Excretion
0.0(0)
Studied by 2 peopleCard Sorting
1/62
Earn XP
Description and Tags
Last updated 2:32 PM on 5/29/23
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
63 Terms
1
New cards
What is excretion?
the process of removing toxic waste of metabolism from the body
2
New cards
Types of excretory organs
Lungs
Liver
Kidneys
Skin
Liver
Kidneys
Skin
3
New cards
Types of metabolic waste
CO2
Nitrogenous waste--> ammonia, urea and uric acid
Bile pigments
Nitrogenous waste--> ammonia, urea and uric acid
Bile pigments
4
New cards
Vessels of the liver
Hepatic artery, hepatic vein, bile duct, hepatic portal vein
5
New cards
Role of the hepatic artery
To bring oxygenated blood to the liver from the heart via the aorta
6
New cards
Role of the hepatic vein
To carry deoxygenated blood from the liver to the heart by rejoining the vena cava
7
New cards
Role of the hepatic portal vein
To carry blood containing products of digestion from the intestines to the liver
8
New cards
Role of hepatocytes
The main liver cells which are highly metabolically active which divide and replicate.
9
New cards
Role of sinusoids
Spaces between hepatocytes where blood from the hepatic artery and portal vein mixes to increase the oxygen content of the substrate-rich blood, allowing hepatocytes to remain active.
10
