Clin Path Unit 5 pt 2
1/117
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
118 Terms
What are the four primary anatomical components of the urinary system?
Two kidneys, two ureters, the urinary bladder, and the urethra.
What is the sequence of the four stages of urine formation?
1. Glomerular filtration, 2. Tubular reabsorption, 3. Tubular secretion, 4. Micturition.
Which molecular characteristics restrict the passage of substances through the glomerular filter?
Large molecular size, heavy weight, and a negative electrical charge.
In what anatomical structure do substances collect immediately after glomerular filtration before passing into the renal tubule?
Bowmans capsule.
What is the primary function of tubular reabsorption in maintaining homeostasis?
The conservation and return of needed substances to the bloodstream.
How is tubular secretion defined in the context of renal physiology?
The transfer of substances from the peritubular capillaries into the renal tubules.
What is the mathematical definition of Specific Gravity (SG) in urinalysis?
The ratio of the weight of urine to the weight of an equal volume of distilled water.
What is the specific gravity value of distilled water?
1.000.
How does the process of concentrated urine formation affect specific gravity?
It increases specific gravity by removing water through tubular reabsorption, leaving more solute.
What is the specific gravity range for isosthenuria?
1.008 to 1.012.
What physical condition does isosthenuria indicate regarding kidney function?
The urine has a specific gravity equal to plasma or the glomerular filtrate.
Which two hormones are primary factors in influencing urinary output volume?
Antidiuretic Hormone (ADH) and Aldosterone.
What are the three primary components of the internal anatomy of the kidney as seen in a sagittal section?
Cortex, medulla, and renal pelvis.
What does GFR stand for in the context of renal blood flow evaluation?
Glomerular Filtration Rate.
Which three non-protein nitrogens (NPNs) are commonly measured in blood chemistry to assess kidney function?
Blood Urea Nitrogen (BUN), Creatinine, and SDMA.
What is the clinical significance of Symmetric Dimethylarginine (SDMA) compared to BUN/Creatinine?
It is used for the early detection of renal dysfunction.
Which species requires uric acid measurement as the primary indicator of renal function?
Avian species (birds).
Why are Dalmatians predisposed to uric acid crystals?
They have a genetic defect that blocks the conversion of uric acid.
What is the procedure for a Phenolsulfonphthalein (PSP) dye clearance test?
Inject the dye IV and withdraw blood after a set time to measure the remaining dye concentration.
What percentage of nephrons must be nonfunctional before elevated waste levels are typically detected in standard blood chemistry?
(75%) of nephrons.
How is 'Azotemia' defined?
The buildup of urea and other nitrogenous wastes in the blood.
How does 'Uremia' differ from simple Azotemia?
Uremia is a toxic condition resulting from the accumulation of urea in the blood, often signaling renal failure.
What is the pathological difference between nephritis and nephrosis?
Nephritis is inflammatory; nephrosis is a non-inflammatory degeneration of tubules (often from toxins).
What fraction of damaged nephrons defines 'renal failure' or renal insufficiency?
2/3 to 3/4 of the total nephron population in both kidneys.
What are the three classifications of Uremia based on its cause?
Pre-renal, Renal, and Post-renal.
Why is urolithiasis considered more common in male animals?
Males have a longer and narrower urethra, making obstruction by stones more likely.
Which two crystal types are most commonly associated with Feline Lower Urinary Tract Disease (FLUTD)?
Struvite and calcium oxalate.
What are the two hallmark clinical signs of cystitis mentioned in the source material?
Dysuria (painful urination) and hematuria (blood in urine).
What is the ideal urine sample for diagnostic testing?
The first morning sample collected mid-stream.
What is the recommended storage procedure if a urine sample cannot be tested within 30 minutes?
Refrigerate the sample and bring it to room temperature before testing.
What are the three essential components of a complete urinalysis evaluation?
1. Physical examination, 2. Chemical examination, 3. Microscopic examination.
What is the minimum volume of urine preferred for a complete urinalysis?
10 mL.
What are the five parameters assessed during the physical examination of urine?
Volume, color, transparency, odor, and specific gravity.
What is the normal urine output volume for an adult dog?
20 to 40 mL/kg of body weight per 24-hour period.
What is the normal urine output volume for an adult cat?
28 mL/kg of body weight per 24-hour period.
Define 'Polyuria'.
The formation and elimination of an abnormally large volume of urine.
Define 'Pollakiuria'.
Frequent urination, typically characterized by small amounts of urine released at each instance.
What are two potential causes for Oliguria?
Fever, shock, dehydration, or high environmental temperatures.
Why is 'Anuria' in a male cat considered a medical emergency?
Obstruction prevents urine elimination, leading to potential kidney damage from back-pressure.
Which two pigments are responsible for the normal light yellow to amber color of urine?
Urochrome and Urobilin.
What does green-brown or yellow-brown urine typically indicate?
The presence of bile pigments.
Red or reddish-brown urine is a clinical sign of which three possible conditions?
Hematuria, hemoglobinuria, or myoglobinuria.
How should the color of urine be evaluated to ensure accuracy?
Hold the sample up against a white piece of paper.
What term describes urine with large particles visible to the naked eye, resembling a 'snow globe'?
Flocculent.
A sweet or fruity odor in urine is a clinical indicator of what substance?
Ketones (likely associated with diabetes).
What is the most accurate tool for measuring urine specific gravity in a clinical setting?
A refractometer.
Under what condition will urine appear pale but have a high specific gravity?
Diabetes mellitus.
What calculation is performed when a urine specific gravity is 'off the scale' of the refractometer?
Dilute with equal parts distilled water, then multiply the last two digits of the new reading by two.
Why should reagent strips not be used to determine urine specific gravity?
They are extremely inaccurate for this specific parameter.
What is the standard pH range classification for urine?
Acidic is below 7, Alkaline is above 7, and Neutral is exactly 7.
What effect does leaving a urine sample at room temperature for an extended period have on pH?
The urine becomes increasingly alkaline.
What happens to White Blood Cells (WBCs) and Red Blood Cells (RBCs) in highly alkaline urine?
They tend to dissolve or lyse.
What is the normal range for protein in a urine sample?
Absent or trace amounts (1 to 30 mg/dL).
What is 'transient proteinuria'?
A temporary increase in urine protein due to exercise, stress, or high-protein meals.
What specific reagent is used in a turbidity test to detect protein in urine?
Sulfosalicylic acid reagent.
What is the renal threshold for glucose in dogs?
180 mg/dL.
Define 'renal glucosuria'.
Glucose in the urine despite normal blood glucose, indicating a failure of the renal tubules to reabsorb it.
Ketonuria is often associated with which life stages in livestock?
Lactating cows and pregnant ewes (ketosis).
In which species is bilirubinuria always considered abnormal?
Cats, pigs, sheep, and horses.
What precaution must be taken when handling urine samples suspected of containing bile pigments?
Protect the sample from light.
What is the difference between 'hematuria' and 'occult hematuria'?
Hematuria causes visible color change; occult hematuria contains RBCs but no visible color change.
How can a technician differentiate between hematuria and true hemoglobinuria using centrifugation?
After centrifugation, hematuria results in a clear supernatant and red pellet; hemoglobinuria maintains red supernatant/plasma.
What is the cause of 'ghost cells' in a urine sediment exam?
Dilute urine causes Red Blood Cells to lyse and release their hemoglobin, leaving only the membrane.
What is the origin of myoglobin in the urine?
Muscle protein released following severe muscle damage or overexertion.
Why is the nitrite block on a reagent strip considered unreliable in animals?
