RADT 102 EXAM #2 - FLUOROSCOPY
1/70
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
71 Terms
Static means …
not moving
Dynamic means …
moving
What is the HISTORY of FLUOROSCOPY
thomas edison discovered in 1896
screen (zinc-cadmium sulfide) placed over patient’s body in x-ray beam
radiologist looked directly at screen
in 1950, image intensifiers were developed (intensified the light of the image)
before that, they would wear red goggles 30 minutes before the exam to see better
Describe CONES (eyes)
central
less sensitive to low light (threshold of 100 lux)
will respond to bright light
daylight vision (phototopic vision)
perceives COLOR, differences in brightness
perceives fine detail
utilized in fluoroscopy
Describe RODS (eyes)
periphery
sensitive to low light
used in night vision (scotopic vision)
dims objects seen better peripherally
color blind
do not perceive detail
Fluoro is viewed at the same level of brightness as radiographs which is ______
100 - 1000 lux
Fluoro x-ray tube operate at _____ mA, why so low?
0.5 to 5 mA
there is longer exposure time, so you make the mA shorter
KVP is dependent on body section and changes based on section to see everything at a good brightness throughout the body
True
What systems MAINTAIN BRIGHTNESS?
ABC (subset of AEC/AERC)
ABS
AGC
all control, stabilization, gain control
makes sure that the brightness stays the same
A FIXED tube may be mounted no closer than ______ inches or ______ cm to patient
15
38
A MOBILE (c-arm) tube may be brought no closer than ____ inches or ____ cm to patient
12
30
There is LESS radiation if tube is _______
under the table
State the SEQUENCE of FLUOROSCOPY
beam exits the patient (remnant radiation)
hits the INPUT PHOSPHOR (cesium iodide CsI tightly packed needles … great spatial resolution)
converts X-RAYS to VISIBLE LIGHT
hits PHOTOCATHODE (cesium and antimony)
emits ELECTRONS when struck by LIGHT (turns the light into electrons)
the potential difference within the image intensifier tube is a constant 25,000 volts
electrons are accelerated to ANODE
anode is circular plate with hole for electrons to go through
there are lenses to force the electrons together and push them towards and out the anode
electrons hits OUTPUT PHOSPHOR (zinc cadmium sulfide) with high kinetic energy producing an increased amount of light
Each photoelectron at the OUTPUT PHOSPHOR, has ______ more ______ ______
50-75, light, photons
What is the purpose of ELECTROSTATIC LENSES
electrons must be focused for accurate image pattern
these accelerate and focus the electron beam
OLD SCHOOL - light was emitted from output phosphor and then …..
was transmitted as an analog signal via a TV tube called plumbicon/vidicon
NOW - light is emitted from output phosphor and then …
is captured by a CCD or a flat panel system is used
If the DIAMETER of the INPUT PHOSPHOR DECREASES, the overall BRIGHTNESS of the OUTPUT PHOSPHOR _______
decreases
not a good thing
DESCRIBE flux gain
comparing the # of x-rays coming in and the # of light photons coming out
ratio of number of light photons at the output phosphor to the number of x-rays at the input phosphor
# of output light photon / # of input x-ray photons
represents how bright it would be coming out
DESCRIBE minification gain
comparing a change of activated diameter of the input phosphor to the fixed diameter of the output phosphor
ratio of the square of the diameter of the input phosphor the square of the diameter of the output phosphor OR
# of electrons produced at large input screen squared, compressed into the area of small output screen squared
DESCRIBE brightness gain
minification gain x flux gain
increases illumination level of an image
ratio of the intensity of the illumination to the output phosphor to the radiation intensity at the input phosphor
when too low, ABC/AGC/ABS/AERC kick in to fix the brightness
brightness gain of 5000-30,000
When flux, minification, and brightness gain DECREASE, magnification _____, mAs ____, and pt exposure ______
increases, increases, increases
Describe CONVERSION FACTORS
ratio of intensity of illumination at the output phosphor (measured in Candela per meter squared) to the radiation intensity at the input phosphor (mGya per sec)
(Cd/m squared) / (mGya / s)
What is MULTIFIELD IMAGE INTENSIFICATION
allows focal point change to reduce field of view and magnify the image
multifield = the different diameters of input phosphor
Most popular MULTIFIELD IMAGE INTENSIFIER is _______
25/17/12
others are 23/15/10
DESCRIBE multifield image intensification
NUMERIC dimensions refer to the INPUT phosphor (25/17)
SMALLER dimension (25/17) result in MAGNIFIED images
at 25 - all photoelectrons are accelerated to output phosphor
smaller dimension - voltage of focusing lenses is increased
electron focal spot moves away from the output
only the electrons from the center of input strike the output
If the diameter is REDUCES to magnify the image, how does that impact flux, minification and ultimately brightness?
