Kines 350: Exam 5
1/73
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
74 Terms
what is an acid?
can liberate an H+
increases pH
what is a base?
can combine with H+
decreases pH
what is pH?
the potential or “power” of H+
neg log of H+
if 1x change in pH there is a 10x change in concentration
normal blood pH range
normal: 7.4 ± 0.05
acidosis: pH < 7.4
alkalosis: > 7.4
what is OBLA?
onset of blood lactate
4mmol/L lactate
low pH ______ Hgb affinity for O2
reduces
what is the origin of acid-base disturbances?
origin = the primary effect
respiratory or metabolic
Compensation will correct the disturbance (the other steps in)
what is VT2?
defines the severe intensity workout
denoted by hyperventilation (do to accumulation of acid in muscle → overventilation)
what senses the low oxygen, especially during high altitude environments?
peripheral chemoreceptors (like in carotid)
what is metabolic acidosis?
gaining acid through metabolic needs
long term starvation: ketone body accumulation
uncontrolled diabetes: diabetic ketoacidosis (ketone bodies)
high intensity exercise
what is metabolic alkalosis?
loss of acids from body
severe vomiting
kidney disease
prolonged hyperventilation at altitude
exrecise is a condition of _____-osis
acidosis
what are the sources of H+ during exercise?
volatile acids
production of CO2 (results in H+)
organic acids
what types of activities produce acid accumulation?
lasting greater/= 46 seconds
effort: at 100% increases risk, all-out sprint
how does acid-base status effect exercise?
inhibits enzymes in glycolysis, krebs, and oxphos
how are intracellular buffers buffered by extracellular systems
bicarbonate buffering system
Na+ - H+ exchanger and Lactate transporters; MCT
shift protons out of muscles
what is the henderson-hasselbach equation?
the buffering system for H+ ions, and the production of CO2
what is respiratory acidosis?
pH is low
high PCO2
ventilation: low
what is respiratory alkalosis?
the pH is too high
low PCO2
ventilation: high
what is metabolic acidosis?
pH is low
PCO2 is low: because protons coming form somewhere else stimulate ventilation
ventilation: compensates for acidosis (increases)
what is metabolic alkalosis?
high pH
PCO2: high
ventilation: low
how do the kidneys compensate for acidosis?
excess protons are secreted into the proximal convoluted tubule from blood
urinary protons combin with HCO3
CO2 is reabsorbed, ultimately increasing blood HCO3
what are the sources of H+ ions during exercise?
volatile acids
carb, fat, and protein metabolism, and the production of CO2 end product
organic acids
accumulation of products (i.e., glycolysis and lipid metabolism)
what type of acid is the biomarker for exercise acidosis?
organic acid
activities lasting ______ seconds can produce significant amounts of
≥45s
how does the acid-base balance impact performance?
increased [H+]
inhibits enzymes for glycolysis, krebs cycle, and oxphos
impairs muscle contractile process by competing with Ca2+ for troponin binding sites
what are the three lines of defense helping to maintain the acid-base balance
intracellular buffer systems
rapid (seconds)
blood buffer systems (cardiorespiratory compensation)
minutes (seconds-min)
renal
hours-days
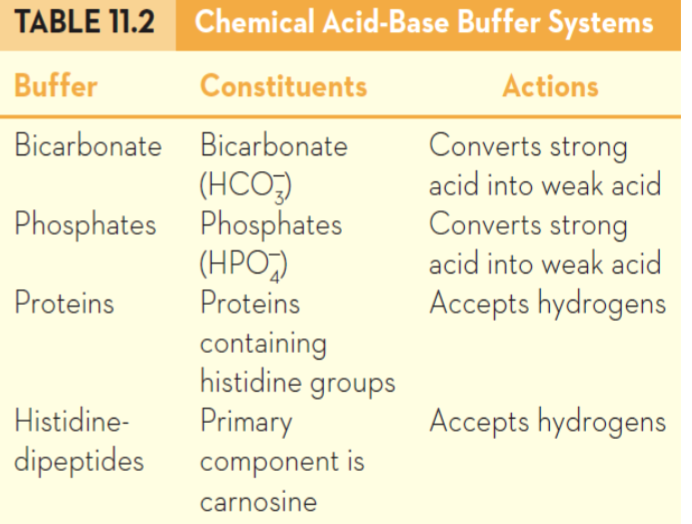
what are buffers, and what are the main intracellular and blood buffers?
Buffers release H+ ions when pH is high and accept H+ when pH is low
intracellular
proteins (carnosine) and bicarbonate
blood (extracellular)
bicarbonate and phosphates
how does fiber type impact intracellular buffer capacity
fast fibers (type II) possess a higher buffering capacity than slow (type I)
how does exercise training impact buffering capacity?
high intensity training improves buffer capacity in both trained and untrained
increases in both carnosine and hydrogen ion transporters
how are intracellular protons buffered by extracellular systems?
bacarb buffering
tansported by Na+ -H+ exchanger (NHE) and lactate transporters (monocarboxylate transporters; MCT)
shifts protons between intracellular and interstitial spaces
how does ventilation maintain acid-base balance
bicarbonate mostly
when [H+] increases → pH decreases and reaction moves left (more CO2)
↑ [H+] stimulates central chemoreceptors to ↑ ventilation
↑ CO2 released from longs, ↑ pH
what does H+ production during exercise depend on?
intensity
amount of muscle mass involved
duration
blood pH _____ with increasing intensity of exercise
declines
muscle pH ____ more dramatically than blood pH
declines
muscles have lower buffering capacity
how do the kidneys maintain the acid-base balance?