Positive results require dietary nitrate and significant bladder incubation time, leading to false negatives.
What are the standard settings for centrifuging a urine sample for sediment analysis?
3 to 5 minutes at 1000 to 1500 rpm.
How is urine sediment typically viewed under a microscope for identification and counting?
Scan on 10x for casts, then identify and count cells/crystals on 40x/45x in 10 fields.
What is considered the 'normal' amount of RBCs and WBCs per high-power field (hpf) in urine?
Less than 5/hpf.
Which epithelial cell is the largest and originates from the vagina, vulva, or prepuce?
Squamous epithelial cell.
What do increased numbers of transitional epithelial cells indicate?
Pyelonephritis or cystitis.
What does the presence of renal epithelial cells in urine sediment indicate?
Renal tubule disease.
How is 'pyuria' defined?
An excessive number of White Blood Cells in the urine.
What specific protein forms the matrix of all urinary casts?
Tamm-Horsfall protein (secreted by renal epithelial cells).
Which type of cast is considered the 'basic protein cast' and can be seen after exercise or stress?
Hyaline cast.
What is the clinical significance of a waxy cast?
It represents the final stage of cast degeneration and indicates chronic, severe damage to renal tubules.
How can a technician differentiate between fat droplets and RBCs in urine sediment?
Apply Sudan III stain; fat droplets will appear orange or red.