New cards
Reason for mixing blood in the sinusoids
Increases the oxygen content of the blood from the hepatic portal vein
11
New cards
Role of Kupffer cells
To ingest foreign particles and help protect against disease
12
New cards
Role of canaliculi
To have bile secreted into them and carry it into the bile ductules which take it to the gall bladder
13
New cards
Role of the bile duct
To carry bile from the liver to the gall bladder so it can be stored until required to emulsify fats in the small intestine
14
New cards
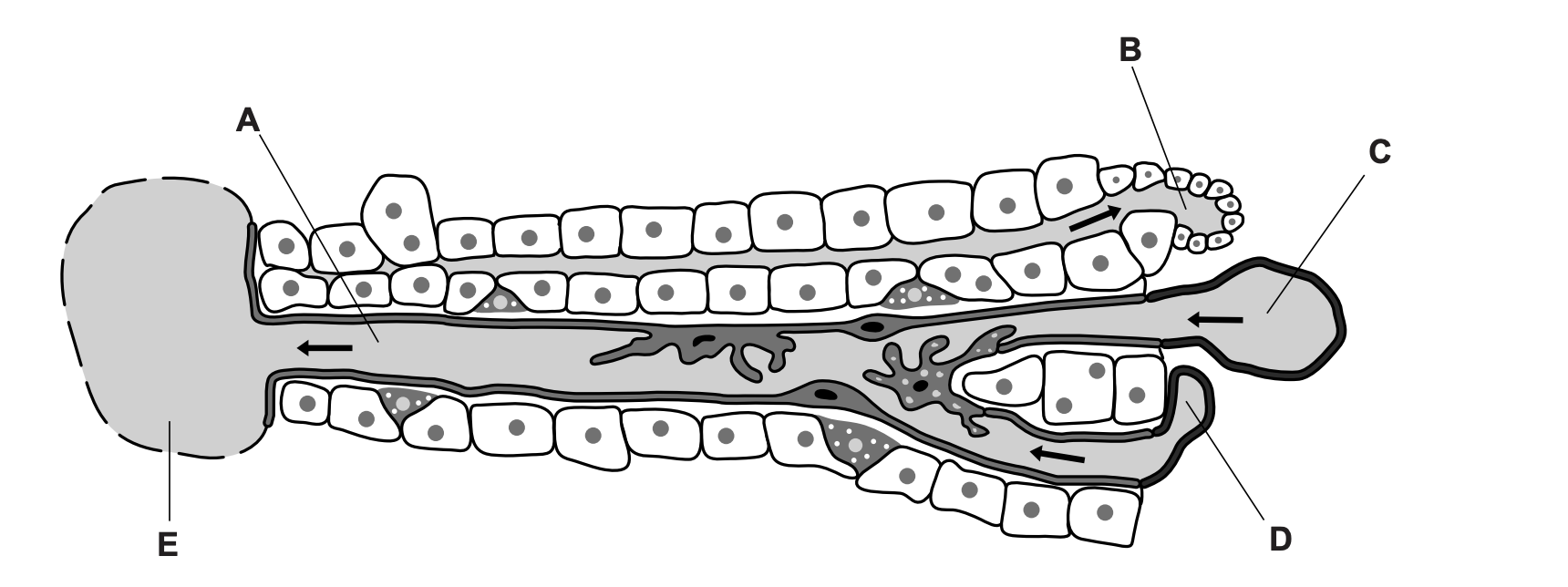
Label part A-E
A sinusoid ;
B (branch of) bile duct ;
C (branch of) hepatic portal vein ;
D (branch of) hepatic artery / arteriole ;
E (branch of) hepatic / central , vein ;
B (branch of) bile duct ;
C (branch of) hepatic portal vein ;
D (branch of) hepatic artery / arteriole ;
E (branch of) hepatic / central , vein ;
15
New cards
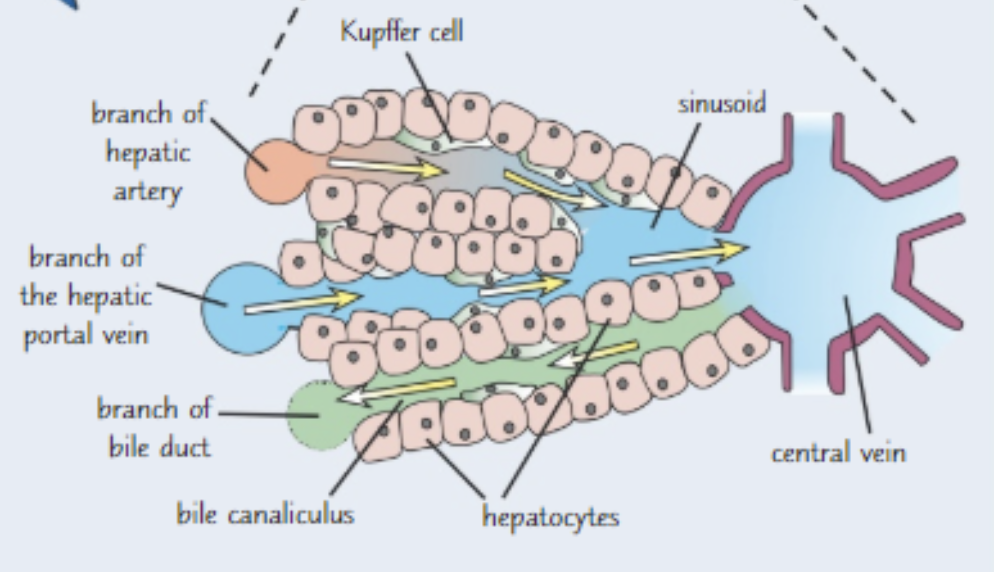
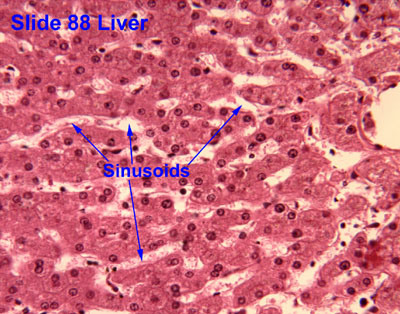
histology of liver
- Hepatocytes arranged in lobules
- Sinusoids in between hepatocytes are blood-filled spaces
- Kupffer cells phagocytize microbes & foreign matter
- Sinusoids in between hepatocytes are blood-filled spaces
- Kupffer cells phagocytize microbes & foreign matter
16
New cards
What are the 3 functions of the liver?