reduces flux, reduces minification, brightness goes down
increases pt exposure because the ABC increases the mAs to get the right brightness
What are the PROS of using a SMALLER DIMENSION
only central region of input is used
spatial resolution is better (kinda like the umbra)
lower noise, higher contrast resolution
What are the CONS of using a SMALLER DIMENSION
minification gain is reduced = dimmer image
to compensate must increase mA
increases pt dose
What does a BEAM SPLITTING MIRROR do
splits the beam to be sent to additional recording devices
What is an ABS sensor
bumps up mA to maintain brightness
Why is it easy to convert a conventional fluoro unit to a digital one?
there is already a system to take light and digitize it
DESCRIBE digital fluoro
image acquisition is FASTER
can post process
has TWO monitors
operates in radiographic mode
MA station is around 400 in flat panel mode
time isn’t longer as the process isn’t as long so the patient dose will be lower
Describe PULSED PROGRESSIVE FLUOROSCOPY
generator can be switched on and off rapidly
broken into different time frames
interrogation / extinction
each must have times of less than 1 ms
What is INTERROGATION TIME (pulsed progressive fluoroscopy)
tube switched on and meets selected levels of kVp and mA
What is EXTINCTION TIME (pulsed progressive fluoroscopy)
time required for the tube to be switched off
duty cycle - time tube is energized
Describe FLAT PANEL IMAGE RECEPTORS (FPIR)
they are beginning to replace CCD’s
made of CESIUM IODIDE pixel detectors
lighter, smaller than image intensifiers
improvement to image as the SPATIAL RESOLUTION is uniform and distortion free
HIGH DQE
improved contrast