Which crystal is described as having a 'coffin lid' appearance?
Struvite (Triple Phosphate).
The 'back of an envelope' appearance is characteristic of which crystal?
Calcium oxalate dihydrate.
The presence of calcium oxalate monohydrate crystals is a hallmark of what condition?
Antifreeze (ethylene glycol) poisoning.
Which crystal is 6-sided, hexagonal, and indicates renal tubular dysfunction?
Cystine crystal.
What crystal type is commonly found in the alkaline urine of horses and rabbits?
Calcium carbonate.
What type of sediment resembles folding ribbons and is common in equine urine?
Mucus threads.
How are yeast cells identified in a urine microscopic exam?
They appear as colorless, ovoid structures, often showing 'budding' and double refractive walls.
What is the common name for the bladder worm of the dog and cat?
Capillaria plica.
Which parasite is known as the 'Giant Kidney Worm' of dogs?
Dioctophyma renale.
What is the standard reporting method for crystals and bacteria in a urinalysis report?
Categorized as few, moderate, or many.
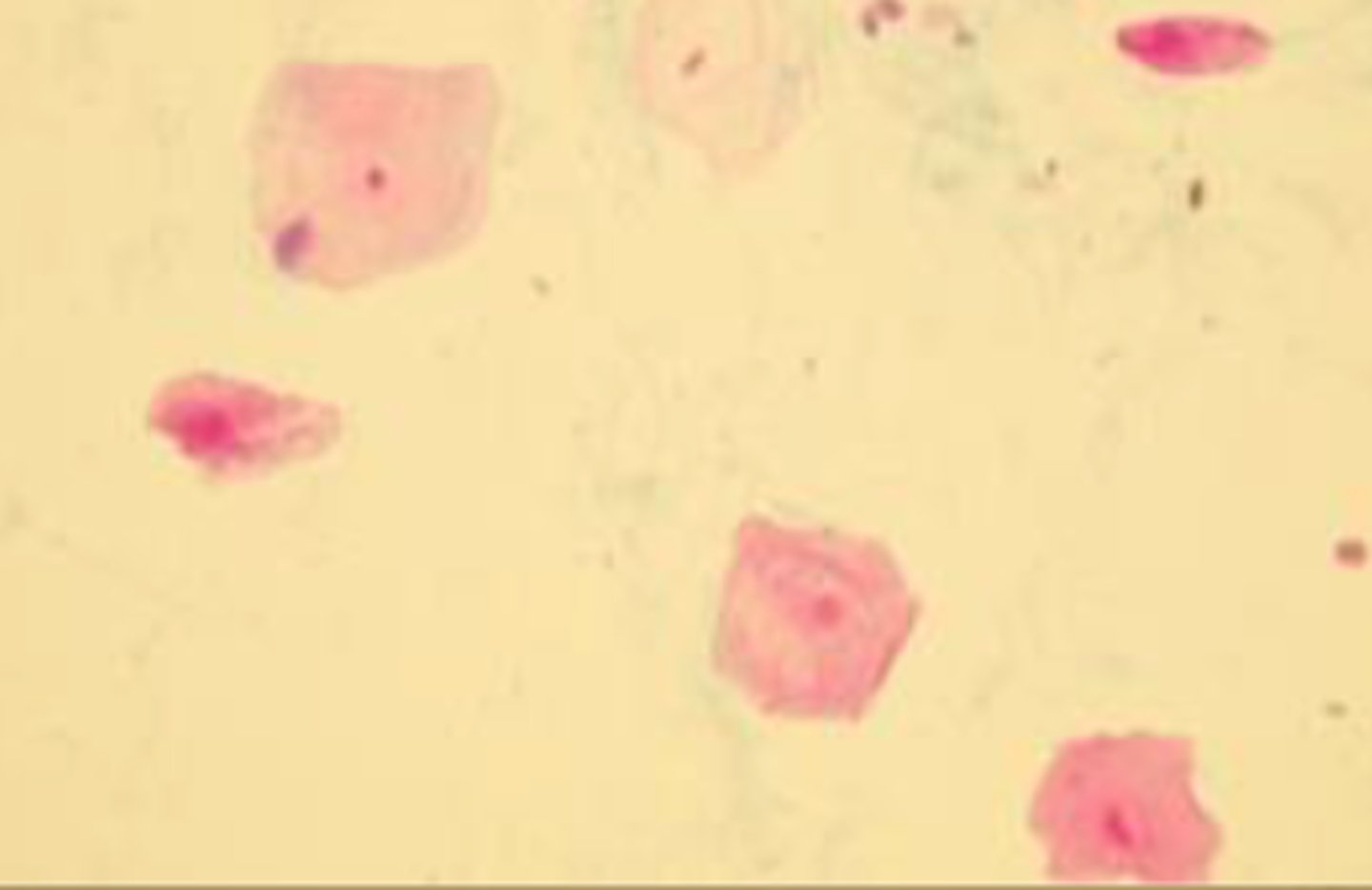
Squamous epithelial cells
- Originates from vagina, vulva or prepuce
- Distal urinary system
- Largest epithelial cells
- Flat, irregular shaped, small round nucleus
- Not a significant finding
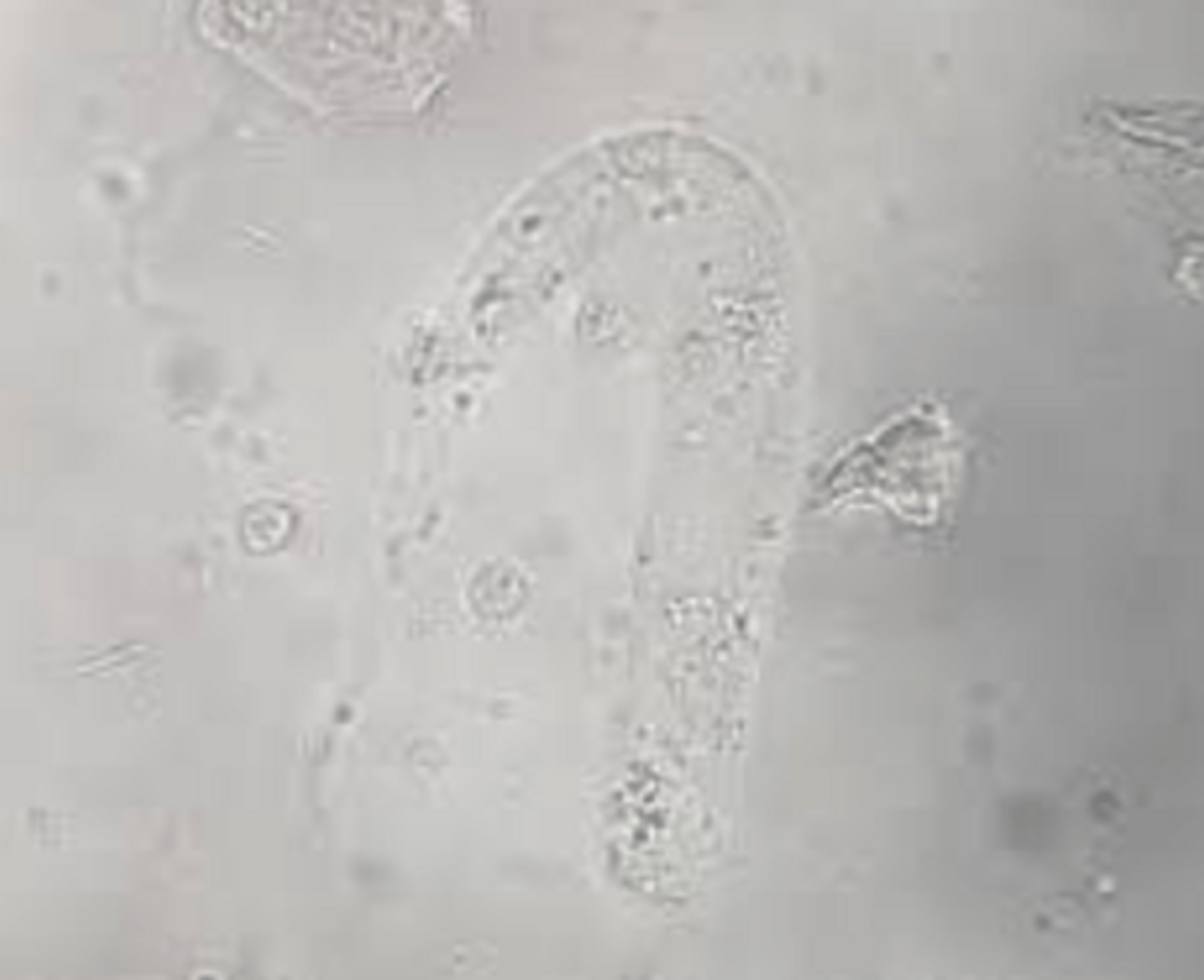
Transitional epithelial cells
- Originates from bladder, ureters, renal pelvis, or proximal urethra
- Round or pear shaped
- Granular appearance
- Larger nucleus
