Physical Diagnosis 2: Unit 1 Material
1/179
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
180 Terms
When is an abdominal exam performed?
(1) As part of the comprehensive physical examination
(2) When patient presents with signs or symptoms of an abdominal disease process
(3) When the patient's musculoskeletal complaint could be referred from a visceral source
What is the sequence of an abdomen examination?
(1) Inspection
(2) Auscultation
(3) Percussion
(4) Palpation
Why do we do auscultation before percussion and palpation for an abdomen exam?
Percussion/palpation can cause some movement and activity of the intestines, which might change your auscultation
What is the serous membrane that lines the cavity of the abdomen and forms a protective cover for many of the abdominal structures?
Peritoneum
What constitutes the greater and lesser omentum?
Double folds of the peritoneum around the stomach
What is the fan-shaped fold of the peritoneum, which covers most of the small intestine and anchors it to the posterior abdominal wall?
Mesentery
How long is the G.I. Tract?
27-foot tube from the mouth to the anus
What are the parts of the G.I. Tract?
(1) Esophagus (10 inches long)
(2) Stomach
(3) Small Intestine (21 feet long)
(4) Large Intestine (colon; 4.5 to 5 feet long)
Functions of the Alimentary Tract (3)
(1) Ingest and digest food
(2) Absorbs nutrients, electrolytes, and water
(3) Excrete waste products
What moves food along the alimentary tract? What controls this?
Peristalsis
Controlled by the autonomic nervous system
Esophagus
— 10-inch collapsible tube
— connects the pharynx to the stomach
— posterior to the trachea
Descends through the mediastinal cavity, travels through the diaphragm and enters the stomach at the cardiac orifice
Stomach
— lies transversely in the upper abdominal cavity, just below the diaphragm
— 3 sections: fundus, body, and pylorus (most distal portion)
— secretes hydrochloric acid and digestive enzymes that break down fats (gastric lipase) and proteins (pepsin)
— little absorption takes plave
Small Intestine
— begins at the pylorus and is coiled in the abdominal cavity
— joins the large intestine at the ileocecal valve
— 3 sections: duodenum (C-shaped curve around the head of the pancreas), jejunum (gradually becomes thicker), and ileum
—
Where does the common bile duct and pancreatic duct open into?
Duodenum at the duodenal papilla
What prevents backward flow of fecal material from the large intestine into the ileum?
Ileocecal valve
Large Intestine
Aka colon
— starts at the cecum (blind pouch about 2-3 inches long)
— main function = absorb water and transport waste
— mucous glands secrete alkaline mucus
— live bacteria
What process does the bacteria use in the large intestine to decompose undigested food, unabsorbed amino acids, cell debris, and dead bacteria?
Putrefaction
Liver is composed of how many lobes?
4
Liver Functions
(1) Metabolize fats and carbohydrates
(2) Convert amino acids into glucose
(3) Synthesize fats from carbohydrates and proteins
(4) Store vitamins and iron
(5) Detoxify harmful substances
(6) Produce antibodies and blood coagulants
(7) Synthesize bile
(8) Convert waste from fat to water soluble
What is the pear-shaped, sac-like organ recessed in the liver?
Gallbladder
Functions of the gallbladder
Concentrates and stores bile (made of cholesterol, bile salts, and pigments)
Bile is released into cystic duct (joins with the hepatic duct to form the common bile duct) and maintains alkaline pH of the small intestine and permit emulsification of fats for absorption
Pancreas
— lies behind and beneath the stomach, with its head resting in the curve of the duodenum
— exocrine gland: acinar cells produce digestive enzymes
— endocrine gland: islet cells produce insulin and glucagon
Spleen
— lies above the left kidney and just below the diaphragm
— white pulp = lymphoid tissue that filters blood
— red pulp = capillary network that allows for storage and release of blood
Kidneys
— Located in the retroperitoneal space of the upper abdomen
— Extends from about T12 to L3
— right is usually slightly lower than the left (because of large liver above)
— produces renin and erythropoietin, as well as the active form of vitamin D
Vasculature in the abdomen
Abdominal portion of the descending aorta (just left of midline)
Branches:
— iliac arteries (2 - formed from division of the aorta at about the umbilicus)
— splenic artery
— renal arteries
Pancreatic buds, the liver, and the gallbladder all begin to form during what week of gestation?
Week 4
Note: intestine already exists as a single tube
What is meconium?
