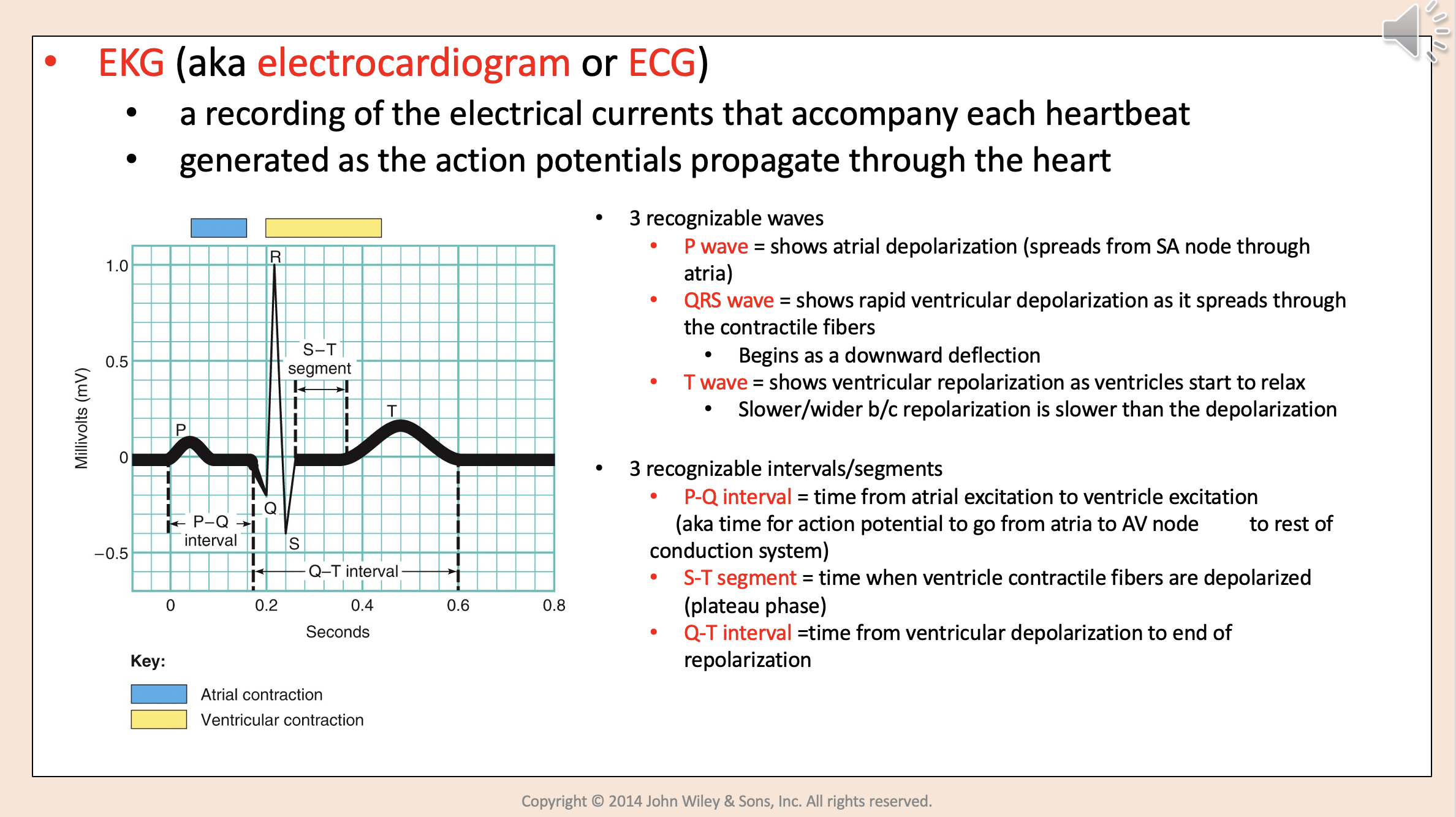
A recording of the electrical currents that accompany each heart beat.
Generated as the action potentials propagate through the heart.
