W4L2: Peptides, Lipids, Nucleosides & Gases
1/31
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
32 Terms
What prevents peptides, nucleosides, lipids & gases from being classified as ‘true’ neurotransmitters?
They do not satisfy all of the following criteria:
Present in presynaptic terminals
Released from presynaptic terminals after neuron fires
Existence of receptors on postynaptic neurons
What is a peptide?
2 or more amino acids which are the result of protein hydrolysis
Act similarly to neurotransmitters in that they can transport compounds between membranes, lowering the potential of neurons firing
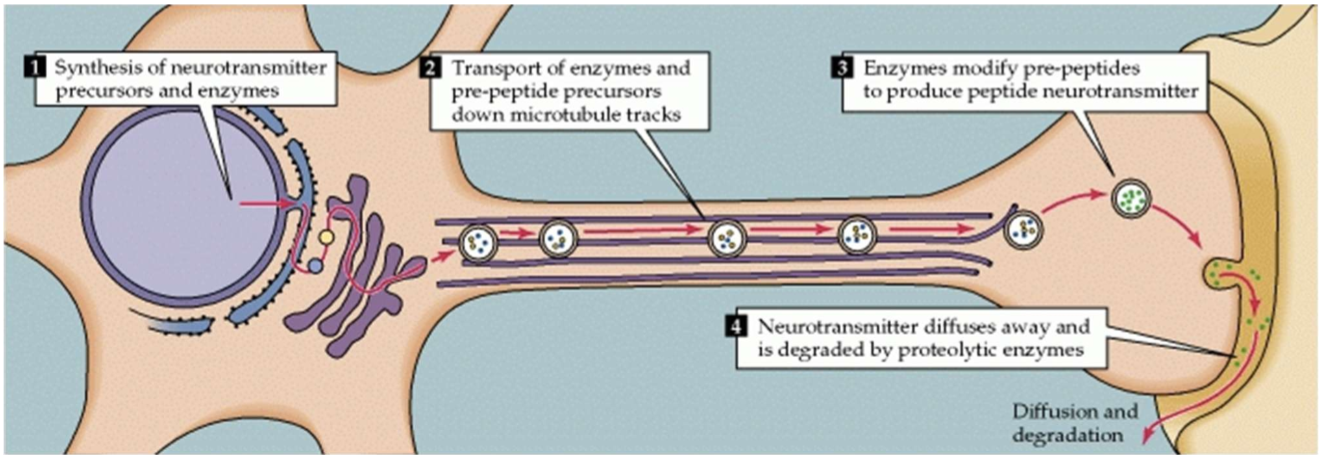
Where does peptide ‘synthesis’ & release occur?
Most peptides are not ‘synthesised’ but are the products of protein hydrolysis w/n the terminal button
Proteins/peptides transported down the axon & modified in the terminals
Commonly released alongside other neurotransmitters/neuromodulators to wither ^ or v its effectiveness
What is the best-known family of peptide neurotransmitters?
Endogenous opioids; originate internally & act on opioid receptors (mostly pain receptors)
What is the difference between endogenous opioids & opiates?
Endogenous opioids: originate internally
Opiates: drugs (e.g. morphine, heroin & opium)
What are opiates best known for?
Their analgesic (pain relief) & euphoric properties (especially in heroin)
How does historical use of opium show how pharmacokinetics influences the addictiveness of drugs?
