Neurologic Trauma
1/19
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
20 Terms
Head injury
A broad classification that includes any injury to the head as a result of trauma
2.9 million ER visits in the United States; majority are for a mild traumatic brain injury (TBI)
About 56,800 people die related to TBI; about 30% of all injury-related deaths
Most common cause of TBIs is falls
Groups at highest risk for TBI:
children 0 to 4 years old
adolescents ages 15 to 19 years
adults 65 years and older
higher in males
Prevention is the best approach
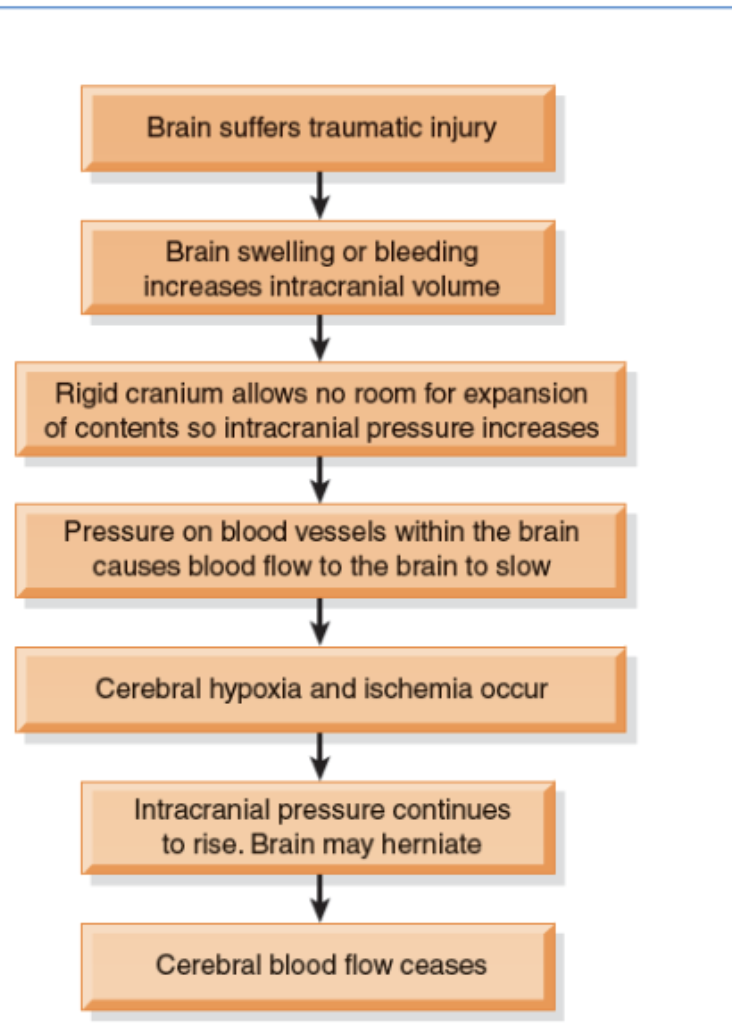
What is the patho of traumatic head injury?
Primary injury: consequence of direct contact to head/brain during the instant of initial injury
Contusions, lacerations, external hematomas, skull fractures, subdural hematomas, concussion, diffuse axonal
Secondary injury: damage evolves over ensuing days and hours after the initial injury
Caused by cerebral edema, ischemia, or chemical changes associated with the trauma
Scalp Wounds and Scull Fractures (manifestations)
Manifestations depend on the severity and location of the injury
Scalp wounds
Tend to bleed heavily and are portals for infection
Skull fractures
Usually have localized, persistent pain
Fractures of the base of the skull
Bleeding from nose pharynx or ears
Battle sign—ecchymosis behind the ear
CSF leak: halo sign—ring of fluid around the blood stain from drainage
Brain Injury (Open v Closed etc.)