HCO3 is secreted by the glomeruli (cannot be directly reabsorbed)
converts to CO2 + H2O, then can be absorbed
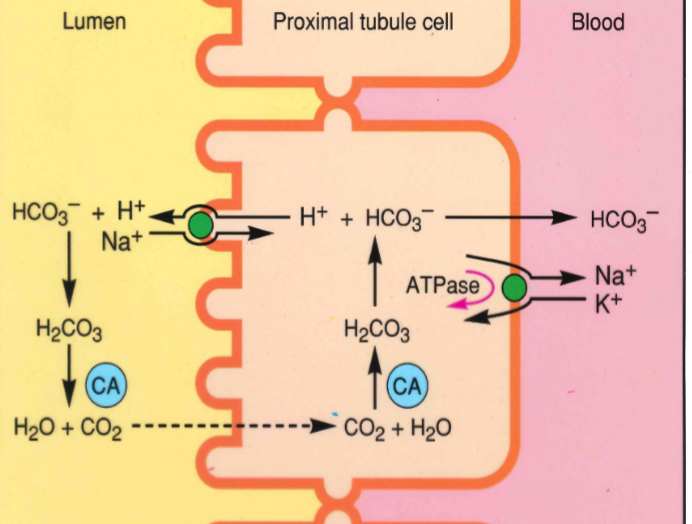
what occurs in the kidney during blood acidosis
excess protons are secreted into the PCT
urinary protons combine with HCO3
CO2 is reabsorbed, increasing blood HCO3
what happens in the kidney during blood alkalosis
excess HCO3 is secreted, less absorbed
restores in about 2-3 days
What is the combined gas law?
PV = nRT
described the relationship between temperature, pressure, volume and moles
what is daltons law?
total pressure is the sum of partial pressure
PP = concentration x total pressure
defines diffusion gradient for gas exchange
bound gases do not participate
why are partial pressures important in physiology
PP is the fraction of total (barometric) pressure that a gas exerts
PP = Fgas x Pbar
what is barometric pressure?
the sum of all partial pressures
PO2 + PCO2 + Pn2 = Pbar
what is the relationship with altitude and oxygen?
the percentage of O2 does not change, but since the air is thinner, the partial pressure is less
what is hyperoxic and hypoxic?
hyperoxic: Higher PO2 than sea level
>21% O2
hypoxic: lower PO2 than sea level
hypoxic hypoxia: breathing low FiO2 (fraction of inspired oxygen) gas at sea level
hypobaric hypoxia: breathing air while altitude
<21% O2
what are the ranges of altitude?
Adaptive range: 5000-11,500
Maladaptive range: 11,500 - 18,000
Death zone: >18,000
If hypoxia limits training, performance will suffer
what are the atmospheric conditions at high altitude?
lower atmospheric pressure
lower air density
lower PiO2
lower PH2O
lower air temperature
impacts thermoregulation
lower PH20 (dehydration)
more solar radiation
in general, what types of events benefit from atmospheric training?
sprinting
What is the relationship between VO2max and altitude
decreased at higher altitudes
about 1% decrease every 100m
low altitudes:
Decreased VO2max results from lower oxygen extraction
moderate altitudes:
decreased arterial PO2 contributes to reductions in VO2max
higher elevations:
max cardiac output is less
how does altitude impact submaximal exercise?
higher HR and CO
lower oxygen content of arterial blood
higher ventilation (stimulated by peripheral chemoreceptors)
increased lactic acid concentration in submaximal exercise
what is the lactate paradox?
with higher altitude, the lower peak lactate
a transient phenomenon
upon exposure: higher HR, ventilation, and lactate during exercise
after 4+ weeks: glycolytic capacity recovers, lactate response recovers
likely people are just failing and quitting, they are at lower workload
what are the strategies to compete at altitude?
get in, get out
arrive ASAP before competing and leave ASAP
acclimate for at least 2 wks, preferably 6
reduce intensity to 60-70% normal
work up to full intensity over 2 weeks
may be incorporated in taper
what are the adaptations for residents at altitude?
have complete adaptations in arterial O2 and VO2max (usually have one or the other
produce more RBC: higher hemoglobin concentration (counters desaturation by low PO2)
Greater oxygen saturation: greater pulmonary blood flow (increased ventilation)
What is acclimation?
prolonged exposure
blood adaptations:
erythropoietin stimulates RBC production
muscle:
decrease fiber areas (20-25%)
decrease krebs cycle enzymes (20-50%)
cardiorespiratory:
chronic exposure >2,500m/8,000 generally does not increase VO2max
metabolic
shift toward CHO metabolism
what is HIF (hypoxia-inducible factor) pathways?