1. Carbohydrate metabolism (glucose storage)
2. Deamination of excess amino acids
3. Detoxification
2. Deamination of excess amino acids
3. Detoxification
17
New cards
Role of the liver in storing glycogen when blood sugar rises and drops
When blood glucose levels rise, stimulates beta cells and insulin levels rise and stimulate hepatocytes to convert glucose to glycogen for storage.
When blood sugar levels drop, stimulates alpha cells and glucagon levels rise and stimulate hepatocytes to convert glycogen into glucose for use in reactions.
When blood sugar levels drop, stimulates alpha cells and glucagon levels rise and stimulate hepatocytes to convert glycogen into glucose for use in reactions.
18
New cards
Process of deamination
\
* The amino group (-NH2) atom of an amino acid is removed, and an extra hydrogen atom
\
* NH2 and the hydrogen atom combine to form **ammonia** (**NH3**)and **keto acid**
\
* The remaining **keto acid** (a type of organic acid) may enter the **Krebs cycle** (in the mitochondria) to be **respired**, be converted to **glucose**, or converted to **glycogen or fat for storage**
\
\
\
* The amino group (-NH2) atom of an amino acid is removed, and an extra hydrogen atom
\
* NH2 and the hydrogen atom combine to form **ammonia** (**NH3**)and **keto acid**
\
* The remaining **keto acid** (a type of organic acid) may enter the **Krebs cycle** (in the mitochondria) to be **respired**, be converted to **glucose**, or converted to **glycogen or fat for storage**
\
\
\
19
New cards
\
\
20
New cards
Name for the process of making urea in deamination
Ammonia combines with CO2 to form UREA via ornithine cycle
Ammonia is converted to UREA as it's less soluble/toxic
Urea then diffuses through blood plasma via bilayer of hepatocytes and it is transported to kidneys
2NH3 + CO2------> CO(NH2)2 (urea) + H20
\
Ammonia is converted to UREA as it's less soluble/toxic
Urea then diffuses through blood plasma via bilayer of hepatocytes and it is transported to kidneys
2NH3 + CO2------> CO(NH2)2 (urea) + H20
\
21
New cards
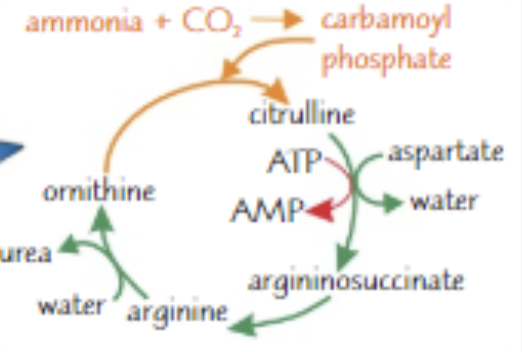
Draw the ornithine cycle
\
22
New cards
What is transamination?
Conversion of one amino acid into another
23
New cards
Lactate Metabolism
Excess lactate is absorbed by hepatocytes
Lactate is converted to pyruvate for aerobic respiration
Rest of lactate is converted to glucose for maintaining blood glucose conc
Lactate is converted to pyruvate for aerobic respiration
Rest of lactate is converted to glucose for maintaining blood glucose conc
24
New cards
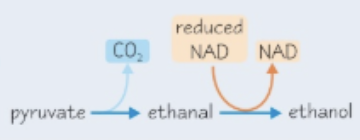
Alcohol metabolism in the liver
* The enzyme **alcohol dehydrogenase** converts **ethanol** into a molecule called **ethanal**, which is then converted into other molecules that enter respiration e.g acetic acid
25
New cards
What condition does excess alcohol cause?
cirrhosis
26
New cards
What is required for the break down of ethanol and fatty acids?