End product of fetal metabolism — first BM after birth (green color)
Produced at about 17 weeks
When is the gestational tract capable of adapting to extrauterine life?
By 36 to 38 weeks gestation
Elasticity, musculature, and control mechanisms reach adult levels of function by what age?
2-3 years of age
What is the size of the liver at birth?
Very large due to:
— metabolic and glycogen storage organ
— remains the heaviest organ in the body
Pancreatic islet cells are developed by what age?
12 weeks of gestation (start producing insulin)
What is the spleen very active in during fetal development and through the first year of life?
Active in blood formation
Afterward, the spleen aids in destruction of blood cells and functions as a lymphatic organ for immunological response
When does nephrogenesis begin?
During the second embryological month
When is the kidney able to produce urine?
By 12 weeks
When does development of new nephrons cease?
By 36 weeks of gestation
What happens to abdominal wall muscles during pregnancy?
Stretch and lose tone
The umbilicus flattens/protrudes and may get stretch marks as well
What happens to the abdominal organs during pregnancy? What are some effects?
Organs are displaced = affects function
— heartburn (relaxation of the lower esophageal sphincter)
— gallstones
— urinary stasis and urgency
— constipation (GI transit time slows) or flatus
— hemorrhoids (later in pregnancy)
— diminished bowel sounds
What is a line of pigmentation at the midline, that can develop during pregnancy?
Linea nigra
What happens to the functional abilities of the GI tract in the older adult?
— motility slows
— secretion and absorption may slow
— changes may impair digestive ability and may result in food intolerances in the older adult
What happens to the liver in older adults?
Liver size decreases and it loses some ability to metabolize certain drugs
