Uark Human Anatomy Becker Exam 2
1/426
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
427 Terms
Parts of the Skeletal System
Skeleton, Cartilage, Ligaments
Axial Skeleton
Skull, spine, thoracic cage
Appendicular Skeleton
Limbs, pectoral girdle, pelvic girdle
Functions of the Skeletal System
1. Support
2. Movement/Locomotion
3. Storage of Ca and P04
4. Blood Cell Production
5. Protection
What Makes Up Osseous Tissue?
-Matrix of Bone
-Collagen fibers
-Bone Cells
Matrix of Bone consists of:
- hydroxyapatite crystals (Calcium Phosphate and Calcium Hydroxide)
- Enables bone to resists compression
- 2/3 of bone mass
Collagen Fibers:
- makes up 1/3 of bone mass
- gives bone tensile strength
Bone Cells (Osteocytes and other cells)
account for 2% of bone mass
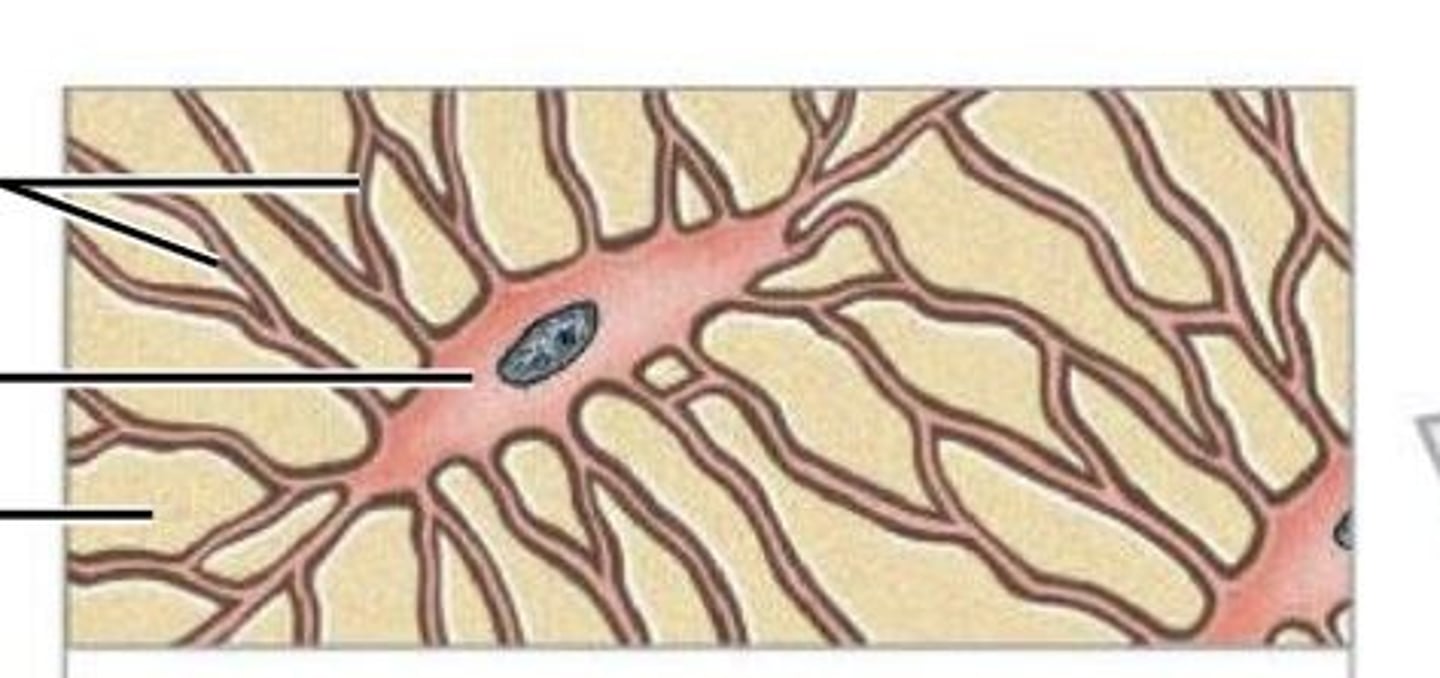
Osteocyte
mature bone cell that maintains the bone matrix
