Artificial Pancreas 2
1/16
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
17 Terms
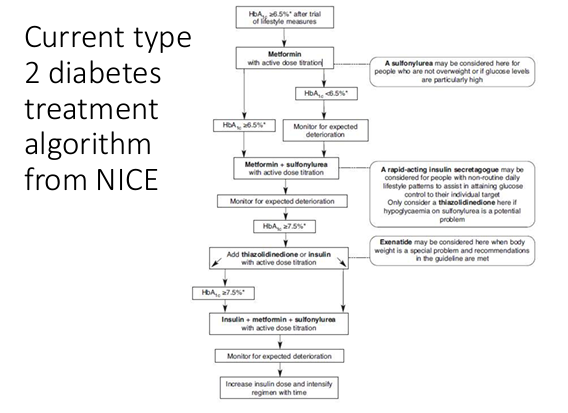
What are some monitoring and treatment considerations
By the time symptoms of T1DM nearly 90% of the b cells have been destroyed
Immediate treatment with insulin is started and needs to be maintained for life
For glucose control we need to be aware of blood glucose levels to know how much insulin to deliver
What are some things to consider in blood glucose monitoring
Spot test vs continuous
Manual vs dynamic and responsive
What until recently does a diabetic patient had to do
Take blood sample consider the result
Calc insulin needed and consider what type
Inject required amount of insulin
Check blood glucose levels
Account for any unexpected changes in glucose
What are the components for a glucose biosensor
analyte: glucose
bioreceptor: e.g. enzyme “recognises” analyte
transducer: converts response into a signal
display: shows signal on meter
What are monitoring considerations
Who needs to know glucose level
Why? how often
What else needs monitoring
HbA1c, other biomarkers, physical signs of complications
Data access and role of AI in developing better treatment responses
Can we make unpredictable humans more predictable
Can we be spontaneous
We will return to this in next lecture
What are some classic complications of diabetes
retinopathy- can lead to blindness
neuropathy- nerve damage
nephropathy- can lead to kidney failure
How is HbA1c is monitored
HbA1C is a useful tool in monitoring for patient and clinician needs a blood sample. Measured using immunoassay, ion-exchange high-performance liquid chromatography, boronate affinity and enzymatic assays
What are some clinical measures needed for good quality control considerations
inter/intra assay variation, “drift”, non-specific binding, sensitivity, precision
Sampling errors
What is the Dexcom usage story
Auto-applicator inserts sensor just beneath the skin
Every 5 minutes sensor measures glucose and sends data to transmitter worn as a stick-on patch
Transmitter sends glucose readings to Dexcom receiver or smartphone
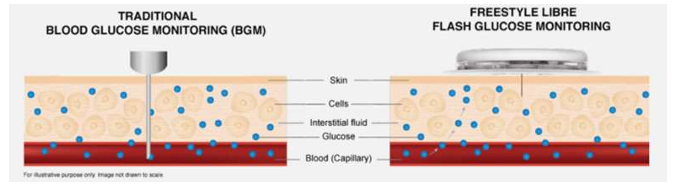
Why is CGM better than finger prick
CGM is superior to finger-prick monitoring because it provides near-continuous glucose readings, trend information, and alerts for hypo-and hyperglycaemia, allowing better day-to-day glucose control with fewer finger pricks
How does a CGM sensor work?
Sensor- has filament coated in glucose sensing enzymes- detects glucose in interstitial fluid
Sensor worn for number of days before being replaced and available for 24 hours a day
Implantable sensors can be used for longer- consist of a larger capsule compared to thin filaments in other CGMs
Sensor interacts with transmitter above skin to sends data to the receiver or smartphone app
What does regular frequent monitoring and crafty algorithms do
Allows for good BG estimates and insulin requirements
How does calibration work in CGM
Now perform the first calibration a few hours after sensor insertion, when the sensor warm-up period has completed, and subsequent ones every 12-14h, employing a simple first-order time-independent linear function as the calibration law
How does a CGM measure glucose
in ISF ie different compartment to blood need to account for the gradient between BG and IG
What did original CGM devices do for calibration
Initially CGM devices had to be calibrated daily with a capillary reading. Newer CGMs no longer need calibration and remove need for calibration
Long term benefits of CGM
Mortality stats are improving with advances in monitoring and treatment but still early
Mortality and side-effects data over next 20 years will give a better reflection of benefits of CGMs and insulin advances
What have been considerations for a wearable CGM
Accuracy
How would you improve CGM currently available in UK?
Algorithms