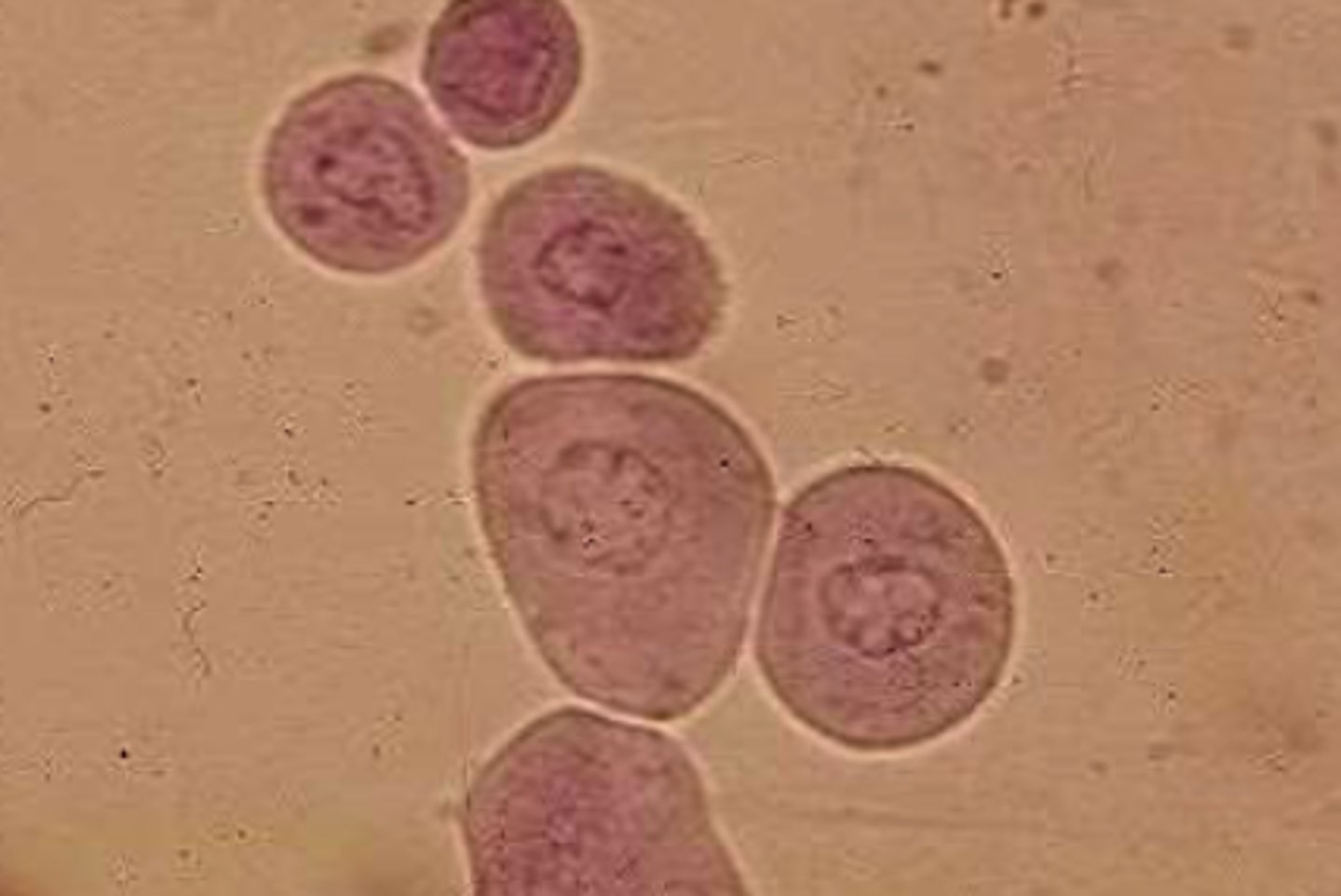
Renal epithelial cells
- Normal to see 0-1 in each field
- Increased number indicates cystitis, pyelonephritis, or renal tubule disease
- Come from kidneys
- Smaller than other cells but slightly larger than WBCs
- Large, round nucleus
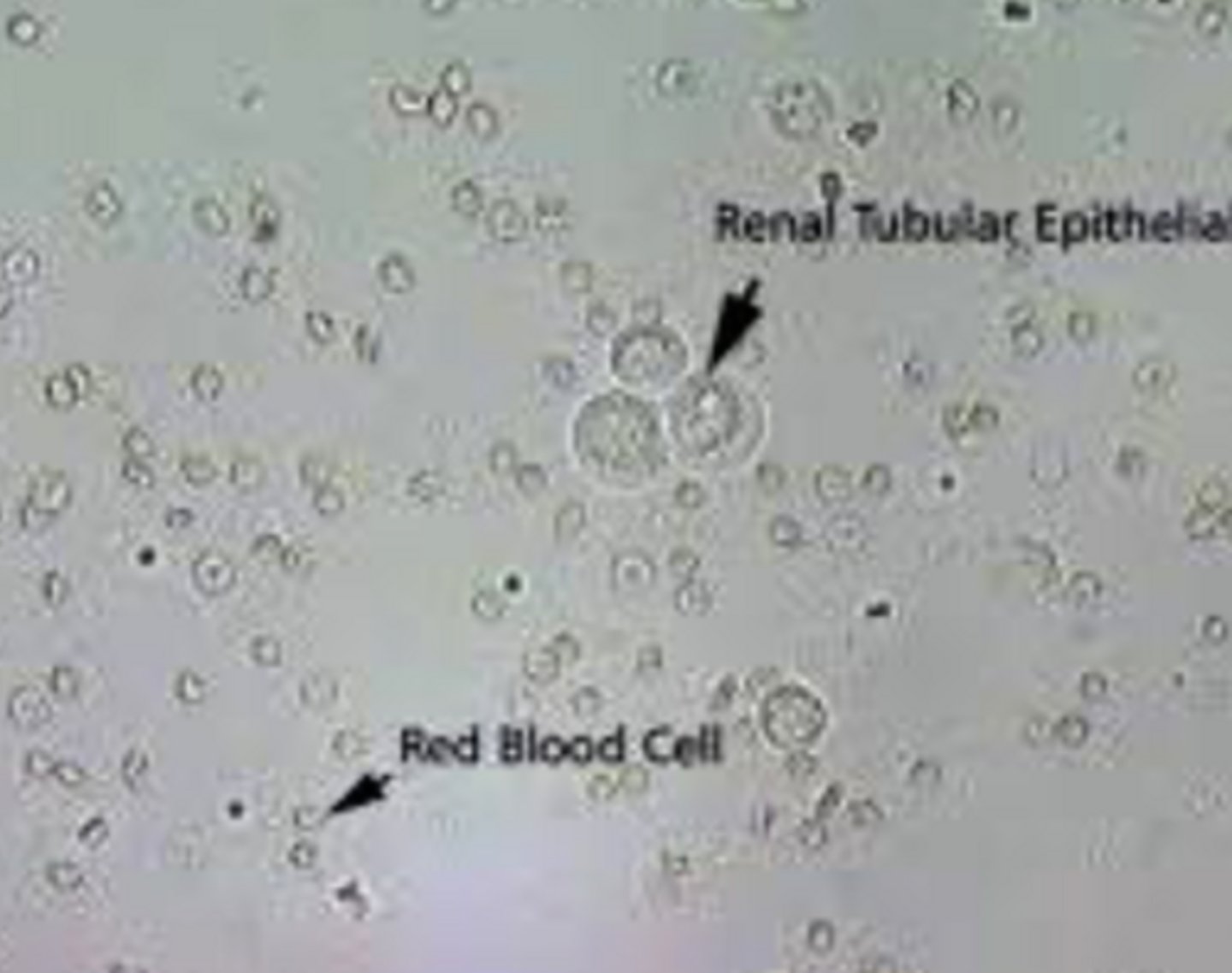
Bacteria
- Small amount seen in free catch
- Should see none in cysto or catheterization
- Look for background movement
- Rods or cocci
- Identify on high dry
- Indicates UTI
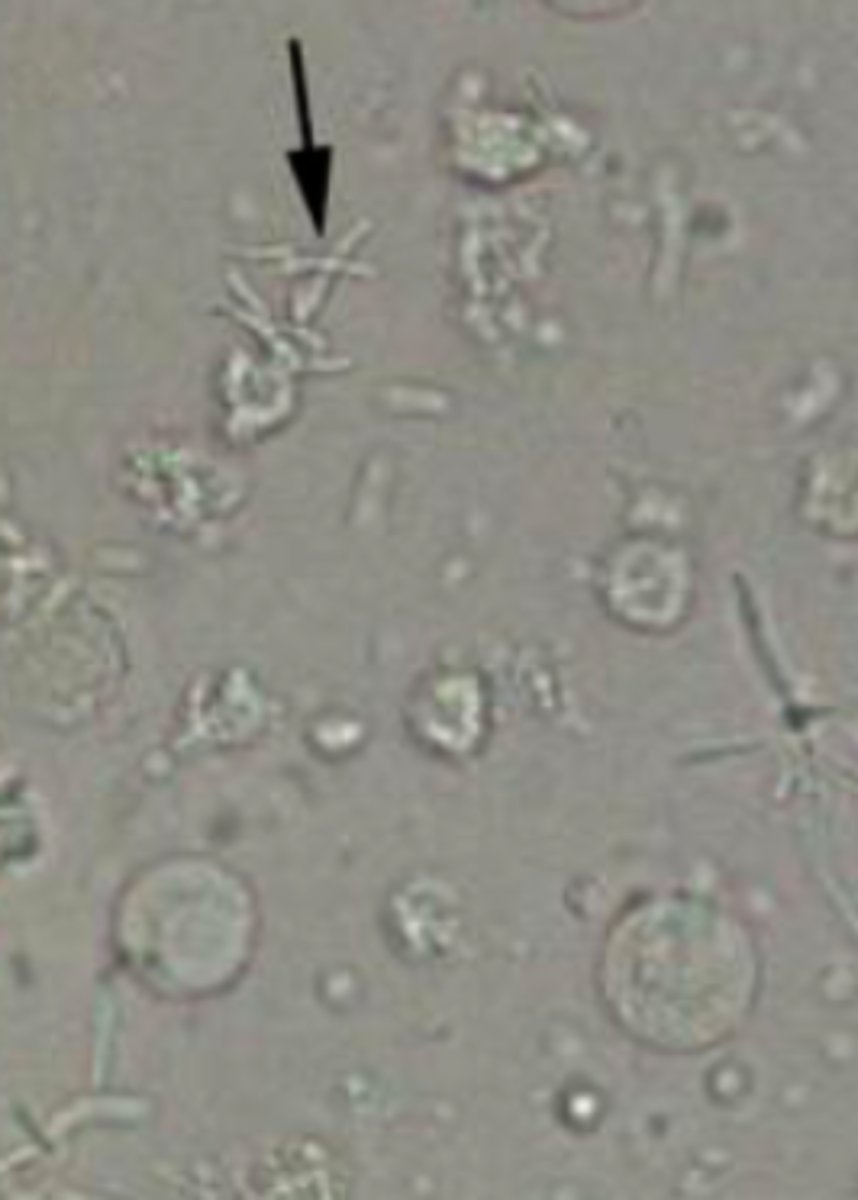
Yeast
- Rare
- Colorless, oval, double refractile walls
- Often confused with RBCs or lipids
- Caused by contamination
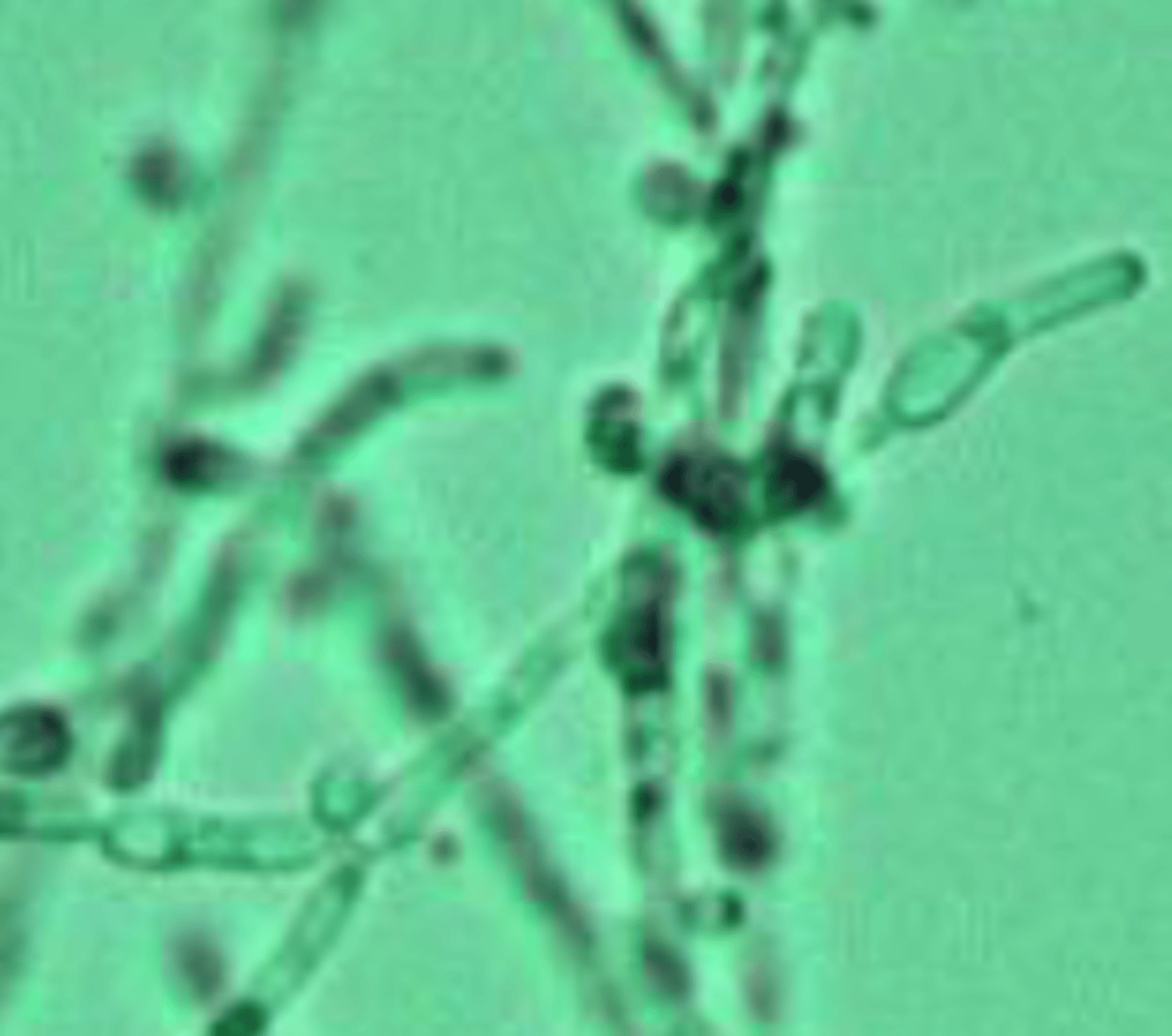
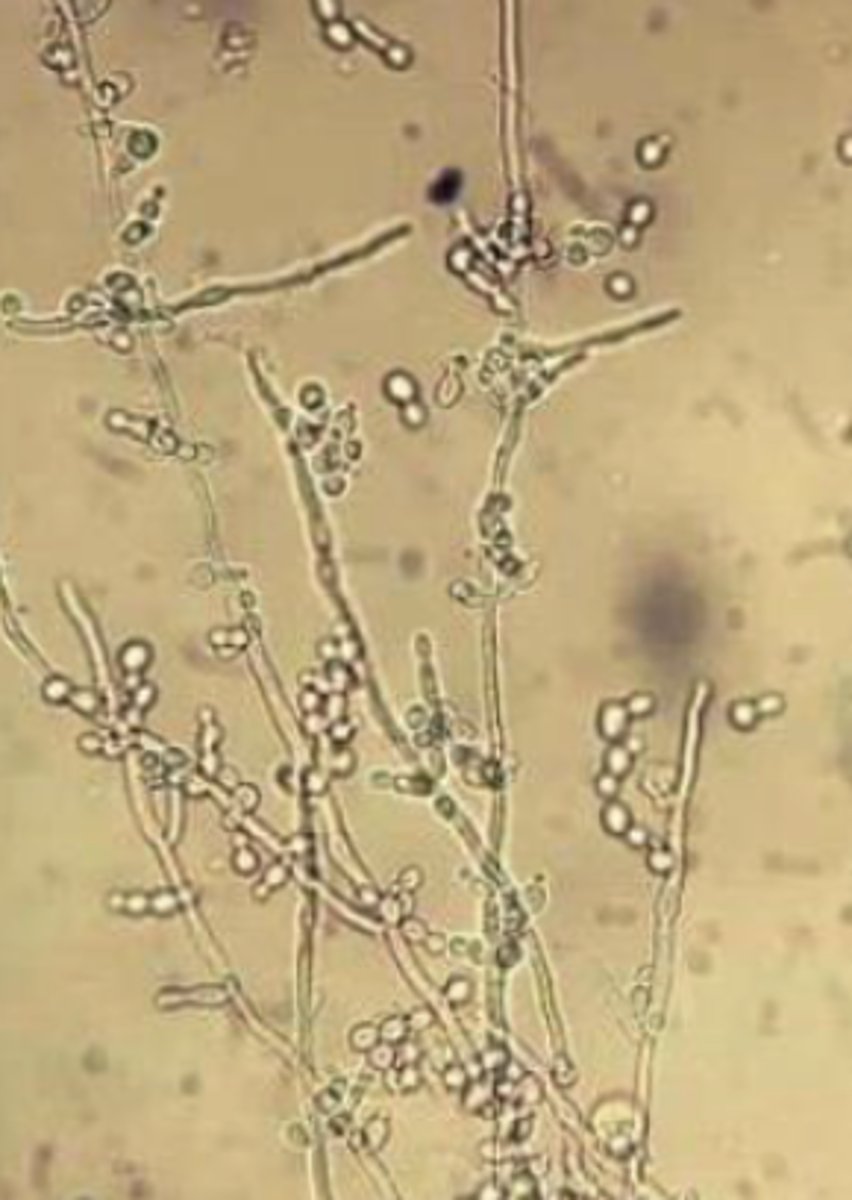
Fungi
- Rare