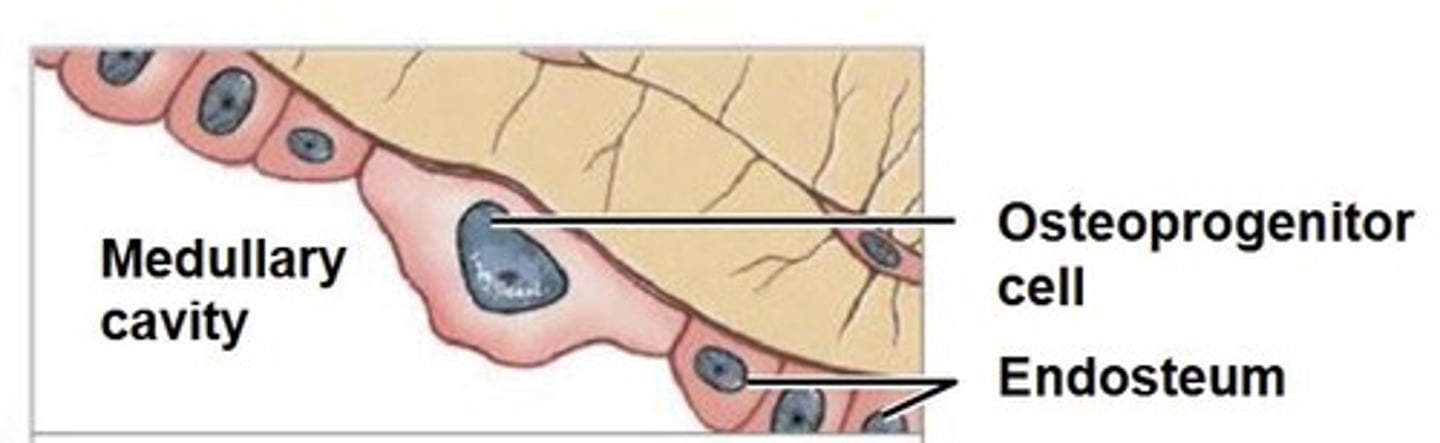
Osteoprogenitor cell
Stem cell that divides to produce osteoblasts
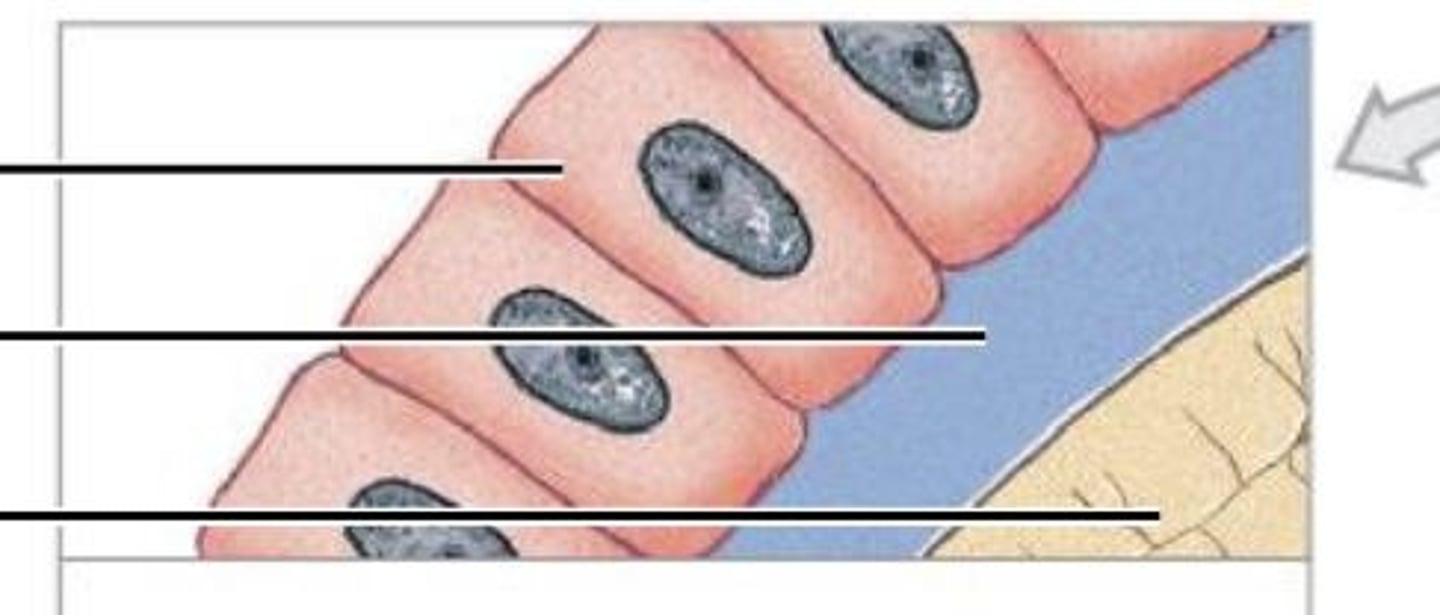
Osteoblast
Immature bone cell that secretes osteoid, the organic bone matrix
Osteoclast
multinucleate cell that secretes acid and enzymes to dissolve bone matrix
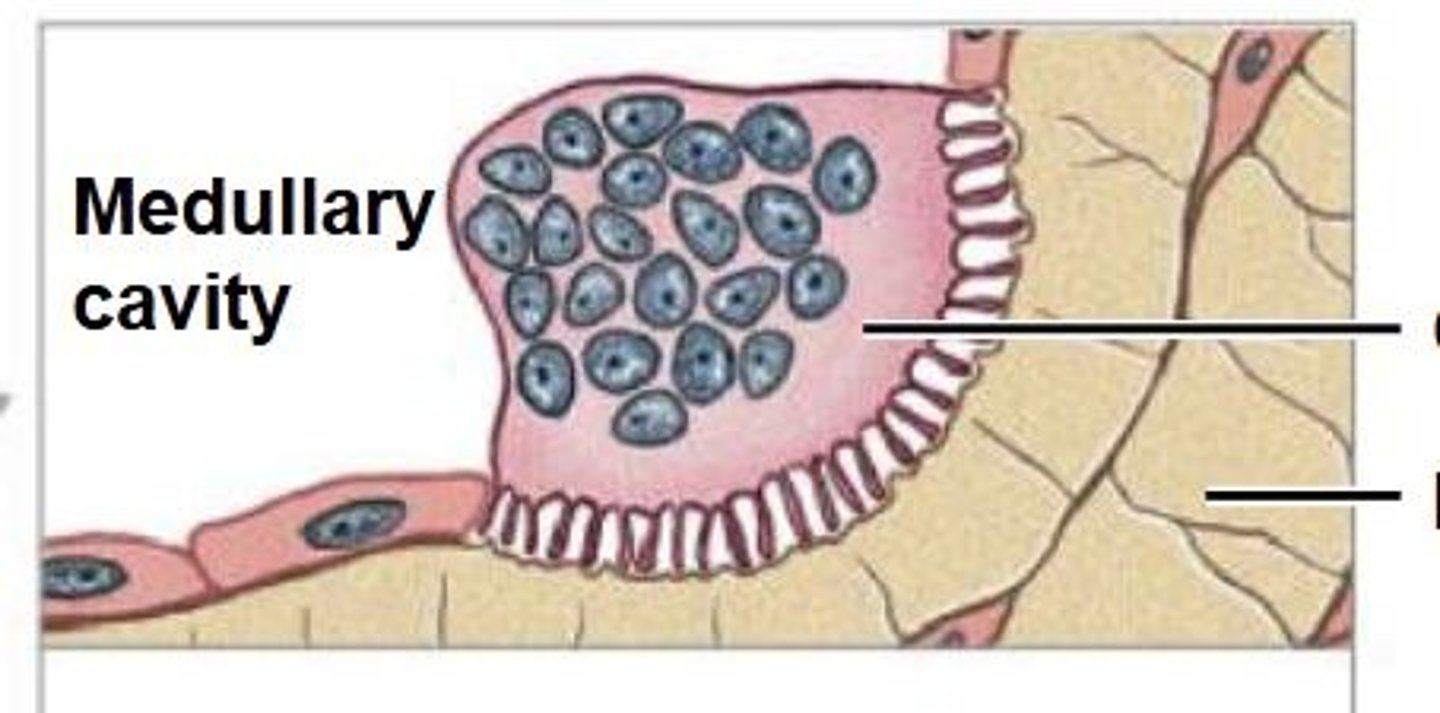
Osseous Tissue Types
compact bone and spongy bone
Compact bone
-dense and solid
-forms walls of bone
-resists parallel compression
Spongy bone
-surrounds medullary cavity
-resist multi directional or light strain
-open network of struts and plates
Epiphysis
ends of long bones
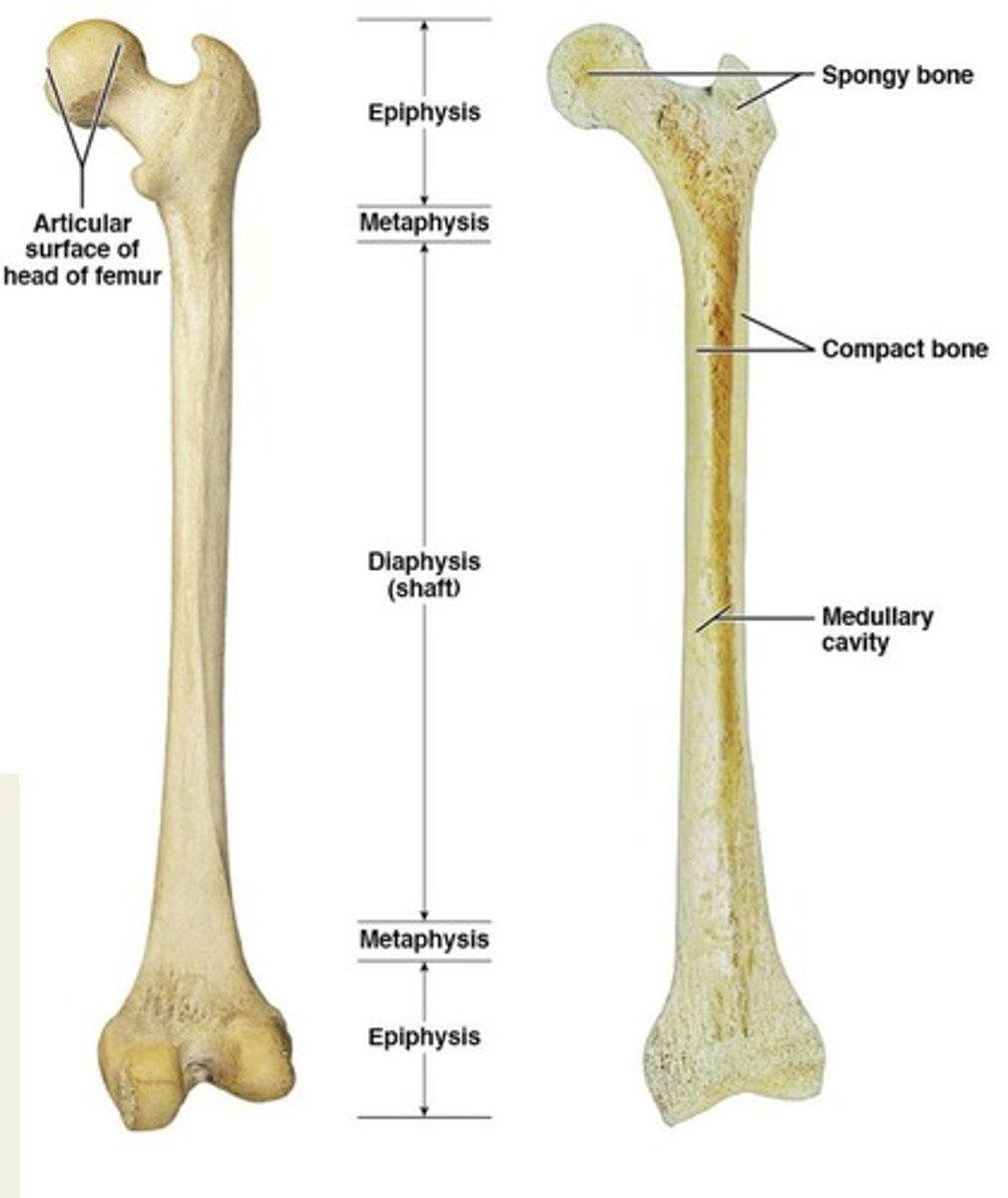
Diaphysis
shaft of long bones
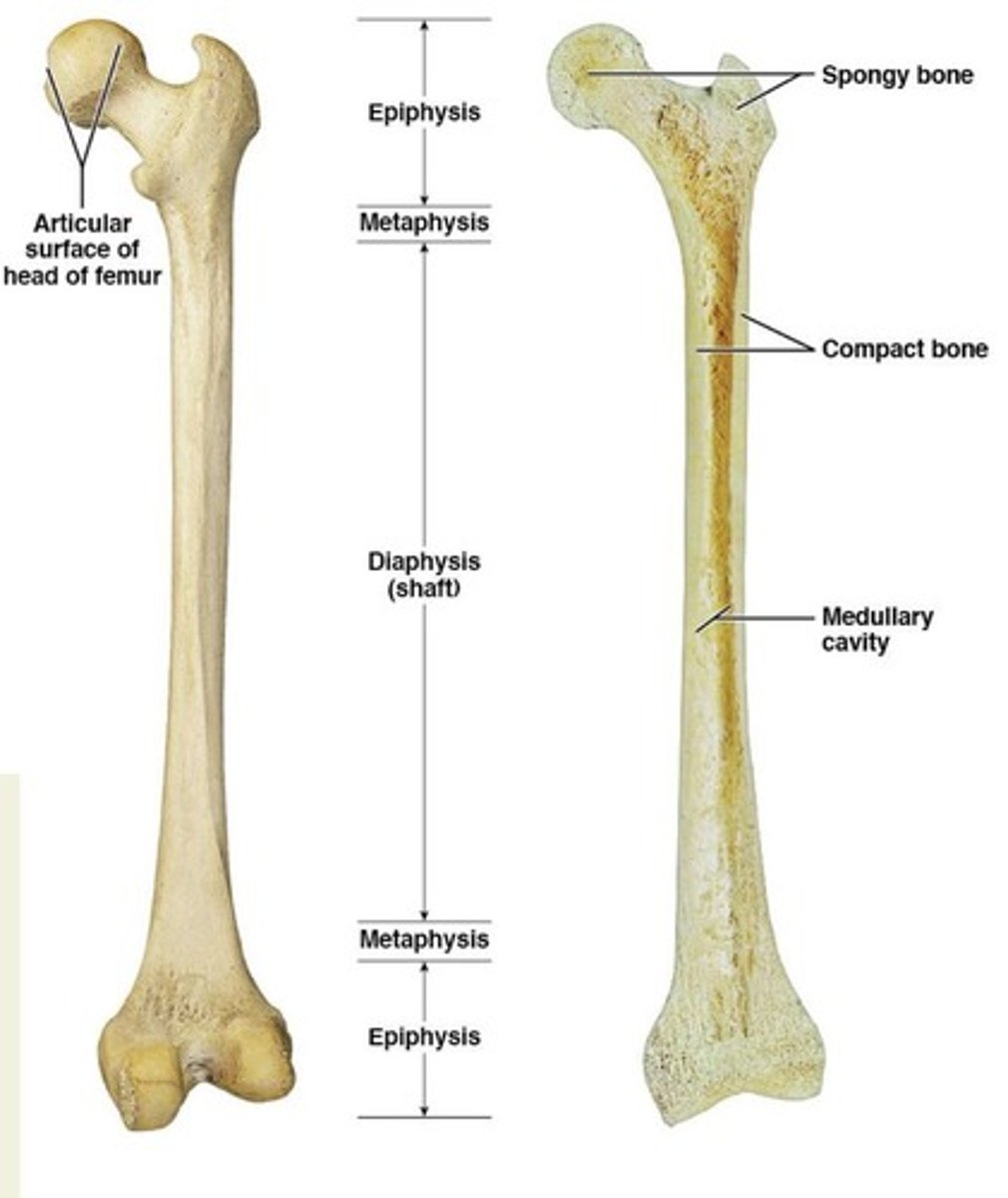
Metaphysis
transition between epiphysis and diaphysis
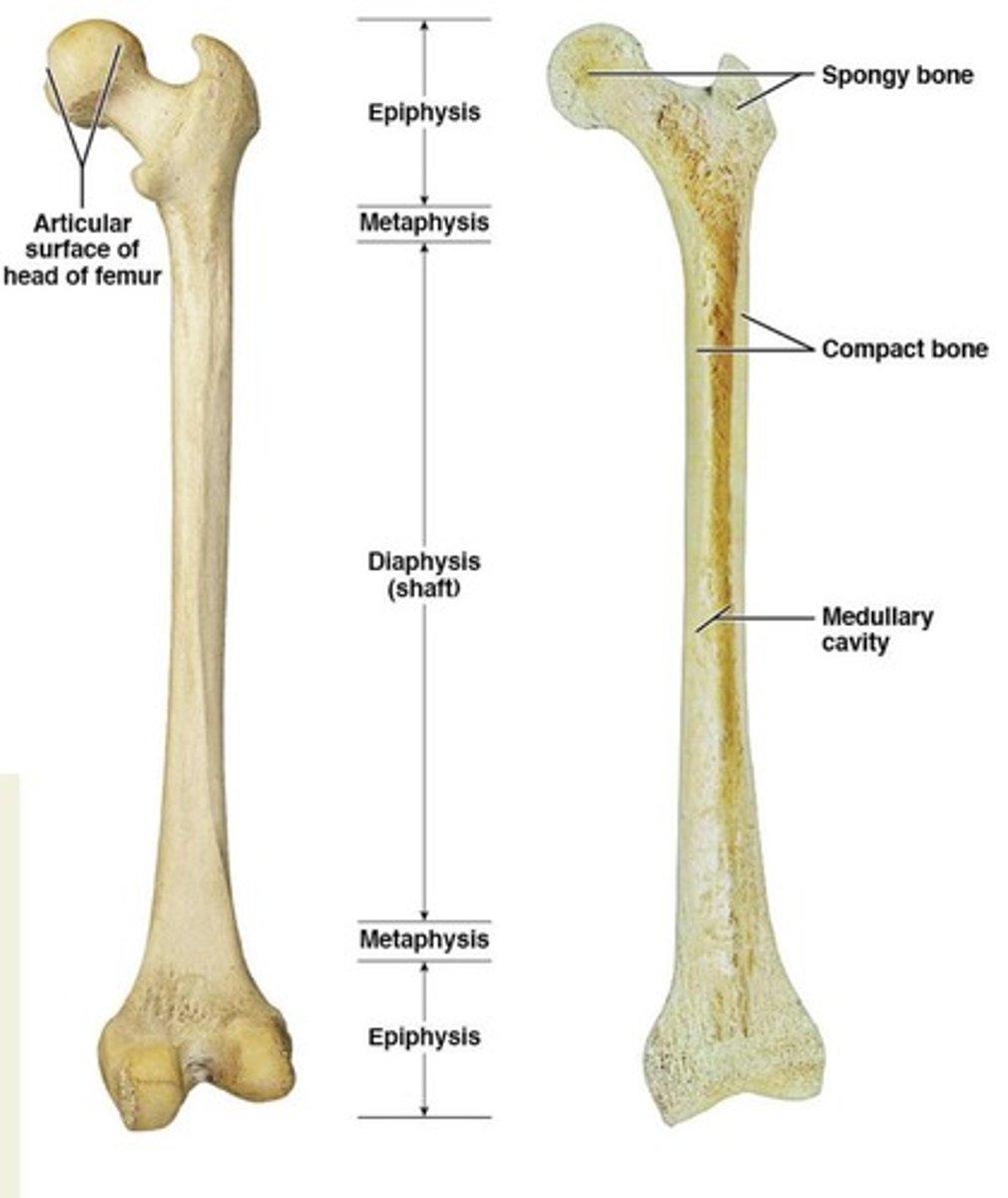
Periosteum