What is the SEQUENCE of a CCD
x-ray interacts with scintillation material
sent to capacitors which convert light into electrical charge
charge sent to ADC
Describe a CCD
structure is a silicon chip
made of cesium iodide (structured phosphor reducing light spread)
lenses or fiber optics focus light onto chip
used in fluoro, c-arms for trauma biopsy
Describe BINNING
allows charges from adjacent pixels to be combined on the sensor before the charge is read out through the amplifier, the dominant noise source on a CCD
this results in faster readout speeds and improved signal to noise ratios with reduced spatial resolution
WITH BINNING →
combines charges as they drop into readout
instead of 4 pixels, there are two
LESS things being read out on amplifiers = LESS noise
QUICKER process
WITHOUT BINNING →
MORE NOISE
MORE SPATIAL RESOLUTION, but COMPROMISED due to increased noise
SLOWER process
Describe CMOS
Complementary metal oxide semiconductor
highly efficient and inexpensive
more susceptible to noise so lower quality, lower resolution and lower sensitivity as compared to CCD
converts light into electrons, stored in capacitors within the pixel then to ADC
List COMPARISONS between CCD and CMOS
CMOS sensors are more susceptible to noise
light sensitivity of a CMOS chip is lower than a CCD
CMOS uses very little power compared to CCD
CMOSs are inexpensive compared to CCD sensors
CMOS chips are intended for shorter period and have lower quality, lower resolutions, lower sensitivity
pixel fill factor is greater with CCDs than CMOSs
What are the ADVANTAGES of a CCD
relatively inexpensive compared to a TFT flat panel system