May be an increase of biliary lipids resulting in the formation of gallstones
What happens to the pancreas in older adults?
No significant physiological changes
Abdomen Examination Preparation
— good light
— full exposure of abdomen
— empty bladder
— supportive pillows
— drapes
Patient positioned supine with knees flexed:
— stand on the patient's right
— observe neutral, breath hold, and half sit-up
4 Quadrants of the Abdomen
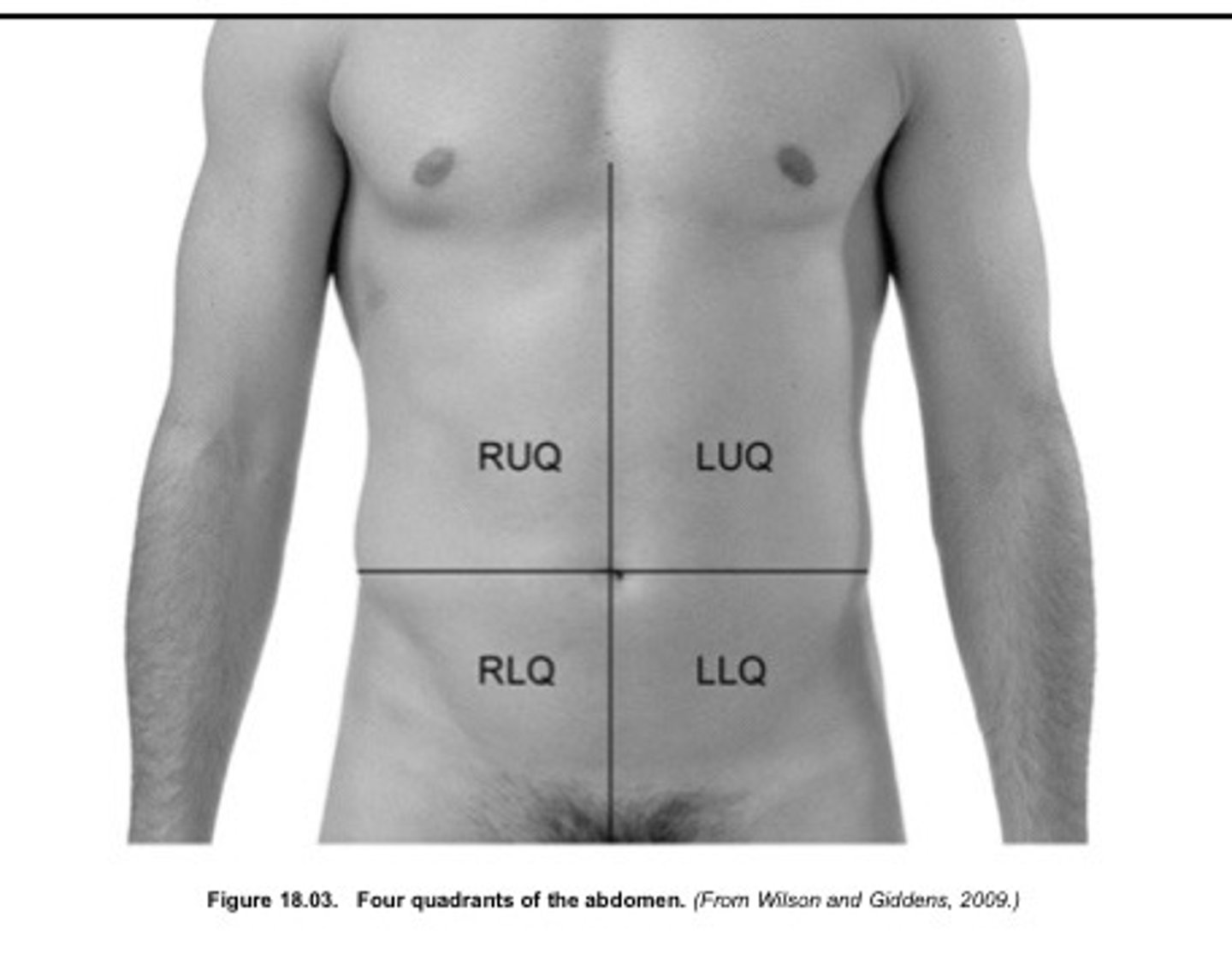
What are the lines that divides the nine regions of the abdomen?
2 Horizontal Lines:
(1) Across the lowest edge of the costal margin
(2) Across the edge of the iliac crest
2 Vertical Lines running bilaterally from the midclavicular line to the middle of the inguinal (Poupart) ligament, approximating the lateral borders of the rectus abdominis muscles
What are the 9 regions of the abdomen?
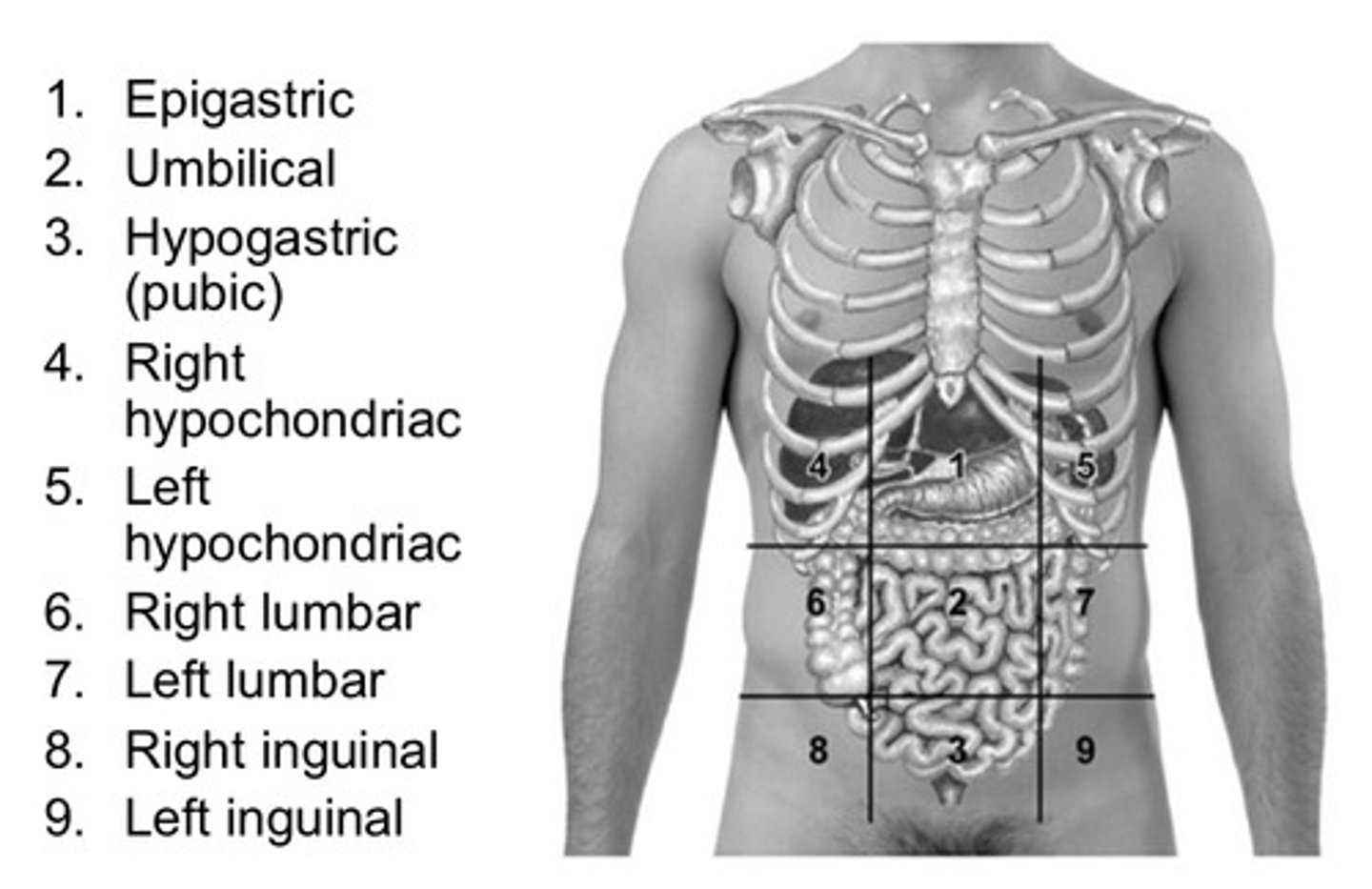
What are the 6 main structures found in the right hypochondriac region?
(1) right lobe of liver
(2) gallbladder
(3) portion of the duodenum
(4) hepatic flexure of colon
(5) portion of right kidney
(6) right adrenal gland
What are the 3 structures found in the right lumbar region?
(1) ascending colon
(2) lower half of right kidney
(3) portion of duodenum and jejunum
What are the 6 structures found in the right inguinal region?
(1) cecum
(2) appendix
(3) lower end of ilium
(4) right ureter
(5) right spermatic cord
(6) right ovary
What are the 4 structures found in the epigastric region?
(1) pylorus
(2) duodenum
(3) pancreas
(4) portion of the liver
What are the 4 structures found in the umbilical region?
(1) omentum
(2) mesentery
(3) lower part of duodenum
(4) Jejunum and ileum
What are the 3 structures found in the hypogastric (pubic) region?
(1) ileum
(2) bladder
(3) uterus (if enlarged)
What are the 6 structures in the left hypochondriac region?
(1) stomach
(2) spleen