Closed TBI (blunt trauma): acceleration/deceleration injury occurs when the head accelerates and then rapidly decelerates, damaging brain tissue
Open TBI (penetrating): object penetrates the brain or trauma is so severe that the scalp and skull are opened
Concussion: a temporary loss of consciousness with no apparent structural damage
Contusion: more severe injury with possible surface hemorrhage
Symptoms and recovery depend on the amount of damage and associated cerebral edema
Longer period of unconsciousness with more symptoms of neurologic deficits and changes in vital signs
Diffuse axonal injury: widespread axon damage in the brain seen with head trauma. Patient develops immediate coma
Intracranial bleeding
Epidural hematoma
Subdural hematoma
Acute and subacute
Chronic
Intracerebral hemorrhage and hematoma
Concussion
Patient may be admitted for observation or sent home
Observation of patients after head trauma; report immediately
Observe for any changes in LOC
Difficulty in awakening, lethargy, dizziness, confusion, irritability, anxiety
Difficulty in speaking or movement
Severe headache
Vomiting
Patient should be aroused and assessed frequently
Location of Epidural, Subdural, and Intracerebral Hematomas
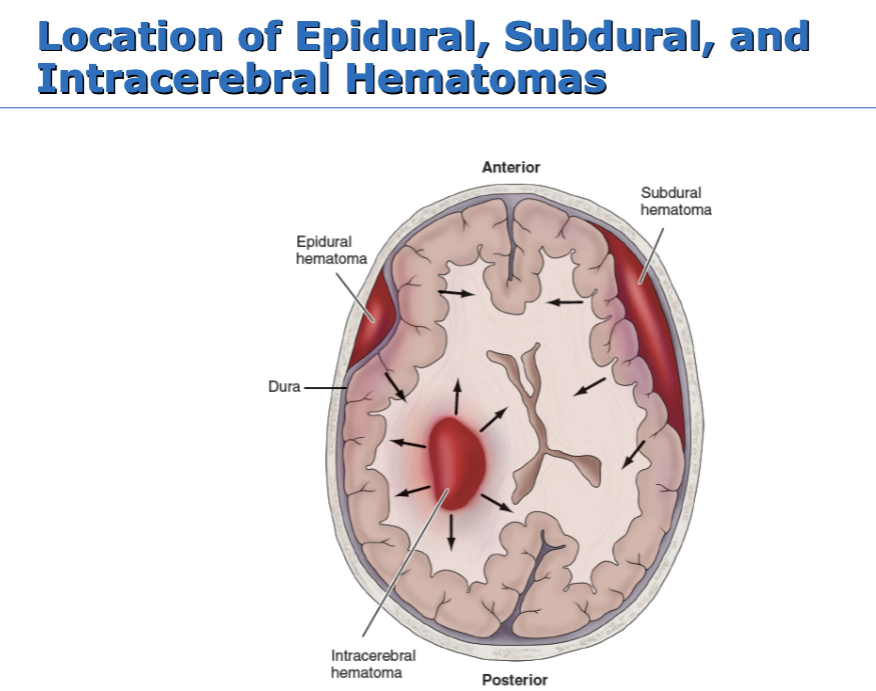
Epidural Hematomas
Blood collection in the space between the skull and the dura
Patient may have a brief loss of consciousness with return of lucid state; then as hematoma expands, increased ICP will often suddenly reduce LOC (S&S)
An emergency situation!
Treatment includes measures to reduce ICP, remove the clot, and stop bleeding (burr holes or craniotomy)
Patient will need monitoring and support of vital body functions; respiratory support
Subdural Hematomas
Collection of blood between the dura and the brain
Acute or subacute
Acute: symptoms develop over 24 to 48 hours
Subacute: symptoms develop over 48 hours to 2 weeks
Requires immediate craniotomy and control of ICP
Chronic
Develops over weeks to months
Causative injury may be minor and forgotten
Clinical signs and symptoms may fluctuate
Treatment is evacuation of the clot
Intracerebral Hematomas
Hemorrhage occurs into the substance of the brain
May be caused by trauma or a nontraumatic cause
Treatment
Supportive care
Control of ICP
Administration of fluids, electrolytes, and antihypertensive medications
Craniotomy or craniectomy to remove clot and control hemorrhage; this may not be possible because of the location or lack of circumscribed area of hemorrhage
Management of the Patient with a Head Injury
Assessment and diagnosis of the extent of injury with initial physical and neurologic examinations
CT and MRI scans are the main neuroimaging diagnostic tools
Positron emission tomography (PET) for assessing brain function
Assume cervical spine injury until it is ruled out
Apply cervical collar and maintain until cleared
Therapy to preserve brain homeostasis and prevent secondary brain injury
Stabilize cardiovascular and respiratory function to maintain cerebral perfusion/oxygenation
Control of hemorrhage and hypovolemia
Maintain optimal blood gas values
Treat increased ICP and cerebral edema
Surgery if indicated
Monitor ICP and drain CSF as needed
What are the supportive measures with Head Injury?
Respiratory support: intubation and mechanical ventilation
Seizure precautions and prevention
NG tube to manage reduced gastric motility and prevent aspiration
Fluid and electrolyte maintenance
Pain and anxiety management
Nutrition
How is patient with traumatic brain injury assessed?