superficial layer of compact bone, everywhere besides within a joint, multi cell layer
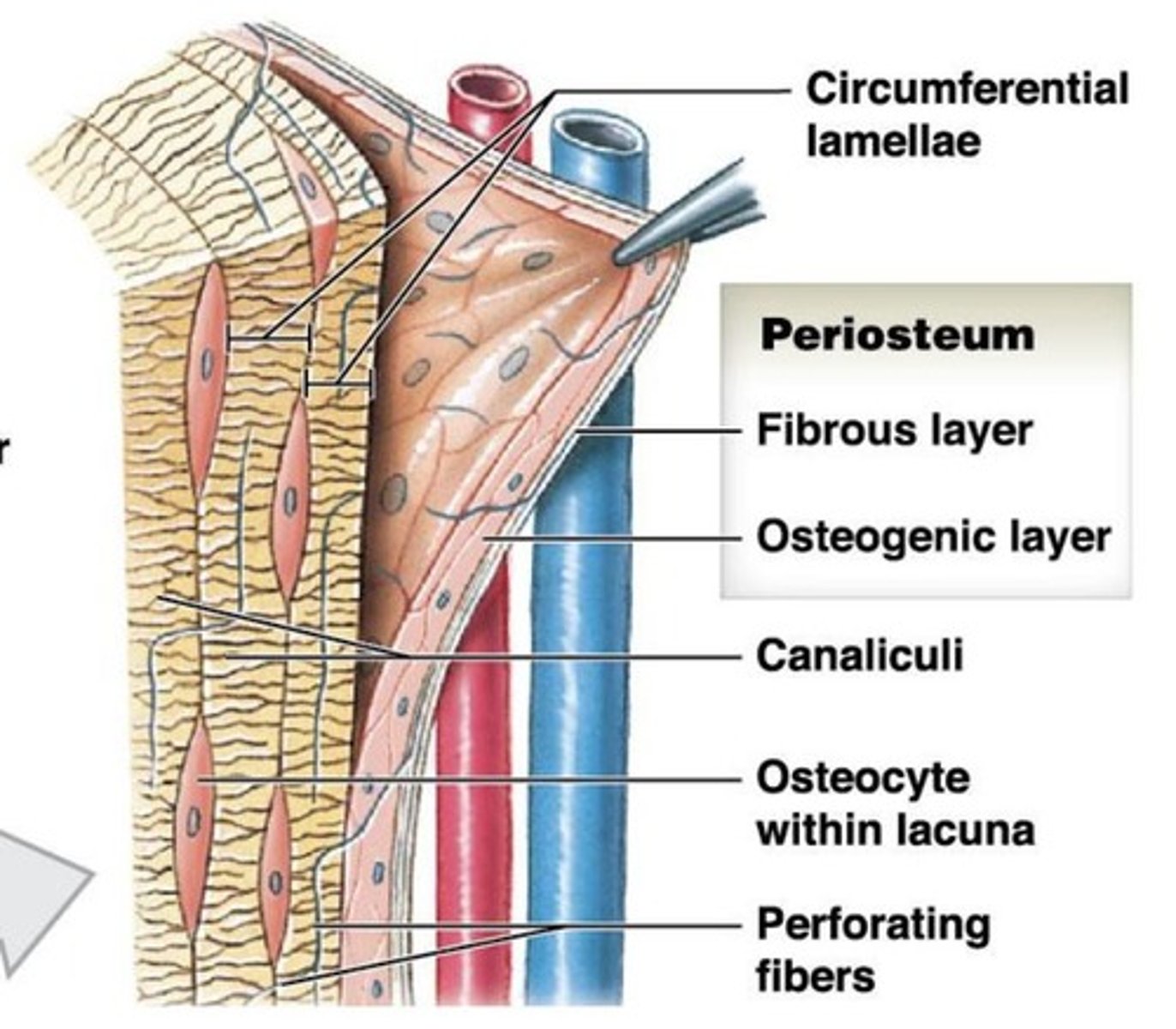
Functions of Periosteum
- Isolates and protects bone from surrounding
- Attachment for circulatory and nervous supply
- Bone growth and repair
- Attachment site for tendons and ligaments
Endosteum
inside bone, lines the medullary cavity, perforating canal, and central canal
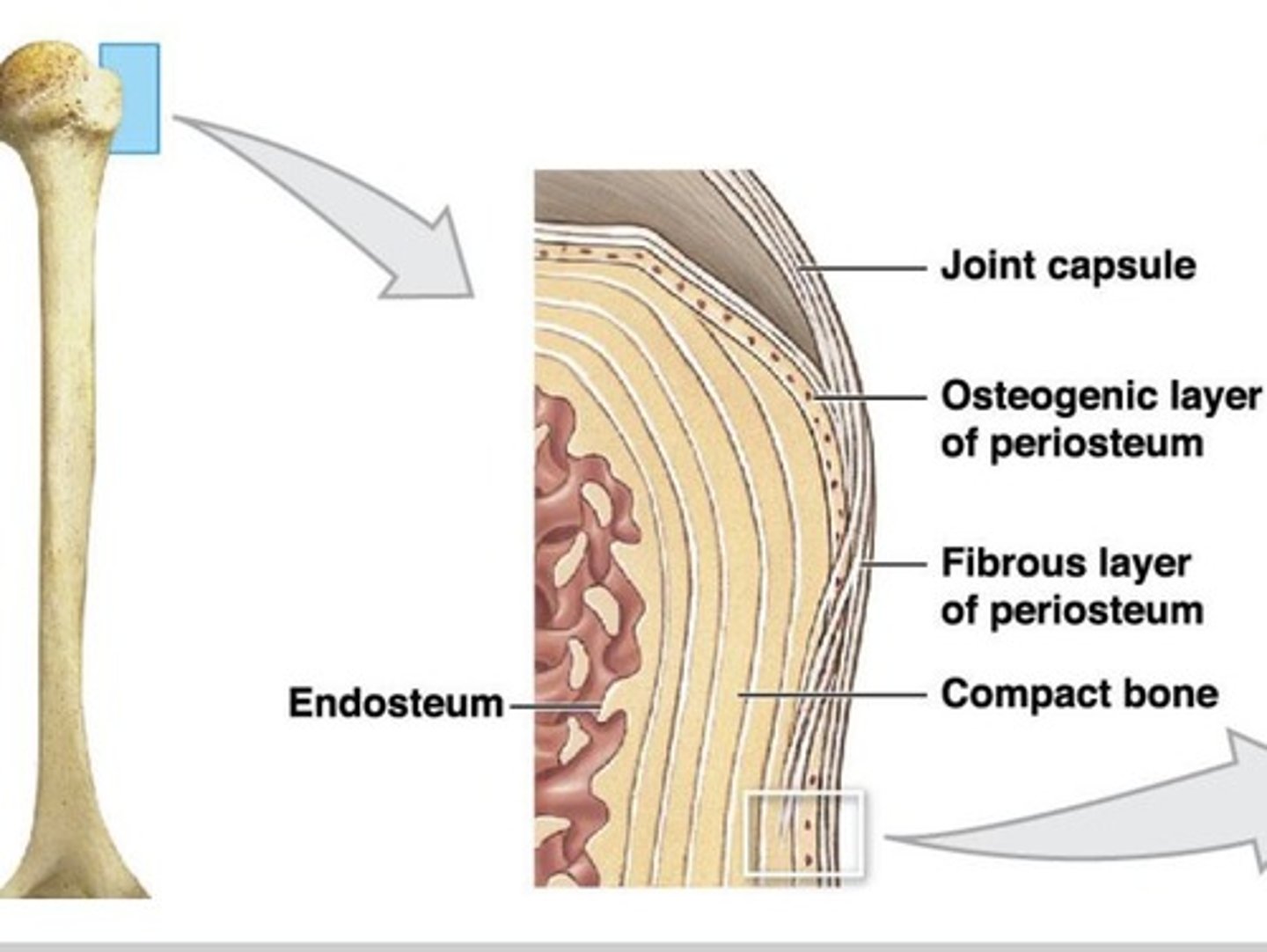
Both the Endosteum and Periosteum have:
- Osteoblast: produces matrix
- Osteoprogenitor cells: produce osteoblasts
- Osteoclast: breakdown matrix
Appositional growth
- Osteoblasts in periosteum add bone to matrix to surface.
- Forming circumferential lamellae on out surface
- Osteons are formed
- Osteoclasts break down layer below endosteum to enlarge medullary cavity
Why do bones change shape?
Bones change shape in response to strain
Factors regulating bone growth
- Minerals
- Vitamins
Minerals affecting bone growth
calcium, phosphate, magnesium, citrate, carbonate, sodium
Vitamins affecting bone growth
A: stimulates osteoblasts
C: collagen formation and osteoblast differentiation
D: used for increase in Ca and PO4 absorption in kidneys
What do hormones do?
work to regulate plasma Ca 2+ levels
Thyroxine and Growth hormone
- influence basal metabolic rate of bone cells
- maintain activity in epiphyseal region for growth
estrogen and testosterone
-stimulate osteoblast activity causing growth spurts during puberty
-maintain bone density in adults
Parathyroid Hormones
- stimulate osteoclast
Calcitonin (produced by thyroid gland)
- inhibits osteoclasts
- decreases circulation Ca2+
Osteoporosis
a bone disease that weakens bones and causes them to likely break
Sutural Bone
found in-between flat bones, small, flat, oddly shaped.