EKG
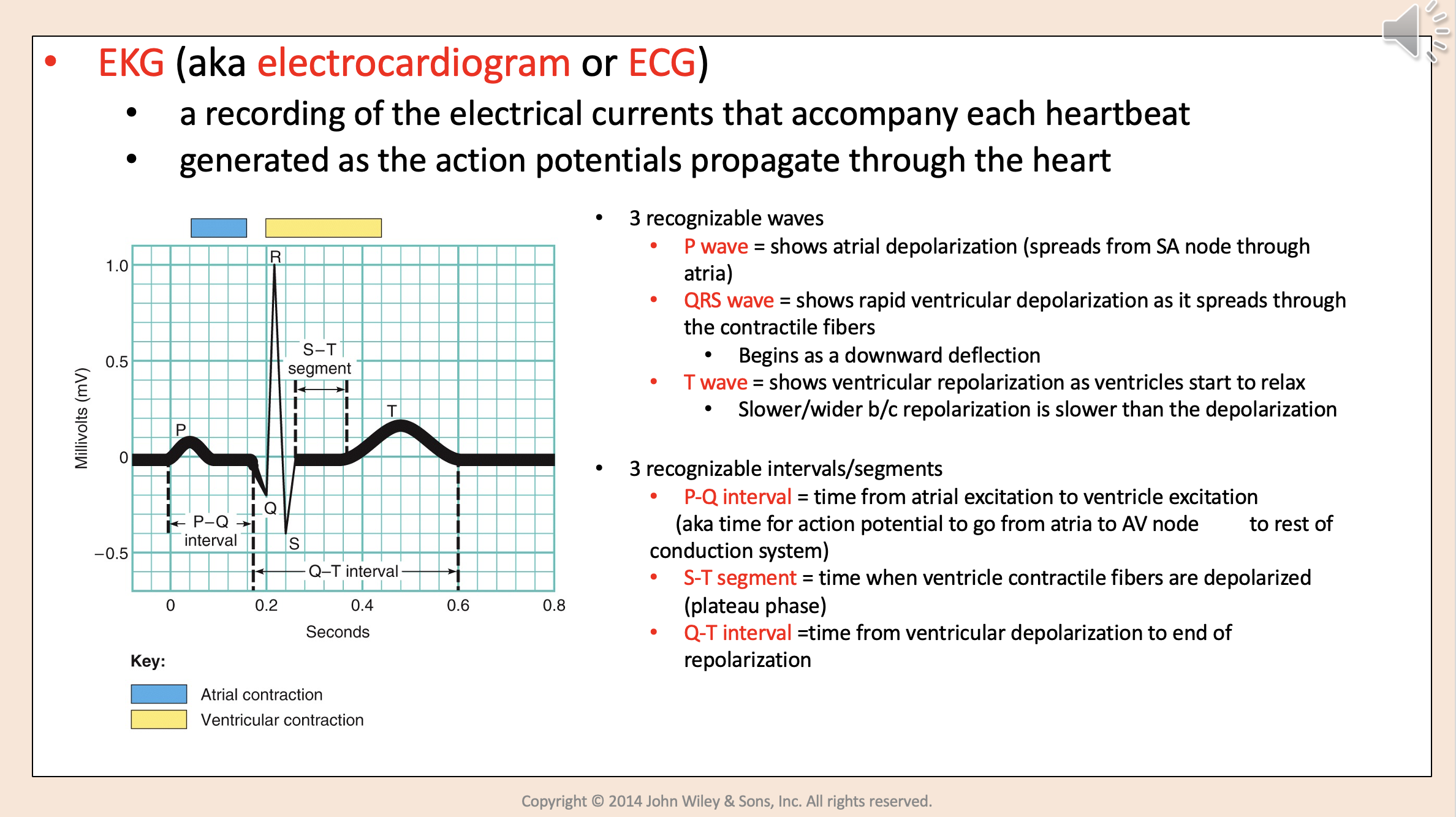
3 recognizable waves:
P wave
QRS wave
T wave
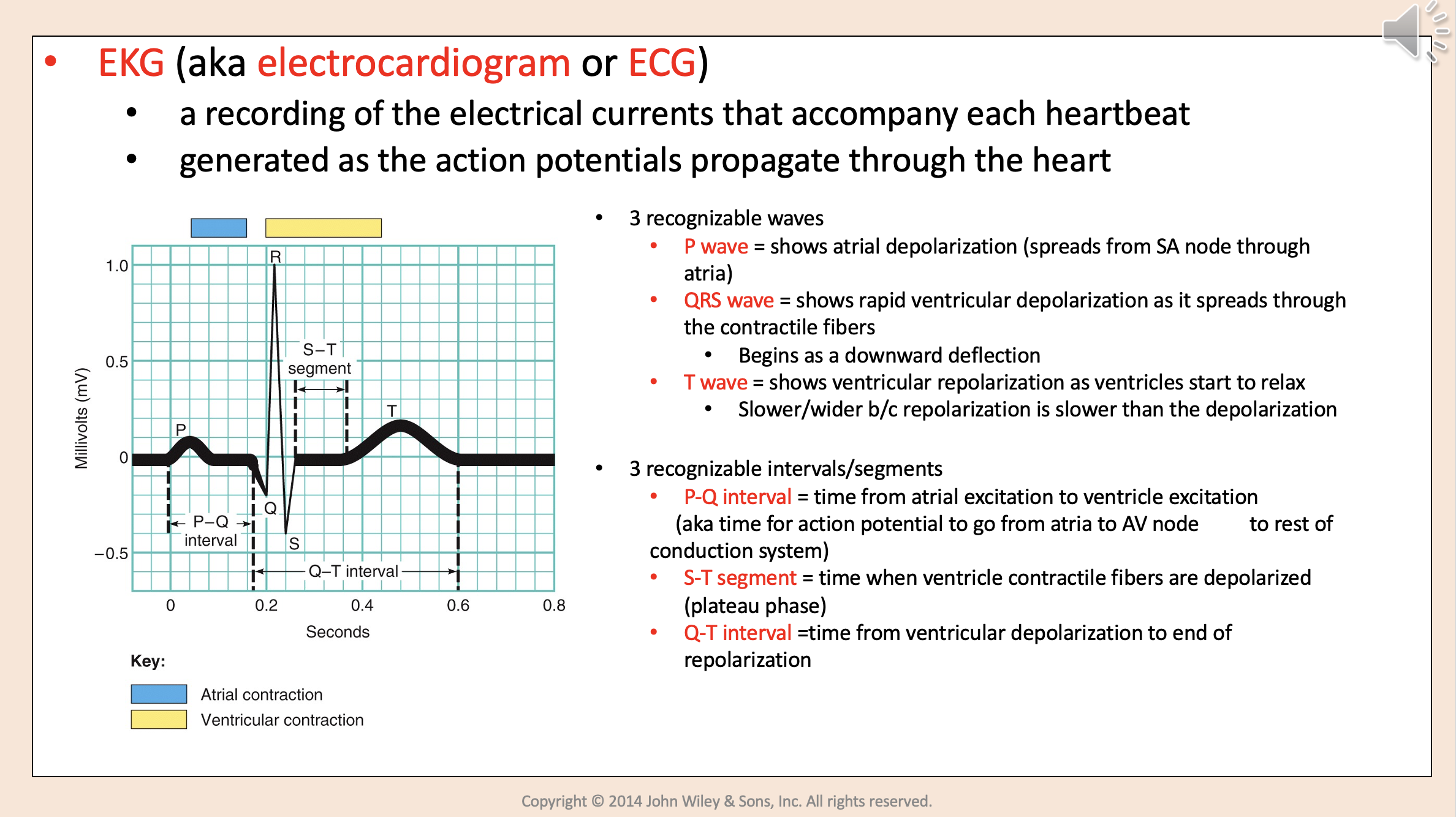
Shows atrial depolarization (spreads