(3) tail of pancreas
(4) splenic flexure
(5) upper pole of left kidney
(6) left adrenal gland
What are the 3 structures in the left lumbar region?
(1) descending colon
(2) lower half of the left kidney
(3) portions of the jejunum and ileum
What are the 4 structures in the left inguinal region?
(1) sigmoid colon
(2) left ureter
(3) left spermatic cord
(4) left ovary
What does a glistening, taut appearance of the abdomen suggest?
ascites
What is Cullen sign? What does it indicate?
Bluish periumbilical discoloration
Suggests intraabdominal bleeding
Striae of the abdomen
— often result form pregnancy
— new = pink or blue >> old = silvery, white color
— can also be caused by abdominal tumors or ascites
If Cushing disease, they remain a purple color
What does protrusion of the navel indicate?
Umbilical hernia
What characteristic do most hernias have?
Most are reducible = contents can be pushed back into place
What is the term for separation of the rectus abdominis muscles?
Diastasis recti
Occurs most often in pregnancy and the postpartum period (little clinical significance)
What can limited movement of the abdomen potentially indicate?
Peritonitis
What can cause marked pulsations of the abdomen?
(1) increased pulse pressure
(2) abdominal aortic aneurysms
Pulsations may be subtly noticeable in very thin patients (still palpate and double check)
What are normal bowel sounds?
Clicks and gurgles that occur irregularly and range from 5 to 35 per minute
Generalized, so most often they can be assessed adequately by listening to a few places
What is the term for loud, prolonged gurgles?
Borborygmi (stomach growling)
What can cause increased bowel sounds?
— gastroenteritis
— early intestinal obstruction
— hunger
What do high-pitched tinkling sounds suggest?
Intestinal fluid and air under pressure (as an early obstruction)
What can cause decreased bowel sounds?