Pneumatized
hollow and contain numerous air pockets
ex. ethmoid bone
Short bones
external surface are covered by compact bone
ex. carpal bones
Irregular bones
complex shapes with short, flat, notched, or ridged surfaces
ex. vertebra
Flat bones
thin, roughly parallel surfaces of compact bone
ex. parietal bone
Long bone
long and slender bones
ex. humerus, femur, tibia, radius, ulna
Sesamoid bone
round, small, and flat
ex. patella
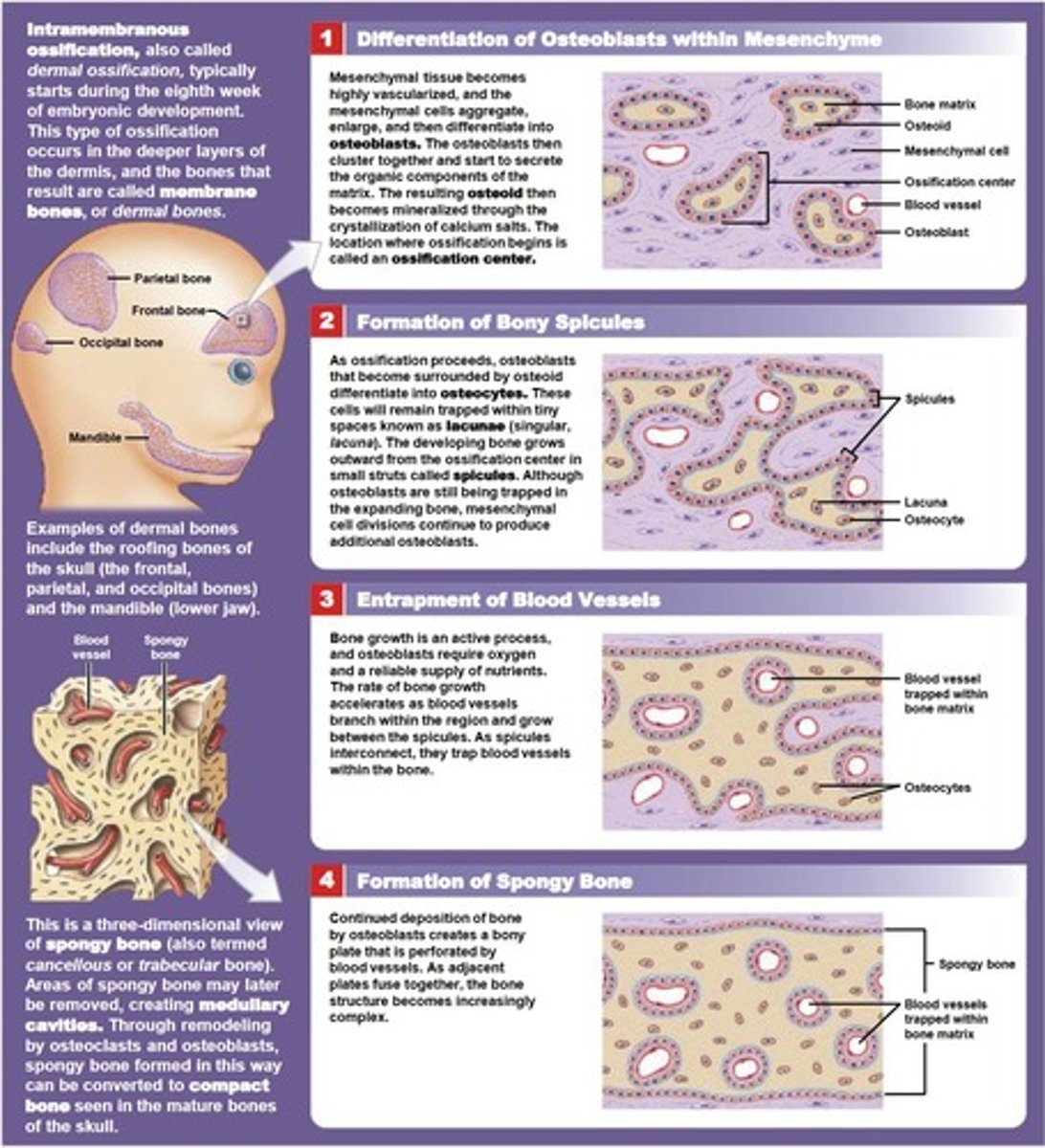
intramembranous ossification
process of creating bone from connective tissue, without going through a cartilage stage
Endochondral Ossification
process of bone formation from a pre-existing cartilage model
Steps of intramembranous ossification
1. Mesenchymal cells multiply and condense into a nodule.
2. A membrane surrounds the nodule.
3. Osteoprogenitor cells change into osteoblasts.
4. Osteoblasts line the nodule and secrete an extracellular matrix (ECM).
5. Woven bone forms.
6. Woven bone is remodeled and replaced by mature lamellar bone.
Steps of endochondral ossification
1. Formation of Cartilage model
2. Calcification of Cartilage
3. Formation of Bone Collar
4. Development of Primary Ossification Center
5. Formation of Medullary Cavity
6. Formation of Secondary Ossification Centers
7. Epiphyseal Plate Formation
8. Maturation and Remodeling
Functions of the Axial Skeleton
- Houses Central Nervous System (CNS)
- House senses
- Allows for sound production and communication
- Feeding
- Breathing
- Attachment points for appendicular system
throatic cage
-Ribs
-Sternum
-Thoracic vertebrae
-Costal Cartilage
Suture
dense fibrous connective tissue
Sinuses
- produces mucus
- Resonate sound
- Lighten skull
- Humidifies air
What are joints?
where 2 bones meet made up of fluid, cartilage, or fibrous tissue
Synarthrosis Joints
no movement
types of synarthrosis joints
fibrous, cartilaginous, bony fusion
fibrous synarthrosis
two or more bones are held together by a thin layer of dense, fibrous connective tissue (Sutures - skulls and Periodontal ligaments - tooth)
Cartilaginous synarthrosis
diaphysis and epiphyseal ends are bound together by an epiphyseal cartilage (sternum)
Bony Fusion synarthrosis
joint where boundary between them disappears making a longer bone (frontal bone)
Amphiarthrosis
some movement
fibrous amphiarthrosis
bones connected by collagen fibers
ex. between tibia and fibula, fibula and talus
Cartilaginous amphiarthrosis
bones connected by fibrous cartilage
ex. pubic symphysis and intervertebral discs
Diarthrosis (synovial)
free movement
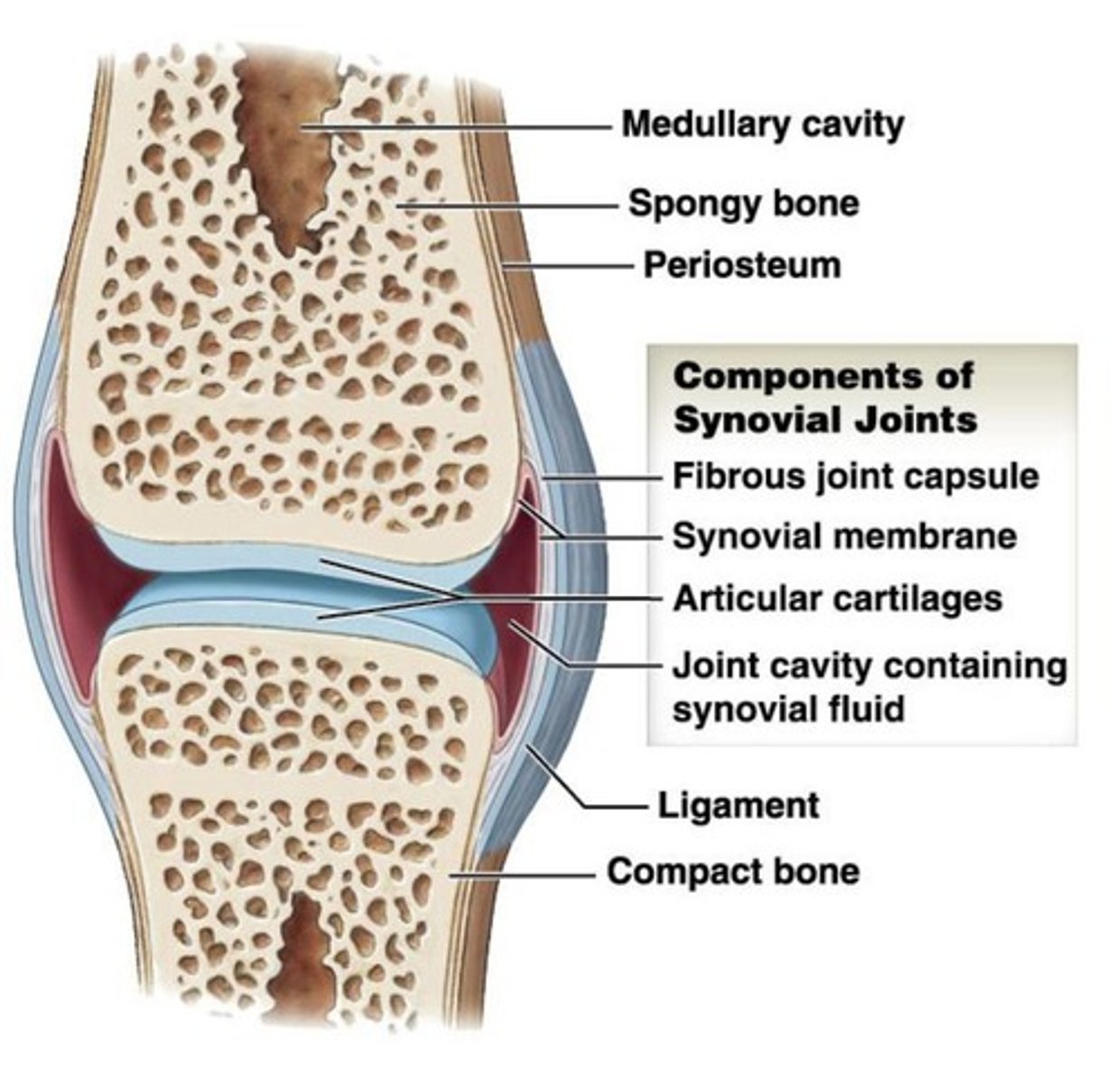
synovial joints
- are covered by articular cartilages and therefore are not in direct contact with one another.