from SA node through atria)
P wave
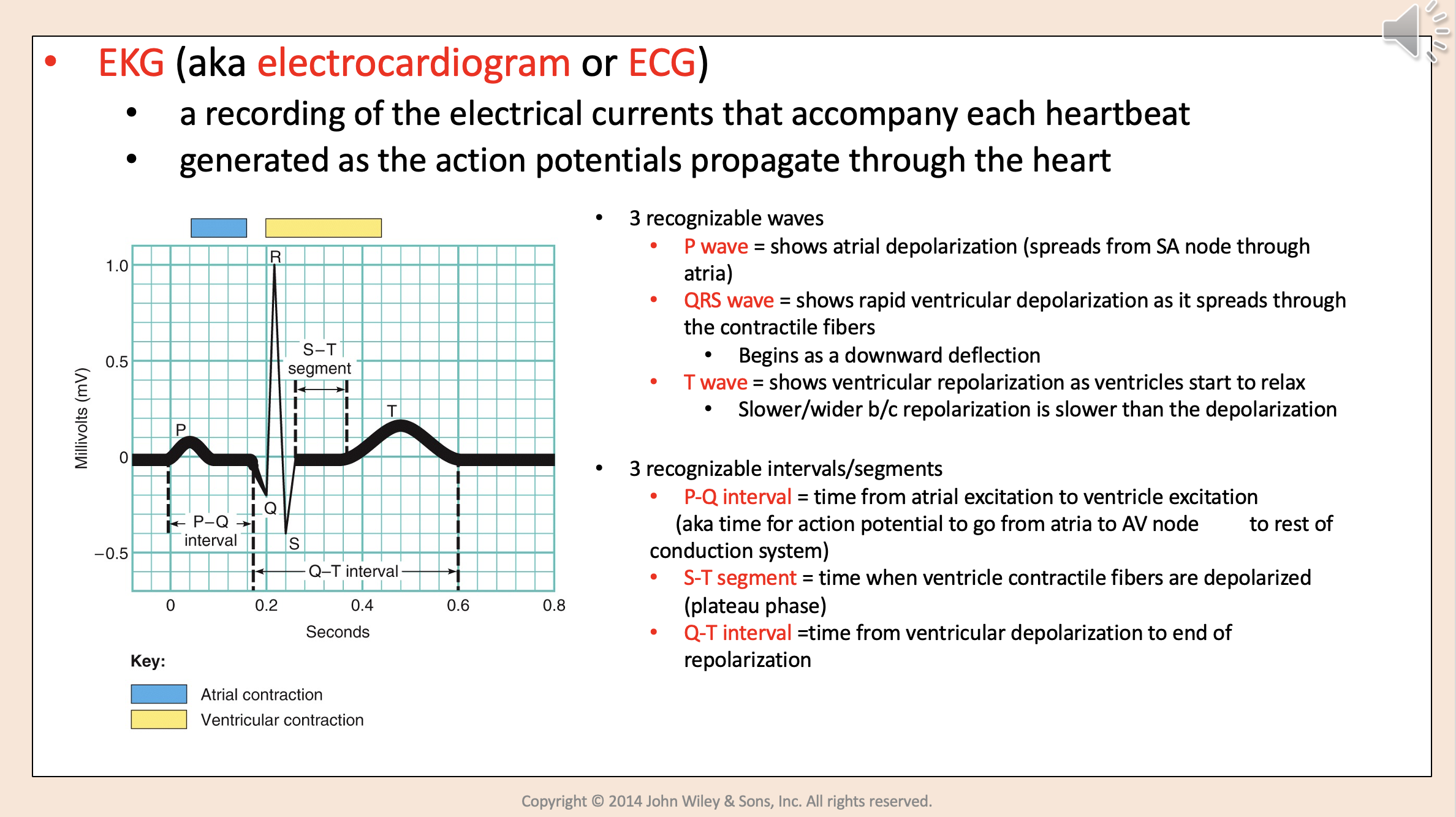
Shows rapid ventricular depolarization as it spreads through the contractile fibers.