hypoxia is main stimulus for HIF
it binds to a protein
portion of DNA transcription activated
leads to genes beneficial for endurance exercise
erythropoiesis
angiogenesis
more glycolytic enzymes
more vasodilation
but inhibits mTOR
what is the optimal hypoxic prescription?
frequency: at least 22hr/day
intensity: altitude 2300±200m
time: 4wks
type: consider either method to create hypoxia and maintaining high quality exercise training
live high train low
what is the main takeaway of the live high, train low study?
that hypoxia does seem to have a little positive impact
But likely that elite athletes training with elite athletes pushed each other for improvement
what are the mechanisms for performance in hypoxic environments
blood
increased RBC (increased O2 transport)
non-blood (muscle)
increased efficiency of mitochondrial metabolism (decrease O2 used at fixed rate)
what are the challenges of high altitude climbing?
dont have particularly high VO2max
altitude sickness: loss of appetite, weight loss reduced type I and type II muscle fiber size
successful climbers: great capacity for hyperventilation (increases alveolar PO2)
acid-base considerations of altitude acclimation
early exposure stimulates peripheral chemoreceptors, causes hyperventilation
increased ventilation and PAO2
increased PACO2
Respiratory alkalosis develops in minutes (from hyperventilation)
reduces stimulation of central chemoreceptors
may contribute to mountain sickness
over days: urinary excretion of excess HCO3 helps restore acid base status
what are the medical problems with living and working at altitiude?
polycythemia: excessive EPO response, increases blood viscosity
acute mountain sickness (ASM)
high altitude pulmonary edema: accumulation of fluid in lungs
high altitude cerebral edema (HACE): accumulation of fluid in cranial cavity
what is acute mountain sickness (AMS)
headaches, loss of appetite, nausea, vomiting
cheyne-stokes breathing: sleep disturbances, CO2 accumulation (periodic)
treated: DESCEND ASAP
golden rules of altitude sickness
rule 1:
if you are ill at altitude, your symptoms are altitude sickness otherwise
rule 2:
if you have symptoms, do not go higher
rule 3:
if you are feeling ill or getting worse, or cannot walk heel to toe in a straight line, or have SOB at rest, descend
rule 4:
person with altitude sickness should always be accompianied
what are homeotherms?
we as humans can maintain a constant core temperature
about 37 C
< 34 and > 45 BAD
what is the thermal gradient
ideal gradient is about 4 C
distal portions cooler than core temperature
what is the heat balance equation
loss/gain = metabolism ± conduction ± evaporation ± convection ± radiation
can be modeled to determine the magnitude of gain or loss
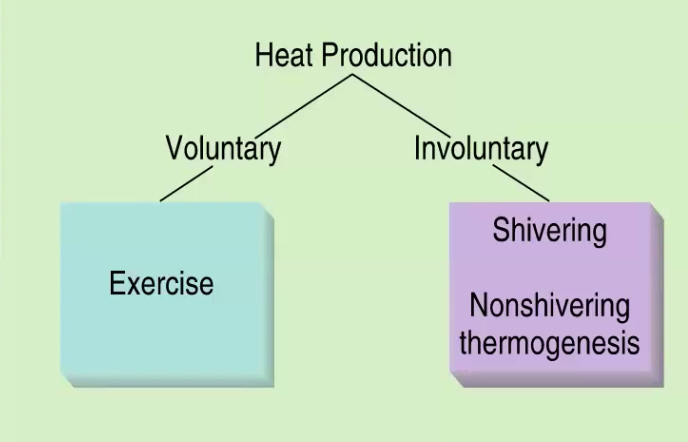
what is heat production by metabolism
voluntary
exercise
involuntary
shivering
thyroxine
catecholamines
conduction mechanism of heat gain and loss
transfer of body heat by direct contact
convection mechanism of heat gain and loss
transfer of heat by motion of molecules at the surface of the skin
disruption of boundary layer
radiation mechanism of heat gain and loss
infrared emission to or from a body (like radiating heat)
primary mechanisms for heat loss at rest
evaporation mechanism of heat gain and loss
heat lost with water conversion from liquid to vapor
primary avenue of heat loss during exercise
biggest in heat loss
how does evaporation and condensation regulate body heat?
The conversion of water (sweat) from liquid to gas
requires a pressure gradient between skin and air (not wet air)
Evaporation rate depends on:
temperature and relative humidity
convective currents around the body
SA of skin exposed
Responsible for more than 60% of heat loss
what modes can you expect to see heat losses?
conduction: heat loss due to contact with another surface
convection: heat transferred to air or water
radiation: biggest for at rest
how does body heat balance during graded exercise?
an increase in body temperature is related to exercise intensity
mechanisms of heat loss
evaporation:
convection and radiation
what are the thermal events during graded exercise?
as exercise intensity increases
heat production increases
linear increase in body temperature
higher net heat loss
as ambient temperature increases
heat production is constant
lower convective and radiant heat loss
higher evaporative loss
as humidity increases
heat production remains constant
similar convective and radiant heat loss
lower evaporative heat loss