- help reduce friction within the joint
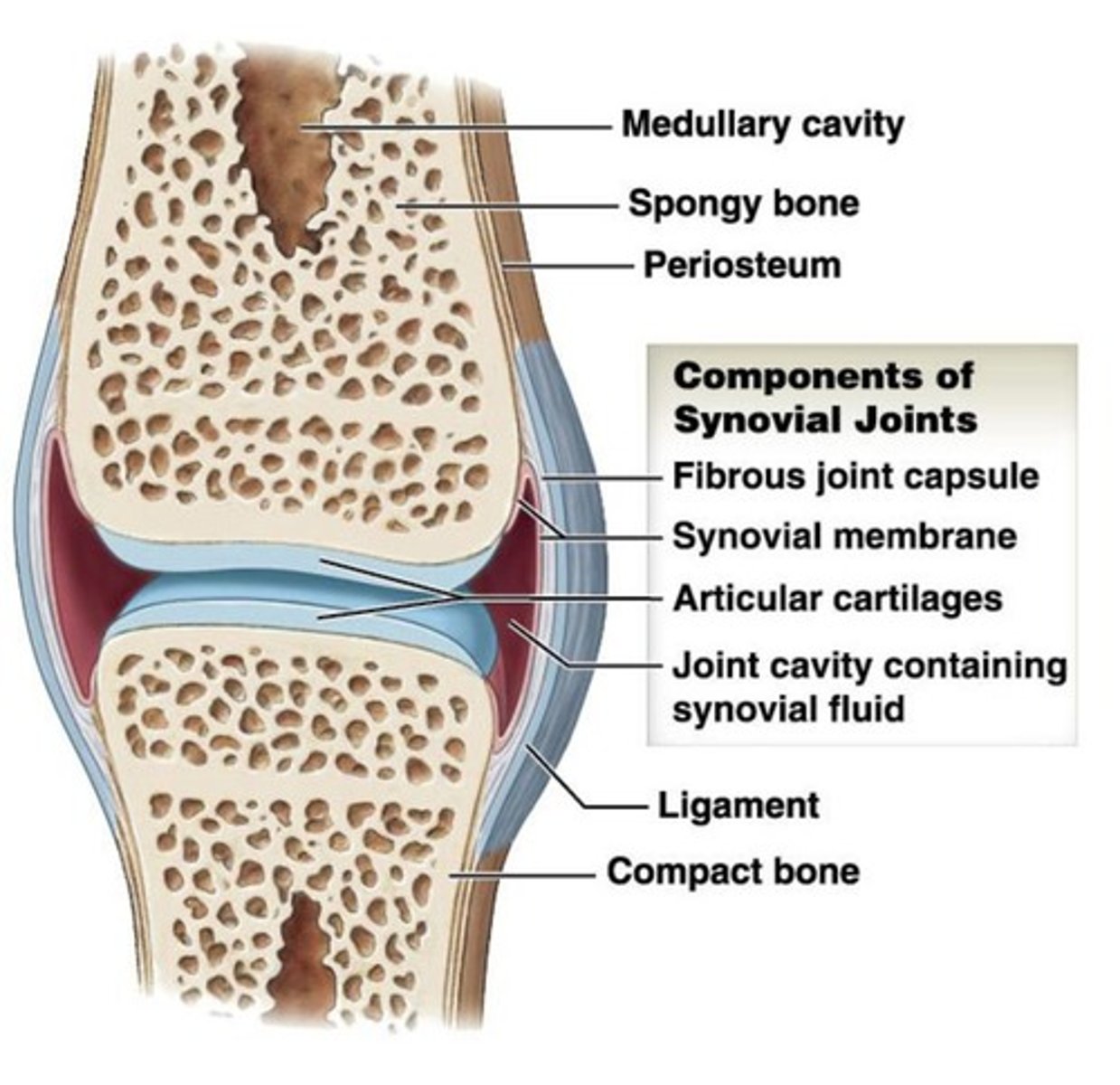
Synovial Fluid functions
- Lubrication and friction reduction
- Nutrient distribution
- Shock absorption
Ligaments
fibrous bands of tissue that connect bones or organs together. They are made of collagen, elastic fibers, and connective tissue.
Tendons
a fibrous connective tissue connecting bone to muscle allowing for movement by transmitting the force of muscle contraction to the skeletal system
Bursae
small, fluid-filled pockets in connective tissue that reduce friction and act as shock absorbers.
Strength vs Mobility in Joints
the more mobile a joint is then the weaker it is, stronger joints permits less movement
Abduction
is movement away from the longitudinal axis of the body in the frontal plane. (thing moving away from the body)
Adduction
towards the body
Flexion
is movement in the anterior-posterior plane that decreases the angle between the bones of the joint.
Extension
increases the angle between the bones of the joint
hyperextension
any movement in which a limb is extended beyond its normal limits, resulting in joint damage
circumduction
involves moving the arm in a circle, as when drawing a large circle on a chalkboard in one continuous motion
Rotation of head
left rotation or right rotation think shaking head
internal rotation (medial rotation)
anterior surface of the limb rotates inward, toward the anterior surface of the body
external rotation (lateral rotation)
turning outward
pronation
moves the wrist and hand from the palm-facing-front position to the palm-facing-back position.
supination
opposing movement of pronation
Special Movements
Special terms apply to specific joints or unusual types of movement
Eversion
motion of the foot that turns the sole outward
inversion
opposite of eversion
Dorsiflexion
movement of the foot towards the head, pointing foot up
Lateral flexion
the vertebral column bends to the side
Plantar flexion
pointing foot down, standing on tiptoes
Protraction
moving a part of the body anteriorly in the horizontal plane
Retraction
reverse movement of protraction
ex. returning jaw to normal position
Opposition
special movement of the thumb that produces pad-to-pad contact of the thumb with the palm or any other finger
Reposition
opposite movement that returns the thumb and fingers to their normal position
Elevation
structure moving in an inferior direction
Depression
structure moving in an superior direction
What is the orbit made of?