NAD
27
New cards
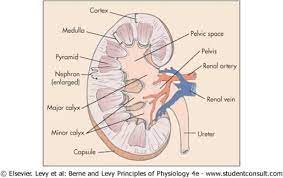
structure of kidney
cortex- contains the glomerulus, as well as the Bowman’s capsule, proximal convoluted tubule, and distal convoluted tubule of the nephrons
medulla- contains the loop of Henle and collecting duct of the nephrons
renal vein
renal artery
ureter- carries urine from the kidney to the bladder
medulla- contains the loop of Henle and collecting duct of the nephrons
renal vein
renal artery
ureter- carries urine from the kidney to the bladder
28
New cards
Role of Bowmans Capsule
Filters blood, massive pressure forcing out the liquid and anything dissolved in the liquid but red blood cells, white blood cells, platelets and proteins remain in the blood.
29
New cards
Role of cortex of kidney
high density of capillaries as it is the site of blood filtration
30
New cards
Role of medulla of kidney
nephron tubules which make the kidney pyramids and collecting ducts.
regulates urine conc
regulates urine conc
31
New cards
Role of renal vein
deoxygenated blood away from kidney
32
New cards
role of renal artery
oxygenated blood to kidney
33
New cards
Role of pelvis in kidney
collects urine before it passes down to the bladder.
34
New cards
Role of ureter
tube carrying urine from kidneys to urinary bladder
35
New cards
Why do podocytes usually don't undergo mitosis?
are differentiated / specialized
G0 (phase of cell
cycle) / resting phase
G0 (phase of cell
cycle) / resting phase
36
New cards
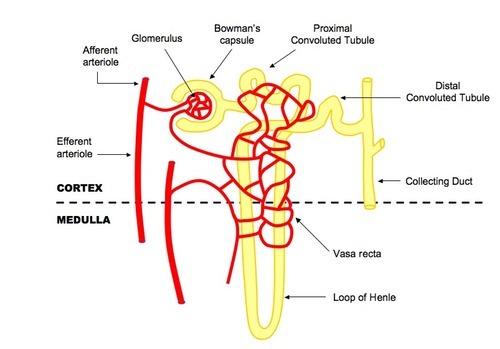
Structure of nephron
Bowerman's capsule (cup shaped structure) containing the glomerulus= ultrafiltration takes place.
Glomerulus= capillaries where pressure forces all solutes in the blood plasma to be forced through the capillary walls e.g ions, amino acids, glucose, urea, water. Proteins and erythrocytes do not pass through as they are too large.
Proximal Convoluted Tubule (PCT)= First coiled region of the tubule, where products needed in the blood (ions, glucose, amino acids etc) are reabsorbed
Loop of Henle: A long loop of tubule which spans the cortex and medulla, used to concentrate the urine. A salty environment is created in the medulla in order to cause water to osmose of water out of the nephron on the falling limb, and the impermeable rising limb
allows salts to diffuse out maintaining salty conditions.
Distal Convoluted Tubule (DCT) =Second coiled region of the tubule, where osmosis and diffusion of solutes occurs in order to fine tune the water potential and pH of the blood.
Collecting Duct= Urine travels through the collecting duct down to the pelvis. More fine tuning occurs, as ADH creates aquaporins to allow the exit of excess water.
Glomerulus= capillaries where pressure forces all solutes in the blood plasma to be forced through the capillary walls e.g ions, amino acids, glucose, urea, water. Proteins and erythrocytes do not pass through as they are too large.
Proximal Convoluted Tubule (PCT)= First coiled region of the tubule, where products needed in the blood (ions, glucose, amino acids etc) are reabsorbed
Loop of Henle: A long loop of tubule which spans the cortex and medulla, used to concentrate the urine. A salty environment is created in the medulla in order to cause water to osmose of water out of the nephron on the falling limb, and the impermeable rising limb
allows salts to diffuse out maintaining salty conditions.
Distal Convoluted Tubule (DCT) =Second coiled region of the tubule, where osmosis and diffusion of solutes occurs in order to fine tune the water potential and pH of the blood.
Collecting Duct= Urine travels through the collecting duct down to the pelvis. More fine tuning occurs, as ADH creates aquaporins to allow the exit of excess water.
37
New cards
Parts of the glomerulus that filter
Endothelial cells in the wall, basement membrane, podocytes
38
New cards
How can the glomerulus perform its function?