Begins as a downward deflection.
QRS wave
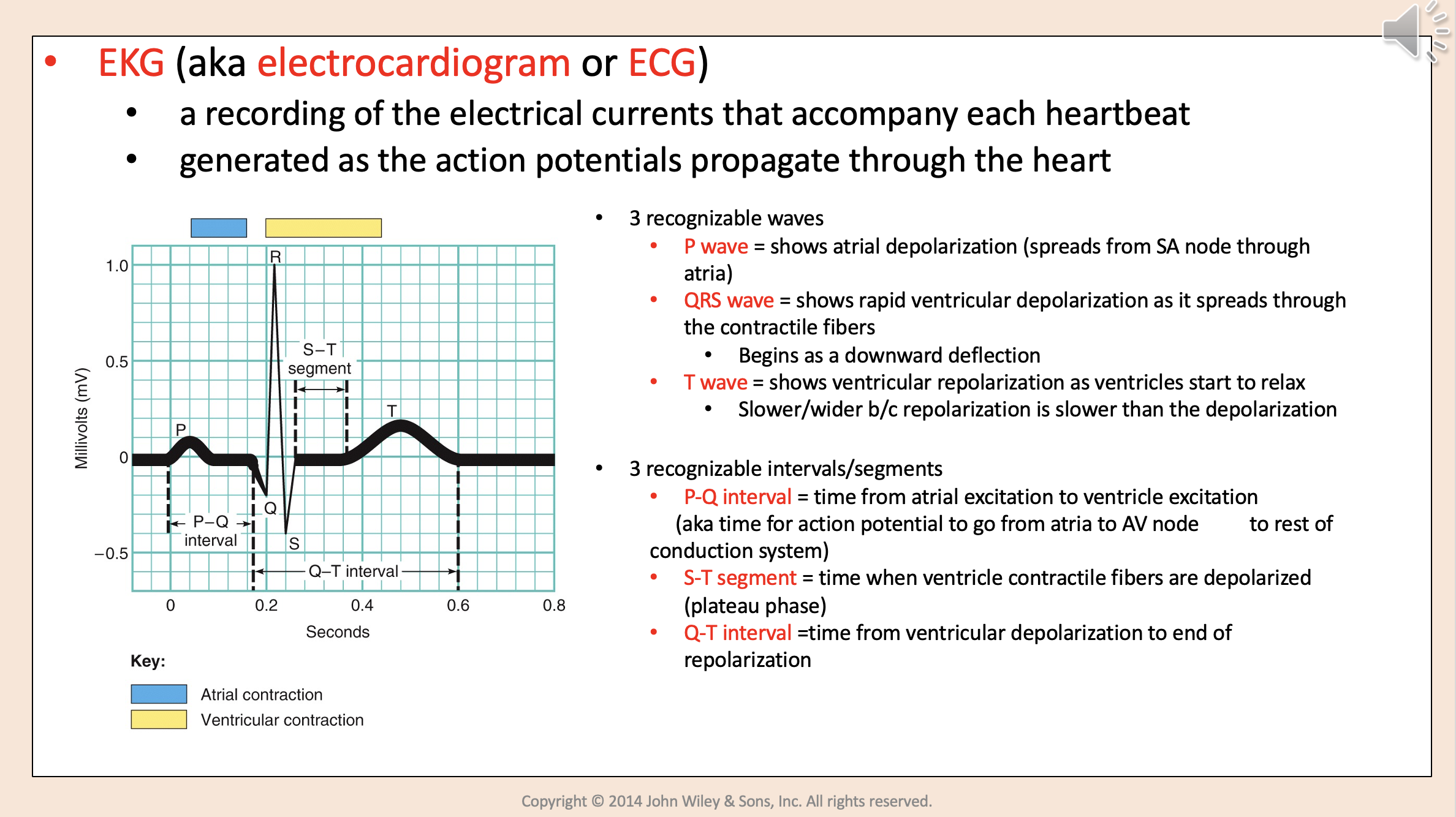
Shows ventricular repolarization as ventricles start to relax.
Slower/wider b/c repolarization is slower than the depolarization.