- Hyphae (branches)
- Very serious -- let doctor know immediately
Hyaline casts
- Most basic
- Clear, colorless, and highly refractile
- Parallel sides and rounded ends
- Can be easily obscured if light is up too high (have dim light)
- Low numbers are normal
- Seen with exercise or stress
Granular casts
- Most commonly seen
- Due to degeneration of renal epithelial casts or WBC casts
- Course or fine
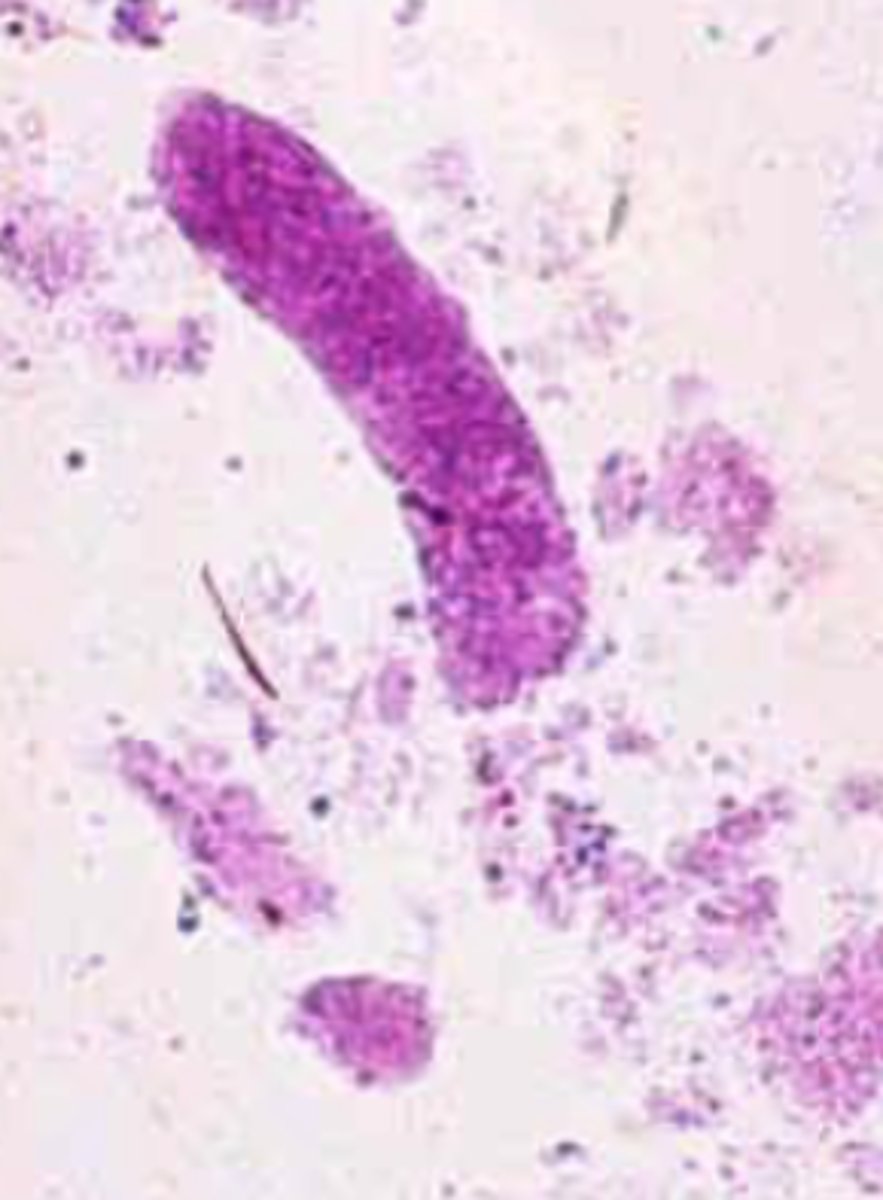
Epithelial cell casts
- Picked up from cell walls or tubule walls
- Stay in tubules long enough → degenerates into coarse granular cast then fine granular cast
- Indicates renal cell necrosis or tubular damage
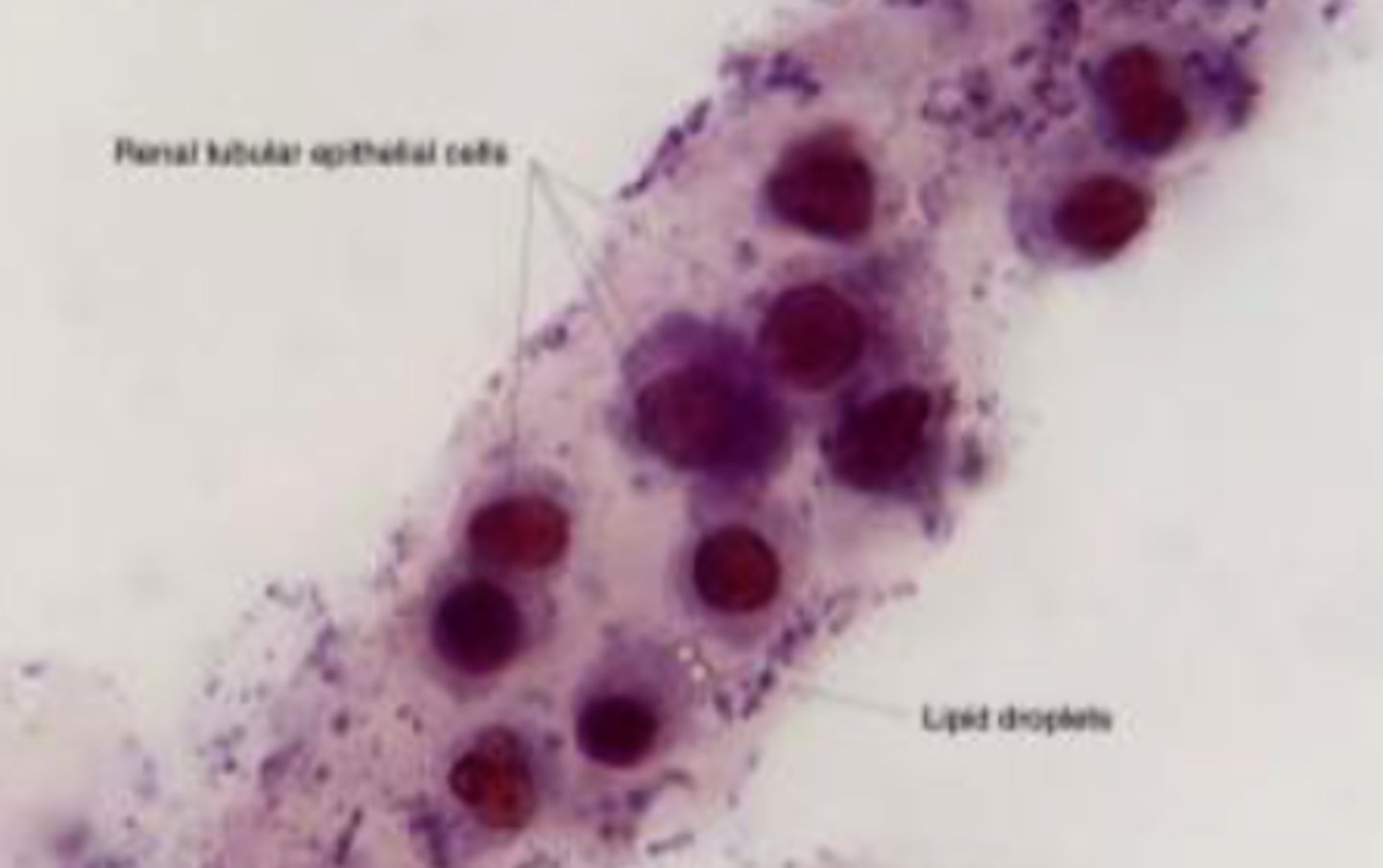
RBC/erythrocyte casts
- Appear yellow/orange color