they are modular, making them easy to repair, replace and upgrade
What is a DISADVANTAGE of a CCD
CCDs result in demagnification, which requires for pixels to reduce in size, reducing DQE
Image intensifiers receive the _______, convert it to ______ and increases the ______ ______ 5000-30,000 times
remnant x-ray beam, light, light intensity

RED
the 25 intensifier (25/17/12)

ORANGE
the 17 intensifier (25/17/12)

YELLOW
the 12 intensifier (25/17/12)
converges before the focal point, almost like increased OID
the converging of electrons is farther away from output phosphor which causes the increased magnification

BLACK
moves the table (control button)

GRAY
tilts the table (control button)

PINK
fluoro button (control button)

PURPLE
capturing a signal image (control button)

GREEN
collimation (control button)
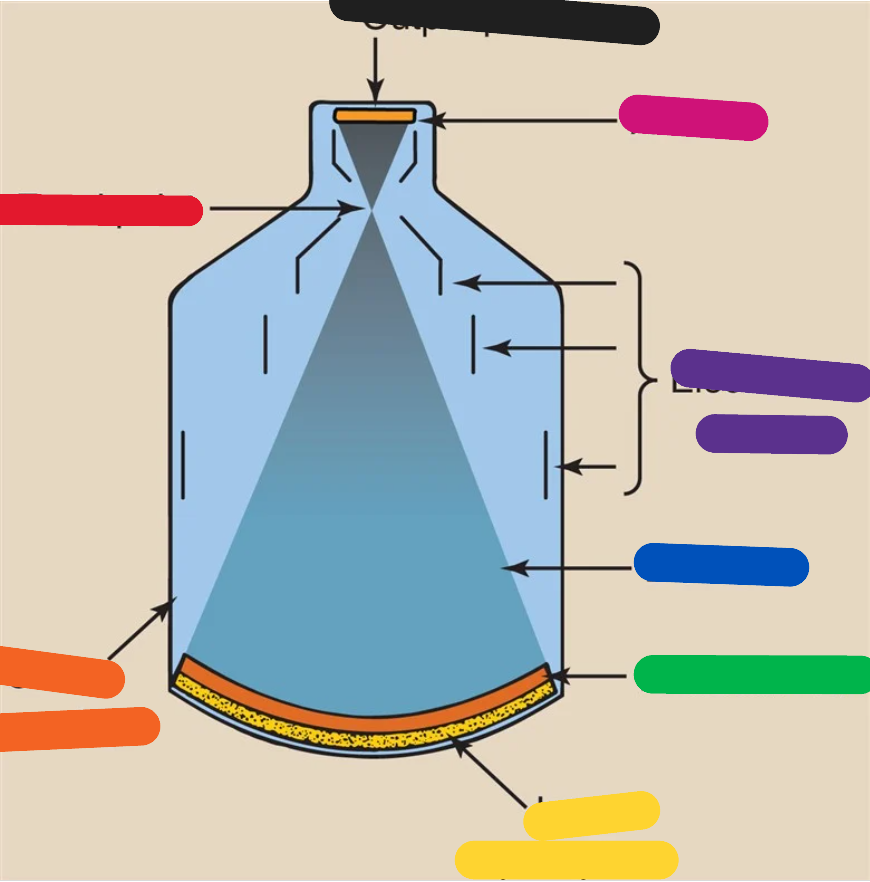