1. afferent arteriole has a bigger diameter than efferent arteriole
2. build up of high hydrostatic pressure
3 endothelium allow ultrafiltration ;
2. build up of high hydrostatic pressure
3 endothelium allow ultrafiltration ;
39
New cards
Formation of urine steps
ultrafiltration, reabsorption, secretion
40
New cards
Ultrafiltration
Blood enters a coiled network of vessels called the glomerulus from the afferent arteriole at high hydrostatic pressure.
Basement membrane containing endothelium cells acts as a 1st filter allows small ions like sodium, potassium, glucose, water, urea and some amino acids to be part of the filtrate whilst preventing larger products in the blood such as erythrocytes and white blood cells from being filtered.
Podocytes acts as a 2nd filter and further hydrostatic pressure forces small molecules into Bowmans capsule.
The glomerular filtrate then passes to the proximal convoluted tubule (pct) where the filtrate undergoes selective reabsorption.
Basement membrane containing endothelium cells acts as a 1st filter allows small ions like sodium, potassium, glucose, water, urea and some amino acids to be part of the filtrate whilst preventing larger products in the blood such as erythrocytes and white blood cells from being filtered.
Podocytes acts as a 2nd filter and further hydrostatic pressure forces small molecules into Bowmans capsule.
The glomerular filtrate then passes to the proximal convoluted tubule (pct) where the filtrate undergoes selective reabsorption.
41
New cards
Where does selective reabsorption occur?
proximal convoluted tubule (PCT)
42
New cards
Adaptations of proximal convoluted tubules
Microvilli to increase surface area
folded basement membrane to increase surface area mitochondria to produce ATP for active transport
folded basement membrane to increase surface area mitochondria to produce ATP for active transport
43
New cards
Selective reabsorption process
Glucose, vitamins, hormones and amino acids are selectively reabsorbed in the PCT back into the blood by active transport
\
Some Na+ ions are reabsorbed so water moves out via osmosis and is also reabsorbed.
\
This makes the filtrate more concentrated
\
Some Na+ ions are reabsorbed so water moves out via osmosis and is also reabsorbed.
\
This makes the filtrate more concentrated
44
New cards
What happens at the ascending limb, loop of henle and descending limb
1. As you move down the descending limb the filtrate gets more concentrated with Na+ and Cl-
2. At the bottom of the loop of henle the filtrate is hypertonic (very high salt concentration)
* so salt moves out by diffusion
3. As you move up the ascending limb the salt concentration of salt inside the filtrate decreases and becomes isotonic (salt conc inside and outside the filtrate is the SAME)
4. Salts move out by active transport and water stays inside the ascending limb
45
New cards
What happens at the distal convoluted tubule/collecting duct for water reabsorption when you are DEHYDRATED AND HYDRATED?
The volume of water absorbed is controlled by a hormone called anti-diuretic hormone (ADH) which increases the number of aquaporins in the cell membrane of the collecting ducts causing more water to be reabsorbed.
\
WHEN DEHYDRATED:
* more ADH released
* DCT walls become more permeable
* more water is reabsorbed
* highly concentrated urine
\
WHEN HYDRATED:
* less ADH released
* DCT walls become less permeable
* less water is reabsorbed
* very dilute urine
\
WHEN DEHYDRATED:
* more ADH released
* DCT walls become more permeable
* more water is reabsorbed
* highly concentrated urine
\
WHEN HYDRATED:
* less ADH released
* DCT walls become less permeable
* less water is reabsorbed
* very dilute urine
46
New cards
Explain how a longer loop of Henle prevents excessive water loss
More Na+ ions are pumped out of ascending limb
This builds a greater water potential gradient
This allows reabsorption of more water form the collecting duct
This builds a greater water potential gradient
This allows reabsorption of more water form the collecting duct
47
New cards
Adaptation of the loop of Henle
It's a countercurrent multiplier
48
New cards
Adaptation of the distal convoluted tubule
Lots of mitochondria in the walls for active transport
49
New cards
What is osmoregulation?
control of water and salt levels in blood
50
New cards
Role of hypothalamus in osmoregulation?