England: pain relief liquid
China: smoked through pipes
Shows how addictive drugs can be depending on their method of consumption;
Smoking → 'euphoria'
Orally → slower effects
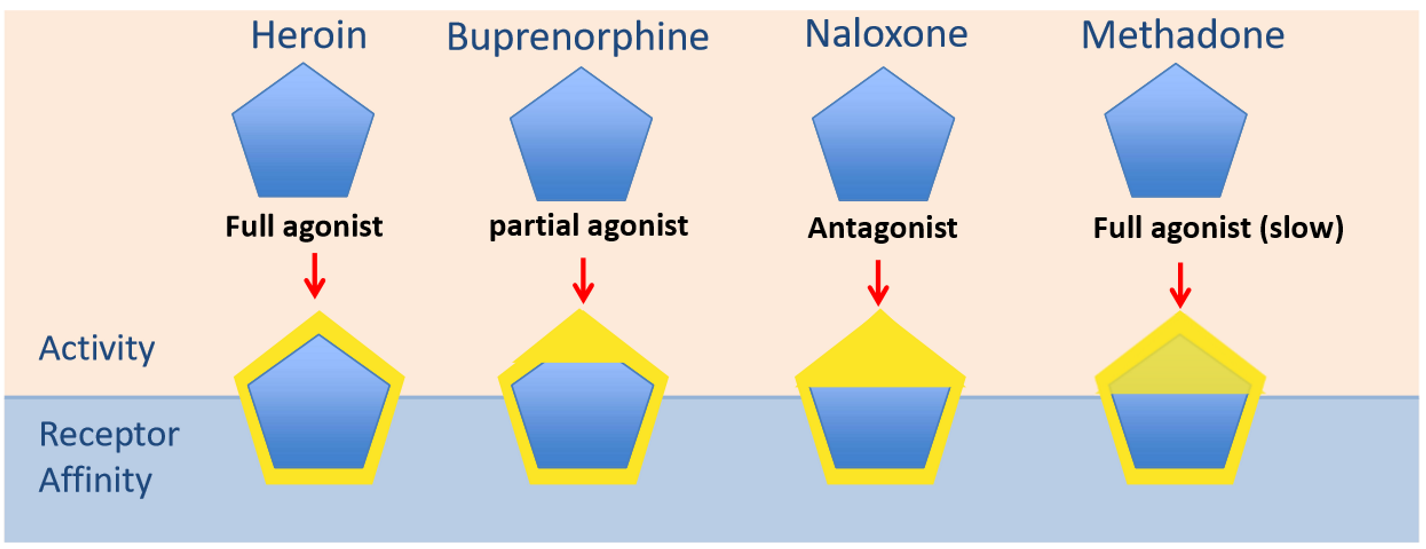
What is heroin?
A highly addictive full endogenous opioid agonist (fully activates opioid mu receptors) which is not particularly neurotoxic, but causes death by respiratory failure.
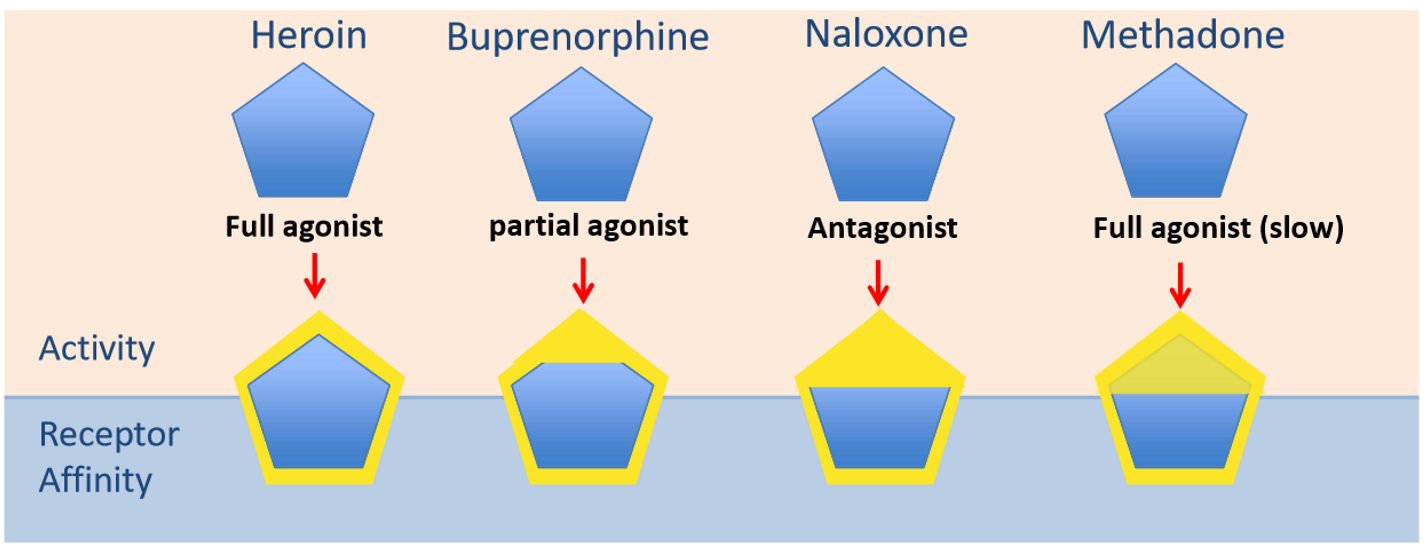
What is buprenorphine & what is it used for?