RED (image intensifier tube)
focal point
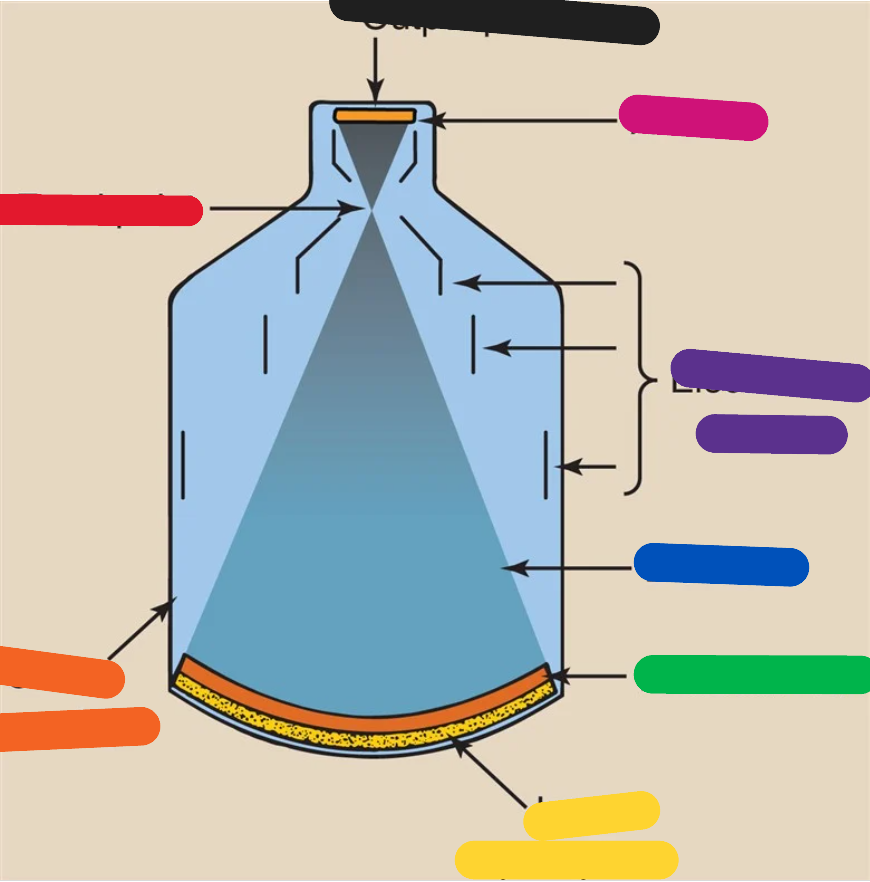
ORANGE (image intensifier tube)
glass envelope
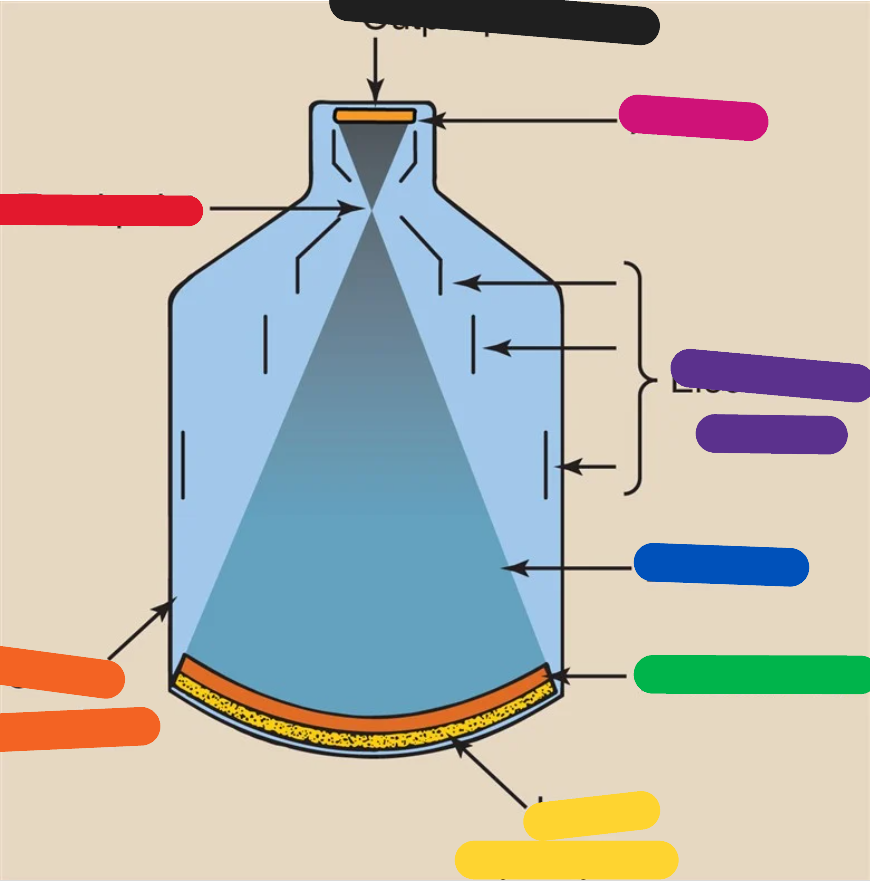
YELLOW (image intensifier tube)
input phosphor
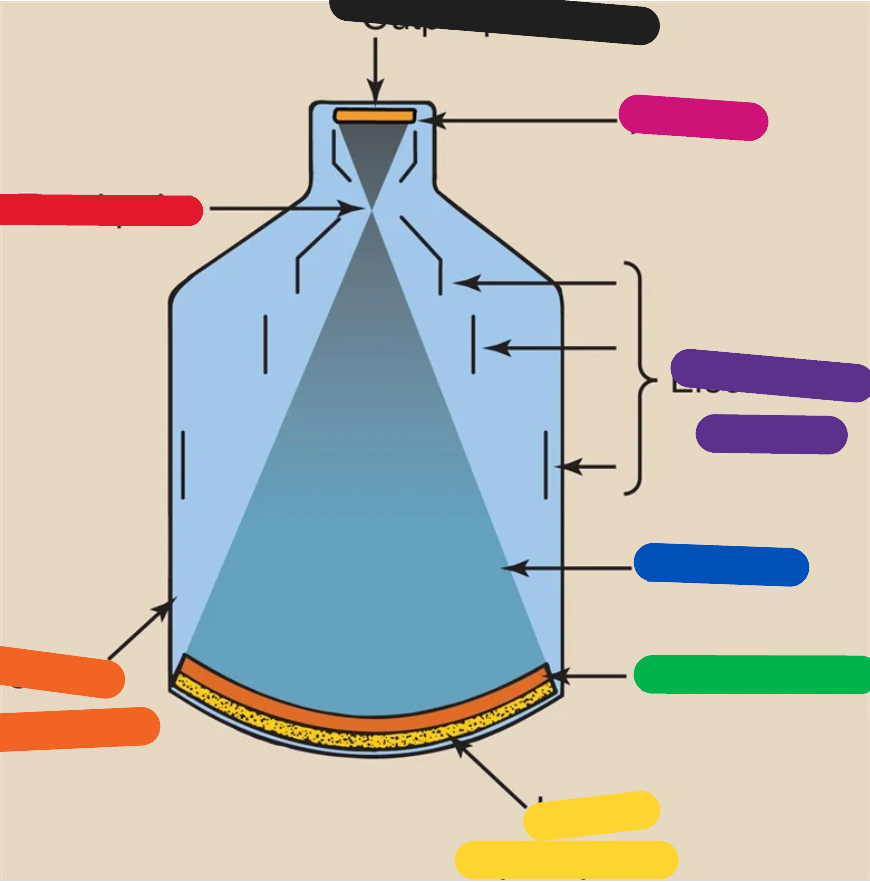
GREEN (image intensifier tube)
photocathode
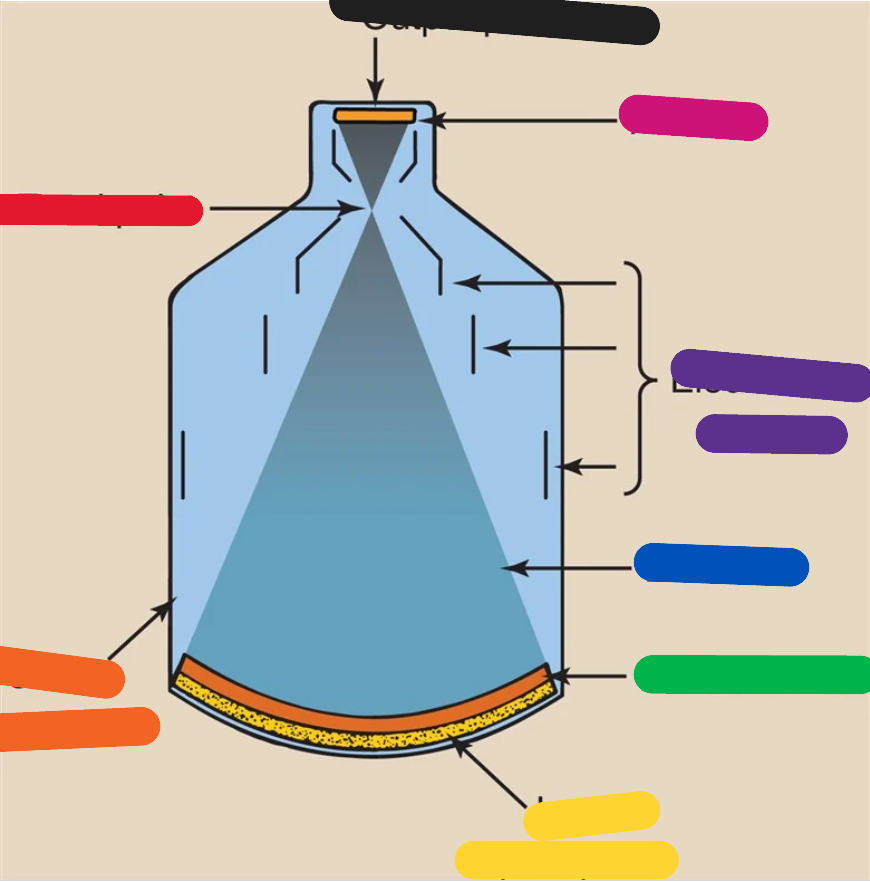
BLUE (image intensifier tube)
electrons
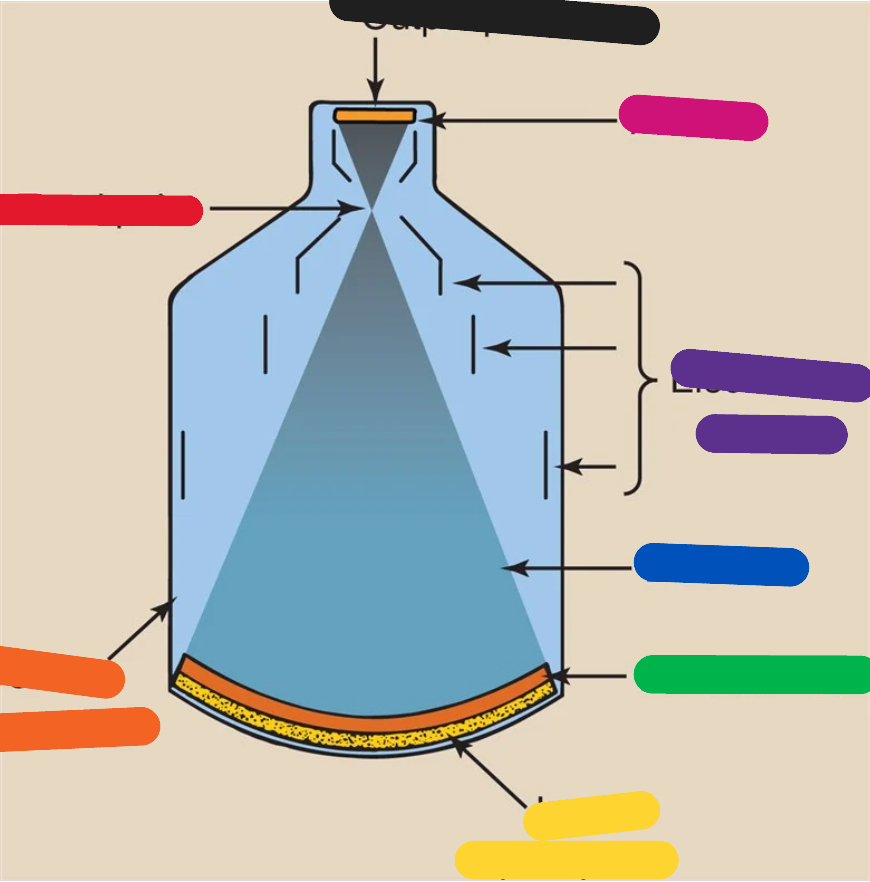
PURPLE (image intensifier tube)
electrostatic lenses
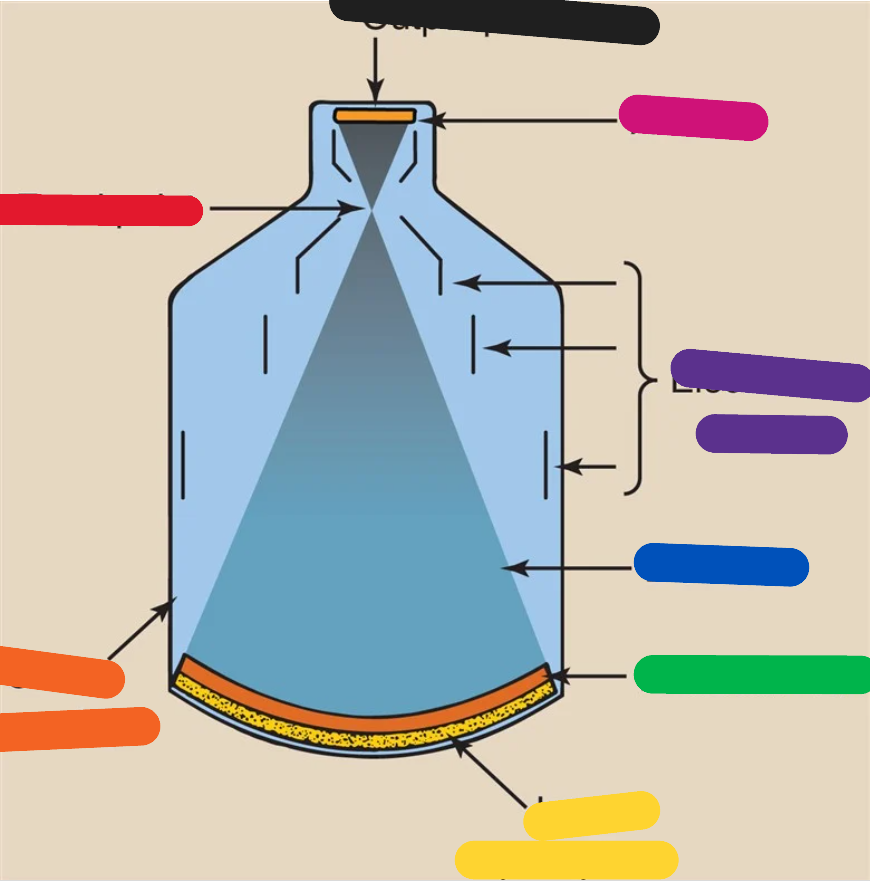
PINK (image intensifier tube)
anode
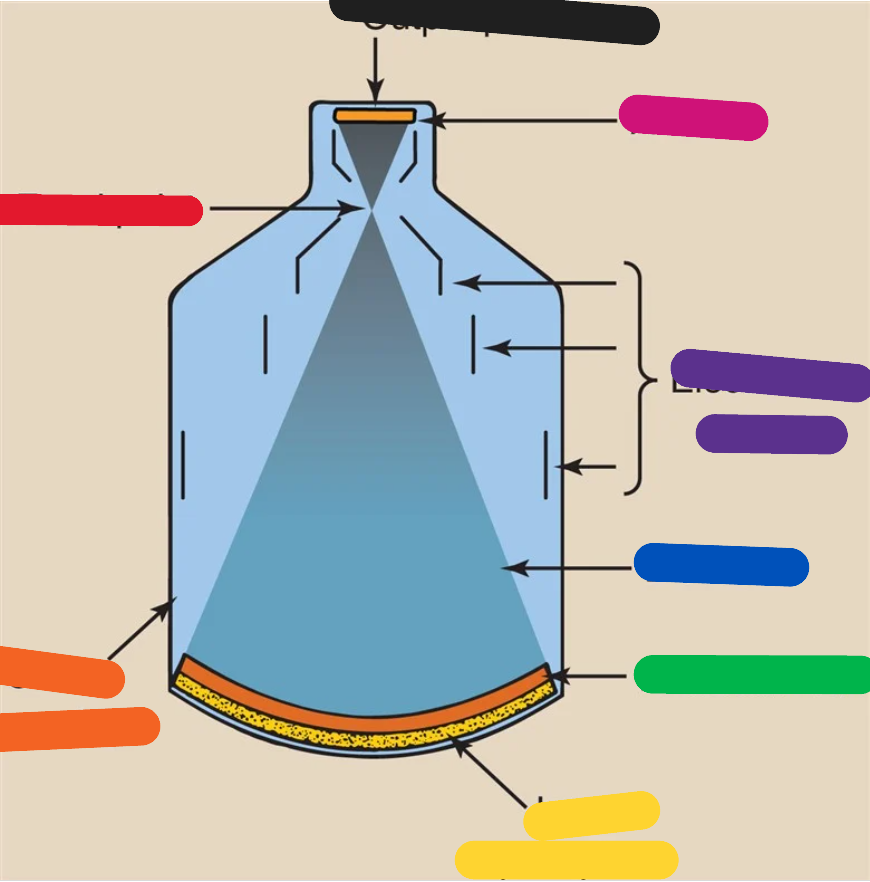
BLACK (image intensifier tube)
output phosphor
What is the GREATER DENSITY formula?
mAs x kVp squared / SID squared x grid conversion factor
How do you turn VOLTS into KILOVOLTS
/1000
What is the INPUT PHOSPHOR made out of?
cesium iodide (CsI)
What is the OUTPUT PHOSPHOR made out of?
zinc-cadmium sulfide
What is the PHOTOCATHODE made out of?
thin metal layer composed of cesium and antimony compounds
ELECTROSTATIC LENSES aka ….
focusing lenses
1 x-ray: _____ photons
3000
Pulse progressive fluoro also avoids _____ _______
thermal overloading
List the ADVANTAGES of a CCD device
HIGH spatial resolution
HIGH SNR
HIGH DQE
no warm-up required
NO spatial distortion
NO maintenance
unlimited life
UNAFFECTED by magnetic fields
linear response
LOWER patient radiation dose
List the ADVANTAGES of a FLAT-PANEL IMAGE RECEPTOR (over a CCD)
distortion free images
constant image quality over the entire image
improved contrast resolution over entire image
HIGH DQE at all radiation dose levels
rectangular image area couples to similar image monitor
UNAFFECTED by external magnetic fields