- Stained - purple/pink color
- Indicates bleeding in renal tubules
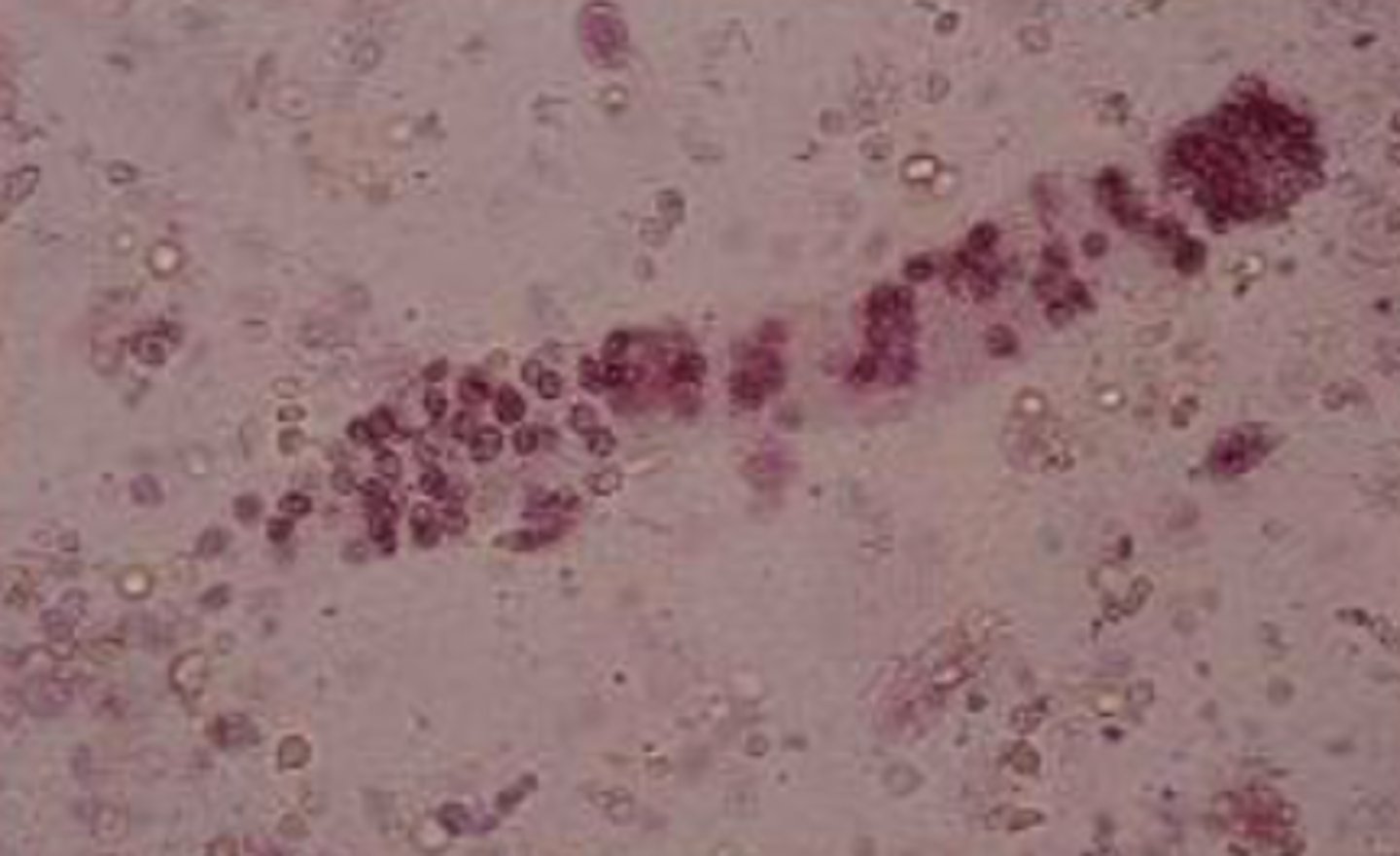
WBC/leukocyte casts
- Slightly larger than RBCs
- Granular appearance
- Indicates inflammation of kidneys
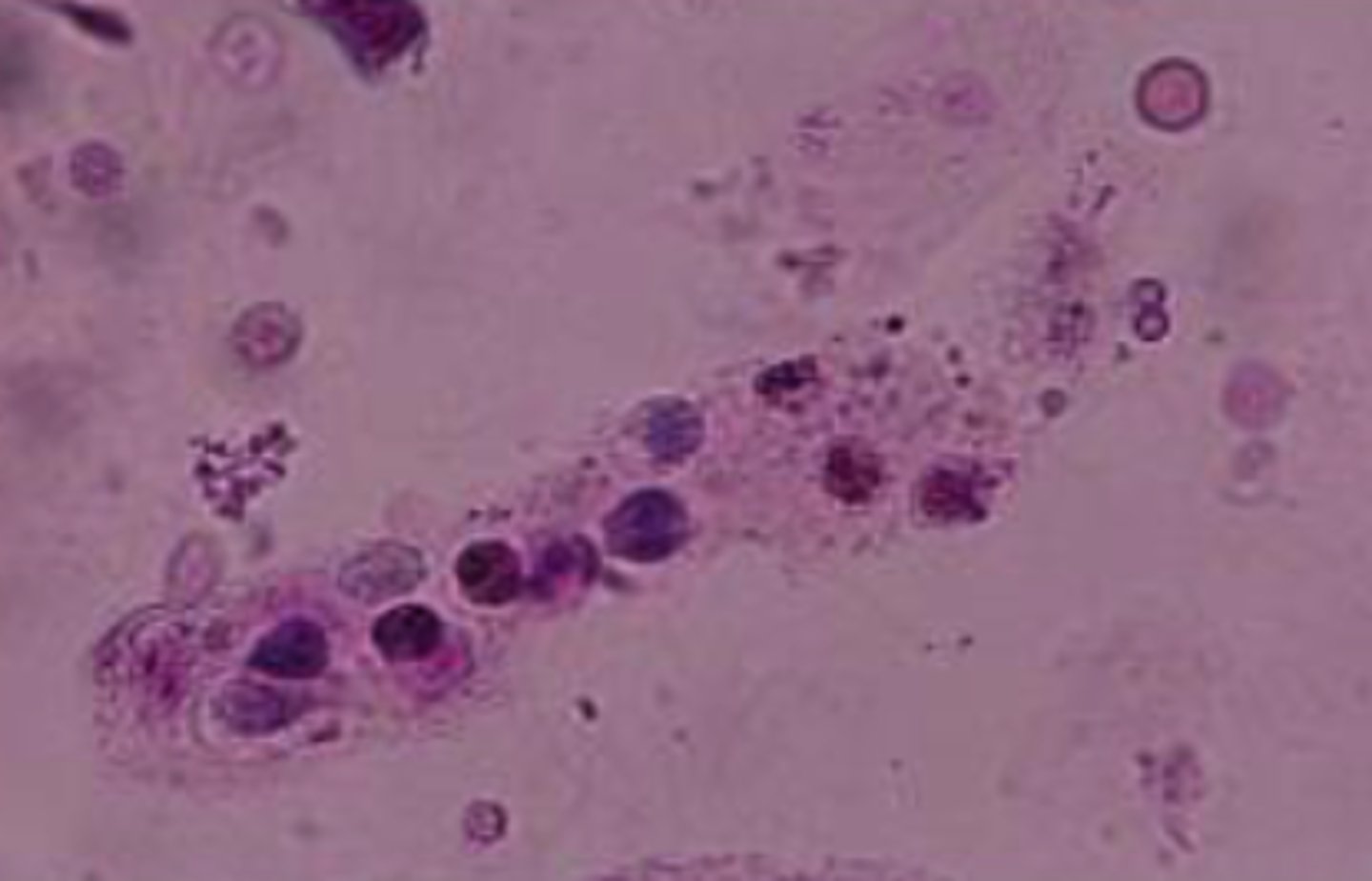
Waxy casts
- Last stage in degeneration process
- Does not have parallel sides
- Broken, craters
- Edges more blunt
- Wider than hyaline
- Indicates severe damage to renal tubules
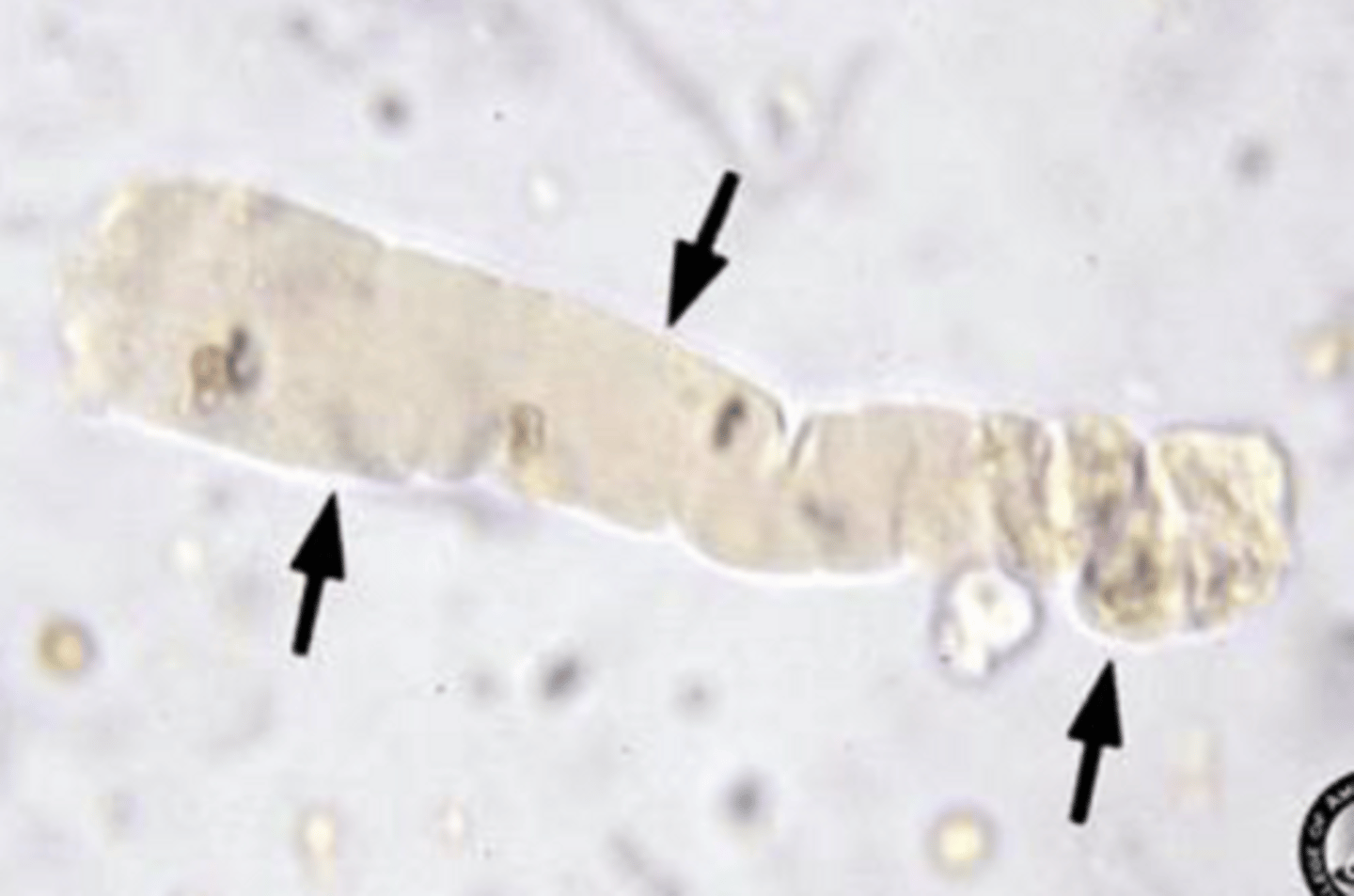
Fatty casts
- Seen more frequently in cats with renal disease or dogs with diabetes
- Have small fat droplets
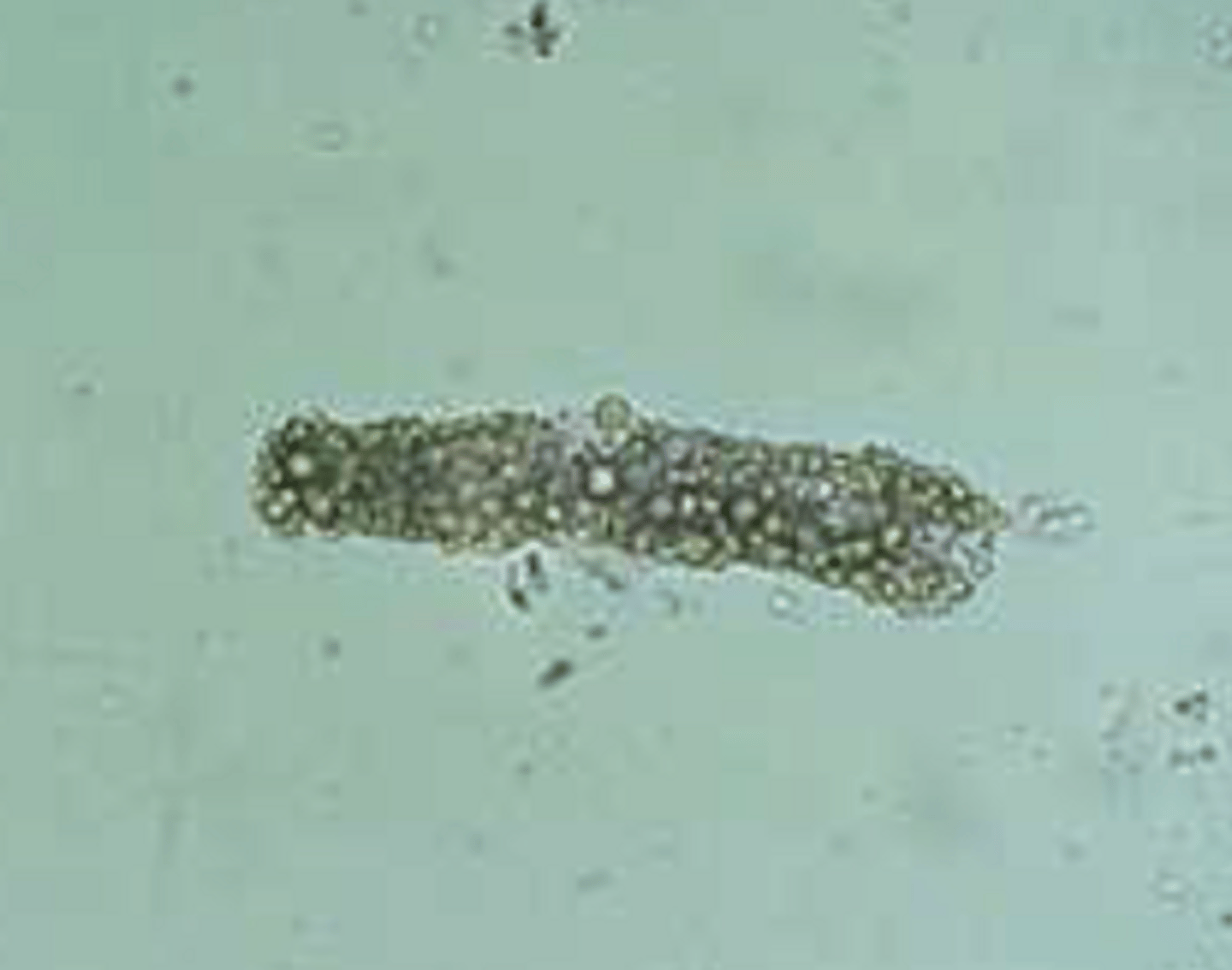
Cylindroid casts
- Look similar to hyaline casts but have tapered end
- Not really any indications