9- Chronic venous insufficiency. Clinical presentation, physical and imaging examination, treatment.
1/26
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
27 Terms
what is chronic venous insufficiency
blood pools in the veins, straining vessel walls
functional venous valves are impaired→ sswelling, ulcer formation
what is the etiology of CVI
changes in microcirculation
valve insufficiency
occlusion- thrombosis
lymphatic flow obstruction
impaired muscle pump function
other
increasing age, female, prolonged standing, obesity, smoking, pregnancy, prior thrombosis, preior extremity trauma
what is the pathomechanism of varicose veins
elevated venous pressure
incompetence of venous valves
reflux of blood into superficial veins back into extremity
further increase of venous pressure
formation of varicose veins
what is the pathomechanism of CVI
varicose vein formation
extravasation of protein and leukocytes
release of free radicals → damage of capillary BM
leakage of plasma proteins → oedema
decrease O2 supply
tissue hypoperfusion and hypozia
inflammation and atrophy
possible ulcer formation
what are the main complaints in CVI
swelling of legs and ankles
pain, lower extremity discomfort
cramping
itching, tingling, numbness
what are the skin findings of CVI
yellow- brown or re brown skin pigmentation
RBC breakdown → haemosiderin release + accumulation
oedema formation
telangiectasis
spider veins
lipodermatosclerosis
venous ulceration
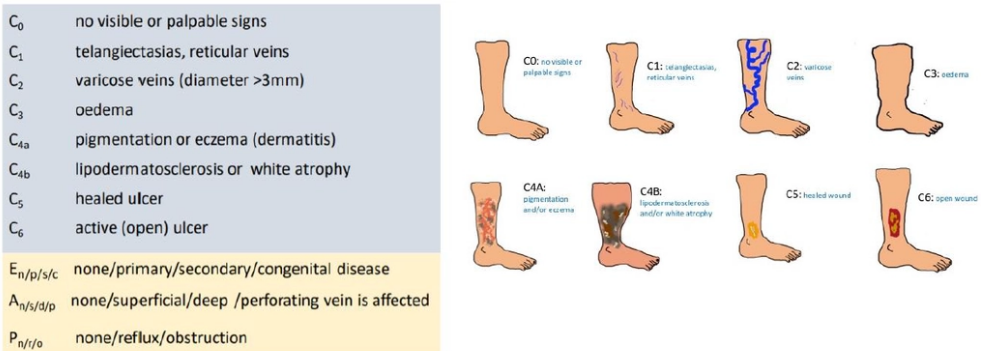
how do you classify CVI
CEAP classification
C-clinical
E-etiological
A-anatomical
P-pathophysiological
what can be seen on physical examination in CVI
Trendelenburg test
examines function of superficial and perforating venous valves
supined position with legs elevated → tourniquet is applied to compress superficial veins → leg is lowered
how can you interpret the trendelenburg test
normal
no filling of superficial veins- flows from superficial to perforating veins
Tren. 1 positive
if stasis- rapid filling from deep to superficial venous system
insufficient perforating veins
Tren. 2 positive
after stasis removal, rapid filling within superficial venous system
insufficient superficial valves
what are ways to diagnose CVI
- Duplex US
- detect reflux, obstruction, mapping prior intervention
- chek blood flow and direction
- MRV- venography
- visualise → in complicated cases
- venous plethysmography
- non invasive measurement of the venous refill time via infrared light
what is the most common venous disease that needs intervention
- venous thromboembolism
- 3rd most common CV disease
what is the imagine modality of choice for venous disease
- US first imaging
- CTA, MRA can be used to plan subsequent intervention
what is the treatment of venous thrombosis
- selective catheter thrombolysis of acute DVT
what is post thrombotic syndrome
- chronic, long term complication of DVT
- affects 30-60% of patients within 2 years of the event, with 10% developing venous ulcerations
what are the types of thrombolysis
- systemic
- selective- catheter into thrombus
what is the systemic thrombolysis
- inefficient
- insufficient recanalization
what are the disadvantages of selective thrombolysis
- time consuming intervention
- major bleeding complication
what is mechanical thrombectomy
- faster clot reduction
- greater surface area than thrombolysis
- mechanical aspiration
- hydrodynamic (reolytic) devices
- high pressure recirculation system for thrombus dissolution and aspiration
what is chronic venous occlusion
- insufficient collateralisation of ilio caval occlusion → post thrombotic complaints, leg ulcers
what is the treatment of chronic venous occlusion
- not responding cases of conservative therapy→ revascularisation procedures
- surgical interventions are invasive- only considered in cases of failed endovascular intervention
- after successful recanalisation appropriate anticoagulation → further angiology follow ups are needed
what are the catheter based interventions
- puncture sites- jugular, femoral, GSV
- pre dilation with balloon→ using long self expanding stents
- post dilation balloon
what are the open surgical treatment of venous diseases
- varicose veins- endovenous surgery, varicectomy
- rarely in thrombophlebitis- GSV, LSV ligation
- proximal (ilio femoral) deep vein thrombosis
- superior vena cava- PTA, stent
- inferior vena cava
- acute thrombosis- lysis, thrombus aspiratio, cava filter
- chronic stenosis/ occlusion- PTA, stent
- tumour thrombus- cava thrombectomy
What are the types of contemporary varicose vein surgeries
- thermal procedures
- non thermal procedures
what are the thermal procedures for varicose veins
- radiofrequency
- mono/bipolar
- laser
- different wavelength
- linear/ radial fiber
- steam
- cryostripping
what are the non thermal procedures for varicose veins
- foam sclerotherapy
- mechanochemical ablation
- glue- cyanoacrylate
what is radiofrequency catheter ablation
- RF energy affect collagen in vein wall
- fast ablation
- lumen decreases, vein closure and scarring
describe a traditional varicectomy
- crossectomy
- stripping
- perforant vein ligation
- side branch remova