Water out of osmoreceptors causes hypothalumus to shrink
Triggers the produce ADH
Triggers the produce ADH
51
New cards
What is the role of ADH in osmoregulation
ADH increases the number of aquaporins in the cell surface membrane of collecting ducts causing the absorption of more water
Triggers the activation of cAMP second messenger
Urine becomes more concentrated
Triggers the activation of cAMP second messenger
Urine becomes more concentrated
52
New cards
Which parts of the nephron are affected by ADH?
distal convoluted tubule and collecting duct
53
New cards
How do the endocrine and nervous systems work together to increase water reabsorption from the collecting duct using aldosterone and ADH?
__**Endocrine system**__
* • hypothalamus causes the release of ADH from pituitary aldosterone released from the adrenal cortex
* • ADH released from the pituitary gland
* • ADH binds to receptors on the cell membranes of collecting duct cells …
* • … and this increases permeability to water (regulated by aquaporins)
\
__**Nervous system:**__
* • hypothalamus is part of the nervous system
* • osmoreceptors in the hypothalamus detect a low water potential in the blood
* • ADH is produced in the hypothalamus
* correct reference to negative feedback
\
__**Aldosterone:**__
* • sodium ions pumped out of collecting duct cells (into tissue fluid) (and potassium ions pumped in)
* • lowers water potential in tissue fluid
* • concentration gradient established
* • sodium ions reabsorbed from the collecting duct lumen
* • water diffuses into collecting duct cells / out of lumen via osmosis.
* • hypothalamus causes the release of ADH from pituitary aldosterone released from the adrenal cortex
* • ADH released from the pituitary gland
* • ADH binds to receptors on the cell membranes of collecting duct cells …
* • … and this increases permeability to water (regulated by aquaporins)
\
__**Nervous system:**__
* • hypothalamus is part of the nervous system
* • osmoreceptors in the hypothalamus detect a low water potential in the blood
* • ADH is produced in the hypothalamus
* correct reference to negative feedback
\
__**Aldosterone:**__
* • sodium ions pumped out of collecting duct cells (into tissue fluid) (and potassium ions pumped in)
* • lowers water potential in tissue fluid
* • concentration gradient established
* • sodium ions reabsorbed from the collecting duct lumen
* • water diffuses into collecting duct cells / out of lumen via osmosis.
54
New cards
What can cause kidney failure?
● Kidney infections cause inflammatory damage = change in glomerular filtration rate (rate at which filtrate flows through kidney).
● Kidney stones.
● Uncontrolled diabetes.
● High blood pressure damages capillaries of glomeruli = larger molecules pass into urine.
● Kidney stones.
● Uncontrolled diabetes.
● High blood pressure damages capillaries of glomeruli = larger molecules pass into urine.
55
New cards
Describe effects of kidney failure
● Build-up of toxic waste products e.g. urea causes symptoms such as vomiting.
● If kidneys cannot remove excess water from blood, fluid accumulation leads to swelling.
● Disruption to electrolyte balance can make bones more brittle or increase water retention.
● If kidneys cannot remove excess water from blood, fluid accumulation leads to swelling.
● Disruption to electrolyte balance can make bones more brittle or increase water retention.
56
New cards
What is the importance of electrolyte balance
* **Excess** **potassium ions** in the blood can lead to abdominal cramps, tiredness, muscle weakness and even paralysis
* A build-up of sodium can cause disorientation, muscle spasms, higher blood pressure and general weakness
\
* A build-up of sodium can cause disorientation, muscle spasms, higher blood pressure and general weakness
\
57
New cards
Treatments for kidney failure
renal dialysis- haemodialysis/ peritoneal (removal of toxic waste products)
kidney transplants
kidney transplants
58
New cards
How does haemodialysis work?