— peritonitis
— paralytic ileus (intestines shut down)
Absent bowel sounds are typically associated with what?
Abdominal pain and rigidity
Absent bowel sounds = no sounds after 5 minutes of continuous listening
THIS IS A SURGICAL EMERGENCY
What are the high-pitched sounds that are heard in association with respiration?
Friction rubs
What do friction rubs indicate in the abdomen?
Indicates inflammation of the peritoneal surface of the organ from a tumor, infection, or infarct
Commonly at the liver and spleen (that's where you want to listen)
Rare in the abdomen
How do you tell the difference between a friction rub in the liver or lungs?
Need a CT scan
What are the harsh or musical intermittent auscultatory sounds that may reflect blood flow turbulence and indicate vascular disease?
Bruits
"Whooshing" sound (low-pitched)
Bruits are heard best with which part of the stethoscope?
Bell
Are bruits well-localized?
Yes — right over the artery with the issue
Where do you want to check for bruits in the abdomen?
— Epigastric region
— Aortic artery
— Renal arteries
— Iliac arteries
— Femoral arteries
Over the abdomen you should not really hear any vascular sounds at all
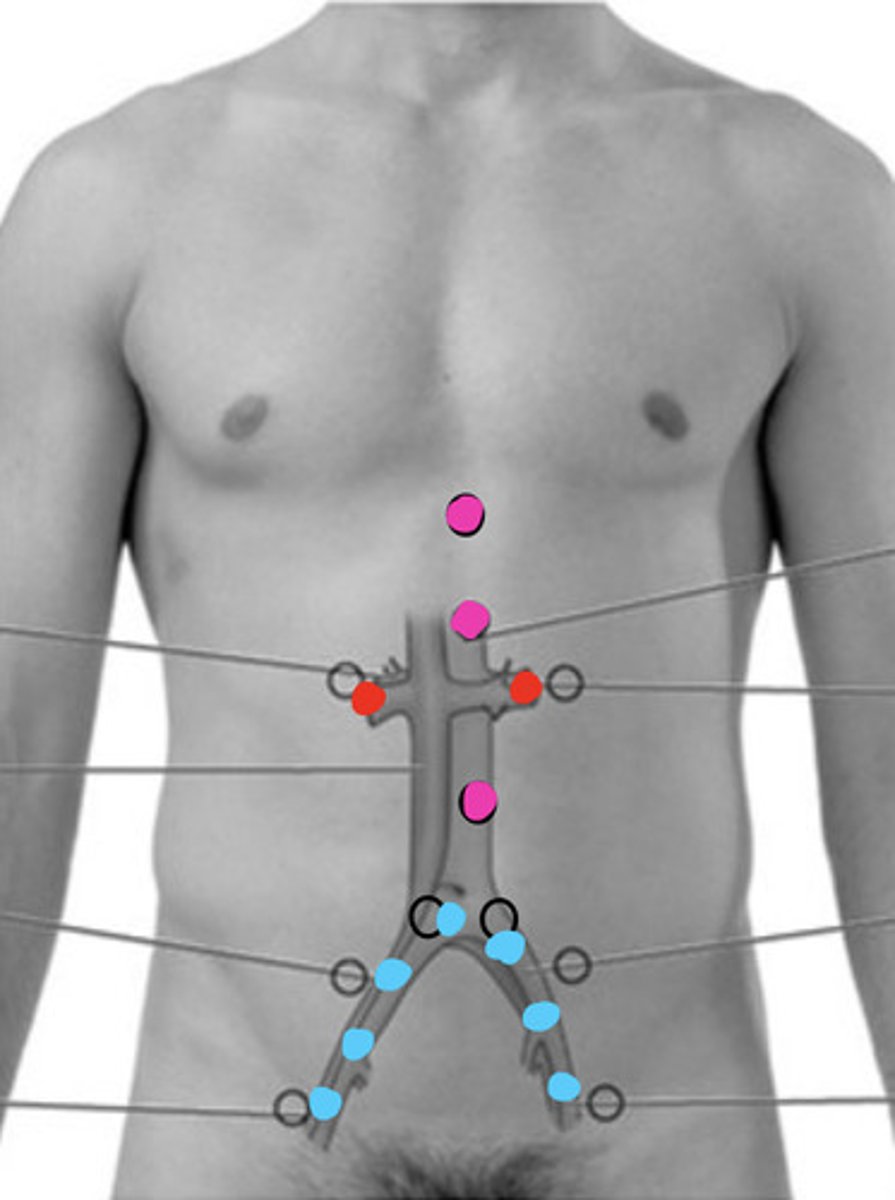
What is a soft, low-pitched and continuous sound in the abdomen heard best with the bell of the stethoscope?