Partial opioid agonist
Similar downstream effects to heroin (small degree of stimulation), used as maintenance treatment for heroin (b/c it is a partial agonist → only stimulates it to a small degree)
Not as addictive → doesn't produce the same 'high'
Very strong affinity to the receptor → prevents people w/ heroin addiction from feeling 'high', even if they do take heroin subsequent to buprenorphine (b/c it is being dominated by the buprenorphine
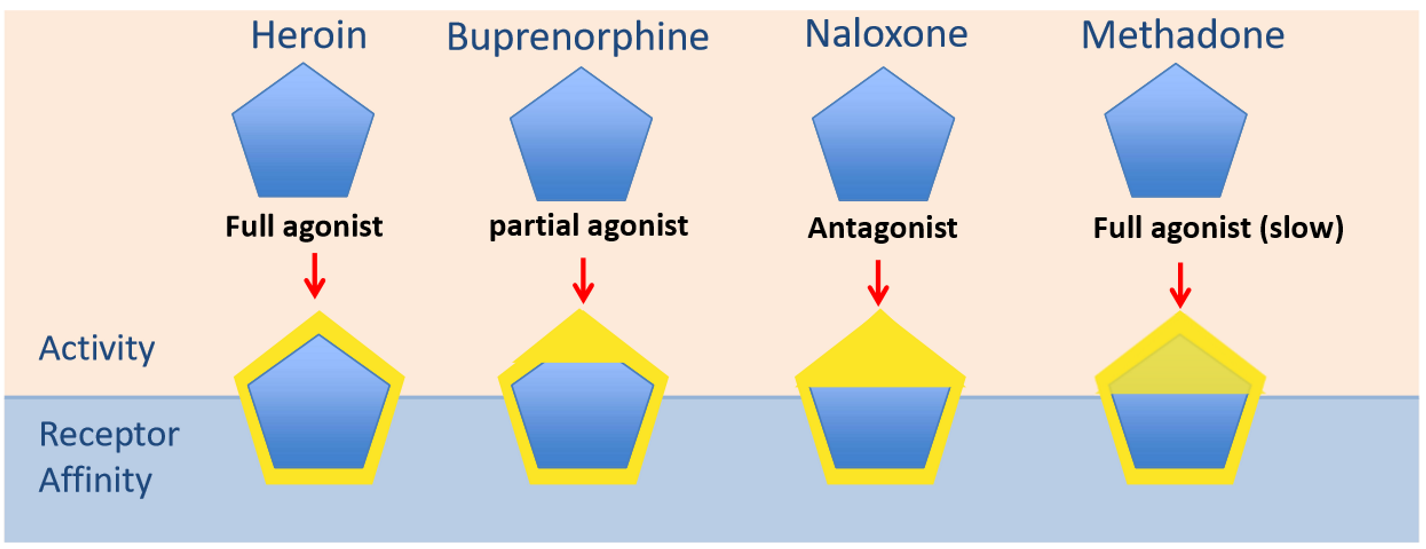
What is naloxone & what is it used for?