Health history with focus on the immediate injury, time, cause, and the direction and force of the blow
Baseline assessment
LOC—Glasgow Coma Scale
Frequent and ongoing neurologic assessment
Multisystem assessment
What is the nursing interventions for the patient with traumatic brain injury?
Ongoing assessment and monitoring are vital
Maintain adequate airway
Monitor neurologic function
LOC with GCS
Vital signs
Motor function
Other neurologic signs
I&O and daily weights
Monitor blood/urine electrolytes, osmolality and blood glucose
Early initiation of nutritional therapy
Improve coping and support of cognitive function
Preventing sleep pattern disturbance
Support of family
Provide and reinforce information
Measures to promote effective coping
Setting of realistic, well-defined short-term goals
Referral for counseling
Support groups
Strategies to prevent injury
Assessment of oxygenation
Assessment of bladder and urinary output
Assessment for constriction caused by dressings and casts
Padded side rails
Mittens to prevent self-injury; avoid restraints
Reduce environmental stimuli
Adequate lighting to reduce visual hallucinations
Measures to minimize disruption of sleep–wake cycles
Skin care
Measures to prevent infection
Maintaining body temperature
Maintain appropriate environmental temperature
Use of coverings: sheets, blankets to patient needs
Administration of acetaminophen for fever
Cooling blankets or cool baths; avoid shivering
Spinal Cord Injury
294,000 persons in the United States live with disability from SCI
Causes include MVAs, falls, violence (gunshot wounds), and sports-related injuries
Males account for 78% of SCIs
Average age of injury is 43
Risk factors include young age, male gender, alcohol and drug use
Major causes of death are pneumonia, pulmonary embolism (PE), and sepsis
Pathophysiology of Spinal Cord Injury
The result of concussion, contusion, laceration, or compression of spinal cord
Primary injury: result of the initial trauma and usually permanent
Secondary injury: SCI includes edema and hemorrhage
Major concern for critical care nurses
Treatment is needed to prevent partial injury from developing into more extensive, permanent damage
How is patient with spinal cord injury assessed?
Monitor respirations and breathing pattern
Lung sounds and cough
Monitor for changes in motor or sensory function; report immediately
Assess for spinal shock
Monitor for bladder retention or distention, gastric dilation, and ileus
Temperature; potential hyperthermia
With neurogenic shock: cold or hot, hypotension, bradycardia, warm dry skin bc of vasodilation
What is the nursing interventions for the patient woth spinal cord injury?
Promoting effective breathing and airway clearance
Monitor carefully to detect potential respiratory failure
Pulse oximetry and ABGs
Lung sounds
Early and vigorous pulmonary care to remove secretions
Suctioning with caution
Breathing exercises
Assisted coughing
Humidification and hydration
Improving mobility
Maintain proper body alignment
If not on a specialized rotating bed, turn only if spine is stable and as indicated by physician
Monitor blood pressure with position changes
PROM at least four times a day
Use neck brace or collar when patient is mobilized
Move gradually to erect position
Strategies to compensate for sensory and perceptual alterations
Measures to maintain skin integrity
Temporary indwelling catheterization or intermittent catheterization
NG tube to alleviate gastric distention
High-calorie, high-protein, high-fiber diet
Bowel program and use of stool softeners
Traction pin care
Hygiene and skin care related to traction devices
Spinal shock v Neurogenic shock
Spinal shock
A sudden depression of reflex activity below the level of spinal injury
Muscular flaccidity, lack of sensation and reflexes
Neurogenic shock
Caused by the loss of function of the autonomic nervous system
Blood pressure, heart rate, and cardiac output decrease
Venous pooling occurs because of peripheral vasodilation
Paralyzed portions of the body do not perspire
What is autonomic dysreflexia?
Acute emergency!
Occurs after spinal shock has resolved and may occur years after the injury
Occurs in persons with SC lesions above T6
Autonomic nervous system responses are exaggerated
Symptoms: severe pounding headache, sudden increase in blood pressure, profuse diaphoresis, nausea, nasal congestion, and bradycardia
Triggering stimuli: distended bladder (most common cause), distention or contraction of visceral organs (e.g., constipation), or stimulation of the skin
Anthing even wrinckle in sheet, somthing pressing on skin, constipation etc. → place in siting position
What is the nursing interventions for autonomic dysreflexia?
Place patient in seated position to lower BP
Rapid assessment to identify and eliminate cause
Empty the bladder using a urinary catheter or irrigate or change indwelling catheter
Examine rectum for fecal mass
Examine skin
Examine for any other stimulus
Administer ganglionic blocking agent such as hydralazine hydrochloride (Apresoline) IV
Label chart or medical record that patient is at risk for autonomic dysreflexia
Instruct patient in prevention and management