T wave
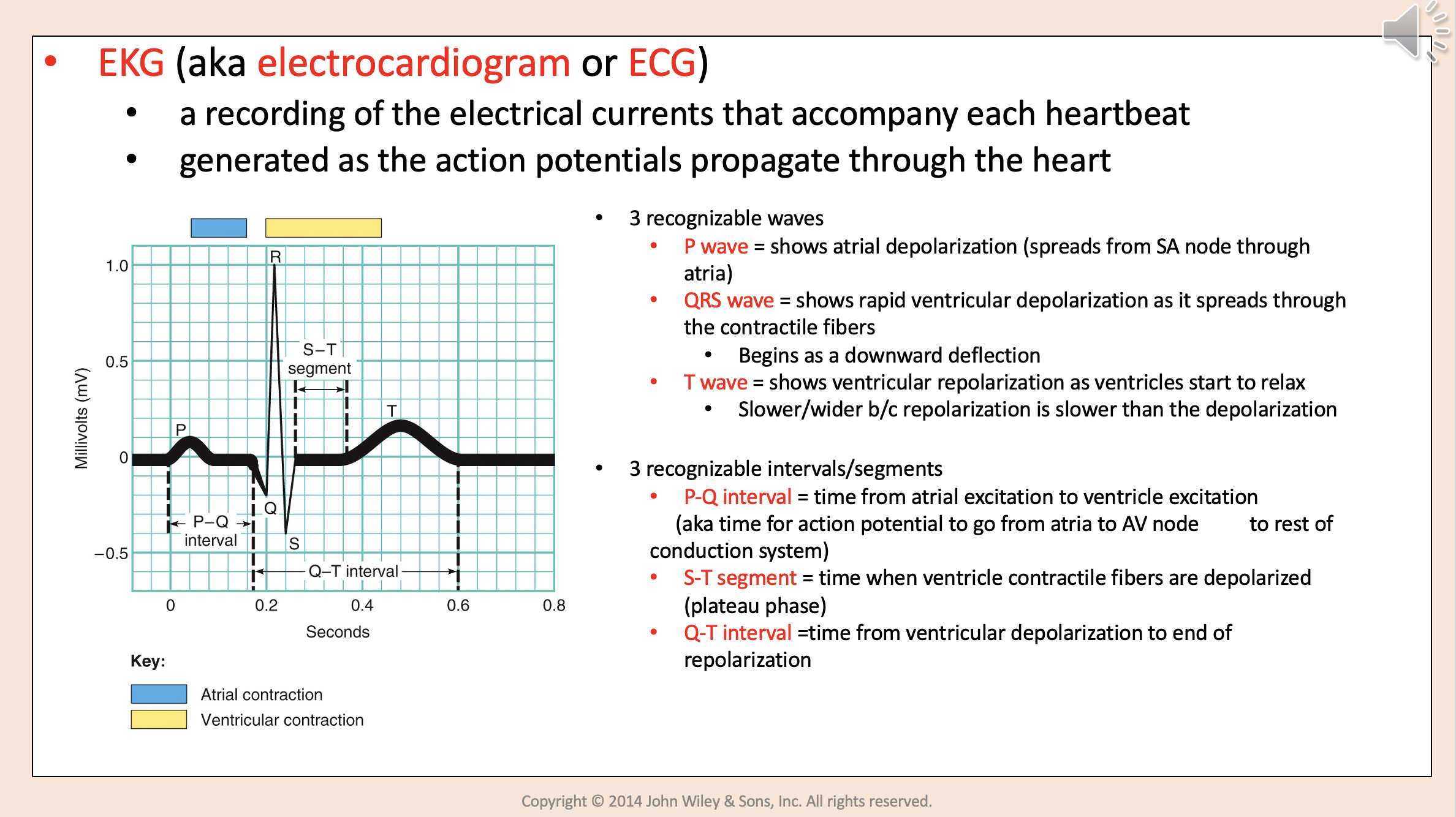
3 recognizable intervals/segments:
P-Q interval.
S-T segment.
Q-T interval.