Full opioid antagonist
Used commonly as an emergency medicine → blocks action of the µ receptor completely
Suppresses the NS
Can't be as a long-term treatment b/c it is a full antagonist--> immediate withdrawal symptoms
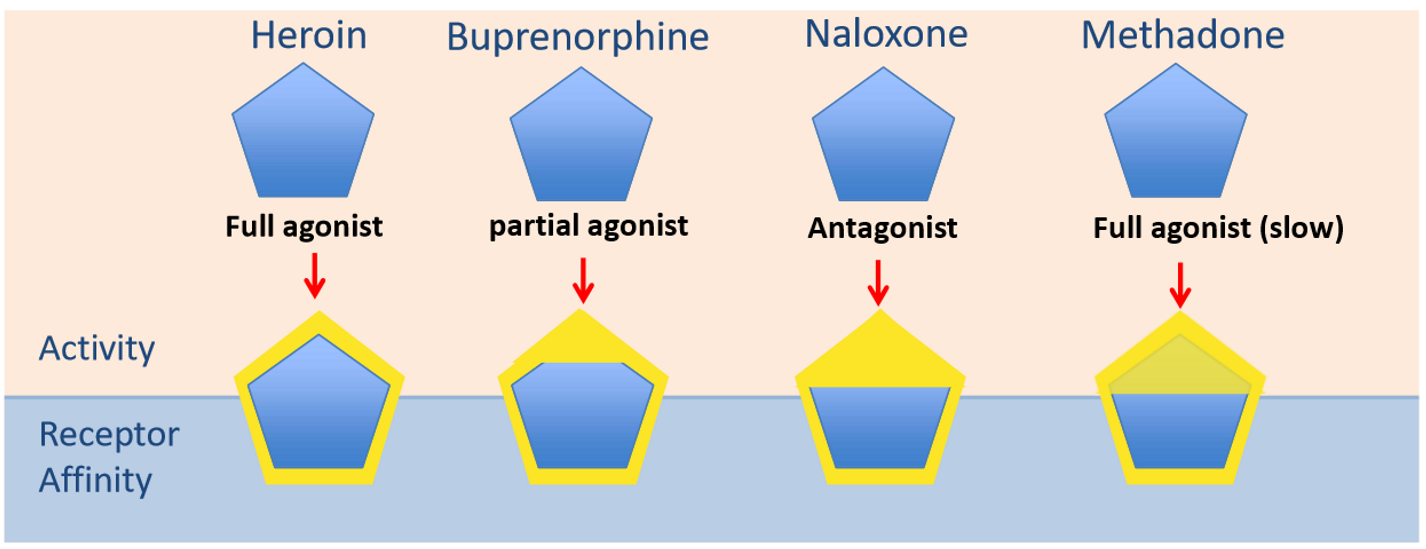
What is methadone & what is it used for?
Full opioid agonist
Very similar to heroin → used in heroin maintenance treatment
Nowhere near as addictive b/c the effects are very slow i.e. don't get the 'high' that comes w/ heroin use
What are lipids?
Naturally occurring molecules that include fats, waxes, etc.
Hydrophobic / lipophilic
Main biological function = energy storage, signalling, + providing structural components of cell membrane
How are lipid neurotransmitters/neuromodulators produced
It is still unclear
What are endocannabinoids & what do they act on
Endocannabinoids: best known lipid neurotransmitters in the brain
Act on CB1 & CB2 receptors
CB1: responsible for psychological effects
CB2: found in the peripheral tissue
What is the effect of CB1 receptor activation?
Shortens the duration of APs in the presynaptic neuron → v neurotransmitter release
Regulation of presynaptic neurons + release of neuromodulators; receptors modulate the modulators
What is THC?
The active ingredient in cannabis/marijuana that acts on CB1 receptors, primarily in the hippocampus, to prevent the release of neurotransmitters & hence lowering memory functioning
Therapeutically used to reduce nausea, relieve asthma attacks, & relieve glaucoma
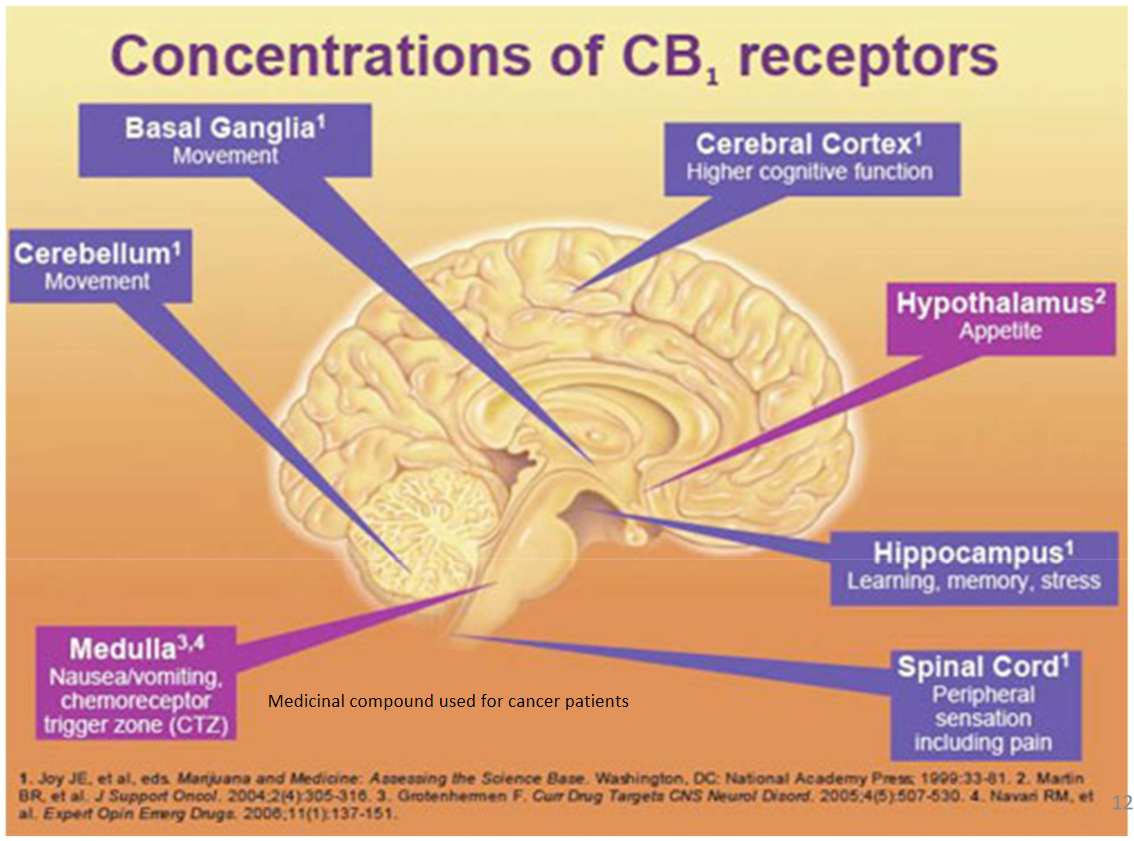
Provide some examples of how different effects are produced when CB1 receptors are activated in different areas of the brain
Describe the timeline of medicinal cannabis use in Australia
2016: Access to Medicinal Cannabis Act passed in Victoria
2017: Children w/ severe intractable Epilepsy were the first group to access cannabis
Current (VIC): any medical practitioner can prescribe medicinal cannabis if they believe it is clinically appropriate to do so
MPs do not need to gain accreditation or be specialists in a particular field
Medicinal cannabis being considered as treatment for epilepsy, pain, & multiple sclerosis
What are nucleosides & how are they obtained?
A subunit of nucleic acids, including the nitrogenous base + pentose sugar