Venous hum
When does a venous hum occur?
Occurs with increased collateral circulation between portal and systemic venous systems
Where do you listen to observe for a venous hum?
— epigastric region
— around the umbilicus
What is the function of percussion of the abdomen? (4)
(1) Assess the size and density of organs
(2) Detect the presence of fluid (ascites)
(3) Detect the presence of air (gastric distention)
(4) Detect the presence of fluid-filled or solid masses
Where do you need to test percussion?
All 9 regions of the abdomen to get a sense of overall tympany and dullness (2/3 spots in each region)
What is the predominant sound during percussion of a normal abdomen?
Tympany (because of air in the stomach and intestines)
You will have some dullness over organs and a distended bladder
What is the usual liver span?
Approximately 6 to 12 cm
How should the border of the liver change as the patient takes in a deep breath?
The lower border of the liver should move downward 2-3 cm
What is the usual span of the spleen?
6-9th intercostal space
What is the semilunar region that is defined by the sixth rib superiorly, the midaxillary line laterally, and the left costal margin inferiorly? What is the significance of this region?
Traube space
This area is typically tympanic because it overlies the fundus of the stomach
Provocative Percussion
Percussion with the goal to provoke pain
Also called fist percussion
NOTE: Don't do this until the very end!!
Light palpation of the abdomen
Light, systemic palpation of all nine regions
— used to identify muscular resistance and areas of tenderness
Initially, avoid any areas that have already been identified as problem spots
Moderate palpation of the abdomen
Moderate pressure as an intermediate step to gradually approach deep palpation
Deep palpation of the abdomen
Necessary to thoroughly delineate abdominal organs and to detect less obvious masses
What should you watch for during palpation of an abdominal exam?
Watch the patient's face for pain during palpation
What is the patient position for abdominal palpation?
Knees MUST be raised
How can you determine if a mass is superficial (in abdominal wall) or intraabdominal?
Have the patient lift their head from the table = abdominal muscle contraction
If the mass is in the abdominal wall, it will remain palpable
If the mass is in the abdominal cavity, it will be more difficult to feel through the contracted abdominal muscles
Palpation of the umbilical ring
Palpate the umbilical ring and around the umbilicus
— area should be free of bulges, nodules, and granulation
— umbilical ring should be round and free of irregularities (potential for herniation)
— umbilicus may be either slightly inverted or everted, but it should not protrude
What “normal” things can feel like abnormalities?
(1) kidneys (need to be pretty deep, but might feel a kidney)
(2) Fecal mass in the cecum or sigmoid colon (lower right or left of the abdomen)
(3) Uterus (really only if pregnant)
(4) Aorta (normally its pretty deep and pulses, but may be noticeable if large)
(5) Sacral promontory (again...you would need to be really deep)
(6) Bladder (sometimes if full)
What organs do you need to palpate for an abdominal exam?
(1) Liver
(2) Gallbladder
(3) Spleen
(4) Left and Right Kidneys
(5) Aorta
(6) Urinary Bladder
Is a normal spleen palpable?
No — if palpable, it is probably enlarged and there's an issue
Ascites assessment
Ascites = pathologic increase in fluid in the peritoneal cavity
Percuss for:
— dullness and resonance
— shifting dullness
— fluid wave
(1) Test for shifting dullness (compare percussion in supine and each side...the dull sound from fluid should move position when change patient position)
(2) Testing for fluid wave
Rebound Tenderness
Performed at the END of the examination to test for peritoneal inflammation
Press in with the tips of the fingertips and quickly release >> if peritoneum is inflamed, there will be a sharp pain as the fingers are pulled away and the abdomen goes back to its original position
Iliopsoas Muscle Test
Performed when you suspect appendicitis
Lift the patient's right leg and instruct the patient to hold to cause contraction of hip flexors (give some resistance if no pain originally) >> if causes pain, then positive for potential appendicitis
Obturator Muscle Test
Performed when you suspect a ruptured appendix or a pelvic abscess
While in supine, have the patient flex the leg at the hip and knee to 90 degrees >> rotate the leg laterally and medially >> pain in the right hypogastric region is a positive sign