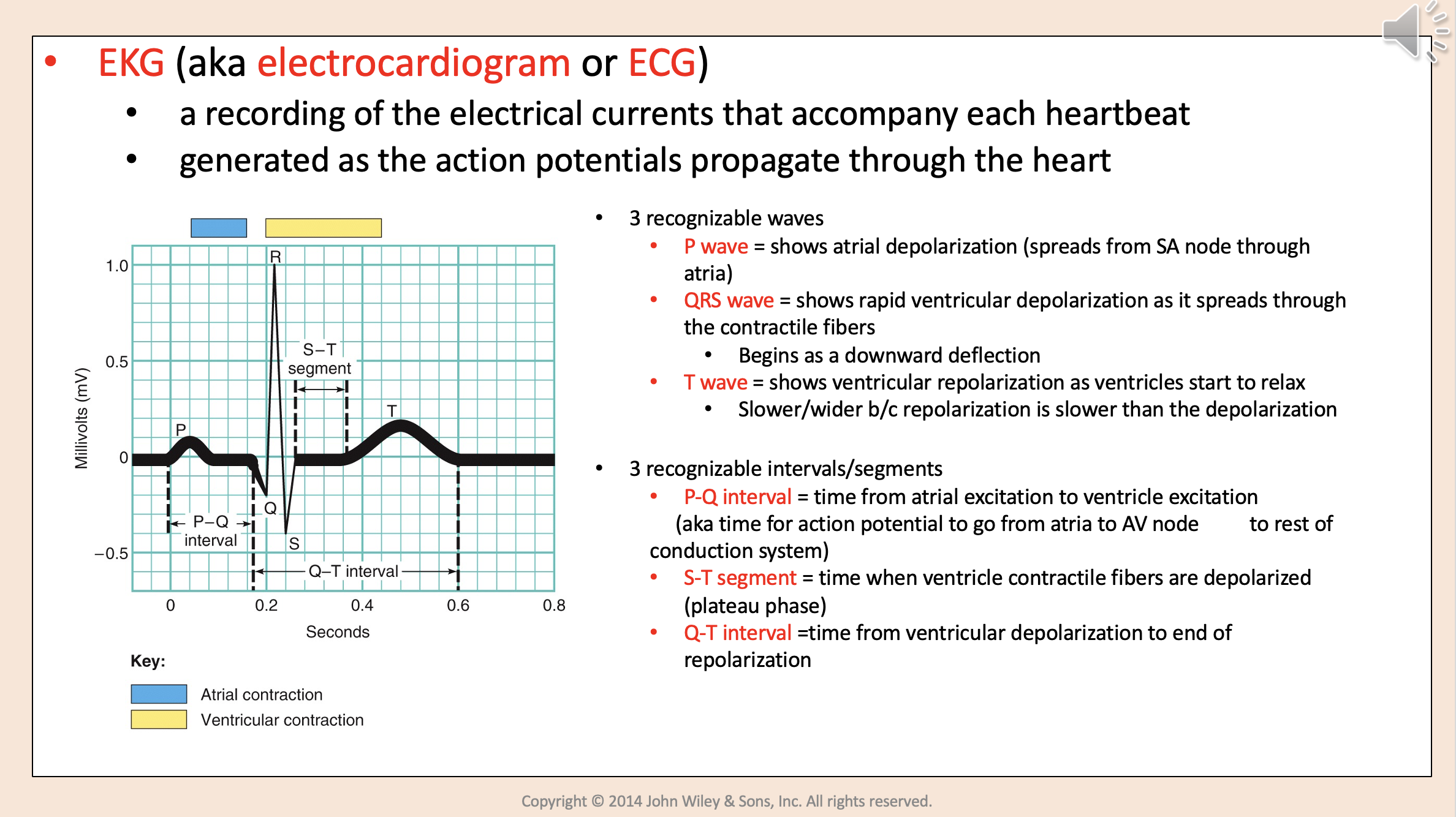
Time from atrial excitation to ventricle excitation.
aka time for action potential to go from atria to AV node to rest of conduction system.
P-Q interval
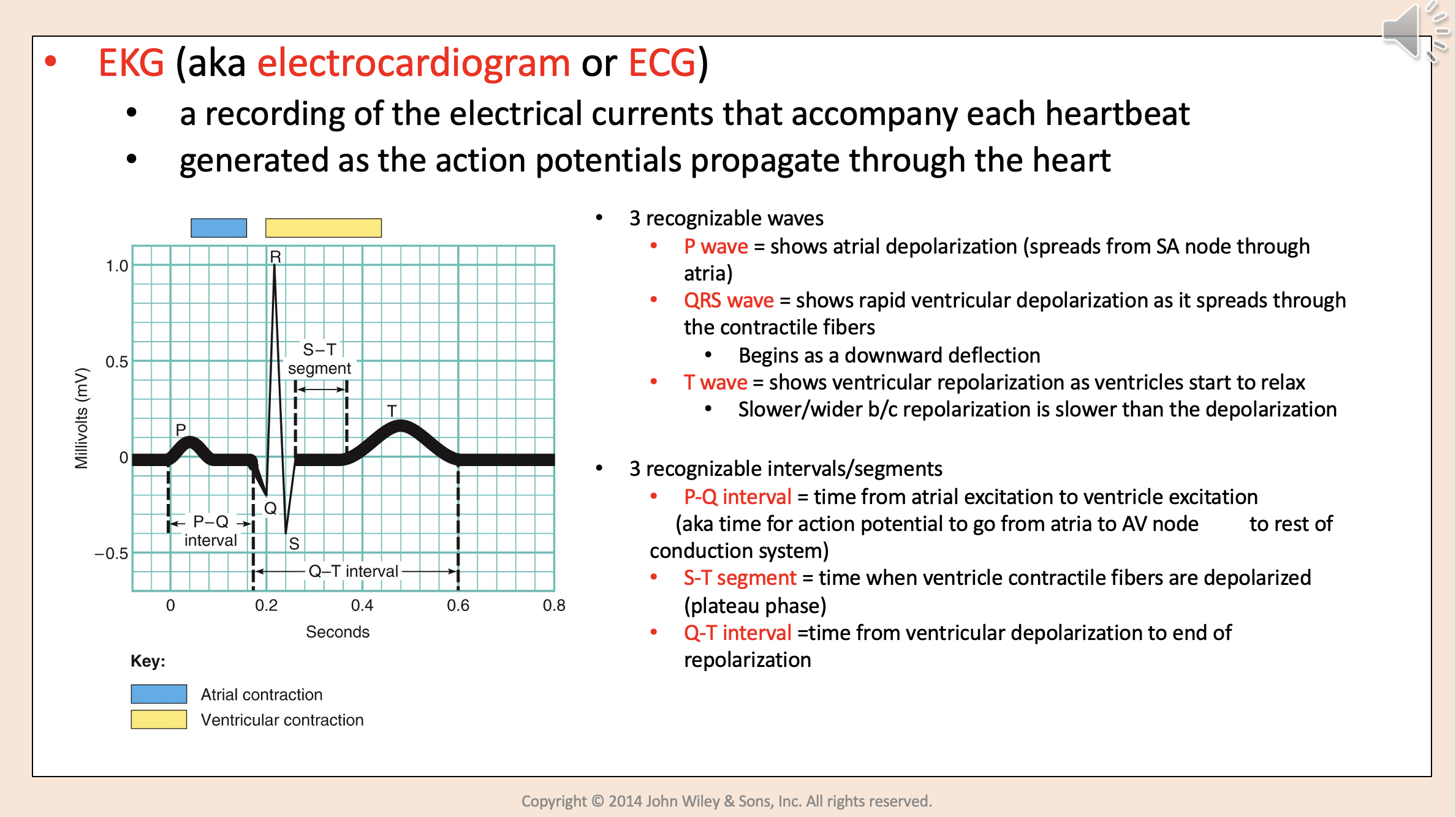
Time when ventricle contractile fibers are depolarized (plateau phase)
S-T segment
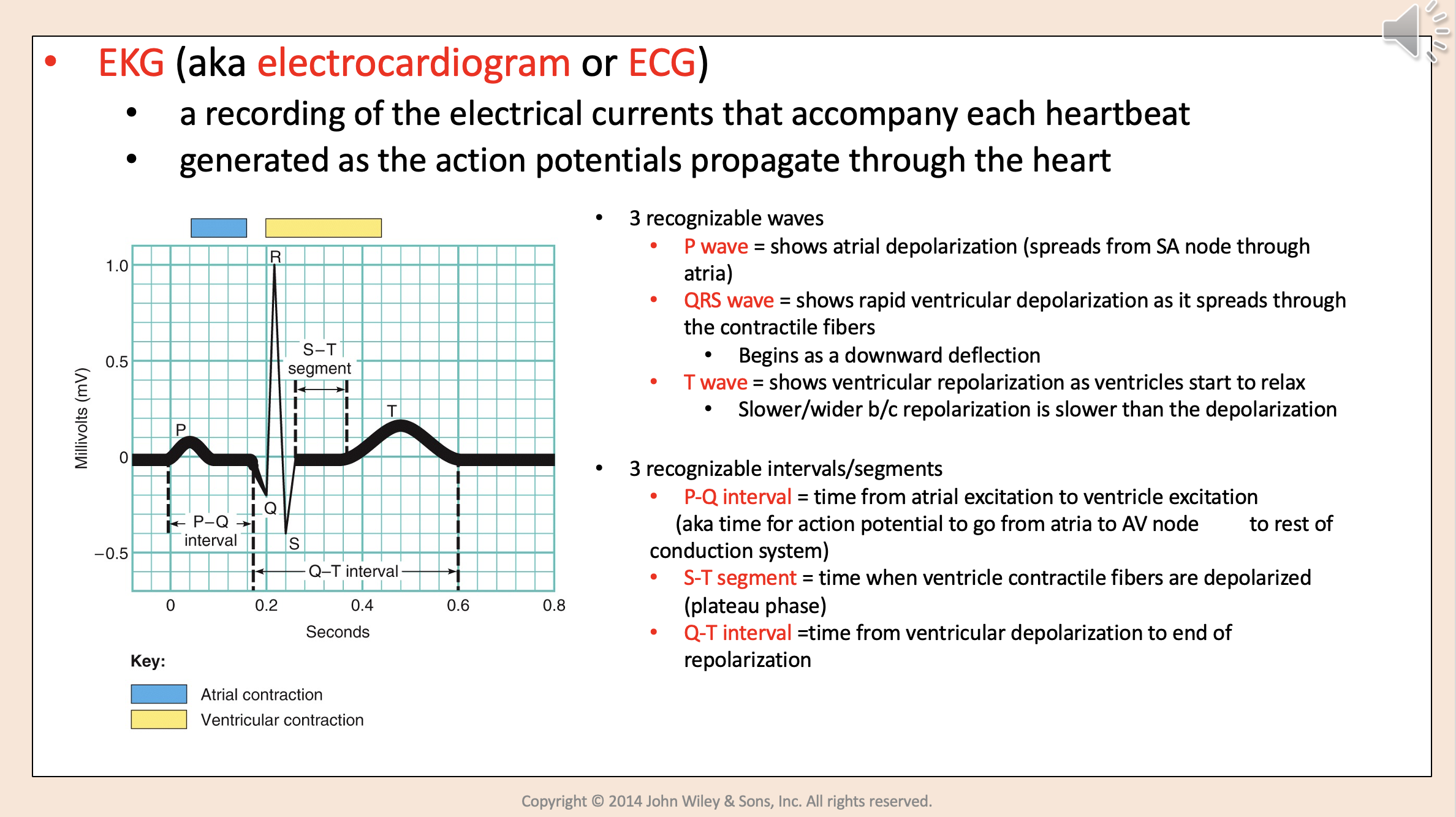
Time from ventricular depolarization to end of repolarization