Usually obtained by hydrolysis of nucleic acids
Often ‘co-transmitters’; modulate the release of other transmitters
What is adenosine?
A nucleoside that forms from the breakdown of ATP, the primary energy source in cells for transport & enzymes
How do adenosine levels fluctuate throughout the day?
Adenosine levels gradually rise throughout the day when ATP is used, promoting sleep & suppressing arousal in normal conditions
Stimulates cells which suppress the NS
What happens at synapses where adenosine is the primary neurotransmitter?
High post-synaptic firing → sleepiness
What is caffeine & how does it work?
Adenosine receptor antagonist which blocks the natural action of adenosine
Adenosine ^ firing rate in brain areas which promote sleepiness so caffeine ^ alertness by v the firing/activation of these neurons
‘Caffeine crash’ when the effect wears off b/c all of the adenosine is still in the synaptic cleft
What is a gas?
An air-like fluid substance which expands freely to fill any space available, irrespective of its quantity
What are the 2 gases that neurons use as neurotransmitter?
Nitric oxide (NO)
Carbon monoxide (CO)
What is nitric oxide?
A gas involved in vasodilation by increasing the size of blood vessels to increase blood to areas that are highly metabolically active
NOT nitrous oxide (NO2) = laughing gas/nangs
What & where is nitric oxide produced from in the brain?
Produced from Arginine (amino acid)
Produced in subpopulation of 1-2% of neurons in the cortex
What is the function of nitric oxide in the brain?
Unclear
Involved in learning & memory through effects on synaptic plasticity
Dilates blood vessels in regions of the brain that become metabolically active
How is nitric oxide different to other neurotransmitters?
NOT synthesised & stored in vesicles
Produced throughout the cell (incl. dendrites) & diffuses out of the cell as soon as it is produced
Does NOT activate receptors i.e. simply enters the neighbouring cell
Very short lived & is degraded/reacted w/n a few seconds of being produced
What is the site of action of nitric oxide?
Can act on several nearby neurons, even those not connected by a synapse, BUT
Short half-life of NO → it’s action will be restricted to a limited area, w/o the necessity for enzymatic breakdown or cellular reuptake