- frontal bone
- maxilla bone
- lacrimal bone
- ethmoid bone
- sphenoid bone
- zygomatic bone
Muscles anchored by hyoid bone
- tongue
- larynx
How many cervical vertebrae are there
7
how many thoracic vertebrae are there
12
how many lumbar vertebrae are there
5
How many sacral vertebrae are there
1
how many coccygeal vertebrae are there
1
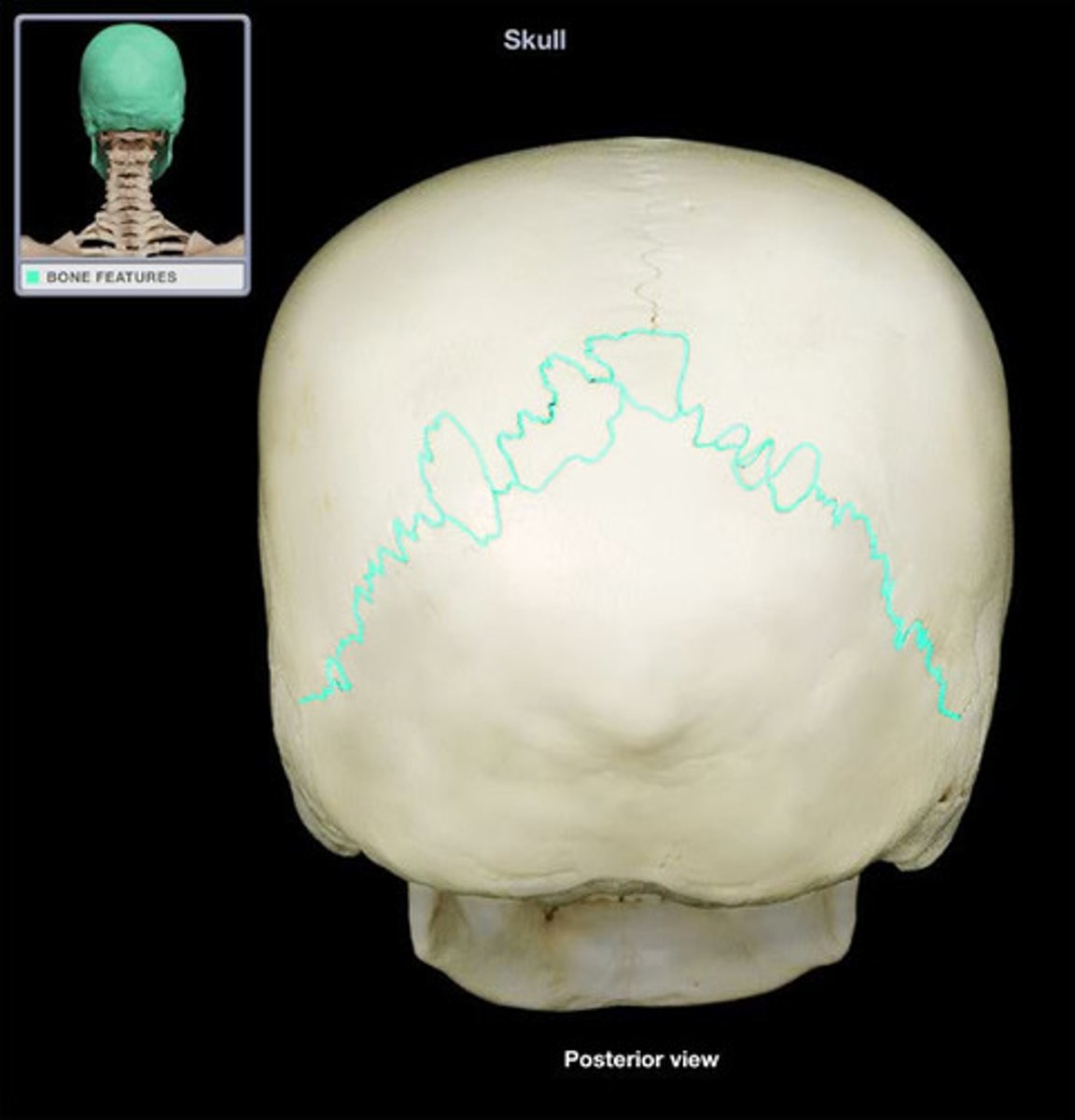
lambdoid suture
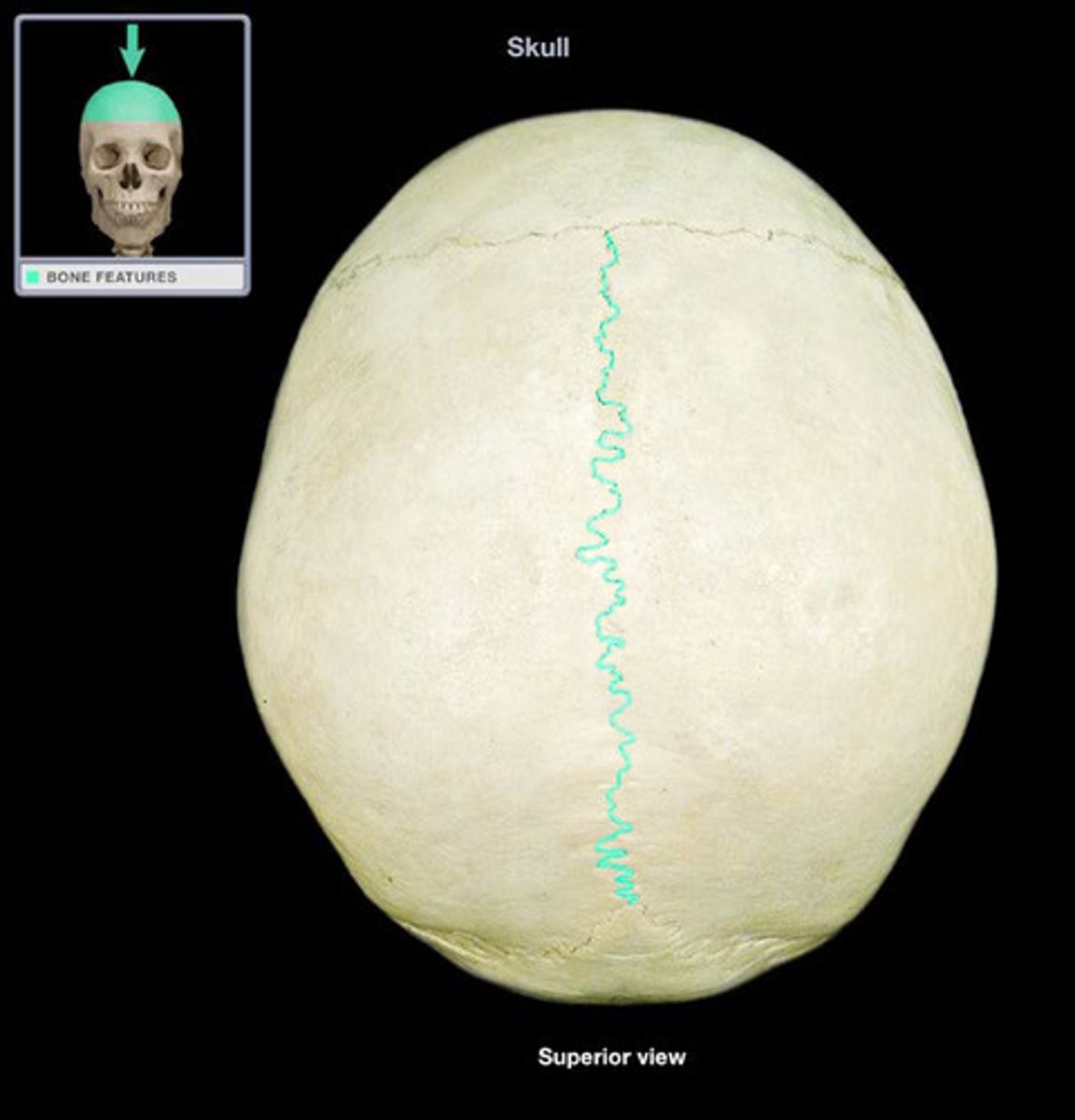
Sagittal suture
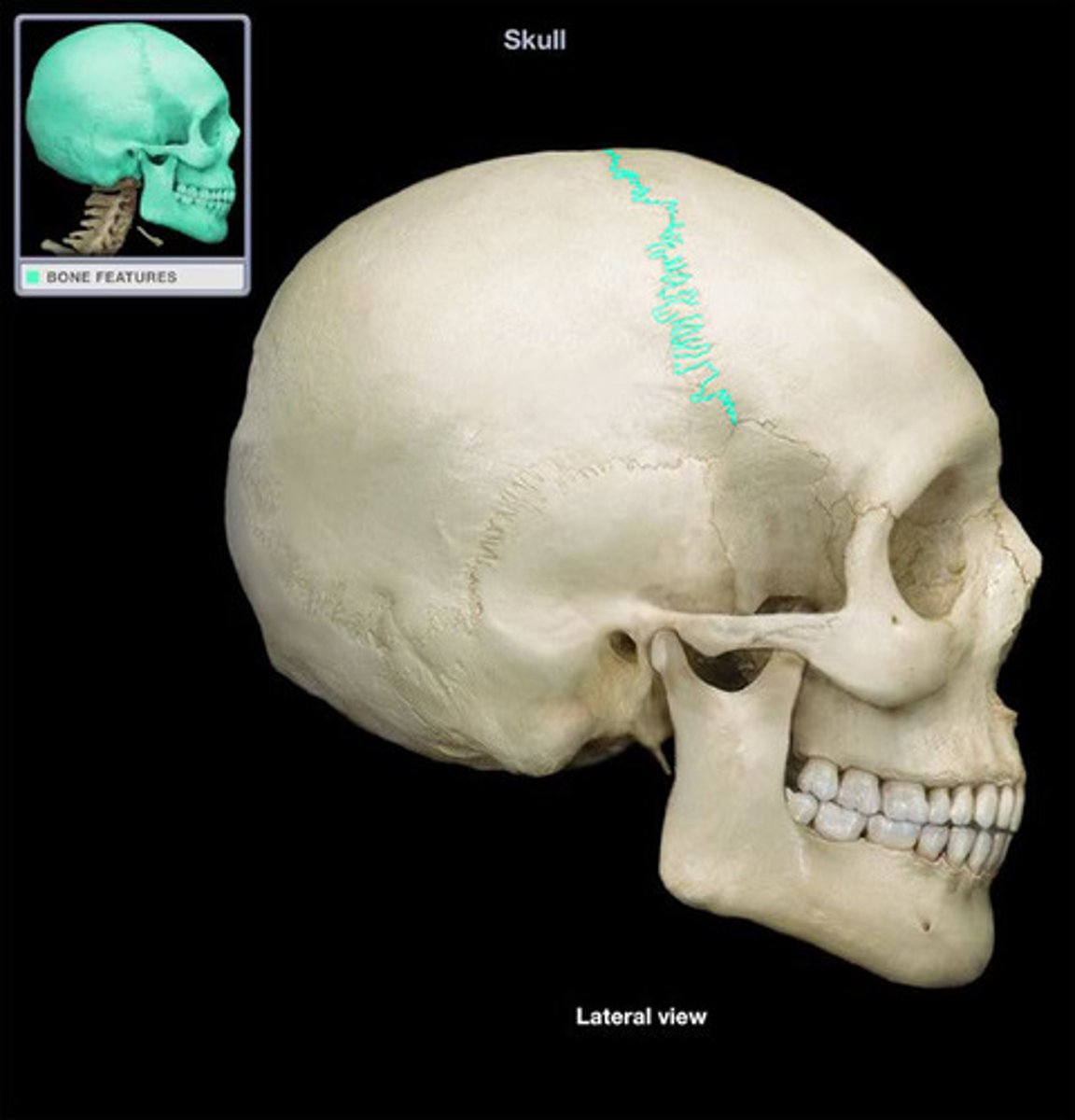
Coronal suture
Squamous suture
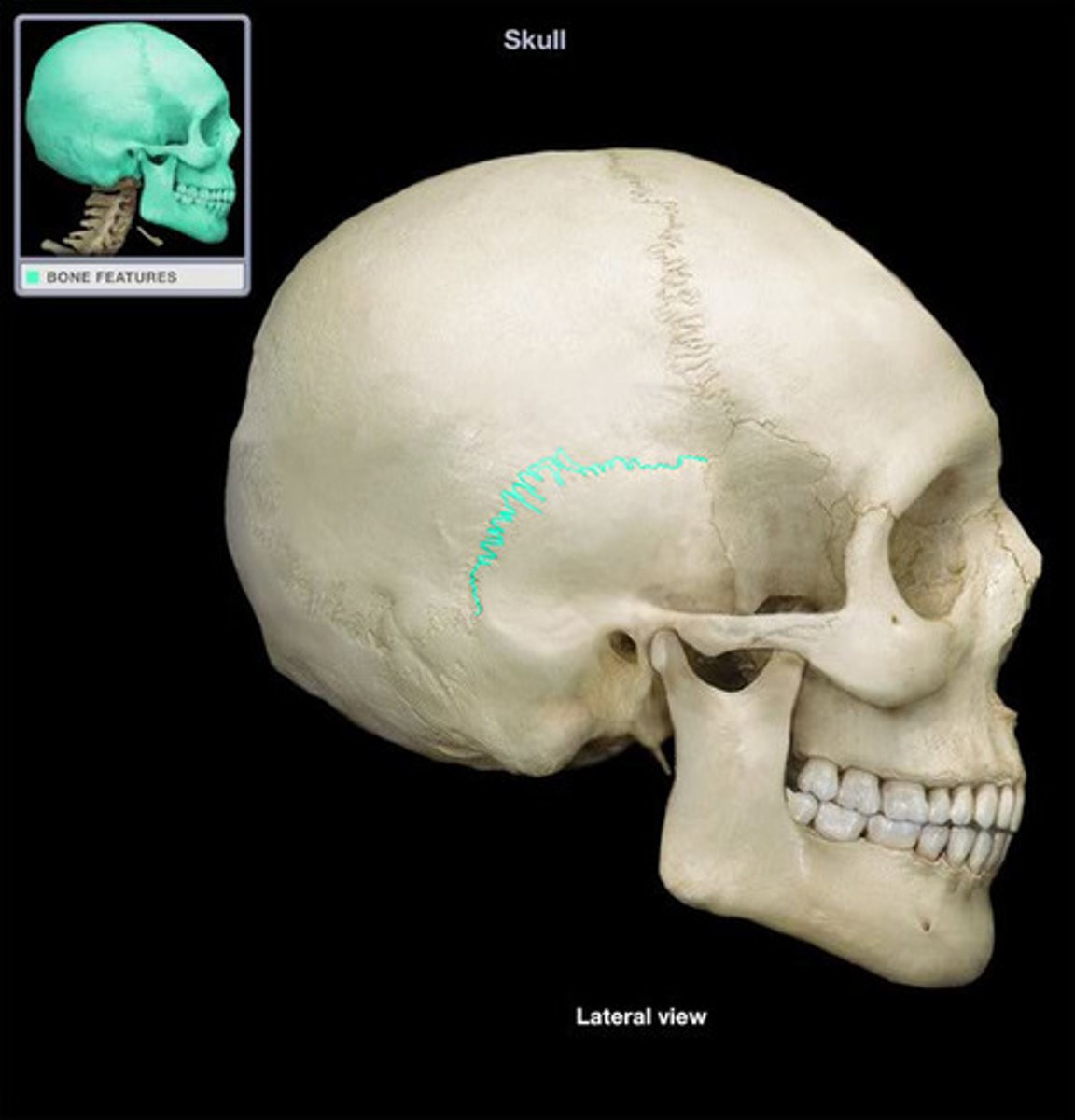
Frontonasal suture
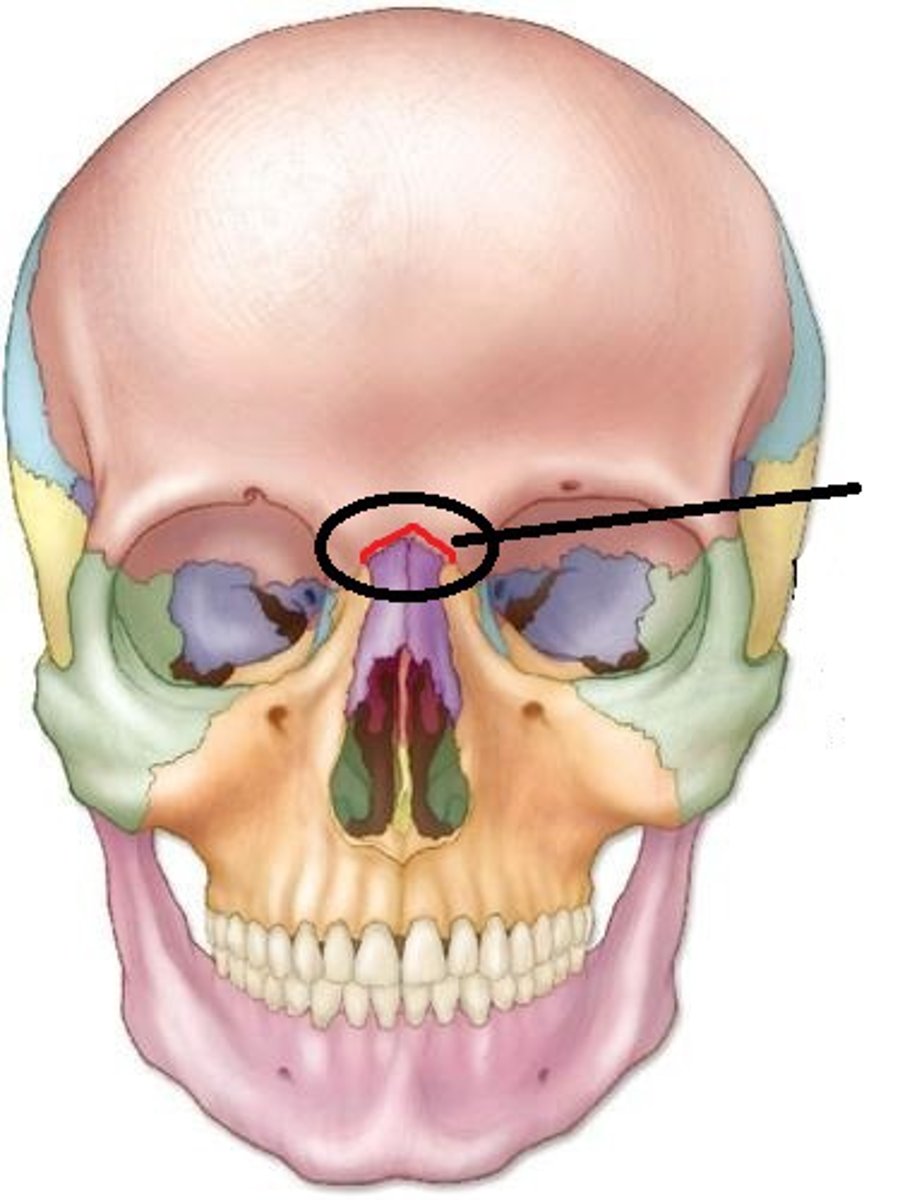
Maxilla Bone