Q-T interval
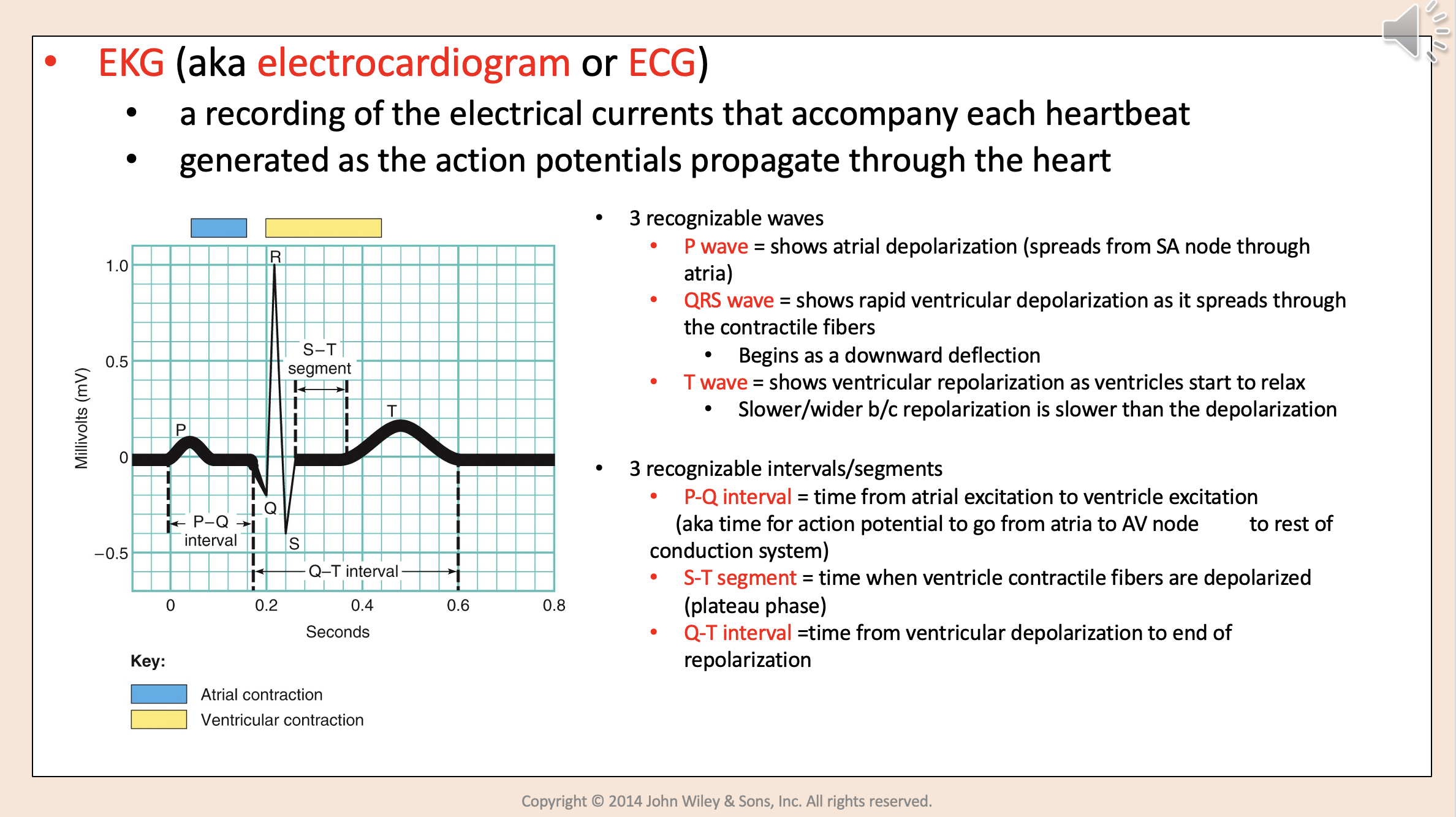
All the events associated with one heart beat (aka systole and diastole of atria & ventricles)
cardiac cycle

Atria contract & Ventricles relaxed
atrial Systole

Ventricles contract & atria relaxed
ventricular systole

Period of time when all 4 valves are closed & ventricular volume remains the same
isovolumetric contraction

amount ejected = EDV-ESV
stroke volume

Atria & ventricles are BOTH relaxed
relaxation period

A period of time when all 4 valves are closed & blood volume remains the same
isovolumetric relaxation

Amount of blood the heart pumps per minute
cardiac output

stroke volume (SV) x heart rate (HR)
CO

Maximum percentage of increase in CO one can achieve above their resting level
cardiac reserve