* A **machine** known as a **haemodialyser**, which acts as an artificial kidney
* Partially permeable dialysis membranes **separate** the patient's **blood** from the **dialysis fluid** (known as the **dialysate**)
* The blood is passed through **tubes** of **dialysis membrane**, which are surrounded by **dialysate**
* The dialysate contains substances **needed** in the blood (e.g. **glucose** and **sodium ions**) in the **right concentrations**
* As the dialysate contains a **glucose** concentration **equal** to a **normal blood sugar level**, this prevents the net movement of glucose across the membrane as **no concentration gradient** exists
* As the dialysis fluid contains a **salt** concentration **similar to the ideal blood concentration**. The fluid in the machine is **continually refreshed** so that **concentration gradients are maintained** between the dialysis fluids and the blood
* Importantly, the dialysate contains **no urea**
* This causes urea to diffuse down its concentration gradient **from the blood into the dialysate** and is eventually disposed of
* The haemodialyser is designed so that the patient's blood and the dialysate flow in **opposite directions**, creating a concentration gradient along the length of the dialyser component of the machine
* This means that each time blood circulates through the machine, some more of the urea it contains passes into the dialysate until almost all of it is removed
* The drug **heparin** is added to the blood as it is an **anticoagulant** (blood thinner) that **prevents the formation of blood clots**
* Partially permeable dialysis membranes **separate** the patient's **blood** from the **dialysis fluid** (known as the **dialysate**)
* The blood is passed through **tubes** of **dialysis membrane**, which are surrounded by **dialysate**
* The dialysate contains substances **needed** in the blood (e.g. **glucose** and **sodium ions**) in the **right concentrations**
* As the dialysate contains a **glucose** concentration **equal** to a **normal blood sugar level**, this prevents the net movement of glucose across the membrane as **no concentration gradient** exists
* As the dialysis fluid contains a **salt** concentration **similar to the ideal blood concentration**. The fluid in the machine is **continually refreshed** so that **concentration gradients are maintained** between the dialysis fluids and the blood
* Importantly, the dialysate contains **no urea**
* This causes urea to diffuse down its concentration gradient **from the blood into the dialysate** and is eventually disposed of
* The haemodialyser is designed so that the patient's blood and the dialysate flow in **opposite directions**, creating a concentration gradient along the length of the dialyser component of the machine
* This means that each time blood circulates through the machine, some more of the urea it contains passes into the dialysate until almost all of it is removed
* The drug **heparin** is added to the blood as it is an **anticoagulant** (blood thinner) that **prevents the formation of blood clots**
59
New cards
Feature of haemodialysis machines that makes them more efficient
Blood and dialysis fluid form countercurrent exchange system
60
New cards
How does peritoneal dialysis work?
* Dialysate is introduced to the **abdominal cavity** through a **catheter** (a thin tube that enters a part of the body)
* Urea, other metabolic waste products and excess substances diffuse **from the blood supply** across the abdominal lining (known as the peritoneum) **into the dialysate**
* This dialysate is then removed and replaced with more
* Urea, other metabolic waste products and excess substances diffuse **from the blood supply** across the abdominal lining (known as the peritoneum) **into the dialysate**
* This dialysate is then removed and replaced with more
61
New cards
What can urine test for?
\-ketones→
* suggests the person has diabetes mellitus
\
\-proteins→
* person's **blood pressure may be too high**
* **kidney infection** or that there is something wrong with their **blood filtration mechanism**
\-nitrate ions→
* indicate the person has a **bacterial infection** in the **urinary tract**
* suggests the person has diabetes mellitus
\
\-proteins→
* person's **blood pressure may be too high**
* **kidney infection** or that there is something wrong with their **blood filtration mechanism**
\-nitrate ions→
* indicate the person has a **bacterial infection** in the **urinary tract**
62
New cards
How can urine samples be used to test for pregnancy?
Monoclonal antibodies bind via complementary binding to HGC on the stick.
The antibodies are attached to dyes
Triggering an appearance of colour
The antibodies are attached to dyes
Triggering an appearance of colour
63
New cards
How can urine samples be used to test for drugs such as anabolic steroids?
Gas chromatography measures time for urine to pass through and the steroid to pass through